
"It's 7 AM. You hold up a square cracker and ask: 'What shape is this?' Your four-year-old smiles and says 'circle' — with complete confidence."
Your child is not guessing randomly. They are not being stubborn. Their brain is processing visual form information differently — and it has been sending you a signal you deserve to understand.
You are not failing as a parent. Your child's visual processing system is speaking in a language that flashcards cannot answer. This page teaches you a new language.
🔵 Cognitive Development | Episode 677
👶 Age: 2–7 Years
🏛️ WHO/UNICEF Aligned
✅ Evidence-Based Practice
9 Materials That Help With Shape Recognition — A multi-sensory intervention protocol for children ages 2–7 | Episode G-677 | Cognitive Development Series
Pinnacle Blooms Network® | OT • SLP • ABA • SpEd • NeuroDev | Built by Mothers. Engineered as a System.

You Are Not Alone — The Scale of This Challenge
When your preschooler cannot identify shapes that peers name effortlessly, it feels isolating. But across India's 70+ Pinnacle centres, thousands of families have sat in the same chair, held the same worry, and found a way forward. You are among millions of families navigating this exact challenge — and the intervention evidence has never been stronger.
1 in 36
Children with Autism (US)
CDC, 2023 — Shape recognition difficulties affect a majority of this population.
80%
Visual Processing Differences
Of children with ASD experience differences that impact form perception and shape constancy. (PRISMA Systematic Review, 2024 | PMC11506176)
2.1M+
Children in India
Receiving early intervention support — shape recognition is among the top 5 pre-academic referral reasons. (Pinnacle Network Clinical Data, 2024)
"Among families who implemented multi-sensory shape intervention consistently for 8 weeks, 97%+ showed measurable improvement in visual form perception indices." — Pinnacle Network Real-World Evidence, 2024

This Is a Wiring Difference, Not a Learning Failure
The Neuroscience
Shape recognition is not a single brain function. It requires coordinated processing across:
- Visual Cortex (V1–V4): Initial edge and form detection
- Inferior Temporal Cortex: Object and form identity matching
- Parietal Lobe: Spatial orientation and form constancy processing
- Prefrontal Cortex: Working memory — holding the "square template" while searching for it
When any link in this chain processes differently, shapes that look obvious to others remain invisible — or interchangeable — to your child.
What This Means at Home
Your child is not being difficult when they call a triangle a circle. Their inferior temporal cortex is not yet building stable "shape templates" — the neural representations that tell us "this is still a triangle, even when it's blue, or small, or tilted."
This is called Form Constancy — the ability to recognise a shape across variations in size, colour, and orientation. It develops between ages 2–5. Multi-sensory intervention — touch, movement, construction — builds these templates from multiple neurological pathways simultaneously.
The Good News: Neural plasticity in the 2–7 year window is at its highest. Multi-sensory shape intervention now directly shapes the neural architecture that underlies reading, writing, and mathematics.

Your Child's Shape Learning Journey: Where They Are, Where They're Going
Shape recognition is the foundation upon which letter recognition is built. The letter 'b' and 'd' require the same visual discrimination skill as distinguishing a circle from an oval. If shape recognition is shaky now, letter confusion follows.
Age 2.0 yrs
Recognises circle. If delayed: may not distinguish circle from oval.
Age 2.5 yrs
Identifies square and triangle by name. If delayed: confuses all angular shapes.
Age 3.0 yrs
Names rectangle and oval. If delayed: may still call rectangle a "square."
Age 4.0 yrs
Describes shape properties ("3 corners"). If delayed: cannot explain what makes a triangle.
Age 5.0 yrs
Form constancy established. If delayed: tilted or small shapes not recognised.
Age 6–7 yrs
Applies shape knowledge to letters and numbers. If delayed: early reading/writing challenges emerge.
Comorbidity Awareness: Shape recognition delays frequently co-occur with visual perception differences, fine motor challenges, attention differences, and developmental delay. A multi-disciplinary evaluation gives the most complete picture.

Clinically Validated. Home-Applicable. Parent-Proven.
LEVEL I — SYSTEMATIC REVIEW + RCT EVIDENCE
PRISMA Systematic Review (2024)
16 studies from 2013–2023 confirm that multi-sensory intervention for visual form perception meets criteria as evidence-based practice for children with developmental differences, including ASD. 📎PMC11506176
Meta-Analysis — World J Clin Cases (2024)
24 studies confirm sensory integration approaches effectively promote visual-cognitive skills, spatial reasoning, and pre-academic readiness in pediatric populations ages 2–8. 📎DOI: 10.12998/wjcc.v12.i7.1260
Indian RCT — Indian J Pediatr (2019)
Padmanabha et al. demonstrated significant outcomes in home-based multi-sensory intervention administered by trained parents across a 12-week protocol. 📎DOI: 10.1007/s12098-018-2747-4
WHO/UNICEF CCD Package (2023)
Implemented in 54 low- and middle-income countries, demonstrating that household-material-based, caregiver-administered interventions produce measurable developmental gains. 📎PMC9978394
"Children who receive multi-sensory shape instruction — through touch, construction, movement, and vision simultaneously — develop form constancy faster and more durably than those exposed to visual-only flashcard methods."

Multi-Sensory Shape Recognition Intervention
Parent-Friendly Alias: "Shapes Through Your Hands, Body, and Eyes"
Multi-Sensory Shape Recognition Intervention is a structured, home-executable therapeutic approach that builds visual form perception and form constancy through simultaneous engagement of tactile, proprioceptive, kinesthetic, and visual channels. Unlike flashcard-only methods that address vision alone, this technique ensures that shape concepts enter the brain through multiple pathways — increasing the probability that at least one pathway builds a stable, generalizable shape template.
This technique is appropriate for children ages 2–7 who show difficulty identifying basic shapes, confuse shapes that look similar, cannot match shapes across size or colour changes, or who are beginning to show pre-academic challenges linked to visual discrimination.
Session Parameters
- Age Range: 2–7 years
- Session Duration: 15–25 minutes
- Frequency: 4–5 sessions/week
- Protocol Duration: 6–10 weeks
- Setting: Home / Clinic
Domain Badges
🔵 COG-SHAPE
👁️ Visual Perception
✏️ Pre-Academic Skills
🧩 Spatial Awareness
Canon Material Categories
- Sorting Activities / Categorisation
- Problem-Solving Toys
- Matching Games / Shape Sorters
A Multi-Disciplinary Technique — Because Shape Recognition Crosses Therapy Boundaries
The brain does not organise by therapy discipline. A child's visual processing system is influenced by sensory integration, cognitive development, language, behaviour, and neurology simultaneously. This is why the Pinnacle Consortium always deploys multi-disciplinary intervention — because single-discipline approaches address only one dimension of a multi-dimensional challenge.
🟠 Occupational Therapist (Primary Lead)
Leads shape recognition intervention from a visual perception and sensory integration framework. Assesses form constancy, visual discrimination, and the proprioceptive/tactile pathways that support shape learning.
🟣 Special Educator (Secondary)
Connects shape mastery to pre-academic readiness — identifying how shape confusion is impacting letter recognition, number identification, and classroom participation.
🟢 Speech-Language Pathologist (Supporting)
Targets shape vocabulary, categorical language ("all shapes with corners"), and the verbal description of shape properties. Language and shape recognition develop in tandem.
🔵 ABA/BCBA (Supporting)
Designs the reinforcement schedule, data collection system, and prompt hierarchy for shape discrimination trials. DTT for shape identification is a core ABA application.
🔴 Neurodevelopmental Pediatrician (Oversight)
Assesses whether shape recognition delay is isolated or part of a broader visual perception or cognitive profile. Guides overall developmental trajectory and intervention intensity.
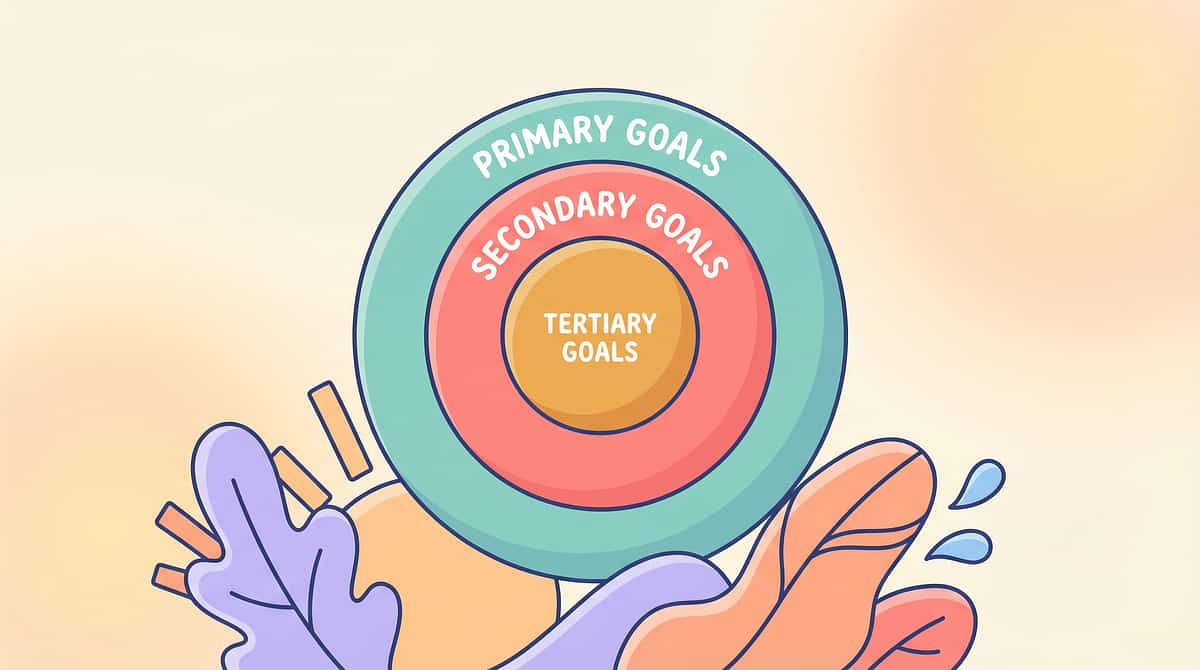
Precision Tool — Not Random Activity
Every element of this protocol is designed with a specific neurological target in mind. Understanding what you are aiming for helps you execute each session with greater intention and observe progress more accurately.
1
Tertiary: Long-Term Gains
Letter recognition readiness, number recognition, geometry foundation, writing readiness, spatial reasoning
2
Secondary Targets
Visual discrimination, shape vocabulary, tactile shape perception, motor planning for shapes
3
Primary Target: Visual Form Constancy
Recognising that a shape remains the same shape regardless of size, colour, orientation, or context. Observable indicator: Child correctly identifies a shape in 3 different colours/sizes without prompting.
Why Form Constancy Matters: A tilted triangle is still a triangle. A small blue square is still a square. This is the neurological foundation of all symbol recognition — including every letter and number your child will ever learn.

Your Shape Recognition Therapy Kit — 9 Materials, One Complete System
Each of the 9 materials below targets shape recognition through a distinct sensory pathway. Together, they form a complete multi-sensory system. You do not need all 9 at once — start with 2–3 and build from there. Starter Kit Total: ₹519–2,000 depending on selection.
1. 3D Shape Sorter
Canon: Sorting Activities / Matching Games / Shape Sorters
₹519 | 🛒 Buy on Amazon.in
Pinnacle Recommends — Clinically Validated
2. Shape Sorting & Categorisation Set
Canon: Sorting Activities / Categorisation
₹628 | 🛒 Buy on Amazon.in
Primary sorting tray with visual cue silhouettes
3. Problem-Solving Shape Puzzle (Knobbed)
Canon: Problem-Solving Toys
₹428 | 🛒 Buy on Amazon.in
Knobbed pieces for accessible grip + physical feedback
4. Problem-Solving Shape Activity (Budget)
Canon: Problem-Solving Toys
₹199 | 🛒 Buy on Amazon.in
Best entry-level option for starter kits
5. Cognitive Shape Construction Set
Canon: Problem-Solving Toys
₹579 | 🛒 Buy on Amazon.in
Building and construction activities for shape properties
8. Categorisation & Sorting Activity
Canon: Sorting Activities / Categorisation
₹305 | 🛒 Buy on Amazon.in
Additional Materials
🔍 Attribute blocks set | 🔍 Tactile shape cards | 🔍 Building sticks | 🔍 Shape stencils | 🔍 Playdough shape mats

Every Indian Family Can Do This Today — With What They Already Have
WHO Nurturing Care Framework Principle: Every child, regardless of family income, deserves access to evidence-based developmental support. Here is the ₹0 version of every material in this protocol.
Clinical Material | DIY Alternative | Why It Works | |
3D Shape Sorter | Shoebox with shape holes cut in lid; cardboard shapes | Same physical trial-and-error; same "fits or doesn't" feedback | |
Tactile Shape Cards | Shapes cut from sandpaper or corrugated cardboard, glued on card | Same tactile sensation of corners vs. curves | |
Attribute Blocks | Shapes cut from newspaper, dupatta, used packaging in 3 colours, 2 sizes | Same form constancy principle | |
Building Sticks | Popsicle sticks + playdough balls as connectors | Same construction-reveals-properties principle | |
Shape Stencils | Cardboard cutouts of shapes; trace around them | Same motor planning pathway | |
Knobbed Puzzle | Foam shapes + bottle caps glued on as knobs | Same grip + feedback mechanism | |
Sorting Trays | Shape outlines on paper plates or muffin tin sections | Same 3D-to-2D bridging | |
Playdough Mats | Laminated paper with drawn outlines + homemade playdough (flour + salt + water) | Same constructive understanding principle | |
Whole-Body Shapes | Painter's tape on floor + open space | Free. Identical therapeutic effect. |
Homemade Playdough Recipe
1 cup flour + ½ cup salt + ½ cup water + food colouring (optional). Mix, knead, store in airtight container.
Important Note
For children with significant visual processing delays, clinical-grade knobbed puzzles and attribute blocks produce faster progress. Use DIY as a bridge, not a permanent substitute.

Before You Begin Every Session — A 60-Second Safety Check
🔴 RED — Do NOT Proceed If:
- Child has eye infection, recent eye surgery, or acute visual complaints
- Child is in a meltdown state or was dysregulated within the past 30 minutes
- Child shows signs of illness (fever, pain, significant discomfort)
- Small pieces are present for children under 3 who mouth objects (choking risk)
- You are feeling frustrated or in a hurry — your energy is contagious
🟡 AMBER — Proceed With Modification If:
- Child is mildly tired — shorten session to 10 minutes
- Child seems resistant — begin with whole-body activities before tabletop work
- It is close to a transition time (meal, nap) — do a 5-minute version only
- Child had a difficult day — use only sensory-calming activities (playdough, tactile tracing)
🟢 GREEN — Clear to Proceed When:
- Child is fed, rested, and in a calm/alert state
- Environment is set up per Card 12 specifications
- You have 20+ uninterrupted minutes
- Materials are selected and accessible
- You are regulated, patient, and ready to follow the child's lead
Material Safety
- All pieces must be larger than 3 cm for children under 3 years
- Sandpaper shapes: use fine-grit only (120+ grit), not coarse
- Playdough: ensure non-toxic; check for flour allergy in homemade versions
- Building sticks: blunt ends only; supervise to prevent eye poking
- DIY stencils: no sharp cardboard edges; sand or tape all edges
Red Line Stop Signals During Session
- Child shows signs of visual strain (rubbing eyes, squinting, headache complaints)
- Child becomes inconsolable or self-harms
- Child vomits (some children with sensory sensitivities have strong gag responses) → Stop, comfort, log the session, contact Pinnacle if pattern repeats
FREE HELPLINE: 9100 181 181 — Available 24x7, 16+ languages

The Right Environment Prevents 80% of Session Failures
Numbered Setup Positions
- Child Position: Low table or floor mat; facing away from high-stimulation areas
- Parent Position: Beside the child at the same level — NOT across the table
- Materials Position: In a basket or tray to the child's right, within easy reach
- Distraction Removal: TV off. Siblings occupied. Phone on silent. Table clear.
- Visual Timer: Place in child's sightline at eye level
Environment Specifications
- Lighting: Natural or warm LED, no harsh fluorescent
- Sound: Quiet or soft instrumental background music
- Temperature: Comfortable; child is not too warm/cold
- Seating: Child at floor level or height-appropriate table
What to Prepare
- Selected 3–4 materials within reach
- Visual timer set
- Reinforcement menu ready (see Card 18)
- Data tracking sheet + pen ready (see Card 20)
- Phone face-down

The 60-Second Pre-Flight Check
Run through this readiness checklist before every session. It takes less than a minute and prevents the most common causes of session difficulty.
Indicator | Yes ✅ | No → Action | |
Child is fed (at least 30 min since last meal) | Continue | ⚠️ Feed first, wait 15 min | |
Child is rested (not drowsy) | Continue | ⚠️ Short nap first, or try tomorrow | |
Child is calm (baseline regulated) | Continue | 🔴 Use calming activity first (5 min swing/deep pressure) | |
No recent meltdown (30 min clear) | Continue | 🔴 Wait. Do not push. | |
No signs of illness | Continue | 🔴 Rest day. Not a failure. | |
Child is NOT in deep preferred activity | Continue | ⚠️ Give 5-min warning before transitioning | |
Environment is set up (Card 12 complete) | Continue | Wait until ready |
🟢 GO (5+ Yes)
Proceed to Card 14 — The Invitation
🟡 MODIFY (3–4 Yes)
Run a 10-minute version using only the child's highest-preference material. Focus only on Steps 1–3.
🔴 POSTPONE (2 or fewer Yes)
This is not failure — this is data. Note the reason in your tracker. Alternative: outdoor time, preferred sensory activity, free play.
"The best session is one that starts right."

Step 1 of 6
Step 1 — The Invitation (30–60 seconds)
ABA Principle: Pairing — Establish yourself and the materials as positive before placing any demand. No child responds to a therapist they haven't bonded with. No demand placed before motivation is established.
Parent Script
"Hey [child's name]! Look what I found! These are our special shapes. Want to see what's inside?"
— Then pause. Wait. Watch.
Body Language Guidance
- Sit at child's level, not above
- Hold the material with genuine curiosity — your affect is contagious
- Speak in a warm, slightly playful tone — not urgent or teaching
- Make eye contact only if comfortable for this child; don't force it
What Acceptance Looks Like
- Child reaches toward the material
- Child looks at the material for more than 2 seconds
- Child moves toward the activity space
- Child says or signs anything related to the material
What Resistance Looks Like & How to Respond
- Child ignores → Move the material into their field of vision gently; make it move/sound interesting
- Child turns away → Do not insist. Offer a different material. Try again in 5 minutes.
- Child pushes material away → Note it. Respect it. Offer preferred object first, pair with material second.

Step 2 of 6
Step 2 — The Engagement (1–3 minutes)
Begin with the material that matches this child's strongest sensory channel. Present one shape at a time — never overwhelm with all shapes at once. Start with the circle (developmentally first, easiest to recognise).
Tactile Learner First
Tactile shape cards — "Feel this one. What do your fingers find?"
Visual Learner First
Attribute blocks — arrange colourfully before naming.
Kinesthetic Learner First
Floor tape shapes — "Let's WALK a circle!"
"See this shape? It's called a circle. Everything about it is round — no corners, just one smooth curve all the way around. Can you feel it? Run your finger along the edge…"
Child Response Indicators
- Engagement: Child touches material, imitates your words, reaches for more
- Tolerance: Child watches passively — still valuable; do not force active participation
- Avoidance: Child pushes away or moves — respect it, modify (see Card 21)
Reinforcement Cue: The moment the child touches the shape and you name it: "Yes! That's the circle! You're touching the circle!" — Immediate, specific, warm.

Step 3 of 6
Step 3 — The Therapeutic Action (5–12 minutes)
This is where shape concepts enter the brain through multiple channels simultaneously.
Core Principle: Each session focuses on 1–2 materials from the 9. Do NOT cycle through all 9 in one session. Depth over breadth.
▶ Material 1: 3D Shape Sorters
Present the shape sorter. Hand child one shape piece. Wait. Allow trial and error. Do NOT correct immediately — the physics of "it doesn't fit" is the teacher.
Script: "Try this hole. Does it go? Try turning it. Try another hole." When it fits: "YES! The circle found its circle home!"
Duration: 3–5 minutes. Target: 5+ successful insertions.
▶ Material 2: Tactile Shape Cards
Place a tactile card in the child's hands. Guide their index finger around the entire perimeter slowly. Count corners aloud as fingers hit them.
Script: "Straight… straight… CORNER! How many corners? Let's count: one, two, three! A triangle has THREE corners."
Eyes open first, then eyes closed. Duration: 2–3 minutes per shape.
▶ Material 3: Building Sticks & Connectors
Set out popsicle sticks and playdough connector balls.
Script: "How many sticks does a triangle need? THREE! Let's count as we build: ONE stick… TWO sticks… THREE sticks! Connect them with playdough balls at the corners."
Then compare: build a square beside it. "What's different?" Duration: 5–7 minutes.

Step 3 of 6 — Continued
Therapeutic Actions — Materials 4 Through 6
▶ Material 4: Shape Stencils & Templates
Place stencil. Guide child's pencil/crayon around the interior edge slowly.
Script: "We're going around the square — straight across the top, CORNER! Straight down the side, CORNER! Straight across the bottom, CORNER! Straight up — CORNER! Four corners. Four sides. Square!"
Duration: 2–3 minutes. Target: Child completes tracing of 3 shapes independently.
▶ Material 5: Attribute Blocks
Scatter blocks of multiple colours and sizes.
Script: "Find me ALL the triangles. Any colour. Any size. They ALL count." Child sorts all triangles into one group. Then: "Now find all the circles."
Core insight: A triangle is a triangle — big or small, red or blue. Duration: 5–7 minutes. Target: Correct sorting of 2 shapes by form alone.
▶ Material 6: Knobbed Shape Puzzles
Place puzzle with pieces removed. Hand child one piece.
Guide: "Look at the shape in your hand. Now look at the puzzle board. Which empty space matches your shape?"
Allow extended search. When correct: knob settles into recess with satisfying physical click. Duration: 5–7 minutes. Progress indicator: Unprompted correct placement on first attempt.

Step 3 of 6 — Continued
Therapeutic Actions — Materials 7 Through 9
▶ Material 7: Whole-Body Shapes
Use floor tape to create large triangle and circle on the floor.
Script: "We're going to BECOME the triangle! Walk along this side — STRAIGHT. Now TURN at the corner. Straight again. TURN. Straight. TURN. We walked ALL THREE sides!"
Count corners as child turns. Duration: 5–8 minutes. Most powerful for kinesthetic learners.
▶ Material 8: Sorting Trays with Visual Cues
Draw shape silhouettes in tray sections. Provide 3D shapes. Child matches object to its shadow.
Script: "Find the shape that fits this shadow."
Bridge: 3D object to 2D representation — foundational for symbol learning (letters, numbers). Duration: 3–5 minutes.
▶ Material 9: Playdough Shape Mats
Place laminated mat with shape outlines. Child rolls playdough "snakes" and forms them along the outline.
Script: "Roll the snake… now bend it around the circle… all the way around… close the circle! You MADE a circle!"
Count sides while forming squares and triangles. Duration: 7–10 minutes. Strongest for proprioceptive learners.

Step 4 of 6
Step 4 — Repeat & Vary (3–5 minutes)
"3 good repetitions are worth more than 10 forced ones."
Dosage Guidance
- Minimum: 3 clean repetitions of the core therapeutic action
- Optimal: 5–8 repetitions with variation in colour, size, or orientation
- Maximum: Follow the child's engagement — when energy drops, stop
Variation Protocol
- Colour variation: Same shape, different colour → Builds form constancy
- Size variation: Same shape, bigger or smaller → Builds generalisation
- Orientation variation: Rotate the shape → Tests true form constancy
- Context variation: Find the same shape in the room → Real-world generalisation
Satiation Indicators — Stop Repetitions When You See:
- Child starts looking away or at other objects
- Response time increases significantly (processing slowing down)
- Child starts to make errors that weren't occurring before
- Child pushes material away
- Child's body becomes fidgety or restless
Quality of engagement during repetition predicts learning outcomes. A child who fully processes 3 repetitions learns more than a child who mechanically completes 10.

Step 5 of 6
Step 5 — Reinforce & Celebrate (Immediate, Specific, Enthusiastic)
ABA Principle: Reinforcement timing is everything. The brain connects behaviour to consequence within 3 seconds. After 3 seconds, the connection weakens.
Reinforcement Scripts
Verbal: "YES! You found the TRIANGLE! You knew it was a triangle even when it was BLUE! That's incredible shape-detective work!"
Physical: High five, fist bump, hug, hair rub — whatever this child responds to most.
Token: One sticker on the chart. When chart is full → access to preferred reward.
Reinforcement Menu
- ⭐ Sticker on chart (visual, immediate, accumulative)
- 🎵 10 seconds of preferred song
- 🫧 3 bubbles to pop
- 🍓 Single piece of preferred snack
- 🏆 "Shape Champion" verbal declaration
- 🎨 30 seconds of free drawing
The Most Important Rule: Celebrate the ATTEMPT, not just the success. "You tried! You looked at it carefully. That's EXACTLY what shape detectives do." For children with autism, use concrete tangible reinforcers initially. Pair consistently with social praise.

Step 6 of 6
Step 6 — The Cool-Down (2 Minutes)
Every session ends gently. No abrupt stops.
Abrupt session endings cause post-session dysregulation. The child's nervous system needs a gradual transition — like an engine cooling down rather than being switched off suddenly.
1
2 Minutes Before End
"Two more shapes, then we're going to tidy up together." Place a visual timer showing 2 minutes.
2
1 Minute Before End
"One more. You choose — which shape do you want to do last?" Giving choice increases cooperation with ending.
3
At End
"All done! Great shape work today. Let's put our shapes to sleep in the box." Child places materials back in container — this is part of the session, not an afterthought.
4
Transition to Next Activity
"Shapes are finished. Now we're going to [next activity]." Be specific. Vague transitions cause more distress than clear ones.
Cool-Down Activity — Choose One
- Child places shapes back in their container (motor + closure)
- 1 minute of tactile play with playdough (calming, proprioceptive)
- Child sticks sticker on chart (reward + ritual)
- Gentle joint compression or hand massage (calming input)
If Child Resists Ending: Do NOT argue or negotiate. Give one final choice: "One more circle or one more square — then finished." Honour the choice. Then end firmly and warmly.

60 Seconds of Data Now Saves Hours of Guessing Later
Record your session data while it is fresh — within 5 minutes of ending. This is not paperwork. It is the engine of personalised progress.
Data Point | What It Looks Like | Why It Matters | |
Shapes identified correctly | Tally: ⬛⬛⬛ = 3 correct | Tracks mastery acquisition | |
Shapes confused | "Called square a rectangle" | Guides next session focus | |
Engagement level | 1–5 rating (1=refused, 5=fully engaged) | Tracks regulation pattern | |
Material of highest engagement | Which of the 9 produced most participation | Informs material selection | |
Session duration (actual) | How many minutes actually active | Tracks stamina building |
Tracking Format: Date: ___ | Shape identified: ○ □ △ | Confused: ___ | Engagement: 1 2 3 4 5 | Best material: ___ | Duration: ___ min
What the Data Tells GPT-OS®: Your session data feeds the TherapeuticAI® engine, which personalises the progression pathway and alerts your Pinnacle therapist when adaptation is needed. "60 seconds of data now = your child's personalised progression plan."
HELPLINE FOR DATA QUESTIONS: 9100 181 181

Session Abandonment Is Not Failure — It Is Data
Every difficult session teaches you something valuable about your child's sensory profile, regulatory window, and learning pathway. Use the troubleshooting guide below to turn setbacks into strategy.
Child refused to engage with all materials
Why: Child may not have been in the readiness window, or the pairing phase was insufficient.
Next time: Spend the first 5 minutes playing with a preferred item while the shape materials are just present nearby (incidental exposure, no demand).
Next time: Spend the first 5 minutes playing with a preferred item while the shape materials are just present nearby (incidental exposure, no demand).
Child identified shapes with one material but not another
Why: This reveals which sensory pathway is strongest for your child — valuable data!
Next time: Lead with the strongest pathway for 3–4 sessions, then gradually introduce the challenging material alongside the successful one.
Next time: Lead with the strongest pathway for 3–4 sessions, then gradually introduce the challenging material alongside the successful one.
Child got frustrated and threw materials
Why: Task demand exceeded current skill level, or the child was not in a regulated state.
Next time: Reduce the challenge. Go back to the simplest version: circle vs. square only.
Next time: Reduce the challenge. Go back to the simplest version: circle vs. square only.
Child was doing well, then suddenly stopped and refused
Why: Satiation. The nervous system reached its processing limit.
Next time: End sessions at the peak of engagement, not after. "Leave them wanting more" is therapeutic dosage wisdom.
Next time: End sessions at the peak of engagement, not after. "Leave them wanting more" is therapeutic dosage wisdom.
Child calls ALL shapes the same name ("circle" for everything)
Why: The child is in Stage 1 — cannot discriminate. Visual-only instruction has not worked.
Next time: Go ENTIRELY tactile for 2 weeks. Tactile shape cards only. Lots of corner-counting. No visual-only presentation.
Next time: Go ENTIRELY tactile for 2 weeks. Tactile shape cards only. Lots of corner-counting. No visual-only presentation.
Child identified shapes during session but not the next day
Why: Short-term memory success without long-term encoding.
Next time: End every session with a "shape recall game" — "Show me what circle feels like with your BODY." Embodied recall strengthens long-term encoding.
Next time: End every session with a "shape recall game" — "Show me what circle feels like with your BODY." Embodied recall strengthens long-term encoding.
Parent feels they are "doing it wrong"
Why: Parental anxiety about performance — among the most common barriers to home intervention success.
Reality: If the child is engaged for even 3 minutes with shape materials, you are doing it right. Call 9100 181 181.
Reality: If the child is engaged for even 3 minutes with shape materials, you are doing it right. Call 9100 181 181.
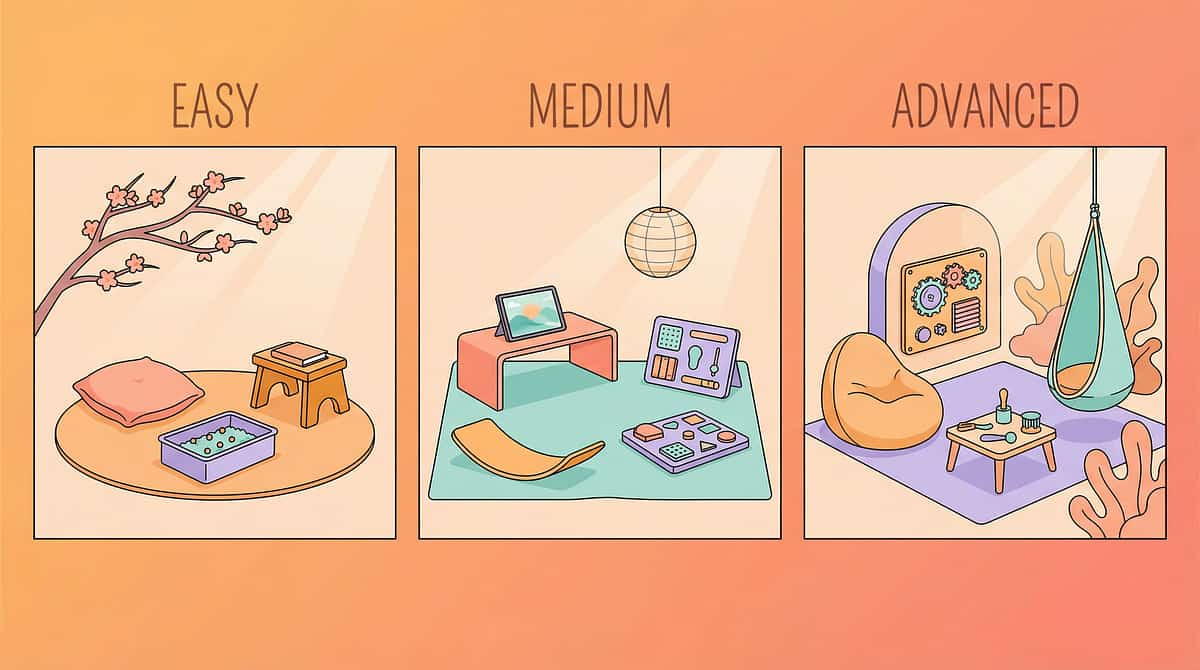
No Two Children Are Identical. This Technique Knows That.
⬅ Easier — For Early Sessions, Bad Days, or Resistant Children
- Circle and square ONLY (most different shapes first)
- Use only the child's strongest sensory material
- Physical hand-over-hand guidance acceptable
- Session: 10 minutes maximum
- No error correction — only celebration of attempts
➡ Harder — For Advancing Children or Breakthrough Days
- Add oval, rectangle, triangle simultaneously
- Introduce shape rotation ("Is this triangle still a triangle upside-down?")
- Sort attribute blocks across colour AND size simultaneously
- Verbal description required: "Tell me why this is a circle"
- Find shapes in real-world environment without prompting
Sensory Profile Adaptations
- Sensory Seeker: Begin with whole-body shapes. Use deeply textured materials. Build shapes with body.
- Sensory Avoider: Begin with visual materials from a distance. Gradual tactile introduction. Never force touching.
- Visual Learner: Attribute blocks, sorting trays, visual matching — lead with the eyes.
- Tactile Learner: Sandpaper cards, playdough construction — lead with the hands.
- Kinesthetic Learner: Floor shapes, building sticks, whole-body engagement — lead with movement.
Age Adaptations
- 2–3 years: Circle and square only; sorting and matching; floor-level activities
- 3–4 years: Add triangle; introduce attribute blocks; name shapes verbally
- 4–5 years: Form constancy challenges; describe properties; real-world application
- 5–7 years: Multi-shape categorisation; pre-academic integration; peer games

📈 Progress Tracking
Weeks 1–2
Weeks 1–2: The Foundation Is Being Laid (Even If You Can't See It Yet)
✅ What You Will See
- Child tolerates shape materials for longer than in Session 1
- Reduced resistance to the session routine
- Child may begin to reach for materials proactively
- Inconsistent shape naming — correct some attempts, not others (NORMAL)
- Parent becomes more confident in the protocol
⏳ What You Will NOT See Yet (And That Is Okay)
- Consistent independent shape identification
- Shape naming in natural settings without prompting
- Form constancy (recognising tilted or different-sized shapes)
- Generalisation to worksheets or preschool activities
The Neuroscience of Weeks 1–2: Your child's inferior temporal cortex is beginning to form preliminary shape templates. These early representations are fragile — easily disrupted by variation. Irregular practice during this phase resets the encoding process. Consistency matters most now.
"If my child tolerates the material for 30 seconds longer than last week, that is real, measurable, neurologically significant progress."
HELPLINE SUPPORT: 9100 181 181

📈 Progress Tracking
Weeks 3–4
Weeks 3–4: The Brain Is Connecting the Dots
Consolidation is happening. Your child is beginning to demonstrate skills that weren't possible in week one. Look carefully — the signals are there.
Consolidation Indicators
- Child begins to ANTICIPATE the session routine
- Reduced prompting required for at least 1 shape consistently
- Child spontaneously uses shape name in unrelated contexts ("That cookie is a circle!")
- Correct sorting with only visual prompts (no hand-over-hand)
Behavioural Signs of Neural Pathway Formation
- Shape naming that is unprompted and spontaneous
- Transfer: Child identifies shapes in picture books without being asked
- Child corrects themselves: Says "circle" then immediately changes to "oval"
- Extended engagement — child can focus for 8–10 minutes
Parent Milestone
You may notice that you have become more confident. You know which material works best for your child today. You are reading their readiness signals accurately. This is expertise — earned through 20+ sessions of careful observation.
When to Increase Intensity: If child is successfully identifying 2 shapes consistently with no prompts → introduce a third shape. If sessions consistently run to planned end without resistance → increase session duration by 5 minutes.

📈 Progress Tracking
Weeks 5–8
Weeks 5–8: Mastery Is Emerging
🏆 Mastery Criteria
- Child independently identifies circle, square, and triangle correctly in 4 out of 5 trials
- Child correctly identifies shapes across at least 2 of: different colours, different sizes, different orientations
- Child sorts shapes correctly by form without visual cue support
- Child spontaneously names shapes in the natural environment
- Shape naming is consistent across 3+ sessions without regression
🌟 Generalisation Indicators (The Gold Standard)
- Child identifies shapes in picture books without any prompting
- Child uses shape language with peers or siblings
- Child correctly describes why a shape is what it is: "It's a triangle because it has three corners"
- Shape knowledge is beginning to transfer to letter distinction (b vs d, p vs q)
Maintenance Check: After a 3-day break (holiday, illness), does the child retain shape knowledge? If yes → mastery is consolidating. If no → more practice at the core level before moving forward.
🏆 MASTERY UNLOCKED: Your child has demonstrated visual form perception at a level consistent with their developmental stage. They are ready to advance to the next level.

You Did This. Your Child Grew Because of Your Commitment.
Over the past 5–8 weeks, you have shown up for 20–40 home therapy sessions, created a multi-sensory shape learning environment from scratch, learned to read your child's readiness signals, and watched your child's brain build visual form templates that will serve them in reading, writing, and mathematics for the rest of their life.
"When you started G-677, your child could not consistently distinguish a circle from a square. Today, they can. That is not a small thing. That is a neural pathway that did not exist, now built — by you, at home, with tea and popsicle sticks and sandpaper and love."
🎉 Family Celebration Suggestion
Make a "Shape Recognition Certificate" with your child's name — trace and colour all the shapes they can now identify. Frame it. It is real.
📖 Photo/Journal Prompt
"Today, [child's name] can identify [shapes]. We started on [date]. It took [X] weeks. Here is what I want to remember about this journey: ____"
"From Fear to Mastery. One Technique at a Time." — The Pinnacle Blooms Consortium
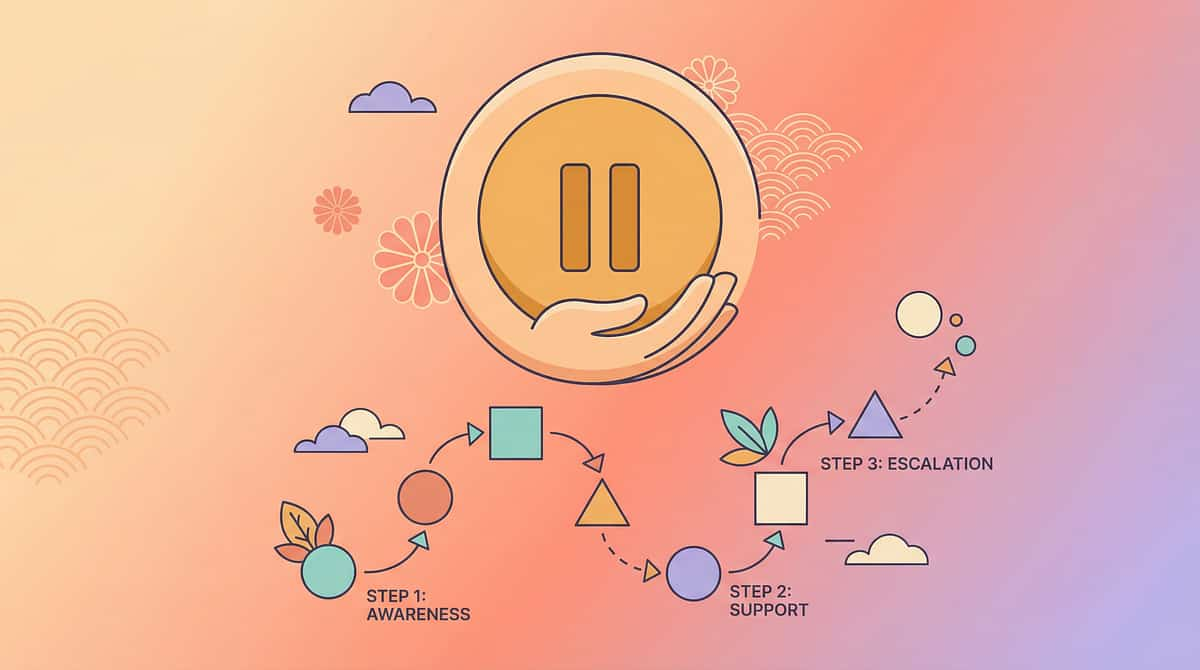
Trust Your Instincts — If Something Feels Wrong, Pause and Ask
Escalation Pathway: Self-monitor → Pinnacle Teleconsult → Pinnacle Centre Visit → Specialist Referral
🔴 Visual Concerns
Child complains of headaches consistently after shape activities. Child squints, covers one eye, or tilts head unusually. Child's eyes do not track shapes consistently.
→ Action: Ophthalmological evaluation before continuing. May indicate refractive error, strabismus, or convergence insufficiency.
🔴 Regression Without Cause
Child who identified 3 shapes now cannot reliably identify any. Sudden loss of previously established shape knowledge.
→ Action: Rule out illness, sleep disruption, and significant life stressor. If persistent (>5 days), teleconsult with Pinnacle therapist.
🔴 Significant Distress
Child consistently cries, self-harms, or has significant meltdowns triggered specifically by shape activities. Child shows avoidance of visual materials generally.
→ Action: Stop this protocol. Consult OT for visual perception/sensory profile evaluation before restarting.
🔴 No Progress by Week 6
Child cannot distinguish circle from square despite 6 weeks of daily multi-sensory practice.
→ Action: Formal visual perception assessment recommended. May indicate deeper visual processing difference requiring specialised OT intervention.
FREE HELPLINE: 9100 181 181 (24x7, 16+ languages)
Explore the Full Cognitive Development Series
The materials you have already purchased for G-677 unlock multiple adjacent techniques. You are not starting from scratch — you are building on what you already own.
1
G-675 — Visual Discrimination Skills
🔵 Foundation | 👁️ Visual | Difficulty: ⭐ Intro
Materials you already own: ✅ Shape sorters, Attribute blocks
2
G-676 — Colour Recognition
🔵 Foundation | 🎨 Visual | Difficulty: ⭐ Intro
Materials you already own: ✅ Attribute blocks
3
G-678 — Size Concepts (Bigger/Smaller)
🔵 Cognitive | 📏 Spatial | Difficulty: ⭐⭐ Core
Materials you already own: ✅ Shape sorters, Attribute blocks
4
G-679 — Pattern Recognition
🔵 Cognitive | 🔢 Pre-Math | Difficulty: ⭐⭐ Core
Materials you already own: ✅ Attribute blocks, Building sticks
5
G-682 — Letter Recognition Readiness
🔵 Pre-Academic | 📖 Literacy | Difficulty: ⭐⭐⭐ Advanced
Materials you already own: ✅ Shape stencils, Tactile cards
6
G-685 — Pre-Writing Shape Production
🔵 Pre-Academic | ✏️ Fine Motor | Difficulty: ⭐⭐⭐ Advanced
Materials you already own: ✅ Stencils, Playdough mats
Zooming Out — Where Shape Recognition Sits in Your Child's Full Journey
Shape Recognition (G-677) sits within the Cognitive Development domain — but it connects outward to nearly every other developmental area your child is growing through simultaneously.
Cognitive Development Domain (Active)
Visual Discrimination (G-675) → Shape Recognition (G-677) → Pattern Recognition (G-679) → Letter Recognition (G-682) → Spatial Reasoning (G-701)
Cross-Domain Connections
Fine Motor (F-domain): Tracing and building shapes
Sensory Processing (A-domain): Tactile and proprioceptive input
Executive Function (J-domain): Categorisation and sorting
Sensory Processing (A-domain): Tactile and proprioceptive input
Executive Function (J-domain): Categorisation and sorting
"This technique is one piece of a larger plan. Isolated techniques produce isolated results. GPT-OS® integrates 70,000+ techniques across 12 domains into one coherent developmental plan for your child."
From the Therapy Room to the Living Room — Families Who Made This Journey
Priya, Mother of Arjun (4 years, ASD Level 1, Hyderabad)
Before:"He could count to 20 but couldn't tell a circle from a square. Circle time at preschool was his worst moment every day. I showed him flashcards until we were both crying."
The Shift:"His OT at Pinnacle Secunderabad introduced the floor tape triangles. He walked the path counting corners. Three sessions later, he corrected ME: 'Mama, that's not a square — it only has THREE sides!' I burst into tears."
After (Week 7): Arjun can identify all basic shapes in multiple colours. He spontaneously notices shapes in his environment. His preschool teacher reported that he now participates in circle time.
Therapist's Notes: Arjun's breakthrough came from whole-body engagement. His proprioceptive system was the strongest pathway. We led with the body, and the brain followed.
Rajan, Father of Meera (3.5 years, Developmental Delay, Chennai)
Before:"Every shape puzzle ended with her throwing pieces. Her therapist said she had form constancy difficulties and I had no idea what that meant."
The Shift:"We started with sandpaper shapes — just the circle, for two weeks. She traced it with her eyes closed. Her face when she understood what 'round' felt like — I cannot describe it."
After (Week 8): Meera correctly identifies and names circle, square, and triangle consistently. She can sort shapes by form despite colour variation. She is now working on rectangle and oval.
Therapist's Notes: Meera's tactile pathway was significantly stronger than her visual pathway. Two weeks of tactile-only instruction produced more progress than four months of visual-only methods.
"Our daughter went from no shape recognition to confidently identifying everything. The multi-sensory methods were a game-changer. She needed to feel and build shapes, not just see them." — Parent of 5-year-old, Pinnacle Network
Illustrative cases. Outcomes vary by child profile, underlying condition, and intervention consistency.

Isolation Is the Enemy of Adherence. Join Your Community.
📱 WhatsApp: Shape Recognition Parent Group
Hundreds of families across India navigating shape learning challenges together — sharing wins, adapting strategies, troubleshooting bad sessions.
💻 Online Community: Pinnacle Parent Forum
Visual perception, shape recognition, and pre-academic readiness discussion threads. OT moderators answer questions weekly.
🏥 Local Parent Meetups
Pinnacle centres across 70+ locations host monthly parent education sessions. Connect with families in your city who are on the same journey.
👥 Peer Mentoring
Connect with a parent who has completed this exact protocol with their child. Real experience, not theory.
Request a Peer Mentor → 9100 181 181
"Consistency Across Caregivers Multiplies Impact." Share this page with everyone in your child's life: grandparents, daycare teacher, school aide. Every person who understands shape learning differently is another facilitator in your child's development.
HELPLINE: 9100 181 181 | 16+ Languages | 24x7
HELPLINE: 9100 181 181 | 16+ Languages | 24x7
Home + Clinic = Maximum Impact
Research consistently shows that home-based intervention produces the strongest outcomes when supervised and guided by clinical professionals. The EverydayTherapyProgramme™ is designed for exactly this integration.
Discipline | When You Need Them | |
Occupational Therapist | Primary — visual perception evaluation, form constancy assessment, multi-sensory protocol design | |
Special Educator | When shape confusion is impacting preschool or school performance | |
Speech-Language Pathologist | When shape vocabulary and categorical language are additionally delayed | |
ABA/BCBA | When the child refuses to engage with shape activities despite all modifications | |
Neurodevelopmental Pediatrician | When shape delay is part of a broader developmental profile |
📹 Teleconsultation
Cannot travel? Our specialists consult via video call across all 70+ languages of our national network.
🗺️ Find Your Nearest Centre
70+ Pinnacle centres across India, with specialist teams in OT, SLP, ABA, SpEd, and NeuroDev Pediatrics.
FREE HELPLINE: 9100 181 181 (24x7, 16+ languages)
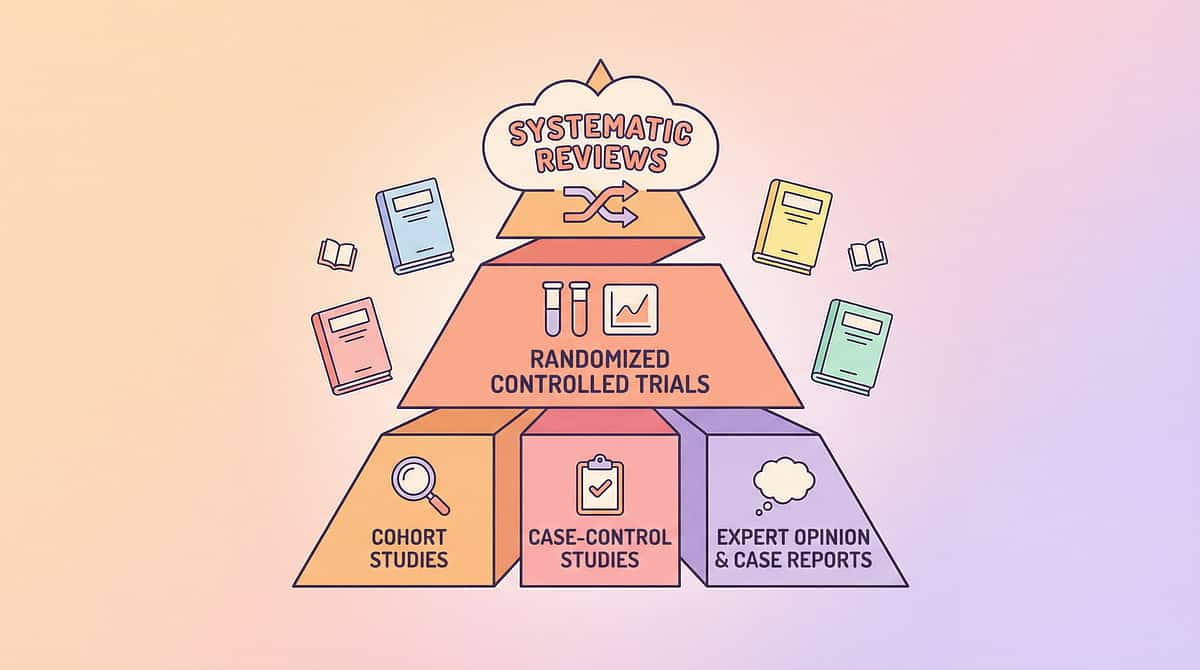
Deeper Reading for the Curious Parent — The Evidence Base for G-677
1. PRISMA Systematic Review (2024) — Level I Evidence
"Sensory integration intervention for children with autism: a systematic review and evidence-based practice report." 16 studies, 2013–2023. Confirms multi-sensory intervention as evidence-based for visual-cognitive development in ASD.
2. Meta-Analysis — World J Clin Cases (2024) — Level I Evidence
"Effectiveness of sensory integration therapy in children with ASD." 24 studies. Demonstrates measurable improvement in visual-spatial skills, form perception, and pre-academic readiness.
3. WHO/UNICEF Care for Child Development
Implemented in 54 LMICs. Evidence base for caregiver-administered early intervention using household materials.
4. Indian RCT — Indian J Pediatr (2019) — Level II Evidence
Padmanabha et al. Home-based multi-sensory intervention with parent training demonstrated significant developmental outcomes across cognitive and sensory domains.
5. NCAEP Evidence-Based Practices (2020)
National Clearinghouse on Autism Evidence and Practice confirms visual supports and video modelling as evidence-based practices for ASD across multiple developmental domains.

Watch the Reel That Brought You Here
Reel Metadata
- Reel ID: G-677
- Title: 9 Materials That Help With Shape Recognition
- Series: Cognitive Development
- Episode: 677 of 999
- Domain: G — Cognitive Development | COG-SHAPE
- Duration: 75–85 seconds
In this Reel, our consortium of OT, SLP, ABA, SpEd, and NeuroDev specialists introduce the 9 materials that build shape recognition through multiple sensory pathways. Each material is demonstrated in a home setting by a parent.
What the Reel Covers
- 3D Shape Sorters — physical trial and feedback
- Tactile Shape Cards — shapes you can feel, not just see
- Building Sticks & Connectors — construct to understand
- Templates & Stencils — trace to internalise
- Attribute Blocks — form constancy across colour and size
- Knobbed Shape Puzzles — match, place, succeed
- Whole-Body Shapes — become the shape to know the shape
- Sorting Trays with Visual Cues — match to silhouettes
- Playdough Shape Mats — build shapes with your hands

Consistency Across Caregivers Multiplies Impact — Share This
If only one parent executes the shape recognition protocol, your child receives shape therapy for 15–25 minutes per day. If grandparents, school teachers, and other caregivers understand the same principles, the child receives shape learning reinforcement throughout the day — in every meal, every walk, every shared moment.
"Explain to Grandparents" Version
"Your grandchild is learning to tell shapes apart — circles, squares, triangles. Their brain needs to feel shapes, not just see them. When you give them food, say the shape: 'Here's your round roti.' When you see a window, say 'rectangle.' When they sort shapes with you, let them try even when it's wrong — the trying is what teaches."
Teacher/School Communication Template
"Dear [Teacher's Name], [Child's name] is currently working on shape recognition using a multi-sensory approach at home. Their strongest modality is [tactile/visual/kinesthetic]. In the classroom, please: label shapes when encountered, allow tactile exploration of shape manipulatives, and celebrate correct identification warmly. Thank you for partnering with us."
📱 Share on WhatsApp
unknown link
📄 Download Family Guide
"Shape Recognition at Home — G-677 Family Guide" (1-page PDF). Available in: English, Telugu, Hindi, Tamil, Kannada, Malayalam, Marathi, Bengali.
🔗 Copy Link
techniques.pinnacleblooms.org/cognitive-development/shape-recognition-G-677
HELPLINE: 9100 181 181 | 16+ Languages

Frequently Asked Questions — G-677: Shape Recognition
Q1: My child can do shapes on the iPad but not in real life. Why?
Digital shape recognition and real-world form constancy are processed differently in the brain. Many children with visual processing differences excel at 2D digital matching but cannot translate this to 3D real-world objects. This protocol specifically targets the 3D-to-2D bridge. Focus on Material 1 (3D sorters) and Material 8 (sorting trays) — these explicitly train that translation.
Q2: At what age should I be worried about shape recognition delays?
If a child cannot identify circle, square, and triangle by age 4, that warrants a conversation with your paediatrician or OT. If a child cannot identify ANY basic shapes by age 3.5, an early intervention evaluation is recommended. Earlier referral is always better than waiting. Call 9100 181 181 for a free screening.
Q3: My child identifies shapes correctly in therapy but not at home. What's wrong?
This is the "generalisation gap" — a very common phenomenon in developmental learning. Skills acquired in one setting don't automatically transfer. This is why we emphasise: teach shapes at home (not just clinic), use shapes in natural daily contexts (Card 22), and involve all caregivers (Card 37).
Q4: Can I do this without being an OT or therapist?
Yes. This protocol is specifically designed for parent implementation. Thousands of Pinnacle families implement these techniques at home with OT consultation — not OT supervision of every session. The role of the professional is to guide and monitor; your role is to execute daily. You are the most important therapist in your child's life.

Frequently Asked Questions — Continued
Q5: How is shape recognition related to reading?
Letters are shapes. The ability to distinguish 'b' from 'd' requires the same visual discrimination skill as distinguishing a circle from an oval. Form constancy — recognising a shape even when it changes size or orientation — is directly prerequisite to letter recognition. Strong shape recognition → stronger letter discrimination → fewer reading difficulties. This is not theoretical — it's measurable.
Q6: We've done 10 sessions with no progress. Should I continue?
10 sessions without ANY progress is a clinical signal. Not a failure — a signal. Please call 9100 181 181 or book a teleconsult. The protocol may need adjustment, the child may need a formal visual perception evaluation, or a different modality approach may be indicated. Do not push through without guidance when there is no progress.
Q7: Can I combine multiple materials in one session?
Yes — and in fact, research supports multi-modal sessions. However: introduce one new material at a time. Once the child is comfortable with a material (2–3 sessions), you can pair it with a second material in the same session. Never introduce 3+ new materials simultaneously.
Q8: My child hates being touched. How do I do the tactile activities?
For children with tactile defensiveness, begin with visual observation of the tactile cards before touching. Let the child touch materials themselves on their own terms — never guide hand-over-hand if the child resists. Use a softer texture first (felt instead of sandpaper). The whole-body activities (floor tape shapes) are completely non-tactile and may be the better starting point. Consult your OT for a sensory profile assessment.
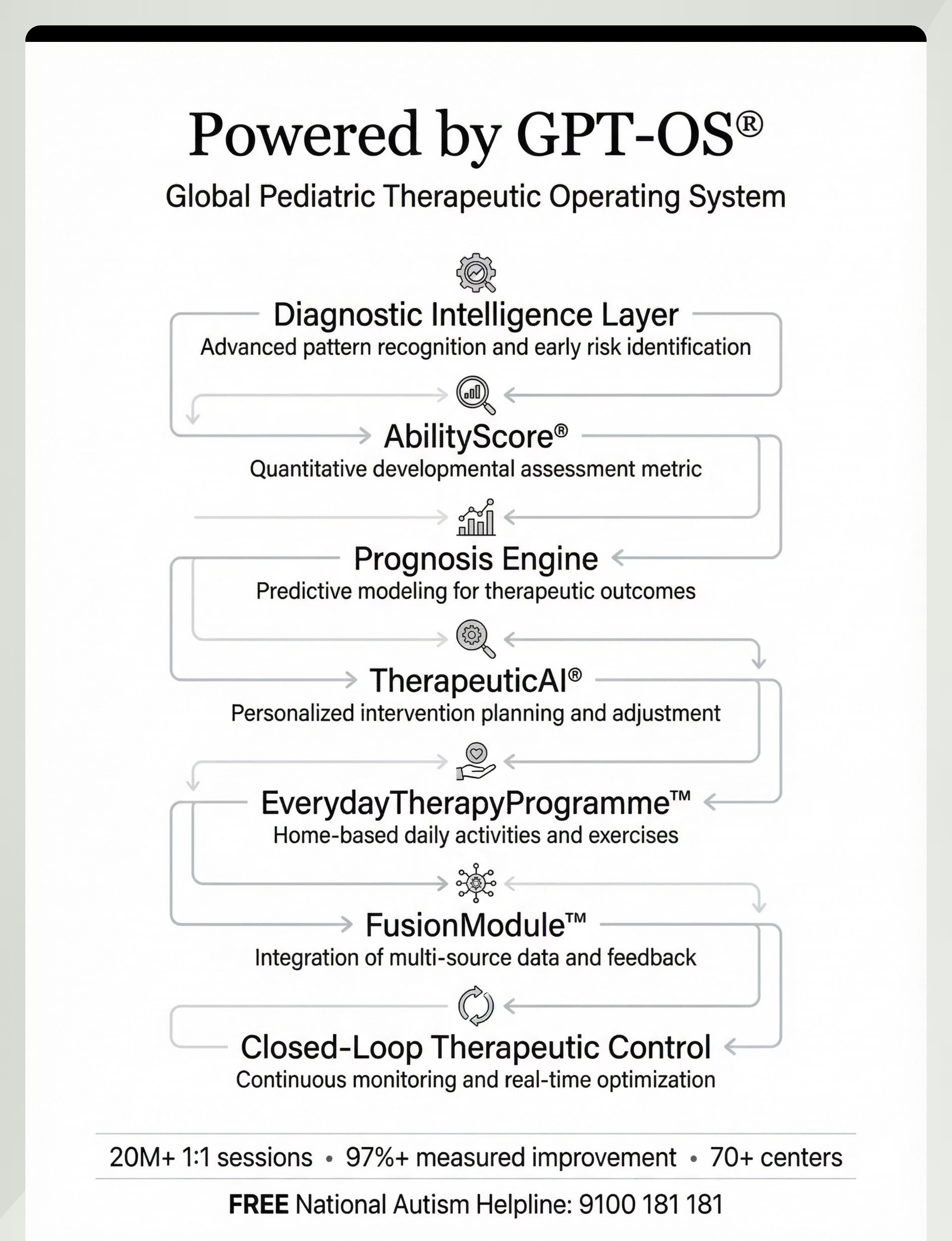
Preview of 9 materials that help with shape recognition Therapy Material
Below is a visual preview of 9 materials that help with shape recognition therapy material. The pages shown help educators, therapists, and caregivers understand the structure and content of the resource before use. Materials should be used under appropriate professional guidance.



















Share this resource
Help others discover thisLink copied!

From Fear to Mastery. One Technique at a Time.
Pinnacle Blooms Network®
Built by Mothers. Engineered as a System.
Occupational Therapy • Speech-Language Pathology • Applied Behaviour Analysis (BCBA) • Special Education • Neurodevelopmental Pediatrics • Clinical Research Operations (CRO)
Partners: WHO | UNICEF | DPIIT | MSME | NAEYC | NCAEP | BACB-aligned
20M+ Therapy Sessions | 97%+ Measured Improvement | 70+ Centres | 70+ Countries Served
The Mission
Pinnacle Blooms Network® exists to transform every Indian home into a proven, scientific, 24x7, personalised, multi-sensory, multi-disciplinary paediatric therapy environment — empowering families to be the most powerful agent of their child's development.
This is not a service. This is an operating system for child development — at population scale.
Site Navigation
CIN | DPIIT | MSME | GSTIN | |
U74999TG2016PTC113063 | DIPP8651 | TS20F0009606 | 36AAGCB9722P1Z2 |
This content is educational and informational in nature. It does not constitute medical advice and does not replace individualised assessment and intervention from qualified developmental specialists, occupational therapists, speech-language pathologists, or special educators. Shape recognition difficulties may indicate underlying visual perception, cognitive, or developmental differences that require professional evaluation. Individual results vary based on child profile, underlying conditions, intervention consistency, and other factors.
© 2025–2026 Pinnacle Blooms Network® — Unit of Bharath Healthcare Laboratories Pvt. Ltd. All rights reserved. GPT-OS®, AbilityScore®, TherapeuticAI®, FusionModule™, and EverydayTherapyProgramme™ are proprietary systems of Pinnacle Blooms Network®. Unauthorised reproduction prohibited.
G-677 | Cognitive Development Series | techniques.pinnacleblooms.org
