
Independence Isn't a Luxury. It's the Destination.
Your child CAN learn to eat, dress, toilet, and stay safe — with the right protocol at the right time. The mealtimes that last 90 minutes and end in tears. The diapers at age 6 that no one talks about. The inability to button a shirt, brush teeth, or recognize that a stove is hot. These aren't just inconveniences — they're the barriers between your child and the independent, dignified life they deserve.
You are about to access 110+ clinically validated daily living skills intervention techniques — each designed for home implementation, evidence-graded, and developed by the world's largest pediatric therapy consortium. 🏥 Pinnacle Blooms Network® — India's #1 Autism & Child Development Therapy Chain | 🌍 70+ Centers | 21 Million+ Therapy Sessions | 97%+ Measured Improvement | Families from 70+ Countries

You Are Not Alone — The Numbers Speak
Across India and the world, millions of families navigate the same daily challenges. These numbers reflect real children — and real hope when the right interventions are in place.
70%+
Feeding Difficulties
of children with ASD have clinically significant feeding difficulties — including food refusal, texture aversions, and restricted diets. Source: JAMA Pediatrics, 2023
50%+
Delayed Toilet Training
achieve toilet training 1–3 years later than neurotypical peers, creating significant caregiver burden and social participation barriers. Source: Journal of Pediatric Psychology, 2022
60%+
Dressing Challenges
require daily assistance with dressing and grooming beyond the expected developmental age, limiting school readiness and independence. Source: Adaptive Behavior Research, 2021
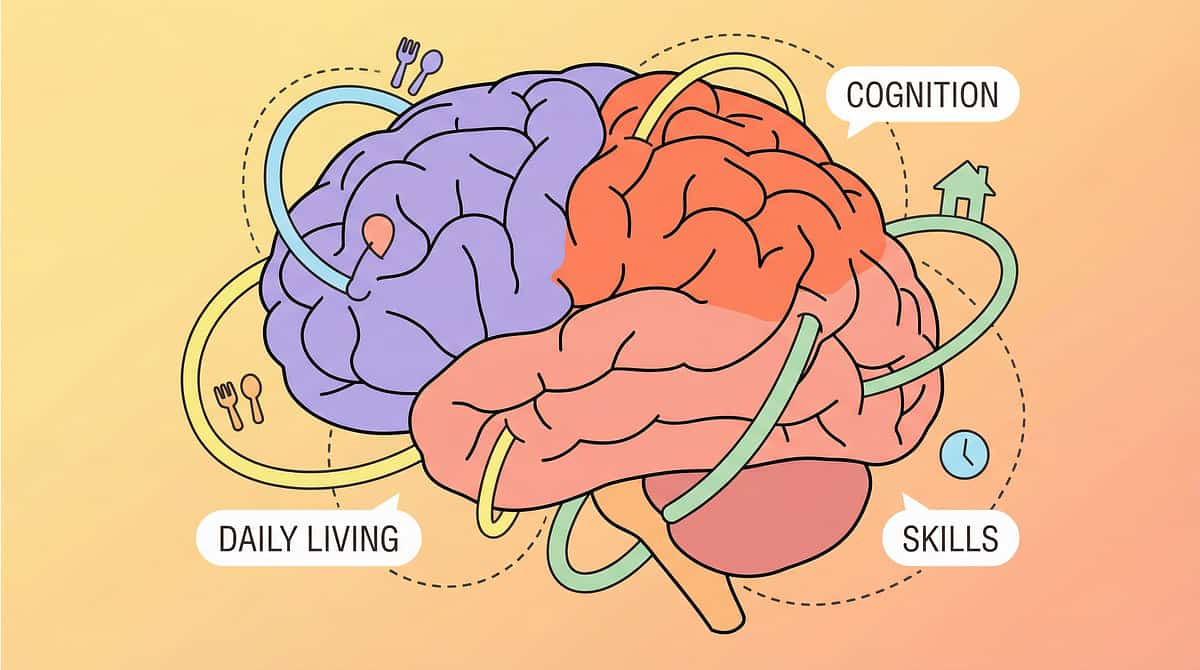
The Independence Brain — Decoded for Parents
Daily living skills are not simple tasks. They require the simultaneous coordination of multiple brain systems — and when any one of those systems is disrupted, the entire skill can break down. Understanding this is the first step to effective intervention.
Motor Planning
The premotor cortex sequences complex multi-step actions. Undoing a button requires 12+ micro-steps in exact order. When motor planning is disrupted (dyspraxia), tasks that look simple become neurologically complex.
Sensory Processing
The somatosensory cortex and insula manage feeding's oral motor demands, taste/texture tolerance, and hunger recognition. Toileting demands interoceptive awareness — detecting internal bladder and bowel signals in real time.
Executive Function
The prefrontal cortex governs task initiation, sequencing, working memory, and completion monitoring. A child may know HOW to brush teeth but lack the executive function to start, sequence, and complete the process without external scaffolding.
Memory Systems
The hippocampus and basal ganglia encode routines into procedural memory through consistent repetition. The basal ganglia transforms effortful tasks into automatic habits — but requires structured, repeated practice to do so.
Evidence: PMC9978394 | Occupational therapy motor planning research | ASHA feeding guidelines
Clinically Validated. Globally Recognized. Home-Applicable.
Level I Evidence
The Strongest Evidence Base
Task analysis, visual supports, video modeling, and systematic instruction are classified as evidence-based practices for daily living skill development (NCAEP, 2020). Behavioral toilet training protocols have robust RCT support across multiple systematic reviews. Feeding interventions combining SLP oral motor approaches with ABA behavioral strategies show the strongest outcomes for children with ASD.
WHO/UNICEF Alignment
The Nurturing Care Framework identifies responsive feeding, hygiene, and safety as core components of nurturing care. The Care for Child Development (CCD) package provides caregiver-implemented daily living skill protocols used across 54 countries — making this approach globally validated.
Parent-Implemented
Parents trained in task analysis and visual support systems achieve daily living skill outcomes comparable to therapist-implemented programs, with the added advantage of naturalistic practice across every daily routine — morning, mealtime, bath, and bedtime.
References
- NCAEP 2020 — Evidence-Based Practices Report
- ASHA Feeding & Swallowing Guidelines
- PMC9978394 — WHO CCD Package
- WHO Nurturing Care Framework 2018
- Cochrane Review: Toilet Training Interventions
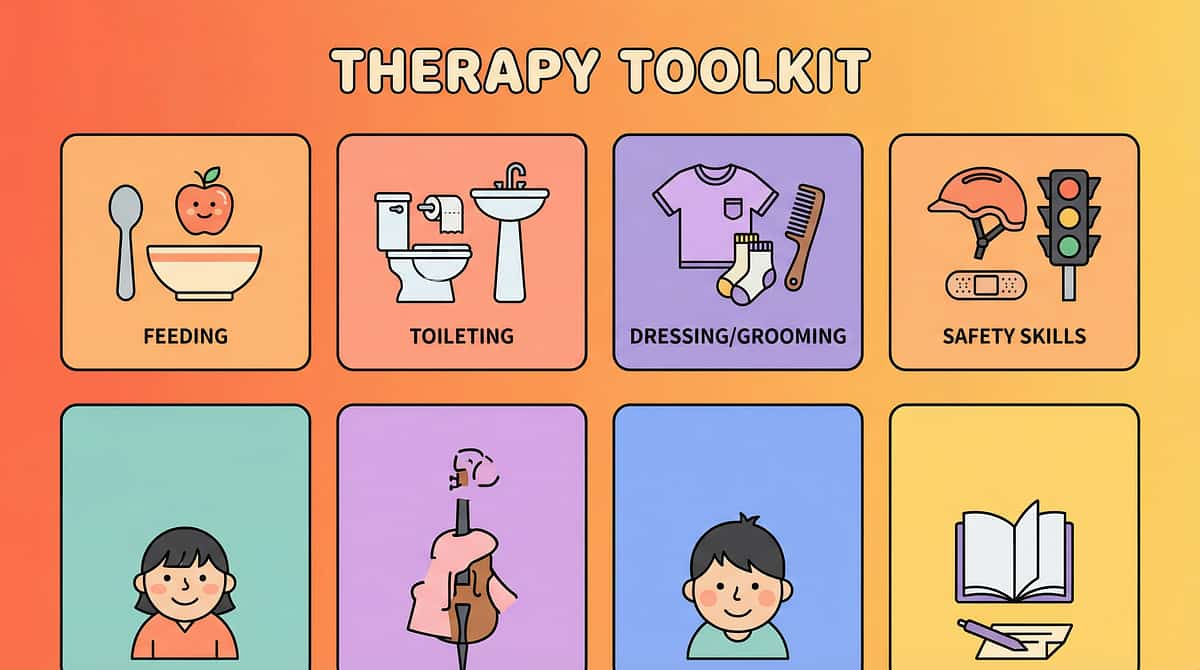
4 Subdomains. 110 Techniques. Evidence-Based. Home-Executable.
Every technique in this library is ordered from foundational to advanced, clinician-drafted, and designed for parents to implement in the natural home environment — no specialized clinic required.
🍽️ Feeding and Eating
Subdomain E1 | Reels E-451 to E-490
40 Techniques — from food acceptance hierarchies to independent utensil use
🚽 Toileting
Subdomain E2 | Reels E-491 to E-520
30 Techniques — from interoceptive awareness to full independent toileting
👕 Dressing & Grooming
Subdomain E3 | Reels E-521 to E-550
30 Techniques — from sock tolerance to full morning routine independence
🛡️ Safety Skills
Subdomain E4 | Reels E-551 to E-560
10 Techniques — from hazard recognition to emergency response protocols

Subdomain E1 | 40 Techniques | Reels E-451 to E-490
🍽️ Feeding and Eating
You've spent an hour preparing a meal your child used to tolerate — and today, they won't even sit at the table. The gagging at new textures, the meltdowns when foods touch, the anxiety around mealtimes that has made every meal feel like a battle you can't win. You watch other children eat freely and wonder what you're doing wrong. You're not doing anything wrong — your child's brain is processing taste, texture, smell, and oral sensation differently, and the pathway to mealtime success is learnable.
The insula and somatosensory cortex govern sensory integration during eating. For many children with ASD, the oral sensory system is hyper- or hypo-responsive, making ordinary textures feel unbearable. Hunger signals from the interoceptive system may also be dulled or distorted, further disrupting mealtime participation.
Technique Areas Covered
- Food acceptance hierarchies and systematic desensitization
- Texture chaining and food texture laddering
- Oral motor strengthening and jaw stability
- Utensil use training (spoon, fork, adaptive tools)
- Mealtime routine structuring and visual schedules
- Hunger and satiety interoceptive awareness
- Self-feeding independence and portion management
- Drinking from cups, straws, and open cups
- Food exploration play and sensory tolerance
- Reinforcement-based food acceptance protocols
Lead Disciplines
OT · ABA · SLP (Feeding)

Subdomain E2 | 30 Techniques | Reels E-491 to E-520
🚽 Toileting
The diapers at age 6, 7, or 8 that no one talks about openly — but that shape your entire day. The anxiety of school trips, the social exclusion that comes with not being toilet trained, the physical discomfort your child experiences but cannot communicate. You've tried everything you can think of, and nothing has worked. You're exhausted, and your child is confused. There is a structured pathway — and it works.
Toileting requires interoceptive awareness — the ability to detect internal signals from the bladder and bowel. In children with ASD, the interoceptive system is frequently under-responsive, meaning the signal to use the toilet arrives late or not at all. Combined with sensory sensitivities to the bathroom environment and difficulty with sequencing, toileting becomes a multi-system challenge that requires systematic, compassionate intervention.
Technique Areas Covered
- Interoceptive body signal awareness training
- Bathroom desensitization and sensory tolerance
- Scheduled voiding and timed toilet training protocols
- Visual supports: toilet sequence picture schedules
- Reinforcement systems for toilet approach and sitting
- Clothing management during toileting
- Hygiene skills: wiping, flushing, handwashing
- Nighttime dryness and pull-up fade protocols
- Generalization across school and community bathrooms
- Bowel training and constipation management strategies
Lead Disciplines
OT · ABA

Subdomain E3 | 30 Techniques | Reels E-521 to E-550
👕 Dressing and Grooming
Every school morning is a negotiation — the tags in shirts that feel like needles, the socks that have to come off and on twelve times before they feel right, the meltdown over a hairbrush that has derailed your entire morning. Getting dressed takes 45 minutes. You're late again. You love your child completely, and you're also completely worn down. These are not behavioral problems — they are sensory and motor planning challenges with evidence-based solutions.
The premotor cortex manages the 30+ sequential micro-steps involved in dressing. The somatosensory cortex processes every touch sensation — seams, fabric textures, waistbands, and the feeling of water or brushes on skin. When either system is dysregulated, even the simplest dressing task becomes an overwhelming neurological event requiring careful, structured scaffolding.
Technique Areas Covered
- Backward and forward chaining for dressing sequences
- Sensory desensitization: tags, textures, waistbands
- Fastener skills: buttons, zippers, snaps, velcro, laces
- Sock and shoe tolerance and independent wearing
- Hair brushing and hair washing desensitization
- Face washing and toothbrushing motor sequences
- Nail cutting tolerance and procedural compliance
- Visual dressing schedule and picture prompt systems
- Seasonal clothing adaptation and weather dressing
- Independence fading: reducing adult physical prompts
Lead Disciplines
OT · ABA

Subdomain E4 | 10 Techniques | Reels E-551 to E-560
🛡️ Safety Skills
Your child ran toward the road before you could blink. They touched the hot pan because they didn't understand the danger. They opened the front door to a stranger without hesitation. Safety is the domain that keeps you awake at night — because the stakes are the highest. Children with ASD are four times more likely to experience accidental injury than neurotypical peers, and many lack the judgment and inhibitory control to recognize danger independently.
Hazard recognition and inhibitory response are governed by the prefrontal cortex and amygdala. Children with ASD often have atypical threat-detection pathways, reduced fear responses to genuine dangers (such as traffic or hot surfaces), and impulsivity from executive function challenges. Safety skills must be taught explicitly, repeatedly, and across environments — they do not generalize automatically.
Technique Areas Covered
- Traffic and road safety awareness and pedestrian rules
- Hot surface and kitchen hazard recognition
- Stranger safety and door-opening rules
- Water safety: pool, bath, and open water
- Emergency protocol: calling for help, 112/100
- Elopement prevention and supervision awareness
- Safe vs. unsafe touch — personal safety fundamentals
- Medicine and cleaning product hazard recognition
- Fire safety: smoke, exit, stop-drop-roll
- Generalization drills across home, school, community
Lead Disciplines
OT · ABA · Special Education
Domain E: Daily Living Skills — Complete Subdomain Index
Use this index to navigate directly to the subdomain most relevant to your child's current priority. Techniques within each subdomain are ordered from foundational to advanced.
Daily Living Skills Connects Across the Developmental Spectrum
Daily living skills do not exist in isolation. Every skill your child masters in Domain E ripples across the entire developmental ecosystem — and disruptions in other domains affect daily living progress in turn.
🎯 Domain A — Sensory Processing
Sensory hypersensitivity to textures, smells, sounds, and touch directly drives feeding refusal, dressing meltdowns, and bathroom avoidance. Sensory regulation interventions must run in parallel with daily living skill training to unlock progress.
🗣️ Domain B — Communication
A child who cannot communicate hunger, discomfort, or the need to use the toilet is significantly disadvantaged in daily living skill development. Functional communication — even via AAC or picture exchange — dramatically accelerates toileting and feeding outcomes.
🧩 Domain D — Behavior
Challenging behaviors during mealtimes, bathroom routines, and dressing sequences are often function-based responses to sensory discomfort or task demands. Functional behavioral assessment informs daily living skill intervention design at every step.
🏃 Domain F — Motor Skills
Fine motor control governs utensil use, fastener skills, and grooming tool management. Gross motor stability underpins safe toileting posture and independent dressing. Motor skill deficits must be identified and targeted alongside daily living interventions.
📚 Domain H — School & Academic
Independent toileting, lunchbox management, and personal hygiene are prerequisites for school inclusion. Daily living skill deficits are among the primary barriers to full mainstream classroom participation and peer social acceptance.
👨👩👧 Domain K — Family & Caregiver Support
Caregiver confidence, stress regulation, and consistent implementation are the single largest predictor of daily living skill outcomes at home. Family wellbeing and daily living skill progress are inseparable — both must be supported simultaneously.

Drafted by a Multi-Disciplinary Consortium
Every technique in this library has been developed, reviewed, and evidence-graded by a consortium of six disciplines — ensuring clinical accuracy, therapeutic safety, and home-implementation feasibility.
Clinical Research Organization (CRO)
Evidence grading, systematic review analysis, PubMed citation mapping, and regulatory compliance across all 110 techniques.
NeuroDevelopmental Pediatricians
Neurological pathway validation, medical safety review, and comorbidity management guidance across all subdomains.
Occupational Therapists (OT)
Sensory-motor integration frameworks, daily living skill protocols, adaptive equipment recommendations, and environmental modification strategies.
Speech-Language Pathologists (SLP)
Communication integration, feeding therapy protocols, oral motor assessment, and AAC integration for non-speaking children.
Board Certified Behavior Analysts (BCBA)
Functional analysis, data-driven programming design, reinforcement system architecture, and behavior reduction strategies.
Special Educators (SpEd)
Academic integration frameworks, IEP and IFSP goal mapping, structured teaching methodologies, and inclusion strategies for school settings.

About Pinnacle Blooms Network®
India's Largest Autism & Child Development Therapy Ecosystem
Founded by Dr. Koti Reddy Saripalli — technology pioneer (India's first Java Community Process member, Asia's first Microsoft Certified Solution Developer) who pivoted to healthcare after his own son's misdiagnosis. That personal journey became a mission of global scale: building the world's most rigorous, data-driven pediatric therapy ecosystem — built by parents, engineered as a system, governed by science.
70+
Therapy Centers
Across India, with 500+ licensed therapists serving families from 70+ countries
21M+
Therapy Sessions
Documented, with ~70 data points each — generating the world's largest pediatric therapy dataset
97%+
Measured Improvement
Verified via AbilityScore® across 1.47 billion+ clinical data points
Mission: Empowering 900 million kids, parents & families worldwide to be self-sufficient and part of the mainstream world. | Revenue: ₹120+ Crore (FY26) — 67% YoY growth
GPT-OS® — The World's First Pediatric Therapeutic Operating System
SaMD under CDSCO
13+ Patents (IPO & WIPO)
ISO 13485:2016
ISO/IEC 27001:2022
AbilityScore®
Universal 0–1000 developmental metric built from 400+ data points across 25 gold-standard assessments. Your child's baseline — precisely measured.
TherapeuticAI®
21M+ sessions and 1.47B data points powering personalized intervention intelligence. The more children it serves, the smarter it becomes.
Personal Development Kernel (PDK)
A living developmental profile for your child — updated in real time as skills are acquired, mastered, and generalized.
Everyday Therapy Program (ETP)
9 personalized goals + 9 matched techniques per session, delivered daily — bridging clinic and home seamlessly.
For Daily Living Skills, GPT-OS® Delivers:
- 🎯 Daily Living Skills profile mapping across all 4 subdomains
- 📊 Technique recommendation based on profile, age, and available materials
- 📈 Week-by-week progress tracking calibrated to evidence-based timelines
- 🔄 Adaptive pathway adjustment as your child progresses

Core Therapy Materials for Daily Living Skills Interventions
Every technique in Domain E references specific Canon Materials — curated, clinically validated tools available through Pinnacle's materials catalogue. These are the tools that make home implementation possible.
Material | Primary Use in Domain E | Link | |
Visual Routine Strips (ADL) | Step-by-step picture schedules for dressing, toileting, and mealtime routines | ||
Oral Motor Tool Kit | Chewy tools, vibrating toothbrushes, and oral sensory desensitization instruments | ||
Toilet Training Pack | Visual toilet sequence cards, reward charts, and moisture alarm systems | ||
Adapted Dressing Board | Practice boards with buttons, zippers, snaps, and laces for isolated skill training | ||
Food Exploration Kit | Textured food introduction tools, divided plates, and food hierarchy prompt cards | ||
Sensory Desensitization Kit | Graduated tactile tools for hairbrushing, nail cutting, and grooming tolerance | ||
Adapted Utensil Set | Weighted, angled, and ergonomic spoons and forks for self-feeding training | ||
Safety Skills Picture Cards | Hazard identification, stranger safety, and emergency response visual prompts | ||
First-Then Board (ADL) | Visual contingency tool for motivating compliance with daily living routines |

⚠️ Safety First — Daily Living Skills Intervention Red Flags
The following signs require immediate pause of home intervention and professional consultation. These are safety-critical warning signs specific to daily living skills domains.
🔴 Severe Feeding Refusal or Weight Loss
If your child is losing weight, refusing all food groups, or showing signs of malnutrition or dehydration — stop home food introduction protocols and seek immediate pediatric consultation.
🔴 Choking, Gagging to Vomiting, or Aspiration Signs
Frequent coughing during meals, wet/gurgly voice after eating, or recurrent chest infections may indicate aspiration. Requires immediate SLP feeding evaluation.
🔴 Severe Self-Injurious Behavior During Routines
Biting, head-banging, or self-scratching during dressing, grooming, or toileting routines signals a need for immediate BCBA functional behavioral assessment before continuing.
🔴 Persistent Bowel or Bladder Medical Issues
Chronic constipation, fecal impaction, urinary tract infections, or encopresis require medical evaluation before any behavioral toileting protocol is initiated or continued.
🔴 Elopement or Acute Safety Risk
If your child is eloping, accessing dangerous areas (stove, road, water), or showing no understanding of immediate physical danger — escalate to professional support immediately.
Escalation Pathway
Step 1 — Self-resolve: Pause intervention → ensure physical safety → provide co-regulation tools
Step 2 — Teleconsult: Pinnacle National Helpline 9100 181 181 (16+ languages, 24/7)
Step 3 — In-person:Find your nearest Pinnacle center
Step 2 — Teleconsult: Pinnacle National Helpline 9100 181 181 (16+ languages, 24/7)
Step 3 — In-person:Find your nearest Pinnacle center

Your Daily Living Skills Intervention Journey — The 12-Week Arc
Evidence shows that consistent, structured daily living skill intervention produces measurable functional gains within 12 weeks. Progress is not linear, but it is predictable — here is what to expect.
Weeks 1–2: Foundation
~15% progress — Baseline assessment, routine mapping, material introduction, and rapport-building. Your child becomes familiar with the structure and you establish consistency.
Weeks 3–4: Emerging
~35% progress — First signs of engagement with the protocol. Brief, partial skill attempts appear. Reinforcement systems begin to take hold. Celebrate every micro-step.
Weeks 5–8: Consolidation
~65% progress — Skills practiced with increasing independence. Generalization to new settings begins. Prompt fading accelerates. Families report meaningful daily relief.
Weeks 8–12: Integration
~90% progress — Skills become functional in daily contexts, maintained with reduced external support. The routine is now owned by your child. This is the destination.

What Every Technique Page Delivers
Each of the 110 technique pages follows the Pinnacle 40-Card Narrative Architecture — a consistent, comprehensive structure that takes you from recognition to mastery. No technique page leaves you wondering what to do next.
Recognition Moment
Your specific daily struggle, decoded in parent language — so you know immediately you're in the right place and this technique addresses your child's exact challenge.
Neuroscience Explained
What is happening in your child's brain — explained clearly, without jargon. Understanding the "why" transforms frustration into compassion and strategic thinking.
Evidence Grade & Citations
Level I–IV evidence grading with direct PubMed references. Every technique is traceable to the peer-reviewed science that validates it.
Step-by-Step Protocol
10–15 minute daily session guides — precise enough for a first-time implementer, flexible enough for an experienced therapist to adapt.
Materials, Progress & Troubleshooting
Canon Materials with purchase links · Progress indicators with measurable milestones · Troubleshooting guides · Safety alerts · Progression pathways to the next technique.
Every page: PubMed-referenced · WHO/UNICEF-aligned · Consortium-drafted · GPT-OS®-integrated

Real Families, Real Outcomes
These stories represent the thousands of families who have walked this path — and found their way through to the other side.
"My son was 7 years old and still in diapers. We had tried everything. Within 3 weeks of following the E2 toileting protocol — the scheduled voiding system and the visual toilet sequence cards — he had his first successful independent bathroom trip. By week 10, he was fully toilet trained at school too. I cannot describe what that moment felt like."
— Mother of 7-year-old, Pinnacle Blooms Network, Hyderabad
"Mealtimes were our biggest battleground. My daughter would gag at the sight of anything orange. We started the food acceptance hierarchy from E1 — just exploring food with her hands first. Six months later, she is eating 22 different foods. She asked for dal rice last week. I cried at the dinner table."
— Father of 5-year-old, Pinnacle Blooms Network, Bengaluru
"Getting dressed used to take 45 minutes and end in a meltdown every single morning. The backward chaining technique from E3 changed everything. We started with just pulling up trousers the last two centimeters. Three months later, my son dresses himself completely and gets to school on time. Our mornings are peaceful now."
— Mother of 8-year-old, Pinnacle Blooms Network, Chennai

Domain E Research Index — Daily Living Skills Evidence Base
All 110 techniques in Domain E are grounded in peer-reviewed, internationally recognized evidence. The following citations represent the primary evidence base for this domain.
NCAEP 2020 — Evidence-Based Practices for Children with ASD
National Clearinghouse on Autism Evidence and Practice. Identifies task analysis, video modeling, and visual supports as Level I EBPs for daily living skill development. National Professional Development Center, UNC Chapel Hill.
WHO Nurturing Care Framework (NCF, 2018)
World Health Organization & UNICEF. Identifies responsive feeding, hygiene, and safety as core nurturing care components. Used in 54+ countries as the foundational framework for early childhood intervention. WHO Geneva.
PMC9978394 — WHO Care for Child Development Package
Systematic review of caregiver-implemented developmental intervention programs across low- and middle-income countries, including India. Validates parent-implemented daily living skill protocols. PubMed Central.
Cochrane Review: Toilet Training Interventions for Children with ASD
Systematic review and meta-analysis of behavioral toilet training protocols. Supports scheduled voiding, reinforcement-based approaches, and visual schedules as evidence-based strategies. Cochrane Database of Systematic Reviews.
ASHA Feeding & Swallowing Practice Guidelines
American Speech-Language-Hearing Association clinical practice guidelines for pediatric feeding and swallowing disorders, including sensory-based feeding difficulties in children with ASD. ASHA, 2021.
AOTA — Occupational Therapy Practice Framework (OTPF-4)
American Occupational Therapy Association. Defines daily living skills (ADL and IADL) as primary occupational therapy domains. Provides the theoretical framework for task analysis and environmental modification. AOTA, 2020.
JAMA Pediatrics (2023) — Feeding Difficulties in ASD
Large-scale epidemiological study establishing 70%+ prevalence of clinically significant feeding difficulties in children with ASD. Key reference for subdomain E1 prevalence data and intervention urgency.
Indian Journal of Pediatrics — ASD Early Intervention (India-specific)
Indian Academy of Pediatrics (IAP) and Rehabilitation Council of India (RCI) joint guidelines for developmental skill intervention in Indian children with ASD. Informs cultural adaptation of feeding, toileting, and grooming protocols for Indian family contexts.
Journal of Pediatric Psychology (2022) — Toilet Training Delays in ASD
Establishes 50%+ of children with ASD achieving toilet training 1–3 years later than neurotypical peers. Supports urgency of early, structured toileting intervention. Key reference for subdomain E2 baseline data.
Explore All 12 Intervention Domains
Daily Living Skills is Domain E in the Pinnacle Blooms Network® intervention library — a comprehensive 12-domain architecture covering every aspect of child development.
Domain | Name | Link | |
A | 🎯 Sensory Processing | ||
B | 🗣️ Communication | ||
C | 💛 Social-Emotional Development | ||
D | 🧩 Behavior | ||
E | 🏠 Daily Living Skills — YOU ARE HERE | ||
F | 🏃 Motor Skills | ||
G | 🎮 Play & Cognitive Skills | ||
H | 📚 School & Academic | ||
I | 🔄 Transitions & Life Events | ||
J | 🌍 Community & Outings | ||
K | 👨👩👧 Family & Caregiver Support | ||
L | 🏥 Therapy Implementation |
Why Pinnacle GPT-OS® for Daily Living Skills?
The difference between a general approach and a GPT-OS®-powered program is the difference between hoping and knowing. Here is exactly what sets this system apart.
Dimension | Typical Approach | Pinnacle GPT-OS® | |
Evidence Base | Single therapist's training and experience | Consortium-drafted: CRO + OT + SLP + BCBA + SpEd + NeuroDev Pediatricians | |
Personalization | Generic protocol applied to all children | AI-mapped individual profile across all 4 daily living subdomains | |
Continuity | 1–2 hours per week in clinic only | 24/7 home protocols integrated with clinic sessions via ETP | |
Materials | Whatever happens to be available | Canon Materials with purchase links, setup guides, and session protocols | |
Progress Tracking | Subjective therapist notes | Data-driven milestones via AbilityScore® (0–1000 scale) | |
Intelligence | Individual therapist's experience | 1.47 billion data points via TherapeuticAI® — and growing | |
Improvement Rate | Variable, rarely measured or reported | 97%+ measured improvement — verified, documented, transparent |
For Therapists, Educators & Pediatricians
Dual-Use: Parent Handouts + Clinical Reference
Every technique page in Domain E is designed for dual use. Parents receive clear, accessible implementation guides in plain language. Clinicians receive the full evidence citations, functional level targeting, IEP goal alignment language, and BCBA-compatible data collection frameworks — all in the same document. This is a clinical resource that travels home with the family.
Clinical Applications
- Map directly to IEP and IFSP daily living goals
- Use Research Index for clinical documentation and insurance authorization
- Assign specific technique pages as parent homework between sessions
- Track generalization from clinic to home via the ETP data layer
- Reference discipline-specific guidelines (AOTA, ASHA, BACB) embedded in each page

Daily Living Skills — Frequently Asked Questions
Answers to the questions parents and caregivers ask most frequently when beginning daily living skills intervention at home.
Can I really implement these techniques at home without a therapist present?
Yes — this is by design. Every technique in Domain E is written specifically for parent implementation in the natural home environment. Research consistently shows that parent-implemented daily living skill programs, when following structured protocols with visual supports, achieve outcomes comparable to clinic-based programs. The home advantage is real: generalization is built in from day one because skills are learned where they will be used.
How long before I see results?
Most families observe first skill attempts within 2–4 weeks of consistent daily implementation. Functional independence — performing the skill without adult prompting in daily contexts — typically emerges between weeks 8 and 12. Individual timelines vary based on skill complexity, the child's current ability level, consistency of implementation, and concurrent support. Our 12-Week Arc (Card 17) provides realistic expectations for each phase.
What age range do these techniques apply to?
Domain E techniques are designed for children aged 2 through 18, with developmental level (not chronological age) as the primary targeting criterion. Foundational techniques begin at the earliest developmental levels. Advanced techniques extend to adolescent and pre-adult independence preparation. AbilityScore® assessment identifies the precise entry point for your child regardless of age.
Where should I start if my child has challenges across multiple subdomains?
Start with the subdomain that creates the greatest daily burden for your family — or the one that, if resolved, would have the highest positive impact on your child's social participation. For most families, this is toileting or feeding. Begin with the first (foundational) technique in that subdomain's reel sequence. Do not attempt multiple subdomains simultaneously in the first month — depth before breadth produces better outcomes.
Do I need to purchase special materials?
Many techniques require only everyday household items and free printable visual supports. Where specific Canon Materials are recommended (such as oral motor tools, adapted utensils, or dressing boards), they are listed with purchase links and clear rationale for their clinical value. You can begin all foundational techniques immediately without purchasing anything, and add materials as you progress.
When should I seek professional help rather than implementing at home?
Please review Card 16 (Safety Protocols) for the complete list of red flags requiring immediate professional consultation. As a general guide: if your child shows medical complications (weight loss, aspiration, bowel issues), significant self-injurious behavior, or acute safety risks — professional evaluation should precede home implementation. Pinnacle's 24/7 helpline (9100 181 181, 16 languages) can help you make this determination in real time.

Internationally Aligned. Nationally Regulated. Globally Trusted.
Pinnacle Blooms Network® and GPT-OS® operate under the highest international standards of clinical evidence, data governance, patient safety, and regulatory compliance — giving families worldwide the confidence to trust this system with their most important work.
International Clinical Standards
✅ WHO Nurturing Care Framework (2018)
✅ WHO Care for Child Development Package
✅ UNICEF MICS Framework
✅ NCAEP 2020 Evidence-Based Practices
✅ NICE Clinical Guideline CG170
✅ SIGN (Scottish Intercollegiate Guidelines)
✅ WHO Care for Child Development Package
✅ UNICEF MICS Framework
✅ NCAEP 2020 Evidence-Based Practices
✅ NICE Clinical Guideline CG170
✅ SIGN (Scottish Intercollegiate Guidelines)
National Regulatory Compliance
✅ CDSCO SaMD (Software as Medical Device)
✅ Indian Academy of Pediatrics (IAP)
✅ Rehabilitation Council of India (RCI)
✅ Rights of Persons with Disabilities Act 2016 (RPwD)
✅ CIN: U85110TG2019PTC132498
✅ Indian Academy of Pediatrics (IAP)
✅ Rehabilitation Council of India (RCI)
✅ Rights of Persons with Disabilities Act 2016 (RPwD)
✅ CIN: U85110TG2019PTC132498
Quality & IP Assurance
✅ ISO 13485:2016 — Medical Device Quality
✅ ISO/IEC 27001:2022 — Information Security
✅ 13+ Patents filed with IPO & WIPO
✅ WIPO International Patent Protection
✅ Registered trademarks: GPT-OS®, AbilityScore®, TherapeuticAI®
✅ ISO/IEC 27001:2022 — Information Security
✅ 13+ Patents filed with IPO & WIPO
✅ WIPO International Patent Protection
✅ Registered trademarks: GPT-OS®, AbilityScore®, TherapeuticAI®

Start Your Child's Daily Living Skills Journey — Now
You have everything you need to begin. The evidence is here. The protocols are here. The support is here. These three steps will take you from this page to your child's first session today.
Step 1: Identify Your Priority
Identify the daily living challenge that creates the most daily burden for your family — mealtimes, toileting, dressing, or safety. Scroll up to the corresponding subdomain card and enter that subdomain first.
Step 2: Choose Your First Technique
Enter your chosen subdomain page. Techniques are ordered from foundational to advanced — begin with Technique 1. Read the full technique page before your first session. Prepare the environment and any listed materials.
Step 3: Implement, Track, and Progress
Run your first 10–15 minute session following the protocol exactly. Record what happened using the progress indicators on the technique page. Return daily. Review your GPT-OS® dashboard weekly. Advance when the mastery criteria are met.
Join 2 Million+ Families on This Journey
You are not walking this path alone. Two million families across India and 70+ countries are using Pinnacle Blooms Network® resources to build their children's independence — one skill, one day, one celebration at a time. Connect, share, and find your community.
🌐 Main Portal
pinnacleblooms.org — Your complete hub for resources, assessments, center locations, and family support
📰 Latest News
News & Research — Stay current with the latest evidence, Pinnacle updates, and autism research breakthroughs
👨👩👧 Parent Resources
Family Resource Library — Guides, videos, and tools designed specifically for caregivers implementing therapy at home
📞 24/7 Helpline
9100 181 181 — Available in 16 languages, 24 hours a day, 7 days a week. Our team is always here when you need guidance, reassurance, or urgent support.

From Dependence to 'I Did It Myself.' One Skill at a Time.
Every child deserves the dignity of independence. Every parent deserves to witness the moment their child completes a task — alone, proudly, confidently. That moment is the destination. And with the right protocol, the right tools, and the right support — it is reachable.
Pinnacle Blooms Network®
Built by Mothers. Engineered as a System. Governed by Science.
70+ Centers | 21M+ Sessions | 97%+ Measured Improvement
70+ Centers | 21M+ Sessions | 97%+ Measured Improvement
The Consortium
CRO · SLP · OT · BCBA · SpEd · NeuroDev Pediatricians
Six disciplines. One purpose. Your child's independence.
Six disciplines. One purpose. Your child's independence.
Powered by GPT-OS®
AbilityScore® · TherapeuticAI® · Personal Development Kernel · Everyday Therapy Program
The world's first pediatric therapeutic operating system.
The world's first pediatric therapeutic operating system.

Legal & Compliance
Medical Disclaimer: This content is educational in nature. It does not replace evaluation, diagnosis, or treatment by a licensed healthcare professional. Always consult your child's therapy team before beginning any new intervention. In case of medical emergency, contact your local emergency services immediately.
Bharath Healthcare Laboratories Pvt Ltd | CIN: U85110TG2019PTC132498 | © 2026 Pinnacle Blooms Network®
GPT-OS®, AbilityScore®, TherapeuticAI®, and Pinnacle Blooms® are registered trademarks of Bharath Healthcare Laboratories Pvt Ltd. 13+ Patents | ISO 13485:2016 | ISO/IEC 27001:2022 | CDSCO SaMD
Preview of daily living skills Therapy Material
Below is a visual preview of daily living skills therapy material. The pages shown help educators, therapists, and caregivers understand the structure and content of the resource before use. Materials should be used under appropriate professional guidance.
Share this resource
Help others discover thisLink copied!
Continue Exploring →
Domain E is one chapter in a 12-domain library of evidence-based intervention. Continue your journey by exploring adjacent domains — or return to the full domain map to choose your next focus area.
