
"My daughter flaps her hands at home — and honestly, I find it kind of endearing. It's just her thing. But at school, in crowded places, or when something unexpected happens, the flapping becomes something different entirely. Her whole body gets involved. She rocks violently, hums so loudly, covers her ears and shakes. It's like her normal stimming gets dialled to 100 when she's stressed. The teachers say it's disruptive. But I can see she's not trying to disrupt — she's trying to cope. She can't tell me what's wrong in those moments. The stimming IS her telling me something is wrong. I don't want to stop her. I know she needs it. But I want to help her feel less stressed so her body doesn't have to work so hard alone." — A mother, navigating this with love















Commercial Material | DIY / Household Alternative | Why It Works | |
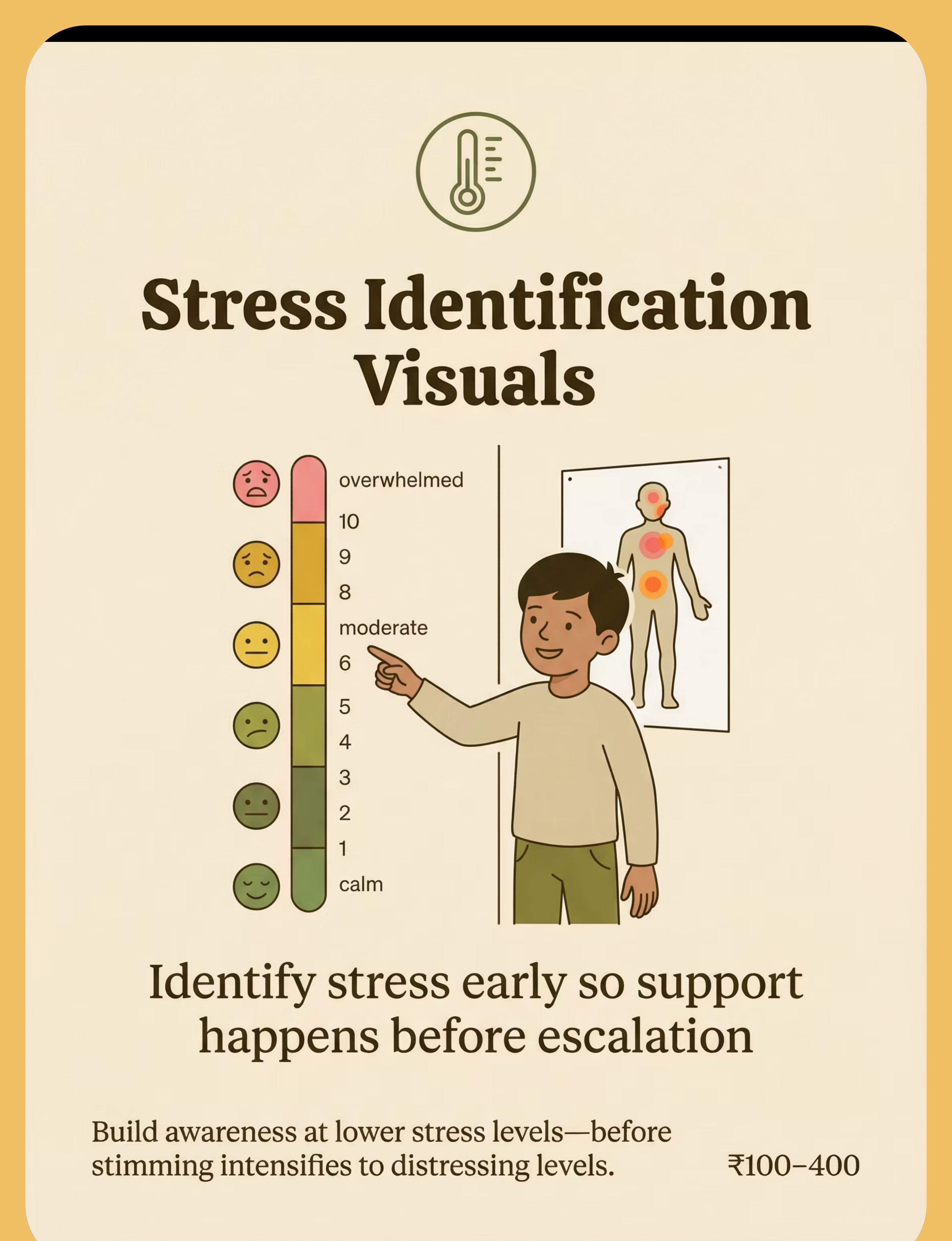
Stress Thermometer | Draw a 1–10 scale on cardboard with emojis; laminate with tape | Visual representation of internal state — identical function | |
Portable Sensory Kit | Small ziplock bag: rubber eraser, smooth stone, fabric swatch, dried pasta for texture | Variety of tactile input — core regulatory principle unchanged | |
Weighted Lap Pad | Fabric pouch filled with rice or dried lentils (~500g–1kg); stitch closed | Proprioceptive deep pressure — same neural mechanism | |
Compression Vest | Snug-fitting undershirt or thin wetsuit top; firm hug from caregiver | Deep pressure to trunk — same vagal activation | |
Calm-Down Space | Corner of room with bedsheet draped over two chairs; add cushion and one fidget | Environmental refuge — spatial containment triggers calm | |
Therapy Swing | Hammock between doorframe hooks; towel swing held by parent | Vestibular input — linear swinging activates calming circuits | |
Noise-Canceling Headphones | Tightly fitted soft earmuffs from hardware store (~₹150) | Auditory reduction — reduces sensory overload trigger | |
Visual Schedule | Photos printed on phone, arranged in sequence on refrigerator with magnets | Predictability — cognitive load reduction regardless of format | |
Co-Regulation Card | Handwritten card: "I need you" with hand-drawn heart | Communication bridge — the message, not the medium, matters |


Set Up Your Space: The Regulation Environment
Spatial precision prevents 80% of session failures. This setup takes 5 minutes and changes everything. Lighting Warm, soft. Dimmer preferred. Overhead fluorescents OFF. Draw blinds to 50% — soft filtered light only. Your nervous system is light-sensitive under stress — your child's even more so. Sound Less than 50dB ambient. White noise at 40dB if needed. Remove ticking clocks, loud ventilation fans, or unpredictable sound sources. Auditory predictability is as important as auditory volume. Temperature & Seating 22–24°C. Cooler is better for regulation. Child at floor level or low seating. Parent at same height — not above, not looming. This one adjustment signals safety before a word is spoken. Visual Environment Remove: screens/devices (unless used as auditory tool) · high-clutter visual surfaces · other people (siblings, visitors) during initial protocol · strong smells · multiple competing colors. Material Positions Sensory kit on low shelf accessible to child · calm space corner with bean bag and weighted blanket folded and ready · visual schedule at eye level · timer visible to child · movement tool centered in available space · auditory tools (headphones) within reach.

60-Second Pre-Session Assessment: Is Your Child Ready?
"The best session is one that starts right." Check each indicator honestly. This takes 60 seconds and sets the entire session trajectory. Indicator GREEN ✅ AMBER 🟡 RED ❌ Current stress level 1–4 (calm to mildly elevated) 5–6 (noticeably stressed) 7–10 (escalating/crisis) Last meal Within 2 hours 2–3 hours ago >3 hours / hungry Sleep last night Adequate (age-appropriate) Slightly reduced Significantly poor Recent stressor None in last 2 hours Minor stressor Major stressor/meltdown Child's engagement signals Eye contact, receptive posture Passive, neutral Avoidance, turning away Your (caregiver) state Calm, regulated Mildly stressed Significantly stressed Medical status Fully well Minor sniffles Unwell/fever 🟢 ALL/MOSTLY GREEN → PROCEED Move to Step 1: The Invitation 🟡 2–3 AMBER → MODIFY Soft materials only · No new introductions · 5–10 minutes max · Focus on co-regulation presence 🔴 ANY RED → POSTPONE Offer water, snack, comfort item · Sit near without demands · Wait 20–30 min and recheck · "Session abandonment is not failure — it's data"

"Hey [child's name]. I can see things feel big right now. That's okay. I'm right here with you. Would you like to try something that might feel nice?"
😐 No clear response, not avoiding → Stay present 30 more seconds
🚫 Turns away, covers ears, vocalizes distress → Offer calm presence only; do not introduce material

If child is currently... | Start with... | |
Hand-flapping intensely | Sensory kit — tactile fidget that matches hand input | |
Rocking hard | Wobble cushion OR guide toward rocking chair | |
Covering ears / vocalizing | Noise-canceling headphones + calming playlist (offer, don't place) | |
Biting hands | Chew tube — hold near their mouth, let them take it | |
Pacing / moving constantly | Clear a path; let them pace; place weighted lap pad on route | |
Curled in corner | Sit near. Offer weighted blanket. Don't speak. Just be. |
"I've got this [name of tool]. Sometimes it helps when things feel big. Want to try it? You can hold it."


Material | Target Duration | Satiation Signal | |
Stress Scale check-in | 1–2 times per session | Child stops engaging with scale | |
Sensory fidget | Continuous 5–10 min | Child puts tool down voluntarily | |
Weighted lap pad | 10–20 min continuous | Child removes it or shifts uncomfortably | |
Chew tool | As needed during session | Child stops chewing and sets aside | |
Calm space | Child-directed duration | Child emerges voluntarily | |
Swing/movement | 10 min rhythmic; 3–5 min vigorous | Child slows movement, climbs off | |
Headphones | As needed; child-controlled | Child removes them | |
Visual schedule reference | 2–3 times during session | Child references independently | |
Co-regulation presence | Full session duration | Child moves away independently |


"We're almost done with our regulation time. Two more minutes, and then we're all done." (Set visual timer. Child watches the time drain — predictability in the transition itself.)


Dimension | EASIER (Start Here) | STANDARD | HARDER (Mastery) | |
Stress Scale | Parent-guided: "Is this how you feel?" with pointing | Child points independently | Child rates verbally without visual | |
Sensory Kit | Parent offers one item | Child chooses from two items | Child independently retrieves kit and selects tool | |
Calm Space | Parent accompanies to space | Parent guides child to door | Child independently transitions when stressed | |
Visual Schedule | Parent reads schedule aloud together | Child references with prompt | Child references independently before transition |



🌳 Weeks 5–8: The Regulation System Is Operating
Progress Arc · Weeks 5–8 This is the phase where the work becomes visible, measurable, and undeniable. Use these specific criteria to assess mastery. Mastery Criteria Observable Behavior Independent stress identification Child uses stress scale without prompt 3+ times per week Independent tool access Child retrieves sensory kit or goes to calm space without adult guidance ≥50% of opportunities Stimming intensity reduction Stress-stim intensity ≤6/10 during previously 9/10 stressor situations Recovery time Post-stressor regulation achieved within 15 minutes vs. 45+ minutes at baseline Safe alternative use Self-injurious stimming reduced ≥70%; child redirects to safe alternative independently Generalization Regulation skill demonstrated in ≥2 environments (home + school, or home + community) ≥4/6 Criteria Met Progress to D-381 (Anxiety-Related Behaviors) — you have built the regulatory foundation. 2–3/6 Criteria Met Stay at D-380 and strengthen with professional OT support. You are close — targeted support accelerates the final gap. Fewer than 2/6 Met Schedule AbilityScore® assessment via 9100 181 181. Additional professional profiling will unlock the specific gap.

"You didn't just teach your child regulation tools. You taught yourself to see their stimming differently — as communication, as neurology, as the body's intelligence. That shift in you will change their life more than any single technique."


Technique | Focus | Difficulty | Materials You Have | |
D-378 | Sensory Seeking Behaviors | 🟡 Core | Core Fidget Kit, Movement Tools | |
D-379 | Sensory Avoidance Behaviors | 🟡 Core | Visual Schedule, Headphones | |
D-381 | Anxiety-Related Behaviors | 🟡 Core | Stress Scale, Co-Regulation Tools | |
D-382 | Transition-Related Behaviors | 🟢 Intro | Visual Timer, First-Then Board | |
D-385 | Safe Stim Alternatives Deep-Dive | 🔴 Advanced | Chew Tools, Fidgets | |
D-390 | Self-Regulation Skills Full Protocol | 🔴 Advanced | All D-380 Materials |

Your Questions, Answered by the Pinnacle Consortium
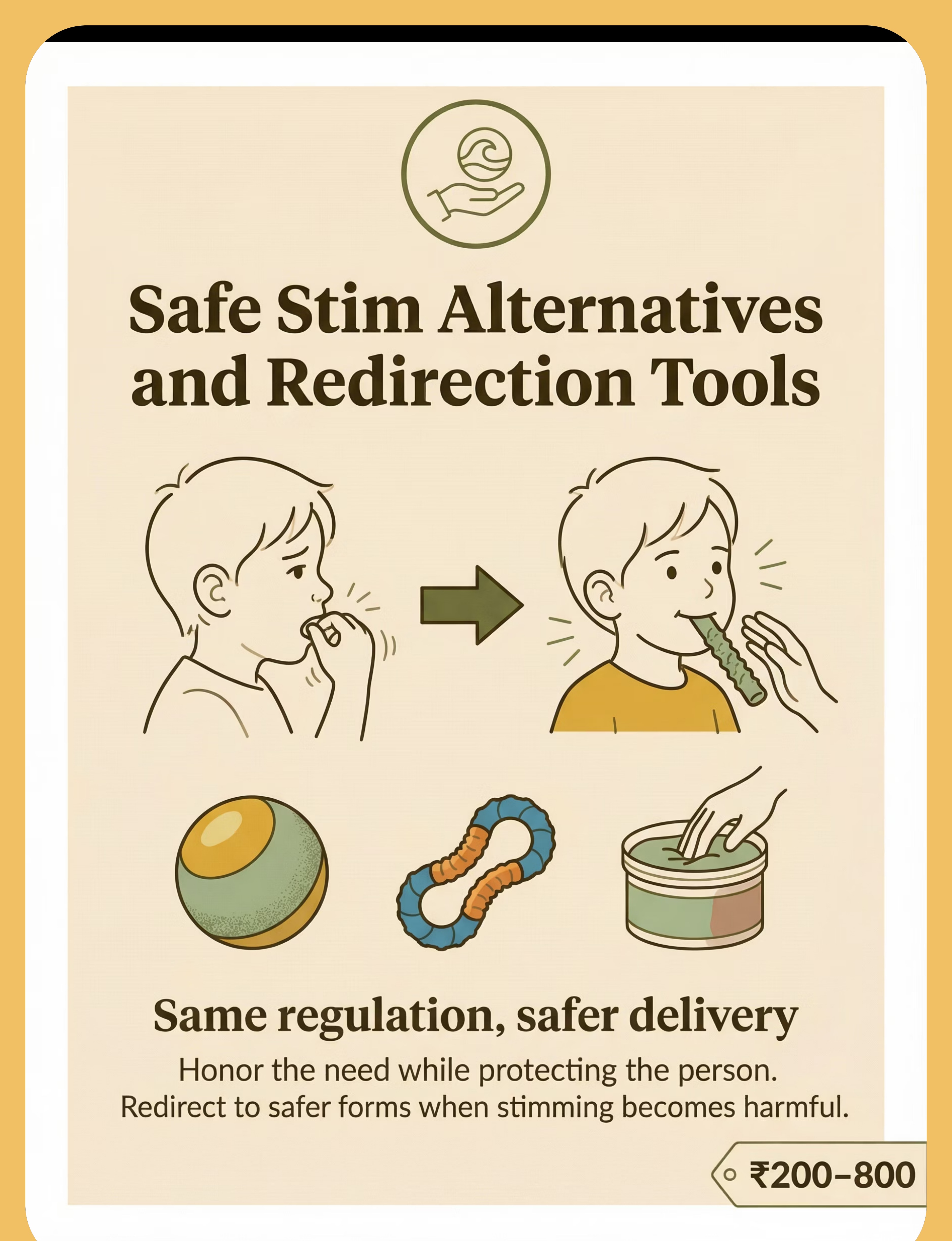
Generated from actual parent queries at Pinnacle centers and the online community. These are the questions every family asks. ❓ Should I try to stop my child's stimming? No — and this is the single most important thing you can take from this page. Stimming is a healthy, adaptive regulatory mechanism. Suppressing it causes harm — it forces the nervous system to regulate without its primary tool, often leading to anxiety, meltdowns, or internalized distress. Redirect to safer alternatives ONLY when the stim is causing physical injury. ❓ How do I know which of the 9 materials to start with? Start with the Portable Sensory Kit and Calm-Down Space — these two provide the broadest coverage. Add weighted tools if your child shows proprioceptive-seeking stims (rocking, crashing). Add auditory tools if sound is a primary trigger. Add stress identification visuals when your child is regulated enough to learn them. Layer — don't introduce all 9 at once. ❓ My child refuses every tool I offer. What do I do? Tools are being introduced at peak stress (too late) or haven't been paired with positive experience. Introduce every tool during calm, low-demand play time first. Let the child explore freely with no expectation. After 2 weeks of positive exposure, offer during low-level stress. Never introduce a new tool during a crisis moment. ❓ How long will this take to show results? Weeks 1–2: tolerance. Weeks 3–4: pattern formation. Weeks 5–8: measurable reduction. Full independent self-regulation: 3–6 months with consistent practice. Individual variation is significant — children with higher sensory processing needs may need more time. ❓ My child's stimming has become self-injurious. Is this a failure? Absolutely not — it is a signal. Self-injurious stimming indicates the stress load exceeds the current regulation capacity. It requires immediate professional assessment (OT + BCBA) to identify the function and implement a safe alternatives protocol. It is NOT a measure of your parenting or your child's character. Call 9100 181 181 today. ❓ Is it okay for my child to stim at school? Yes — stimming is a regulation need, not a behavior problem. Schools are legally required to accommodate diagnosed sensory needs (under RPWD Act 2016 in India). Subtle fidgets, quiet space access, and headphone permission are standard reasonable accommodations. Use the school communication template on the Share card to request these. ❓ Can my neurotypical child use these materials too? Yes — regulation tools benefit all nervous systems. Fidgets, weighted lap pads, calm-down spaces, and visual timers are used in general education classrooms worldwide. Any child under high stress will benefit from these supports. Ask GPT-OS® → Book a Teleconsultation → 9100 181 181
Preview of 9 materials that help with stress increased stimming Therapy Material
Below is a visual preview of 9 materials that help with stress increased stimming therapy material. The pages shown help educators, therapists, and caregivers understand the structure and content of the resource before use. Materials should be used under appropriate professional guidance.

















Share this resource
Help others discover this