
9 Materials That Help With Scratching Others
D-385 | Pinnacle Blooms Network® | Behavior & Flexibility Domain
👶 Ages 1–10
🏠 Home + Clinic
⏱ 8–12 Week Protocol

Your child scratched you again today. And you're standing in the kitchen with marks on your arms, wondering how much more you can take.
Behind every scratch is a need that hasn't found the right words — or the right release.
"You are not failing. Your child's nervous system is speaking in the only language it currently knows. Our job — together — is to teach it better ones." — Pinnacle Blooms Consortium | OT • ABA • SLP • SpEd • NeuroDev
"The scratches started when my daughter was about two. At first, we thought it was a phase. But it didn't stop. She'd scratch me, her father, her grandmother. Deep scratches that left marks for days. Other parents would pull their children away when they saw us coming. What I didn't understand then was that the scratching wasn't about wanting to hurt. It was communication." — Mother, Pinnacle Network Family
WHO Nurturing Care Framework (2018): Parental awareness directly impacts early developmental outcomes.

You Are Not Alone — The Numbers
You are among tens of millions of families globally navigating scratching, aggression, and sensory-driven challenging behavior. This is not a parenting failure. This is a neurodevelopmental reality — and it has evidence-based solutions.
80%
Sensory Difficulties
Children with ASD experience sensory processing difficulties — PRISMA Systematic Review, 2024
1/36
ASD Diagnosis Rate
Children diagnosed with autism in the US (CDC 2023). ~1 in 68 estimated in India (NIMHANS)
97%+
Measured Improvement
At Pinnacle with function-based intervention across 20M+ 1:1 sessions
India has an estimated 18 million children on the autism spectrum. Scratching behavior is documented across cultures, languages, and socioeconomic strata as one of the most common challenging behaviors in developmental delay. You are not alone in this room.
Research: PMC11506176 — PRISMA 2024 Systematic Review | PMC10955541 — Meta-analysis, World J Clin Cases 2024 | DOI: 10.12998/wjcc.v12.i7.1260

Scratching is not defiance. It's a nervous system speaking.
When we understand the neurology behind scratching, we stop fighting the child and start addressing the actual cause. Five distinct brain pathways can drive this behavior.
🔴 Sensory-Seeking
The somatosensory cortex is under-stimulated. The child's nervous system craves tactile feedback — the resistance, the texture, the sensation.
🟠 Communication Overload
When verbal pathways are underdeveloped, the child uses the body to communicate. Scratching = "No." "Stop." "I'm overwhelmed."
🟡 Emotional Dysregulation
The prefrontal cortex — which governs impulse control — is still developing in all children under 7, and may be significantly delayed in children with ASD.
🟢 Escape/Avoidance
The nervous system learned that scratching ends aversive situations. This is operant conditioning — the brain found an effective tool and keeps using it.
🔵 Proprioceptive Regulation
Deep pressure input can be paradoxically organizing for a dysregulated nervous system seeking heavy proprioceptive input.
"This is a wiring difference, not a behavior choice. Intervention changes the wiring — not the child."
Frontiers in Integrative Neuroscience (2020): DOI: 10.3389/fnint.2020.556660

Where This Sits in Development
Your child is at a specific point on a developmental journey. Understanding the typical timeline helps you calibrate expectations and respond with precision rather than panic.
Ages 12–24 Months
Scratching developmentally typical — cause-effect learning, limited impulse control
Ages 2–4 Years
Should reduce as language and impulse control emerge
Ages 4–7 Years
Persistence here signals unmet sensory or communication needs requiring attention
Ages 7–10+ Years
Requires structured intervention and a formal Functional Behavior Assessment (FBA)
🧠 Typical Development
Most children naturally reduce scratching by ages 3–4 as language and impulse control develop. For children with delays, this transition is delayed — not absent.
🔍 What Commonly Co-Occurs
Sensory processing difficulties, language delay, emotional regulation challenges, transition anxiety, tactile sensitivity or seeking, attention differences.
🗺 The Forward Path
With function-based intervention, most children show measurable reduction in scratching within 6–12 weeks. Full resolution typically follows communication mastery.
WHO Care for Child Development Package (2023): PMC9978394 | WHO/UNICEF CCD Package

The Evidence Behind This Approach
This is not a theory. This is a clinically validated, multi-disciplinary, evidence-based approach — backed by systematic reviews, RCTs, and international health frameworks.
📄 PRISMA Systematic Review (2024)
16 articles confirming sensory integration intervention as evidence-based practice for children with ASD. Published in Children journal. PMC11506176
📄 Meta-Analysis (World J Clin Cases, 2024)
24 studies. SI therapy effectively promotes social skills, adaptive behavior, sensory processing, and motor skills. PMC10955541
📄 Indian RCT (Indian J Pediatr, 2019)
Home-based sensory interventions demonstrated significant outcomes in Indian pediatric populations. DOI: 10.1007/s12098-018-2747-4
📄 NCAEP EBP Report (2020)
Visual supports, reinforcement, and FCT classified as evidence-based practices for autism. NCAEP 2020
📄 WHO NCF (2018) + UNICEF CCD (2023)
International frameworks validating caregiver-delivered home intervention at population scale.
🛡️ EVIDENCE GRADE: I-A — Systematic Review + RCT Level Evidence | ✓ 16+ Studies | 2013–2024 | ✓ ASD Populations | ✓ Home-Applicable
"Clinically validated. Home-applicable. Parent-proven across 20 million sessions at Pinnacle Blooms Network®."
"Clinically validated. Home-applicable. Parent-proven across 20 million sessions at Pinnacle Blooms Network®."

What This Technique Is
Formal Name
Function-Based Scratching Intervention with Multi-Modal Replacement Strategy (D-385)
Parent Name
"The 9 Materials That Help With Scratching Others"
Domain
D — Behavior, Flexibility & Safety | Series: Challenging Behaviors & Safety | Episode 385
Protocol Parameters
👶 Ages 1–10 | ⏱ 10–20 min/day | 📅 Daily | 📈 Observable change: 6–12 weeks | 🏠 Home + School + Community
Clinical Definition
Function-based behavioral intervention using multi-modal sensory replacement, augmentative communication supports, and reinforcement systems to reduce scratching aggression.
What That Means For You
Teaching your child's nervous system a better language — by giving their hands something acceptable to scratch, giving their voice something to say, and rewarding safe hands.
Canon Material Categories
📦 Sensory Scratch Alternatives
📦 Deep Pressure Tools
📦 Communication / AAC Cards
📦 Calm-Down Kit
📦 Visual Schedules
📦 Social Stories
📦 Protective Materials
📦 Emotion Tools
📦 Reinforcement Menus

Who Uses This Technique
No single discipline owns this technique. Every discipline has a piece of it. Scratching behavior crosses therapy boundaries because the brain doesn't organize by therapy type.
Occupational Therapist
Primary lead for sensory functions. Conducts sensory processing evaluation, designs sensory diet, prescribes scratch alternatives and deep pressure tools, trains proprioceptive regulation strategies.
Speech-Language Pathologist
Primary lead for communication functions. Assesses language and AAC needs. Designs and implements PECS/AAC boards. Trains functional communication replacement for scratching.
BCBA / ABA Specialist
Primary lead for behavioral functions. Conducts Functional Behavior Assessment (FBA). Identifies function. Designs reinforcement systems. Tracks data.
Special Educator
Implements visual schedules, social stories, and predictability supports in school/home environments. Coordinates with family on consistency across settings.
NeuroDev Pediatrician
Rules out pain, illness, or medical causes for scratching. Coordinates pharmacological support if appropriate. Provides developmental diagnosis context.
"This technique crosses therapy boundaries because the brain doesn't organize by therapy type. At Pinnacle, FusionModule™ ensures all five disciplines work as one coordinated intervention — not five separate agendas."

What This Technique Targets
Scratching is the symptom. These are the actual targets — from the immediate observable behavior all the way to long-term social inclusion and independent regulation.
Target | Intervention Material | |
Sensory seeking | Sensory scratch alternatives + deep pressure tools | |
Communication | AAC cards + communication boards | |
Dysregulation | Calm-down kit + emotion identification tools | |
Transition anxiety | Visual schedules + social stories | |
Behavior motivation | Reinforcement systems | |
Physical harm reduction | Protective strategies (nail care + clothing) |
PMC10955541 — Meta-analysis: SI therapy effectively promoted social skills, adaptive behavior, sensory processing and motor skills across 24 studies.

The 9 Materials: An Overview
Nine clinically validated materials — available across India — that together address every function driving scratching behavior. Total investment: ₹100–₹2,000. Every material has a ₹0 household alternative.

1. Sensory Scratch Alternatives
Textured scratch pads, velcro strips, corrugated cardboard panels, silicone texture mats. ₹100–500

2. Deep Pressure Tools
Weighted lap pad (10% body weight), compression vest, resistance putty/therapy dough. ₹300–2,000

3. Communication Cards / AAC
Laminated STOP | NO | BREAK | HELP | I WANT cards. PECS-compatible. Portable card ring. ₹100–800

4. Calm-Down Kit
Fidgets, sensory bottle, stress ball, breathing tools, noise-reducing headphones, visual strategy cards. ₹200–800

5. Visual Schedule & Transition Supports
Visual schedule board, activity picture cards, first-then boards, countdown timer, transition objects. ₹200–600

6. Social Stories
Personalized book: "Sometimes I feel upset. I can use gentle hands." Visual reminder cards. ₹100–400

7. Protective Clothing & Nail Care
Child-friendly nail clippers, sensory-friendly clothing, protective arm covers, first aid supplies. ₹100–500

8. Emotion Identification Tools
Feelings chart, body awareness map, emotions scale (1–5 Zones model), check-in cards. ₹100–500

9. Reinforcement System
Token board, reward sticker chart, reward jar. Safe hands behavior reinforcement. ₹100–400

Materials 1–3: Sensory & Communication Essentials
Material 1 — Sensory Scratch Alternatives
Canon: Sensory Tools | ₹100–500
Textured scratch pads, scratch art boards, velcro strips, corrugated cardboard panels, silicone texture mats. Provides the same tactile feedback as scratching — safe, acceptable target. The child's nervous system receives the proprioceptive input it craves without causing harm.
🛡️ Pinnacle Recommends
Material 2 — Deep Pressure & Proprioceptive Tools
Canon: Sensory Tools | ₹300–2,000
Weighted lap pad (10% body weight), compression vest, resistance putty/therapy dough, heavy work items. Deep pressure input is a powerful organizer for dysregulated nervous systems seeking intense proprioceptive feedback throughout the day.
🛡️ Pinnacle Recommends
Material 3 — Communication Cards / AAC Supports
Canon: Communication Supports | ₹100–800
Laminated cards: STOP | NO | BREAK | HELP | TOO LOUD | I WANT | ALL DONE. PECS-compatible. Portable card ring. These cards give the child a voice — a way to say what they need before their body says it for them through scratching.
🛡️ Pinnacle Recommends

Materials 4–6: Regulation, Routine & Narrative
Material 4 — Calm-Down Kit
Canon: Regulation Materials | ₹200–800
Portable kit: fidgets, sensory bottle, stress ball, breathing tools (pinwheel/Hoberman sphere), noise-reducing headphones, visual strategy cards. The calm-down kit teaches children to self-regulate before reaching the point of overflow. Portability is essential — the kit travels with the child.
🛡️ Pinnacle Recommends
Material 5 — Visual Schedule & Transition Supports
Canon: Visual Supports | ₹200–600
Visual schedule board, activity picture cards, first-then boards, countdown timer, transition objects. Scratching frequently spikes at transitions — when unpredictability creates anxiety. Visual schedules remove that uncertainty, giving the child a map of what's next so the nervous system can prepare.
🛡️ Pinnacle Recommends
Material 6 — Social Stories (Gentle Hands)
Canon: Narrative Learning Materials | ₹100–400
Personalized social story book: "Sometimes I feel upset. I can use gentle hands. Scratching hurts. I will use my calm kit." Visual reminder cards reinforce the message between sessions. Narrative personalisation drives neural encoding — using the child's own name throughout amplifies the impact.
🛡️ Pinnacle Recommends

Materials 7–9: Safety, Emotion & Reinforcement
Material 7 — Protective Clothing & Nail Care
Canon: Safety & Protective Materials | ₹100–500
Child-friendly nail clippers + file, long-sleeved sensory-friendly clothing, protective arm covers for caregivers, first aid supplies. This is the immediate harm-reduction layer of the protocol — reducing injury risk while the therapeutic work progresses over weeks.
🛡️ Safety First
Material 8 — Emotion Identification Tools
Canon: Emotional Regulation Supports | ₹100–500
Feelings chart (calm / a little upset / very upset), body awareness map, emotions scale (1–5 Zones model), check-in cards, emotion vocabulary books. A child who can name a feeling is a child who has one more second before the scratch. Emotional vocabulary is the bridge between body state and communication.
🛡️ Pinnacle Recommends
Material 9 — Reinforcement System (Safe Hands)
Canon: Reinforcement Menus | ₹100–400
Token board, sticker chart, reward jar. The reinforcement system makes safe hands the most rewarding choice the child can make.
🏆The Rosette Imprint Reward Jar — ₹589 | Buy on Amazon.in →
🏆1800+ Reward Stickers Pack — ₹364 | Buy on Amazon.in →
✓ Pinnacle Canon Products
🚀START HERE (₹500–800 total): 1. Scratch alternatives (DIY with household textures = ₹0) | 2. 3 communication cards (print + laminate = ₹50) | 3. Reward sticker chart → ₹364 on Amazon.in | 4. Stress ball (₹100–200)

DIY & Zero-Cost Alternatives
Every technique on this page can be executed today with household items. WHO/UNICEF principle: no family left behind. The science is in the technique, not the brand.
Material | Clinical Option | Household DIY | Why It Works | |
Scratch Alternatives | Sensory scratch pad ₹200 | Velcro from old bag or corrugated cardboard | Tactile feedback is texture-based — free materials work equally well | |
Deep Pressure | Weighted lap pad ₹800 | Fill a shopping bag with rice/sand (10% body weight) | Proprioceptive input is weight-based — rice works as well as commercial product | |
Communication Cards | Laminated set ₹100 | Draw pictures on A4 paper, laminate with tape: STOP/BREAK/HELP | Any consistent visual representation teaches the replacement behavior | |
Calm-Down Kit | Sensory kit ₹500 | Sandwich bag: rice-filled sock, small toy, one textured cloth piece | Portability and consistency matter more than material quality | |
Visual Schedule | Schedule board ₹400 | Whiteboard + drawings or phone photos of activities in sequence | Predictability is the function — the medium doesn't matter | |
Social Story | Printed book ₹200 | A4 paper, drawn/printed pictures, stapled with child's name throughout | Narrative personalisation drives neural encoding — handmade = equally effective | |
Emotion Tools | Commercial chart ₹200 | Draw 3 faces: calm, upset, very upset. Use mirror to practice together | Emotional vocabulary is built through interaction, not product quality | |
Reinforcement Chart | Token board ₹150 | Draw 5 circles on paper. Child draws star/tick for safe hands | The reinforcement principle is behavioral — paper works exactly like commercial boards |
Every single material in this protocol has a ₹0 household alternative. Start today.

⚠️ Safety Gate — Read Before Proceeding
Before beginning any session, run through this three-level safety check. Your child's safety and your own emotional regulation are clinical prerequisites — not optional steps.
🔴 DO NOT PROCEED IF:
- Child has broken skin, open wounds, or active skin infection
- Scratching caused injuries requiring medical attention in past 48 hours
- Child is in acute medical distress, illness, or high fever
- Child appears dissociated, severely distressed, or non-responsive
- You feel unsafe or unable to respond calmly
- Siblings/pets cannot be safely separated during session
If any RED flag applies: Contact Pinnacle Helpline 9100 181 181 before proceeding.
🟡 MODIFY BEFORE PROCEEDING IF:
- Child is overtired, hungry, or has missed medication
- Child has had a significant emotional event in past 2 hours
- Environment is noisy, chaotic, or cannot be controlled
- You're feeling overwhelmed, anxious, or reactive yourself
- Child is showing early dysregulation signs (flushed, rocking, avoiding eye contact)
If AMBER: Address the underlying condition first. Offer food, rest, quiet. Attempt modified session only.
🟢 SAFE TO PROCEED WHEN:
- Child is calm, regulated, or at baseline
- Basic needs met: fed, rested, toileted
- Environment is prepared and quiet
- Materials are assembled and tested for safety
- You are calm, regulated, and ready to respond with empathy
- No competing demands for the next 20 minutes
STOP SIGNAL: Immediately stop and create physical safety distance if you observe: escalating aggression despite redirection | uncontrolled emotional flooding | self-injurious behavior | your own emotional regulation breaking down.

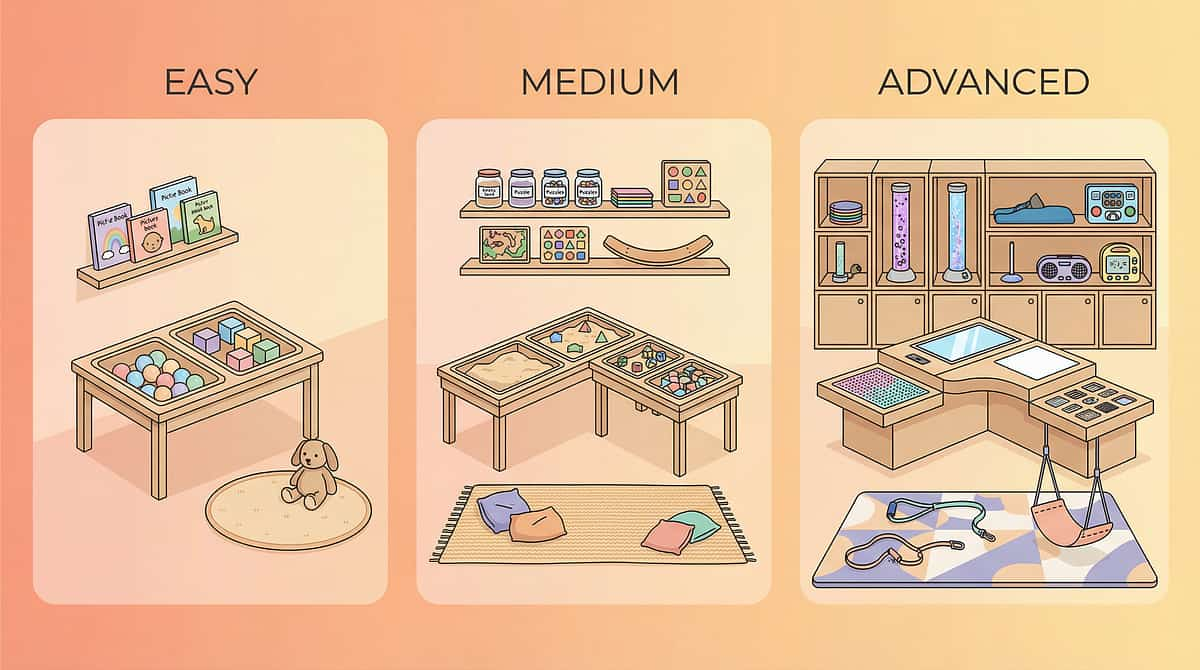
Set Up Your Space
The right environment prevents 80% of session failures before they start. A structured, predictable physical space is itself a therapeutic intervention — it communicates safety to the nervous system before the session begins.
Environment Setup Checklist
- ☐ TV off | siblings in another room | phone on silent
- ☐ Reduce overhead lighting 20% | close windows if street noise
- ☐ Temperature: 22–25°C ideal — overheating increases dysregulation
- ☐ All 9 materials within arm's reach, not behind child
- ☐ Parent at same level as child (floor, low stool) — NOT looming above
- ☐ Child always has an unobstructed exit from the space
- ☐ Designated calm corner visible from child's position
- ☐ Data sheet accessible for immediate post-session use
Space Configuration
Position 1 — Materials Station: Scratch alternatives, cards, and kit arranged within reach at child's eye level. Not behind or above the child.
Position 2 — Child (Center): Seated on floor or low chair. Low center of gravity reduces escape behavior and increases engagement.
Position 3 — Parent/Caregiver: Same level as child, arm's length away — not looming above. Side-by-side is more therapeutic than face-to-face for many children.
Calm Corner: A low-stimulation spot visible from child's position. This is the landing zone if dysregulation peaks during the session.
🕐Total session: 10–20 minutes | 🎯Active technique time: 5–10 minutes | ❄️Cool-down: 3–5 minutes
SI Theory (Ayres): Structured therapeutic environment is a core principle. Meta-analysis confirms 1:1 individual sessions in structured environments were most effective. PMC10955541

Pre-Session Readiness Gate
60 seconds before you begin. The best session starts right. Run this quick assessment before every session — and remember: before you ask "Is my child ready?" ask "Am I ready?"
✅ GO — All 5 Present
- Child is calm, not in meltdown
- Eye contact or physical availability present
- Basic needs met (fed, rested)
- No recent major emotional event
- Child shows interest or neutrality
⚠️ MODIFY — 3–4 Present
Some dysregulation present. Distracted but responsive. One need unmet. Minor event in past hour. Needs warm-up time.
Use simplified 5-minute version. Offer one material. No structured demands. Follow child's lead.
🔴 POSTPONE — Fewer Than 3
Acute distress or meltdown. Completely unavailable. Multiple unmet needs. Major event in past 2 hours. Active refusal or aggression.
Offer alternative regulated activity. Record "session postponed" as data. No pressure.
Parent Regulation Check:Before you ask "Is my child ready?" — ask: "Am I ready?" If you are stressed, rushed, or triggered by a previous scratching incident: Take 3 slow breaths first. Regulate yourself. You are the co-regulator.

Step 1: The Invitation
⏱ 30–60 Seconds
ABA Pairing Principle
Drawing your child into the session through playful, low-demand engagement. No demands yet. Pure positive pairing. This is ABA's "pairing" principle meeting OT's "just-right challenge."
Script for Parents
"Hey [child's name], look what I have!" [Hold up their favourite material — the one from the calm-down kit or a preferred fidget] "Want to explore with me for a bit?" [Sit near them, not in front of them. Let them come to the material.]
If no engagement after 90 seconds, MODIFY to free exploration only.
Acceptance Cues — What to Look For
- ✓ Child glances at or reaches toward material
- ✓ Body turns toward you
- ✓ Vocalizes, points, or approaches
- ✓ Relaxed posture, no active avoidance
Resistance Cues — What to Do
- Child turns away → Move material to side view, don't pursue
- Child vocalizes protest → "Okay, no worries. I'll leave it here." [withdraw]
- Child moves away → Follow slowly, place material in sight, give 30 seconds

Step 2: The Engagement
⏱ 1–3 Minutes
20% Through Session
Introducing the therapeutic materials with your child already engaged. The goal here is exploration — not performance. The child interacts with the material on their terms, guided gently by you.
🔴 For Sensory Function Scratching
"Look at this scratch pad. Feel how rough this is! This feels SO scratchy. Show me how you scratch it."
Demonstrate scratching the surface yourself. Exaggerate the satisfaction. Redirect hands from anything soft to the scratch alternative.
🟠 For Communication Function Scratching
"I know you want to tell me something. Let's find the card."
Lay out 3 cards: STOP | BREAK | HELP. "Which one feels right? Show me." Honor the card immediately.
🟡 For Regulation Function Scratching
"Let's check your body. How are you feeling?"
Use feelings chart. Offer calm-down kit. "I'm going to sit with you. We'll use the kit together."
ENGAGED
Move to Step 3
TOLERATING
Continue, add gentle narration, no demands
AVOIDING
Step back, offer free exploration, reduce expectations

Step 3: The Therapeutic Action
⏱ 5–10 Minutes
The Active Ingredient
Executing the primary therapeutic action for this child's specific scratching function. This is the core of the session — the moment where real neural rewiring begins.
Sensory-Seeking: Scratch Alternative Protocol
- Present scratch pad, textured fabric square, sandpaper piece
- Say: "When your fingers want to scratch, use THIS" — guide hand to material
- Let child scratch to satisfaction — don't cut short
- Practice the redirect: child reaches toward your arm → gently intercept → redirect to scratch pad → "Scratch here"
Communication Function: FCT Training
- Lay out 3–5 communication cards in front of child
- Create a mild, safe opportunity for the child to want something
- Wait 3 seconds for spontaneous card use BEFORE any prompt
- The moment child touches card → IMMEDIATELY honor the request
- Practice 5–7 trials across different communication targets
Dysregulation/Emotion: Regulation Toolkit Training
- Use feelings chart: "Show me where you are right now"
- Together, access calm-down kit before dysregulation peaks
- Practice breathing tool: 3 slow breaths together
- Deep pressure: weighted lap pad or firm hand squeeze
- Name what you observe: "Your body is getting full. Let's empty it."
PMC10955541 — Meta-analysis: 40-min therapy sessions showed maximum effectiveness. Home sessions 10–20 min; core therapeutic action 40–60% of session time.

Step 4: Repeat & Vary
⏱ 3–5 Minutes
"3 good, engaged repetitions > 10 forced, reluctant repetitions."
Material | Target Reps | Satiation Signal | |
Scratch alternatives | 5–10 redirects | Child pushes material away | |
Communication cards | 5–7 trials | Consistent spontaneous use | |
Calm-down kit | 2–3 complete cycles | Regulated state achieved | |
Emotion identification | 3–5 check-ins | Child checks independently | |
Reinforcement earning | 3–5 safe hands moments | Engagement with chart |
Scratch Alternative Variations
- Change texture (smooth → medium → rough → very rough)
- Change location (table → floor → vertical wall mount)
- Change grip (fingertip → full hand → whole palm)
Communication Card Variations
- Change the need expressed per trial
- Change environment (kitchen → living room → garden)
- Add a new card to the array each week
Calm-Down Kit Variations
- Rotate the tool used each session
- Have child choose which tool to use first
- Add a breathing countdown visual
Satiation Indicators — When to Stop: Child pushes material away twice | Attention drifts despite re-engagement | Engagement time drops below 10 seconds per rep | Child initiates a transition to another activity
Step 5: Reinforce & Celebrate
⏱ Immediate — Within 3 Seconds
ABA Timing Principle
Timing > Magnitude. An immediate small reward does more than a delayed big one. The window: within 3 seconds of the desired behavior.
For Using Scratch Alternative
"YES! You scratched the PAD! Safe hands! I am so proud of you!"
For Using Communication Card
"You used your BREAK card! That is AMAZING. Here's your break."
For Accessing Calm-Down Kit
"You picked up your fidget when you felt upset. THAT is huge. That is exactly what we're working toward."
For Gentle Touch
"Gentle hands! I felt that! That was SO gentle. Safe hands. Token!"
Week 1:
1 token per single safe hands moment
Weeks 2–3:
3 tokens → small preferred activity
Week 4+:
Gradually fade to natural social reinforcement
NEVER remove earned tokens. Removing earned reinforcement is a clinical error that destroys trust and accelerates the behavior you are trying to reduce.

Step 6: The Cool-Down
⏱ 3–5 Minutes
No Session Ends Abruptly
Abrupt endings are a primary trigger for post-session dysregulation — which can include scratching. The transition OUT of a session is as therapeutic as the session itself.
Step 6a — The Warning (30 seconds before end)
"Two more [reps/cards/kit uses], then we're all done. [Child's name], two more, then snack time." Show visual timer counting down 30 seconds.
Step 6b — The Closure Ritual (1 minute)
"All done with scratch pad time. Let's put it away together." Child participates in material put-away — proprioceptive input, sense of control. "You did such important work today. Safe hands day!"
Step 6c — The Bridge Activity (2–3 minutes)
3 deep breaths using breathing tool | Sensory bottle: shake and watch | One preferred low-demand book or simple puzzle | Quiet sitting with preferred comfort item
Step 6d — The Transition Statement
"Scratch pad time is all done. Next is [name next activity from visual schedule]." Show the visual schedule. Resistance to ending: offer "one more" ONE time only. Never negotiate beyond that.

Capture the Data: Right Now
📊 Within 60 Seconds of Session End
60 seconds of data now saves hours of guessing later. Consistent data collection is what separates intuition from evidence — and what proves your child is making progress even when it doesn't feel that way.
Session Tracker — D-385
DATE: __________ TIME: __________
1. SCRATCHING TODAY
Number of scratching incidents today: [ ]
Less than yesterday? [ YES ] [ SAME ] [ MORE ]
Number of scratching incidents today: [ ]
Less than yesterday? [ YES ] [ SAME ] [ MORE ]
2. ALTERNATIVE USE
Scratch alternative used: [ YES ] [ NO ]
Communication card used: [ YES ] [ NO ]
Calm kit accessed: [ YES ] [ NO ]
Scratch alternative used: [ YES ] [ NO ]
Communication card used: [ YES ] [ NO ]
Calm kit accessed: [ YES ] [ NO ]
3. ENGAGEMENT RATING (1–5)
Session engagement: 1 2 3 4 5
(1=refused, 5=fully engaged)
Session engagement: 1 2 3 4 5
(1=refused, 5=fully engaged)
NOTES: _________________________
What the Data Means Over Time
Week 1
Baseline. Expect no change. Just measure consistently.
Weeks 2–3
Any reduction in scratching incidents = evidence of function-based impact beginning.
Week 4+
Alternative use frequency should increase as scratching decreases.
Week 8+
Spontaneous alternative use without prompting = mastery indicator.

🔧 What If It Didn't Go As Planned?
"Session abandonment is not failure — it's data. The technique needs adjustment, not you."
Problem 1: Child refused to engage with any material
Why it happened: Wrong timing, wrong material, environment wasn't ready, session followed a recent scratching incident.
Next time: Do readiness check more carefully (Card 13). Let child choose the material from the 9 options. Start with what the child finds most appealing — even if it's not the "ideal" material.
Problem 2: Child used scratch alternative briefly, then scratched me anyway
Why it happened: Scratch alternative hasn't been sufficiently paired with reinforcement yet. Redirect happened too late.
Next time: Reinforce IMMEDIATELY when child uses alternative (even for 1 second). Intercept redirect EARLIER — catch the raised hand before contact. Increase appeal of scratch alternative.
Problem 3: Child wouldn't use communication cards — just kept escalating
Why it happened: Child doesn't yet have the motor/cognitive link between the card and the outcome. Needs more teaching trials during calm times.
Next time: Practice communication cards during CALM periods — not as crisis intervention. 5–10 practice trials/day when child is regulated. Honor the card immediately every single time.
Problem 4: Scratching got worse after we started the protocol
Why it happened: Extinction burst — a normal, expected increase in behavior when a previously effective strategy stops working. It's a sign the intervention is working.
Next time: Maintain the protocol. The burst is temporary. Document the peak, then expect rapid reduction. Contact Pinnacle helpline if escalation is severe: 9100 181 181
Problem 5: I lost my calm during the session
Why it happened: You're human. Repeated scratching is physically and emotionally painful. Caregiver regulation is real and valid.
Next time: Build your own regulation plan first. Have a co-caregiver available if possible. If you lose regulation: pause session, take your own breath, return when calm. Never escalate.
Problem 6: Child only calm at home — scratches at school too
Why it happened: Skills learned in one environment need explicit generalization training to transfer. This is expected — not a setback.
Next time: Send materials to school. Share the discipline guide and teacher template with the teacher. Request a consistency coordination meeting.
Problem 7: Nothing seems to be working after 3 weeks
Why it happened: Function may be misidentified. Protocol may need formal Functional Behavior Assessment.
Next time: Contact Pinnacle Helpline 9100 181 181. Request BCBA/OT-led FBA. Scratching that persists with no function-matched intervention requires professional assessment.

Adapt & Personalize
No two children are identical. No two sessions need to be. The protocol is a framework — not a rigid script. Use this personalization guide to shape each session to your child's current profile.
🔴 Sensory Seeker
Emphasize scratch alternatives and deep pressure heavily. These children need MORE tactile/proprioceptive input, not less.
- High-resistance textures prioritized
- Heavy work throughout day
- Multiple scratch alternative stations around home
🟡 Sensory Avoider
Introduce materials gently, at distance first. Never force contact. Build tolerance gradually with graded exposure.
- Very gradual texture introduction
- Light touch tolerated first
- Child controls all contact with materials
🔵 Communication-First
Prioritize AAC and communication cards above sensory work. Scratching will reduce fastest when communication needs are met.
- FCT is primary intervention
- Ensure every card use is honored immediately
- Build vocabulary before building sensory tolerance
Ages 1–3
Parallel play with scratch alternatives. No formal demands. Sensory exploration only. Communication = 1–2 simple cards maximum.
Ages 3–6
All 9 materials applicable. Structured sessions 10–12 minutes. Emotion identification begins. Social stories introduced.
Ages 6–10
Full protocol. Sessions 15–20 min. Child begins to self-monitor. Data sheets can involve child. Generalization to school prioritized.
Week 1–2: What to Expect
📅 Establishing Phase
15%
Protocol Progress
You are in the foundation-laying phase. Neural groundwork — not yet harvesting results.
✅ Real Progress (even if it doesn't feel like it)
- Child tolerates scratch alternative for 5 seconds longer than Day 1
- Child glanced at the communication card once without prompting
- One scratching incident was preceded by a micro-pause before the scratch
- Calm-down kit was accessed once with full adult prompting
- You completed 5 sessions without either of you melting down
⚠️ What Is NOT Progress Yet (and that's okay)
- Scratching has not reduced yet — Week 1–2 is baseline, not change
- Child doesn't spontaneously use alternatives
- Communication cards are consistently ignored
- You feel like nothing is working
"In weeks 1–2, you are laying neural groundwork — not yet harvesting results. The families who reached Week 8 are the 97%."
PMC11506176 — Systematic review: SI intervention outcomes emerge across 8–12 week timelines. Early-phase indicators focus on tolerance, not mastery.
Week 3–4: Consolidation Signs
📅 Consolidation Phase
40%
Protocol Progress
Neural pathway formation is measurably underway. You should begin to see early spontaneous behaviors.
🧠 Neural Pathway Formation Indicators
- Child reaches for scratch alternative without being reminded (1–2 times/week)
- Communication card used spontaneously even once = massive milestone
- Child anticipates the session — approaches materials or goes to designated space
- Pre-scratching tension recognized by parent earlier than before
- Child accepts the verbal redirect more readily than in Week 1
📊 Data Should Show
- Scratching frequency: any downward trend (even 5–10% reduction counts)
- Alternative use: increasing frequency per session
- Session engagement: higher average score than Weeks 1–2
Behavioral Changes Signaling Neural Adaptation
- Child starts self-talking during pre-scratch moment: "scratch pad"
- Emotional window before scratching gets slightly longer
- Child uses communication card to request break and actually waits for it
"You may notice you're more confident too. Your intervention timing is sharper. Your scripts are more natural. You have become a more skilled co-regulator. That's the consolidation on your side."
Week 5–8: Mastery Indicators
📅 Mastery Phase
75%
Protocol Progress
Approaching mastery. The skills are becoming part of the child's behavioral repertoire.
🏅 Self-Regulation Mastery Criteria
- ☐ Child independently accesses scratch alternative when triggered (no prompting)
- ☐ Communication card used consistently across 3+ settings
- ☐ Calm-down kit accessed independently at pre-escalation stage
- ☐ Scratching incidents reduced by 70%+ from baseline week
- ☐ Child can verbalize or indicate: "I'm upset" before physical behavior
🏅 Generalization Indicators
- Skill appearing in environments beyond the practice setting
- Grandparent reports child showed them the scratch pad
- Teacher notes communication card use in classroom
- Child uses regulation tool during community outing
When to Move Forward vs. Stay
- Move forward: Mastery criteria met at home AND one other setting
- Strengthen: Mastery at home only — generalize to school/community before advancing
- Seek support: No progress toward mastery at 8 weeks → Professional evaluation warranted
🏅 "Mastery Unlocked" Criteria: 5 consecutive days of scratching incidents below 20% of original baseline = MASTERY.
Celebrate This Win 🎉
You did this.
"Your child scratches less — or no longer scratches — because you showed up, every day, for 8 weeks. That is one of the most loving, disciplined, evidence-based things a parent can do."
Identified the Function
You found what was driving the behavior — not just the behavior itself.
Built a New Pathway
Your child's nervous system has a new, safe route to get what it needs.
Gave Them Words
Your child has tools and language instead of just "no."
Demonstrated Love
You showed your child: "I understand you. I'm trying to help you."
You arrived at Card 01 scared, with scratch marks on your arms. You leave this protocol empowered, with evidence, skills, and a child who has new tools. That journey is yours. No one else did it for you.

🚨 Red Flags: When to Pause
Even in the progress and celebration zone, these signs mean pause and seek professional support. This is empowerment through awareness, not fear. Knowing when to escalate is clinical wisdom.
🔴 Behavior Escalation
- Scratching frequency has increased (not an extinction burst) for more than 10 consecutive days
- New aggressive behaviors added (biting, hitting, pinching) while scratching reduces
- Scratching causes wounds requiring medical treatment
🔴 Child Distress
- Child appears to be in physical pain during sessions (check for undetected illness)
- Child is showing signs of severe anxiety about sessions
- Sleep disruption, appetite changes, or withdrawal appearing alongside behavior
🔴 Family Impact
- Siblings or other family members sustaining regular injuries
- Parent/caregiver emotional regulation consistently breaking down
- Child being excluded from school or community settings
🔴 Protocol Non-Response
- No measurable change in scratching frequency after 6 weeks of consistent execution
- Child has not used any single alternative even once after 4 weeks
Level 1
Self-resolve → Review adaptation guide. Adjust protocol. Continue.
Level 2
Teleconsult → 9100 181 181 (FREE, 16+ languages, 24x7)
Level 3
Clinic visit → Book at nearest Pinnacle center
Level 4
Urgent assessment → BCBA + OT + SLP formal FBA + sensory eval

The Progression Pathway
D-385 is one node in a larger developmental journey. Understanding where you are — and where you're going — helps you build a coherent long-term intervention plan for your child.
D-383: Hitting Others
Prerequisite technique — same behavior cluster, shared materials
D-384: Biting Others
Prerequisite technique — oral-sensory function overlap
D-385: Scratching Others
← YOU ARE HERE — Current technique
D-386: Hair Pulling
Next-level: same behavior cluster, shared kit materials
D-395: Self-Regulation
Mastery path: deepens the root cause work across all behavior domains
Long-Term Developmental Goal: This technique feeds directly into: Social Safety Readiness Index → Community Inclusion → School Readiness → Peer Relationships → Independent Emotional Regulation.
Domain D: Behavior, Flexibility & Safety | Position 385 of 420+ Domain D techniques
Domain D: Behavior, Flexibility & Safety | Position 385 of 420+ Domain D techniques
If communication is the primary function: A parallel track through B-221: Communication Building will accelerate your Domain D outcomes significantly. The two tracks reinforce each other.
Related Techniques in This Domain
You may already own materials for several of these. The reinforcement system, communication cards, and calm-down kit you've built for D-385 transfer directly to every technique in this cluster.

D-383: Hitting Others

D-384: Biting Others

D-386: Hair Pulling

D-387: Kicking Others

D-395: Self-Regulation

B-221: Communication Building
✅If you implemented D-385, you already have materials for D-383, D-384, D-386, D-387. The reinforcement system, communication cards, and calm-down kit transfer directly. Your investment compounds across every related technique.
Your Child's Full Developmental Map
D-385 is one technique in one domain of your child's complete developmental profile. Seeing the full picture helps you prioritize intervention sequencing and understand how this work connects to everything else.
Domain D — Behavior & Flexibility
Your current work. 420+ techniques. The domain that most visibly affects family safety and community inclusion.
Domain A — Sensory Processing
Directly connected. Sensory function drives much of Domain D behavior. Parallel sensory work accelerates outcomes.
Domain B — Communication
If scratching has communication function, Domain B work will accelerate Domain D outcomes significantly.
Domain C — Self-Regulation
The root system beneath all behavioral work. Every skill built in D-385 feeds Domain C mastery.
"GPT-OS® maps your child's AbilityScore® across all 12 domains, connecting D-385 data to your child's full therapeutic profile."See Your Child's Full GPT-OS® Profile →

Families Who've Been Here
20 million sessions. Thousands of families. Stories that began exactly like yours — with scratch marks and questions and a fierce love that didn't know where to go.
Communication Function Scratching — Pinnacle Hyderabad
"My son scratched his teachers, his therapist, his little sister. We had been asked to leave three playgroups. I had marks on my arms I had to explain to concerned friends."
After 8 weeks:"He doesn't scratch anymore. Not because he changed who he is — he learned better ways to communicate. His first independent use of the BREAK card was the day I cried in relief for the first time in two years."
Therapist's Notes: This child's scratching was 85% communication function. FCT training with 6 communication cards reduced incidents from 14/day to less than 1/day within 8 weeks.
Sensory Function Scratching — Pinnacle Bangalore
"She scratched everything. Not just people — furniture, walls. She seemed to need it the way she needed air. We didn't understand that her nervous system was starving for that input."
After 6 weeks:"She has a scratch station in every room now. Corduroy fabric, sandpaper board, the commercial scratch pad. She goes to those. Her OT called it 'sensory substitution' and it worked exactly as promised."
OT-guided sensory diet. Commercial + DIY alternatives used in combination.
"The most common mistake families make is trying to eliminate scratching without identifying its function. When we don't give the nervous system an alternative path to the same input, the behavior simply migrates to a new form. Function-based intervention is not optional — it's the mechanism." — Pinnacle OT Specialist, 7 years clinical experience
Illustrative case narratives. Identifying details changed for privacy. Outcomes vary by child, function, and implementation consistency.

Connect With Other Parents
Isolation is the single biggest barrier to home-based intervention adherence. Parents who are connected to other families navigating the same challenges are significantly more likely to complete the protocol. You don't have to do this alone.
Challenging Behaviors Parent WhatsApp Group
Families specifically navigating scratching, hitting, biting. Daily support. Experienced parent mentors. Therapist-moderated. Join Group →
Pinnacle Parent Forum — Domain D
Online forum. Post questions. Share progress. Get responses from therapists and experienced parents. Access Forum →
Local Parent Meetup
Pinnacle center-hosted monthly parent circles. In-person. City-specific. Find Nearest Meetup →
Peer Mentor Matching
Connect 1:1 with a parent who has navigated scratching behavior and achieved mastery. Volunteer mentor network. Request Mentor Match →
"The moment I met another mother whose son scratched — I realized I wasn't a bad mother. I was a mother who needed information and community. Both changed everything." — Pinnacle Network Parent, Year 2

Your Professional Support Team
Home-based intervention is powerful. Clinic-guided intervention is more powerful. Home + clinic = maximum impact. Pinnacle's 70+ centers and teleconsultation platform mean professional support is always within reach — wherever you are in India.
🏃 For Sensory Scratching
Occupational Therapist
Sensory evaluation + sensory diet design + scratch alternative prescription
🗣 For Communication Scratching
Speech-Language Pathologist
AAC assessment + FCT program design + PECS implementation
🧩 For Behavioral Scratching
BCBA / Behavior Analyst
Functional Behavior Assessment + reinforcement system design + data review
Not Near a Center?
All Pinnacle consultations are available via teleconsult. Professional-grade therapy from your home, in your language.
📞 FREE National Helpline
9100 181 181
FREE • 24x7 • 16+ Languages. No appointment needed. Staffed by trained clinicians. Call now for guidance on any step of this protocol.
Pinnacle therapy services are covered under several major health insurance providers. Contact 9100 181 181 for current coverage status.

The Research Library
The evidence base behind everything on this page. Sourced, linked, and transparent. Every technique, every material recommendation, every timeline reflects published science reviewed by the Pinnacle Clinical Consortium before it reaches any parent.
📄 PMC11506176 | Children (2024)
PRISMA Systematic Review: 16 articles, 2013–2023. Sensory integration intervention confirmed as evidence-based practice for ASD children. View on PubMed →
📄 PMC10955541 | World J Clin Cases (2024)
Meta-analysis: 24 studies. Sensory integration therapy promotes social skills, adaptive behavior, sensory processing, and motor skills. View on PubMed →
📄 PMC9978394 | WHO CCD Package
WHO/UNICEF Care for Child Development: Evidence-based caregiver guidance implemented in 54 low- and middle-income countries. View on PubMed →
📄 Padmanabha et al., Indian J Pediatr (2019)
Indian RCT: Home-based sensory interventions in Indian pediatric population. Significant outcomes demonstrated. DOI: 10.1007/s12098-018-2747-4
📄 NCAEP Evidence-Based Practices Report (2020)
Visual supports, reinforcement, and FCT classified as evidence-based practices for autism in the United States. Access Report →

Frequently Asked Questions
Q1: How do I know what FUNCTION is driving my child's scratching?
Observe the pattern: When does scratching happen? What immediately precedes it? What happens right after? Sensory-function scratching is relatively consistent regardless of context. Communication-function scratching happens when the child wants or doesn't want something. Dysregulation scratching follows overwhelm. For a formal assessment, contact a BCBA (see Professional Support card).
Q2: My child scratches at school but not at home after we started the protocol. Normal?
Yes. Skills learned in one environment need explicit generalization training to transfer. Send materials to school. Share the teacher communication template. Request a school coordination meeting to align strategies across settings.
Q3: Can I use all 9 materials at once?
Start with 2–3 most relevant to the suspected function. For sensory function: start with scratch alternatives + reinforcement. For communication: cards + reinforcement. Introducing all 9 at once can overwhelm both child and parent. Add materials as the child masters each one.
Q4: My child scratches themselves too — is this the same technique?
Self-scratching (D-405) has some overlap but requires different considerations — especially if skin damage is occurring. This page addresses scratching others. For self-scratching, see Reel D-405 or contact 9100 181 181 for specific guidance.
Q5: How often should we do formal sessions?
Daily formal sessions (10–20 minutes) are optimal for Weeks 1–4. From Week 5, formal sessions can reduce to 5x/week as the child generalizes skills. The materials should always be accessible even outside formal sessions — availability matters more than frequency at the mastery stage.
Q6: The scratch alternatives aren't working — my child only wants to scratch skin.
Escalate the texture intensity: higher-resistance sandpaper, dense velcro, very rough burlap. Some children need the alternative presented closer to the moment of scratching — intercept, redirect, praise. Contact Pinnacle OT for sensory evaluation if texture alternatives consistently fail after 2 weeks of escalation.
Q7: Is this technique appropriate if my child doesn't have an autism diagnosis?
Yes. Scratching behavior occurs across children with and without diagnosis — language delays, sensory processing differences, emotional regulation challenges. The function-based approach works regardless of diagnosis because it addresses the neurological and communicative mechanism, not the diagnostic label.
Q8: When should scratching behavior require medication?
Medication is considered when behavior is severe, causing significant injury, hasn't responded to intensive behavioral + sensory + communication intervention over 12+ weeks, or there is a clear neurological/psychiatric component. This decision is made by a NeuroDevelopmental Pediatrician in coordination with the behavioral team. Contact 9100 181 181 for referral guidance.
Preview of 9 materials that help with scratching others Therapy Material
Below is a visual preview of 9 materials that help with scratching others therapy material. The pages shown help educators, therapists, and caregivers understand the structure and content of the resource before use. Materials should be used under appropriate professional guidance.








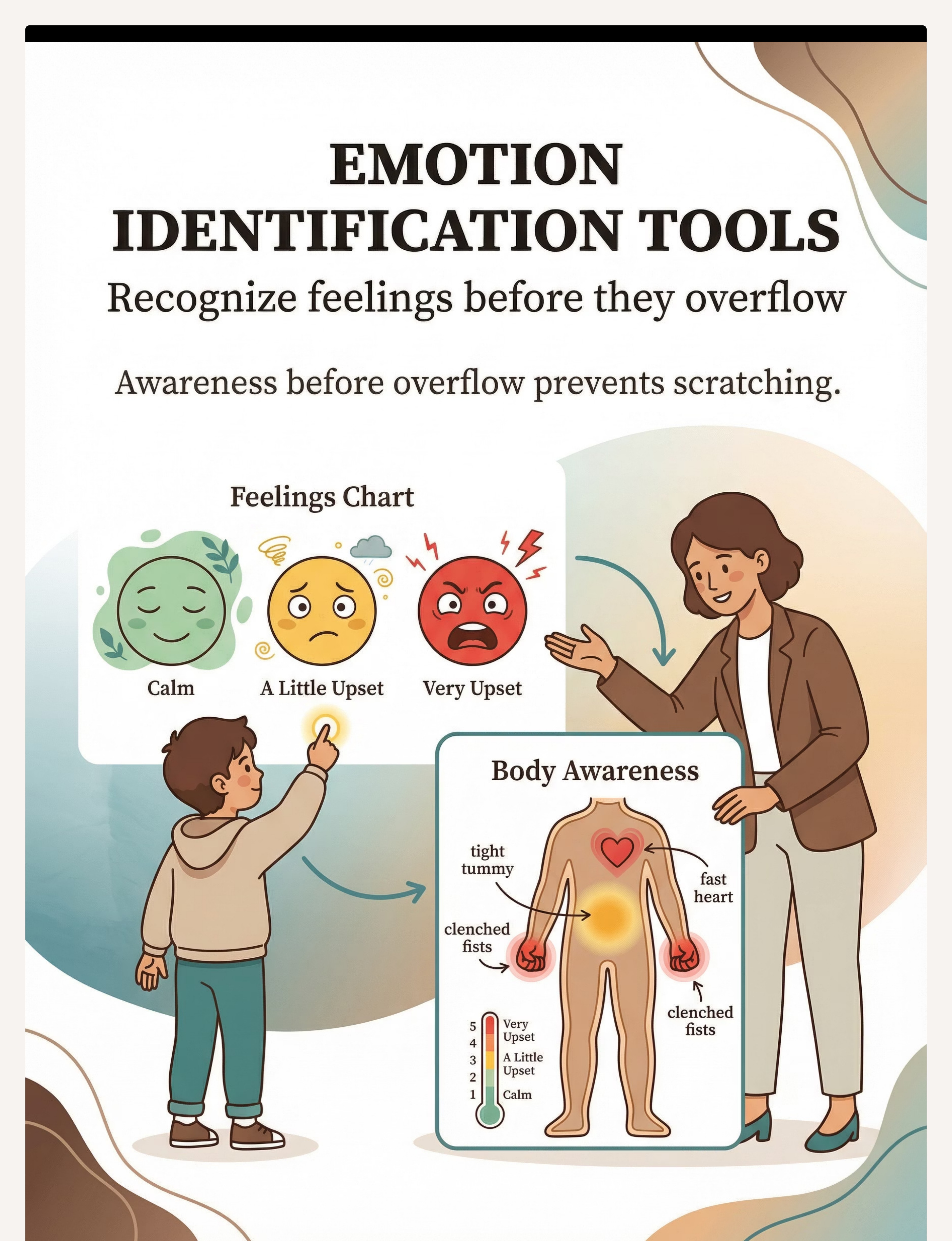










Share this resource
Help others discover thisLink copied!

Your Next Step: Start Today
You have everything you need. The science is clear. The materials are accessible. The protocol is structured. Your child's hands can be safe. Start today.
20M+
1:1 Sessions
Delivered across the Pinnacle Blooms Network®
97%+
Measured Improvement
With function-based intervention
70+
Centers
Across India + 70+ countries served
🌸 PINNACLE BLOOMS NETWORK® — The Pinnacle Promise
"From fear to mastery. One technique at a time."
Built by Mothers. Engineered as a System. | OT • SLP • ABA/BCBA • SpEd • NeuroDev Pediatrics • CRO | Powered by GPT-OS® | WHO/UNICEF Aligned • PubMed Sourced
📞FREE Helpline: 9100 181 181 | Available in 16+ languages | 24 hours | 7 days
"From fear to mastery. One technique at a time."
Built by Mothers. Engineered as a System. | OT • SLP • ABA/BCBA • SpEd • NeuroDev Pediatrics • CRO | Powered by GPT-OS® | WHO/UNICEF Aligned • PubMed Sourced
📞FREE Helpline: 9100 181 181 | Available in 16+ languages | 24 hours | 7 days
This content is educational. It does not replace functional behavioral assessment by qualified professionals. Aggressive behaviors that cause injury, are frequent, or significantly impact functioning require individualized assessment by licensed behavior analysts, psychologists, or developmental specialists. Always ensure safety first. Individual results may vary. Statistics represent aggregate outcomes across the Pinnacle Blooms Network®.
© 2026 Pinnacle Blooms Network®, unit of Bharath Healthcare Laboratories Pvt. Ltd. All rights reserved. Content created by the GPT-OS® Content Engine under consortium specification. | CIN: U74999TG2016PTC113063 | DPIIT: DIPP8651 | MSME: TS20F0009606 | GSTIN: 36AAGCB9722P1Z2 | techniques.pinnacleblooms.org
