
Back and Forth. All Day. Every Day.
Your son rocks. At the dinner table, his chair creaks with the steady rhythm. On the couch, in the car seat, at his school desk — back and forth, always, the same unconscious motion. You've tried telling him to stop, but his body finds the rhythm again before either of you notices. Family stares. Teachers worry. You wonder: is this a problem? A solution? Both?
9 Materials That Help With Constant Rocking — meeting the need the movement is trying to fill.
You are not failing. Your child's nervous system is speaking. And we understand exactly what it's saying.
🔬 Pinnacle Blooms Consortium
Sensory Solutions Series — A-084
Ages 2–12

You Are Among Millions
Constant rocking is one of the most commonly reported vestibular-seeking behaviours in paediatric development. It occurs across neurotypical and neurodivergent populations alike. When it persists beyond early toddlerhood and occurs continuously throughout the day, it signals a nervous system communicating a specific sensory need — one that can be systematically understood and addressed.
80%
Sensory Difficulties
of children with ASD experience sensory processing difficulties including vestibular seeking
1 in 54
Children in India
identified with autism spectrum conditions — each with a unique sensory profile
21M+
Families Worldwide
globally navigate repetitive motor behaviours including body rocking
In India alone, with an estimated 18 million individuals on the autism spectrum, sensory processing challenges including body rocking affect millions of children and families. Pinnacle Blooms Network serves these families across 70+ centres with 20M+ documented therapy sessions. You are not alone. You are among millions whose children's bodies seek rhythm — and there is a science-backed path forward.

The Vestibular System: Your Child's Internal Rhythm Engine
What's Happening
Deep inside your child's inner ear sits the vestibular system — the brain's movement processing centre. It detects every tilt, turn, and shift of the head, telling the brain: "Where am I in space? Am I moving? How fast?"
The Difference
In children who rock constantly, this system is often hypo-responsive — it needs more movement input than typical to register and process spatial information. The brain essentially turns up the volume on its need for movement signals.
What Rocking Does
Your child's body has discovered that rhythmic back-and-forth motion generates consistent vestibular input — feeding the system that craves it. The rocking isn't random. It's the nervous system's self-designed sensory diet. It's organised. It's purposeful. It's intelligent.
The Critical Reframe
This is a wiring difference, not a behaviour choice. Your child rocks because their vestibular system processes movement differently — not because they're being defiant, seeking attention, or developing a "bad habit." When we understand what the rocking is seeking, we can provide that input through varied, appropriate, and often more efficient means. That's what these 9 materials do.
📚 Frontiers in Integrative Neuroscience (2020): Comprehensive framework for evaluating sensory integration treatment in ASD. DOI: 10.3389/fnint.2020.556660
Your Child's Developmental Waypoint
Understanding where your child sits on the developmental timeline helps calibrate both your expectations and your intervention approach. Rocking is a normal part of early motor development — the question is whether it has modulated appropriately over time.
1
0–6 Months
Rhythmic movements common and typical — head rocking and body rocking before sleep are normal developmental patterns.
2
6–18 Months
Rocking frequency typically peaks as part of typical motor exploration and self-soothing. Entirely expected at this stage.
3
18 Months–3 Years
Most children naturally reduce rocking frequency as the vestibular system matures and motor repertoire expands.
4
3–12 Years ← Current Challenge Zone
Persistent, constant rocking beyond this window warrants evaluation — the vestibular system may need additional support.
Body rocking commonly co-occurs with: other vestibular-seeking behaviours (spinning, swinging excessively), proprioceptive seeking (crashing, jumping, heavy play), auditory processing differences, attention and focus challenges, anxiety, and sleep difficulties. If you recognise multiple patterns, a comprehensive developmental assessment provides the full picture.

Clinically Validated. Home-Applicable. Parent-Proven.
🛡️ Evidence Grade: Level I–II
Systematic Reviews + RCTs
Systematic Review (2024)
16 articles from 2013–2023 confirm: sensory integration intervention meets criteria to be considered evidence-based practice for children with ASD. Vestibular-based approaches showed consistent positive outcomes for sensory-seeking behaviours.
Meta-Analysis (2024)
24 studies analysed: Sensory integration therapy effectively promoted social skills, adaptive behaviour, sensory processing, and motor skills. 40-minute sessions showed maximum effectiveness. Individual 1:1 sessions produced strongest outcomes.
Indian RCT (2019)
Home-based sensory interventions demonstrated significant outcomes in the Indian paediatric population. Parent-administered sensory protocols showed measurable improvement when guided by professional frameworks.
🔗 DOI: 10.1007/s12098-018-2747-4
20M+ exclusive 1:1 therapy sessions across the Pinnacle Blooms Network with 97%+ measured improvement rate across sensory processing and self-regulation challenges — the largest real-world evidence dataset for paediatric developmental intervention in India.
Sensory Diet for Vestibular-Seeking Body Rocking
Parent-Friendly Name: "Meeting the Rocking Need — The 9-Material Approach"
A sensory diet for vestibular-seeking body rocking is a structured, multi-material approach to understanding and addressing the sensory needs that drive constant rocking behaviour. Rather than suppressing the rocking, this approach uses 9 categories of therapeutic materials to: (1) provide direct vestibular input more efficiently than rocking alone, (2) address complementary proprioceptive needs through deep pressure and heavy work, (3) offer rhythmic alternatives through bouncing, vibration, and music, (4) enable context-appropriate alternatives through fidget tools, and (5) structure proactive sensory input throughout the day through movement breaks and sensory diet planning.
🧩 Domain
Sensory Processing + Self-Regulation + Vestibular
👶 Ages
2–12 years
⏱️ Duration
10–30 min per session (varies by material)
🔄 Frequency
Daily sensory diet; individual materials 2–5× daily
Code: SENS-VEST-ROCK
Domain A: Sensory Processing
Sub-domain: Vestibular Seeking

A Multi-Disciplinary Approach
Because the brain doesn't organise by therapy type, meeting a child's vestibular needs effectively requires coordination across disciplines. Each professional brings a unique lens — together, they create a comprehensive, precisely calibrated sensory intervention.
Occupational Therapist (Primary Lead)
Designs the comprehensive sensory diet, selects vestibular and proprioceptive materials, conducts sensory processing evaluation, and monitors regulation progression. The OT understands which specific vestibular inputs your child needs and calibrates material selection accordingly.
Board Certified Behaviour Analyst (BCBA)
Conducts functional analysis of rocking — when it occurs, what triggers it, what maintains it. Designs data collection systems and implements reinforcement strategies for using alternative materials, ensuring the sensory approach aligns with behavioural goals.
NeuroDevelopmental Paediatrician
Rules out medical contributors. Evaluates rocking within the broader developmental profile. Provides diagnostic clarity — is the rocking isolated vestibular seeking, or part of a larger neurodevelopmental pattern? Prescribes therapy intensity.
Special Educator
Adapts the classroom environment for movement needs. Implements fidget alternatives and movement breaks in educational settings, ensuring the child's sensory needs don't interfere with learning — and that learning accommodates the child's neurological profile.
📚 Adapted UNICEF/WHO Nurturing Care Framework for SLPs (2022): DOI: 10.1080/17549507.2022.2141327

Precision Targets — Not a Random Activity, a Precision Tool
Parents will observe progress as a sequence: decreased rocking frequency → use of alternative materials with prompts → spontaneous choice of alternatives → context-appropriate strategy selection → well-regulated engagement. Each stage represents measurable neurological reorganisation — not just behaviour change.
📚 Meta-analysis (World J Clin Cases, 2024): SI therapy effectively promoted social skills, adaptive behaviour, sensory processing, and motor skills across 24 studies. PMC10955541

Your 9-Material Toolkit — Everything You Need
Each of the 9 material categories below targets a specific sensory need that drives constant rocking. Together, they form a complete, evidence-based toolkit that meets vestibular, proprioceptive, and rhythmic needs throughout the day.
1
Therapy Swing System
2
Rocking Seating Options
3
Weighted & Compression Items
4
Movement Break Cards & Systems
5
Bouncing & Vibration Tools
6
Heavy Work Equipment
Canon: Gross Motor & Movement | Weighted cart, climbing equipment, crawl tunnel, resistance bands
🔗Canon Link
🔗Canon Link
7
Rhythm & Music Tools
8
Fidget & Movement Alternatives
9
Sensory Diet Planning Tools
Total Investment Range: Essential Starter Kit: ₹1,000–5,000 | Complete 9-Material Toolkit: ₹8,800–70,000 | 🔗Full 687 Product Database

Every Family Can Start Today — Regardless of Budget
The WHO Nurturing Care Framework emphasises equity-focused, context-specific interventions. These household alternatives follow the same sensory principles as clinical-grade materials. Every child deserves access to evidence-based support — income is not a barrier.
Buy This | Make This (Zero-Cost Alternative) | |
Therapy swing (₹3,000+) | Standard playground swing used daily — 15 min morning + evening. Hammock tied between trees. Blanket swing held by two adults. | |
Rocking chair (₹2,000+) | Any wooden rocking chair (often ₹500 secondhand). Sit on a stability ball. Cross-legged rocking on a pillow. | |
Weighted blanket (₹1,500+) | Heavy quilt folded double. Rice-filled fabric bag. Firm, sustained bear hugs (20 seconds). | |
Movement break cards (₹200+) | Paper cards with hand-drawn activities: "10 jumps," "spin 5 times," "wall push-ups x10," "bear walks." Set phone timer every 45 minutes. | |
Therapy ball (₹1,000+) | Bouncing on bed (supervised). Hopping on the spot. Jumping rope. Rolling on the ground. | |
Heavy work equipment (₹500+) | Carrying grocery bags, pushing furniture, pulling a wagon of toys, wall push-ups, crab walks, wheelbarrow walks, kneading dough. | |
Rhythm instruments (₹300+) | Pots and wooden spoons as drums. Rice in sealed containers as shakers. Clapping games. Dance parties to rhythmic music. | |
Fidget tools (₹200+) | Rubber bands on chair legs for foot movement. Smooth stones in pockets. Fabric scraps with different textures. | |
Sensory diet planner (₹100+) | Paper schedule on the wall. Written list of activities by time of day. Simple tally marks on a notebook page. |
When professional-grade materials are non-negotiable: If your child requires specific vestibular input intensity that household items cannot safely provide, or if an OT has recommended specific therapeutic equipment, prioritise the clinical recommendation. 📚 WHO NCF Handbook (2022) | PMC9978394

Safety First — Read This Before Using Any Material
🔴 DO NOT PROCEED IF:
Child has a recent head injury, ear infection, or balance disorder diagnosis. Child shows nausea, extreme dizziness, or disorientation after movement. Seizure disorder triggered by vestibular input (consult neurologist first). Weighted items exceed 10–15% of child's body weight. Any material covers the child's face or restricts breathing. Equipment is damaged or not age-appropriate. Child is severely distressed.
🟡 MODIFY AND MONITOR IF:
Child has mild sensory defensiveness alongside vestibular seeking — start gentle. Child is recovering from illness — reduce intensity and duration. Child is unusually tired or hungry — meet basic needs first. You're using DIY materials — inspect thoroughly before each use. This is the first time using a new material — introduce gradually over 3–5 sessions.
🟢 PROCEED WHEN:
Child is fed, rested, and in a generally regulated state. Materials are properly assembled and inspected. Environment is clear of hazards. Parent/caregiver is fully present and attentive. You've read all material-specific safety notes.
Therapy Swings
Require proper installation and weight-rated hardware. Never leave child unsupervised. Watch for nausea after spinning.
Weighted Items
Follow the 10% of body weight rule. Never during unsupervised sleep for children under 5. Never over the face.
Trampolines & Heavy Work
Require safety net for minis, one child at a time, supervision always. Heavy work: effort, not maximum exertion — stop if pain occurs.
📚 Indian Journal of Pediatrics RCT (2019): Home-based sensory interventions safety protocols for parent-administered sessions. DOI: 10.1007/s12098-018-2747-4
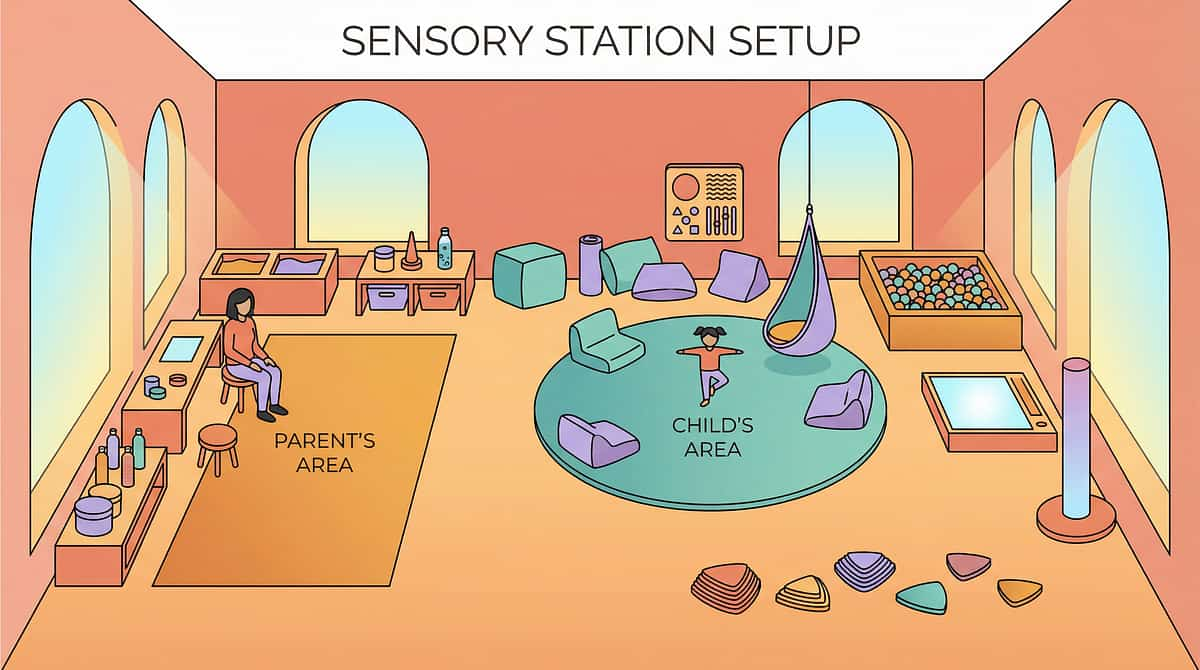
Your Home Sensory Station — Setting the Stage
Room Layout — 5 Key Positions
Vestibular Zone (Corner A)
Therapy swing or hammock mounted with proper hardware. Clear swing arc — nothing within 1.5 metres of full swing path. Padded yoga mat underneath.
Rocking Station (Corner B)
Rocking chair positioned against wall (prevents tipping). Wobble cushion on regular chair nearby. Books and calming activities placed here — the "permitted rocking" zone.
Heavy Work Zone (Open Area)
Clear floor space for pushing, pulling, crawling. Weighted items stored nearby. Resistance bands attached to sturdy furniture.
Rhythm Corner
Drums, shakers, and music tools near a speaker. Mat for dance and movement activities.
Parent Position
Within arm's reach of vestibular zone. Clear sight line to all activity areas. Seated at child's level when possible.
Environment Checklist
- Remove visual clutter from the immediate area
- Control noise level — reduce competing sounds
- Ensure adequate but not harsh lighting
- Room temperature comfortable — movement generates heat
- Fidget tools and movement break cards visible on wall
- Timer visible to both parent and child
- Sensory diet schedule posted at child's eye level

The 60-Second Pre-Session Check
Every effective session begins with a readiness check — a brief scan of your child's current state before introducing any sensory material. Starting from the right baseline makes the difference between a productive session and a difficult one.
1
Fed & Rested
Child has eaten within the last 2 hours and slept adequately — not hungry or overtired.
2
Emotionally Regulated
No meltdown or significant distress in the last 30 minutes. No signs of illness: fever, ear pain, or nausea.
3
Not Mid-Activity
Child is not in the middle of a preferred activity — don't interrupt deep engagement.
4
Caregiver Available
Parent/caregiver is calm and fully present — not rushed, not distracted.
🟢 All Checks Passed — GO
Begin with Step 1: The Invitation. You're ready for a full session.
🟡 4–6 Checks — MODIFY
Choose ONE material, reduce session to 5 minutes, maintain playful tone. Don't push for more.
🔴 Fewer Than 4 — POSTPONE
Do a calming activity instead: gentle rocking together, deep pressure hugs, quiet music. Try again later.
"The best session is one that starts right. Postponing is not failure — it's wisdom."

Step 1 of 6
The Invitation — Not a Command
1
For a Swing Session
"Hey [child's name], look at the swing! I wonder what it feels like to fly today? Should we try? I'll push — you tell me how high."
2
For a Rocking Chair
"I set up your special rocking chair. Want to rock while we read? You can rock as much as you want in this chair."
3
For a Movement Break
"It's movement time! Pick a card — which one do you want to try first?" [Show movement break cards]
✅ Acceptance Cues
- Child approaches the material or reaches for it
- Child stops rocking briefly and orients toward you
- Any verbal or non-verbal assent
⚠️ Resistance Cues
Child turns away, pushes material away, or increases rocking intensity.
Response: "That's okay. It's here when you're ready." Place material within view, step back, try again in 5 minutes. Do NOT force.
⏱️ Timing: 30–60 seconds

Step 2 of 6
The Engagement — Meeting the Material
Therapy Swing
Help the child onto the swing gently. Start with very slow, linear (back-and-forth) movement. Let the child set the rhythm. "Is this good? Want it faster? Slower?" Follow the child's cues at every moment.
Weighted Blanket/Vest
Drape the weighted item gently over the child's lap or shoulders. "How does that feel? Heavy? Cosy?" Observe for 30 seconds. Watch for relaxation signs: shoulders drop, breathing slows, rocking decreases.
Heavy Work
"Can you help me push this box to the wall? I need someone really strong!" Make it a game, not a task. Celebrate the effort generously and specifically.
Engagement ✅
Child actively participates, smiles, requests more → Continue and gradually increase intensity.
Tolerance 🟡
Child accepts passively but doesn't resist → Continue at current level, don't push further.
Avoidance 🔴
Child pulls away, cries, or increases rocking → Stop this material. Try a different one. This is data, not failure.
⏱️ Timing: 1–3 minutes
📚 Systematic review (Children, 2024): Sensory integration intervention with structured material introduction meets EBP criteria. PMC11506176

Step 3 of 6
The Therapeutic Action — The Active Ingredient
Vestibular Materials (Swings, Rocking Chairs, Bouncing)
The child is now receiving direct vestibular input. Maintain the rhythm long enough for the vestibular system to process and organise — minimum 5 minutes for therapeutic effect. Observe: does the rocking elsewhere in the body decrease as the swing/bounce provides input? This is the signal the vestibular system is being fed.
Proprioceptive Materials (Weighted Items, Heavy Work)
The child is receiving deep pressure or muscle resistance. Weighted blanket: maintain for 10–15 minutes minimum. Heavy work: sustained effort (pushing, pulling, carrying) for 3–5 minutes. Observe: does the child appear calmer, more grounded, less driven to move?
Rhythmic Alternatives (Music, Bouncing, Vibration)
The child is channelling the rhythmic need through a different modality. The therapeutic action is active, participatory rhythm creation — drumming, bouncing, dancing. Not passive listening. The child generates rhythm through their own action.
❌ Common Error: Stopping Too Soon
Vestibular input needs sustained duration (5+ minutes) for therapeutic effect. Don't end the session at the first sign of success.
❌ Common Error: Forcing Intensity
Always let the child control speed and force. Parent must be present and engaged — not on their phone.
❌ Common Error: Mixing Too Many Materials
One material per session when starting out. Complexity can be added gradually as the child becomes comfortable.
⏱️ Duration: 5–15 minutes depending on material

Step 4 of 6
Repeat & Vary — Therapeutic Dosage
Vestibular Input
1 sustained session of 5–15 minutes is typically sufficient. Can repeat 2–3× daily if tolerated.
Proprioceptive Input
Heavy work can be repeated frequently — 5–10 brief episodes throughout the day (carrying groceries, pushing chairs, wall push-ups between activities).
Rhythmic Input
5–10 minutes per session. Can happen multiple times daily. Best before transitions and during high-rocking periods.
Movement Breaks
Every 45–60 minutes during structured activities. 3–5 minutes each. This is the backbone of the proactive sensory diet.
Variation Options — To Maintain Engagement
1
Swing Variations
Vary direction (linear, lateral, circular), speed, and position (seated, prone). Each variation stimulates different vestibular pathways.
2
Rocking Chair Variations
Vary activities while rocking: reading, puzzles, talking. The movement remains constant; the engagement changes.
3
Heavy Work Variations
Rotate between pushing, pulling, carrying, and climbing. Variety prevents habituation and maintains therapeutic novelty.
"3 good repetitions are worth more than 10 forced ones." Watch for satiation indicators: child moves away from the material, attention clearly wanders, visible fatigue, or child starts a different activity spontaneously.

Step 5 of 6
Reinforce & Celebrate — The Power of 3 Seconds
When child uses a material instead of rocking
"You chose the swing! That was such a smart choice for your body!"
When child completes a heavy work task
"You pushed that all the way! Your muscles are so strong!"
When child uses a fidget in a quiet setting
"I saw you use your fidget at the table — that's really clever."
Timing
Within 3 seconds of the behaviour. Immediate reinforcement creates the strongest learning signal.
Specificity
Name the exact behaviour: not "good job" but "good job using the swing." Specificity builds understanding.
Celebrate Attempts
Child who walks toward the swing but doesn't get on still earns reinforcement. Progress, not perfection.
Important Frame: We are NOT reinforcing "not rocking." We are reinforcing "using alternative materials." The frame is expansion, not elimination. Reinforcement options: verbal praise, high-five, preferred activity for 2 minutes, sticker toward a larger reward.

Step 6 of 6
The Cool-Down — Ending Well
"Two more pushes on the swing, then we're all done for now." [After 2 pushes]: "All done! That was great swinging. Let's slow down together."
1
Slow Rhythmic Wind-Down
Slow, gentle rocking together — yes, rocking is permitted here as a regulated cool-down. This validates the child's primary strategy while marking the transition.
2
Deep Pressure Reset
Firm hug, weighted blanket on lap, or quiet breathing: "Let's take 3 big belly breaths together." This grounds the nervous system.
3
Material Put-Away Ritual
Child helps put materials back — proprioceptive input + routine closure. This builds both muscle work and predictable endings.
4
Transition with Visual Cue
"Swing time is done, now it's [next activity] time." Let child carry a fidget tool as they move to the next activity as a transition bridge.
⏱️ Timing: 1–2 minutes
📚 Visual supports classified as evidence-based practice for autism (NCAEP, 2020). 🔗https://ncaep.fpg.unc.edu/

60 Seconds of Data Now Saves Hours of Guessing Later
Recording a few simple data points immediately after each session transforms your home practice from "something we try" into a personalised, evidence-generating intervention. This data directly feeds the GPT-OS® system and helps your therapist calibrate the next recommendation.
1. Materials Used Today
☐ Swing ☐ Rocking chair ☐ Weighted items ☐ Movement break ☐ Bouncing ☐ Heavy work ☐ Rhythm/music ☐ Fidget tools ☐ Sensory diet plan
2. Engagement Level
😊 Highly engaged → 😐 Tolerating → 😞 Resisted → ❌ Session abandoned
Circle the one that best describes today's session.
Circle the one that best describes today's session.
3. Rocking After Session
↓↓ Noticeably less → ↓ Slightly less → ↔ Same → ↑ Slightly more → ↑↑ Noticeably more
Bonus — if time permits: Duration of session (minutes), time of day (Morning/Midday/Afternoon/Evening), child's state before session (Calm/Moderate/Dysregulated).
"This data feeds GPT-OS® and helps your therapist personalise the next recommendation. Every data point improves the system for your child and for millions of others."

It Didn't Go Perfectly? That's Normal. Here's What To Do.
❓ "My child refused to get on the swing/use the material"
Why: Novelty anxiety. Sensory-seeking children can paradoxically resist new sensory experiences.
Fix: Place the material in the room for 2–3 days without asking the child to use it. Let them observe and approach on their own terms. Model it yourself: "Mum is going to swing for a bit."
Fix: Place the material in the room for 2–3 days without asking the child to use it. Let them observe and approach on their own terms. Model it yourself: "Mum is going to swing for a bit."
❓ "The rocking got WORSE after using the material"
Why: Some vestibular input can temporarily increase arousal before organising — this is nervous system processing, not failure.
Fix: Follow vestibular activity with heavy work to "ground" the input. If rocking consistently increases, reduce intensity and duration. Consult your OT.
Fix: Follow vestibular activity with heavy work to "ground" the input. If rocking consistently increases, reduce intensity and duration. Consult your OT.
❓ "My child only wants ONE material and refuses all others"
Why: That material is meeting a specific need effectively. This is information, not a problem.
Fix: Use the preferred material consistently for 2 weeks. Then slowly introduce a second material alongside the preferred one. Expansion is gradual.
Fix: Use the preferred material consistently for 2 weeks. Then slowly introduce a second material alongside the preferred one. Expansion is gradual.
❓ "The session lasted only 2 minutes before my child walked away"
Why: Two minutes of engagement IS progress — especially in early sessions.
Fix: Accept short sessions. 2 minutes × 5 sessions/day = 10 minutes of sensory input. Frequency can compensate for duration.
Fix: Accept short sessions. 2 minutes × 5 sessions/day = 10 minutes of sensory input. Frequency can compensate for duration.
❓ "Other family members criticise the approach"
Why: Extended family often lack understanding of sensory processing neuroscience.
Fix: Share the brain science card with them. Frame it as: "The therapist recommended this specific approach." The family guide in Card 37 is designed for exactly this conversation.
Fix: Share the brain science card with them. Frame it as: "The therapist recommended this specific approach." The family guide in Card 37 is designed for exactly this conversation.
❓ "My child became severely distressed during the session"
Why: The material may have triggered sensory overload, or the child was not in a regulated starting state.
Fix: Stop immediately. Provide deep pressure — firm hug or weighted blanket. Return to baseline. Review the readiness check for next time. Do NOT force re-engagement today.
Fix: Stop immediately. Provide deep pressure — firm hug or weighted blanket. Return to baseline. Review the readiness check for next time. Do NOT force re-engagement today.
"Session abandonment is not failure — it's data. Every attempt teaches you and your child something."

No Two Children Are Identical — Adapt This to Yours
1
Easier Version
1 material, 2–5 min, passive acceptance OK, parent-directed. For: first 1–2 weeks, bad days, new materials, ages 2–3.
2
Standard Version
2–3 materials per day, 10–15 min, active engagement, child-directed choices. For: established routine, moderate engagement, ages 3–8.
3
Advanced Version
Full 9-material rotation, 20+ min, independent material selection, contextual modulation practice. For: weeks 5+, highly engaged children, ages 6–12.
Vestibular SEEKER (rocks intensely, seeks fast movement)
Prioritise: Therapy swings (fast, linear), trampoline, spinning. Increase duration and intensity of vestibular input. Follow with heavy work to ground the input.
Vestibular AVOIDER who also rocks (paradoxical pattern)
Prioritise: Slow, linear rocking chair (controlled, predictable). Avoid fast or unpredictable movement initially. Build tolerance gradually — 10% increase per week.
Rocks Primarily When ANXIOUS
Prioritise: Weighted/compression items, rocking chair, calming music. Focus on predictability and control — child chooses when and how. Address anxiety triggers alongside sensory needs.
Rocks Primarily When BORED/UNDERSTIMULATED
Prioritise: Movement breaks, heavy work, rhythm instruments. Schedule sensory activities every 30–45 minutes during low-stimulation periods — proactive input before boredom sets in.

Progress Arc
Weeks 1–2
Weeks 1–2: Tolerance, Not Transformation
What You MAY See
- Child tolerates 1–2 new materials for brief periods (even 2 minutes counts)
- Slight reduction in rocking intensity during or immediately after material use
- Child shows curiosity toward materials — approaching, touching, observing
- Rocking may temporarily increase in some contexts (nervous system recalibrating — not a setback)
What Is NOT Expected Yet
- Dramatic reduction in rocking frequency
- Independent material selection
- Contextual modulation
- Complete behaviour change
"If your child sat in the rocking chair for 3 minutes today when last week they wouldn't even sit in it — that is real, measurable, neurologically significant progress. The vestibular system is beginning to trust this new input source."
This is the patience phase. Your brain wants dramatic change. Your child's nervous system needs time to build new pathways. Two weeks of consistent exposure creates the foundation. The visible changes come in Weeks 3–4.
📚 Systematic review (Children, 2024): SI intervention outcomes emerge across 8–12 week timelines. Early-phase indicators focus on tolerance and participation rather than skill mastery. PMC11506176

Progress Arc
Weeks 3–4
Weeks 3–4: The Nervous System Is Reorganising
Consolidation Indicators
Child begins to anticipate sensory sessions — moves toward materials, requests swing or bounce. Rocking intensity noticeably reduced during and for 30–60 minutes after vestibular input. Child accepts 2–3 different materials without resistance.
Emerging Spontaneous Behaviours
Child walks toward the swing without being invited. Sits in the rocking chair by choice during free time. Requests bouncing or drumming. Uses fidget tools when offered in structured settings.
When to Increase Complexity
Add a new material from the 9-material toolkit. Extend session duration by 2–3 minutes. Increase frequency of movement breaks. The nervous system is ready for more.
"You may notice you're more confident too. You're reading your child's signals better. You're anticipating the high-rocking times and providing input before the need builds. You're becoming your child's sensory strategist."

Progress Arc
Weeks 5–8
Weeks 5–8: Mastery Emerging
🏆 Mastery Criterion 1
Rocking is less constant — occurs in specific contexts (excitement, stress, concentration) rather than continuously throughout the day.
🏆 Mastery Criterion 2
Child uses 3+ different materials/strategies without prompting. Independent material selection is emerging.
🏆 Mastery Criterion 3
Contextual modulation emerging: rocking chair at home, fidget tool at school, movement break between activities — right tool, right context.
🏆 Mastery Criterion 4
Vestibular needs met proactively through daily routine — sensory diet running smoothly as natural part of the day.
🏆 Mastery Criterion 5
Functional improvement in 2+ areas: attention, social participation, sleep, or engagement in structured activities. Family members notice the change.
Maintenance Check: Reduce structured sessions to see if regulation maintains. If rocking increases when the sensory diet stops — the sensory diet is working; continue it. If regulation maintains with reduced input — the nervous system has built new pathways.

You Did This. Your Child Grew Because of Your Commitment.
Weeks ago, you arrived at this page confused — wondering if your child's constant rocking was a problem, a solution, or both. You didn't know if you should stop it, allow it, or do something different.
Now you know: it was the nervous system speaking. You learned to listen. You learned to answer — with swings and rocking chairs, with weighted blankets and movement breaks, with drums and bouncing balls and heavy work and fidget tools. You built a sensory diet. You met the need.
The rocking may not be gone entirely. Your child may still rock sometimes — when excited, when stressed, when deeply concentrating. And that's okay. Because now they have choices. The rocking is no longer the only tool in the box. It's one strategy among many. And when your child rocks in their rocking chair while reading at bedtime — that's not a problem. That's self-regulation.
📸 Family Celebration Suggestion
Take a photo of your child using their favourite material from the 9-material toolkit. Save it. In 6 months, look at it and remember: you built this.
🌟 Share Your Journey
Other families are right now where you were weeks ago. Your experience is their hope. Consider sharing your journey with the Pinnacle community.

Trust Your Instincts — When to Pause and Ask
🚩 Rocking has significantly INCREASED despite consistent sensory diet for 4+ weeks
The sensory diet may need recalibration — the vestibular input provided may not match the child's specific need. Consult your occupational therapist for a revised sensory profile assessment.
🚩 Child has begun HEAD BANGING in addition to rocking
This raises immediate safety concerns. Seek consultation with a developmental specialist and OT without delay. Do not attempt to manage head banging with home materials alone.
🚩 Child appears DISORIENTED, nauseous, or unsteady after vestibular activities
Over-stimulation of the vestibular system. Stop vestibular input immediately. This response may indicate specific vestibular processing patterns requiring professional assessment.
🚩 Child has LOST previously achieved skills
Developmental regression in speech, social engagement, or daily living skills requires immediate medical evaluation regardless of context.
🚩 Rocking accompanied by NEW concerning behaviours
Self-injury, extreme aggression, or complete social withdrawal alongside rocking requires comprehensive developmental and behavioural assessment.
🚩 Child appears to be in PAIN while rocking or resists being stopped with extreme distress
Rule out ear infections, dental pain, GI discomfort, or other medical causes that may be driving the rocking as a pain-coping mechanism.
Self-Resolve
Adjust technique at home
Teleconsultation
Pinnacle OT video call
In-Person Clinic
Centre visit
Full Assessment
Comprehensive developmental evaluation
Your Child's Journey: Where You've Been and Where You're Going
This technique feeds into the Sensory Processing Index and Self-Regulation Index within GPT-OS® — tracking your child's journey toward well-modulated vestibular processing and diverse self-regulation strategies for life readiness.
Path A — Vestibular Seeking Remains Primary
→ A-088: Child Seeks Intense Movement Constantly
→ K-1100: Understanding Vestibular Seeking (deep parent education)
→ K-1100: Understanding Vestibular Seeking (deep parent education)
Path B — Co-Occurring Repetitive Behaviours
→ A-085: Child Has Hand Flapping
→ A-086: Child Makes Repetitive Sounds
→ A-086: Child Makes Repetitive Sounds
Path C — Anxiety-Driven Rocking
→ Anxiety regulation technique series
→ Emotional self-regulation toolkit
→ Emotional self-regulation toolkit

More Sensory Solutions — Techniques You Can Explore
Your investment in this 9-material toolkit carries forward. Many of the materials you've already acquired apply directly to the techniques below — you've already started building your sensory library.

A-082: 9 Materials for Constant Spinning
Core | Uses: Therapy swing, weighted items, movement breaks ✓

A-083: 9 Materials for Crashing Into Things
Core | Uses: Heavy work equipment, weighted items ✓

A-085: 9 Materials for Hand Flapping
Core | Uses: Fidget tools, rhythm instruments ✓

A-086: 9 Materials for Repetitive Sounds
Core | Uses: Rhythm instruments, sensory diet tools ✓
This Technique Is One Piece of a Larger Plan
Current Technique Position
Domain A — feeding into the Sensory Processing Index and Self-Regulation Index. Addressing vestibular seeking through this sensory diet also positively impacts:
- Domain D: Emotional Regulation — expanded calming strategies
- Domain G: Gross Motor — through heavy work and movement
- Domain C: Social — reduced socially interfering behaviours
- Domain I: Academic — improved sustained attention
The Larger Plan
"This technique is one piece of a larger plan. GPT-OS® maps your child's entire developmental landscape and coordinates interventions across all domains — so no need is addressed in isolation."

Real Families. Real Progress. Real Hope.
Before — Parent, Hyderabad
"The rocking was constant — his chair, his car seat, standing, sitting, everywhere. The pediatrician said he'd grow out of it, but he didn't. Every surface he sat on became a rocking surface. Teachers complained. Family stared."
After (12 Weeks) — Parent, Hyderabad
"When we started OT, they explained it wasn't a 'bad habit' — his nervous system needed that input. We got a swing, started a sensory diet, bought a rocking chair for his room, and built heavy work into every day. The rocking isn't constant anymore. He has other ways to get what he needs now."
Before — Parent, Bangalore
"She rocked so intensely during school that her desk moved across the floor. Other kids teased her. She didn't even know she was doing it."
After (8 Weeks) — Parent, Bangalore
"The wobble cushion was a game-changer for school. At home, the trampoline before homework made everything easier. Her teacher says the desk doesn't move anymore. She still uses her wobble cushion every day — but by choice now, not by compulsion."
"Both families show the typical pattern: the rocking doesn't disappear — it transforms. From constant and unmodulated to occasional and contextual. The child's regulatory toolkit expands from one strategy to many."
— Senior Occupational Therapist, Pinnacle Blooms Consortium
⚠️ Illustrative cases; individual outcomes vary by child profile.

You Are Not Doing This Alone
Connection with others who understand your experience is itself a form of support. The Pinnacle community connects parents navigating the same challenges with shared wisdom, professional guidance, and the simple comfort of being understood.
Sensory Processing Parent Community
WhatsApp group for parents navigating vestibular seeking, body rocking, and sensory regulation challenges. Share strategies, ask questions, find understanding from parents who've been exactly where you are.
Pinnacle Parent Meetups
Monthly meetups at your nearest Pinnacle centre. Connect with families in your city who understand. Find your nearest centre: pinnacleblooms.org/centers
Peer Mentoring
Connect with an experienced parent who has completed this same journey. They've been where you are. Their wisdom is yours. Request a peer mentor through the Pinnacle community portal.
Pinnacle Online Community
Forum for deeper discussions, resource sharing, and daily support. Join at
"Your experience helps others. Consider sharing your journey — the parent who is right now where you were weeks ago is looking for someone exactly like you."
Home + Clinic = Maximum Impact
Find Professional Support
Your Primary Therapy Team for Constant Rocking
- 🧠Occupational Therapist — specialising in sensory integration (Primary Lead)
- 📊BCBA — for functional analysis and reinforcement strategies
- 🏥NeuroDevelopmental Paediatrician — for diagnostic context and prescription
Teleconsultation Available
Can't visit a centre? Video consultations are available nationwide.
📱 Book online: pinnacleblooms.org/teleconsult
📞 Or call: 9100 181 181 (FREE, 24/7, 16+ languages)
📱 Book online: pinnacleblooms.org/teleconsult
📞 Or call: 9100 181 181 (FREE, 24/7, 16+ languages)
Why Both Matter
Home-based intervention is powerful. Professional guidance makes it precise. The sensory diet you're building at home becomes dramatically more effective when calibrated by an occupational therapist who understands your child's specific vestibular processing profile.
Start at home now. Consult an OT for precision calibration. Both together is where the deepest impact lives.

The Science Behind What You're Doing
For the curious parent and the clinician seeking rigour — the evidence base behind this approach is robust, multi-source, and internationally validated.
1. PRISMA Systematic Review (2024) — Level I
16 articles confirm SI intervention is EBP for children with ASD. 🔗PMC11506176
2. Meta-Analysis: SI Therapy Efficacy (2024) — Level I
24 studies: SI therapy promotes social skills, adaptive behaviour, sensory processing, motor skills. 🔗PMC10955541
3. Indian RCT: Home-Based SI (2019) — Level II
Padmanabha et al.: Home-based sensory interventions demonstrate significant outcomes in the Indian paediatric population. 🔗 DOI: 10.1007/s12098-018-2747-4
4. WHO CCD Package (2023) — Level I Policy
Age-specific caregiver recommendations across 54 countries with measured child development outcomes. 🔗PMC9978394
5. NCAEP Evidence-Based Practices (2020)
Sensory-based interventions and visual supports classified as EBPs for autism. 🔗ncaep.fpg.unc.edu
Additional sources: SPD Foundation | WHO Nurturing Care Framework | Ayres Sensory Integration foundational research

Your Data Powers the System That Powers Your Child's Progress
What GPT-OS® Learns From This Technique
- Which materials most effectively reduce rocking for children with this vestibular profile
- Optimal dosage patterns — frequency, duration, time of day
- Progression timelines for similar presentations
- Which children need earlier professional intervention vs. home-based success
Privacy Assurance
Your data is encrypted, anonymised at the population level, and never shared with third parties. GPT-OS® complies with Indian data protection standards. Your child's individual data is accessible only to you and your authorised therapy team.
"Your data helps every child like yours. And every child like yours helps your child."

Watch the 60-Second Video: 9 Materials That Help With Constant Rocking
🎬 Reel A-084
9 Materials That Help With Constant Rocking
Sensory Solutions Series — Episode 84
Domain: Sensory Processing + Self-Regulation + Vestibular
Duration: 60 seconds
Sensory Solutions Series — Episode 84
Domain: Sensory Processing + Self-Regulation + Vestibular
Duration: 60 seconds
What You'll See
All 9 materials demonstrated by a Pinnacle Blooms therapist: therapy swings, rocking chairs, weighted items, movement breaks, bouncing tools, heavy work, rhythm instruments, fidget alternatives, and sensory diet planning. Visual reference for everything you've read on this page.
Why Video Matters
Video modelling is classified as an evidence-based practice for autism (NCAEP, 2020). Seeing a therapist demonstrate materials through video significantly improves parent skill acquisition — making this reel a clinical tool, not just content.

Consistency Across Caregivers Multiplies Impact
If only one parent knows the approach, it's limited. When every caregiver — spouse, grandparent, teacher, nanny — understands the function of rocking and the 9-material strategy, the child receives consistent, around-the-clock sensory support. That's when transformation accelerates.
Family Guide (1-Page PDF)
Print-ready summary of the 9 materials, key safety notes, and daily schedule template. Designed to go on the fridge or wall of every room where the child spends time.
"Explain to Grandparents" Version
Simplified, non-clinical explanation of why the child rocks and what the materials do. Designed for extended family who may not understand sensory processing — warm, accessible, and non-judgmental in tone.
Teacher/School Communication Template
Professional letter explaining sensory needs, recommended accommodations (wobble cushion, movement breaks, fidget tools), and contact information for your OT. In India, the RPWD Act (2016) supports accommodations for children with developmental differences.
📱 Share via WhatsApp
Pre-formatted message with page link
📧 Share via Email
Email template with key takeaways
🔗 Copy Link
techniques.pinnacleblooms.org/sensory-processing/9-materials-constant-rocking
📚 WHO CCD Package: Multi-caregiver training is critical for intervention generalisation and maintenance. PMC9978394

Common Questions About Rocking and Sensory Strategies
Q1: Is constant rocking a sign of autism?
Body rocking is common in autism but is not exclusive to autism. Many neurotypical children rock for sensory regulation. Rocking alone is not diagnostic — it should be evaluated within a comprehensive developmental assessment that considers the full profile, including communication, social interaction, play, and behavioural patterns.
Q2: Should I try to stop my child from rocking?
Generally, no — not through force or repeated "stop" commands. Rocking serves a regulatory function for your child's nervous system. Suppressing it without providing alternatives creates frustration without addressing the underlying need. This 9-material approach provides alternative ways to meet the same need.
Q3: Will my child ever stop rocking completely?
Many children (and adults) continue some degree of rhythmic movement as a regulatory strategy — this is normal and healthy. The goal is not elimination but modulation: reducing constant, interfering rocking to occasional, contextual, well-managed rocking alongside a diverse toolkit of other strategies.
Q4: How long before I see results?
Most families notice initial tolerance of materials in weeks 1–2, consolidation in weeks 3–4, and meaningful regulation changes in weeks 5–8. Consistent daily sensory diet implementation is key. Results vary by child — some respond faster, some need longer timelines.
Q5: Can I implement these materials without an OT?
You can absolutely start with the materials and strategies in this guide. Many families achieve meaningful improvement through home implementation. However, an OT's comprehensive sensory evaluation can identify your child's specific vestibular processing profile and calibrate the approach for maximum effectiveness. We recommend both: start at home now, consult an OT for precision calibration.
Q6: What if the school won't allow movement breaks or fidget tools?
You have a right to request accommodations for your child's sensory needs. The school letter template in Card 37 provides professional language. An occupational therapist's written recommendation carries clinical authority. In India, the RPWD Act (2016) supports accommodations for children with developmental differences.
Q7: My child only wants to swing and ignores all other materials. Is that okay?
Yes, for now. The child's preferred material is clearly meeting their strongest need — use it consistently. Introduce additional materials gradually alongside (not instead of) the preferred one. Expansion is a months-long process, not a days-long one.
Q8: Is rocking harmful to my child physically?
Gentle to moderate rocking is not physically harmful. Intense rocking that involves head banging, causes bruising, or moves heavy furniture warrants safety assessment. The rocking itself doesn't damage the brain or body — it's a neurological regulatory strategy.
Didn't find your answer? 🤖 GPT-OS® Parent Chat | 📞9100 181 181 (FREE, 24/7) | 📅Book a teleconsultation

You've Read the Science. You Understand the Need. Now Start.
🟢 Start This Technique Today
Launch your first sensory session using the 9-material protocol. Begin with Step 1: The Invitation. Track your data after the session.
📞 Book a Consultation
Connect with a Pinnacle Blooms OT for personalised sensory diet design. Call: 9100 181 181 | Book online: pinnacleblooms.org/teleconsult
🔄 Explore Next Technique
🔬Validated by the Pinnacle Blooms Consortium
OT • SLP • ABA • SpEd • NeuroDev • CRO
20M+ sessions | 97%+ improvement | 70+ centres
Powered by GPT-OS® Therapeutic Intelligence
Preview of 9 materials that help with constant rocking Therapy Material
Below is a visual preview of 9 materials that help with constant rocking therapy material. The pages shown help educators, therapists, and caregivers understand the structure and content of the resource before use. Materials should be used under appropriate professional guidance.




















Share this resource
Help others discover thisLink copied!

From Fear to Mastery. One Technique at a Time.
"Every parent who arrives at this page arrives scared, confused, or exhausted. By the time they reach this card, they understand the science, hold the tools, and own the confidence to transform their home into a therapeutic environment. From fear to mastery — that is the Pinnacle promise. And this is just one technique among 70,000+."
🔬 Pinnacle Blooms Consortium
CRO | Occupational Therapy | Speech-Language Pathology | Applied Behaviour Analysis | Special Education | NeuroDevelopmental Paediatrics
📞 FREE National Autism Helpline
9100 181 181 — 24/7, 16+ languages. No question too small. No family turned away.
🌐 techniques.pinnacleblooms.org
Built by Mothers. Engineered as a System. Powered by GPT-OS® Therapeutic Intelligence.
Medical Disclaimer: This content is educational. It does not replace assessment by a licensed occupational therapist, developmental specialist, or healthcare provider. Persistent repetitive motor behaviours, especially when accompanied by other developmental concerns, should be evaluated within a comprehensive developmental and sensory processing assessment. Individual results may vary. Statistics represent aggregate outcomes across the Pinnacle Blooms Network.
© 2025 Pinnacle Blooms Network®, unit of Bharath Healthcare Laboratories Pvt. Ltd. All rights reserved. CIN: U74999TG2016PTC113063 | DPIIT: DIPP8651 (Govt. of India) | GSTIN: 36AAGCB9722P1Z2
