
When Colors Feel Like Too Much
Your daughter covers her eyes the moment she walks into her colourful classroom. She says the yellow walls "hurt." Red makes her anxious — she won't touch red crayons, refuses red plates, melts down at birthday parties surrounded by colourful balloons. People say she's being dramatic. You see something else entirely. You see genuine pain.
You are not failing. Your child's visual system is speaking. And there is a name, a science, and a pathway for this.
Color Sensitivity Accommodation & Coping Materials
9 Evidence-Based Tools
Developed by the Pinnacle Blooms Network® — Consortium of Pediatric OT • SLP • BCBA • Special Education • NeuroDevelopmental Pediatrics

You Are Not Alone — The Numbers
Color sensitivity is one of the most common — and most misunderstood — forms of visual sensory processing difference. Millions of families worldwide are navigating this exact challenge.
80%
Children with Autism
display sensory processing difficulties, including visual sensory over-responsivity (PRISMA Systematic Review, Children, 2024; PMC11506176)
1 in 7
General Population
children experience clinically significant sensory processing challenges that impact daily functioning (Ahn et al., 2004; Ben-Sasson et al., 2009)
46%
Peak Prevalence
of visual stress and chromatic sensitivity in school-age populations, with higher rates in neurodivergent children (Irlen Institute; Wilkins et al., 2001)
Across India's 472 million children, an estimated 33–38 million may experience sensory processing differences. Pinnacle Blooms Network has served families navigating visual sensory challenges across 70+ centres and from 70+ countries. Your child is not alone. You are not alone.

What's Happening in Your Child's Brain
Your child's eyes work fine. The difference is in how their brain processes colour information — and understanding this changes everything.
The Neuroscience, Made Clear
Retinal Level: Cone cells detecting colour wavelengths may have different sensitivity thresholds. Certain wavelengths — often red/yellow or fluorescent spectrum — trigger a stronger signal than in typical visual systems.
Cortical Level: The visual cortex has a lower threshold for "too much." What registers as pleasant stimulation in a typical brain registers as overwhelming intensity in your child's brain.
Cross-Modal Impact: In some children, colour input triggers the autonomic nervous system — activating fight-flight-freeze responses. This is why their body responds as though under threat.
Cumulative Load: Brief exposure may be tolerable, but sustained exposure overwhelms the system — which is why your child comes home exhausted after a school day in a colourful classroom.
The Key Message
This is a wiring difference, not a behaviour choice. Not dramatic. Not picky. Neurological.
Light enters the eye → retinal cone cells respond to wavelength → optic nerve transmits the signal → the visual cortex interprets colour → the limbic system (amygdala) may trigger an emotional or autonomic response.
The over-responsivity occurs at the visual cortex level — moderate colour input is interpreted as intense stimulation. This neurological reality is the foundation for every accommodation strategy in this guide.
Source: Frontiers in Integrative Neuroscience (2020) — DOI: 10.3389/fnint.2020.556660
Where This Sits in Development
Colour sensitivity doesn't appear from nowhere — it emerges and evolves across childhood. Understanding the developmental timeline helps you know where your child is, and where they're headed.
0–12 Months
Visual system developing. Preferences for faces and high contrast. Colour perception matures gradually.
12–24 Months
Colour naming begins. Early signs of visual preference or avoidance may appear.
2–4 Years ★
Common Emergence Zone. Colour sensitivity becomes apparent as environments grow more chromatic — preschool, playdates, birthday parties. Verbal children begin reporting discomfort.
4–7 Years
School environments intensify exposure. Classroom decorations, colourful supplies, group activities amplify challenges. Cumulative load becomes a daily factor.
7–12 Years
Self-awareness develops. Child may build coping strategies or avoidance patterns. Advocacy skills can now be actively taught.
Comorbidity Awareness: Colour sensitivity frequently co-occurs with light sensitivity, pattern sensitivity, visual clutter overwhelm, general sensory over-responsivity, migraine conditions, Irlen Syndrome/Scotopic Sensitivity, and anxiety disorders. Screening for co-occurring visual and sensory challenges is recommended.

The Evidence Behind This Technique
Level II Evidence
Clinically Validated
Home-Applicable
Supported by systematic reviews, meta-analyses of sensory integration interventions, and clinical consensus across occupational therapy, developmental optometry, and visual processing research.
PRISMA Systematic Review (Children, 2024)
16 articles from 2013–2023 confirm sensory integration intervention meets criteria as evidence-based practice for children with ASD. Environmental modification is a first-line intervention for sensory over-responsivity. (PMC11506176)
Meta-Analysis (World J Clin Cases, 2024)
24 studies demonstrate sensory integration therapy effectively promotes adaptive behaviour, sensory processing improvement, and functional skills. (PMC10955541)
Indian RCT (Indian J Pediatrics, 2019)
Home-based sensory interventions demonstrated significant outcomes in Indian paediatric populations, validating parent-administered sensory accommodation protocols. (Padmanabha et al.)
AOTA Practice Guidelines
The American Occupational Therapy Association endorses environmental modification and sensory tool provision as primary interventions for visual sensory over-responsivity.

The Technique — What It Is
A-071
Domain A: Sensory Processing
Age 2–12 Years
Formal Name
Color Sensitivity Environmental Accommodation & Coping Materials Protocol
Parent-Friendly Alias
"The Color Toolkit" — 9 materials that help your child manage a world full of overwhelming colours.
Specifications
Setting: Home + School + Community
Duration: Ongoing — daily accommodation + structured sessions 2–3× per week, 10–20 min each
Difficulty: Introductory (environmental) to Core (tolerance building)
Duration: Ongoing — daily accommodation + structured sessions 2–3× per week, 10–20 min each
Difficulty: Introductory (environmental) to Core (tolerance building)
Definition
Color Sensitivity Accommodation is a structured, evidence-based approach that uses environmental modification, filtering tools, portable coping devices, gradual tolerance-building materials, and self-advocacy training to help children with chromatic hypersensitivity function and participate in environments that would otherwise cause distress, meltdowns, or withdrawal.
This is not about "fixing" your child. It is about equipping them.
The 9 Canon Materials
- Tinted Glasses & Lenses
- Neutral Environment Materials
- Visual Shields
- Lighting Tools
- Gradient Materials
- Safe Colour Materials
- Decompression Tools
- Advocacy Tools
- Colour-Reduced Supplies

Who Uses This Technique
Colour sensitivity affects the whole child — which is why it requires a whole team. This technique crosses therapy boundaries because the brain doesn't organise by therapy type.
Occupational Therapy
The OT leads environmental assessment, sensory profiling, material selection, and desensitisation protocols. Designs the sensory diet integrating colour accommodation into daily routines. Primary discipline lead.
Developmental Optometry
Conducts comprehensive visual processing assessment. Rules out underlying visual conditions. Evaluates for Irlen Syndrome/Scotopic Sensitivity. Prescribes precision-tinted lenses when indicated.
BCBA
Designs systematic desensitisation programmes using gradient materials. Develops reinforcement schedules. Creates data collection systems. Trains self-advocacy communication behaviours.
Special Educator
Implements classroom accommodations. Coordinates environmental modifications with school administration. Integrates colour-reduced materials into academic activities.
NeuroDevelopmental Paediatrician
Screens for co-occurring conditions including migraine, anxiety, and neurological conditions affecting visual processing. Provides medical documentation supporting accommodation requests.

What This Technique Targets
Colour sensitivity accommodation works across multiple levels — from the immediate neurological response to long-term social participation and family wellbeing.
Primary Target
Visual Sensory Modulation — reducing the neurological impact of chromatic input. Observable indicators: decreased eye-covering in colourful spaces, reduced meltdown frequency, extended tolerance duration, self-initiated use of coping tools.
Secondary & Tertiary Targets
Secondary: Environmental tolerance, self-regulation, self-advocacy — including attending birthday parties with accommodation and requesting tools proactively.
Tertiary: Academic participation, social connection, family quality of life, and emotional well-being — decreased anxiety, increased confidence and sense of agency.

What You Need — The 9 Primary Materials
Every material in the Color Toolkit serves a specific therapeutic purpose. Most families begin with under ₹2,000 in essential items — and many substitutes are free.
# | Material | Canon Category | Price Range (INR) | Source | |
1 | Tinted Glasses & Lenses | Visual Filtering Tools | ₹500–15,000 | Local optician / Amazon.in | |
2 | Neutral Environment Materials | Environmental Modification | ₹500–10,000+ | Home furnishing stores | |
3 | Colour-Reduced School Supplies | Daily Tools | ₹200–1,500 | Stationery stores / Amazon.in | |
4 | Portable Visual Shields | Portable Coping Tools | ₹300–2,000 | Office supplies / DIY | |
5 | Lighting Modification Tools | Environmental Modification | ₹500–5,000 | Electrical stores / Amazon.in | |
6 | Colour Gradient Materials | Tolerance Building | ₹300–1,500 | Art supplies / Paint stores | |
7 | Single-Colour Safe Materials | Safe Access Tools | ₹200–1,500 | Art/toy stores / Amazon.in | |
8 | Visual Decompression Tools | Recovery Tools | ₹200–1,500 | Sensory shops / DIY | |
9 | Advocacy & Communication Tools | Communication Tools | ₹0–500 | DIY / Free templates |
Total Investment Range: ₹0–15,000. Most families start under ₹2,000. Essential starters: identify child's safe colours (zero cost), create one neutral space at home, and trial basic tinted glasses (₹500–2,000).

DIY & Substitute Options
Equity Principle
Every family, regardless of economic circumstance, can implement colour sensitivity accommodation today. The WHO/UNICEF Nurturing Care Framework emphasises context-specific, equity-focused interventions. Below are zero-cost and low-cost alternatives for every material category.
Buy This | Make This (Zero/Low Cost) | |
Precision tinted glasses (₹5,000–15,000) | Start with inexpensive coloured sunglasses in grey, rose, or amber tint (₹100–300 from local vendor). Once a helpful tint is identified, invest in a quality pair. | |
Neutral bedding & furnishings (₹2,000–10,000) | Flip colourful bedsheets to the plain white reverse side. Cover bright furniture with plain cotton sheets. Remove colourful decorations from child's room. | |
Colour-reduced school supplies (₹500–1,500) | Cover colourful folders with brown paper bags. Wrap pencil cases in neutral fabric. Use black electrical tape over bright logos. | |
Portable visual shields (₹500–2,000) | Create a foldable desk shield from a neutral-coloured cardboard box. Use a plain cap to reduce peripheral colour input. Carry a plain manila folder for visual blocking. | |
Smart LED bulbs (₹800–2,000) | Replace overhead fluorescent with a warm-toned table lamp (₹200–500). Use plain white cloth draped over a lampshade to soften light. | |
Colour gradient art sets (₹500–1,500) | Collect free paint sample swatches from hardware stores — arrange from grey to coloured. Mix white paint into existing paints to create pale versions. | |
Advocacy cards (₹200–500) | Hand-write or print on plain paper: "Colours are overwhelming me. I need a visual break." Laminate with clear tape. Practice scripts at home. Free. |
Why Substitutes Work: The therapeutic principle is identical — reducing chromatic input, providing sensory refuge, and building agency. A cardboard desk shield filters the same visual field as a ₹2,000 commercial screen. What matters is consistent use, not price. Non-Negotiable: If colour sensitivity is severe or impacts reading, a developmental optometrist assessment cannot be substituted.

Safety First — Before You Begin
Understanding when to pause, when to proceed with caution, and when it's safe to begin at home is essential before introducing any accommodation tools.
1
🔴 DO NOT PROCEED — Refer Immediately If:
- Child reports persistent headaches or nausea with colour/light exposure → Refer to paediatric neurologist
- Child has difficulty reading or tracking text (words "move" or "swim") → Refer to developmental optometrist
- Colour sensitivity appeared suddenly, not lifelong → Seek medical evaluation
- Child has seizure history and colour exposure triggers episodes → Medical management required first
- Child reports visual disturbances: flashing, spots, halos → Ophthalmological assessment needed
2
🟡 PROCEED WITH CAUTION:
- Never force exposure to problematic colours — flooding causes trauma and increases sensitivity
- Gradient tolerance building must always be child-led — if distress appears, stop immediately
- Portable shields should support participation, not enable permanent isolation
- Monitor cumulative sensory load — allow recovery time between colour-intense activities
- Safe colours may change over time — reassess periodically
3
🟢 SAFE TO BEGIN AT HOME:
- Environmental modification of child's bedroom and primary space
- Basic tinted glasses trials (inexpensive, non-prescription)
- Colour-reduced school supplies selection
- Safe colour identification through observation and gentle conversation
- Advocacy card creation and self-advocacy practice
- Decompression toolkit assembly
Child State Requirements: Begin accommodation introduction when the child is calm, fed, and rested — not during or immediately after a colour-triggered meltdown. The first introduction should always be in the child's safe space.

Setting Up Your Space
A well-organised home environment is the foundation of the entire Color Toolkit. Setup takes 1–3 hours for the initial audit; material procurement can happen gradually over 1–2 weeks.
Zone 1 — The Safe Space
Audit chromatic load in the child's bedroom. Remove or cover the most intense items first. Target: a reliably neutral visual environment with natural textures — wood, cotton, linen — providing warmth without chromatic intensity. Neutral bedding, muted curtains, warm-toned lighting (2700–3000K). This space is the child's sensory reset button. Non-negotiable.
Zone 2 — The Tool Station
Accessible to the child independently. Includes: tinted glasses, portable visual shield (folded, ready to grab), decompression kit (eye mask, calming bottle, neutral imagery), advocacy cards (in child's bag for school and outings), and safe-colour art supplies in a separate, clearly labelled box.
Zone 3 — The Practice Area
For optional gradient work if pursuing tolerance building. Well-lit area with warm lighting. Gradient materials organised from neutral to coloured. Colour tolerance tracking chart on wall. Timer for structured sessions. Reinforcement items ready.
Environmental Audit Checklist
- Child's bedroom chromatic load assessed and reduced
- At least one neutral safe space established
- Lighting reviewed — fluorescent replaced with warm alternatives where possible
- Child's school bag contains: tinted glasses, portable shield, advocacy cards
- Decompression toolkit assembled and child knows its location
- School informed of colour sensitivity
- Family informed of accommodation approach

Is Your Child Ready?
Before beginning structured sessions, confirm all readiness indicators are in place. Environmental accommodation itself — creating the safe space, reducing chromatic load — is a powerful intervention that requires no structured session. Start there if any items below are "Not Yet."
Safe Space Established
Child has at least one reliably neutral environment where they can decompress freely.
Basic Tools Available
At minimum: a tinted glasses trial and a decompression kit assembled and accessible.
Child Is Calm Right Now
Not during or after a meltdown. Sessions begin from a regulated baseline only.
Safety Card Read
Parent has reviewed Card 11 — red flags understood, referral pathways known.
Safe Colours Identified
You know which colours feel comfortable for your child through observation and conversation.
Session Timing Chosen
A calm period is selected — not before a demanding activity. Recovery time is available afterwards.
Accommodation-Only Families: If you are not pursuing active tolerance building, you can move directly to tracking your child's accommodation use and environmental tolerance. The structured protocol steps below are specifically for families also pursuing gradual, child-led tolerance expansion using gradient materials.

Step 1 of 6
The Invitation
The Invitation Script
"Hey [child's name], I have something interesting to show you. You know how some colours feel really big and loud to you? I've been learning about that, and I have some cool new tools that might help. Want to see?"
Do:
- Frame as exploration, not therapy
- Use the child's own language for their experience
- Offer choice — "Want to try today, or tomorrow?"
- Show tools in the safe space
- Let curiosity lead
Don't:
- Say "We need to work on your colour problem"
- Force participation in any form
- Introduce tools in a colour-overwhelming environment
- Rush the explanation
Child's Agency
If the child says "not today" — respect it completely. Revisit tomorrow. The invitation should feel safe, not obligatory. A child who feels forced will resist all tools.
Session Timing
2–3 minutes for invitation and tool introduction. Keep it light, brief, and joyful.

Step 2 of 6
Engagement & Exploration
In the safe space, introduce 2–3 tools — not all 9 at once. Let the child explore each one physically. No expectations, no performance. Just exploration.
Tinted Glasses
"These are like sunglasses for colours. They make bright colours quieter. Want to try them on?" Let the child look around the room. Notice any reactions — even a moment of calm is meaningful.
Safe Colour Materials
"I noticed you really like [safe colour]. I got some art supplies in just that colour, so you can always have colours that feel good." Give child the safe-colour box as their own.
Advocacy Card
"This card tells people that colours can feel too big for you, and that you need a break. You can show it to your teacher or anyone. It's YOUR card." Practice together.
Reading the Child
Engaged & Curious
Continue exploring more tools at the child's pace.
Interested but Cautious
Slow down. Stay with one tool longer before moving on.
Disinterested
Wrap up warmly. Leave tools visible for independent discovery.
Distressed
Stop immediately. Return to safe-space comfort. No pressure today.
Session timing: 5–10 minutes. Follow the child's energy, not a timer.

Step 3 of 6
The Therapeutic Action
Choose the track that best fits your child's readiness. Both tracks are valid — accommodation alone is a complete intervention.
Track A — Accommodation Practice
All families. Take one real-world scenario the child regularly encounters and practice using tools BEFORE the actual event.
Script Example: "Tomorrow we're going to the store. Let's practice. Put on your glasses. Good. Here's your advocacy card in your pocket. If the colours feel too big, you can tell me 'too much' and we'll take a break in the car. Let's practice saying it: 'The colours are too much. I need a break.'"
Track B — Gradient Tolerance Building
Optional. Child-led only. Using gradient materials, invite the child to explore colour strips starting from the grey/neutral end.
"See how this strip starts really quiet? And it gets a little more colourful as it goes? Can you point to where it starts to feel too much?"
Mark that point. Celebrate it. "That's your edge right now. Every edge is different, and yours is perfect."
Duration: 5–8 minutes for the core action. Never exceed the child's tolerance. 3 good minutes are worth more than 10 forced minutes. The session's therapeutic value comes from the quality of engagement, not its length.

Step 4 of 6
Repeat & Vary
Repetition builds the neural pathways that make tool use automatic. Variation prevents satiation and keeps engagement alive. Aim for 2–3 repetitions with one small variation each time.
Role Reversal
Child plays the teacher while parent practises showing the advocacy card. Children learn deeply through teaching.
Stuffed Animal Practice
The child's toy "has colour sensitivity" — child teaches the toy how to use tools. Builds mastery through play.
Story Creation
Together create a simple story about a character who uses their Color Toolkit to navigate a colourful world with confidence.
Photo Practice
Show photos of upcoming environments — school, party venue — and plan tool use together. Reduces anticipatory anxiety.
Satiation Indicators — When to Stop
- Child starts looking away or fidgeting with tools absently
- Responses become mechanical rather than engaged
- Child says "I'm done" or "Can we stop?"
- Energy drops noticeably or any sign of rising distress
Principle: 3 good, engaged repetitions > 10 forced ones. Always end on a positive moment. Session timing: 3–5 minutes for the repetition segment.

Step 5 of 6
Reinforce & Celebrate
Reinforcement must be immediate (within 3 seconds), specific, and enthusiastic. Generic "good job" loses the association — name exactly what the child did.
"You tried on the glasses and looked around the whole room! That was brave!"
"You told me 'too much' right when you felt it — that's exactly what you'll do at school!"
"You pointed to your edge on the colour strip. That takes real self-knowledge."
Reinforcement Menu
Verbal Praise
Specific to what they did. Never generic.
Activity Reward
"After practice, let's do [preferred activity] together."
Token System
Earn stars toward a chosen reward (BCBA-designed if possible).
Natural Consequence
Successfully attending a party — the natural reward of coping well.
Safe-Colour Reward
Art time with their safe-colour supplies as celebration.
Celebrate Effort, Not Just Tolerance: "You practised using your tools" is as important as "You tolerated more colour today." Effort is always reinforcement-worthy.

Step 6 of 6
Cool-Down & Transition
After every structured session — whether accommodation practice or gradient work — provide deliberate decompression time. Skipping cool-down leaves residual sensory activation that may amplify the child's next colour encounter.
The Transition Ritual
Create a consistent signal that marks the end of structured practice and the return to regular activity. Consistency makes transitions predictable and safe for the child's nervous system.
- A specific phrase: "Color Toolkit practice is done for today. Well done."
- Putting tools back in their designated spot together
- A gentle hand squeeze or high-five as a closing marker
Why Cool-Down Matters
The visual system needs recovery time after any deliberate engagement with chromatic stimuli. A proper cool-down reduces residual activation, supports emotional regulation, and ensures the child exits the session feeling safe — not depleted.
Cool-down also provides a natural window for brief, gentle reflection: "How did that feel? What was easy? What was hard?"

Tracking Your Child's Progress
Consistent tracking turns observations into evidence — showing you what's working, what needs adjustment, and where your child is growing. Track weekly for best results.
1
Accommodation Use Log
Which tools did child use this week? (glasses / shield / advocacy card / safe colours / decompression kit). How often? Did child self-initiate, or did a parent prompt?
2
Environmental Tolerance Log
Environments successfully navigated with tools: classroom, store, party, restaurant, playground. Duration tolerated before needing a break. Recovery time after colour-intense experiences.
3
Gradient Progress
Current tolerance point on gradient strip (note date and colour level). Any shifts in problematic or safe colours over time.
4
Behavioural Indicators
Meltdown frequency in colourful environments (decreasing / stable / increasing). Self-advocacy instances. Emotional state around colour encounters (anxious / cautious / neutral / confident).

When It's Not Working — Troubleshooting
Every child's journey is different. When the expected progress doesn't appear, systematic troubleshooting identifies the cause and recalibrates the approach.
"My child refuses to wear the tinted glasses."
Try different frame styles — some children are sensitive to frames touching their face. Try clip-on options. Let the child choose the frame themselves. Start with very short wearing periods (30 seconds) with immediate reinforcement. Never force.
"The safe space doesn't seem to help."
Audit for hidden chromatic sources: natural light bringing colour from outside, coloured reflections, or lighting that isn't truly warm. Also check noise and other sensory inputs — the space must be multi-sensorially calm, not just visually neutral.
"Colour sensitivity seems to be getting worse."
Check cumulative load factors: new school decorations, seasonal changes, holiday decorations. If sensitivity genuinely worsens with new symptoms, seek professional assessment — new visual or neurological concerns may be emerging.
"School won't accommodate."
Use the advocacy template (Card 37) to formally document the need. Request a meeting with the SENCO/inclusion coordinator. Frame as an access issue, not a preference. Pinnacle can provide supportive documentation for enrolled families.
"Child copes at home but melts down at school."
Home vs. school difference is common. School adds cumulative load, fluorescent lighting, social pressure, and no safe-space access. Focus school accommodations on: seating position, lighting modification, portable shield access, scheduled visual breaks, and a quiet neutral space.
"Other family members don't believe colour sensitivity is real."
Share the neuroscience explanation (Card 3) and the WHO/UNICEF research context (Card 5). Use the family guide resource (Card 37). A brief conversation with the child's OT or paediatrician often helps sceptical family members understand.

Personalising This Technique
The Color Toolkit is not a one-size-fits-all protocol. Every child's sensitivity profile, age, and developmental needs shape how the technique is delivered.
By Severity
Mild
Safe-colour identification + basic environmental adjustments. Gradient work may progress quickly. Advocacy training empowers independent management.
Moderate
Full 9-material toolkit. Consistent accommodation across environments. Gradual tolerance building with professional OT guidance. Regular school communication.
Severe
Professional assessment mandatory. Precision-tinted lenses may be needed. Intensive environmental modification. Accommodation-first with very gradual, professionally supervised tolerance work only.
By Age
2–4 Years
Parent manages all accommodation. Sensory-friendly environment is the primary intervention. Simple language: "glasses help" and "quiet space."
5–8 Years
Begin self-advocacy training. Child learns to use tools independently. Gradient work can begin if child-led. School accommodation formally documented.
9–12 Years
Self-advocacy becomes the primary focus. Child manages their own toolkit. Peer education if child consents. Increased independence in deploying coping strategies.
By Sensory Profile
- Sensory Avoider: Prioritise accommodation and filtering tools. Gradient work very slow and gentle.
- Mixed Profile: Provide rich tactile/auditory input alongside colour-reduced visual environment.
- Colour-Specific: Adjust material selection to target specific trigger colours (commonly red, yellow, fluorescent).
Progress Arc
Week 1–2
Week 1–2: What to Expect
In weeks 1–2, you are building the foundation. You are not yet expecting the child to "toleratye" colourful environments. You are establishing safe infrastructure.
The child knows where their tools are
They've seen the glasses, touched the shield, located the safe space — even if they haven't used them yet.
The child has language for their experience
Even if it's just "too much" or pointing to the advocacy card — this is enormous. It's the beginning of self-advocacy.
Environmental modifications are in place
Bedroom is neutral, warm lighting installed, school notified, safe colours identified.
You've had 2–3 exploratory sessions
No pressure, just familiarisation with tools. Curiosity, not compliance.
Parent Emotional Preparation: These first two weeks may feel slow. You're building invisible infrastructure. The child's nervous system needs time to register that new options exist. Trust the process. If your child tolerates wearing the tinted glasses for even 10 seconds longer than last week — that is real, measurable progress. Note it in your tracker.

Progress Arc
Week 3–4
Week 3–4: Consolidation Signs
By weeks 3–4, the neural pathways encoding "tools exist" and "safe space is available" are strengthening. The shift from accommodation as a parent-managed process to child-initiated coping begins here.
Self-Initiated Tool Reach
Child picks up glasses before entering a challenging space without being prompted. This is the first major milestone.
Safe Space Use
Child goes to their neutral space when overwhelmed, rather than reaching full meltdown first. The space is working as a sensory reset button.
Advocacy Emergence
Child uses words, cards, or gestures to communicate colour overwhelm before reaching dysregulation. A profound developmental achievement.
Reduced Anticipatory Anxiety
Child is less anxious about upcoming colourful events when they know their tools are coming with them.
Safe Colour Confidence
Child freely uses safe-colour materials and may begin experimenting with adjacent hues independently.
Parent Milestone: You may notice you're more confident too. The anxiety of "will there be a meltdown?" starts to soften as you see your child developing agency. When the child is consistently using tools across familiar environments, introduce one new environment per week — always with tools, always with recovery time afterwards.

Progress Arc
Week 5–8
Week 5–8: Mastery Indicators
By weeks 5–8, accommodation has moved from structured practice to integrated daily life. Measure against where you started — the contrast will be striking.
Independent Tool Deployment
Child manages their own Color Toolkit across multiple environments — home, school, community — without parent initiation.
Effective Self-Advocacy
Child communicates needs to various adults and peers, and receives appropriate accommodation in response.
Extended Tolerance
Duration in colourful environments has measurably increased. Compare tracker data from Week 1 — the numbers tell the story.
Faster Recovery
After colour-intense experiences, child recovers faster and with less support than at the start of the programme.
Emotional Regulation
Child shows frustration or mild discomfort with colour challenges rather than full dysregulation or meltdowns.
Mastery Unlocked: When the child independently navigates a previously impossible colourful environment — birthday party, colourful classroom, busy store — using their tools and advocating for their own needs, they have achieved functional mastery of this technique.

Celebrate This Win
To the Parent Reading This:You did this. When the world told you your child was "being dramatic," you saw the truth. When others suggested forcing exposure, you chose accommodation. When it felt slow, you trusted the science. When it felt hard, you kept showing up.
They Moved From Overwhelm to Agency
Your child learned that their sensory experience is valid, manageable, and not something to be ashamed of.
They Developed Self-Knowledge
They now understand their own visual system in a way that will serve them throughout life — in school, relationships, and work.
They Can Advocate for Themselves
The ability to name a need and request accommodation is a life skill that extends far beyond colour sensitivity.
Celebrate Together
- Let your child choose a celebration activity in their comfort zone
- Create a "My Color Toolkit Hero" certificate together
- Take a photo at a place that used to be impossible — the colourful playground, the birthday party, the busy store
- Share the milestone with a supportive family member or therapist
Red Flags — When to Pause
Safety Alert
Trust your instincts. If something feels wrong, pause and ask a professional. It is always better to consult too early than too late.
⚠️ New Visual Symptoms
Child reports seeing flashing lights, spots, halos, or "things moving" that weren't present before. → Ophthalmological/neurological assessment needed immediately.
⚠️ Headaches Increasing
Colour exposure consistently triggers headaches lasting more than 30 minutes. → Paediatric migraine evaluation. Possible Irlen Syndrome assessment.
⚠️ Rapidly Expanding Sensitivity
Child who previously tolerated blues now finds all colours overwhelming. Rapid expansion may indicate an underlying condition change. → Comprehensive visual processing and neurological assessment.
⚠️ Regression After Progress
Child who achieved tool-supported coping reverts to baseline despite continued tool access. Reassess environment (new stressors?), check tool condition, consider professional re-evaluation.
⚠️ Physical Symptoms Beyond Visual
Nausea, dizziness, or loss of balance in response to colour exposure. → Medical evaluation — these suggest neurological involvement.
⚠️ Emotional Deterioration
Increasing anxiety, depression, or school refusal related to colour sensitivity despite accommodation. → Mental health support needed alongside sensory intervention.
Self-resolve
Try home strategies and monitor symptoms
Teleconsult
Speak with Pinnacle OT for guidance
In-person OT
Comprehensive sensory evaluation
Specialist referral
Optometry, then neurology if needed
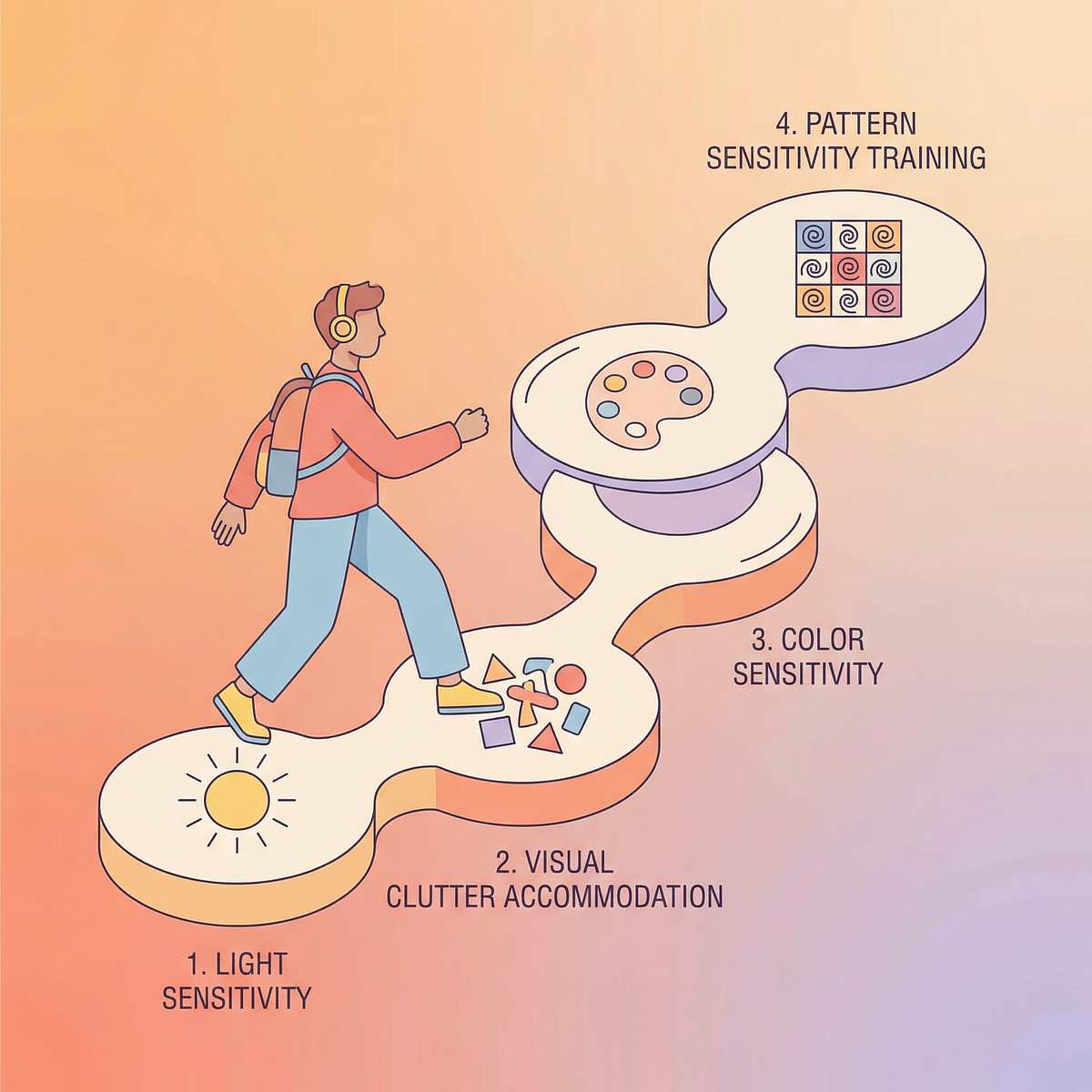
The Progression Pathway
A-071 is one step in a carefully sequenced visual sensory processing programme. Understanding where you came from and where you're heading gives the whole journey context and direction.
1
A-069
Bright Light Sensitivity Materials — light sensitivity tools and accommodation. Prerequisite.
2
A-070
Visual Clutter Accommodation — visual environment simplification. Prerequisite.
3
★ A-071
Color Sensitivity Accommodation & Coping Materials. YOU ARE HERE.
4
A-072
Pattern Sensitivity Materials — similar accommodation approach applied to visual pattern overwhelm. Next step.
If Child Mastered Accommodation
→ A-072: Pattern Sensitivity — accommodation approach applied to visual pattern overwhelm.
→ A-073: Visual Overwhelm & Eye Contact — visual processing support for social engagement.
For Broader Environmental Tolerance
→ A-075: Busy Stores/Environments — multi-sensory environment coping strategies.
Long-Term Goal: Full participation in age-appropriate activities across all environments with self-managed accommodation — sensory confidence that carries into adolescence and adulthood.

Related Techniques in This Domain
If you purchased materials for A-071, you already have key items for 4 of these 6 related techniques. The Pinnacle Canon Material system ensures your investment serves multiple therapeutic goals.
Technique | Key Materials | Materials You May Already Own | Difficulty | |
A-069: Bright Light Sensitivity | Sunglasses, dimmer switches, blackout curtains | ✅ Tinted glasses, lighting tools overlap | Intro | |
A-070: Visual Clutter Accommodation | Organizers, visual barriers, simplified spaces | ✅ Neutral spaces, portable shields overlap | Intro | |
A-072: Pattern Sensitivity Materials | Pattern-blocking tools, simplified visuals | ✅ Tinted glasses, decompression tools overlap | Core | |
A-073: Visual Overwhelm & Eye Contact | Visual schedules, gaze scaffolds | ✅ Portable shields, advocacy tools overlap | Core | |
A-075: Busy Environment Coping | Multi-sensory coping kits, preparation tools | ✅ Decompression kit, advocacy cards overlap | Core | |
A-079: Screen Time Visual Management | Blue light filters, timer tools, break protocols | ✅ Tinted glasses, lighting tools overlap | Advanced |
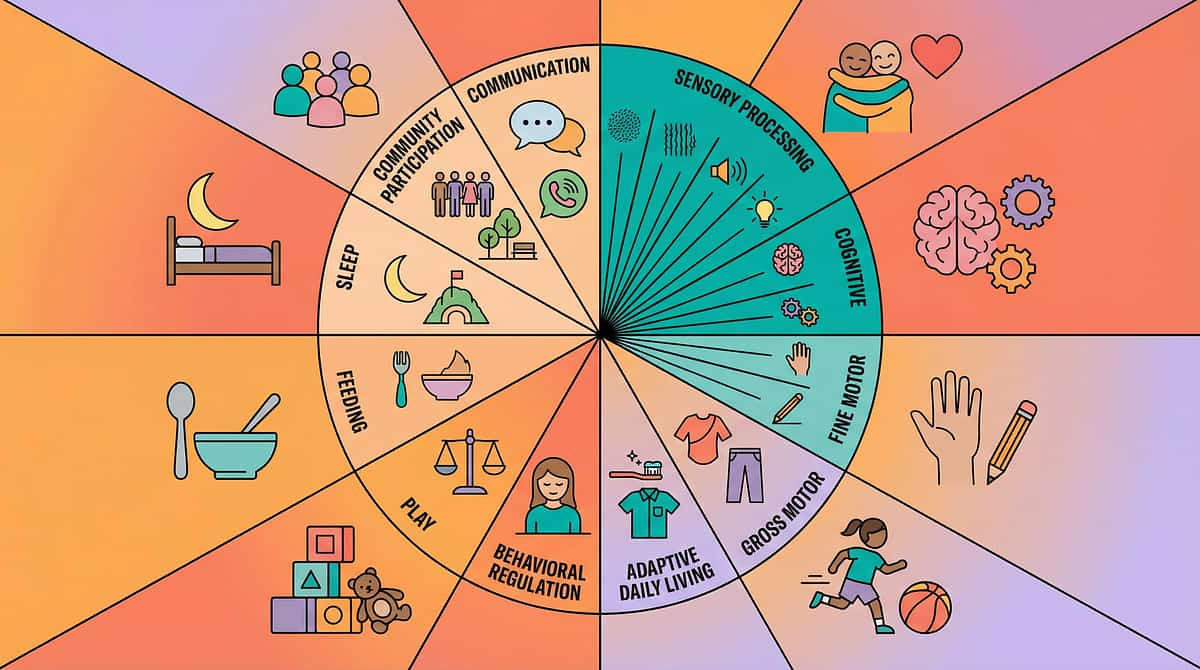
Your Child's Full Developmental Map
Color sensitivity accommodation addresses sensory processing, but it also touches adaptive skills, communication, social participation, and emotional regulation. This technique is one piece of a larger, integrated plan.
★ Domain A: Sensory Processing
This technique lives here — but its impact radiates outward to touch almost every other domain in your child's developmental profile.
Connected to Every Domain
When connected to GPT-OS®, this technique integrates with your child's full developmental profile across all 12 domains — showing how progress in sensory processing supports communication, social participation, academic function, and emotional regulation simultaneously.

Family Stories — You Are Not the First
Behind every data point is a family who found a way through. These stories are shared with care — names changed, outcomes illustrative; individual results vary.
Priya, Mother of Aanya (Age 5) — Hyderabad
"Birthday parties were impossible. Aanya would see the balloons and immediately melt down — she said the colours were 'attacking' her. We started with tinted glasses and neutral safe spaces. We found her safe colours — soft blues and greens — and built from there. Her school agreed to seat her by the window, away from rainbow decorations. Now she can attend parties with her glasses, takes breaks when needed, and even wore a light purple dress to her friend's birthday last month. The world is still colourful, but she has tools to navigate it."
Raj & Meena, Parents of Arjun (Age 8) — Bangalore
"We spent two years thinking Arjun was just 'fussy.' When his OT explained colour sensitivity, everything clicked — why he only wore grey, why he couldn't concentrate in his decorated classroom. The Color Toolkit changed our family. We created his neutral bedroom, got him amber-tinted glasses, and taught him to say 'I need a visual break.' Last month he won an award for academic improvement — because he can finally concentrate without fighting his own visual system."
Lakshmi, Grandmother of Devi (Age 4) — Rural Andhra Pradesh
"In our village, nobody understood why Devi screamed near the red temple decorations. The helpline [9100 181 181] connected us to a therapist who explained it on the phone. We couldn't buy special glasses, but we made a cardboard shield, found her safe colours (blue and white), and created a calm corner with a white sheet. Simple things. Free things. But they changed everything."

Join Your Community
Parenting a colour-sensitive child can feel isolating — especially when those around you don't understand. Your community of fellow families does. Peer support demonstrably improves intervention outcomes and reduces parental stress.
WhatsApp Community
Join the Pinnacle Sensory Support WhatsApp Community — real-time peer support, shared strategies, and celebration of milestones from families who have walked this path.
Parent Forum
The Pinnacle Parent Forum — Visual Sensory Processing section — connects you with families navigating colour sensitivity, pattern sensitivity, light sensitivity, and related challenges.
Local Meetups
Find parent meetups near you — in-person connection with families who understand. Search by city through the Pinnacle community platform.
Peer Mentoring
Connect with an experienced parent who has navigated colour sensitivity accommodation for their child. Request a peer mentor match through the helpline: 9100 181 181.

Your Professional Support Team
Home + Clinic = Maximum Impact. Environmental accommodation provides the daily foundation. Professional assessment and therapy provide the clinical precision. Together, they deliver outcomes neither achieves alone.
Therapist Matching for Colour Sensitivity
Primary: Occupational Therapist with Sensory Integration specialisation
Supporting: Developmental Optometrist / Vision Specialist
If Irlen Syndrome suspected: Certified Irlen Screener
Remote Families
Full sensory processing consultation, environmental audit guidance, and material selection support delivered via video call. Available in 16+ languages across India and 70+ countries.
Find Your Nearest Pinnacle Centre
70+ centres across India offer in-person OT sensory evaluation, developmental optometry referral pathways, and multi-disciplinary team coordination for colour-sensitive children.
Or Start by Phone
The FREE National Autism Helpline operates 24×7 in 16+ languages. Trained counsellors will guide you through your first steps, answer questions about colour sensitivity, and help you access the right professional support for your child's needs.
The Research Library
The evidence base for colour sensitivity accommodation spans systematic reviews, randomised controlled trials, international clinical guidelines, and specialist research from multiple therapeutic disciplines.
PRISMA Systematic Review (Children, 2024)
16 articles, 2013–2023. Sensory integration confirmed as evidence-based practice for ASD. Environmental modification is first-line. → PMC11506176
Meta-Analysis (World J Clin Cases, 2024)
24 studies. Sensory integration therapy effectively promotes adaptive behaviour and sensory processing. → PMC10955541
Padmanabha et al. (Indian J Pediatr, 2019)
Home-based sensory interventions demonstrated significant outcomes in Indian paediatric populations. → DOI: 10.1007/s12098-018-2747-4
WHO Nurturing Care Framework (2018/2023)
Equity-focused, multi-disciplinary approach to early childhood development intervention across 54+ countries. → nurturing-care.org

How GPT-OS® Uses Your Data
Privacy Protected
Encrypted
Your Data. Your Control.
Six-step Data Flow
Parent records session
Logs Color Toolkit session
Re-measurement confirms
Progress validated and recorded
TherapeuticAI refines
Personalised recommendations tuned
AbilityScore updates
Adjusts measured ability metrics
Sensory processing index
GPT-OS analyzes incoming data
Daily programme adjusts
EverydayTherapy updates guidance
What GPT-OS® Learns From Your Data
- Which tint colours are most effective for your child's specific wavelength sensitivities
- Optimal session duration and frequency for your child's tolerance-building pace
- Environmental factors that most impact your child's visual sensory load
- Progression patterns that predict when your child is ready for next-level techniques
Privacy Assurance
- Data encrypted under Indian IT Act (2000) and international data protection standards
- Used solely for your child's therapeutic optimisation and anonymised population research
- You control your data: view, export, or delete at any time through your GPT-OS® dashboard
- No data shared with third parties without explicit consent
Population Impact: Your anonymised data helps improve recommendations for every child with colour sensitivity worldwide.

Watch the Reel
Sensory Solutions Series
Episode 71
Reel A-071 — 9 Materials That Help With Color Sensitivity
Watch the therapist-presented overview of all 9 materials, see them in use with children, and hear the clinical rationale — all in under 90 seconds. Presented by a Pinnacle Blooms Certified Paediatric Occupational Therapist with Sensory Integration specialisation.
This Reel is part of the Pinnacle Blooms 999 Sensory Solutions Series — the most comprehensive video library of evidence-based paediatric therapy material guidance available anywhere in the world.
Video modelling is classified as an evidence-based practice for autism (NCAEP, 2020). Multi-modal learning improves parent skill acquisition significantly over text-only formats.

Share This With Your Family
Consistency across caregivers multiplies impact. If only one parent uses the Color Toolkit, your child has support 50% of the time. When every caregiver understands and implements accommodation, the child's entire world becomes navigable.
The Grandparent Version"Your grandchild's brain processes colours more intensely than most people. Bright colours feel overwhelming — like very loud noise feels to you. When they cover their eyes or get upset in colourful places, it's not dramatics — it's their nervous system saying 'too much.' Help them by keeping things calm, letting them wear their special glasses, and giving them breaks in quiet spaces."
Share This Page
Send via WhatsApp, email, or copy the direct link to share with grandparents, teachers, other caregivers, and extended family members who interact with your child regularly.
Download Resources
Family Guide (1-page PDF) • Simplified Grandparent Version • Teacher Communication Template • School Accommodation Request Letter — all available to download and share immediately.

Frequently Asked Questions
The questions most parents ask — answered clearly, without jargon.
Is colour sensitivity the same as Irlen Syndrome?
Not always. Irlen Syndrome (Scotopic Sensitivity) is a specific visual processing condition that responds to precision-tinted lenses. Colour sensitivity can exist independently as part of broader sensory processing differences. If your child has significant reading difficulty alongside colour sensitivity, Irlen screening is recommended.
Will my child always have colour sensitivity?
Some children's sensitivity reduces over time with accommodation, neural maturation, and gradual tolerance building. Others maintain lifelong sensitivity they learn to manage independently. Both outcomes are normal. The goal is functional participation, not elimination of sensitivity.
Can colour sensitivity be "cured"?
Colour sensitivity is a neurological processing difference, not a disease. The accommodation-first approach equips the child for lifelong management — similar to how glasses manage vision differences. Some children expand their tolerance significantly; others use tools indefinitely. Both represent success.
My child is only 2. Is it too early to start?
Environmental modification (neutral safe space, warm lighting, reduced chromatic load) can begin at any age. Structured tool introduction and self-advocacy training are most effective from age 3–4 onward, when the child can participate actively.
How do I get my child's school to accommodate?
Use the School Accommodation Request Letter template (Card 37). Document specific accommodations needed. Request a meeting with the class teacher and inclusion coordinator. Provide clinical documentation where available. Pinnacle can provide supportive letters for enrolled families.
Are tinted glasses safe for children?
Yes, when properly fitted and with UV protection. Basic tinted glasses are non-prescription and carry no risk. Precision-tinted lenses should be prescribed by a qualified professional. Ensure child-sized frames for safety and comfort. Not for use whilst cycling or in situations requiring full field vision.
What if my child's trigger colours are everywhere (like red and yellow)?
Red and yellow are among the most commonly reported trigger colours. Focus on filtering (tinted glasses reduce intensity of all colours), environmental modification of controllable spaces, portable shields for uncontrollable spaces, and decompression after exposure. With tools, even ubiquitous colours become manageable.
Does insurance cover sensory processing therapy?
Coverage varies by provider and region. In India, the Pinnacle Blooms FREE National Autism Helpline (9100 181 181) can guide you through funding options, insurance navigation, and government scheme eligibility.

Your Next Step — Start Now
You've read the science. You've seen the evidence. You have the tools. Now: Act.
🟢 Primary Action
Launch a GPT-OS® guided session for A-071 and begin your child's Color Toolkit journey today — with personalised, step-by-step guidance powered by 20M+ therapy sessions of clinical intelligence.
🔵 Secondary Action
Book a consultation with a Pinnacle Sensory Specialist — in-person or via teleconsultation — for a comprehensive sensory assessment, environmental audit, and personalised material selection guidance.
🟣 Tertiary Action
Explore the next technique in the progression pathway: A-072 Pattern Sensitivity Materials — applying the same evidence-based accommodation approach to visual pattern overwhelm.
📞FREE National Autism Helpline: 9100 181 181 — 16+ languages, available 24×7
Validated by the Pinnacle Blooms Network® Consortium
OT • SLP • BCBA • Special Education • NeuroDevelopmental Pediatrics • Clinical Research
Preview of 9 materials that help with color sensitivity Therapy Material
Below is a visual preview of 9 materials that help with color sensitivity therapy material. The pages shown help educators, therapists, and caregivers understand the structure and content of the resource before use. Materials should be used under appropriate professional guidance.




















Share this resource
Help others discover thisLink copied!

The Pinnacle Promise
From Fear to Mastery. One Technique at a Time.
You arrived on this page worried about a child who covers her eyes in colourful rooms. You leave with a 9-material toolkit, evidence-based protocols, professional support pathways, and a community that understands.
Your child's visual system works differently. And now, your family has the infrastructure to navigate that difference with confidence, with tools, and with the full support of a consortium of experts who have dedicated their careers to exactly this.
Exclusive 1:1 Sessions
Clinical intelligence powering every recommendation
Measured Improvement
Across families served by the Pinnacle Blooms Network
Centres Worldwide
Across India and 70+ countries served globally
Pinnacle Blooms Network® Mission: Transforming every home into a 24×7, evidence-based, multi-disciplinary, integrated therapeutic centre for children with developmental differences. Powered by GPT-OS®.
This content is educational and does not replace assessment by a licensed occupational therapist, developmental optometrist, or healthcare provider. Persistent colour sensitivity should be evaluated within a comprehensive sensory processing assessment. Individual results vary. Statistics represent aggregate outcomes across the Pinnacle Blooms Network.
CIN: U74999TG2016PTC113063 | DPIIT: DIPP8651 | MSME: TS20F0009606 | GSTIN: 36AAGCB9722P1Z2
© 2026 Pinnacle Blooms Network®, unit of Bharath Healthcare Laboratories Pvt. Ltd. All rights reserved.
techniques.pinnacleblooms.org | pinnacleblooms.org | 9100 181 181
techniques.pinnacleblooms.org | pinnacleblooms.org | 9100 181 181
