
"You are not failing. Your child's nervous system is speaking. The gagging is real — it is involuntary, physiological, and neurological. Not a behavior. Not drama. Not manipulation. Your child deserves to breathe without fear, and that starts here."


"This is a wiring difference, not a behavior choice. Your child's brain is doing exactly what it's supposed to do when it detects danger — the difference is that the danger threshold is set far too low. Ordinary smells are being flagged as threats."

- Gustatory (taste) sensitivity — affecting food acceptance and nutrition
- Tactile over-responsivity — particularly around the face and mouth
- Anxiety — anticipatory anxiety about potential smell exposures
- Food refusal — smell-based rejection before any tasting occurs
- Social avoidance — withdrawing from environments where smells are present
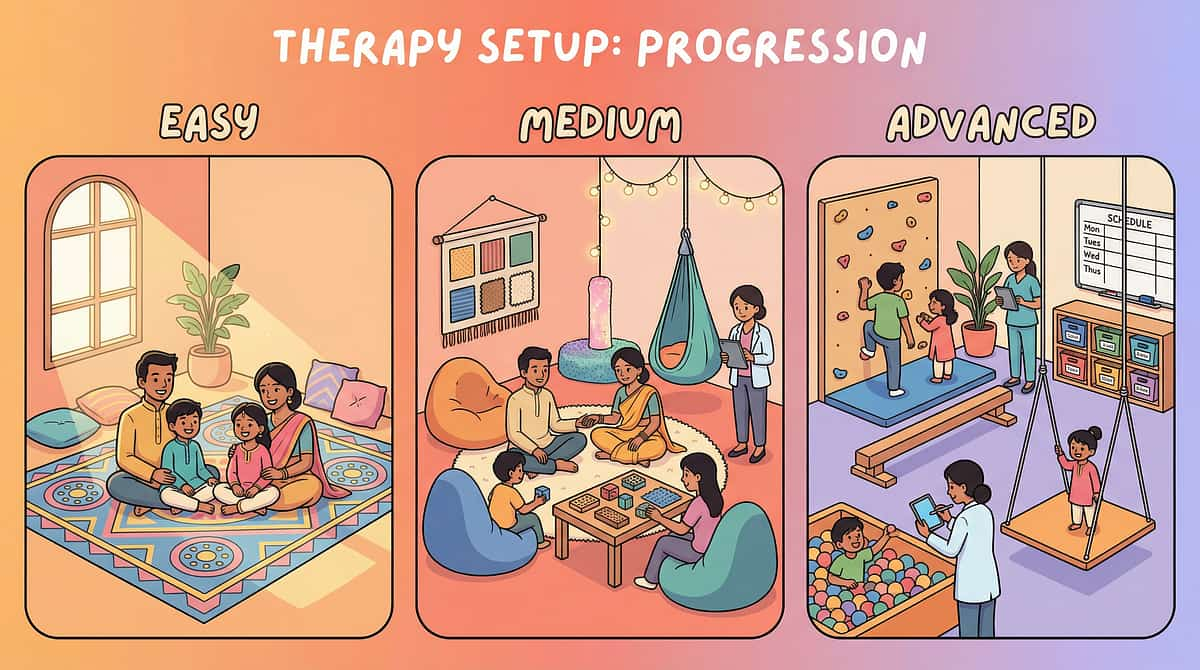
"From severe aversion → to managed sensitivity → to functional tolerance. This is a journey, not a single event. And your child's nervous system has the capacity to adapt when supported correctly."

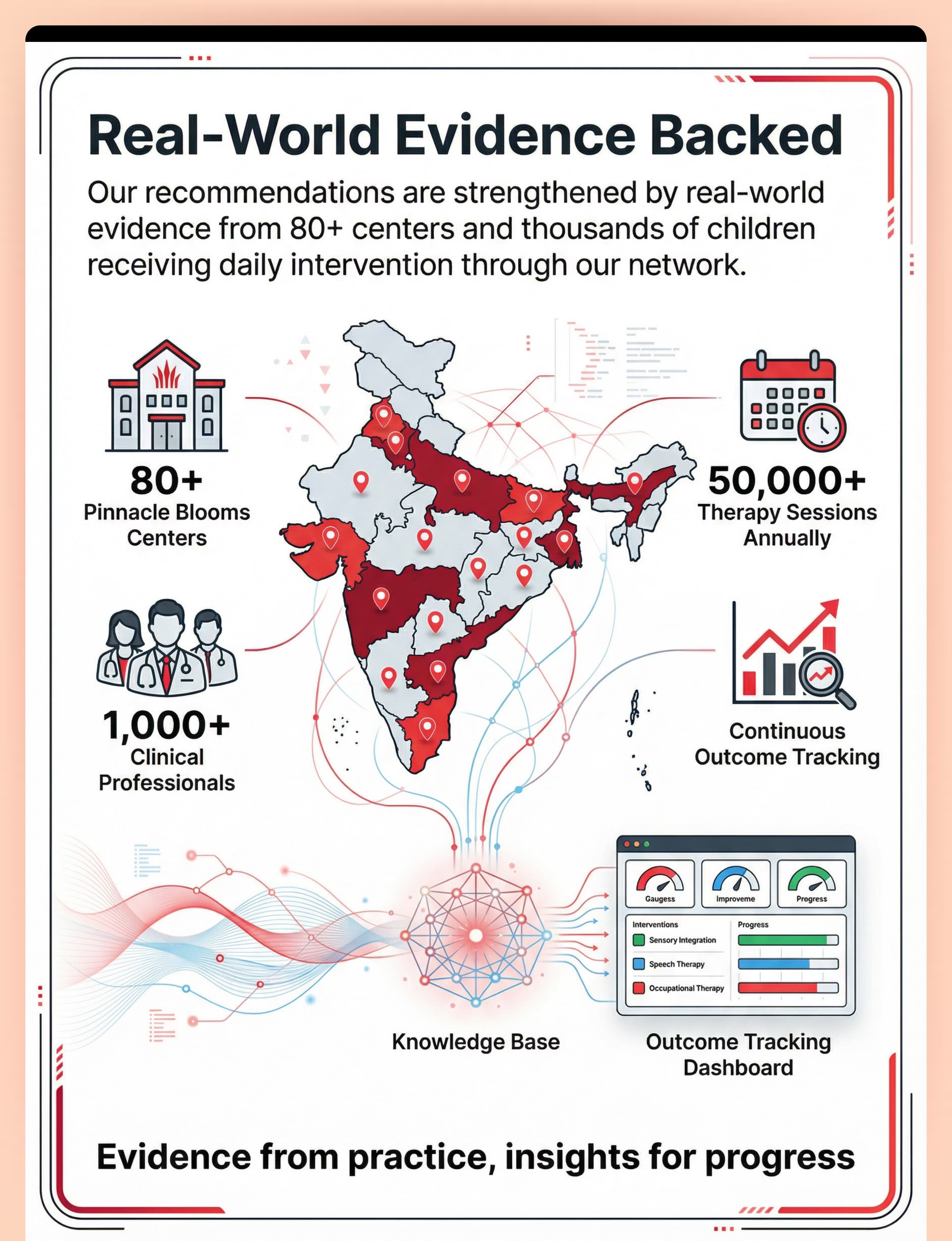
"Clinically validated. Home-applicable. Parent-proven. These are not experimental approaches — they are evidence-based strategies deployed across 70+ Pinnacle centers and refined through 20 million+ therapy sessions."






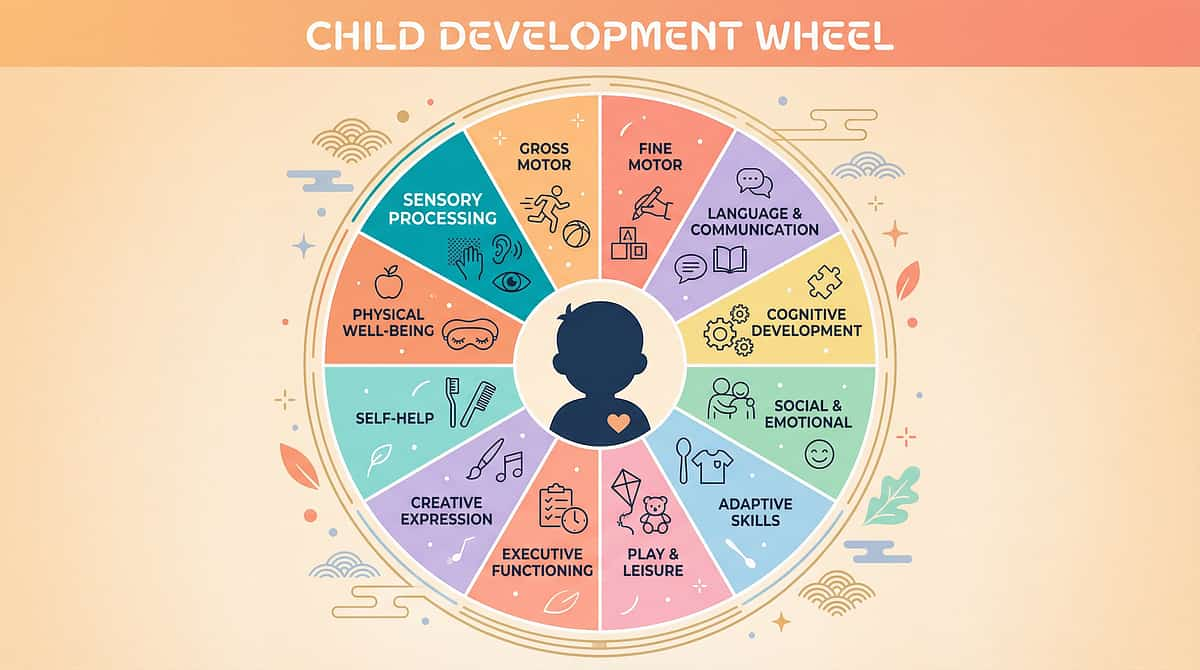
"This technique crosses therapy boundaries because the brain doesn't organize by therapy type. Your child's olfactory sensitivity affects feeding (SLP), daily participation (OT), behavioral patterns (ABA), and medical wellbeing (Pediatric). That's why Pinnacle's FusionModule™ coordinates all four disciplines into a single intervention pathway."
What This Targets — Precision Outcomes
🎯 Primary Targets (Core Skills) Reduction in gagging frequency when exposed to environmental smells Increased tolerance duration in challenging olfactory environments Successful use of protection strategies (masks, preferred scents, escape protocols) Expanded participation in previously avoided environments (cafeteria, kitchen, public spaces) 🔶 Secondary Targets (Related Improvements) Reduced anticipatory anxiety about potential smell exposures Improved food acceptance through smell-related feeding protocols Enhanced self-advocacy — the child can communicate their needs Decreased social avoidance and isolation 🟢 Tertiary Developmental Gains (Long-Term) Improved nutritional status through expanded food repertoire Increased school attendance and academic engagement Stronger social participation and peer relationships Greater family participation in outings, travel, and community events Enhanced emotional regulation and self-confidence Observable Behavior Indicators: Parents — watch for these: child enters a previously avoided room even briefly, child uses their scent bracelet independently, child communicates "I need to leave" instead of melting down, child tolerates a meal environment for longer than baseline. Research Evidence: Meta-analysis (World J Clin Cases, 2024): Sensory integration therapy effectively promoted social skills, adaptive behavior, sensory processing, and motor skills across 24 studies. 📎 Reference: PMC10955541

🏷️ Canon: Sensory Regulation Tools
💰 ₹300–1,500
🏷️ Canon: Aromatherapy/Scent Kit
💰 ₹200–800
🏷️ Canon: Environmental Modification
💰 ₹3,000–15,000
🏷️ Canon: Environmental Modification
💰 ₹200–800
🏷️ Canon: Aromatherapy/Scent Kit
💰 ₹500–2,000
🏷️ Canon: Visual Schedules
💰 ₹100–400
🏷️ Canon: Sensory Tent/Calm Space
💰 ₹500–3,000
🏷️ Canon: Deep Pressure + Breathing Tools
💰 ₹500–3,000
🏷️ Canon: Communication Cards
💰 ₹100–300

Material | Buy This | Make This (₹0 Cost) | |
Scent Shield | Activated Charcoal Mask (₹300–1,500) | Layer a regular cloth mask with a charcoal insert from aquarium supplies. Dab child-approved essential oil on mask exterior. | |
Aromatherapy Bracelet | Lava Bead Bracelet (₹200–800) | One drop of preferred essential oil on a cotton ball in a small container, or corner of a handkerchief. Refresh daily. | |
Air Purifier | HEPA+Carbon Purifier (₹3,000–15,000) | Open windows for cross-ventilation. Use baking soda bowls in key rooms. Cook with exhaust fan on and kitchen door closed. | |
Fragrance-Free Products | Full product swap (₹200–800) | Audit products for fragrances. Start with items touching child's skin: unscented soap, rinse clothes twice, avoid fabric softener. | |
Desensitization Kit | Graded Scent Jars (₹500–2,000) | Work with OT. Create scent hierarchy: sealed container at distance → very diluted scent → gradual approach. Child controls pace. | |
Visual Schedule | Printed Schedule Cards (₹100–400) | Hand-draw a daily smell schedule on paper. Use clock symbols for cooking, cleaning, outings. Give 10-minute advance warning. | |
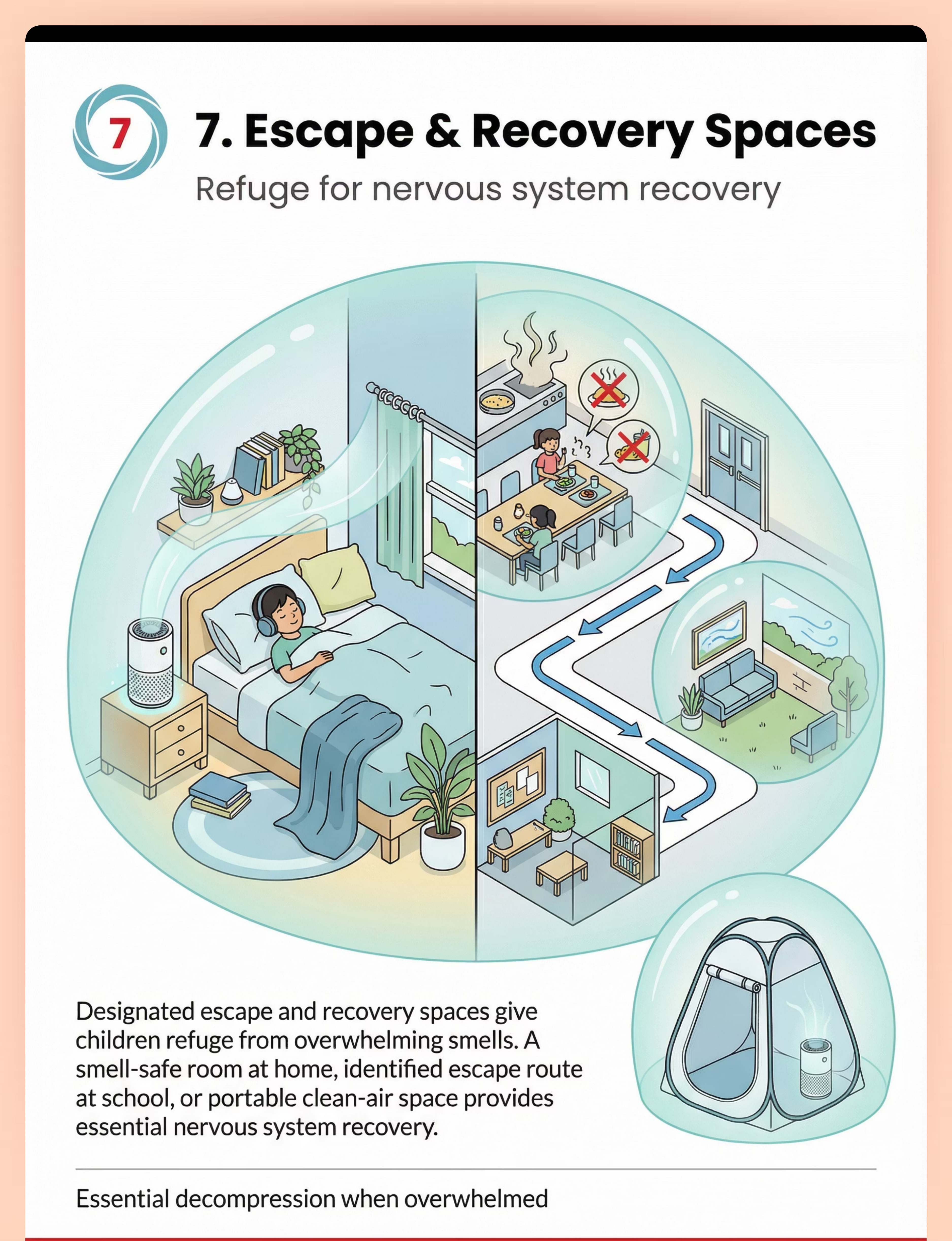
Escape Space | Pop-Up Tent Kit (₹500–3,000) | Designate child's bedroom as smell-safe sanctuary. Remove all scented products. Keep window crackable. Add calming items. | |
Calming Tools | Weighted Blanket (₹500–3,000) | Deep pressure: tight hugs, heavy blanket from home. Breathing: bubble breaths, counted exhales. Heavy work: wall pushes. | |
Communication Cards | Printed Card Set (₹100–300) | Write on an index card: "I have smell sensitivity. Some smells make me feel very sick. I may need to step away." |

- Child is experiencing active vomiting (not gagging) — seek medical evaluation
- Child has unexplained weight loss or failure to thrive
- Signs of dehydration from frequent vomiting episodes
- Smell sensitivity is of sudden new onset (may indicate neurological issue)
- Known GERD, cyclical vomiting, or GI condition not medically managed
- Child shows other new neurological symptoms alongside smell sensitivity
- Significant anxiety component — pair with anxiety management first
- Tactile sensitivity to masks — trial mask wear during calm times first
- Child in a heightened anxiety state — use protection-only, no desensitization
- Some "unscented" products still have chemical smells — trial individually
- New materials may have their own smell — air out 24+ hours before use
- Medical causes ruled out or being managed
- Child is in a regulated emotional state
- Parent has identified specific smell triggers and can describe intensity
- Materials pre-tested for child acceptability
- Escape route identified and accessible
- Child is not hungry, tired, or recently stressed
- Essential oils: Never apply undiluted to skin. Keep away from eyes. Some oils not safe for children under 6 — verify with pediatrician.
- Charcoal masks: Ensure proper fit and breathing space. Child should never feel restricted.
- Air purifiers: Choose ozone-free models. Some units produce motor sounds — consider auditory sensitivity.
- Desensitization: NEVER force exposure. Professional guidance essential. Some children sensitize (worsen) rather than desensitize — monitor carefully.
RED LINE: "Stop immediately if: gagging intensifies to repeated vomiting, child becomes severely distressed and cannot be calmed, child develops new physical symptoms, or child's food intake drops significantly. Trust your instincts — if something feels wrong, pause and ask."
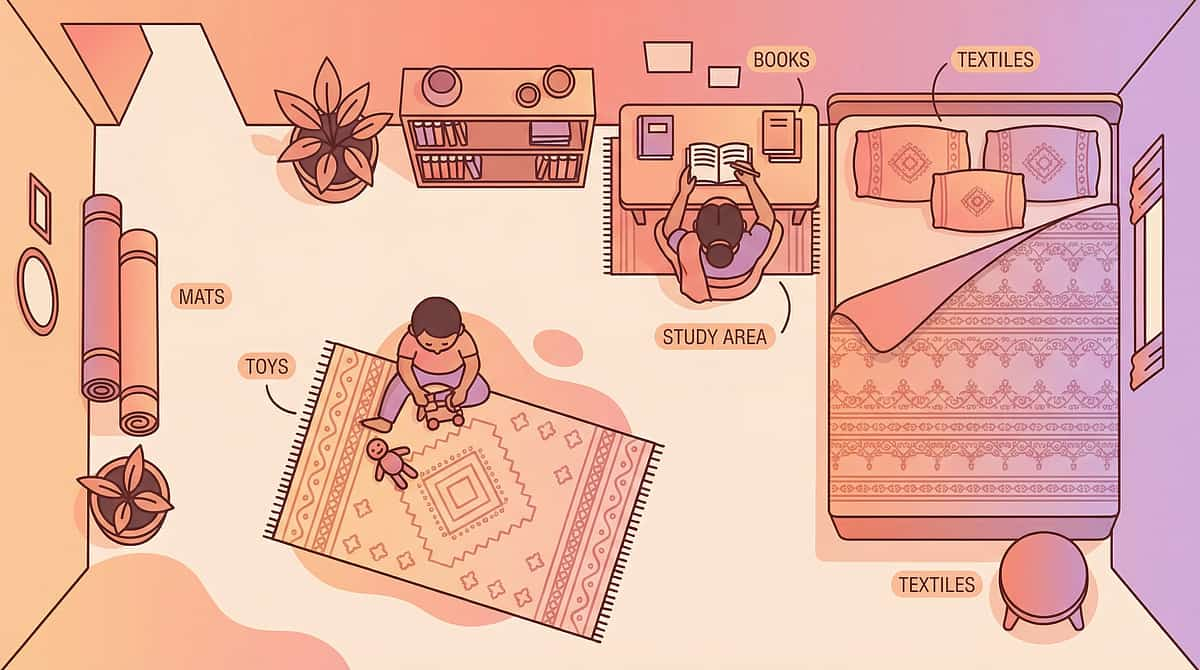
- Provide a letter to the teacher explaining olfactory sensitivity
- Request seating away from cafeteria doors, cleaning supply storage, and bathrooms
- Establish standing permission to leave to a pre-identified clean-air space
- Provide the child's portable protection kit (mask, scent tool, communication card)

If POSTPONE: Deep breathing together, preferred activity, time in smell-safe sanctuary. "The best session is one that starts right."


"Hey [child's name], I have something cool. Remember your special smell bracelet? Would you like to wear it today? We can put your favorite smell on it."
- Sit at child's level or slightly below
- Present the material casually — NOT as a "therapy tool"
- Use warm, playful tone — not clinical
- Hold the scent tool near you first, not thrusting it toward the child
- Smile. Relax your own body language.
- Child looks at the tool with interest
- Child reaches for or accepts the tool
- Child allows the scent to be applied
- Child puts on the bracelet or holds the scent tool
- Child turns away → Place tool nearby. "It's here whenever you want it."
- Child says no → "That's okay. It's yours whenever you're ready."
- Child shows distress → Abort this session. Move to calming strategy.

"Let's put one tiny drop of your favorite smell on the bracelet. You tell me if it's too much or just right."
- Add one drop of preferred essential oil to lava bead or fabric
- Hold it at arm's length first — let the child control the approach distance
- Wait for the child to lean in or bring it closer — never move the scent toward the child's face
- If the child sniffs and smiles: "You found your safe smell!"

- ❌ Using the child's actual trigger smells — too early. Use neutral, mild scents first.
- ❌ Moving the scent closer without the child's permission
- ❌ Skipping the child's self-rating — the child must maintain control
- ❌ Extending the session past the child's tolerance window

- Child says "I'm done" or equivalent
- Child's engagement drops noticeably
- Child starts to show signs of stress not present earlier
- Child has completed 3+ successful cycles — celebrate and end on success
The Golden Rule: "3 good reps > 10 forced reps." End when the child is successful, not when they're exhausted.

"You are so brave! You detected the smell, you used your bracelet, and you stayed comfortable the whole time. That is exactly what a smell-shield champion does!"

"One more practice, and then we're all done for today. You can choose what we do after."




Data Point | How to Record | Example | |
Gagging Episodes Today | Tally count: How many gagging episodes during the practice session? | III (3 episodes) | |
Tolerance Duration | Time: How long did the child engage before showing stress? | 4 minutes 30 seconds | |
Strategy Used | Circle: Which strategy did the child prefer today? | Bracelet ✓ |
- Child's self-reported smell scale rating (1-3)
- New environments successfully entered today
- Notes: anything unusual or breakthrough moments
"60 seconds of data now saves hours of guessing later. Your observations are the raw material from which progress becomes visible."

"Session abandonment is not failure — it's data. Your child just told you exactly where their threshold is. That information is valuable."

Aspect | Ages 3–5 | Ages 6–9 | Ages 10–14 | |
Approach | Playful, game-based | Story-based, detective theme | Self-management, independence | |
Tool Access | Parent controls all tools | Child begins to self-select | Child manages own protection kit | |
Session Length | 2–3 minutes | 5–10 minutes | 10–20 minutes | |
Tracking | Visual cue cards | Written self-rating scales | Digital self-monitoring |

- Child tolerates the preferred scent tool being present (not necessarily using it)
- Child begins to accept wearing or holding the scent bracelet during calm moments
- Environmental modifications show impact: child appears calmer in purified bedroom
- Gagging episodes may not decrease yet — this is normal at this stage
- Child may show curiosity about the protection tools
"If your child allows the aromatherapy bracelet to be placed on the table near them without removing it — that is real progress. If your child sniffs the preferred scent once without pulling away — that is real progress."
- Gagging elimination — far too early
- Entering the cafeteria comfortably — not yet
- Independent strategy use — still learning

- Anticipatory behavior: child prepares before entering challenging spaces
- Self-regulation attempt: child takes deep breaths when smelling something strong
- Spontaneous generalization: child uses the strategy in settings where it wasn't specifically practiced
"You may notice you're more confident too. You've gone from 'I don't know what to do' to 'I have a plan.' That confidence is contagious — your child feels it."

- Child independently selects and uses preferred protection strategy before entering challenging environments
- Gagging episodes reduced by 50%+ from baseline in at least 2 settings
- Child can remain in previously avoided environments for functional durations (complete a meal, attend a class period, participate in a family outing)
- Child can communicate their needs to unfamiliar adults using their advocacy tools
- Child demonstrates recovery — when overwhelmed, uses escape → regulation → return sequence
- Strategy use appearing in settings where it was NOT specifically practiced (friend's house, restaurant, car)
- Child adapts the strategy independently (chooses mask for strong smells, bracelet for mild smells)
- Child begins to distinguish between "uncomfortable but manageable" and "I need to leave" — nuanced self-awareness
- Reduce structured practice sessions to 1x per week
- Monitor: do strategies persist without the structured protocol? If yes → maintenance achieved
- If strategies fade without practice → return to 2–3x per week and reassess
"5–8 weeks ago, your child could not walk into the school cafeteria. Today, they carry their smell shield kit, know how to use it, and participate in spaces that were previously impossible. You made that happen."

- Weight loss or failure to thrive from food avoidance
- Dehydration from frequent vomiting episodes
- New onset of smell sensitivity not present before
- Smell sensitivity combined with new neurological symptoms (headaches, vision changes, balance issues)
- Complete school avoidance developing or worsening
- Severe social isolation — child withdrawing from all social contact
- Desensitization making things worse — gagging increasing
- Anxiety escalating — new fears or avoidance beyond smell
- Overall functioning declining despite intervention
- No measurable progress after 4 weeks of consistent implementation
- Child becoming resistant to the protocol or materials
- Family stress increasing rather than decreasing
- Other sensory challenges emerging or worsening
"Trust your instincts — if something feels wrong, pause and ask. You know your child better than any protocol does."


Technique | Difficulty | Materials Overlap | Key Focus | |
A-6: Oral Sensory Seeking | Core | Aromatherapy Kit, Oral Motor Tools | Oral sensory input needs | |
A-20: Smell Sensory Seeking | Intro | Aromatherapy Kit, Scent Jars | Smell-seeking behaviors | |
A-47: Gagging/Vomiting Around Food Textures | Advanced | Feeding Tools, Desensitization Kit | Texture-based gagging | |
A-84: Food Texture Acceptance Materials | Core | Feeding Tools, Visual Supports | Expanding food repertoire | |
A-115: Emotion Body Awareness | Core | Emotion Cards, Body Maps | Interoceptive awareness | |
A-117: Next Sensory Topic | Core | Coming Soon | Upcoming technique |


From the Therapist's Notes: "Olfactory hypersensitivity with gagging is among the most impactful but also among the most responsive sensory challenges when families commit to environmental modification. The protection-first approach — making the world safe for the child rather than demanding the child tolerate an unsafe world — is the breakthrough most families need."

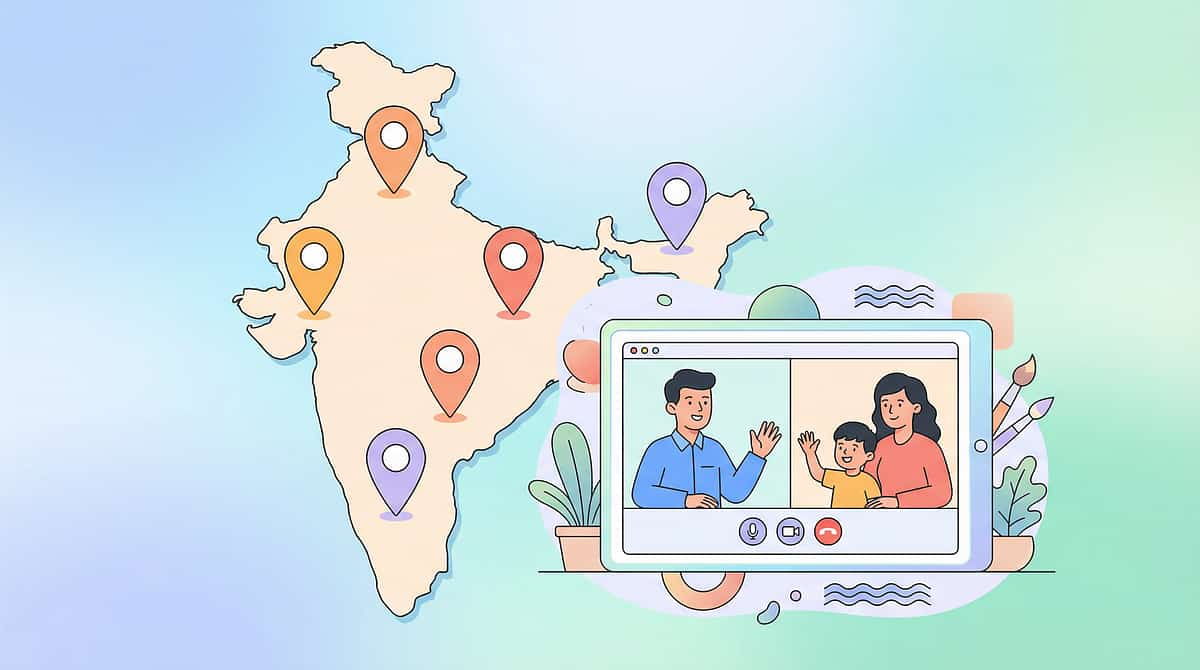


"Home + clinic = maximum impact. Professional guidance accelerates what families build at home."

- WHO Nurturing Care Framework (2018): nurturing-care.org/ncf-for-ecd
- SPD Foundation & STAR Institute Research: spdstar.org
- Ben-Sasson A, et al. (2009): Meta-analysis of sensory modulation symptoms in ASD
- Miller LJ, et al. (2007): Concept evolution in sensory integration — proposed nosology
- Tavassoli T, et al. (2014): Sensory over-responsivity in adults with ASD

- Which protection strategies work best for YOUR child's specific trigger profile
- Optimal session timing and duration based on your child's response patterns
- When to progress, when to maintain, and when to modify
- Cross-domain insights: how olfactory tolerance improvement affects feeding, social participation, and school attendance
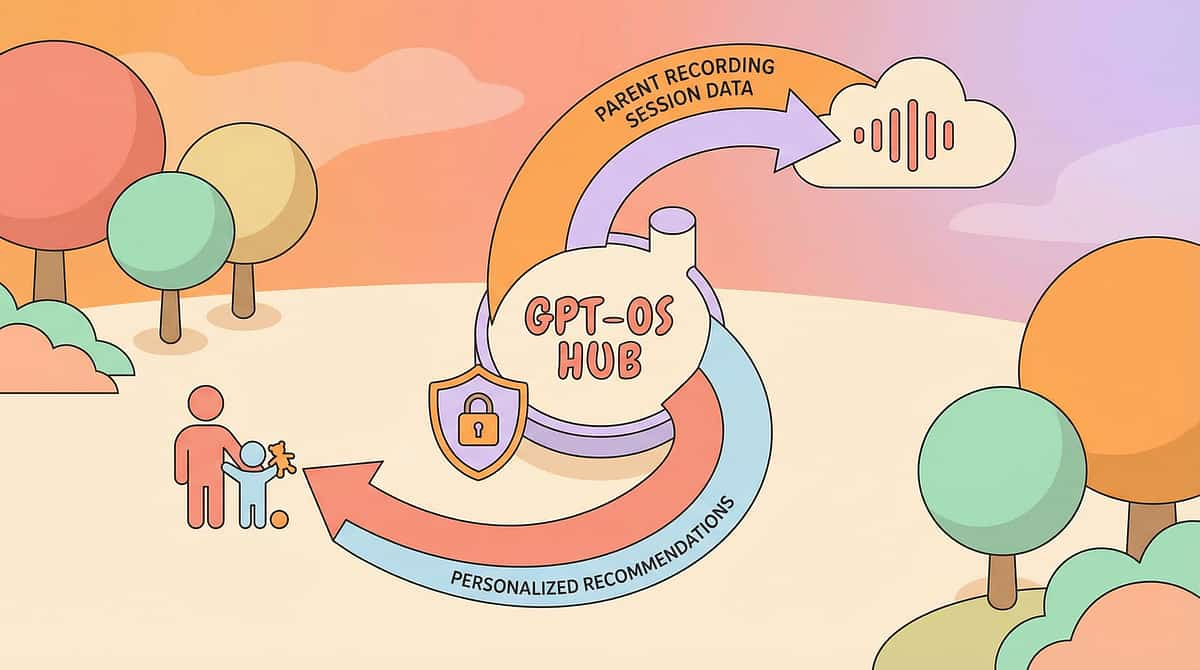
"Your data helps every child like yours. When 70+ centers and thousands of families contribute session data, GPT-OS® improves recommendations for all families navigating olfactory sensitivity."




Preview of 9 materials that help when child gags at smells Therapy Material
Below is a visual preview of 9 materials that help when child gags at smells therapy material. The pages shown help educators, therapists, and caregivers understand the structure and content of the resource before use. Materials should be used under appropriate professional guidance.


















Share this resource
Help others discover this
Patent-protected across 160+ countries | 20M+ exclusive 1:1 therapy sessions | 97%+ measured improvement
