

"My daughter couldn't leave anything incomplete. If a puzzle piece was missing, she'd melt down. If a song ended before the final note, she'd scream. If I stopped reading mid-sentence, she'd become inconsolable. She had to close every door, finish every video, complete every pattern. I used to think she was being controlling or rigid. I'd try to teach her flexibility by intentionally leaving things incomplete — which only made everything worse. Her psychologist explained that her brain has a strong need for closure — for patterns to be complete. It's neurological, not defiance." — Mother of a 6-year-old, Pinnacle Network

📞FREE National Autism Helpline (16+ languages): 9100 181 181 | pinnacleblooms.org


📞9100 181 181 — FREE | 16+ languages | 24×7


This is NOT stubbornness, rigidity, or a behavior problem. It is a neurological processing style where the brain strongly registers "incompleteness" as aversive — as real as physical discomfort.
The intervention principle: Rather than fighting the need (which fails and increases distress), we work WITH it — providing appropriate pattern completion outlets that satisfy the drive and, over time, build genuine tolerance for real-world incompleteness.




- Select puzzle at child's mastery level — completion should take 5–15 minutes
- Count all pieces BEFORE giving to child. Verify completability.
- Lay out pieces face-up for younger / face-down for older children
- Use language: "Let's build this together. Every piece has a home."
- Allow child to place the final piece — this is the closure moment. Do NOT take it from them.
- Celebrate: "Done! All pieces home. Complete!"
- Record: engagement duration, affect at completion

- Begin with simple AB patterns (red-blue-red-blue-?)
- Present pattern strip with final element missing
- Offer 3–4 choices: "Which one comes next?"
- Allow child to place the completing piece
- Confirm together: "Yes! The pattern is complete!"
- Progress: AB → ABC → AABB → picture sequences → complex visual sequences

- Prepare sorting materials with a FINITE, countable set (e.g., exactly 20 bears)
- Tell child the total: "We have 20 bears. When they're all sorted, we're done."
- Provide clear sorting containers (muffin tin, divided tray)
- Allow sorting at child's pace. Do not interrupt mid-sort.
- Celebrate completion: "All sorted! Every bear has its home. Done!"
- Record time, engagement quality, affect at completion

- ✅ Child is calm (not actively distressed)
- ✅ Child has eaten and is not hungry
- ✅ It has been 30+ minutes since last significant meltdown
- ✅ Environment is reasonably quiet and predictable
- ✅ You (the caregiver) are calm and have 10+ minutes
- ✅ All materials are present and counted (no missing pieces!)
- ✅ Child is familiar with the material (or curiosity is present)

🗣️ "Hey, I've got something really satisfying for us. Look — all these pieces, and they all have one right home. Want to help everything find its place?"

🗣️ "OK, let's see — this piece, where does it go? [pause — let child try] ... Yes! It goes right there. One home found. How many more?"


Time of Day | Activity | Duration | Purpose | |
🌅 Morning | Puzzle or Sorting | 5–10 min | Regulate before demands | |
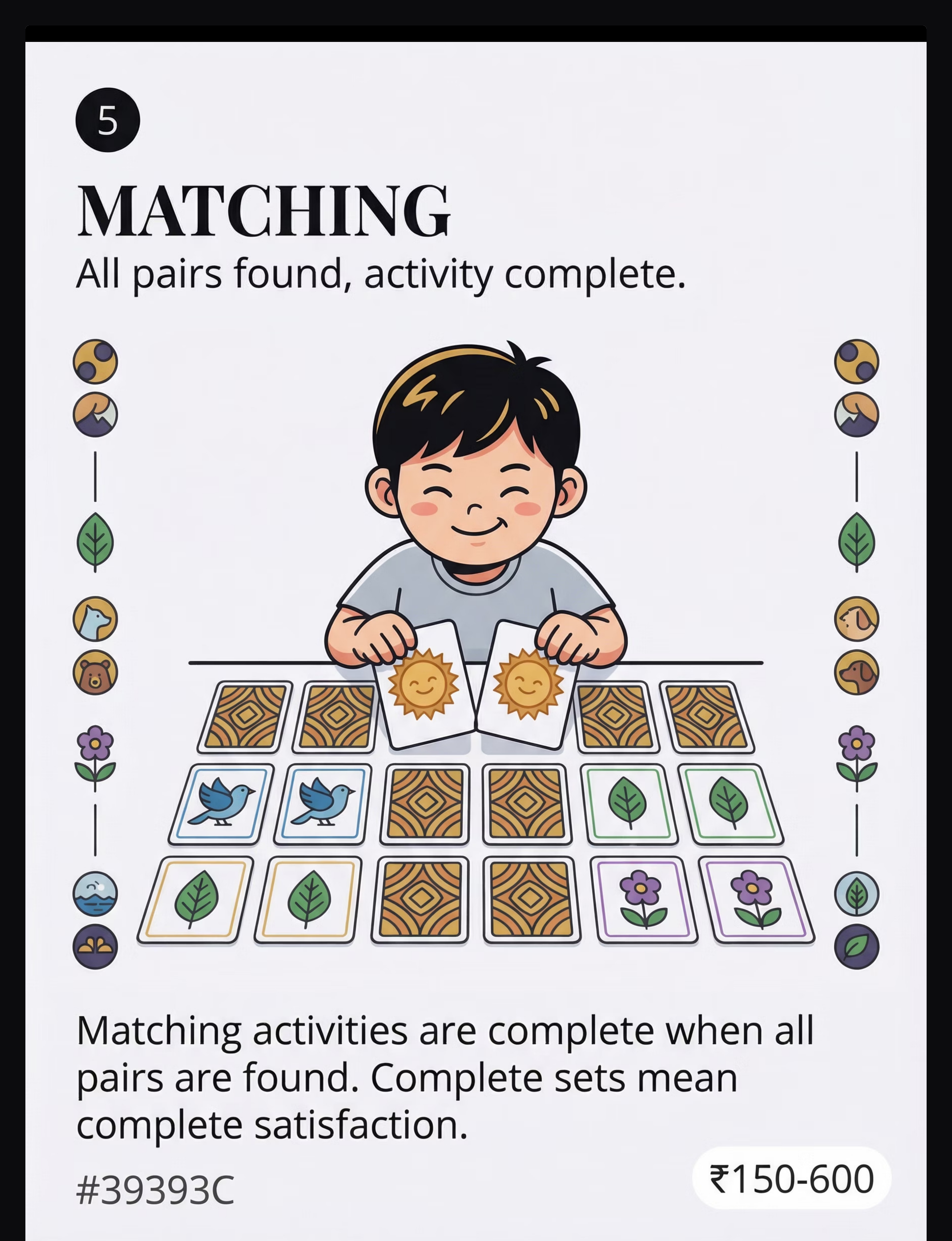
☀️ Mid-day | Pattern Cards or Matching | 5 min | Reset between tasks | |
🌇 Afternoon | Workbook page or Checklist | 5–10 min | Transition buffer | |
🌙 Evening | Construction set or Sequencing | 10–15 min | Calm before sleep |
- Rotate materials: puzzle → sorting → pattern cards → matching (same principle, different medium)
- Increase complexity weekly: 6 pieces → 12 → 24 → 48
- Personalize: use child's interest theme (dinosaur puzzle, vehicle sorting, etc.)
- Social variation: sometimes parallel, sometimes collaborative
- Child looks away repeatedly and doesn't return
- Energy drops suddenly
- Mild agitation or loss of interest
- 3+ errors in a row where success was previous pattern


🗣️ "Two more pieces, then we put the puzzle away until tomorrow. It will wait for us." (After 2 pieces:) "All done for now! The puzzle is complete and it's staying safe right here. We'll see it tomorrow."

○ Puzzle ○ Pattern Cards ○ Sorting
○ Sequencing ○ Matching ○ Workbook
○ Construction ○ Checklist ○ Timer
😣 1 — 😟 2 — 😐 3 — 😊 4 — 😁 5
- Which materials provide the highest completion satisfaction
- Which time-of-day positions are most effective
- When to progress the difficulty level






- Child engages with completion material (even briefly — 2 minutes counts)
- Child shows SOME positive affect at completion (even mild)
- Distress episodes AFTER completion activities are slightly less intense
- Child begins to associate specific material with completion satisfaction
- You (parent/caregiver) feel more confident in how to present activities
- Child still distressed when non-completion activities are interrupted — this comes later
- Child still needs completion of ALL media/games/meals — flexibility builds slowly
- Progress isn't linear — there will be "regression" days



"Most parents who walk into the Pinnacle system are exhausted. They have tried everything. They have cried in bathroom stalls after meltdowns in supermarkets. And then they find that the answer wasn't to fight the need. It was to meet it. You are doing something that most of the world doesn't understand. You are building neurological capacity through daily, patient, scientifically-grounded love. That is extraordinary work." — Pinnacle Blooms Network® Clinical Consortium
Request: AbilityScore® Assessment + Cognitive Flexibility + Anxiety Screening
Professional Pathway: Psychology Assessment → OT Sensory Profile → Anxiety Screening → FusionModule™ Coordinated Plan
Sub-domain | Code | Stage | GPT-OS® Stage | |
Sensory Rigidity | D-375 | Explore | Pre-skill | |
Routine Rigidity | D-376 | Explore | Emerging | |
Transition Challenges | D-377 | ← Previous | Developing | |
Pattern Completion Needs | D-378 | 📍 You Are Here | Approaching | |
Flexibility Building | D-379 | → Next | Proficient | |
Interruption Tolerance | D-380 | Future | Independent |
Request your child's current score at a Pinnacle centre or via: 📞9100 181 181

Time | Activity | Material | Duration | Purpose | |
🌅 7:30am | Morning completion | 12-piece puzzle | 10 min | Regulate before demands | |
☀️ 11am | Sorting task | Rainbow Sorting Set | 5 min | Reset between tasks | |
🌤️ 2pm | Pattern completion | Pattern cards | 5 min | Decompress transition | |
🌆 4pm | Construction | LEGO with instructions | 15 min | Deep engagement | |
🌙 7pm | Checklist review | Day's completion record | 2 min | Satisfaction review | |
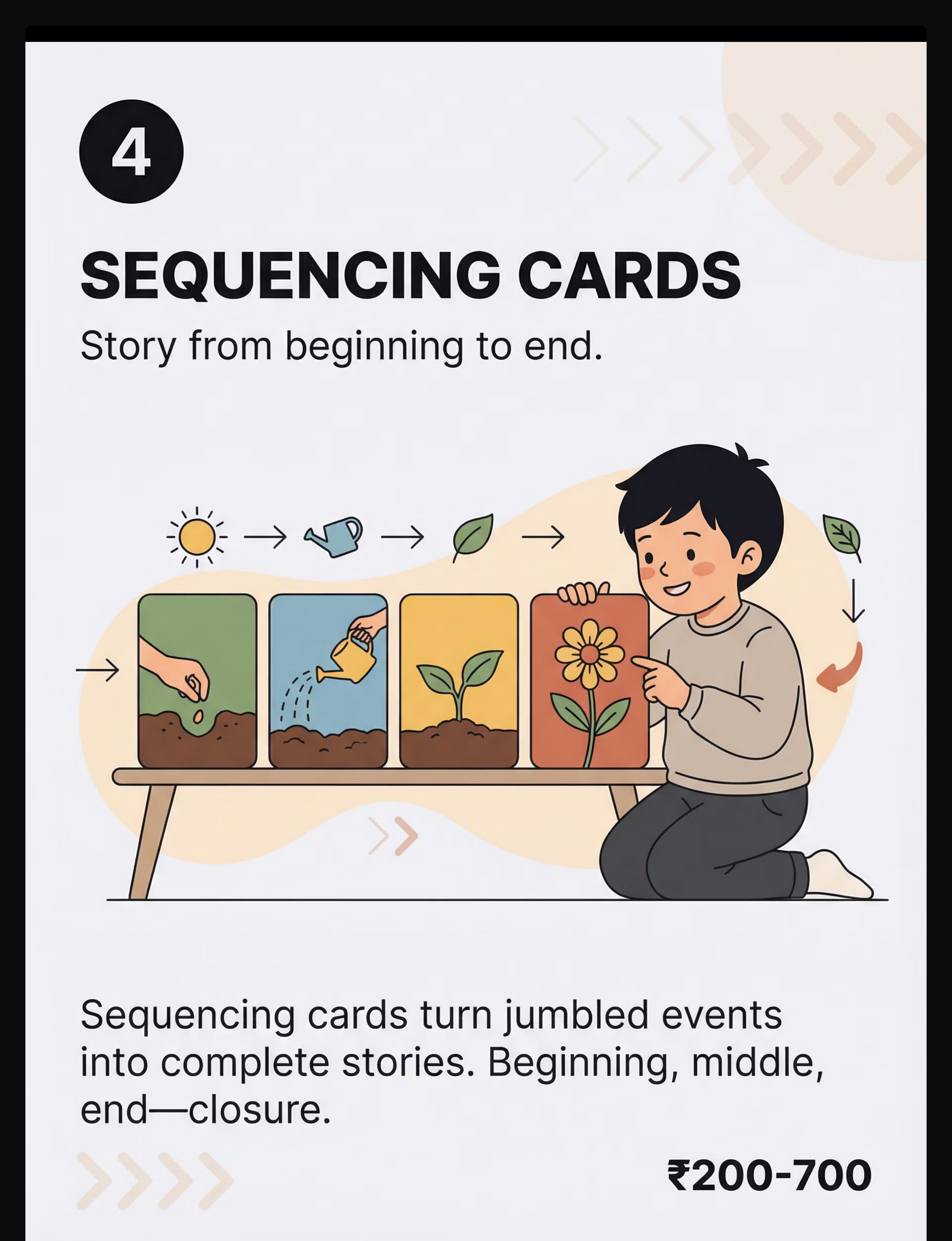
😴 8:30pm | Sequencing | 4-card story sequence | 5 min | Narrative closure for day |
1 × 6-piece knob puzzle · 1 × sorting task (10 items, 2 categories) · 1 × 3-card sequence · 1 × simple pattern strip
This is your regulation toolkit. Deploy when distress is building — before it peaks.
📞9100 181 181 — Personalized completion diet planning available
Service | Lead Discipline | What You'll Get | |
AbilityScore® Assessment | NeuroDev + Psychology | Baseline severity score + complete developmental profile | |
Cognitive Flexibility Evaluation | Psychology + OT | Pattern completion severity + anxiety screening | |
Occupational Therapy | OT | Sensory diet + completion diet design | |
Applied Behavior Analysis | BCBA | Structured flexibility building protocol | |
Parent Training | All disciplines | Home implementation coaching | |
EverydayTherapyProgramme™ | GPT-OS® | Daily home micro-intervention plan | |
FusionModule™ | All disciplines | Converged multi-disciplinary plan |
📞9100 181 181 — FREE consultation guidance | Find a Centre


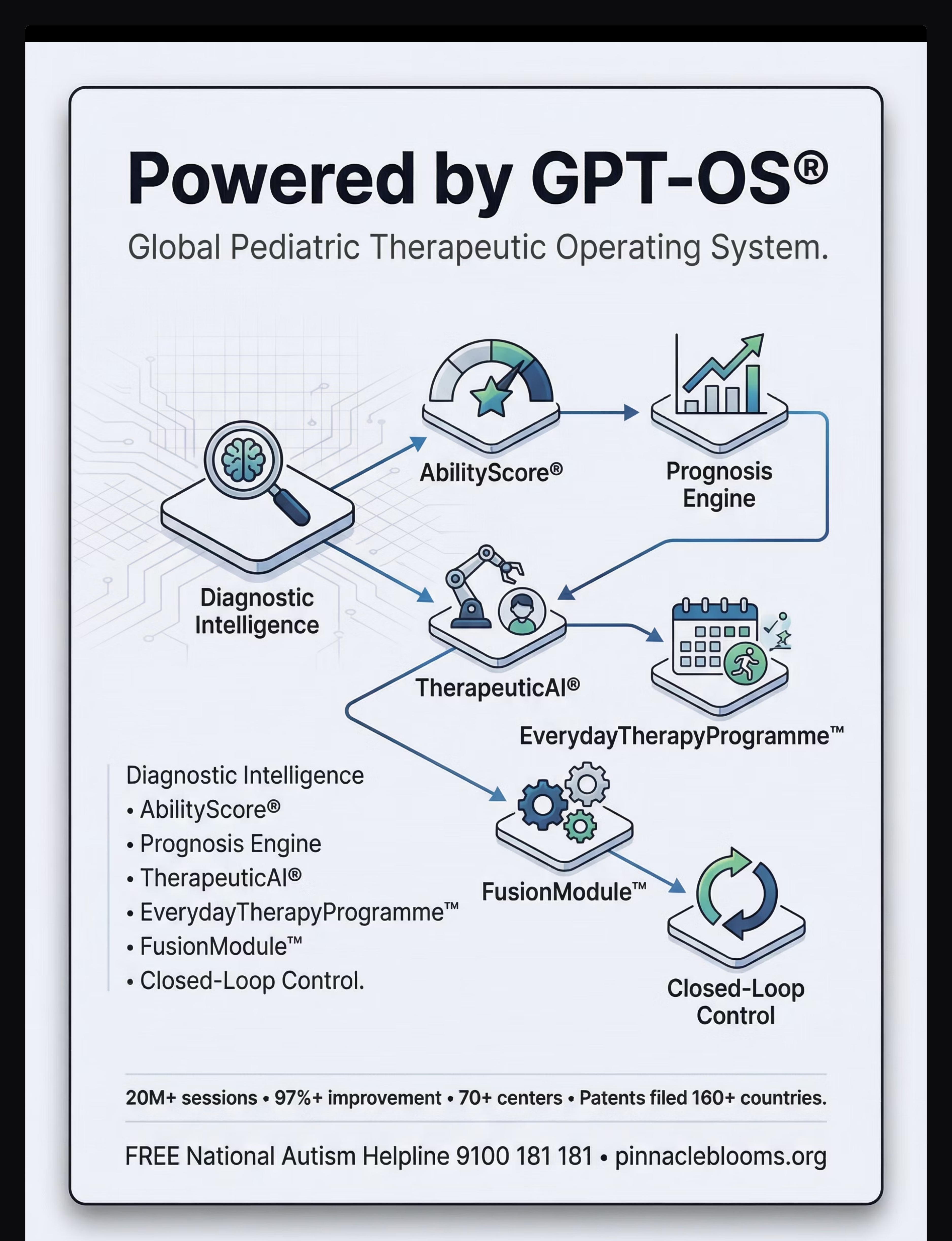
Powered by GPT-OS®
Global Pediatric Therapeutic Operating System Data Transparency When you log a session, your anonymized data updates your child's Cognitive Flexibility Readiness Index, feeds the TherapeuticAI® plan adjustment algorithm, and contributes to population-level patterns that improve recommendations for all children. Privacy: All data is encrypted, anonymized, and governed under Indian DPDP Act compliance standards. Proof Strip 20M+ 1:1 sessions logged 97%+ measured improvement 70+ centres across India 160+ countries — patents filed 📞 9100 181 181 | pinnacleblooms.org



Preview of 9 materials that help with pattern completion needs Therapy Material
Below is a visual preview of 9 materials that help with pattern completion needs therapy material. The pages shown help educators, therapists, and caregivers understand the structure and content of the resource before use. Materials should be used under appropriate professional guidance.















Share this resource
Help others discover this
"From fear to mastery. One technique at a time."
Every technique page on techniques.pinnacleblooms.org is a door. Behind each door is a family — scared, exhausted, searching. Our consortium's singular purpose is to walk through that door with them, with the full weight of 20 million therapy sessions, evidence-based practice, and human expertise.
Your child's brain can learn flexibility. It starts with completion.