
9 Materials That Help With Sensory Sleep Environment
When your child's senses won't let them rest — 9 clinician-validated materials that transform your child's bedroom into a sensory-supportive sleep environment. Backed by 20M+ therapy sessions.
Technique D-450
Domain: Sleep / Sensory Processing / OT

"Their body is exhausted. Their senses won't allow rest."
The tag. The light. The sound under the door. The way the sheet feels. Things you don't register — your child's nervous system catalogs every single one.
Every evening you watch your child lie in bed — tired, but unable to settle. You've removed every obvious distraction. Still, they're awake. Adjusting covers. Turning. Noticing things you can't even detect.
You are not failing. Their sensory system is not misbehaving. It is simply wired differently — and bedtime is when that difference matters most.
📞 FREE National Autism Helpline: 9100 181 181 | Available 24×7 | 16+ Languages

Millions of Families Navigate This Exact Bedtime
Sensory sleep difficulties are not parental failure, child noncompliance, or behavioral defiance. They are the predictable outcome of a nervous system that processes sensory input with greater intensity and precision than neurotypical systems. Every parent on this page is already doing their best.
Sensory Processing Difficulties
80% of children with ASD experience sensory processing difficulties — PRISMA Systematic Review, Children (2024) PMC11506176
Sleep Difficulties in Autism
80% of children with autism have significant sleep difficulties, with sensory factors being a primary driver — Journal of Autism & Developmental Disorders
Therapy Sessions
21M+ sessions across Pinnacle Network demonstrate sleep-sensory intervention efficacy — Pinnacle Blooms Network® Real-World Evidence Database
PMC11506176
PMC10955541
WHO NCF 2018
The Neuroscience, Translated
Thalamus — The Sensory Gatekeeper: In neurotypical brains, the thalamus filters sensory signals before they reach awareness. In sensory-processing differences, this gating is reduced — more signals reach the cortex at full amplitude.
Reticular Activating System — The Alertness Switch: At bedtime, this system needs to downshift. Unfiltered sensory input — a light, a sound, a tag — keeps it activated. The brain cannot shift to sleep mode while the RAS is signaling "threat/novelty."
Amygdala — The Alarm Centre: Sensory overload activates threat pathways even when no actual threat exists. This triggers cortisol release — the opposite of what sleep requires.
What's Happening in Your Child's Brain
This is a wiring difference, not a behavior choice. The bedroom environment can be engineered to work with this nervous system, not against it.
Frontiers in Integrative Neuroscience (2020)

Where This Sits in Development
Understanding your child's developmental stage helps you calibrate expectations — and recognize that the window of highest intervention responsiveness is right now.
Ages 0–2
Sensory regulation develops. Foundation period — sensory differences first emerge.
Ages 2–4 ★
Sleep consolidation, routine dependence. Peak environmental sensitivity — your child may be here.
Ages 4–7
Self-regulation emerging. Modifiable period — highest intervention responsiveness.
Ages 7–10
Growing self-awareness. Child can begin articulating sensory needs.
Ages 10–12
Self-advocacy skills. Child leads their own sensory environment design.
Sensory processing differences respond to environmental engineering. The window of greatest impact is now — and the tools are simpler than you think.

Clinically Validated. Home-Applicable. Parent-Proven.
Evidence Grade: Level I-A
Systematic Review + RCT Support
PRISMA Systematic Review (Children, 2024)
16 studies, 2013–2023. Sensory Integration Intervention meets Level I Evidence criteria as evidence-based practice for ASD. Environmental sensory modification shows significant sleep onset and duration improvements.
PubMed: PMC11506176
Meta-Analysis (World J Clin Cases, 2024)
24 studies — Sensory integration therapy effectively promotes adaptive behavior, sensory processing regulation, and daily living skills including sleep.
PubMed: PMC10955541
Indian RCT — Padmanabha et al. (2019)
Home-based sensory interventions demonstrate significant outcomes in Indian pediatric population — directly applicable to family-delivered protocols.
DOI: 10.1007/s12098-018-2747-4
NCAEP Evidence-Based Practices (2020)
Environmental modifications and sensory-based interventions classified as evidence-based practices for autism across all age groups.
NCAEP 2020
📞 FREE National Autism Helpline: 9100 181 181

What Is Sensory Sleep Environment Engineering?
The Technique Defined
Parent Alias: "Building a bedroom your child's nervous system can actually rest in."
Sensory Sleep Environment Engineering is the systematic, evidence-based modification of a child's bedroom across all sensory modalities — visual, auditory, tactile, proprioceptive, olfactory, and thermal — to reduce sensory barriers to sleep and provide sensory inputs that support nervous system down-regulation.
Unlike generic sleep hygiene advice, this approach is individualized to the child's specific sensory profile. The bedroom is treated as therapeutic infrastructure, not merely a sleeping space.
Domain D — Sleep & Self-Care
Sensory Processing
OT Lead
Technique Specs
Age Range: 2–12 years
Frequency: Nightly — ongoing environmental management
Setup Time: 15–30 min initial | 2 min nightly maintenance
Professional Lead: Occupational Therapist (OT)
Home Delivery: Full — parent/caregiver executable
📞9100 181 181 — FREE Autism Helpline
Who Uses This Technique?
This technique crosses therapy boundaries because the brain doesn't organize by therapy type. At Pinnacle, 5 disciplines converge through FusionModule™ to ensure every aspect of your child's sleep is addressed.
Occupational Therapist (Primary Lead)
Conducts formal sensory profile assessment (Sensory Profile 2/SPM), designs individualized environmental modification protocol, trains caregivers, monitors tolerance progression.
BCBA / Behavioral Analyst
Addresses behavioral sleep patterns co-occurring with sensory issues, designs reinforcement systems, conducts functional assessment when sleep avoidance has behavioral function.
NeuroDev Pediatrician
Rules out medical causes (sleep apnea, restless legs, melatonin deficiency), provides diagnostic clarity on ASD/ADHD, monitors medical aspects of sleep quality.
Special Educator
Extends sensory environment principles to school rest periods, trains classroom staff on portable sensory supports, aligns home and school sensory strategies.
What This Technique Targets
Precision over guesswork. Here's exactly what we're changing — from primary sleep onset targets to long-term developmental gains your child builds over weeks of consistent support.
🎯 Primary Target
Sleep Onset Time — Reducing time from lights out to sleep from 1–3 hours (common in sensory-impacted children) to 15–30 minutes through environmental sensory alignment.
Secondary Targets
Reduction in night wakings triggered by environmental inputs. Elimination of bedtime behavioral resistance. Decrease in sleep-related anxiety about darkness, sounds, and textures.
Developmental Gains
Daytime emotional regulation. Learning consolidation (sleep is the primary memory consolidation window). Family stress reduction. Child's self-awareness of their own sensory needs.
✓ Child settled in bed within 20 minutes
✓ Fewer position changes and cover adjustments
✓ No distress vocalizations about environmental sensory factors
✓ Child requests specific sensory supports — self-advocacy emerging
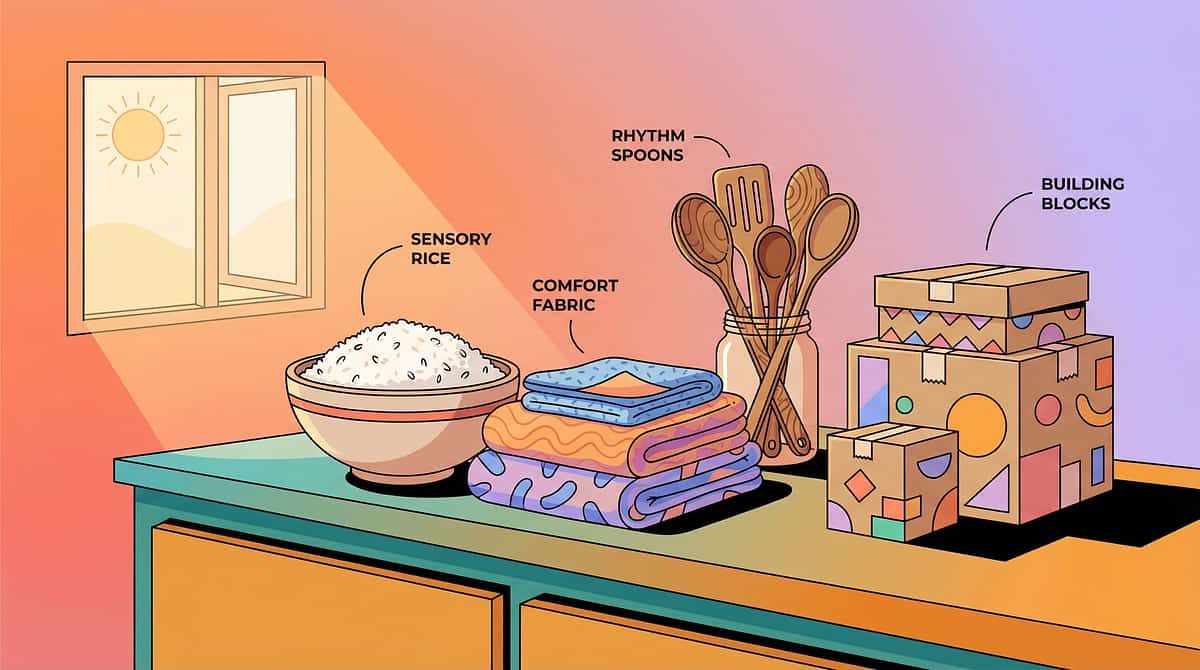
9 Materials. 6 Sensory Modalities. One Sleeping Child.
Each material addresses a specific sensory channel. Together, they systematically reduce every barrier your child's nervous system encounters at bedtime.
# | Material | Modality | Price Range |
1 | 🌑 Blackout Curtains | Visual | ₹1,000–5,000 |
2 | 🔊 White Noise Machine | Auditory | ₹500–3,000 |
3 | 👕 Sensory-Friendly Sleepwear | Tactile | ₹500–2,000 |
4 | 🛏️ Temperature-Regulating Bedding | Tactile/Thermal | ₹1,000–5,000 |
5 | 🪨 Weighted Blanket (10% body weight) | Proprioceptive | ₹2,000–6,000 |
6 | 🧥 Compression Sleepwear / Sleep Sack | Proprioceptive | ₹800–3,000 |
7 | 🟠 Red/Orange Nightlight (Circadian-Friendly) | Visual/Circadian | ₹200–1,000 |
8 | 🌿 Calming Scent Diffuser (Lavender) | Olfactory | ₹500–2,000 |
9 | 🛌 Body Pillow / Positioning Support | Proprioceptive | ₹500–2,000 |
Starter Kit Recommendation: Essential 3 to begin — Light Management + Sound Management + Sensory Sleepwear. Total starting investment: ₹1,200–7,000 depending on child's profile.

DIY & Zero-Cost Alternatives — Start Tonight
Every material on the list has a ₹0 version. WHO Equity Principle: Evidence-based interventions must be accessible regardless of economic status. Sensory environment engineering requires intelligence, not expenditure.
Material | Commercial Option | DIY / ₹0 Alternative |
Blackout Curtains | True blackout curtains ₹1,000+ | Tape dark bedsheets over window frame. Cover indicator lights with black electrical tape. |
White Noise Machine | Dedicated device ₹500+ | Free white noise YouTube or app on old phone placed outside room. Fan (₹0 if owned). |
Sensory-Friendly Sleepwear | Specialty seamless ₹500+ | Cut all tags from existing pajamas. Turn inside out so seams are external. Wash repeatedly to soften. |
Temperature Bedding | Bamboo/cooling sheets ₹1,000+ | Layer thin cotton sheets for adjustment. Remove one layer when too hot. |
Weighted Blanket | Commercial ₹2,000+ | Fill a pillowcase with dry lentils/rice to 10% of body weight. Use thin outer pillowcase for comfort. |
Compression Sleepwear | Specialty ₹800+ | Snug-fitting cotton leggings + long-sleeve shirt. Or swimming suit under pajamas. |
Red Nightlight | Specialty ₹200+ | Red cellophane over existing nightlight. Red LED bulb in lamp. |
Scent Diffuser | Cool-mist ₹500+ | Cotton ball with 1 drop lavender near (not on) pillow. Only if no olfactory sensitivity. |
Body Pillow | Large pillow ₹500+ | Roll existing blanket into a long cylinder. Sew shut inside a pillowcase. |
A black electrical tape strip over a smoke detector indicator light can transform a child's sleep more than a ₹5,000 purchase.

Safety First — Read This Before You Modify Anything
Some configurations are not safe for all children. Review this carefully before your first night of implementation. When in doubt, call our helpline before proceeding.
🔴 STOP — Absolute Contraindications
• Weighted blankets: NEVER for children under 2 years
• NEVER if child cannot remove independently
• NEVER for children with respiratory, cardiac, or mobility conditions
• Compression sleepwear: NOT for children who show aversion to pressure
• Scent diffuser: NEVER if child has asthma, respiratory issues, or olfactory hypersensitivity
• Body pillow: Ensure no suffocation risk for children under 3
• NEVER if child cannot remove independently
• NEVER for children with respiratory, cardiac, or mobility conditions
• Compression sleepwear: NOT for children who show aversion to pressure
• Scent diffuser: NEVER if child has asthma, respiratory issues, or olfactory hypersensitivity
• Body pillow: Ensure no suffocation risk for children under 3
🟡 CAUTION — Proceed Carefully
• Introduce ONE change at a time — changing everything simultaneously makes it impossible to identify what helped
• Weighted blanket: Start at 8% body weight, assess, increase to 10% if tolerated
• Scent: Start with ONE drop in diffuser
• Red light: Ensure it is not shining directly in child's eyes
• Weighted blanket: Start at 8% body weight, assess, increase to 10% if tolerated
• Scent: Start with ONE drop in diffuser
• Red light: Ensure it is not shining directly in child's eyes
🟢 SAFE — For All Children
• Blackout curtains (standard window installation)
• White noise at safe volume (under 50 decibels at child's ear)
• Sensory-friendly sleepwear (check no residual irritants)
• Temperature-regulating bedding (ensure no overheating)
• White noise at safe volume (under 50 decibels at child's ear)
• Sensory-friendly sleepwear (check no residual irritants)
• Temperature-regulating bedding (ensure no overheating)
If child shows increased distress, signs of respiratory difficulty, or attempts to remove materials forcefully — stop immediately. The intervention needs adjustment, not persistence.
📞 9100 181 181 — FREE Autism Helpline | Consult before beginning if child has medical complexities
📞 9100 181 181 — FREE Autism Helpline | Consult before beginning if child has medical complexities

Set Up Your Space — The Sensory Bedroom Audit
Do this before night one. A systematic room-by-room review ensures every sensory input is controlled before your child enters the space. Use this as your pre-sleep checklist every evening.
Room Setup Positions
[WINDOW] ← Blackout curtains + check for light leaks at edges
[DOOR] ← Check hallway light leak — add draft stopper
[BEDSIDE] ← White noise machine positioned toward door/window
[BED POSITION] ← Away from direct window line if light-sensitive
[NIGHTLIGHT] ← Red/orange, positioned across room, not facing bed
[DEVICES] ← Cover all indicator lights (router, AC, TV standby)
[DIFFUSER] ← Near door — never next to child's face
[BODY PILLOW] ← Positioned alongside child's preferred sleep side
Pre-Sleep Sensory Checklist
□ Visual: All uncontrolled light sources eliminated or controlled
□ Auditory: White noise on, volume calibrated, positioned correctly
□ Tactile: Sensory-safe sleepwear confirmed, bedding layers appropriate
□ Proprioceptive: Weighted blanket / compression / body pillow positioned per child's profile
Temperature Target: 18–22°C (65–72°F) — optimal sleep temperature for children
What to Remove: Toys that light up, make sounds, or spin. Screens (even in standby). Strong-scented items if child has olfactory sensitivity. Cluttered visual environment — this can increase arousal.

Is Your Child Ready? — The 60-Second Readiness Gate
The best bedtime session is one that starts when the child's nervous system is ready — not when the clock says it should be. Run this quick check before beginning the nightly sequence.
✅ GO — All 5 for Green Light
☑ Child is fed — hunger is a significant arousal factor
☑ Physical movement in past 2–3 hours (not in last 30 minutes)
☑ No major distress event in past 60 minutes
☑ Room setup completed (Card 12 checklist done)
☑ Child showing tiredness signs (yawning, reduced activity, rubbing eyes)
☑ Physical movement in past 2–3 hours (not in last 30 minutes)
☑ No major distress event in past 60 minutes
☑ Room setup completed (Card 12 checklist done)
☑ Child showing tiredness signs (yawning, reduced activity, rubbing eyes)
⚠️ MODIFY — Adjust the Session
⚠ Child is significantly dysregulated — run a 10-minute calming sequence first
⚠ Room temperature not yet ideal — adjust before starting
⚠ A new element is being introduced tonight for the first time — preview with child awake
⚠ Room temperature not yet ideal — adjust before starting
⚠ A new element is being introduced tonight for the first time — preview with child awake
🛑 POSTPONE — Tonight Is Maintenance Only
Child is ill, in pain, or has had a significantly traumatic day. Familiar environment only tonight. No new materials. Comfort and consistency over protocol advancement.

Step 1: The Sensory Invitation
Not a Command — A Welcome
Children with sensory processing differences respond to predictability and agency. Demanding sleep creates resistance. Inviting comfort creates cooperation.
"It's time to help your body rest. Your room is all set up to feel just right for you — let's go check how it feels tonight."
The Sensory Preview Ritual (3 Minutes)
Enter the bedroom together
Child touches bedding — "Does this feel right tonight?"
Child checks white noise — "Does this sound feel good?"
Check light level together — "Is this the right amount of dark?"
Child chooses weighted blanket OR body pillow OR neither — child-led selection
The sensory preview gives the child agency and reduces anticipatory anxiety. It also provides you with real-time sensory feedback about what the child needs tonight — sensory needs vary night to night.

Step 2: The Wind-Down Bridge
From Day to Rest
Children with sensory processing differences often cannot switch from daytime arousal to sleep-readiness instantaneously. The nervous system needs a 15–20 minute "descent ramp." These four components work together to signal to the brain that rest is coming.
1. Proprioceptive Loading (5 min)
Heavy work to joints and muscles helps the nervous system down-regulate. Options: carrying heavy laundry basket to room, "sandwich squeezes" between pillows, pushing against the wall, bear hugs.
2. Auditory Transition (starts now)
White noise machine turned on during wind-down — not just at sleep time. This conditions the brain to associate the sound with relaxation before the child even reaches the bedroom.
3. Visual Dimming (5 min before bed)
All bright lights off. Only red/orange nightlight or dim lamp on. Blue-spectrum light eliminated — blue light suppresses melatonin and delays sleep onset significantly.
4. Tactile Preparation (2 min)
Sensory-friendly sleepwear on. Check comfort. Child provides feedback. This ritual communicates to the nervous system: the transition to rest has officially begun.
"Your body is getting ready to rest. The room is all the right feeling for you."

Step 3: The Sensory Environment Activation Sequence
The core therapeutic action: systematic, modality-by-modality sensory environment confirmation. This takes 3–5 minutes and ensures every sensory input is calibrated to your child's profile for tonight.
1. Visual (30 sec)
Blackout curtains fully drawn — check edges for light leaks. Red/orange nightlight confirmed on if needed. All device indicator lights covered.
2. Auditory (30 sec)
White noise confirmed on at calibrated volume. Child confirms "the sound feels okay."
3. Tactile (1 min)
Child in sensory-friendly sleepwear in bed. Sheets confirmed comfortable. Blanket layers appropriate for tonight's temperature.
4. Proprioceptive (1 min)
Weighted blanket OR compression sleepwear OR body pillow — based on child's choice tonight. Child confirms "this feels right."
5. Olfactory (30 sec)
Diffuser on if appropriate for this child — never for olfactory-sensitive children. Only if a conditioned sleep cue has been established.
"Your room is all set up for your body to rest. Everything feels right tonight."

Step 4: The Settling Period
10–15 Minutes to Safety
The nervous system needs 10–15 minutes to believe the environment is safe. This is not inaction — this is the most important phase of the protocol.
Minutes 0–5
Parent remains nearby, not in bed. Minimal interaction. White noise active. Brief calm responses if child seeks interaction: "Everything is set for you. Your body is resting."
Minutes 5–10
Most children show visible physical relaxation — decreased limb movement, slower breathing, fewer cover adjustments. The parasympathetic shift is occurring.
Minutes 10–15
Sleep onset typically occurs for children in properly calibrated sensory environments. If not by 15 minutes, assess and troubleshoot (see Troubleshooting card).
Transition Exit Script: "I'm going to step just outside. Your room is all set. I'll check on you in two minutes." Return as promised, then gradually increase the interval. Predictability is the foundation of trust.

Step 5: Reinforce & Celebrate
Reinforce Cooperation, Not Just Outcome
ABA reinforcement must occur within 3 seconds of the target behavior — settling cooperatively, accepting the environment, staying in bed. The goal is to strengthen the association, not create bedtime excitement.
Natural Reinforcers (Preferred)
• Verbal praise delivered calmly (not excitedly — excitement re-activates arousal): "Your body is resting so well. You're doing beautifully."
• Physical contact if tactilely acceptable: gentle hand on shoulder
• Verbal narrative: "I can see your body getting nice and heavy and comfortable."
Token Economy (If System Is in Place)
Morning-delivered token/sticker for successful settling — awarded at breakfast, not at bedtime, to avoid arousal.
What NOT to Do
❌ High-energy celebration at bedtime — re-activates the RAS
❌ Promise rewards contingent on staying asleep — not controllable by child, creates anxiety
❌ Multiple goodnight cycles — creates behaviorally maintained bedtime avoidance
Every night your child settles a little more readily in the sensory-calibrated environment — that is neural pathway formation. You are building their nervous system's capacity to rest.

Step 6: The Cool-Down & Exit
No Abrupt Endings
How you leave the room matters as much as how you set it up. A graduated withdrawal builds the child's trust in the environment itself — rather than in your physical presence alone.
Phase 1 — Physical Presence
Sitting outside doorway, visible but not engaging. Duration: 5–10 minutes. Your presence reassures without reinforcing dependency.
Phase 2 — Scheduled Check-Ins
Brief returns every 10–15 minutes as promised. Duration: 30 seconds. Script: "Everything's still set for your rest. Goodnight." Predictability prevents anxiety.
Phase 3 — Independent Settling
Gradual extension of check-in intervals. Most children within 2–3 weeks of consistent sensory environment establish independent settling.
The Transition Object Bridge: A consistent comfort object (soft toy, ₹425 on Amazon.in) bridges the parent's physical absence — it carries the association of safety and signals continuity even when you're not in the room.

Capture the Data — Right Now
60 seconds of data tonight prevents months of guessing. The pattern across 7 nights shows you whether sensory modifications are working — and gives your OT the precision information needed for targeted adjustments.
Sleep Onset Time
Time child was in bed → Time visible settling observed. Record as minutes: e.g., "22 minutes tonight."
Sensory Environment Rating (1–5)
1 = significant distress about environmental factors. 5 = settled with no sensory complaints. Circle tonight's rating.
Any New Sensory Issue?
Was there a new sensory complaint tonight? (New light source? Sound? Clothing issue?) Yes / No — if Yes, note what it was.
GPT-OS® Data Flow
Your tracking data → TherapeuticAI® → Pattern recognition across 20M+ sessions → Personalized protocol adjustment → EverydayTherapyProgramme™ update → Next week's recommendations
Why This Data Matters
Without data, you're estimating. With data, your OT can make precision adjustments at your next appointment. Your tracking also contributes to population-level learning — helping every child like yours, globally.
📞 9100 181 181 — Link to GPT-OS® home tracking tools | Download D-450 Sleep Sensory Tracker
What If It Didn't Go As Planned?
Most nights won't be perfect. Session abandonment is not failure — it is data. Every difficult night teaches you something about what your child's nervous system needs. Here is the exact fix for each common scenario.
Child identified a new sensory issue we hadn't addressed
Why: As other sensory barriers are removed, new ones become detectable — this means previous modifications are working. Fix: Log it. Address tomorrow — one change at a time.
Child rejected the weighted blanket tonight
Why: Sensory needs fluctuate with stress levels, illness, emotional state. Fix: Offer choice — blanket, compression, body pillow, or none. Do not insist.
Child is more distressed in the modified environment
Why: A change that removes a familiar sensory cue can initially increase arousal. Fix: Introduce changes more gradually. Revert for 2 nights. Introduce one element at a time with 3-night assessment periods.
White noise is disturbing child more than helping
Why: Some auditorily sensitive children are more sensitive to sound than silence. Fix: Try pink noise vs white vs brown vs fan. Try significantly lower volume. Trial silence as a test.

Adapt & Personalize — Your Child's Profile Is Unique
Your child's sensory profile is one-of-a-kind. Their bedroom environment must be too. Use these axes to calibrate your setup to their specific pattern of over- and under-responsiveness across each sensory channel.
👁️ Visual Sensitivity
Light Avoider: Maximum darkness — blackout curtains only
Light Seeker: Blackout + red/orange nightlight
Light Seeker: Blackout + red/orange nightlight
🔊 Auditory Sensitivity
Sound Avoider: White noise masking essential
Sound Neutral: Optional / fan only
Sound Neutral: Optional / fan only
👕 Tactile Sensitivity
Tactile Avoider: Seamless, tagless, loose — sensory-friendly sleepwear + light blanket
Tactile Seeker: Compression sleepwear + weighted blanket
Tactile Seeker: Compression sleepwear + weighted blanket
🪨 Proprioceptive Needs
Doesn't Seek Pressure: Body pillow / light contact
Strongly Seeks Pressure: Weighted blanket + compression combination
Strongly Seeks Pressure: Weighted blanket + compression combination
🌿 Olfactory Profile
Smell Sensitive: Scent-free environment — NO diffuser
Smell Neutral: Lavender diffuser as conditioned cue
Smell Neutral: Lavender diffuser as conditioned cue
Age Modifications: Ages 2–4: Simpler setup, more parental presence, slower graduated withdrawal. Ages 5–8: Child begins selecting materials, increasing agency. Ages 9–12: Child leads sensory audit, self-advocacy training begins.

Weeks 1–2: You Are Building the Neural Association
Progress: 15%
It doesn't feel dramatic yet — but it is. Weeks 1–2 are about establishing the foundation: acceptance, familiarity, and the very beginning of the brain's association between this environment and safety.
What Progress Looks Like in Weeks 1–2
✓ Child accepts the sensory environment without major protest
✓ Fewer verbal complaints about specific sensory elements
✓ Sleep onset time has decreased by even 5–10 minutes — this is measurable progress
✓ Child begins pointing to preferred elements: "I want the heavy blanket tonight"
What Is Not Yet Progress (And That's Okay)
• Consistent fast settling — not expected yet
• Child sleeping through the night — this comes later
• Child not requesting parental presence — this takes weeks
If your child lies under the weighted blanket for 3 more minutes without adjusting compared to last week — that is real progress. That is neural pathway formation.

Weeks 3–4: The Nervous System Begins to Trust
Progress: 40%
Consolidation phase. The nervous system is beginning to recognize this environment as safe — and that recognition is starting to happen faster each night.
✓ Child begins requesting specific sensory elements proactively: "White noise on, please"
✓ Bedtime resistance reducing — less negotiation, fewer reasons to delay
✓ Sleep onset time now consistently under 30 minutes
✓ Parent exit accepted within 5 minutes more readily than Week 1
✓ Night wakings due to environmental sensory triggers decreasing
When a child starts requesting their sensory environment elements — they are demonstrating that their brain has successfully associated those inputs with safety and rest. This is the moment the environment begins working autonomously.
Parent Milestone: You may notice you feel more confident too. Bedtime is no longer dread — it is a protocol. That calm confidence communicates safety to your child.

Weeks 5–8: Sleep Independence Is Emerging
Progress: 70%
The environment is doing its job. Mastery is not the absence of sensory needs — it is your child knowing those needs and meeting them with growing independence.
Mastery Emergence Indicators
✓ Sleep onset consistently under 20 minutes
✓ Child sets up their own environment — chooses blanket, checks noise, adjusts light
✓ Night wakings from sensory causes rare or eliminated
✓ Child can articulate: "I need the heavy blanket because I feel wiggly"
✓ Child sets up their own environment — chooses blanket, checks noise, adjusts light
✓ Night wakings from sensory causes rare or eliminated
✓ Child can articulate: "I need the heavy blanket because I feel wiggly"
Generalization Beginning
✓ Sensory environment principles beginning to generalize — child advocates for similar setups elsewhere: hotel, grandparents' house, school rest periods
"Our daughter doesn't need us to set up her room anymore. She turns on her white noise, gets under her weighted blanket, arranges her body pillow, and is asleep in 15 minutes. Six months ago, bedtime took 2 hours. The same child, the same nervous system — but now the environment is working with her, not against her." — Parent, Pinnacle Network

Celebrate the Milestone — You Built This
A child who once took 2 hours to settle, who lay awake cataloging every sensory input, who experienced bedtime as overwhelming — now rests in an environment engineered to their nervous system's needs.
Visual Environment
A sensory-safe visual space — controlled light, no random stimulation
Auditory Environment
A predictable auditory environment — consistent white noise masking
Tactile Comfort
Sensory-safe sleepwear and appropriate bedding layers confirmed nightly
Self-Advocacy
A child who knows their own sensory needs and is beginning to advocate for them
You became a sensory environment engineer without a certificate. You observed, you tested, you adjusted, you persisted. Your child's improved sleep is the direct result of your informed, patient, consistent intervention.
Each night of better sleep supports: memory consolidation, emotional regulation, immune function, learning readiness, and family wellbeing.

Red Flags — When to Escalate
Sensory sleep difficulties can have medical layers. Know when to escalate — these signals indicate that professional evaluation is needed beyond the home protocol.
🚩 Sleep improvements plateau despite thorough sensory modification
Consider: Sleep study — sleep apnea is significantly more common in autism and can present as sensory-seeming difficulties. Pediatric sleep specialist referral.
🚩 Breath-holding, gasping, or irregular breathing during sleep
Immediate referral: Pediatric pulmonologist / sleep medicine. This is a medical emergency pattern — do not wait.
🚩 Significant sleep regression after weeks of progress
Consider: Medical illness, anxiety escalation, major life change, puberty onset. Rule out medical before re-attributing to sensory.
🚩 Adequate sleep hours but severely impaired during the day
Consider: Sleep quality (not just quantity) — sleep architecture disorders, insufficient REM/deep sleep. Sleep specialist referral.
🚩 Sensory profile appears to be worsening over time
Consider: Sensory processing differences associated with new diagnoses — formal developmental evaluation recommended.
📞9100 181 181 — FREE National Autism Helpline. Our OT and NeuroDev teams can guide escalation pathways, arrange sleep specialist coordination, and integrate medical findings into your child's GPT-OS® profile.
Your Child's Pathway Forward
Sensory Sleep Environment Engineering is one layer of the sleep independence architecture. Here is where you are — and where you can go next.
1
Before This
D-448: Bedtime Resistance
D-449: Sleep Routine
D-449: Sleep Routine
2
🌟 You Are Here
D-450: Sensory Sleep Environment Engineering
3
Next Steps
D-451: Morning Routine Independence
D-452: Nighttime Fears & Anxiety
D-446: Sleep Initiation
D-447: Night Waking
D-452: Nighttime Fears & Anxiety
D-446: Sleep Initiation
D-447: Night Waking
Long-Term Goal: Sleep Independence Readiness — child sleeps consistently in a sensory-adapted environment with self-management of preferences, generalizing to new environments including travel, school, and family visits.

Related Techniques in the Sleep Cluster
These techniques work together. You already own materials for 4+ of these techniques from your D-450 kit — making the next steps immediately accessible.
Code | Technique | Difficulty | Materials You Already Have |
D-448 | Bedtime Resistance | ⭐ Foundation | Transition objects from this kit |
D-449 | Sleep Routine | ⭐ Foundation | Visual timer + white noise |
D-451 | Morning Routine Independence | ⭐⭐ Core | Sensory sleepwear |
D-452 | Nighttime Fears & Anxiety | ⭐⭐ Core | Red nightlight + body pillow |
D-446 | Sleep Initiation | ⭐⭐ Core | Weighted blanket |
D-447 | Night Waking | ⭐⭐ Core | White noise + compression |
Domain D — Sleep, Self-Care & Daily Living Skills

Your Child's Full Developmental Map
Sleep is one domain. Here is the whole child — and how the sleep environment connects to every other area of development.
Domain | Area | Connection to D-450 |
A | Sensory Processing | Direct — sensory modulation is foundational to this technique |
B | Social Communication | Indirect — sleep quality drives social readiness the following day |
C | Emotional Regulation | Direct — sleep deprivation doubles emotional dysregulation episodes |
D | Sleep & Self-Care | ← YOU ARE HERE |
E | Motor Development | Indirect — rest supports motor learning consolidation overnight |
F | Cognitive & Learning | Direct — sleep is the primary memory consolidation window |
G | Language | Indirect — sleep deprivation measurably impacts language processing |
H | Executive Function | Direct — sleep drives prefrontal cortex function and planning |
K | Family Systems | Direct — bedtime battles are a whole-family systems issue |

Real Families. Real Bedrooms. Real Sleep.
"Our son would lie awake for hours, bothered by things we couldn't detect — the smoke detector light, the AC hum, the way his pajamas felt. We tried everything randomly. A friend who was an OT suggested we do a sensory audit. We covered indicator lights with black tape, got blackout curtains and a white noise machine, found bamboo pajamas without tags, and tried a weighted blanket. It took three weeks of adjustments. Now he falls asleep in 20 minutes. The same child. The same nervous system. But the room finally speaks his language." — Parent, Pinnacle Blooms Network
Week 1
90 min → sleep onset
Week 3
45 min → sleep onset
Week 6
18 min → sleep onset
Week 10
12 min → MASTERY
20M+
1:1 Sessions
97%+
Measured Improvement
70+
Centers
Connect With the Community
You are not navigating this alone. Millions of families are on this journey — and the collective wisdom of those families, guided by Pinnacle's clinical teams, is available to you right now. Consistency across every caregiver multiplies your impact by 3×.
Pinnacle Parent Network
70,000+ families navigating sensory and developmental challenges. Share your D-450 sleep environment setup, get feedback from experienced parents.
WhatsApp Support Group
Moderated by Pinnacle OT team. Real-time support for bedtime challenges — available when you need it most, including during a difficult night.
Monthly Parent Workshop
Live online sessions on sensory sleep environments. OT-led, evidence-based, and free for Pinnacle families. Real Q&A with specialists.
Professional Support — When and How
This technique empowers you to act today. Professional assessment maximizes impact — especially when sensory differences are complex or affect multiple areas of your child's daily life.
When Home Implementation Is Sufficient
Sensory issues are mild, modifications are making clear progress, and child has no medical comorbidities — continue the home protocol. Track data. Consult if you plateau.
When Professional OT Assessment Is Strongly Recommended
- Sensory differences are significant and you cannot identify specific triggers
- Multiple modifications tried without consistent progress
- Sensory processing differences affect multiple life areas beyond sleep
- Child has autism, ADHD, or other developmental diagnosis
- You want a formal Sensory Profile (Dunn) to guide all interventions
What a Pinnacle OT Will Do
1. Administer formal Sensory Profile 2 assessment
2. Conduct home environment sensory audit (virtual available)
3. Design individualized sensory environment protocol
4. Train you in implementation and troubleshooting
5. Track Sleep Independence Readiness Index via GPT-OS®
📞9100 181 181 | 16+ languages | 24×7 | Free call

The Research Library
The evidence behind this technique — for the curious parent who wants to understand the science supporting every recommendation in this guide.
Level IV — International Framework
WHO Nurturing Care Framework (2018) + WHO/UNICEF CCD Package (PMC9978394)
Level III — EBP Classification
NCAEP (2020) — Environmental modifications classified as evidence-based practice for autism
Level II — RCT
Padmanabha et al. Indian J Pediatr (2019) — Home-based sensory intervention, Indian pediatric population. DOI: 10.1007/s12098-018-2747-4
Level I — Meta-Analysis
PMC10955541 — 24 studies, World J Clin Cases (2024). Sensory integration promotes adaptive behavior, sensory processing, motor skills.
Level I — Systematic Review
PMC11506176 — PRISMA review, 16 studies, 2013–2023. "Sensory integration intervention is evidence-based practice for ASD."
AOTA Sensory Processing Evidence Summary
Frontiers Integrative Neuroscience 2020
Circadian Biology Research

How GPT-OS® Uses Your Data
Your sleep data doesn't disappear. It makes every child's protocol smarter — yours and thousands of others navigating the same sensory landscape.
What GPT-OS® Learns from D-450 Data
• Which sensory modalities respond fastest to modification
• Optimal weighted blanket weight range by age/weight profile
• Whether light or sound sensitivity is primary barrier for a child's cluster profile
• Sleep onset time trajectory across the 8-week intervention window
Population-Level Impact
When 10,000 families track their D-450 modifications, the pattern data shows every new family exactly which modifications are most likely to work for their child's specific profile. Your data helps every child like yours — globally.
Privacy: Data is anonymized and aggregated. Full DPDPA (India) compliance.

Share This With Your Family
Consistency across every caregiver multiplies impact by 3×. When grandparents, school staff, and other caregivers understand the sensory environment principles — they can replicate the setup wherever your child sleeps.
"Explain to Grandparents" Script
"[Child's name]'s room is set up in a very specific way to help their nervous system relax at bedtime. Please: Keep blackout curtains fully closed. Turn on the white noise machine (the round device by the window). Use the specific pajamas that are laid out — not any others. Offer the heavy blanket — it helps them feel calm. This is therapy, not preference. Consistency is essential."
Teacher Communication Template
"Our child has sensory processing differences that affect sleep. We are implementing D-450 Sensory Sleep Environment protocol. For school rest periods, please: [sensory accommodations as per child's OT plan]."

Frequently Asked Questions
Every question parents ask — answered by the Pinnacle Blooms Consortium clinical team. These FAQs are drawn from the most common concerns raised across 70,000+ families in the Pinnacle network.
Q: My child refuses the weighted blanket but seems to need pressure. What else can I try?
Compression sleepwear provides similar proprioceptive input without blanket weight. Some children prefer the "hug from inside" of compression. Try both, or body pillow for contact without either. Preference varies night to night — always offer choice.
Q: We've tried blackout curtains but my child is afraid of the dark. How do we balance this?
Blackout curtains eliminate uncontrolled light, then introduce a red/orange nightlight under your control. You manage the light — your child is no longer managed by random light sources. The nightlight provides visibility while blackout gives you control.
Q: What weighted blanket weight is right for my child?
Standard recommendation: 10% of body weight. Start slightly below (8%) and adjust up if child tolerates well. For a 20kg child: 2kg blanket as the starting point. Never exceed 10% of body weight.
Q: How long before I see meaningful improvement?
Weeks 1–2: Acceptance of environment. Weeks 3–4: Faster settling. Weeks 5–8: Consistent sleep onset under 20 minutes. If no progress by Week 4 despite consistent implementation, professional OT evaluation is strongly recommended.
Q: My child sleeps well at home but not at grandparents'. What should we do?
Build a portable sensory kit: travel white noise machine (or phone app), child's own pillowcase/fitted sheet, travel-sized weighted lap pad, familiar comfort toy. The goal is replicating key sensory elements, not the whole room.
Q: Should I tell my child's teacher about the sensory sleep modifications?
Yes — proactively. Sensory patterns that affect sleep also affect the classroom. Sharing the OT-designed sensory profile enables environmental accommodations (seating, lighting, sound levels) that support regulatory capacity during school hours.

You've Read the Science. You Have the Materials. Tonight Can Be Different.
Every piece of knowledge you need is in your hands. Every material has a zero-cost alternative. Every step has been clinician-validated across 20 million therapy sessions. The only thing left is to begin.
20M+
Therapy Sessions
Validating this protocol
97%+
Measured Improvement
Across the Pinnacle Network
70+
Centers
Across India
📞 FREE National Autism Helpline: 9100 181 181 | Available 24×7 | 16+ Languages | Free Call | No Appointment Needed
Preview of 9 materials that help with sensory sleep environment Therapy Material
Below is a visual preview of 9 materials that help with sensory sleep environment therapy material. The pages shown help educators, therapists, and caregivers understand the structure and content of the resource before use. Materials should be used under appropriate professional guidance.




















Share this resource
Help others discover thisLink copied!
The Pinnacle Promise
Pinnacle Blooms Network®
Technique D-450
From fear to mastery. One technique at a time.
Pinnacle Blooms Network® exists to transform every home into a proven, scientific, 24×7, personalized, multi-sensory, multi-disciplinary therapy environment — accessible to every family, in every language, at every income level. Not as a distant ambition. As an operating fact, delivered through GPT-OS®.
Occupational Therapy
OT lead for sensory environment design
Speech-Language Pathology
Communication integration across domains
Applied Behavior Analysis
Behavioral reinforcement systems
Special Education
School-home strategy alignment
NeuroDev Pediatrics
Medical oversight and diagnostics
Medical Disclaimer: This content is educational. It does not replace individualized sensory processing assessment and intervention planning with licensed occupational therapists and healthcare professionals. Sensory processing differences require professional evaluation. Sleep difficulties may have medical causes requiring evaluation. Individual results may vary.
© 2025 Pinnacle Blooms Network®, unit of Bharath Healthcare Laboratories Pvt. Ltd. All rights reserved.
CIN: U74999TG2016PTC113063 | DPIIT: DIPP8651 (Govt. of India) | MSME: Udyog Aadhaar | GSTIN: 36AAGCB9722P1Z2
CIN: U74999TG2016PTC113063 | DPIIT: DIPP8651 (Govt. of India) | MSME: Udyog Aadhaar | GSTIN: 36AAGCB9722P1Z2
