

"My son has to touch every doorknob three times before he can walk through. He washes his hands until they're raw and bleeding, and still doesn't feel clean. He asks me the same question forty times a day, and my answer never satisfies him. The rituals eat hours of his day. They're getting worse, not better. And when I try to stop them — the panic in his eyes is so real, so desperate, that I feel like I'm torturing him. I don't understand what's happening inside him. I just know that something has taken hold of my child, and it won't let go."


↓ OBSESSION → Intrusive thought generates overwhelming anxiety
↓ COMPULSION → Ritual performed to reduce distress
↓ BRIEF RELIEF → Anxiety decreases temporarily
↓ REINFORCEMENT → Brain learns: "the ritual saved you"
↓ ESCALATION → Next time, more ritual required
ERP therapy produces measurable neurological changes — literally rewiring the alarm circuit. (Saxena & Rauch, 2002; Rotge et al., 2008)


Gold Standard Treatment Classification
- March & Mulle RCT (1998): ERP produced significant symptom reduction in 87% of pediatric OCD cases — landmark trial establishing ERP as first-line treatment
- POTS Study (2004): Multi-site RCT — combined ERP + medication superior to either alone; ERP alone significantly superior to medication alone
- Meta-analysis (2021): 16 RCTs confirm ERP as most effective psychological treatment, with large effect sizes (d > 1.0)
- Pinnacle Real-World Evidence: 20M+ therapy sessions | 97%+ measured improvement in Behavioral Flexibility Readiness Index



# | Material | Canon Category | Price Range | DIY? | |
1 | Anxiety / SUDS Thermometers | Behavior/Feelings Thermometer | ₹150–500 | ✅ Free | |
2 | Externalization Tools (OCD Monster Kit) | Emotion Cards / Social Stories | ₹100–400 | ✅ Free | |
3 | Fear Ladders & Exposure Hierarchies | Visual Supports | ₹100–400 | ✅ Free | |
4 | Response Delay Timers | Visual Timer | ₹300–800 | ✅ Phone timer | |
5 | Thought Challenging Cards | Cognitive Tools | ₹200–600 | ✅ DIY cards | |
6 | Competing Response Tools | Fidget Tool Set / Therapy Putty | ₹200–700 | ✅ Stress ball | |
7 | Exposure Practice Kits | Therapy/Sensory Materials | ₹100–600 | ✅ Household items | |
8 | Calming Strategy Toolkit | Calm-Down Kit | ₹300–900 | ✅ DIY kit | |
9 | Victory Trackers | Reinforcement Menus | ₹150–500 | ✅ Paper chart |

- Before every exposure session
- During the wait period
- After the urge passes
- To track progress across weeks
- Home, therapy room, classroom (discreet pocket version)
- Draw or print thermometer with 0–10 scale
- Create personal anchors in the child's own words
- Practice rating during calm times (not just anxiety)
- Use during every exposure — rate before, during, after
- Graph the decrease — show child their own habituation curve
- "Nice try, OCD, but I'm not doing your ritual today."
- "I hear you, Brain Bully. I'm not listening."
- "That's just my OCD lying to me. I know the truth."
- "Boring! I already know that trick."
- Drawing paper + markers — ₹0–200
- "Worry Monster" figurine — ₹200–500
- Externalization storybooks (Huebner's What to Do When Your Brain Gets Stuck) — ₹400–800
- "Boss Back Journal" — ₹100–300
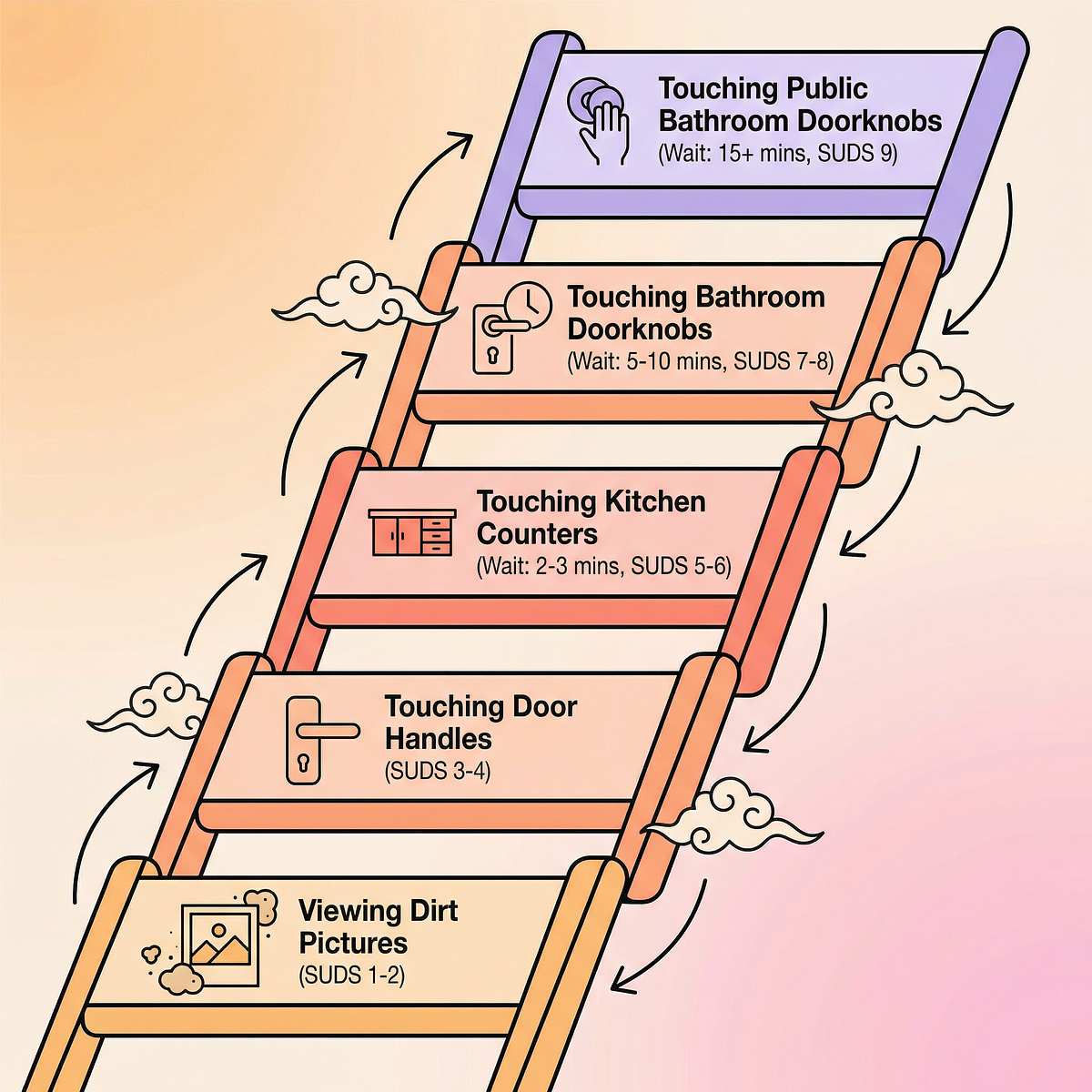
- Fear ladder template (printable) — ₹0 DIY
- Visual step chart poster — ₹100–300
- Progress tracking stickers — ₹50–200
- "Brave Ladder" goal-setting worksheets — ₹100–300

The 60-Second Pre-Session Check. Don't skip this.
Before beginning any ERP session, run through this readiness gate. A session with poor readiness produces zero therapeutic benefit — and may set back progress. The best session is one that starts right. 🟢 GO — 7/7 Checks Child has eaten in the last 2 hours Child is not currently in meltdown No significant illness today No triggering event in last 30 minutes At least 20 minutes available Materials are ready and organized Parent is calm and patient Proceed with planned session. 🟡 MODIFY — 5–6/7 Use simplified version, shorter duration, lower rung on the fear ladder. Don't push for a full session — a partial win still counts. 🔴 POSTPONE — <5/7 Skip today. Do a calming activity instead. Tomorrow is also a session day. Postponing is not failure. 📞 9100 181 181 — When in doubt, call us. Free guidance available 24×7.

- "Hey, want to do 10 minutes of bossing back [child's OCD name]? I'll be right here."
- "It's brave time. Should we pick an easy step or a medium one today?"
- "Remember how you got [OCD name] down to a 5 last week? Want to try for a 4 today?"
- Refer to the victory tracker: "Look how many wins you already have"
- Let child choose today's rung — agency increases compliance
- Remind child of the specific, immediate reward waiting
- ❌ "You have to do this" — creates power struggle
- ❌ "It's for your own good" — dismissive of real distress
- ❌ Starting during high anxiety — wait for regulated state

"Before we start, let's check your thermometer. What number are you at right now? What number do you think you'll reach when we start the exposure? Let's see if your prediction is right."

Step 3 — The Exposure: Face it without the ritual. This is the treatment.
The Core Therapeutic Action: Present the feared situation. Support the child through the anxiety — WITHOUT allowing the compulsive ritual. Stay present. Don't reassure. Don't rush. Monitor SUDS every 2–3 minutes. Continue until SUDS drops by at least 2 points from peak. For Checking Compulsions Leave the house after checking the lock once. Parent covers the lock with a cloth so it can't be re-checked. Stay out for 10 minutes. For Washing Compulsions Child touches "mildly contaminated" surface (per fear ladder rung). Parent is present but does NOT permit handwashing for the designated wait period. For Ordering/Arranging Intentionally move one object slightly out of arrangement. Child sits with discomfort for 5 minutes without fixing it. For Reassurance-Seeking Parent script: "I know you're anxious. I love you. I'm not going to answer that question because answering feeds the OCD. I'm right here with you." Duration: 10–45 minutes depending on rung difficulty. Critical: No partial rituals. No substitution rituals. No reassurance. Complete response prevention is essential. | PMC10955541 — 40-minute sessions showed maximum effectiveness 📞 9100 181 181 — Real-time support during difficult sessions


Canon Category: Reinforcement Menus | Behavior Support. After each completed exposure: child adds a sticker to Victory Tracker → progress toward reward milestone is visible → verbal reinforcement follows immediately. | ABA reinforcement principles | PMC11506176

- Breathing card (deep breathing visual prompt)
- Stress ball / fidget tool for hands
- Comfort item (soft toy, weighted blanket)
- Transition object — signals "therapy is done, free time now"
"I hear you. The brave part is done. Your brain worked hard today. Time to rest it."

How to Record: GPT-OS® in-app tracker at pinnacleblooms.org/gpt-os (preferred) | Downloadable PDF tracker | Simple notebook: Date | Rung | Peak SUDS | End SUDS | Notes
"Your data helps TherapeuticAI® refine the personalized plan for your child. Every session recorded makes the next recommendation more precise."

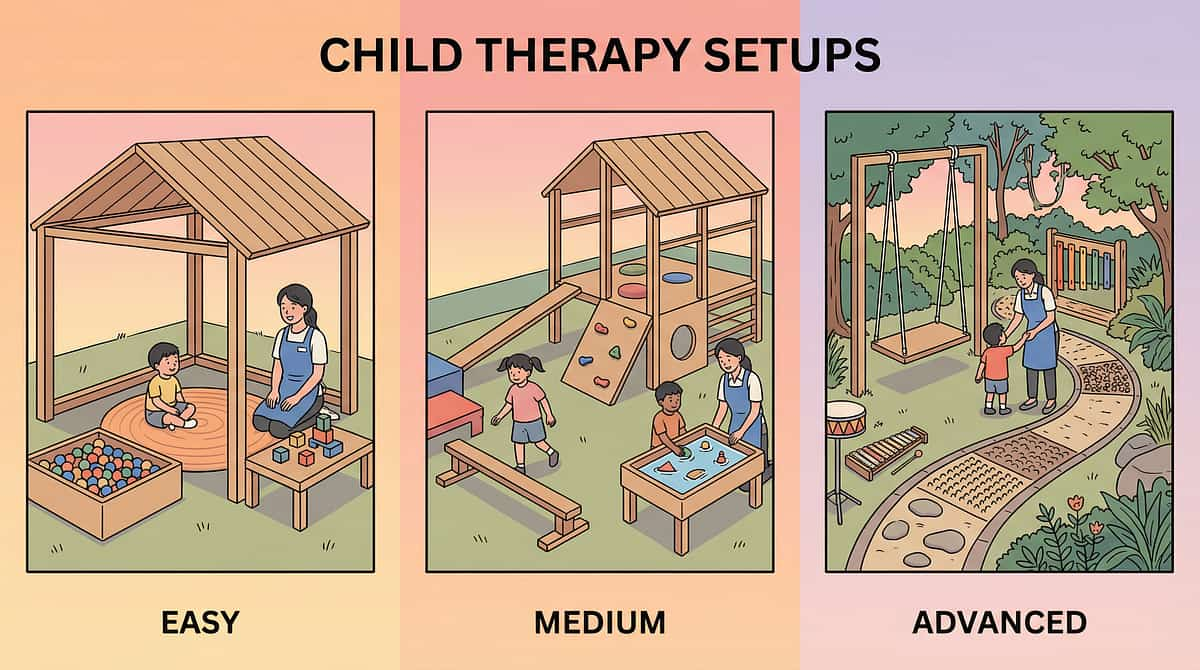

- Play-based exposure framing
- Parent leads more actively
- Shorter sessions: 5–10 min
- Heavier emphasis on reward and externalization
- Simpler SUDS: 3-point scale (okay / worried / very worried)

- More visual supports throughout
- More gradual hierarchy steps
- Additional sensory calming supports
- More session structure and predictability
- Distinguish OCD-driven vs. autism-driven behaviors with therapist

- Start with imaginal exposures before in-vivo
- More preparation time per rung
- More calming toolkit between repetitions
- Consider intensive outpatient for severe OCD
- Psychiatric evaluation for medication if needed

"If your child's SUDS dropped from 8 to 5 during one exposure — that's genuine neurological progress. Celebrate it." | Reference: PMC11506176 — early-phase ERP indicators


ERP outcome literature — functional improvement emerges at 8–12 weeks | PMC2797569

"Six months ago, mornings took two hours. Last week, he got ready for school in twenty minutes. He checked the lock once, said 'nice try, OCD,' and walked to the car. He looked at me and said, 'Mom, I'm stronger than it now.' I cried all the way to school. Happy tears." — Parent, Pinnacle Network (Illustrative case; outcomes vary by child profile)

- Child expressing thoughts of self-harm or suicidal ideation
- Complete inability to function — can't leave home, eat, or attend school
- Rapid symptom escalation — new rituals appearing daily
- Sudden onset after infection (possible PANDAS/PANS — requires medical evaluation)
- Child in acute panic with no de-escalation possible
- Parent feeling unsafe or overwhelmed
- No SUDS decrease after 4+ consecutive sessions on same rung
- Family accommodation increasing rather than decreasing
- Child refusing all ERP engagement for 2+ weeks
- Covert mental rituals identified
- New OCD themes emerging while treating original ones
- SUDS fluctuates day to day — expected
- Some sessions better than others — normal
- Setbacks after illness or school exams — expected, not regression
- Progress slower than hoped — 8–12 weeks is standard

Technique | Title | Difficulty | Primary Material | |
C-293 | Anxiety & Worry Management | 🟢 Intro | Feelings thermometer | |
C-294 | Rigid Routines & Change | 🟡 Core | Visual schedule | |
C-296 | Rigid Thinking Patterns | 🟡 Core | Thought cards | |
C-297 | Perfectionism in Children | 🟡 Core | Progress journals | |
C-300 | Reassurance-Seeking | 🔴 Advanced | Scripts + boundaries | |
D-361 | Stimming & Repetitive Behaviors | 🟡 Core | Sensory kit |

You are not the only family in this battle. Not even close.
"We didn't know what ERP was when our daughter's OCD started. We thought stricter parenting was the answer. We tried — it made everything worse. When we finally found a system that extended therapy into our home, everything changed. She's 11 now and she catches herself before rituals. She calls the OCD 'the lying brain' and she bosses it back. We're not done, but we're not prisoners anymore." — Mother, Hyderabad, Pinnacle Network "My 9-year-old had checking compulsions so severe he couldn't leave the house. We had canceled family holidays, birthday parties, everything. The fear ladder felt impossibly hard at first. The first exposure took 40 minutes and was brutal. But it worked. Six months later he's at step 8 and counting. The victory tracker on his wall is covered in stickers. He's proud." — Father, Chennai, Pinnacle Network Consortium Note: Every story represents a different journey. Outcomes vary. What is universal: the mechanism works. ERP, properly implemented, reduces compulsive behaviors in the vast majority of children who engage with it. 📞 9100 181 181

These materials support ERP. They do not replace it. Here's when to call.
Seek ERP Therapist If: Compulsive behaviors consume >1 hour/day Family life revolving around accommodating rituals Child cannot function at school due to compulsions Home ERP attempts not producing progress after 3–4 weeks Any red flags from the escalation card Pinnacle Evaluation Pathway FREE Helpline call: 9100 181 181 — first-level guidance and center referral AbilityScore® Assessment: Comprehensive developmental baseline OCD/Anxiety Specialist Assessment: Differential diagnosis, ERP-specific planning FusionModule™ Therapy Plan: Psychology + OT + BCBA + NeuroDev coordinated 70+ Centers Nationwide Hyderabad • Chennai • Bangalore • Mumbai • Delhi + 65 more cities pinnacleblooms.org/find-center Teleconsultation Can't reach a center? Book online teleconsultation. care@pinnacleblooms.org | pinnacleblooms.org/teleconsult Integrated Team Psychology (OCD/ERP) | Psychiatry (if medication indicated) | OT (sensory + motor) | BCBA (reinforcement + data) | Parent Coaching (accommodation reduction) 📞 9100 181 181 — FREE | 24×7


- 📲WhatsApp: Share C-295 page with family members
- 📧Email: Send to spouse, grandparents, teachers, school counselor
- 🔗Copy Link: techniques.pinnacleblooms.org/emotional-regulation/compulsive-behaviors-c295
- 📄Family Guide (1-page PDF): "What Our Child Is Working On and How to Help"
- 📄Teacher Communication Template: Supporting a student managing compulsive behaviors
- 📄Accommodation Reduction Guide: "How to Stop Feeding OCD (Gradually)"


20M+ Sessions | 97%+ Improvement | 70+ Centers | OT • Psychology • BCBA/ABA • SpEd • NeuroDev
CIN: U74999TG2016PTC113063 | DPIIT: DIPP8651 | MSME: TS20F0009606 | GSTIN: 36AAGCB9722P1Z2
Preview of 9 materials that help with compulsive behaviors Therapy Material
Below is a visual preview of 9 materials that help with compulsive behaviors therapy material. The pages shown help educators, therapists, and caregivers understand the structure and content of the resource before use. Materials should be used under appropriate professional guidance.




















Share this resource
Help others discover this
"From the ritual that holds all the power — to the child who holds their own power back. From fear to mastery. One technique at a time."
OT | Psychology | BCBA/ABA | SpEd | NeuroDevelopmental Pediatrics
70+ Centers | 70+ Countries Served
🌐 pinnacleblooms.org
✉ care@pinnacleblooms.org