
Understanding & Preventing Behaviour
20 evidence-based intervention techniques for children with autism — from behaviour functions and ABC data to proactive strategies and positive reinforcement. Subdomain D1 | Pinnacle Blooms Network®
Domain D: Behaviour
Subdomain D1
Evidence-Based | NCAEP 2020

The Paradigm Shift
Behaviour Is Communication
Every behaviour — including the ones that frighten, exhaust, and confuse you — is your child's brain producing the best available response to an internal state or environmental demand. The behaviour is not the problem. The behaviour is the symptom. The problem is the unmet need underneath.
The Four Functions of Behaviour
- Sensory / Automatic — produces internal sensory stimulation
- Attention — produces social attention, positive or negative
- Escape / Avoidance — removes or prevents an aversive stimulus
- Tangible / Access — produces access to a preferred item or activity
The ABC Framework
A = Antecedent — what happened BEFORE the behaviour
B = Behaviour — exactly what the child DID
C = Consequence — what happened AFTER; what did the child GET or AVOID?
Applied Behaviour Analysis (ABA) teaches us: all behaviour is functional — it serves a purpose. Identifying that purpose — the function — is the key to lasting, compassionate change.

D-341
Technique 01 of 26
Why Behaviours Happen
They're hitting. Screaming. Refusing. Running. And you ask the question every parent asks: "WHY?" Not "why is this happening TO me" — but "why is this happening FOR them?" Every behaviour has a reason. Every behaviour has a function. And once you understand the function, you have the key.
The brain doesn't produce random behaviour. Every action is a neural output in response to an input. Behaviours that worked in the past — that got a need met — are repeated. When the child hits and the demand is removed, the brain learns: hitting = escape. When the child screams and the parent comes, the brain learns: screaming = attention. The behaviour is the brain's most efficient solution to a problem, even when that solution is socially inappropriate.
Behaviour as Communication
"What is this behaviour TELLING me?" — the detective mindset: observe, record, analyse, hypothesise, test.
Why Punishment Fails
Punishment without understanding the function doesn't address the need. The behaviour returns — or escalates.
Rule Out Medical First
Always rule out pain, illness, or seizure before a behavioural explanation. Medical causes come first.
The Four Functions
Sensory, Attention, Escape, Tangible — every behaviour fits one (or more) of these four categories.
Evidence Level I — Functional Behaviour Assessment (FBA) is the gold standard. Interventions based on FBA are significantly more effective than those chosen without functional understanding. NCAEP 2020 | Cooper, Heron & Heward | BACB | PMC9978394

D-342
Technique 02 of 26
Identifying Behaviour Functions
Same behaviour. Completely different function. Child A screams in class to escape the work. Child B screams in class to get attention. Same scream — completely different intervention. If you treat both the same, you'll succeed with one and fail with the other. Function identification is everything.
The same motor output (screaming) can be driven by entirely different neural circuits depending on the reinforcer. Escape-driven screaming is amygdala-mediated. Attention-driven screaming is reward-mediated via the nucleus accumbens. Sensory-driven screaming is self-stimulatory brainstem arousal regulation. The topography is the same; the function is different — and only function-based intervention works.
The Key Question
"What does the child GET or AVOID through this behaviour?" Answer this and you have the function.
Multiple Functions
Some behaviours serve more than one function simultaneously — assessment must test each possibility carefully.
Function vs. Form
Don't treat the topography — treat the function. Function-based intervention outperforms function-blind approaches by 80%+.

D-343
Technique 03 of 26
Finding Behaviour Triggers
WHAT sets it off? The demand? The transition? The noise? The person? The time of day? The food they didn't eat? Triggers are the antecedents that predict behaviour — and finding them is the first step toward prevention. Triggers activate the amygdala (threat/mismatch detection) or the reward system (anticipation of preferred item), and the behaviour pathway fires in response.
Trigger Categories
Sensory, demand, social, transition, deprivation, physiological — each category points to a different preventive strategy.
Immediate vs. Cumulative
The "last straw" phenomenon: today's meltdown may be the result of an accumulated day of smaller stressors, not just the final trigger.
Pattern Tracking
Time, place, person, activity — a trigger tracking diary reveals patterns invisible in the heat of the moment.
Indian Daily Life Mapping
School bus, crowded home, homework time, mealtime — context-specific trigger mapping for Indian family routines.

D-344
Technique 04 of 26
ABC Data Collection
The parent's most powerful tool: a notebook and a framework. A = Antecedent (what happened before). B = Behaviour (exactly what the child did). C = Consequence (what happened after). Record 10 incidents and patterns emerge. Patterns reveal functions. Functions reveal interventions.
ABC data converts subjective experience — "they always melt down for no reason" — into objective pattern analysis. The human brain is poor at detecting behavioural patterns in real-time due to emotional involvement. Written data removes the emotional filter and reveals what is actually happening, creating the foundation for every evidence-based next step.
01
Describe Behaviour Objectively
"Hit sibling with open hand on arm" — not "was aggressive." Specificity is everything in data collection.
02
Record the Full Antecedent
Include time, place, activity, people present, last meal, last sleep — the complete picture before the behaviour.
03
Record What Child Got or Avoided
The consequence column reveals the function: did the demand stop? Did a parent appear? Was an item provided?
04
Collect Minimum 10 Data Points
Pattern recognition requires sufficient data. Share your completed ABC data with your BCBA or therapist for analysis.

D-345
Technique 05 of 26
Finding Behaviour Patterns
You've collected two weeks of ABC data. Now: what does it MEAN? Patterns emerge — behaviour happens at the same time, with the same person, during the same activity, or after the same trigger. The pattern IS the answer. Research shows 80% of behaviour becomes predictable once patterns are clearly identified and analysed.
Pattern Types to Look For
- Time-based: morning vs. afternoon, weekday vs. weekend
- Person-based: with Amma vs. Papa vs. teacher
- Activity-based: during homework vs. free play
- Sensory-state: after noisy environment vs. quiet
From Pattern to Prevention
Once a pattern is detected, prediction becomes possible — and prediction enables prevention. Your PFC (analytical brain) decodes the child's behavioural patterns most effectively with 10+ data points. Create a hypothesis from the pattern, then test it by modifying the antecedent and observing the result.

D-346
Technique 06 of 26
Sensory-Driven Behaviour
They flap. They spin. They rock. They hum. They chew everything. They crash into furniture. These behaviours happen regardless of who is present — in empty rooms, alone or in company. The behaviour produces its own reward: sensory input the nervous system craves. This is the one function that doesn't require a social mediator — making it the hardest to modify, because the reinforcement cannot be controlled by others.
Identifying Sensory Function
Ask: Does this behaviour happen with or without an audience? If yes — it's likely sensory/automatic.
Match the Sensory Input
Provide the SAME sensory experience through an acceptable channel — proprioceptive, vestibular, visual, auditory, or tactile.
Sensory Diet as Prevention
Proactive sensory input throughout the day reduces the intensity of sensory-seeking behaviour reactively.
When to Leave It Alone
If the behaviour is not harmful, it may be self-regulation. Suppressing it without meeting the need causes escalation.

D-347
Technique 07 of 26
Attention-Seeking Behaviour
They scream — and you come running. They throw a toy — and you say "Don't do that!" Every response — even a negative one — is attention. Social attention activates the reward system regardless of whether the attention is positive ("good job!") or negative ("stop that!"). For a child starved of social connection, negative attention is better than none.
The intervention is elegantly simple in principle: flood them with attention for appropriate behaviour, and strategically withhold attention for inappropriate behaviour. But implementation requires consistency across all caregivers — the technique teaches: "How do I get the people I love to notice me?"
Identify the Function
Ask: Does the behaviour STOP when no one is watching? If yes — attention is the function.
Planned Ignoring
Withhold attention for target behaviour — but ONLY when safe. Planned ignoring without replacement teaching is insufficient.
Teach Appropriate Requesting
Teach "Excuse me," a tap on the shoulder, or a visual signal — an easier, socially appropriate way to request attention.
The Attention Bank Account
Deposit more than you withdraw. Proactive positive attention throughout the day reduces attention-seeking behaviour dramatically.

D-348
Technique 08 of 26
Escape-Motivated Behaviour
Homework presented — tantrum. Teeth brushing — bolting. Getting dressed — screaming. The behaviour WORKS: the demand is withdrawn, the task is abandoned, the aversive experience stops. The child has learned: behaviour X = escape from thing I don't want to do. This is the most common function in school-age children with ASD.
Escape behaviour is negatively reinforced — the removal of an aversive stimulus strengthens the behaviour. The trap: every time you withdraw the demand after the behaviour, you strengthen it for next time. Escape extinction must always be paired with teaching a replacement — never used alone.
Demand Fading
Reduce difficulty until success is achievable, then gradually increase demands as tolerance builds.
Teach "I Need a Break"
Functional Communication Training: give them a better, acceptable way to escape — before the problem behaviour starts.
High-p Request Sequence
Easy → Easy → Easy → Hard. Build momentum with achievable requests before introducing the difficult demand.
⚠️ Critical Warning
NEVER use escape extinction without first teaching a replacement behaviour. Replacement teaching must come first.

D-349
Technique 09 of 26
Tangible-Driven Behaviour
They see the iPad. They MUST have it. NOW. Screaming begins. Escalates. Continues until the iPad is handed over. The brain has learned: intensity of behaviour = speed of access. Tangible-driven behaviour is positively reinforced — each time the item is provided after the behaviour, the behaviour-reward association strengthens.
The Escalation Trap
Giving in after 10 minutes of screaming teaches: scream for 10 minutes. The next episode will be at least 10 minutes. Avoid the trap by teaching requesting before the situation escalates.
What You'll Learn
- Teaching appropriate requesting: "I want iPad please"
- Building tolerance for "no" and "later"
- Visual schedules for preferred item access
- Distinguishing tangible function from routine function
- Delayed reinforcement and graduated access

D-350
Technique 10 of 26
Setting Events
Same demand. Same environment. Same antecedent — but TODAY they melt down and yesterday they didn't. Why? Setting events are the background conditions that increase the probability of behaviour. Poor sleep, missed meal, illness, change in routine, family stress — the invisible context that makes triggers MORE triggering.
Setting events alter the brain's baseline state. Poor sleep → elevated cortisol → lower PFC capacity → lower threshold for amygdala activation → same trigger produces bigger response. Setting events don't cause behaviour; they lower the threshold. Understanding them explains why behaviour is inconsistent across days — and why some days require a fundamentally different approach.
Sleep & Rest
The #1 setting event. Even one hour of lost sleep measurably reduces PFC regulatory capacity and increases reactivity.
Food & Hunger
Missed meals or late snacks lower blood glucose — the PFC is the first brain region to lose capacity under metabolic stress.
Illness & Pain
Subclinical pain — an earache, constipation, or headache — dramatically lowers behavioural thresholds without obvious symptoms.
Routine Disruption
Festival days, exam season, travel, family visitors — predictable Indian household disruptions that require proactive planning.

D-351
Technique 11 of 26
Sleep Affects Behaviour
They slept four hours. Today will be a war zone. Sleep deprivation is the #1 setting event for behavioural escalation — and 50–80% of children with ASD have significant sleep difficulties. Every hour of lost sleep directly reduces the PFC's regulatory capacity and increases the amygdala's reactivity — more alarm, less brake.
Melatonin production (pineal gland) is often atypical in ASD, contributing to difficulty falling asleep, staying asleep, and achieving restorative sleep cycles. The result: a chronically sleep-deprived child whose behavioural threshold is significantly lower than their well-rested potential — every single day.
Sleep Hygiene Protocol for ASD
Dark room, consistent bedtime, screen curfew 60 minutes before sleep, sensory-appropriate bedding and pyjamas.
Melatonin Guidance
Evidence supports melatonin use in ASD sleep difficulties. Discuss dosing, timing, and formulation with your NeuroDev physician.
Adjust Expectations on Poor-Sleep Days
Lower demands, increase support, reduce transitions, and plan more sensory regulation time on days following poor sleep.
Indian Household Sleep Challenges
Joint sleeping arrangements, heat, noise, and power cuts — practical strategies for real Indian home conditions.

D-352
Technique 12 of 26
Hunger Affects Behaviour
"Hangry" is real neuroscience. Blood glucose drops → PFC function drops → behavioural threshold drops. The prefrontal cortex is the most metabolically demanding brain region — consuming 20% of the body's glucose. When blood glucose falls, the PFC is the first region to lose capacity. For children with food selectivity, regular nutrition is already compromised — a missed snack or late meal tips the balance.
The Glucose-Behaviour Connection
ASD + food selectivity = chronic mild glucose instability → chronic mild PFC impairment → lower behavioural threshold every day. Meal scheduling is a behaviour intervention.
Practical Strategies
- Schedule meals and snacks every 2–3 hours for young children
- Always carry a portable snack kit of accepted foods
- Ask "When did they last eat?" before any behavioural analysis
- Consider Indian meal timing: late dinners, school tiffin adequacy
- Lower demands and expectations around mealtimes

D-353
Technique 13 of 26
⚠️ THE MOST IMPORTANT BEHAVIOUR CARD: Sudden behaviour change — especially self-injury, head-banging, or aggression with no environmental trigger — may indicate PAIN. Medical evaluation must come first.
Pain Causes Behaviour
Sudden behaviour change — especially self-injury, head-banging, aggression, or screaming with NO identifiable environmental trigger — may indicate PAIN. Ear infections. Toothaches. Constipation (extremely common in ASD). Reflux. Headaches. The child who cannot communicate pain expresses it through behaviour.
Pain activates the insular cortex and anterior cingulate cortex. When the child cannot verbalize pain, the distress signal routes through the only available output: behaviour. Self-injury near the pain site — head-hitting for ear infection, face-slapping for toothache, stomach-pressing for constipation — is a critical diagnostic clue that every caregiver must know.
⚠️ Rule 1: Medical First
Sudden behaviour change = medical evaluation BEFORE behavioural intervention. Always. No exceptions.
Pain Indicators in Non-Verbal Children
Changes in eating, sleeping, posture, self-injury location, facial grimacing — learn to read pain without words.
Common Hidden Pain in ASD
Constipation, dental pain, ear infections, reflux, and headaches are frequently under-identified in non-verbal children.
Teaching Pain Communication
"I hurt" + body part pointing on a body map chart — functional communication training for pain expression.

D-354
Technique 14 of 26
Environment Modifications
Change the environment, not the child. If the classroom is too loud, add noise-reduction. If visual clutter triggers dysregulation, simplify the space. If the demand is too high, reduce it. Environmental modification is the most under-utilised and most effective behaviour prevention strategy available — because it addresses the antecedent before the behaviour begins.
Modifying the environment modifies the antecedent → reduces the trigger → reduces the behaviour. Proactive strategies are 3–5x more effective than reactive strategies — and environmental modification is the most proactive tool you have.
Sensory Modifications
Lighting adjustments, noise-reduction, seating options, visual simplification — targeted sensory-environment changes.
Demand Modification
Reduce quantity, increase support, offer choices — match environmental demands to the child's current regulatory capacity.
Indian Home Modifications
A budget guide (₹) for practical, accessible environmental modifications in Indian homes and classrooms.
Classroom Accommodation Letter
A ready-to-use template to request evidence-based environmental accommodations from your child's school.

D-355
Technique 15 of 26
Preventing Behaviour Problems
The best intervention happens before the behaviour. Prevention means: triggers identified + setting events managed + environment modified + replacement skills taught + schedule predictable + sensory needs met. When prevention works, the behaviour never occurs — and that is always the best outcome.
Prevention keeps the PFC online by reducing the total demand on the regulation system below the threshold. Below threshold = PFC manages = no behaviour. Above threshold = amygdala takes over = behaviour. Prevention is about staying below the threshold — every minute of every day.
Prevention Checklist
Sensory needs, schedule, transitions prepared, snack/sleep adequate, demands matched to ability, reinforcement accessible.
Daily Prevention Routine
A consistent morning-to-night prevention protocol that reduces cumulative stress and maintains regulatory capacity.
Prevention Plan Template
"Behaviour Prevention Plan" template for home and school — shareable with all caregivers and team members.
The 80/20 Rule
Prevention is 80% of effective behaviour management. Reactive strategies — however well-designed — are only 20%.

D-356
Technique 16 of 26
Proactive Strategies
Prevention in practice: eight specific, actionable proactive strategies that keep the brain's regulation system below the behaviour threshold. Each strategy reduces uncertainty (ACC activation), increases predictability, or lowers arousal (parasympathetic activation). Together, they create a system of support that makes challenging behaviour less likely before it ever begins.
Visual Schedule
The #1 proactive strategy — reduces uncertainty, increases predictability, and supports independent transitions throughout the day.
First-Then Boards
Visual contingency support for demand situations: "First homework, then iPad" — makes expectations concrete and manageable.
Transition Warnings
5-minute, 2-minute, and 1-minute countdowns — using visual timers — to prepare the brain for an upcoming change.
Priming & Pre-Teaching
Preview the day or activity before it begins. Familiarity reduces amygdala threat detection and supports smooth engagement.
Choice-Making
Increases perceived control, reducing escape-motivated behaviour in demand situations.
High-p Request Sequence
Easy → Easy → Easy → Hard: build momentum before introducing the challenging demand.
Environmental Arrangement
Set the physical space to support success — before the child enters it.

D-357
Technique 17 of 26
Replacement Behaviours
The golden rule of behaviour change: NEVER remove a behaviour without giving a better one. If the child screams for attention → teach them to tap your shoulder. If they hit to escape → teach them to say "break please." The replacement must serve the same function as the problem behaviour — but through an acceptable channel.
Replacement behaviours must be: easier to perform than the problem behaviour, produce the same consequence (same function met), and be reinforced more reliably. The brain switches to the replacement only if it's a better deal — less effort for the same or better reward. If the replacement is harder or less effective, the brain stays with the original.
1
Function Match
Select a replacement that meets the exact same function as the problem behaviour — not just a convenient alternative.
2
FCT Teaching
Functional Communication Training — the #1 replacement behaviour strategy, backed by the strongest Level I evidence.
3
Immediate Reinforcement
Reinforce the replacement immediately and consistently — every single time, especially in the early stages of teaching.
4
Fade Support Over Time
Gradually reduce prompting and reinforcement density as the replacement behaviour becomes fluent and independent.

D-358
Technique 18 of 26
Positive Reinforcement
Catch them being GOOD. The most powerful behaviour change tool in existence: when they do something right, make sure something good happens. Positive reinforcement increases the probability of behaviour recurring — it is not bribery, it is neuroscience. And it is the foundation of every ethical, modern behaviour intervention.
Positive reinforcement activates the dopamine-mediated reward pathway — ventral tegmental area → nucleus accumbens → PFC. Each reinforced behaviour strengthens the neural pathway, increasing the probability of that behaviour recurring. Reinforcement literally builds neural connections — it is the mechanism of learning itself.
Find Effective Reinforcers
Not all children are motivated by the same things. Conduct a reinforcer assessment — preferred activities, sensory rewards, social connection — to find what truly motivates YOUR child.
Timing Is Everything
Reinforce IMMEDIATELY after the desired behaviour — within 1–3 seconds. Delayed reinforcement loses its association with the target behaviour and reduces effectiveness dramatically.
Token Systems & Reward Charts
Visual reinforcement systems that bridge the gap between behaviour and reward — making the contingency visible and motivating.
Avoid Reinforcer Satiation
Rotate reinforcers to maintain their power. What works today may lose effectiveness — build a varied reinforcer menu.

D-359
Technique 19 of 26
Consistent Responses
Amma says no. Papa says yes. Teacher ignores it. Grandma gives in. The child receives four different responses to the same behaviour — and the brain learns: keep trying different people until someone gives me what I want. Inconsistency is the #1 saboteur of any behaviour intervention. Indian joint families — with multiple caregivers, each with different rules and emotional responses — are consistency's greatest challenge.
Inconsistent reinforcement creates an intermittent reinforcement schedule — the most resistant-to-extinction schedule in all of behavioural science. If the child succeeds even 1 in 10 times, the brain learns: persist. Consistency means the same behaviour produces the same consequence, from ALL caregivers, in ALL environments, EVERY time.
Family Consistency Meeting
Bring ALL caregivers together — Amma, Papa, Nani, Dadi, older siblings — to agree on one shared response plan before implementation begins.
Written Behaviour Plan
A simple, visible written plan shared with everyone who cares for the child — including school staff and extended family members.
The 80% Rule
80% consistency is the minimum threshold for behaviour change. Below this level, the intervention will not produce reliable results — even a well-designed one.
School-Home Consistency
Align home and school responses using a shared communication system — consistent consequences across all environments maximise progress.

D-360
Technique 20 of 26
Teaching What TO Do
The capstone of Subdomain D1. The entire paradigm shift condensed into one principle: STOP telling them what NOT to do. START teaching them what TO do. "Don't run" → "Walk." "Stop screaming" → "Use your words." "Don't hit" → "Hands on your lap." The brain cannot efficiently process a negative instruction — it must first process the forbidden action, then inhibit it, then generate an alternative.
Positive instruction activates a single motor plan. Negative instruction requires four neural computations. For a brain with limited processing capacity, the choice is clear. Tell them what you WANT, not what you don't want — and show them how to do it before the situation arises.
"Do" Language
Replace "Don't" with "Do." 10 most common negative instructions reframed positively — immediate, actionable language shifts.
Visual "Do" Cards
Picture cards showing the desired behaviour — not the problem behaviour — posted in the environments where they're needed most.
Pre-Teaching
Teach the desired behaviour BEFORE the problem situation occurs. Practice in calm moments — not in the middle of a crisis.
The Philosophy
Assume they WANT to do the right thing — and SHOW them how. Children with ASD don't lack motivation; they often lack the map.
9 Canon Materials:Visual Schedule · Social Stories · First-Then Board · Reward Charts · Communication Board · Calm-Down Kit · Emotion Cards · Visual Timer · Video Modeling
Lead:📋 ABA (BCBA) · 🧠 Psychology | SpEd · SLP · OT · NeuroDev

D-361
Technique 21 of 26
Extinction Procedures
The behaviour has been working for years. Screaming gets the iPad. Hitting ends the demand. Crying brings Amma running. Extinction means: the behaviour no longer produces the consequence it has always produced. The reinforcer is withheld — consistently, every time — until the brain learns the behaviour is no longer effective.
Critical warning: before extinction begins, expect an extinction burst — behaviour gets WORSE before it gets better. Louder. More intense. More frequent. This is the brain escalating because the old strategy isn't working. If you give in during the burst, you've reinforced the most extreme version of the behaviour. Extinction only works when paired with a replacement behaviour that meets the same function.
"Extinction Burst"
Behaviour intensifies before it decreases. Prepare for it. Plan for it. Do NOT give in during it — giving in teaches the brain to escalate further.
"Function-Matched Extinction"
Withhold only the specific reinforcer maintaining the behaviour. Attention-maintained: ignore. Escape-maintained: don't remove the demand.
"Planned Ignoring"
For attention-maintained behaviour: no eye contact, no verbal response, no physical reaction. Neutral face. Consistent. Every adult in the environment.
"Never Use Alone"
Extinction without a replacement behaviour is incomplete and potentially harmful. Always pair with FCT or another function-matched replacement.
9 Canon Materials:Visual Schedule · Social Stories · First-Then Board · Reward Charts · Communication Board · Calm-Down Kit · Emotion Cards · Visual Timer · Video Modeling
Lead:📋 ABA (BCBA) · 🧠 Psychology | SpEd · SLP · OT · NeuroDev
D-362
Technique 22 of 26
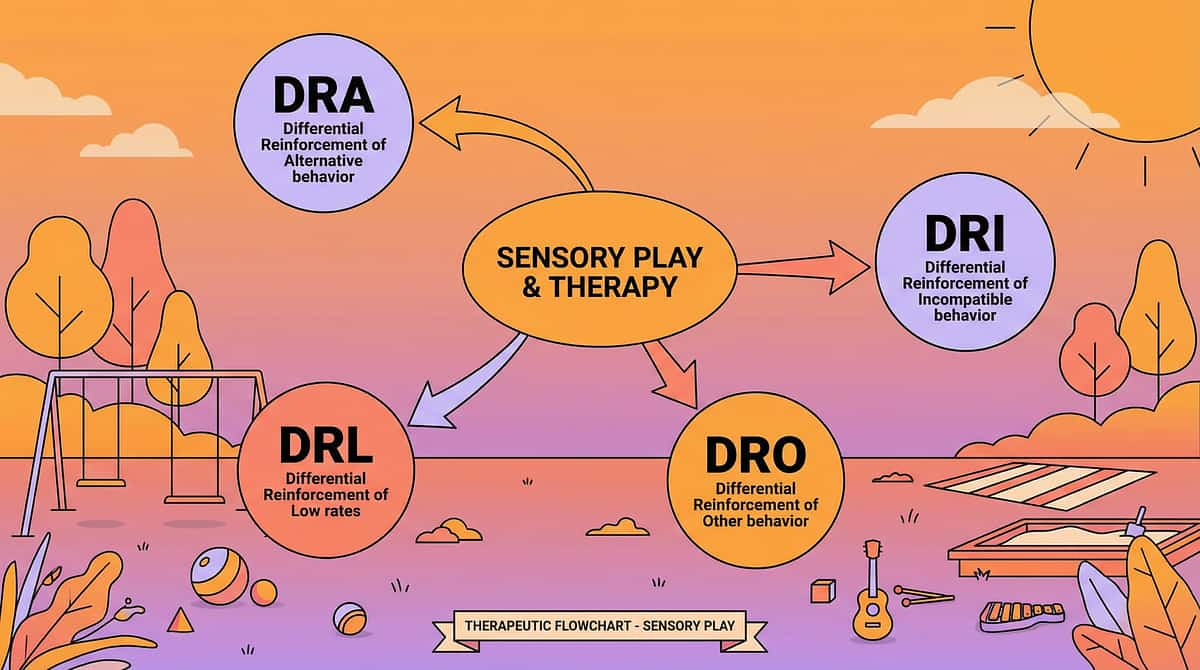
Differential Reinforcement
You can't just stop reinforcing the problem behaviour — you need to actively reinforce the RIGHT behaviour at the same time. Differential Reinforcement is the science of reinforcing what you WANT while withholding reinforcement for what you don't want. It's the engine behind every successful behaviour change plan.
Four types, each matched to a different goal: DRA (Differential Reinforcement of Alternative behaviour) — reinforce the replacement. DRI (Differential Reinforcement of Incompatible behaviour) — reinforce a behaviour that physically cannot occur at the same time as the problem behaviour. DRO (Differential Reinforcement of Other behaviour) — reinforce the absence of the problem behaviour for a set time period. DRL (Differential Reinforcement of Lower rates) — reinforce when the behaviour occurs less frequently than a set criterion.
1
DRA
Reinforce the alternative. Child asks for break instead of hitting → immediately reinforce the asking. The replacement gets better and better.
2
DRI
Reinforce the incompatible. Child can't run AND sit simultaneously. Reinforce sitting → running decreases without ever addressing it directly.
3
DRO
Reinforce the absence. Set a timer: if the behaviour does NOT occur in 5 minutes → reinforce. Gradually extend the interval.
4
DRL
Reinforce lower rates. Behaviour is acceptable at low frequency but problematic when excessive. Reinforce when it stays below the threshold.
9 Canon Materials:Visual Schedule · Social Stories · First-Then Board · Reward Charts · Communication Board · Calm-Down Kit · Emotion Cards · Visual Timer · Video Modeling
Lead:📋 ABA (BCBA) · 🧠 Psychology | SpEd · SLP · OT · NeuroDev

D-363
Technique 23 of 26
Token Economy Systems
Immediate reinforcement is powerful — but life doesn't always allow it. Token economies bridge the gap: the child earns a token (star, sticker, chip, point) immediately after the desired behaviour, and exchanges tokens for a preferred reward later. The token becomes a conditioned reinforcer — it predicts the reward, and the brain responds to it as if it were the reward itself.
Token economies are among the most researched and replicated behaviour support tools in ABA. They work across ages, settings, and behaviour targets. They teach delayed gratification — a critical executive function skill. They make reinforcement visible, predictable, and motivating. And they give the child a sense of agency: I earned this. I chose this reward. I am in control of my outcomes.
Design the Board
Choose tokens the child finds motivating (stars, stickers, chip, point, characters). Set the exchange rate: how many tokens = how big a reward. Start small — 3 tokens for a preferred activity.
Define Target Behaviours
Be specific. Not "be good" — but "sit at the table for 5 minutes," "use words to ask," "complete one worksheet." Measurable. Observable. Achievable.
Deliver Tokens Immediately
Token must follow the behaviour within seconds. Pair with specific verbal praise: "You asked nicely — here's your star!" The pairing builds the token's value.
Honour the Exchange
When the child earns the reward, deliver it immediately and enthusiastically. The system only works if the child trusts it completely.
9 Canon Materials:Visual Schedule · Social Stories · First-Then Board · Reward Charts · Communication Board · Calm-Down Kit · Emotion Cards · Visual Timer · Video Modeling
Lead:📋 ABA (BCBA) · 🧠 Psychology | SpEd · SLP · OT · NeuroDev

D-364
Technique 24 of 26
Crisis & De-escalation
The meltdown has started. The window for prevention has closed. Now the only goal is safety — theirs and yours. Crisis de-escalation is not about stopping the behaviour. It's about reducing arousal, maintaining connection, and keeping everyone safe until the nervous system can regulate itself back to baseline.
The escalation cycle has five stages: Calm → Trigger → Agitation → Acceleration → Peak → De-escalation → Recovery. Most parents intervene at Peak — the worst possible moment. Effective crisis response begins at Agitation, before the behaviour reaches its peak. Recognise the early warning signs. Reduce demands. Reduce stimulation. Increase safety. And then — wait.
"Reduce Demands Immediately"
At agitation stage: remove all non-essential demands. This is not giving in — this is strategic de-escalation. The demand can return after regulation.
"Lower Stimulation"
Dim lights. Reduce noise. Create physical space. Move to a calmer environment if possible. The nervous system cannot regulate in a high-stimulation environment.
"Stay Regulated Yourself"
Your nervous system co-regulates theirs. If you escalate, they escalate. Slow your breathing. Lower your voice. Soften your body language. Be the calm.
"Post-Crisis Debrief"
After full recovery (not during): reconnect warmly, review what happened, and plan for next time. Never debrief during or immediately after the peak.
9 Canon Materials:Visual Schedule · Social Stories · First-Then Board · Reward Charts · Communication Board · Calm-Down Kit · Emotion Cards · Visual Timer · Video Modeling
Lead:📋 ABA (BCBA) · 🧠 Psychology | SpEd · SLP · OT · NeuroDev

D-365
Technique 25 of 26
Generalisation of Behaviour
They do it perfectly in therapy. They do it perfectly at home with you. And then — at school, at the mall, at Nani's house — it's like the skill never existed. This is the generalisation problem: skills learned in one setting, with one person, using one set of materials, don't automatically transfer. Generalisation must be deliberately taught.
The science of generalisation has three dimensions: Across settings (home, school, community), across people (Amma, Appa, teacher, grandparent), and across materials (different toys, different worksheets, different environments). A skill is not truly learned until it generalises across all three. Every behaviour support plan must include a deliberate generalisation strategy — or the gains will remain trapped in the therapy room.
Train Loosely
Vary the materials, instructions, and settings from the very beginning of teaching. Don't wait until the skill is "perfect" in one context before introducing variation.
Multiple Exemplars
Teach with many different examples of the same concept. Not one red ball — many red objects. Not one "please" situation — many different request contexts.
Natural Environment Teaching
Move practice into real-life settings as early as possible. The supermarket, the park, the classroom — where the skill actually needs to work.
Involve All Adults
Every caregiver, teacher, and family member must use the same language, the same prompts, and the same reinforcement. Inconsistency kills generalisation.
9 Canon Materials:Visual Schedule · Social Stories · First-Then Board · Reward Charts · Communication Board · Calm-Down Kit · Emotion Cards · Visual Timer · Video Modeling
Lead:📋 ABA (BCBA) · 🧠 Psychology | SpEd · SLP · OT · NeuroDev

D-366
Technique 26 of 26
Building a Behaviour Support Plan
Every technique in this subdomain is a tool. A Behaviour Support Plan (BSP) is the blueprint that puts all the tools together into a coherent, coordinated system. Without a plan, interventions are reactive, inconsistent, and short-lived. With a plan, every adult in the child's life is working from the same map — in the same direction — toward the same goals.
A complete BSP has six components: (1) Behaviour definition — precise, observable, measurable. (2) Functional Behaviour Assessment — the WHY behind the behaviour. (3) Antecedent strategies — what to change BEFORE the behaviour. (4) Teaching strategies — what replacement behaviour to teach. (5) Consequence strategies — how to respond when the behaviour occurs and when it doesn't. (6) Data collection plan — how to measure progress and know when to adjust.
"Start with the FBA"
No BSP without a Functional Behaviour Assessment. The function drives every other component. Guessing the function = guessing the intervention.
"Write It Down"
A verbal agreement is not a plan. A written BSP ensures consistency across all caregivers, settings, and time. It also creates accountability.
"Review Monthly"
Behaviour changes. The plan must change with it. Schedule monthly data reviews and update the plan based on what the data shows — not what you feel.
"Team Approach"
The BSP is built and implemented by a team: BCBA, parents, teachers, therapists. No single person can carry it alone. Shared ownership = shared success.
9 Canon Materials:Visual Schedule · Social Stories · First-Then Board · Reward Charts · Communication Board · Calm-Down Kit · Emotion Cards · Visual Timer · Video Modeling
Lead:📋 ABA (BCBA) · 🧠 Psychology | SpEd · SLP · OT · NeuroDev
Subdomain D1
Full Technique Index
All 26 Techniques at a Glance
Every one of the 26 techniques in Subdomain D1: Understanding & Preventing Behaviour — evidence-based, function-focused, and designed for real families navigating real challenges. Each technique links to 9 therapy materials and a full 40-card deep-dive guide.
D-341: Why Behaviours Happen
The foundation — behaviour as communication, the four functions, and the detective mindset.
D-342: Identifying Behaviour Functions
Same behaviour, different function — why function identification changes everything.
D-343: Finding Behaviour Triggers
Antecedent analysis — trigger categories, pattern tracking, and Indian daily life mapping.
D-344: ABC Data Collection
The parent's most powerful tool — recording antecedents, behaviours, and consequences systematically.
D-345
Behaviour Patterns
D-346
Sensory-Driven Behaviour
D-347
Attention-Seeking
D-348
Escape-Motivated
D-349
Tangible-Driven
D-350
Setting Events
D-351
Sleep & Behaviour
D-352
Hunger & Behaviour
D-353
Pain Causes Behaviour
D-354
Environment Modifications
D-355
Preventing Behaviour
D-356
Proactive Strategies
D-357
Replacement Behaviours
D-358
Positive Reinforcement
D-359
Consistent Responses
D-360
Teaching What TO Do
D-361
Extinction Procedures
D-362
Differential Reinforcement
D-363
Token Economy Systems
D-364
Crisis & De-escalation
D-365
Generalisation of Behaviour
D-366
Building a Behaviour Support Plan
Preview of understanding preventing behaviour Therapy Material
Below is a visual preview of understanding preventing behaviour therapy material. The pages shown help educators, therapists, and caregivers understand the structure and content of the resource before use. Materials should be used under appropriate professional guidance.
Share this resource
Help others discover thisLink copied!
Pinnacle Blooms Network®
Ready to Go Deeper?
Each of the 20 techniques in this subdomain has a full 40-card deep-dive guide with implementation steps, printable materials, video supports, and culturally adapted Indian family strategies. Our GPT-OS® platform delivers personalised guidance for your child's specific behaviour profile — available 24/7.
Get Professional Support
Our BCBA, psychology, OT, SLP, and NeuroDev team is available for functional behaviour assessments and individualised behaviour support plans. 21M+ therapy sessions delivered.
Explore More of Domain D
Subdomain D1 is the foundation. Continue your journey with D2: Specific Behaviours, and explore all domains in the Pinnacle Blooms intervention framework.
Breadcrumb:Home → Behaviour (Domain D) → Understanding & Preventing Behaviour (D1) | Evidence Base: NCAEP 2020 | Cooper, Heron & Heward | BACB Ethics Code | PMC9978394 | WHO NCF 2018