
"His body won't stop moving. Not because he won't try. Because his nervous system needs something the chair can't give him."
The moment his bottom touches the chair, his body starts moving in every direction. He rocks. He bounces. He swings his legs so hard the table shakes. He tips the chair backward. Somehow still trying to write while contorted into impossible positions. You've tried reminders, consequences, rewards, different chairs. Nothing works for more than two minutes.
9 Materials That Help When Your Child Can't Sit Still
"You are not failing. Your child's nervous system is speaking. And we know exactly what it's saying."
Sensory Solutions Series — Episode 83
Motor Regulation + Sensory Processing
Ages 3–12 | 9 Materials

You Are Not Alone. The Numbers Say So.
Millions of families worldwide are navigating this exact challenge every day. Your child's inability to sit still is one of the most common reasons families seek occupational therapy support — a well-understood neurological pattern with proven solutions.
80%
Autism + Sensory
of children diagnosed with autism display sensory processing difficulties affecting sitting, attention, and motor regulation. PRISMA Systematic Review, Children (2024) | PMC11506176
1 in 5
Movement-Seeking
school-age children demonstrate significant movement-seeking behaviours that interfere with classroom participation — across ALL neurotypes. WHO developmental monitoring data
20M+
Therapy Sessions
exclusive 1:1 sessions delivered by the Pinnacle Blooms Network addressing sensory processing and motor regulation challenges across 70+ centres. Pinnacle Blooms Network® Clinical Data
2.8M
Indian Families
are navigating movement-seeking behaviours right now. With 1 in 100 children estimated on the autism spectrum in India (INCLEN Trust, Lancet 2018), and 80% displaying sensory differences, you are far from alone.

What's Happening in Your Child's Brain When the Body Won't Stop Moving
The Vestibular System (Balance & Movement)
Deep inside your child's inner ear is the vestibular system — the brain's GPS for balance, spatial orientation, and head position. In some children, this system requires significantly MORE movement input than typical to achieve regulation. Sitting still doesn't create calm — it creates sensory deprivation that the nervous system experiences as uncomfortable or even intolerable.
The Proprioceptive System (Body Position & Force)
In every muscle and joint, receptors send the brain constant information about where the body is in space. Some nervous systems require much more of this input. The constant movement — pushing against the chair, bouncing, rocking — is the body seeking deep pressure and resistance that organises the nervous system.
The Key Insight
"This is a wiring difference, not a behaviour choice. Your child's brain is literally asking for movement input. The constant motion isn't defiance — it's the nervous system's way of trying to regulate itself."
Arousal Regulation
Movement helps maintain optimal alertness for some brains. Sitting still leads to under-arousal (zoning out) or over-arousal (agitation). Movement is the thermostat — not a distraction but a cognitive scaffold that makes learning possible.
Research: Frontiers in Integrative Neuroscience (2020) establishes the neurological basis for sensory-based interventions in ASD. DOI: 10.3389/fnint.2020.556660
Where This Sits in Your Child's Developmental Journey
Understanding the developmental timeline helps parents and caregivers see this challenge in its proper context — as a waypoint, not a destination.
0–12 Months
Vestibular system develops rapidly. Infants seek rocking, bouncing, swinging. Movement is normal and expected.
1–3 Years
Toddlers in constant motion. Running, climbing, spinning are developmental necessities. Movement needs are high and socially accepted.
3–5 Years ⚠️ Challenge Zone
Environmental demands for sitting increase dramatically. Preschool circle time, structured activities. Children whose nervous systems need more movement begin to stand out.
5–8 Years ⚠️ Peak Impact
School demands sitting 4–6 hours per day. The gap between environmental demand (stillness) and neurological need (movement) reaches maximum. Behavioural concerns escalate.
8–12 Years
With appropriate support, children develop compensatory strategies, build core strength, and learn to use sensory tools. Without support, academic underachievement and self-esteem erosion follow.
Movement-seeking commonly co-occurs with: Autism Spectrum Conditions (80%), ADHD, Sensory Processing Disorder, Developmental Coordination Disorder, and Anxiety. Your child's position on this timeline is a waypoint, not a destination.

The Evidence Behind Sensory-Based Seating and Movement Interventions
🛡️ Level I–II — Strong Evidence
Systematic Reviews + Meta-Analyses + RCTs
Systematic Review (2024)
16 peer-reviewed articles (2013–2023) confirm sensory integration intervention meets evidence-based practice criteria for children with ASD. PRISMA methodology. Published in Children (MDPI). PMC11506176
Meta-Analysis (2024)
Across 24 studies, sensory integration therapy effectively promoted social skills, adaptive behaviour, sensory processing, and gross/fine motor skills. World Journal of Clinical Cases. PMC10955541
Indian RCT (2019)
Home-based sensory interventions demonstrated significant outcomes in Indian paediatric populations. Padmanabha et al., Indian Journal of Pediatrics. DOI: 10.1007/s12098-018-2747-4
NCAEP Classification (2020)
Sensory integration is classified as an evidence-based practice by the National Clearinghouse on Autism Evidence and Practice — the gold standard for autism intervention evidence.
Clinically validated. Home-applicable. Parent-proven. These are not experimental strategies — they are established interventions deployed across 70+ Pinnacle centres with 20M+ sessions of outcome data.

Sensory-Based Seating and Movement Regulation — Multi-Material Intervention Protocol
The 9 Tools That Help a Moving Body Learn to Sit
A structured approach that works WITH the nervous system's movement needs — not against them.

Motor Regulation
Building the body's ability to start, stop, and control movement.

Sensory Processing
Channelling sensory input so the nervous system feels organised.

Attention & Focus
Regulated bodies create the conditions for sustained attention.

Self-Regulation
Teaching the nervous system to find its own equilibrium.

Who Uses This Technique — Across Therapy Disciplines
This technique crosses therapy boundaries because the brain doesn't organise by therapy type. Your child needs a coordinated, multi-disciplinary approach for maximum impact.

Occupational Therapist (Lead)
The OT leads this intervention — assessing the child's sensory profile, selecting materials, calibrating intensity, and designing the individualised protocol.

Board Certified Behaviour Analyst (BCBA)
Applies reinforcement principles to build sitting tolerance, tracks behavioural data on seated duration, fidget use, and break requests.

Speech-Language Pathologist (SLP)
Integrates oral motor tools that provide proprioceptive input to the jaw while supporting speech — a dual-purpose sensory-communication intervention.

Special Educator (SpEd)
Adapts the classroom environment — standing desks, alternative seating, movement break schedules, and fidget policies that don't disrupt peers.

NeuroDevelopmental Paediatrician
Evaluates whether movement-seeking reflects sensory processing differences, ADHD, autism, or developmental coordination disorder — providing diagnostic clarity that guides the whole approach.

What This Targets — Precision, Not Guesswork
🎯 Primary Targets
- Sitting tolerance duration — from seconds to sustainable seated work periods
- Motor hyperactivity regulation during seated tasks
- Vestibular-proprioceptive sensory seeking management
- Postural control — building core stability
- Self-regulation of movement needs
🔵 Secondary Targets
- Attention and focus during seated activities
- Academic task completion rates
- Mealtime and homework participation
🟢 Tertiary Targets
- Social acceptance and peer relationships
- Self-esteem and academic achievement
- Adaptive behaviour in community settings
- Self-advocacy skills

The 9 Materials — What You Need
Each material below addresses a specific sensory need. Start with one or two that match your child's most prominent pattern, then layer additional supports as confidence grows. The "Pinnacle Recommends" badge marks the highest-value items.

1. Wobble Cushions & Dynamic Seating
📦 Seating & Positioning | ₹500–2,000
⭐ Pinnacle Recommends








Essential Starters (Budget Limited): Wobble cushion (₹500–1,000 — most versatile single item) + Resistance band for chair (₹150–300 — inexpensive, effective). Total: under ₹1,300.

Can't Order Online? Make It Today With What You Have.
The science isn't in the product — it's in the sensory input. A ₹50,000 wobble cushion and a partially inflated balloon provide the same vestibular input principle: an unstable surface that allows controlled movement while seated. The nervous system responds to the input, not the price tag.
Buy This | Make This (Zero Cost) | Why It Works | |
Wobble Cushion (₹500–2,000) | Partially inflate a balloon inside a pillowcase. Fold a yoga mat. Partially deflated beach ball on chair. | Unstable surface creates vestibular input while seated | |
Resistance Band (₹150–600) | Thick rubber band or old bicycle inner tube around chair legs. Old elastic waistband. Dupatta fabric tied firmly. | Foot resistance provides proprioceptive feedback | |
Weighted Lap Pad (₹600–2,500) | Fabric pouch filled with rice, dried beans, or sand. Weight ≈ 5–10% of child's body weight. Double-stitch seams. | Deep pressure input calms the nervous system | |
Fidget Tool (₹100–800) | Atta dough with extra firmness. Balloon filled with rice/flour. Textured fabric squares from old clothing. | Hand proprioception reduces whole-body movement | |
Compression Clothing (₹800–3,000) | Snug athletic wear, one size smaller. Swimsuit under school uniform. | Continuous body-awareness input throughout the day | |
Core Strengthening (₹500–2,500) | Plank challenges (free). Yoga poses for kids. Crab walks. Superman pose. Playground climbing. | Builds postural stability needed for seated work |
Zero-Cost Minimum Viable Protocol: Wall pushups → folded blanket on chair → rubber band on chair legs → movement breaks every 20 minutes → atta dough for hand fidgeting. Total cost: ₹0.

Safety First — Before You Begin
Safety is non-negotiable. Review this traffic-light system before introducing any material. If in doubt, always consult your Pinnacle Occupational Therapist.
🔴 DO NOT PROCEED IF:
- Child has spinal cord, vertebral, or severe musculoskeletal conditions
- Child has recently had surgery or medical procedure
- Weighted items: child weighs less than 10 kg (consult OT)
- Compression clothing: child has respiratory difficulties or circulatory issues
- Child is in extreme distress, meltdown, or shutdown state
- Any material causes visible pain, distress, or panic
🟡 PROCEED WITH MODIFICATIONS IF:
- Child is mildly tired → use lower-intensity materials (fidgets over wobble cushion)
- Child resists a specific material → offer an alternative; never force
- DIY materials show wear → replace immediately
- Child becomes overstimulated → remove, reduce intensity, try again another day
- First-time use → introduce in a calm, safe environment with full supervision
🟢 PROCEED WHEN:
- Child is fed, rested, and in a relatively regulated state
- Environment is safe (no sharp edges near wobble seating, clear floor)
- All materials inspected (seams intact, bands not frayed)
- Parent/caregiver is present and attentive
- Clear start and stop expectations are established
Weighted lap pads: Weight must NOT exceed 10% of body weight. Child must be able to remove independently. No use during sleep for young children. Resistance bands: Check regularly for wear. Teach appropriate use — feet only, no hands.

Set Up Your Space — The 2-Minute Room Preparation
The right environment removes friction before the session even begins. Two minutes of preparation makes the difference between a child who engages and one who doesn't.

Clear the Floor
Remove furniture hazards within 1 metre of the seating area. The child needs space to move without risk.

Lay Out Materials
Place all 9 materials within arm's reach before calling the child. Searching mid-session breaks regulation momentum.

Set the Sensory Environment
Dim harsh overhead lights. Reduce background noise. A calm sensory environment primes the nervous system before you begin.
Move furniture hazards
Clear a 1-metre radius around the seating spot.
Lay out materials
All 9 items visible and within reach.
Adjust lighting & sound
Dim lights, reduce noise, close doors.
Check your own state
A regulated parent co-regulates the child. Take one breath.

Is Your Child Ready? — The 60-Second Readiness Check
The best session is one that starts right. Run through this observable checklist before every session — it takes under a minute and saves significant frustration.
✅ Fed
Not hungry, not just eaten a large meal
✅ Rested
Not overtired, not just woken from sleep
✅ Calm State
Not mid-meltdown, not post-meltdown
✅ Recent Movement
Had some movement opportunity in the last hour (not returning from prolonged car ride)
✅ No Illness
No fever, no stomach complaints, no visible discomfort
✅ Ready Environment
Materials prepared and inspected. Space set up per Card 12.
🟢 ALL GREEN → GO
Begin with Step 1: The Invitation.
🟡 1–2 AMBER → MODIFY
Use lighter version: skip wobble cushion, reduce seated expectation by 50%, offer more frequent movement breaks.
🔴 ANY RED → POSTPONE
Offer a calming activity (deep pressure hug, quiet space, comfort object) and try again when the child's state shifts. Postponement is not failure — it is clinical judgement.

Step 1 of 6 | ⏱️ 30–60 seconds
Step 1 — The Invitation
How you introduce a sensory tool sets the tone for whether your child will accept or reject it. Lead with curiosity and play, never demand.
For Wobble Cushion
"Hey [name], I have something cool for your chair today. Want to try this squishy cushion? It wobbles when you sit on it — you can bounce a little while you work!"
For Resistance Band
"Look what I put on your chair — it's like a bouncy thing for your feet! Want to feel how it stretches?"
For Weighted Lap Pad
"I have something heavy and cosy for your lap. Some kids say it feels like a warm hug on their legs. Want to try it?"
Body Language Rules
- Get to child's eye level
- Show genuine curiosity and playfulness
- Offer the material — don't place it
- Let the child touch, explore, decide
- No demand language ("you have to," "you need to")
Variations by Age
- Ages 3–5: Make it a game. "This is a magic sitting cloud!"
- Ages 6–8: Appeal to science. "This is what astronauts use to help their bodies focus."
- Ages 9–12: Appeal to autonomy. "Some people find this helps them concentrate. Want to experiment?"

Step 2 of 6 | ⏱️ 1–3 minutes
Step 2 — The Engagement
Before any seated work demand, allow free exploration of the chosen material. The child's nervous system needs to meet the tool before it can benefit from it.
Wobble Cushion
"Sit down and feel how it moves. Try bouncing a little. Try rocking side to side. Find the way that feels best for your body." Allow 1–2 minutes of free exploration.
Resistance Band
"Put your feet on it. Try pushing. Try pulling. You can kick it gently or just rest your feet and push. See what feels good." Let the child discover their preferred movement pattern.
Weighted Lap Pad
"Let me put this on your lap. Feel how heavy it is? Some kids like it right in the middle, some like it closer to their knees. Where feels best?" Adjust based on child's preference.
✅ Engagement (Ideal)
Child explores with curiosity, tries different movements, body starts to calm
🔵 Tolerance (Acceptable)
Child allows the material but doesn't actively engage. Keep it — passive input is still input.
⚠️ Avoidance (Modify)
Child actively pushes away or shows distress → switch to alternative material, try again another day
Reinforcement cue (within 3 seconds of engagement): "I love how you're trying that cushion! Your body looks like it's finding what it needs."

Step 3 of 6 | ⏱️ 5–15 minutes (build gradually)
Step 3 — The Therapeutic Action: Seated Work WITH Sensory Support
Now introduce the seated activity while the sensory supports are in place. The key shift: the child is not sitting still. The child is sitting SUPPORTED — movement is happening through controlled channels while functional participation continues.
What This Looks Like in Practice
- Child on wobble cushion doing maths homework — gently bouncing and shifting while writing
- Child's feet pushing against resistance band while listening to a story being read
- Weighted lap pad on thighs while colouring — shoulders slightly lower, body slightly calmer
- Fidget in non-dominant hand while dominant hand writes spelling words
- Compression vest under school shirt providing constant body-awareness input during group lesson
Seated Duration Goals (build gradually)
- Week 1: 3–5 minutes of supported seated work
- Week 2: 5–8 minutes
- Week 3–4: 8–12 minutes
- Month 2+: 12–20 minutes
Common Execution Errors:❌ Starting with too long a seated period ❌ Removing the sensory support mid-task ❌ Comparing to neurotypical peers ❌ Treating the sensory tool as a reward to be earned — it's a regulation requirement, not a privilege.
Step 4 of 6 | ⏱️ 3–5 minutes (variation introduction)
Step 4 — Repeat & Vary: Therapeutic Dosage
Sensory-based seating and movement supports should be used DAILY — not as special "therapy time" but integrated into the child's natural routine. Variation prevents habituation and keeps the nervous system engaged.
Morning
Heavy work before school (wall pushups, carrying backpack) → compression vest on → wobble cushion at school desk → resistance band on chair → movement break every 20–30 minutes
After School
Heavy work transition → homework with wobble cushion + fidget + weighted lap pad → movement break → continue
Dinner
Wobble cushion at dining chair → resistance band → keep meals to 15–20 minutes
Evening
Core strengthening play → body awareness activities → calming compression for wind-down
Variation Options (Prevent Habituation)
- Alternate between wobble cushion and flat firm cushion on different days
- Try different resistance band tensions (lighter for calm days, heavier for high-energy days)
- Rotate fidget tools weekly (the brain habituates to the same input)
- Change movement break activities (jumping jacks → wall pushups → animal walks → yoga poses)
"3 good minutes > 10 forced minutes."

Step 5 of 6 | ⏱️ Immediate — within 3 seconds of desired behaviour
Step 5 — Reinforce & Celebrate
Reinforcement must be immediate (within 3 seconds), specific (name the exact behaviour), and enthusiastic (genuine, not performative). This is the neurological glue that makes the behaviour stick.
"Look at you — you sat and finished that whole page! Your body found what it needed."
"You used your wobble cushion the whole time. That's your body learning to regulate."
"You asked for a movement break before you got frustrated — that's amazing self-awareness."
"Three minutes of sitting today! That's a whole minute more than yesterday."
What to Celebrate
✅ Any increase in seated duration (even 30 seconds)
✅ Using a sensory tool independently
✅ Requesting a movement break (self-regulation!)
✅ Returning to seat after a break without being asked
✅ Using words to describe body needs ("I'm wiggly," "I need to move")
"Celebrate the attempt, not just the success."

Step 6 of 6 | ⏱️ 1–2 minutes
Step 6 — The Cool-Down: Transitioning Out Gracefully
Transitions are vulnerable moments. A well-managed cool-down prevents the dysregulation that can undo the gains of the session and makes the child more willing to sit next time.
Transition Warning (give notice)
"Two more minutes of work, then we're done with sitting time." / "One more problem, then movement break!" Predictability reduces resistance.
Cool-Down Activity (1–2 minutes)
Deep pressure hug or squeeze hands together. Slow animal walks (turtle, bear) — NOT energising ones. Breathing: "Smell the flower, blow out the candle" (3 slow breaths).
Material Put-Away Ritual
"Let's put the cushion back. You carry the lap pad to the shelf. The fidget goes in the box." This builds ownership, routine, and executive function.
If Child Wants to Continue Sitting
Wonderful! Let them. This is success. Do not interrupt a child who has achieved voluntary sustained sitting.
If Child Resists Transition
Use "First-Then" board: "First put away materials, then [preferred activity]." Extend the cool-down and increase calming input if needed.

Capture the Data — Right Now. 60 Seconds.
Without data, you can't see the slow, steady progress. A child who goes from 2 minutes to 7 minutes over a month is making extraordinary gains — but without a record, you'll only remember that they still can't sit for 20 minutes "like other kids."
Seated Duration
How many minutes did the child remain in their seat today? Use your phone timer during the session — not a retrospective estimate.
Material Used
Which sensory support(s) were in place? (wobble / band / weight / fidget / compression / multiple)
Regulation Rating
1–5 scale: 1 = constant movement, couldn't engage | 3 = some movement, partially engaged | 5 = well-regulated, task-focused
Sample Entry: Feb 28, 2026 | Homework | Wobble + Band | 7 min seated | Rating: 3 | Notes: Asked for break at 7 min (good self-regulation!)
"60 seconds of data now saves hours of guessing later."

What If It Didn't Go as Planned? — Troubleshooting
Every session won't be perfect. That's not failure — that's data. The nervous system is not a machine. Here is how to read what went wrong and what to do next.
My child refused to sit on the wobble cushion at all
Don't force it. Introduce the cushion as a toy first — let them jump on it, squeeze it, sit on it themselves without any task attached. Forced use creates aversion. Voluntary exploration creates buy-in. Try again tomorrow with zero pressure.
My child fell off the wobble cushion twice
The cushion may be over-inflated. Deflate it by 20% so the wobble is gentler and the base is wider. Also check: is the child's feet flat on the floor? Dangling feet remove the stabilising feedback loop. Use a footrest if needed.
The resistance band snapped or came loose mid-session
Check the band's attachment points before every session — this is a non-negotiable safety step. Replace bands every 3 months or when you see any discolouration, thinning, or micro-tears. Keep a spare band in your kit.
My child was MORE dysregulated after the session than before
This is a sign of sensory overload, not failure. You may have introduced too many materials at once, or the session ran too long. Next session: use only one material, reduce duration by 50%, and end before the child shows any signs of fatigue. Build up slowly.
My child used the fidget tool as a distraction, not a support
This is common in the first two weeks. The tool is novel — novelty is inherently distracting. Reduce the visual complexity of the fidget (plain over patterned), introduce it during a low-demand activity first, and pair it with a clear verbal cue: 'This is your focus helper.'
I don't see any change after two weeks
Two weeks is the observation window, not the results window. Check your data: is seated duration trending upward even by 30 seconds per session? That is progress. If there is genuinely zero change across 14 sessions, consult your OT — the sensory profile assessment may need to be revisited.
The Golden Rule of Troubleshooting
Change only ONE variable at a time. If you change the material, the duration, and the environment simultaneously, you will never know what worked. Isolate. Observe. Adjust.

Document What Went Wrong
A one-line note after each difficult session is worth more than an hour of guessing later. Write: what happened, when it happened, and what you changed.

When to Call Your OT
If the same problem repeats across 5+ consecutive sessions despite adjustments, it's time to loop in your therapist. Bring your session notes — they will tell the story faster than memory.

Adapt & Personalise — Because No Two Children Are Identical
There is no single protocol that works for every child. Use this guide to dial the approach up or down based on your child's current state, sensory profile, and developmental stage.
🌀 Sensory Seeker
Craves movement, crashes, spins. Prioritise: Heavy work before sitting, wobble cushion with maximum wobble, resistance band with heavy resistance, compression clothing. These children need MORE input to satisfy the drive.
🪑 Postural Weakness
Tires quickly, slumps, compensates with unsafe positions. Prioritise: Core strengthening (daily), therapy ball for seated work, supportive alternative seating. These children need STRENGTH, not just sensory input.
🎯 Attention-Linked Movement
Moves to think. Prioritise: Fidget tools, standing desk option, movement breaks, resistance band for feet. These children need COGNITIVE SCAFFOLDING through movement.

Progress Arc | Week 1–2
Week 1–2: What to Expect — Setting Realistic Expectations
Weeks 1–2 are about tolerance and exploration, not mastery. You are building neural pathways. Neural pathways don't form overnight. Be patient with your child AND with yourself — you are learning a new system together.
✅ What IS Progress at This Stage
- Child tolerates the sensory material on/near them (even if not engaging with task)
- Seated duration increases by even 30–60 seconds from baseline
- Child shows curiosity about the materials (touching, exploring, asking about them)
- Movement intensity may INCREASE initially (normal! — the child is exploring new input)
❌ What is NOT Expected Yet
- Sitting for 20 minutes independently
- Sitting without any sensory support
- Eliminating all fidgeting and movement
- Sitting still "like the other kids"
"If your child tolerates the wobble cushion for 3 minutes today and only tolerated it for 1 minute last week — that is real, measurable, clinically significant progress."
Patience Metric: If your child showed ANY improvement in seated duration, ANY reduction in chair-tipping, or ANY willingness to try a sensory tool — you are on the right track. Systematic review (Children, 2024): Sensory integration intervention outcomes emerge across 8–12 week timelines. PMC11506176

Progress Arc | Week 3–4
Week 3–4: Consolidation — The Neural Pathways Are Forming
By weeks 3–4, something significant is starting to happen beneath the surface. The nervous system has encountered these sensory inputs repeatedly and is beginning to expect and use them. Watch for these consolidation indicators.
Child anticipates and reaches for sensory tools without prompting
This is a major milestone — the child's nervous system has learned to seek appropriate input.
Seated duration consistently 5–8 minutes with support
Consistency is more meaningful than occasional peaks. A consistent 6 minutes beats a one-off 12-minute session.
Movement breaks are used effectively — child returns to seat afterward
This shows emerging self-regulation: the child uses the break and comes back. That's executive function in action.
Some generalisation emerging spontaneously
Child may sit on the wobble cushion during TV time, or request heavy work activities unprompted. The skill is spreading beyond the structured session.
"You may notice you're more confident too — less anxious about homework time, less dreading dinner. Your confidence IS the intervention. It changes how you approach your child."

Progress Arc | Week 5–8
Week 5–8: Mastery — Your Child Is Building Sustainable Skills
🏆 Mastery Phase
75% Progress Milestone
Sustained Seated Work
15–20 minutes with sensory support during structured academic or play activities
Independent Tool Use
Child manages their own regulation toolkit — selecting, placing, and using tools without prompting
Self-Initiated Breaks
"I need a break" — before dysregulation. This is self-regulation at its highest functional level.
Visible Core Strength
Less slumping, better posture tolerance, fewer compensatory positions. The body is getting stronger.
Generalisation
Home, school, community. Using wobble cushion at school independently. Sitting through restaurant meals with one movement break.
Self-Advocacy
Child can articulate their needs: "My body needs to move right now." This skill will serve them for life.
Maintenance Check: Does improvement persist on days when you forget to set up the supports? If yes → underlying capacity is building. If no → supports are still needed (and that's completely fine — glasses don't cure vision, but they make seeing possible).

Celebrate This Win. You Earned It.
"You did this. Five to eight weeks of daily effort, of setting up materials, of being patient when sessions failed, of capturing data, of believing in the science when progress felt invisible. Your child grew because of YOUR commitment."
You didn't just help your child sit still — you helped their nervous system learn to regulate itself. You helped them access the world on their own terms.
📸 Document This Milestone
Write down what your child can do today that they couldn't do 8 weeks ago. This record will sustain you through the harder days ahead. Take a photo. This is the before-and-after your child deserves to see someday.
🍽️ Family Celebration Suggestion
Go out for a meal together — and notice how different it is now. Notice the wobble cushion on the chair, the compression vest under the shirt, the calm that wasn't possible 8 weeks ago. This is the change you built.
📖 Journal Prompt
"Before, my child could ___. Now, my child can ___. The moment I knew it was working was ___." Write it down. You'll want to remember this.

Red Flags — When to Pause and Seek Professional Guidance
Even after celebration and progress, staying alert to concerning patterns is part of good clinical practice at home. Trust your instincts — if something feels wrong, pause and ask.
🚩 Regression After Initial Progress
Child was improving but suddenly returned to baseline or worse — may indicate new stressor, illness, medication change, or co-occurring condition requiring evaluation.
🚩 Extreme Distress with ANY Sensory Material
Not mild reluctance (normal) but true panic, crying, or meltdown when sensory tools are introduced — may indicate a more complex sensory profile needing professional assessment.
🚩 Physical Complaints
Child reports pain, numbness, tingling, or visible skin irritation from weighted items or compression. Requires immediate discontinuation and medical review.
🚩 Movement Pattern Changes
New movements that look different from the original seeking pattern — tics, stereotypies, or motor patterns that seem involuntary. Require neurological evaluation.
🚩 No Progress After 8 Weeks
If materials are being used correctly and consistently with zero measurable improvement — the underlying mechanism may not be sensory-seeking. A comprehensive evaluation is needed.
🚩 Safety Concerns
Child frequently falls from alternative seating, uses materials unsafely despite teaching, or movement pattern creates risk of injury to self or others.
The Progression Pathway — Where You've Been, Where You're Going
Understanding where this technique sits in the broader therapeutic sequence helps you navigate to what's next — and appreciate how far you've already come.
← Prerequisites (What Came Before)
- A-081: Child Seeks Constant Spinning — vestibular seeking patterns
- A-082: Child Crashes Into Everything — proprioceptive seeking patterns
→ Next-Level Options
- A-090: Child Has Difficulty with Focus & Attention

Related Techniques in Motor Regulation & Sensory Processing
Your investment in A-083 materials unlocks access to at least 4 additional technique protocols — the wobble cushions, resistance bands, and weighted lap pads you already own appear across all these techniques.
A-090: Child Has Difficulty with Focus & Attention
Difficulty: Advanced | 🎯 Attention Tools
K-1020: Understanding Sensory Seeking Behaviour
Parent Education | 📚 Knowledge Module
Your Child's Full Developmental Map
A child who can't sit still often also has challenges in attention, social participation, academic performance, and self-care. Intervention in one domain feeds progress in all connected domains.
🟢 Current Domain: Motor Regulation / Sensory Processing
A-083 lives here. You have made measurable progress in this domain. This is your foundation.
🔵 Adjacent Active Domains
Attention & Focus | Self-Regulation | Adaptive Behaviour | Fine Motor | Social Participation
Progress in motor regulation creates automatic downstream improvements in all of these domains.

Families Who've Been Here — Before and After
Family 1 — From: "Can't stay for 30 seconds"
Before: "He couldn't stay in his chair for thirty seconds. Literally — we timed it. The school was sending notes home daily."
What they did: Wobble cushion and resistance bands. Heavy work before seated times — wall pushups, carrying his backpack full of books. Compression undershirt on school days. Scheduled movement breaks every twenty minutes with a visible timer.
After (4 months): "He can do fifteen to twenty minutes before he needs a break. He's still the wiggliest kid in class. But he can learn now. His teacher said it's like a different child." — Parent, Pinnacle Network
Family 2 — From: "Under the table in two minutes"
Before: "Dinner was a war zone. She'd be under the table within two minutes."
What they did: Wobble cushion on dining chair, heavy work before meals (carrying dishes, pushing chairs), fidget tool at the table, and meals kept to 15 minutes.
After: "She sits through dinner most nights. Not perfectly still — she bounces on the cushion and fiddles with her putty. But she's AT the table. She's part of the family meal. That's everything." — Parent, Pinnacle Network
From the Therapist's Notes: "In both cases, the intervention wasn't about eliminating movement. It was about channelling movement into appropriate tools while meeting the underlying sensory need. When the nervous system gets what it requires, functional participation becomes possible." — Pinnacle OT Clinical Team. Illustrative cases; individual outcomes vary by child profile.

Connect With Other Parents — You Don't Have to Do This Alone
The journey of supporting a child with movement-seeking needs is profoundly personal — but it doesn't have to be solitary. Thousands of families in our network are walking the same path right now.
WhatsApp Parent Community
Join the Sensory Seeking Parent WhatsApp group — daily tips, real stories, and peer support from families who understand exactly what your mornings look like.
Pinnacle Parent Online Forum
Ask questions, share wins, and get answers from experienced parents and Pinnacle therapists. Available in multiple Indian languages.
Peer Mentoring Programme
Want to talk to a parent who's been through this? Pinnacle's peer mentoring programme connects you with experienced families who've navigated the same challenges.
Local Parent Meetups
Find in-person parent gatherings near you. Because some conversations are best had face-to-face, over chai, with someone who truly understands.
Your Professional Support Team — Home + Clinic = Maximum Impact
Home strategies and clinical therapy are not alternatives — they are multipliers. Every technique you implement at home extends the impact of every clinic session your child attends.
70+ Centres Across India
Find your nearest Pinnacle Blooms centre with Occupational Therapists, BCBAs, SLPs, and NeuroDevelopmental Paediatricians.
Teleconsultation (India + 70 Countries)
Not near a centre? Pinnacle offers teleconsultation across India and internationally. Same clinical quality, from your home.
FREE National Autism Helpline
📞9100 181 181 — 16+ languages — 24/7 — Free. "One call. No obligation. A trained counsellor who understands."
Therapist Match for A-083: Primary — Occupational Therapist (Sensory Integration Certified). Secondary — BCBA (behaviour), SLP (communication), NeuroDevelopmental Paediatrician (medical oversight). All coordinated through GPT-OS® FusionModule™.
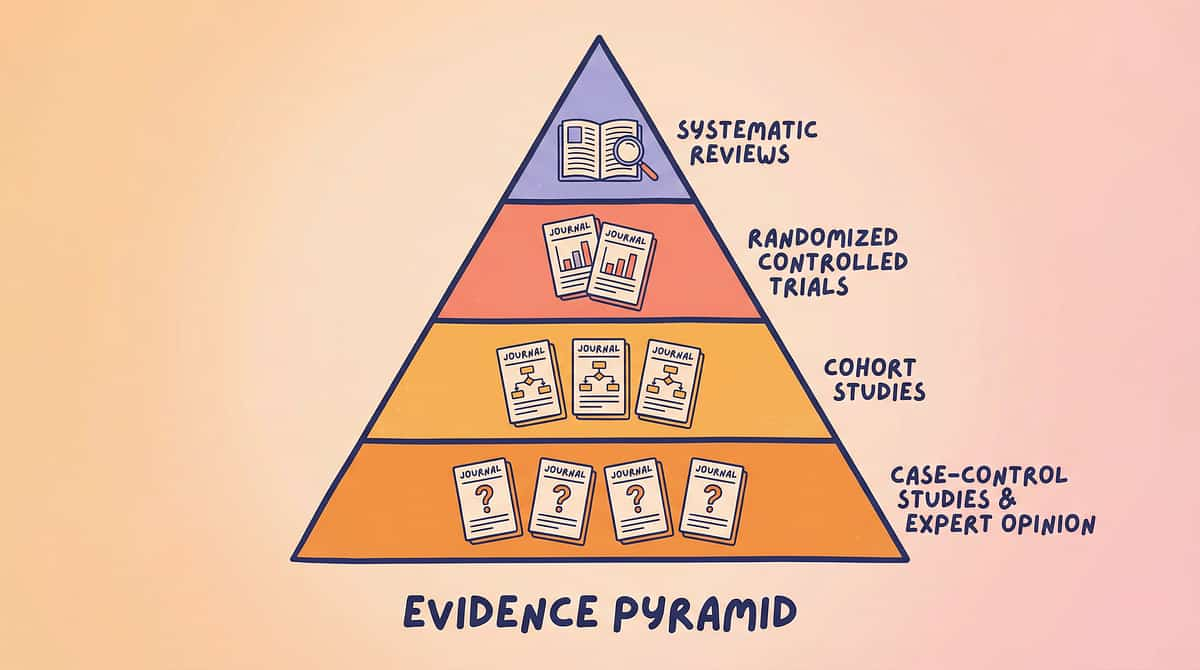
The Research Library — For the Curious Parent
Every recommendation in this protocol is grounded in peer-reviewed evidence. Here is the research base, organised so that any parent — or any clinician — can verify our claims independently.
Core Evidence
Based on systematic reviews and meta-analyses.
Clinical Trials
Involving randomised controlled trials for efficacy.
Supporting Studies
Includes observational and cohort research data.

📗 Systematic Review — SI as Evidence-Based Practice (2024)
16 articles (2013–2023) confirm SI intervention meets evidence-based criteria for children with ASD. PRISMA methodology. Read on PubMed → PMC11506176
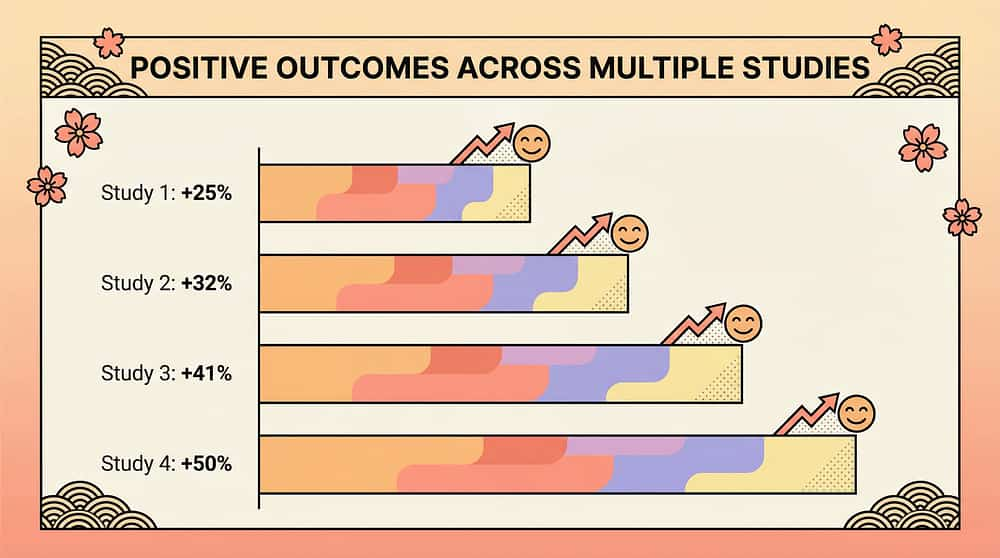
📗 Meta-Analysis — SI Therapy Effectiveness (2024)
24 studies. SI therapy effectively promoted social skills, adaptive behaviour, sensory processing, and motor skills. Read on PubMed → PMC10955541

📗 Indian RCT — Home-Based Sensory Interventions (2019)
Padmanabha et al. demonstrated significant outcomes for home-based sensory interventions in Indian paediatric populations. Read on PubMed → DOI: 10.1007/s12098-018-2747-4
📗 WHO Care for Child Development Package
Evidence-based caregiver recommendations implemented across 54 countries. Read on PubMed → PMC9978394

📗 NCAEP Evidence-Based Practices for Autism (2020)
Sensory integration classified as evidence-based practice by the national clearinghouse — the gold standard. Read the Report →

How GPT-OS® Uses Your Data — Transparency, Privacy, Personalisation
Parent Records Session
GPT‑OS Analyzes Patterns
Generate Recommendations
Auto‑Adjust Intervention
What GPT-OS® Learns from A-083 Data
- Which materials produce the greatest seated duration gains for your child's profile
- Optimal movement break frequency and intensity
- Time-of-day patterns (morning vs. afternoon regulation differences)
- Material combinations that work best together
- When to increase demand and when to reduce it
🔒 Privacy & Data Protection
- All data encrypted (ISO/IEC 27001 certified)
- Data used only for your child's therapeutic benefit
- No data shared with third parties without explicit consent
- Compliant with Indian IT Act and international data protection standards
Population-Level Impact: When you record that wobble cushions worked better for your sensory-seeking child, GPT-OS® learns that pattern and improves recommendations for the next similar family. 20M+ sessions of collective intelligence.

Watch the Reel — A-083: 9 Materials That Help When Child Can't Sit Still
Watch a Pinnacle Occupational Therapist demonstrate each of the 9 materials — showing exactly how to introduce them, how the child responds, and what regulation looks like in real time. Video + text = maximum learning.
Reel A-083
Sensory Solutions Series — Episode 83
Motor Regulation + Sensory Processing
Wobble Cushions
Resistance Bands
Weighted Lap Pads
Fidget Tools
Movement Breaks
Compression Clothing
Alternative Seating
Heavy Work
Core Strengthening
Research: Video modelling is classified as an evidence-based practice for autism (NCAEP, 2020). Multi-modal learning improves parent skill acquisition.

Share This With Your Family — Consistency Across Caregivers Multiplies Impact
Research is clear: interventions fail when they only happen in one setting with one caregiver. When grandparents, teachers, and other family members understand and apply the same approach, your child's gains accelerate dramatically.
💬 "Explain to Grandparents" Simplified Version
"Your grandchild's body needs more movement than usual to stay calm and focused. This isn't bad behaviour — it's how their nervous system is wired. We're using special cushions and tools that let them move a little while sitting. Please don't tell them to 'sit still' — let the tools do their work."
📋 Teacher/School Communication Template
"Dear [Teacher], [Child's name] has been assessed by a paediatric occupational therapist and requires sensory accommodations for seated work. The following tools have been recommended: wobble cushion, resistance band, fidget tool. These are not toys — they are clinically prescribed regulation supports. We would appreciate your partnership. Pinnacle Blooms: 9100 181 181."

Frequently Asked Questions
Will my child ever sit still without these tools?
Many children develop self-regulation strategies over time and need fewer supports as core strength, body awareness, and neural pathways mature. Some children will always benefit from some level of sensory support — and that's perfectly fine. The goal isn't eliminating the need but meeting it appropriately. Think of these tools like glasses: you don't "cure" the need; you support it.
Is this ADHD? Should I get medication?
Movement-seeking can be a feature of ADHD, autism, sensory processing differences, or typical development with high movement needs. A NeuroDevelopmental Paediatrician can evaluate whether ADHD is present and whether medication, sensory strategies, or both are appropriate. They are not mutually exclusive — they often work best together.
The school won't allow wobble cushions. What do I do?
Request a meeting to discuss sensory accommodations. Bring documentation from your child's OT. In India, the Rights of Persons with Disabilities Act (2016) supports reasonable accommodations in educational settings. Pinnacle offers school consultation services — call 9100 181 181.
My child uses the fidget as a toy, not a tool. How do I fix this?
Switch to a less engaging fidget (plain stress ball, textured fabric). Establish rules: "Fidget stays in your hand, not on the table." If the child can't use it in the background, it's the wrong fidget. Some children do better with foot-based input (resistance band) than hand-based.
How much should the weighted lap pad weigh?
Standard guideline: 5–10% of the child's body weight. For a 20 kg child, that's 1–2 kg. Start lighter and increase if needed. The child must be able to remove it independently. If in doubt, consult your OT.
We can't afford these materials. Are DIY versions really effective?
Yes. The science is in the sensory input, not the product. A folded yoga mat provides similar vestibular input to a ₹2,000 wobble cushion. Rice in a fabric pouch provides similar deep pressure to a ₹2,500 weighted lap pad. Card 10 has complete zero-cost alternatives for every material.
Can this make things worse?
If the wrong material is used for the wrong child, it can increase dysregulation (e.g., a sensory-avoiding child given too much stimulation). This is why the Adapt & Personalise card matters. If you see worsening, stop, reassess, and consult a professional. Session data from your tracker will help identify the pattern.
How long do we need to keep doing this?
Sensory needs are ongoing for most children who have them. The tools may change, the intensity may reduce, and the child's self-management skills will grow — but the underlying wiring difference is part of who they are. The goal is teaching the child to meet their own needs, not eliminating the needs themselves.

Your Next Step — Start Now
You have the knowledge. You have the materials. You have the protocol. The only thing left is to begin. Your child's nervous system has been waiting for this support. Today is the day you provide it.
🏛️ Consortium Validated
OT • SLP • ABA • SpEd • NeuroDev • CRO — Drafted by 6 disciplines. Backed by 21 million sessions.
📞 Free Helpline 24/7
9100 181 181 — FREE — 16+ languages — "One call changes the trajectory."
Preview of 9 materials that help when child cant sit still Therapy Material
Below is a visual preview of 9 materials that help when child cant sit still therapy material. The pages shown help educators, therapists, and caregivers understand the structure and content of the resource before use. Materials should be used under appropriate professional guidance.




















Share this resource
Help others discover thisLink copied!

The Pinnacle Promise
"From fear to mastery. One technique at a time."
A parent arrived at Card 01 scared, confused, and exhausted — watching their child fail at something the world demands but their body can't deliver. By Card 40, that parent understands the neuroscience, has the materials, knows the protocol, has tracked progress, and belongs to a community.
The child's body hasn't changed. But the support system around it has. And that changes everything.
🏛️ Pinnacle Blooms Network®
Clinical Research Organisation • Paediatric SLPs • Paediatric OTs • BCBAs • Special Educators • NeuroDevelopmental Paediatricians
Aligned with: WHO • UNICEF • NCAEP • Indian Academy of Paediatrics
⚖️ Medical Disclaimer
This content is educational. It does not replace assessment by a licensed occupational therapist, developmental paediatrician, or healthcare provider. Individual results may vary. Statistics represent aggregate outcomes across the Pinnacle Blooms Network.
© Copyright & Attribution
© 2025 Pinnacle Blooms Network®, unit of Bharath Healthcare Laboratories Pvt. Ltd. CIN: U74999TG2016PTC113063 | DPIIT: DIPP8651 | MSME: Udyog Aadhaar TS20F0009606 | GSTIN: 36AAGCB9722P1Z2
techniques.pinnacleblooms.org | Powered by GPT-OS® | Built by Mothers. Engineered as a System.
