
"They'll hold it for six hours rather than use a public toilet."
You've tried everything. Bribing. Waiting. Reasoning. Carrying them in. The automatic flush fires and the meltdown begins in the stall doorway — again. Your family plans every outing around whether there's a home toilet nearby.
E-504 · Public Restroom Refusal Intervention
ADL & Self-Care Series · Episode 504
"You are not failing. Your child's nervous system is speaking — and today you find out exactly what it's saying."

You Are Among Millions of Families Navigating This Exact Challenge
80%
Sensory Difficulties in ASD
of children with ASD experience clinically significant sensory processing difficulties
1 in 36
Autism Prevalence
children diagnosed with autism in India — an estimated 18 million families affected
75%
Toileting Challenges
of children with sensory processing differences show toileting-related challenges
Public restroom refusal is not rare. It is not your child being stubborn. Across Pinnacle's 70+ centres and 20M+ sessions, toileting avoidance in public settings is among the top 15 presenting challenges in the 3–12 age group. The sensory assault of a public restroom — 80–90 dB hand dryers, unpredictable automatic flushes, echoing tile acoustics, industrial cleaning odours — is genuinely overwhelming for sensitised nervous systems.
"When a child holds their urine for 6+ hours rather than use a public toilet, their nervous system has decided the threat is real — even if the threat is a hand dryer." — Pinnacle OT Consortium
PRISMA Systematic Review, 2024 · PMC11506176 | WHO/CDC prevalence consensus 2023 | Sensory Profile research, Dunn 2014

This Is a Wiring Difference, Not a Behaviour Choice
The Sensitised Auditory System
In children with sensory processing differences, the auditory cortex fails to habituate to repeated sound stimuli. The hand dryer that triggers a startle reflex in session one will trigger the same reflex in session fifty — unless systematic desensitisation occurs. This is not a choice. The brain is applying the same neural mechanism that kept our ancestors alive.
The amygdala — the brain's threat-detection centre — encodes the automatic flusher as "danger." Once this association is formed, the predictive brain creates anticipatory anxiety before even entering the restroom. This is identical to PTSD threat-prediction mechanisms, just scaled to a sensory trigger.
Why Avoidance Feels Right
Leaving (or never entering) the restroom eliminates distress immediately. This negative reinforcement powerfully strengthens avoidance behaviour. Each successful escape teaches the brain: "Avoidance works. Do it again." Without intervention, this pattern self-perpetuates.
The Good News
Neuroplasticity means this wiring can change. Systematic desensitisation with sensory accommodations creates new neural pathways. The brain can learn: "Hand dryer is loud — AND I am safe." This learning happens through accumulated successful exposures.
Frontiers in Integrative Neuroscience (2020): DOI: 10.3389/fnint.2020.556660

Your Child Is Here. Here Is Where We're Heading.
Age 2
Home toilet established
Age 3
Familiar away-from-home toilets (grandma's)
Age 4–5
Typical public restroom comfort develops
Age 6–8
Community access with tools if needed
Age 9–12+
Independent, flexible public toileting
Your child may currently be in the "home-only toileting / public avoidance" zone — this is where E-504 begins. Most children with sensory sensitivities or anxiety do not naturally habituate, and a single negative experience can create lasting fear associations that actively prevent developmental progression.
Typical toilet training involves gradual environmental expansion: home → familiar away-from-home toilets → novel public restrooms. Children with sensory processing differences, anxiety disorders, or autism may require structured support to make this progression. With systematic desensitisation and sensory accommodations, most children reach community-access toileting within 4–16 weeks.
WHO Care for Child Development Package 2023 | PMC9978394 | Padmanabha et al., Indian J Pediatr 2019: DOI:10.1007/s12098-018-2747-4

Clinically Validated. Home-Applicable. Parent-Proven.
🛡️ Level I Evidence
Systematic Review + Meta-Analysis
16 Studies · 2013–2023 · PRISMA Confirmed
Key Finding: Sensory integration intervention meets evidence-based practice criteria for children with ASD, with significant improvements in sensory processing, adaptive behaviour, and social skills.
Study | Finding | Reference |
PRISMA Systematic Review (2024) | Sensory integration intervention is evidence-based for ASD | PMC11506176 |
Meta-analysis, World J Clin Cases (2024) | Significant improvement in sensory processing, social skills, motor skills | PMC10955541 |
Indian RCT — Padmanabha et al. (2019) | Home-based sensory interventions show significant outcomes | DOI:10.1007/s12098-018-2747-4 |
WHO NCF Household-Based Interventions | Context-specific, parent-administered interventions effective across 54 LMICs | PMC9978394 |
NCAEP EBP Report (2020) | Visual supports, social stories, reinforcement — all EBP for autism | NCAEP 2020 |
"Deeper reading for the curious parent: Search PMC11506176 on PubMed.gov"

Public Restroom Desensitisation Protocol
Parent Alias: "The Freedom Kit"
What It Is
A multi-sensory accommodation and systematic desensitisation protocol that reduces avoidance of public restrooms in children with sensory processing differences, anxiety disorders, or autism.
The technique combines environmental modifications (blocking sensory triggers), portable accommodations (tools the child carries), cognitive preparation (social stories, visual timers), and graduated exposure with reinforcement — transforming public restrooms from threat environments into manageable, eventually comfortable spaces.
Protocol At a Glance
- 📁 Domain: ADL & Self-Care (Domain E)
- 🎯 Category: Toileting Independence
- 👶 Ages: 3–12
- ⏱️ Sessions: 5–30 minutes
- 🔁 Frequency: Daily practice during desensitisation phase
- 📍 Settings: Home bathroom (practice) → Public restrooms (graduated exposure)
Sensory Protection
Visual Supports
Reinforcement
Anxiety Management

The Brain Doesn't Organise by Therapy Type. Neither Does This Technique.
Occupational Therapy (Primary Lead)
OTs address the sensory integration basis: auditory over-responsivity, tactile defensiveness, olfactory sensitivity, and interoception difficulties. OT designs the desensitisation hierarchy and selects sensory accommodation tools.
ABA / BCBA (Behaviour Architecture)
BCBAs design the reinforcement system — breaking the avoidance cycle through graduated exposure, positive reinforcement schedules, and functional behaviour assessment to identify specific maintaining conditions.
Speech-Language Pathology
SLPs create social stories and visual sequence cards. For non-verbal or minimally verbal children, SLPs develop AAC supports that allow the child to signal needs and distress during exposure.
Special Education
SpEd professionals coordinate school-based accommodations: private bathroom access, permission for sensory tools, scheduled toilet times. Generalisation from home to school settings is a SpEd speciality.
NeuroDevelopmental Paediatrics
NeuroDev doctors assess for underlying anxiety disorders, check for medical complications from chronic holding (UTIs, bladder dysfunction, constipation), and determine if pharmacological support for severe anxiety is warranted.
"Five disciplines. One integrated protocol. Because your child's nervous system doesn't divide itself by therapy type."
Your Complete Public Restroom Toolkit
Nine materials. One manageable challenge. Here is everything your child needs — from sensory protection to emotional anchoring to motivation.
🎧 1. Noise-Canceling Headphones
Block 80–90 dB hand dryers and echoing sounds
🚽 2. Auto-Flush Sensor Covers
Child controls when flush occurs — no surprises
🪑 3. Portable Seat Covers
Familiar, clean surface on every toilet
⏱️ 4. Visual Countdown Timers
Show child exactly how long exposure will last
📖 5. Social Stories
Mental rehearsal before physical exposure
🌿 6. Calming Scent Products
Familiar pleasant smell masks overwhelming odours
🧸 7. Comfort Items
Brings emotional security into the challenging space
🚿 8. Travel Potty / Seat Insert
Consistent toilet experience regardless of location
⭐ 9. Reward Systems
Creates competing motivation that overrides avoidance
Starter Kit: ₹1,300–6,800 total for essentials. Minimum viable kit: Headphones + Sensor covers + Social story + Reward chart. Full toolkit: All 9 materials.

Material 1: Noise-Canceling Headphones / Ear Defenders
Why This Material
Hand dryers in public restrooms produce 80–90 dB of noise — equivalent to a motorcycle at close range. For children with auditory over-responsivity, this sound does not simply seem loud; it registers as a genuine threat signal in the amygdala. Noise-canceling headphones reduce this input to manageable levels, allowing the child's nervous system to remain regulated during exposure.
Pinnacle Recommends: NRR 20+ dB, over-ear, kid-sized. Look for lightweight, snug-fit designs the child can put on independently.
Practical Details
- Canon Category: Sensory Protection — Auditory
- Price Range: ₹800–4,000
- Search on Amazon.in: "kids noise canceling headphones ear defenders"
- Budget tip: Construction foam ear plugs (₹50) offer low NRR but are a valid starting point
- Key principle: Put headphones on before approaching the restroom, when the child is still calm
Pro Tip
Practice wearing headphones during preferred activities — watching TV, car rides — before bathroom exposure. The headphones become associated with good experiences first, removing resistance.

Material 2: Automatic Flush Toilet Sensor Covers
Why This Material
The unpredictable automatic flush is frequently the single most traumatising element of a public restroom experience for sensory-sensitive children. Unlike hand dryers, the flush is sudden, close, and impossible to predict. A sensor cover blocks the infrared beam, ensuring the toilet will not flush until the child (or parent) decides — returning control to the child at a moment when control is everything.
Practical Details
- Canon Category: Environmental Control — Toileting
- Price Range: ₹200–600
- Search on Amazon.in: "automatic toilet flush sensor cover sticker"
- Budget option: Post-it notes work as emergency covers — check they fully cover the sensor
- Pro tip: Carry 3+ covers per outing. Some restroom sensors are positioned on the tank side rather than the back — always check placement before the child enters the stall.

Material 3: Portable Toilet Seat Covers / Disposable Seat Liners
Why This Material
Tactile defensiveness — heightened sensitivity to unfamiliar textures — is common in children with sensory processing differences. A cold, hard, unfamiliar public toilet seat can be an overwhelming tactile trigger. Portable seat covers provide a consistent, familiar surface that reduces this barrier and helps the child focus on the exposure rather than the sensation beneath them.
Reusable fabric covers provide a more consistent tactile experience than paper equivalents and can be washed and carried in the toolkit bag.
Practical Details
- Canon Category: Sensory Protection — Tactile
- Price Range: ₹150–800
- Search on Amazon.in: "disposable toilet seat cover travel"
- DIY alternative: Layered toilet paper arranged on seat, or parent's jacket placed temporarily
- Key insight: The therapeutic principle is identical whether commercial or DIY — the brain responds to the familiar texture, not the brand
Material 4: Visual Countdown Timers
Why This Material
One of the primary drivers of public restroom anxiety is unpredictability: the child does not know how long the ordeal will last. A visual timer transforms an open-ended, overwhelming experience into a bounded, predictable one. When the child can see the time reducing, they can tolerate the discomfort — because the end is visible. This is the same principle used in exposure therapy for adults: knowing the duration makes endurance possible.
Practical Details
- Canon Category: Visual Supports — Timing
- Price Range: ₹200–1,200
- Search on Amazon.in: "time timer visual countdown kids"
- Free alternative: Time Timer app on phone (visual mode, no alarm sound)
- Sand timers work offline and are durable in a kit bag
- Critical: Set duration BEFORE child enters. Never extend the timer mid-session without child's agreement.

Material 5: Social Stories / Visual Sequence Cards — Public Restrooms
Why This Material
Social stories — short, first-person narratives that describe a situation, the child's likely feelings, and what to do — allow the child to rehearse the experience cognitively before encountering it physically. This mental rehearsal reduces novelty anxiety and gives the child a framework for interpreting their own responses.
The most effective social stories are custom photo-based, using images of the child's actual toolkit and real restroom environments they will encounter. A story created with your phone camera and printed at ₹5/page at a local shop is more powerful than any commercially produced book.
Practical Details
- Canon Category: Visual Supports — Narrative
- Price Range: ₹100–500 (commercial) or ₹20–50 DIY
- Search on Amazon.in: "social story autism bathroom visual schedule"
- DIY method: Photograph your restroom tools + a public restroom, print on phone, laminate at ₹5/page
- SLP coordination: Ask your speech-language pathologist to help script the narrative for your child's communication level
- Update the story as new levels are achieved — add a "I did it!" page with a photo

Material 6: Calming Scent Products / Portable Aromatherapy
Why This Material
The olfactory system has a direct, rapid pathway to the limbic system — the brain's emotional processing centre. Industrial cleaning chemicals and restroom odours can trigger immediate threat responses in children with olfactory sensitivity. A familiar, preferred scent applied to the child's wrist or clothing creates a portable olfactory anchor — a signal of safety that the child controls and can access by simply raising their wrist.
Importantly, the child should choose their preferred scent. Ownership over the calming tool dramatically improves compliance.
Practical Details
- Canon Category: Sensory Regulation — Olfactory
- Price Range: ₹150–600
- Search on Amazon.in: "essential oil rollerball lavender kids calming"
- DIY alternative: Small amount of preferred lotion on child's wrist, or parent's familiar perfume on a cloth
- Safety: Dilute to 1% for children under 12. Always test for allergic reaction on a small skin area first.

Material 7: Portable Comfort Items / Transitional Objects
Why This Material
Transitional objects — small, beloved items the child carries — serve as emotional anchors. They are a physical connection to the safety of home, brought into the threatening environment. The psychological mechanism is identical to why adults keep photos of loved ones in difficult situations: a tangible reminder that safety and connection exist.
Any small object the child loves qualifies: a smooth pebble, a tiny figurine, a piece of familiar fabric. The child must choose it themselves — imposed comfort objects do not carry the same emotional weight.
Practical Details
- Canon Category: Anxiety Management — Emotional Anchoring
- Price Range: ₹100–500 (or ₹0 — any object already loved)
- Search on Amazon.in: "pocket fidget toy squeeze stress ball kids"
- DIY option: Smooth pebble from garden, piece of favourite fabric, small toy already owned
- Key script: "Your [toy name] is coming with you." Place in child's hand or pocket before approaching the restroom.

Material 8: Travel Potty / Portable Toilet Seat Insert
Why This Material
For children in the early phases of the desensitisation hierarchy, a portable toilet seat insert or foldable travel potty creates a consistent, familiar toilet experience regardless of location. This bridges the gap between the child's comfortable home toilet and the completely unfamiliar public restroom fixture. It is particularly useful during the Level 4–5 phase, when the child is beginning to approach and sit on the toilet.
This tool can be gradually faded as tolerance builds — its purpose is transition, not permanent dependence.
Practical Details
- Canon Category: Adaptive Equipment — Toileting
- Price Range: ₹500–2,500
- Search on Amazon.in: "foldable travel potty portable toilet seat insert"
- DIY desensitisation: During home practice phase, move the child's home potty seat to the bathroom door, then progressively into the bathroom, before introducing the travel version in public
- Fading plan: Once Level 6 is achieved consistently, gently introduce sitting on the public seat directly with just the disposable cover

Material 9: Reward Systems / Sticker Charts / Token Economy
Why This Material
Avoidance is powerfully reinforced by immediate relief. To compete with this, the reward system must provide equally immediate and tangible positive reinforcement for approach behaviour. A sticker chart, token jar, or points system creates a visible, accumulating record of courage that motivates the child to continue approaching rather than avoiding.
Critical principle: Reward the attempt and the exposure — not only successful toilet use. A child who walked to the door deserves a sticker. A child who entered the stall deserves a sticker. Progress is built on celebrated attempts.
Practical Details
- Canon Category: Reinforcement — Motivation
- Price Range: ₹100–400
- Search on Amazon.in: "sticker reward chart children behavior"
- DIY alternative: Handwritten chart, small pieces of coloured paper as tokens, verbal praise + privilege (extra 5 min screen time)
- Token economies: Tokens accumulate toward a larger child-chosen reward — increases motivation for multi-session effort
- Timing: Reinforce within 3 seconds of the desired behaviour. Timing matters more than magnitude.

Every Family Can Start Today — Regardless of Budget
WHO/UNICEF Equity Principle: No child should be denied therapeutic access due to material cost.
Material | Buy Option | ₹0 DIY / Household Alternative |
Noise Protection | Kids ear defenders ₹800–2,000 | Cotton balls in ears · Construction foam ear plugs ₹50 · Parent's hands over child's ears during hand dryer |
Sensor Covers | Commercial sensor stickers ₹200–600 | Post-it notes · Small square of opaque tape · Business card + rubber band |
Seat Covers | Disposable paper covers ₹150–500 | Layered toilet paper on seat · Parent's jacket placed temporarily |
Visual Timer | Time Timer device ₹500–1,200 | Free timer app on phone (visual only, no alarm) · Parent counts down aloud ("10… 9… 8…") |
Social Story | Printed books ₹200–500 | DIY: Photograph tools + restroom, print on phone, laminate at ₹5/page |
Calming Scent | Essential oil rollerball ₹200–500 | Preferred lotion on child's wrist · Parent's familiar fragrance on cloth |
Comfort Object | Fidget toy ₹100–300 | Any small beloved toy already owned · Smooth pebble · Piece of familiar fabric |
Travel Potty | Foldable travel potty ₹500–2,500 | Child's home potty seat moved gradually into bathroom during practice phase |
Reward Chart | Printed sticker chart ₹100–300 | Handwritten chart · Coloured paper tokens · Verbal praise + screen time privilege |
The therapeutic principle is identical whether you use a ₹3,000 ear defender or a ₹50 foam ear plug: reduce auditory input to manageable levels. The brain doesn't care about the brand — it cares about the decibels reduced.
PMC9978394 — WHO NCF CCD Package: household-material interventions validated in 54 LMICs · DOI:10.1007/s12098-018-2747-4 — Indian RCT confirming home-based intervention efficacy

Safety First: Read Before You Proceed. Every Time.
🔴 STOP — Do Not Proceed If:
- Child is in acute medical distress (fever, UTI symptoms, abdominal pain — seek medical care first)
- Child has had recent severe trauma related to restrooms (abuse-related association — refer to psychologist before any restroom exposure work)
- Child is currently in meltdown or extreme dysregulation — wait until baseline is restored
- You plan to physically force the child — forced exposure is contraindicated and will worsen avoidance
- Child shows signs of urinary retention causing pain — medical emergency, see doctor today
🟡 MODIFY — Proceed With Caution If:
- Child has current constipation or digestive discomfort — address medically first
- Child is in an unfamiliar location for the first time — start with quieter, single-occupancy family restrooms
- Child has significant anxiety disorder diagnosis — involve psychologist before proceeding
- Using essential oils — dilute to 1% for children under 12; test for allergic reaction first
🟢 PROCEED — When:
- Child is in regulated baseline state (not hungry, not overtired, not dysregulated)
- All tools are prepared and accessible before approaching the restroom
- You have a 15+ minute time buffer — not rushing
- Child has been prepared with the social story
- You are in a calm state yourself (children regulate to their parent's nervous system)
Medical Note: Children with prolonged holding history may have developed UTIs, bladder dysfunction, or constipation. If your child reports pain when toileting, consult a paediatrician before starting this protocol. NeuroDev Paediatrics at Pinnacle can assess via teleconsultation: 9100 181 181.

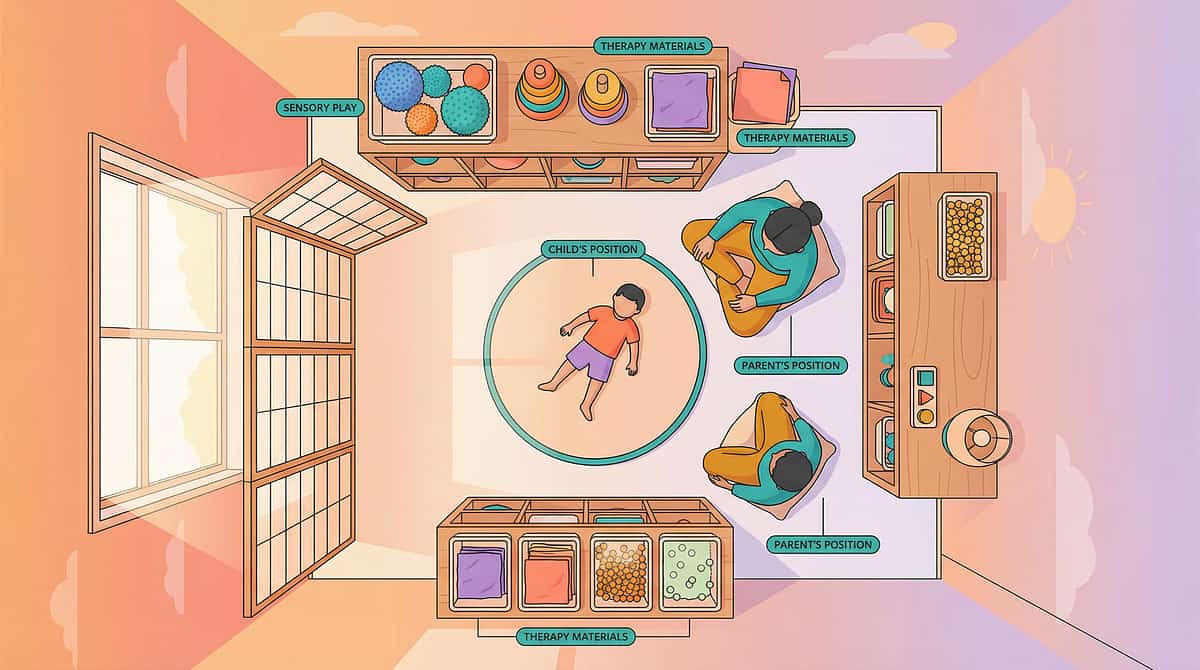
Spatial Precision Prevents 80% of Session Failures. Set Up Before You Invite.
1
Tools Bag Ready
All materials assembled in one bag before approaching bathroom. Child can see the bag — its visibility reduces uncertainty.
2
Timer Positioned
Visual timer placed where child can see it throughout the entire session. Test it once before inviting the child.
3
Headphones On Early
On during approach — when still calm — not at the restroom door. Being calm when headphones go on creates better association.
4
Sensor Covered First
Parent covers auto-flush sensor before child enters stall. This step happens before, not during the child's entry.
5
Seat Cover Applied
In place before child sits. Seat cover is ready, not introduced at the moment of sitting.
6
Exit Clear & Reward Visible
Child can see the door is not locked. Sticker chart or token jar visible. Never physically block exit — perceived escape route reduces anxiety.
Environmental checklist: Single-occupancy family restroom when possible · Manageable lighting · 15+ minute time buffer · Child is not at maximum bladder urgency · Your phone is silenced.

The 60-Second Readiness Check — Before Every Single Session
Readiness Checklist
- Child has eaten in the last 2 hours (hunger amplifies dysregulation)
- Child is not overtired (nap completed if applicable)
- No meltdown in the past 30 minutes
- No signs of illness (fever, tummy ache, cold)
- Child is not at maximum bladder urgency
- Your emotional state is calm (co-regulation anchors theirs)
- All tools are in the bag and ready
Decision Gate
- All 7 checked 🟢 GO — Proceed to Step 1: The Invitation
- 5–6 checked 🟡 MODIFY — Use shorter timer, lower demand (just enter and exit, no toilet use required)
- 4 or fewer 🔴 POSTPONE — 15-min calming activity first: proprioceptive input (jumping, wall push-ups), then re-assess
If Postponing
Do: Heavy work (carrying groceries, wall push-ups), deep pressure, preferred sensory activity. Re-assess. If regulated → Go. If not → Reschedule entirely. Never push through extreme dysregulation.
Step 1: The Invitation
Step 1 of 6
"Hey, want to do our brave bathroom practice? You get your headphones, I have your timer, and there's a sticker waiting. You decide when we're done."
Why This Wording Works
- "Brave" — names the courage, not the fear
- "Your headphones" — the tools belong to them, not imposed
- "You decide when we're done" — restores sense of control (core anxiety reducer)
- "A sticker waiting" — activates approach motivation before the request registers as threat
Body Language Guidance
- Get to child's eye level
- Neutral/warm expression — not tense, they will read your anxiety
- Casual, not rushed
- Tools bag visible but not thrust at them
What Acceptance Looks Like
- Verbal "yes" or movement toward the bag
- Goes quiet and becomes compliant (some children accept silently)
- Reaches for headphones independently
Resistance and How to Modify
- "No" or physical pull-away → Reduce the ask: "How about we just walk to the bathroom door? You don't have to go in."
- Ignoring → Try 5 minutes later; do a preferred activity together first for pairing
- Meltdown beginning → Postpone (return to readiness check)
Timing: 30–60 seconds for invitation. If not accepted in 2 minutes, try the modified ask.

Step 2: The Engagement
Step 2 of 6
"Headphones on first — good. Here's your timer, I'm setting it for [30 seconds / 1 minute / 2 minutes]. Here's [comfort object]. Now we walk together."
🎧 Headphones
Child puts them on independently if able; assist if needed. Say: "Now all the loud sounds are smaller."
⏱️ Timer
Show child the time remaining. Say: "When this runs out, we're done. You can watch it the whole time."
🚽 Sensor Cover
Parent applies before child enters stall, discreetly. Say: "I covered the flusher. It won't flush until we say so."
🧸 Comfort Object
Place in child's hand or pocket. Say: "Your [toy name] is coming with you."
Immediate reinforcement cue: When child puts on headphones: "Yes! Brave choice. Headphones on." Specific, enthusiastic, within 3 seconds. Timing: 1–3 minutes from headphones on to approaching bathroom.

Step 3: The Therapeutic Action — Graduated Exposure Hierarchy
Step 3 of 6
Do not skip levels. Do not push to the next level until the current level is comfortable across 3+ sessions.
Level 1 — Proximity
Walk to the hallway outside the public restroom. Pause. Timer 30 seconds. Headphones on. Exit. Celebrate. That is the whole session for complete refusers.
Level 2 — Threshold
Walk to the restroom entrance. Child can see inside but does not enter. Timer: 30–60 seconds. Headphones on. Exit. Celebrate.
Level 3 — Entry
Enter the restroom. Stand near the entrance — do not approach a stall. Timer: 30–60 seconds. Headphones on. Exit. Celebrate.
Level 4 — Stall Approach
Walk to a stall. Touch the door. Timer: 1 minute. All tools deployed. No sitting required. Exit. Celebrate.
Level 5 — Stall Entry
Enter stall. Close door. Sit on toilet fully clothed — no pants-down requirement. Timer: 1–2 minutes. All tools deployed. Exit. Celebrate.
Level 6 — Use
Enter stall, all tools deployed, use toilet. Exit. Major celebration.
Level 7 — Fading Accommodations
Gradually over weeks: timer duration decreases, sensor cover may be removed, headphones used selectively. This is months-long work — do not rush.
PMC10955541 — 40-minute sessions showed max efficacy; home-based shorter sessions acceptable · Systematic desensitisation literature: graduated exposure hierarchy for specific phobias

Step 4: Repeat and Vary
Step 4 of 6
The Dosage Principle
3 good repetitions at a given level > 10 forced repetitions.
- Frequency: Daily practice in home bathroom + weekly real-world exposure attempts
- Duration: 5–15 minutes per session total
- Timeline: Expect 4–16 weeks to move through the full hierarchy
When to Increase Level
Child has completed current level 3+ times with distress rating ≤2 → ready for next level.
Variation Options
- Variation A — Different Restrooms: Home bathroom (daily) → familiar single-occupancy family restroom → quieter public restrooms (libraries > malls > airports)
- Variation B — Tool Fading: After 3 consistent successful sessions at a level, try removing one tool. Re-introduce immediately without comment if distress spikes.
- Variation C — Child Leads: At Level 4+, allow: "You decide when we go in." Autonomy accelerates habituation.
- Variation D — Imaginal Rehearsal: Read social story before every real-world attempt. Add new pages as levels are achieved.
Satiation indicators — stop if you see: Child's engagement drops significantly and does not recover · Child actively refuses subsequent repetitions · Distress is not reducing across the session (distress should reduce within session per exposure theory).

Step 5: Reinforce and Celebrate
Step 5 of 6
Reinforce within 3 seconds of the desired behaviour. Timing matters more than magnitude.
The Reinforcement Script
- Level 1: "You walked to the bathroom! That was SO brave. Sticker goes RIGHT here."
- Level 3: "You went INSIDE the bathroom. That is huge. I'm proud of you."
- Level 6: "You used the public toilet. You did it. [Child's name], that was incredible."
Reinforce the Attempt, Not Only the Success
If child attempted Level 3 but distress spiked and you dropped to Level 2: reinforce the attempt. "You tried to go inside. That's brave. Sticker."
Reinforcement Menu
- 🌟 Sticker on chart immediately
- 🎯 Token toward bigger reward
- 👏 High-five + specific verbal praise
- 📱 5 extra minutes of preferred activity
- 🍬 Small edible reward (if appropriate)
- 🧸 Special privilege ("pick the next TV show")
Never:
- Express disappointment at any level of completion
- Compare to siblings or other children
- Withhold reinforcement as punishment
- Say "you almost did it" as the only feedback

Step 6: The Cool-Down
Step 6 of 6
No session ends abruptly. Transitions are therapeutic.
1
Transition Warning
Say 2 minutes before ending: "Two more, then all done. Two more times. Then we're finished and you get [reward]." At 1 minute: "One more time." At end: "All done! Amazing work."
2
Pack Away Together
Child participates in returning headphones to bag. Say: "You're the keeper of the headphones." Ownership of tools continues outside the session.
3
Hand Washing
With preferred soap — this becomes part of the restroom success routine, not a sensory chore.
4
Brief Walk Away
Physical transition out of the anxiety zone. Deliver reward immediately upon exiting restroom area.
5
Neutral Conversation
Talk about anything other than the session. Do not debrief verbally ("that was hard") — redirecting forward prevents rehearsal of difficulty.
If child resists ending: This is a good sign! Maintain session structure. Use the timer: "Timer says all done. Timer doesn't lie." Provide reinforcement immediately. Allow 5 minutes of quiet preferred activity before entering a stimulating environment.
Capture the Data: 60 Seconds. Three Numbers. Right Now.
Why This Data Matters
Three weeks of session data will show your therapist exactly where the exposure hierarchy is working and where it is stalling. Data captured within 60 seconds of session end is 3× more accurate than end-of-day recall. This data enables protocol adaptation and drives GPT-OS® personalised recommendations.
Offline Option
Download the E-504 Session Log PDF — print weekly, file in therapy binder. One page per week, simple tick-box format.
Immediate Post-Session Tracker
- Session Date + Location (home / family restroom / mall / other)
- Level Attempted (1–7) + Level Completed (1–7)
- Child Distress Rating (1=calm, 5=extreme)
- Duration in restroom (seconds/minutes)
- Tools used: Headphones · Sensor cover · Seat cover · Timer · Story · Scent · Comfort item · Travel potty · Reward chart
- Optional notes

When It's Not Working: Every Stall. Every Problem. We've Seen It Before.
Problem 1: Child Refuses to Put On Headphones
Try different styles: over-ear vs. ear plugs vs. construction earmuffs. Let child choose. Practice wearing headphones during preferred activities (TV, car rides) before bathroom exposure — so headphones become associated with good experiences first.
Problem 2: Sensor Cover Falls Off Mid-Session
Use sticky tape to secure it. Carry 3+ covers per outing. Apply cover before child enters stall. Check sensor placement — some restrooms have sensors on the tank side rather than the back.
Problem 3: Compliant at Home, Refuses Same Level in Public
This is expected. Home and public restrooms are different stimuli. Return to Level 1 in the public setting, even if the child is at Level 5 at home. Build up each new location from Level 1. Generalisation eventually occurs.
Problem 4: Progress Is Extremely Slow — Weeks at Same Level
Check: Is the reward sufficiently motivating? Is the current level actually at the child's tolerance ceiling? Consider consulting an OT for a sensory profile assessment. Some children need additional sensory processing work before restroom desensitisation can proceed.
Problem 5: Child Was Progressing Then Regressed
Regression is normal, especially after illness, major life change, or a single bad experience. Return to the previous comfortable level without comment. Regression is not failure — it is the exposure hierarchy requesting more time at a given step.
Problem 6: Family Members Undermine the Protocol
Consistency across caregivers is essential. Share the Family Guide (Card 37). One forced session can erase weeks of progress. Use the school communication template to align teachers.
Adapt to Your Child: Every Sensory Profile Is Unique
For the Sensory Avoider (Over-Responsive)
- Start at Level 1 regardless of age
- Maximise all accommodations (highest-NRR headphones available)
- Never enter a busy restroom — start with single-occupancy family restrooms only
- Timer: start at 15–30 seconds maximum
- Keep real-world sessions rare initially (1× weekly), more frequent at home
For the Sensory Seeker (Under-Responsive)
- May struggle with interoception — not sensing need to toilet until urgent
- Focus on body awareness + scheduled toileting + timed voiding
- Exposure hierarchy may proceed faster
- Add proprioceptive input before sessions (jumping, wall push-ups)
Age-Based Modifications
- Ages 3–5: Keep entirely play-based. Toy goes to the bathroom too. Social story is a picture book. Reward is immediate small treat.
- Ages 6–8: Child can begin naming their fear and using the timer independently.
- Ages 9–12: Child can participate in designing the exposure hierarchy. Ownership accelerates progress.
Difficulty Calibration
Start at the level where the child is currently comfortable — then add one step. Not two. Not the level you wish they were at. The just-right challenge principle: enough stretch to build tolerance, not enough to trigger shutdown.

Weeks 1–2: Progress Is Measured in Seconds, Not Success
ACT IV — The Progress Arc
✅ You May See
- Reduced resistance to putting on headphones at home
- Child tolerates looking at social story without distress
- Child walks 3 steps closer to the restroom entrance than last week
- Decreased distress duration when an exposure attempt does not succeed
❌ Do Not Expect Yet
- Child using a public restroom
- Absence of distress
- Generalisation to multiple locations
Week 1–2 is the hardest phase. You are building trust and introducing tools into a child who has been avoiding this challenge for months or years. You are not failing if this phase is slow. You are doing exactly what the protocol requires. If your child has had 3+ positive tool-introduction sessions, you are ready for Weeks 3–4.
PMC11506176 — Sensory integration outcomes emerge across 8–12 week timelines; early-phase indicators focus on tolerance, not mastery

Weeks 3–4: These Are the Real Indicators of Progress
🧠 Child Asks for Headphones Before You Offer Them
They have associated headphones with safety, not imposition. This is a significant shift in neural association.
🧠 Child Pauses at the Restroom Entrance Rather Than Pulling Away
Fight-or-flight activation is reducing. Curiosity and tolerance are beginning to replace immediate avoidance.
🧠 Child Reads Social Story Independently or Requests It
Cognitive preparation is being internalised. The child is using tools proactively rather than reactively.
🧠 Distress Reduces More Quickly Within a Session
Habituation is occurring. The nervous system is learning: "I can tolerate this." This is measurable neuroplasticity in real time.
🧠 Child Mentions Something Specific About the Restroom
Verbal processing indicates reduced avoidance. When children can talk about the feared stimulus, they are processing it — a healthy sign.
When to increase level: Child has completed current level 3+ times with distress rating ≤2 → ready for next level. Not before.
Weeks 5–8: This Is Where Families Feel the Change
Level 6 Achieved
Child uses a public restroom in a familiar setting for the first time.
Spontaneous Initiation
Child requests to go to the bathroom during an outing — without prompting.
Second Location
Child begins generalising to a second public restroom location.
Family Milestone
A full restaurant visit or mall trip completed without bathroom crisis.
"We went to a restaurant and he used the bathroom there for the first time ever. He had his headphones and the sensor cover. He was quick, but he did it. I cried in the parking lot." — Parent, Pinnacle Network (illustrative; outcomes vary)
What to do at this stage: Document the first Level 6 success with a photo. Begin practising at a second location. Gently begin discussing fading one accommodation (child's choice). Maintain daily home practice.
Every Level Crossed Is a Neural Pathway Earned. Celebrate Every One.
1
Headphones On ✓
Brave first step: tools accepted
2
Walked to the Door ✓
Proximity achieved
3
Went Inside ✓
Entry level mastered
4
Found a Stall ✓
Stall approach achieved
5
Sat Down ✓
Stall entry mastered
6
First Public Use ✓
Level 6 — the breakthrough
7
Second Location ✓
Generalisation beginning
8
On My Own ✓
Independence achieved
You have been carrying this challenge for a long time. Every session you ran, every tool you packed, every time you stayed calm when you were internally panicking — that was you being your child's nervous system co-regulator. Their progress is yours too.

Know When to Escalate. The Protocol Is Powerful. A Therapist Is More Powerful.
🚨 Call Your Therapist or Pinnacle Helpline (9100 181 181) If:
- No progress after 8+ weeks of consistent daily practice
- Child experiencing medical complications from holding (UTI symptoms, pain, constipation)
- Child's anxiety is generalising beyond bathrooms to other settings
- Child shows signs of significant anxiety disorder (school refusal, eating changes, sleep disruption)
- You suspect OCD contamination patterns (extensive ritual washing, cannot tolerate any uncertainty)
- Exposure sessions consistently escalate distress rather than reducing it within 10 minutes
- Child has disclosed something distressing about a restroom experience
What a Therapist Can Add
- OT: Comprehensive Sensory Profile assessment
- BCBA: Functional Behaviour Assessment
- Psychologist: Anxiety disorder evaluation and CBT components
- NeuroDev: Medical assessment + medication consideration if severe
📞Free National Helpline: 9100 181 181 — Available 24×7 in 16+ languages. Free. Immediate. Staffed by trained Pinnacle consortium professionals. pinnacleblooms.org/find-a-center

You Already Have Some of These Materials. Here's What to Try Next.
E-502: Toilet Training Resistance
Difficulty: Intro | Materials: Visual schedules, rewards
You own: Reward chart ✓

E-503: Nighttime Bedwetting Support
Difficulty: Core | Materials: Moisture alarm, visual schedule
New materials needed

E-505: Hair Washing Battles
Difficulty: Core | Materials: Visual timer, comfort items
You own: Timer ✓ Comfort item ✓

A-112: Auditory Sensitivity Management
Difficulty: Advanced | Materials: Noise-canceling headphones
You own: Headphones ✓
✅If you have completed E-504's toolkit, you already own materials for 4 of the 6 related techniques above. Your investment goes further than one challenge.

Families Who Were Where You Are. Now Where You Want to Be.
ACT V — Community & Ecosystem
"We couldn't go anywhere. My son would hold it for 6+ hours rather than use a public toilet. The automatic flushers terrified him. We started with sensor covers and headphones — just those two things. Then social stories, quieter restrooms, and a reward chart. It took four months, but now he uses public restrooms. Our world opened up again."
— Parent, Pinnacle Network, Hyderabad
"My daughter is 8. She was still using the car as a portable toilet when we were out. When we added the portable seat cover and the lavender scent bracelet — something clicked. She went from zero to using family restrooms within 6 weeks. The smell was the key for her."
— Parent, Pinnacle Network, Bengaluru
"Our OT told us to stop focusing on the toilet and start focusing on the tools. The moment we gave our son control — his headphones, his sensor cover, his timer — the refusal changed. He felt like HE was managing it. That was the turning point."
— Parent, Pinnacle Network, Mumbai
Illustrative testimonials. Individual outcomes vary. Statistics represent aggregate outcomes across Pinnacle Blooms Network®.

Professional Support Is Near You — 70+ Pinnacle Centres Across India
Services Available for E-504
- 🦾 Occupational Therapy (Sensory Integration) — All centres
- 🧠 ABA/BCBA (Behavioural Desensitisation) — All centres
- 🧬 NeuroDevelopmental Paediatrics — Select centres
- 💬 SLP (Social story development) — All centres
- 📱 Teleconsultation — Anywhere in India, 9100 181 181
Book Your Appointment
Pinnacle operating data: 70+ centres, 20M+ sessions, 97%+ measured improvement rate, serving families from 70+ countries.

See the Materials in Action
E-504 — 9 Materials That Help With Public Restroom Refusal
The Pinnacle Blooms Network® therapy reel that accompanies this technique page demonstrates all 9 materials in a ~75-second guided walkthrough: headphones on approach, sensor cover placement, visual timer use during practice, and reward delivery after successful exposure.
- 📁 ADL & Self-Care Series · Episode 504
- 🏷️ Domain E · ADL + Sensory + Anxiety Management
- 👤 Presented by: Pinnacle OT + ABA Consortium
- ⏱️ Duration: ~75 seconds
NCAEP 2020: Video modelling is evidence-based practice for autism · Multi-modal learning improves parent skill acquisition
Preview of 9 materials that help with public restroom refusal Therapy Material
Below is a visual preview of 9 materials that help with public restroom refusal therapy material. The pages shown help educators, therapists, and caregivers understand the structure and content of the resource before use. Materials should be used under appropriate professional guidance.




















Share this resource
Help others discover thisLink copied!

The Pinnacle Promise
"From fear to mastery. One technique at a time."
Pinnacle Blooms Network® is India's largest multi-disciplinary paediatric therapy consortium — 70+ centres, 20M+ 1:1 therapy sessions, 97%+ measured improvement rate, serving families from 70+ countries through the GPT-OS® platform. This technique page is part of a library of 70,000+ intervention techniques designed to transform every home into a 24×7, personalised, multi-sensory, multi-disciplinary paediatric therapy environment.
This content is produced by the Pinnacle Blooms Consortium — Occupational Therapists, Speech-Language Pathologists, ABA/BCBA Therapists, Special Educators, NeuroDevelopmental Paediatricians, Clinical Research Officers, Mothers, Fathers, Families, and Caregivers — guided by WHO, UNICEF, and international evidence-based practice standards.
⚠️Medical Disclaimer: This content is educational. It does not replace individualised assessment and intervention from licensed occupational therapists, behavioural therapists, or medical professionals. Persistent public restroom refusal may require comprehensive evaluation for sensory processing differences, anxiety disorders, or medical complications from chronic holding. Seek professional help for persistent symptoms or significant distress. Individual results may vary. Statistics represent aggregate outcomes across the Pinnacle Blooms Network®.
© 2025 Pinnacle Blooms Network®, unit of Bharath Healthcare Laboratories Pvt. Ltd. All rights reserved.
CIN: U74999TG2016PTC113063 | DPIIT: DIPP8651 (Govt. of India) | MSME: TS20F0009606 | GSTIN: 36AAGCB9722P1Z2
techniques.pinnacleblooms.org/adl-self-care/public-restroom-refusal-E-504
