
9 Materials That Help With Hand Flapping — Understand the need. Expand the options. Transform regulation.

"The first time my daughter's teacher called to mention the flapping, I cried in the parking lot. I thought I was the only one. I wasn't. Not even close." — Parent, Pinnacle Network



"Sensory integration intervention effectively promotes social skills, adaptive behavior, sensory processing, and motor skills in children with autism spectrum disorder." — World Journal of Clinical Cases, Meta-Analysis, 2024

What it does: Provides hands, arms, and the nervous system with the deep pressure, resistance, vibration, and tactile feedback that flapping seeks — through purposeful, functional, socially flexible alternatives.
Who it's for: Children ages 2–12 with autism, sensory processing differences, motor stereotypies, or any child whose hands seek proprioceptive input for self-regulation.





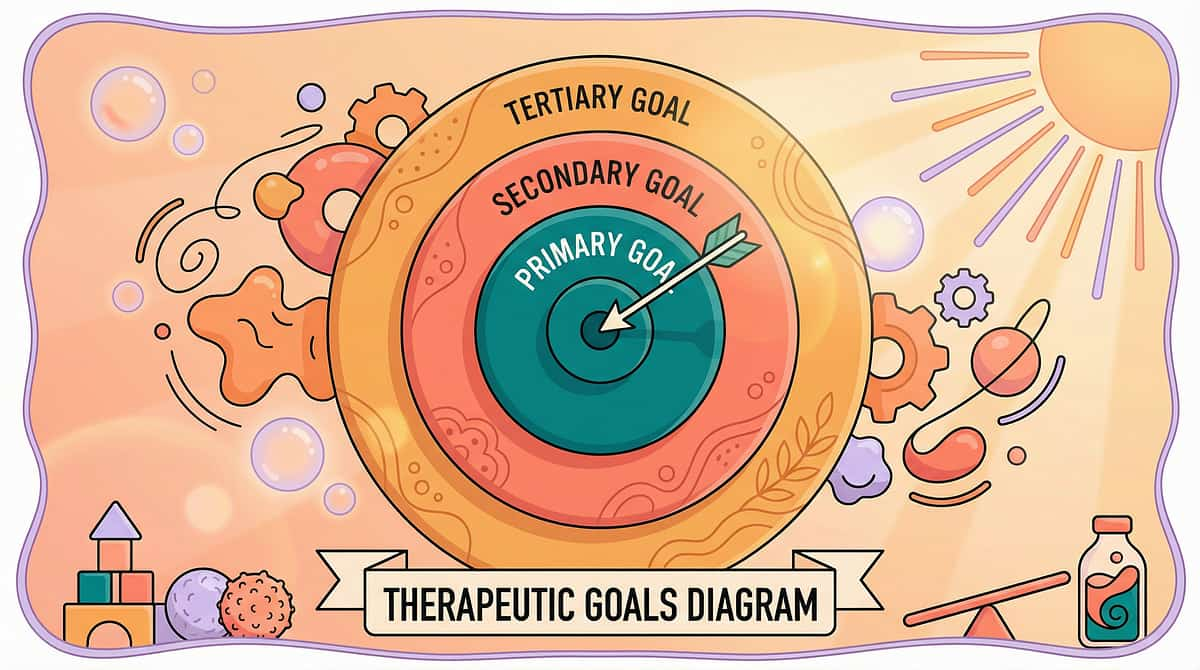
Target Level | You Will See | Timeline | |
Primary | Child reaches for toolkit material instead of flapping (in some contexts) | Weeks 4–8 | |
Primary | Reduced flapping duration when toolkit is available | Weeks 2–4 | |
Secondary | Child can name or indicate their sensory need | Weeks 6–12 | |
Secondary | Improved attention following sensory input | Weeks 2–6 | |
Tertiary | Child self-monitors sensory state and prevents dysregulation | Months 3–6 |

💰 ₹200–600 | Search: "therapy putty resistance levels"
💰 ₹100–800 | Search: "sensory fidget toys autism"

💰 ₹300–1000 | Search: "weighted wrist bands children OT"

💰 ₹150–600 | Search: "hand grip exerciser therapy"

💰 ₹300–1500 | Search: "handheld vibrating massager children"

💰 ₹400–1200 | Search: "compression gloves children autism"

💰 ₹200–1000 | Search: "therapy resistance bands heavy work kit"

💰 ₹200–800 | Search: "kinetic sand sensory bin"

💰 ₹150–700 | Search: "massage roller hand therapy"

Material | Zero-Cost Substitute | Why It Works | |
Resistance Putty | Homemade dough: 2 cups flour, 1 cup salt, 2 tbsp cream of tartar, 2 tbsp oil, 2 cups water — cook until dough forms; add less water for more resistance | Same proprioceptive resistance principle | |
Fidget Toys | Knotted rope, folded cloth, dried beans in a small bag, rubber band collection | Tactile + mild proprioceptive input | |
Weighted Wrist Bands | Sew fabric tubes, fill with rice or sand, add velcro. Start: 100–200g per wrist | Weight = proprioceptive input regardless of source | |
Hand Strengthening Tools | Clothespins (pinching), spray bottles (squeezing), roll of clay, wet sponges to wring | Resistance = proprioceptive feedback | |
Vibrating Massager | Electric toothbrush handle on hands/arms (brief, supervised) | Receptor response is identical | |
Compression Gloves | Tight bicycle gloves (fingerless), elasticised bandage wrap (light) | Compression principle unchanged | |
Heavy Work Kit | Carry filled backpack, push laundry basket, pull full water bucket, do wall push-ups | Heavy work is activity-based; equipment optional | |
Sensory Bins | Basin of dry rice/lentils + small plastic figures to find, or sand in a tray | Tactile + mild proprioceptive input via digging | |
Massage Tools | Rough cloth or towel for friction massage, tennis ball to roll under palm, fingers for joint compression | Deep pressure doesn't require equipment |

• Hands/skin show irritation, injury, or infection
• Child is ill, feverish, or significantly sleep-deprived
• Self-injurious behavior during flapping — consult OT/BCBA first
• Sudden onset of new stereotypy patterns — rule out medical cause
• Child is hungry or fatigued — reduce intensity
• First introduction of any new material — 30-second exposure first
• Allergies: Check wheat/gluten for flour-based putty; latex for rubber-based materials
• Environment is prepared
• You have 10–20 minutes of uninterrupted time
• Child is familiar with at least one toolkit material
💡Lighting: Natural or soft warm light. No harsh fluorescent.
🌡️Temperature: Comfortable — not hot (increases dysregulation).
📱Screens: All screens off — for the parent too.
🧹Floor Space: 2 square meter clear area if heavy work included.
⏱️Timer: Visual timer visible to child (sand timer or countdown app).
📦Materials: Pre-selected 2–3 options maximum. Choice overload is dysregulating.
- Other children's toys not in use today
- Strong smells (perfume, candles)
- Any recently distressing objects
- Pets if they cause distraction
① Putty + fidgets within arm's reach
② Bin / heavy work at the side
③ Massage tools accessible nearby
④ Child on floor or low chair, stable position
⑤ Parent seated at the same level

60 Seconds. 7 Questions. One Decision. The Best Session Is One That Starts Right.
ACT III: THE EXECUTION Indicator ✅ Green 🔶 Modify ❌ Postpone Last meal 1–2 hrs ago 30 min ago Hungry/just ate Sleep last night Good (age-typical) Slightly tired Overtired Current arousal Calm or mildly alert Slightly elevated Meltdown/shutdown Response to name Responds Delayed response Not responding Physical state No illness signs Mild restlessness Ill/distressed Flapping intensity Baseline Elevated Continuous, intense Last meltdown >4 hours ago 2–4 hours ago <2 hours ago 5–7 ✅ Green Full session. All materials available. 3–4 ✅ Green Shortened session. 1 familiar material only. 5 minutes max. Fewer than 3 ✅ Postpone today. Offer calming input: gentle weighted blanket, dim room, quiet. If Modify — Simplified Version: Bring one piece of familiar putty. Sit together. No demands. Let the child's hands do what they need. Be present. That IS the session today. ABA Antecedent Manipulation: Setting event conditions determine intervention effectiveness | Pinnacle Clinical Pre-Session Readiness Protocol

Every Protocol Begins with an Invitation. Never a Command.
STEP 1 ⏱️ 30–60 seconds Parent Script "I have something for your hands. Want to see?"OR"Time for hand time. Come sit with me for a minute."OR (non-verbal): Silently place one piece of putty on the table between you and wait. Body Language • Get to the child's level — sit on the floor if needed• Relaxed posture, no urgency in expression• Hold the material casually — explore it yourself first• Slow movements. No sudden presentation. ✅ Acceptance Cues — What to Look For Child looks at material | Child moves toward material | Child reaches out | Child's body softens | Flapping pauses or changes quality 🔶 Resistance Cues — What to Do Child turns away: Don't push. Sit quietly 30 more seconds. Try one different material.Child walks away: Follow (if appropriate) or let them. Today's invitation is for information.Child becomes distressed: End invitation. No force. Data collected. ABA Principle: This is pairing — building positive association between the material and the parent's presence before any demand is placed. Rushed pairing = failed sessions later. ABA Pairing Procedures: Establishing motivating operations before demand placement | OT Just-Right Challenge: Matching task to current capacity



Material | Target Reps | Satiation Signs | Don't Exceed | |
Putty | 5–10 squeeze cycles | Hands slow, interest wanders | 15 min continuous | |
Fidget | 3–5 min continuous | Child puts down unprompted | Child's choice | |
Weighted bands | 20–30 min wear | Child removes or distress | 30 min per session | |
Grip exerciser | 10 reps × 2–3 sets | Fatigue, avoidance | Hand fatigue | |
Vibration | 1–3 min per area | Child pulls away | 5 min per session | |
Compression gloves | Up to 2 hours | Circulation check | Per OT guidance | |
Heavy work | 5–10 min session | Fatigue, refusal | Exhaustion | |
Sensory bin | 5–15 minutes | Interest wanes | Child's choice | |
Massage | 2–5 minutes | Child signals stop | Child's choice |

✅"You squeezed! That's what your hands needed!"
✅"Look at you! Hands working hard!"
✅ (Non-verbal): Thumbs up + smile + brief shoulder touch if accepted
❌"I'm so proud you're using this instead of flapping" — frames flapping as wrong
✅"I love how you tried the putty" — reinforce toolkit use, not suppression
Tier 2 — Token system: Sticker on chart after each successful sensory session (5 stickers = preferred activity).
Tier 3 — Natural consequence: After heavy work → preferred calming activity. After putty → free fidget time.


Child's engagement level: 1–5 scale (1=rejected, 5=fully engaged). Example: "4 — sustained for 8 min"
Flapping before vs. during: Estimate: more/same/less. Example: "Less during putty, returned after"
- "She always rates 4 or 5 with putty but 1 with vibration."
- "He's most regulated on days when we start with heavy work."
- "Engagement doubles when sessions happen before transitions."

Session Abandonment Is Not Failure. It Is Data.
Every session — good or difficult — teaches you something. The troubleshooting guide below gives you a clear path forward for the seven most common session challenges parents encounter. Child refused all 9 materials Why: Sensory profile may not align with these material types, or today's arousal state made any input intolerable.Next time: Slow down the invitation phase (Card 14). Pre-pair materials over 3–5 days before expecting engagement. Try materials in a different context (bathtime, outdoor play). Child engaged briefly then ran away Why: The sensory input met the need quickly — or the session duration exceeded the child's tolerance window.Next time: 30-second engagement = success at this stage. Build duration gradually. Keep invitation language completely demand-free. Child flapped more during/after the session Why: Some highly stimulating materials (vibration, heavy work) can activate before they calm.Next time: Follow stimulating materials with calming ones. Heavy work → compression or weighted bands. Sequence matters. Child used the material incorrectly (threw putty, chewed fidget) Why: The child is exploring through their primary sensory modality — this is information about their sensory profile.Next time: For oral seekers — consult OT about oral motor tools. For throwers — provide heavier, more resistive materials in a safer context. Parent ran out of patience mid-session Why: Completely normal. Managing your own regulation while supporting your child's is genuinely hard.Next time: Shorter sessions (5 minutes) until confidence builds. Tag-team with another caregiver. You cannot pour from an empty cup. Child used toolkit AND flapped — "it didn't work" Reframe: Sensory toolkit use and flapping are not mutually exclusive. Co-occurrence is progress. "My child squeezed the putty for 4 minutes AND flapped at the end. That's 4 minutes of new regulatory behavior that didn't exist last week." Can't tell if it's helping Why: Short-term effects can be subtle. Without data (Card 20), changes are invisible.Next time: Implement the tracker for 2 weeks. Patterns emerge that single-session observation cannot reveal. ABA Troubleshooting: Functional analysis principles applied to session-level problem solving | Antecedent modification from behavioral literature
1 material → 3 materials → All 9
Soft putty → Medium → Extra-firm
5 seconds → 2 minutes → 10+ minutes
Parent-guided → Child-led → Independent
Home only → + School → All contexts
Ages 4–6: Fidgets + putty + heavy work games. 10 minutes. Mix structured and play.
Ages 7–10: Full toolkit. Introduce self-selection and self-monitoring.
Ages 10–12: Child designs own sensory diet. Parent is support, not director.
For Mixed Seekers (proprioceptive + tactile): Open each session with sensory bin (tactile entry), then transition to putty or fidgets. Massage tools to close.
For Sensory Avoiders who incidentally flap: Start with lightest materials: soft putty, compression gloves (passive input), massage tools at low pressure. Never force.
For Non-Verbal Children: Use choice boards — photos of 3 materials → child points to preferred → that's the session material. Builds communication AND sensory self-advocacy simultaneously.

In Weeks 1–2, You Are Building Trust Between the Toolkit and the Nervous System.
ACT IV: THE PROGRESS ARC Foundation Phase Progress is real but subtle in weeks 1–2. Track it. What Progress Actually Looks Like (Week 1–2) ✅ Child allows material near their body (even without engaging)✅ Child tolerates one material for 10+ seconds longer than day 1✅ Child shows curiosity (looks, approaches)✅ Flapping intensity slightly lower during material exposure✅ You feel slightly more confident introducing materials What Is NOT Progress Yet (and that's fine) ❌ Child preferring toolkit over flapping — too soon❌ Consistent independent use — not expected❌ Dramatic flapping reduction — not yet❌ Generalization to school — not this phase Patient Metric: "If your child tolerates a material for 10 seconds longer than last week — that is real, measurable, clinical progress. Track it on your Card 20 sheet. Write it down." Weeks 1–2 are the hardest. The novelty of the toolkit may provoke resistance. Flapping may temporarily increase because you've introduced change into the sensory environment. This is normal. Stay consistent. You are building the habit before you see the benefits. PMC11506176: SI intervention outcomes emerge across 8–12 week timelines. Early-phase indicators: tolerance and participation rather than skill mastery


Mastery Is Not the Absence of Flapping. It Is the Presence of Choice.
Mastery Phase Weeks 5–8: independent use emerging in multiple contexts. ✅ Independent Access Child accesses sensory toolkit in at least 1–2 contexts without prompting. ✅ Self-Advocacy Emerging Child can indicate (verbally, gesture, or AAC) when they need sensory input. ✅ Regulatory Flexibility Child accepts 3+ different materials from the toolkit. Multiple pathways to regulation established. ✅ Generalization Toolkit use spreading to new settings: grandparents' home, in the car, at school. Child requests a specific material by name or picture. 🏆 D-362 Mastery Unlocked: Child has used toolkit independently in at least 3 different settings over 2 consecutive weeks.Next steps: ✅ Stay if mastery is emerging but not stable (reinforce 2 more weeks) | ✅ Progress to D-363 Rocking & Swaying | ✅ Deepen with material deep-dive protocols PMC10955541 (2024): Sensory integration therapy across 24 studies showed effective promotion with measurable outcomes | BACB mastery criteria standards

Your child's nervous system didn't change overnight. But your understanding of it did. And that understanding is the most powerful therapy tool in this entire toolkit.

Why it matters: Self-injury changes the clinical picture entirely — the sensory need may be more intense or the function may be different.
What to do: Stop home protocol. Contact OT/BCBA for functional behavior assessment.
Why it matters: Change can signal medical cause, medication effect, or significant anxiety increase.
What to do: Teleconsult with developmental pediatrician before continuing.
Why it matters: Regression + increased stereotypy = medical evaluation priority.
What to do: Pause all behavioral interventions. Seek urgent developmental pediatrician review.
What to do: Discontinue that specific material. Teleconsult with OT for material adjustment.
Why it matters: Parent regulation is prerequisite for child regulation.
What to do: Pause sessions. Contact helpline for caregiver support resources.
Why it matters: This material set may not match this child's sensory profile. OT assessment needed.
What to do: Book AbilityScore® assessment. OT sensory processing evaluation.
📞FREE National Autism Helpline: 9100 181 181 | 16+ Languages | 24×7
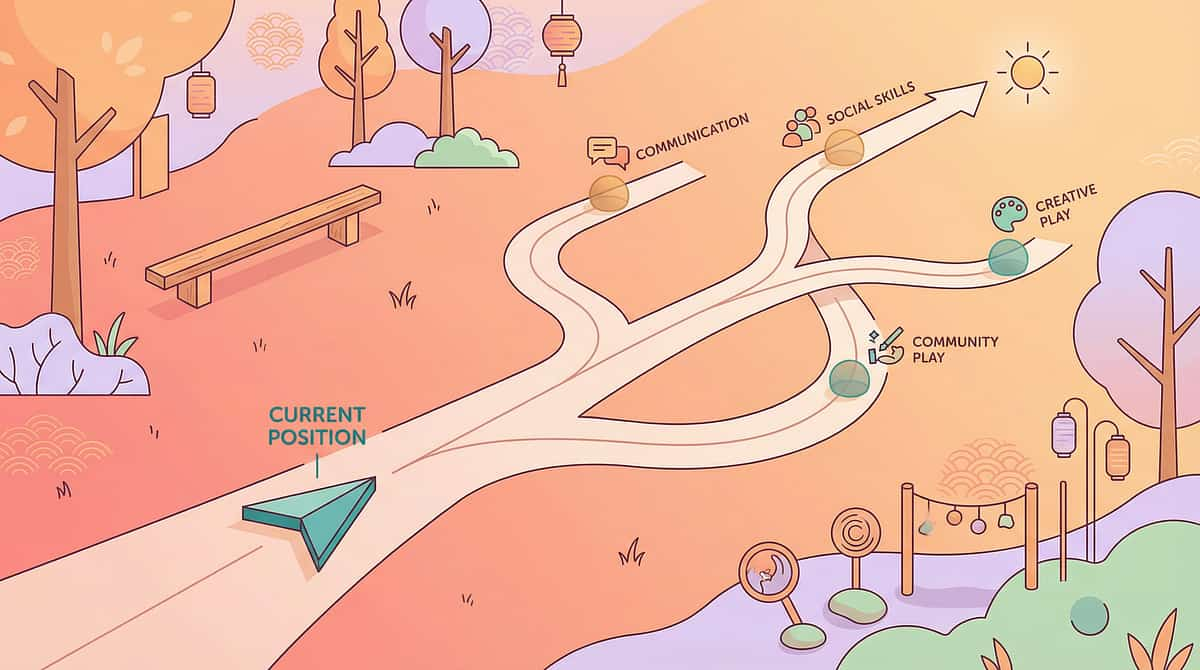
You Are Not Done. You Are On a Journey With a Clear Forward Path.
Completing D-362 doesn't close a chapter — it opens a pathway. Your child's sensory regulation toolkit is now the foundation for the next level of growth. If flapping is the primary challenge → D-363 Rocking and Swaying (similar proprioceptive profile, materials you already own) If environments are the primary trigger → D-364 Sensory Overload Management If toolkit is working but needs systematizing → D-370 Full Sensory Diet Design If school generalization is the goal → D-365 Generalization Across Settings Long-Term Developmental Goal: This technique feeds into: Sensory Regulation Readiness Index → Body Awareness Readiness Index → Self-Regulation Readiness Index → Environmental Participation Readiness Index WHO Developmental Milestones Framework + domain-specific sequencing literature | GPT-OS® developmental trajectory mapping
Technique | Code | Difficulty | Materials You Own | |
9 Materials for Rocking & Swaying | D-363 | 🔵 Core | Weighted bands, heavy work kit | |
Sensory Overload Management | D-364 | 🟡 Advanced | Compression gloves, fidgets | |
Transition Preparation Tools | D-360 | 🟢 Intro | Fidgets, visual timers | |
Environmental Structure | D-361 | 🟢 Intro | Sensory bins, calm space setup | |
Sensory Diet Planning | D-370 | 🟡 Advanced | All 9 materials from D-362 | |
Generalization Across Settings | D-365 | 🟡 Advanced | Portable kit from D-362 |
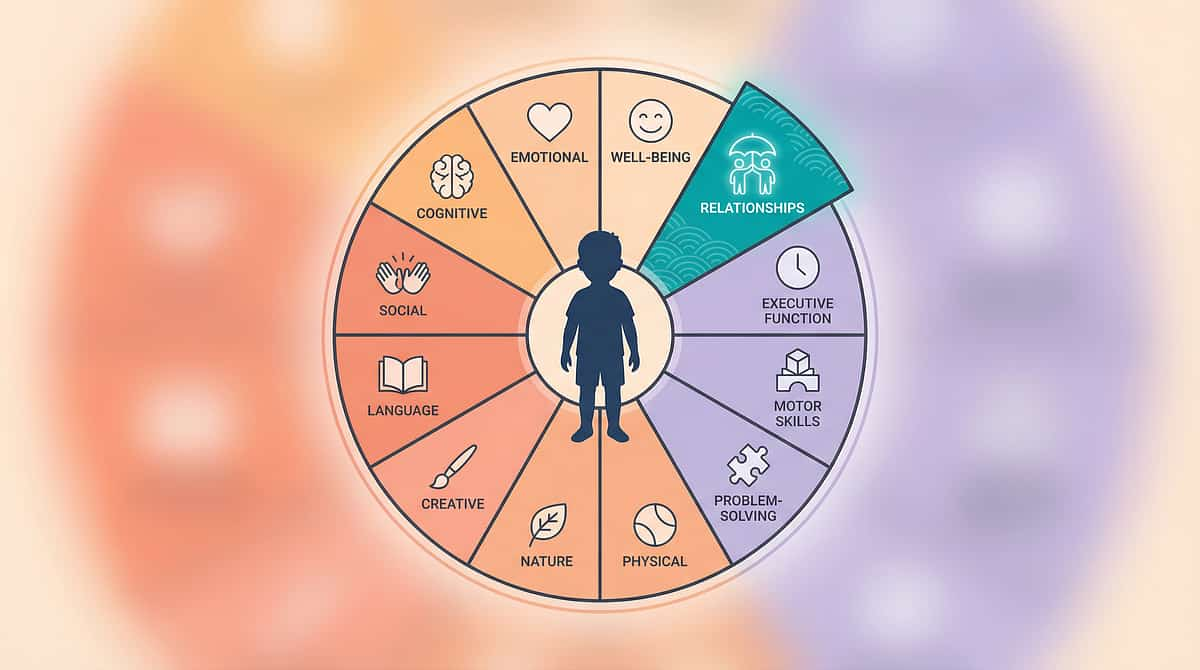

(Anonymized case. Identifying details changed. Outcomes vary.)
(Parent, Pinnacle Network. Anonymized.)
"The most common turning point we see: the moment a parent stops asking 'how do I make the flapping stop?' and starts asking 'what does my child need right now?' That shift in question changes everything." — Pinnacle OT Consortium

→ pinnacleblooms.org/community/sensory-regulation
→ pinnacleblooms.org/forum/domain-d
→ pinnacleblooms.org/centers
→ Request mentor: 9100 181 181
"Your journey through D-362 will become the map for another parent who is where you were at Week 1. Consider sharing your story."
→ pinnacleblooms.org/centers
📞 Book OT consultation: 9100 181 181
→ pinnacleblooms.org/teleconsult
- Standardized sensory processing assessment — not guesswork
- Precise material intensity matching to your child's profile
- Sensory diet design across all 12 hours of your child's waking day
- School consultation and teacher coordination
- AbilityScore® progress tracking across all 12 domains
No appointment needed for the helpline. Call to discuss, then book.
• Individual child data never shared with third parties
• DPIIT-registered data practices: DIPP8651 (Govt. of India)
• Compliant with IT Act 2000 and Digital Personal Data Protection Act 2023
- Diagnostic Intelligence: Sensory processing profile identification
- TherapeuticAI®: Material-to-profile matching algorithms
- EverydayTherapyProgramme™: Daily sensory diet embedding
- Prognosis Engine: 8-week outcome trajectory based on response data
- Closed-Loop Control: Session data → plan → re-measure → adapt


📧Email — Send to school teacher, grandparents, doctor
🔗Copy Link — techniques.pinnacleblooms.org/behavior-regulation/hand-flapping-materials-D-362
→ pinnacleblooms.org/resources/D-362-family-guide
"[Child's name] sometimes flaps their hands when excited or overwhelmed. This is their nervous system asking for sensory input — not misbehavior. When you see it, please don't hold their hands down. Instead, offer them their sensory putty or fidget toy from the bag I've packed. These materials give their brain what it needs. We're building their ability to self-regulate. Your support makes this work."
"Dear [Teacher name], [Child's name] has been working with our OT on a sensory diet that includes 9 specific materials for proprioceptive regulation. Hand flapping is a sensory-seeking behavior, not a behavioral challenge. I'd like to schedule a 15-minute consultation to discuss classroom accommodations — fidgets at the desk, compression gloves during focused work, and heavy work breaks before demanding tasks."


Available in: Telugu, Hindi, Tamil, Kannada, Malayalam, Bengali, Marathi, Gujarati, Punjabi, Odia, Assamese, Urdu, English + 3 more. No registration. No appointment. Just call.
Preview of 9 materials that help with hand flapping Therapy Material
Below is a visual preview of 9 materials that help with hand flapping therapy material. The pages shown help educators, therapists, and caregivers understand the structure and content of the resource before use. Materials should be used under appropriate professional guidance.




















Share this resource
Help others discover this
From Fear to Mastery. One Technique at a Time. — The Pinnacle Blooms Consortium
Pinnacle Blooms Network® exists to transform every home into a proven, scientific, personalized, multi-disciplinary pediatric therapy environment — accessible to every family, regardless of geography or income, through the power of the GPT-OS® Global Pediatric Therapeutic Operating System. 🔄 Return to Top Begin again with Card 01 — recognition grounds every visit. ➡️ Next: D-363 9 Materials That Help With Rocking & Swaying — your toolkit is already 90% ready. 🏠 Browse All Techniques techniques.pinnacleblooms.org — 999 evidence-based technique pages 📞 Get Help Now 9100 181 181 | FREE | 16+ Languages | 24×7 Medical Disclaimer: This content is educational and does not replace individualized assessment with licensed occupational therapists, behavior analysts, or developmental specialists. Hand flapping and motor stereotypies can be associated with various conditions; professional evaluation is recommended. The goal is not elimination of all stereotypy but supporting regulation and expanding options. Individual results may vary. Statistics represent aggregate outcomes across the Pinnacle Blooms Network. Always consult qualified healthcare professionals before implementing therapeutic protocols. Statutory Identifiers: CIN: U74999TG2016PTC113063 | DPIIT Recognition: DIPP8651 (Govt. of India — Startup India) | MSME: Udyog Aadhaar TS20F0009606 | GSTIN: 36AAGCB9722P1Z2 © 2025–2026 Pinnacle Blooms Network® | A unit of Bharath Healthcare Laboratories Pvt. Ltd. | Content developed under GPT-OS® Content Engine | Technique Code: D-362 | Published: techniques.pinnacleblooms.org/behavior-regulation/hand-flapping-materials-D-362 ← D-361: Environmental Structure | → D-363: 9 Materials That Help With Rocking & Swaying 📞 FREE National Autism Helpline: 9100 181 181 | 16+ Languages | 24×7