


Your Child Isn't Choosing the Problem Behavior. They're Using the Only Tool They Have.
The Neuroscience All behavior serves a function. The prefrontal cortex — the brain's "what should I do?" decision center — requires explicit learning to generate socially appropriate alternatives. Children with autism frequently show differences in: Prefrontal-limbic connectivity — the pathway linking impulse to alternative selection Working memory load — under stress, the brain cannot retrieve abstract verbal rules Inhibitory control — the neurological "brake" that requires practiced alternatives to engage The behavioral vacuum principle: When a behavior is suppressed without a replacement, the same neurological need simply finds a new behavior. The "whack-a-mole" effect parents describe is real neurological evidence of an unmet function. Plain English for Parents Your child hits because hitting works — it ends conflict, gets attention, or escapes a demand. Their brain has learned: "This behavior produces the outcome I need." You cannot simply remove that tool. You must install a better one. When you teach an alternative that works just as well — or faster — the brain naturally shifts. Not because the child is "choosing to behave." Because the new pathway is more efficient. Clinical Term: Functional Replacement Behavior Teaching | Differential Reinforcement of Alternative Behavior (DRA) — Frontiers in Integrative Neuroscience (2020) | DOI: 10.3389/fnint.2020.556660


Source | Finding | |
NCAEP Evidence-Based Practices (2020) | Functional Communication Training classified as an evidence-based practice for autism across all age groups | |
BACB Professional Standards | Differential Reinforcement of Alternative Behavior (DRA) — foundational behavioral intervention with decades of RCT support | |
Journal of Positive Behavior Interventions | 70–80% reduction in challenging behaviors when replacement behaviors are systematically taught | |
Padmanabha et al., Indian J Pediatr (2019) | Home-based behavioral skill teaching shows significant outcomes in Indian pediatric population |

Parent-Friendly Alias: Teaching What TO Do
Code: D-360
Domain: Applied Behavior Analysis / Positive Behavior Support
Age Range: 2–12 years
Session Duration: Integrated throughout the day
Frequency: Continuous — every time the target situation arises
Discipline Lead: BCBA/ABA Primary | SLP Co-lead | OT Supporting

"The brain doesn't organize by therapy type. A child who hits because they can't communicate needs their SLP to give them a voice and their BCBA to make that voice more rewarding than the fist." — Pinnacle Blooms Consortium Clinical Lead


9 Materials. Clinically Chosen. Home-Ready.
These 9 materials span three functional categories — visual alternatives (Cards, Charts), practice tools (Puppets, Video), and reinforcement systems (Tokens, Rewards). A starter kit of ₹500–800 covers the essentials for most families. Instead Of Cards / Choice Board Visual Supports — shows child what to do instead of the problem behavior. 🔍 Search Amazon.in Social Story Books Social Narratives — teaches behavior through relatable stories. 🔍 Search Amazon.in Hand Puppets / Role-Play Props Role-Play Materials — safe practice of alternative behaviors. 🔍 Search Amazon.in Communication Cards / PECS System AAC Supports — gives children without verbal language a functional voice. 🔍 Search Amazon.in Stress Balls / Calm-Down Kit Sensory Regulation Tools — provides sensory alternative to problem behavior. 🔍 Search Amazon.in Video Model on Tablet Video Modeling — evidence-based visual demonstration of the alternative behavior. NCAEP 2020 classified. Problem-Solving Chart Visual framework for generating alternatives. 🔍 Amazon.in Prompt Reminder Cards Behavior prompt cards reviewed before challenging situations. 🔍 Amazon.in Token Board / Reward Chart Reinforcement system — ₹364 | 🛒 Buy on Amazon.in or ₹589 Premium | 🛒 Buy on Amazon.in

Every Child Deserves This. Regardless of Budget.
WHO/UNICEF Equity Principle: Household-material interventions are equally effective when the therapeutic principle is maintained. The therapeutic value is in the function, not the material. Buy This Printed Instead Of Cards (laminated) Social Story Book Hand Puppets Communication Card Ring Calm-Down Kit Box Video Model on Tablet Problem-Solving Chart (printed) Prompt Cards (laminated) Token Board (purchased) Make This (₹0) Cut paper, draw or print pictures, slip into ziplock bag 5 sheets of A4 paper folded and stapled; draw scenes or print photos Two socks from the drawer Sticky notes on the fridge Shoebox + soft cloth, rice bag, paper pinwheel Phone recording of child or parent demonstrating the alternative Draw on a whiteboard or cardboard with marker Index cards with handwritten reminders Sticker chart on paper Zero-Cost Starter Kit: (1) Draw 3 "Instead Of" cards for your child's most common behaviors. (2) Write a 5-sentence social story tonight. (3) Use two socks for your first role-play session tomorrow morning. | PMC9978394

Read This Before You Begin. Every Time.
🔴 RED — Do Not Proceed If: Child is in active meltdown or severe distress — wait minimum 30 minutes after calm Child is ill, in pain, or has not slept Target behavior involves self-injury or aggression posing immediate safety risk — call 9100 181 181 first You are unable to respond consistently for the next 15–30 minutes 🟡 AMBER — Modify Your Approach If: Child is tired but not dysregulated — shorten practice to 1 role-play only You are emotionally activated — ground yourself first; your nervous system regulates theirs There has been a recent behavioral incident — allow 60-minute recovery period before teaching 🟢 GREEN — Safe to Proceed When: Child is regulated, fed, and rested You have 10–30 minutes of consistent availability Materials are prepared and accessible before the session begins You have reviewed the target alternative behavior for today's session RED LINE — Stop Immediately If: The child becomes aggressive, self-injurious, or escalates beyond what you can safely manage. Session abandonment is not failure. It is data. Document what happened and call your Pinnacle therapist.FREE National Helpline: 9100 181 181 (Available 24x7, 16+ languages) | DOI: 10.1007/s12098-018-2747-4
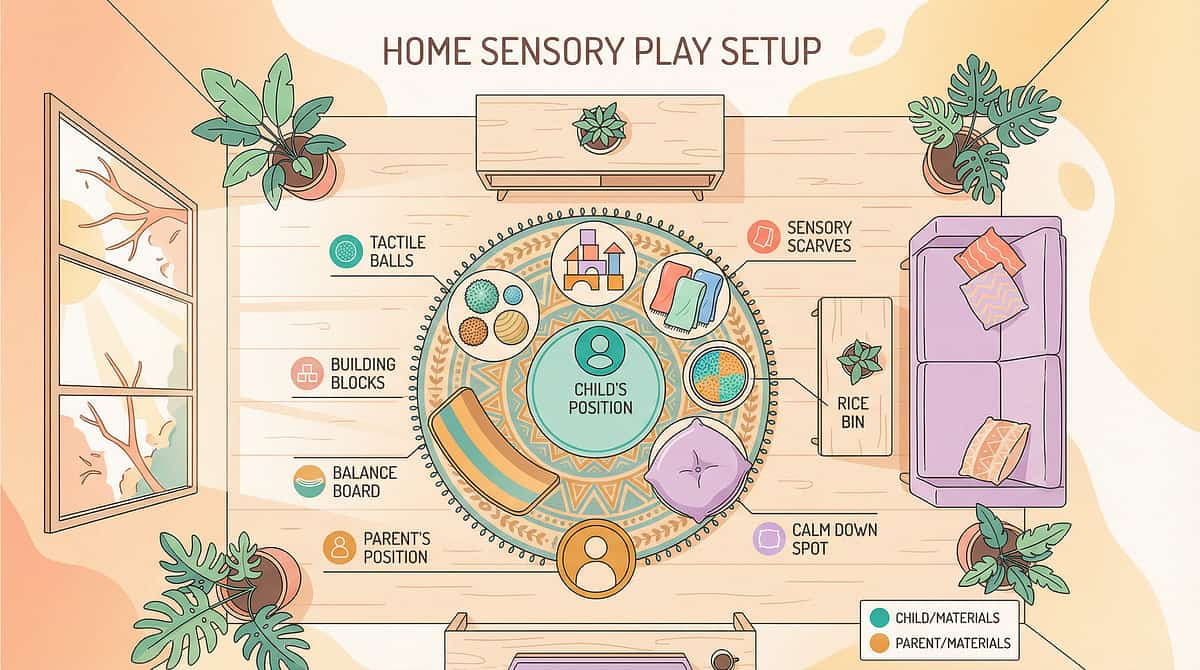
- Instead Of cards — posted at child's eye level on a nearby wall
- Calm-down kit — accessible in the corner, not hidden
- Communication cards — on a ring, within arm's reach of child
- Token board — visible to child throughout the session
- Distraction removal — TV off, tablets face-down, siblings in another room if possible
- Your phone — on silent but accessible for data capture
- Lighting: Natural light preferred; avoid harsh fluorescent
- Sound: Background noise below 50 dB; avoid competing audio
- Temperature: Comfortable; sensory comfort is a prerequisite for learning
- Space: Enough room for the child to move if they need motor breaks
- 60–90 minutes after waking (alert but not overstimulated)
- After a preferred activity (motivation is high)
- NOT immediately before meals or sleep

Indicator | ✅ GO | ⚠️ MODIFY | ❌ POSTPONE | |
Regulated state | Calm, engaged | Slightly unsettled | Crying, melting down | |
Fed and hydrated | Meal within 2 hours | Snacked but not full meal | Hungry | |
Rested | Normal sleep | Slightly tired | Sleep-deprived | |
No recent incident | 60+ min since behavior | 30–60 min since incident | Within 30 min | |
Open to interaction | Eye contact, approaching | Tolerating presence | Actively avoiding | |
Your readiness | Calm and focused | Slightly stressed | Overwhelmed |

Step 1: The Invitation — Begin With Invitation, Not Instruction
Step 1 of 6 ⏱ 30–60 seconds | Get to the child's eye level. Open posture — no crossed arms, no tension. Voice: warm and genuinely curious, not directive. Physical distance: 60–90 cm — close enough for connection, far enough for autonomy. "Hey [child's name], I have something really cool to show you. Can I show you something?"or"We're going to practice something — and you get to use the puppet / the cards / the kit. Ready?" What Acceptance Looks Like Child orients toward you Child makes eye contact (even briefly) Child moves toward or touches the material Child vocalizes or gestures toward the activity Resistance → Modification Turns away: Bring material to their field of vision; reduce demand Says "no": Offer choice: "Puppet or cards — which one first?" Continues current activity: Join them briefly, then introduce No response: Wait 10 seconds, offer once more, then postpone ABA Pairing Procedures: Establishing motivating operations before demand placement reduces avoidance and increases engagement rate. | OT "Just-Right Challenge" principle


Target Behavior | Function | Replacement | Protocol | |
Hitting when wanting something | Access | "Can I have a turn?" / hand card | Model → prompt → reinforce | |
Screaming when frustrated | Escape / attention | Break card / "I need a break" | Model card use → honor immediately | |
Running away from demand | Escape | "I need help" / raise hand | Teach break request → deliver break | |
Grabbing toys | Access | "May I have?" / exchange card | Model exchange → give item → praise | |
Throwing objects | Sensory / escape | Squeeze stress ball / ask for break | Calm-down kit + communication card |

Step 4: Repeat & Vary — Repetition Builds Neural Pathways. Variation Prevents Rigidity.
Step 4 of 6 ⏱ 3–5 minutes | Target: 3–8 practice trials per session. "3 excellent, reinforced, joyful repetitions outperform 20 forced, reluctant ones." Trials 1–3: Minimum Target Same scenario, full support. Build the pathway. Reinforce every attempt. Trials 4–6: Consolidation Zone Begin to vary the partner or location. Introduce slight changes to confirm learning is generalizing. Trials 7–8: Strength Zone Change emotional intensity or material prop. Building robust, flexible behavior. Variation Protocol After 2–3 successful trials with the same scenario: change the communication partner (other parent, sibling) | change the physical location (kitchen → bedroom) | change the emotional intensity (mild → higher frustration) | change the material prop (card → words → gesture). The 3 Good Reps Rule: If you get 3 successful, independent, reinforced trials — stop. Let the child end on success. The nervous system consolidates during rest, not during exhaustion. Stop if child seeks another activity, stops looking at materials, or reinforcer effectiveness drops.

Step 5: Reinforce & Celebrate — Timing Matters More Than Magnitude.
Step 5 of 6 ⏱ Immediate — within 3 seconds of behavior. Celebrate the attempt, not just the perfect execution. You are building the behavior, not auditing it. Verbal Praise — Always "YES! You asked for help — that is exactly what we do!""BRILLIANT! You used your break card instead of running!""I saw you choose to ask instead of hit. That's YOUR new superpower." Natural Consequence — Always Give the item they asked for; grant the break they requested. This teaches: "The alternative WORKS. It gets me what I need." Token Economy 1 token = used alternative behavior. 3 tokens = 5-min preferred activity. 5 tokens = choice from reinforcement menu. Token Board ₹364 | Premium ₹589 Social Celebration High five, hug (if tolerated), thumbs up. A child who tries to hand the card but doesn't quite manage it yet deserves a "good try!" + guided completion + full reinforcement. FREE National Autism Helpline: 9100 181 181 | pinnacleblooms.org | ABA Reinforcement Principles: Immediate, specific reinforcement increases behavior occurrence. | BACB Ethical Guidelines

"Two more times, and then we're all done for today." [After 2 trials:] "All done! Great work today."
- Child-led play for 3–5 minutes
- Preferred sensory activity (swing, squeeze, brush)
- Snack or hydration
- Quiet book time
- Outdoor movement
- Do not force an abrupt ending
- Offer 1 more choice: "One more or all done?"
- Use a visual timer if the child responds to it
- Deliver a preferred item upon successful transition

Alternative used: ___ times (any prompt level)
Problem behavior: ___ times
Today's mood: 😐😊😄
- Frequency of alternative behavior use per day
- Frequency of problem behavior per day
- Prompt level needed — full model → gesture → verbal → independent


- Use picture exchange (PECS) or AAC device as the replacement
- One symbol = one function (HELP picture = request for help)
- Accept any approximation: pointing, reaching, vocalizing toward the card
- Move to verbal problem-solving scripts: "What can I do when...?"
- Introduce the problem-solving framework
- Practice in abstract scenarios, not just lived situations
- Calm-down alternatives must provide EQUIVALENT sensory input
- If child hits for proprioceptive input: replace with heavy work (push-ups, carrying, wall push)
- Reduce the intensity of the practice scenario — high arousal blocks alternatives
- Run practice in neutral emotional context, never when escalated
- Ages 2–4: Single picture, single word or gesture. Maximum 1 alternative per session.
- Ages 5–7: 2–3 word phrase + picture. 2–3 scenarios per session.
- Ages 8–12: Verbal scripts, problem-solving frameworks. Self-monitoring tools.

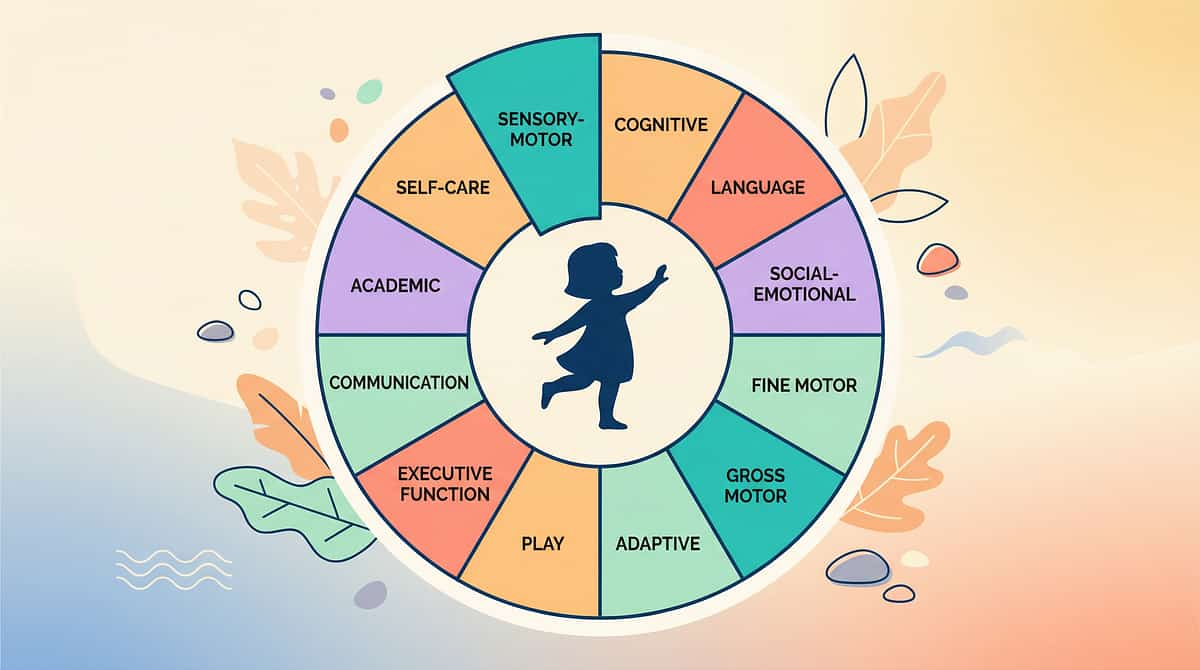
Progress in Weeks 1–2 Looks Nothing Like Mastery — And That's Exactly Right
Progress Arc — Week 1–2 ✅ What You WILL See Child notices the Instead Of card or material when you present it One or two unprompted attempts at the alternative (even imperfect) Slight reduction in intensity (not necessarily frequency) of problem behavior Increased tolerance for the teaching session itself ⏳ What You Will NOT See Yet Spontaneous use of the alternative without prompting Complete cessation of the problem behavior Generalization to other settings or caregivers "If your child tolerates the role-play for 90 seconds longer than last week — that is real, measurable neural progress. The brain is beginning to register a new option." Parent Milestone — Week 2: You have delivered this consistently. That alone is the intervention. Most parents experience hope mixed with doubt at this stage. Keep the data. The data will reassure you when your feelings can't. | PMC11506176



You spent weeks watching your child struggle with behaviors that seemed impossible to change. You learned the science. You gathered the materials. You practiced when you were tired, when sessions didn't go perfectly, when you doubted whether anything was working.
And then it worked.
Your child reached for the card instead of hitting. Your child said "I need a break" instead of running. Your child handed you the HELP card and waited.
That is not a small thing. That is a new neural architecture. That is your child's future — and you built it.

More Tools in Your Behavior Support Arsenal
The materials you've already gathered for D-360 — Calm-Down Kit, Token Board, Communication Cards, Instead Of Charts — cover four of the six related techniques below. Your investment compounds. Technique Code Difficulty Materials You Already Have Self-Regulation Skills D-358 🟡 Core Calm-Down Kit ✓ Consistent Responses D-359 🟢 Intro Token Board ✓ Environmental Structure D-361 🟡 Core Prompt Cards ✓ Antecedent Interventions D-362 🟡 Core Visual Schedules Functional Communication Training D-375 🔴 Advanced Communication Cards ✓ Token Economy Systems D-380 🟡 Core Token Board ✓ Browse Full Behavior Domain →

The Shift: His BCBA did a functional assessment. The function was access — he wanted the toy. We taught him to say "my turn please" using a picture card. Reinforced every attempt. Immediately. Within 3 weeks, hitting dropped 70%.
After: By week 6, Arjun was using "my turn please" spontaneously — at home, at school, at his cousin's house. His BCBA called it generalization. We called it a miracle.
— Parent, Pinnacle Hyderabad | Illustrative case; outcomes vary
The Shift: The scream was an escape behavior. We taught her to raise her hand and say "I need help please" or hand us a break card. Gave the break immediately, every time, without negotiation.
After: Eight weeks later, she raises her hand when she's stuck. The screaming occurs maybe once every two weeks on very difficult days. But the skill is real.
— Parent, Pinnacle Bengaluru | Classic FCT protocol response
"The families who see the fastest results are the ones who stop focusing on the problem behavior and start obsessing over the alternative. The child isn't choosing to be better — they're choosing the better deal." — BCBA, Pinnacle Blooms Network

You Are Not Doing This Alone. There Is a Community Waiting.
📱 WhatsApp — Teaching What TO Do Strategies Parents specifically working on replacement behavior teaching. Share wins, troubleshoot failures, and ask questions in real time. Join WhatsApp Group → 💬 Pinnacle Online Parent Forum Longer discussions, resource sharing, therapist Q&A threads, weekly live sessions with Pinnacle BCBAs. Join Forum → 📍 Local Pinnacle Parent Meetups Monthly in-person meetups at 70+ Pinnacle centers across India. Find your city. Find Nearest Meetup → 🤝 Peer Mentoring Parents who have completed D-360 and are 6+ months into the journey. Real experience, no clinical distance. Request a Peer Mentor → "If this page helped you, your story could be the one that helps the next family find the courage to start. Consider sharing your journey." | WHO NCF: Community engagement is a core principle. Parent support networks improve intervention adherence and outcomes. | FREE National Autism Helpline: 9100 181 181
Need | Specialist | How to Access | |
Functional Behavior Assessment | BCBA / ABA Therapist | In-clinic or teleconsultation | |
AAC / Communication Card Setup | Speech-Language Pathologist | In-clinic or home visit | |
Sensory-based alternatives | Occupational Therapist | In-clinic | |
School generalization plan | Special Educator | Home/school coordination | |
Medical evaluation (if needed) | NeuroDev Pediatrician | In-clinic |
Study | Finding | Link | |
NCAEP Evidence-Based Practices (2020) | FCT is an evidence-based practice for autism across all ages | ncaep.fpg.unc.edu | |
World J Clin Cases (2024), 24 studies | Alternative skill teaching showed significant improvement in problem behavior, communication, and social participation | ||
Children (2024), 16 articles | Behavioral interventions meet EBP criteria for ASD across 2013-2023 | PMC11506176 | |
Indian J Pediatr (2019) | Home-based behavioral skill teaching with parent training: significant outcomes in Indian pediatric population | DOI: 10.1007/s12098-018-2747-4 | |
WHO CCD Package (2023) | Home-based caregiver-delivered interventions effective across 54 low- and middle-income countries | PMC9978394 |
- Which of the 9 materials produces fastest replacement behavior acquisition for this child's profile
- Optimal reinforcement schedule for this child's reinforcer preferences
- Generalization trajectory — when to introduce the next environment
- Red flag detection — early identification of stalled progress requiring professional review
- All data is encrypted at rest and in transit
- Individual child data is never shared without consent
- Aggregate (anonymized) patterns improve all 70,000+ technique recommendations
- DPDPA (India) compliant | GDPR aligned for international families
"Your data helps every child like yours. When 20 million sessions converge, the intelligence becomes sovereign-grade — capable of predicting, preventing, and accelerating outcomes no single clinic could see."

"The most important shift in behavior support is moving from 'stop doing that' to 'do this instead.' Every challenging behavior is a child's attempt to meet a need. Your job isn't to take away their tool. It's to give them a better one." — Pinnacle Behavior Specialist

"We're using D-360 — Teaching What TO Do. Instead of 'don't hit/don't scream/don't grab,' we're teaching [child's name] what to do INSTEAD.
• Wanting something → hand HELP card or say "may I have a turn"
• Frustrated → squeeze stress ball or say "I need a break"
• Needs something → point to the picture card
EVERY TIME they use the alternative: praise immediately + give what they asked for. DON'T give attention/items after the problem behavior. Consistency is the medicine."


You Have Everything You Need. Start Today.
Every day of consistent practice is a day the neural pathway gets stronger. You don't need perfect conditions. You need today's 10 minutes, today's materials, and today's willingness to try. 🚀 Start This Technique Today Launch a GPT-OS® guided D-360 session — personalized to your child's profile and today's readiness level. Start Now → 📅 Book a BCBA Consultation Professional protocol setup and troubleshooting in 30 minutes. In-clinic or teleconsultation available. Book Now → → Explore Next: D-361 Environmental Structure — the next technique in the Domain D pathway. Proactively design your home to prevent problem behaviors before they start. D-361 → ✓ Validated by BCBA • SLP • OT • SpEd • NeuroDev Pediatrics | ✓ Evidence-Grade: Level I | NCAEP 2020 | BACB Standards | ✓ 20M+ Sessions | 97%+ Measured Improvement | 70+ Centers | FREE National Autism Helpline: 9100 181 181 | Available 24x7 | 16+ languages
Preview of 9 materials that help teaching what to do Therapy Material
Below is a visual preview of 9 materials that help teaching what to do therapy material. The pages shown help educators, therapists, and caregivers understand the structure and content of the resource before use. Materials should be used under appropriate professional guidance.




















Share this resource
Help others discover this
We exist to transform every home into a proven, scientific, 24x7, personalized, multi-sensory, multi-disciplinary, integrated pediatric therapy environment — for every family, in every economic condition, in every geography. No child should have their potential limited by access to clinical expertise. GPT-OS® is our answer. — Pinnacle Blooms Network®