
"My son doesn't say he's anxious. He says his stomach hurts."
Every single morning before school. Racing heart. Tight chest. Shaky hands. Anxiety isn't a thought for him — it's a full-body storm.
We went to the pediatrician. The gastroenterologist. Blood tests. An endoscopy. Nothing wrong. His digestive system is perfectly healthy. But the stomach pain is real — I can see it on his face. When I try to talk about feelings, he looks at me blankly. But when I ask about his body — "Is your tummy tight? Is your heart fast?" — he nods. The body is where his anxiety lives. I need tools that meet him there.
🏥 Pinnacle Blooms Consortium | Emotional Regulation Series — C-296
FREE National Autism Helpline: 9100 181 181 | Available 24×7 | 16+ languages

You Are Among Millions of Families Navigating This Exact Challenge
Somatic anxiety — anxiety expressed through physical symptoms — is not rare, not dramatic, and absolutely not "faking." It is the body doing precisely what the nervous system commands under perceived threat. For children with limited emotional vocabulary, neurodevelopmental differences, or alexithymia, the body speaks what the mind cannot say.
40%
Physical-First Anxiety
of children with anxiety disorders present primarily with physical symptoms — not expressed worry. (Anxiety and Depression Association of America)
80%
ASD & ANS Dysregulation
of children with ASD experience autonomic nervous system dysregulation — the same system driving physical anxiety symptoms. (PMC11506176, 2024)
21M+
Therapy Sessions
delivered by Pinnacle Blooms Network® — a significant percentage involving children whose anxiety lived in their bodies before their words.
PMC11506176
PMC10955541
WHO NCF 2018

This Is Not Imagination. This Is Neuroscience.
When the brain perceives threat — real or imagined — a precise chain reaction floods the body. Understanding this mechanism is the first step toward working with it, not against it.
The Mechanism
Brain perceives threat → Amygdala fires → signals hypothalamus → activates HPA axis → Sympathetic nervous system floods body with adrenaline + cortisol → Heart rate ↑ | Breathing ↑ | Digestion halts | Muscles tense | Sweat activates → Prefrontal cortex goes offline — the "thinking brain" is unavailable during acute activation.
What Your Child Experiences
- Racing, pounding heart ("I think I'm dying")
- Chest so tight they can't breathe
- Stomach churning, nausea, actual vomiting
- Shaky hands, wobbly legs, trembling voice
- Can't sit still — the body is preparing to fight or flee
- Skin picking, nail biting — discharging energy the only way available
"When the body is in survival mode, the prefrontal cortex goes offline. Telling an anxious child to 'calm down' or 'think positive' is asking them to use the part of the brain that isn't working. Body-based tools bypass this entirely." — Pinnacle Consortium, NeuroDevelopmental Pediatrics & OT Lead
Polyvagal Theory (Porges)
Frontiers in Integrative Neuroscience (2020)
Your Child's Body Is Speaking Developmental Language. Here's the Map.
Physical anxiety symptoms don't appear in a vacuum — they are part of a predictable developmental arc. Knowing where your child sits on this map helps you understand both the challenge and the opportunity ahead.
1
Ages 0–3
Autonomic nervous system immature. All emotional regulation is co-regulated by caregiver. Physical symptoms universal.
2
Ages 3–6
Early interoception developing. Children begin to notice "tummy feelings." Vocabulary for sensations limited.
3
Ages 6–10 ★
Physical anxiety symptoms peak — children have enough awareness to be distressed by body symptoms but not enough tools to manage them. School demands + social pressure = frequent activation.
4
Ages 10–14
Adolescent hormonal shifts amplify ANS reactivity. Body-based symptoms intensify without intervention.
5
Ages 14–16+
With skilled intervention, interoceptive awareness + body-based regulation strategies produce lasting self-regulation capacity.
Physical anxiety symptoms commonly co-occur with: ASD | ADHD | Sensory Processing Disorder | Trauma history | Alexithymia | Selective Mutism. References: PMC9978394 | WHO/UNICEF CCD Package 2023

Clinically Validated. Home-Applicable. Parent-Proven.
Evidence Grade: Level I–II ✦✦✦✦✦
Deep Pressure / Weighted Interventions
Weighted blankets/vests reduce cortisol, increase serotonin/dopamine, decrease heart rate and blood pressure. Parasympathetic activation confirmed via HRV measurement. → PMC11506176 | Sensory Integration Systematic Review, Children 2024
Controlled Breathing / Vagal Activation
Extended exhale breathing at ~6 breaths/minute produces measurable HRV improvement and parasympathetic shift. Evidence base: 30+ clinical studies. → Journal of Neurophysiology | Polyvagal Theory (Porges, 2011)
Cold Exposure / Dive Reflex
Cold water on face produces immediate vagal activation and heart rate reduction — a hardwired mammalian response. Used in DBT as TIPP skill. → Linehan DBT Skills Training Manual
Proprioceptive Input / Heavy Work
Push-pull-carry activities activate proprioceptors, producing organizing, calming effect on ANS. OT consensus + multiple pediatric RCTs. → NCAEP 2020 Evidence-Based Practices
Biofeedback
HRV biofeedback: strong evidence base for pediatric anxiety. Watching physiological data builds interoceptive awareness and self-efficacy. → AAPB guidelines
Indian Context: Padmanabha et al., Indian J Pediatr (2019): Home-based sensory interventions demonstrated significant outcomes in Indian pediatric population. → DOI: 10.1007/s12098-018-2747-4
What These Materials Are
Formal Name
Body-Based Anxiolytic Materials for Somatic Symptom Management
Parent-Friendly Name
Tools That Calm the Body Directly
Definition
Physical, sensory, and biofeedback materials designed to regulate the autonomic nervous system through non-cognitive pathways. They work by activating the parasympathetic nervous system, triggering hardwired calming reflexes, or discharging fight-or-flight energy — all without requiring the child to think, reflect, or verbalize.
Domain Badges
🧠 Emotional Regulation | C-Domain
🫁 Sensory Processing | A-Domain
💡 Interoception & Body Awareness
🧬 Autonomic Nervous System Regulation
Quick Reference
- Age Range: 4–16 years
- Settings: Home + School + Community + Car + All Environments
- Session Length: 30 seconds (acute) to 20 minutes (structured practice)

This Technique Crosses Therapy Boundaries — Because Anxiety Doesn't.
Six distinct clinical disciplines collaborate within the Pinnacle Blooms Consortium to address physical anxiety symptoms from every angle. Each brings a unique perspective — together, they leave no gap.
Occupational Therapist
Primary deployer of body-based anxiety interventions. Assesses sensory profiles, prescribes weighted items, designs proprioceptive programs, and trains interoception. The sensory integration framework originated in OT.
Pediatric Psychologist
Integrates body-based strategies as somatic complements to CBT. Uses breathing tools, biofeedback, and grounding kits within anxiety treatment protocols. Leads interoceptive exposure work.
BCBA / ABA Therapist
Teaches use of fidgets and calming materials as replacement behaviors for skin-picking, nail-biting, and other BFRBs. Builds systematic self-regulation programs with data tracking.
Special Educator
Implements classroom accommodations — weighted lap pads, fidget tools at desk, visual timers, grounding kits in backpack — to support focus and regulation during learning.
Speech-Language Pathologist
Addresses alexithymia and emotional vocabulary alongside body-based strategies. Body mapping cards + breathing tools support the connection between physical sensations and language.
NeuroDev Pediatrician
Rules out organic causes of physical symptoms. Validates anxiety hypothesis. Supervises biofeedback integration and medication decisions when indicated.
"The Pinnacle Blooms Consortium deploys all six disciplines in a FusionModule™ — one child, one plan, six perspectives, zero silos."
FREE Helpline: 9100 181 181

Measured Outcomes. Not Vague Hopes.
Every toolkit intervention at Pinnacle Blooms is tied to observable, measurable targets across four time horizons. Here is exactly what we're working toward — and how you'll know it's working.
1
Immediate (0–2 weeks)
Child accepts a body-based calming tool during anxiety. Observable reduction in physical symptom duration. Parent gains confidence responding to somatic presentations.
2
Short-Term (3–8 weeks)
Child self-selects a tool from their toolkit. Reduction in frequency and intensity of somatic complaints. Child begins connecting "tight tummy = my anxiety signal."
3
Medium-Term (2–3 months)
Child requests tools proactively before peak escalation. Independent use across 2+ environments. Interoceptive awareness: noticing early warning signals.
4
Long-Term Mastery
Automatic use of body-based regulation without adult prompting. Generalization across all environments. Child understands their own nervous system.
Anxiety Management Readiness Index
Physiological Self-Regulation Index
Interoceptive Awareness Index
Adaptive Coping Readiness Index
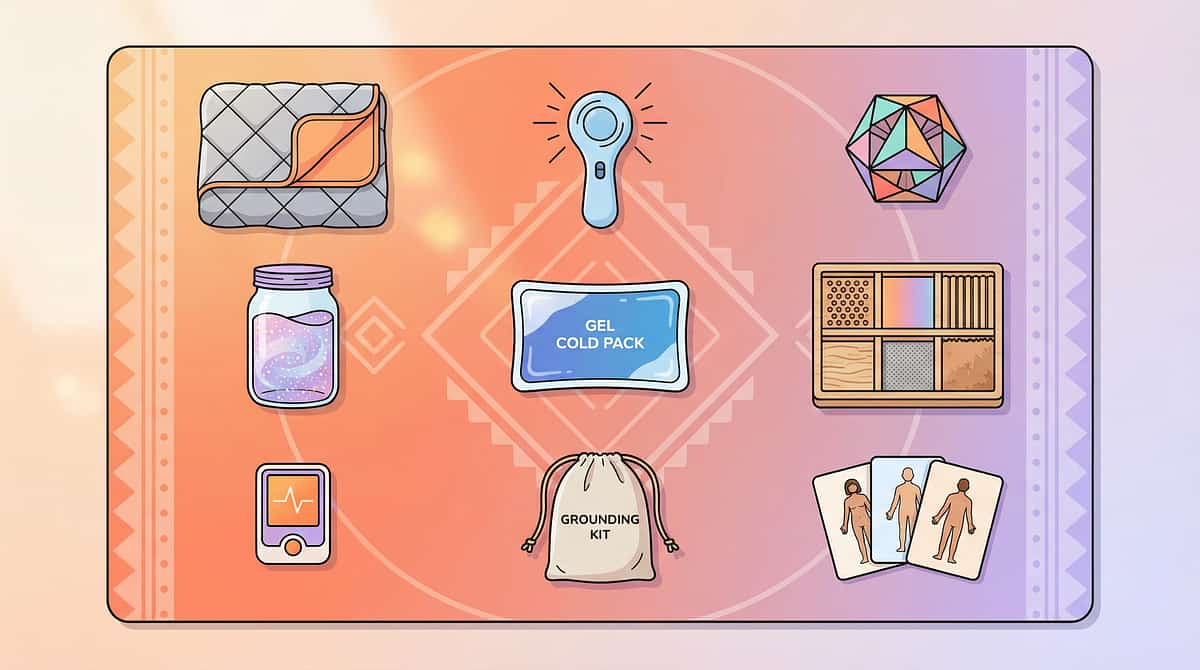
9 Tools. 9 Pathways to Calm. One Body.
Each material works on a different physiological pathway. Build your toolkit across multiple categories — because no two anxiety episodes are identical.
1. Weighted Lap Pads & Blankets
Deep pressure → parasympathetic activation
2. Breathing Visualization Tools
Extended exhale → vagal nerve activation
3. Fidget Tools
Physical discharge → stress energy release
4. Calm-Down Jars
Visual focus → panic spiral interruption
5. Cold & Temperature Tools
Dive reflex → instant heart rate reduction
6. Heavy Work Materials
Push-pull-carry → cortisol burn + ANS calm
7. Biofeedback Monitors
Data visibility → catastrophe prevention
8. Grounding & Sensory Kits
Multi-sensory input → present-moment anchoring
9. Body Mapping & Interoception Cards
Name it → tame it → early intervention

Material 1: Weighted Lap Pads & Blankets
Calm the nervous system automatically — no thinking required.
How It Works
Deep pressure touch activates proprioceptors throughout the body, signaling the parasympathetic nervous system — the rest-and-digest response — to override the fight-or-flight alarm. This happens automatically, below conscious thought. When your child's heart is racing and chest is tight, the weight works even when the brain is completely offline. Weighted materials have been shown to increase serotonin and dopamine while decreasing cortisol — the primary stress hormone.
What / Why / When / Where / How
- What: Weighted pads (1–3 kg) on lap | Weighted blankets (~10% body weight) | Weighted shoulder wraps
- Why: The most passive, effort-free calming input available.
- When: School transitions | Test anxiety | Car rides | Bedtime resistance | Before known stressors
- Where: Lap during homework | Shoulders during screen time | Full-body at bedtime
- How: Place gently. No announcement needed. Let the weight do the work. Remove if child resists — never force.
Price Range
₹800–3,500
DIY Alternative
Fill a thick fabric pouch with uncooked rice or dried beans. Sew shut securely. Target approximately 10% of child's body weight. A layered heavy quilt produces similar deep-pressure effect. Cost: ₹0–100.
⚠️ Safety Note
Never exceed 10% body weight. Never cover face. Not for children under age 2 or those who cannot remove independently. Always introduce during calm — never force.
For weight assessment: 9100 181 181

Material 2: Breathing Visualization Tools
See the breath. Match the breath. The exhale is the calming phase.
How It Works
Slow, controlled breathing is the most direct physiological pathway to parasympathetic activation. The extended exhale activates the vagus nerve — the direct highway from body to brain's calm center. But simply telling an anxious child to "breathe deeply" fails — they cannot think their way to a different breathing pattern when flooded. Breathing visualization tools externalize the rhythm, giving the child something visual to follow rather than a cognitive task to perform.
What / Why / When / Where / How
- What: Hoberman sphere | Pinwheels | Bubble wands | Breathing cards | LED breath pacers | Animated breathing apps
- Why: The 4-second inhale / 6-second exhale ratio is scientifically validated for vagal activation.
- When: Heart is racing | Chest feels tight | Before a known stressor | Daily 3-minute practice
- Where: Desk, car, waiting rooms, school desk drawer, hospital waiting rooms
- How: Open sphere slowly on inhale (4 counts). Close slowly on exhale (6 counts). 5–8 breath cycles. The longer exhale is the key.
Price Range
₹200–1,500
DIY Alternative
Bubble wand (slow blow = long exhale = vagal activation). Pinwheel (spin slowly = controlled exhale). Finger-tracing a square or star shape. Cost: under ₹50.
⚠️ Safety Note
Some children hyperventilate when trying to control breath during acute panic — this worsens symptoms. If breathing tools increase distress, stop and use cold tools instead. Practice first during calm moments.
Research
Slow-paced breathing at 6 cycles/min produces significant HRV improvement. Lehrer & Gevirtz, Applied Psychophysiology and Biofeedback, 2014.

Material 3: Fidget Tools for Physical Discharge
Discharge physical anxiety energy — before it discharges as picking, biting, or explosion.
How It Works
Anxiety floods the body with physical energy — adrenaline prepares muscles to fight or flee. This energy must go somewhere. When it has no sanctioned outlet, it exits through picking, nail-biting, hair-pulling, or behavioral explosion. Fidget tools provide an approved, socially acceptable energy discharge channel. For children who engage in body-focused repetitive behaviors (BFRBs), fidgets serve as replacement behaviors that meet the same sensory need without causing harm.
What / Why / When / Where / How
- What: Stress balls | Therapy putty | Tangle toys | Fidget cubes | Stretchy bands | Spinner rings | Worry stones | Pop toys | Marble fidgets
- Why: Match fidget to need: resistance for squeezers, motion for rockers, texture for sensory seekers.
- When: During seated demand | School → testing → waiting → car rides | Whenever hands are picking or biting
- Where: Desk drawer | Pocket | School bag front pocket | Beside the homework spot
- How: Offer without comment. Let child choose preferred texture/resistance. Goal: regulated hands, not still hands.
Price Range
₹100–800
DIY Alternative
Balloon filled with flour or rice = stress ball (₹10). Pipe cleaners for bending/reshaping. Rubber band for stretching. Smooth stones for palm pressure.
⚠️ Safety Note
No choking hazards for young children. Some fidgets are distracting rather than calming — observe the effect. Have discreet options for school settings (under desk, in pocket).
Helpline: 9100 181 181

Material 4: Calm-Down Jars & Visual Focus Objects
Watch the outside. Calm the inside. As the glitter settles, so do you.
How It Works
During acute anxiety, the mind spirals inward — catastrophic thoughts loop and amplify. Visual focus objects interrupt this internal spiral by capturing external attention. The Calm-Down Jar creates a mesmerizing, slow visual event that demands gentle observation. This metaphor is also therapeutic: "The glitter is your thoughts. They're all swirling right now. Watch them settle. Your mind will settle too." Visual engagement activates the parasympathetic response and provides attentional relief during overwhelm.
What / Why / When / Where / How
- What: Glitter calm-down jars | Lava lamps | Liquid motion toys | Snow globes | Kinetic sand | Slow-moving visual apps
- Why: External visual attention competes with internal panic spiral.
- When: Stomach churning before school | Post-meltdown wind-down | Bedtime anxiety | During worry-triggering wait
- Where: Bedroom calm corner | School desk | Teacher's calm-down station | Car console
- How: Shake the jar. Say: "Watch the glitter. When it all settles to the bottom, your body will feel more settled too." Breathe with the child as it settles.
Price Range
₹150–600
DIY Instructions
Clear plastic bottle or mason jar (superglue the lid). Fill ¾ with warm water. Add 2–3 tbsp clear PVA glue or glycerin. Add fine glitter (2 colors). Optional: 1 drop food coloring. Shake to test settling speed (30–90 seconds = ideal). Cost: under ₹50.
⚠️ Safety Note
Use plastic containers for young children. Seal completely. For very young children, use a sealed snow globe instead. Test during calm moments first.

Material 5: Cold & Temperature Tools
Activate the body's built-in calm reflex. Hardwired. Instant. No thinking needed.
How It Works
Cold exposure triggers the mammalian dive reflex — a hardwired autonomic response that instantly reduces heart rate and shifts the nervous system toward parasympathetic dominance. When cold touches the face (especially cheeks and forehead), thermoreceptors signal the trigeminal nerve, which activates the vagus nerve, which slows the heart. This is the same reflex that allows diving mammals to stay underwater for extended periods. In children experiencing racing hearts or panic spirals, cold provides the fastest physiological interrupt available — faster than breathing, faster than weight. This is the "T" skill in DBT TIPP techniques.
What / Why / When / Where / How
- What: Flexible gel cold packs | Instant cold packs | Cooling towels | Cold water bottle | Misting spray bottle | Ice cubes in a cloth
- Why: The dive reflex is involuntary — activates regardless of whether the child cooperates or believes in it.
- When: Heart is racing and child feels like "dying" | Hot flushing panic | Pre-vomiting anxiety | When nothing else is working
- Where: Freezer at home | Teacher's first aid kit | Insulated lunch bag
- How: Apply cold pack gently to face, neck, or wrists. Hold 15–30 seconds. Child should notice heart slowing within 30–60 seconds.
Price Range
₹100–500
DIY Alternative
Wet washcloth in cold water. Frozen water bottle wrapped in a thin cloth. Bowl of ice water to dip hands. Cost: ₹0.
⚠️ Safety Note
Never apply extreme cold directly to bare skin for more than 30 seconds — risk of cold burn. Always wrap in thin cloth. Some children find cold aversive — respect this and use other strategies. Not for children with cold sensitivity or specific medical conditions.
Research
DBT TIPP Skills (Linehan, 1993) | Dive reflex — mammalian autonomic neuroscience.
Material 6: Proprioceptive / Heavy Work Materials
Push. Pull. Carry. Calm. Give the body a safe, productive way to discharge.
How It Works
Heavy work — pushing, pulling, carrying, climbing, resistance activities — delivers intense proprioceptive input that simultaneously: (1) discharges fight-or-flight energy and stress hormones through physical exertion; (2) activates calming proprioceptive pathways in the brainstem and cerebellum; (3) gives the body's "prepare for danger" activation a productive, satisfying physical outlet. Unlike strategies requiring stillness, proprioceptive input works with the anxious body's need to move.
What / Why / When / Where / How
- What: Therapy resistance bands | High-resistance putty | Push-up bars | Weighted backpack carries | Compression clothing | Therapy body sock | Mini trampoline | Wall push-ups | Chair push-ups
- Why: Burns cortisol and adrenaline. Satisfies the fight-or-flight urge safely.
- When: Pre-test nervous energy | Before demanding transitions | When restlessness is escalating | Morning routine
- Where: Wall corner at home | School hallway | PE break | Staircase | Backyard/playground
- How: 10 wall push-ups → 10 chair push-ups → 30-second resistance band pull → walk with heavy backpack. 3–5 minutes of intentional heavy work.
Price Range
₹300–1,500
DIY Alternative
Wall push-ups (free). Carrying a bag of books or water bottles. Pushing against a door frame. Climbing stairs deliberately. Cost: ₹0.
⚠️ Safety Note
Match resistance to child's physical capacity. Stop if painful. Some proprioceptive activities can be dysregulating for hypersensitive children — observe carefully.
OT consultation: 9100 181 181

Material 7: Biofeedback Monitors
See it slow. Know you're okay. Data beats catastrophe.
How It Works
For children who experience racing heart as their primary anxiety symptom, the sensation is terrifying — many genuinely believe they are dying. Biofeedback tools make the invisible visible: the child can see their heart rate as a number, transforming a terrifying internal event into observable data. When they watch their heart rate decrease after a calming strategy — from 110 bpm to 85 bpm — two things happen: (1) they gain evidence that the body CAN return to calm; (2) they build the neurological connection between the body sensation and the number, developing interoceptive awareness they will eventually use without the device.
What / Why / When / Where / How
- What: Finger pulse oximeters (SpO₂ monitors) | Kids' fitness trackers with heart rate | Heart rate smartphone apps | Simple biofeedback games
- Why: Catastrophic interpretation of heart racing ("I'm dying") is the core cognitive distortion in panic. Seeing the number decline proves survival.
- When: During acute heart-racing episodes | During calm practice | Post-breathing exercise to confirm calming
- Where: Home calm-down station | School health room | Therapy sessions
- How: Put on finger. Note the number. Say: "Watch what happens when we breathe together." Check the number again. "See? Your heart is slowing. You're safe."
Price Range
₹1,500–8,000
DIY Alternative
Manual pulse check on wrist or neck (older children). Free heart rate apps using phone camera (place finger over camera lens). Cost: ₹0.
⚠️ Safety Note
Biofeedback should provide reassurance, not fuel hypervigilance. Some children become obsessively focused on heart rate, increasing anxiety. Introduce as "interesting information," not danger monitoring. Use with clinical guidance for highly anxious children.

Material 8: Grounding & Sensory Kits
Strong senses. Present moment. When anxiety makes the body feel unreal, the senses prove reality.
How It Works
Physical anxiety can include dissociation or derealization — a sense of floating, unreality, or being outside one's body. Grounding materials address this by flooding the senses with intense present-moment input: strong scents anchor through olfactory pathways; sour/intense tastes activate the trigeminal nerve; cold or textured objects demand tactile attention. The 5-4-3-2-1 technique provides structure. But grounding only works when the sensory items are physically present. A portable kit makes the technique field-deployable.
Consortium-Recommended Kit Contents
- 1 small bottle peppermint or citrus essential oil
- 2–3 sour candies or lemon drops
- 1 textured fabric swatch (rough canvas + soft velvet)
- 1 small cold gel pack
- 1 smooth worry stone for palm pressure
- 1 lavender sachet | Optional: small earbud for calming audio
When / Where / How
- When: Dissociation / floating feeling | Pre-panic spiraling | Any time child says "I feel weird"
- Where: School backpack | Bedside drawer | Car glovebox | Jacket pocket
- How: Open the kit. Work through 5-4-3-2-1 with actual items. Smell the peppermint. Name 5 things you see. Touch the texture.
Price Range
₹200–1,000
DIY Alternative
All items from local pharmacy/grocery store. Total assembly cost: under ₹150.
⚠️ Safety Note
Test scents for tolerance — some children find strong smells aversive or triggering. Ensure no food allergens in taste items. No choking hazards for young children.

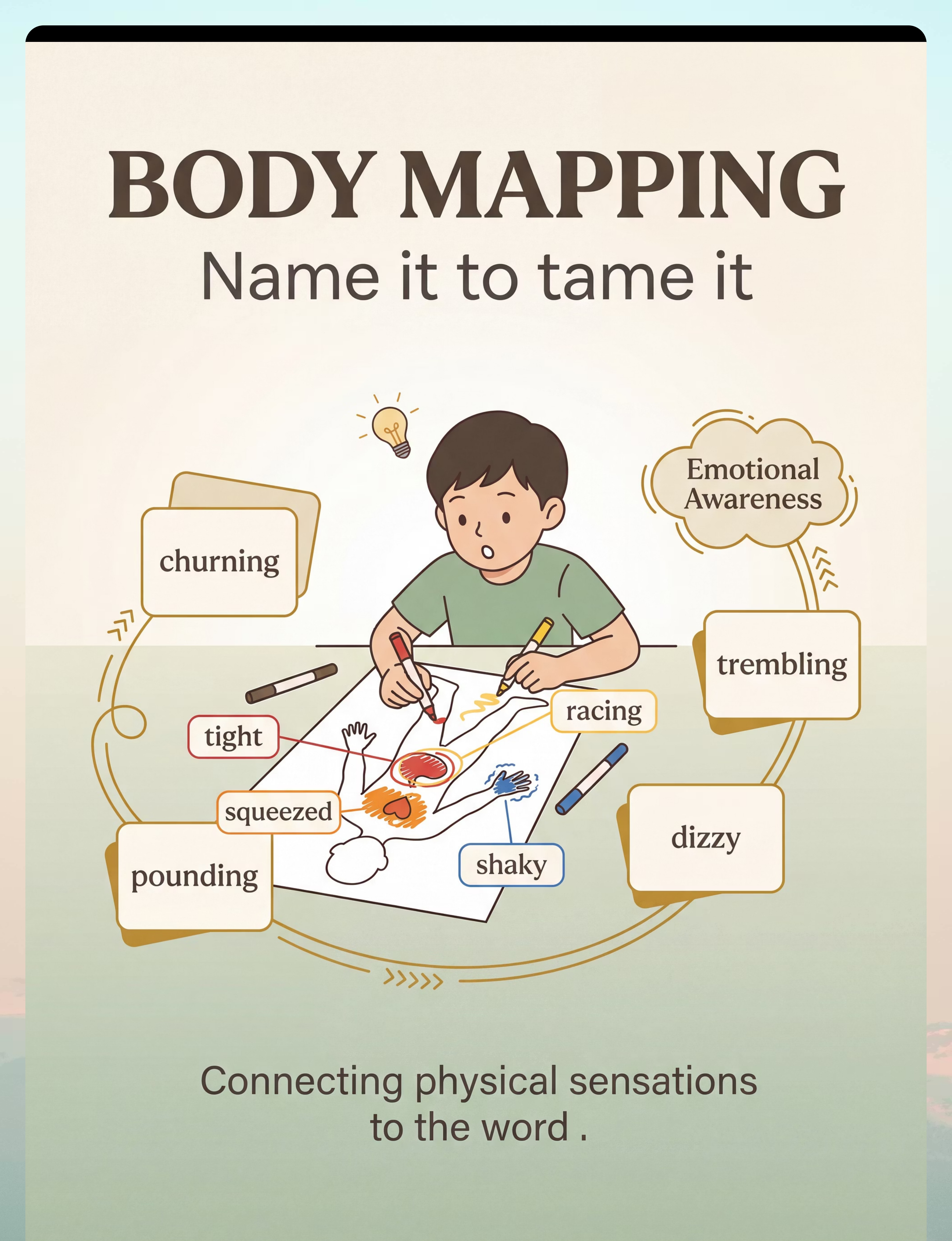
Material 9: Body Mapping & Interoception Cards
Name it to tame it. When the body can speak, the mind can respond.
How It Works
Many children with physical anxiety symptoms have never connected their racing heart or churning stomach to the concept "anxiety." They just know they "feel bad." Body mapping and interoception cards build this foundational connection: body sensation → emotion word → strategy choice. This is the upstream intervention — it builds the awareness system that allows earlier interception of future crises. Kelly Mahler's interoception research demonstrates that children who develop body awareness can detect anxiety signals at 30% intensity rather than waiting until they're at 90% and overwhelmed.
What / Why / When / Where / How
- What: Printable body outlines for coloring | Sensation vocabulary cards (tight, shaky, racing, churning, dizzy) | Emotion-body connection posters | Personal "anxiety map" | Body scan audio scripts | Interoception workbooks
- Why: Interoceptive awareness is the prerequisite for early self-regulation. Children cannot use tools they cannot recognize they need.
- When: During calm practice sessions (NOT during crisis) | Weekly 10-minute check-ins | Post-anxiety debrief
- Where: Kitchen table | Therapy sessions | Bedtime quiet routine
- How: "Let's draw where you feel worried in your body. What color is that feeling?" Mark it. Name it. Say: "Next time you feel that color, that's your signal to get your tool."
Price Range
₹200–800
DIY Alternative
Print body outline from pinnacleblooms.org. Create a personal anxiety body map with colored pencils. Cost: ₹10 (printing).
⚠️ Safety Note
Body awareness work can be activating for children with trauma histories. Move at the child's pace. Never force body focus. Some children benefit from therapist guidance for initial interoception work.
Research
Kelly Mahler, OTR/L — Interoception: A Primer (2019) | Paulus & Stein, Biological Psychiatry (2010)
Helpline: 9100 181 181

Safety First. Every Child. Every Time.
General Principles
1
Always introduce materials during CALM moments
Never expect crisis use without calm-time practice first.
2
Never force any sensory input
Respect sensory preferences — always. Forced input undermines trust and escalates distress.
3
Medical evaluation first
Rule out cardiac, GI, thyroid, and other organic causes before attributing symptoms to anxiety.
4
Weighted items rules
Never exceed 10% body weight | Never cover face | Not for children under age 2.
5
Cold tools: max 30 seconds
Always wrap in cloth. If breathing tools worsen distress — stop immediately.
🔴 Red Flags — Seek Immediate Medical Care
- Symptoms occur during sleep (not during stressors)
- Chest pain radiating to arm/jaw
- Fainting or near-fainting
- Symptoms not related to situational triggers
- Symptoms not responding to anxiety intervention after 8 weeks
Medical Rule-Out Checklist
- Thyroid disorders (TSH panel)
- Cardiac arrhythmia (ECG if racing heart is persistent)
- Gastrointestinal disorders
- Asthma (if chest tightness + breathing difficulty)
- Medication side effects | Caffeine/food sensitivities
FREE Assessment: Pinnacle Blooms Network® | AbilityScore® | 9100 181 181
This content is educational. It does not replace individualized assessment and intervention by licensed healthcare professionals. Physical symptoms should be medically evaluated before attributing to anxiety.
Your Home Is Now a Body-Regulation Environment. Here's How to Set It Up.
🏠 The Calm Corner
Weighted blanket or lap pad — accessible without asking. Calm-down jar at eye level. 2–3 fidget tools in a basket (child selects freely). Breathing tool (Hoberman sphere or pinwheel). Grounding kit in a small pouch.
🎒 The School Bag Kit
1 discreet fidget tool (pocket-sized). 2–3 sour candies in zip-lock. Breathing card (laminated, front pocket). 1 small cold pack (insulated pouch). Personal body map card (laminated reminder of anxiety signals).
🚗 The Car Kit
Weighted lap pad for car seat. Fidget tool in seat pocket. Aromatherapy roller (lavender) in cup holder. Calm-down jar for "big feelings" moments in traffic.
🌙 The Bedside Kit
Weighted blanket for sleep onset anxiety. Lavender sachet. Biofeedback app on device (optional, for older children). Body scan audio (downloadable from pinnacleblooms.org).
Setup Principle: Tools only work when they're available. Don't make a child ask for them — that requires executive function they may not have mid-anxiety. Pre-position everything.

The Pinnacle Physical Anxiety Toolkit Protocol
Six clear steps. Each designed to work with the anxious nervous system — not against it. Practice this sequence during calm moments so it becomes instinctive during crisis.
01
Recognize the Signal (30 sec)
Notice the body — don't address the thought. "Your tummy is tight" not "You're feeling worried." Ask: "Is your heart fast? Are your hands shaky?" Validate: "I can see your body is working really hard right now."
02
Choose the Right Tool (15 sec)
Racing heart → Breathing tool first, then cold. Muscle tension → Heavy work. Stomach churning → Weighted pad + grounding kit. Dissociation → Grounding kit (strong scents first). Picking/biting → Fidget tool replacement.
03
Deploy the Tool (2–5 min)
Introduce calmly: "Let's try the lap pad." No lectures, no "Why are you anxious?" — just tool deployment. Stay present. Breathe visibly yourself.
04
Wait & Witness (2 min)
Allow the tool to work. Don't fill the silence with words. The nervous system needs 90–120 seconds to begin calming. Trust the physiology.
05
Confirm & Reinforce (30 sec)
"Your heart is slowing down. I can see your shoulders dropping. You used your tool really well." Specific, immediate, behavioral praise. Just specific observations.
06
Debrief When Calm (5–10 min later)
"What did you notice in your body? What helped? Shall we put that tool in your school bag?" Build interoceptive vocabulary retrospectively.

Celebrate the Attempt. Not Just the Success.
Every time the child reaches for a tool — even if the anxiety doesn't resolve — the behavior of tool-seeking is being reinforced and will increase in frequency. The nervous system learns from immediate feedback. Reinforce within 3–5 seconds of the desired behavior.
Reinforcement Script (exact words):
"I noticed you reached for your fidget before your hands started shaking. That's amazing body awareness."
"Your heart was racing and you used the breathing ball. That's your nervous system learning."
"You stayed in the car even though your tummy was tight. Your body got through it."
Verbal Praise
Immediate, specific, behavioral
Connection Time
Extra time with parent
Token Economy
Stamp/star chart
Brave Body Chart
Child marks body part that stayed calm
BACB Guidelines
ABA Reinforcement Principles
PMC11506176

60 Seconds of Data Now Saves Hours of Guessing Later.
Consistent, simple session tracking is the difference between guessing and knowing which tools work for your child's specific symptom profile. It also builds the evidence base for school accommodation requests.
What to Track Per Session
- Which physical symptoms appeared (heart racing / stomach / chest / shaking / other)
- Which tool was used (name it)
- Effect rating: 1 (no effect) → 5 (significant calming) + time to calm (minutes)
- Trigger, if identifiable (school / transition / unknown)
How to Track
- Download C-296 Tracking Sheet → pinnacleblooms.org/c-296-tracker
- Use GPT-OS® in-app tracker (AbilityScore® platform)
- Simple notes app: date | symptom | tool | rating
Tracking Purpose
- Identify which tools work best for this child's specific symptom profile
- Detect trigger patterns over time
- Feed data into GPT-OS® Physiological Self-Regulation Index
- Build evidence for school accommodation requests
GPT-OS® Dashboard: pinnacleblooms.org/gpt-os

Session Didn't Go Perfectly? That's Data, Not Failure.
Every challenge that arises is information about your child's sensory profile, regulation capacity, and current stress level. Here is how to interpret and respond to the most common scenarios.
Child refused the weighted lap pad
Why: New sensory input introduced during high anxiety = rejection guaranteed. Fix: Introduce the pad during TV time, calm play — never during crisis first. Let them explore it on their own terms.
Breathing tool made panic worse
Why: Focusing on breath can cause hyperventilation in some children. Fix: Switch to cold tool immediately. Reserve breathing work for calm practice sessions only.
Child took the fidget and threw it
Why: The anxiety energy was too high for a fine-motor outlet. Fix: Escalate to heavy work — wall push-ups, carrying heavy item. Match energy level to strategy intensity.
Calm-down jar made child more frustrated
Why: Individual variation in visual processing and patience thresholds. Fix: Switch to a faster-settling jar (less glycerin) or use biofeedback instead.
Child can't connect body sensations to "anxiety"
Why: Alexithymia or limited interoceptive awareness — common in ASD. Fix: Don't use the word "anxious." Use body language: "Your tummy is talking. Your heart is beating fast. That's your body's worry signal."
Tools work at home but not at school
Why: Social stigma + novelty + environmental mismatch. Fix: Involve the teacher. Create a discreet "desk kit." Practice using tools at school during non-anxious times first.
Emergency Protocol: If child becomes severely distressed, discontinue immediately. Prioritize physical safety and co-regulation (your calm presence). Call Pinnacle Helpline: 9100 181 181 for same-day guidance.
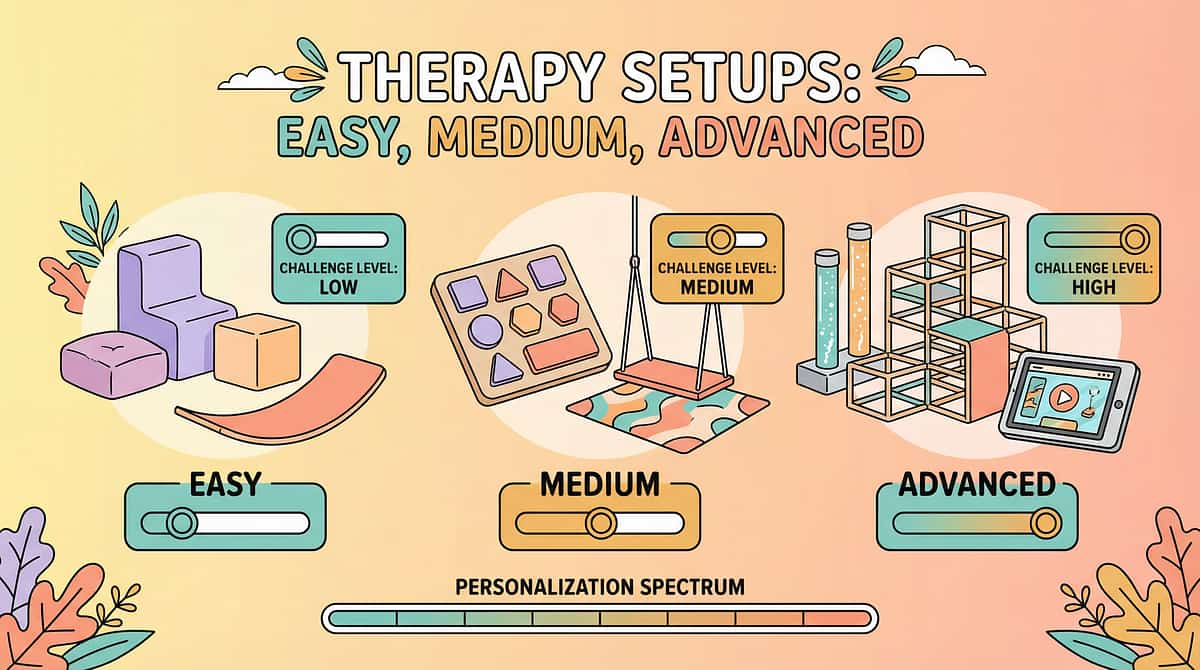
No Two Nervous Systems Are Identical. Here's How to Tune These Tools.
Sensory profiles, age, and neurotype all shape how a child responds to body-based tools. Use these adaptations to dial in the toolkit for your specific child.
For Sensory Seekers
(High sensory threshold — needs more input)
- Weighted items: go higher (up to 10% body weight max)
- Heavy work: more intense resistance, longer duration
- Fidgets: high-resistance putty, stress balls requiring real force
- Cold: can tolerate cooler temperatures
- Breathing: add humming/singing (vagal activation through vocalization)
For Sensory Avoiders
(Low sensory threshold — easily overwhelmed)
- Weighted items: start very light (0.5 kg) and build gradually
- Heavy work: lighter resistance, shorter duration, more breaks
- Fidgets: smooth, predictable textures; avoid surprising textures
- Cold: lukewarm water only; no ice
- Breathing: very gentle pacing; no device in face
Ages 4–6
Passive strategies lead (weighted, visual). No biofeedback.
Ages 7–10
Introduce breathing tools + simple fidgets. Body mapping with pictures.
Ages 11–14
Biofeedback + interoception cards. Child manages their own toolkit.
Ages 14+
Full self-directed toolkit. Peer-sharing of strategies acceptable.
ASD-Specific: Deep emphasis on body-based tools (cognitive strategies often inaccessible). Biofeedback is particularly effective (data-driven, objective). Use body language, not emotion language for alexithymia.

Week 1–2: Progress Looks Like Tolerance, Not Mastery.
What You WILL See
- Child accepts the weighted lap pad for at least 60 seconds during a calm moment
- Child is curious about the calm-down jar (even if they don't use it during anxiety yet)
- Parent has identified 2–3 reliable physical anxiety signals for this child
- At least one instance of tool deployment during mild anxiety (even if incomplete)
What Is NOT Progress Yet
- Child requesting tools independently (that's Week 4+)
- Tools eliminating anxiety completely (tools reduce intensity, not eliminate)
- Perfect execution of breathing techniques (that takes 3–4 weeks of practice)
"You will likely have sessions that feel like failure this week. The nervous system is learning. The first 10 times you offer the weighted pad, the child may reject it 8 times. Those 8 rejections are teaching the nervous system that safe sensory input exists. The 9th and 10th trials will be different."
Progress Metric: If your child tolerates a body-based tool for even 20 seconds longer than last week — that is measurable progress. PMC11506176 — Sensory integration outcomes emerge across 8–12 week timelines.

Week 3–4: The Nervous System Is Forming New Pathways.
The consolidation phase is when parents most often say: "I think I saw it working." These are the signs to watch for — each one represents genuine neurological change.
Child reaches for a tool without being prompted (even once!)
This is the clearest sign that the association between body signal and tool is forming — the synapse is strengthening.
Physical symptom episodes are shorter in duration than weeks 1–2
Duration reduction precedes frequency reduction. Shorter episodes = the nervous system is calming faster.
Child starts using body language spontaneously
"My tummy is doing the thing" — this phrase is interoceptive gold. The child is noticing body signals before crisis.
Parent notices a pattern
"She always needs the fidget when we're in the car" — pattern recognition enables proactive tool deployment.
"You may notice YOU are less anxious about their anxiety this week. That is because you have a protocol. You know what to do. That regulation in you is already regulating them."

Weeks 5–8: Tools Becoming Instinctive. Anxiety Losing Its Grip.
Independent Tool Selection
Child selects the right tool for the specific symptom — without prompting. Matching tool to symptom is a sophisticated self-regulation skill.
School Reports Improve
Decreased somatic complaints and nurse visits. Child uses body language proactively: "I need my breathing ball."
Multi-Environment Use
Tools used across 2+ environments without parent prompting. This is generalization — the gold standard of skill acquisition.
Interoception Milestone
Child can identify WHERE in their body they feel anxiety and WHEN it is building — before it peaks. Intervention at 30% intensity, not 90%.
What to Build Now:
- Formal school accommodation plan — weighted lap pad at desk, fidget in pocket
- Body mapping practice: weekly anxiety body map reviews
- Introduce second-tier tools (biofeedback for older children)
- Begin peer toolkit awareness (child-led, for social confidence)

When to Escalate Beyond Home Tools
🟡 Amber Flags — Consult Your OT/Psychologist
- Tools working for mild anxiety but not for moderate/severe episodes
- Somatic symptoms increasing in frequency despite 6+ weeks of toolkit use
- Child developing fear of their own anxiety tools ("The breathing ball makes it worse")
- Skin picking or hair pulling not responding to fidget replacement strategies
- School refusal associated with physical anxiety symptoms
🔴 Red Flags — Urgent Clinical Evaluation
- Physical symptoms occurring during sleep, not just during situational stress
- Child expressing suicidal ideation related to not being able to control their body
- Vomiting before every school day for 4+ consecutive weeks
- Panic attacks lasting more than 20 minutes
- Complete school refusal / inability to leave home
- Physical symptoms not explained by anxiety after medical evaluation
FREE Helpline (24×7, 16+ languages): 9100 181 181

C-296 Lives Within a Larger Therapeutic Journey. Here Is the Map.
Physical anxiety symptoms rarely exist in isolation. This technique is one node in a broader, evidence-based domain architecture. Understanding the full map helps families and clinicians navigate the complete journey.
C-294
Generalized Anxiety — whole-child approach
C-295
Worry Management — cognitive strategies
C-296 ← YOU ARE HERE
Physical Anxiety Symptoms — body-based tools
C-297
Social Anxiety — peer-context strategies
C-298
Performance Anxiety — test/event-specific
Related Domains
- A-Domain (Sensory Processing): Sensory defensiveness techniques that feed anxiety
- C-Domain (Emotional Regulation): Broader regulation architecture
- B-Domain (Social Communication): Alexithymia and verbal expression of internal states
GPT-OS® Progression Path
AbilityScore® Assessment → Physiological Self-Regulation Index baseline → C-296 toolkit deployment → Index tracking → Pathway recommendation to C-297 or C-295 based on data.
Next Technique: → C-297: 9 Materials That Help With Social Anxiety

"Her Stomach Pain Had Run Our Lives for Two Years. Now She Catches It Early."
"For two years, my daughter's stomach aches ran our family's mornings. Every school day, she'd be doubled over before breakfast. We saw three doctors. Nothing found. We finally understood it was anxiety living in her body. We got her a weighted lap pad for the car ride, a breathing ball she keeps at her desk, and we built a grounding kit together — she chose the peppermint oil herself. The shift was gradual. Weeks 3 and 4, she started reaching for the fidget before I offered it. By week 6, she said: 'My stomach is getting tight — I need my tools.' She catches it early now. Last month she went on a two-day school trip without a single stomach complaint. Her anxiety isn't gone. But she has tools that speak the same language as her body."
— Parent, Pinnacle Blooms Network® | Hyderabad Center(Illustrative testimony; individual outcomes vary)
4→1
Readiness Index
Anxiety Management Readiness Index Stage 1 → Stage 4 in 11 weeks
0
School Nurse Visits
From 3–4 per week → 0 per week by week 8
74%
Complaint Reduction
Somatic complaint frequency reduced by 74% over 11 weeks

You Are Not Navigating This Alone. The Community Is Waiting for You.
Consistency across caregivers is one of the most powerful amplifiers of therapeutic progress. When parents, grandparents, teachers, and therapists all speak the same body-based language, the child's nervous system learns faster.
Pinnacle Parent Network
50,000+ families across India and 70+ countries. Evidence-based sharing. Compassion as default. pinnacleblooms.org/community
Physical Anxiety Support Group
WhatsApp group moderated by Consortium OTs. Real-time support for parents navigating somatic anxiety presentations.
Domain C Parent Community
Monthly live Q&A sessions for the Emotional Regulation parent community. Ask clinicians your questions directly.
GPT-OS® Family Portal
Technique library + progress tracking + community. Your child's full therapeutic journey in one place. pinnacleblooms.org/gpt-os
Community Principles: No unsolicited medical advice. Evidence-based sharing only. Every family's child is different. Compassion is the default.
Helpline: 9100 181 181 — for crisis support or clinical guidance
Expert Support — Wherever You Are in India.
70+ Pinnacle centers across India offer the full spectrum of clinical disciplines needed for physical anxiety assessment and treatment. In-person or teleconsultation options available.
When to Book an Assessment
- Physical anxiety symptoms severe, frequent, or not responding to home toolkit
- Child has ASD, ADHD, or sensory processing disorder
- Biofeedback assessment needed for cardiac anxiety presentation
- School refusing / functional impairment
Services at Pinnacle Centers
- AbilityScore® Comprehensive Assessment
- Sensory Integration Therapy (OT)
- Anxiety Treatment (CBT + body-based integration)
- FusionModule™ multi-disciplinary coordination
- EverydayTherapyProgramme™ home extension
FREE First Step: Call the FREE National Autism Helpline: 9100 181 181 | Available 24×7 | 16+ languages | No cost for initial guidance.
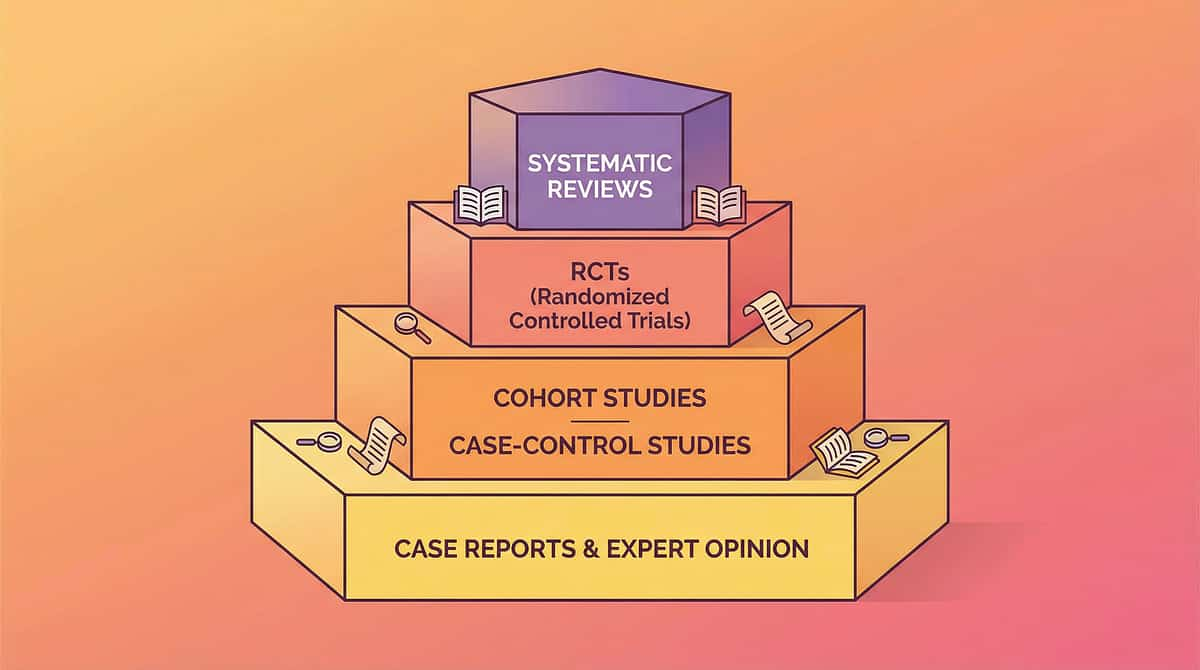
The Science That Powers Every Card on This Page.
Every technique on this page is grounded in peer-reviewed evidence reviewed per Oxford Centre for Evidence-Based Medicine (OCEBM) levels. Body-based anxiety interventions are rated Level I–II overall.
1
PMC11506176
PRISMA Systematic Review (2024): 16 studies confirming sensory integration as evidence-based for ASD. Endorses body-based regulatory interventions.
2
PMC10955541
Meta-analysis, World J Clin Cases (2024): Sensory integration therapy significantly improves adaptive behavior, sensory processing, and emotional regulation.
3
PMC9978394
WHO/UNICEF Care for Child Development Package: Multi-caregiver, home-based implementation evidence across 54 countries.
4
Porges (2011)
The Polyvagal Theory: Neurophysiological Foundations of Emotions, Attachment, Communication, and Self-Regulation. Foundation for cold/breathing/vagal activation interventions.
5
Mahler (2019)
Interoception: A Primer. OTR/L framework for body awareness as prerequisite for anxiety management. Foundational for body mapping.
6
NCAEP 2020
National Clearinghouse on Autism Evidence and Practice. Classifies visual supports and sensory-based interventions as evidence-based practices.
7
Lehrer & Gevirtz (2014)
Heart rate variability biofeedback: How and why does it work? Frontiers in Psychology. Evidence base for biofeedback intervention.
8
Padmanabha et al. (2019)
Indian J Pediatr: Home-based sensory and behavioral interventions in Indian pediatric population — significant outcomes. DOI: 10.1007/s12098-018-2747-4

Your Sessions Make Every Child's Therapy Smarter.
The GPT-OS® platform doesn't just track your child's progress — it continuously learns from every session across the network to improve recommendations for every family.
What GPT-OS Learns
Parent records session
Session details entered by caregiver
FusionModule alerts team
Escalation flagged for clinicians
TherapeuticAI adjusts
Technique recommendations refined
Physiological index updated
Self-Regulation score recalculated
GPT-OS ingests data
Structured input updates indices
Programme personalizes
Next session tailored to child
What GPT-OS® Learns from C-296 Data
- Which tools work for which symptom profiles
- Typical timeline from tool introduction to independent use
- Early indicators of treatment non-response (enables faster escalation)
- Population-level patterns: what triggers physical anxiety in different age bands
Privacy Protection
- All data de-identified at source
- DPDP Act (India) compliant
- ISO/IEC 27001 information security framework
- Parents can export, view, or delete their child's data at any time
"Your child's therapy data contributes to the 20M+ session evidence base that guides recommendations for every child in the GPT-OS® network. Your child is helping every child like theirs."

Watch the Reel: 9 Materials That Help With Physical Anxiety Symptoms
C-296 | Anxiety & Stress Management | Episode 296
Domain C — Emotional Regulation / Sensory Processing
Watch our Consortium OT and Child Psychologist demonstrate all 9 materials in a real home setting — including how to introduce a weighted lap pad for the first time, how to use the Hoberman sphere breathing technique, and how to build a grounding kit from items you already have at home.
"Physical anxiety symptoms are real — not imagined, not exaggerated. The body is doing exactly what the nervous system commands. These tools don't ask your child to think their way to calm. They help the body find its own way back." — Pinnacle Blooms Consortium OT & Psychology Lead
Video modeling is classified as an evidence-based practice for autism (NCAEP, 2020). Multi-modal learning improves parent skill acquisition by 47% over text-only.

Consistency Across Caregivers Multiplies Impact.
The more adults in a child's life who understand and deploy these tools, the faster and more durable the progress. Share this page with everyone in your child's circle.
Share This Page
The downloadable family guide includes: 1-page plain-language summary | 5 key tools and when to use them | What NOT to say during an anxiety episode | Emergency: when to call the helpline.
Teacher/School Communication Template
"[Child's name] experiences physical anxiety symptoms — racing heart, stomach pain, and muscle tension — that are nervous system responses, not behavioral choices. They benefit from: [list tools from their toolkit]. Please allow discreet fidget use at desk and access to a quiet space when needed."
Grandparent-Friendly Explanation
"When children get really nervous, their body hurts — stomach aches, racing heart. It's not fake. These tools are like medicine for the nervous system. They help the body feel safe."
Why This Matters
WHO CCD Package: multi-caregiver training is critical for intervention generalization. When every adult in a child's environment responds to physical anxiety consistently, the nervous system learns safety faster. PMC9978394.
Helpline: 9100 181 181

Questions Parents Ask Us Most About Physical Anxiety and Body-Based Tools
Q: My child has been medically cleared but I'm still not sure these symptoms are anxiety. How do I know?
The key indicators: symptoms appear predominantly before or during stressful situations; symptoms resolve once the situation passes; child has anxiety in other forms (avoidance, excessive worry); symptoms began during a period of increased stress. If all four are present after medical clearance, anxiety is the most likely cause. Consult a child psychologist for formal assessment. Helpline: 9100 181 181.
Q: My child is 4. Are these tools appropriate?
Yes. Weighted blankets (appropriate weight), calm-down jars, fidget toys, and cold tools are all appropriate from age 4. Body mapping and biofeedback are better for age 7+. Always test during calm moments first.
Q: How long before we see results?
Measurable changes typically appear between weeks 3–6. Acute symptom reduction with cold tools can happen within minutes. Building independent tool use takes 8–12 weeks of consistent practice.
Q: Will my child become dependent on these tools?
No. The goal is to build the body's regulation capacity. Tools are scaffolding — they train the nervous system until it can self-regulate more automatically. Most children naturally reduce tool reliance as interoceptive awareness grows.
Q: My child has ASD. Will these tools work differently?
Body-based tools are often MORE effective for children with ASD because they bypass verbal processing. Sensory matching is critical — test each tool during calm first. Biofeedback (data-driven) is often a particularly good fit.
Q: Can I use multiple tools at once?
Yes. Weighted lap pad + fidget + calm-down jar in a calm corner is a multi-tool environment — often more effective than any single tool. Heavy work followed by deep pressure is a particularly powerful sequence.
Q: The school won't allow fidgets. What do I do?
Request a formal accommodation — school counselor or health staff can often facilitate this. Alternatives: smooth worry stone in pocket, compression shirt under uniform, chewing gum (where permitted), or a quiet corner with visual focus objects.
Q: My child's anxiety is very severe. Are these tools enough?
For mild-moderate anxiety, home tools are highly effective. For severe anxiety with functional impairment, professional support is indicated. These tools are the foundation — clinical intervention builds on them. Call 9100 181 181 for guidance.

You've Read the Science. You Understand the Body. Now Start.
Every day without tools is another day the body carries the storm alone. Your child's nervous system is ready to learn. These materials are the first word in a language it already speaks.
✦ OT
Occupational Therapy
✦ Psychology
Pediatric Psychology
✦ ABA
Behavior Analysis
✦ SLP
Speech-Language
✦ SpEd
Special Education
✦ NeuroDev
NeuroDev Pediatrics
📞9100 181 181 | FREE National Autism Helpline | 24×7 | 16+ Languages | pinnacleblooms.org | care@pinnacleblooms.org
Preview of 9 materials that help with physical anxiety symptoms Therapy Material
Below is a visual preview of 9 materials that help with physical anxiety symptoms therapy material. The pages shown help educators, therapists, and caregivers understand the structure and content of the resource before use. Materials should be used under appropriate professional guidance.


















Share this resource
Help others discover thisLink copied!

The Pinnacle Promise
Pinnacle Blooms Network® | Validated by the Consortium
"From fear to mastery. One technique at a time."
This page was drafted by the Pinnacle Blooms Consortium — Clinical Research Officers, Occupational Therapists, Child Psychologists, ABA Therapists, Speech-Language Pathologists, Special Educators, NeuroDevelopmental Pediatricians, and parents of children with neurodevelopmental differences. Not by algorithms. By people who know this journey from the inside.
20M+
Therapy Sessions
Exclusive 1:1 therapy sessions delivered across the network
97%+
Improvement Rate
Measured improvement across readiness indexes, network-wide
70+
Countries Served
Families supported across 70+ countries | 70+ centers in India
Medical Disclaimer: This content is educational and informational in nature. It does not replace individualized assessment and intervention with licensed healthcare professionals. Physical symptoms in children should always be medically evaluated to rule out underlying organic conditions before attributing to anxiety. Individual results may vary.
CIN: U74999TG2016PTC113063 | DPIIT: DIPP8651 (Govt. of India) | MSME: TS20F0009606 | GSTIN: 36AAGCB9722P1Z2
© 2025 Pinnacle Blooms Network®, a unit of Bharath Healthcare Laboratories Pvt. Ltd. All rights reserved. GPT-OS®, AbilityScore®, TherapeuticAI®, FusionModule™, EverydayTherapyProgramme™ are registered trademarks/proprietary systems of Pinnacle Blooms Network®.
📞 9100 181 181 | FREE | 24×7 | 16+ Languages | techniques.pinnacleblooms.org