
Toileting — 30 Evidence-Based Interventions
Toilet training, potty training, enuresis & bathroom independence for children with autism. Structured, sensory-informed, and built for real families — across all 30 challenges your child may face.
Subdomain E2
Domain E: Daily Living
Pinnacle Blooms Network®

E-491 · Readiness & Foundations
E-491: 9 Materials That Help With Toilet Training Readiness
"When should I start toilet training?" The most anxious question from every ASD parent. Friends' children were trained at 2. Yours is 4. 5. 6. The pressure from family is relentless. But starting before the child is READY creates failure, frustration, and toileting trauma that makes eventual training harder.
The Neuroscience
Readiness requires FOUR independent systems to be minimally functional: (1) Interoceptive awareness — some signal that bladder or bowel is full. (2) Motor sequencing — ability to walk to bathroom and manage basic clothing. (3) Communication — ANY way to indicate need. (4) Ability to sit for 1–3 minutes — postural stability and attention.
What You'll Learn
- 12-point readiness checklist — objective criteria, not guesswork
- When to START (readiness signs present) vs. when to WAIT (build prerequisites)
- When to START ANYWAY with an adapted approach (older child — E-513)
- ⚠️ Medical clearance FIRST — constipation check before training begins
- Preparing the bathroom and preparing the family
- Realistic timeline expectations: weeks to months, not days
📊 Level I Evidence — NCAEP 2020 | PMC9978394
📋 ABA (BCBA) · 🤲 OT · SLP · Paediatrician
E-492 · Readiness & Foundations
E-492: 9 Materials That Help With Autism Toilet Training
ASD-specific toilet training is NOT the same as neurotypical toilet training. The 3-day methods don't work. "They'll do it when ready" doesn't work. ASD toilet training requires structured, systematic, multi-sensory, individualized intervention — often over weeks to months — and it works.
Step 1 · Data Collection
Wet/dry checks every 30 minutes for 2 weeks to identify the child's individual elimination pattern and HIGH-PROBABILITY times.
Step 2 · Scheduled Sits
Place the child on the toilet at high-probability times — not randomly. Structure replaces the internal signal the child may not yet feel.
Step 3 · Immediate Reinforcement
Reinforce ANY elimination on the toilet — immediately and powerfully. The association between toilet and reward must be stronger than the comfort of diapers.
Step 4 · Fade the Schedule
As interoception develops, gradually extend intervals — eventually transitioning to fully child-initiated toileting.
⚠️ Resolve constipation medically BEFORE starting behavioral ASD toilet training. Indian toilet adaptations included — Western seat vs. Indian squat techniques both covered.
📊 Level I Evidence — NCAEP 2020 · 80%+ success with structured protocol

E-493 · Readiness & Foundations
E-493: 9 Materials That Help With Nonverbal Toilet Training
How do you toilet train a child who can't say "I need to go"? This is the #1 challenge cited by parents of minimally verbal children. Verbal language is NOT required for toilet training. The communication pathway simply needs to be built through an alternative — and equally reliable — channel.
Communication Options
- Picture card handed to parent (on child at ALL times — lanyard, wrist velcro, belt)
- ASL toilet sign — a simple hand sign any child can learn
- AAC toilet button — programmed, easily accessible, always charged
- Leading parent to bathroom by hand
- Pointing to bathroom photo on the wall
- Pulling at diaper or pants — a valid pre-verbal signal
The Golden Rule
The communication system must be faster and easier than having an accident. If expressing the need requires more effort than the alternative, the child will choose the alternative — every time. Simplicity is survival.
Teach the exchange relentlessly: urge → give card/sign/press button → immediate bathroom access → reinforcer.
📊 Level I Evidence — AAC-supported toilet training · NCAEP 2020

E-494 · Readiness & Foundations
E-494: 9 Materials That Help With Interoception for Toileting
They don't FEEL it. The bladder fills, the signal fires — but the insular cortex doesn't process it into conscious awareness. They don't know they need to go until the accident is already happening. This isn't defiance. It's a sensory processing deficit of internal body signals — and it can be taught.
Delayed Signal
Feel the urge — but too late to act on it. The signal exists; processing speed is the challenge.
Reduced Signal
Feel "something" faintly. Not strong enough to trigger action. The signal is present but too weak.
Confused Signal
Feel "something" but cannot identify what. Hunger, bladder, discomfort — all feel the same.
Absent Signal
No signal at all. The bladder fills to capacity with zero conscious awareness until overflow.
The Mahler interoception curriculum builds awareness of ALL body signals before targeting bladder and bowel specifically. Scheduled sits provide external structure while internal awareness develops over months of consistent practice.
📊 Level I Evidence — NCAEP 2020 | Mahler Interoception Research

E-495 · Readiness & Foundations
E-495: 9 Materials That Help When a Child Refuses Toilet Sitting
They won't SIT. Not on the potty. Not on the toilet. Not for one second. They arch, scream, run, go rigid. Before any toileting can happen, the child must be able to sit on the toilet for at least 1–3 minutes without distress. Sitting refusal is almost always the first barrier — and it has nothing to do with compliance.
This gradual progression respects the child's nervous system. Rushing the hierarchy creates panic and sets training back weeks. Take as many days at each step as needed — success at every stage is the goal.
Sensory Adaptations
- Padded or fabric seat cover (cold seat is a major aversion)
- Step stool so feet are flat — security through proprioception
- Grab bars or toilet handles for stability
- Preferred toy, book, or tablet available ONLY during sitting
⚠️ Critical Rules
- NEVER physically force sitting — creates lasting toileting trauma
- Test both potty chair AND toilet seat reducer — responses vary
- Reinforce the ATTEMPT, not just successful sitting
- Keep the caregiver calm — anxiety is contagious
📊 Level I Evidence — Graduated exposure + sensory adaptation · NCAEP 2020

E-496 · Readiness & Foundations
E-496: 9 Materials That Help With Toilet Fear
Genuine TERROR. Screaming at the bathroom door. Crying when carried toward the toilet. Physical fight to avoid the room. Toilet fear in ASD is not about the toilet as we understand it — it's about the toilet as the child experiences it: a cold, echoing, loud, wet, unpredictable sensory nightmare with a hole that things disappear into.
The Hole
Things go down and don't come back. Some children fear falling IN. Some experience body products as part of themselves — flushing feels like losing a piece of who they are.
The Flush
One of the loudest sounds in a child's environment — 80–85 dB — unpredictable timing, reverberating in hard-surface acoustics. Covered in depth in E-497.
The Echo
Hard bathroom surfaces amplify every sound — including the child's own voice, crying, and the sounds of their own body.
The Unknown
What's down there? What might come UP? For a child with a literal, visual-thinking mind, these questions are not irrational — they are reasonable extrapolations.
⚠️Never force a terrified child onto the toilet. A single forced encounter creates phobic conditioning that can take months to undo. Desensitise first — always.
📊 Level I Evidence — Systematic desensitisation for toilet anxiety · NCAEP 2020

E-497 · Specific Challenges
E-497: 9 Materials That Help With Flush Fear
The FLUSH. The single most common toilet-related fear in ASD. The flush sound registers approximately 80–85 dB — as loud as a food blender — amplified by hard bathroom surfaces. Unexpected. Violent. The water rushes. For a sound-sensitive child, the flush is not a minor inconvenience. It is an auditory assault.
Far-away flush
Hear flush from outside room
Doorway flush
Hear flush from doorway
Inside-room flush
Hear flush inside room
Observe flush
Watch flush from a distance
Child-controlled
Child flushes themselves
The key insight: control reduces fear. When the child holds the flush lever themselves, the unpredictability that drives the terror is removed. They choose when it happens — and that changes everything.
Immediate Strategies
- Do NOT flush while child is on or near toilet — flush AFTER they leave the room
- Ear defenders during flush (temporary, not permanent)
- Record flush sound on phone → play at low volume → gradually increase
Public Bathroom Tip
Auto-flush toilets are a major trigger. Cover the sensor with a sticky note before the child enters the stall. This one small act prevents hundreds of panic episodes at restaurants, malls, and schools.
📊 Level I Evidence — Sound desensitisation + control provision · NCAEP 2020

E-498 · Specific Challenges
E-498: 9 Materials That Help When a Child Only Poops in a Diaper
Urinates on the toilet. Refuses to defecate on the toilet. Asks for a diaper, goes to their corner, poops in the diaper. Every single time. This is one of the most common and most misunderstood toileting challenges in ASD — and it has a clear neurological explanation.
The basal ganglia has encoded standing + diaper = safe defecation. Sitting on the toilet presents the wrong position, wrong sensation, wrong proprioceptive feedback. The brain rejects the new context — not out of stubbornness, but out of deep neurological certainty. Gradual transition is the only reliable path.
Step 1
Poop in diaper — anywhere in the house. Baseline established, no pressure.
Step 2
Poop in diaper, but in the bathroom. The LOCATION shifts first.
Step 3
Poop in diaper sitting on the closed toilet lid. Position shifts next.
Step 4
Poop in diaper sitting on the open toilet. The sensation context shifts.
Step 5
Poop in a cut-open or hole-cut diaper placed on the toilet seat.
Step 6
Poop on the toilet without diaper. The full transition is complete. This may take 4–12 weeks — and that is completely normal.
⚠️NEVER withhold the diaper and force toilet use. This creates bowel withholding (E-499) — a far more serious and medically complex problem.
📊 Level I Evidence — Gradual transition from diaper to toilet · NCAEP 2020

E-499–500 · Specific Challenges
E-499–500: 9 Materials That Help With Bowel Withholding & Constipation
⚠️Medical Priority — both conditions require paediatrician/GI evaluation before behavioral intervention; constipation affects 30–50% of children with ASD and is the #1 hidden cause of toileting problems.
They hold it. Days. Sometimes a week. They clench, cross their legs, go rigid — actively preventing defecation. This is a fear-driven behavior with a neurological loop: previous painful bowel movement → amygdala tags defecation as "painful" → pelvic floor contracts instead of relaxing → stool retained → hardens → next movement more painful → more withholding. Constipation causes overflow incontinence that looks like accidents but is actually impaction. Both require medical resolution BEFORE behavioral training.
The Withholding Cycle
Pain → Hold → Harden → More Pain → Impaction → Overflow Incontinence. Breaking the cycle requires stool softening medically first.
Medical Management
Stool softeners (PEG/Miralax), fibre + hydration, Indian fibre foods (papaya, isabgol, ragi, ripe banana), physical activity, toilet positioning (step stool, knees above hips, lean forward), clockwise abdominal massage.
The Golden Rule
You cannot toilet train a constipated or withholding child. Fix the plumbing first. Resolve the medical issue. Then train.
📊 Level I Evidence — Medical constipation management + anxiety-based intervention · NCAEP 2020
NASPGHAN guidelines
⚠️ Paediatrician/GI evaluation mandatory

E-501–502 · Specific Challenges
E-501–502: 9 Materials That Help With Daytime Accidents & Nighttime Wetting
Accidents are expected in ASD toilet training — both daytime and nighttime. Daytime accidents are not regression unless they form a meaningful pattern. Nighttime wetting (nocturnal enuresis) is developmentally normal until age 6–7 in neurotypical children and commonly persists longer in ASD. Night dryness requires two maturational processes: vasopressin (ADH) reducing urine production during sleep, AND an arousal response to bladder fullness strong enough to wake the child. Both develop on the brain's timeline — not the family's.
Build an Accident Log
Record every daytime accident: WHEN (time of day), WHERE (location), WHAT (urine/stool), and WHAT DOING (activity). Within 2 weeks, a pattern almost always emerges — and the pattern tells you where to intervene.
Daytime Strategies
Scheduled toileting every 60–90 minutes; activity-interrupt training; rule out medical causes (UTI, constipation); neutral response to accidents — no shame, no punishment; Indian school context: spare clothes in bag, coordinate with class teacher.
Nighttime Management
Reduce fluids 2 hours before bed; toilet immediately before sleep; waterproof mattress cover (practical management, not defeat); bedwetting alarm (moisture sensor + arousal conditioning — 60–80% effective over 8–12 weeks, gold standard behavioral intervention).
Medical Referral
Sudden daytime accident increase → UTI/constipation check. Persistent nighttime wetting past age 7 → medical evaluation for ADH levels, bladder capacity, UTI, diabetes insipidus. NEVER punish nighttime wetting — it is fully involuntary.
A calm, data-informed response to accidents — rather than an emotional or punitive one — keeps the training relationship intact and protects the child's emerging sense of competence around toileting.
📊 Level I Evidence — Data-driven accident analysis + bedwetting alarm · NCAEP 2020

E-503 · Specific Challenges
E-503: 9 Materials That Help With School Bathroom Refusal
Dry all day at school — because they hold it for 6–8 hours. Won't use the school toilet. Come home desperate and rush to their bathroom. This is not a minor inconvenience. A child holding urine or stool for a full school day faces real medical risks — UTI, constipation, and bladder stretching — along with serious impacts on concentration and behavior in the classroom.
Why School Bathrooms Fail ASD Children
- Unfamiliar toilets — different from home
- Echo, chemical smells, other children's sounds
- Lack of privacy — broken or absent doors
- Poor hygiene conditions — especially in Indian schools
- Social anxiety — fear of peers knowing they're toileting
Accommodation Strategies
- Access to staff toilet — quieter, private, cleaner
- Scheduled bathroom times before the rush
- Bathroom buddy for anxiety support
- Own portable seat cover in school bag
- Gradual exposure: visit when empty → sit clothed → use when quiet
- RPwD 2016 right to reasonable bathroom accommodation
An advocacy letter to the school principal, coordinated with the class teacher, can transform the school toileting experience. Pinnacle Blooms provides a template in the technique materials — use it without hesitation. This is your child's right.
📊 Level I Evidence — School bathroom accommodation + generalisation · NCAEP 2020

E-504 · Specific Challenges
E-504: 9 Materials That Help With Public Restroom Refusal
Can use the home toilet perfectly. Refuses any public toilet. Restaurant, mall, temple, hospital, relative's house — all refused. Family outings become limited by the child's bladder capacity. Travel feels impossible. This is generalisation failure: the toileting skill is locked to the home bathroom template, and every other bathroom is neurologically foreign territory.
1
Familiar Relative's Bathroom
Start with the most similar, least threatening environment. Practice BEFORE urgent need arises.
2
Close Friend's Home
A trusted, familiar social setting. Bring the portable kit — the consistent elements travel with the child.
3
Quiet Restaurant
Lower sensory load than a mall. Visit at off-peak times. Preview the bathroom before the meal.
4
Busy Public Setting
Mall, airport, hospital. Portable kit deployed. Sensor covered. Success built on the previous three stages.
The portable bathroom kit — own seat cover, familiar toilet visual, hand sanitiser, air freshener — provides consistent sensory elements across all environments. The child's nervous system registers familiar cues even in unfamiliar spaces. Practice BEFORE crisis, never during.
📊 Level I Evidence — Systematic generalisation across bathroom settings · NCAEP 2020

E-505 · Skills & Independence
E-505: 9 Materials That Help With Independent Wiping
The most under-discussed toileting skill. They can toilet independently — but can't wipe. At school, this means either an adult must assist (a serious dignity and age-appropriateness concern) or the child doesn't wipe at all (a hygiene and infection risk). Independent wiping is the bridge between toilet training and true bathroom independence.
Why Wiping Is Hard
- Reaching behind the body — bilateral coordination + shoulder flexibility
- Proprioceptive feedback — applying correct pressure without seeing
- Tactile tolerance — touching a messy body area
- Motor planning — front-to-back direction for hygiene
- Completeness monitoring — "Am I clean?" without visual confirmation
Wiping Progression
- Dry practice with playdough or clay on a model
- Wet wipe practice — easier to handle than dry paper
- Toilet paper practice — final and most demanding step
- "Check the paper" — visual inspection for completeness
- Long-handled wiping tool as adaptive aid if needed
🇮🇳Indian Advantage: Water-based cleaning (lota/mug + hand or jet spray) is often SIMPLER than paper wiping for children with ASD. The motor pattern is more intuitive, the feedback is immediate, and the "completeness" signal is clearer. Consider teaching this first.
📊 Level I Evidence — Task analysis + adapted wiping tools · NCAEP 2020

E-506 · Skills & Independence
E-506: 9 Materials That Help With Body Signal Recognition
Beyond awareness — this card teaches the child to recognise, label, and act on body signals for toileting. "That feeling in your tummy means 'toilet time.'" In neurotypical development, this three-step neural pathway forms automatically. In ASD, it requires deliberate, systematic construction — through hundreds of practice repetitions.
Child Acts
Child Labels
Insular Detects
Each link in this chain must be explicitly taught and reinforced. The chain is built by catching pre-toileting behaviors in real time — fidgeting, crossing legs, holding the groin area — and using them as teaching moments: "Your body is telling you something. What is it?" Prompt the label. Prompt the action. Celebrate the recognition.
Body Signal Vocabulary
"Tummy is full" · "Tummy is pushing" · "Need to go" — simple, concrete, consistent language for every caregiver to use.
Visual Body Maps
Illustrated maps showing WHERE the feeling lives — pointing to the bladder/bowel region makes the abstract concrete for visual-thinking children.
Celebrate the Signal
"You FELT it and TOLD me — that's amazing!" Reinforce the recognition itself, not just the outcome. Signal awareness is the skill to build.
📊 Level I Evidence — Interoception curriculum + toileting integration · NCAEP 2020 | Mahler

E-507 · Skills & Independence
E-507: 9 Materials That Help With Toilet Playing
They play with the water. Put toys in. Unroll entire rolls of toilet paper. Splash. Flush repeatedly. Toilet playing may feel exasperating — but it has a clear explanation. The bathroom is a ready-made sensory playground: water provides temperature, movement, tactile, and auditory input all at once. If the child is sitting there with nothing else to do, exploration is the natural result.
Understand Before Redirecting
Water play and paper unrolling provide genuine sensory input that the child is seeking. The goal is not to eliminate the sensory need — it's to redirect it to appropriate times and contexts outside the bathroom.
Practical Strategies
- Water play and paper play during designated sensory time — not bathroom time
- Toilet rules visual (laminated on wall): "Sit. Go. Wipe. Flush ONCE. Wash."
- Toilet paper holder with lock — pre-tear appropriate amount
- Provide appropriate sitting activity: one special fidget or book, toilet-only
- Toilet lock when unsupervised if water play causes flooding or plumbing issues
📊 Level I Evidence — Environmental management + alternative reinforcement · NCAEP 2020
E-508 · Skills & Independence
E-508: 9 Materials That Help With Fecal Smearing Prevention
During toileting, access to stool is at its maximum: the diaper is removed, stool has been produced, and hands are free. Prevention within the toileting routine requires reducing the access window, providing alternative sensory input, and teaching an immediate post-toileting completion sequence — so that no gap exists between stool production and clean hands.
Minimize the Access Window
Quick diaper change protocol — have wet wipe ready BEFORE diaper is removed. The gap between exposure and clean-up is the risk window.
Provide Hands-Occupied Sensory Input
Fidget toy or putty placed in hands at the start of every diaper change or toilet sit — before hands become available for smearing.
Clothing Barriers
Onesies, back-fastening garments, or belt systems during unsupervised periods — reduce overnight and nap-time access entirely.
Immediate Hand Washing
Toilet → sink must be ONE unbroken sequence. No gap. No distraction. Wet wipe or soap at the toilet, not across the room.
📊 Level I Evidence — Environmental management within toileting protocol · NCAEP 2020
E-509 · Skills & Independence
E-509: 9 Materials That Help With Visual Toileting Supports
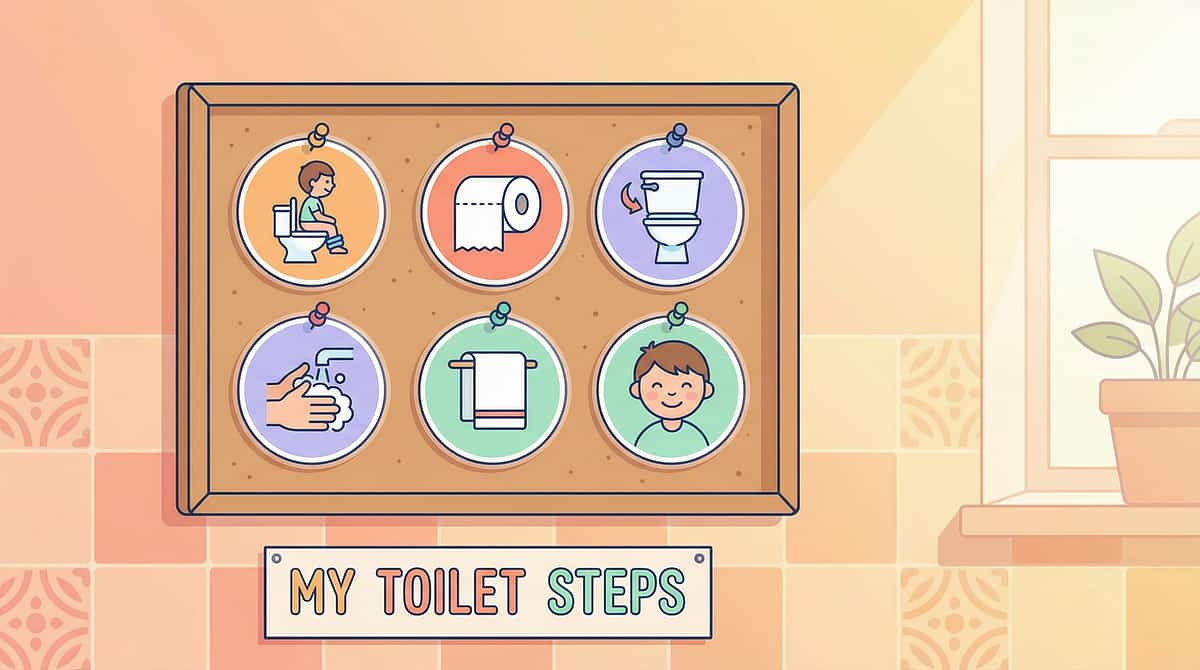
Visual supports are the single most effective accommodation for ASD toilet training — referenced in every major study and protocol. The toilet routine sequence — laminated, velcro, step-by-step, mounted at child eye-height — transforms an overwhelming multi-step process into a manageable, predictable, self-directed visual checklist. Every ASD bathroom should have one.

Steps 1–4
Walk to bathroom → Light on → Pants down → Sit on toilet

Steps 5–7
Wait → Wipe (front to back) → Pants back up

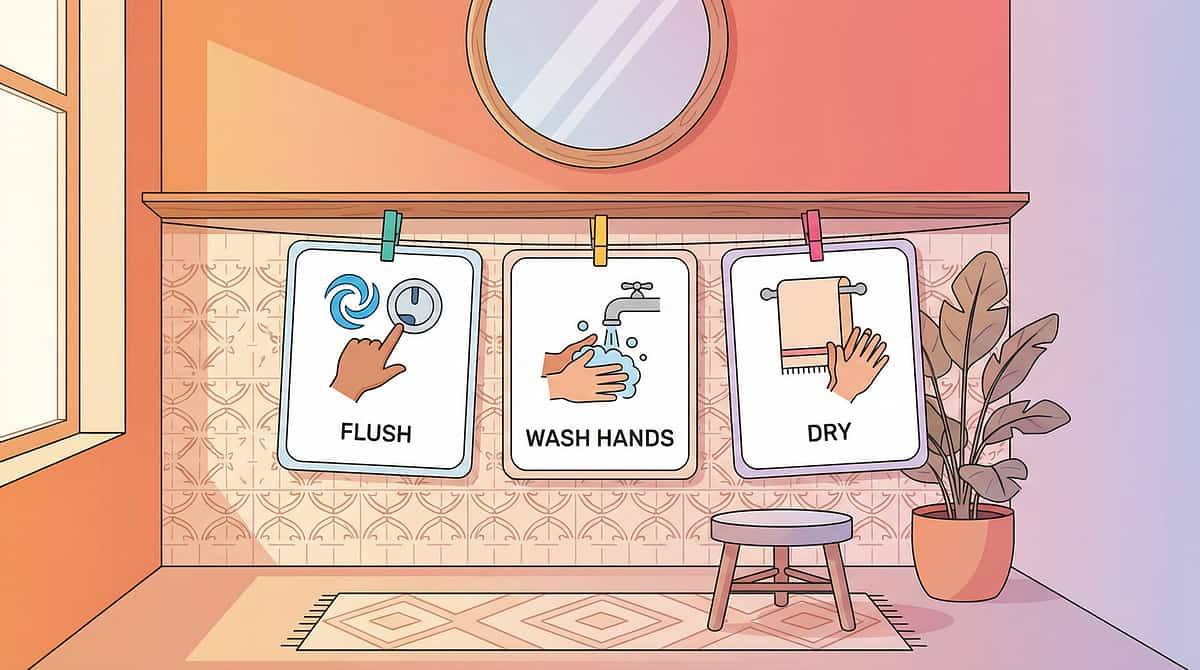
Steps 8–10
Flush → Wash hands → Dry hands. The sequence is COMPLETE.
Use photos of YOUR child's actual bathroom — not stock icons — for maximum recognition. Include the lota or jet spray step for Indian bathrooms. Laminate, mount with velcro check-offs, and teach the child to move each step from "to do" to "done." The visual schedule becomes the prompt — not the adult.
📊 Level I Evidence — Visual supports improve outcomes across all ASD toilet training studies · NCAEP 2020

E-510 · Skills & Independence
E-510: 9 Materials That Help With Bathroom Sensory Issues
The bathroom is a multi-sensory assault: cold hard surfaces, echoing acoustics, bright overhead lights, chemical smells, wet floors, a cold toilet seat, and the flush. Every sensory system is challenged simultaneously. For the ASD nervous system, the bathroom risk assessment reads clearly: sensory pain → avoid.
Sensory Challenge | The Problem | The Solution | |
Cold toilet seat | Tactile aversion on contact | Padded or fabric seat cover | |
Echo acoustics | Sound amplification → auditory overload | Soft mat on floor, towel on wall | |
Bright overhead light | Visual hypersensitivity | Dimmer switch or nightlight | |
Chemical smells | Olfactory aversion | Switch to unscented products | |
Wet/slippery floor | Tactile + safety anxiety | Bath mat with non-slip backing | |
Loud flush | Auditory assault | Flush after child leaves (initially) | |
Hand dryer | Extreme auditory trigger | Personal towel instead |
🇮🇳Indian Budget Note: All bathroom sensory modifications can be implemented for approximately ₹500–₹2,000 total. When the bathroom is the barrier, fix the bathroom first — then train the toileting.
📊 Level I Evidence — Sensory-adapted bathroom environments · NCAEP 2020

E-511 · Skills & Independence
E-511: 9 Materials That Help With Different Toilet Locations
Uses home toilet perfectly. Won't use any other toilet. Grandparent's house, school, friend's house, hotel — all refused. The toileting skill is locked to one specific bathroom. This is the same generalisation failure that affects eating locations (E-470): the basal ganglia encodes toileting as a location-specific procedure, and changing any variable disrupts the entire routine.
The Portable Toilet Kit
The solution to location specificity is portable consistency. The kit travels with the child and provides the same sensory anchors in every bathroom:
- Own seat cover (same tactile input)
- Familiar visual routine card (same visual sequence)
- Known hand soap scent (same olfactory anchor)
- Small reward (same reinforcement)
Generalisation Hierarchy
- Home bathroom → baseline mastery
- Grandparent's or familiar relative's bathroom
- Close friend's home bathroom
- School bathroom (staff toilet first)
- Public bathrooms — quiet venues first
Visit new bathrooms for exploration before urgent need. Preview photos of each new bathroom's toilet before the visit to reduce anticipatory anxiety.
📊 Level I Evidence — Systematic generalisation · NCAEP 2020
E-512 · Skills & Independence
E-512: 9 Materials That Help After Toilet Regression
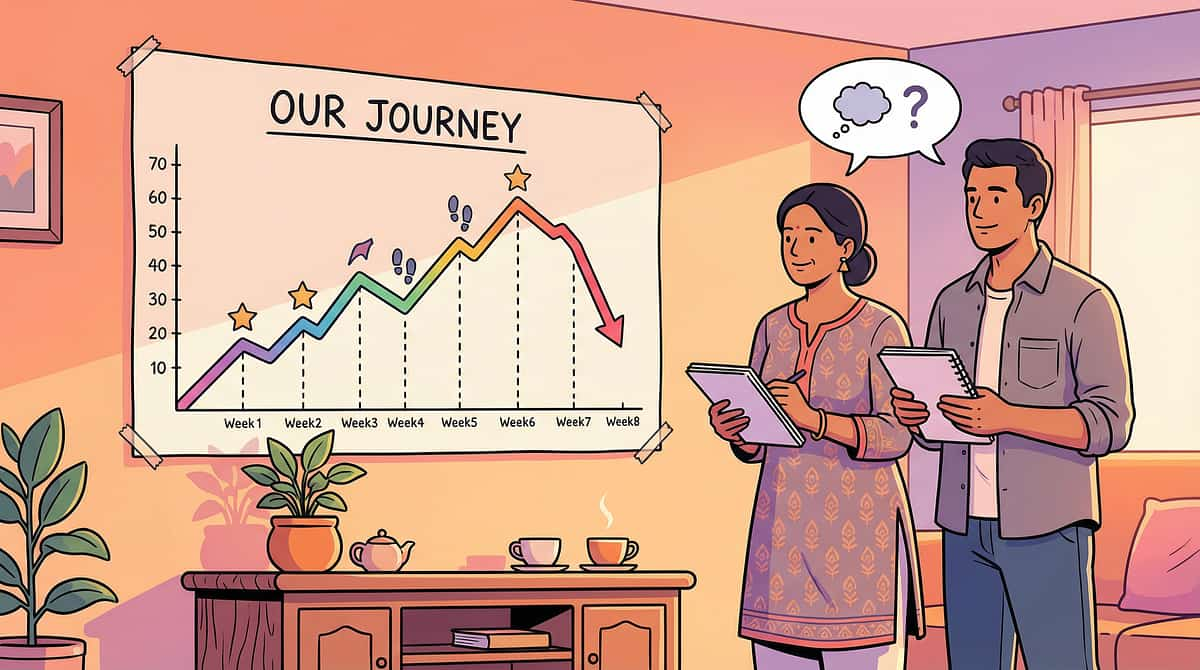
They WERE trained. Dry for weeks. Months. Then — accidents return. Toileting lost. Regression. The most demoralising experience for parents who invested months of patient effort. But regression is common, expected, and fully recoverable. And it almost always has a traceable cause.
Check Medical First
⚠️ Before any behavioral response: UTI screen, constipation check, review any new medications. Medical causes account for a significant proportion of regressions.
Conduct a Stress Audit
What changed? New school, new sibling, home move, family stress, teacher change, schedule disruption? The toileting skill often fractures under systemic stress.
Return to Last Success
Go back to the LAST step that was consistently successful — not back to zero. The foundation exists. Rebuild from the solid ground that remains.
Reframe the Narrative
Regression ≠ failure. The learning was real. The skill exists. Under stress, even consolidated skills temporarily retreat. This is neurology, not character.
Avoid blame in both directions — not the child's fault, not the parent's fault. Regression is a signal from the nervous system. Respond with data, calm, and a clear retraining plan.
📊 Level I Evidence — Medical evaluation + retraining protocol · NCAEP 2020
E-513 · Advanced & Independence
E-513: 9 Materials That Help With Older Child Toilet Training
Your child is 7. 8. 10. 12. Still in diapers. You've tried before. Failed. The shame compounds with age. School becomes impossible. Social participation narrows. It is not too late. It is NEVER too late. But older child toilet training requires fundamentally different approaches than toddler training — age-appropriate language, dignity preservation, and modified protocols that respect the older child as a whole person.
Why Older Training Is Different
The basal ganglia has had years to encode diaper as the toileting context — making it harder to override. But older children also have greater cognitive capacity: they can understand explanations, use visual supports independently, self-monitor progress, and participate meaningfully in their own training plan. That capacity is an asset.
Protocol Adaptations
- Age-appropriate language — no "potty" language, no toddler potty chairs
- Adult bathroom throughout — full dignity preserved
- Private training sessions — never in front of peers or siblings
- Modified Azrin and Foxx protocol for older children
- Pull-ups vs. underwear decision made collaboratively
- School toileting plan with dignity and teacher coordination
- ⚠️ Medical clearance + GI assessment before starting
📊 Level I Evidence — Adapted protocols for older children and adolescents · NCAEP 2020

E-514 · Advanced & Independence
E-514: 9 Materials That Help With Toilet Communication
They may FEEL the urge. They may KNOW they need to go. But they can't TELL anyone in time. The communication gap between sensation and expression is precisely where accidents happen — and it's a gap that can be systematically closed through functional communication training targeting toileting specifically.
Feel Urge & Label Signal
Express Need
Caregiver Responds
Internalize Co-Regulation
Every link in this chain can break independently. The signal may not be detected (interoception failure). The label may not be available (vocabulary gap). The expression may be too slow (motor planning for speech). The environment may not support it (no pictures available, caregiver doesn't see the sign). Teach ALL links. In ALL environments. With ALL caregivers.
Caregivers must be trained to respond immediately to every toilet communication attempt — every second of delay increases accident risk. There must be zero social cost to expressing the need.
📊 Level I Evidence — FCT for toileting · NCAEP 2020
E-515 · Advanced & Independence
E-515: 9 Materials That Help With Nighttime Training
Daytime dry. Nighttime: pullup every night. Nighttime training is entirely separate from daytime — different neural mechanisms, a different maturation timeline, and a different intervention approach. No amount of behavioral pressure can accelerate ADH production. The intervention meets the biology where it is.
Fluid Management
Reduce fluid intake 2 hours before bedtime. Toilet immediately before sleep. Sets the bladder up for success through volume reduction.
Bedwetting Alarm
Moisture sensor in underwear + alarm by bed. When triggered: wake, toilet, change, reset. Over 8–12 weeks, arousal conditioning develops. 60–80% success rate.
Mattress Protection
Waterproof cover as standard practice — not shame, not punishment. Practical management that keeps the process low-stress for the whole family.
Medical Referral
No improvement after 12 weeks of alarm use → medical evaluation. Desmopressin (ADH medication) is a NeuroDev decision — not a first line, but a valid pathway for persistent cases.
📊 Level I Evidence — Bedwetting alarm (60–80% success over 8–12 weeks) · NCAEP 2020
E-516 · Advanced & Independence
E-516: 9 Materials That Help With Toilet Schedule
Until interoception is reliable, the toilet schedule is the scaffolding. Scheduled sits at regular intervals prevent accidents by ensuring the child is on the toilet when elimination is likely — regardless of whether they feel the urge. Structure replaces the internal signal the child may not yet have. And repeated success on the toilet builds the very associations that eventually allow interoception to develop.
Building the Schedule
Step 1: Two-week wet/dry chart — check every 30 minutes. Map individual elimination patterns with precision.
Step 2: Identify HIGH-PROBABILITY times: after waking, after every meal (gastrocolic reflex fires 15–30 minutes post-meal), before bed, before leaving the house.
Step 3: Add regular 60–90 minute intervals between anchored times.
Schedule Execution
- 3–5 minute sits — not 30 seconds, not 30 minutes
- Visual timer for duration — child can see the endpoint
- Phone alarm or dedicated visual timer for interval prompts
- Reinforce SITTING first, regardless of output
- Fade schedule gradually as interoception develops
- Final goal: fully child-initiated toileting, no prompts needed
📊 Level I Evidence — Scheduled toileting is foundational to all ASD toilet training protocols · NCAEP 2020
E-517 · Advanced & Independence
E-517: 9 Materials That Help With Boys Standing to Pee
Standing urination is a motor-spatial skill requiring hand-eye coordination for aim, stream control through pelvic floor management, height estimation, and clothing management — simultaneously, while balancing. It's a complex task disguised as a simple one. It should be introduced only after reliable sitting urination is established — not concurrently.
Target Practice
Floating targets in the bowl — a Cheerio, ping pong ball, commercial color-changing toilet target sticker — provide concrete visual feedback for aim. Gamification of a motor skill.
Height and Stability
Step stool if needed for appropriate height. Trunk stability for standing balance while hands are occupied with clothing and aim management.
Clothing Management
Elastic waistbands only during initial training — no buttons, zips, or belts. One hand manages clothing, one hand manages direction.
Clean-Up Responsibility
Missing the target is part of learning — AND cleaning up is part of the skill. Teach both without shame.
🇮🇳Indian Context: Indian squat toilet standing technique and outdoor urination for travel situations are both included in the technique materials — practical for family outings and rural settings.
📊 Level I Evidence — Motor skills teaching within toileting protocol · NCAEP 2020
E-518 · Advanced & Independence
E-518: 9 Materials That Help With Bathroom Independence
The full independence card. The goal of every technique in this subdomain. The child who can: recognise urge → go to bathroom → manage clothing → sit → eliminate → wipe → dress → flush → wash hands → dry → exit. The complete sequence. Independently. Without prompts. When they go to the bathroom without anyone knowing — that's independence.
Independent
Visual
Verbal
Gestural
Physical
Full independence integrates every skill built across E-491 through E-517. Backward chaining — fading prompts from the LAST step first — builds a sense of completion and ownership from the very beginning of independence training. The child finishes the sequence themselves before they start it themselves.
Independence Checklist
Track each step as: independent / verbal prompt / physical prompt. The data shows exactly where to focus fading efforts.
Self-Monitoring
Visual checklist the child marks themselves — transitioning from adult monitoring to self-monitoring is the final leap.
Maintenance
Independence achieved is not independence maintained automatically. Ongoing monitoring with decreasing frequency ensures the skill consolidates across settings, people, and time.
📊 Level I Evidence — Task analysis + systematic prompt fading · NCAEP 2020

E-519 · Advanced & Independence
E-519: 9 Materials That Help With Handwashing After Toilet
Toileting without handwashing is incomplete. Handwashing must be permanently linked to toileting as a non-negotiable final step — so automatic that the sequence feels unfinished without it. In a post-COVID world, this is both a personal hygiene skill and a public health responsibility.
The 7-Step Sequence
Wet hands → Add soap → Rub front of hands → Rub back of hands → Rub between fingers → Rub thumbs → Rinse → Dry
Visual sequence mounted at the sink — not inside the toilet area — to prompt the NEXT step at the right location.
Sensory Considerations
- Water temperature: preset to comfortable — neither cold shock nor scalding
- Soap: unscented, preferred texture (liquid vs. bar — test both)
- Duration: "Happy Birthday" song twice = 20 seconds, or visual timer at sink
- Towel preferred over air dryer — eliminates major auditory trigger
- Indian backup: hand sanitiser when water access is unavailable in public
The critical teaching principle: toilet → sink must become one unbroken sequence. Never allow an interruption between finishing the toilet and starting handwashing. The habit is built in the gap — or not built at all.
📊 Level I Evidence — Task analysis + visual supports for handwashing · NCAEP 2020
E-520 · Advanced & Independence
E-520: 9 Materials That Help With Clothing Management for Toilet
The capstone of Subdomain E2. Clothing management — pulling pants down, managing underwear, handling skirts and dresses, pulling everything back up, navigating buttons and zips — is often the first barrier to independent toileting. The child may be neurologically toilet-ready but clothing-unready. Fix the clothing, and the toileting often follows.
Adaptive Clothing First
Elastic waistbands ONLY until fully independent — no buttons, no zips, no belts, no snaps. Remove the fine motor barrier completely during training.
Pull-Down Practice
Practice with favourite pants when NOT toileting — reduces performance anxiety. The clothing skill must be automatic before it can be deployed under urgency.
Pull-Up Practice
The hardest step — requires standing balance, bilateral hand coordination, and correct force calibration. Practice separately, multiple times daily.
Indian Clothing
Salwar kameez dupatta management, dhoti considerations, school uniform adaptations — all covered in technique materials with practical Indian-context guidance.
9 Canon Materials:Visual Schedule · Social Stories · First-Then Board · Reward Charts · Visual Timer · Communication Board · Calm-Down Kit · Emotion Cards · Sensory Play Materials
📋 ABA (BCBA) · 🤲 OT · SLP · SpEd · NeuroDev · Paediatrician
📊 Level I Evidence — Adaptive clothing + fine/gross motor development · NCAEP 2020
Preview of toileting Therapy Material
Below is a visual preview of toileting therapy material. The pages shown help educators, therapists, and caregivers understand the structure and content of the resource before use. Materials should be used under appropriate professional guidance.
Share this resource
Help others discover thisLink copied!
All 30 Techniques — Quick Reference
Every technique in Subdomain E2, organized by section. Each links to a dedicated 40-card deep-dive with 9 canon materials, detailed protocols, and Indian-context adaptations.
Code | Technique | Primary Focus | |
E-491 | 12-point checklist · When to start, wait, or adapt | ||
E-492 | ASD-specific structured protocol · Data collection · Reinforcement | ||
E-493 | Picture cards · AAC · Signs · Exchange teaching | ||
E-494 | Mahler curriculum · Body signal awareness building | ||
E-495 | Graduated exposure · Sensory adaptations · Zero force | ||
E-496 | unknown link | Systematic desensitisation · Social stories · Hierarchy | |
E-497 | unknown link | Sound desensitisation · Child-controlled flushing · Auto-flush management | |
E-498 | Six-step gradual diaper-to-toilet transition | ||
E-499 | ⚠️ Medical first · Break the pain-withholding cycle | ||
E-500 | ⚠️ Medical first · Diet · PEG · Indian fibre foods | ||
E-501 | Accident log · Scheduled toileting · Neutral response | ||
E-502 | Maturational perspective · Bedwetting alarm · Fluid management | ||
E-503 | Accommodation · Advocacy · Gradual exposure · RPwD 2016 | ||
E-504 | Portable kit · Generalisation hierarchy · Auto-flush management | ||
E-505 | Wiping progression · Jet spray advantage · Front-to-back rule | ||
E-506 | Signal → label → action chain · Body vocabulary | ||
E-507 | unknown link | Sensory redirection · Environmental management · Toilet rules visual | |
E-508 | Access reduction · Hands-occupied strategies · Clothing barriers | ||
E-509 | 10-step laminated sequence · Velcro check-off · Indian adaptations | ||
E-510 | Sensory audit · Solutions per modality · Budget ₹500–₹2,000 | ||
E-511 | Portable kit · Generalisation hierarchy · Preview photos | ||
E-512 | Medical first · Stress audit · Rebuild from last success | ||
E-513 | Dignity-first · Age-appropriate language · Modified Azrin and Foxx | ||
E-514 | FCT · Multi-modal communication · Caregiver response training | ||
E-515 | Full alarm protocol · Fluid management · Desmopressin pathway | ||
E-516 | Data-driven scheduling · Timer prompts · Gradual fading | ||
E-517 | Target practice · Motor-spatial skill development · Step stool | ||
E-518 | Full sequence independence · Backward chaining · Self-monitoring | ||
E-519 | 7-step sequence · Sensory soap selection · Unbroken toilet-to-sink | ||
E-520 | Elastic waistbands first · Pull-down practice · Indian clothing adaptations |
