
"She bounces on the couch. She bounces on her bed. She bounces while eating breakfast. And if there's nothing to bounce on — she jumps."
You've tried telling her to stop. You've tried consequences. You've tried fidget toys. Nothing works for more than thirty seconds. Because this isn't about willpower. This is her nervous system speaking.

You Are Not Alone
Thousands of Families Have Been Exactly Where You Are
Across 70+ Pinnacle Blooms centres and 20 million+ therapy sessions, proprioceptive-vestibular seeking — the clinical term for what you're seeing — is among the most common sensory profiles in children with autism and sensory processing differences.
68%
Sensory-Seeking in ASD
Of children with ASD demonstrate sensory-seeking behaviours (Baranek et al., 2006)
1 in 6
Daily Functioning Impact
Children experience sensory processing challenges significant enough to affect daily life (Ben-Sasson et al., 2009)
83%
Parent-Reported Improvement
Report improvement when appropriate sensory outlets replace suppression strategies (Pinnacle Blooms, 2024)
"I finally took her to the paediatrician, who observed her bouncing in the exam room the entire visit and said it looks like 'sensory seeking behaviour' and that she probably needs 'proprioceptive input.' But I don't really understand what that means or what to actually do about it in practical terms." — Parent, Pinnacle Blooms Network
If your child bounces constantly — on chairs, on couches, in line, during dinner — you are reading exactly the right page. This page was built for you.
The Science
The Bouncing Isn't Defiance. It's Neurology.
Your child's brain processes sensory information differently. Two intertwined systems drive the bouncing need — and understanding them changes everything about how you respond.
Proprioceptive System
Every time your child lands from a bounce, their joints compress and muscles engage. This sends signals to the brain: "I am here. I am grounded. I am organised." Children who seek bouncing have higher proprioceptive thresholds — they need more of this input to feel regulated than neurotypical peers.
Vestibular System
The up-and-down rhythm of bouncing provides vestibular input — the brain's movement GPS. Rhythmic, predictable vestibular input is profoundly organising. The bounce-land-bounce-land pattern is one of the most regulating movement patterns available to the nervous system.
The Combined Effect
Bouncing uniquely combines proprioceptive (landing impact) + vestibular (vertical movement) input in a rhythmic pattern. This is why your child doesn't just fidget — they specifically bounce. Their nervous system has identified the most efficient way to get what it needs.
Key Reframe: Your child isn't choosing to be disruptive. Their body is demanding movement that provides proprioceptive and vestibular input. A child with a "full tank" of this input is often calmer, more focused, and better able to sit still when required.
Research: Sensory integration framework — Ayres (1972, 2005); Proprioceptive-vestibular interaction — Dunn's Model (1997); Neural threshold theory — Journal of Autism and Developmental Disorders | PubMed: PMC11506176

Developmental Context
When Bouncing Seeking Appears — And What It Means at Each Stage
Bouncing seeking typically becomes noticeable between ages 2–4 and may persist through childhood if the underlying sensory need isn't met. This isn't a phase children "grow out of" — it's a neurological profile that can be supported.
1
Ages 2–3
High movement drive is normal. Bouncing seeking beyond typical becomes apparent when intensity, duration, and compulsivity exceed peers. Inability to calm from bouncing is a key indicator.
2
Ages 4–6
School entry amplifies impact. Classroom expectations for sitting conflict directly with the bouncing need. This is often when parents first hear "your child can't sit still" from teachers.
3
Ages 7–9
Social impact emerges. Peers begin to notice. The child may feel frustrated by their own inability to stop bouncing. Self-awareness grows alongside the need.
4
Ages 10–12
Compensatory strategies develop. Without intervention, children may suppress bouncing in public but release it explosively at home. With appropriate outlets, self-management becomes possible.
WHO Nurturing Care Framework (2018) | UNICEF Early Childhood Development Indicators | PMC9978394

Evidence Grade: Level I–II
What the Research Says — Systematic Reviews, Meta-Analyses, and RCTs
This protocol is not built on clinical opinion alone. It is grounded in the strongest available evidence — peer-reviewed, consortium-validated, and home-applicable.
Systematic Review — Children (2024)
A PRISMA model review of 16 articles (2013–2023) confirms sensory integration intervention meets criteria for evidence-based practice for children with ASD. Outcomes include improved sensory processing, social skills, adaptive behaviour, and motor skills. → PubMed: PMC11506176
Meta-Analysis — World Journal of Clinical Cases (2024)
Across 24 controlled studies, sensory integration therapy effectively promoted social interaction, adaptive behaviour, sensory processing, and motor development. 40-minute sessions showed maximum effectiveness. → PubMed: PMC10955541
Indian RCT — Indian Journal of Pediatrics (2019)
Home-based sensory interventions demonstrated significant outcomes in Indian paediatric populations, establishing the evidence base for parent-administered sensory protocols. → DOI: 10.1007/s12098-018-2747-4 (Padmanabha et al.)
WHO CCD Implementation (2023)
The Care for Child Development Package implemented across 54 low- and middle-income countries demonstrates that caregiver-delivered developmental interventions are effective and scalable. → PubMed: PMC9978394
✅ Clinically validated | ✅ Home-applicable | ✅ Parent-proven | Validated by the Pinnacle Blooms Consortium: OT • SLP • BCBA • SpEd • NeuroDevelopmental Pediatrics • CRO
This content is educational and informational. It does not replace assessment by a licensed occupational therapist or healthcare provider.

Technique A-089
Structured Proprioceptive-Vestibular Bouncing Protocol
"The Bouncing Solution" — Channelling Your Child's Bouncing Need Into Appropriate Outlets
A structured sensory intervention that provides rhythmic proprioceptive (joint compression through landing) and vestibular (vertical movement) input through designated bouncing outlets. Rather than suppressing the bouncing, this protocol channels it through appropriate materials at scheduled intervals — reducing inappropriate bouncing by meeting the nervous system's legitimate input needs.
1
Domain
A — Sensory Processing / Proprioception / Vestibular / Self-Regulation
2
Age Range
2–12 years
3
Session Duration
10–20 minutes (home); scheduled micro-breaks throughout the day
4
Frequency
Daily sensory diet; 3–5 structured sessions per day minimum for moderate–intense seekers
5
Setting
Home + School + Therapy + Outdoor
Canon Materials: Mini Trampoline / Rebounder • Wobble Cushions / Seating Discs • Compression Vest / Body Sock • Balance & Vestibular Equipment

Who Uses This Technique
This Technique Crosses Therapy Boundaries — Because the Brain Doesn't Organise by Therapy Type
Occupational Therapy (OT) — Primary Lead
OTs specialise in sensory integration and are the primary designers of sensory diets. They assess the child's sensory profile, determine the intensity and frequency of proprioceptive-vestibular input needed, and prescribe specific materials and schedules. The bouncing protocol sits at the core of OT-designed sensory intervention.
Applied Behavior Analysis (ABA) — Secondary
BCBAs integrate bouncing as a self-regulation tool within behavioural programming. Bouncing breaks become part of antecedent strategies — scheduled sensory input that prevents dysregulation before it occurs. ABA frameworks provide the reinforcement scheduling that maintains engagement with appropriate outlets.
Speech-Language Pathology (SLP) — Secondary
SLPs recognise that a dysregulated child cannot participate in language therapy. Pre-session bouncing protocols prepare the child's nervous system for focused attention. Rhythmic bouncing also supports breath control and vocal regulation.
Special Education + NeuroDev Paediatrics
Special educators implement classroom accommodations (wobble cushions, bouncy bands). NeuroDevelopmental Paediatricians differentiate sensory seeking from ADHD and co-occurring conditions, ensuring the correct intervention pathway.
Reference: Adapted UNICEF/WHO Nurturing Care Framework for SLPs (2022) — DOI: 10.1080/17549507.2022.2141327
What This Targets
Precision Targeting — This Isn't a Random Activity
The core skill targeted is the child's ability to achieve and maintain a regulated nervous system state through appropriate sensory input. Observable primary indicators include decreased inappropriate bouncing on furniture, ability to sit for increasing durations, and reduced sensory-seeking intensity after structured bouncing sessions.
Bouncing on furniture decreases
Child uses designated outlets voluntarily
Requests bouncing breaks appropriately
Attention span increases after bouncing sessions
Can inhibit bouncing for reasonable periods when needed
Meta-analysis (World J Clin Cases, 2024): SI therapy effectively promoted social skills, adaptive behaviour, sensory processing, and motor skills across 24 studies. PMC10955541

Materials 1–3 of 9
9 Materials That Channel the Bounce
Material 1: Mini Indoor Trampoline / Rebounder
The direct answer to bouncing needs. Rhythmic vertical movement that fills the proprioceptive-vestibular tank through an appropriate outlet. The trampoline is the flagship tool of this protocol — it provides maximum combined proprioceptive and vestibular input in a single piece of equipment.
💡Pinnacle Recommends: Trampoline with safety handle bar for children under 8. Ensures balance support and reduces fall risk during therapeutic bouncing sessions.
Price range: ₹2,000–8,000 | Buy on Amazon.in
Material 2: Bouncy Seat Cushions / Wobble Cushions
Micro-bouncing while seated — the classroom-compatible solution. Wobble cushions allow the child to receive continuous proprioceptive and micro-vestibular input while appearing to sit still. This is the single most important school accommodation tool in this protocol.
Price range: ₹800–2,500 | Buy on Amazon.in
Material 3: Hippity Hop Balls / Hopper Balls
Intense full-body bouncing with active muscle engagement. The child sits on the ball and bounces using leg drive, combining sitting-bouncing proprioceptive input. Excellent for post-school decompression sessions and high-intensity seeking moments.
Price range: ₹500–1,500 | Buy on Amazon.in

Materials 4–6 of 9
9 Materials — Continued
Material 4: Pogo Sticks / Foam Pogo Jumpers
Controlled bouncing that builds coordination while filling the sensory need. Foam pogo jumpers are safe for indoor use and are appropriate for children as young as 3. They add a motor planning component — the child must balance while bouncing — making each session doubly therapeutic.
Price range: ₹600–3,000 | Buy on Amazon.in | Product ref: CRIYALE Kids Pogo Jumper
Material 5: Body Sock / Compression Wear
Passive proprioceptive input through deep pressure — for when bouncing isn't possible. Compression clothing provides ongoing gentle pressure against the body, offering continuous low-level proprioceptive input that maintains regulation between active bouncing sessions. Ideal for school, meals, and travel.
Price range: ₹800–4,000 | Buy on Amazon.in
Material 6: Jump Rope & Jump Games
Rhythmic bouncing anywhere — portable, inexpensive, and coordination-building. Jump rope requires no equipment beyond the rope itself, making it the most accessible tool in the protocol. The rhythmic nature of skipping makes it particularly regulating.
Price range: ₹100–800

Materials 7–9 of 9
9 Materials — Final Three
Material 7: Bouncy Bands / Chair Leg Bands
Leg bouncing with purpose — proprioceptive input under the desk. A resistance band stretched between the front two legs of a school or home chair allows the child to push and bounce their feet against it continuously and silently. One of the most classroom-invisible tools available.
Price range: ₹400–1,200
Material 8: Sensory Diet Activity Cards
Structured bouncing breaks throughout the day — proactive regulation. Cards specify the type, duration, and sequence of bouncing activities, giving the child (and caregivers, teachers, and grandparents) a clear, consistent schedule. Structure makes the sensory diet sustainable.
Price range: ₹200–1,000
Material 9: Crash Pad / Landing Mats
Jump and land with safe impact — intense proprioceptive input for deep seekers. The crash pad allows children who need maximum proprioceptive input (intense seekers) to jump from a height and land with deep joint compression. This is the highest-intensity tool in the protocol and should be reserved for children whose need is not met by trampolines alone.
Price range: ₹3,000–15,000
🛒Essential Starter Kit (3 items): Mini trampoline with handle + Wobble cushion for desk + Foam pogo jumper = ₹3,400–13,500 — covers home, school, and active play needs.

DIY & Substitutes
Every Family Can Start Today — Regardless of Budget
The WHO/UNICEF Equity Principle ensures every parent, regardless of economic status, can execute this technique TODAY with household items. Not every family can order from Amazon — and this protocol was designed with that reality in mind.
Material | Zero-Cost / DIY Alternative | Why It Works | |
Mini Trampoline | Old mattress on the floor; jumping jacks; dance jumping | Same vertical rhythmic movement pattern | |
Wobble Cushion | Partially deflated beach ball on chair; folded towel | Creates unstable sitting surface requiring micro-balance adjustments | |
Hopper Ball | Bouncing while holding parent's hands; bouncing on bed with supervision | Provides combined sitting-bouncing proprioceptive input | |
Pogo Jumper | Jumping over low obstacles in rhythm; counting-jump games | Structured rhythmic jumping with motor planning demands | |
Compression Wear | Tight-fitting bike shorts + tight undershirt; DIY body sock from stretchy fabric tube | Provides ongoing gentle compression against the body | |
Jump Rope | Any rope; jumping games drawn on floor; hopscotch with chalk | Rhythmic vertical movement available anywhere | |
Chair Bands | Exercise band or thick rubber band around chair legs | Provides resistance for feet to push against | |
Sensory Diet Cards | Homemade cards: "50 jumps," "bounce 2 minutes," "pogo 20 times" | Structures and schedules the sensory input | |
Crash Pad | Stack of couch cushions; pile of pillows; thick blanket bundle on floor | Soft landing surface for jump-and-crash proprioceptive input |
⚠️When the clinical-grade material is non-negotiable: For intense sensory seekers, DIY alternatives may not provide sufficient input intensity. If the child's sensory need is not met by household substitutes, the clinical-grade trampoline or crash pad may be a necessary investment.
Reference: WHO Nurturing Care Framework (2018): context-specific, equity-focused interventions. CCD Package implemented across 54 LMICs. PMC9978394

Safety First
Safety Gate — Read This Before Your First Session
1
🔴 RED — DO NOT PROCEED IF:
- The child has a history of seizures triggered by rhythmic movement (consult neurologist first)
- There is an active orthopaedic injury to legs, ankles, knees, hips, or spine
- The child is post-surgical without physician clearance for jumping activities
- The child has diagnosed hypermobility syndrome / Ehlers-Danlos without OT guidance
- Medical conditions affecting balance, bone density, or cardiovascular function exist
2
🟡 AMBER — PROCEED WITH PROFESSIONAL GUIDANCE IF:
- The child has a diagnosed seizure disorder (even if well-controlled)
- Significant vestibular hypersensitivity coexists with vestibular seeking (mixed sensory profile)
- The child shows signs of escalation rather than regulation from bouncing
- There are behavioural concerns about safety awareness during high-energy activities
- The child is under 2 years of age
3
🟢 GREEN — PROCEED WITH STANDARD SUPERVISION:
- Ensure bouncing surface is appropriate for the child's weight and age
- Clear space: minimum 6 feet from walls, furniture, and sharp edges
- One bouncer at a time on trampolines
- Check ceiling clearance for standing jumps
- Inspect equipment regularly for wear, loose screws, torn fabric
- Weighted compression items: maximum 5–10% of child's body weight
🛑STOP IMMEDIATELY IF: The child reports pain in any joint • Dizziness or nausea occurs • Behaviour escalates rather than regulates • Loss of coordination beyond expected • Child is unable to stop bouncing even after satiation (requires professional assessment)
Reference: Home-based sensory intervention safety protocols — Padmanabha et al., Indian J Pediatr, 2019 | Pinnacle Blooms clinical safety protocols

Space Setup
Transform Your Home Into a Sensory-Smart Space — In 30 Minutes
1
The Bouncing Zone (Primary)
Choose one area as the designated bouncing zone — flat, level surface; minimum 8×8 feet clear space; away from glass, sharp furniture, and stairs; good lighting; non-slip flooring or mat beneath equipment. This is where the trampoline, crash pad, and hopper ball live permanently.
2
The Seated Regulation Zone (Secondary)
The homework desk, dining table, or any seated activity area. Wobble cushion sits on the chair; bouncy bands attach to chair legs. Requirements: stable chair on level surface; cushion properly inflated for the child's weight.
3
The Portable Kit (On-the-go)
A small bag containing: foam pogo jumper, jump rope, one sensory diet card set, and compression undershirt. This kit travels to school, grandparents' house, restaurants, and any setting where bouncing needs may arise.
4
Sensory Diet Schedule (Visible)
Post the sensory diet schedule on the refrigerator and share with school: morning bounce (before school), homework bounce (before sitting), dinner bounce (before mealtime), free bounce (as needed), bedtime compression (wind-down). Start with every 60–90 minutes and adjust.

Step 1 of 6
Readiness Check — Is Your Child Ready Right Now?
The 60-Second Check Before Every Session
Child State ✅
- Alert and awake (not drowsy, not post-nap groggy)
- Not in active distress or meltdown — regulate first, then provide input
- Fed within the last 2 hours (not hungry; not immediately post-meal for crash activities)
- No recent injury to legs, ankles, or back
- Wearing appropriate clothing (not restrictive; shoes off for trampoline)
- No signs of illness (fever, nausea, headache)
Environment ✅
- Bouncing zone is clear and safe
- Equipment is assembled and inspected
- Adult supervisor is present and attentive
- Other children/pets are clear of the bouncing area
- Timer or phone is ready for session tracking
Parent State ✅
- You are calm and present (your regulation co-regulates your child)
- You have 15–20 minutes without interruption
- You understand today's session plan
- You have the tracking sheet ready
If any red check: Pause. Address the barrier first. A calm start leads to a regulated session. The technique works best when child, environment, and parent are all ready.

Step 2 of 6
The Warm-Up Invitation — Child-Led Entry
Duration: 2–3 Minutes
❌ Don't Command
"Time to bounce." — This frames the activity as a directive, reducing the child's ownership and buy-in.
✅ Do Invite
"Your trampoline is ready. Want to come bounce with me?" — Warm, child-led framing increases engagement and gives the child agency over their own regulation.
For younger children (2–5): Begin bouncing yourself or demonstrate with a stuffed animal. "The trampoline misses you! Let's see how high Teddy can bounce!"
For older children (6–12): "I know your body needs some bounce time before homework. The trampoline's set up — 5 minutes before we start?"
Critical principle: The bouncing is not punishment or a chore. It is the child's right to sensory input. Frame it as a positive: "Your body needs this, and I'm making sure you get it."
Child-led entry: Let the child choose which bouncing material to start with. Choice increases buy-in and gives the child ownership of their own regulation.
If the child resists: Check readiness factors, ensure the invitation is warm not directive, and consider starting with compression wear before transitioning to bouncing.
Step 3 of 6
Building the Rhythm — The Therapeutic Core
Duration: 3–5 Minutes
Once the child is bouncing freely, begin to add rhythm. The rhythmic pattern is what makes bouncing therapeutic rather than random. Structured, predictable bouncing is more organising to the nervous system than free-form jumping.
1
Counting Bounces
"Let's count to 20 together! One... two... three..." Counting adds cognitive engagement to the sensory input, doubling the regulatory benefit and supporting language development simultaneously.
2
Rhythmic Music or Clapping
Clap a steady beat for the child to bounce to. Play a familiar song. External rhythm entrains the child's internal rhythm — connecting the movement to the brain's timing circuits.
3
Follow the Leader — Speed Modulation
"Can you bounce fast? Now slow... now fast... now sloooow..." Speed modulation teaches the child that they can control the intensity — the beginning of self-regulation awareness.
Why rhythm matters: Rhythmic, predictable input activates the cerebellum's timing circuits, which connect directly to attentional systems. This is why structured bouncing improves focus, and random jumping sometimes doesn't.
Watch for the "zone" — the calm, focused expression that indicates the nervous system is receiving and processing the input. This is the look you're aiming for.
Reference: Rhythmic sensory input and cerebellar timing — neuroscience of sensory integration literature | PMC10955541

Step 4 of 6 — Trampoline Protocol
The Core Bouncing Protocol — Trampoline
Duration: 5–10 Minutes Total
1
Free Bouncing
50 bounces (counting together) on mini trampoline with handle. Unstructured entry allows the child to self-direct their initial input before adding guided structure.
2
Directed Bouncing
"Bounce and touch your head... bounce and clap... bounce and reach for the sky." Adds motor planning and cognitive engagement.
3
Heavy Landing Practice
"Bounce and LAND like a rock — heavy, heavy feet." Maximises proprioceptive input through intentional joint compression on landing — the most regulating part of the bounce cycle.
4
Rhythm Shift
10 fast bounces, 5 slow bounces, 10 fast, 5 slow. Teaches the child nervous system modulation — the ability to move between alert and calm states on demand.
5
Cool-Down Bouncing
Progressively smaller bounces until standing still. This gradual deceleration is critical — it prevents abrupt sensory cut-off and prepares the transition to the next activity.

Step 4 of 6 — Hopper & Pogo Protocols
The Core Bouncing Protocol — Hopper Ball & Pogo Jumper
Hopper Ball Protocol
- Hop across the room and back — 3 lengths
- Hopper races with parent (if two hoppers available)
- "Hop to the target" — bounce to touch items placed around the room
- Speed variations: slow careful hops → fast power hops → slow again
The hopper ball combines sitting posture with full-body bounce, making it ideal for children who need proprioceptive input from both the sitting position and the impact of landing.
Pogo Jumper Protocol
- 30 consecutive jumps (counting together)
- "Jump to the beat" with clapping or music
- Balancing challenge: can you pogo for 10 seconds without falling?
- Creative challenges: pogo with eyes closed (foam pogo only, supervised)
Foam pogo jumpers build balance and motor planning alongside proprioceptive-vestibular input. The coordination challenge adds an extra layer of neural engagement, enhancing the regulatory benefit.
Child Response Spectrum:Ideal — calm-alert, rhythmic, showing "the zone" expression. Acceptable — energetic, enthusiastic, slightly unstructured but participating. Concerning — escalating energy, increasing agitation, loss of coordination, or distress. Stop and assess if concerning signs appear.

Step 4 of 6 — Wobble Cushion Protocol
The Wobble Cushion Protocol — Seated Regulation at School and Home
The wobble cushion protocol is designed for seated activities — homework, meals, classroom instruction — where active bouncing is not possible. It delivers continuous micro-proprioceptive and micro-vestibular input while the child appears to be sitting still.
1
Place Cushion Before Activity
Position the wobble cushion on the chair before homework or dinner begins. The child should be in place before the seated demand is introduced — not mid-task.
2
Allow Free Micro-Bouncing (2 Minutes)
Let the child self-regulate with unrestricted movement on the cushion for the first two minutes. Don't prompt stillness — let the body take what it needs.
3
Introduce "Still Body, Bouncy Seat"
Gently coach: "Can you keep your upper body still while your seat does the bouncing?" This begins to build the motor distinction between controlled movement and seated focus.
4
Gradually Extend Still Periods
30 seconds → 1 minute → 2 minutes → 5 minutes. This progressive increase in sitting tolerance is the core skill-building arc of the wobble cushion protocol.

Step 5 of 6
The Dosage Principle — Repetitions That Regulate
3 Good Reps > 10 Forced Reps
Trampoline
50–200 bounces per session (3–5 sessions per day)
Hopper Ball
3–5 room lengths per session
Pogo Jumper
30–100 jumps per session
Wobble Cushion
Continuous during seated activities
Jump Rope
50–100 jumps or 2–3 minutes
Crash Pad
5–10 jumps per session
Variation options to prevent habituation: Switch between materials within a session (2 minutes trampoline → 2 minutes hopper → 2 minutes pogo); add cognitive challenges (bounce while naming animals, counting backward, singing); add motor challenges (bounce while catching a ball, balance a beanbag on head); introduce social bouncing with a sibling or parent.
Satiation Indicators — When the Child Has Had Enough: Spontaneously stops bouncing • Becomes calm and focused (the goal state!) • Shifts interest to a non-movement activity • Body relaxes — shoulders drop, jaw unclenches. Do NOT force continued bouncing after satiation. The child's nervous system is telling you the tank is full.
Step 6 of 6 — Reinforce
Mark the Win — Reinforcement That Builds the Habit
Duration: 1–2 Minutes
Reinforcement timing: Immediate, specific, enthusiastic. The natural consequence of bouncing — the calm, organised feeling — is the primary reinforcer for sensory seekers. Help the child notice and name it.
"Your body worked SO HARD on that bouncing! Look how calm you feel now."
"You bounced 100 times and now your body is ready. That's amazing self-regulation!"
"Your nervous system needed that input and you gave it exactly what it needed. That's smart body management."
"You know what your body needs and you took care of it. That's a skill most adults don't have." — For older children
Natural consequence reinforcement: "How does your body feel right now? Calmer? More ready? That's the bouncing working."
Token economy (optional): A bouncing chart with stickers for completed sensory diet sessions rewards the routine — not just the bouncing itself. Consistency is what transforms the protocol into lasting regulation.
⚠️What NOT to do: Never withhold bouncing as punishment. The child needs the input to function. Withholding sensory input is like withholding food from a hungry child.

Step 6 — Cool-Down
From Bounce to Calm — The Transition Protocol
Duration: 2–3 Minutes
1
Slow the Bouncing Gradually
Don't stop abruptly. "Let's make our bounces smaller... smaller... tiny bounces... standing still." Gradual deceleration prevents sensory cut-off and maintains the regulatory benefit into the transition.
2
Heavy Work Transition
After bouncing, 5 wall push-ups or "bear walks" across the room. The heavy muscle work deepens the proprioceptive input and transitions from vestibular to pure proprioceptive — a deeper, longer-lasting regulatory state.
3
Compression Option
If the child wears compression clothing, put it on now. Deep pressure extends the regulatory effect of the bouncing session, bridging the gap until the next scheduled input.
4
Grounding Moment
"Put both feet flat on the floor. Feel how strong and still they are. Your body got what it needed." This brief somatic awareness moment anchors the regulatory state.
5
Transition to Next Activity
The child should now be in a calm-alert state — ideal for homework, meals, classroom instruction, or social interaction. The post-bounce window lasts 30–90 minutes. Plan demanding activities within this window.
If the child doesn't want to stop: This may indicate the sensory tank isn't full yet. Extend by 2–3 minutes with diminishing bounces, or switch to a lower-intensity material (bouncy bands or wobble cushion). Note the duration for future sessions.

Data & Tracking
Track to Transform — The Bouncing Data Sheet
Tracking is what separates a sensory activity from a therapeutic protocol. Data reveals patterns, confirms progress, and guides adjustments. Even simple daily tracking transforms your observations into evidence-based decisions.
Time | Material | Duration | Intensity Before (1–5) | Intensity After (1–5) | Focus After (1–5) | Notes | |
Morning | Trampoline | 8 min | 5 | 2 | 4 | Good session, calm for breakfast | |
Pre-homework | Pogo jumper | 5 min | 4 | 2 | 3 | Needed 2 extra minutes | |
Pre-dinner | Hopper ball | 6 min | 5 | 1 | 5 | Best session — sat through dinner! |
Which materials work best?
What time of day is need highest?
How long does regulation last?
Is seeking intensity decreasing?
Are there triggers increasing the need?

Troubleshooting
When It Doesn't Go as Planned — The Consortium Troubleshooting Guide
1
❓ "The bouncing seems to make my child MORE hyper, not calmer."
Solution: (1) Slow the bouncing rhythm — fast bouncing can be alerting rather than calming; (2) Add heavy landing emphasis — "bounce and LAND heavy" increases proprioceptive input which is always calming; (3) Shorten the session and add compression during bouncing; (4) If escalation persists, seek comprehensive OT sensory processing evaluation.
2
❓ "My child won't use the trampoline — they prefer bouncing on the couch."
Solution: (1) Place the trampoline directly in front of the couch and redirect; (2) Put a wobble cushion on the couch as a transitional step; (3) Make the trampoline more appealing: music, games, counting, parent co-bouncing; (4) Accept a transition period — old habits take time to replace.
3
❓ "The wobble cushion at school is 'too noticeable' and the teacher doesn't want it."
Solution: (1) Share this page with the teacher; (2) Request a formal accommodation through the school's support system; (3) Try bouncy bands (less visible) as an alternative; (4) Compression undershirt worn under school uniform is invisible. → School Consultation
4
❓ "The bouncing works for 30 minutes then the child needs to bounce again."
Solution: This is expected. Sensory input doesn't last forever — it's like eating: you get hungry again. The solution is NOT longer sessions but MORE FREQUENT sessions. Build bouncing into the daily schedule every 60–90 minutes for moderate seekers, every 30–60 minutes for intense seekers.
5
❓ "My child bounces even MORE after getting trampoline time."
Solution: Differential considerations: (1) The child may have a sensory processing pattern where vestibular input is alerting rather than calming — try pure proprioceptive input instead (heavy work, carrying heavy items, wall push-ups) without the vestibular bounce component; (2) Consult an OT for a comprehensive sensory profile assessment.

Personalise the Protocol
Make This YOUR Child's Protocol — The Difficulty Slider
⬅️ Easier Version
For bad days, younger children, or beginners. Reduce bounces to 20–30 per session. Use only one material per session. Shorter sessions: 3–5 minutes. More parent involvement: hold hands while bouncing, bounce together. Lower intensity: gentle bouncing only, no crash activities.
🎯 Standard Version
50–100 bounces per session. 2 materials per session. 10–15 minute sessions. Child-led with parent supervision. Mix of bouncing intensities. This version suits most moderate seekers following the first two weeks.
➡️ Harder Version
For intense seekers or breakthrough days. 100–200+ bounces per session. Multiple materials: trampoline → hopper → crash pad sequence. 15–20 minute sessions. Add cognitive and motor challenges during bouncing. Include crash pad activities for maximum proprioceptive input.
Age Adaptations
Toddlers (2–3)
Mini trampoline with handle ONLY. Parent holds hands. Sessions 3–5 minutes maximum. Body sock exploration with full supervision.
Preschool (4–5)
Add foam pogo jumper, hopper ball, crash pad with low jump height. Sessions 5–10 minutes.
School Age (6–9)
Full protocol access. Begin self-management training: "When do you feel like you need to bounce?"
Pre-teen (10–12)
Self-directed sensory diet. Rebranding: "exercise break" may be more socially acceptable. Rebounder marketed as exercise equipment.

Sensory Profile Variations
Adapting the Protocol for Different Sensory Profiles
Pure Bouncing Seeker
Follow the protocol as written — maximum bouncing outlet access. This child benefits most directly from all nine materials and the full frequency schedule. Track satiation patterns carefully.
Mixed Seeker-Avoider
The child seeks bouncing but may avoid certain textures, sounds, or visual input. Ensure the bouncing environment is free of aversive stimuli — no loud music if the child has auditory sensitivity, no bright flashing lights, no scratchy clothing.
Seeker + ADHD
Combine the bouncing protocol with clear behavioural structure. Shorter, more frequent sessions. Clear visual transitions. Timer-based sessions with explicit start and stop cues. The sensory protocol and ADHD management are complementary, not competing.
Mastery ≠ Elimination: Mastery does NOT mean the child never needs to bounce. It means the child manages the need constructively. They will likely always need more proprioceptive-vestibular input than peers — mastery is managing it, not eliminating it.
Progress Arc — Weeks 1–2
Weeks 1–2: Tolerance, Not Transformation
Progress Bar: ████░░░░░░ ~15%
In the first two weeks, you will not see the bouncing disappear. That is not the goal yet. What you will see is the beginning of neural pathway formation — subtle, encouraging, and worth celebrating.
✅ What You WILL See
- Child begins to recognise the trampoline/hopper as "their bouncing place"
- Redirections from furniture to trampoline become easier (3 redirects → 1 redirect)
- Post-bouncing calm periods may be slightly longer (even 5 minutes more is progress)
- Child may begin requesting bouncing time — this is excellent, it means they're connecting the input with the relief
❌ What Is NOT Progress Yet
- The bouncing on furniture hasn't stopped (it won't — yet)
- The classroom bouncing is unchanged (classroom accommodation takes time to implement)
- The child still bounces during dinner (the sensory diet schedule is still being established)
The Patience Principle
"If your child voluntarily walks to the trampoline instead of bouncing on the couch even ONCE this week — that's a neural pathway forming."
Parent milestone: You'll notice yourself reframing. Instead of "stop bouncing," you'll say "let's go use the trampoline." This shift in YOUR language is the first sign of the approach working.
Sensory integration intervention outcomes emerge across 8–12 week timelines. PMC11506176

Progress Arc — Weeks 3–4
Weeks 3–4: The Neural Pathways Are Forming
Progress Bar: ████████░░ ~40%
Child spontaneously goes to bouncing equipment without prompting
Furniture bouncing decreases by 30–50%
Post-bouncing focus periods extend to 30–60 minutes
Child anticipates the sensory diet schedule: "Is it trampoline time?"
Mealtime sitting improves — may sit through most of a meal with wobble cushion
School feedback begins to shift: "she seems calmer after lunch"
Behavioural changes signalling neural pathway formation: Child reaches for compression wear before a transition • Says "I need to bounce" instead of just bouncing (verbalised awareness = huge progress) • Reduced intensity of bouncing needed to achieve regulation • Tolerates brief periods of no-bouncing without dysregulation
"You may notice you're more confident too. You understand the need, you have the tools, and you're seeing it work. This confidence is as important as any material."
Progress Arc — Weeks 5–8
Weeks 5–8: Mastery Emerging — Your Child Is Self-Regulating
Progress Bar: ████████████████████ ~75%
✅ Self-Selects Equipment
Child reaches for bouncing equipment when feeling dysregulated — without prompting from any adult.
✅ Furniture Bouncing Down 70%+
Or redirects in under 10 seconds when it does occur.
✅ Social Inhibition
Can inhibit bouncing for 5+ minutes when socially required — short classroom instruction, restaurant wait, assembly.
✅ Independent Accommodations
Uses wobble cushion and bouncy bands independently at school and home.
✅ Sensory Diet as Routine
Protocol implemented without resistance — the sensory diet has become part of the daily rhythm.
✅ Social Impact Reducing
Peer relationships improving as the "weird bouncing" has decreased enough to reduce social friction.
Generalisation indicators: Skill appears in new settings — child uses wobble cushion at grandparents' house, bounces at park before entering a store. Family members report improvement without being prompted. Teacher independently notes improvement.
Maintenance check: Does regulated behaviour persist during a 2-day period without structured bouncing? If yes → mastery consolidating. If the child immediately dysregulates without structure → continue the protocol and extend the timeline.

Celebrate This Win
You Did This. Your Child Grew Because of Your Commitment.
Five to eight weeks ago, you were watching your child bounce on every surface in your home, hearing "your child can't sit still" from teachers, and wondering if the bouncing would ever stop.Today, your child has appropriate outlets. They know what their body needs. They can tell you "I need to bounce." They can sit through homework with a wobble cushion. They can make it through dinner. They have tools.
That didn't happen because the bouncing magically stopped. It happened because YOU understood the need, YOU set up the environment, YOU maintained the sensory diet, and YOU advocated for accommodations at school and beyond.
📸Family Celebration Suggestion: Take a photo of your child bouncing joyfully on their trampoline. Put it on the refrigerator. This is not a picture of a problem — it's a picture of a solution. Every bounce is a brain being organised.
Red Flags
Trust Your Instincts — If Something Feels Wrong, Pause and Ask
🚩 Red Flag 1: Bouncing Is ESCALATING Despite the Protocol
What it looks like: The child needs more bouncing, not less, and the intensity is increasing weekly. Why it matters: More complex sensory profile may exist beyond proprioceptive-vestibular seeking alone. What to do: Seek comprehensive OT sensory processing evaluation.
🚩 Red Flag 2: Bouncing Is Accompanied by PAIN or Joint Complaints
What it looks like: Child complains of knee pain, ankle pain, or back pain during or after bouncing. Why it matters: May indicate hypermobility, growth plate concerns, or orthopaedic issues. What to do: Pause bouncing. Consult paediatrician. Resume only with medical clearance.
🚩 Red Flag 3: The Child Appears DISSOCIATED During Bouncing
What it looks like: Blank stare, unresponsive to name, rhythmic bouncing with no apparent awareness. Why it matters: May indicate bouncing is serving an emotional regulation function rather than pure sensory input. What to do: Note the pattern and discuss with the child's therapy team.
🚩 Red Flag 4: Bouncing ONLY at Specific Times (After Specific Events)
What it looks like: Bouncing increases dramatically after school, after family conflict, or after specific triggers. Why it matters: The bouncing may be anxiety/stress-driven rather than purely sensory. What to do: Address emotional triggers alongside the sensory approach.
🚩 Red Flag 5: NO Improvement After 8 Weeks of Consistent Protocol
What it looks like: Faithful execution of the protocol with no observable change. Why it matters: The sensory profile may require a different intervention approach. What to do: Professional reassessment recommended.
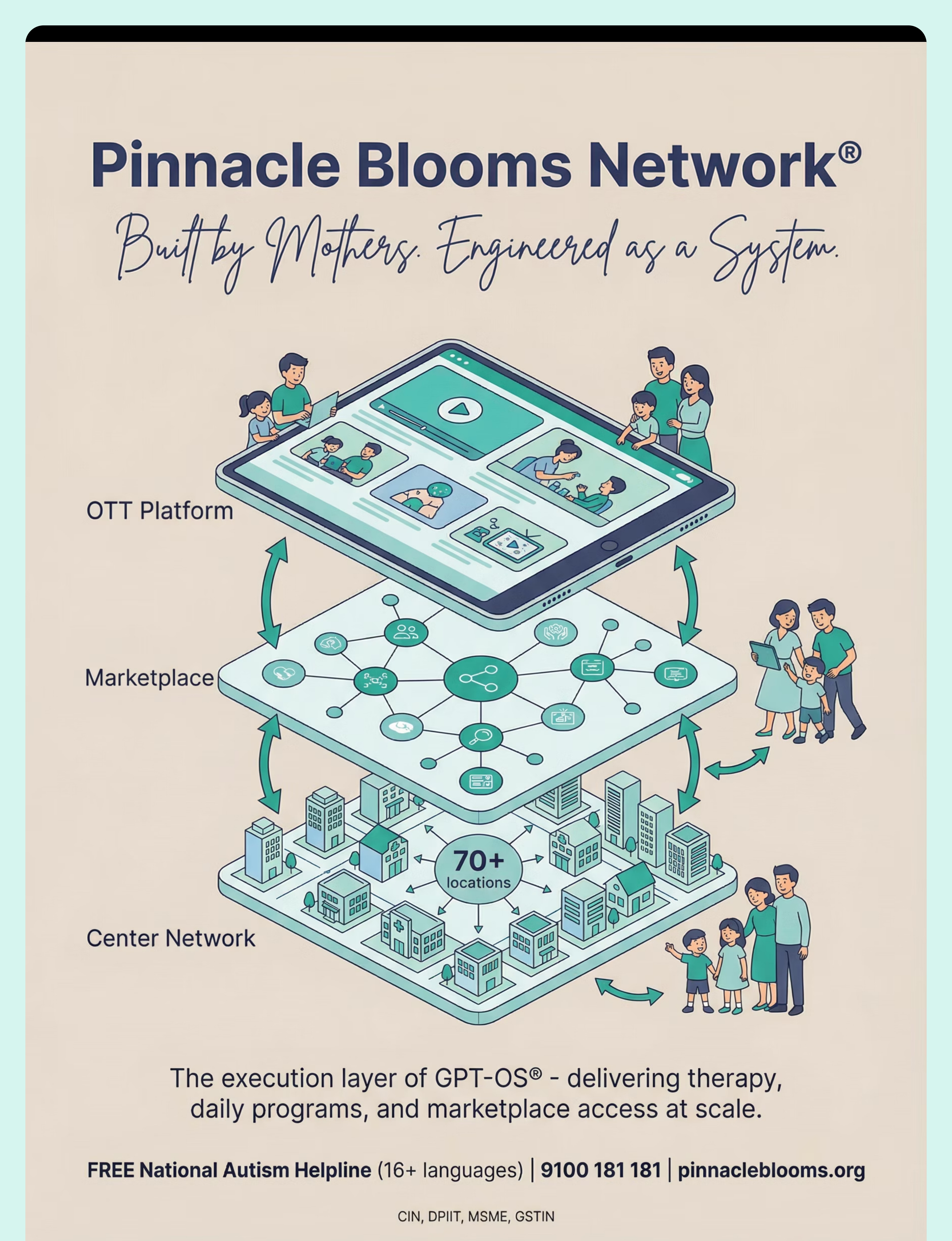
FREE National Autism Helpline: 9100 181 181 (16+ languages, 24×7)

Progression Pathway
Where You Are — And Where You're Going
Your work on A-089 builds directly on the proprioceptive and vestibular foundations of A-087 and A-088. As the bouncing seeking resolves, the pathway ahead branches based on your child's profile — towards generalised movement regulation, oral seeking, or visual seeking, depending on what co-occurs.
Path A — Bouncing Resolving
→ A-092: Can't Sit Still Protocol (generalised movement seeking beyond bouncing)
Path B — Oral Seeking Co-occurs
→ A-090: Mouthing & Chewing Seeking Protocol (oral proprioceptive needs)
Path C — Visual Seeking Co-occurs
→ A-091: Visual Stimming Seeking Protocol (visual input regulation)
Long-term developmental goal: Self-regulated sensory processing — the child independently identifies and meets their sensory needs using appropriate strategies, across all settings, without adult prompting.
Related Techniques
Techniques in the Sensory Seeking Cluster
The bouncing protocol rarely exists in isolation. Most children with proprioceptive-vestibular seeking also present with co-occurring sensory profiles across vestibular, proprioceptive, oral, and visual domains. These related techniques form the full sensory seeking cluster.
A-087: Spinning Seeking
Vestibular domain — co-occurring vestibular need via rotational movement. Often the closest co-occurring profile to bouncing seeking.
A-088: Crashing Seeking
Proprioceptive domain — co-occurring impact need. Children who both bounce and crash often have the most intense proprioceptive thresholds.
A-090: Mouthing & Chewing Seeking
Oral proprioceptive domain — co-occurring oral seeking. Frequently seen alongside bouncing in the same child profile.
A-091: Visual Stimming
Visual processing domain — co-occurring sensory profile. Visual seeking may accompany movement seeking in a broader sensory-seeking pattern.
A-092: Can't Sit Still
Movement regulation domain — the progression target once bouncing seeking is managed. Addresses generalised movement seeking beyond bouncing.
A-093: Constant Movement
Global motor regulation — advanced progression for children with pervasive movement seeking across all movement types and settings.

12 Developmental Domains
Your Child's Journey Across 12 Developmental Domains
Cross-Domain Impact of the Bouncing Protocol: Your work in Domain A (Sensory Processing) directly enables progress in Domain B (communication improves when the child is regulated), Domain C (social participation improves when inappropriate bouncing decreases), Domain E (cognitive focus improves with sensory needs met), and Domain G (emotional regulation builds on sensory regulation as its foundation).
Every technique exists within a developmental web. Progress in one domain creates cascading benefits across others. The AbilityScore® tracks this multi-domain impact, giving you and your therapy team a complete developmental picture.

Professional Support
When You Need Professional Support — We're Here
When to Seek Professional Help
You've followed this protocol for 8+ weeks with minimal improvement
Your child's bouncing is accompanied by other concerning behaviours
You need a comprehensive sensory processing evaluation and formal diagnosis
You want a professionally designed sensory diet tailored specifically to your child
School accommodation advocacy requires professional documentation and support
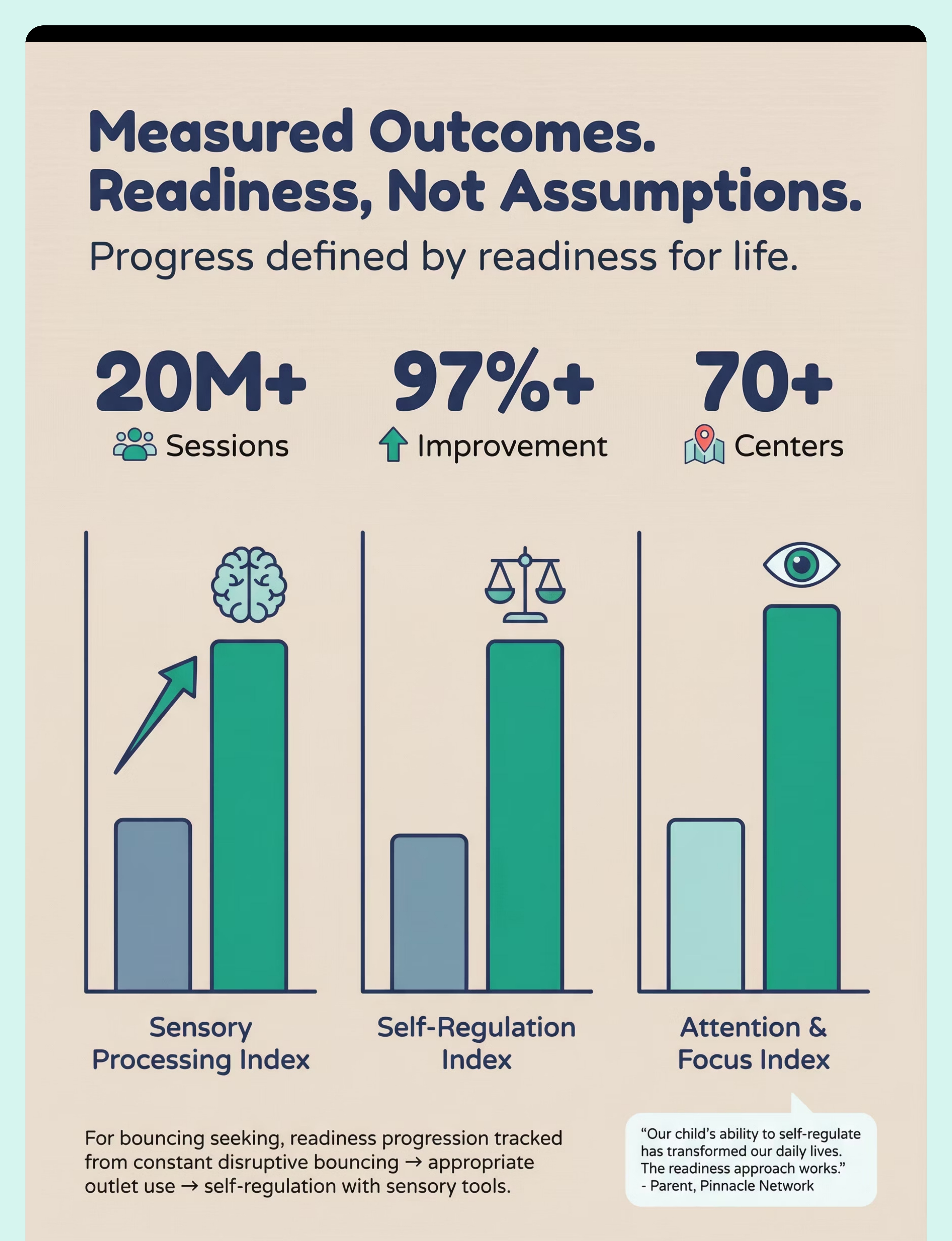
70+
Centres Across India
20M+
Therapy Sessions Delivered
97%+
Measured Improvement Rate
For families outside India: Pinnacle's teleconsultation services are available globally. The GPT-OS® platform enables remote assessment, therapy planning, and ongoing monitoring from anywhere in the world.

GPT-OS®
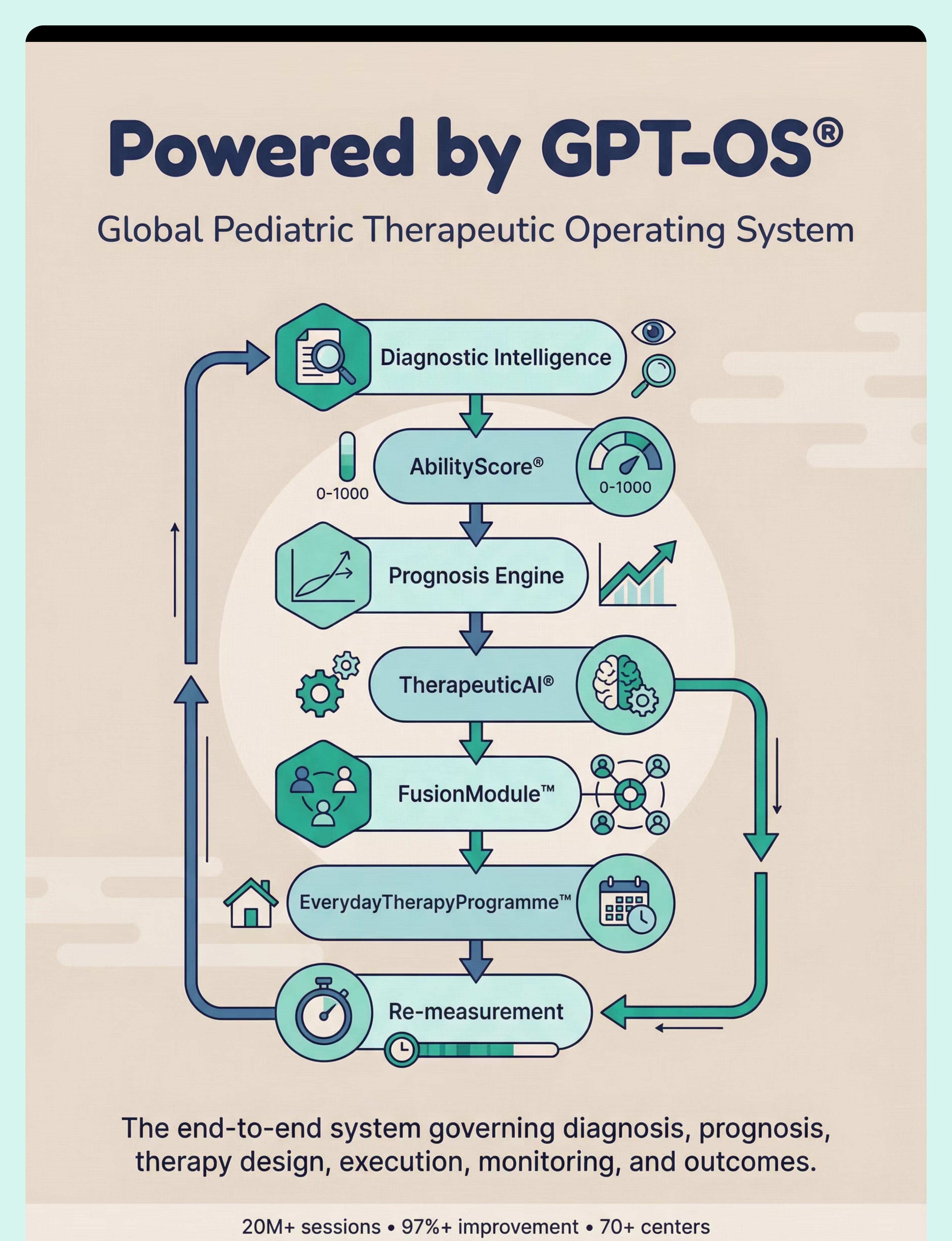
Powered by GPT-OS® — Global Paediatric Therapeutic Operating System
This protocol is one of 70,000+ intervention techniques governed by GPT-OS® — the end-to-end operating system for paediatric therapeutic intelligence, built from 20 million+ real therapy sessions.
Diagnostic Intelligence Layer
Converts 591+ structured observations across 349 skills and 79 developmental abilities into standardised diagnostic clarity.
AbilityScore®
A universal developmental score (0–1000) establishing baseline, severity, and longitudinal change — comparable across time, therapists, and centres.
Prognosis Engine
Predicts developmental trajectories using historical response patterns from 20M+ real therapy sessions.
TherapeuticAI®
Determines therapy focus, intensity, sequencing, and escalation thresholds — always executed under licensed human clinical authority.
FusionModule™
Coordinates speech, OT, behaviour, special education, and medical inputs into a single converged therapeutic pathway for every child.
EverydayTherapyProgramme™
Translates clinical plans into daily, home-executable micro-interventions — this page is part of that system.

Watch the Reel
Watch: 9 Materials That Help With Bouncing Seeking
A-089 — Sensory Solutions Episode 89 | 60 Seconds
1
Mini Trampoline
The direct answer to bouncing needs
2
Bouncy Seat Cushions
Bouncing while staying seated
3
Hopper Balls
Active bouncing with full-body work
4
Pogo Jumpers
Controlled bouncing with skill-building
5
Compression Wear
Passive proprioceptive input
6
Jump Rope
Rhythmic bouncing anywhere
7
Chair Bands
Leg bouncing with purpose under the desk
8
Sensory Diet Cards
Scheduled input throughout the day
9
Crash Pads
Jump and land with maximum proprioceptive impact

FAQ — Part 1
Frequently Asked Questions — Part 1 of 2
Q1: Is bouncing seeking the same as ADHD?
A: Not necessarily. Bouncing seeking is a sensory processing pattern; ADHD is an attention-regulation condition. They can co-occur, but they're different things requiring different (complementary) approaches. Sensory seeking involves specific input-seeking behaviour that results in regulation; ADHD involves broader attention and impulse challenges. A professional evaluation can differentiate.
Q2: Will my child ever stop needing to bounce?
A: The intensity typically decreases as the child develops self-regulation strategies and the nervous system matures. Most children don't "grow out of" the higher sensory threshold, but they learn to manage it. Many adults with similar profiles are drawn to running, cycling, or gym workouts — the need channels into healthy outlets over time.
Q3: How many bounces per day does my child need?
A: There's no universal number. Start with 50–100 bounces 3–5 times per day and observe. If the child remains dysregulated between sessions, increase frequency. If the child is well-regulated, the current dosage is working. Track and adjust using the daily data sheet (Card 20).
Q4: Can I use this protocol without an OT evaluation?
A: Yes — this protocol is designed for parent-led execution based on the Pinnacle Blooms Consortium's guidelines. However, if your child has complex needs, co-occurring conditions, or doesn't respond to the protocol within 8 weeks, an OT evaluation is strongly recommended.
Preview of 9 materials that help with bouncing seeking Therapy Material
Below is a visual preview of 9 materials that help with bouncing seeking therapy material. The pages shown help educators, therapists, and caregivers understand the structure and content of the resource before use. Materials should be used under appropriate professional guidance.

















Share this resource
Help others discover thisLink copied!

FAQ — Part 2
Frequently Asked Questions — Part 2 of 2
Q5: Is the trampoline safe for my 2-year-old?
A: Mini trampolines with handle bars are appropriate for children 2+ with direct adult supervision. Choose a trampoline specifically rated for the child's weight. Always supervise. One child at a time — never two children bouncing simultaneously on a mini trampoline.
Q6: What if my school refuses to allow wobble cushions or bouncy bands?
A: Advocate through the formal accommodation process. This page and the teacher communication template provide evidence-based justification. Contact Pinnacle's school consultation service for professional support: → School Consultation | Helpline: 9100 181 181
Q7: Can this protocol be used alongside medication for ADHD?
A: Yes. Sensory intervention and medication address different mechanisms. Many families find that appropriate sensory support reduces the behavioural load, which may inform medication discussions with their physician. Always consult the prescribing doctor before adjusting medication.
Q8: How do I know if my child's bouncing is sensory seeking vs. anxiety?
A: Sensory seeking bouncing typically occurs across all settings, is present even when the child is happy, results in regulation (calmer after bouncing), and seems driven by the body. Anxiety-driven bouncing increases with specific triggers, accompanies other anxiety signs, and may not regulate with bouncing alone. Both can co-occur.
