


What Is Tactile Defensiveness?
The nervous system has two tactile modes: protective (danger detection) and discriminative (texture identification). In tactile over-responsivity, the protective system is overactive. It interprets light touch — like grass blades on skin — as potentially dangerous and triggers fight, flight, or freeze. Grass is uniquely challenging: thousands of individual blades creating unpredictable contact points, variable moisture, slight prickliness, temperature variation, and clinging. For a child whose "volume dial" is already turned to maximum, this is sensory overload. This Is Neurological Not dramatic. Not chosen. Not manipulation. The child is not choosing their response. Their brain is telling them they are in danger. Why Forcing Doesn't Work Picking a child up and placing them on grass confirms to their nervous system that grass IS dangerous — because the experience becomes traumatic. Gradual desensitization is the evidence-based path forward. Reference: Frontiers in Integrative Neuroscience (2020) — DOI: 10.3389/fnint.2020.556660




# | Material | Price (₹) | Purpose | |
1 | Artificial Grass Samples & Turf Squares | 200–800 | Controlled indoor grass exposure — start soft, progress to realistic | |
2 | Therapeutic Brushing Protocol Tools (Wilbarger-Style) | 300–600 | Calms the WHOLE tactile system — requires OT training ⚠️ | |
3 | Graded Texture Exposure Bins | 400–1,200 | Step-by-step texture hierarchy from cotton to real grass | |
4 | Weighted & Compression Clothing | 800–2,500 | Deep pressure calms the nervous system BEFORE exposure | |
5 | Transitional Footwear (Water shoes, grip socks) | 300–800 | Participate NOW while building tolerance for later | |
6 | Preferred Activity Pairing Materials (Bubbles, toys, snacks) | 200–600 | Build positive associations — grass predicts fun | |
7 | Dry vs. Wet Grass Practice Materials | 100–300 | Start with easier conditions, build to harder | |
8 | Proprioceptive Preparation Activities (Trampoline, weighted items) | 500–2,000 | Heavy work BEFORE grass exposure for nervous system readiness | |
9 | Social Stories & Visual Supports | 200–500 | Predictability reduces anxiety — prepare the mind, prepare the body |

- Artificial grass samples (₹200–800) — soft-to-realistic turf progression
- Texture exposure bins (₹400–1,200) — graduated container sets
- Compression vest (₹800–2,500) — calibrated deep pressure
- Transitional footwear (₹300–800) — water shoes, grip socks
- Social stories (₹200–500) — professionally illustrated, structured narrative
- Proprioceptive equipment (₹500–2,000) — mini trampoline, resistance bands
- Request FREE turf samples from local flooring stores. Cut textured green fabric from old towels.
- Any plastic container: cotton balls → dry rice → dry pasta → shredded paper → grass clippings
- Tight-fitting athletic wear or lycra swim shirts. Firm hugs before exposure.
- Old socks with rubber dots (fabric paint). Gradually cut toes off for progressive exposure.
- Phone photos: "Today I will try touching grass. First I sit on the blanket. Then I touch with one finger."
- Wall push-ups, carrying heavy books in a backpack, wheelbarrow walks, jumping on mattress on floor

- Child has open wounds or skin irritation on contact areas
- Child is acutely ill, feverish, or recovering from illness
- Child has had a severe meltdown within the past 30 minutes
- Grass has been treated with pesticides, fertilizers, or chemicals
- Child shows signs of anaphylactic grass allergy (hives, swelling — different from sensory aversion)
- You have not received OT training for the Wilbarger brushing protocol (Material #2 only)
- Child is tired, hungry, or dysregulated → do proprioceptive prep first, shorten session
- Weather is extreme → use indoor materials only
- Child is recovering from a difficult day → reduce demands, increase reinforcement
- Multiple people are present (overstimulation risk) → do private sessions first
- Child is fed, rested, and in a regulated state
- Materials are clean and age-appropriate
- Environment is quiet and controlled
- You have 15–20 uninterrupted minutes
- Preferred reinforcers are prepared and ready

- Choose a quiet room with minimal distractions
- Place texture bin or artificial grass sample on the floor on a towel (easy cleanup)
- Position preferred reinforcers within YOUR reach, not child's (you control delivery)
- Place visual schedule/social story where child can see it
- Remove shoes and socks if working on foot tolerance, or short sleeves for arm tolerance
- Designate a "safe zone" — a blanket or mat the child can retreat to if overwhelmed
- Choose dry, warm afternoon (warmest, driest grass conditions)
- Lay a blanket as home base with preferred items already there
- Position at the EDGE of grass, not the center
- Have transitional footwear ready and accessible
- Complete proprioceptive preparation BEFORE reaching the grass area
- Have exit strategy planned — child can return to blanket at any time, no negotiation


Parent Script — Say These Words:
"Look what I have! Want to see something interesting? Come sit with me. You don't have to touch anything. Just come look."

Script:
"Watch me touch this. See? It feels [describe: bumpy, soft, tickly]. I wonder what it feels like on my finger... My finger says it's a little scratchy but okay! Want to try just one finger?"


Step 4 — Repetitions Build Neural Pathways
Duration: 3–5 minutes Target: 3–5 quality reps Repetition is how the nervous system rewires. Each quality contact at the current level sends a signal: this is safe, this is manageable, this is not a threat. But repetition without engagement is noise. A child who joyfully touches grass 3 times is building stronger neural pathways than one who grimaces through 10 forced contacts. Quality always outranks quantity. "3 good reps > 10 forced reps." Variations to Maintain Engagement Touch with different body parts (fingers, palm, back of hand, forearm) Touch different textures at same difficulty level (different artificial grass samples) Hide small preferred toys in the texture (treasure hunt motivation) Use different locations in the room for generalization Vary time of day across sessions to build flexibility Satiation Indicators — When to Stop Child becomes restless or disengaged Response quality decreases (half-hearted touches) Child starts negotiating to end the session Child has completed 5 quality repetitions Honor these signals. Ending on success — before satiation — keeps tomorrow's session positive.



Data Point | How to Record | Example | |
Level reached | Number 1–9 from the hierarchy | "Level 3 — multi-finger touch" | |
Duration of contact | Seconds of voluntary contact | "Held contact for 5 seconds" | |
Distress level | 1–5 scale (1=calm, 5=meltdown) | "2 — slightly uncomfortable but continued" | |
Reinforcer used | Name the reinforcer delivered | "Bubbles + verbal praise" | |
Notes | Any environmental factors | "Tired from school — shorter session" |

Problem | Why It Happened | What to Do | |
Child refused to come near the material | Demand was too high or child wasn't regulated | Start with JUST watching you touch it. No demand on child. Pair your touching with their preferred music or show. | |
Child touched but immediately became distressed | Level was too advanced or contact duration too long | Drop back one level. Reduce contact to 1–2 seconds. Increase reinforcement density. | |
Child was fine indoors but panicked outside | Outdoor environment adds unpredictable variables (wind, insects, wetness, heat) | Normal. Indoor tolerance ≠ outdoor tolerance. Maintain indoor practice while doing outdoor VISUAL-ONLY exposure. | |
Child regressed after a good week | Illness, sleep disruption, stress, or nervous system fluctuation | Take a 2-day break. Resume at the last comfortable level. Not regression — recalibration. | |
Another caregiver forced grass contact | Well-meaning but counterproductive — sets the nervous system back | Share Card 37 (Family Guide). Explain that forcing creates trauma, not tolerance. Resume gradual protocol after 3–5 day break. |
"Session abandonment is not failure — it's data."

- Child may approach the material without leaving the room (even without touching)
- Reduced protest when materials are brought out — the routine becomes familiar
- Willingness to watch you interact with textures without distress
- Brief 1–3 second touches beginning at lower hierarchy levels
- Beginning to associate session time with positive reinforcement and good feelings
- Barefoot grass tolerance — that comes much later
- Spontaneous grass approach without prompting
- Outdoor generalization of indoor progress
"If your child tolerates the artificial grass for 3 seconds longer than last week — that's real progress."



"Backyard birthday parties. Grass angels. Barefoot summers. You are building this, one session at a time."

Sign | What It May Mean | What to Do | |
No improvement after 8 weeks of consistent practice | May need professional sensory evaluation and modified approach | Book OT evaluation at Pinnacle (see Card 33) | |
Grass aversion is WORSENING despite gradual approach | Protocol may be too aggressive, or underlying anxiety needs addressing | Pause all grass work for 2 weeks. Consult OT immediately. | |
Multiple severe texture aversions limiting daily life | Broader sensory modulation disorder requiring comprehensive intervention | Comprehensive sensory evaluation needed across all domains | |
Tactile sensitivity affecting feeding, dressing, hygiene | Systemic tactile defensiveness beyond grass alone | Full OT sensory integration assessment — this is urgent | |
Child shows self-injurious behavior during grass exposure | Distress level exceeds the child's coping capacity entirely | Stop immediately. Do not resume without professional guidance. | |
Regression in previously tolerated textures | Possible medical contributor, stress, or environmental change | NeuroDev Pediatrician evaluation recommended promptly |
📞 Free Helpline: 9100 181 181 | 16+ languages | 24×7






"When my daughter was three, she screamed if a single blade of grass touched her foot. Birthday parties were impossible. Parks were minefields. After six months of gradual desensitization with our OT at Pinnacle — starting with artificial grass samples indoors and working through a texture progression — she's now five and runs barefoot across our lawn. Last week she made grass angels. GRASS ANGELS. I never thought I'd see her lying in the grass by choice, laughing."
— Parent, Pinnacle Network
"We started with the texture bins. Cotton balls, then rice, then shredded paper, then artificial grass. It took 10 weeks before my son would touch the artificial grass sample. But once he did — once his nervous system learned it was safe — the transfer to real grass took only 3 more weeks. He now plays in the garden wearing water shoes. We're working toward barefoot. Every step is a victory."
— Parent, Pinnacle Network


Meta-Analysis (World J Clin Cases, 2024): 24 studies confirm SI therapy efficacy — PMC10955541
Frontiers in Integrative Neuroscience (2020): Neurological framework for sensory interventions — DOI: 10.3389/fnint.2020.556660
WHO/UNICEF Care for Child Development Package (2023) — PMC9978394
NCAEP Evidence-Based Practices Report (2020)
Proof: 20M+ 1:1 sessions • 97%+ measured improvement • 70+ centers • Patents filed across 160+ countries



Your Questions, Answered
These are the questions Pinnacle Blooms families ask most often — gathered from teleconsultations, parent support groups, and helpline calls across 70+ countries. Read through all of them. The answer to your question may help you understand your neighbor's question too. How long until my child can walk barefoot on grass? Timelines vary significantly. Some children reach barefoot tolerance in 6–8 weeks of daily practice. Others take 3–6 months. The pace must be child-led. Consistent daily practice produces faster results than sporadic attempts. Progress is rarely linear — expect plateaus and small regressions as normal parts of the journey. Is this just a phase they'll grow out of? Some children do naturally desensitize over time. However, children with sensory processing differences often do NOT habituate automatically and may carry texture aversions into adolescence and adulthood without structured support. Early, systematic intervention produces the best long-term outcomes. Can I do the Wilbarger brushing protocol at home without an OT? No. The Wilbarger protocol MUST be taught by a trained occupational therapist. Incorrect pressure, direction, or frequency can increase defensiveness rather than reduce it. Never attempt without professional training — this is the one non-negotiable in the entire protocol. What if my child has a grass allergy, not a sensory issue? Grass allergy produces hives, redness, swelling, sneezing, or itching. Sensory aversion produces freezing, pulling away, distress, and meltdowns without skin changes. If you see skin reactions, consult a pediatric allergist before beginning any sensory work. My family thinks I should just force them onto the grass. What do I say? Share Card 03 (the neuroscience card). Forcing confirms to the nervous system that grass IS dangerous — because the forced experience is traumatic. Gradual desensitization recalibrates the threat threshold instead. Share this page or the Family Guide from Card 37. Do I need to buy all 9 materials? No. Start with the Essential Starter Kit: artificial grass samples + texture bin materials + water shoes + bubbles + social story = under ₹1,500. Add others as needed. See Card 10 for zero-cost DIY alternatives for every item. When should I involve a professional? See Card 27 (Red Flags). If there's no improvement after 8 weeks of consistent practice, if multiple severe texture aversions exist, or if sensitivity affects feeding, dressing, or hygiene — seek comprehensive OT evaluation immediately. Can this technique work for sand, fabric, and other texture aversions too? Yes. The same graded desensitization principles apply across all textures. The hierarchy and specific materials change, but the methodology is identical. See related techniques in Card 29 — many materials you've already gathered will transfer directly. Ask GPT-OS® Your Question Book a Teleconsultation

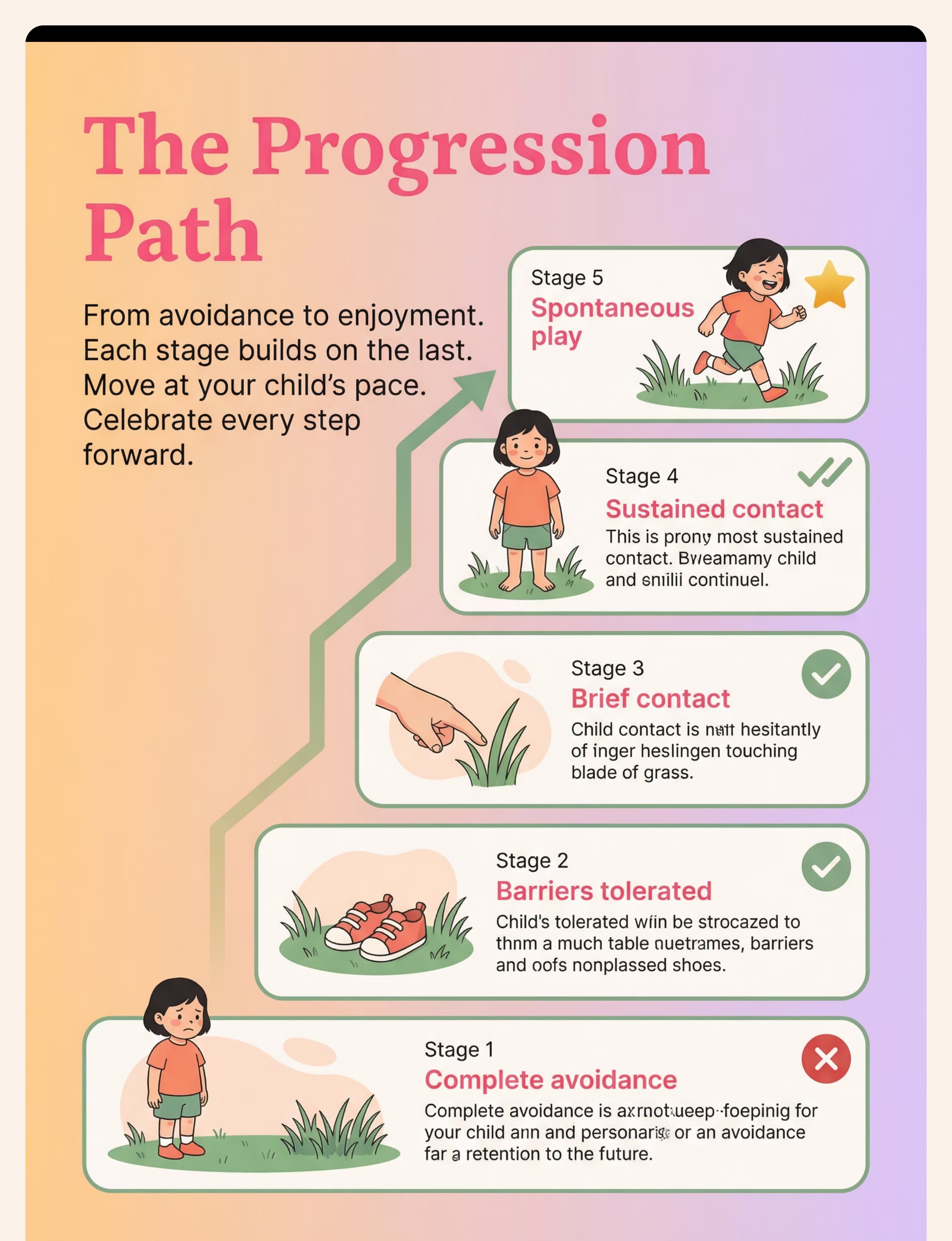
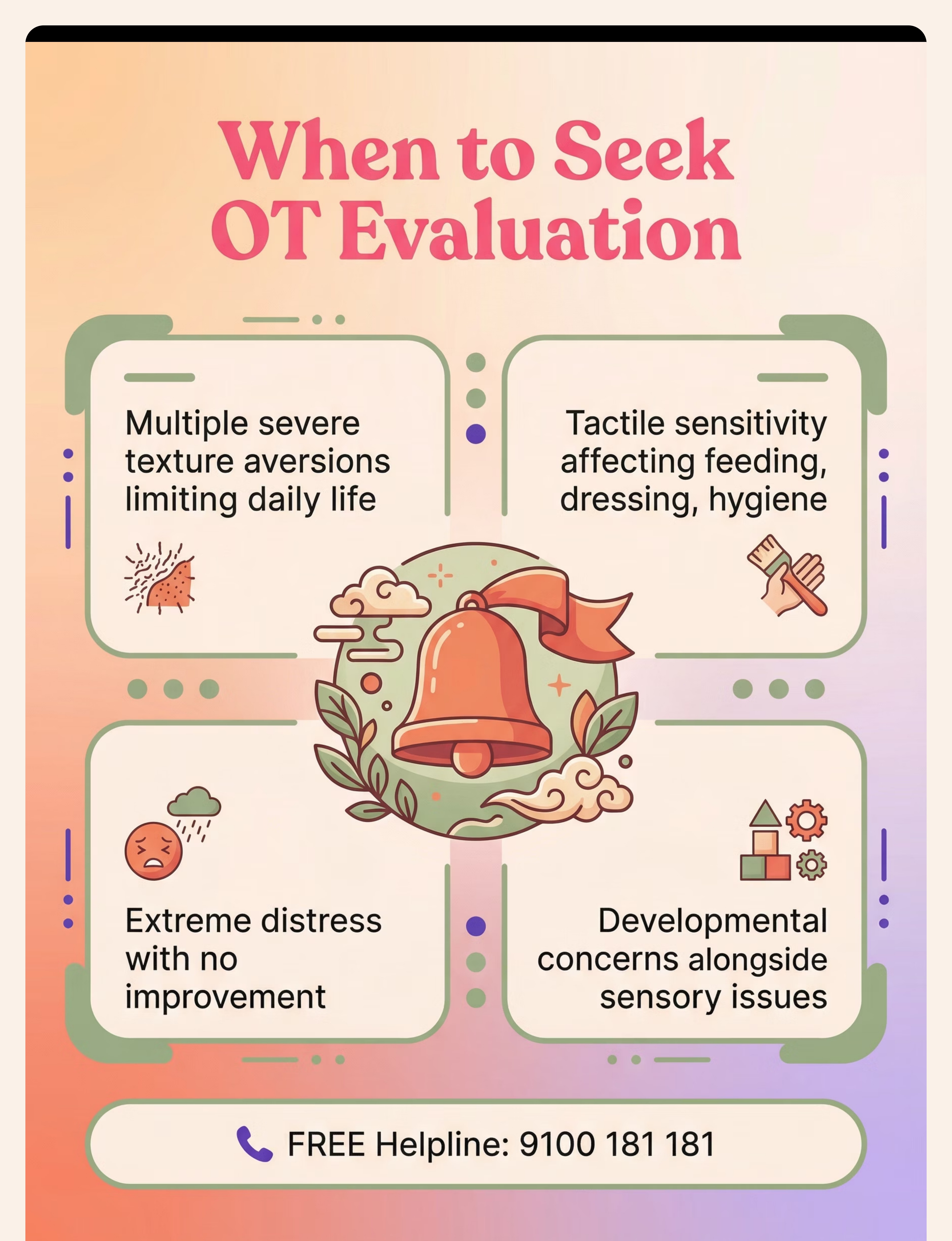
Preview of 9 materials that help with grass texture aversion Therapy Material
Below is a visual preview of 9 materials that help with grass texture aversion therapy material. The pages shown help educators, therapists, and caregivers understand the structure and content of the resource before use. Materials should be used under appropriate professional guidance.















Share this resource
Help others discover this
Statutory Identifiers: CIN: U74999TG2016PTC113063 | DPIIT: DIPP8651 (Govt. of India) | MSME Udyog Aadhaar: TS20F0009606 | GSTIN: 36AAGCB9722P1Z2
© 2025 Pinnacle Blooms Network®, unit of Bharath Healthcare Laboratories Pvt. Ltd. All rights reserved.
Website:pinnacleblooms.org | Helpline: 9100 181 181 | Email:care@pinnacleblooms.org
