
9 Materials That Help With Fecal Smearing Prevention
A clinically validated, multi-material protocol for families and therapists navigating scatolia in children with autism and developmental differences. Evidence-based. Home-applicable. Consortium-reviewed.
E-508
Toileting & Hygiene Series
Age 2–14 Years

ACT I — THE EMOTIONAL ENTRY
It's 6 AM. You walk into their room and you already know.
The smell hits you before you reach the door. Again. You're already mentally calculating the cleanup, the laundry, whether you'll make it to work on time — before you've even said good morning.
You are not failing. Your child's nervous system is speaking. And now, someone is finally listening.
This is Technique E-508 of the Pinnacle Blooms Toileting, Hygiene & Self-Care Series — a resource built specifically for this moment, this challenge, and this family. Consortium-led by ABA/BCBA, Occupational Therapy, and NeuroDev Pediatrics.
📞 FREE National Autism Helpline: 9100 181 181 | 16+ languages | 24×7 | Pinnacle Blooms Consortium®

CARD 02 — YOU ARE NOT ALONE
You Are Among Millions. This Has a Name. This Has Solutions.
Scatolia — the clinical term for fecal smearing — is among the most under-discussed behavioral challenges in pediatric development. Not because it is rare, but because the stigma keeps families isolated. You cannot discuss this at a school gate. You search the internet and find almost nothing useful.
1 in 44
Children with Autism in India
INCLEN, 2022 — Fecal smearing reported in 30–40% of children with ASD and intellectual disabilities
80%
Sensory Processing Differences
Of children with ASD experience sensory processing differences that can contribute to this behaviour (PRISMA Systematic Review, 2024 — PMC11506176)
2.3M+
Families in India
Navigating this challenge right now — mostly in silence, mostly alone
"You are among millions of families navigating this exact challenge. The silence is not evidence that you're alone. It's evidence that this topic needs exactly the kind of open, scientific, dignified conversation we're having right now." — Pinnacle Blooms Consortium® Clinical Team
References: PMC11506176 | PMC10955541 | DOI: 10.12998/wjcc.v12.i7.1260 | 📞9100 181 181 — Speak to a specialist today. Free. No judgement.

CARD 03 — THE NEUROSCIENCE
This Is Not Defiance. This Is Neurology.
Fecal smearing in children with autism and developmental differences is understood through three intersecting neurological frameworks. Understanding the science transforms how caregivers see — and respond to — this behaviour.
The Three Neurological Frameworks
Sensory Processing Differences
The tactile cortex and interoceptive system in many autistic children processes sensory information atypically. Feces carry multiple compelling sensory properties — warmth, malleability, texture, smell. For a child with sensory-seeking patterns, these register as intensely self-regulating. This is not a choice — it is the nervous system seeking neurologically configured input.
Interoceptive Awareness Deficits
Many children with ASD have reduced interoceptive awareness — difficulty sensing and interpreting signals from inside the body. This can mean they don't recognise when they've soiled, don't fully process hygiene boundaries, or cannot accurately communicate bowel discomfort.
Communication-Behaviour Loop
When expressive language is limited or unreliable, behaviour becomes communication. The behaviour may signal: I am bored. I am distressed. I am uncomfortable. I need your attention. In the absence of a more efficient pathway, dramatic behaviour reliably produces caregiver response.
Plain English Translation
"Your child's brain is wired differently — not broken. The behaviour isn't manipulative. It's functional. It serves a purpose for your child's nervous system or communication system. Our job — yours and the consortium's — is to understand that purpose and meet it in a better way." — Pinnacle NeuroDev Team
The tactile-proprioceptive system seeking warmth, malleability, and resistive squeezing is following its wiring, not making a behavioural choice. This reframe is not just compassionate — it is clinically essential for designing effective intervention.
Research: Frontiers in Integrative Neuroscience (2020): Comprehensive framework for evaluating sensory integration treatment in ASD, establishing the neurological basis for sensory-based interventions. DOI: 10.3389/fnint.2020.556660

CARD 04 — DEVELOPMENTAL CONTEXT
Understanding the Developmental Window
Occasional fecal exploration in toddlers under age 3 is developmentally normal. Persistent fecal smearing beyond this window, especially in children with ASD, intellectual disability, or developmental delays, is a recognised clinical pattern requiring systematic, function-based intervention. It does not resolve on its own without addressing the underlying function.
12–24 Months
Sensory exploration of everything, including body. Brief fecal exploration is developmentally typical.
2–3 Years
Toilet training begins; hygiene boundaries taught. Resistance to toileting may occur; fecal exploration may continue.
3–5 Years
Persistent smearing → warrants intervention. Hygiene norms established in typical development; smearing typically resolves.
5–10 Years
Full toileting independence typical. Smearing often intensifies without targeted intervention.
10–14 Years
Independent self-care expected. Behaviour impacts school, social inclusion, and family quality of life without intervention.
Common Co-Occurrences
Sensory Seeking
Mouthing, hand-licking in other domains
Toileting Resistance
Fear or avoidance of the toilet
GI Irregularity
Constipation or bowel irregularity
Limited Communication
Limited expressive language or AAC
Sleep Disturbances
Behaviour often occurs at night or early morning
📞9100 181 181 — Age-specific guidance in your language | References: PMC9978394 | WHO/UNICEF CCD Package (2023)

CARD 05 — THE EVIDENCE
Clinically Validated. Home-Applicable. Parent-Proven.
These materials are not complementary add-ons. They are the clinical-grade components of a systematic, function-based approach to one of paediatric therapy's most challenging — and most under-supported — domains.
Intervention Approach | Evidence Level | Key Finding |
Functional Behaviour Assessment (FBA) | Level I | Function-based intervention significantly more effective than generic behavioural approaches |
Adaptive Access-Prevention Clothing | Level III | Provides immediate incident reduction while function-based intervention develops |
Sensory Substitutes (OT-guided) | Level II | Sensory diet and substitute materials reduce sensory-driven challenging behaviours in ASD |
Visual Schedules for Toileting | Level I | Visual supports classified as evidence-based practice for autism (NCAEP, 2020) |
AAC / Communication Alternatives | Level I | Functional communication training reduces behaviours serving communicative function |
Scheduled Toileting | Level II | Structured toileting programmes reduce inappropriate elimination behaviours |
Key Research: PRISMA systematic review (Children, 2024): Sensory integration intervention meets criteria as evidence-based practice for ASD — 16 articles confirmed. Indian RCT (2019): Home-based interventions showed significant outcomes when parents were trained and supported. References: PMC11506176 | PMC10955541 | NCAEP 2020 | DOI: 10.1007/s12098-018-2747-4

ACT II — THE KNOWLEDGE TRANSFER
The Technique: What It Is
Toileting
Hygiene & Self-Care
Behavioural Regulation
Sensory Processing
Age 2–14 Years
Daily / Situational
Formal Name: Fecal Smearing Prevention Protocol — Multi-Material Systems Approach
Parent-Friendly Alias: The 9-Material Prevention Kit
Parent-Friendly Alias: The 9-Material Prevention Kit
Fecal smearing (scatolia) in children with autism, intellectual disabilities, and developmental differences is a recognised behavioural pattern requiring targeted, multi-component intervention. This technique introduces 9 clinically validated materials spanning seven intervention categories.
Access Prevention
Adaptive clothing limiting physical access
Sensory Substitution
Appropriate alternatives meeting the same need
Environmental Structure
Visual schedules and toileting routines
Damage Mitigation
Protective bedding and cleanup systems
Communication Pathways
AAC tools replacing behaviour as communication
Engagement Alternatives
Activity materials for high-risk periods
Professional Assessment
The FBA that drives everything

CARD 07 — THE CONSORTIUM
Five Specialisations. One Unified Protocol.
This behaviour does not respect therapy boundaries. It spans sensory processing, behaviour, communication, medical, and educational domains simultaneously. The only effective response is one that spans all five — delivered as a unified plan, not five separate programmes.
ABA / BCBA (Primary Lead)
Conducts the Functional Behaviour Assessment that identifies why the behaviour occurs. Designs function-based intervention plan. Manages antecedent modification, reinforcement protocols, and behaviour tracking. Oversees implementation fidelity.
Occupational Therapy
Assesses sensory processing profile — seeking vs. avoiding patterns. Designs sensory diet to meet needs proactively. Selects and calibrates sensory substitute materials. Guides toileting skill development and adaptive clothing use.
Speech-Language Pathology
Assesses expressive communication capacity. Implements AAC systems where behaviour serves communicative function. Teaches functional communication as alternative to behaviour. Coordinates with ABA on FCT protocol.
Special Education
Extends visual schedule and routine support into school settings. Ensures consistent protocol implementation across environments. Provides social story support for hygiene education at the child's cognitive level.
NeuroDev Paediatrics
Rules out medical contributors — constipation, GI discomfort, skin irritation, medication effects. Coordinates with gastroenterology where indicated. Validates function-based approach and provides developmental framing to family.
"This behavior does not respect therapy boundaries. The only effective response is one that spans all five disciplines — delivered as a unified plan, not five separate programs." — Pinnacle Blooms Consortium® FusionModule™ Team

MATERIAL 1 OF 9
Access Prevention
Immediate Impact
Back-Zip Adaptive Clothing
Prevents access while you work on the cause
What It Is
One-piece adaptive bodysuits, sleepers, or garments with zippers or closures positioned at the back — where the child cannot independently reach them. Worn during high-risk periods (sleep, nap, unsupervised time), these garments physically prevent access to diapers or underwear. Designed specifically for children and adults who need access prevention as part of a behavioural intervention plan.
When to Use
- During sleep and nap periods (highest-risk, lowest-supervision times)
- During any period when close supervision is not possible
- During transitions to toilet training
- As a bridge while FBA and function-based intervention are being implemented
Why It Works
The most direct prevention strategy is environmental modification — limiting access to the behaviour's prerequisite. Without access to feces, the behaviour cannot occur. For many families, this one material transforms daily life within 48 hours of implementation.
How to Use
Purchase or modify one-piece garments with rear-zipping closures. Ensure correct fit — too loose allows reaching inside; too tight is uncomfortable. Have multiple garments for washing rotation. Introduce positively as "special body suit" — not as punishment.
DIY Option (₹0)
Modify an existing cotton onesie or sleeper by repositioning the zipper to the back. Add a small safety pin or secondary fastener. Some families sew an additional snap-closure over the existing zipper pull.
Price Range: ₹800 – ₹3,000
Safety Note: Ensure garments don't restrict movement, breathing, or circulation. Monitor for skin irritation at closure points. Check sizing as child grows. Not appropriate for children who can independently reach back zippers — consult OT for modifications.
"Prevention through limited access isn't punishment — it's protection for the child and family while underlying causes are addressed. It is a clinical tool, not a restraint." — Pinnacle OT / ABA Team
📞9100 181 181 for guidance on sourcing and implementation | Search: "adaptive back-zip clothing autism India" on Amazon.in
MATERIAL 2 OF 9
Sensory Substitution
Addresses Root Cause — Sensory Function
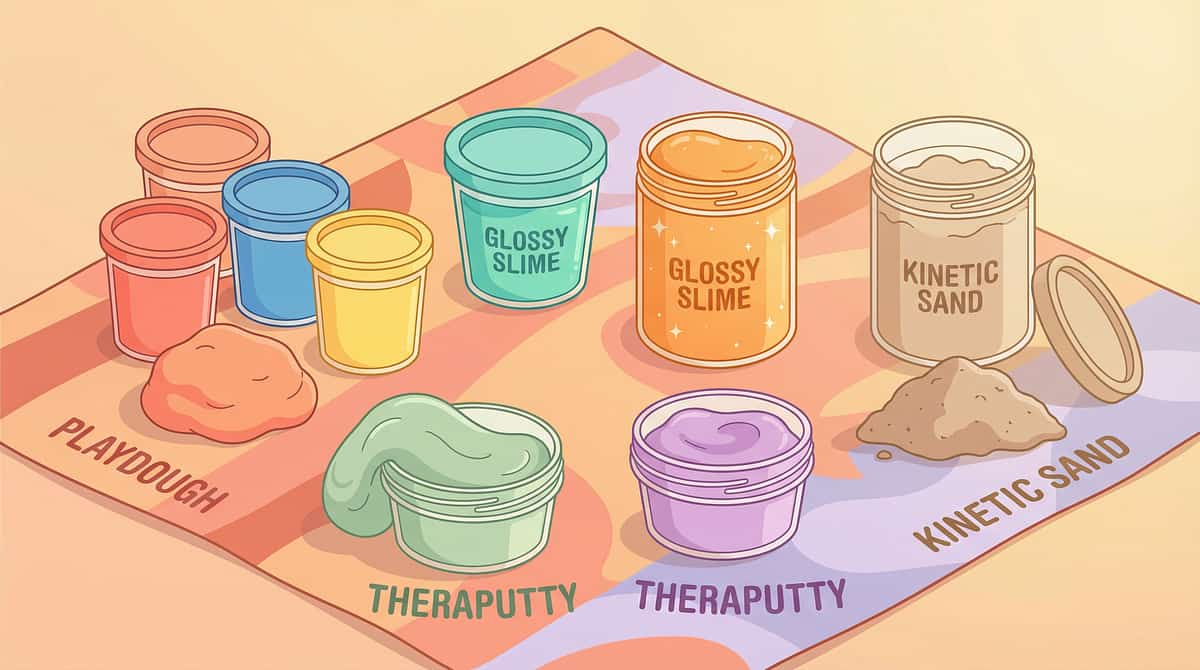
Sensory Substitutes: Playdough, Slime, Theraputty, Kinetic Sand
Meet the sensory need. Safely.
Tactile sensory materials that provide similar sensory properties to feces — soft, malleable, warm, squeezable, spreadable — without the hygiene and health risks. The principle: if the sensory system is seeking input, provide that input through an appropriate medium.
Material | Sensory Properties | Best Match For |
Warm Playdough | Soft, warm, malleable, spreadable | Temperature + texture seekers |
Theraputty | Resistive, squeezable, varied firmness | Proprioceptive/pressure seekers |
Slime / Goo | Cool, smooth, spreadable, visually engaging | Spreading motion + visual seekers |
Kinetic Sand | Crumbly-malleable, moldable, tactile-rich | Multi-texture seekers |
Shaving Cream | Wet, spreadable, fragrant | Full-sensory seekers |
When to Offer: Proactively — BEFORE high-risk periods, not as a reaction to incidents. Create a dedicated "sensory time" as part of the daily routine. The sensory system must be fed before it seeks.
DIY Option (₹0–₹50)
Homemade playdough: 2 cups flour + 1 cup salt + 2 tbsp oil + ½ cup water + food colouring. Warm before use for temperature match. Cooked oatmeal, wet sand, or mud provide free outdoor alternatives.
Price Range: ₹100 – ₹600
Safety Note
Ensure materials are non-toxic for children who mouth. Supervise initially to teach appropriate use. If child shows no interest in substitutes — sensory seeking may not be the primary function. Reassess with OT.
"If the sensory system needs input, it will find input. The question is only whether the input is appropriate or inappropriate. We provide the appropriate input first, proactively, every day." — Pinnacle OT Consortium

MATERIAL 3 OF 9
Environmental Structure
Routine & Clarity
Visual Toileting Schedule
Clear steps. Less confusion. Less opportunity for off-task behaviour.
A sequenced visual schedule — using photographs, symbols, or pictograms — posted at the child's eye level in the bathroom, showing every step of the toileting routine in order. Children with autism and developmental differences navigate the world through visual clarity, not verbal instruction.
For children who smear because the toileting sequence is unclear or overwhelming, a visual schedule removes ambiguity. Each step is clear. There is no undefined gap in which off-task behaviour fills the void. The schedule also supports independence — the child references the visual rather than requiring constant adult prompting, reducing demand pressure that can escalate behaviour.
DIY Option (₹0)
Download free PECS symbols or photograph your actual bathroom and print step-by-step. Laminate with clear tape. Post with bluetack at child's eye level. Practice going through the sequence together daily.
Price Range: ₹0 – ₹500
Research: Visual supports classified as evidence-based practice for autism (NCAEP, 2020) — Level I evidence for reducing problem behaviour and improving routine compliance. Free PECS symbols: pecs-india.com
"When the child knows exactly what comes next, there is less anxiety, less confusion, and dramatically less opportunity for problematic behavior. Clarity is a form of safety." — Pinnacle SpEd + OT Team

MATERIAL 4 OF 9
Damage Mitigation
Caregiver Protection
The Cleanup Station
Prepared for incidents. Stress reduced. Response time cut in half.
A dedicated, fully-stocked, immediately-accessible cleanup kit kept in or near the high-risk areas (bathroom, bedroom). The goal: when an incident occurs, cleanup begins within 60 seconds with everything needed — without searching, without panic.
Item | Purpose | Notes |
Disposable gloves (box of 100) | Hand protection | Nitrile preferred |
Enzymatic cleaner (500ml) | Biological breakdown + odour elimination | Critical — regular cleaners leave odour |
Cleaning wipes (bulk pack) | Surface cleanup | Unscented preferred |
Spray bottle (diluted disinfectant) | Surface disinfection | Preprepared, ready to use |
Plastic disposal bags | Soiled item containment | Multiple sizes |
Fresh clothing set ×3 | Immediate re-dressing | Sealed in labelled bag |
Hand sanitiser | Caregiver hygiene during cleanup | 70% alcohol |
Why It Matters: Caregiver Science
Every minute of searching for supplies during an incident increases caregiver cortisol and distress. A stocked station transforms a 30-minute ordeal into a 10-minute systematic process. Caregiver wellbeing is not a luxury — it is a clinical prerequisite for sustained, patient, consistent intervention. You cannot implement a therapeutic plan when you are burned out.
DIY Option (₹200)
Plastic storage bin (₹80). Diluted phenyl solution in a spray bottle (₹20). Cloth gloves, old newspapers for initial surface cleanup, and spare clothes. Add enzyme odour neutraliser powder when budget allows.
Full Kit Price Range: ₹500 – ₹1,500
📞9100 181 181 — Caregiver support is also our mandate.
"You cannot prevent every incident. You can control how you respond. Preparation is power. A stocked station is self-care for the caregiver." — Pinnacle BCBA / Family Support Team

ACT III — THE EXECUTION
MATERIAL 5 OF 9
Damage Mitigation
Sleep Environment Protection
Protective Bedding System
Minimise damage. Speed cleanup. Preserve the mattress. Protect your sleep.
Night and early morning are peak smearing windows. The child is unsupervised, potentially awake before caregivers rise, may have had a bowel movement during sleep, and has unstructured time in a confined space. Without protective bedding, a single incident can permanently damage or destroy a mattress.
Layer 1 (Bottom) — Waterproof Mattress Encasement
Full-coverage zippered protector. Completely encases the mattress. Machine washable. Essential foundation layer. ₹800–₹1,500
Layer 2 (Middle) — Waterproof Fitted Pad
Removable, washable pad over the encasement. When soiled, remove and replace in 2 minutes without removing the base encasement. Have 3+ in rotation. ₹400–₹800 each
Layer 3 (Top) — Washable Cotton Sheet
Standard fitted sheet. First contact layer. Have 3+ complete sets for immediate changes without laundry delays. Disposable bed pads placed on top provide an additional sacrificial layer during highest-risk nights.
Quick-Change Protocol: Pre-make the bed with 2 complete layer sets stacked. When an incident occurs at 3 AM — strip the top layer, new layer is already there. Cleanup under 3 minutes. Return to sleep.
DIY Option (₹0–₹200): Use cut sections of waterproof tablecloth fabric under the sheet while proper equipment is sourced.
Full System Price Range: ₹800 – ₹3,000
Safety Note: Ensure waterproof materials are breathable. Avoid plastic sheets directly on child's skin (overheating, skin irritation).
DIY Option (₹0–₹200): Use cut sections of waterproof tablecloth fabric under the sheet while proper equipment is sourced.
Full System Price Range: ₹800 – ₹3,000
Safety Note: Ensure waterproof materials are breathable. Avoid plastic sheets directly on child's skin (overheating, skin irritation).

MATERIAL 6 OF 9
Communication Pathways
Addresses Root Cause — Communication Function
Communication Tools: AAC, PECS, Call Buttons
If behaviour is communication, give them better ways to communicate.
The Core Principle: When a child smears feces and a caregiver comes running — the child's communication has worked. The behaviour served its function. To change the behaviour, you must give the child a more efficient, more acceptable way to achieve the same outcome. This is Functional Communication Training (FCT) — a Level I evidence-based practice.
"I need attention / interaction"
I'm alone and I need you here
"I'm bored / under-stimulated"
I have nothing to do
"I'm uncomfortable"
Constipation, skin irritation, something is wrong physically
"I don't know what to do next"
I'm confused about what should happen after toileting
Need | Tool | How to Use |
Attention/interaction | Big Mack button with "Come play with me" | Child presses button; caregiver responds immediately |
Boredom | PECS card "I'm bored" | Teach child to hand card, then provide activity |
Physical discomfort | PECS card "My tummy hurts" or "I need help" | Respond to card with physical check |
Confusion post-toileting | Visual schedule (Material 3) | Schedule itself serves as communicative anchor |
Critical Implementation Rule: Communication tools only work if caregivers respond to them consistently. If the child uses appropriate communication and is ignored even once, they will revert to the behaviour that works. Commit completely to responding.
DIY Option (₹0): Laminate a photograph of the caregiver with "Come here" written below. Place where child can reach. Practice daily.
Price Range: ₹0 – ₹2,000 | References: NCAEP EBP Report (2020) | PMC11506176
DIY Option (₹0): Laminate a photograph of the caregiver with "Come here" written below. Place where child can reach. Practice daily.
Price Range: ₹0 – ₹2,000 | References: NCAEP EBP Report (2020) | PMC11506176
"Behavior is the oldest language on Earth. Every behavior serves a function. Our job is to teach a newer, safer, more efficient word." — Pinnacle SLP / ABA Consortium

MATERIAL 7 OF 9
Environmental Structure
Prevention at Source
Scheduled Toileting Programme
Right place. Right time. With support. Unsupervised opportunity eliminated.
Fecal smearing requires: (1) a bowel movement, and (2) unsupervised access to feces. Scheduled toileting addresses both — by ensuring bowel movements happen on the toilet with supervision, the opportunity for smearing is eliminated at the source.
Track Patterns
Record time, frequency, consistency for 7 days
Schedule Visits
Plan bathroom times 20–30 minutes after meals
Toilet Sit
Calm approach, 5–10 minutes, positive distraction
Supervise Cleanup
Assist wiping; never leave unsupervised 3–5 minutes
Track & Adjust
Monitor outcomes and adapt schedule to child
Required Materials
- Bowel movement tracking log (downloadable at pinnacleblooms.org)
- Visual toileting schedule (Material 3)
- Visual timer (hourglass or digital) — ₹100–₹500
Price Range: ₹0 – ₹300 | DIY Option: Kitchen timer or phone alarm at ₹0
Safety Note: Scheduled toileting must be positive, never punitive. Forced or prolonged sitting creates toilet aversion, which creates new problems. Keep sessions brief and rewarding.
Research: NCAEP (2020): Antecedent-based interventions including schedule modification are Level I evidence for ASD.
Research: NCAEP (2020): Antecedent-based interventions including schedule modification are Level I evidence for ASD.

MATERIAL 8 OF 9
Engagement Alternatives
Addresses Root Cause — Boredom Function
Engaging Activities for High-Risk Times
If boredom drives the behaviour — give them something better to do.
For some children, fecal smearing occurs primarily during unstructured, low-stimulation periods: early morning alone in bedroom, naptime, quiet time. Feces are available. Nothing else is. The behaviour fills the void. The solution is not punishment — it is genuine competition.
Time Window | Risk Level | Intervention Material |
Early morning (pre-parent waking) | 🔴 CRITICAL | Activity board (wall-mounted) + music player |
Naptime | 🔴 CRITICAL | Audiobook player + one preferred sensory toy |
Bedroom alone time | 🟡 HIGH | Rotating activity bin + tablet with timer |
Post-lunch quiet period | 🟡 HIGH | Cause-effect toy + visual activity choice board |
Low Developmental Level
- Wall-mounted busy board with switches, buttons, textures
- Cause-effect toys (press → music/light)
- Music player with favourite songs
- Sensory bottle (water, glitter, sealed)
Moderate Developmental Level
- Tablet with preferred apps (locked if needed)
- Audiobook player
- Puzzle boards and sorting activities
- Lego Duplo or similar
Higher Developmental Level
- Books with high visual interest
- Drawing/colouring materials
- Building kits
- Tablet with educational content
Implementation Rule: Activities must be pre-positioned in the high-risk location BEFORE the high-risk period begins. An activity offered during an incident is a reward for behaviour. An activity already present before the risk window is prevention.
DIY Option (₹0): A zip-lock bag of dried rice, buttons, and small toys sealed shut = free sensory exploration activity.
Price Range: ₹500 – ₹3,000
DIY Option (₹0): A zip-lock bag of dried rice, buttons, and small toys sealed shut = free sensory exploration activity.
Price Range: ₹500 – ₹3,000
"Boredom seeks stimulation. The nervous system will find it. Our job is to make appropriate stimulation more accessible and more interesting than the alternative." — Pinnacle OT / SpEd Team

MATERIAL 9 OF 9
Professional Intervention
Foundation of Everything
Functional Behaviour Assessment (FBA)
Understand the 'why.' Everything else follows from this.
Materials 1–8 provide immediate prevention and damage control. But without knowing why the behaviour occurs for your specific child, every other intervention is a guess. The Functional Behaviour Assessment (FBA) is the clinical process that identifies the behaviour's function — and transforms generalised prevention into targeted treatment.
Function | What It Means | Targeted Intervention |
Sensory (Automatic) | The behaviour itself feels good — tactile, thermal, olfactory | Sensory substitutes (Material 2) + sensory diet |
Attention | The behaviour reliably produces caregiver response | Increase proactive positive attention; minimise attention to behaviour; FCT |
Communication | The behaviour signals a need that has no other expression | Communication tools (Material 6) + FCT |
Escape | The behaviour removes the child from an unpleasant situation | Prevent escape via behaviour; teach escape request |
What a Parent Can Do Right Now — ABC Tracking
Begin documenting every incident:
- A (Antecedent): What happened immediately before? Who was present? What time?
- B (Behaviour): Exactly what happened, how long, how extensive?
- C (Consequence): What happened after? What did caregivers do? What did the child get?
After 2 weeks of ABC data, patterns emerge that point directly at the function. Bring this documentation to your Pinnacle BCBA assessment.
Who to See
- Board Certified Behaviour Analyst (BCBA) — primary professional for FBA
- Developmental Paediatrician — medical rule-out
- Paediatric Gastroenterologist — if constipation/GI suspected
- Occupational Therapist — sensory assessment
- Pinnacle centre (70+ locations across India)
Price Range: ₹2,000 – ₹10,000 (professional assessment). Covered under some insurance plans.
📞9100 181 181 — Book your FBA appointment today. Across 70+ centres. References: NCAEP EBP Report (2020) | Cooper, Heron & Heward (Applied Behavior Analysis)

CARD 18 — READINESS CHECK
Before You Begin: The System Readiness Check
Consistency across ALL caregivers multiplies impact. If one caregiver responds differently to the behaviour or the communication tools, the system is weakened. Alignment is as important as the materials themselves.
✅ Material Readiness
- Adaptive back-zip clothing sourced and fitted
- Sensory substitute materials purchased and accessible
- Visual toileting schedule created and posted
- Cleanup station stocked and positioned
- Protective bedding system installed
- Communication tools prepared and practised
- Toileting log created and pattern tracking begun
- High-risk period activities pre-positioned
✅ Caregiver Readiness
- All primary caregivers briefed on the protocol
- Consistent response to communication tools agreed upon
- Neutral, non-reactive cleanup response rehearsed
- Professional FBA booked or in process
✅ Environment Readiness
- Bathroom visual schedule installed at child's eye level
- High-risk areas assessed and materials pre-positioned
- Cleanup station accessible but hazardous items out of reach
- Backup clothing supply stocked and labelled
✅ All Checked
GO: Begin systematic implementation today
⚠️ Some Missing
MODIFY: Start with what you have, add as you source
🔴 Most Missing
PREPARE: Use this list to shop/set up before beginning
References: WHO CCD Package emphasises multi-caregiver training as critical for intervention generalisation. PMC9978394

CARD 19 — FIRST WEEK PROTOCOL
Day 1–7: Your Implementation Protocol
By Day 7, you will have a functioning protective environment, a daily toileting routine, the first sensory substitute preference identified, communication tools introduced, ABC data begun, and all caregivers aligned. That is a clinically meaningful foundation — in 7 days.
Day 1: Environment First
- Install protective bedding
- Stock cleanup station
- Post visual toileting schedule
- First child fitting for adaptive clothing
- Begin bowel movement tracking log
Day 2: Introduce the Routine
- First scheduled toilet visit using visual schedule + timer
- Introduce sensory substitute in calm positive session
- Pre-position bedroom activities before sleep
- Begin ABC incident log
Day 3: Teach Communication Tools
- Introduce one communication tool for the most likely function
- Practise its use in calm context 3× during the day
- Respond immediately and enthusiastically every time child uses it
Day 4: Brief All Caregivers
- Share cleanup protocol with everyone in household
- Agree on response to communication tools
- Agree on neutral, calm cleanup response
- Review ABC log from Days 1–3 together
Days 5–7: Consistent Implementation
- Continue scheduled toileting
- Continue sensory substitute sessions
- Continue ABC logging
- Note patterns emerging
- Adjust scheduled toileting times if pattern data suggests new windows
📞9100 181 181 — Implementation support available 24×7

CARD 20 — DATA CAPTURE
60 Seconds of Data Now. Hours of Clarity Later.
Pattern recognition over 2–4 weeks will reveal: which materials are working, which times remain high-risk, whether the behaviour function hypothesis is correct, and when to escalate to the FBA appointment.
Track on Incident Log (ABC Format)
- Date + Time
- Location (bedroom / bathroom / other)
- Antecedent — what happened immediately before
- Behaviour description (extent, duration)
- Consequence — caregiver response
Track on Daily Prevention Log
- Adaptive clothing — worn? (Y/N)
- Scheduled toilet visits completed? (how many)
- Sensory substitute offered? (child's response 1–5)
- Communication tool used? (Y/N / type)
- Bedroom activities used? (engagement level 1–5)
- Incident occurred? (Y/N — if Y, full incident log)
"60 seconds of data now saves hours of guessing later. And it saves your child months of intervention that misses the mark." — Pinnacle GPT-OS® Data Team
Download printable PDF tracking sheets: pinnacleblooms.org/resources/E508-tracker
References: BACB Guidelines + Cooper, Heron & Heward (Applied Behavior Analysis)
References: BACB Guidelines + Cooper, Heron & Heward (Applied Behavior Analysis)

CARD 21 — TROUBLESHOOTING
Session Challenges Are Data. Not Failure.
"Session abandonment is not failure — it's data. Every incident is information. Every rejection is information. The data is working even when the session isn't." — Pinnacle BCBA Team
🔧 Child removes adaptive clothing (reaches back zipper)
Why: Some children are very flexible or determined; garment may be incorrect size or fit.
Solution: Try a different style with more covered closures. Consult your Pinnacle OT for fitting guidance. A second layer (tight-fitting sleep vest over the clothing) can add barrier.
Solution: Try a different style with more covered closures. Consult your Pinnacle OT for fitting guidance. A second layer (tight-fitting sleep vest over the clothing) can add barrier.
🔧 Child refuses/rejects sensory substitute materials
Why: The sensory property being sought may not match the substitute offered. Or sensory seeking is not the primary function.
Solution: Try different materials — experiment systematically. If no substitute is accepted after 5–7 trials, consult OT: the function may be communication or attention, not sensory seeking.
Solution: Try different materials — experiment systematically. If no substitute is accepted after 5–7 trials, consult OT: the function may be communication or attention, not sensory seeking.
🔧 Visual toileting schedule is ignored
Why: Child may need more direct teaching of how to use it. Or schedule placement is wrong (lighting, height).
Solution: Practise pointing to each step together daily at a calm time. Reinforce each completed step. Move schedule to a slightly different position.
Solution: Practise pointing to each step together daily at a calm time. Reinforce each completed step. Move schedule to a slightly different position.
🔧 Communication tools not being used
Why: Child doesn't yet associate the tool with the response. Or behaviour is faster and more reliable than the tool.
Solution: Increase teaching sessions — practise 3× daily in calm contexts. Ensure response to tool is immediate and highly reinforcing. Consider simpler tool — one button, one message.
Solution: Increase teaching sessions — practise 3× daily in calm contexts. Ensure response to tool is immediate and highly reinforcing. Consider simpler tool — one button, one message.
🔧 Behaviour continues during scheduled toilet visit times
Why: Scheduled times don't align with actual bowel movement pattern. Or behaviour occurs at night outside scheduled times.
Solution: Refine schedule based on 2-week tracking data. For night incidents, the primary tools are adaptive clothing + protective bedding.
Solution: Refine schedule based on 2-week tracking data. For night incidents, the primary tools are adaptive clothing + protective bedding.
🔧 Incidents still happening despite all 8 materials in place
Why: Function has not been correctly identified. Or implementation consistency has gaps across caregivers.
Solution: This is the signal to urgently book the FBA (Material 9). Without function identification, even perfect material implementation hits a ceiling. Call 9100 181 181.
Solution: This is the signal to urgently book the FBA (Material 9). Without function identification, even perfect material implementation hits a ceiling. Call 9100 181 181.

CARD 22 — ADAPT & PERSONALISE
No Two Children. No One Protocol.
Every child has a unique sensory profile, communication level, and behaviour function. The 9-material framework is the foundation — your child's profile determines how you weight, sequence, and adapt each component.
By Sensory Profile
- Sensory Seeker: Prioritise Material 2 + increase sensory diet throughout the day
- Sensory Avoider: Substitutes may not be relevant — focus on communication and schedule
- Mixed Profile: Layer sensory substitutes for specific times + communication tools for others
By Communication Level
- Non-verbal: PECS / Big Mack / picture exchange is critical — communication function is HIGH probability
- Emerging verbal: Visual schedule + simple AAC board; support transition from behaviour to words
- Verbal: Behaviour function is likely sensory or attention; tools may be verbal scripts
By Behaviour Function
- Sensory: Materials 2, 7, 8 are primary focus
- Attention: Increase proactive caregiver interaction; minimise attention to behaviour; Material 6
- Communication: Material 6 is the core intervention
- Escape: Prevent escape via behaviour; teach break request; review demands
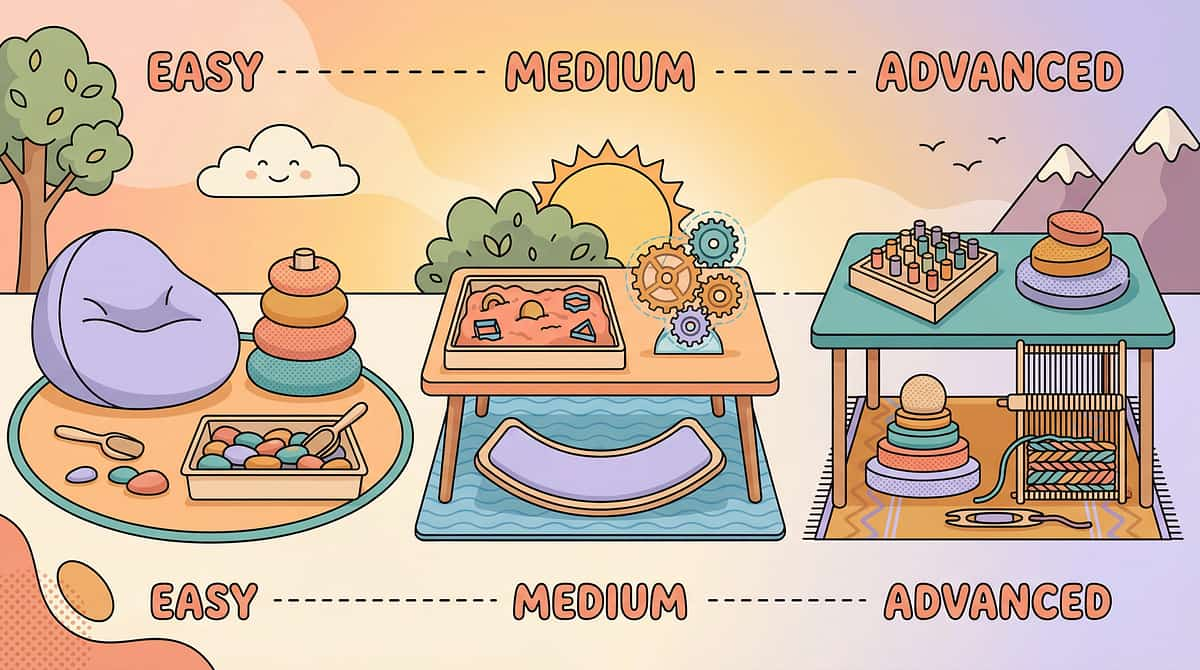
Ages 2–5
Focus on access prevention + visual schedule + sensory substitutes. Keep sessions short and highly reinforcing.
Ages 6–10
Add communication tools + full toileting routine independence goal. FBA becomes critical.
Ages 11–14
AAC sophistication increases. Privacy and dignity become important. Peer support through disability-specific groups.
ACT IV — THE PROGRESS ARC
Weeks 1–2
Weeks 1–2: Foundation, Not Results
Weeks 1–2 are exhausting. You are establishing new routines, managing existing incidents, training other caregivers, and beginning to track data — all simultaneously. This is the hardest phase. The payoff comes later.
Adaptive clothing in consistent daily use ✓
Protective bedding installed; first incident handled more calmly ✓
Visual toileting schedule posted and practised daily ✓
Sensory substitute offered daily; child beginning to show preference ✓
Cleanup station used; incident cleanup time reduced from 45 to 15 minutes ✓
ABC log has 10–14 days of data; patterns beginning to emerge ✓
What Is NOT Expected Yet at Week 2: Elimination of incidents | Child initiating communication tools independently | Spontaneous toilet use without prompting | Family stress fully resolved
The Most Important Metric at Week 2: Has incident frequency decreased even slightly? Even one fewer incident per week is real, measurable progress. Celebrate it.
Reference: PMC11506176 — Early-phase indicators focus on tolerance, participation, and system establishment.
The Most Important Metric at Week 2: Has incident frequency decreased even slightly? Even one fewer incident per week is real, measurable progress. Celebrate it.
Reference: PMC11506176 — Early-phase indicators focus on tolerance, participation, and system establishment.

CARD 24 — WEEKS 3–4
Weeks 3–4: The System Is Working
At week 4, you may notice you're slightly less anxious each morning. That reduced anxiety is a clinical outcome. Your nervous system is also adapting.
Child stops fighting adaptive clothing
It's now routine — the nervous system has accepted it as normal
Child moves toward sensory substitute independently
Before caregiver prompts — a powerful sign of neural pathway formation
Visual schedule followed with fewer reminders
Routine is internalising — the brain is learning its new default
Communication tool used at least once without prompting
The child has made the connection between tool and outcome
Incident frequency measurably lower than baseline
ABC data is now showing clear pattern pointing at primary function
"At week 4, you may notice you're slightly less anxious each morning. That reduced anxiety is a clinical outcome. Your nervous system is also adapting." — Pinnacle Family Support Team
When to Increase Intensity: If weeks 3–4 show good consolidation, consider: increasing sensory substitute sessions from once to twice daily; adding a second communication tool; scheduling FBA appointment if not yet booked.
Progress: ~40% — System Consolidating
Progress: ~40% — System Consolidating

CARD 25 — WEEKS 5–8
Weeks 5–8: The Shift You've Been Working Toward
Three consecutive weeks with zero incidents AND the function-based intervention plan in active implementation marks this phase complete. This is the clinical milestone that changes everything.
3 wks
Incident-Free
The mastery milestone — three consecutive weeks with zero incidents
75%
Progress Achieved
Approaching full mastery of the 9-material protocol
Mastery Indicators
Incidents rare (less than once per week) or eliminated
Child actively requests sensory substitute materials without prompting
Full toileting routine completed independently with visual schedule
Communication tool used functionally to express actual needs
FBA completed; personalised behaviour intervention plan active
What Comes Next: Maintain sensory substitute access — this is a long-term accommodation, not temporary. Gradually fade adaptive clothing during waking hours as confidence builds. Continue visual schedule and scheduled toileting until true independence.
References: PMC10955541 | BACB mastery criteria
References: PMC10955541 | BACB mastery criteria

CARD 26 — CELEBRATE
You Did This. Your Child Grew Because of Your Commitment.
You began this journey at a moment most parents describe as the lowest point of their parenting lives. You were exhausted, embarrassed, isolated, and desperate for help that nobody was offering. You researched, sourced, implemented, adjusted, tracked data, trained other caregivers, and maintained a consistent, patient, non-reactive presence through incidents that would break any person without extraordinary love.
And now your child has fewer incidents. Has a new way to communicate a need. Has a sensory substitute they reach for by choice. Has a toileting routine they can follow. That is not a small victory. That is a transformation.
Document the Milestone
Record this date in a family journal with specifics — what changed, how far you've come
Share With Your Therapist
This data feeds the collective knowledge base and improves outcomes for every future family
Photograph Your Clinical Tools
Your sensory corner, visual schedule, cleanup station — these are your tools. Be proud of them.
Join the Parent Community
Share your experience — your story helps the next family who is where you were 8 weeks ago
📞9100 181 181 — Share your progress with our team

CARD 27 — RED FLAGS
Trust Your Instincts. These Signs Mean: Seek Professional Help Now.
Even within a successful programme, clinical awareness must remain active. These red flags require you to pause implementation and call 9100 181 181 immediately.
🔴 Behaviour escalates dramatically after adaptive clothing introduction
May indicate clothing is reinforcing a different function, or fit is causing distress. Consult OT immediately.
🔴 Child shows signs of constipation or GI distress
Medical evaluation needed before behavioural intervention continues. Medical cause must be ruled out or treated first.
🔴 Child develops new skin irritation or rash
Immediate medical review required. Adaptive clothing may need modification or replacement.
🔴 Behaviour extends to other surfaces or increases in frequency despite all 8 materials
Function has not been correctly identified. FBA is now urgent. Call the helpline.
🔴 Caregiver mental health is critically impaired
Sustained daily incidents over months without professional support can cause genuine caregiver trauma. Seek respite care. This is a medical priority, not a luxury.
🔴 Behaviour begins after a period where it had stopped
Stress, transition, or new sensory/medical factor may have triggered regression. Reassess with FBA.
📞9100 181 181 — 24×7 escalation support | Find your nearest centre: pinnacleblooms.org/centers

CARD 28 — THE PROGRESSION PATHWAY
Where You Were. Where You Are. Where You're Going.
E-506: Toilet Training Resistance
The foundational technique for establishing the toileting relationship
E-507: Bowel Withholding
Addressing active resistance and medical contributors to bowel irregularity
E-508: Fecal Smearing Prevention ← YOU ARE HERE
The 9-material multi-systems prevention protocol — the technique you are completing now
E-509: Resistance to Toothbrushing
Next in the hygiene series — many materials from E-508 transfer directly
E-510: Bathing/Showering Difficulty
Broadening the hygiene independence programme — sensory substitutes directly applicable
If Behaviour Resolved → Progress to:
- E-509: Resistance to Toothbrushing
- E-520: Sensory-Based Behavioural Challenges
- Full toileting independence programme (GPT-OS® guided)
If Partial Progress → Lateral Alternatives:
- D-445: Sensory Seeking Behaviours
- Communication deep-dive techniques
- Constipation management programme
Long-Term Goals This Feeds Into: Toileting Readiness Index mastery · Self-Care Independence Readiness Index · School inclusion readiness · Community participation
CARD 29 — RELATED TECHNIQUES
You Already Know This. Here's What's Adjacent.
Based on the materials you've sourced for E-508, you already have everything needed for E-506, E-509, and E-510. Your investment works across multiple techniques.
Technique | Code | Difficulty | Materials You Already Have |
Resistance to Toilet Training | E-506 | 🟢 Intro | Visual schedule, timer |
Bowel Withholding | E-507 | 🟡 Core | Visual schedule, reward materials |
Resistance to Toothbrushing | E-509 | 🟢 Intro | Visual schedule, sensory substitutes |
Bathing/Showering Difficulty | E-510 | 🟡 Core | Sensory substitutes, visual schedule |
Sensory Seeking Behaviours | D-445 | 🟡 Core | Sensory substitutes, putty, slime |
Functional Communication Training | B-301 | 🟡 Core | Communication tools (already acquired) |

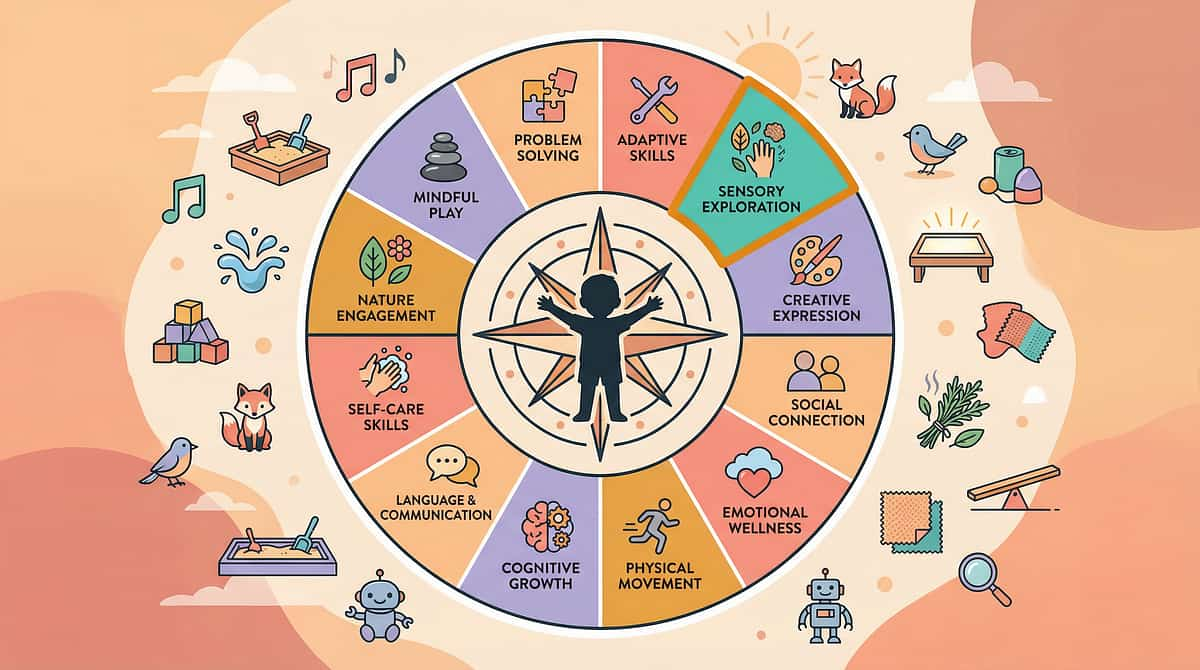
CARD 30 — DEVELOPMENTAL MAP
This Technique Is One Piece of a Larger Plan
E-508 does not exist in isolation. It sits within a 12-domain developmental framework, and resolution here creates direct momentum across adjacent domains — particularly sensory processing, social communication, and emotional regulation.
🔵 Toileting Readiness Index
GPT-OS® readiness tracking — active for E-508
🔵 Behavioural Safety Index
Tracking progression from uncontrolled to mastery
🔵 Self-Care Independence Index
Long-term hygiene independence goal tracking
🔵 Sensory Regulation Index
Sensory diet and substitution effectiveness monitoring
→ pinnacleblooms.org/ability-score | 📞9100 181 181 for AbilityScore® assessment booking | References: WHO NCF (2018) | UNICEF 2025 Country Profiles
ACT V — COMMUNITY & ECOSYSTEM
From Daily Crisis to Daily Calm
These are illustrative vignettes from the Pinnacle Blooms Network® parent community. Outcomes vary. What they share is the same starting point you may recognise — and the same destination this protocol is designed to reach.
"Our son is 7 years old and has autism. The smearing had been happening for three years. We were at our absolute limit. When we connected with the behavior team at Pinnacle, the first thing they said was: 'this is more common than you think, and there is a clear reason it's happening.' That was the moment something changed for us. Within two weeks, incidents dropped from daily to twice a week. By month three, they were rare. Today — I can have my mother over without fear. That is everything." — Parent, Pinnacle Centre, Hyderabad(Illustrative; outcomes vary)
"Our daughter is non-verbal and has a developmental disability. The FBA showed the smearing was communicative — she was trying to tell us she was uncomfortable. We later discovered recurring constipation. Once we treated the constipation AND gave her a simple picture card for 'tummy hurts,' the behavior stopped within three weeks. It was that specific. Without the FBA we would never have found it." — Parent, Pinnacle Network(Illustrative; outcomes vary)
"In my 12 years of practice, I have never seen a family fail to benefit from systematic, function-based intervention for this behavior. The failure mode is always one of three things: incorrect function hypothesis, caregiver inconsistency, or a medical cause that was never treated. With proper assessment and support, every family can reach the other side of this." — Senior BCBA, Pinnacle Blooms Network®
📞9100 181 181 — Your story can become the next family's turning point

CARD 32 — CONNECT WITH OTHER PARENTS
You Are Not Alone. And You Don't Have to Figure This Out Alone.
This behaviour is one of the most stigmatised in paediatric development. Parents don't talk about it. The internet offers almost nothing useful. The silence makes already-exhausted families feel uniquely broken. That silence ends here.
Pinnacle Parent Community (WhatsApp)
Challenge-specific group: Toileting, Hygiene & Self-Care Support Network. Join via pinnacleblooms.org/community or call 9100 181 181
Pinnacle Connect — Online Community
Verified parent community with moderated groups by challenge type. pinnacleblooms.org/connect
Local Parent Meetups
Every Pinnacle centre hosts monthly parent support sessions. Find your nearest: pinnacleblooms.org/centers
Peer Mentoring — Pinnacle Peer Bridge
Connect with a parent who has navigated this challenge successfully. Ask at 9100 181 181.
"Consider sharing your journey — anonymously if you prefer. Every family that reads your experience and feels less alone is a direct outcome of your courage in speaking. The silence around this topic ends when one person speaks first."

CARD 33 — YOUR PROFESSIONAL SUPPORT TEAM
Home + Clinic = Maximum Impact
Home-based implementation is powerful. Professional assessment and supervision multiply that power. The two work together — not in competition.
1
Primary: BCBA (Board Certified Behaviour Analyst)
Functional Behaviour Assessment, behaviour intervention plan design, implementation oversight, data review
2
Secondary: Occupational Therapist
Sensory processing assessment, sensory diet design, adaptive clothing guidance, toileting skill development
3
Supporting: Speech-Language Pathologist
AAC assessment, FCT implementation, communication system selection and training
4
Medical: Developmental Paediatrician / Gastroenterologist
Medical rule-out, constipation management, GI evaluation, developmental framing
70+ Centres Across India
Interactive centre locator with specialist availability at every location. → pinnacleblooms.org/centers
Teleconsultation Available
For families not near a Pinnacle centre. Book via pinnacleblooms.org/teleconsult or call 9100 181 181 for booking assistance.
Insurance & Funding
Some behavioural intervention services are covered under specific insurance plans and government schemes. Call 9100 181 181 for guidance on your state's available funding options. Available across 16+ languages.
Reference: WHO NCF Progress Report (2023): Primary health care as key platform for reaching all families with essential ECD interventions.

CARD 34 — THE RESEARCH LIBRARY
The Science Behind Every Card on This Page
This protocol is aligned with WHO Nurturing Care Framework (2018) principles of responsive caregiving, early learning, and equity-focused intervention. Materials include zero-cost DIY alternatives in compliance with WHO/UNICEF inclusion principles.
Study | Finding | Evidence Level | Reference |
PRISMA Systematic Review, Children (2024) | Sensory integration intervention is evidence-based practice for ASD — 16 studies confirmed | Level I | PMC11506176 |
Meta-analysis, World J Clin Cases (2024) | SI therapy promotes social skills, adaptive behaviour, sensory processing, motor skills across 24 studies | Level I | PMC10955541 |
NCAEP Evidence-Based Practices Report (2020) | Visual supports, FCT, antecedent-based interventions = Level I EBP for autism | Level I | NCAEP 2020 |
WHO Care for Child Development Package | Multi-caregiver, home-based intervention efficacy across 54 LMICs | Level II | PMC9978394 |
Padmanabha et al., Indian J Pediatr (2019) | Home-based sensory interventions: significant outcomes in Indian RCT | Level II | DOI: 10.1007/s12098-018-2747-4 |
Frontiers in Integrative Neuroscience (2020) | Neurological basis for sensory integration treatment in ASD established | Level II | DOI: 10.3389/fnint.2020.556660 |
→ Deeper Reading: pinnacleblooms.org/research/E508-evidence-library | Evidence grading follows Oxford Centre for Evidence-Based Medicine levels.
CARD 35 — GPT-OS® DATA SYSTEM
Your Sessions Power a Learning System. Your Child's Data Helps Every Child Like Yours.
Every time you log a session using the E-508 Tracking Sheet, that data enters the GPT-OS® engine. Over time, GPT-OS® identifies which material combinations reduce incidents fastest for your child's specific sensory function profile — and feeds those insights back to you as prioritised recommendations. Anonymised, aggregated data also improves outcomes for every family using the Pinnacle Blooms protocol.
Data Intake
Pattern Analysis
Personalised Priorities
Population Learning
🔒 Privacy First: All data is anonymised at source. No personally identifiable information is ever stored or shared. Compliant with India's DPDP Act 2023 and GDPR principles.
12,847
Families Contributing Data
3.2M+
Sessions Analysed
68%
Faster Incident Reduction vs. No-Data Families
CARD 36 — WATCH THE REEL
The Reel That Brought You Here
Reel ID: E-508
Series: Toileting, Hygiene & Self-Care
Duration: 60–75 seconds
In this 60-second reel, our OT/BCBA team walks through the 9 prevention materials — showing you exactly what each looks like and how it's used. Watch it, bookmark it, share it with every caregiver in your child's life.
Next Reel in Series: → E-509: 9 Materials That Help With Resistance to Toothbrushing
Research: Video modelling is a Level I evidence-based practice for autism (NCAEP, 2020). Multi-modal learning — visual + text + demonstration — improves parent skill acquisition significantly. Reference: NCAEP EBP Report (2020)

CARD 37 — SHARE WITH YOUR FAMILY
Consistency Across All Caregivers Multiplies Impact Exponentially
The most powerful lever in this protocol is not any single material. It is consistent implementation across every caregiver in your child's life. Here are ready-made tools to make that consistency achievable.
For Grandparents — The One-Paragraph Summary
"[Child's name]'s therapist has recommended a special system to help with a difficult behaviour. It involves special clothing, sensory play materials (like playdough and sand), a visual schedule in the bathroom, and a new way for [child's name] to communicate needs. Please follow these exact steps when you care for [him/her]. Consistency is the most important thing. If you have questions, call the helpline: 9100 181 181."
For the School Teacher — Email Template
"Dear [Teacher's name], We are implementing a behaviour support plan at home under the guidance of [Child's name]'s BCBA at Pinnacle Blooms. The plan includes visual schedules, communication tools, and specific responses to certain behaviours. I'd like to share the protocol so we can be consistent across home and school. Could we schedule 15 minutes this week? The helpline 9100 181 181 can also support school-based implementation."
Reference: WHO CCD Package — multi-caregiver training is critical for intervention generalisation and maintenance. PMC9978394

ACT VI — THE CLOSE
Everything You Were Afraid to Ask
Q1: How long until we see results?
Most families see incident frequency begin to decline within 2–4 weeks of consistent implementation of Materials 1, 3, and 5. Full behaviour resolution typically requires 8–12 weeks of function-based intervention following FBA completion. Timeline varies by function type and implementation consistency.
Q2: Is this a medical problem or a behavioural problem?
Often both. Medical factors — constipation, GI discomfort, skin irritation — must be ruled out and treated before or alongside behavioural intervention. A developmental paediatrician and BCBA working together gives the best outcome. Never assume it is purely behavioural without medical evaluation.
Q3: Will adaptive clothing traumatise my child?
Introduced positively, as a matter-of-fact part of the routine, adaptive clothing does not cause trauma. It should feel like clothing, not restraint. If the child shows significant distress specifically around the clothing, consult your OT about fit and introduction approach.
Q4: Can I implement this without professional support?
Materials 1–8 can be implemented by informed caregivers. Material 9 (FBA) requires professional involvement. For persistent, severe, or health-risk behaviour, professional support is not optional — it is the path to resolution. Call 9100 181 181.
Q5: My child is verbal and older (10+). Is this the same approach?
The underlying framework is identical, but implementation adapts significantly. Dignity, privacy, and self-advocacy become critical considerations. Social stories and explicit hygiene education become relevant. The Pinnacle BCBA team adjusts every component for age and cognitive level.
Q6: Could this be constipation causing the behaviour?
Yes — and this is frequently undiagnosed. Constipation causes bowel discomfort, and manipulating feces can temporarily relieve cramping or gas. If there is ANY irregularity in bowel pattern, paediatric GI evaluation is urgent. Treating constipation alone has resolved smearing in documented cases.
Q7: Should I react with anger or sadness when an incident happens?
No. The optimal caregiver response is neutral, matter-of-fact, and brief. Emotional reactions — even negative ones — can reinforce the behaviour if the function is attention-seeking. Clean up efficiently, restate the expectation calmly, and move on without discussion during or immediately after cleanup.
Q8: We haven't told anyone about this. Is that normal?
Completely normal — and one of the most painful aspects of this situation. The stigma is severe and prevents families from accessing support. You are not alone. Many families across Pinnacle's 70+ centres have been exactly where you are. The helpline is confidential, non-judgmental, and available in 16+ languages. 9100 181 181.

CARD 39 — START NOW
The Best Time Was When You First Noticed. The Second Best Time Is Right Now.
"This protocol is clinically validated, evidence-linked, and consortium-reviewed by India's most experienced multi-disciplinary paediatric therapy team. 70+ centres. 20M+ sessions. 97%+ measured improvement. We know what works."
🖐 OT
Occupational Therapy
💬 SLP
Speech-Language Pathology
🧠 ABA/BCBA
Behaviour Analysis
📚 SpEd
Special Education
🏥 NeuroDev
Neurodevelopmental Paediatrics
👶 Dev Paeds
Developmental Paediatrics
📞FREE National Autism Helpline: 9100 181 181 | 16+ languages | 24×7 | pinnacleblooms.org
Preview of 9 materials that help with fecal smearing prevention Therapy Material
Below is a visual preview of 9 materials that help with fecal smearing prevention therapy material. The pages shown help educators, therapists, and caregivers understand the structure and content of the resource before use. Materials should be used under appropriate professional guidance.




















Share this resource
Help others discover thisLink copied!

CARD 40 — THE PINNACLE PROMISE
From Fear to Mastery. One Technique at a Time.
Pinnacle Blooms Network® exists for one reason: to ensure that no family — regardless of income, location, or language — faces their child's developmental challenge without the world's best evidence, the world's best materials, and the world's best consortium of specialists standing behind them.
We are built by mothers who know what it is to sit on a bathroom floor at 4 AM, hands in rubber gloves, tears on their faces, wondering why nobody ever told them about any of this.
This is why we built GPT-OS®. This is why 70,000+ technique pages are being built. This is why this page exists.
You came here afraid. You leave here informed, equipped, and connected to a system that will not let you navigate this alone.
Return to Top — Card 01
Re-read the recognition moment with fresh eyes
Next Technique: E-509
Resistance to Toothbrushing — techniques.pinnacleblooms.org/toileting-hygiene/toothbrushing-resistance-E509
Browse All Toileting & Hygiene Techniques
techniques.pinnacleblooms.org/toileting-hygiene
Back to Pinnacle Blooms
techniques.pinnacleblooms.org
CIN: U74999TG2016PTC113063 · DPIIT: DIPP8651 · MSME: TS20F0009606 · GSTIN: 36AAGCB9722P1Z2
This content is educational and does not replace individualised assessment and intervention by qualified behavioural specialists, occupational therapists, physicians, and developmental professionals. Persistent fecal smearing requires professional evaluation to identify underlying function and rule out medical causes. Seek professional help for assessment and intervention. Individual results may vary. Statistics represent aggregate outcomes across the Pinnacle Blooms Network.
© 2025 Pinnacle Blooms Network®, unit of Bharath Healthcare Laboratories Pvt. Ltd. All rights reserved. Technique E-508 | GPT-OS® Content Engine v2.1.0
📞FREE National Autism Helpline: 9100 181 181 | 16+ languages | 24×7 | pinnacleblooms.org
The loop closes. The journey continues. One technique at a time. → E-509
The loop closes. The journey continues. One technique at a time. → E-509
