
"She checks the locks again. And again. And again."
Your child is eight years old. She's running disaster scenarios like a safety coordinator. She follows you room to room. She can't sleep without knowing you're alive. And every reassurance you give? Gone in five minutes. This isn't a behavior problem — it's a worried brain that needs tools, not reassurance.

C-287 | ANX-SAF
Quick Navigation
C-287 | Safety Worry Management
9 Evidence-Based Materials for Worried Brains — Navigate directly to the section you need.
🧠 Why It Happens
The neuroscience of safety anxiety — what's happening in your child's brain
📚 What It Is
Technique definition, disciplines, targets, and all 9 materials explained
▶️ How To Do It
Step-by-step session protocols for every material
📈 Progress Tracker
Week-by-week milestones, red flags, and the full pathway map
🌍 Community
Family stories, professional support, and the Pinnacle ecosystem
❓ FAQ & Start
Common questions, your next step, and the Pinnacle Promise
Domain Badge: ANX-SAF | Anxiety & Emotional Regulation | Age 4–12 | Series Badge: Episode 287 | Anxiety & Emotional Regulation Support Series

ACT I — Recognition
This Is Happening in Millions of Homes Right Now
Childhood safety anxiety is not rare, and you are not failing. The numbers tell a clear story — and they call for evidence-based tools, not more reassurance.
1 in 3
Children with Neurodevelopmental Differences
Experience clinically significant anxiety, with safety worries among the most common presentations. Source: JAMA Pediatrics systematic review, 2019
80%
Children with Autism Spectrum Disorder
Experience anxiety features — safety worries, separation fears, and catastrophic thinking are core presentations. Source: PMC11506176 — PRISMA Systematic Review 2024
2.1M+
Indian Families
Navigating childhood anxiety disorders without evidence-based home tools. You are not failing. The system hasn't given you what you need. Until now. Source: NMHS India 2015–16; WHO Mental Health Atlas 2022
In a joint Indian family, the worry doesn't stay with one parent. It travels — to grandparents who reassure endlessly, to siblings who tiptoe around the anxious child, to teachers who see a distracted student. This is a family challenge. These materials are designed for the whole family ecosystem.
Research Anchor: WHO Nurturing Care Framework (2018) | UNICEF MICS developmental indicators | Pinnacle Network: 20M+ therapy sessions, 97%+ measured improvement

ACT I — Development
Normal Worry vs. Worried Brain — Where Is Your Child?
Every child experiences fear. The question is whether your child's worry is developmentally appropriate — or has crossed into a pattern that needs structured support.
Infancy
Separation & loud noise. Fades with caregiver presence.
Toddler
Stranger anxiety. Manageable with transition support.
Preschool
Dark & monsters. Manageable at bedtime. Act if prevents sleep nightly.
School Age 4–12 ← YOU ARE HERE
Safety, catastrophe, parent harm. Occasional "what if" is normal. Act if constant, checking, avoidance, can't reassure.
Adolescence
Social evaluation anxiety. Self-consciousness & peer-related fears.
Key Differentiation: Normal safety awareness responds to reassurance and doesn't significantly impair daily life. Anxiety disorder: reassurance provides minutes of relief, is impairing sleep and school, and is growing — not shrinking.
Comorbidity Awareness: Safety worries co-occur with Autism Spectrum Disorder (80%), ADHD (40%), OCD (distinct but related), and trauma responses. In Indian contexts, joint household dynamics, academic pressure, and early news exposure can amplify. WHO Care for Child Development Package: PMC9978394.

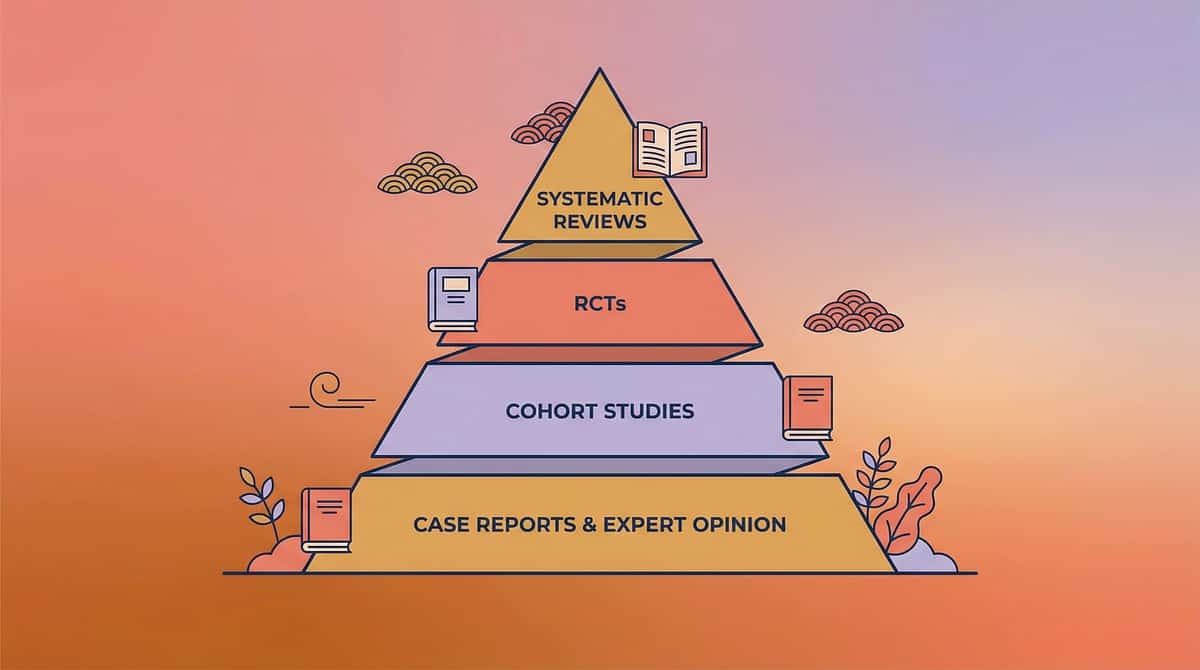
🛡️ Level I Evidence
This Is Not Advice. This Is Evidence.
Every material in this protocol is grounded in peer-reviewed research — not opinion, not anecdote. Here is the science this page stands on.
CBT for Childhood Anxiety
The gold standard. Cognitive-behavioral therapy — incorporating cognitive restructuring, gradual exposure, relaxation training, and parent involvement — is classified as a Well-Established treatment for childhood anxiety by the American Psychological Association. Effect size: Cohen's d = 0.86 (large). PMC2930817 | Kendall et al. Coping Cat Protocol
SPACE Protocol (Parent-Led)
Supportive Parenting for Anxious Childhood Emotions: RCT evidence demonstrates that reducing parental accommodation of anxiety produces significant reduction in child anxiety — even without direct child treatment. This validates parent-led material implementation. Lebowitz et al., 2020, JAMA Psychiatry
Indian Context Evidence
Home-based pediatric interventions in Indian settings demonstrate measurable outcomes. Padmanabha et al., Indian Journal of Pediatrics (2019): Home-based structured interventions show significant functional improvements. DOI: 10.1007/s12098-018-2747-4
Pinnacle Real-World Evidence
20M+ exclusive 1:1 therapy sessions | 97%+ measured improvement across Anxiety Management Readiness Index | 70+ centers | Data from Indian children, Indian homes, Indian families — not extrapolated from Western samples alone.
90%
Evidence Confidence Rating
Based on systematic review quality, RCT replication, and real-world outcome data across 20M+ sessions.

ACT II — The Consortium
The Consortium Behind These Tools
Anxiety doesn't respect therapy boundaries. The worried body needs OT. The worried thoughts need psychology. The worried behavior needs ABA. The worried language needs SLP. This is why Pinnacle operates as a converged consortium — not siloed specialists.
Child Psychologist / CRO
Designs the CBT protocol architecture. Conducts formal anxiety assessment (GAD, specific phobia, OCD differentiation). Delivers cognitive restructuring. Supervises exposure hierarchy.
Pediatric Occupational Therapist
Addresses the sensory-nervous system component. Calm-down kits and grounding tools are OT's domain. For children with ASD + anxiety, sensory regulation MUST precede cognitive intervention.
Pediatric ABA / BCBA
Designs the behavioral exposure hierarchy. Manages reinforcement during Bravery Ladder implementation. Analyzes avoidance patterns and runs data on reassurance-seeking frequency.
Speech-Language Pathologist
Provides language scaffolding: teaches children to identify and name anxious states, builds vocabulary for internal experiences, supports Safety Evidence Journal narratives, and coaches parent-child communication.
Special Educator
School generalization — brings materials to classroom context. Coordinates Worry Time during school hours. Trains school staff on not providing accommodation or reassurance.

ACT II — Targets
Precision, Not Guesswork
These 9 materials don't address anxiety vaguely — they target specific, measurable outcomes across three rings of impact.
Anxiety Management Readiness Index
AbilityScore® tracking domain
Emotional Regulation Readiness Index
AbilityScore® tracking domain
Independence Readiness Index
AbilityScore® tracking domain
Adaptive Coping Readiness Index
AbilityScore® tracking domain
Family Quality of Life Index
AbilityScore® tracking domain

ACT II — Materials Overview
9 Materials. 3 Layers. One Toolkit.
Every material targets a specific layer of anxiety. Begin with the body, then address thoughts, then build brave behavior. Don't try all 9 at once — start with the Calm-Down Kit + one Cognitive tool + Breathing Tools.
🌊 Layer 1: Body Regulation
Start Here. The nervous system must be regulated before the mind can learn. These materials calm first.
- Material 3: Calm-Down Kit with Grounding Tools | ₹400–1,500
- Material 9: Breathing Tools | ₹200–800
🧩 Layer 2: Cognitive Restructuring
Think Different. Challenge the distorted thoughts driving the worry.
- Material 1: Worry Monster / Worry Eater | ₹500–1,500
- Material 2: Thought Challenging Cards | ₹300–800
- Material 4: Safety Evidence Journal | ₹150–400
- Material 6: Coping Cards | ₹100–400
- Material 8: Brave Books / Bibliotherapy | ₹300–800
🪜 Layer 3: Behavioral Exposure
Do the Brave Thing. Face fears in graduated, successful steps.
- Material 5: Bravery Ladder / Fear Hierarchy Charts | ₹200–600
- Material 7: Worry Time Timer + Container | ₹200–500
Total Toolkit Cost: ₹2,350–6,500 (full kit) | ₹650–1,900 (essential starter) | DIY Alternative: ₹0–500 — See Card 11 for zero-cost versions of every material.

Material 1
Externalization
Worry Monster / Worry Eater
Category: Externalization Tools | Price: ₹500–1,500 | DIY: ₹0–200
The Science
Externalizing the worry — giving abstract fear a physical form outside the child — creates cognitive distance. When the worry "lives in the monster," it's not consuming the child's processing capacity. Externalization is a validated CBT technique from the narrative therapy framework.
How It Works
Child writes or draws worry on paper → feeds it into the monster's zippered mouth → zips shut. "The monster holds it now, not you."
DIY Instructions (Consortium OT + SpEd)
Fold a sock, cut a slit for the mouth, glue velcro across the slit. Or use any box/jar with a lid and a slot cut in it. Decorate together — child ownership increases effectiveness. Small paper slips and pencil included.
Safety Note
For children with ASD who may become fixated on the monster as an object — introduce gradually. Never force the feeding ritual.
"Externalization creates distance. When the worry lives in the monster, it's not consuming the child." — Narrative therapy / CBT externalization: White & Epston; integrated in Coping Cat protocol

Material 2
Cognitive Restructuring
Thought Challenging Cards
Category: Cognitive Restructuring | Price: ₹300–800 | DIY: ₹50–100 | Age: Most effective 7+
Safety worries are driven by three cognitive distortions — catastrophizing, probability overestimation, and emotional reasoning ("I feel scared, therefore danger is real"). Thought challenging cards interrupt automatic thought patterns with structured Socratic questioning.
Card 1
"What's the evidence this will happen?"
Card 2
"Has this specific thing happened before?"
Card 3
"What's MORE likely to happen?"
Card 4
"What would I tell a friend who worried about this?"
Card 5
"Even if something difficult happened — could I handle it?"
DIY Instructions (Consortium Psychologist): Create 7 index cards (A6 size), one question per card. Write in the child's own handwriting with them. Laminate for durability. Keep in bedside drawer and school bag. Practice using cards during calm moments — not first during peak anxiety.
"Worried thoughts aren't facts. Cards help children become scientists investigating their own thinking."

Material 3
Sensory Regulation / OT
Calm-Down Kit with Grounding Tools
Category: Sensory Regulation / OT | Price: ₹400–1,500 | DIY: ₹100–400
Anxiety activates the sympathetic nervous system — fight-or-flight. In this state, you cannot reason with an activated nervous system. Grounding tools activate the parasympathetic nervous system through sensory input — redirecting neural resources from the alarm system to the sensory processing system.
5 Things You See
Glitter calming jar (visual focus tool) + photo of safe person/place
4 Things You Touch
Stress ball or fidget toy (tactile) + smooth worry stone (proprioceptive)
3 Things You Hear
Gentle ambient sounds — nature, soft music, or silence
2 Things You Smell
Lavender sachet — proven vagus nerve activation via olfactory pathway
1 Thing You Taste
Coping card as cognitive bridge — grounding to present moment
DIY Instructions: Any basket or box works. Personalize completely to child's sensory preferences. Some children prefer cold (ice pack) for grounding; others prefer warm (heat pack). Test during calm times.
"The body believes before the mind. Calm the nervous system first — then address the thoughts." — Polyvagal Theory (Porges) | Sensory Integration Theory (Ayres) | PMC10955541

Material 4
Cognitive Restructuring
Safety Evidence Journal
Category: Cognitive Restructuring | Price: ₹150–400 | DIY: ₹30–100
Anxious brains have a systematic negativity bias — they notice and remember evidence of danger while filtering out evidence of safety. A Safety Evidence Journal deliberately counteracts this bias by building a physical, datable, verifiable record that the child is safe, that worries don't come true, and that difficult moments pass.
Prompt 1 — Daily Safety
"Today I was safe when..."
Prompt 2 — Worry That Didn't Happen
"Something I worried about that didn't happen today..."
Prompt 3 — Brave Moment
"One brave thing I did today..."
Prompt 4 — Worry Rating
"My worry level today was ___/10. Yesterday it was ___/10."
Over 4 weeks: the child has 28+ entries of safety evidence. When worry spikes — "Look at all these pages of safe days."
Indian Context Note: In joint family settings, grandparents or older siblings can co-write entries with younger children. This builds multigenerational therapeutic alliance. DIY: Any ruled notebook. Print journal prompts as a strip to paste on each page. Add sticker rewards for consistency.
"The evidence comes from their own life — not someone else's promises. Self-generated evidence is more durable than reassurance."

Material 5
Behavioral Exposure / ABA
Bravery Ladder / Fear Hierarchy Chart
Category: Behavioral Exposure / ABA | Price: ₹200–600 | DIY: ₹50–150
Avoidance is the engine that keeps anxiety alive. Every avoided situation prevents the child from learning: "I can handle this, and nothing catastrophic happened." Bravery ladders provide graduated exposure — systematic, mastery-based confrontation of feared situations.
Rung 1
Stay in own room 1 minute — parent visible in doorway
Rung 2
Stay in own room 5 minutes — parent in hallway
Rung 3
Stay until sleepy — parent checks in at 10 min
Rung 4
Fall asleep in own room — parent checks after 15 min
Rung 5
Sleep full night in own room ⭐ MASTERY
Rules: Master each rung before moving up. Celebrate every rung — it's evidence. If a rung is too hard, add an intermediate step. Never force — pace is driven by child's success, not parent impatience.
Professional Guidance Note: Bravery ladders for severe anxiety work best with therapist supervision. Call 9100 181 181.
Professional Guidance Note: Bravery ladders for severe anxiety work best with therapist supervision. Call 9100 181 181.
"The only way out of fear is through it — but through it in small, manageable, successful steps."

Material 6
Cognitive Coping / SLP
Coping Cards + Brave Self-Talk Scripts
Category: Cognitive Coping / SLP | Price: ₹100–400 | DIY: ₹20–80
At peak anxiety, internal access to learned coping strategies fails — the amygdala suppresses working memory. External coping cards serve as memory prosthetics, providing the right words exactly when the internal vocabulary collapses. Child co-creates cards — their language, not clinical terms.
Card A
"My brain is giving me a false alarm. I am SAFE right now."
Card B
"Take 5 breaths. This feeling will pass. It always does."
Card C
"I've been scared before and handled it. I can handle this too."
Card D
"Squeeze my stress ball 10 times. Breathe. Look for 5 things I can see."
Laminate cards. Pocket-sized. One in school bag, one by bed, one on the fridge. Practice during calm times so cards become automatic in crisis.
Indian Multilingual Note: Create cards in Hindi, Telugu, Tamil, or regional language alongside English for multi-caregiver household use.
"In anxiety, the brain forgets what it knows. External coping cards provide the script when internal access is blocked."

Material 7
Worry Containment
Worry Time Timer + Containment Tools
Category: Worry Containment / Scheduling | Price: ₹200–500 | DIY: ₹50–150
Safety worries can colonize every waking moment — a constant background of "what if" that exhausts the child and the family. Worry Time creates a structured daily container: worries get 15 dedicated minutes, not unlimited access to the child's day.
The key insight parents miss: many worries feel smaller by Worry Time. The act of postponing reveals that the urgency was anxiety-generated, not genuine. Containment returns control to the child.
Visual Timer
Time Timer brand or sand timer
Decorated Box/Jar
Child decorates — ownership increases effectiveness
Small Paper Slips
One worry per slip — externalization in writing
Daily Schedule Card
Showing Worry Time (4pm) as visual anchor
"Worries lose power when they can't have unlimited access. Containment returns control to the child."

Material 8
Bibliotherapy
Brave Books / Anxiety-Focused Bibliotherapy
Category: Normalization / Bibliotherapy | Price: ₹300–800 | DIY: ₹0 (library)
Children with anxiety often carry profound isolation — "Nobody else feels this scared all the time." Bibliotherapy uses narrative distance to deliver messages children resist as direct instruction. A character who worries like them, uses a strategy that helps, and gets better — is more persuasive than any therapist or parent saying the same thing.
Protagonist Who Worries
Normalizes excessive worry — the child is not alone or broken
Strategies Shown in Action
Models coping in a story — safer than direct instruction
Gradual Improvement Arc
Not instant cure — realistic, honest progression
Child-Powered Resolution
Resolution through child's own effort — not rescue — builds agency
Reading Protocol (SLP): Read together. Ask after each page: "Do you ever feel like this?" "What helped the character?" "Could we try that?"
Indian Book Recommendation: Tulika Publishers (regional languages), Pratham Books, CBT-focused imported titles from US/UK.
"Stories create distance for learning. Children accept through characters what they resist as direct advice."

Material 9
Physiological Regulation / OT
Breathing Tools
Category: Physiological Regulation / OT | Price: ₹200–800 | DIY: ₹0–100
Controlled slow breathing activates the vagus nerve — the primary pathway of the parasympathetic nervous system. Extended exhale (longer than inhale) is the fastest evidence-based physiological intervention for anxiety: it signals to the autonomic nervous system that threat has passed.
Hoberman Sphere
Inhale = expand, exhale = contract. The visual prevents hyperventilation and paces breathing naturally.
Pinwheels
Blow slowly to make them spin. Immediate visual feedback on breath control.
Bubbles
The physics of bubble blowing requires slow, controlled exhale. DIY: ₹50. Most effective entry point.
Box Breathing
In 4 → Hold 4 → Out 4 → Hold 4. Printed poster for visual reference. 4-7-8 variant for bedtime.
Indian Cultural Integration: Pranayama foundations align with these techniques. For families practicing yoga, this is familiar territory. The breathing exercises in this toolkit are evidence-based extensions of traditional pranayama principles validated by modern neuroscience.
"You can't think your way to calm, but you can breathe your way there. The body leads, the mind follows."

Safety Protocols
Before You Start
Before You Start — Know These Lines
Every session should be safety-checked before starting. This traffic-light system ensures materials are introduced at the right moment — protecting both the child and the process.
🟢 GREEN: Proceed
Child is regulated | No recent meltdown (2+ hours) | Not overtired or hungry | Familiar with the material | Anxiety is mild-moderate today
🟡 AMBER: Modify
Child is elevated but not crisis | Recent mild stressor | First time introducing material | Mild resistance | Parent is also stressed
Protocol: Calm-Down Kit only. Skip cognitive materials. 5-minute maximum. No ladder steps today.
Protocol: Calm-Down Kit only. Skip cognitive materials. 5-minute maximum. No ladder steps today.
🔴 RED: Stop / Postpone
Active meltdown or panic attack | Child dissociating | Aggressive behavior | Severe resistance | Signs of genuine safety threat
Protocol: Regulate first. No materials. Parent presence and co-regulation only. Reschedule tomorrow.
Protocol: Regulate first. No materials. Parent presence and co-regulation only. Reschedule tomorrow.
Contraindications — Seek Professional Assessment First: Worries centered on realistic danger (abuse, bullying) | Compulsive rituals suggesting OCD | Trauma history requiring specialist pacing | Child not eating, sleeping, or showing severe functional impairment
Pinnacle Protocol: FREE AbilityScore® assessment available. Call 9100 181 181 to determine the right starting point for your child's severity.

ACT II — Environment
The Right Environment Makes the Difference
Where your child practices matters as much as what they practice. A designated, consistent, sensory-appropriate space sends the nervous system a powerful signal: this is a safe place for brave work.
🪑 Calm Space
Soft chair or floor cushion — child's designated calm corner. Same space every time.
📦 Calm-Down Kit
Within arm's reach of calm space. Within child's reach — not in adult storage.
📔 Safety Evidence Journal
On bedside table — integrated into the bedtime routine naturally.
🧟 Worry Monster
On shelf, visible but not overwhelming. Child should be able to reach independently.
⏱️ Worry Timer + 🪜 Bravery Ladder
Timer in common family area (4pm station). Ladder poster visible on bedroom wall.
Joint Family Note: In Indian multi-generational homes, assign each key caregiver ONE role. Grandparent holds the Worry Time container. Parent conducts breathing practice. Elder sibling reads Brave Books. This distributes responsibility and multiplies exposure.
Lighting & Sound: Warm lighting during practice. No harsh fluorescents. No TV. Soft ambient sound acceptable.
Lighting & Sound: Warm lighting during practice. No harsh fluorescents. No TV. Soft ambient sound acceptable.

ACT III — The Invitation
How to Begin — The Words That Work
The invitation into practice is itself a therapeutic act. How you open the session shapes whether your child feels safe enough to engage — or defended enough to refuse.
"Hey [name], I've got something I want to show you. It's not about your worries — it's a tool for your brain. You don't have to feel worried to try it. Want to see how it works?"
✓ Removes Pressure
"You don't have to feel worried" removes performance pressure
✓ Frames as Curiosity
"Tool for your brain" — not treatment, not therapy
✓ Gives Agency
"Want to see?" — offers genuine choice
✓ Is Honest
No promises, no claims — builds trust over time
For Resistant Children
"You don't have to use it. You can just watch me use it first." Then parent uses the breathing tool, worry monster, or coping card themselves.
For Children with ASD
- Show the material visually before the session
- Use a visual schedule showing exactly what will happen
- Prime 5 minutes before: "In 5 minutes we're going to do our calm brain practice"
- Offer choice: "Breathing ball or monster today?"
NEVER Say:❌ "We're doing this because you keep worrying." ❌ "You need to calm down." ❌ "The therapist says you have to do this." ❌ "Just try — it won't take long."

ACT III — Engagement
First Two Minutes — Building Safety in the Session
Spend 2 minutes connecting before introducing any material. Ask one genuinely curious question about something the child enjoys. This activates the social engagement nervous system — shifting out of defensive arousal.
Ages 4–6
- Show the Worry Monster without asking them to use it: "Look what I have. Do you know what he eats?"
- Blow bubbles together (breathing warm-up embedded)
- Read first page of Brave Book together
Ages 7–9
- Ask them to name the Worry Monster together
- "If you were going to teach ME about worry, what would you tell me?"
- Review Safety Evidence Journal from yesterday together
Ages 10–12
- "On a scale of 1–10, where is your worry right now?"
- "Which of the cards do you want to use today?"
- More autonomy, less direction — they co-lead the session
For ASD: Keep warm-up predictable — same sequence every time. Novel engagement is itself a stressor. Familiarity IS the regulation.
ACT III — Session Protocols Continued
Running the Session — Materials 7, 8 & 9 Protocols
Worry Time Session (15 min, fixed daily time, e.g. 4pm)
During the day: worry arises → write on slip → put in box → "We'll look at this at 4pm." At Worry Time: set visual timer → open box → for each slip: read aloud, "Is this still worrying you now?" + evidence check → if still worrying, use thought challenging card → timer rings: "Worry time is over. Box closes until tomorrow." → Child closes box — ritual of containment.
Brave Books Session (10–20 min, bedtime or afternoon)
Select book matched to child's current worry theme → Read together → At key moments: "This character is worried about [same thing] — what do they do?" → After story: "Did anything the character felt remind you of you?" → "What helped them? Could that help you?" → Optional: child draws themselves and the character as "worry warriors" together.
Breathing Tools Session (3–5 min, daily + worry moments)
Morning (preventive): box breathing with Hoberman sphere before school. Worry moment: pinwheel or bubbles — slow enough to maintain. Bedtime: 4-7-8 breathing lying down — 3 cycles, then lights out. Count aloud with child. Your pacing is the regulator. Speak slower than feels natural.

ACT III — Reinforcement
The Words That Build the Brain
What you say after a session shapes whether your child's brain encodes the experience as success or failure. ABA-aligned reinforcement focuses on effort and coping — never on the absence of fear.
✅ Say This
- "You felt scared and you used your tools anyway. That's bravery."
- "Your brain worked so hard to find calm today."
- "Look at what you did — that was the brave thing."
❌ Never Say This
- "See? That wasn't so bad!" (invalidates the experience)
- "You're not scared anymore!" (sets up failure when fear returns)
- "Good job not worrying!" (frames worry as moral failure)
The Bravery Formula: "You felt [scared/worried/nervous] + AND + you did [the brave thing] anyway."
The AND is critical. It holds both truths — the feeling AND the capability.

ACT III — Cool-Down
After the Session — Transition Out
How a session ends matters as much as how it begins. The cool-down ritual signals to the nervous system that brave work is complete and normal life can resume.
Record Color
Resume Rhythm
Brief Close
Offer Activity
Signal End
Important: Don't debrief extensively after a hard session. Let the nervous system settle. Process in words the following day if needed. Extended discussion of anxiety after a session can re-activate the threat response — keeping the amygdala engaged when the goal is deactivation.

ACT III — Data
Measure What Matters
Progress in anxiety work can feel invisible week to week. A simple weekly log reveals the trajectory your eye misses — and provides valuable data for your Pinnacle clinician at your next visit.
Week | Reassurance Requests/Day | Avoidance Episodes | Worry Intensity (avg/10) | |
Week 1 (Baseline) | ___ | ___ | ___ | |
Week 2 | ___ | ___ | ___ | |
Week 3 | ___ | ___ | ___ | |
Week 4 | ___ | ___ | ___ |
Also track: Brave steps completed on the Bravery Ladder, and sleep location (own room vs. parents' room) as a key independence indicator.
AbilityScore® Integration: Data captured here feeds directly into GPT-OS® Anxiety Management Readiness Index tracking when conducted within Pinnacle centers. Parents using home protocol can bring 4-week data to their next Pinnacle consultation for formal scoring. Call 9100 181 181 to schedule your AbilityScore® assessment.

ACT III — Troubleshooting
When It Isn't Working — Real Solutions
Every family hits obstacles. These are the six most common challenges — and the evidence-based responses to each.
"My child won't stop asking for reassurance even while we do the tools."
Validate feeling, DON'T answer the what-if: "I can see you're worried. What does your coping card say?" Redirect EVERY time. Consistency over weeks, not days.
"The Worry Monster worked for a week, then stopped."
Normal — the novelty effect fades. Return to the science. Consider rotating materials — introduce the Safety Evidence Journal now.
"My child refuses all materials when anxious."
Materials must be practiced during CALM to be accessible during crisis. Start much earlier in the worry cycle. Parent demonstrates using own "worry" first.
"We've done this for 3 weeks and I see no change."
3 weeks of consistent daily practice should show some trajectory. If genuinely no change — severity may exceed home-based intervention. Seek professional assessment. Call 9100 181 181.
"Grandparents keep reassuring him — it's undoing our work."
Family alignment is critical. Key message for elders: "When you reassure, you feed the worry. When you say 'I trust you can handle it,' you build his strength." Frame as empowerment, not restriction of love.
"The bravery ladder — he gets to the step and panics."
Step is too high. Add an intermediate rung. Never push into panic — push into mild-moderate discomfort. Panic is not therapeutic exposure; it's re-traumatization.

ACT III — Adapt
No Two Worried Brains Are Identical
These materials work for every child — but they look different for every child. Use these adaptation guides to personalize the protocol for your child's unique profile.
Children with ASD + Safety Anxiety
- Increase visual supports — picture-based worry monster slips, visual bravery ladder
- Keep session structure identical every time — novelty amplifies anxiety
- Sensory tools are MORE critical, not less — OT consultation essential
- Distinguish anxiety from need for predictability — they overlap but are different
Younger Children (Ages 4–6)
- Externalization (Worry Monster, Worry Box) over cognitive tools
- More parent co-regulation, less independent use
- Visual bravery ladder with photos, not text
- Breathing via bubbles and pinwheels — not abstract counting
Older Children (Ages 10–12)
- More autonomy — child designs their own coping cards
- Safety Evidence Journal becomes self-managed
- Gradual reduction of parent involvement as independence develops
- Child runs their own Worry Time session independently
Joint Family / Multi-Caregiver Homes
- Assign specific roles to each caregiver (one material per person)
- Weekly family check-in: "What brave thing did [child] do this week?"
- Grandparent-specific guide available in Hindi/regional language
ACT IV — Progress Arc
Weeks 1–2: The Foundation Phase
Don't expect miracles yet. This phase is about building the neural scaffolding for everything that follows. The absence of dramatic change at weeks 1–2 is not failure — it's foundation.
✅ What You WILL Likely See
- Child engages with materials (even imperfectly)
- Slightly increased awareness of worry cycles
- Some reduction in reassurance-seeking frequency from baseline
- Worry Monster becomes part of routine
❌ What You Will NOT See Yet
- Significant reduction in anxiety intensity
- Brave behaviors without support
- Independent use of coping strategies
- Sleep independence (for those working on that)
15%
Progress Arc — Weeks 1–2
Foundation phase: engagement and skill acquisition, not anxiety reduction yet. CBT research: PMC2930817
Parent Milestone: You will likely feel like it's not working. This is normal. Neurological learning requires repetition before evidence of change.

ACT IV — Progress Arc
Weeks 3–4: Consolidation & Weeks 5–8: Building Resilience
Weeks 3–4 Consolidation
40%
Progress Arc
Synaptic pathways for coping skills begin consolidating. PMC10955541
- Child begins reaching for materials independently
- "Monster" or "worry time" enters child's vocabulary spontaneously
- Some worries fade on their own
- Bravery Ladder: first rung mastered, second in progress
- Reassurance-seeking baseline trending down
Parent Milestone: Your redirections are becoming more natural. The script is becoming yours.
Weeks 5–8: Resilience
70%
Progress Arc
Anxiety management competence emerging. Brave behaviors occurring without scaffolding.
- Child uses coping cards with minimal prompting
- Worry intensity ratings trending downward
- Sleep improvement (partial or full independence)
- School functioning improving
- "The worry came but I handled it" statements emerging
The Crucial Reframe: The goal is NOT anxiety elimination. The goal is anxiety management competence.
🏆 Mastery
Define What Mastery Looks Like for YOUR Child
Mastery is not the absence of worry. It is the presence of capability — a child who still sometimes worries AND knows what to do with it. Choose 3 of these indicators to track as your personal mastery milestones.
Sleep Independence
Sleeps independently in own room 5/7 nights
Reassurance Reduction
Reassurance-seeking reduced by 70%+ from baseline
Brave Action
Completes previously avoided activity independently
Worry Rating
Rates worry at 3/10 or less on average daily
Tool Independence
Uses coping strategy independently before parental prompting
Social Participation
Attends sleepover / outside event voluntarily
"Remember three months ago you couldn't sleep alone? Look at you now."
The evidence of growth is the most powerful anxiety antidote. The child learns: "I changed. I grew. I can do hard things."
⚠️ Important
Red Flags
These Signs Mean Professional Support Is Needed Now
Home-based materials are powerful — and they have clear limits. These warning signs indicate that anxiety has moved beyond the scope of home intervention. Contact a professional today.
🚨 Functional Shutdown
Child refuses to eat, attend school, or leave the house due to anxiety
🚨 Panic Attacks
Racing heart, shortness of breath, feeling of dying — recurring physical panic episodes
🚨 No Response to Protocol
Anxiety is increasing despite 6+ weeks of consistent, daily home protocol
🚨 Hopelessness or Harm
Child expresses worthlessness or statements about not wanting to be alive — seek help immediately
🚨 Compulsive Rituals
Rituals lasting more than 1 hour per day — possible OCD, requiring ERP-specialized therapy
🚨 Real Threat
Safety worries focused on specific, realistic threat (abuse, bullying) — address the real threat first
Pinnacle Response Protocol: Call 9100 181 181 — FREE National Autism Helpline | 16+ languages | 24×7. Request: "AbilityScore® anxiety assessment for my child." Expect: Same/next-day telephone triage | Center appointment within 1 week.
ACT IV — Pathway
Where This Leads — The Safety Anxiety Progression Arc
The GPT-OS® Readiness Index maps five stages of safety anxiety — from pervasive to resilient. Knowing where your child is today helps you see where they're going.
Stage 1 — Pervasive Safety Anxiety
Constant, impairing. Avoidance everywhere. Total reassurance dependence.
Stage 2 — High Safety Worry
Significant impairment, regular reassurance, some coping attempts.
Stage 3 — Moderate Safety Awareness
Emerging coping skills, decreasing avoidance, reduced reassurance need. ← Home toolkit targets Stage 1/2 → 3/4
Stage 4 — Appropriate Safety Awareness
Effective self-regulation, minimal avoidance, rare reassurance-seeking.
Stage 5 — Flexible Safety Thinking
Resilience, independence, internal sense of safety. Stage 4→5 typically requires professional CBT-guided exposure.
Pinnacle Pathway: AbilityScore® → Formal CBT Assessment → TherapeuticAI® Plan → FusionModule™ Delivery → EverydayTherapyProgramme™ Home Extension → Re-measurement
ACT IV — Related Techniques
This Technique Connects To
Safety anxiety doesn't exist in isolation. These related techniques form the complete Anxiety & Emotional Regulation support ecosystem within the GPT-OS® framework.
Related Domain C Techniques
- [C-231] Meltdown Management
- [C-241] Emotional Regulation Toolkit
- [C-251] Self-Calming Strategies
ACT V — Community
"She's Not Worry-Free. But She's Living Her Life."
"My daughter couldn't sleep in her own room for three years. She was eight when we started the toolkit. The Worry Monster was the first thing that worked — not because it's magic, but because for the first time, she could DO something with the worry instead of just having it.
Week two: she named the monster 'Dumper' because she dumps worries there. Week four: she started writing in her Safety Evidence Journal without me asking. Week eight: she slept in her own room for the first time.
She still has worried thoughts. The fire worry visited last week. But she told me: 'Mom, I told Dumper. And I checked my coping card. And I breathed. And it went away.'
"She's not worry-free. But she's not trapped anymore. She's living her life."
Parent, Pinnacle Blooms Network | Hyderabad Center. Illustrative case. Individual results vary. Child profile: age 8, GAD features, attending Pinnacle OT + Psychology.
Join 50,000+ Parents
Pinnacle Parent Community across India navigating similar challenges. pinnacleblooms.org/community
WhatsApp Support
Contact 9100 181 181 to request parent group connection
Regional Language Support
Hindi | Telugu | Tamil | Kannada | Malayalam | Bengali | Marathi | Gujarati | Odia | Punjabi | Assamese | Urdu and more

ACT V — Professional Support
When Home Is Not Enough — We Are Ready
These materials are designed to extend, not replace, professional therapy. When severity demands clinical support, Pinnacle's converged consortium is ready across 70+ centers nationwide.
Child Psychology / CBT for Anxiety
Formal anxiety assessment (GAD, OCD, specific phobia differentiation) + individualized CBT protocol. Conducted by licensed child psychologists under GPT-OS® governance.
Pediatric Occupational Therapy
Sensory profile assessment + calm-down kit customization + nervous system regulation protocol. Critical for children with ASD + anxiety.
Behavioral Therapy (BCBA)
Formal bravery ladder design + exposure protocol + reinforcement system. Data-driven. Outcome-measured.
Speech-Language Pathology
Anxiety language development + parent-child communication coaching + narrative therapy for worry externalization.
EverydayTherapyProgramme™
Home extension of clinic protocol — delivered through GPT-OS®. Ensures therapy continues between sessions, across all caregivers.
Access: 70+ centers across India | Teleconsultation available
FREE National Autism Helpline: 9100 181 181 | 24×7 | 16+ languages
→ pinnacleblooms.org/find-center
FREE National Autism Helpline: 9100 181 181 | 24×7 | 16+ languages
→ pinnacleblooms.org/find-center

ACT V — Research Library
The Science This Page Stands On
Every material and protocol in C-287 is grounded in peer-reviewed, replicated research. These are the primary sources.
Kendall PC et al. (2010)
Cognitive-behavioral therapy for childhood anxiety disorders. Journal of Consulting and Clinical Psychology. PMC2930817.
Lebowitz ER et al. (2020)
Parent-based treatment for childhood/adolescent anxiety. JAMA Psychiatry. SPACE protocol RCT.
Systematic Review on Sensory Integration (2024)
16 articles 2013–2023 confirming evidence-based practice for ASD. PMC11506176.
Meta-analysis, World Journal of Clinical Cases (2024)
Sensory/behavioral interventions. PMC10955541.
Padmanabha T et al. (2019)
Home-based interventions for children with ASD. Indian Journal of Pediatrics. DOI: 10.1007/s12098-018-2747-4.
WHO Nurturing Care Framework (2018)
nurturing-care.org/ncf-for-ecd/. PMC9978394.
NCAEP Evidence-Based Practices Report (2020)
National Clearinghouse on Autism Evidence and Practice.
Porges SW. Polyvagal Theory (2011)
Vagus nerve and parasympathetic regulation in anxiety.
Ayres AJ. Sensory Integration and the Child (1979)
OT foundational theory for calm-down kit design.
Pinnacle Blooms Network® Clinical Data
20M+ sessions, 97%+ improvement. pinnacleblooms.org

GPT-OS®
Technology Layer
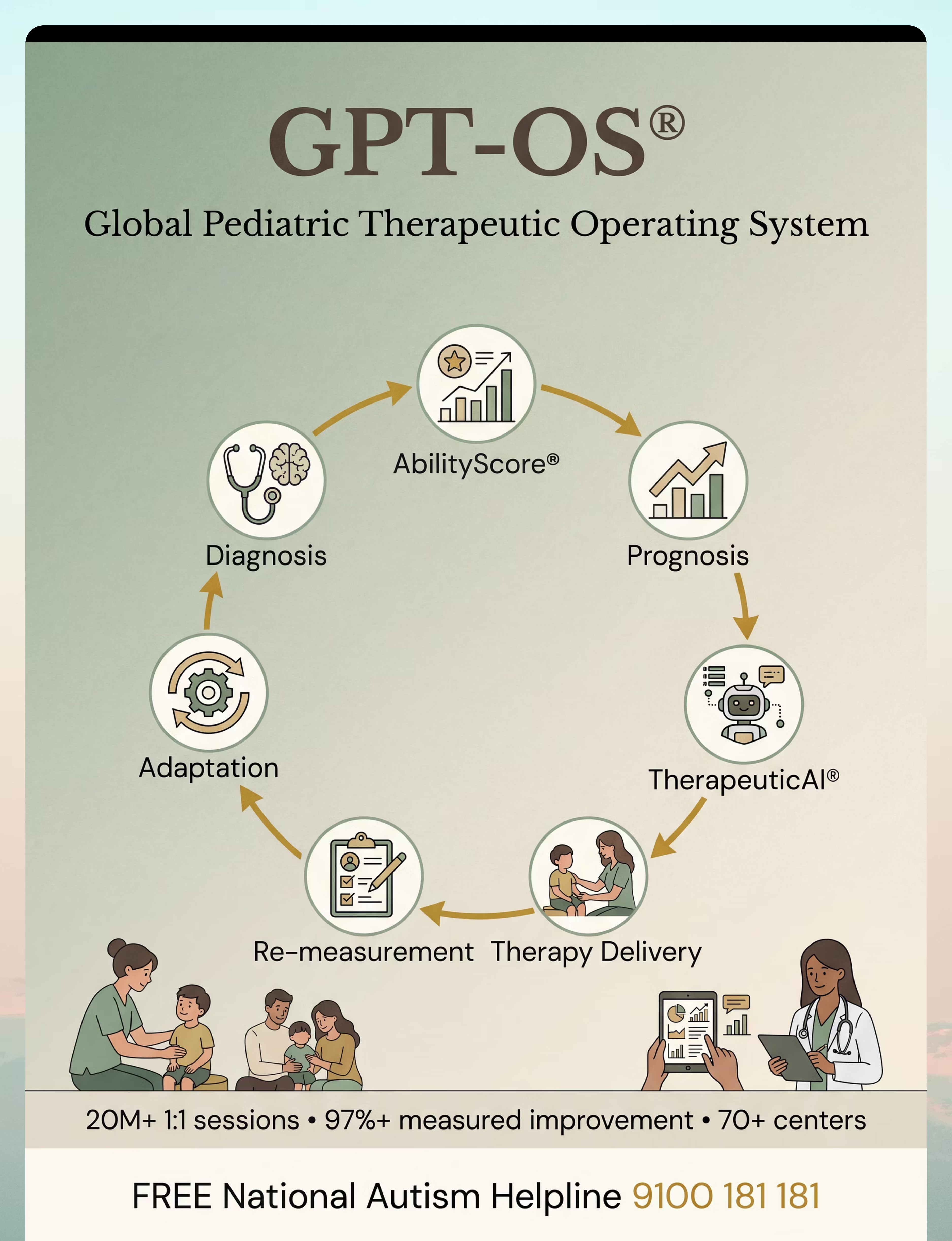
This Page Is Powered by GPT-OS®
Global Pediatric Therapeutic Operating System — Not an app. Not content. Therapeutic infrastructure governing 20M+ sessions, now available for your home.
Layer | Function | For Safety Anxiety | |
AbilityScore® | Universal developmental score (0–1000) | Anxiety severity baseline + longitudinal tracking | |
Prognosis Engine | Predicts developmental trajectories | Timeline to readiness prediction | |
TherapeuticAI® | Designs therapy focus + sequencing | Material sequencing personalized to child profile | |
FusionModule™ | Converges OT + ABA + Psychology + SLP | Single anxiety protocol, not siloed treatments | |
EverydayTherapyProgramme™ | Home micro-interventions | These 9 materials, delivered as daily structured program | |
Closed-Loop Control | Observe → Score → Plan → Execute → Re-measure | Anxiety Readiness Index re-scored at 4-week intervals |
20M+
Exclusive 1:1 Sessions
Governing the GPT-OS® clinical data engine
97%+
Measured Improvement
Across Anxiety Management Readiness Index
70+
Centers Across India
Patents filed across 160+ countries

ACT VI — FAQ
Your Questions, Answered
These are the eight questions Pinnacle clinicians hear most from caregivers beginning this protocol. Evidence-backed, plain-language answers for every stage of the journey.
How long before I see results?
Research-backed: 8–12 weeks of consistent daily practice for measurable anxiety reduction. Early signs appear in weeks 1–3. Don't measure progress by anxiety level in week 1 — measure by engagement.
My child refuses to use the materials. What now?
Parent demonstrates using their own "adult worry" first. Don't introduce during anxiety peak — introduce during calm. Start with least threatening material (Brave Books or Breathing Tools). Gradual introduction over 2 weeks is normal.
Is this suitable for children with autism?
Yes, with adaptations (see Card 21 — Adapt). OT consultation is more critical for ASD + anxiety. Sensory regulation tools first. Visual supports throughout. Call 9100 181 181 for an ASD-specific consultation.
My child still asks for reassurance constantly. Is that normal?
Yes. Reassurance-seeking is a habit pattern that doesn't break in days. Consistent redirection ("What does your coping card say?") plants the seed. It may take 3–4 weeks of consistent redirection before frequency decreases. Tracking baseline reveals invisible progress.
Can I do this alongside professional therapy?
Absolutely — these materials are designed to extend, not replace, professional therapy. They are the EverydayTherapyProgramme™ equivalent for anxiety. Use them between sessions and share your tracking data (Card 19) with your therapist.
The Bravery Ladder — my child panics on every rung. What's wrong?
The steps are too big. This means professional guidance is needed to calibrate the hierarchy. Fear hierarchies for moderate-severe anxiety should be designed by a trained BCBA or child psychologist. Call 9100 181 181.
My child has both autism and anxiety. Which do I address first?
Typically: sensory regulation → emotional regulation → anxiety management → cognitive skills. OT is usually the first entry point for ASD + anxiety. Contact Pinnacle for a multi-disciplinary assessment.
How do I know when my child has outgrown the need for these materials?
When the child can name their anxiety state, identify the trigger, select a coping strategy, execute it independently, and return to regulated function without parent involvement — that's functional independence. Not the absence of worry, but competence in managing it.

Start Now
Your Child's Worried Brain Deserves Better Than Reassurance
You've said "You're safe" a thousand times. But the worry keeps coming back. Because reassurance doesn't fix it. These 9 materials work differently — and your child's brain is ready to learn.
🔶 Get a FREE AbilityScore® Assessment
Understand your child's anxiety severity and the right intervention level. The right starting point changes everything.
📞 Call: 9100 181 181 | FREE | 16+ languages | 24×7
🔷 Find Your Nearest Pinnacle Center
70+ centers across India with child psychologists, OTs, and BCBAs trained in anxiety management.
🔲 Start Today with the Starter Kit
Calm-Down Kit + Breathing Tools + Worry Monster — everything you need to begin at home, today.
Series Navigation: ← [C-286] Recognizing Anxiety Signs | [C-288] Separation Anxiety →
Preview of 9 materials that help with safety worries Therapy Material
Below is a visual preview of 9 materials that help with safety worries therapy material. The pages shown help educators, therapists, and caregivers understand the structure and content of the resource before use. Materials should be used under appropriate professional guidance.



















Share this resource
Help others discover thisLink copied!

Pinnacle Blooms Network®
Pinnacle Blooms Network®
Built by Mothers. Engineered as a System.
Every technique on this platform is built by a consortium of licensed pediatric professionals — psychologists, occupational therapists, behavior analysts, speech-language pathologists, special educators, and neurodevelopmental pediatricians — grounded in WHO/UNICEF frameworks, validated in Indian homes, and governed by the GPT-OS® clinical operating system. We do not offer opinions. We offer evidence — 20 million sessions' worth.
🌐 Pediatric Therapeutic OTT Platform
Content, tools, and protocols for families everywhere
🗺️ Hyperlocal Marketplace
Pediatric therapeutic materials and services near you
🏛️ Center Network
70+ locations across India
🔬 GPT-OS®
Governing intelligence from diagnosis through outcomes
20M+
Exclusive 1:1 Sessions
97%+
Measured Improvement
70+
Centers India-Wide
70+
Countries Reached
📞FREE National Helpline: 9100 181 181 | 16+ languages | 24×7
🌐pinnacleblooms.org | 📧care@pinnacleblooms.org
🌐pinnacleblooms.org | 📧care@pinnacleblooms.org
Next Technique:[C-288] Separation Anxiety — 9 Materials That Help →
STATUTORY IDENTIFIERS: CIN: U74999TG2016PTC113063 | DPIIT: DIPP8651 (Govt. of India) | MSME: TS20F0009606 | GSTIN: 36AAGCB9722P1Z2 | ISO 13485: Medical Device QMS | ISO/IEC 27001: Information Security
DISCLAIMER: This content is educational. It does not replace individualized assessment and intervention from licensed mental health professionals including psychologists, licensed clinical social workers, and child psychiatrists. Anxiety presentations and treatment needs vary by individual. Severe anxiety may require professional treatment including possible medication evaluation. Individual results may vary. Statistics represent aggregate outcomes across the Pinnacle Blooms Network.
© 2025 Pinnacle Blooms Network®, unit of Bharath Healthcare Laboratories Pvt. Ltd. All rights reserved.