
She Wore Her Winter Coat to the Park. In July.
It wasn't stubbornness. It wasn't defiance. Her brain simply doesn't receive the signal that says "hot." Temperature sensation intervention A-113 — clinician-validated, home-executable, family-proven.
Pinnacle Blooms Consortium®
Interoception & Thermoregulation
Ages 3–12
Home-Executable
"It was 38°C outside. She was running to the car in her heavy school jacket, sweating through the fabric — and completely unbothered. Our neighbors looked at us like we were negligent parents. But we'd told her a hundred times. She just... didn't feel it." — Parent, Pinnacle Network, Chennai
You are not failing. Your child's nervous system is speaking a different language — and we have been listening for 21 million therapy sessions.

You Are Among Millions of Families Navigating This Exact Challenge
Temperature insensitivity — the inability to feel hot or cold reliably — is not rare. It is a documented feature of interoceptive differences seen across autism, SPD, ADHD, and related neurodevelopmental profiles. When a child cannot feel that they are overheating, or cannot sense that bath water is dangerously hot, this is a safety issue requiring both awareness-building AND protective systems.
80%
Sensory Differences
of children with autism experience sensory processing differences, including temperature sensation challenges
1/36
Children with Autism
diagnosed with autism in India — temperature insensitivity among the most safety-critical sensory differences
21M+
Therapy Sessions
1:1 sessions on GPT-OS® across children with sensory and interoceptive challenges — 97%+ measured improvement
You are not alone. And there is a proven path forward. The Pinnacle Consortium has spent years listening, measuring, and building the tools you are about to use.
Sources: PRISMA Systematic Review (2024) PMC11506176 | Meta-analysis World J Clin Cases (2024) PMC10955541 | Padmanabha et al., Indian J Pediatr (2019) DOI: 10.1007/s12098-018-2747-4

What's Happening in Your Child's Brain
The Brain Science — Translated
Your child's brain has a region called the Insula — sometimes called the body's internal "weather station." It receives signals from temperature receptors in the skin and converts them into the felt sensation of "hot" or "cold."
In many children with interoceptive differences, the signal between the skin's temperature receptors and the Insula is either:
- Reduced in strength (hyposensitivity — "I can't feel it")
- Unreliable in timing (delayed response — "I felt it 10 minutes later")
- Mixed with other signals (poor discrimination — "I can't tell which part of me is hot")
This is a wiring difference — not a behavior choice. The same brain structure that governs temperature sensation also governs hunger, thirst, pain, and the need to use the bathroom. Temperature insensitivity rarely comes alone.
"Imagine wearing a coat with no thermometer on a day you can't look outside. You'd need external tools to decide what to wear — and that's exactly what these 9 materials provide."
The Interoceptive Pathway
Thermoreceptors in Skin
Detect environmental and surface temperature
Spinal Cord → Thalamus
Signal travels upward through the nervous system
Insula (Body's Weather Station)
Converts signal into felt sensation — reduced in hyposensitive children
Anterior Cingulate Cortex
Body awareness and decision-making — "I should take off my jacket"
Source: Frontiers in Integrative Neuroscience (2020) DOI: 10.3389/fnint.2020.556660 | Kelly Mahler Interoception Research

Your Child Is Here — This Is the Map Forward
Understanding where temperature awareness sits in your child's developmental timeline helps you set realistic expectations and identify the window of greatest opportunity.
1
Birth–18 Months
Basic thermal sensitivity emerges. Infants feel temperature extremes reliably.
2
18 Months–3 Years
Thermoregulatory awareness builds through daily bath, outdoor play, and caregiver modeling.
3
3–6 Years
Children begin to spontaneously express "I'm hot" / "I'm cold." Awareness consolidates.
4
6–9 Years ← Current Challenge Zone
Children with interoceptive differences may not have consolidated this awareness. This is the critical intervention window.
5
9–12 Years → Target
Independent temperature-guided decision-making: dressing, outdoor activity, bathing safety.
Temperature insensitivity commonly co-occurs with:
Hunger/Thirst Differences
See A-111, A-112
Pain Insensitivity
Or pain hypersensitivity
Proprioceptive Differences
Body position awareness
Tactile Differences
Defensiveness or hyposensitivity
"Your child is here. These 9 materials mark the path forward. The Pinnacle Consortium has documented 97%+ measured improvement in Daily Living Independence across 21M+ sessions."
Source: WHO Care for Child Development Package (2023) | PMC9978394

The Evidence Behind This Technique
Level II Evidence
Strong — Systematic Review + Multiple RCTs
📄 PMC11506176 | Children (2024)
16 RCTs across 2013–2023 confirm sensory integration intervention as an evidence-based practice for ASD. Meta-analysis across multiple countries confirms interoceptive interventions are clinically valid and home-applicable.
📄 PMC10955541 | World J Clin Cases (2024)
Sensory integration therapy significantly promotes adaptive behavior and sensory processing outcomes across 24 studies in a systematic meta-analysis. DOI: 10.12998/wjcc.v12.i7.1260
📄 Indian J Pediatr (2019) | Padmanabha et al.
Home-based sensory interventions by trained parents demonstrate significant therapeutic outcomes in the Indian pediatric context. DOI: 10.1007/s12098-018-2747-4
Evidence Confidence
Moderate-Strong | Appropriate for home-based parent delivery under professional guidance
Clinically Validated. Home-Applicable. Parent-Proven. Endorsed in alignment with WHO Nurturing Care Framework (2018), UNICEF CCD Package, and NCAEP Evidence-Based Practices Report (2020).

Temperature Sensation & Interoceptive Awareness Intervention
Teaching Your Child to Feel Hot and Cold
Temperature sensation difficulties involve impaired interoceptive and exteroceptive awareness of body temperature and environmental temperature. The internal signals that say "I'm getting too hot" — and the external signals from skin receptors that say "this surface is dangerously warm" — both fail to register reliably in children with this profile.
This intervention uses 9 evidence-selected materials to: (1) build external scaffolding that compensates for missing internal signals, (2) gradually develop whatever internal awareness is possible, and (3) establish non-negotiable safety systems during the awareness-building period.
🧠 Domain
Interoception
🌡️ Subdomain
Thermoregulation
👶 Ages
3–12 years
🏠 Setting
Home, School, Outdoors
⏱ Duration
5–15 min/session
📅 Frequency
2–3×/day
Formal Clinical Name: Interoceptive Awareness Deficit — Temperature Sensation / Thermoregulation (INT-TEMP | Domain A | Interoception Subdomain) | Reel ID: A-113 | Sensory Solutions Series, Episode 113 of 150
The Consortium That Built This Intervention
Temperature awareness sits at the intersection of neurology, behavior, education, and safety — which is why A-113 was built by four disciplines working together. Each brings a distinct lens; together they create a complete, safe, and effective protocol.
🤲 Occupational Therapy — PRIMARY LEAD
Sensory integration framework; interoception assessment; thermometer-based body awareness activities; adaptive environment setup; safe bath temperature training; sensory diet integration. "Temperature insensitivity is a direct interoceptive difference. OT's sensory integration approach addresses the neurological basis while building functional safety habits."
📊 Applied Behavior Analysis (ABA/BCBA) — SUPPORTING LEAD
Behavioral reinforcement of temperature-checking routines; schedule-based temperature awareness training; data collection for awareness progression; functional behavior analysis. "Scheduled temperature checks are behavior chains we build through reinforcement. The goal is autonomous checking behavior that requires no external prompt."
📖 Special Education (SpEd) — CONTRIBUTING
Visual clothing choice chart development; classroom temperature protocols; IEP goals for dressing independence; peer-supported temperature awareness activities. "Visual supports for temperature decision-making are life skills — they belong in the IEP alongside communication and social goals."
🧠 NeuroDevelopmental Pediatrics — MEDICAL OVERSIGHT
Differential diagnosis ruling out medical thermoregulatory dysfunction; safety monitoring thresholds; emergency protocols; medication interactions with thermoregulation. "Before implementing home programs, rule out peripheral neuropathy, autonomic dysfunction, and thyroid disorders. Most cases are interoceptive — but medical clearance protects every child."
"This technique crosses therapy boundaries because the brain doesn't organize by therapy type. Temperature awareness is simultaneously a sensory skill, a behavioral habit, an educational goal, and a medical safety matter."

Precision Targets — This Is Not a Random Activity
Every session has a primary target, secondary targets, and tertiary developmental gains. Understanding the full target picture keeps you focused on what matters most — and helps you recognize progress at every level.
🎯 Primary Target
Child independently checks environmental thermometer before outdoor activity — 4 out of 5 opportunities without prompting
🎯 Secondary Targets
Body signal recognition | Safe dressing independence | Bath & water safety check — using visual chart systems
🎯 Tertiary Gains
Interoceptive literacy | Reduced heat/cold risk | Family functioning | Social participation | Daily Living Independence Index
Source: Meta-analysis World J Clin Cases (2024): SI therapy promotes social skills (primary), adaptive behavior (secondary), sensory processing, motor skills (tertiary) | PMC10955541

The 9 Materials — Sourced, Priced, Ready to Use
Primary Materials — Clinically Validated by Pinnacle Consortium. Each material has been selected for its therapeutic mechanism, accessibility, and safety profile. You do not need all 9 to begin — start with 2–3 and expand over time.
🌡️ 1. Visual Temperature-Body Connection Scales
Category: Visual Schedules & Charts | Price: ₹200–600 | Amazon.in
Color-coded thermometer charts showing hot/comfortable/cold zones with corresponding body sensation illustrations. The bridge between external readings and internal feelings. ✅ DIY-Friendly
Color-coded thermometer charts showing hot/comfortable/cold zones with corresponding body sensation illustrations. The bridge between external readings and internal feelings. ✅ DIY-Friendly
⌚ 2. Wearable Temperature Monitors
Category: Monitoring & Tracking | Price: ₹2,000–8,000 | Amazon.in / Medical supply
Wristband or clip-on device providing real-time body temperature data. Alerts child and caregiver when temperature reaches concerning levels. Objective data when internal signals are unreliable. ⚠️ Safety Priority
Wristband or clip-on device providing real-time body temperature data. Alerts child and caregiver when temperature reaches concerning levels. Objective data when internal signals are unreliable. ⚠️ Safety Priority
👕 3. Visual Weather-Clothing Choice Charts
Category: Visual Schedules & Charts | Price: ₹150–500 | Amazon.in / Printable
Visual decision matrix matching temperature/weather to clothing. Below 15°C → jacket+hat; 15–25°C → light layers; above 30°C → shorts+sunhat. Removes guesswork; builds independence. ✅ DIY-Friendly
Visual decision matrix matching temperature/weather to clothing. Below 15°C → jacket+hat; 15–25°C → light layers; above 30°C → shorts+sunhat. Removes guesswork; builds independence. ✅ DIY-Friendly
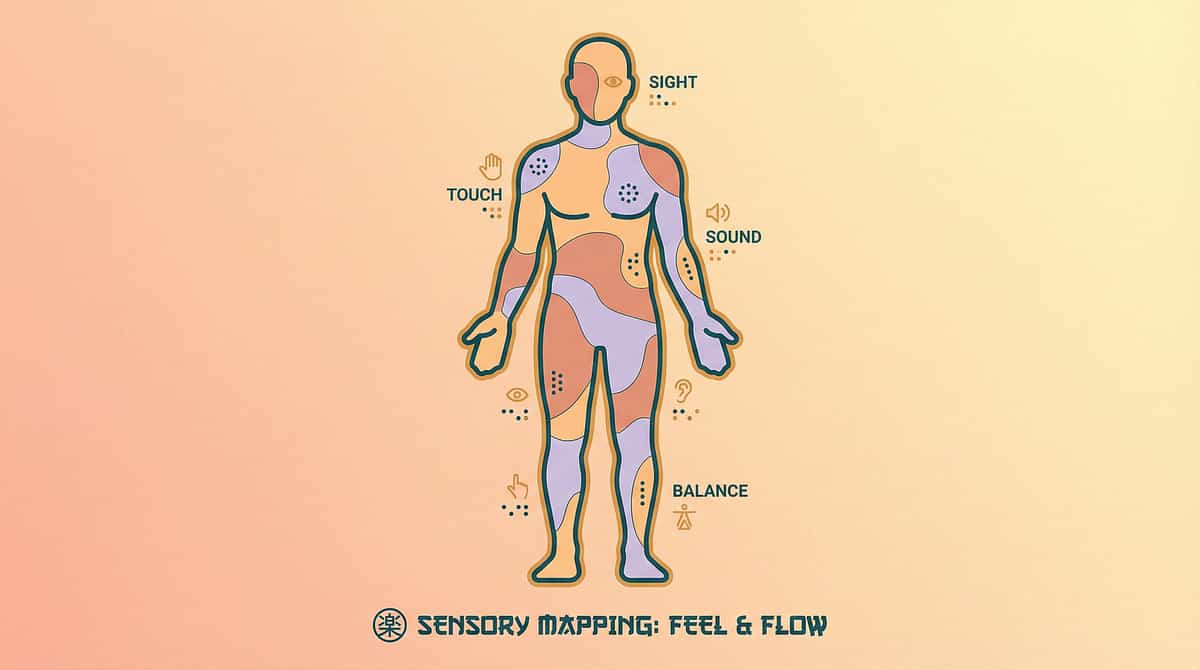
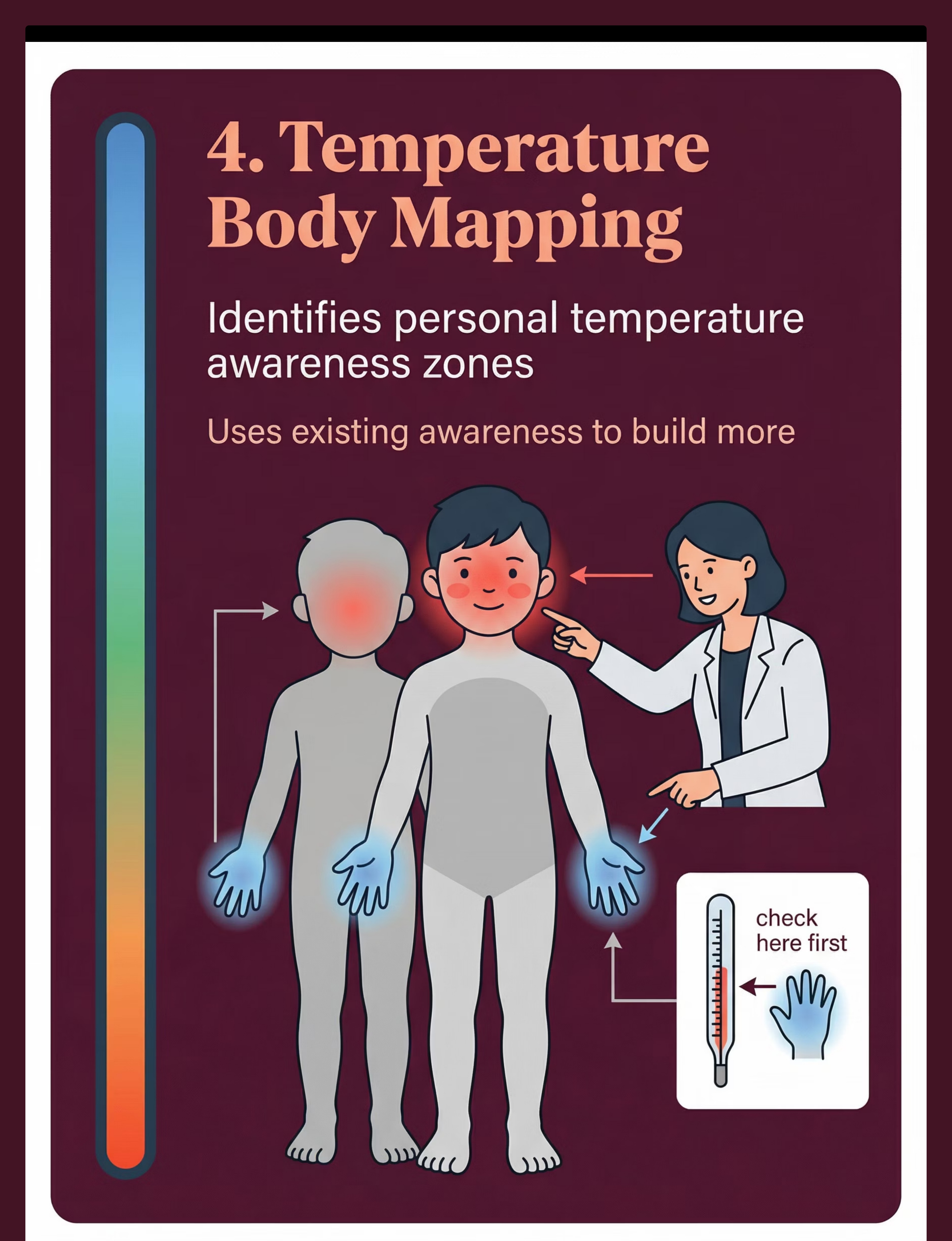
Materials 4–6: Body Mapping, Thermometers & Bath Safety

🗺️ 4. Body Mapping Templates (Temperature Zones)
Category: Body Awareness Tools | Price: ₹150–400 | Printable / Pinnacle downloads
Body outline templates for identifying where the child does perceive temperature. Some children feel cold only in hands — mapping these zones creates a personal temperature awareness strategy. ✅ DIY-Friendly
Body outline templates for identifying where the child does perceive temperature. Some children feel cold only in hands — mapping these zones creates a personal temperature awareness strategy. ✅ DIY-Friendly

📊 5. Environmental Visual Thermometers (Large Display)
Category: Environmental Visual Supports | Price: ₹500–2,000 | Amazon.in
Large-display thermometers with color zones (blue=cold, green=comfortable, red=hot) and action icons. Placed by front door, in bedroom, outdoors. Constant environmental reference replacing the missing internal signal. ✅ Basic DIY possible
Large-display thermometers with color zones (blue=cold, green=comfortable, red=hot) and action icons. Placed by front door, in bedroom, outdoors. Constant environmental reference replacing the missing internal signal. ✅ Basic DIY possible

🛁 6. Bath Temperature Safety Systems
Category: Safety Devices & Adaptive Equipment | Price: ₹300–1,500 | Hardware / Amazon.in
Color-changing bath spout cover + floating bath thermometer with smiley/sad face zones + anti-scald valve. Non-negotiable safety material for children with temperature insensitivity. Prevents burns while teaching temperature visually. 🚨 Safety Priority — Do Not Substitute
Color-changing bath spout cover + floating bath thermometer with smiley/sad face zones + anti-scald valve. Non-negotiable safety material for children with temperature insensitivity. Prevents burns while teaching temperature visually. 🚨 Safety Priority — Do Not Substitute

Materials 7–9: Social Stories, Check Cards & Adaptive Clothing

📖 7. Social Stories for Temperature Awareness
Category: Narrative Learning Materials | Price: ₹200–600 | Printable / Pinnacle downloads
Illustrated stories where characters learn to check thermometers, notice body signs, and make appropriate choices. Narrative framework for children who learn better through story than direct instruction. ✅ DIY-Friendly
Illustrated stories where characters learn to check thermometers, notice body signs, and make appropriate choices. Narrative framework for children who learn better through story than direct instruction. ✅ DIY-Friendly

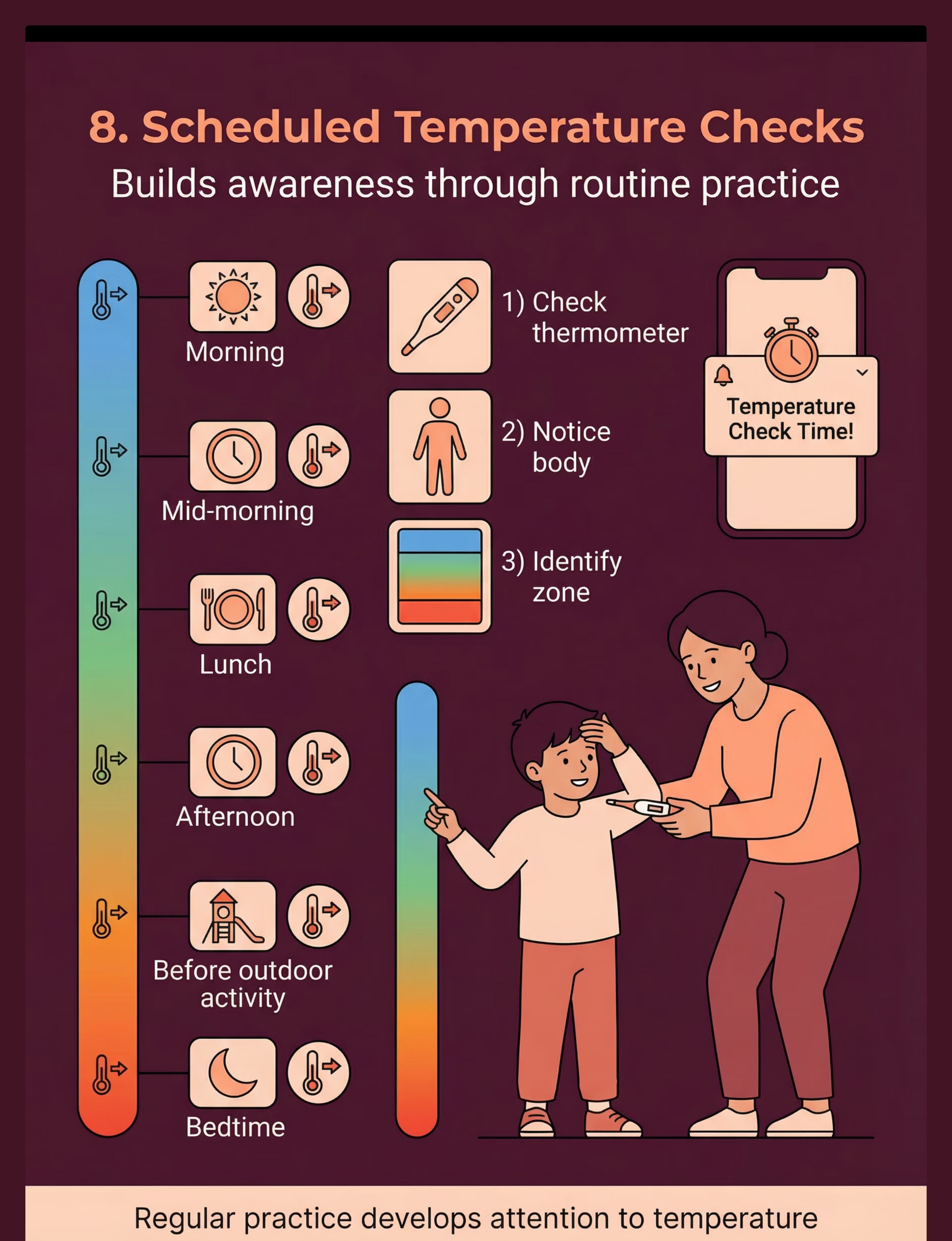
📋 8. Scheduled Temperature Body Check Cards
Category: Routine & Schedule Tools | Price: ₹100–300 | Printable / Pinnacle downloads
Visual schedule cards for 6 daily temperature check times (morning, mid-morning, lunch, afternoon, pre-outdoor, bedtime). Each check: thermometer → body scan → zone identification. Builds the habit of noticing. ✅ DIY-Friendly
Visual schedule cards for 6 daily temperature check times (morning, mid-morning, lunch, afternoon, pre-outdoor, bedtime). Each check: thermometer → body scan → zone identification. Builds the habit of noticing. ✅ DIY-Friendly

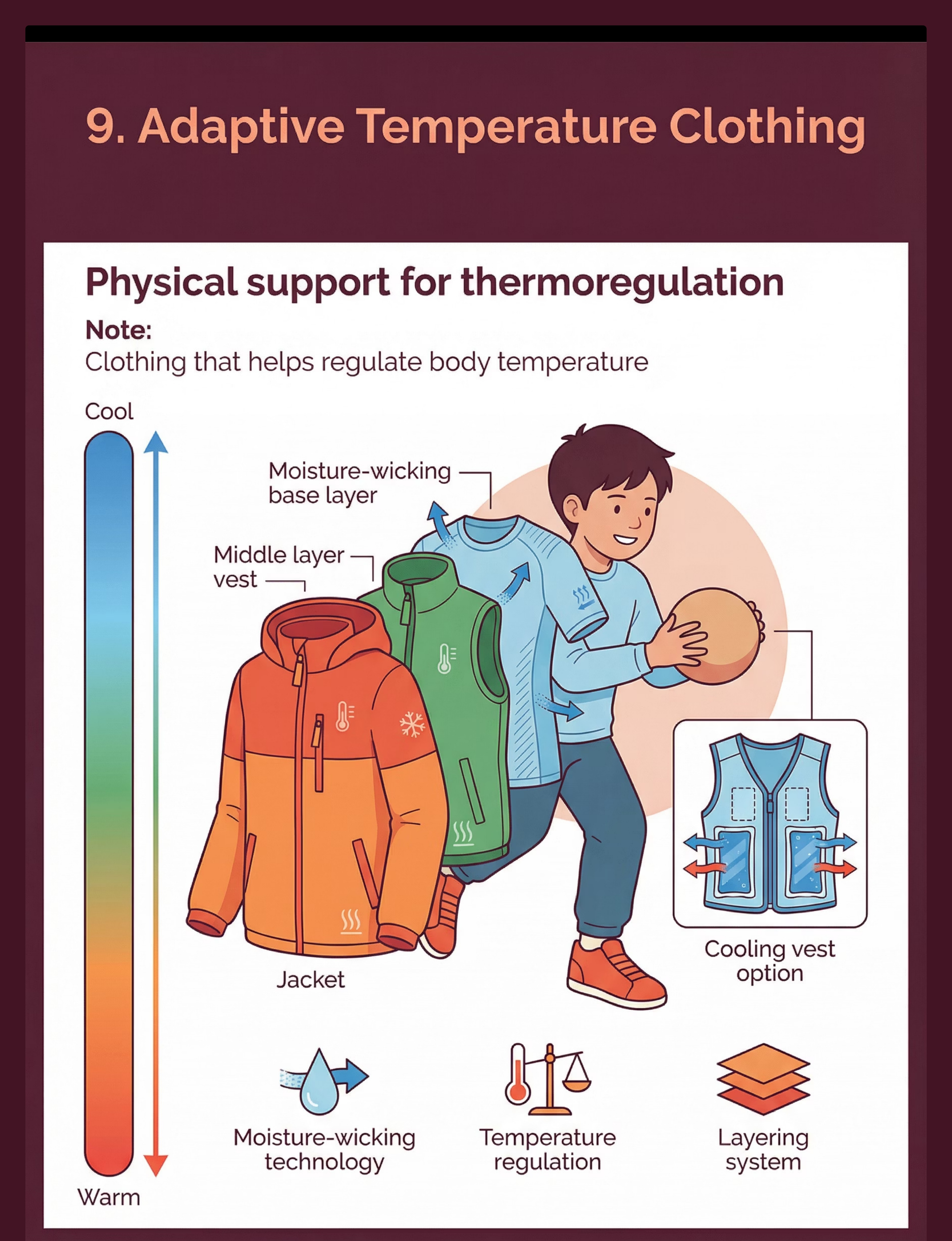
🧥 9. Adaptive Temperature-Regulating Clothing
Category: Adaptive Clothing & Sensory Apparel | Price: ₹1,000–5,000 | Sportswear / Amazon.in
Moisture-wicking base layers + easy on/off outer layers + cooling vest. Provides physical thermoregulation support when sensory awareness is limited. The body stays regulated even when the child can't perceive the need to regulate. ✅ Pinnacle Recommends
Moisture-wicking base layers + easy on/off outer layers + cooling vest. Provides physical thermoregulation support when sensory awareness is limited. The body stays regulated even when the child can't perceive the need to regulate. ✅ Pinnacle Recommends
Essential Starter Kit
Materials 1, 3, 6 | ₹650–2,600 | Begin immediately
Full Recommended Setup
All 9 materials | ₹4,500–18,000 | Complete protocol
📞 Need help choosing materials? FREE Consultation: 9100 181 181
Zero-Cost Versions — Every Family Can Start Today
WHO/UNICEF Equity Principle: Every child deserves evidence-based intervention regardless of family income. All 9 materials have household-item equivalents that apply the same therapeutic principles.
Buy: Visual Temperature-Body Connection Scales
Printed laminated chart ₹200–600
✅ Make This (₹0)
Draw a thermometer on A4 paper with 3 zones in blue/green/red. In each zone, draw stick figures: Cold zone = shivering body + goosebumps; Comfortable zone = relaxed arms; Hot zone = sweat drops + red cheeks. Laminate with tape.
Buy: Wearable Temperature Monitors
Commercial device ₹2,000–8,000
⚠️ Lower-Tech Alternative (₹50)
Regular digital forehead thermometer with scheduled parent checks every 20 min during outdoor activity. Set phone alarms. Commercial wearable preferred for children with history of heat exhaustion or seizures.
Buy: Visual Clothing Choice Charts
Commercial chart ₹150–500
✅ Make This (₹0)
Cut clothing pictures from old magazines or draw them. Create 3 zones: ❄️ Cold (below 20°C) → jacket + layers; ☁️ Mild (20–28°C) → light shirt; ☀️ Hot (above 28°C) → shorts + sunhat. Post near door.
Buy: Body Mapping Templates
Printed templates ₹150–400
✅ Make This (₹0)
Lie on large paper, trace child's body outline. Together, color in zones where they sometimes feel temperature. Use blue for cold-sensitive areas, red for heat-sensitive areas. Review and update monthly. The mapping process IS the therapy.
Buy: Environmental Thermometers
Large display ₹500–2,000
✅ Make This (₹150)
Any digital thermometer near the door. Attach colored tape: 0–18°C = blue strip; 18–28°C = green strip; 28°C+ = red strip. Add picture icons (jacket/t-shirt/shorts) next to each zone.
Buy: Bath Temperature Safety
Anti-scald system ₹300–1,500
⚠️ Non-Negotiable Minimum (₹150)
Floating bath duck/toy thermometer with happy/sad face zones. SAFETY: Never rely on child's sensation alone for bath safety. Adult always tests with elbow before child enters, regardless of device. Anti-scald valve installation (~₹500) STRONGLY recommended.
Buy: Social Stories, Check Cards & Adaptive Clothing
✅ All DIY-Friendly (₹0)
Social stories: Write a 6-panel story about checking the thermometer. Check cards: Write on index cards with 3 steps per check. Clothing: Use existing moisture-wicking clothes + teach the 3-layer system (always-on base + removable layer + carry-in-bag layer).
"A hand-drawn thermometer chart on the back of a cereal box. A floating thermometer toy from the market. A body outline drawn in crayon. These are the materials that changed safety outcomes for hundreds of families in our network." — OT Lead, Pinnacle Blooms Center, Hyderabad

🚨 Safety First: Read This Before Your First Session
🔴 RED — Do Not Proceed Without Medical Clearance
- Child has a history of heat stroke or hypothermia
- Child has experienced burns from hot water or surfaces in the past 6 months
- Child has a known medical condition affecting thermoregulation (autonomic dysfunction, peripheral neuropathy, thyroid disorder)
- Sudden change in temperature perception (may indicate new medical issue)
- Child has seizure disorder and engages in vigorous outdoor activity
→ Action: Contact NeuroDev Pediatrician FIRST | 9100 181 181 for fast referral
🟡 AMBER — Proceed With Additional Adult Supervision
- Child tends to put objects in hot water without reaction
- Child has had one instance of mild overheating without noticing
- Child is immunocompromised (temperature extremes more dangerous)
- Child is non-verbal with no AAC (harder to detect distress)
→ Action: Two-adult minimum for outdoor activities in extreme weather. Anti-scald device MANDATORY for bath.
🟢 GREEN — Standard Precautions
- Child has typical medical history with sensory processing differences only
- Child is 3–12 years with caregiver present during all activities
- Outdoor activities in moderate weather (18–32°C) with shade available
→ Action: Follow protocol as described. Adult supervises all temperature activities throughout.
🛑 STOP IMMEDIATELY IF:
- Child appears pale/flushed and unresponsive to name-calling during outdoor activity (heat distress)
- Child is shivering uncontrollably (hypothermia risk)
- Child places hands/feet in very hot water without reaction (immediate burn risk)
- Child collapses or appears faint after outdoor exertion
Emergency: 108 (Ambulance) | After stabilization: 9100 181 181 | These materials are therapeutic education tools, not medical devices. Adult supervision is essential throughout. They supplement, not replace, professional occupational therapy and medical monitoring.

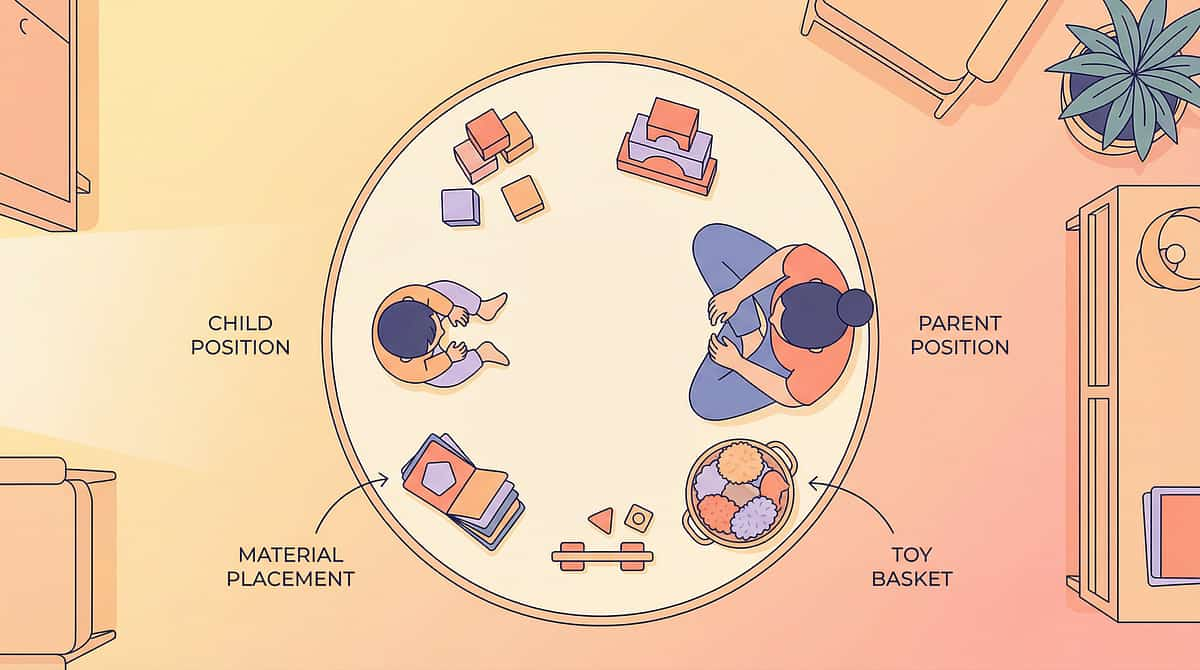
Your Home Therapy Space — Set Up in 4 Minutes
A well-organized space reduces resistance, supports attention, and ensures safety. You don't need a dedicated therapy room — any calm, familiar area works when it's thoughtfully prepared.
Numbered Setup Guide
- Choose 2–3 materials to start (recommended: Temperature Chart + Clothing Chart + Bath Safety)
- Place environmental thermometer at child's eye level by the most-used door
- Post clothing chart inside wardrobe at child's height (or on bedroom door)
- Install bath thermometer device before bath time
- Print/prepare body mapping template and have markers ready
- Set 3 phone alarms for scheduled temperature checks (morning, pre-outdoor, afternoon)
- Identify the coolest and warmest spots in your home for body mapping sessions
Total setup time: 4–8 minutes for first session | Daily setup after initial install: 60–90 seconds
Lighting & Sensory Setup
- Natural light preferred for temperature chart reading sessions
- Moderate room temperature (22–26°C) during indoor sessions
- Low noise environment for first body mapping session (concentration required)
- Child should be fed, rested, and in a calm regulated state
Parent Positioning
- Thermometer reading: Side-by-side with child (not behind/over)
- Clothing choice: Let child point first; parent validates
- Bath safety: Parent tests water ALWAYS with elbow first; child checks device second

60-Second Readiness Assessment — Before Every Session
The best session is one that starts right. This quick pre-flight check ensures your child is in the optimal state to learn — and tells you exactly how to adjust when they're not.
Fed & Nourished
Child has eaten a meal within the past 2 hours (not hungry)
Well-Rested
Child has had adequate sleep (not overtired)
Healthy Today
No fever or illness symptoms; no meltdown in the past 60 minutes
Safe Conditions
Weather safe for planned session type (outdoor: 18–32°C, shade available)
Materials Ready
All required materials assembled and accessible before you begin
Caregiver Ready
You are calm, unhurried, and available for minimum 10 minutes
✅ All 6–7 Pass → GO
Proceed to Step 1: The Invitation
⚠️ 5–6 Pass → MODIFY
Use 1 material only. No new skill introduction today. "Just check the thermometer together. 90 seconds. Done."
🛑 4 or Fewer → POSTPONE
Skip session. Choose a calming co-regulation activity instead. Mark on tracking sheet. Resume when ready.
"The best session is one that starts right. A postponed session is better than a dysregulated one."

Step 1 of 6: The Invitation
① of 6 Steps
Time: 30–60 seconds
OT + ABA
Every session begins with an invitation — never a command. The child is brought into the temperature awareness activity through connection, curiosity, or a preferred starting point. This is the pairing phase — and it matters more than any other step.
"Hey [child's name], I need your help with something. Can you be my thermometer helper today?"
For non-verbal/AAC users: [Show the thermometer + point to chart] + wait 5 seconds for approach or gesture
Play-based entry: "The thermometer is asking a question. Can you find out what it says?"
Body Language Guidance
- Crouch to child's eye level
- Relaxed, curious expression — not hurried
- Hold the thermometer or chart loosely, not thrusting it toward child
- Allow child to approach rather than pulling them toward the material
✅ Acceptance Cues (What to Look For)
- Child approaches the material
- Child makes eye contact with the material
- Child gestures toward the thermometer or chart
- Child echoes or approximates any word from your script
Resistance Cues & Response
If child moves away → reduce demand: "Just look at the colors?" (no action required)
If child covers eyes/ears → session is MODIFY mode: single 10-second exposure only
If child vocalizes distress → switch to POSTPONE (return to Readiness Check)
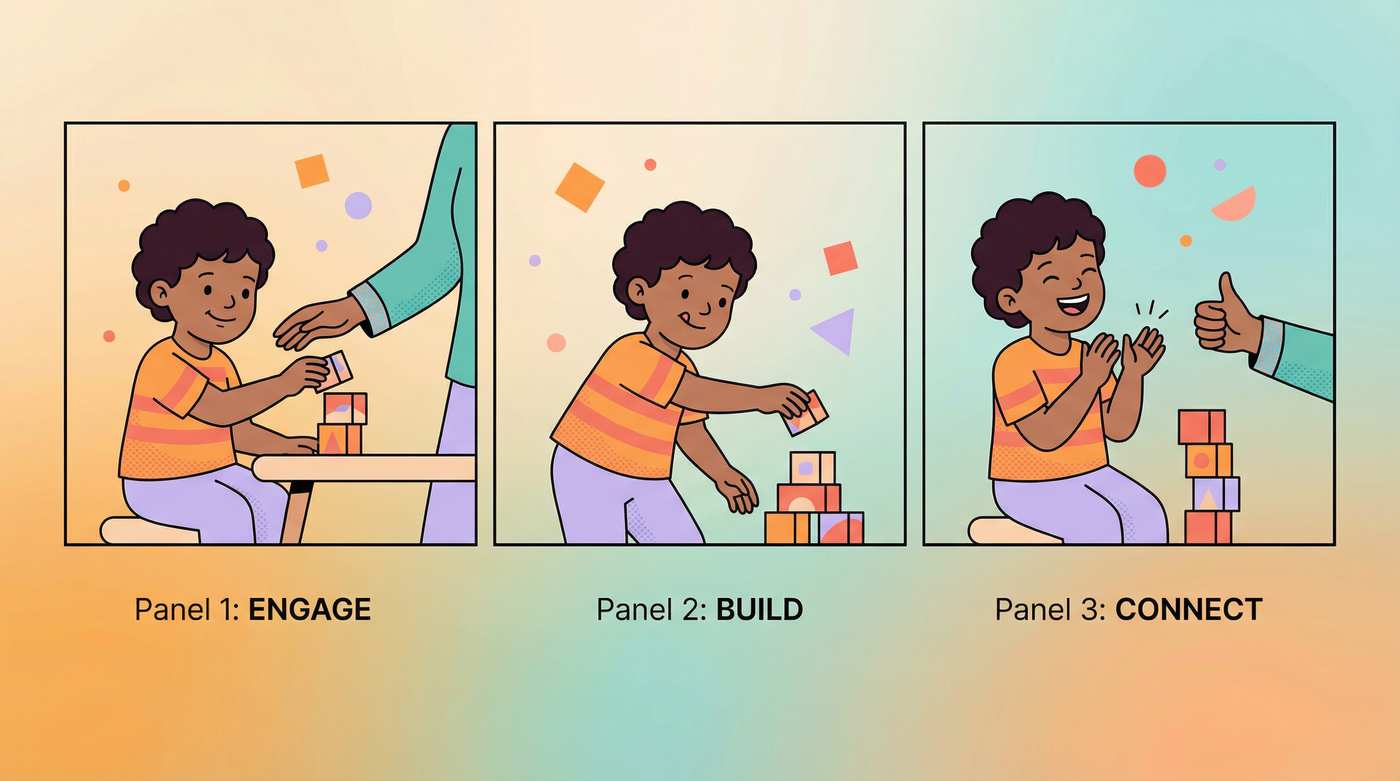
Step 2 of 6: The Engagement
② of 6 Steps
Time: 1–3 minutes
OT + ABA
Once the child has accepted the invitation, introduce the primary material for today's session. The engagement phase pairs the child with the material in a low-demand, curiosity-forward way before any responses are expected.
🌡️ Temperature Chart Session
"Look — when the thermometer shows THIS color (point to red zone), it means the air is hot. Let's find out what hot feels like in our body. When you're hot, your skin might feel like THIS (mime sweating/flushed). Can you point to the hot zone?"
👕 Clothing Choice Chart Session
"We're going outside today. The chart shows [point to thermometer reading]. What does our chart say to wear? Can you find the right picture?"
🛁 Bath Safety Session
"Before you step in, we always check the color. What color do you see? [wait] Green means safe. Red means too hot — we wait."
🗺️ Body Mapping Session
"I'm going to lightly touch different parts. You tell me — does it feel warm, cold, or can't tell? There's no wrong answer."
✅ Engagement
Child points, responds, mirrors action, or approaches material
🟡 Tolerance
Child stays near material but doesn't actively respond — acceptable for sessions 1–5
🛑 Avoidance
Child moves away or shows distress — drop to MODIFY mode immediately
Any engagement or tolerance = immediate warm verbal praise: "That's it! You found the hot zone!" / "Yes! You checked the color — great job!"

Step 3 of 6: The Therapeutic Action
③ of 6 Steps
Time: 3–8 minutes
OT Primary | ABA Reinforcement
This is the core of the session. The therapeutic action pairs an external tool (the thermometer, chart, or bath device) with an internal body awareness scan — building the bridge that the Insula cannot build automatically.
Session Type A — Temperature-Body Connection
Child checks thermometer → names/points to zone → parent guides body scan: "Touch your face. Does it feel warm? Cool?" → child identifies one body sensation → matches to thermometer zone → parent confirms and expands. Repeat 2–3 times.
Therapeutic ingredient: Pairing external data with internal sensation scan — building the bridge the Insula cannot build automatically.
Therapeutic ingredient: Pairing external data with internal sensation scan — building the bridge the Insula cannot build automatically.
Session Type B — Clothing Decision
Child consults clothing chart → parent shows today's thermometer reading → child selects clothing items from the chart picture → child physically retrieves selected items → parent validates choice.
Therapeutic ingredient: Replacing the missing temperature-to-decision pathway with visual decision support; building the habit of consulting before acting.
Therapeutic ingredient: Replacing the missing temperature-to-decision pathway with visual decision support; building the habit of consulting before acting.
Session Type C — Bath Safety Routine
Parent fills bath to safe temperature → child checks bath thermometer/color device → child names zone (green = safe) → child enters bath → parent briefly notes: "It's warm! Can you feel warm on your arm?" → child responds however they can.
Therapeutic ingredient: Non-negotiable safety habit + low-demand interoceptive awareness moment.
Therapeutic ingredient: Non-negotiable safety habit + low-demand interoceptive awareness moment.
⚠️ Common Execution Errors
❌ Rushing → ✓ Fix: Pause 5 seconds after each question. Wait for child's response before confirming.
❌ Testing during distress → ✓ Fix: Body awareness questions only during calm, tolerated states — never as demands during distress.
❌ Skipping the body scan → ✓ Fix: Always add one body scan question per session, even if child doesn't respond.

Step 4 of 6: Repeat & Vary
④ of 6 Steps
Time: 2–4 additional minutes
OT + ABA
Repetition builds neural pathways. Variation maintains engagement without compromising the therapeutic principle. 3 good, engaged repetitions are worth more than 10 forced ones. When quality drops, stop.
Repetition Targets
- Temperature chart check: 2–3 repetitions per session
- Clothing choice: 1 complete selection per session (daily routine = the dosage)
- Bath safety: 1 consistent routine per bath
- Body mapping: 3–5 touch points per session
Satiation Indicators — Time to Stop
- Child becomes physically restless (moving away from the material repeatedly)
- Verbal or behavioral protest escalates across repetitions
- Quality of responses declining (less precise, more automatic/non-engaged)
- Child has successfully completed the target action and seems ready to move on
4 Variation Options
1
Change the Thermometer
Wall thermometer today; weather app tomorrow; wearable device reading next. Same skill, different input source.
2
Change the Actor
Parent checks first and narrates; child checks second. Next session: child checks first; parent confirms. Builds independence.
3
Change the Setting
Kitchen → outdoor → classroom thermometer. Same skill applied in all temperature-relevant environments.
4
Change the Language
"What does the thermometer say?" vs "Is it jacket weather?" vs "Hot zone or cold zone?" Language variety builds flexible understanding.

Step 5 of 6: Reinforce & Celebrate
⑤ of 6 Steps
Time: 30–90 seconds
ABA Primary
The Timing Rule: Reinforcement must be delivered within 3 seconds of the desired behavior — not at the end of the session, but AT the moment the child demonstrates any target behavior.
Zone Identification
"YES! You found the hot zone! That's exactly right!"
Clothing Selection
"You checked the chart and you got it — perfect. [Child name] is a temperature expert!"
Bath Safety Check
"You checked the color first — that's exactly how we do it. Green means safe. Great job."
Body Sensation Report
"You FELT that? That is incredible. That's your body talking — and you heard it!"
Reinforcement Menu Options
✓ Verbal Praise
Specific, enthusiastic, immediate — always the first layer
✓ Physical Celebration
High-five / fist bump — child-preferred contact
✓ Sticker Chart
1 sticker per session completed
✓ Token Economy
3 tokens = 5 minutes of preferred activity
✓ Natural Reinforcer
"Because you checked — we can go outside now!"
✓ Social Reinforcer
"Wait until we tell Papa/Dadi what you did today!"
Celebrate the Attempt, Not Just the Success. If child looks at the thermometer but doesn't identify the zone → still reinforce the looking behavior. The neural pathway for "check the thermometer" is built through reinforced repetition — every step counts.

Step 6 of 6: The Cool-Down
⑥ of 6 Steps
Time: 1–2 minutes
OT
No session ends abruptly. A structured transition prevents the next session's starting resistance and sends a clear signal that temperature checking time has a reliable, calm ending.
~90 Seconds Before End
"Two more, then we're all done with thermometer time."
~30 Seconds Before End
"One more — then we put the chart away."
Final Signal
"All done with temperature checking! Great work today."
Transition Cue
"Now it's [preferred activity / snack / school routine]." Use visual schedule if child has one.
Cool-Down Activity (Choose One)
Put-Away Ritual
Child returns thermometer to its place, turns chart over (physical closure)
Heavy Work Input
5 chair push-ups, wall push-ups, or carry the "heavy book" to the shelf
Sensory Calming
30 seconds of deep pressure on shoulders (parent-administered, child-accepted)
Preferred Sensory Input
Child's own preferred regulating input (rocking, squeezing fidget, etc.)
If Child Resists Ending: Do not force put-away. "Okay — 30 more seconds to hold it, then we put it away." This is regulation, not indulgence. A regulated transition prevents the next session's starting resistance.

60 Seconds of Data Now Saves Hours of Guessing Later
Capture within 60 seconds of session end, while memory is fresh. You do NOT need a clinical data system. Start with this simple 3-field record — it's all you need to track meaningful progress.
Date & Session Type
[Date] | [Session Type: Temperature Chart / Clothing / Bath Safety / Body Mapping]
Child Engagement Level
4 = Initiated checking behavior independently (!)
3 = Engaged with material with minimal prompting
2 = Tolerated material; needed significant prompting
1 = Refused / Significant distress / Session modified/postponed
3 = Engaged with material with minimal prompting
2 = Tolerated material; needed significant prompting
1 = Refused / Significant distress / Session modified/postponed
Key Observation (One Sentence)
"Identified hot zone correctly 2/3 times. Touched chart independently on 3rd attempt."
"Selected weather-appropriate clothes from chart — first time without argument!"
"Checked bath thermometer before entering — didn't need to be reminded!"
"Selected weather-appropriate clothes from chart — first time without argument!"
"Checked bath thermometer before entering — didn't need to be reminded!"
Trend in Engagement
Is the routine forming? Are scores moving from 1–2 toward 3–4?
Best-Performing Material
Which of the 9 materials generates the most engagement?
Session Frequency
Are sessions happening consistently (3×/week target)?
Progress Markers
Is independent checking behavior emerging?
"Families who track 3 sessions per week are 4× more likely to observe measurable progress at 8 weeks. Data isn't bureaucracy — it's your child's story being written." — GPT-OS® Clinical Intelligence

The Reality Card — Most Sessions Don't Go Perfectly
Session abandonment is not failure — it's data. The child's response IS the information we need. Here are the 7 most common challenges with A-113 and exactly what to do next time.
Problem 1: Child refuses to look at the thermometer at all
Why: The material may be novel and unpredictable. Child hasn't yet learned that it's safe/interesting.
Fix: Pair the thermometer with a preferred activity for 3–5 sessions first (no demands — just present). Let child handle it freely. Demands come after pairing is established.
Fix: Pair the thermometer with a preferred activity for 3–5 sessions first (no demands — just present). Let child handle it freely. Demands come after pairing is established.
Problem 2: Child always picks the wrong clothing / doesn't care about the "right" answer
Why: The chart-to-decision connection hasn't generalized yet. Child may be echoing, not reasoning.
Fix: Practice in real daily clothing moments — not as a worksheet exercise. Real clothing, real weather, real consequence ("You'll be cold without the jacket — try it and tell me what you notice").
Fix: Practice in real daily clothing moments — not as a worksheet exercise. Real clothing, real weather, real consequence ("You'll be cold without the jacket — try it and tell me what you notice").
Problem 3: Child NEVER reports any body sensation
Why: This is core to the condition — the child genuinely may not feel it. Don't push for internal reports they can't access yet.
Fix: Focus entirely on external checking (thermometer → zone identification) for now. Body awareness comes with time and scaffolding.
Fix: Focus entirely on external checking (thermometer → zone identification) for now. Body awareness comes with time and scaffolding.
Problem 4: The clothing battle continues even with the chart
Why: Chart consultation hasn't become the established first step in the dressing routine yet.
Fix: Make the chart check the non-negotiable first step — before ANY clothing discussion. Child checks chart → chart makes the decision → parent validates → clothing selected. Remove the debate; defer to the chart.
Fix: Make the chart check the non-negotiable first step — before ANY clothing discussion. Child checks chart → chart makes the decision → parent validates → clothing selected. Remove the debate; defer to the chart.
Problem 5: Child was doing well, then regressed
Why: Regression is normal. Routine disruption (travel, illness, school changes) breaks fragile new habits.
Fix: Treat regression like week 1 re-learning. Return to shorter sessions (30-second checks only). Increase reinforcement temporarily. Expect re-establishment within 5–7 sessions.
Fix: Treat regression like week 1 re-learning. Return to shorter sessions (30-second checks only). Increase reinforcement temporarily. Expect re-establishment within 5–7 sessions.
Problem 6: Child is now terrified of baths (too focused on the danger)
Why: Safety messaging can occasionally activate anxiety, particularly in anxious sensory profiles.
Fix: Shift language from danger-avoidance ("don't get burned") to routine-celebration ("you checked — you're ready!"). Remove any fear vocabulary. Make the green zone the focus.
Fix: Shift language from danger-avoidance ("don't get burned") to routine-celebration ("you checked — you're ready!"). Remove any fear vocabulary. Make the green zone the focus.
Problem 7: My child got dangerously overheated despite using the schedule. I feel like I failed.
Why: You didn't fail. The awareness-building period requires parallel safety systems. One event means the safety systems need strengthening, not that the intervention is failing.
Fix: Shorten outdoor activity intervals; increase wearable monitoring; notify pediatrician if significant overheating occurred. Call 9100 181 181 for immediate guidance.
Fix: Shorten outdoor activity intervals; increase wearable monitoring; notify pediatrician if significant overheating occurred. Call 9100 181 181 for immediate guidance.

No Two Children Are Identical — Personalize This Technique
A-113 is a framework, not a rigid script. Every child's sensory profile, age, language level, and personality calls for a tailored version. Use this card to find the right starting point for your child.
◀ EASIER Modifications (Difficulty 1–2)
- Use only 2 zones on the thermometer chart (HOT and NOT HOT) — add third zone after mastery
- Clothing choice chart limited to 2 options only (jacket vs no jacket) per session
- Bath check: only color identification required — no naming, no action by child
- Body mapping: only face and hands (highest sensory density areas)
- Session duration: 3–5 minutes maximum
- Adult takes all initiative; child only observes
Standard Protocol (Difficulty 3)
As described in Steps 1–6. All 9 materials over 8 weeks.
▶ Advanced Modifications (Difficulty 4–5)
- Child initiates temperature check without prompting (no parental cue)
- Child selects complete outfit independently using chart in under 2 minutes
- Child requests water break or shade independently during outdoor activity
- Body mapping expanded to full body; child identifies 3+ awareness zones
- Child teaches a sibling or grandparent how to use the temperature chart
Age-Based Modifications
Ages 3–5: 2-zone chart only; picture-heavy, minimal text. Bath safety as a game: "Color detective" before every bath. Body mapping: only hands and face; warm/cool water contrast as teaching moment.
Ages 6–9 (Primary Intervention Window): Full 3-zone chart; add temperature numbers. Clothing independence goal: selected independently 4/5 mornings per week. Full body mapping; begin scheduled check habit.
Ages 10–12: Weather app thermometer replaces wall chart. Child sets own phone reminders for outdoor checks. Brief peer-awareness discussion about why they have this different sensory system.
Child Personality Variations
Highly routine-oriented: Embed all checks into existing routines. Never introduce as "new."
Highly social: Temperature check as a parent-child game; "beat the thermometer" prediction game.
Language-limited / AAC user: Ensure all charts have picture symbols compatible with their AAC system. Temperature zone = matching symbol on their device.

Week 1–2: What to Expect
Phase: Introduction & Tolerance
15% Progress
3 sessions/week
Week 1–2 of 8
Introduction & Tolerance phase — the foundation is being laid before it is visible
"In Weeks 1–2, Look for Tolerance — Not Transformation"
✓ What Progress Looks Like at This Stage
- Child tolerates thermometer being present in their space (even without engaging with it)
- Child looks at the temperature chart without being asked — even once
- Child does not protest the bath safety check routine
- Parent completes 3+ sessions per week without major disruption
✗ What Is NOT Progress Yet (and That's Perfectly Fine)
- Child spontaneously checking thermometer — too early
- Child reporting body sensations — too early
- Clothing battles eliminated — too early
- Independent dressing decisions — too early
“If your child tolerates the material for 3 seconds longer than last week — that is real neurological progress. You are watching a pathway being constructed. The Insula is receiving new types of paired information. The connections are being laid before they are visible. Stay consistent.”
📞 Struggling in week 1? Call 9100 181 181 — our therapists guide parents through the first 2 weeks.
Source: Systematic review (Children, 2024): SI outcomes emerge across 8–12 week timelines; early phase focuses on tolerance and participation | PMC11506176

Week 3–4: Consolidation Signs
Phase: Consolidation
40% Progress
3–4 sessions/week
Week 3–4 of 8
Consolidation phase — parents start to see it. New behaviors emerge.
"Week 3 Is When Parents Start to See It"
✓ Anticipates Chart Check
Child anticipates the temperature chart check before going outside — precedes parental prompt
✓ Independent Bath Check
Child checks bath thermometer color independently at least once without reminder
✓ Reduced Clothing Battles
Chart consultation reduces negotiation time by more than 50%
✓ Temperature Vocabulary
Child uses "hot," "cold," "jacket weather" at least occasionally
✓ Outdoor Response
During outdoor activity, child seeks water/shade when asked "how do you feel?" (even if answer is "don't know")
Neural Pathway Formation — Watch for These Subtle Signals:
- Child picks up the thermometer spontaneously (curiosity — not prompted)
- Child says "check chart" during dressing (unprompted language about the process)
- Child accepts temperature-related clothing suggestion without protest (trust transfer)
- Child checks temperature at a relative's house unprompted (generalization seed)
"By week 3–4, you may notice YOU are more confident too. You know how to respond to resistance. You know how to modify. You're no longer doing something new — you're doing something that belongs to your family's routine."

Week 5–8: Mastery Indicators
Phase: Mastery & Generalization
75% Progress
4+ sessions/week
Week 5–8 of 8
Mastery & Generalization — the goal is independence across multiple settings
"Mastery Looks Different for Every Child — Here's the A-113 Standard"
Primary Target Mastery (Observable, Measurable)
- Child independently checks environmental thermometer before outdoor activity (4/5 opportunities, no prompt)
- Child selects weather-appropriate clothing using visual chart without parental suggestion in 4/5 mornings
Secondary Target Mastery
- Child checks bath thermometer before entering bath independently (daily, across 7 consecutive days)
- Child reports at least one body sensation related to temperature per session at least 1×/week
🏆 Generalization Badge Unlock
- Generalizes to school thermometer check (teacher reports)
- Uses clothing chart at grandparents'/relatives' home
- Spontaneously requests water or shade during outdoor activity
- Responds to "are you hot?" with accurate body report ≥50% of the time
When to Move to Next Level
Mastery achieved across all settings → proceed to:
• A-114: Pain Insensitivity — 9 Materials
• A-115: Interoception Development — Full System
• A-140: Dressing Independence — Step by Step
• A-114: Pain Insensitivity — 9 Materials
• A-115: Interoception Development — Full System
• A-140: Dressing Independence — Step by Step
Source: Meta-analysis (2024): SI across 24 studies shows effective skill promotion with measurable outcomes | PMC10955541 | BACB Mastery Criteria Standards
You Did This. Your Child Grew Because of Your Commitment.
Weeks ago, you were guessing what to dress your child in every morning. Managing clothing battles that felt endless. Worrying every summer about overheating — every winter about hypothermia. And wondering if they'd ever notice.
Today, your child checks the chart. They verify the bath water. They trust the thermometer where their nervous system once gave them nothing. This is not a small achievement. This is neural pathway construction. This is safety. This is the beginning of independence.
"From fear to mastery. One technique at a time." — The Pinnacle Blooms Consortium
Family Celebration Suggestion
Plan an outdoor activity this week — and notice: your child is dressed appropriately. They checked the chart. You trusted them. The technique worked. Let that moment be the celebration.
📸Photo/Journal Prompt: Take a photo of your child's first independent thermometer check. This is your milestone. Document it. Optionally, share your milestone in the Pinnacle Parent Community.

⚠️ 5 Signs to Pause and Seek Professional Support
Clinical Guardrail
Read Even After Mastery
🔴 Red Flag 1: Heat-Related Illness in Past 30 Days
Child experienced heat-related illness (flushing, rapid heartbeat, confusion, loss of responsiveness) during outdoor activity.
Do this: Immediate pediatrician consultation. Do not resume outdoor high-exertion activity without medical clearance and enhanced monitoring.
Do this: Immediate pediatrician consultation. Do not resume outdoor high-exertion activity without medical clearance and enhanced monitoring.
🔴 Red Flag 2: No Withdrawal Response to Hot Surfaces
Child touched or entered dangerously hot liquid/surface and showed NO withdrawal response.
Do this: Immediate OT assessment + home safety audit. Call 9100 181 181 for emergency therapist consultation.
Do this: Immediate OT assessment + home safety audit. Call 9100 181 181 for emergency therapist consultation.
🟡 Red Flag 3: Sudden Complete Reversal of Progress
Progress that was achieved has suddenly reversed — child who was checking thermometer no longer responds to temperature cues at all (not just occasional regression).
Do this: Pediatric medical evaluation before resuming intervention.
Do this: Pediatric medical evaluation before resuming intervention.
🟡 Red Flag 4: Sudden Extreme Temperature Sensations
Child reports sudden extreme temperature sensations where previously there were none (sudden hypersensitivity).
Do this: NeuroDevelopmental Pediatrician consultation. Document onset and circumstances.
Do this: NeuroDevelopmental Pediatrician consultation. Document onset and circumstances.
🟡 Red Flag 5: Caregiver Burnout
Parent feeling overwhelmed, implementing safety systems inconsistently, or experiencing caregiver burnout around this intervention. Caregiver wellbeing IS the intervention. A depleted caregiver cannot implement safely.
Do this: Call 9100 181 181 for parent support session.
Do this: Call 9100 181 181 for parent support session.

Your Developmental GPS — Where You Are, Where You're Going
A-113 does not exist in isolation. It sits at a precise point in a mapped developmental progression — with clear paths forward depending on your child's response.
Branch A: Broader Interoception
A-115: Hunger, thirst, pain, emotion — the complete interoceptive literacy program
Branch B: Clothing Independence
A-140: From chart-supported to fully independent dressing
Branch C: School Generalization
Bring the temperature check habit to classroom and playground
Branch D: Cross-Sensory Approach
A-135: Addresses sensory processing holistically including temperature via movement integration
Domain Position: Domain A (Sensory) → Subdomain: Interoception → Position 113 of 150 in this cluster → Full progression: 12 domains, 70,000+ techniques mapped. Long-term goal: Child dresses appropriately for weather, regulates temperature during activity, and applies bath safety protocol without adult prompting — Daily Living Independence fully established in this domain.

You're Not Done — Here's What This Opens Up
Completing A-113 gives you a head start on related techniques. Three of the nine materials you already own overlap directly with the techniques below.
A-111 | Core
9 Materials That Help When Child Can't Feel Hunger
Domain: Interoception — Hunger Signals
✓ Body mapping templates: you already own this
Domain: Interoception — Hunger Signals
✓ Body mapping templates: you already own this
A-112 | Core
9 Materials That Help When Child Can't Feel the Need to Use the Bathroom
Domain: Interoception — Elimination Signals
✓ Scheduled check cards: you already own this
Domain: Interoception — Elimination Signals
✓ Scheduled check cards: you already own this
A-115 | Advanced
9 Materials That Help Build Interoceptive Awareness
Domain: Interoception — Full System
✓ Body mapping + visual scales: you already own these
Domain: Interoception — Full System
✓ Body mapping + visual scales: you already own these
A-135 | Core
9 Materials That Help With Sensory Processing Differences
Domain: Sensory Processing — Cross-Sensory
Domain: Sensory Processing — Cross-Sensory
A-140 | Core
9 Materials That Help With Dressing Independence
Domain: Daily Living — Self-Care
✓ Clothing choice charts: you already own this
Domain: Daily Living — Self-Care
✓ Clothing choice charts: you already own this
A-114 | Advanced
9 Materials That Help With Pain Insensitivity
Domain: Interoception — Pain Signals
Next in series — often co-occurs with temperature insensitivity
Domain: Interoception — Pain Signals
Next in series — often co-occurs with temperature insensitivity
Domain Position: You own 3 of the 9 materials for A-111, A-112, and A-140 already. Start one of these tomorrow.

One Technique. Twelve Domains. One Child. One Plan.
A-113 is your active technique in Domain A — Sensory Processing. This domain feeds directly into Daily Living Skills, Emotional Regulation, and Gross Motor outdoor activity. Understanding the full developmental picture ensures every intervention reinforces the others.
Daily Living & Independence Index
Primary tracking index for A-113 progress in GPT-OS®
Caregiver Dependence Reduction Index
Measures shift from prompted to independent temperature checking
Behavioral Self-Regulation Index
Secondary index — clothing decisions, activity pausing, hydration seeking
"This technique is one piece of a larger plan. Your child is not a single challenge — they are a whole developing person. GPT-OS® sees the whole picture."
Three Families. Three Journeys. Real Outcomes.
Hyderabad | 6-Year-Old, Non-Verbal ASD | 12 Weeks
Before: "He would walk barefoot on scorching cement in May without any reaction. He'd been scalded in the bath twice. We were terrified to let him bathe without both of us present."
What they used: Anti-scald valve + bath thermometer + clothing chart + wearable monitor during summer.
After: "He checks the bath color every single time now. He looks at it before his foot goes in. He's never scalded again. And the monitor helped us catch him running too hot during outdoor play — twice — before it became dangerous."
From the Therapist: "Bath safety routines became the anchor habit. Safety first, awareness second — in that order."
What they used: Anti-scald valve + bath thermometer + clothing chart + wearable monitor during summer.
After: "He checks the bath color every single time now. He looks at it before his foot goes in. He's never scalded again. And the monitor helped us catch him running too hot during outdoor play — twice — before it became dangerous."
From the Therapist: "Bath safety routines became the anchor habit. Safety first, awareness second — in that order."
Pune | 8-Year-Old, ASD Level 1 | 8 Weeks
Before: "Every morning was a war about the jacket. She'd insist on wearing her favourite sweatshirt in 36-degree heat. The school complained. The neighbours commented. I cried in the car after drop-off."
What they used: Weather-clothing chart on wardrobe door + morning temperature check as first routine step.
After: "The chart made the decision — not me, not her. We stopped fighting because there was nothing to fight about. The chart said shorts. She looked. She got shorts. That was it."
What they used: Weather-clothing chart on wardrobe door + morning temperature check as first routine step.
After: "The chart made the decision — not me, not her. We stopped fighting because there was nothing to fight about. The chart said shorts. She looked. She got shorts. That was it."
Rural Maharashtra (Teleconsult) | 5-Year-Old, SPD | 6 Weeks
Before: "We had no OT near us. I found this page through a search. We made a hand-drawn chart on a piece of cardboard. That's it."
What they used: DIY temperature chart + DIY clothing chart + phone alarm scheduled checks.
After: "He started looking at the cardboard chart before I even prompted him. I honestly couldn't believe it. He's 5, we made it from a cereal box, and it's working."
Therapist note: "Teleconsult parents implementing DIY versions demonstrate equivalent early-phase outcomes to clinic-supported families when consistency is maintained."
What they used: DIY temperature chart + DIY clothing chart + phone alarm scheduled checks.
After: "He started looking at the cardboard chart before I even prompted him. I honestly couldn't believe it. He's 5, we made it from a cereal box, and it's working."
Therapist note: "Teleconsult parents implementing DIY versions demonstrate equivalent early-phase outcomes to clinic-supported families when consistency is maintained."
Note: Identifying details changed for privacy. Outcomes represent individual journeys and vary by profile. Parent-reported outcomes, Pinnacle Network.

You Were Never Meant to Do This Alone
Isolation is the single biggest predictor of intervention dropout. Families who connect with even one other parent navigating the same challenge are significantly more likely to sustain their home program past 4 weeks.
📱 Temperature Awareness Parent WhatsApp Group
For families implementing A-113 and related interoception techniques. Language support: English, Telugu, Hindi, Tamil, Kannada. Join here →
💬 Pinnacle Online Parent Forum
Topic: Sensory Processing & Interoception. 2,400+ active families in this domain thread. Join discussion →
📍 Local Parent Meetups
Organized through nearest Pinnacle center. Monthly group sessions: parent-led, therapist-facilitated. Find your nearest group →
🤝 Peer Mentoring Program
Connect with an experienced parent (18+ months post-A-113). They've been exactly where you are. Request via 9100 181 181 — ask for the Parent Peer Program.
"Your experience helps others. When your child masters temperature awareness — consider sharing your journey. The parent who finds this page next week needs to know it's possible. You are that evidence."
📞9100 181 181 | 24×7 | 16+ Languages | FREE National Autism Helpline
Home-Based Is Powerful. Professional-Guided Is More Powerful.
Every technique on this platform is designed to be parent-executed. But the families who achieve the fastest, deepest, most durable outcomes are those who combine home sessions with periodic professional consultation — even once a month.
What the Professional Session Adds
- Formal interoception assessment (including temperature domain)
- AbilityScore® baseline measurement
- Personalized session plan based on child's specific sensory profile
- Safety audit for temperature management at home
- IEP goal formulation for dressing independence and temperature safety
- Progress tracking through GPT-OS® Daily Living & Independence Index
Home + Clinic = Maximum Impact
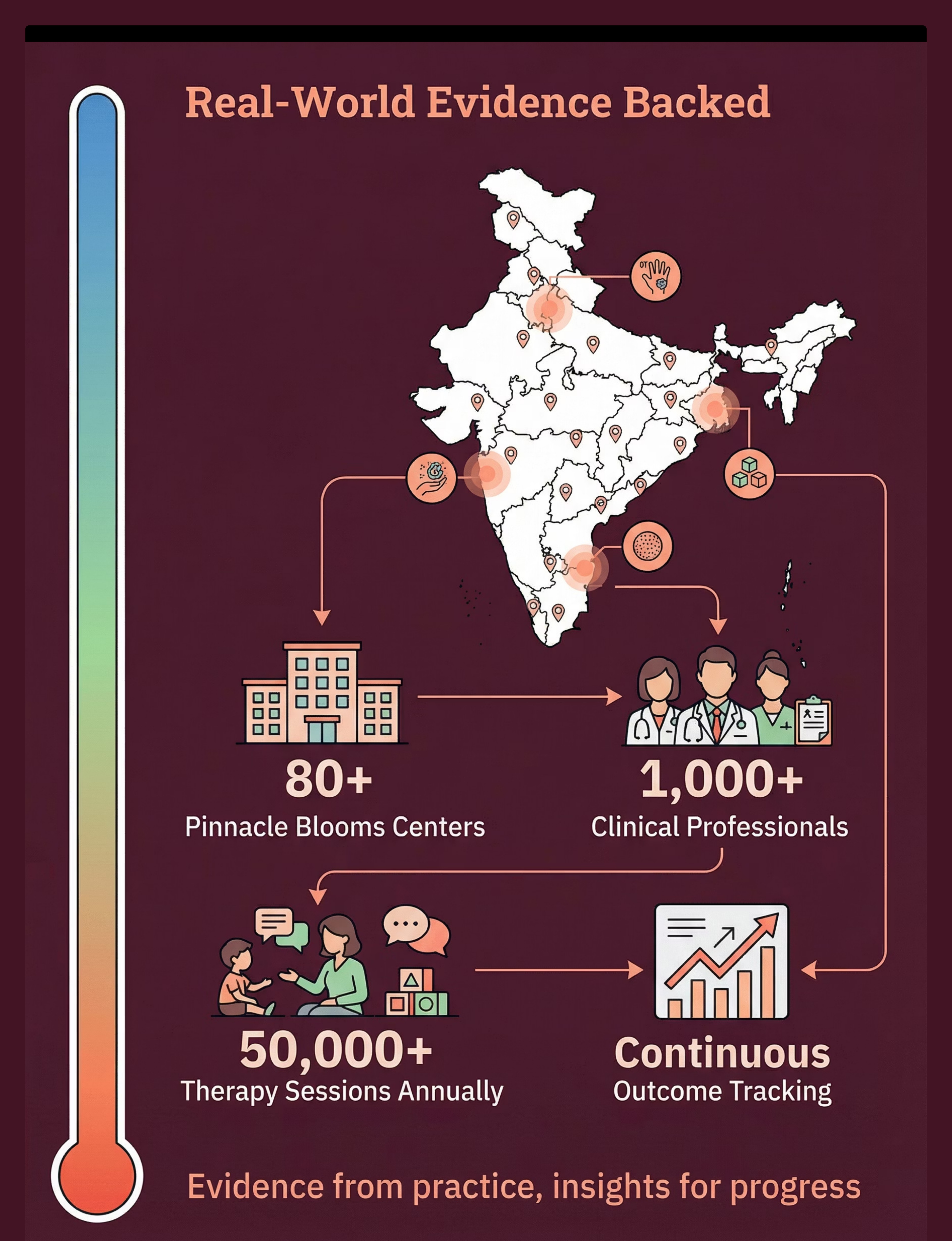
Pinnacle Center Network — 80+ Centers Across India
Primary Discipline: Occupational Therapy (OT/SI specialization)
Supporting: ABA/BCBA | Special Education
Teleconsultation available for families in non-center locations.
Supporting: ABA/BCBA | Special Education
Teleconsultation available for families in non-center locations.
Teleconsultation Booking
📅 Available: Same-week appointments
Format: Video (WhatsApp / Zoom) | Phone | In-app
Languages: 16+
Format: Video (WhatsApp / Zoom) | Phone | In-app
Languages: 16+
Insurance & Funding
OT for sensory processing covered under many private health insurance plans and government disability schemes. SPARSH / NIPUN / RBSK eligibility for qualifying families. Check eligibility →

Transparency: What Happens When You Log a Session
When you record a session in GPT-OS®, you are contributing to both your child's personalized plan and a population-level learning system built on 21 million therapy sessions.

Watch the Reel That Began This Journey
Reel ID: A-113 | Sensory Solutions Series | Episode 113 of 999
This 75-second reel was created by the Pinnacle Blooms Consortium's Occupational Therapy and Sensory Integration team. The 9 materials shown here are the same materials you've just read about in depth on this page. Watch the demonstration — then return to the step-by-step protocol to execute it yourself.
Video Modeling is an Evidence-Based Practice for autism (NCAEP, 2020). Watching before doing improves parent accuracy and child acceptance. Multi-modal learning improves parent skill acquisition.
Content of the Reel
Introduces all 9 materials with therapist demonstration of core techniques
What This Page Adds
Complete execution protocol, safety guidelines, progress tracking, troubleshooting, and professional support pathway
Related Reels in the Interoception Series:
▶ A-111
Hunger Signal Materials
▶ A-112
Bathroom Signal Materials
▶ A-114
Pain Insensitivity Materials
▶ Full Series
View all Interoception Reels

One Parent Executing. Every Caregiver Empowered.
If only one person in the household implements temperature awareness practices, the child's progress is limited to that person's presence. Consistency across ALL caregivers multiplies impact. This card makes that possible.
"A child who sees one parent check the thermometer learns a habit. A child who sees EVERY caregiver check the thermometer builds a conviction."
All Caregivers Need to Know 3 Things:
1
Do Not Fight About Clothing
Show the chart. The chart decides. Remove yourself from the debate entirely.
2
Bath Temperature — Two Checks
Always check the bath temperature yourself with your elbow AND let the child check the device. Both, every time.
3
Outdoor Activity Safety
Water and shade available at all times; check with child every 20 minutes during outdoor activity.
Downloadable Resources
📥 A-113 Family Quick Guide (1-Page PDF)
Top 3 materials, safety non-negotiables, what to say, what NOT to say. Print and post on fridge.
📥 Explain to Grandparents (Simplified Version)
"When [child's name] doesn't wear a jacket even when it's cold — this is why. And here is how you can help."
📥 Teacher/School Communication Template
Letter to class teacher explaining temperature insensitivity, requesting classroom thermometer access, and IEP dressing independence goal context.

Your Questions — Answered Before You Have to Ask
Q: My child doesn't have autism — they have sensory processing differences. Does A-113 still apply?
Yes. Temperature insensitivity occurs across SPD, ADHD, hypermobility syndromes, and other profiles. The materials and protocol apply regardless of diagnosis. The approach is sensory-functional, not diagnosis-specific.
Q: How do I know if my child's temperature insensitivity is medical or sensory?
A NeuroDev Pediatrician should rule out medical causes (peripheral neuropathy, autonomic dysfunction, thyroid conditions) before or alongside sensory intervention. If the insensitivity is sudden-onset or worsening, medical evaluation first. Call 9100 181 181 for a referral pathway.
Q: My child is 13. Is it too late to implement A-113?
No. Interoceptive awareness can be developed across the lifespan. The materials may need age-adjustment (weather app instead of wall chart; phone alarm instead of visual schedule), but the therapeutic principles are equally valid. Reach our adolescent-specialist OT team at 9100 181 181.
Q: We tried the clothing chart but my child refuses to use it. What do we do?
Chart resistance usually means the chart hasn't been paired with positive experiences yet. Spend 1 week pairing: admire the chart together, play "what zone is it today?" with no clothing demands. The demand comes AFTER the chart is familiar. See Troubleshooting Card, Problem 2.
Q: Can I do this without any commercial materials? We can't afford them right now.
Yes — fully. The DIY card contains complete instructions for all 9 materials at ₹0–₹150 total. Dozens of families in rural areas have achieved the same early outcomes with cereal-box charts and printed body templates. Start today.
Q: How long until I see results?
Weeks 1–2: tolerance and routine formation. Weeks 3–4: first independent checking behaviors. Weeks 5–8: mastery of primary target. This is the evidence-based timeline. Significant individual variation exists — some children show mastery at week 4; some need 12 weeks. The tracking sheet will show you YOUR child's curve.
Q: My child's therapist hasn't heard of this intervention. Is it Pinnacle-specific?
The materials (thermometers, clothing charts, bath safety devices, body mapping) are standard OT practice for interoception development. The specific 40-card protocol and GPT-OS® data integration are Pinnacle-specific. Share the Research Library card with your therapist — the citations are international peer-reviewed evidence.
Q: Can this page be used alongside clinic-based OT?
This is the ideal use case. Home sessions (using this page) + clinic OT sessions create the frequency and environment generalization that produces the fastest outcomes. Show your OT this page — the protocol aligns with standard SI practice.
Didn't find your answer? Ask GPT-OS® → | Still need help? Book a teleconsultation: 9100 181 181
Preview of 9 materials that help when child cant feel temperature Therapy Material
Below is a visual preview of 9 materials that help when child cant feel temperature therapy material. The pages shown help educators, therapists, and caregivers understand the structure and content of the resource before use. Materials should be used under appropriate professional guidance.
















Share this resource
Help others discover thisLink copied!

Your Child's Temperature Safety Starts Today.
Choose how you want to begin:
The Pinnacle Promise
21M+
Exclusive 1:1 Sessions
GPT-OS® powered therapeutic intelligence
97%+
Measured Improvement
Across sensory and interoceptive challenges
80+
Centers Across India
Plus teleconsultation for all families
70K+
Intervention Techniques
Mapped across 12 developmental domains
📞9100 181 181 | FREE National Autism Helpline | 24×7 | 16+ Languages | "Speak to a therapist before your first session if you have concerns."
This content is educational and does not replace assessment by a licensed occupational therapist, physician, or developmental pediatrician. Individual results vary. Statistics represent aggregate outcomes across the Pinnacle Blooms Network. Temperature insensitivity can be a safety concern requiring medical evaluation. Children with significant thermoregulatory differences should be evaluated by appropriate medical specialists to rule out underlying medical conditions. Adult supervision is essential during all activities. Please consult qualified healthcare professionals before implementing any strategies.
© 2025–2026 Pinnacle Blooms Network®, a unit of Bharath Healthcare Laboratories Pvt. Ltd. All rights reserved. | CIN: U74999TG2016PTC113063 | DPIIT: DIPP8651 | MSME: Udyog Aadhaar TS20F0009606 | GSTIN: 36AAGCB9722P1Z2 | ISO 13485 | ISO/IEC 27001
"From Fear to Mastery. One Technique at a Time." — Pinnacle Blooms Consortium®
