
"My child has to have everything exactly the same, every single time. The same route to school — if I take a different turn, complete meltdown. The same cup for milk — if it's in the dishwasher, crisis. The same bedtime routine — skip one step, an hour of screaming. We can't travel. We can't have people over. We walk on eggshells trying to keep everything exactly the same to avoid the next explosion. But we can't keep the world the same forever."

"When your child melts down because you took a different route to school, they are not being dramatic. Their amygdala fired a genuine distress signal. The brain said 'threat.' They responded the way any of us respond to a threat — with fight, flight, or freeze."

Study | Key Finding | |
NCAEP 2020 Report | Visual supports classified as Evidence-Based Practice for ASD | |
PMC11506176 (2024 PRISMA) | Visual schedule interventions show significant reduction in transition-related behavior across 16 studies | |
PMC10955541 (Meta-analysis, 2024) | Sensory regulation interventions improve behavioral flexibility across 24 studies | |
Padmanabha et al., 2019 | Home-based interventions demonstrate equivalent outcomes to clinic-based when parent-trained | |
WHO/UNICEF CCD Package | Multi-caregiver, structured visual intervention across 54 LMICs confirms generalizability |

Age Range | 2–12 years | |
Setting | Home + School + Community | |
Frequency | Daily integration (not discrete sessions) | |
Duration | Long-term — 6–18 months for significant flexibility gains |


- Tolerance for announced changes (showing change card without meltdown)
- Transition smoothness between activities (using timers without resistance)
- Coping strategy initiation during distress (independently reaching for toolkit)
- Reduction in meltdown intensity and duration
- Reduction in family avoidance behaviors ("walking on eggshells" index)
- Increased parental confidence in introducing variation
- Generalization of flexibility to school and community settings
- Interoceptive awareness (recognizing own regulation state)
- Executive function development (set-shifting, cognitive flexibility)
- Anxiety management capacity (generalizable beyond sameness contexts)
- Social participation (events, visitors, travel)





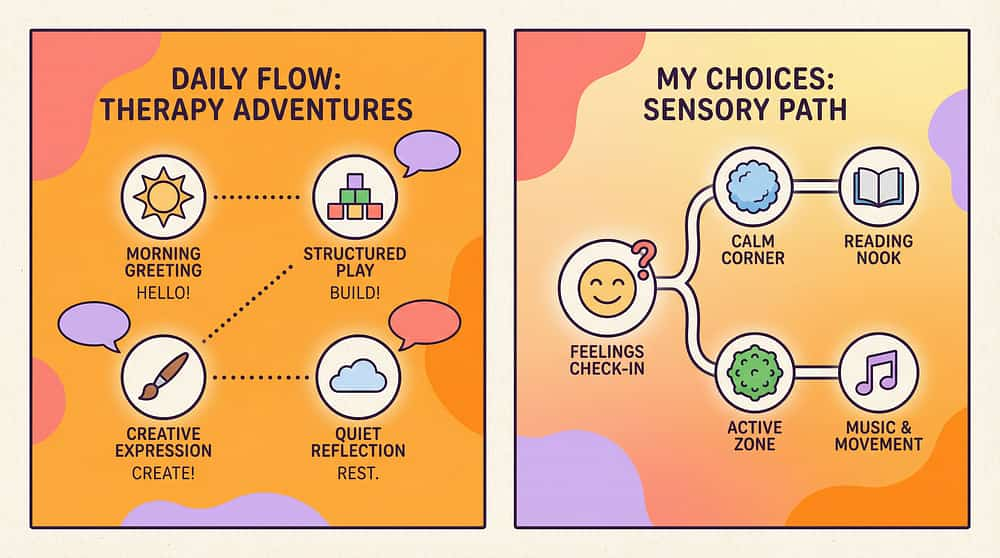




"These strategies must work for families in Nagpur and in New York, in a village with no Amazon delivery and in a city with same-day shipping. The neuroscience works regardless of the price of the tool." — WHO/UNICEF Equity Principle

- Child is currently in meltdown or severely dysregulated
- Child has not eaten or is sleep-deprived
- Child shows signs of illness (sensory sensitivity heightens)
- Rigidity appears to be OCD-driven (compulsive rituals, washing, checking) — requires specialist pathway
- Any flexibility intervention causes self-injurious behavior or aggression
- Child had a difficult morning (use simplified version; skip flexibility games today)
- Sibling conflict or household stress is elevated (maintain core routines; postpone flexibility practice)
- New medications recently started (monitor for behavioral changes before introducing new materials)
- Child is fed, rested, regulated
- No recent major disruptions (illness, move, school change)
- Core routine is established and predictable (do not introduce flexibility before the routine feels safe)
- Comfort object is accessible throughout
- Never introduce new materials during a meltdown
- Never remove comfort object as "motivation" for flexibility
- Never flood the child with multiple changes simultaneously
- Never punish rigidity — it escalates anxiety and rigidity
- Seek professional evaluation if rigidity causes harm to safety/health/nutrition

- ☐ Visual schedule mounted at child's eye level
- ☐ Comfort object within child's reach at all times
- ☐ Calming toolkit bag accessible (not hidden away)
- ☐ Timer visible to child
- ☐ First-Then board ready with current activity pictures
- ☐ Worry box within reach for anticipated changes
- ☐ Screens OFF during flexibility practice sessions
- ☐ Predictability cards prepared for any known upcoming changes
- ☐ Quiet, low-sensory environment (reduce ambient noise/light if possible)
- ☐ YOU are calm — your regulation co-regulates theirs




Game | What Changes | Stakes | |
Opposite Day | One small thing reversed (different chair, different cup) | Zero — it's playful | |
Story Twist | Change the ending of a familiar story | Low — fiction | |
Role Reversal | Child plays parent for 5 minutes | Low — fun | |
Surprise Box | Pick from a box of silly tasks (make an animal sound, wear glasses) | Low — silly | |
Game Rule Change | Take existing game, change one rule | Low — child can decide |
"You just did something different! That's what flexible thinkers do!"

- Review today's visual schedule together
- Name any changes on the schedule
- "Is there anything you're worried about today?" → child draws or writes it → places in worry box
- Review change journal: "Look how many changes you've already survived!"
- Pack calming toolkit if going out
- Review what happened today
- Note any changes encountered and how child coped
- Add to change journal: Date | What changed | How I felt | What helped | What happened
- Celebration: "That was different from usual. You handled it."
- Read social story if tomorrow has a known change
"Every entry is evidence. The journal proves — to your child and to their nervous system — that changes have been survived before. This is your child's personal scientific dataset of flexibility."


- Change card shown today? (Y/N)
- Child's distress level during change: 1 (none) → 5 (severe meltdown)
- Calming toolkit used? (Y/N)
- Flexibility game played today? (Y/N)
- One flexibility win today (free text)
- Worry box used today? (Y/N)
- Predictability card used today? (Y/N)

Problem | Solution | |
Child destroys or ignores visual schedule | Make it more concrete (real photos vs. icons); involve child in making it; place at exact eye level | |
Social stories increase anxiety for days before change | Shorten lead time; introduce story day-of, not days before; simplify language | |
Calming toolkit is rejected during distress | Toolkit was not practiced enough during calm; reintroduce during 100% calm play sessions first | |
Timer causes more meltdowns | Timer was introduced for high-demand transitions first; start with timers for transitions TO preferred activities | |
Flexibility games trigger real distress | Stakes are too high; try even smaller changes; return to 100% routine for one week before trying again | |
First-Then board is refused | The THEN item is not motivating enough; ask child directly what they want | |
Change journal becomes rumination | Stop reviewing journal entries before sleep; use only as celebration, not analysis |

- Child examines visual schedule (curiosity replaces immediate refusal)
- Comfort object is carried more deliberately
- One transition completes with timer (even if reluctantly)
- Child puts one worry in worry box
- Smooth transitions without distress
- Accepting changes without protest
- Requesting flexibility games
"If your child looked at the change card for 3 seconds before melting down (vs. immediately melting down before) — that is real, measurable neural progress. You are watching a brain learn."
"You may also notice YOU are more confident. That shift in parent confidence is itself therapeutic — co-regulation flows both ways."


"These are not small moments — they are neurons firing new pathways."


Technique | Domain | Difficulty | Materials Overlap | |
D-371 Transition Difficulties | Behavioral | Intro | Timer, First-Then | |
D-372 Routine Dependence | Behavioral | Intro | Visual Schedule | |
D-374 Flexibility in Play | Behavioral | Core | Flexibility Games | |
D-375 Adapting to New Situations | Behavioral | Core | Predictability Cards | |
C-250 Emotional Regulation | Emotional | Core | Calming Toolkit | |
D-380 Anxiety Management | Behavioral | Advanced | Worry Box, Social Stories |

"Our son's rigidity controlled our entire family. We couldn't go anywhere, change anything, or have people over. Meltdowns were daily. We started with the visual schedule and change cards — just that first, nothing else. After three weeks, he started looking at the schedule before I showed him. That was the first sign. We added the calming toolkit next. Then social stories. Gradually, he stopped refusing to hear about changes. He started asking 'what will happen?' instead of shutting down. The worry box became his idea — he'd bring us worries we didn't even know he had. After a year, we took our first family trip in three years. He was anxious. He used his toolkit on the plane. He had his comfort bunny. We'd built a predictability sequence for the hotel. He coped. Not perfectly — but he COPED. He even said: 'That was different. I survived it.' He's still a routine-oriented kid. He always will be. But he's not a prisoner of rigidity anymore. And neither are we."
You Are Not Navigating This Alone.
Whether you're a parent in the middle of a difficult week, a professional seeking clinical support, or a grandparent trying to understand — the Pinnacle community is here. Pinnacle Parent Community 🌐 Connect with parents navigating sameness insistence globally 💬 Share your change journal wins 📱 WhatsApp community: "Behavioral Flexibility Families" 🎯 Weekly GPT-OS® guided flexibility challenge For Professionals Pinnacle Consortium Training Portal EverydayTherapyProgramme™ professional certification GPT-OS® clinical integration pathway FREE National Autism Helpline 📞 9100 181 181 — 24×7, 16+ languagesAvailable to parents, caregivers, educators, and professionals across India and the global diaspora pinnacleblooms.org | care@pinnacleblooms.org


Source | Key Contribution | |
PMC11506176 (2024 PRISMA) | Visual supports in ASD — significant reduction in transition-related behavior across 16 studies | |
PMC10955541 (Meta-analysis, 2024) | Sensory integration + behavioral outcomes — 24 studies | |
NCAEP Evidence-Based Practices Report (2020) | Visual supports classified as Evidence-Based Practice for ASD | |
Padmanabha et al., Indian J Pediatr 2019 | Home-based interventions — equivalent outcomes to clinic-based when parent-trained | |
DOI: 10.3389/fnint.2020.556660 | Neurological basis for sensory interventions (Frontiers in Integrative Neuroscience) | |
WHO Nurturing Care Framework (2018) | Multi-caregiver structured visual intervention across 54 LMICs | |
WHO/UNICEF CCD Package (2023) — PMC9978394 | Global health equity in intervention delivery |

See These 9 Materials in Action.
Watch the D-373 Reel — Behavioral Flexibility in Children Series, Episode 373. Presented by the Pinnacle Blooms Consortium: SLP, OT, BCBA, SpEd, and NeuroDev specialists. 🎬 Reel D-373: "9 Materials That Help With Sameness Insistence" | Behavioral Flexibility Series | Embed video player at: YouTube/Vimeo link to be added at publication What You'll See in This Reel Visual schedule with change card being used in a real home environment Child accessing calming toolkit during a moment of distress — then self-regulating Parent and child reading a social story during calm bedtime routine Visual timer countdown with peaceful transition to next activity Parent and child playing flexibility game together, laughing Child writing in change journal after surviving a change — "I did it" Related Reels D-371 Transition Difficulties D-372 Routine Dependence D-374 Flexibility in Play Research: NCAEP 2020 — Video modeling as evidence-based practice for ASD

Consistency Across Caregivers Multiplies Impact.
"The child who succeeds at home but not at school has only half the intervention. Caregiver consistency is the multiplier." Share this resource with every person in your child's life. 📱 Share with Co-Parents & Grandparents The Quick Explanation: "When [child's name] gets upset about changes, it's not stubbornness. Their brain genuinely feels unsafe when something is different. Here's how to help: (1) Never force a change suddenly. (2) Show them what will happen. (3) Give them the calming bag. (4) Wait. (5) Celebrate when they cope." 📚 Share with Teachers Teacher Communication Template: "Dear [Teacher's name], [Child] uses a visual schedule and change cards to manage transitions. Please provide advance notice of any schedule changes if possible. The calming toolkit in [child]'s backpack is a therapeutic tool prescribed by our therapy team. Please allow access when distress signals appear." 📱 Share via WhatsApp 📧 Share via Email ⬇️ Downloadable Family Guide: One-page PDF summary — "9 Materials for Sameness Insistence — Quick Reference for Every Caregiver" | Research: PMC9978394 | WHO CCD Package — multi-caregiver training evidence

Questions Real Parents Ask Our Consortium.
My child is 10 — is it too late to start? No. While earlier intervention produces faster outcomes, the neuroplasticity required for flexibility-building is present throughout childhood and into adolescence. Children at 10, 11, 12 show measurable gains with consistent visual support and graduated exposure. The tools may need to be more sophisticated — written journals vs. picture journals; self-directed toolkit use vs. parent-prompted. My child insists on sameness about food only. Is this the same? Food-based sameness is often sensory-driven (texture, taste, smell, color, temperature) rather than anxiety-driven. This may require OT evaluation for sensory profile and feeding therapy. Visual schedules and predictability cards still help for mealtimes, but forced exposure to new foods without sensory assessment can increase rigidity. Call 9100 181 181 for guidance. My partner thinks I'm "coddling" the child by accommodating routine. This is one of the most common family conflicts around sameness insistence. Share Card 3 (brain science) with them. The evidence is clear: accommodating core routines while building flexibility at the edges is the evidence-based approach. Forcing change without support does not teach flexibility — it increases anxiety and rigidity. How do I know if this is OCD rather than autism-related rigidity? Key distinction: OCD rituals are performed to NEUTRALIZE a specific fear. Autism-related sameness is about predictability and sensory consistency. A psychologist or psychiatrist should make this distinction — it changes the treatment pathway significantly. Call 9100 181 181 for assessment referral. What if my child refuses ALL 9 materials? Start with the ONE material your child tolerates most. Usually, the comfort object is the entry point — it requires no active engagement from the child. From there, the visual schedule is second. Do not rush. One material, mastered, is worth more than nine materials resisted. How do I handle sameness insistence during travel? Predictability cards are your primary tool. Build a detailed visual sequence of the journey. Carry comfort object. Research the destination in advance (hotel room photos, restaurant photos). Start with short trips (1 night, familiar destination) before longer journeys. Each successful trip adds to the change journal. Does medication help? Medication for co-occurring anxiety (if clinically assessed) may reduce the severity of the anxiety component driving sameness insistence, making behavioral interventions more effective. This is a clinical decision requiring psychiatry/NeuroDev evaluation. Materials-based intervention is recommended with or without medication. 📞 9100 181 181. How do I explain sameness insistence to my child's school? Use the teacher communication template from Card 37. The key message: this is a neurological difference requiring visual supports and advance preparation — not a behavior management issue. IEP/504 accommodations can formalize this. Our SpEd team can provide documentation support. Didn't find your answer? Ask GPT-OS® Book a Teleconsultation

Preview of 9 materials that help with sameness insistence Therapy Material
Below is a visual preview of 9 materials that help with sameness insistence therapy material. The pages shown help educators, therapists, and caregivers understand the structure and content of the resource before use. Materials should be used under appropriate professional guidance.




















Share this resource
Help others discover this
"From fear to mastery. One technique at a time. We exist to transform every home into a proven, scientific, 24×7, personalized, multi-sensory, multi-disciplinary integrated therapy center — for every child, in every country, regardless of economic circumstance. This is not a service. This is a system. This is GPT-OS®."
CIN: U74999TG2016PTC113063 | DPIIT: DIPP8651 (Govt. of India) | MSME: TS20F0009606 | GSTIN: 36AAGCB9722P1Z2