
"Done!" They call out. Again. And you walk down the hall. Again.
Your child is nine. Maybe ten. Maybe older. And they still can't finish this on their own. Independent wiping is a skill. Not a character trait. Not willpower. A skill — and skills can be taught.
E-505 | Pinnacle Blooms Network®
Occupational Therapy Validated

ACT I — THE EMOTIONAL ENTRY
You Are Not Failing. Your Child's Motor Planning System Needs Targeted Support.
The underwear in the laundry tells the story. The avoided school bathroom tells another. The question — "Why doesn't my body work right?" — breaks something in you. You've demonstrated. Explained. Tried everything you know. And you're still stuck in this daily cycle that no parenting book prepared you for.
You are not failing. Millions of families are navigating this exact challenge. Independent wiping is a precision skill requiring the simultaneous coordination of six neurological systems — and your child's nervous system needs targeted, structured support to integrate them.
WHO Nurturing Care Framework (2018): Early identification of skill deficits and responsive parental action directly improve developmental outcomes. nurturing-care.org/ncf-for-ecd/

Card 02 — You Are Not Alone
Millions of Families Are Navigating This Exact Challenge Right Now.
1 in 36
Children with Autism
Diagnosed in the US (CDC 2023)
80%
Sensory Differences
of children with ASD show sensory processing differences affecting self-care
40–60%
Need Explicit Instruction
of children with developmental differences need explicit toileting hygiene instruction beyond age 6
Wiping independence is one of the most common — and least discussed — self-care challenges in paediatric occupational therapy. It is not rare. It is not your child being difficult. It is a skills gap that affects millions of children with autism, ADHD, developmental coordination disorder (dyspraxia), sensory processing differences, and intellectual disabilities worldwide.
In India, where Pinnacle Blooms Network® operates 70+ centres serving children from across 70 countries, this challenge appears in nearly every family's journey at some stage. You are among millions navigating this.
Citations: PRISMA Systematic Review (2024): PMC11506176 | World J Clin Cases Meta-analysis (2024): PMC10955541

Card 03 — Brain & Body
This Is a Motor Planning and Sensory Processing Challenge. Not a Behaviour Problem.
Independent wiping requires the simultaneous coordination of six neurological systems. Understanding what's actually happening in your child's brain and body changes everything — including how you approach support.
Motor Planning (Praxis)
The brain must sequence a multi-step action — reach, position, wipe, check, repeat — without being able to see the target area. Children with dyspraxia struggle to plan unfamiliar motor sequences.
Fine Motor Control
Gripping and tearing toilet paper, maintaining grip during wiping, modulating pressure — these require precise finger and hand muscle coordination that many children haven't yet consolidated.
Gross Motor Reach
Reaching behind and underneath the body while maintaining seated balance requires significant shoulder mobility and trunk rotation — genuinely difficult for children with hypotonia or low muscle tone.
Proprioceptive Processing
The sense that tells you where your arm is in space without looking. Reduced proprioceptive awareness means the arm goes in the wrong direction or applies incorrect pressure.
Tactile Discrimination
The sensory signal that tells you "you're clean now." When interoceptive and tactile feedback is impaired, this signal doesn't register — leading to under-wiping or endless wiping.
Executive Sequencing
Remembering the order of steps, self-monitoring completion, deciding when to stop. Children with ADHD and autism frequently struggle with multi-step executive sequences.
"This is not a child who won't wipe. This is a child whose nervous system hasn't yet integrated all six systems required for independent wiping." — Pinnacle Blooms Network® OT Consortium
Citation: Frontiers in Integrative Neuroscience (2020): Comprehensive neurological framework for sensory processing treatment in ASD. DOI: 10.3389/fnint.2020.556660

Card 04 — Developmental Timeline
Typical Timeline: Ages 4–6. Your Child's Timeline: Different. Both Are Real.
WHO and UNICEF developmental guidelines establish age 4–6 as the typical window for wiping independence — but these are population medians, not individual mandates. Children with autism, ADHD, developmental coordination disorder, sensory processing differences, or intellectual disabilities frequently fall in the extended learning range of ages 6–12 and beyond.
Neurotypical Children
Often acquire wiping through observation and minimal instruction — the six neurological systems integrate with little explicit support.
Children with Developmental Differences
Require explicit, systematic instruction targeting the specific skill components they struggle with. The path is different — not absent.
Commonly co-occurring conditions: Autism Spectrum Disorder | ADHD | Developmental Coordination Disorder (Dyspraxia) | Sensory Processing Disorder | Hypotonia | Intellectual Disability | Anxiety
Citations: WHO Care for Child Development Package (2023) | UNICEF MICS developmental monitoring indicators | PMC9978394

Card 05 — The Evidence
This Is Not Guesswork. This Is Occupational Therapy Science Applied at Home.
LEVEL I — SYSTEMATIC REVIEW SUPPORTED
Study | Key Finding | Source | |
PRISMA Systematic Review (2024) | 16 articles confirm sensory integration therapy is evidence-based practice for ASD | PMC11506176 | |
Meta-analysis, World J Clin Cases (2024) | Sensory integration therapy improves adaptive behaviour, motor skills, and self-care across 24 studies | PMC10955541 | |
Indian RCT, Indian J Pediatrics (2019) | Home-based sensory interventions with parent delivery show significant outcomes | DOI:10.1007/s12098-018-2747-4 | |
AOTA Practice Guidelines | OT-led ADL intervention including toileting hygiene is evidence-based and recommended for paediatric populations | aota.org | |
NCAEP (2020) | Task analysis and visual supports are evidence-based practices for autism | NCAEP 2020 Report |
"Clinically validated. Home-applicable. Parent-proven. Backed by 20M+ therapy sessions at Pinnacle Blooms Network®."

ACT II — THE KNOWLEDGE TRANSFER
Technique E-505: The Independent Wiping System
What It Is
A structured, OT-informed approach to building independent toilet hygiene in children who struggle with the motor planning, sensory processing, fine motor, or sequencing demands of wiping.
How It Works
Adaptive tools immediately reduce barriers. Visual supports scaffold the cognitive sequence. Systematic skill-building progressively builds motor independence — targeting whatever specific component is blocking the child.
When & Where
Every toileting event becomes a natural practice opportunity. Used at home, school, and community settings. Ages 4–12 with adaptations for older children.
🏷️ Domain
Toileting / Self-Care / ADL
🏷️ Type
Adaptive + Remedial + Skill-Building
🏷️ Age Range
4–12 years (with adaptations for older)
🏷️ Session
Every toileting event (natural practice)
Citation: American Occupational Therapy Association (AOTA): OT for activities of daily living (ADLs) is evidence-based practice for children with developmental differences. aota.org

Card 07 — Who Uses This Technique
This Technique Crosses Therapy Boundaries — Because the Brain Doesn't Organise by Therapy Type.

🏥 Occupational Therapy (Primary Lead)
OTs conduct the comprehensive ADL assessment — identifying which of the six skill components is the primary barrier for this child. They prescribe adaptive equipment, therapeutic positioning, and the systematic skill-building programme, and provide hands-on parent training.

🧠 ABA / Behavioural Therapy (Secondary)
BCBAs build the systematic skill-acquisition programme: task analysis breaking wiping into teachable steps, forward or backward chaining, reinforcement schedules to motivate practice, and data collection to track progress objectively.

🗣️ Speech-Language Pathology (Supportive)
SLPs address the cognitive-linguistic dimension: understanding and following multi-step sequences, vocabulary for body awareness and hygiene, social scripts for requesting help appropriately, and visual schedule comprehension.

📚 Special Education (Supportive)
Special educators integrate toileting hygiene into daily living skills curricula, create IEP goals for self-care independence, coordinate school bathroom accommodations, and ensure consistent support across educational settings.
For a multi-disciplinary assessment: 9100 181 181 | FREE
Card 08 — What This Targets
Independent Wiping Is a Precision Skill. This System Targets the Exact Barriers Blocking Your Child.
Observable Behaviour Indicators
✅ Attempts wiping independently without calling for help
✅ Uses appropriate amount of toilet paper
✅ Performs front-to-back direction correctly
✅ Visually checks paper and repeats until clean
✅ Completes routine at school and unfamiliar bathrooms
✅ Reports confidence with sleepovers and overnight activities
Citation: Meta-analysis (World J Clin Cases, 2024): Sensory integration and adaptive OT interventions improve adaptive behaviour, motor skills, and self-care functional independence across 24 studies. PMC10955541

Card 09 — The 9 Materials
9 Materials That Address the 9 Different Reasons Children Struggle with Independent Wiping.
Most children need only 2–3 of these. Your OT identifies which ones. Here they all are.

Material 1 of 9
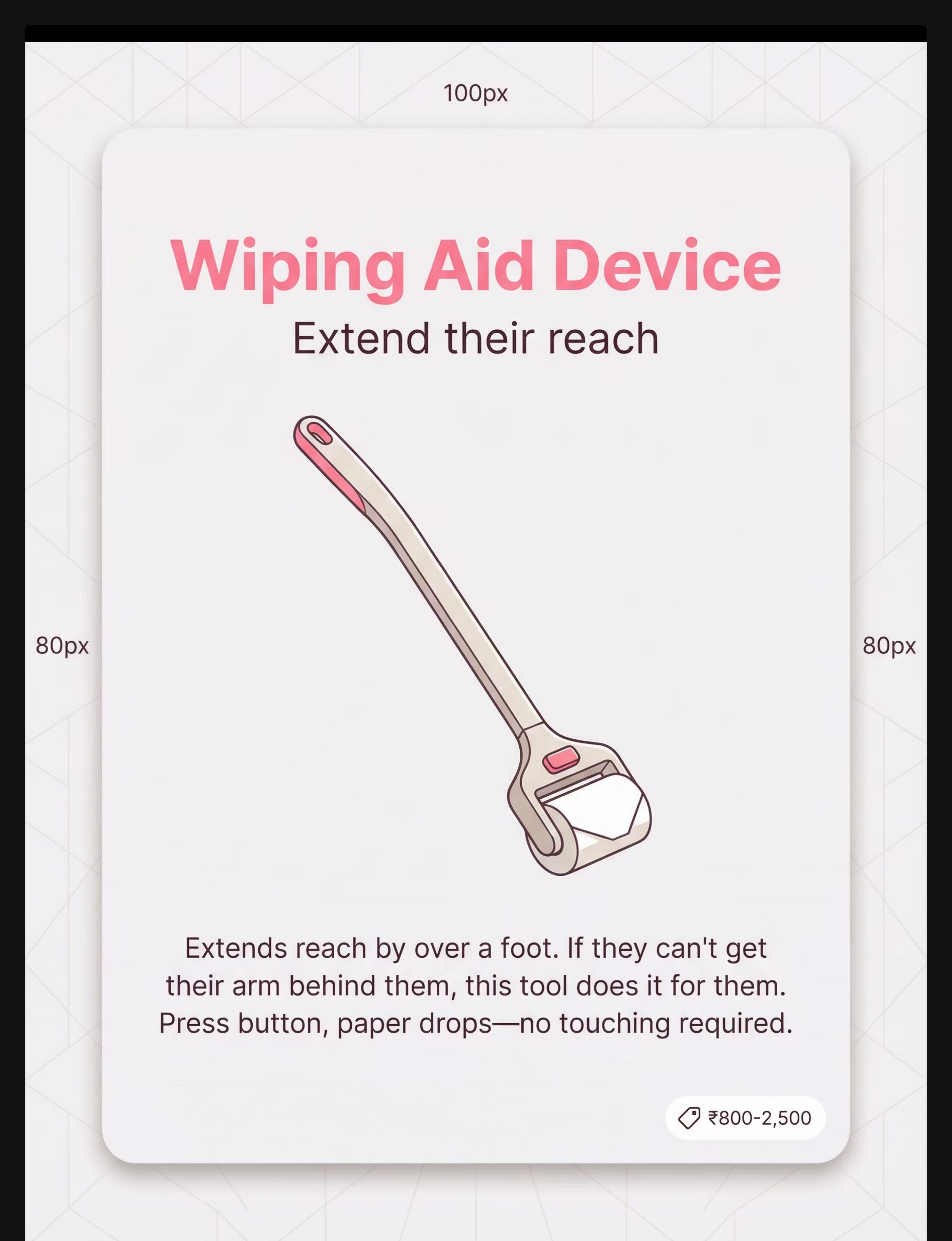
Wiping Aid Device (Toilet Paper Aid)
📌 Addresses
Reach Barrier
💰 Cost
₹800–2,500
A long-handled device (30–45cm) that holds toilet paper and includes a button-release mechanism. Extends reach by 30–45cm, eliminating the need to reach behind the body. The child approaches from front or side. No touching required.
This single tool removes the gross motor reach barrier entirely — making it the most impactful first material for children whose primary barrier is shoulder mobility or trunk rotation.
Search: "toilet paper aid India" on Amazon.in
Material 2 of 9
Flushable Wet Wipes (Sensitive / Unscented)
📌 Addresses
Cleaning Effectiveness + Sensory Feedback
💰 Cost
₹200–600/month
Fragrance-free, sensitive-skin flushable wipes. The moisture provides more effective cleaning with less effort and delivers clearer tactile feedback — the child can more easily detect when they are clean.
Ideal for children who struggle to get clean with dry paper due to motor coordination difficulties or reduced tactile discrimination. The wet sensation provides a more legible sensory signal of contact and cleanliness.
Search: "flushable wet wipes unscented India" on Amazon.in

Material 3 of 9
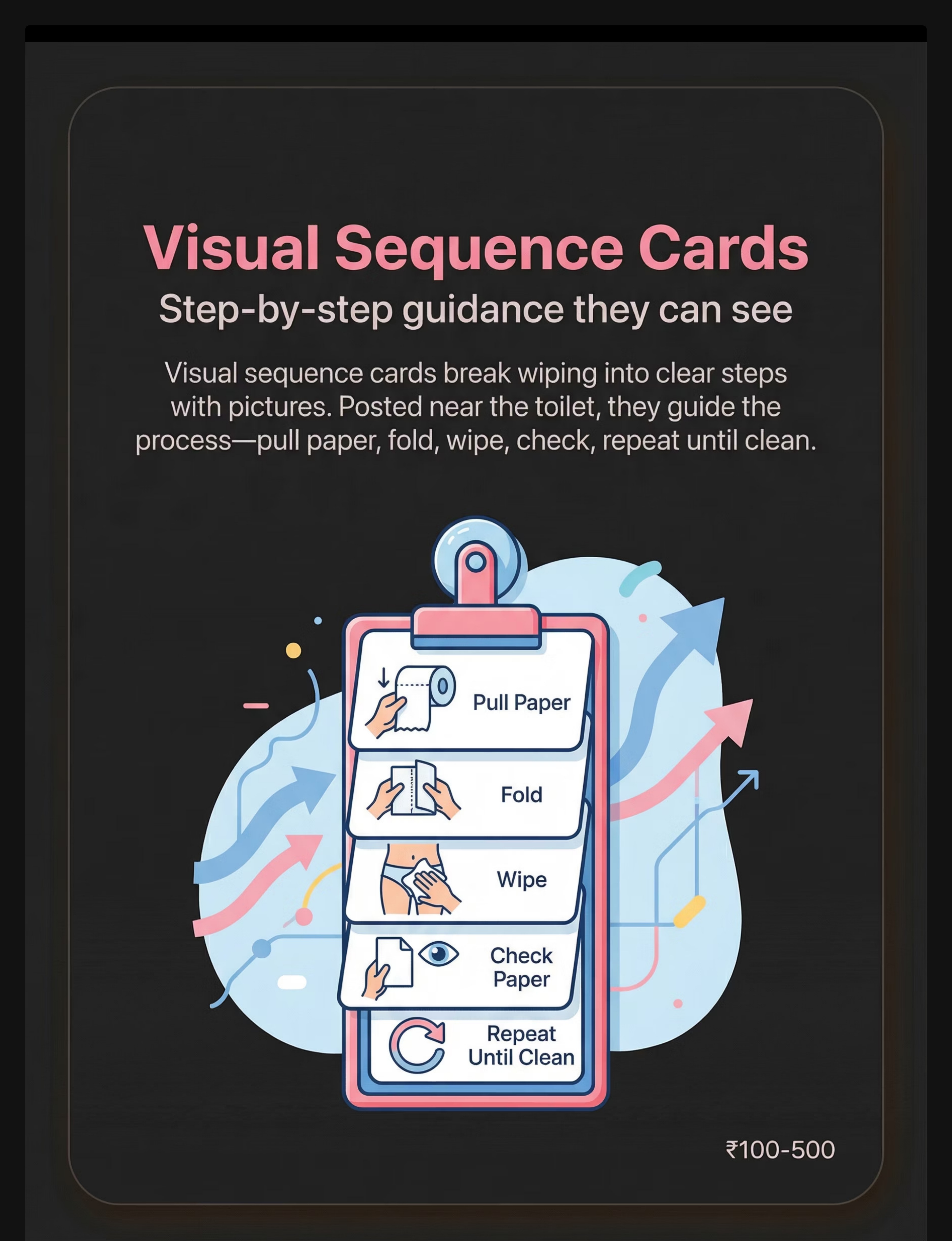
Visual Step-by-Step Wiping Sequence Cards
📌 Addresses
Executive Sequencing / Memory
💰 Cost
₹100–500
Laminated picture cards showing each step: Pull paper → Fold → Reach → Wipe front-to-back → Check paper → If dirty repeat → If clean, stand → Flush → Wash hands. Posted at child's eye level near the toilet.
This externalises the executive sequence completely — removing the demand for the child to hold all steps in working memory simultaneously. The routine of looking at the cards must be explicitly taught.
Search: "visual schedule cards toilet" on Amazon.in

Material 4 of 9
Toilet Paper Amount Guide (Visual Marker)
📌 Addresses
Paper Quantity Management
💰 Cost
₹50–300 (or free DIY)
Coloured tape on wall marking "pull to here," a marked toilet paper holder, or a container of pre-folded paper stacks (3–4 squares each). Removes the abstract "use enough paper" demand entirely.
For children with executive function deficits, the instruction "use enough paper" is meaningless. A concrete visual reference transforms an impossible judgement into a simple match task — pull paper until it reaches the red line.
DIY option: Coloured tape from any hardware store. ₹50.

Material 5 of 9
Practice Doll for Technique Training
📌 Addresses
Motor Learning / Body Awareness
💰 Cost
₹300–1,500
Any basic doll used for wiping motion practice outside the toilet. Apply washable marker or play-dough to simulate residue. The child practises reach, wipe direction, paper check, and repeat — when they CAN see what they're doing.
This is transformative because it removes the hardest part of in-toilet learning (the child cannot see the area they're cleaning). Doll practice builds the motor programme in a visible, low-pressure context before transferring to the real situation.
Search: "practice doll basic" on Amazon.in

Material 6 of 9
Bidet Attachment or Portable Bidet Sprayer
📌 Addresses
Motor Coordination Barrier (alternative method)
💰 Cost
₹1,500–8,000
Attaches under existing toilet seat, connects to water supply — no electricity needed. Water does the cleaning; paper only pat-dries. Reduces the complex wiping motion to a simple drying task.
For children who cannot master traditional wiping technique due to motor planning barriers, the bidet represents a dignified, permanent independence solution — not a workaround. Water cleans; the child needs only to pat-dry, a far simpler motor task. In Indian homes, a hand-held lota/mug of water is an excellent zero-cost equivalent.
Search: "bidet toilet attachment India" on Amazon.in

Material 7 of 9
Toilet Footstool + Positioning Supports
📌 Addresses
Postural Stability / Reach
💰 Cost
₹500–3,000
A sturdy, slip-resistant footstool grounds feet for stability during wiping. A raised toilet seat or toilet frame with armrests provides something to hold while reaching.
When the body is unstable, the brain dedicates all its motor resources to maintaining balance — nothing is left for wiping. Grounding the feet and providing upper body support removes the balance demand entirely. When the body is stable, the arms can work.
Search: "toilet footstool children India" on Amazon.in

Material 8 of 9
Completion Check Tools (Light-Coloured Paper + Mirror)
📌 Addresses
Sensory Completion Awareness
💰 Cost
₹100–500
Light-coloured toilet paper shows residue more clearly. A small unbreakable mirror mounted near the toilet allows paper inspection. Visual rule: "White paper = done. Brown paper = wipe again."
For children whose tactile discrimination system doesn't reliably signal cleanliness, this tool replaces the absent internal signal with an external visual one. It transforms "am I done?" — an unanswerable question — into a simple, learnable visual check anyone can execute.
Search: "unbreakable bathroom mirror" on Amazon.in

Material 9 of 9
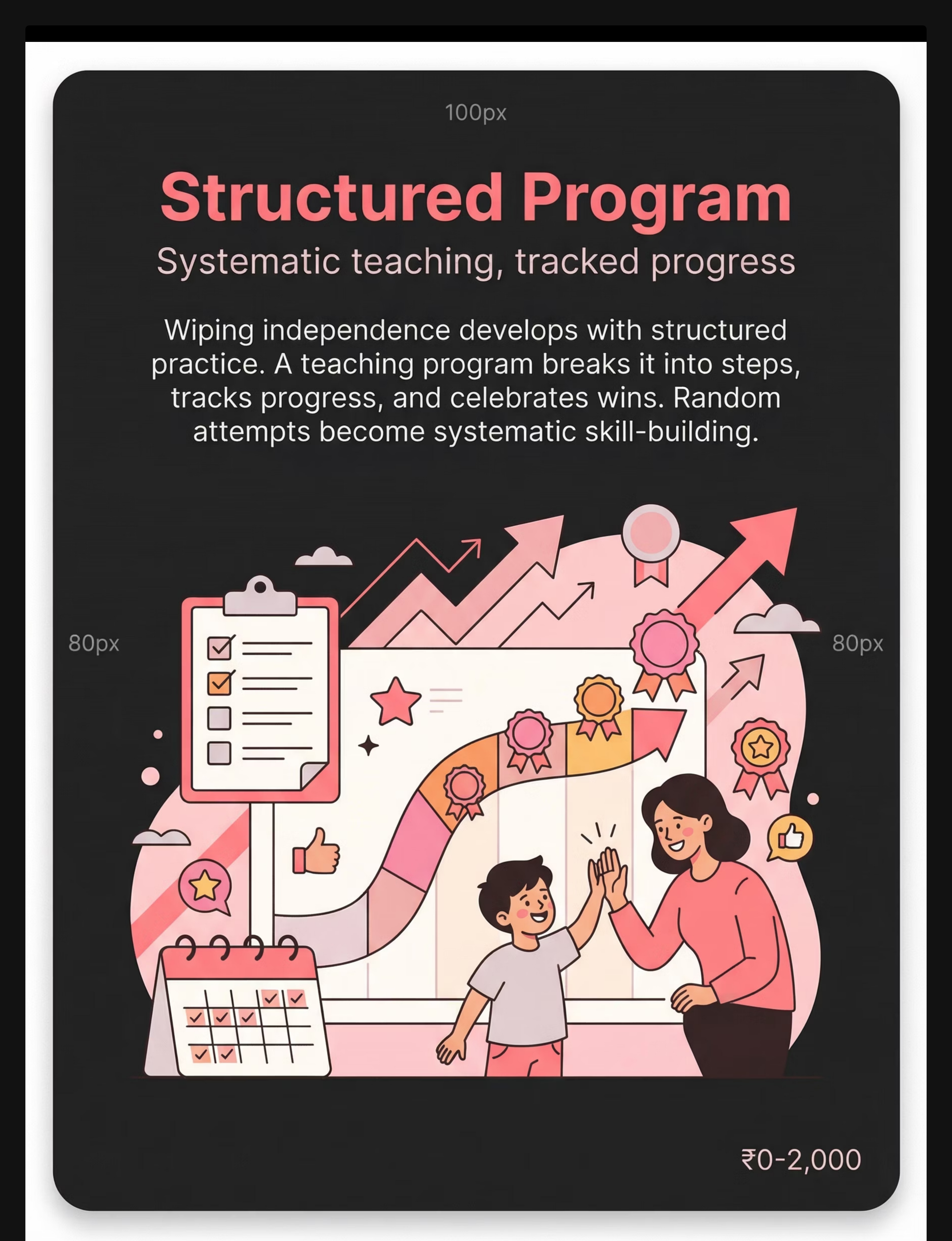
Structured Teaching Programme + Progress Tracker
📌 Addresses
Systematic Skill-Building
💰 Cost
₹0–2,000
Task analysis worksheet (steps of wiping), sticker/progress chart, prompting hierarchy reference. Transforms random attempts into a systematic forward or backward chaining skill-building programme.
Without documentation, progress is invisible. Without a structured programme, practice is inconsistent. The tracker and task analysis together turn daily toileting opportunities into a measurable, evidence-based skill-building curriculum. Download the Pinnacle Free Tracker to get started.
Pinnacle Recommends — Starter Kit for Most Families: Visual Sequence Cards + Paper Amount Guide + Wet Wipes + Positioning Support + Consistent Teaching Approach. Not all 9 materials are needed for every child. Your OT identifies the right 2–3 for your child. Materials guidance: 9100 181 181

Card 10 — DIY & Zero-Cost Substitutes
Every Material Has a Household Substitute. Your Child Can Start Today — Regardless of Budget.
Every family, regardless of economic access, can execute this technique with household items. The WHO/UNICEF Equity Principle underpins this: equivalent outcomes are achievable in low-resource settings.
Material | Buy Version | DIY / Free Substitute | |
Wiping Aid | ₹800–2,500 | Cardboard tube + tape-wrapped grip (temporary bridge); or teach standing wipe position | |
Wet Wipes | ₹200–600/mo | Damp soft cloth squares (washable), or small spray bottle of water beside toilet | |
Visual Cards | ₹100–500 | Hand-draw with stick figures on thick paper, laminate with packing tape, tape to wall | |
Paper Amount Guide | ₹50–300 | Coloured tape on wall: "Pull to red line" = right amount. Free with tape already at home | |
Practice Doll | ₹300–1,500 | Any stuffed toy or rolled blanket. Use chocolate spread or washable paint for simulation | |
Bidet | ₹1,500–8,000 | Small hand-held mug/lota of water (common in Indian homes) — child rinses, then pat-dries | |
Footstool | ₹500–3,000 | Stack of textbooks wrapped in non-slip mat. Stable plastic storage container (tested for weight) | |
Completion Check | ₹100–500 | Hold paper toward light source. White = done rule works with standard paper | |
Progress Tracker | ₹0–2,000 | Hand-draw grid on paper. Sticker chart from local stationery shop ₹20 |
Citation: WHO Nurturing Care Framework (2018): Context-specific, equity-focused interventions with household materials demonstrate equivalent outcomes in low-resource settings. PMC9978394 | WHO CCD Package (2023)

Card 11 — Safety First
Read This Before Every Session. 60 Seconds. Non-Negotiable.
🔴 RED — DO NOT PROCEED if:
Child has active skin irritation, rash, or open wounds in the perianal area | Child is showing significant distress, meltdown, or high anxiety | Child has expressed explicit fear or trauma associated with bathroom routines | Materials contain known allergens | Bidet water temperature has not been tested
🟡 AMBER — MODIFY if:
Child is tired, hungry, or slightly dysregulated (use simplified version) | Child resists doll practice (switch to alternative method) | Positioning support feels unstable (recheck all non-slip elements) | Child shows signs of constipation or discomfort (address medical issue first)
🟢 GREEN — PROCEED when:
Child has just had a bowel movement (ideal natural practice opportunity) | Child is calm, cooperative, and not in distress | All materials are within child's reach | Parent/caregiver is present and calm | Visual sequence cards are posted and visible
⚠️ STOP immediately if: Child becomes highly distressed or begins to cry | Signs of pain during practice | Complete shutdown or behavioural escalation | Any adverse skin reaction to materials
Critical Hygiene Safety: Always teach front-to-back wiping direction, especially for girls. Improper direction significantly increases UTI risk. This must be explicitly taught and consistently reinforced across ALL caregivers.
Citation: Indian Journal of Pediatrics RCT (2019): Safety protocols for parent-administered home sessions. DOI: 10.1007/s12098-018-2747-4
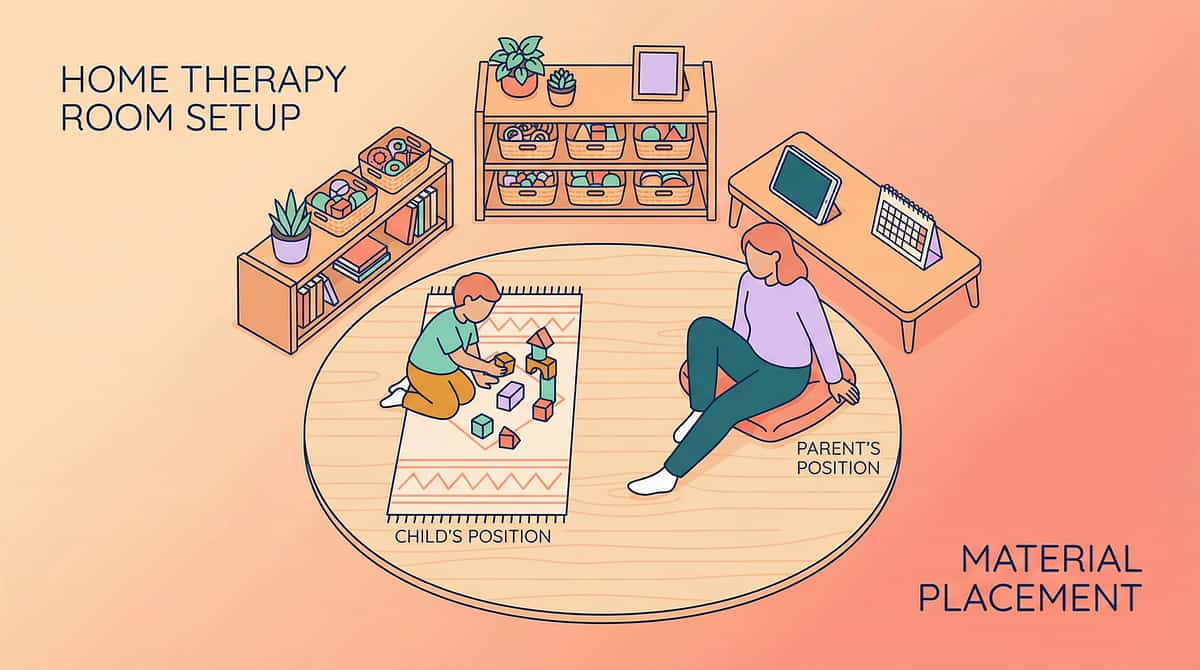
Card 12 — Set Up Your Space
Spatial Precision Prevents 80% of Session Failures. Set This Up Once. Use It Every Time.
A child cannot compensate for a poorly set-up environment. When the environment is wrong, the skill looks absent — but it's the setup that failed.
Visual Sequence Cards
Posted at child's eye level (not adult eye level) — left wall or directly behind toilet
Toilet Paper Roll
Within easy reach with paper amount guide (coloured tape) visible on roll
Wet Wipes Container
Accessible without standing, within arm's reach while seated on toilet
Footstool
Positioned so child's feet rest flat and firmly — non-slip surface essential
Wiping Aid
Within reach if using — placed on nearby surface at seated reach height
Non-Slip Mat
On floor around toilet base. All fragranced products removed if child has sensory sensitivities
Door Position
Partially closed for privacy — adult can assist if needed but space feels private
Progress Tracker
Accessible for post-session recording — ideally posted just outside or inside bathroom door
School/Teacher Note: Share this card with your child's school nurse or classroom aide. School bathroom setup matters equally. Use identical visual cards at school for consistent prompting.

ACT III — THE EXECUTION
Is Your Child Ready? Pre-Session Readiness Check
The best practice session is one that starts right. Check these indicators before each natural toileting opportunity.
Indicator | ✅ GO | ⚠️ MODIFY | ❌ POSTPONE | |
Recent meal | 2+ hrs since last meal | Slightly hungry | Clearly hungry/irritable | |
Emotional state | Calm, cooperative | Slightly distracted | Meltdown, highly anxious | |
Recent bowel movement | Just occurred | 30+ min ago | No BM opportunity | |
Physical health | Healthy | Mild tiredness | Illness, pain, skin irritation | |
Time available | 10+ minutes | 5–10 min (shorten) | Under 5 min (rushed) | |
Environment ready | Setup complete | Minor adjustments needed | Not set up |
✅ 5–6 Green
PROCEED with full protocol
⚠️ 3–4 Green
MODIFY — adult assists most steps, child does 1–2 independently
❌ Under 3 Green
POSTPONE — offer calming activity, try at next natural opportunity

Step 1 of 6
Step 1: Invite, Don't Command
"[Name], let's try the bathroom routine together. You're going to be the one doing the steps — I'll be right here. Let's look at our picture cards first."
Body Language Guidance
Position yourself at child's eye level or slightly below. Use a warm, matter-of-fact tone — not nervous, not loud. Hold up the visual sequence card as you speak. Give child 10–15 seconds to orient before any action.
What Resistance Looks Like & How to Modify
- Verbal refusal: "Okay. We'll do this when you're ready. Let's check in after [preferred activity]."
- Physical avoidance: Do NOT pursue. Wait for next natural BM opportunity.
- Partial engagement: Accept this as success. Try one step only.
ABA Principle — Pairing: The bathroom routine must be associated with predictability, calm, and success — not demand, pressure, or shame. Trust precedes skill.
Timing: 30–60 seconds | Helpline for parent coaching: 9100 181 181

Step 2 of 6
Step 2: Introduce the Material and the Sequence
The child is on the toilet following a bowel movement. Now introduce the material that addresses their primary barrier — starting with just one material, not all nine simultaneously.
If Using Wiping Aid
"Here's our helper tool. See how long it is? You don't have to reach all the way back — the tool does that. Let me show you first, then you try."
If Using Visual Sequence Cards
"Let's look at our steps. Step 1 says... [point to card]. Can you do that? Good. Now Step 2..."
If Using Wet Wipes
"We're going to use a wipe today. It's wet — it gets cleaner faster. Here's how we hold it..."
Offer material at child's natural reach — don't extend or force
Allow 5–10 seconds for child to orient to material before prompting action
Comment on the child's attempt, not the outcome: "You reached for the wipe — great start"
Child touching or holding material counts as engagement. Begin verbal praise immediately.
Timing: 1–3 minutes

Step 3 of 6
Step 3: Execute the Wiping Sequence — The Core 7-Step Protocol
Prompting Hierarchy — Fade Over Time
1
Hand-Over-Hand
Full physical guidance — adult hand covers child's hand completely
2
Partial Physical
Guide elbow, not full hand — child's hand is more independent
3
Gestural
Point to sequence card step — no physical contact
4
Verbal Only
"What's next?" — child looks to cards or memory
5
Visual Only
Child reads sequence cards independently — adult silent
Critical safety note — if child wipes back-to-front: Redirect immediately. "Oops — let's go the other way. Front to back." This is a hygiene safety issue, not just a technique error. Redirect calmly and consistently every single time.
Duration: 3–8 minutes depending on bowel movement and child's skill level
Step 4 of 6
Step 4: Practice Dosage and Variation
Natural practice > scheduled practice. Every bowel movement is a practice opportunity. Daily natural occurrence = ideal repetition frequency.
Weekly Practice Target
Natural BM opportunities: Use ALL of them (typically 1/day = 7 sessions/week)
Doll/model practice: 2–3 additional non-toilet sessions per week for technique training
School sessions: Aim to include school bathroom once daily if possible
Variation Methods to Maintain Motivation
- Backward chaining: Adult does all steps EXCEPT the last one. Child completes final step. Then last two. And so on.
- Forward chaining: Child masters Step A to independence. Then A+B. Then A+B+C.
- Alternate steps: Some days Step D "check"; other days steps A+B
- Vary materials: Alternate wet wipes and dry paper once technique begins generalising
"3 correct repetitions with genuine engagement > 10 forced attempts."
Step 5 of 6
Step 5: Reinforce Immediately and Specifically
ABA Gold Rule: Reinforcement must be immediate (within 3 seconds), specific (name what they did), and proportionate (match child's preferences).
For the Attempt
"You reached for the wipe all by yourself! That took courage."
For the Check Step
"You looked at the paper! That's exactly what our OT showed us. You did it."
For First Fully Independent Clean Check
"You just took care of yourself. By yourself. That is a HUGE deal. Remember this moment."
Reinforcement Menu — Select by Child Preference
☐ Verbal praise (always use, regardless of other reinforcers)
☐ Sticker on progress chart (visible, cumulative)
☐ Token toward preferred reward (defined by family)
☐ Special privilege (extra screen time, choice of activity)
☐ Physical affirmation (high five, fist bump — if preferred by child)
☐ Natural consequence: "Because you did this yourself, we have time for [preferred activity]"
NEVER: Comment negatively on residue or mess | Compare to siblings or peers | Withdraw reward for imperfect execution
Step 6 of 6
Step 6: Close the Session Intentionally
Never end abruptly. Abrupt endings create post-session dysregulation and resistance to future sessions. The cool-down transition is part of the protocol — not optional.
"Great work. You're all done with bathroom time. Let's wash hands — and then [transition to preferred activity]."
Next Activity
Calm Input
Exit Together
All Done
Hand Wash
If child resists ending: "Two more, then we're all done." Use a visual timer if available — NCAEP evidence-based practice for autism.
Visual Timer Options: ₹200–500 (Time Timer® style) | or free phone timer with simple visual countdown | Citation: NCAEP (2020): Visual supports for transitions are evidence-based practice for autism.
Card 20 — Capture the Data
60 Seconds of Data. Weeks of Insight. Do This Before You Leave the Bathroom.
Progress in wiping independence is often invisible to parents in the moment. Data reveals what you can't see: "Last week child needed physical guidance on all 7 steps. This week, only steps 3 and 4." That's massive progress — invisible without documentation.
1
Date & Session Number
Record today's date and which session number this is (cumulative)
2
Independent Steps
Which steps did child complete independently? Paper → Fold → Reach → Wipe → Check → Repeat → Stand → Flush → Hands
3
Prompting Level Used
Full physical / Partial physical / Gestural / Verbal / Visual only / Independent
4
Resistance Level
Rate 1–5 scale (1 = fully cooperative, 5 = significant refusal)
5
Today's Win
Free text — "First time used check step!" — one specific positive to record
GPT-OS® Integration: If your child is on a GPT-OS® Everyday Therapy Programme™, log this session in the app to update your child's Toileting Independence Readiness Index.
Card 21 — Troubleshooting
Every "Failure" Is Diagnostic Data. Here's What It's Telling You.
🚫 "Won't reach behind at all"
Root cause: Reach barrier (shoulder mobility, body awareness, fear)
Solution: Introduce wiping aid device (Material 1). Try standing wipe technique. Book OT assessment for shoulder/trunk rotation evaluation.
Solution: Introduce wiping aid device (Material 1). Try standing wipe technique. Book OT assessment for shoulder/trunk rotation evaluation.
🚫 "Wipes but never gets clean"
Root cause: Inadequate paper, poor pressure, motor coordination
Solution: Switch to wet wipes (Material 2). Review wiping motion with doll practice (Material 5). Ensure adequate paper amount (Material 4).
Solution: Switch to wet wipes (Material 2). Review wiping motion with doll practice (Material 5). Ensure adequate paper amount (Material 4).
🚫 "Uses half a roll every time"
Root cause: Paper quantity executive function deficit / no completion awareness
Solution: Paper amount guide (Material 4). Teach and practise "check the paper" rule (Material 8). Pre-fold paper stacks.
Solution: Paper amount guide (Material 4). Teach and practise "check the paper" rule (Material 8). Pre-fold paper stacks.
🚫 "Wipes once and considers done"
Root cause: Sensory discrimination deficit — can't feel whether clean
Solution: Intensive completion check training (Material 8). Doll practice with chocolate/marker simulation of dirty/clean paper inspection.
Solution: Intensive completion check training (Material 8). Doll practice with chocolate/marker simulation of dirty/clean paper inspection.
🚫 "Completely refuses / meltdown at suggestion"
Root cause: Anxiety, past shame experiences, sensory overload
Solution: Go entirely back to doll practice. Re-establish trust and positive associations. Consider OT assessment for anxiety-based toileting avoidance. Do NOT force.
Solution: Go entirely back to doll practice. Re-establish trust and positive associations. Consider OT assessment for anxiety-based toileting avoidance. Do NOT force.
🚫 "Works at home, falls apart at school"
Root cause: Generalisation deficit, environmental differences, social anxiety
Solution: Replicate home setup at school (send visual cards). Request school accommodations. Begin active generalisation training with OT support.
Solution: Replicate home setup at school (send visual cards). Request school accommodations. Begin active generalisation training with OT support.

Card 22 — Personalise for Your Child
No Two Children Have the Same Wiping Barrier. Here's How to Personalise the Approach.
Easier Version | Standard | Harder Version | |
Adult completes all steps; child only does final "flush" | Child completes 3–4 steps with visual prompts | Child completes full sequence independently; introduce new bathroom environments | |
Pre-folded paper provided | Child tears from roll using amount guide | Child manages full roll independently | |
Wet wipes only | Wet wipe finish, dry paper for main | Dry paper only | |
Wiping aid for all sessions | Wiping aid for reach; attempt unaided at end | Fully unaided technique mastered |
Sensory Avoider (Tactile Hypersensitivity)
- Start with gloves for doll practice if direct paper contact is aversive
- Use softest available toilet paper or wet wipes
- Introduce materials slowly over multiple sessions
- Reduce bathroom sensory load (lower lighting, reduce noise)
Sensory Seeker (Reduced Tactile Sensitivity)
- Emphasise visual paper check — rely on sight not sensation
- Use completion check mirror
- Firm pressure during wiping (proprioceptive input)
- Practise "check 3 times" rule regardless of feeling clean
Age-Based Modifications
Ages 4–6
Doll practice primary. Adult does 90% of steps. Child does final check/flush only.
Ages 6–8
Forward chaining — add one step per 1–2 weeks of consistent practice.
Ages 8–12
Backward chaining often more motivating — end with achievement.
Ages 12+
Privacy paramount. Minimal adult involvement. Wiping aid + visual card independence focus.
ACT IV — THE PROGRESS ARC
Weeks 1–2: Building Trust, Not Mastery.
"In Weeks 1–2, you are planting. Not harvesting. Consistency of approach matters more than perfection of outcome. Every calm, non-shaming session deposits trust into the learning account."
✅ Child tolerates parent staying nearby during wiping attempt
Rather than insisting on full adult takeover — this is engagement and progress.
✅ Child looks at visual sequence cards without prompting
Self-initiated reference to the cards signals developing executive awareness.
✅ Child attempts Step A independently at least once
Even one independent paper grab is a neurological milestone worth recording.
✅ Reduced verbal protest compared to baseline
"I can't!" decreasing in frequency = building self-efficacy.
✅ Doll practice sessions completed 2–3 times without refusal
Tolerance of the practice setting predicts real-world skill transfer.
What is NOT expected yet: Independent completion of full sequence | Correct technique on first attempt | Consistent performance every session
Progress: ▓▓▓░░░░░░░░░░░░░░░░░15% — Trust phase in progress
Weeks 3–4 — Consolidation
Weeks 3–4: Neural Pathways Are Forming. Watch for These Signs.
✅ Child reaches for visual sequence card independently before being prompted
✅ Child verbalises or points to next step while on toilet ("Now fold it")
✅ At least 1–2 steps consistently independent (no prompts needed)
✅ Doll practice: child correctly models dirty/clean paper discrimination 80%+ of trials
✅ Reduced frustration and emotional dysregulation during sessions
✅ Child reports at least one successful independent step unprompted ("I did the wipe part!")
"In Week 3–4, you may notice you're more confident too. The panic of 'this will never work' is being replaced by 'I can see this moving.' Trust that."
When to increase intensity: if child consistently achieving 3+ steps independently → add next step in chaining sequence. If highly motivated → introduce brief school bathroom generalisation attempt.
Progress: ▓▓▓▓▓▓▓▓░░░░░░░░░░░40% — Neural consolidation phase

Weeks 5–8 — Skill Acquisition
Weeks 5–8: The Skill Is Forming. Real Independence Is Within Reach.
✅ Steps Achieved
Child completes 5–6 of 7 core steps independently
✅ Prompting Reduced
Down to visual cue only — child reads sequence card independently
✅ Direction Consistent
Front-to-back direction reliably executed without verbal correction
✅ Check Step Reliable
Paper check step executed before deciding complete
✅ Adult Confirmation Fading
Completion achieved without adult confirmation at least 50% of sessions
✅ Generalisation Begins
First independent session at school, grandparent's home, or unfamiliar bathroom
The hardest part isn't learning at home. It's using the skill in a different bathroom. The first successful independent wipe at school, a friend's house, or a relative's home is a developmental milestone equal in significance to first steps.
Progress: ▓▓▓▓▓▓▓▓▓▓▓▓▓▓░░░░░70% — Skill acquisition phase

Card 26 — Celebrate the Milestones
These Are Real Milestones. Celebrate Them Like It.
🏅 First Independent Step
"They reached for the paper themselves."
🏅 First Paper Check
"They looked at the paper and knew what to do."
🏅 First Complete Independent Wipe
"They did ALL the steps."
🏅 First School Bathroom
"They did it away from home."
🏅 First Sleepover
"They went and came back clean and confident."
🏅 Independence Master
"We don't need to help anymore."
"Your child being able to wipe themselves independently will change their life. Not metaphorically — literally. The shame they feel today will dissolve. The sleepovers they avoid will become normal. The school bathroom fear will become routine. Every single step you celebrate now is a brick in their foundation of dignity."
Parent reflection prompt: Write down your child's first independent success. The date. What they said. What you felt. You will want to remember this moment.

Card 27 — Red Flags
Some Children Need Professional OT Assessment. Here's When.
Age 8+ and Completely Dependent
No independent steps despite consistent home effort — comprehensive OT assessment required to identify specific neurological barriers.
6+ Weeks of Consistent Home Programme with No Progress
If measurable progress hasn't emerged after genuine consistent implementation, professional-led assessment will identify what's missing.
Known Motor or Developmental Differences Not Yet Assessed
Hypotonia, suspected DCD, or other motor differences require professional prescription of appropriate adaptive equipment and techniques.
Multiple Self-Care Areas Simultaneously Delayed
Wiping + dressing + eating + bathing all delayed simultaneously points to broader ADL skill profile requiring systematic multi-domain assessment.
Significant Behavioural Distress or Avoidance
Self-harm, extreme avoidance, or distress around toileting may indicate anxiety-based avoidance requiring clinical support beyond home techniques.
Chronic Physical Issues
Chronic skin problems, perianal rash, or recurrent UTIs from inadequate hygiene — or child avoiding bowel movements entirely (constipation risk is a serious medical concern).
What an OT Assessment Provides
- Comprehensive fine motor, gross motor, and sensory processing evaluation
- Identification of the specific neurological barriers for THIS child
- Prescription of appropriate adaptive equipment
- Systematic intervention programme with professional delivery
- School consultation and IEP goal recommendations
- Parent training programme
Access Professional Support
FREE OT Assessment Guidance:
📞 9100 181 181
📞 9100 181 181
Book AbilityScore® Assessment:
pinnacleblooms.org/assessment
pinnacleblooms.org/assessment
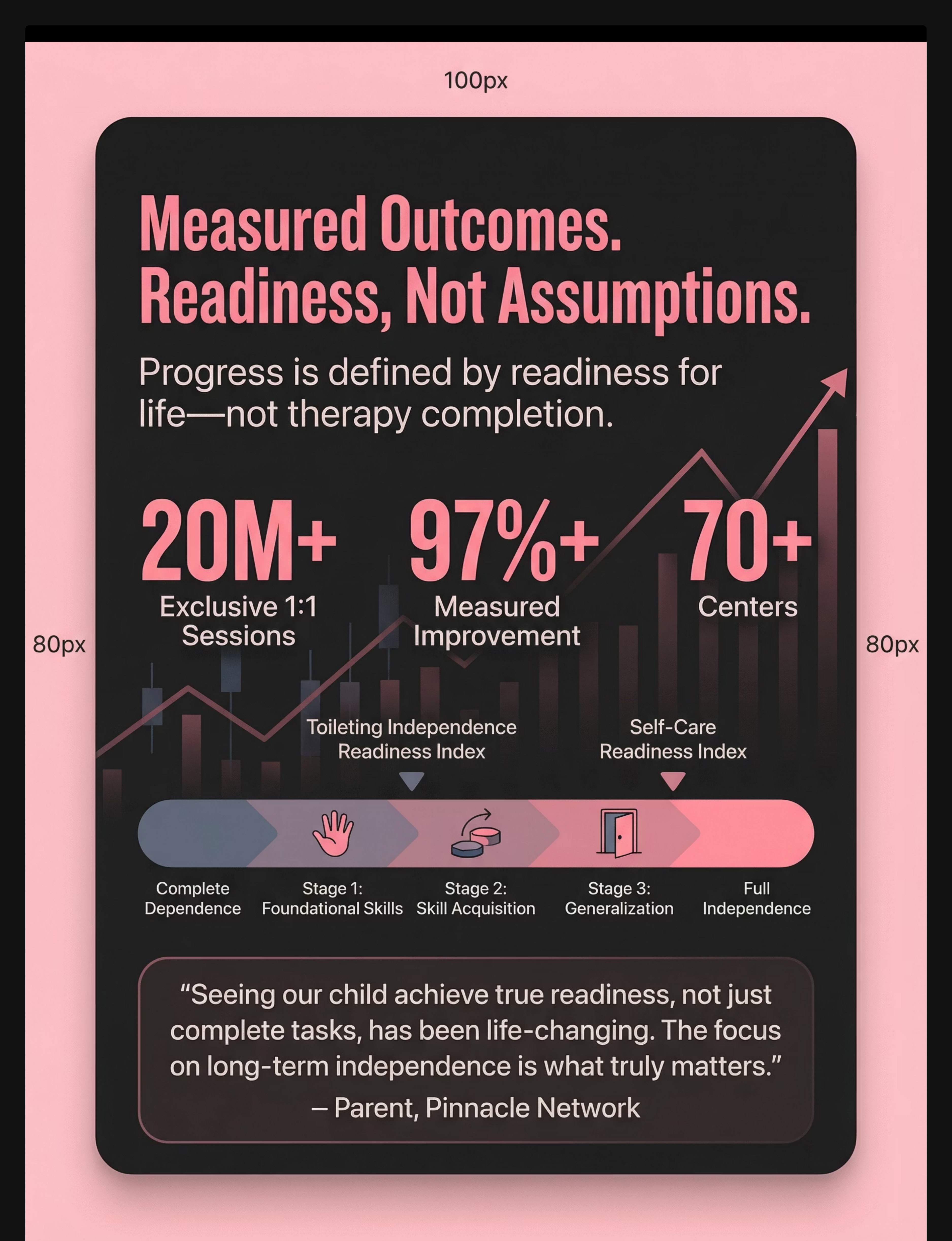
Card 28 — Your Progression Pathway
You Are Here. Here Is Where You're Heading. Here Is the Full Path.
Stage 1 — Complete Dependence
Adult does all wiping. Child is not yet participating in any step.
Stage 2 — Participation with Max Support
Child assists with 1–2 steps. Adult guides all others. Trust and pairing established.
Stage 3 — Adapted Independence
Independent with tools (wiping aid, wet wipes, visual cards). Dignified, complete outcome.
Stage 4 — Prompted Independence
Independent without tools at home. Visual cards may still be used. Adult present but not guiding.
Stage 5 — Full Independence
Independent in any setting — school, grandparents' home, camp, community bathroom. No prompts required.
Lateral alternatives if this path isn't working: Bidet method (bypass traditional wiping) | Standing wipe technique (if seated reach is the barrier) | OT-led intensive block programme (rapid skill acquisition approach)
Long-term goal: Full community participation — sleepovers, residential camps, independent school bathroom use, overnight trips — without wiping-related anxiety.

Card 29 — Related Techniques
Independent Wiping Is One Skill in a Self-Care Ecosystem. Here Are the Connected Techniques.

E-503 | School Bathroom Refusal
Domain: Toileting Anxiety | Difficulty: Core
"When they hold it all day and come home to a crisis."
"When they hold it all day and come home to a crisis."

E-504 | Toilet Training Resistance
Domain: Toilet Training | Difficulty: Intro
"Before wiping independence comes toilet training confidence."
"Before wiping independence comes toilet training confidence."

E-506 | Public Bathroom Avoidance
Domain: Community Toileting | Difficulty: Advanced
"When independence at home doesn't generalise to the outside world."
"When independence at home doesn't generalise to the outside world."

E-508 | Hand Washing Independence
Domain: Self-Care / Hygiene | Difficulty: Core
"The skill that immediately follows wiping. Build the full sequence."
"The skill that immediately follows wiping. Build the full sequence."
"You already have materials for these": Visual sequence cards work for ALL self-care sequences | Footstool useful for hand-washing reach too | Progress tracker template applies to all self-care skills
Preview of 9 materials that help with independent wiping Therapy Material
Below is a visual preview of 9 materials that help with independent wiping therapy material. The pages shown help educators, therapists, and caregivers understand the structure and content of the resource before use. Materials should be used under appropriate professional guidance.















Share this resource
Help others discover thisLink copied!

The Pinnacle Promise
"From fear to mastery. One technique at a time."
Every child deserves the dignity of independence. Every family deserves the knowledge to build it. Pinnacle Blooms Network® exists to close the gap between a clinical evidence base and a parent's home — one precise, scientifically-grounded technique at a time, at scale, for every family, in every language.
Medical Disclaimer: This page is educational and informational. It does not constitute individualised medical, occupational therapy, or behavioural advice. Persistent toileting hygiene difficulties may indicate underlying motor, sensory, or developmental conditions requiring professional evaluation. Individual outcomes vary based on child profile, baseline skills, and intervention intensity. Statistics represent aggregate outcomes across the Pinnacle Blooms Network®. Seek professional evaluation for persistent or severe concerns.
Browse full series: techniques.pinnacleblooms.org/self-care/toileting-series
CIN: U74999TG2016PTC113063 | DPIIT: DIPP8651 (Govt. of India) | MSME: TS20F0009606 | GSTIN: 36AAGCB9722P1Z2 | © 2025 Pinnacle Blooms Network®, unit of Bharath Healthcare Laboratories Pvt. Ltd. All rights reserved. | Built by Mothers. Engineered as a System.™
