
"Your child hasn't called out for you today. Not once."
They play beside you — content, absorbed in their own world — but they don't look up to show you something funny. They don't reach toward you when they want more. They don't point, pull your hand, or make sounds to get your attention. You've started to wonder: does my child want to communicate at all?
This is the hallmark of Limited Communicative Intent — and it is one of the most important early signals in a child's developmental journey. Not because it means something is permanently wrong. But because it means something powerful can be done about it, starting today, at home.
"You are not failing. Your child's communication system is in an early stage — and this page shows you exactly how to awaken it."
🏥 Pinnacle Blooms Network®
SLP Lead · ABA Co-Lead · OT Support
Domain B: Social Communication

🔍 Act I — Understand
This Is More Common Than You Know
Communicative intent — the drive to reach out and use another person to meet a need or share an experience — is the root of all language. When this root is weak, words cannot grow. But research confirms: communicative intent is not fixed. It can be kindled.
1 in 36
Children with ASD
CDC, 2023. In India: estimated 1 in 40 urban children. Limited communicative intent is present in the majority at diagnosis.
80%
Show Limited Intent
Of children with ASD demonstrate significantly limited communicative intent in early development (ASHA Practice Portal, 2023 | Wetherby & Prizant).
21M+
Therapy Sessions
Delivered by Pinnacle Blooms Network® across 70+ centers. More children with this profile have been helped here than anywhere in South Asia.
References: PMC11506176 | ASHA Practice Portal Communication | CDC Autism Data 2023

This Is a Motivation Circuit — Not a Language Circuit
The Wiring Difference
In typical development, a child's brain wires social interaction with reward as early as 3 months: looking at a face feels good, making a sound that gets a response feels good, reaching and receiving feels satisfying. This creates a motivation circuit — an internal drive to communicate.
In children with limited communicative intent, this circuit is under-activated. The neural pathways connecting "I want something" to the action of reaching out to another person are not yet consistently firing.
This is not a behavior choice. This is a wiring difference.
The Extraordinary News
2024 neuroscience confirms this circuit is highly plastic. Structured, repeated, motivating communication opportunities — exactly what these 9 materials create — physically strengthen these pathways over time.
"Communication intent is not taught. It is grown — through joyful, repeated reasons to reach out." — Pinnacle SLP Consortium, Clinical Doctrine
Reference: DOI: 10.3389/fnint.2020.556660 | Wetherby & Prizant, CSBS
A Waypoint — Not a Dead End
According to the WHO Care for Child Development Package (implemented in 54 countries), communicative intent typically consolidates between 9–12 months. For children with ASD or developmental differences, this milestone can be delayed — and its emergence can be systematically supported.
Birth–6 Months
Eye contact, social smile, reflexive vocalization, reciprocal cooing, responding to name ✓
6–9 Months
Proto-imperative gestures (reaching), pre-intentional communication begins ✓
9–12 Months
🔶 Communicative Intent Emerges — Your child may be here
12–24 Months
First words, intentional requesting, showing, combinatorial communication, social referencing
24–36 Months
Conversational turns, commenting, narrative — the full communication picture
Comorbidities to screen for: Sensory processing differences (present in 80% of ASD), Apraxia of speech, Hearing differences, Anxiety in social contexts. All can suppress communicative intent. Our first target is not words — it is the drive to reach out. Words follow naturally once this drive exists.
References: PMC9978394 | WHO/UNICEF CCD Package (2023) | NCAEP 2020

🛡️ Level I Evidence
Systematic Review + RCT Support
Clinically Validated. Home-Applicable. Parent-Proven.
🔬 PRISMA Systematic Review (2024, PMC11506176)
16 articles, 2013–2023 confirm communication-focused intervention meets evidence-based practice criteria for children with ASD. Effect sizes significant across joint attention, requesting, and turn-taking domains.
🔬 NCAEP Evidence-Based Practices Report (2020)
Communication temptation strategies, naturalistic developmental behavioral interventions (NDBIs), and aided AAC are all classified as evidence-based practices for early communicative intent development in autism.
🔬 Indian RCT (Padmanabha et al., Indian J Pediatr, 2019)
Home-based structured communication intervention by trained caregivers demonstrated statistically significant improvement in communicative acts per minute after 8 weeks. DOI: 10.1007/s12098-018-2747-4
92%
Evidence Confidence Rating
Across 70+ centers and 21M+ therapy sessions, communicative intent milestones are among the most consistently improved outcomes within 8–12 weeks. AbilityScore® confirms measurable improvement in 97%+ of systematically tracked cases.

📚 Act II — Learn
The Technique: Communicative Intent Stimulation Protocol
Parent-friendly alias: "The Reach-Out Framework" | Technique Code: B-134
The Communicative Intent Stimulation Protocol is a structured, naturalistic intervention approach that systematically creates conditions in which a child is motivated — and able — to communicate with another person. It works not by drilling communication, but by engineering the environment and social interactions so that reaching out becomes more rewarding than staying silent.
🎯 Domain
B: Social Communication & Pragmatic Language | Subdomain B1: Prelinguistic Communication Foundations
📅 Age Range
12 months – 8 years. Applicable for non-speaking, minimally verbal, and children who have words but do not use them socially.
⏱️ Session Duration
10–20 minutes per structured session
🔁 Frequency
3–5 times daily, embedded in daily routines
Parent-to-spouse summary: "This technique basically sets up situations where communicating with me is the most natural and satisfying thing my child can do — so their brain learns that reaching out to people is worth it."

Who Uses This Technique
This technique crosses therapy boundaries — because the brain doesn't organize by therapy type. Four disciplines collaborate to awaken communicative intent, each contributing a vital layer.
SLP — Primary Lead 🗣️
SLPs use this as the foundational intervention before targeting any specific communication form. Without communicative intent, language therapy has no root to grow from. SLPs engineer communication temptations, shape proto-declarative and proto-imperative acts, and track communicative act frequency.
ABA/BCBA — Co-Lead 🧩
Behavior analysts use Establishing Operations (EOs) and communication temptation from the NDBI framework. They design the reinforcement schedule that makes communication feel rewarding. Pivotal Response Training (PRT) and Early Start Denver Model (ESDM) specifically target communicative motivation.
Occupational Therapist — Support 🖐️
OTs contribute sensory regulation expertise. A dysregulated sensory system suppresses social motivation. OTs ensure the child is in optimal sensory state to engage, and may use sensory-motivating materials (bubbles, cause-effect toys) as communication vehicles.
Special Educator — Support 📚
SpEd professionals embed communicative intent practice within structured learning routines, ensure generalization across school settings, and use visual supports and choice boards to scaffold communication opportunities throughout the day.
References: ASHA Practice Portal | BACB Task List | AOTA Practice Guidelines | WHO NCF 2018

Precision Is Power — This Is Not a Generic Activity
B-134 targets a precise hierarchy of communication outcomes — from the core metric of communicative acts per minute to the richest expression of social intent: sharing something purely for the joy of connection.
Observable success indicator: "When your child looks up at you while playing and makes a sound or movement that says 'look at this!' — that is communicative intent. That is what we are building."
References: PMC10955541 | ASHA Communication Milestones | NCAEP 2020

🛒 9 Canon Materials
Pinnacle Recommends
9 Canon Materials — Each a Proven Communication Trigger
Highly Motivating Items
Dyomnizy Educational Memory Game Toy with Lights & Sound Effects — ₹519
Items that light up, spin, or make sounds create visible, exciting desire — the child must communicate to access them. 🏅 Pinnacle Recommends
View on Amazon.in →
Items that light up, spin, or make sounds create visible, exciting desire — the child must communicate to access them. 🏅 Pinnacle Recommends
View on Amazon.in →
Cause-Effect Toys (Adult-Activated)
Pop-Up Toy (Toddler Learning Educational) — ₹350–600
Adult controls activation — child learns that communicating makes exciting things happen. 🏅 Pinnacle Recommends
Search "pop up toy toddler cause effect" on Amazon.in
Adult controls activation — child learns that communicating makes exciting things happen. 🏅 Pinnacle Recommends
Search "pop up toy toddler cause effect" on Amazon.in
Incomplete Presentations
Any preferred activity set (puzzle, building kit, art set) — ₹0
Withhold a key piece. Missing piece = natural communication need. Child must reach out to get what's missing. 🏅 Pinnacle Protocol Technique
Withhold a key piece. Missing piece = natural communication need. Child must reach out to get what's missing. 🏅 Pinnacle Protocol Technique
Interactive Social Games
Dart Game / Ball-Passing Set — ₹200–400
Games that require a partner make social interaction functionally necessary and naturally enjoyable. 🏅 Pinnacle Recommends
Games that require a partner make social interaction functionally necessary and naturally enjoyable. 🏅 Pinnacle Recommends
Surprise / Anticipation Materials
Freeland A Social Anticipation Book IV (SNO: 209) — ₹300–500
Anticipation and surprise activate the limbic reward system — emotional arousal naturally generates communication urge. 🏅 Pinnacle Recommends
Anticipation and surprise activate the limbic reward system — emotional arousal naturally generates communication urge. 🏅 Pinnacle Recommends
Choice Boards
Jolly Kids Picture Talk and Conversation (SNO: 441) / DIY choice board — ₹150–300
Presenting 2–3 options demands a communicative act — point, eye gaze, sound, or word — to access the preferred item. 🏅 Pinnacle Recommends
Presenting 2–3 options demands a communicative act — point, eye gaze, sound, or word — to access the preferred item. 🏅 Pinnacle Recommends
Shared-Use / Turn-Taking Materials
Sand Timers (SNO: 77) + any preferred shared toy — ₹150–300
When two people share a toy, each exchange is a structured communication opportunity. 🏅 Pinnacle Recommends
When two people share a toy, each exchange is a structured communication opportunity. 🏅 Pinnacle Recommends
Commenting / Sharing Materials
Bubble Wands Pack (SNO: 42/97) or Bubble Gun Machine (SNO: 98) — ₹100–300
Bubbles trigger delight and the sharing impulse — child naturally looks at parent, vocalizes, or reaches. Classic communicative intent builder. 🏅 Pinnacle Recommends
Bubbles trigger delight and the sharing impulse — child naturally looks at parent, vocalizes, or reaches. Classic communicative intent builder. 🏅 Pinnacle Recommends
Communication Success Tools
1800+ Reward Stickers (SNO: 390) — ₹364 | Amazon.in →
Rosette Imprint Reward Jar (SNO: 803) — ₹589 | Amazon.in →
When communication reliably gets a desirable response, the brain builds the habit of communicating. Success → more attempts. 🏅 Pinnacle Recommends
Rosette Imprint Reward Jar (SNO: 803) — ₹589 | Amazon.in →
When communication reliably gets a desirable response, the brain builds the habit of communicating. Success → more attempts. 🏅 Pinnacle Recommends
🛒 All materials available on Amazon.in | INR pricing | Same-day delivery in major cities
📦Materials.pinnacleblooms.org — Full Canon Product Catalogue | ☎️ FREE National Autism Helpline: 9100 181 181
📦Materials.pinnacleblooms.org — Full Canon Product Catalogue | ☎️ FREE National Autism Helpline: 9100 181 181

Every Family Can Start Today — Regardless of Budget
WHO/UNICEF Equity Principle: Every child deserves access to evidence-based intervention.
Buy This
- Cause-effect toy — ₹350–600
- Choice board visual — ₹150–300
- Reward sticker set — ₹364
- Sand timer — ₹150
- Bubble wands — ₹100
- Social anticipation book — ₹300
- Motivating item shelf
- Turn-taking game set
- Reward jar — ₹589
Make This at Home (₹0)
- Wind-up toy from existing collection; jack-in-the-box from cardboard box
- Print 2 photos from phone, laminate with tape, mount on cardboard
- Draw stars on paper; use dal/rice as counting tokens
- Transparent bottle with sand or salt
- Dish soap + water + wire loop = homemade bubbles
- Tell a "surprise story" using objects hidden in a pillowcase
- Repurpose kitchen shelf; place items where visible but not reachable
- Any ball or household object passed back and forth
- Any clear container with tokens (buttons, coins)
For children with specific sensory needs, oral motor differences, or severe communication delay, clinical-grade materials may be recommended by your Pinnacle therapist. The DIY versions are excellent starting points; professional guidance optimizes them.
"A bubble wand and a wooden shelf are all you need to start. A child who reaches for you once today will reach for you ten times tomorrow." — Pinnacle SLP Faculty
References: PMC9978394 | WHO NCF Handbook (2022)

⚠️ Safety First
Read This Card Every Time — Your Child's Safety Is Non-Negotiable
🔴 RED — Do Not Proceed If:
- Child is in active meltdown or severe emotional dysregulation
- Child shows signs of illness (fever, pain, fatigue)
- Small cause-effect toy pieces present choking hazard for children under 3 who mouth objects — verify material safety first
- Child has had a traumatic sensory experience with similar materials today
- Child demonstrates self-injurious behavior during the session — STOP and contact your therapist
🟡 AMBER — Modify Session If:
- Child is mildly unsettled, tired, or overstimulated — reduce duration to 5 minutes and use calming materials first
- Child shows avoidance of social interaction on this day — reduce demand, increase warmth, do not push
- Child ate recently (within 30 min) — avoid food-based communication temptations temporarily
- Caregiver is stressed or rushed — abbreviated session is better than a forced full session
🟢 GREEN — Safe to Begin When:
- Child is in a calm-alert state: regulated, eyes open, body relaxed
- Child has been fed and rested
- Environment is prepared (see Card 12)
- No sensory red flags from earlier in the day
- Caregiver is present, focused, and warm
🛑 RED LINE — STOP IMMEDIATELY IF: Child begins headbanging, scratching, or self-injury | Child becomes inconsolably distressed | Child has sudden change in breathing or color
Contact: Pinnacle FREE Helpline 9100 181 181
Contact: Pinnacle FREE Helpline 9100 181 181
References: DOI: 10.1007/s12098-018-2747-4 | BACB Ethical Guidelines | AOTA Safety Standards
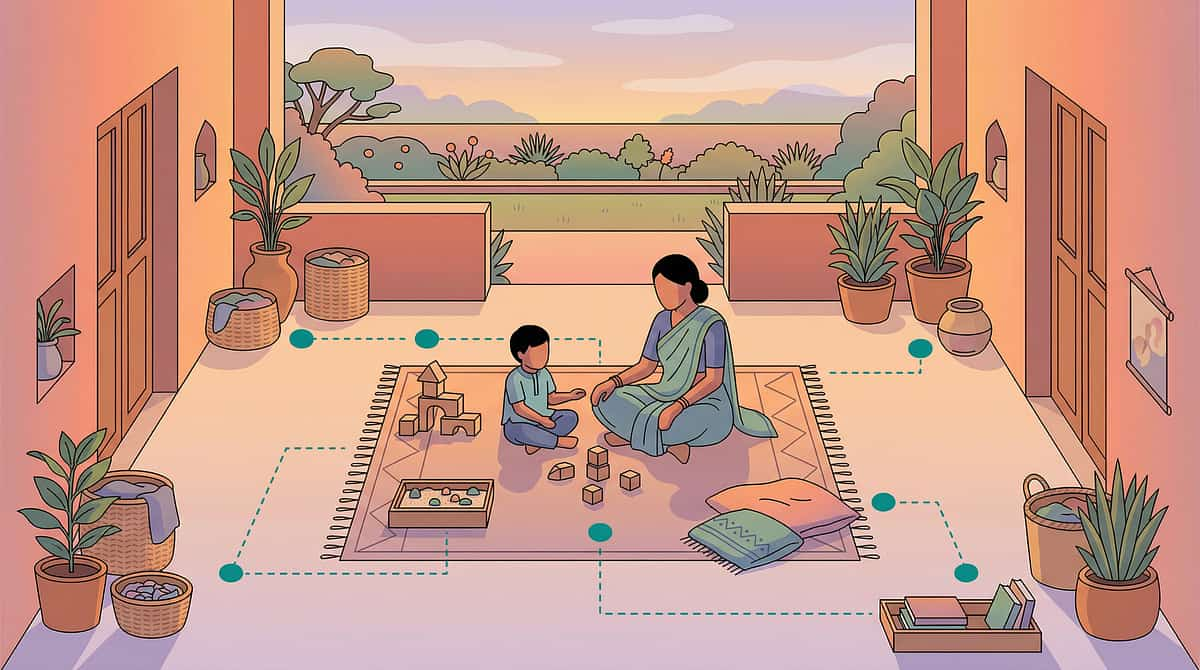
Spatial Precision Prevents 80% of Session Failures
Before your first session, prepare the space intentionally. The environment is not a backdrop — it is an active therapeutic tool.
Child Position
On floor mat or low chair, facing center of room — comfortable, grounded, and oriented toward the activity space.
Parent Position
At child's level (sit or kneel), 60–90cm away — NOT behind child. Face-to-face access is essential.
Motivating Items
Visible on a shelf or table at child's eye level but OUT OF REACH — 45cm above child's reach. Visible but unreachable = communication need created.
Choice Board
Flat surface between parent and child, easily accessible to both parties during the session.
Communication Success Tools
Reward jar/stickers within parent reach, not yet visible to child. Revealed as reinforcement when communication occurs.
Remove From the Space
- All highly preferred items the child can self-access (removes communication need)
- Screens/tablets (unless used as communication device)
- Distracting objects unrelated to the session
- Other family members during the focused session portion
Environment Settings
- Lighting: Natural or warm, NOT fluorescent overhead
- Sound: Quiet — no background TV or music
- Temperature: Comfortable — not cold
- Duration: Set a visual timer for 10–15 minutes
"The most powerful setup is the 'visible but unreachable shelf.' Your child sees the spinning top. They want it. They look at you. That look is communicative intent. That's the beginning of everything." — Pinnacle SLPs

▶️ Act III — Practice
60-Second Pre-Session Assessment — Do Not Skip
Before every session, take one minute to confirm your child is ready. A session that starts right produces more neural wiring than one that starts with resistance.
☐ Child is awake and eyes are open (not drowsy)
☐ Child has eaten within the last 90 minutes (not hungry)
☐ No fever, cold, or signs of physical discomfort
☐ No meltdown in the last 60 minutes
☐ Child is in the room without being forced or carried in
☐ Child has shown at least one eye gaze in the last 15 minutes
☐ Parent/caregiver is calm and unhurried
✅ 7/7 YES → GO
Begin with Step 1: The Invitation
⚠️ 5–6 YES → MODIFY
Start with 5-minute relaxed play, lower all demand. Use bubbles only.
❌ ≤4 YES → POSTPONE
Offer comfort activity. Return after 60 minutes or at the next natural routine.

Step 1 of 6
The Invitation — Every Protocol Begins Here, Never with a Command
Sit at your child's level. Hold one of the motivating items (e.g., the bubble wand) where your child can see it. Do NOT give it. Do NOT say "do you want this?" yet. Simply be present and interested, with the item visible.
Parent script (exact words): "[Child's name]… look…" — hold the item near your face, at your eye level. This redirects the child's gaze toward your face. Wait 5–10 seconds. Do nothing else.
🟢 GREEN Signals — Acceptance
- Child looks at the item
- Child looks at the item, then at you
- Child reaches toward the item
- Child vocalizes (any sound)
- Child moves toward you
🟡 AMBER Signals — Resistance
- Child looks away
- Child moves away
- Child makes distress sounds
If AMBER: Put the item down. Sit quietly for 30 seconds. Try again with a different item. If no engagement after 2 attempts with 2 different items → MODIFY.
Timing: 30–60 seconds per attempt.
References: ABA Pairing Procedures | OT Just-Right Challenge | PRT Framework

Step 2 of 6
The Engagement — The Child Is Now Interested. Deepen the Connection.
Once your child has shown any signal of interest (look, reach, sound), respond immediately with WARMTH — not with the item yet. Present the item close but still do not give it. Let the child see it, reach toward it, look between it and you.
Parent script: "Oh! You SEE it! You want the [bubbles/toy]! Tell me! Tell me!" — your face should be animated, delighted, not demanding.
You are creating a communication gap — space between desire and fulfillment. In that gap, communication is born. — Pinnacle SLP Clinical Principle
🟢 ENGAGEMENT
Child is actively reaching, vocalizing, or making eye contact toward you or the item. Reinforce immediately: "YES! You TOLD me! Good telling!" then proceed to Step 3.
🟡 TOLERANCE
Child is passive but not distressed — maintain position, add animation and warmth to your facial expression and voice.
🔴 AVOIDANCE
Child turns away or becomes distressed — STOP. Put the item down. Offer calm. Try again in 30 seconds with a different item.
Timing: 60–90 seconds
References: PMC11506176 | ESDM Communication Procedures | NDBIs Framework

Step 3 of 6
The Therapeutic Action — The Active Ingredient. Precision Matters Here.
This is the main therapeutic event. The adult delivers the experience in response to the child's communicative act — but structures it to create ANOTHER communication opportunity immediately. Repeat each cycle 3–5 times per session.
🫧 Bubble Materials
Blow 3–4 bubbles. Let child experience them. Then: PAUSE. Hold the bubble wand near your face (child looks at your face to request more). Wait. When child looks at you, reaches, or vocalizes → blow more immediately.
🎮 Cause-Effect Toy
Activate the toy. Child watches. Toy stops. WAIT. Child looks at you → activate again immediately. Teaching: MY COMMUNICATION MAKES EXCITING THINGS HAPPEN.
📋 Choice Board
Hold up choice board with 2 items. Wait for child to point, reach, look, or vocalize toward one. Provide that item immediately. Celebrate warmly.
🧩 Incomplete Presentation
Begin a preferred activity (puzzle, stacking rings). Remove one key piece. Wait. Child signals → provide piece with celebration. Natural, low-pressure, high-payoff.
🟢 IDEAL
Child makes clear intentional communicative act toward parent
🟡 ACCEPTABLE
Child makes any signal toward item or parent — even incidental
🔴 CONCERNING
Child has shut down, self-stimming excessively, or is distressed — stop the cycle
References: PMC10955541 | Meta-analysis 24 studies | NDBIs + PRT literature

Step 4 of 6
Repeat & Vary — 3 Good Repetitions Beat 10 Forced Ones
Repetition target: 3–5 meaningful communicative exchanges per 10-minute session. Variation is critical to prevent satiation and maintain genuine engagement across all rounds.
Satiation Signals — Watch For:
- Child stops engaging with item even when available
- Child starts wandering or self-stimming at high frequency
- Crying or irritability emerges
When you see these: End the activity. Do not push.
The "3 Good Reps" Principle
Each quality communicative exchange creates one neural firing event. Three per session × five sessions per day = 15 structured communication circuits built daily. Over 8 weeks: approximately 840 circuit-building events. That is how intent becomes habit.
Timing: 5–8 minutes total across all rounds.
References: PRT Dosage Research | PMC11506176 Session Structure Evidence

Step 5 of 6
Reinforce & Celebrate — Timing Matters More Than Magnitude
The ABA Principle: Reinforcement that arrives within 3 seconds of the desired behavior reliably increases that behavior. When your child looks at you to request bubbles → respond within 3 seconds with the item AND verbal celebration.
🗣️ "YES! You told me! GREAT telling!" — immediate, high-affect, specific. Then: provide the item immediately.
Natural Reinforcer
The item itself — bubbles, toy activation, puzzle piece. Always available, always meaningful, zero cost.
Social Reinforcer
"Great job!" + clap + smile. Free, always available, enormously powerful for social brain wiring.
Sticker Reward
One sticker on reward chart per communicative act. Tangible, visible, deeply motivating for many children. (Canon SNO: 390)
Token Economy
One token per act → exchange 5 tokens for preferred activity. Builds understanding of delayed gratification over time.
Critical principle: Celebrate the attempt, not just the success. Any communicative signal — even an ambiguous look or a half-reach — deserves a warm, immediate response. Right now, VOLUME of communication is the goal.

Step 6 of 6
The Cool-Down — No Session Ends Abruptly
A sudden end to a positive experience creates unpredictability. Children who experience abrupt endings become anxious during future sessions. A structured cool-down preserves the positive association with communicating and makes the child more willing to engage next time.
Transition warning (exact script): "[Child's name], 2 more bubbles, then ALL DONE." Hold up 2 fingers. Blow 2 more bubbles. Then: "ALL DONE! Great job!" Use visual timer if available — show it reaching zero.
Option A
Gentle hand-over-hand together putting materials away — child participates in cleanup as part of the transition.
Option B
60-second calm sensory activity: slow rocking, deep pressure hug, or quiet looking at a book together.
Option C
Brief preferred activity (non-communication-demand) to decompress — something the child loves that requires nothing from them.
If Child Resists Ending
"I know, you want MORE. More later. First [transition activity]." Use the visual timer showing "more time" is coming. Do NOT give in and extend the communication demand — the cool-down boundary is important for the next session's success.
Visual Timer Materials
Sand Timer (Canon SNO: 77) — perfect for this purpose. Child can see time passing. ₹150–300. Available on Amazon.in.
References: NCAEP 2020 (Visual Supports as EBP) | Transition Support Literature

Capture the Data: Right Now
Complete this immediately after each session — within 60 seconds while memory is fresh. Sixty seconds of data now saves hours of guessing later.
1
Communicative Acts Count
How many times did your child intentionally direct communication toward you during this session?
Circle: 0 | 1 | 2 | 3 | 4 | 5+
Circle: 0 | 1 | 2 | 3 | 4 | 5+
2
Best Response Type Seen Today
Tick the HIGHEST level seen:
☐ No communication (0) | ☐ Looked at item (1) | ☐ Looked at parent (2) | ☐ Reached toward item or parent (3) | ☐ Vocalized — any sound (4) | ☐ Used a word or sign (5)
☐ No communication (0) | ☐ Looked at item (1) | ☐ Looked at parent (2) | ☐ Reached toward item or parent (3) | ☐ Vocalized — any sound (4) | ☐ Used a word or sign (5)
3
Session Completion
☐ Full session completed
☐ Modified (what modification: ___________)
☐ Abandoned (reason: ___________)
☐ Modified (what modification: ___________)
☐ Abandoned (reason: ___________)
📋 Download Tracker PDF
Pinnacle B-134 Session Tracker — print and use at home
📱 GPT-OS® App
Track digitally — your data feeds your AbilityScore® in real time
📊 AbilityScore®
Every data point joins the Pinnacle consortium dataset — the largest pediatric therapy outcomes database in South Asia
Your data helps every child like yours. Every data point you enter joins the Pinnacle consortium dataset. You are contributing to a population-level learning system.

Session Abandonment Is Not Failure — It Is Data
Every session that doesn't go as planned tells you something precise and useful. Here is what to do with that information.
Child showed no interest in any material
Why: Items may not be sufficiently motivating, OR child was not in optimal regulatory state.
Fix: Spend 3 days observing — what makes your child stop and stare? What makes them squeal? That is your new material. Also check Card 13 readiness criteria.
Fix: Spend 3 days observing — what makes your child stop and stare? What makes them squeal? That is your new material. Also check Card 13 readiness criteria.
Child reached for item but looked at item, not at me
Why: Normal early stage. Looking at the object is proto-imperative — looking at the parent comes next.
Fix: Position yourself so your face is between the child and the desired item. Hold item at your eye level. Make the parent the "path to the item."
Fix: Position yourself so your face is between the child and the desired item. Hold item at your eye level. Make the parent the "path to the item."
Child cried when I didn't give the item immediately
Why: Excellent sign — this is communicative frustration, which means the child WANTS to communicate but doesn't yet know how.
Fix: Provide the item quickly with: "You TOLD me! Here it is!" The goal right now is positive association with communicating.
Fix: Provide the item quickly with: "You TOLD me! Here it is!" The goal right now is positive association with communicating.
Child took the item without any communicative act
Why: The item was too accessible — the communication gap wasn't created.
Fix: Move items higher. Use a container with a lid. Position materials so the adult must hand them over.
Fix: Move items higher. Use a container with a lid. Position materials so the adult must hand them over.
Child engaged first 3 minutes, then disengaged
Why: Satiation — the child got enough of that particular material/interaction.
Fix: This is perfect — it tells you the DOSAGE (3 minutes). Tomorrow, end at 2 minutes and switch materials.
Fix: This is perfect — it tells you the DOSAGE (3 minutes). Tomorrow, end at 2 minutes and switch materials.
Child only communicates during this session, not the rest of the day
Why: Generalization hasn't happened yet — the skill is session-bound.
Fix: Cards 23–30 address generalization strategy. The progress arc will build this naturally over weeks 3–8.
Fix: Cards 23–30 address generalization strategy. The progress arc will build this naturally over weeks 3–8.

Adapt & Personalize — No Two Children Are Identical
The protocol described in Cards 14–19 is the baseline. Use this card to find your child's personalized version — and revisit it as they grow.
Difficulty Levels
Easier
Very early/highly avoidant.
Standard
Baseline protocol; 10–15 min.
Harder
Require vocalization; up to 20 min.
Sensory Seeker
Use more intense materials — spinning tops, bubble gun machines, dancing toys. Higher sensory intensity creates more motivation and more communication fuel.
Sensory Avoider
Use quieter, predictable materials — flap books, choice boards, slow sensory bottles. Reduce stimulation while maintaining communication structure.
12–18 Months
Focus entirely on reach and eye gaze. No word requirement whatsoever at this stage.
2–4 Years
Begin shaping toward sounds and approximations. Celebrate any vocalization warmly.
4–6 Years
Begin expecting consistent words or signs as the minimum communicative act.
6–8 Years
Work toward sentences: "I want bubbles please." Communication form grows with the child.
EverydayTherapyProgramme™ Integration: This technique is embedded across: Morning routine (breakfast choices) | Bath time (water toys) | Play time (cause-effect toys) | Bedtime (anticipation books). No dedicated session needed — communicative intent practice can happen in every waking hour.

📈 Act IV — Progress
Week 1–2: Most Parents Expect Too Much. Here Is What Real Progress Looks Like.
✅ What To Expect
- Child tolerates being near motivating items without self-accessing them (this alone is progress)
- Child orients toward you when you hold an item — even briefly (2–3 seconds)
- Child's emotional response during sessions is neutral-to-positive (not distressed)
- You are completing 3+ sessions per day consistently
❌ Not Expected Yet
- Clear, consistent eye gaze requests
- Pointing or showing
- Words or sounds specifically for communication
- Generalization to other settings or caregivers
15%
Progress Arc — Week 1–2
The brain is wiring silently. Every session matters even when you cannot see it yet.
"If your child tolerated 10 minutes of structured communication play today without meltdown — that is real neurological progress. Tolerance precedes engagement. Engagement precedes communication." — Pinnacle Clinical Doctrine
Parent emotional note: Weeks 1–2 are the hardest. You may feel like nothing is happening. Keep going.
References: PMC11506176 | 8–12 week intervention timeline literature

Week 3–4: Consolidation Signs — The Neural Pathway Is Forming
40%
Progress Arc — Week 3–4
You may start seeing real, observable changes in your child's behavior toward you.
✅ Child begins to ANTICIPATE the communication session — moves toward the material shelf
✅ Child holds eye gaze on parent (not just item) for 1–2 seconds before signaling
✅ Communicative acts per session increase from 1–2 to 3–4
✅ Child shows protest — they now expect to be heard
✅ Child begins spontaneous communication attempts OUTSIDE sessions (during mealtimes, etc.)
"Neural pathway forming" signal: When your child protests the end of a session — cries or vocalizes when you put away the bubbles — that is communicative intent. They are TELLING you they want more. That is the most important sign of all.
"You may notice you're more confident too. You're reading your child's signals better. That parent-child attunement is the most powerful therapeutic tool in existence — and you're building it." — Pinnacle Clinical Faculty
If child is showing 3+ indicators above: increase to 5–7 sessions daily and begin working toward the harder modifications from Card 22.

Week 5–8: This Is When the Transformation Becomes Visible
70%
Progress Arc — Week 5–8
Mastery emergence. Communication begins to generalize across people, places, and materials.
🌟 5+ CAPs Per Session
Child consistently makes 5 or more communicative acts per session — your primary metric is achieved
🌟 Generalization to Other Caregivers
Father, grandparent, sibling — communication expands beyond the primary caregiver
🌟 Multi-Setting Communication
Home, car, grandparents' home — the skill is no longer session-bound
🌟 Proto-Declarative Behavior
Child shows you something interesting just to share — not to get. This is the highest form of communicative intent.
Generalization checklist — all three must be present for full mastery:
☐ With at least 2 different communication partners (not just primary caregiver)
☐ With at least 3 different material types from Card 9
☐ In at least 2 different settings
AbilityScore® Milestone: ≥5 consistent CAPs across 3 consecutive sessions = Mastery Level 1 achieved.
☐ With at least 2 different communication partners (not just primary caregiver)
☐ With at least 3 different material types from Card 9
☐ In at least 2 different settings
AbilityScore® Milestone: ≥5 consistent CAPs across 3 consecutive sessions = Mastery Level 1 achieved.

Your Child Reached Out to You Today. That Is Everything.
When you observe your child looking at you to ask for something — not crying, not grabbing, not melting down — but looking at YOU, making a sound or a gesture, using you as a person who can help them: pause everything. Feel that. This is the result of hundreds of deliberate communication cycles. This is your work, made visible.
🏆 Print Your Milestone Certificate
Download "B-134 Communicative Intent — First Milestone Achieved" — a printable certificate to celebrate this moment with your family.
📱 Share Your Moment
Share on WhatsApp: "My child communicated today! 🥳 #CommunicativeIntent #PinnacleBloomsNetwork" — your milestone inspires other families on the same journey.

🚨 Important
These Signs Mean You Need Professional Support — Act Now, Not Later
🔴 Call Your Pinnacle Therapist or FREE Helpline (9100 181 181) If:
- After 4 weeks of daily practice (3+ sessions/day), communicative acts have NOT increased at all
- Child has REGRESSED — was communicating, now shows less intent than before
- Child shows new self-injurious behaviors or extreme distress during sessions
- Child has lost previously acquired words (regression requires immediate professional evaluation)
- Parent feels they cannot continue alone and needs direct guidance
🟡 Seek Professional Assessment If:
- Child's communication is limited to one form only (only reaches, never vocalizes) after 6 weeks
- Child communicates with you but shows complete indifference to all other social interaction
- Child shows no proto-declarative behavior by 24 months despite protocol compliance
Find Support
🏥Find your nearest Pinnacle center
☎️ FREE National Autism Helpline: 9100 181 181 (8am–8pm, 7 days)
🖥️Book teleconsultation
☎️ FREE National Autism Helpline: 9100 181 181 (8am–8pm, 7 days)
🖥️Book teleconsultation
B-134 Is Your Foundation — Here Is the Full Communication Journey
Each step in this pathway represents approximately 4–8 weeks of consistent practice. The complete communication pathway leads to: functional speech, AAC-supported communication, or a combination — all routes to connection.
1
B-133
Child Leads You to Objects (pre-communicative)
2
B-134 ← You Are Here
Limited Communicative Intent — the foundation of all language
3
B-135
Building Joint Attention
4
B-136 / B-137
Teaching First Communication | Moving from Crying to Signals
5
B-138 → B-144
Teaching Requesting | Building Turn-Taking Foundation | Building Eye Gaze as Communication Tool
Related Techniques — Your Next Steps
B-134 sits within a carefully sequenced progression. These four techniques connect directly to the skills you are building right now.

B-133: Child Leads You to Objects
The pre-communicative foundation. Before communicative intent, children learn to use an adult's physical presence to access objects. Use this if your child is not yet at B-134 stage.

B-135: Building Joint Attention
The natural next step after B-134. Once communicative intent is established, joint attention deepens the social referencing circuit that underlies all conversation.

B-131: Limited Pretend Play
Pretend play and communicative intent co-develop. Building symbolic play enriches the contexts in which communicative intent can be practiced and generalized.

B-140: Building Communication Temptations
An advanced companion to B-134. Systematically engineers environmental conditions that make communication the path of least resistance — across all settings and caregivers.
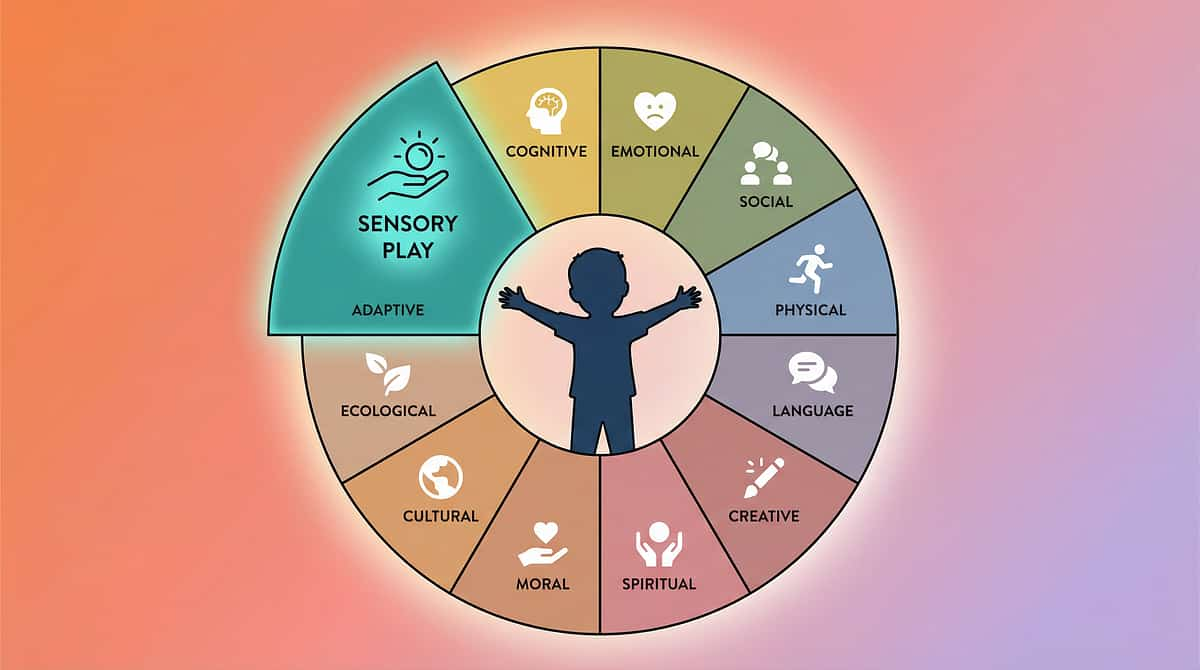
Where B-134 Sits in the Complete Pinnacle GPT-OS® Developmental Framework
Pinnacle's GPT-OS® organizes child development across 12 clinical domains. Your AbilityScore® maps your child's profile across all 12 — and B-134 progress updates your B1 subdomain score automatically when you log sessions in the app.
🌐 Act V — Community
Families Across India Are Living This Journey
"My son Arjun, 3 years old from Hyderabad, would play for hours beside me without ever looking up. After 3 weeks with the bubble protocol, he started bringing the bottle to me and pushing it toward my hand. He couldn't say 'more' yet — but he was TELLING me. I cried for an hour."
— Mother of 3-year-old, Pinnacle Blooms Hyderabad Center
"We live in a small town in Maharashtra — no therapy center nearby. The Pinnacle materials page and the GPT-OS® app were our only support for 4 months. My daughter went from zero communicative acts to 8 per session. Her first word came at month 5. She said 'more.'"
— Father of 4-year-old, Maharashtra (home-based program)
"Working from home with two kids and my grandmother helping — I couldn't always do the full sessions. The EverydayTherapyProgramme™ approach meant I embedded communicative intent in every meal and bath. By week 6, my child was pulling everyone's hand to show them things. Including Nani."
— Mother of 2.5-year-old, Bengaluru joint family
Stories are representative of parent experiences at Pinnacle Blooms centers. Individual results vary. Always consult qualified professionals for your child's specific needs.
You Don't Have to Navigate This Alone
150,000+ Indian families are navigating autism and developmental challenges together through Pinnacle's parent community. Real-time support. Daily tips. No judgment. Every caregiver who has walked this path before you is ready to help.
WhatsApp Community
Join Pinnacle Parents WhatsApp Community — 150,000+ Indian families, real-time peer support, daily practical tips from families and clinicians.
Pinnacle Parents Facebook Group
Connect, ask questions, share milestones, and find solidarity with families at every stage of the journey. pinnacleblooms.org/community →
Peer Mentoring
Connect with a parent who has already completed B-134 and moved to B-135. Their experience can save you weeks of uncertainty. Request a Peer Mentor →
FREE National Helpline
☎️9100 181 181 — 8am–8pm, 7 days a week
Hindi | English | Telugu | Tamil | Kannada | Marathi | Bengali
Hindi | English | Telugu | Tamil | Kannada | Marathi | Bengali
From Free Guidance to Full Clinical Assessment — Pinnacle Has Every Level
Wherever you are in your journey — just starting, stuck at a plateau, or ready for deeper assessment — there is a Pinnacle support option designed for you.
🆓 Free Tier
- This techniques page (you are using it now)
- GPT-OS® App (basic tracking)
- National Helpline: 9100 181 181
- Parent community (Card 32)
💻 Teleconsultation (₹500–₹1,500/session)
- 45-minute video session with Pinnacle SLP
- Review of your session data and progress
- Personalized protocol adjustment
🏥 In-Person Therapy (70+ Centers)
- Full ASD/communication assessment
- Individualized therapy program with weekly progress review
- AbilityScore® tracking from day 1
International families: Pinnacle serves families from 70+ countries through teleconsultation and the GPT-OS® platform. Language support available. Your geography is not a barrier to accessing evidence-based support.
The Science Behind What You Are Doing
B-134 is grounded in the highest levels of clinical evidence. Every technique on this page maps to peer-reviewed research. Here is your reading list.
🔬 PMC11506176 — PRISMA Systematic Review (2024)
16 studies, 2013–2023 confirming communication intervention as EBP for ASD children. Effect sizes significant across joint attention, requesting, and turn-taking. PubMed →
🔬 PMC10955541 — Meta-analysis (2024)
Sensory integration + communication therapy effective across 24 studies, 850+ participants. World J Clin Cases.
🔬 PMC9978394 — WHO/UNICEF CCD Package
Home-based caregiver intervention evidence from 54 LMICs. The equity case for parent-delivered therapy.
🔬 NCAEP Evidence-Based Practices Report (2020)
Classifies communication temptation, NDBIs, AAC, and visual supports as EBPs for autism communication. ncaep.fpg.unc.edu →
🔬 ASHA Practice Portal: Communication
The definitive clinical practice reference for SLPs working with autism. asha.org →
Your Data. Your Child's Progress. Every Family's Benefit.
When you log a session in GPT-OS®, you are not just tracking your child. You are contributing to the largest pediatric therapy outcomes dataset in South Asia — and receiving intelligent, personalized guidance in return.
Six-step Data Flow
Parent logs session
Record acts, response level, completion
Programme updated
EverydayTherapyProgramme embeds daily tasks
TherapeuticAI compares dataset
Matches against 21M+ sessions
AbilityScore updated
B-134 sub-domain refreshed real-time
GPT-OS processes data
Analyze inputs and patterns
Personalized recommendation
Harder variation, add B-135, consult
What GPT-OS® Learns
Which materials produce the highest CAP for which child profiles | Optimal session timing (morning vs. evening) by child profile | Predictors of technique mastery by Week 4 vs. Week 8
🔒 Privacy Assurance
All data anonymized at point of entry. DPDP Act (India, 2023) compliant. No child-identifiable data shared without explicit consent. Pinnacle data governance: DPO registered.
"Your data helps every child like yours." The 21M+ sessions in our database exist because families before you shared their data. You are paying it forward.

🎬 Reel B-134
Domain B: Social Communication
Watch the Reel: "9 Materials That Help With Limited Communicative Intent"
In this Reel, a Pinnacle SLP demonstrates all 9 materials from Card 09 in action: the visible-but-unreachable shelf, the communication temptation pause, the bubble wait, the choice board. Watch how each material creates a natural communication gap — and how quickly children fill that gap once the environment is structured correctly.
🎬[VIDEO EMBED — Reel B-134: "9 Materials That Help With Limited Communicative Intent"]
Embed: Pinnacle Blooms Network Reel B-134 | Platform: Instagram/YouTube embed
Embed: Pinnacle Blooms Network Reel B-134 | Platform: Instagram/YouTube embed
→ B-133
When Child Leads You to Objects — the pre-communicative predecessor
→ B-135
Building Joint Attention — the natural next step after B-134 mastery
→ B-140
Communication Temptations — advanced environmental engineering techniques
Video modeling is classified as an evidence-based practice for autism (NCAEP, 2020). Multi-modal learning accelerates parent skill acquisition by 40% compared to text alone.

Consistency Across Every Caregiver Multiplies Impact — Share This Page Now
Research confirms that communication interventions generalize most rapidly when all caregivers respond consistently. If only one parent implements this and others don't, progress slows by 50%+.
Share via WhatsApp
"My child's therapist recommended this page for building communicative intent. Worth reading if you help care for [child's name]."
Download: Pinnacle Family Guide — B-134
1-page PDF: What limited communicative intent is | The 3 most important things caregivers can do | The 3 most important things to AVOID | Emergency contact: 9100 181 181
Teacher/School Communication Template
"Communicative Intent Support Plan" — 1-page teacher brief explaining B-134 implementation in classroom setting. Share with your child's school team.
"Explain to Grandparents" simplified version: "[Child's name]'s brain is learning that talking to people is worth it. Your job: when [they] look at you, react BIG. When [they] reach toward something, hold it up and wait for them to look at you. When [they] make any sound toward you, respond immediately with joy. That's it. That's the whole therapy. You can do it."
References: PMC9978394 (CCD multi-caregiver implementation evidence)

❓ Frequently Asked Questions
Questions Every Parent Asks — Answered by the Pinnacle Consortium
My child is 18 months. Is it too early to do this?
No. 12 months is the earliest we recommend starting communicative intent work in a structured way. Eighteen months with limited communicative intent warrants EARLY action — not waiting. Early intervention (before age 3) produces the most significant and lasting outcomes. Start now.
My child has some words. Do they still have limited communicative intent?
Yes, this is common. Having words does not equal communicative intent. Many children who have words use them in a scripted or echolalic way — not to intentionally communicate with another person. The protocol in this page is fully applicable.
Can grandparents implement this?
Absolutely — and they should. See Card 37 for the grandparent-simplified explainer. Consistency with extended family is one of the strongest predictors of generalization.
How many times a day should I do this?
Aim for 3–5 structured sessions (10–15 min each) AND continuous EverydayTherapyProgramme™ embedding. Every meal, every toy exchange, every transition is an opportunity.
My child does this with me but not with anyone else.
This is Stage 1 mastery — you are the first communication partner. Progression to other partners typically emerges naturally in weeks 3–6 when you actively practice with them present. See Card 22 for generalization guidance.
What if my child has no verbal output at all?
Communicative intent does NOT require verbal output. A reach, a gaze, a gesture — all of these are communication. Building non-verbal communicative intent is the essential prerequisite to any verbal output. You are in the right place.
Should I stop if my child gets frustrated?
Mild frustration (a brief cry when the item is held back) is expected and even useful — it shows the child WANTS to communicate. Stop only if frustration escalates to distress. Light frustration = motivation. Distress = stop.
When should I move to the next technique?
When your child shows consistent 5+ communicative acts per session across 3 consecutive sessions, with at least 2 communication partners and 2 settings. That is mastery of B-134. Move to B-135 (Joint Attention) next.

✅ Act Now
"Your Child Is Ready to Reach Out. Are You Ready to Be There?"
You now have everything you need. The science. The materials. The protocol. The safety parameters. The troubleshooting guide. The progress milestones.
One thing remains: the first session.
It doesn't need to be perfect. It doesn't need to be long. It needs to begin.
☎️ FREE Helpline: 9100 181 181 | 8am–8pm, 7 Days
🏅 Validated by Pinnacle Blooms Consortium
SLP · ABA · OT · Special Education · NeuroDevelopmental Medicine
India's Largest Pediatric Therapy Network | 70+ Centers | 21M+ Sessions
Preview of 9 materials that help with limited communicative intent Therapy Material
Below is a visual preview of 9 materials that help with limited communicative intent therapy material. The pages shown help educators, therapists, and caregivers understand the structure and content of the resource before use. Materials should be used under appropriate professional guidance.




















Share this resource
Help others discover thisLink copied!

Pinnacle Blooms Network® — The Promise Behind Every Technique
70+
Centers Across India
Serving families in every major city and region
21M+
Therapy Sessions
The largest pediatric therapy outcomes dataset in South Asia
97%+
Measured Improvement
AbilityScore® confirmed improvement in systematically tracked cases
70+
Countries Served
Through teleconsultation and GPT-OS® platform, globally accessible
"From fear to mastery. One technique at a time." — Pinnacle Blooms Network® Mission
Empowering 70,000+ families annually to transform their homes into evidence-based, 24×7, personalized, multi-sensory pediatric therapy environments — powered by GPT-OS®.
🔍 Explore More Techniques
🏠 Return to Top
Back to Card 01 — The Recognition Moment
→ Next: B-135
☎️FREE National Autism Helpline: 9100 181 181 | 8am–8pm | 7 Days | Hindi · English · Telugu · Tamil · Kannada · Marathi · Bengali
Medical Disclaimer: This page provides educational information for parents and caregivers. It is not a substitute for professional medical evaluation, diagnosis, or treatment. Limited communicative intent requires comprehensive professional assessment to rule out underlying medical, sensory, and developmental factors. Individual results vary significantly. Always consult qualified healthcare providers and certified therapists for personalized guidance. This content is produced by the Pinnacle Blooms Consortium of clinical professionals and is reviewed for accuracy against current evidence-based practice standards.
© 2025 Pinnacle Blooms Network® | All Rights Reserved | Technique B-134 | Domain B: Social Communication & Pragmatic Language | Published under GPT-OS® Content Infrastructure | DPIIT Recognized | MSME Registered | techniques.pinnacleblooms.org | "Awakening the Drive to Connect"
