
"I barely touched her arm. She screamed like I'd burned her."
It's bath time. You reach to wash her arm — gently, carefully, the way you always do. She screams. Pulls away. Her whole body tenses like you've pressed a hot iron against her skin. You barely touched her. At school, a classmate bumps her in the lunch line. Full meltdown. The teacher says she's "being dramatic." At the birthday party, another child grabs her hand for a game. She hits them. You leave early. Again.
You've cut every tag from every piece of clothing she owns. You've learned to announce every touch before it happens. You've stopped kissing her goodnight because even that feels like too much for her. Other people think she's overreacting. You know she's not. You can see it in her eyes — this is real.
Light Touch Defensiveness is not drama. It's not attention-seeking. It's a neurological wiring difference — and there are 9 specific materials that help recalibrate it.
You are not failing. Your child's nervous system is speaking. And now, you're going to learn its language.
Pinnacle Blooms Consortium
OT • SLP • ABA • SpEd • NeuroDev • CRO
Research: WHO Nurturing Care Framework (2018) — Early identification and parental awareness directly impacts developmental outcomes. nurturing-care.org/ncf-for-ecd

You Are Not Alone — The Numbers
You are among millions of families navigating this exact challenge. Tactile defensiveness — specifically to light touch — is one of the most common sensory processing patterns in children with autism spectrum conditions, sensory processing differences, and developmental variations. In India alone, with an estimated 1.8 crore children on the autism spectrum, this translates to over 1.4 crore families dealing with touch-related challenges every single day.
80%
Sensory Processing Difficulties
Of children diagnosed with autism experience sensory processing difficulties (PRISMA Systematic Review, 2024)
60–90%
Tactile Over-Responsivity
Of children with SPD show tactile over-responsivity as a primary feature (Sensory integration research literature)
1 in 6
Global Prevalence
Children globally show sensory processing differences significant enough to impact daily functioning
This is not rare. This is not unusual. This is one of the most well-documented sensory patterns in pediatric literature — and one of the most responsive to structured intervention.
Research: PRISMA systematic review (2024): PMC11506176 | Meta-analysis: PMC10955541 | DOI: 10.12998/wjcc.v12.i7.1260

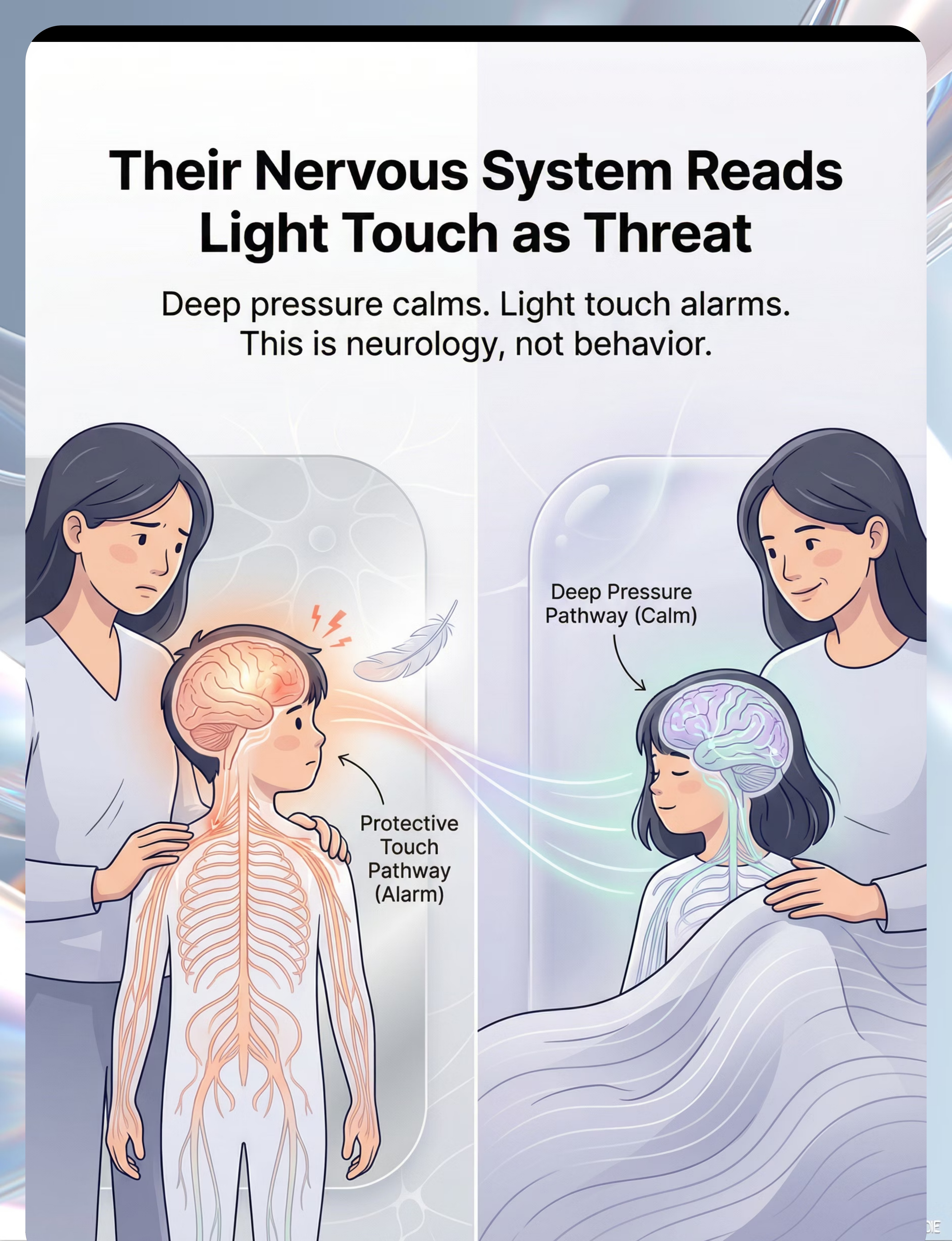
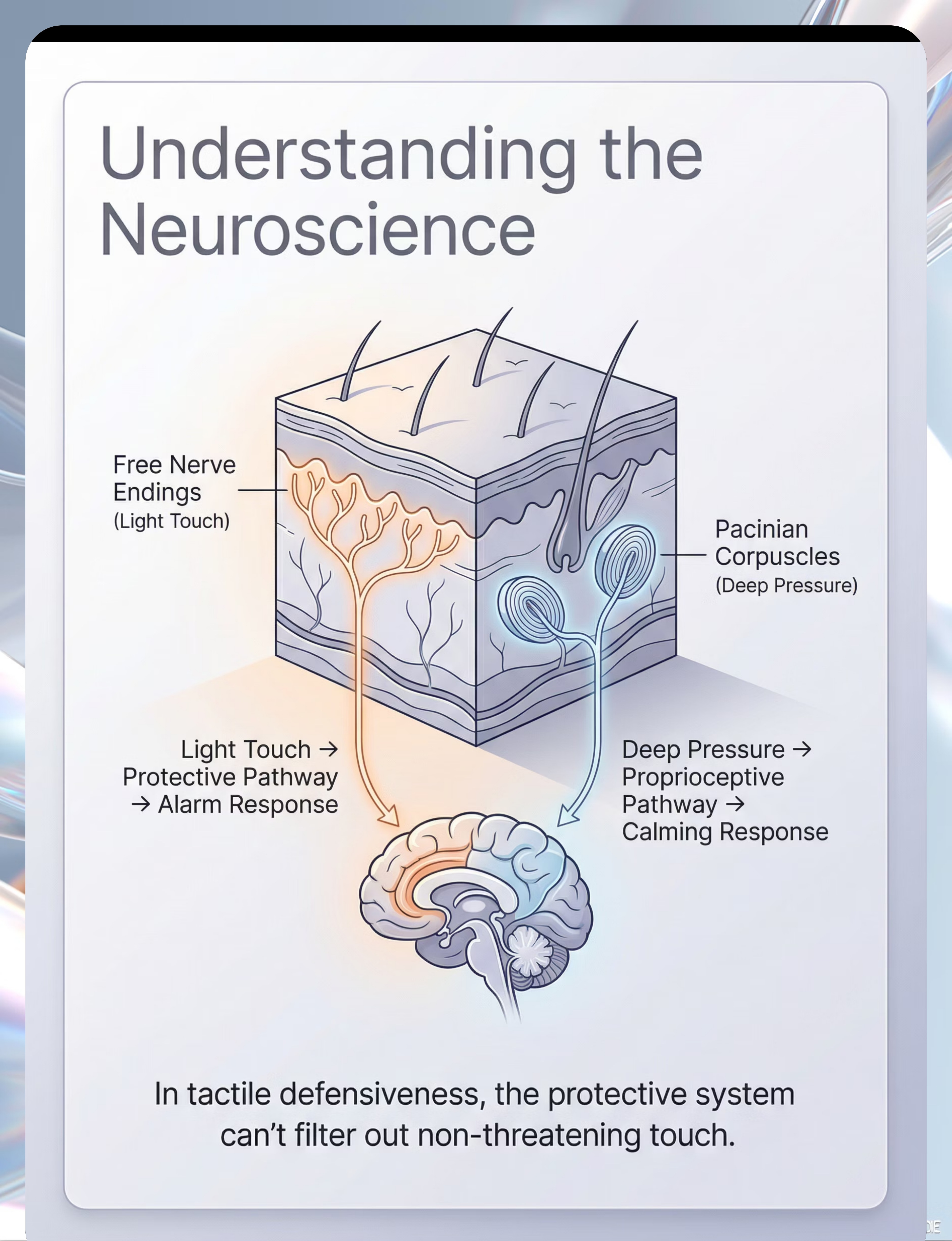
Their Nervous System Reads Light Touch as Threat
Your child has two touch pathways. Everyone does.
Pathway 1 — The Protective System (Light Touch)
Free nerve endings near the skin surface detect light, unexpected touch. In most children, this pathway filters out non-threatening input — a clothing tag, a breeze, a casual brush. In your child, this filter is set too high. Every light touch triggers the alarm.
Pathway 2 — The Calming System (Deep Pressure)
Deeper receptors called Pacinian corpuscles detect firm, sustained pressure. This pathway sends calming signals through the proprioceptive system. This is why your child may seek heavy blankets, tight hugs, or firm pressure — deep input feels safe.
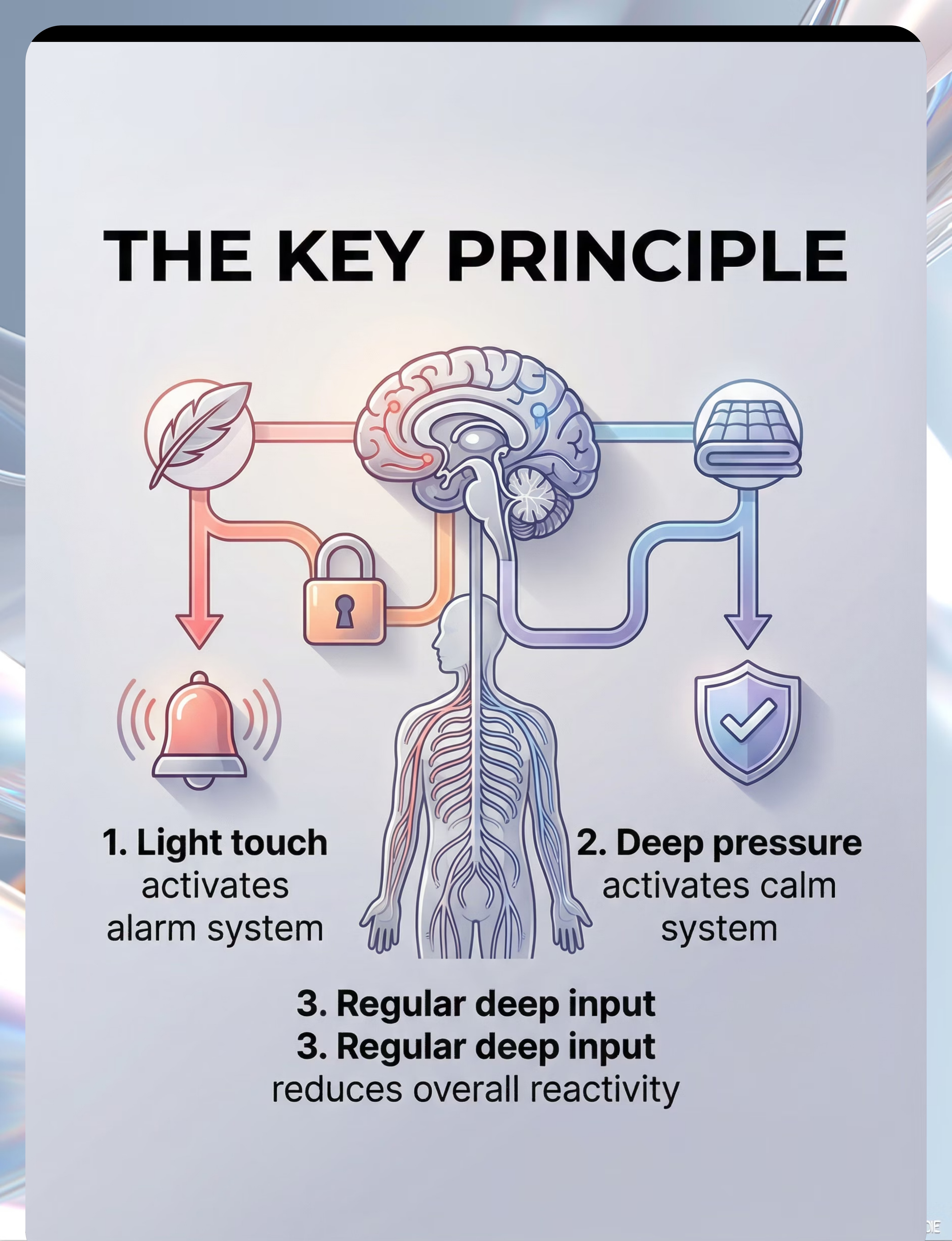
The Paradox Explained: Light touch activates fight-flight-freeze. Deep pressure activates calm-connect-regulate. This is why your child screams at a gentle pat but sleeps peacefully under three heavy blankets. It's not contradiction — it's neurology.
This is a wiring difference, not a behavior choice. Your child is not being dramatic. Their brain is genuinely interpreting gentle touch as a threat signal.
Research: Frontiers in Integrative Neuroscience (2020) — DOI: 10.3389/fnint.2020.556660

Where Light Touch Defensiveness Sits in Development
0–6 Months
Tactile system developing. Primitive protective reflexes dominant. All babies startle to unexpected touch.
6–18 Months
Discriminative touch system maturing. Most infants begin tolerating varied textures and light touch from caregivers. Defensiveness may first emerge here.
18–36 Months ← Identification Window
Parents notice persistent, intense reactions to light touch. Clothing battles begin. Grooming resistance escalates. Social touch becomes problematic. Most families first seek answers here.
3–6 Years
Impact on school readiness. Standing in lines, sitting beside peers, wearing uniforms, tolerating classroom touch. Social isolation risk increases.
6–12 Years
Without intervention, avoidance patterns deepen. Social participation narrows. With intervention, significant improvement is documented.
Comorbidity Awareness: Light touch defensiveness commonly co-occurs with: clothing texture rigidity, messy play avoidance, hair brushing resistance, oral defensiveness (food textures), sleep disruption from bedding textures, and social touch avoidance.
Research: WHO Care for Child Development (CCD) Package | UNICEF MICS indicators | PMC9978394

The Evidence Behind Sensory Integration for Tactile Defensiveness
Evidence Grade: Level I–II
Systematic Reviews + RCTs
Key Finding: A 2024 PRISMA systematic review analyzing 16 articles from 2013–2023 confirms that sensory integration intervention meets criteria to be considered an evidence-based practice for children with ASD. Deep pressure-based interventions showed the strongest effect sizes for reducing tactile defensiveness.
Meta-Analysis (2024)
24 studies confirmed sensory integration therapy effectively promotes sensory processing, social skills, adaptive behavior, and motor skills. Individual 1:1 sessions, 2–3 times per week for 8–12 weeks showed maximum effectiveness. (PMC10955541)
Indian RCT (2019)
Home-based sensory interventions demonstrated significant outcomes in Indian pediatric populations — proving parent-administered protocols work. (DOI: 10.1007/s12098-018-2747-4, Padmanabha et al., Indian J Pediatr)
Neurological Basis (2020)
Comprehensive framework establishing the neural mechanisms by which sensory integration treatment modifies tactile processing in ASD. (DOI: 10.3389/fnint.2020.556660)
Clinically validated. Home-applicable. Parent-proven across 20M+ sessions at Pinnacle Blooms Network®.

ACT II: THE KNOWLEDGE TRANSFER
Deep Pressure Desensitization Protocol for Light Touch Defensiveness
Parent-Friendly Alias: "Calming the Alarm System" — Using 9 specific materials to retrain your child's nervous system to stop reading gentle touch as threat.
A structured, multi-material approach to reducing light touch defensiveness by systematically providing deep pressure input (which calms the nervous system), building predictability around touch (which reduces threat perception), and gradually expanding tactile tolerance (which recalibrates the protective system). This protocol combines 9 evidence-based materials and strategies — some require purchase, several are free techniques, and most have DIY alternatives. The approach works across home, school, and community settings when implemented consistently.
Domain
Sensory Processing → Tactile Processing → Light Touch Over-Responsivity
Age Range
2–12 years
Frequency
Daily (sensory diet), 2–3× weekly (structured sessions)
Setting
Home + School + Community
Investment
₹0–8,000 (many strategies are free)
Canon Materials: Weighted Blanket | Therapy Brush | Vibration Tools | Compression Clothing | Deep Pressure Fidgets | Joint Compressions | Touch Warnings | Texture Play | Sensory Diet

Which Experts Use This — And How
Occupational Therapist (OT) — PRIMARY LEAD
The OT leads tactile defensiveness intervention. They evaluate the sensory profile, design the sensory diet, train parents on the Wilbarger Protocol, select appropriate materials, and monitor progress through standardized assessment. The OT understands the neurological mechanisms and calibrates intervention intensity.
Speech-Language Pathologist (SLP)
Addresses oral defensiveness — a subset of tactile defensiveness affecting the mouth. Manages food texture tolerance, tooth brushing resistance, and oral motor sensitivity using deep pressure oral tools like Z-Vibes and NUK brushes.
Board Certified Behavior Analyst (BCBA)
Designs the reinforcement schedule for texture exposure sessions. Implements systematic desensitization protocols. Tracks behavioral data on defensive responses. Creates tolerance-building programs using ABA principles.
Special Educator
Adapts classroom environments to reduce defensive triggers. Implements touch warning systems in school settings. Modifies group activities to accommodate tactile sensitivity.
NeuroDevelopmental Pediatrician
Rules out medical causes of tactile hypersensitivity. Evaluates neurological contributors. Monitors for medication interactions that may affect sensory processing.
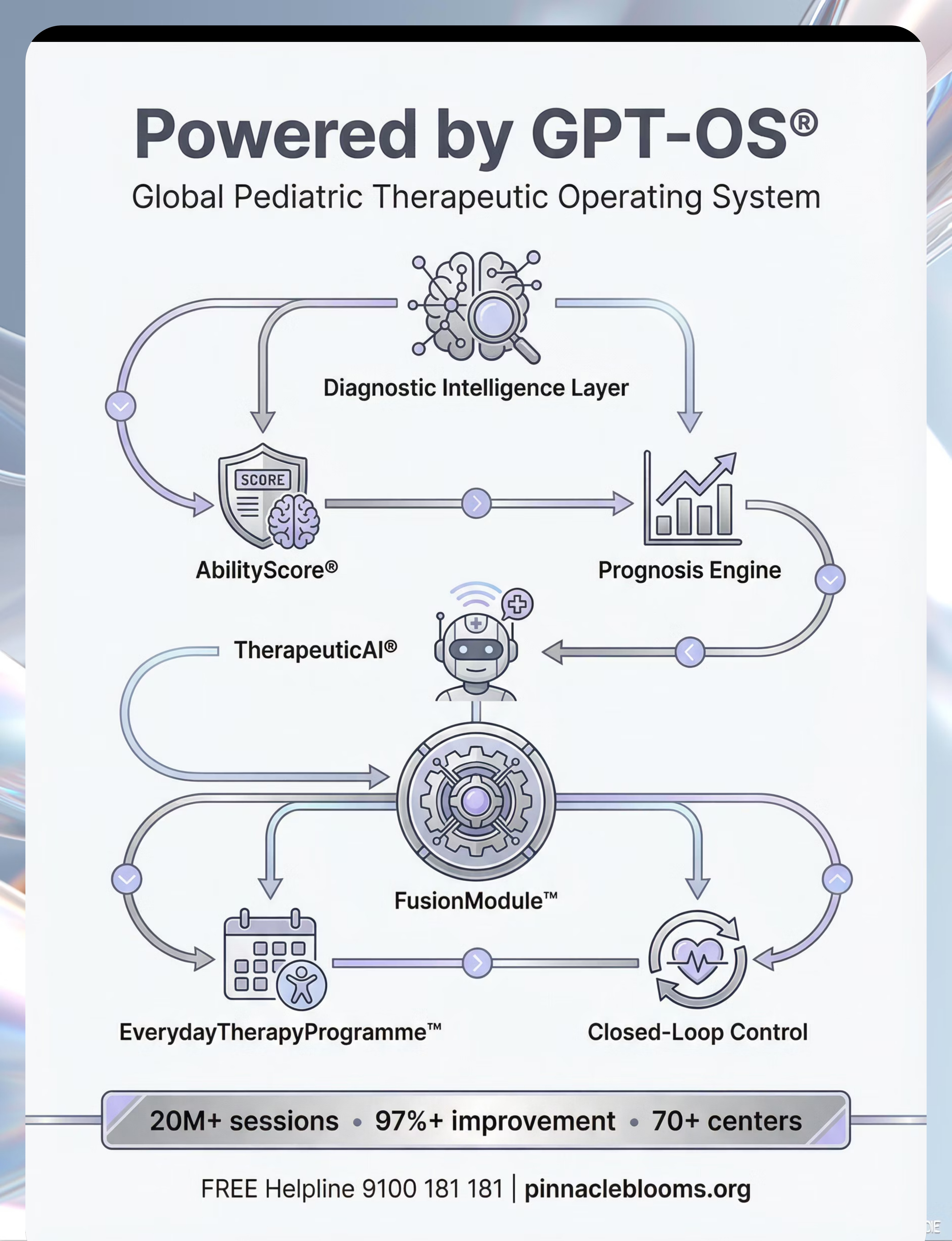
This technique crosses therapy boundaries because the brain doesn't organize by therapy type. GPT-OS® FusionModule™ coordinates all disciplines into a single converged pathway.
Research: Adapted UNICEF/WHO Nurturing Care Framework for SLPs (2022) — DOI: 10.1080/17549507.2022.2141327

What This Technique Targets — Precision, Not Guesswork
The primary target sits at the center: reducing the defensive reaction to light touch — the flinching, screaming, pulling away, and hitting. Secondary targets expand outward to include improved clothing tolerance, reduced grooming battles, and increased comfort near others. The tertiary ring encompasses the broader life impacts — enhanced social participation at birthday parties and school, improved sleep quality, greater independence in daily living, and reduced overall anxiety in sensory-rich environments.
Research: Meta-analysis (World J Clin Cases, 2024): PMC10955541

Your 9 Materials — What to Get
The following 9 materials form your complete toolkit for addressing light touch defensiveness. Some require purchase, several are entirely free techniques, and most have DIY alternatives. Start with the free strategies — they are powerful on their own.

1. Weighted Blanket / Lap Pad
Deep pressure calms the alarm system. ₹2,000–8,000. Weight: ~10% of child's body weight. Use for sleep, seated activities, calming after sensory overwhelm.
2. Therapy Brush (Wilbarger)
Systematic deep pressure to recalibrate touch. ₹300–800. ⚠️ PROFESSIONAL OT TRAINING REQUIRED. Use every 90–120 minutes per OT guidance.

3. Vibrating Massager / Tools
Predictable input prepares the system. ₹500–3,000. Types: handheld massager, vibrating pillow, vibrating hairbrush, Z-Vibe. Use before challenging touch activities.

4. Compression Clothing
Constant calm through steady pressure. ₹800–3,000/garment. Types: compression undershirt, shorts, vest, full bodysuit. Worn daily under regular clothing.

5. Deep Pressure Fidgets
Self-regulation in their hands. ₹100–800. Types: stress balls, therapy putty, squeeze fidgets, hand exercisers. Use during lines, classrooms, crowds.

6. Joint Compressions
Immediate calm through firm pressure. ₹0 — no equipment needed. Firm pressure to shoulder, elbow, wrist, hip, knee, ankle joints. Hold 3–5 seconds each.

7. Touch Warnings
Predictability reduces threat response. ₹0 — system only. Always announce touch before it happens: "I'm going to touch your shoulder now. 3-2-1."

8. Textured Play Materials
Child-led exploration builds tolerance. ₹300–2,000. Types: kinetic sand, therapy putty, water beads, fabric collection, sensory bins. Never forced.

9. Sensory Diet / Heavy Work
Regular deep input keeps the system calm. ₹0–2,000 (mostly free). Activities: carrying groceries, wall push-ups, wheelbarrow walks, climbing. 3–5 times daily.
Pinnacle Recommends
Items 1, 2, 4, and 9 carry the highest evidence base. Total Investment Range: ₹0–8,000. Start with free strategies first.

Can't Buy It? Make It. Every Family Can Start Today.
Material | Buy This | Make This (DIY at Home) | |
Weighted Blanket | ₹2,000–8,000 | Fill a pillowcase with rice or dried beans, sew closed. Layer multiple regular blankets. Use a heavy fleece blanket. | |
Therapy Brush | ₹300–800 | ⚠️ NO DIY SUBSTITUTE. Requires specific surgical brush AND professional OT training. Incorrect technique worsens defensiveness. | |
Vibrating Massager | ₹500–3,000 | Electric toothbrush (without bristles or with soft cap). Battery-operated personal massager. Vibrating toys repurposed. | |
Compression Clothing | ₹800–3,000 | Snug-fitting athletic wear. Bike shorts or tight leggings. Swimsuit worn under clothes. Layered snug undershirts. | |
Deep Pressure Fidgets | ₹100–800 | Homemade stress balls: fill balloons with flour, rice, or playdough. DIY therapy putty from online recipes. | |
Joint Compressions | ₹0 (free) | Already free! Firm pressure to joints, hold 3–5 seconds, release. Wall pushes, hand pressing, self-squeezes. | |
Touch Warnings | ₹0 (free) | Already free! Family rule: always warn before touching. "I'm going to touch your [body part] now. 3-2-1." | |
Textured Play | ₹300–2,000 | Rice, beans, pasta, sand, water. Fabric scraps from old clothes. Homemade playdough. Shaving cream play. | |
Sensory Diet | ₹0–2,000 | All free: carrying groceries, pushing shopping cart, wheelbarrow walks, wall push-ups, playground climbing, swimming. |
The WHO Nurturing Care Framework emphasizes context-specific, equity-focused interventions. Every family, regardless of economic status, can begin this intervention TODAY with household items. The science works the same whether you use a clinical-grade weighted blanket or a pillowcase filled with rice.
Research: WHO NCF (2018) | CCD Package across 54 LMICs | PMC9978394

Safety First — Before You Begin
🔴 RED — DO NOT PROCEED IF:
- Child has respiratory or cardiac conditions — weighted items require medical clearance
- Child is an infant or toddler under 2 years — weighted blankets are NOT safe for infants
- Child cannot independently remove a weighted blanket
- You have not been trained by an OT for the Wilbarger Brushing Protocol
- Child is in severe distress, illness, or post-meltdown state — wait until regulated
- Child has joint hypermobility or joint conditions — joint compressions need OT guidance first
🟡 AMBER — PROCEED WITH CAUTION:
- Weighted blanket weight should be ~10% of child's body weight — never heavier
- Wilbarger brushing: NEVER brush face, chest, or stomach. ONLY arms, legs, and back with FIRM pressure
- Vibration tools: some children are ALSO defensive to vibration — if child reacts negatively, stop immediately
- Compression clothing: firm but NOT restrictive — child must breathe and move freely
- Texture exposure must ALWAYS be child-controlled — NEVER force texture contact
🟢 GREEN — SAFE TO START:
- All free techniques (joint compressions, touch warnings, heavy work) can begin today
- Weighted blanket use during supervised awake time
- Compression clothing during daytime hours
- Child-controlled fidget use and texture exploration
- Scheduled sensory diet activities
RED LINE — STOP IF YOU SEE: Child becomes severely distressed beyond what you can manage; skin irritation, redness, or circulation concerns from compression; breathing difficulty with any weighted item; child's defensiveness WORSENS despite consistent protocol — this means reassessment is needed.
Research: Indian Journal of Pediatrics RCT (2019) — DOI: 10.1007/s12098-018-2747-4
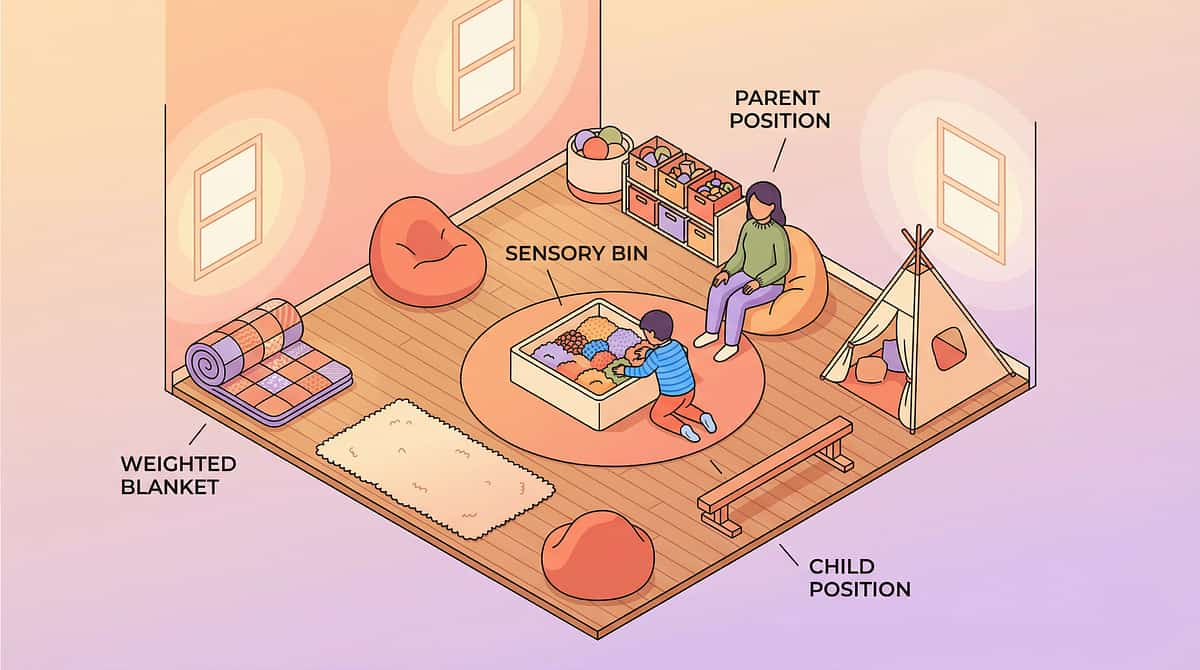
Set Up Your Space — Before the First Session
Quiet Corner
Low lighting, minimal visual clutter. This is where weighted blanket and calming activities happen.
Texture Station
A small table or tray with textured materials arranged from least to most challenging. Child sits in control position with easy escape route.
Heavy Work Zone
Open floor space near a wall for wall push-ups, wheelbarrow walks, and active sensory diet activities.
Parent Position
Beside (not across from) child. Within reach but not crowding. Able to observe face and body cues.
Materials Storage
Organized, labeled, within parent's reach but not overwhelming the child visually.
REMOVE From the Space
- Screens and electronic distractions
- Strongly scented items
- Flickering or fluorescent lighting
- Background noise (TV, music)
- Other children or pets during initial sessions
Environmental Settings
- Temperature: Comfortable — not too warm (heat increases sensitivity)
- Lighting: Warm, steady, dimmable preferred
- Sound: Quiet or soft white noise
- Surface: Carpet, yoga mat, or soft seating
- Clothing: Comfortable, tag-free clothing
Research: Sensory Integration Theory (Ayres) — Environmental setup is a core principle. Meta-analysis: PMC10955541

ACT III: THE EXECUTION
Is Your Child Ready? — 60-Second Pre-Session Check
Fed Recently
Child has eaten within the last 1–2 hours (not hungry, not just finished eating)
Well-Rested
Child has slept adequately (not overtired)
Calm State
Child is in a relatively calm/regulated state (not mid-meltdown or immediately post-meltdown)
No Illness
No illness or pain present today
Space Ready
Environment is set up per the space guide, materials are ready and within parent's reach
Parent Regulated
Parent is calm, focused, and not rushed — your state matters as much as theirs
All Checked → GO
Begin with Step 1: The Invitation
1–2 Unchecked → MODIFY
Use simplified version: heavy work + touch warnings only. Skip texture exposure.
3+ Unchecked → POSTPONE
Not today. Replace with calming sensory activity (weighted blanket, quiet heavy work). Try tomorrow.
"The best session is one that starts right. A skipped session is never wasted — it's respect for your child's state."

Step 1 — The Invitation (30–60 seconds)
What to Do: You're not starting therapy. You're starting play. The child must feel this is a choice, not a command.
"Hey [child's name], I have something cool to show you. Want to come see? You can touch it or just look — whatever you feel like."
Body Language
- Sit at child's level (floor, low chair)
- Keep body relaxed, open, turned slightly sideways
- Have the first material visible but not in the child's space
- Smile — your calm face tells their nervous system "safe"
Reading Responses
Acceptance looks like: Child approaches, looks toward material, asks a question, doesn't leave — any movement toward engagement.
Resistance: Child turns away → "That's okay. It'll be here if you want it later." Child says "no" → Respect immediately. Offer heavy work instead. Child distressed → Stop. Provide deep pressure. Revisit tomorrow.
Timing: 30–60 seconds. If no engagement within 60 seconds, pause. Never force.
Research: ABA Pairing Procedures — establishing motivating operations before demand placement | OT "Just-Right Challenge" principle

Step 2 — The Engagement (1–3 minutes)
Child has shown interest. Now introduce the first material — starting with the DEEPEST pressure option (weighted blanket, compression item, or heavy work), NOT texture exposure. Deep pressure first. Always.
"This is a special heavy blanket. Feel how heavy it is? Some kids say it feels like a hug. Want to try it on your lap? You can take it off anytime."
Show at Arm's Distance
Let child see the material from a comfortable distance without overwhelming them.
Model First
Let child see YOU touch it first. Demonstrate it's safe through your own engagement.
Offer — Let Them Reach
Offer it to the child — let THEM pick it up or pull it toward themselves. Their agency matters.
Apply Gently
If using weighted blanket: drape over lap or shoulders — never wrap over head. If using fidgets: place near child, let them reach for it.
Engagement ✓
Child reaches for, holds, or leans into material → Continue
Tolerance ○
Child accepts but is neutral → Continue gently, offer verbal praise
Avoidance ✗
Child pushes away → "That's fine. Let's try something else" → Switch to joint compressions or heavy work
"You tried it! That was brave. Your body is learning something new."
Research: Systematic review (Children, 2024) — PMC11506176

Step 3 — The Therapeutic Action (3–5 minutes)
This is the active ingredient. You are systematically providing deep pressure input to lower your child's nervous system alarm threshold. Then — and only then — introducing controlled, warned light touch at the child's pace.
1
Phase A — Deep Pressure Loading (2–3 min)
- Weighted blanket on lap/shoulders during preferred activity
- Joint compressions: shoulders → elbows → wrists → hips → knees → ankles (hold 3–5 sec)
- Squeeze fidgets, press into therapy putty
- Heavy work: wall push-ups, carrying weighted backpack, pressing palms together
2
Phase B — Warned Light Touch (1–2 min)
- Announce: "I'm going to touch your arm now. Ready? 3-2-1."
- Touch with FIRM pressure first (not light)
- Gradually reduce pressure over sessions — the desensitization gradient
- Child can say "stop" at any time. Respect immediately.
Common Execution Errors:
❌ Starting with light touch before deep pressure loading → triggers alarm
❌ Skipping the verbal warning → unexpected touch = threat
❌ Applying Wilbarger brush with light strokes → MUST be firm. Light brushing worsens defensiveness.
❌ Pushing through child's "stop" signal → destroys trust, increases defensiveness
❌ Starting with light touch before deep pressure loading → triggers alarm
❌ Skipping the verbal warning → unexpected touch = threat
❌ Applying Wilbarger brush with light strokes → MUST be firm. Light brushing worsens defensiveness.
❌ Pushing through child's "stop" signal → destroys trust, increases defensiveness
Research: Meta-analysis (World J Clin Cases, 2024) — 40-minute therapy sessions showed maximum effectiveness. Home sessions: 10–20 minutes. PMC10955541
Step 4 — Repeat & Vary (3–5 minutes)
Target Repetitions: 3–5 cycles of the Phase A → Phase B sequence per session. Quality over quantity.
Vary Body Parts
Different body parts for joint compressions — arms one round, legs next
Vary Tools
Different fidget tools each round — stress ball, then putty, then squeeze toy
Vary Textures
Different textures for controlled exposure — fabric first, then kinetic sand, then dry rice
Add Playfulness
"Let's see how hard you can push the wall! Can you carry this bag like a superhero?"
Satiation Indicators — When to Stop
- Child's engagement drops noticeably
- Child starts looking away, fidgeting in non-regulatory ways
- Child becomes silly or hyperactive (overstimulation)
- Child explicitly says "done" or "no more"
- Child has been engaged for more than 15–20 minutes total
"3 good repetitions where the child is regulated and engaged are worth more than 10 forced repetitions where they're just enduring. End on success."

Step 5 — Reinforce & Celebrate
Reinforcement — Timing Matters More Than Magnitude: Within 3 seconds of the desired behavior (tolerating touch, engaging with a material, trying something new), deliver reinforcement.
"You let the blanket sit on your lap! Your body handled that really well."
"You squeezed that putty so hard — your hands are getting stronger!"
"I said I'd touch your arm, and you were ready. That was amazing control."
"You told me 'stop' and I stopped. You're the boss of your body."
Reinforcement Menu
- Verbal praise — specific, not generic ("You touched the sand!" not just "Good job")
- Preferred activity time — 5 minutes of a favorite game
- Sticker/token toward a reward chart
- Natural consequence — "Because you wore your compression shirt today, we got through the whole store without a meltdown. That means we had time for the playground."
"Celebrate the attempt, not just the success. A child who tried and stopped is braver than a child who was never asked."
Research: ABA Reinforcement Principles — Immediate, specific reinforcement increases behavior occurrence.

Step 6 — The Cool-Down (2–3 minutes)
Transition Warning
"Two more squeezes of the putty, then we're all done for today."
"One more wall push, and then we can [preferred activity]."
Cool-Down Activity (1–2 min)
- Weighted blanket draped over shoulders while sitting quietly
- Slow, firm joint compressions (calming, not activating)
- Child's preferred calm activity: book, weighted stuffed animal
- Deep breathing if child can do it: "Smell the flower (inhale), blow out the candle (exhale)"
Material Put-Away Ritual
Let the child help put materials away if able. This creates a predictable ending routine. "Blanket goes here. Putty goes in the jar. All done."
Transition Cue
"Great session! Now it's time for [next activity]. Your body did great work today."
If Child Resists Ending
- Offer one more repetition only: "One more, then all done."
- Use a visual timer if helpful
- Never end abruptly — always give 30-second warning
Research: Visual supports classified as evidence-based practice for autism (NCAEP, 2020)

Capture the Data — Right Now (60 Seconds)
Within 60 seconds of session end, record these three data points. This is the foundation of your child's progress story.
Data Point 1: Duration
How many minutes did your child actively participate? _____ minutes
Data Point 2: Tolerance Rating (1–5)
1 = No touch/material tolerated
2 = Deep pressure only
3 = Deep pressure + partial warned light touch
4 = Most touch with preparation
5 = Tolerated some unexpected touch
2 = Deep pressure only
3 = Deep pressure + partial warned light touch
4 = Most touch with preparation
5 = Tolerated some unexpected touch
Data Point 3: Notes
One sentence — what worked? What didn't? Example: "Tolerated weighted blanket 8 min. Accepted arm touch after joint compressions. Refused texture tray today."
Tracking Tools:
- 📋 Downloadable PDF tracking sheet — pinnacleblooms.org/trackers/A-024
- 📱 GPT-OS® in-app tracker — app.pinnacleblooms.org/track
"60 seconds of data now saves hours of guessing later. Your child's progress lives in these numbers."
Research: ABA Data Collection Standards — Cooper, Heron & Heward (Applied Behavior Analysis)

What If It Didn't Go As Planned?
Child Refused to Engage at All
Why: The nervous system wasn't ready. Arousal may have been too high or too low.
Next time: Do 10 minutes of heavy work BEFORE the invitation. Carry groceries. Do wall push-ups. Then try again.
Next time: Do 10 minutes of heavy work BEFORE the invitation. Carry groceries. Do wall push-ups. Then try again.
Tolerated Deep Pressure But Melted Down at Light Touch
Why: The deep pressure loading wasn't enough to lower the alarm threshold. Normal in early sessions.
Next time: Extend Phase A to 5 minutes. Reduce Phase B to a single warned firm touch. Build up gradually.
Next time: Extend Phase A to 5 minutes. Reduce Phase B to a single warned firm touch. Build up gradually.
Wilbarger Brush Made Things Worse
Why: Pressure was too light (activating protective pathway) or technique was incorrect.
Next time:⚠️ DO NOT continue without OT re-training. Light brushing increases defensiveness.
Next time:⚠️ DO NOT continue without OT re-training. Light brushing increases defensiveness.
Child Hit Me When I Touched Them
Why: The nervous system interpreted your touch as an attack. Neurological, not behavioral defiance.
Next time: Always warn 5 seconds before. Start with only joint compressions. Use "3-2-1" countdown. Let THEM initiate touch.
Next time: Always warn 5 seconds before. Start with only joint compressions. Use "3-2-1" countdown. Let THEM initiate touch.
Worked for Days, Then Regressed
Why: Nervous system recalibration is not linear. Illness, poor sleep, stress affect sensory thresholds.
Next time: Expect waves. Regression doesn't erase progress. Return to the working level and rebuild.
Next time: Expect waves. Regression doesn't erase progress. Return to the working level and rebuild.
Child Enjoyed It But I'm Unsure I Did It Right
Why: Engagement is a positive sign. Precise technique can be refined over time.
Next time: Film yourself (for your own review) and share with your OT. Enjoyment + engagement = the right foundation.
Next time: Film yourself (for your own review) and share with your OT. Enjoyment + engagement = the right foundation.
"Session abandonment is not failure — it's data. Every 'failed' session tells you what to adjust next time."

Adapt & Personalize — No Two Children Are Identical
EASIER (Bad Days / Early Sessions)
Use only deep pressure materials (weighted blanket + joint compressions). Skip light touch exposure. Reduce to 5 minutes. Let child direct everything. Focus on heavy work only.
STANDARD (Regular Sessions)
Full Phase A → Phase B protocol. 3–5 repetitions. 10–15 minute sessions. Parent-guided with child choice within structure.
HARDER (Breakthrough Days)
Introduce new textures. Reduce warning time (5→3→1 seconds). Add light touch in new contexts. Extend to 20 minutes. Generalize to school/community.
Sensory Profile Variations
Sensory Avoider: Start slower. More deep pressure. Longer Phase A. Child-controlled everything.
Mixed Profile (seeks deep, avoids light): Leverage the deep pressure seeking — use it as the on-ramp to light touch tolerance.
Age Modifications
Ages 2–4: Play-based, shorter (5–8 min), heavily parent-supported, no verbal scripts required
Ages 5–8: Can begin understanding the "why" — explain the alarm system in simple terms
Ages 9–12: Can participate in designing their own sensory diet, self-monitoring, peer advocacy

ACT IV: THE PROGRESS ARC
Week 1–2: What to Expect
15%
Progress
You've started. That's the hardest part.
What You May See ✓
- Child begins to tolerate weighted blanket for 3–5 minutes (previously would push it off)
- Reduced intensity (not elimination) of reaction to warned touch
- Child starts recognizing the "3-2-1" countdown as a safety signal
- Joint compressions become accepted, possibly sought
- Heavy work activities become a preferred part of routine
What You Won't See Yet ○
- Tolerance of unexpected light touch (this takes months)
- Elimination of clothing sensitivity
- Comfort in crowded environments
- Acceptance of touch from non-family members
"If your child tolerates the weighted blanket for 3 seconds longer than last week — that's real, measurable neurological progress. The brain is rewiring. You can't see it, but the data shows it."
Research: Systematic review (Children, 2024) — PMC11506176

Week 3–4: Consolidation Signs
40%
Progress
Neural pathways are forming.
Consolidation Indicators
- Child begins to anticipate and prepare for touch sessions (may even request them)
- Weighted blanket becomes a go-to calming tool (child reaches for it independently)
- Touch warnings are reducing the defensive response reliably
- Heavy work activities are noticeably calming (you see the difference)
- Grooming tasks (hair brushing, face washing) require fewer battles
- Child may spontaneously touch new textures during play
What the Child May Start Doing Spontaneously
Seeking Compression
Asking for tight hugs, wrapping in blankets — self-initiating the calming input they need.
Self-Regulating With Fidgets
Using fidgets without being prompted — internalizing the strategies you've taught.
Verbalizing Sensory Needs
"That's too light" or "Press harder" — your child is becoming their own sensory translator.
"You may notice you're more confident too. You're reading your child's cues faster. You're adjusting in real time. You're becoming your child's sensory translator."

Week 5–8: Mastery Indicators
75%
Progress
The alarm system is recalibrating.
Mastery Criteria (Observable, Measurable)
- Child tolerates warned light touch from family members without distress
- Clothing tolerance has expanded (previously refused fabrics now tolerated)
- Grooming tasks completed with minimal resistance
- Child can sit beside others without hypervigilance
- Child uses self-regulation strategies independently (self-compression, fidgets, requesting deep pressure)
- Tolerance rating consistently at 3–4 on the 1–5 scale
Generalization Indicators
Outside the Home
Skills appearing at school, grandparents' house, and market
Non-Primary Caregivers
Accepting touch from teachers, therapists, and relatives
Sensory-Rich Environments
Reduced meltdowns at birthday parties and crowded spaces
Maintenance Check: Does tolerance persist when you skip a structured session? If yes — neural pathways are established. If tolerance drops — continue the protocol; more time needed.
🏆 Mastery Unlocked Badge Criteria: Tolerance rating of 4+ for 3 consecutive weeks + generalization to at least 2 settings outside home + independent self-regulation observed.

Celebrate This Win
"You did this."
Remember the screaming when you barely touched her arm? The cut tags in every shirt? Leaving birthday parties early? The looks from other parents?
Look at where you are now.
Your child's nervous system has learned — through your patience, your consistency, your refusal to accept "she's just being dramatic" — that light touch is not an attack. Not because you forced exposure. Because you understood the neurology, respected the pace, and gave their brain what it needed to rewire.
Reduced Tactile Defensiveness
Across home, school, and social settings
Expanded Clothing Tolerance
More fabrics, fewer morning battles
Improved Grooming Independence
Hair, face, nails — with strategies, not tears
Enhanced Social Participation
Parties, playground, peers — a broader world
Self-Regulation Strategies In Place
Your child owns their toolkit for life
Celebrate: Document this milestone. Take a photo of your child doing something that was impossible 8 weeks ago. Write the date. This is evidence of what a parent can do with the right knowledge and the right tools.

Red Flags — When to Pause and Seek Professional Guidance
🚩 Defensiveness is WORSENING
Despite 4+ weeks of consistent intervention — the sensory profile may be more complex than tactile over-responsivity alone. Professional sensory evaluation needed.
🚩 New Avoidance Behaviors
Child is avoiding rooms, people, or activities they previously tolerated. Generalized anxiety may be compounding the sensory issue. Multi-disciplinary assessment recommended.
🚩 Self-Injurious Behavior
Biting self, hitting head, scratching → STOP all light touch exposure. Increase deep pressure only. Seek immediate professional guidance.
🚩 Reactions Intensifying
Not just not improving, but actively intensifying. The protocol may need significant modification. OT reassessment required.
🚩 Parent Overwhelm
Your wellbeing matters. Take a pause. Maintain only the easy strategies (heavy work, weighted blanket) and seek professional support for structured sessions.
Escalation Pathway: Self-resolve (adjust protocol) → Teleconsultation with Pinnacle OT → In-clinic assessment → Comprehensive sensory evaluation
"Trust your instincts — if something feels wrong, pause and ask. Pausing is not quitting. It's recalibrating."
📞FREE National Autism Helpline: 9100 181 181 (16+ languages, 24×7)
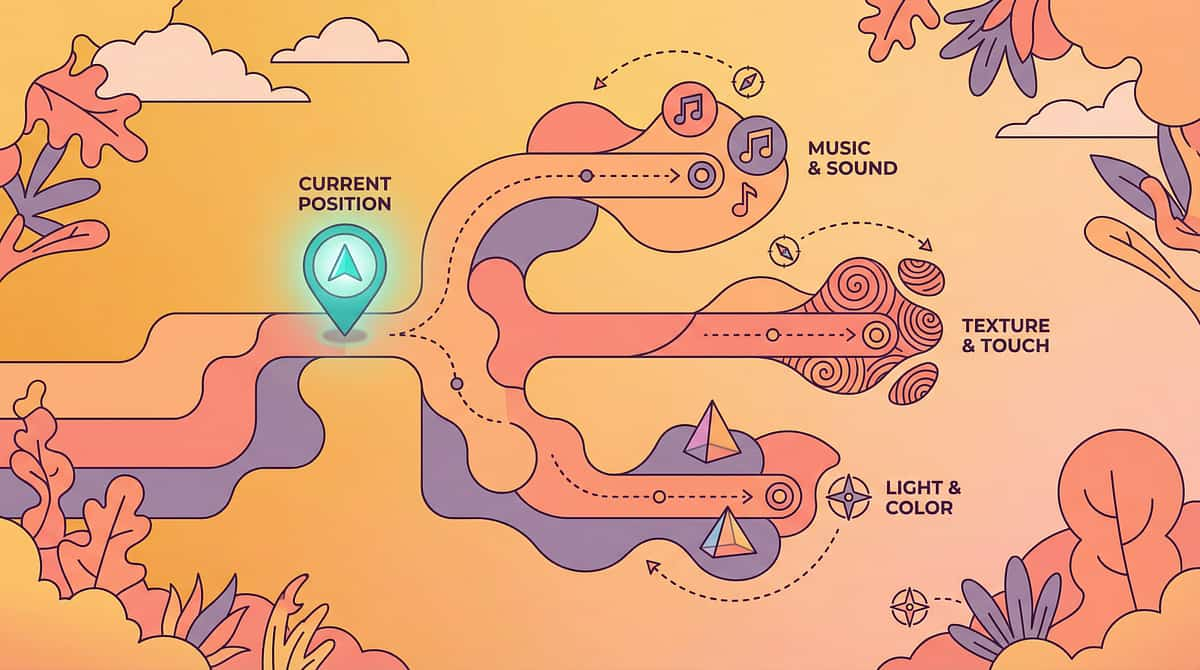
The Progression Pathway — Where You've Been, Where You're Going
Long-Term Developmental Goal: Regulated response to varied touch in varied environments → Independent sensory self-management → Full social participation.
Related Techniques in Sensory Processing — Tactile Domain
Technique | Difficulty | Canon Materials | Already Own? (from A-024) | |
A-023: One-Outfit Rigidity | Core | Compression Clothing, Texture Play | ✅ Yes | |
A-025: Messy Play Avoidance | Core | Texture Play, Sensory Diet | ✅ Yes | |
A-026: Hair Brushing Battles | Core | Vibration Tools, Touch Warnings | ✅ Yes | |
A-030: Hug Avoidance | Intro | Weighted Blanket, Compression, Joint Compressions | ✅ Yes | |
A-035: Grooming Resistance | Advanced | Full Material Set | ✅ Yes | |
A-009: Sand Play Avoidance | Intro | Texture Play, Sensory Bins | ✅ Yes |
You already own materials for every technique in this list. The investment you made for light touch defensiveness equips you for the entire tactile processing domain.
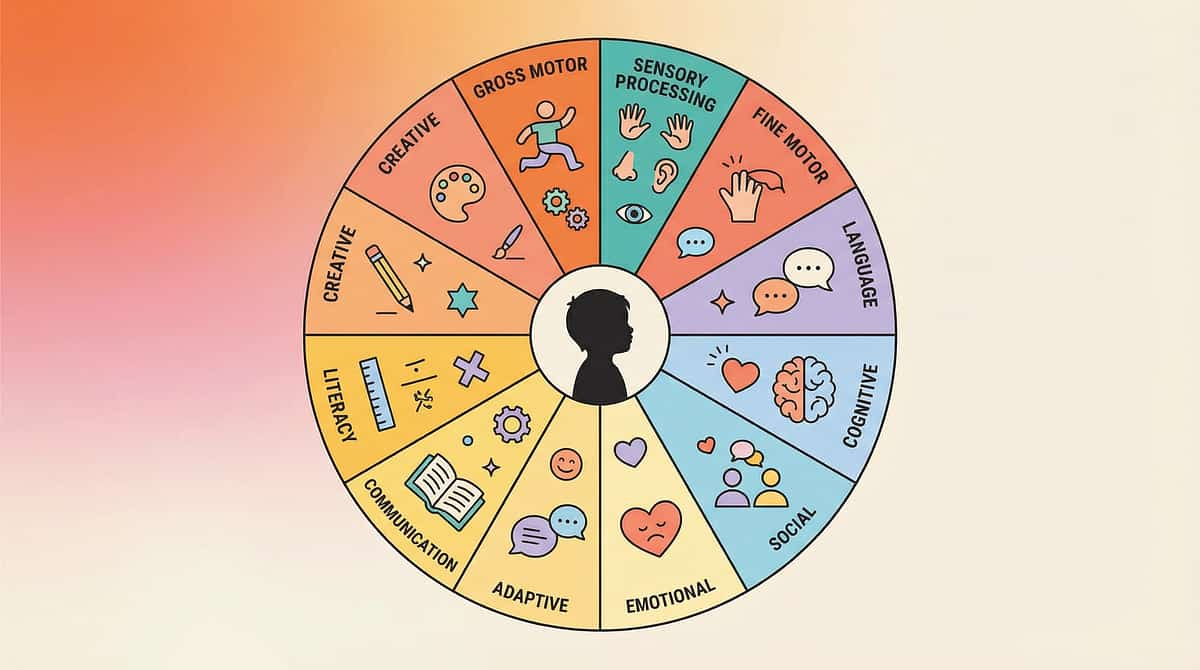
Your Child's Full Developmental Map
A. Sensory Processing ← YOU ARE HERE
B. Motor Development
C. Communication & Language
D. Social Interaction
E. Emotional Regulation
F. Cognitive Development
G. Daily Living Skills
H. Behavioral Regulation
I. Play & Imagination
J. Academic Readiness
K. Parent & Caregiver Knowledge
L. Community & Inclusion
"This technique — deep pressure desensitization for light touch defensiveness — is one piece of your child's developmental map. Sensory regulation feeds into emotional regulation, which feeds into social participation, which feeds into community inclusion. Every domain connects. GPT-OS® maps all of them."
🔗 See your child's full developmental profile → GPT-OS® AbilityScore® Assessment
📞 Request assessment: 9100 181 181
📞 Request assessment: 9100 181 181

ACT V: THE COMMUNITY & ECOSYSTEM
Families Who've Been Here
"A year ago, Meera couldn't stand in line without melting down if someone touched her. Getting dressed took 45 minutes every morning — only two outfits were tolerable. We started with a weighted blanket and touch warnings. The joint compressions became her anchor. By month three, she was wearing her school uniform without meltdowns. Now she handles the school bus, crowded hallways, even accidental bumps. It took time, but she got there."
— Parent, Pinnacle Network (Outcome illustrative; timelines vary by child)
"Aarav's OT trained us on the Wilbarger Protocol. At first I was skeptical — a brush? But the firm pressure made sense once I understood the neurology. Within six weeks, hair washing went from a screaming battle to a 'please warn me first and I'll be okay' situation. He still prefers firm touch. But light touch doesn't send him into panic anymore."
— Parent, Pinnacle Network
"Light touch defensiveness is one of the most rewarding challenges to address because the deep pressure counter-strategy is so immediately calming. Parents often see regulation improvements within 2–3 weeks of consistent sensory diet implementation. The recalibration of light touch tolerance follows over months."— Senior Occupational Therapist, Pinnacle Blooms Network

Connect With Other Parents Navigating Tactile Defensiveness
Pinnacle Sensory Processing Parent Community
WhatsApp Group — Connect with families working on the same challenges. Share strategies, ask questions, celebrate wins. Join → pinnacleblooms.org/community/sensory
Local Pinnacle Parent Meetups
Find other families near your Pinnacle center for in-person support and shared learning. Find your center → pinnacleblooms.org/centers
Peer Mentoring
Connect with an experienced parent who has navigated light touch defensiveness successfully. They've been where you are. Request a peer mentor → pinnacleblooms.org/mentoring
"Your experience helps others. The data you collect, the strategies you adapt, the milestones you document — they inform the system that helps every child like yours. Consider sharing your journey."
Your Professional Support Team
Services for Light Touch Defensiveness
- Occupational Therapy — Sensory Integration (PRIMARY)
- Comprehensive Sensory Processing Evaluation
- Wilbarger Protocol Training for Parents
- Individualized Sensory Diet Development
- Parent Training & Home Programme Design
- EverydayTherapyProgramme™ Implementation
Connect Now
📍Find Your Nearest Pinnacle Center
70+ centers across India → pinnacleblooms.org/centers
70+ centers across India → pinnacleblooms.org/centers
📱Can't Visit In Person?
Teleconsultation with a Pinnacle OT specializing in sensory integration → pinnacleblooms.org/teleconsult
Teleconsultation with a Pinnacle OT specializing in sensory integration → pinnacleblooms.org/teleconsult
📞FREE National Autism Helpline
9100 181 181 (16+ languages, 24×7)
9100 181 181 (16+ languages, 24×7)
🌐 pinnacleblooms.org
"Home + clinic = maximum impact. The strategies on this page extend what your therapist does in the clinic. The therapist refines what you do at home. Together, it's a closed loop."
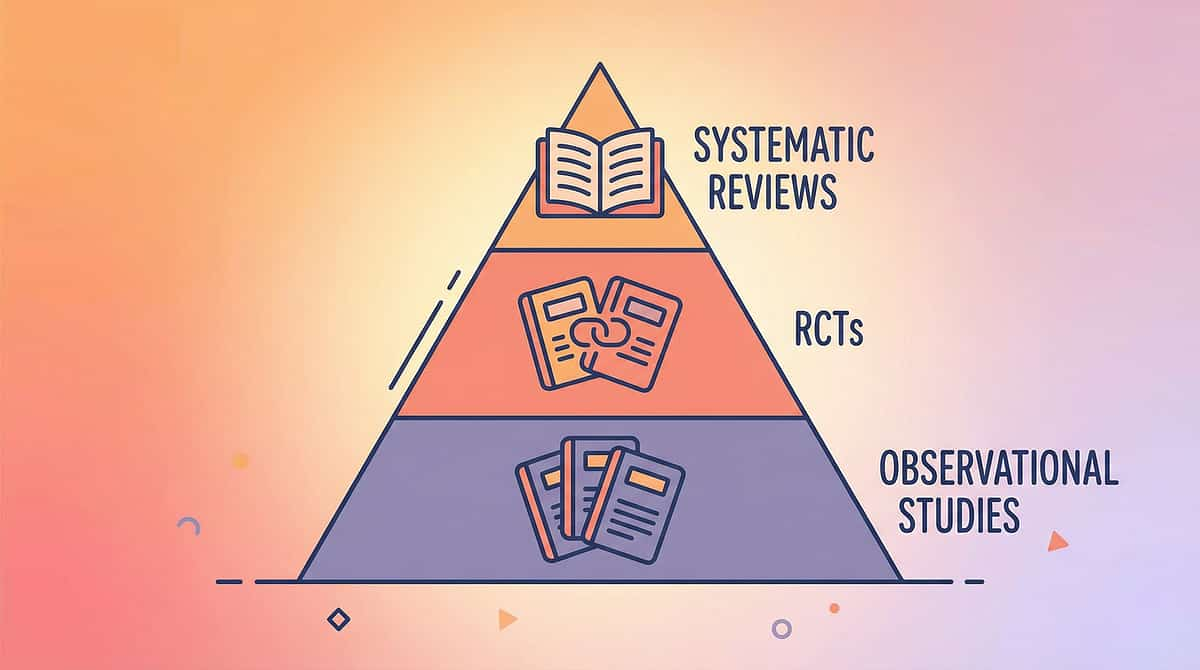
The Research Library — Go Deeper
Level I
Systematic Reviews & Meta-Analyses
Level II
Randomized Controlled Trials
Level III
Cohort Studies
Level IV
Case Studies & Expert Opinion
📄 Systematic Review (2024) — Level I
PRISMA model review of 16 articles (2013–2023) confirming sensory integration as evidence-based practice for ASD. → PubMed: PMC11506176
📄 Meta-Analysis (2024) — Level I
24 studies confirming SI therapy promotes social skills, adaptive behavior, sensory processing, motor skills. 1:1 sessions, 2–3×/week for 8–12 weeks = maximum effect. → PMC10955541 | DOI: 10.12998/wjcc.v12.i7.1260
📄 Indian RCT (2019) — Level II
Home-based sensory intervention efficacy in Indian pediatric population. Padmanabha et al. → DOI: 10.1007/s12098-018-2747-4 (Indian Journal of Pediatrics)
📄 Neurological Framework (2020) — Level III
Comprehensive framework for evaluating SI treatment neural mechanisms in ASD. → DOI: 10.3389/fnint.2020.556660
📄 WHO/UNICEF Frameworks
WHO Nurturing Care Framework (2018) | WHO CCD Package (2023) | UNICEF MICS Indicators → nurturing-care.org/ncf-for-ecd | PMC9978394
📄 NCAEP (2020)
National Clearinghouse on Autism Evidence and Practice: Sensory integration classified as evidence-based practice.
How GPT-OS® Uses Your Data
GPT-OS® learns from your session data to build a personalized intelligence layer for your child.
Tactile Tolerance Profile
Which materials work best, which don't — mapped specifically for your child
Rate of Progress
How quickly the nervous system is recalibrating — calibrated to your child's pace
Optimal Session Design
Best duration, frequency, and material sequence for your child's profile
Environmental Factors
Time of day, sleep, illness — factors affecting sensory thresholds
🔒 Your child's data is encrypted, anonymized for population-level research, and never shared without consent.
🔒 Pinnacle Blooms Network® operates under ISO/IEC 27001 Information Security standards.
🔒 Data is governed under Indian data protection regulations.
🔒 Pinnacle Blooms Network® operates under ISO/IEC 27001 Information Security standards.
🔒 Data is governed under Indian data protection regulations.
"Your data helps every child like yours. When you track a session, your child's response pattern joins 20M+ data points that improve recommendations for every family on the platform."

Watch the Reel — A-024: 9 Materials That Help With Light Touch Defensiveness
Reel A-024
Sensory Processing — Tactile Processing
~75 Seconds
Sensory Solutions Series — Episode 24
What You'll See: A Pinnacle therapist demonstrates each of the 9 materials in action — the weighted blanket calming a child, the Wilbarger brush technique (correct firm pressure), vibration tools preparing the system, compression clothing in daily use, fidgets providing self-regulation, joint compressions for immediate calm, touch warnings creating predictability, texture play building tolerance, and heavy work keeping the baseline regulated.
"Video content reinforces everything on this page through a different learning modality. Watch the demonstrations, then come back here for the full protocol."
▶ Watch on Pinnacle Blooms Instagram / YouTube

Share This With Your Family — Consistency Across Caregivers Multiplies Impact
🔗 Copy Link: techniques.pinnacleblooms.org/sensory-processing/light-touch-defensiveness
Downloadable Resources
📋 Family Guide (1-Page PDF)
Simplified version for grandparents and extended family. What light touch defensiveness is, what to do, what NOT to do.
📋 Teacher Communication Template
A ready-to-send letter explaining your child's tactile needs, the touch warning system, and how the school can help.
📋 Caregiver Quick Card
Laminate and post on the fridge. 5 essential rules: 1) Always warn before touching. 2) Use firm pressure, not light. 3) Never force exposure. 4) Respect "stop." 5) Heavy work before challenging situations.
"If only one person in your child's life uses these strategies, progress is limited. When EVERYONE uses them consistently — parents, grandparents, teachers, babysitters, extended family — the nervous system gets a unified message: touch is predictable, touch is safe."
Research: WHO CCD Package — Multi-caregiver training is critical for generalization and maintenance. PMC9978394

ACT VI: THE CLOSE & LOOP
Frequently Asked Questions
Is light touch defensiveness the same as being "sensitive"?
It's more specific than general sensitivity. Light touch defensiveness is a neurological processing pattern where the protective tactile pathway is overactive. It's measurable, documented in peer-reviewed research, and responsive to structured intervention. This is not personality — it's neurology.
Will my child "grow out of it"?
Some children show natural improvement with neural maturation. However, research indicates that structured intervention significantly accelerates progress and prevents secondary complications (social avoidance, anxiety, reduced participation). Waiting without intervening risks missed developmental windows.
How long until I see results?
Expect tolerance improvements within 2–4 weeks. Meaningful functional changes (grooming, clothing, social touch) typically emerge over 6–12 weeks. Full recalibration may take 3–6 months of consistent intervention. Every child's timeline is unique.
Can I do the Wilbarger Brushing Protocol without an OT?
No. This protocol requires professional training for correct technique, pressure, frequency, and areas to brush. Incorrect technique — particularly light brushing — can worsen defensiveness. Seek OT training before attempting.
My child seeks deep pressure but avoids light touch. Contradictory?
Not at all. It's the most characteristic feature of light touch defensiveness. Deep pressure activates calming pathways. Light touch activates alarm pathways. They are processed through entirely different neural circuits. Your child is self-regulating by seeking what calms them.
Will this affect my child's ability to have relationships?
Untreated tactile defensiveness can limit social touch, impacting peer relationships and family bonding. With intervention, children learn to manage sensory input, communicate needs, and engage in meaningful physical interaction on their terms. The goal is not to eliminate sensitivity — it's to give them strategies to navigate it.
Is this only for children with autism?
No. Light touch defensiveness occurs in children with SPD, developmental delays, premature birth, ADHD, anxiety disorders, and in some typically developing children. The intervention approach is the same regardless of diagnosis.
How do I explain this to my child's school?
Use the Teacher Communication Template from the Share section. Key points: this is neurological, not behavioral; the child needs a touch warning system; firm touch is tolerated better than light touch; heavy work before transitions helps; never force touch-based activities.
Didn't find your answer? 🤖 Ask GPT-OS® → app.pinnacleblooms.org/ask | 📞 Teleconsultation → pinnacleblooms.org/teleconsult

Your Next Step — Start Now
You've read the science. You've seen the evidence. You have the materials list, the DIY alternatives, the step-by-step protocol, the progress milestones, and the troubleshooting guide. Your child's nervous system is waiting for you to begin.
🟢 Start This Technique Today
Launch GPT-OS® guided session for A-024 → app.pinnacleblooms.org/technique/A-024/start
🔵 Book a Professional Consultation
Connect with a Pinnacle OT specializing in sensory integration → pinnacleblooms.org/book | 📞 9100 181 181
⚪ Explore the Next Technique
Browse related techniques in the tactile processing domain → techniques.pinnacleblooms.org/sensory-processing/
Validated by the Pinnacle Blooms Consortium
OT • SLP • ABA • SpEd • NeuroDev • CRO
Preview of 9 materials that help with light touch defensiveness Therapy Material
Below is a visual preview of 9 materials that help with light touch defensiveness therapy material. The pages shown help educators, therapists, and caregivers understand the structure and content of the resource before use. Materials should be used under appropriate professional guidance.
















Share this resource
Help others discover thisLink copied!

The Pinnacle Promise
Pinnacle Blooms Network®
Built by Mothers. Engineered as a System.
OT • SLP • ABA • SpEd • NeuroDev • CRO • Gamma.app Design • Parent Voice
"From fear to mastery. One technique at a time."
A parent arrived on this page scared, exhausted, and wondering if their child would ever tolerate a gentle touch. They leave with a 9-material protocol, evidence-based confidence, a progress roadmap, a professional support team, and a community of families who understand.
That is the Pinnacle promise. That is what 70,000+ technique pages deliver. That is GPT-OS® at work.
Medical Disclaimer: This content is educational. It does not replace assessment by a licensed occupational therapist or sensory integration specialist. Tactile defensiveness requires individualized evaluation to determine underlying factors and appropriate intervention strategies. Individual results may vary. Statistics represent aggregate outcomes across Pinnacle Blooms Network. Sensory integration timelines vary significantly between children.
Navigation:
🔄 Return to Top → Card 01
➡️ Next Recommended Technique → A-025: 9 Materials for Messy Play Avoidance
🔍 Browse All Techniques → techniques.pinnacleblooms.org
🔄 Return to Top → Card 01
➡️ Next Recommended Technique → A-025: 9 Materials for Messy Play Avoidance
🔍 Browse All Techniques → techniques.pinnacleblooms.org
© 2025 Pinnacle Blooms Network®, unit of Bharath Healthcare Laboratories Pvt. Ltd. All rights reserved.
CIN: U74999TG2016PTC113063 | DPIIT: DIPP8651 (Govt. of India)
GPT-OS®, AbilityScore®, TherapeuticAI®, FusionModule™, EverydayTherapyProgramme™ are registered trademarks.
CIN: U74999TG2016PTC113063 | DPIIT: DIPP8651 (Govt. of India)
GPT-OS®, AbilityScore®, TherapeuticAI®, FusionModule™, EverydayTherapyProgramme™ are registered trademarks.
Powered by GPT-OS® | 20M+ sessions | 97%+ measured improvement | 70+ centers | techniques.pinnacleblooms.org
