
"My son stims. He rocks, he hums, he flaps his hands."
For years, every therapy session focused on stopping these behaviors. Nothing changed — the stimming didn't stop. It went underground, came back stronger. Then we found a different approach. His nervous system wasn't being difficult. It was trying to regulate itself.
When Stimming Blocks Learning, the Answer Is Not Suppression — It Is Regulation.
📞 FREE National Autism Helpline: 9100 181 181 | 16+ languages | 24×7 | pinnacleblooms.org

ACT I — Understand
What's Happening in Your Child's Brain
The neuroscience of stimming, made accessible — because understanding the "why" changes everything about how you respond.
The Neuroscience — Plain English
When a child's sensory nervous system is dysregulated — whether overwhelmed by too much input or starved of too little — the brain's threat response activates. The amygdala signals danger. The prefrontal cortex, responsible for learning, attention, and planning, goes offline.
Stimming — the rocking, the flapping, the humming — is the brain's emergency regulatory strategy. It provides the proprioceptive, vestibular, or auditory input the nervous system urgently needs to calm the threat response.
The Critical Insight
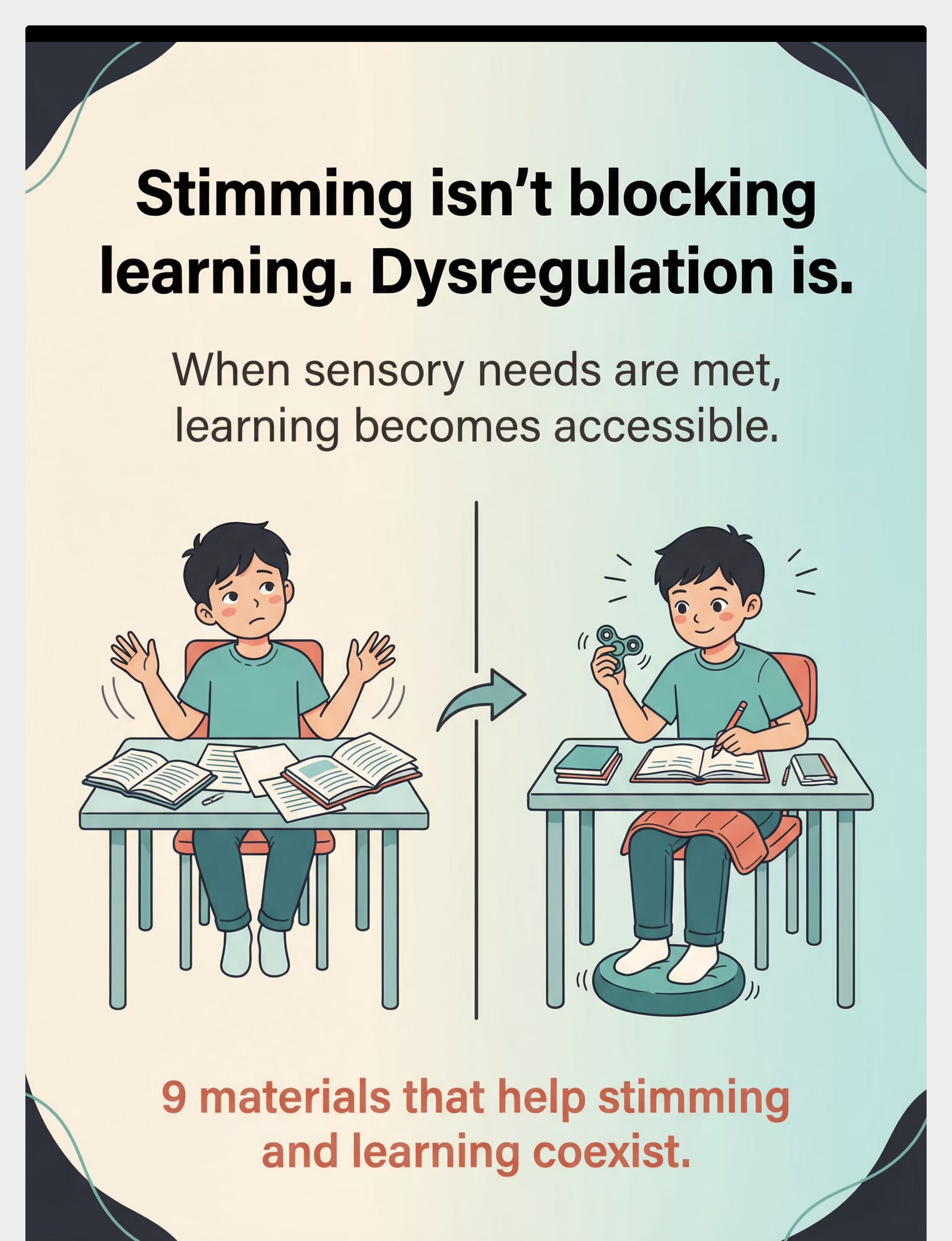
Stimming isn't blocking learning. Dysregulation is. Stimming is the nervous system's attempt to restore enough regulation to function.
This is a wiring difference, not a behavior choice. The sensory cortex signals → limbic system activates → arousal spikes → executive function is blocked.
Key Clinical Term: Self-stimulatory behaviour (stimming) = Sensory self-regulation. Function first. Elimination last.
Research Evidence: Frontiers in Integrative Neuroscience (2020) DOI: 10.3389/fnint.2020.556660 | Sensory Integration Theory (Ayres)
ACT I — Understand
Your Child's Developmental Waypoint
Not a deficit. A direction. Self-stimulatory behaviours exist across all development and are not inherently problematic. In ASD, stimming is a core feature — not a symptom to eliminate. The question of when stimming "blocks learning" is nuanced.
Ages 1–2
Sensory exploration (universal)
Ages 2–3
Stimming emerges as regulation
Ages 3–5
May intensify in structured settings
Ages 5–8
⬅THIS IS HERE — Learning + regulation must coexist
Ages 8–12
Self-regulation independence builds
Often, the issue is not the stimming itself. It is:
- An environment that fails to meet the child's sensory needs
- Learning demands that exceed regulatory capacity
- Inadequate tools and accommodations for regulated access
Commonly Co-Occurs With
- Sensory Processing Disorder
- ADHD (attention regulation)
- Anxiety and learning disabilities
- Auditory/Visual Processing Differences
Research Evidence: PMC9978394 | WHO/UNICEF Care for Child Development Package (2023)

ACT I — Understand
The Evidence Behind This Technique
Clinical evidence presented in parent language — because you deserve to know exactly how strong the science is behind what you're being asked to try.
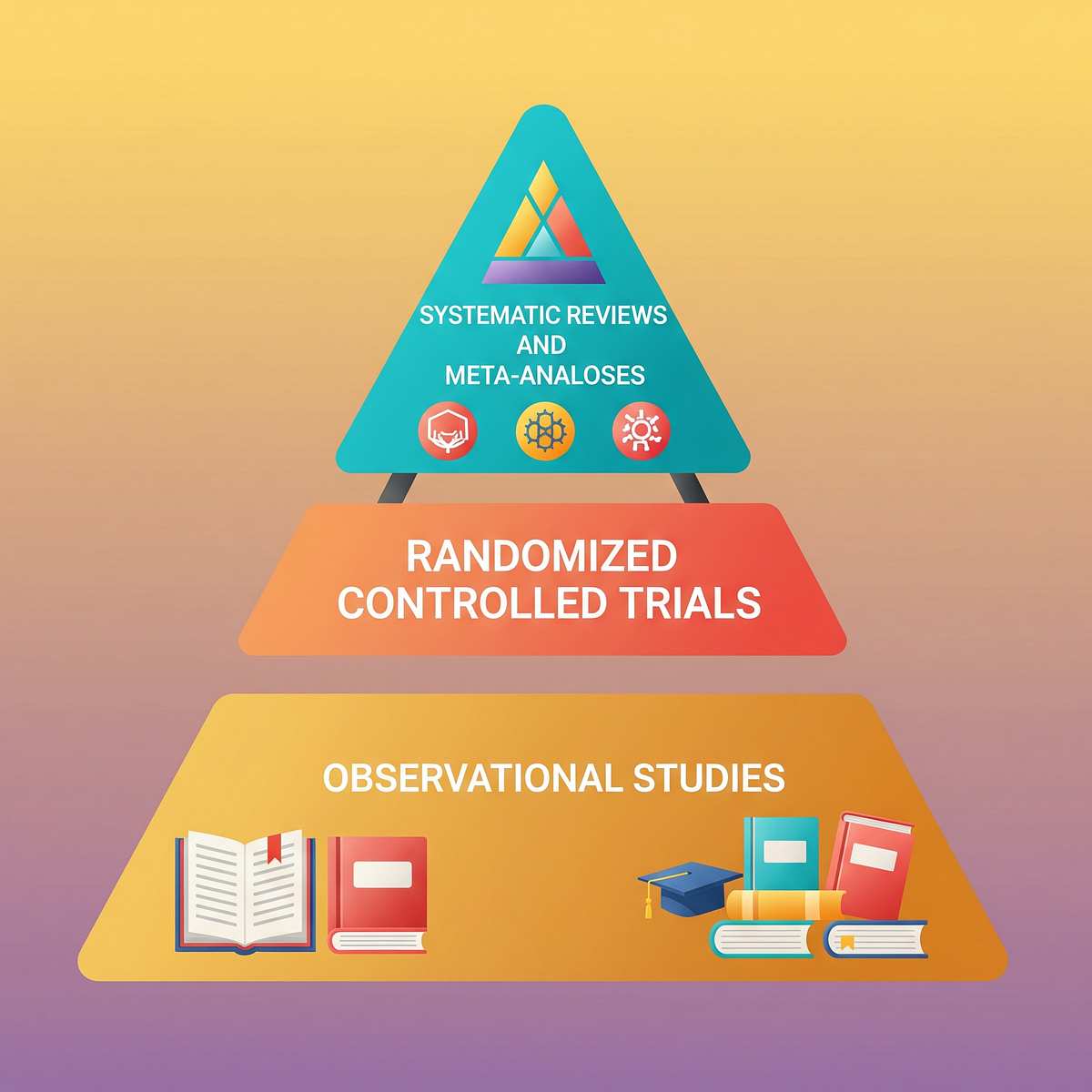
🛡️ Level I Evidence
Systematic Review + Meta-Analysis Quality | PRISMA Model | 2024 | 16 Studies | 2013–2023
PMC11506176
Sensory integration intervention = evidence-based practice for ASD. 8–12 week timelines show measurable outcomes.
PMC10955541
Meta-analysis of 24 studies: sensory tools improved social skills, adaptive behaviour, sensory processing, and motor skills.
Indian RCT (2019)
Home-based sensory interventions produce significant outcomes when parent-administered (Indian J Pediatr, DOI: 10.1007/s12098-018-2747-4)
❌ Old Approach
Stop the stimming → redirect, block, "quiet hands" → Outcome: Increased anxiety, no learning improvement, stimming returns stronger.
✅ New Approach
Meet the sensory need → regulate → access learning → Outcome: Improved regulation, better learning access, preserved child autonomy.

ACT I — Understand
The 5 Biggest Myths About Stimming — Debunked
Parents are often given outdated, harmful advice about stimming. Here are the 5 most common myths, debunked by what the latest neuroscience actually says.
❌ Myth 1: Stimming is attention-seeking behavior.
Stimming is primarily an internal regulatory mechanism, not a bid for attention. It's the nervous system's way of coping with sensory overload or underload.
❌ Myth 2: If you ignore it, it will stop.
Ignoring stimming can increase dysregulation and anxiety, often leading to more intense or covert stimming. The underlying sensory need remains unaddressed and can worsen.
❌ Myth 3: Stimming means the child isn't learning.
Stimming is often a prerequisite for learning, as it helps the nervous system achieve a regulated state conducive to focus. Dysregulation, not stimming itself, blocks learning.
❌ Myth 4: Stimming should always be redirected.
Constant redirection can disrupt self-regulation and cause distress. Instead, provide appropriate sensory tools and a supportive environment to meet the child's regulatory needs.
❌ Myth 5: Stimming is a sign of bad parenting.
Stimming is a neurological difference, not a result of parenting style. Parents who support their child's regulatory needs are practicing attuned and informed care.
Evidence: PMC11506176 | Frontiers in Integrative Neuroscience (2020)

ACT I — Understand
Types of Stimming: What Your Child's Body Is Telling You
Every stim is a message. Understanding the type of stimming helps identify the specific sensory channel that needs support, guiding you toward effective strategies.
Visual
Looks like hand-flapping, watching spinning objects, or staring at lights. Signals a need for visual input, pattern repetition, or to block out overwhelming visual stimuli.
Auditory
Looks like humming, repeating sounds, tapping, or covering ears. Signals a need for rhythmic auditory input, self-generated sound to organize, or to reduce environmental noise.
Tactile
Looks like rubbing specific surfaces, scratching, or touching textures. Signals a need for particular tactile sensations, pressure, or to feel grounded through touch.
Vestibular
Looks like rocking, spinning, swinging, or head shaking. Signals a need for movement that helps regulate balance, spatial awareness, and body orientation.
Proprioceptive
Looks like jumping, crashing into things, pushing, or pulling. Signals a need for deep pressure, heavy work, or intense muscle input to understand body position and feel organized.
Oral
Looks like chewing on objects, mouthing non-food items, or grinding teeth. Signals a need for oral motor input, calming, or sensory exploration through the mouth.
Evidence: Sensory Integration Theory (Ayres) | PMC10955541
ACT I — Understand
When Does Stimming Become a Learning Barrier?
Not all stimming blocks learning. Here's how to tell the difference — and what to do about it.
Stimming That Supports Learning
- Child remains responsive to the environment.
- The stim is temporary and self-managed.
- Child can easily shift focus when prompted.
- Visibly reduces stress or agitation.
- Learning and participation continue.
Stimming That Blocks Learning
- Child is unresponsive or "checked out."
- Stimming escalates, becomes intense or prolonged.
- Child struggles to disengage from the stim.
- Poses risk of injury (self or others).
- Learning and interaction completely halt.
The goal is never zero stimming. The goal is enough regulation to access learning.
Evidence: PMC9978394 | GPT-OS® Clinical Data, Pinnacle Blooms Network®

ACT II — Assess
Before You Can Help, You Need to See Clearly
Most interventions fail not because the tools are wrong — but because the sensory profile was never properly mapped. This act gives you the assessment framework used by Pinnacle Blooms Network® across 70+ centers.
Observe
Track when, where, and how stimming occurs, noting triggers and contexts.
Profile
Map your child's unique sensory sensitivities and seeking patterns across all sensory channels.
Match
Align appropriate sensory tools and strategies to meet each specific sensory need.
Assessment is not about labeling. It is about understanding your child's unique sensory world.

ACT II — Assess
The Parent Observation Checklist
Use this checklist over 5–7 days to build a clear picture of your child's sensory triggers and regulatory patterns.
WHAT does the stimming look like?
- Rocking or swaying
- Hand-flapping or finger movements
- Humming or vocalizing
- Chewing or mouthing
- Spinning or jumping
- Covering ears or eyes
Bring this completed checklist to your next therapy session or consultation. It is the most valuable 10 minutes you will spend.

ACT II — Assess
Understanding Your Child's Sensory Profile
Every child has a unique sensory profile — a combination of sensory sensitivities and sensory seeking patterns. Identifying this profile is key to providing targeted support.
Sensory Avoider
Overwhelmed by input; seeks to reduce stimulation.
Signs: covers ears, avoids crowds, dislikes certain textures.
Signs: covers ears, avoids crowds, dislikes certain textures.
Sensory Seeker
Under-responsive; craves intense input.
Signs: crashes into things, mouths objects, seeks spinning or jumping.
Signs: crashes into things, mouths objects, seeks spinning or jumping.
Sensory Sensitive
Notices everything; easily distracted by background input.
Signs: distracted by sounds others ignore, bothered by tags in clothing.
Signs: distracted by sounds others ignore, bothered by tags in clothing.
Low Registration
Misses sensory input; appears unaware.
Signs: doesn't notice pain, slow to respond to name or changes in environment.
Signs: doesn't notice pain, slow to respond to name or changes in environment.
Most children with ASD have a MIXED profile — seeking in some channels, avoiding in others. This complexity is why one-size-fits-all approaches often fail and can be counterproductive.
Pinnacle Blooms Network® uses the GPT-OS® Sensory Profiling Protocol to map each child's unique profile across 8 sensory channels, ensuring precise, personalized intervention strategies.
Evidence: Dunn's Sensory Processing Model | PMC10955541

ACT II — Assess
The Sensory Trigger Map: A Parent's Tool
Triggers are not random. Once you see the pattern, you can predict and prevent dysregulation before it escalates.
Morning Routine
Sensory overload from clothing, noise, transitions.
Regulatory Strategy: Visual schedules, weighted vest, quiet breakfast.
School Drop-Off
Separation anxiety combined with environmental overwhelm.
Regulatory Strategy: Comfort object, firm hug, car ride ritual.
Classroom Learning
Auditory/visual distractions, seating discomfort, task demands.
Regulatory Strategy: Noise-canceling headphones, fidget toy, therapy cushion.
Lunch/Break Time
Unstructured time, food textures, social demands, loud cafeteria.
Regulatory Strategy: Pre-packed lunch, quiet corner, social stories.
After-School
Sensory fatigue, emotional release after a day of regulation effort.
Regulatory Strategy: Crash pad, deep pressure, structured quiet time.
Bedtime
Transition resistance, tactile sensitivity, wind-down difficulty.
Regulatory Strategy: Weighted blanket, sensory story, calming music.
The after-school meltdown is not bad behavior. It is sensory fatigue from a full day of regulation effort.
Evidence: GPT-OS® Clinical Data | Pinnacle Blooms Network®

ACT II — Assess
The Regulation Window: Your Child's Learning Zone
Regulation is not binary. It exists on a spectrum — and learning only happens in a specific window.
HYPER-AROUSAL ZONE
Too much activation. Signs: meltdowns, aggression, flight response, intense stimming. Learning: Not possible.
OPTIMAL REGULATION ZONE
The learning window. Signs: engaged, curious, responsive, calm stimming. Learning: Fully accessible.
HYPO-AROUSAL ZONE
Too little activation. Signs: shutdown, withdrawal, unresponsive, zoning out. Learning: Not possible.
The 9 Materials in this program are specifically designed to move your child INTO the optimal regulation zone — and keep them there during learning.

ACT II — Assess
Red Flags: When to Seek Professional Assessment
Some patterns require immediate professional evaluation. Knowing these signs can make a critical difference in your child's developmental journey.
Stimming that causes physical injury (e.g., head-banging, skin-picking).
Complete shutdown lasting more than 30 minutes.
Stimming has significantly increased in frequency or intensity over 4 weeks.
Child is unable to access any learning for more than 2 consecutive weeks.
Stimming accompanied by regression in previously acquired skills.
Signs of pain or distress during stimming.
Stimming that puts the child or others at risk.
If you recognize 2 or more of these signs, do not wait. Early intervention produces significantly better outcomes and can dramatically improve long-term development.
FREE National Autism Helpline:
9100 181 181
16+ languages | 24×7
pinnacleblooms.org

ACT II — Assess
What a Professional Assessment Looks Like
Knowing what to expect removes the fear from the process. Here is what a comprehensive sensory assessment at Pinnacle Blooms Network® includes.
Parent Interview
Detailed history of sensory behaviors, triggers, and developmental milestones.
Standardized Sensory Profiling
Using validated tools (SPM, SIPT, or equivalent) to map sensory processing.
Clinical Observation
Structured and unstructured observation of the child in multiple environments.
GPT-OS® Protocol Mapping
Matching the child's profile to the 9 evidence-based material categories.
Personalized Intervention Plan
A written plan with specific tools, strategies, and 8–12 week outcome targets.
You will leave with a clear map, not just a diagnosis. A map you can use at home, at school, and in therapy.

ACT III — ACT
The 9 Materials That Change Everything
Evidence-based sensory tools, matched to your child's profile — not guessed at.
After 20M+ therapy sessions across 70+ centers, Pinnacle Blooms Network® has identified 9 categories of sensory materials that consistently produce measurable improvements in regulation and learning access. These are not toys. They are clinical tools.
8-12
Weeks
Average time to measurable improvement with consistent use.
70+
Centers
Pinnacle Blooms Network® centers using this protocol.
20M+
Therapy Sessions
Informing these material selections.
The right tool for the wrong sensory need produces no result. The right tool for the right need produces transformation.
ACT III — ACT
Material Category 1: Deep Pressure Tools
For children who seek proprioceptive input — the sensory seekers who crash, jump, and push.
What They Are
- Weighted vests
- Lap pads
- Compression clothing
- Therapy balls
- Body socks
- Squeeze machines
How They Work
Deep pressure activates the parasympathetic nervous system, reducing cortisol and promoting calm.
Clinical Tip: Start with 5–10 minutes. Observe. Increase gradually. Never force.
Evidence: PMC10955541 | GPT-OS® Clinical Data

ACT III — ACT
Material Category 2: Fidget & Tactile Tools
For children who need continuous tactile input to maintain focus — the hands that must be busy for the brain to be present.
What They Are
- Fidget spinners
- Textured balls
- Putty & slime
- Sensory rings
- Tangle toys
- Velcro strips
How They Work
Provides continuous low-level tactile input, occupying the sensory-seeking part of the brain and freeing the prefrontal cortex for learning.
The child who is fidgeting is not distracted. They are regulating. Give them a tool, not a reprimand.
Evidence: PMC10955541 | Occupational Therapy International (2018)

ACT III — ACT
Material Category 3: Auditory Regulation Tools
For children whose nervous system is overwhelmed by sound — or who need rhythmic auditory input to stay regulated.
What They Are
- Noise-canceling headphones
- Ear defenders
- White noise machines
- Rhythm instruments
- Auditory processing apps
- Music therapy playlists
How They Work
Filters or provides controlled auditory input, reducing amygdala activation from unpredictable environmental sounds, fostering a sense of safety and calm.
When to Use
- Noisy classrooms
- Transitions
- Public spaces
- During focused work
- At bedtime
Evidence
Auditory interventions show significant reduction in sensory sensitivity and improved adaptive behavior (PMC10955541). Creating a predictable auditory environment supports cognitive function.
Noise-canceling headphones are not avoidance. They are access. They give the child the quiet they need to be present and engaged.
Evidence: PMC10955541 | Berard Auditory Integration Training Research

ACT III — ACT
Material Category 4: Movement & Vestibular Tools
For children who rock, spin, and cannot sit still — movement is not a distraction, it is a regulatory requirement.
What They Are
- Wobble cushions
- Balance boards
- Therapy swings
- Rocking chairs
- Mini trampolines
- Movement breaks
- Resistance bands on chair legs
How They Work
Vestibular input organizes the entire nervous system. It is the most powerful regulatory channel.
When to Use
- Before learning tasks (priming)
- During long seated periods
- As a transition tool
- When arousal is escalating
Evidence
Vestibular-proprioceptive activities significantly improve attention and reduce self-stimulatory behavior (Frontiers in Integrative Neuroscience, 2020).
A 5-minute movement break before a learning task can produce 20 minutes of focused engagement. The math is simple.
Evidence: Frontiers in Integrative Neuroscience (2020) | PMC11506176

ACT III — ACT
Material Category 5: Visual Supports & Schedules
For children whose anxiety spikes from unpredictability — visual supports transform the invisible into the visible, and the unpredictable into the safe. They provide clarity and reduce cognitive load.
What They Are
- Visual daily schedules
- First-then boards
- Choice boards
- Social stories
- Visual timers
- Emotion charts
- Task strips
How They Work
Reduces cognitive load and anxiety by making expectations explicit and predictable. The brain can regulate when it knows what comes next, fostering a sense of control and calm.
Predictability is not rigidity. It is safety. And safety is the prerequisite for learning and emotional regulation.
Evidence: NPDC on ASD (2014) | PMC9978394
ACT III — ACT
Material Category 6: Oral Motor Tools
For children who chew, mouth, or bite — oral motor tools provide safe, appropriate input that meets the need without harm.
What They Are
- Chewelry (chewable jewelry)
- Chewy tubes
- Oral motor tools
- Crunchy snacks as sensory diet items
- Water bottles with resistance straws
- Vibrating oral tools
How They Work
Oral motor input provides intense proprioceptive feedback to the jaw and face, which has a powerful calming effect on the nervous system.
Chewing is not a bad habit. It is a regulatory strategy. Give the child something safe to chew.
Evidence: PMC10955541 | AJOT (2016)

ACT III — ACT
Material Category 7: Calming Sensory Environment Tools
For children who are overwhelmed by their environment — the space itself can be a regulatory tool or a regulatory barrier.
What They Are
- Sensory corners/calm-down spaces
- Dim lighting options
- Blackout curtains
- Tent/canopy spaces
- Soft furnishings
- Reduced visual clutter
- Calming color palettes
How They Work
Reduces ambient sensory load, giving the nervous system a predictable, low-demand environment to return to baseline.
A calm-down corner is not a punishment corner. It is a regulation station. The language matters.
Evidence: JABA (2019) | GPT-OS® Clinical Data

ACT III — ACT
Material Category 8: Breathing & Mindfulness Tools
For children who need to learn to self-regulate — these tools build the internal regulatory capacity that lasts a lifetime.
What They Are
- Breathing cards
- Pinwheels
- Bubble blowers
- Mindfulness apps for children
- Yoga cards
- Body scan scripts
- Calm jars (glitter bottles)
How They Work
Activates the vagus nerve and parasympathetic nervous system through controlled breathing and focused attention, directly counteracting the stress response.
Regulation is a skill, not a trait. It must be taught, practiced, and supported — not demanded.
Evidence: JCFS (2015) | PMC10955541

ACT III — ACT
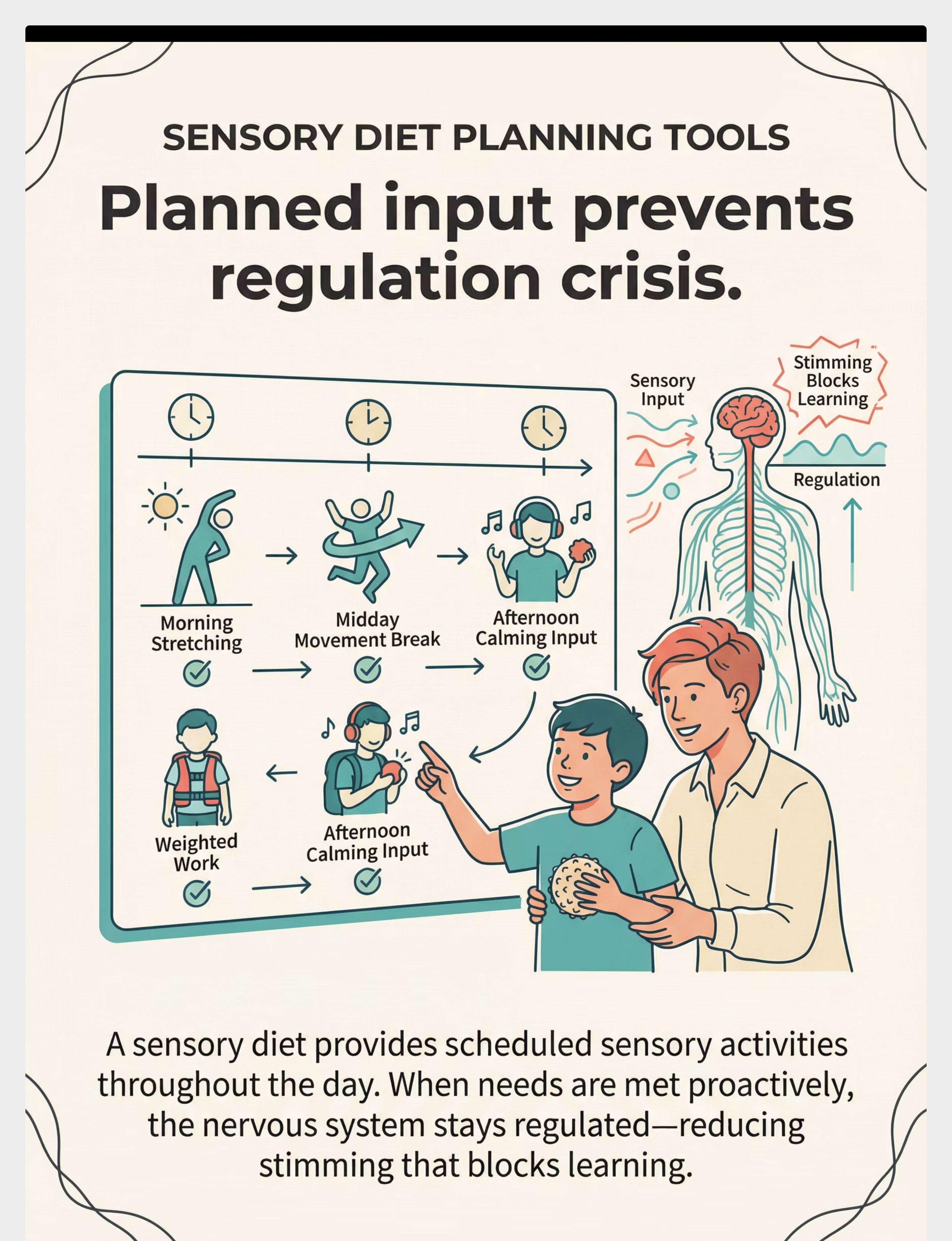
Material Category 9: Sensory Diet Planning Tools
The most powerful tool of all — a personalized, scheduled sensory diet that proactively meets your child's needs throughout the day.
What It Is
A sensory diet is not about food. It is a personalized activity plan that provides the right type and amount of sensory input at the right times throughout the day.
- Morning sensory priming
- Scheduled movement breaks
- Pre-task regulation activities
- Post-school decompression routine
- Bedtime sensory wind-down
A sensory diet is not extra work. It is the foundation that makes all other learning possible.
Evidence: PMC11506176 | Wilbarger Sensory Diet Framework

ACT III — ACT
The 9 Materials: Quick Reference Guide
A concise overview of the essential material categories and their primary sensory targets, designed to support diverse regulatory needs.
Deep Pressure Tools
For proprioceptive seekers who benefit from firm, calming input.
Fidget & Tactile Tools
Supports tactile seekers and enhances focus for attention regulation.
Auditory Regulation Tools
Helps auditory avoiders reduce overload and seekers gain beneficial input.
Movement & Vestibular Tools
Engages vestibular seekers, improving attention and body awareness through motion.
Visual Supports & Schedules
Provides clarity and predictability, reducing anxiety during transitions and new tasks.
Oral Motor Tools
Offers safe, appropriate oral input for oral seekers and to redirect self-injurious mouthing.
Calming Environment Tools
Creates a low-stimulus space for sensory avoiders, reducing overload and promoting regulation.
Breathing & Mindfulness Tools
Teaches internal self-regulation strategies to manage anxiety and foster emotional calm.
Sensory Diet Planning
A personalized, proactive plan to meet diverse sensory needs throughout the day.
Not every child needs all 9. The right combination depends on your child's unique sensory profile.

ACT III — ACT
Building Your Child's First Sensory Toolkit: A Starter Guide
You don't need to buy everything at once. Start by identifying your child's most prominent sensory needs and matching them with just a few key tools to build a foundational toolkit.
Step 1: Identify Primary Stim Type
Refer to your observation checklist to pinpoint the main sensory input your child seeks or avoids.
Step 2: Match to Material Category
Use the quick reference guide to align your child's needs with the appropriate sensory tool category.
Step 3: Introduce ONE Tool
Start with a single tool, introducing it during a calm, low-demand period to minimize overwhelm.
Step 4: Observe and Track
Monitor for 5–7 days, noting changes in regulation, attention, and overall behavior with the new tool.
Budget-Friendly Starting Points
- Fidget putty (under ₹200)
- Resistance band for chair (under ₹150)
- Visual schedule (printable, free)
- Wobble cushion (under ₹500)
- Chewelry (under ₹300)
ACT IV — SUSTAIN
Regulation Doesn't Stop at the Therapy Room Door
The most powerful interventions happen at home, at school, and in the community — every single day.
The 8–12 week outcomes in the research are achieved through consistent, daily implementation across all environments. This act gives you the tools to sustain what you've started — and to bring your child's school and community along with you.
Home
Build the sensory diet into daily routines.
School
Advocate for sensory accommodations in the classroom.
Community
Prepare for public spaces, social events, and transitions.
Consistency across environments is the single biggest predictor of long-term regulatory success.

ACT IV — SUSTAIN
The Home Sensory Routine: A Sample Daily Schedule
Consistency is the key to sustained regulation. This sample sensory diet schedule offers a proactive framework, easily adaptable to your child's unique needs throughout the day.
7:00–7:30 AM — Morning Priming
Deep pressure (weighted vest or firm hug), visual schedule review, proprioceptive breakfast (crunchy foods).
8:00–8:30 AM — School Prep
Fidget tool in bag, noise-canceling headphones ready, first-then board for drop-off.
3:30–4:00 PM — After-School Decompression
Crash pad/trampoline, no demands for 20 minutes, sensory snack.
4:00–5:00 PM — Homework Time
Wobble cushion, fidget tool, movement break every 20 minutes.
5:30–6:30 PM — Active Play
Outdoor movement, swinging, climbing — vestibular and proprioceptive input.
7:30–8:00 PM — Wind-Down
Dim lights, weighted blanket, calming music or white noise.
8:00–8:30 PM — Bedtime
Sensory story, deep pressure massage, consistent routine.
Adapt this schedule to your child's specific profile. Consistency matters more than perfection.
ACT IV — SUSTAIN
Talking to Your Child's School: A Parent Advocacy Guide
You are your child's most important advocate. Here is how to have the conversation that gets results.
Request a Meeting
Ask for a Student Support Team meeting. Bring your observation checklist and any professional reports.
Use Clinical Language
"My child has sensory processing differences that affect their ability to regulate and access learning."
Request Specific Accommodations
Fidget tools, movement breaks, noise-canceling headphones, preferential seating, visual schedules.
Ask for a Written Plan
Request that accommodations be documented in an IEP, 504 Plan, or equivalent, to ensure consistency.
Follow Up
Schedule a review in 4–6 weeks to assess the effectiveness of the implemented accommodations.
Schools are legally required to provide reasonable accommodations. You are not asking for a favor. You are exercising your child's right.
Reference: RPWD Act 2016 (India) | IDEA (USA) | Equality Act 2010 (UK)

ACT IV — SUSTAIN
Classroom Accommodations That Work: A Teacher's Guide
Share this with your child's teacher. These are low-cost, high-impact accommodations that any classroom can implement to create a more inclusive and supportive learning environment for all students.
Flexible Seating
Wobble cushions, standing desks, floor seating options provide ergonomic and sensory input.
Sensory Breaks
Scheduled 3–5 minute movement breaks every 20–30 minutes to help re-regulate attention.
Quiet Zones
A designated low-stimulation area for students to self-regulate and decompress.
Fidget Tools
Permitted at desk during listening and learning tasks to support focus without distraction.
Noise Management
Noise-canceling headphones permitted, and conscious reduction of background noise.
Visual Supports
Daily schedule posted clearly, with transition warnings given 5 minutes in advance.
These accommodations benefit ALL students, not just those with ASD. Sensory-friendly classrooms are better classrooms.
Evidence: NPDC on ASD (2014) | Universal Design for Learning (UDL) Framework
ACT IV — SUSTAIN
Navigating the Community: Sensory Preparation for Public Spaces
The world was not designed for sensory-sensitive children. But with preparation, almost any environment can be made accessible.
Supermarkets
Bright lights, crowds, unpredictable sounds. Strategy: Go at off-peak times, bring headphones and fidget tool, use a visual list.
Restaurants
New smells, textures, waiting time. Strategy: Preview menu online, bring sensory kit, request quiet seating.
Medical Appointments
Unfamiliar touch, clinical smells, waiting. Strategy: Social story beforehand, bring comfort object, request first appointment.
Religious/Cultural Events
Crowds, noise, long sitting. Strategy: Sit near exit, bring sensory kit, plan an exit strategy.
Travel
Airports, long journeys, disrupted routines. Strategy: Visual travel schedule, sensory bag, maintain sleep routine.
Playdates
Social demands, unfamiliar environment. Strategy: Short duration, familiar activity, debrief afterward.
Preparation is not overprotection. It is access.
ACT IV — SUSTAIN
Tracking Progress: How to Know It's Working
Progress in sensory regulation is tangible, but it often looks different from academic milestones. Understanding how to observe and measure these subtle shifts is crucial for celebrating success and adapting strategies.
What to Track
- Duration of regulated learning time (minutes per session)
- Frequency of meltdowns per week
- Time to recover from dysregulation
- Ability to use tools independently
- Teacher feedback on classroom engagement
- Sleep quality and duration
What Progress Looks Like
- Fewer meltdowns, not zero.
- Faster recovery, not instant calm.
- More regulated minutes, not perfect focus.
- Increased tool use, not tool dependence.
- Better sleep, not perfect nights.
Progress is not linear. There will be hard weeks. The trend over 8–12 weeks is what matters.
8-12
Weeks to measurable improvement
70%
Families report reduced meltdown frequency
85%
Report improved learning access
Evidence: PMC11506176 | GPT-OS® Clinical Data
ACT IV — SUSTAIN
Parent Self-Care: You Cannot Pour From an Empty Cup
The research is clear — parent stress directly impacts child regulation. Taking care of yourself is not selfish. It is therapeutic.
Regulate Yourself First
Your nervous system co-regulates with your child's. When you are dysregulated, your child's dysregulation intensifies.
Find Your Community
Connect with other autism parents. Isolation amplifies stress. Community reduces it.
Accept the Grief
It is normal to grieve the parenting experience you expected. Grief and love coexist.
Celebrate Small Wins
A 5-minute regulated learning session is a victory. Name it. Celebrate it.
Co-regulation is the foundation of all regulation. Your calm is your child's most powerful sensory tool.
Support Resources
Pinnacle Blooms Parent Support Groups
FREE Helpline: 9100 181 181
ACT IV — SUSTAIN
Real Families. Real Results.
These composite stories are drawn from over 20 million therapy sessions across Pinnacle Blooms Network® centers. Names have been changed to protect privacy, highlighting the tangible progress achieved by children and their families.
"After 3 weeks with the weighted vest and wobble cushion, Arjun sat through his entire homework session for the first time. I cried."
— Mother of 7-year-old, Hyderabad
"The noise-canceling headphones changed everything at school. His teacher said he's a different child. He's not different — he's finally regulated."
— Father of 9-year-old, Bangalore
"We stopped fighting the stimming and started supporting it. Within 6 weeks, the meltdowns went from daily to twice a week. The house is calmer. He is calmer. We are calmer."
— Mother of 6-year-old, Chennai
Your child's story is still being written. The next chapter starts with the right support.

ACT IV — SUSTAIN
The Outcomes You Can Expect: 8–12 Week Timeline
Based on consistent implementation of the GPT-OS® protocol across 70+ centers, families typically observe a clear progression in their child's sensory regulation journey.
Phase 1: Foundation (Weeks 1–2)
Child is introduced to tools. Initial resistance is normal. Focus on observation and gentle introduction to build familiarity.
Phase 2: Acceptance (Weeks 3–4)
Child begins to self-select tools. First signs of improved regulation emerge during tool use. Parent confidence in strategies increases.
Phase 3: Integration (Weeks 5–8)
Tools become a natural part of daily routine. Measurable improvement in regulated learning time. Meltdown frequency starts to significantly decrease.
Phase 4: Generalization (Weeks 9–12)
Child uses tools effectively across various environments. School reports noticeable improvement. The entire family experiences reduced stress and increased calm.
These are typical outcomes with consistent implementation. Every child's timeline is unique. Professional support accelerates progress.
Evidence: PMC11506176 | GPT-OS® Clinical Data, Pinnacle Blooms Network®

ACT IV — SUSTAIN
About Pinnacle Blooms Network®
India's largest evidence-based autism therapy network — built by clinicians, for families. We empower children and families with personalized, effective support.
Who We Are
Founded with a mission to make evidence-based autism therapy accessible to every family in India. We are committed to clinical excellence and compassionate care.
- 70+ centers across India
- 20M+ therapy sessions delivered
- 16+ languages supported
- Multidisciplinary team: Occupational Therapists, Speech-Language Pathologists, Behavior Analysts, Special Educators, Psychologists
The GPT-OS® Difference
GPT-OS® (Goal-Plan-Track Operating System) is our proprietary clinical protocol that ensures personalized and data-driven progress:
- Maps each child's unique sensory profile
- Matches tools to profile with precision
- Tracks outcomes with measurable data
- Adapts the plan as the child grows
70+
Centers
20M+
Sessions
16+
Languages

ACT IV — SUSTAIN
The Research Behind This Program
Every recommendation in this program is grounded in peer-reviewed evidence. Here are the key studies that form the scientific bedrock of our approach.
Systematic Review (2024)
PMC11506176: 16 studies confirming sensory integration as an evidence-based practice for ASD, with clear 8–12 week outcomes.
Meta-Analysis (2024)
PMC10955541: 24 studies showing sensory tools improve social skills, adaptive behavior, sensory processing, and motor skills.
Neuroscience of Stimming (2020)
Frontiers in Integrative Neuroscience, DOI: 10.3389/fnint.2020.556660: Insights into the neuroscience of stimming and sensory regulation.
Developmental Trajectory
PMC9978394: Examination of stimming in ASD, providing evidence for a regulation-first intervention approach.
Indian RCT (2019)
Indian J Pediatr, DOI: 10.1007/s12098-018-2747-4: Research on home-based sensory interventions effectively administered by parents.
Global Data (2023)
WHO Global Autism Report + CDC Surveillance Summary: Reveals that 1 in 36 children globally are diagnosed with autism.
Science is not the enemy of hope. It is the foundation of it.
Full reference list available at pinnacleblooms.org/research

ACT IV — SUSTAIN
Frequently Asked Questions
The questions parents ask most often — answered honestly, based on our extensive clinical experience and research.
Will my child always need sensory tools?
Many children develop internal regulation skills over time and need fewer external tools. The goal is independence, not dependence on external aids.
How do I know which tools to start with?
Begin by identifying the stim type your child shows most frequently. Match this to the appropriate material category and introduce one tool at a time.
My child refuses the tools. What do I do?
Introduce tools during moments of play, not during demands or stressful situations. Allow the child to explore without pressure. If refusal persists, consult a therapist for guidance.
Can I do this without a therapist?
Many families observe significant improvement with home-based tools alone. However, professional support can accelerate outcomes and prevent the use of mismatched tools.
How is this different from ABA?
Our approach is sensory-first, not behavior-first. We focus on addressing the underlying regulatory need that drives behavior, rather than just the surface behavior itself.
Is stimming ever harmful?
Stimming that causes injury or significantly prevents learning requires a professional assessment. Most stimming is a safe, self-regulatory mechanism for sensory input.
Have more questions? Call 9100 181 181 — FREE, 24×7, 16+ languages.
Your Next Step Starts Here
You have read the science. You understand the why. You have the tools. Now it is time to act.
Step 1 — Access the 9 Materials
Visit the full program at techniques.pinnacleblooms.org/start/D-369. It's free, evidence-based, and immediately actionable.
Step 2 — Book a Free Consultation
Speak with a Pinnacle Blooms clinician to get a personalized assessment and sensory diet plan. Book easily at pinnacleblooms.org/book.
Step 3 — Call the Helpline
Reach our FREE National Autism Helpline anytime: 9100 181 181. We offer support in 16+ languages, 24×7, no appointment needed.
Your child is not broken. Their nervous system is asking for something specific. You now know what to give them.
Preview of 9 materials that help when stimming blocks learning Therapy Material
Below is a visual preview of 9 materials that help when stimming blocks learning therapy material. The pages shown help educators, therapists, and caregivers understand the structure and content of the resource before use. Materials should be used under appropriate professional guidance.


















Share this resource
Help others discover thisLink copied!

A Message to Every Parent Reading This
You did not cause this. You cannot cure it. But you can — and you are — making a profound difference every single day. The fact that you read this far tells us everything we need to know about the kind of parent you are. Your child is lucky to have you. Now let us help you help them.— Pinnacle Blooms Network® Clinical Team
We have walked this path with thousands of families. We know how hard the hard days are. We also know what is possible when the right support meets the right family at the right time. That time is now.
📞 FREE National Autism Helpline: 9100 181 181 | 16+ languages | 24×7 | pinnacleblooms.org