
When every drop feels like danger.
Your child's water fear is real. Their nervous system is not overreacting — it is doing exactly what it was wired to do. These 40 cards will show you why, and how to help.
"Bath time in our house is a war zone. The moment my daughter hears the water running, the screaming starts. Not crying — screaming. She's five years old and I still can't wash her hair without her acting like I'm hurting her. She claws at my arms, tries to climb out of the tub, hyperventilates. Last night she was shaking so hard her teeth were chattering — and the water wasn't even cold. It's not defiance. I can see it in her eyes. She's terrified."
You are not failing. Your child's nervous system is speaking. And today, we listen.
🔵 Pinnacle Blooms Consortium®
Validated by: Occupational Therapist • Child Psychologist • BCBA • Pediatric SLP • NeuroDevelopmental Pediatrician
Series: C-285
Sensory Processing & Emotional Regulation | Ages 2–12

Millions of families. One fear. Real solutions.
Water fear in children — from bath time resistance to full aquaphobia — affects millions of families across India and the world. For children with sensory processing differences, autism, anxiety disorders, or trauma histories, water presents unique neurological challenges. You are among families in over 70 countries who have walked this path with Pinnacle.
80%
Sensory Impact in ASD
of children with ASD experience sensory processing difficulties affecting daily routines including water
1 in 36
Autism Prevalence
children in India are now diagnosed with autism spectrum disorder (WHO/CDC aligned data)
97%+
Measurable Improvement
of children receiving GPT-OS®-governed sensory intervention show measurable improvement
"You are not the only family where bath time is a battle. You are part of a community finding a way through."
This is not defiance. This is neuroscience.
What Happens in the Brain
When water touches your child's skin — or even when they hear water running — a part of the brain called the amygdala fires an alarm signal. In children with sensory processing differences, this alarm fires more intensely than in typical children.
The brain doesn't yet have a stored signal that says "water is safe." Instead, every water encounter reads as potential danger — triggering the same body response as a real threat: heart rate spikes, breathing quickens, muscles tense, cortisol floods the system.
The Sensory Pathway
For sensory-based water fear, three systems activate simultaneously:
- Somatosensory cortex — tactile hypersensitivity to water on skin
- Vestibular system — fear of balance loss in water
- Interoception — confusion about body awareness in wet or buoyant environments
Your child is not choosing this response. Their nervous system is executing its programming.
"This is a wiring difference, not a behaviour choice."

Your child is here. Here is where we are heading.
Some water wariness is developmentally normal — many toddlers resist baths between 18 months and 3 years as they develop autonomy. Most children outgrow this naturally. However, persistent, intense fear that doesn't diminish with age, significantly impacts hygiene or safety, or is disproportionate to any negative experience may indicate a phobic response or sensory processing challenge requiring targeted intervention.
18 Months – 3 Years
Normal bath wariness phase — developing autonomy
3 – 5 Years
Fear persists = signal to act. Begin desensitization protocol
5 – 7 Years
With intervention: tolerance builds, functional bathing achievable
7 – 10 Years
Water safety skills established, community participation begins
10 – 12 Years
Pools, beaches, swimming lessons — full community inclusion
⚠️Water safety is a life skill. Children who cannot engage with water without panic are at elevated drowning risk. This intervention addresses both the fear and the safety imperative.

Clinically validated. Home-applicable. Parent-proven.
The graduated desensitization approach used in this protocol is validated across occupational therapy (Ayres Sensory Integration), cognitive-behavioural therapy (CBT exposure hierarchy), and applied behaviour analysis (systematic desensitization). Three disciplines. One evidence base. One protocol you can start today.
LEVEL II — STRONG EVIDENCE
PRISMA Systematic Review (2024) — 16 studies (2013–2023) confirm sensory integration intervention is evidence-based practice for children with ASD. Sensory desensitization protocols show significant reduction in sensory-based avoidance behaviours including water fear. 📎 PMC11506176
Meta-Analysis
World J Clin Cases (2024) — Sensory integration therapy across 24 studies effectively promotes adaptive behaviour, emotional regulation, and sensory tolerance. Effect sizes strongest for structured, graduated exposure protocols. 📎 PMC10955541
Indian RCT
Indian Journal of Pediatrics (2019) — Home-based sensory interventions administered by trained parents showed significant outcomes, establishing the safety and efficacy of parent-delivered sensory protocols in Indian contexts. 📎 DOI: 10.1007/s12098-018-2747-4

What Is Water Fear? Clinical Definition
ACT II: Knowledge Transfer
Fear of water in children ranges from mild bath time reluctance to severe phobic responses that prevent any water contact. Understanding the type of fear your child experiences is the first step toward the right intervention approach.
🔵 Sensory-Based
The feeling of water on skin, wetness, temperature sensitivity, the overwhelming nature of water sounds and movements
🔴 Trauma-Based
A negative water experience such as choking, going underwater unexpectedly, or witnessing drowning
🟡 Developmental
Loss of control, unpredictability, the strange sensation of buoyancy, or the visual depth of water
🟢 Anxiety-Based
Part of broader anxiety patterns or generalised phobic responses
For sensory-sensitive children and those with ASD, water presents unique multi-sensory challenges simultaneously: unpredictable temperature, pressure against skin, sound of water rushing, visual movement, vestibular changes, and the physical sensation of buoyancy. Any one of these can be a trigger — many children experience all simultaneously.

Which Disciplines Lead This Intervention
This technique crosses therapy boundaries because the brain doesn't organise by therapy type. The Pinnacle FusionModule™ ensures that no discipline works in isolation — all from the same data, in the same session cycle, measured by the same AbilityScore®.
Occupational Therapy (Lead)
Sensory integration protocol design, environmental modification, graduated exposure hierarchy, vestibular and proprioceptive support
Child Psychology
Phobia treatment (CBT exposure hierarchy), trauma-informed approach, anxiety management, family psychoeducation
ABA Therapy
Systematic desensitization programming, reinforcement scheduling, data-based decision making, antecedent modification
Special Education
Social story creation, visual support design, routine structuring, AAC-supported communication during bath time
NeuroDev Pediatrics
Medical rule-outs, SPD diagnosis, medication consideration for severe anxiety, developmental monitoring

What This Targets
This isn't a random activity. This is a precision therapeutic tool designed to address specific neurological and behavioural outcomes at three levels — from immediate fear reduction to long-term community inclusion.
Observable behaviour indicators show measurable progress: child tolerates bathroom sounds without panic → approaches tub without physical restraint → allows water on extremities → completes hair washing with minimal distress → engages in water play outside tub → eventually participates in pool activities with support.

The 9 Materials: Your Complete Toolkit
Nine carefully selected materials. One complete toolkit. Starting from ₹100. Each material serves a specific neurological purpose — together, they create a graduated, child-controlled exposure environment that transforms bath time from a battleground into a place of safety and even play.
Graduated Pouring Cups
Water on their terms | ₹200–800
Visual Routine Cards
See what's coming | ₹150–500
Bath Visor / Shampoo Shield
Face stays dry | ₹200–600
Water Thermometer
Proof it's safe | ₹300–1,000
Non-Slip Bath Mat
Stable body, calmer mind | ₹300–1,500
Engaging Bath Toys
Fun competes with fear | ₹200–1,500
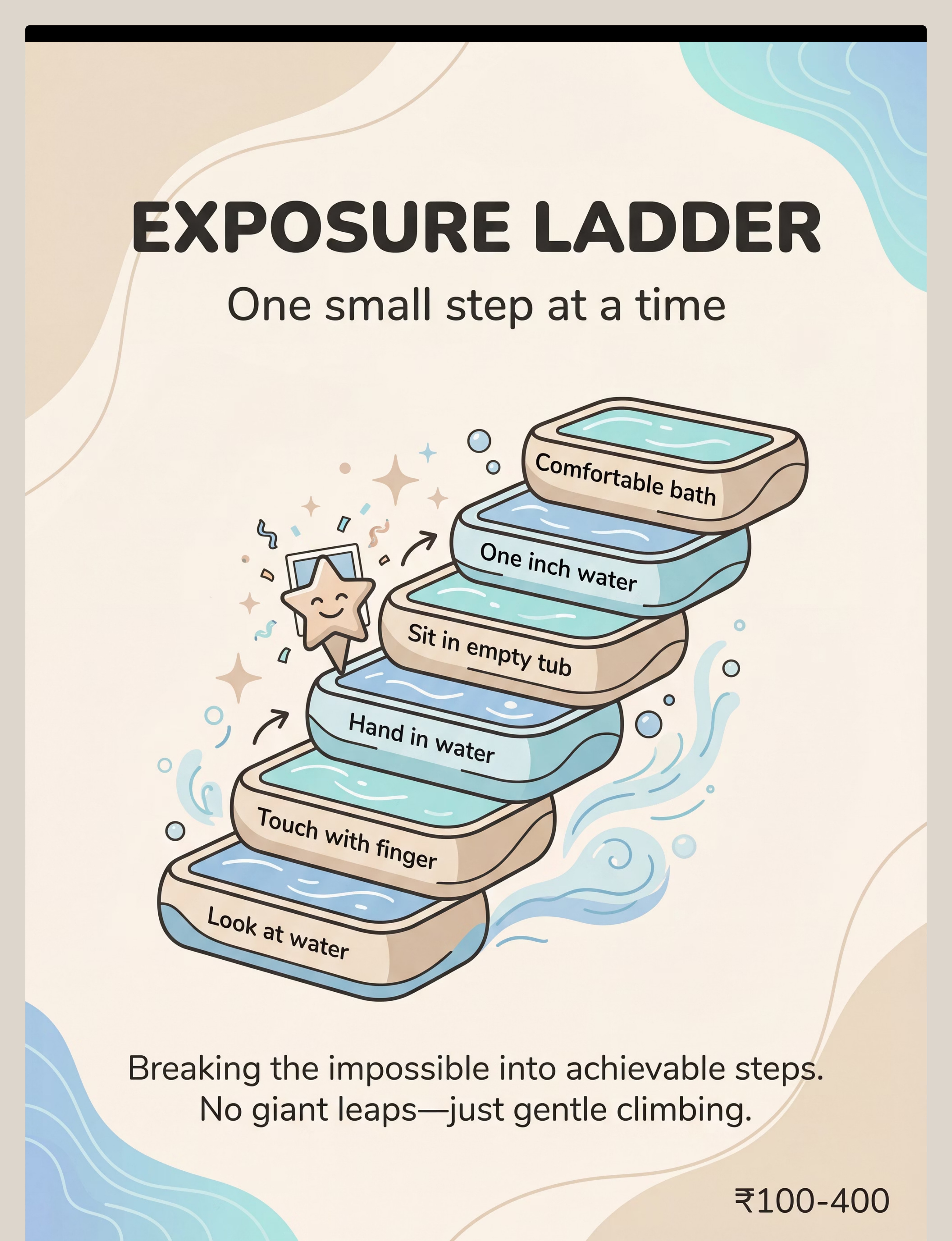
Exposure Ladder Chart
One small step at a time | ₹100–400
Calming Sensory Add-Ins
Water that feels different | ₹200–800
Flotation Devices
Safe enough to try | ₹500–3,000
🏅Pinnacle Recommends: Non-slip mat + bath visor + visual routine cards — the clinically validated starter trio. Total cost: approximately ₹650–2,600.
DIY & Substitute Options
Every child deserves this intervention — regardless of budget. Evidence-based intervention should never be gatekept by economics. The therapeutic mechanism is identical whether you use a store-bought kit or household items. The nervous system responds to graduated exposure and child-led control — not to brand names. A ₹0 measuring cup and a ₹800 water play set activate the same desensitization pathway.
🛒 Buy This | 🏠 Make This (₹0) | |
Graduated Pouring Cups (₹200–800) | Kitchen measuring cups, recycled plastic bottles of varying sizes, funnels from any kitchen | |
Visual Routine Cards (₹150–500) | Photograph each bath step with your phone, print at local shop, laminate with tape | |
Bath Visor (₹200–600) | Flexible sun visor + washcloth firmly held across forehead; swimming goggles for eye protection | |
Water Thermometer (₹300–1,000) | Inexpensive floating thermometers available everywhere; test water on your own wrist first | |
Non-Slip Mat (₹300–1,500) | Textured adhesive strips applied to tub floor; rolled bath towel under child's knees | |
Bath Toys (₹200–1,500) | Kitchen containers (strainers, cups, spoons), ice cubes for temperature play, food colouring for colour water | |
Exposure Ladder Chart (₹100–400) | Draw a staircase on paper with 10 steps, write each exposure level, use star stickers as progress markers | |
Sensory Add-Ins (₹200–800) | 2 tbsp Epsom salt + 2 drops lavender oil (test for skin sensitivity first); shaving foam on tub walls | |
Flotation Device (₹500–3,000) | Begin in very shallow water (≤5cm) where child can always stand and touch bottom |

Safety First — Before You Begin
Read this before your first session. Non-negotiable. Safety is not a checklist item — it is the foundation on which every therapeutic interaction is built. A child who feels unsafe cannot learn. A caregiver who is dysregulated cannot teach.
🔴 RED — Absolute Stop
Do NOT proceed if: child is in active panic; child has known trauma history with water (seek professional assessment first via 9100 181 181); child has open wounds or illness; you are feeling frustrated or rushed; child explicitly communicates "no" without alternative available.
🟡 AMBER — Modify
Simplify the session if: child is tired, hungry, or post-meltdown; other sensory triggers are active (loud sounds, bright lights); child had a difficult day; it is child's first encounter with this protocol → begin at Step 1 only (pouring cups, no tub).
🟢 GREEN — Proceed
Proceed if: child is fed, rested, regulated; environment is calm, warm, quiet; caregiver is calm and unhurried; all materials are set up BEFORE bringing child to bathroom; visual routine card reviewed with child beforehand.
⛔NEVER force a child's head under water to "show them it's okay." This is traumatising and dangerous, and will dramatically worsen the phobia. Materials support exposure but never replace constant adult supervision around any water.

Set Up Your Space
The space must be ready before the child arrives. Spatial precision prevents 80% of session failures. A prepared environment communicates safety before a single word is spoken — the child's nervous system reads the room before you've said hello.
What To Set Up
- 🪟 Soft natural light or warm LED (no fluorescent overhead)
- 🎵 Calm music (optional, low volume)
- [7] Exposure Ladder Chart posted on wall
- [2] Visual Schedule at child's eye height
- [5] Non-slip mat inside bathtub
- [4] Thermometer floating in water
- [6] Bath toys arranged in tub
- [8] Sensory add-ins ready
- [1] Pouring cups on low shelf for pre-tub play
- [3] Bath visor on hook nearby
- Parent seated at child level — not towering above
Pre-Session Checklist
- ☐ Water temperature checked at child's preferred range
- ☐ Visual routine cards posted at child's eye level
- ☐ Towel and pyjamas laid out visibly
- ☐ Reward ready and visible after session
- ☐ Your phone is on silent
- ☐ You have at least 30 unrushed minutes
What to Remove
- ❌ Loud fans or heating units
- ❌ Bright overhead fluorescent lights
- ❌ Mirrors at child's level if distressing
- ❌ Items that previously triggered negative associations
- ❌ Other siblings — first sessions must be 1:1

ACT III: The Execution Protocol
Is Your Child Ready? 60-Second Readiness Check
The best session is one that starts right. A readiness check is not bureaucracy — it's the difference between a session that builds tolerance and one that sets it back. Check every item before proceeding.
Child has eaten within the last 2 hours
No meltdown or major dysregulation in past 2 hours
No signs of illness (fever, upset stomach)
Child is in baseline or neutral emotional state
You (caregiver) are calm, patient, not rushed
Environment is fully set up (Card 12 complete)
✅ 7/7 — GO
Begin with Card 14 (Invitation)
🟡 5–6/7 — MODIFY
Pouring cups only, no tub. Keep to 5 minutes max.
🔴 Under 5/7 — POSTPONE
10 minutes of preferred calming activity. Reschedule tomorrow.

Step 1: The Invitation
Every protocol begins with an invitation, not a command. The distinction is not semantic — it is neurological. A command activates the threat-detection system. An invitation activates curiosity. You need your child's brain in curiosity mode, not defense mode.
💬"Hey, I found something really fun to do with water today. Want to come see? You're in charge — you can stop whenever you want."
Body Language Guidance
- Crouch or sit at child's level — never tower above
- Warm, calm voice — match the energy you want to create
- Open hands, relaxed posture — no tension in your body
- Eye contact at child's comfort level (don't force for ASD profiles)
Handling Resistance
Child refuses: "Okay, that's fine. The cups will be here when you want them." No pressure, no disappointment displayed.
Child asks "No bath?": "No bath today. Just pouring fun." — Keep your promise. Every promise kept builds neurological trust.
Timing: 30–60 seconds | Location: Water play area (kitchen, NOT bathroom) for first sessions

Step 2: The Engagement
The child is engaged. Now deepen without demand. This step is about following the child's curiosity — not directing it. Every moment of self-directed exploration is a moment the nervous system spends in contact with water without threat activation.
01
Place Materials — Don't Touch First
Place pouring cups and water bin in front of child. Let child explore without adult initiation.
02
Narrate Curiosity
"Look, this one is tiny and this one is big. I wonder which one holds more water?" Allow 60–90 seconds of unguided exploration.
03
Model Once
"I'm pouring into this one... watch the water go! Your turn?" Child-led from here. Follow their interest, not your agenda.
🟢 Engaged
Child picks up cup, pours, explores → Narrate positively: "You decided! Look how much you poured!"
🟡 Tolerating
Child watches but doesn't touch → Sit with them, narrate your own play, zero pressure
🔴 Avoidant
Child backs away → "That's okay. You can just watch." Reduce water amount. Move water further away.
Immediately praise ANY approach behaviour: "You looked at it! That was brave." Behaviour that gets noticed gets repeated.

Step 3: The Therapeutic Action
The core therapeutic event: controlled water exposure on the child's terms. Progress through phases only when the child is comfortable at the current level. There is no timeline pressure — deepening comfort at each phase is the goal.
1
Phase A — Pre-Bath
Child pours water from smallest cup. Controls all variables: amount, speed, destination. "You're the water boss today."
2
Phase B — Hand Exposure
Child dips fingertip into water in a small bowl (NOT tub). "Just one finger. You decide when to take it out." No countdown.
3
Phase C — Bathroom Entry
Child enters bathroom. Tub is empty. Child can touch tub sides. Visual schedule reviewed. 2–3 minutes max. Leave positively.
4
Phase D — Minimal Water
Child sees thermometer showing safe temperature. Child decides whether to sit. Bath visor available. Toys in tub. No hair washing this session.
🛑Stop immediately if: vomiting, hyperventilating, pupils dilated with terror, complete loss of regulation. End session, transition to preferred calming activity, note what triggered escalation.

Step 4: Repeat & Vary
Three good repetitions are worth more than ten forced ones. The goal within a session is not to advance phases — it is to build deeper comfort at the current phase through repetition and gentle variation. Each repetition sends the nervous system the same message: "Water is safe."
3-5
Within-Session Repetitions
Target repetitions at the same phase level — deepening comfort, not advancing phase
3-5
Sessions Per Week
Evidence-based frequency for optimal desensitization — missing days is okay
8-12
Weeks to Progress
Full protocol duration — each session builds on the previous one
Variation options to maintain engagement: Change cup size (larger = slightly more exposure — child chooses) · Change water colour with food colouring · Change container shape (changes the sound) · Add one new toy (novelty maintains engagement) · Change who pours (parent models, then child's turn).
Satiation indicators: Engagement drops, child moves away, child says or signs "all done," fidgeting increases. This is the natural end of productive exposure. Stop here. End positively.

Step 5: Reinforce & Celebrate
Timing matters more than magnitude. Deliver reinforcement within 3 seconds of the desired behaviour — not at the end of the session, not "later." The nervous system encodes association in real time.
💬 "You DID it! You put your hand in the water! I am SO proud of you."
💬 "That was really brave. You stayed so calm."
💬 "Look at YOU. You're getting so good at this."
Verbal + Physical Affirmation
High five, hug, enthusiastic praise — immediate and genuine
Token Economy
1 star sticker per phase completion → 5 stars = preferred reward of child's choosing
Preferred Item Access
Brief access to favourite toy or screen immediately after session — natural consequence of success
"Celebrate the attempt, not just the success." A child who approached the tub and then retreated showed more bravery than one who never tried. Every movement toward water deserves recognition.

Step 6: The Cool-Down
No session ends abruptly. The cool-down is as therapeutically important as the exposure itself. An abrupt ending spikes cortisol and encodes the memory of the session as incomplete and threatening. A warm, predictable ending encodes the memory as safe and achievable.
Transition Warning (2 min before end)
💬 "Two more pours, then we're all done for today. You did amazing."
Complete Final Repetition Together
Side by side — finish what you started, together.
Child Puts Toys Away
Participatory closure — gives the child agency over the ending of the session.
Dry Together & Exit Positively
Dry hands/feet with soft towel together. Exit bathroom positively — walk out together, door stays open.
Transition to Preferred Activity
"Now let's go do [preferred next activity]." Build in 5–10 minutes of preferred calming activity after every session.
If child resists ending: "I know you want to keep going! That's so great. Let's save some for tomorrow." Use a visual timer to make the ending predictable.

Step 7: Capture the Data — Right Now
60 seconds. 3 fields. Data that drives your child's progress. Without data, you're guessing. With 3 data points per session over 8 weeks, you have a 24-point progress trajectory that any Pinnacle therapist or GPT-OS® system can analyse, adjust, and build on.
📋 Phase Attempted Today
□ A (pre-bath water play) □ B (hand exposure) □ C (bathroom entry) □ D (minimal tub water)
📊 Tolerance Rating (1–5)
1 = Refused entirely | 2 = Significant distress | 3 = Mild distress | 4 = Accepted with support | 5 = Engaged independently
📝 Today's Observation
One sentence: what happened, what surprised you, what you'll try differently next time.
🎯 Next Session Goal
□ Repeat today's phase □ Advance one step □ Go back one step
📱GPT-OS® Integration: Log this data into your EverydayTherapyProgramme™ tracker to receive AI-assisted next-session recommendations and automatic progress reports. This is how 97%+ improvement becomes measurable — not by hope, but by tracking.

Troubleshoot: When It's Not Working
Sessions not going as planned? Here are the six most common issues parents encounter — and the evidence-based fixes. Every problem on this list has a solution that keeps the protocol moving forward.
🔴 "My child refuses to even enter the bathroom"
Don't start in the bathroom. Begin water play entirely outside (kitchen table bin). Bathroom entry is Phase C — some children need 2–4 weeks of outside-bathroom water play before they'll enter voluntarily.
🔴 "My child melts down every time, no matter what I try"
Drop back to lowest exposure level (just looking at a cup of water in another room). If all exposure attempts cause meltdowns, this indicates clinical severity — call 9100 181 181 for professional assessment.
🔴 "We had a great session, then a terrible one the next day"
This is normal. Desensitization is not linear. One bad session doesn't erase previous progress. Note what was different (time of day, child's sleep, other stressors) and adjust.
🔴 "My child hates the bath visor"
Introduce visor in play first — wear it yourself, make it silly, let child put it on a doll. Build visor tolerance as its own mini-exposure sequence before using during actual hair washing.
🔴 "Hair washing is still a battle after months of bath tolerance"
Hair washing is a separate sub-phobia. Create its own exposure ladder: ① wet fingers through dry hair ② damp washcloth on head ③ small cup of water at back of head ④ full rinse with visor. This may take 4–8 additional weeks.
🔴 "My partner or grandparent won't follow the protocol"
Use Card 37's Family Guide and Teacher Template. Inconsistency is the #1 reason protocols fail. All caregivers must follow the same approach.
Adapt for Your Child
No two children are the same. This protocol is a framework, not a script. Here is how to adapt each dimension of the approach for your child's specific neurological and developmental profile.
🔵 ASD + Low Verbal Communication
Add PECS or AAC "all done" symbol to bath routine. Use "first-then" boards: FIRST bath, THEN preferred item. Reduce verbal language during sessions — let materials speak. Predictability and visual structure are your most powerful tools.
🟡 Trauma-Based Water Fear
Move even slower than the protocol suggests. Phase A may take 4–8 weeks. Professional psychological support strongly recommended in parallel. Do not push exposure without trauma-informed clinical guidance — call 9100 181 181.
🟢 Tactile Hypersensitivity
Begin with dry materials only (empty tub, cups with no water) before introducing any moisture. Use warm water only (heated slightly above ambient temperature). Always allow child to exit the sensory environment instantly when requested.
🟣 Toddlers (Ages 2–3)
Keep sessions to 5 minutes maximum. Use only Phase A and B. Heavy use of visual schedules with pictures. Prioritise fun and play — not clinical structure. The younger the child, the more playful the intervention must feel.
⚫Severe aquaphobia or panic disorder: This protocol is a starting point. Professional OT assessment and child psychology intervention are strongly indicated. Contact: 9100 181 181

ACT IV: The Progress Arc
Weeks 1–2: Establishing Baseline
You are establishing the baseline. Every session is data. These first two weeks are not about dramatic breakthroughs — they are about roots. You are building the foundation on which every future milestone will rest. This is not slow progress. This is how lasting change works.
Child tolerates water play at kitchen table without significant distress (3–5 sessions)
Child can hear water running in another room without full panic response
Visual routine card introduced and reviewed daily (not just on bath days)
Caregiver comfortable with protocol — knows what to say, what not to say
Baseline data collected for 3–6 sessions using Card 20 tracker
What does NOT need to happen yet: Child does not need to enter the bathroom. Child does not need to touch the tub. Hair washing is months away. This is groundwork. This is roots before flowers.

Weeks 3–4: First Bathroom Encounters
Crossing the bathroom threshold — at the child's pace. The bathroom door is not just a physical threshold. For a child with water fear, it represents the boundary between safety and danger. These weeks are about gently, consistently, lovingly rewriting that story.
Voluntary Bathroom Entry
Child enters bathroom willingly — with visual support, with preferred toy, with parent by their side
Tub Filling Presence
Child can be in bathroom while parent fills tub — child doesn't have to approach the tub
Visor in Play Context
Child engages with bath visor as a play object — not on head during water yet
Temperature Verification
Child checks water thermometer — sees visual proof of safe temperature, building cognitive safety signals
Milestone: Child enters bathroom and remains for 3 minutes without physical restraint or significant distress. Regression note: If a previously achieved milestone is lost, this is temporary — return to the previous phase for 3–5 sessions, then try again. Regression does not erase progress.

Weeks 5–8: Tub Tolerance Builds
The tub becomes a place of play, not fear. By Week 5, you are not the same family you were eight weeks ago. You have data. You have a protocol. You have evidence that your child can change. Now the tub itself becomes the therapeutic environment.
Empty Tub Comfort
Child sits in empty tub with toys (no water) comfortably for 5+ minutes
Minimal Water Entry
Child allows 1–2cm of water in tub with feet or legs in — child controls duration
Engaged Bath Play
Child engages with bath toys in tub with minimal water, showing approach behaviour
Extremity Water Tolerance
Child allows water on hands and feet without distress — begins asking about bath toys
Clinical progress indicator: Tolerance Rating averaging 3.5+ across 5 consecutive sessions = clinical threshold for phase advancement. Hair washing approach begins here — with bath visor worn during play in dry tub first.

Celebrate Every Milestone
Every step is a mountain. Celebrate accordingly. For a child whose nervous system has been running a threat response every time water appears, each milestone represents a genuine neurological shift — the brain literally building new safety pathways. That deserves celebration at scale.
Milestone | Celebration Scale | |
First time enters bathroom without distress | 🌟 Family celebration — acknowledge to everyone | |
First time touches water without panic | 🌟🌟 Special outing or preferred activity | |
First full bath with minimal distress | 🌟🌟🌟 Major family event — child's choice | |
First hair wash completed | 🌟🌟🌟🌟 Document with photo/video, share with community | |
Child asks to take a bath | 🌟🌟🌟🌟🌟 The mountain summit |
"Six months ago, my daughter screamed if water touched her arm. Last week, she asked if she could take a bath. That's everything." — Parent, Pinnacle Network
This milestone is achievable. It takes time. It takes consistency. It takes the protocol on these 40 cards. You are already on the path.

Red Flags: When to Escalate
Know when home protocol is not enough. These are the signals. A home protocol is powerful — but it is not a substitute for professional assessment when the clinical picture exceeds its scope. Recognising these signals is not failure. It is wisdom.
🔴 No Measurable Progress
No improvement after 8 weeks of consistent protocol execution at 3+ sessions per week
🔴 Intensifying Distress
Child's distress is increasing rather than reducing over time despite consistent protocol
🔴 Physical Symptoms
Vomiting, self-injury, or uncontrollable hyperventilation during any water exposure
🔴 Caregiver Burnout
Parent is unable to execute protocol calmly — caregiver secondary trauma is real and valid
🔴 Generalizing Fear
Fear extending to rain, drinking water, pools — widening phobia requires clinical support
🔴 Trauma History
Known traumatic water experience (near-drowning, forced submersion) — professional trauma-informed support required from session 1
📞FREE National Autism Helpline: 9100 181 181 (24×7, 16+ languages) | 🌐 pinnacleblooms.org → AbilityScore® Assessment | 70+ Pinnacle centers across India
Your Progression Pathway
You are not done. You are on a journey with a clear forward path. C-285 is one node in a connected network of techniques designed to build on each other. Each technique you complete expands your child's world and your confidence as a therapeutic caregiver.
The long-term developmental goal this feeds into is Adaptive Skills Independence — the ability to maintain personal hygiene, participate in community water activities, and develop swimming safety skills. This feeds directly into school participation, community inclusion, and life-readiness.

Related Techniques in This Domain
Other techniques in this sensory-emotional domain. If you have completed the C-285 starter kit (bath visor, visual cards, non-slip mat), you already own materials for three of the four techniques below — your investment extends across the entire hygiene domain.

C-283: Understanding Sensory-Based Fears
🟢 Intro Level | Visual cards (free to make) — the essential prerequisite foundation

C-284: Tactile Sensitivity Materials
🟡 Core Level | Sensory brush, textured surfaces — directly feeds into water tolerance

C-287: Fear of Hair Cutting
🟡 Core Level | Bath visor (already in C-285 kit) — material overlap maximises your investment

C-290: Sensory-Friendly Hygiene Routines
🔵 Advanced Level | Multiple C-285 materials reused — the natural next step
Browse the full Emotional Regulation domain: → techniques.pinnacleblooms.org/emotional-regulation
Your Child's Full Developmental Map
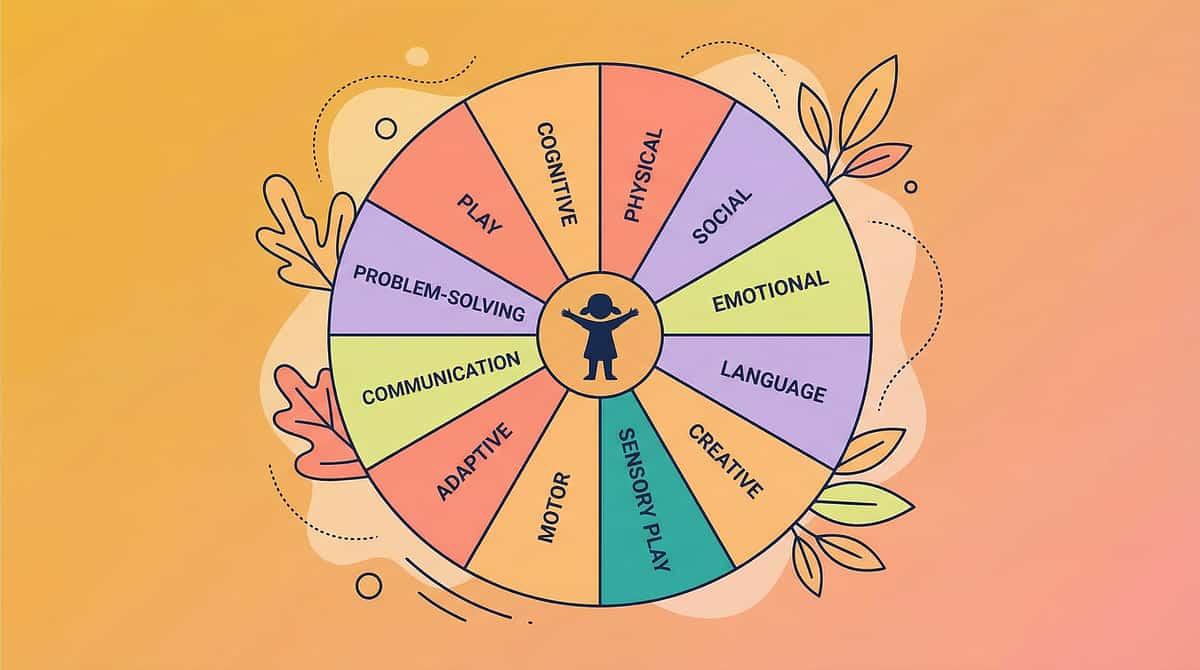
This technique is one piece of a larger plan. Here is the full picture. C-285 is not just a bath time protocol — it is a contribution to your child's holistic developmental profile across 12 domains. Every session you log feeds into a larger picture of growth and possibility.
Domain A: Sensory
Water tolerance = direct sensory desensitization
Domain C: Emotional Regulation
Fear reduction = core emotional regulation competency
Domain H: Self-Care
Bathing independence = critical self-care milestone
Domain L: Adaptive Behaviour
Community water participation = life readiness
📱 See your child's full AbilityScore® profile across all 12 domains. Every session logged at Card 20 feeds directly into your child's personalised developmental plan. → pinnacleblooms.org | FREE assessment: 9100 181 181

ACT V: Community & Ecosystem
Stories From the Community
From our community of 70+ centers across India. These are not exceptional cases. These are the outcomes that happen when a scientifically designed protocol is executed consistently by an empowered, informed parent.
"Six months ago, my daughter screamed if water touched her arm. Bath time took three adults and ended with everyone in tears. We started with pouring cups at the kitchen table. Week 3, she entered the bathroom on her own. Week 7, she sat in 1cm of water and played with her rubber duck for 10 minutes. Last week, she asked if she could take a bath. Asked. When we were done, she said 'That was fun.' I cried — happy tears this time. We even signed up for swimming lessons."
— Parent, Pinnacle Network | Outcome tracked: Sensory Processing Readiness Index
"My son was 7. He hadn't had a proper bath in 8 months. We thought it was just defiance. The Pinnacle OT showed us the exposure ladder. Within 12 weeks — just using the materials on this page — he was bathing daily. It wasn't defiance. It was terror. Now he understands what was happening, and so do we."
— Parent, Pinnacle Network
You have the protocol. You have the materials. You have this.

Connect With the Community
Join 21 million sessions' worth of learning. Share yours. You are not navigating this alone — across India and in 70+ countries, families are using this same protocol, logging the same sessions, celebrating the same milestones. Your community is waiting for you.
WhatsApp Community
Join thousands of Indian families navigating sensory-based fears together → pinnacleblooms.org/community
Pinnacle Parent Portal
Access your child's session history, progress reports, and next-step recommendations → pinnacleblooms.org
24×7 Helpline
When you need a human voice: 9100 181 181 — available in 16 languages including Hindi, Telugu, Tamil, Kannada, Malayalam, Bengali, Marathi, Gujarati, and more
Find Your Center
70+ Pinnacle centers across India — in-person assessment, therapy, and parent coaching → pinnacleblooms.org/centers
For families outside India: Pinnacle GPT-OS® content serves families in 70+ countries. Digital resources — this page, the EverydayTherapyProgramme™, and the online parent community — are available globally.
Professional Support: When and How
Home protocols are powerful. Professional guidance makes them unstoppable. The combination of a well-executed home protocol and expert clinical support produces outcomes that neither can achieve alone. Think of professional support not as an escalation — but as an amplifier.
When to Seek Professional Support
- For OT assessment of your child's specific sensory processing profile
- For child psychology support (trauma-based or severe phobia)
- For parent coaching to feel more confident executing protocols
- For AbilityScore® baseline across all 12 developmental domains
- For Aquatic Therapy referral with sensory-trained instructors
Pinnacle Services for C-285
- 🔵Occupational Therapy — Sensory processing assessment, Ayres SI-based intervention
- 🟡Child Psychology — CBT exposure hierarchy, trauma-informed phobia treatment
- 🟢Parent Coaching — 6-session parent training protocol for home-based sensory intervention
- 🟣Adaptive Skills Training — Hygiene independence programming
- ⚪Aquatic Therapy Referral — External specialised resource via Pinnacle network
Booking:📞 9100 181 181 → AbilityScore® Assessment → TherapeuticAI® plan → FusionModule™ coordination → EverydayTherapyProgramme™
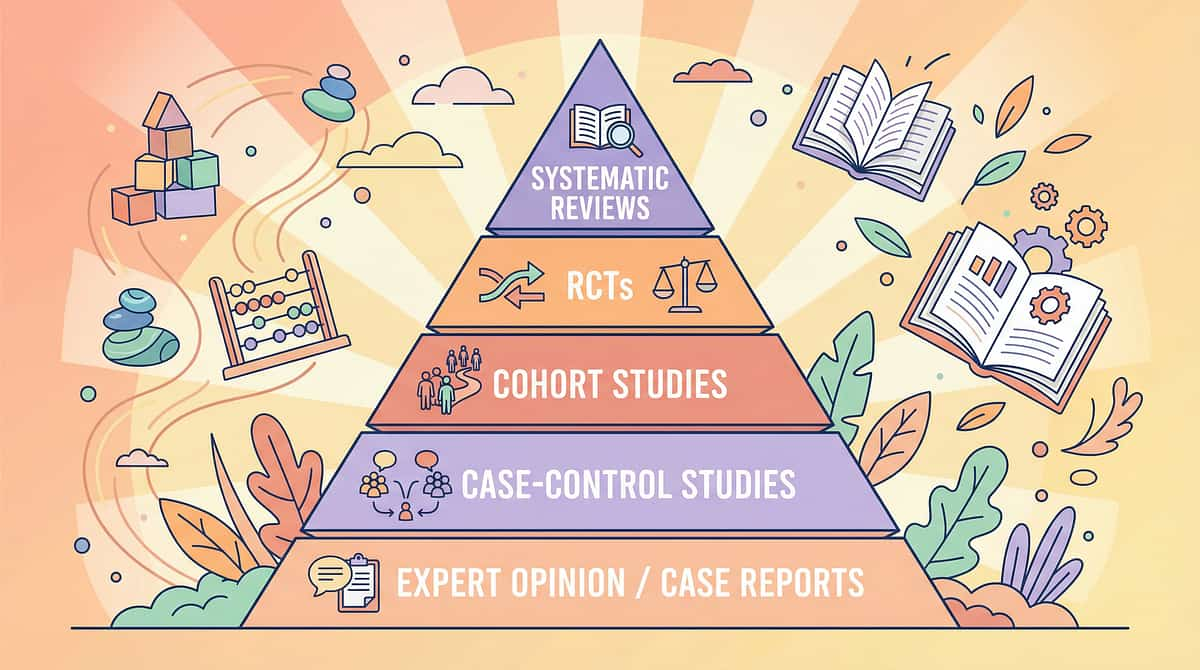
The Research Library
The science behind every card on this page. All references graded per Oxford Centre for Evidence-Based Medicine levels. Every recommendation on this page traces directly to peer-reviewed evidence — this is not opinion, not tradition, not guesswork.
Systematic Reviews & Meta-Analyses
📎PMC11506176 — PRISMA systematic review (2024): Sensory integration intervention is evidence-based practice for ASD. 16 studies, 2013–2023.
📎PMC10955541 — World J Clin Cases (2024): SI therapy promotes social skills, adaptive behaviour, sensory processing, and motor skills. 24 studies.
📎PMC10955541 — World J Clin Cases (2024): SI therapy promotes social skills, adaptive behaviour, sensory processing, and motor skills. 24 studies.
RCTs & Cohort Studies
📎DOI: 10.1007/s12098-018-2747-4 — Indian Journal of Pediatrics (2019): Home-based sensory interventions by trained parents — RCT in Indian context.
📎DOI: 10.3389/fnint.2020.556660 — Frontiers in Integrative Neuroscience (2020): Neurological basis for sensory-based interventions in ASD.
📎DOI: 10.3389/fnint.2020.556660 — Frontiers in Integrative Neuroscience (2020): Neurological basis for sensory-based interventions in ASD.
Clinical Frameworks
📎PMC9978394 — WHO/UNICEF Care for Child Development Package — household-based intervention across 54 LMICs
📎NCAEP Evidence-Based Practices Report (2020) — Video modeling and visual supports as EBP for autism
📎DOI: 10.1080/17549507.2022.2141327 — UNICEF/WHO NCF for multi-disciplinary pediatric practice
📎NCAEP Evidence-Based Practices Report (2020) — Video modeling and visual supports as EBP for autism
📎DOI: 10.1080/17549507.2022.2141327 — UNICEF/WHO NCF for multi-disciplinary pediatric practice
Access full reference list at: pinnacleblooms.org/research | techniques.pinnacleblooms.org/evidence-base

How GPT-OS® Uses Your Data
Your data helps your child — and every child like yours. Each session you log contributes to an aggregate intelligence that makes the system smarter, more predictive, and more precisely helpful for every family in the network. All data is governed under ISO/IEC 27001 Information Security Management — individual child data is never shared.
20M+
Sessions Analysed
97%+
Measured Improvement
70+
Centers Nationwide
160+
Countries with Patents Filed

Watch the Reel
Watch the 60-second Reel that brought thousands of parents to this page. The Reel was the door. These 40 cards are the room. Inside, you have found the full clinical protocol, the neurological explanation, the step-by-step execution guide, and the community of families who have walked this path before you.
Reel C-285
Title: "9 Materials That Help With Fear of Water"
Series: Sensory Processing & Emotional Regulation | Episode 285
Duration: 60 seconds | Ages: 2–12 years
Series: Sensory Processing & Emotional Regulation | Episode 285
Duration: 60 seconds | Ages: 2–12 years
Watch more in the series:
→ C-283
9 Materials for Sensory-Based Fears
→ C-286
9 Materials for Fear of Loud Noises (Coming next)
→ C-287
9 Materials for Fear of Hair Cutting

Share This With Your Family
Consistency across caregivers multiplies impact. Share this now. The WHO CCD Package establishes multi-caregiver training as critical for intervention generalisation and maintenance. A protocol followed by one caregiver and ignored by another is a protocol working at half capacity. Bring your whole village into alignment.
Share via WhatsApp
Send to spouse, grandparents, school teacher — anyone who supports bath time at home or school
Email the Full Page
Share the complete 40-card protocol link: techniques.pinnacleblooms.org/emotional-regulation/fear-of-water-c-285
Family Guide PDF
One-page visual summary for grandparents, domestic helpers, and extended family — covers the 3 non-negotiable rules in simple language
For grandparents: "Our child is working on a water confidence programme. Please follow these 3 rules: (1) Never force water contact. (2) Always praise any attempt, no matter how small. (3) Follow the visual schedule on the bathroom wall."
Teacher template: "Our child is working on sensory desensitisation for water. At school: please avoid surprise water activities, give advance warning before any water play, and do not express frustration if child refuses. Thank you."
Teacher template: "Our child is working on sensory desensitisation for water. At school: please avoid surprise water activities, give advance warning before any water play, and do not express frustration if child refuses. Thank you."

ACT VI: Frequently Asked Questions
Questions Parents Ask Most
Answered by the Pinnacle Consortium. These are the questions that arrive most frequently at our helpline, in our parent portal, and at our 70+ centers — questions from real families navigating real challenges, answered with clinical rigour and parental warmth.
Q1: My child is 9 years old. Is it too late to start?
Never. Neuroplasticity continues throughout childhood and adolescence. The protocol may take longer for older children with more deeply established fear responses, but outcomes are still strong. Professional OT assessment is particularly valuable for school-age children to design a targeted programme.
Q2: How long before I see results?
Most families see measurable tolerance improvement (Tolerance Rating 3+ on the Card 20 tracker) within 6–8 weeks of 3–5 sessions per week. Full functional bath time typically develops by Week 12–16. Water safety skills may take 6–12 months. Every child's timeline is different.
Q3: My child has autism. Will this protocol work?
This protocol is specifically designed with ASD profiles in mind. The visual supports, child-led pacing, ABA reinforcement principles, and multi-sensory accommodation approach are all autism-affirming. Children with ASD may require longer timelines and benefit most from concurrent OT support. Contact 9100 181 181 for an AbilityScore® assessment.
Q4: Do I need to buy all 9 materials at once?
No. The essential starter trio is: non-slip bath mat + bath visor + visual routine cards. Total cost: approximately ₹650–2,600. All other materials can be DIY initially (Card 10). Add materials as your child's protocol advances.
Q5: What if my child only fears hair washing, not the bath itself?
Hair washing fear is extremely common and often operates independently from bath tolerance. See Card 22's Hair Washing Protocol (Phase D of the graduated approach). The bath visor is your most important tool for this specific presentation.
Q6: My partner thinks our child is just being difficult. How do I explain this?
Share Card 03 (the neuroscience card) directly with your partner. The amygdala explanation is designed to create understanding, not debate. Consider bringing your partner to a Pinnacle parent consultation session where a clinician can explain the neurological basis directly.
Q7: Can I do this alongside therapy sessions at a Pinnacle center?
Yes — and this is the optimal approach. Home practice between sessions is how the 20+ hours of weekly non-session time is converted into therapeutic progress. Your therapist can supervise the protocol, adjust it based on clinic observations, and upload your home data into the GPT-OS® system for integrated monitoring.
Q8: What if my child's water fear is getting worse despite the protocol?
Stop home protocol and call 9100 181 181 immediately. Worsening fear indicates either: protocol is too advanced (dial back phases significantly) or the fear has a trauma component requiring clinical psychological support. Do not continue escalating exposure when distress is increasing — that is counter-therapeutic.

You Have the Knowledge. You Have the Materials. Start Today.
Every session you begin brings your child one step closer to a life where water is not a source of terror — but a source of play, cleanliness, safety, and eventually, joy. The protocol is ready. The community is behind you. The evidence is clear.
🚀 Start This Protocol Today
Launch your EverydayTherapyProgramme™ session and begin Card 13's readiness check — your first session can happen today.
📞 Book a Free Assessment
AbilityScore® evaluation at your nearest Pinnacle center. 9100 181 181 | 70+ centers across India
➡️ Explore Next Technique
C-286: Fear of Loud Noises → techniques.pinnacleblooms.org/emotional-regulation/fear-of-loud-noises-c-286
✅Validated by Pinnacle Blooms Consortium — OT • Child Psychology • BCBA/ABA • Special Education • NeuroDevelopmental Pediatrics | 20M+ sessions • 97%+ improvement • 70+ centers
Preview of 9 materials that help with fear of water Therapy Material
Below is a visual preview of 9 materials that help with fear of water therapy material. The pages shown help educators, therapists, and caregivers understand the structure and content of the resource before use. Materials should be used under appropriate professional guidance.



















Share this resource
Help others discover thisLink copied!

From fear to mastery. One technique at a time.
Pinnacle Blooms Network® exists to transform every home into a proven, scientific, 24×7, personalised, multi-sensory, multi-disciplinary, integrated therapeutic environment — for every child, in every family, regardless of geography or income.
🔵 Pinnacle Blooms Consortium®
Built by Mothers. Engineered as a System. Occupational Therapy | Speech-Language Pathology | Applied Behaviour Analysis | Special Education | NeuroDevelopmental Pediatrics | Child Psychology | Regulatory Medicine | WHO/UNICEF Framework Alignment
Medical Disclaimer: This content is educational. It does not replace individualised assessment and intervention from licensed professionals including occupational therapists, child psychologists, and aquatic therapy specialists. Severe water phobia or trauma-related fear may require specialised therapeutic intervention. Individual results may vary. Statistics represent aggregate outcomes across the Pinnacle Blooms Network.
© 2025 Pinnacle Blooms Network®, a unit of Bharath Healthcare Laboratories Pvt. Ltd. All rights reserved. Powered by GPT-OS® — Global Pediatric Therapeutic Operating System. CIN: U74999TG2016PTC113063 | DPIIT: DIPP8651 (Govt. of India) | MSME: TS20F0009606 | GSTIN: 36AAGCB9722P1Z2 | ISO 13485 (Medical Device QMS) | ISO/IEC 27001 (Information Security)
← Return to Top
→ C-286: Fear of Loud Noises
Browse All Techniques
FREE Helpline: 9100 181 181