
Every Morning, You Stand at the Bathroom Door and Wonder If Today Will Finally Be the Day
After the bathroom. After meals. Before eating. After the park. The reminders are endless — and the resistance is exhausting. Your child isn't being difficult. Their nervous system is telling you something important.
E-538 | Self-Care Independence Series
9 Materials That Help With Hand Washing
"You are not failing. Your child's sensory system is navigating a genuinely complex task."
Pinnacle Blooms Network® | OT • SLP • ABA • SpEd • NeuroDev | Consortium-Validated
Self-Care
Hygiene
Sensory Processing
Occupational Therapy
Hand Washing Independence

You Are Not Alone in This
Millions of families worldwide navigate the same daily battle at the bathroom sink. The challenge is real. The prevalence is documented. And the solutions are proven.
80%
Sensory Impact
Of children with autism experience sensory processing difficulties that affect hygiene routines
1 in 36
ASD Prevalence
Children in India are diagnosed with autism spectrum disorder — one of the most common developmental challenges families face
21M+
Sessions Delivered
Therapy sessions by Pinnacle Blooms Network® — including direct OT support for self-care independence
Hand washing resistance isn't stubbornness. A 2024 PRISMA systematic review of 16 studies confirms that sensory processing differences are neurological — not behavioral — in origin. Your child resisting water, soap texture, or the multi-step sequence of hand washing is their nervous system responding exactly as it's wired to respond.
📊 Among families enrolled in Pinnacle's GPT-OS® program, hand washing independence is among the top 5 most-requested self-care outcomes from parents of children ages 3–10.
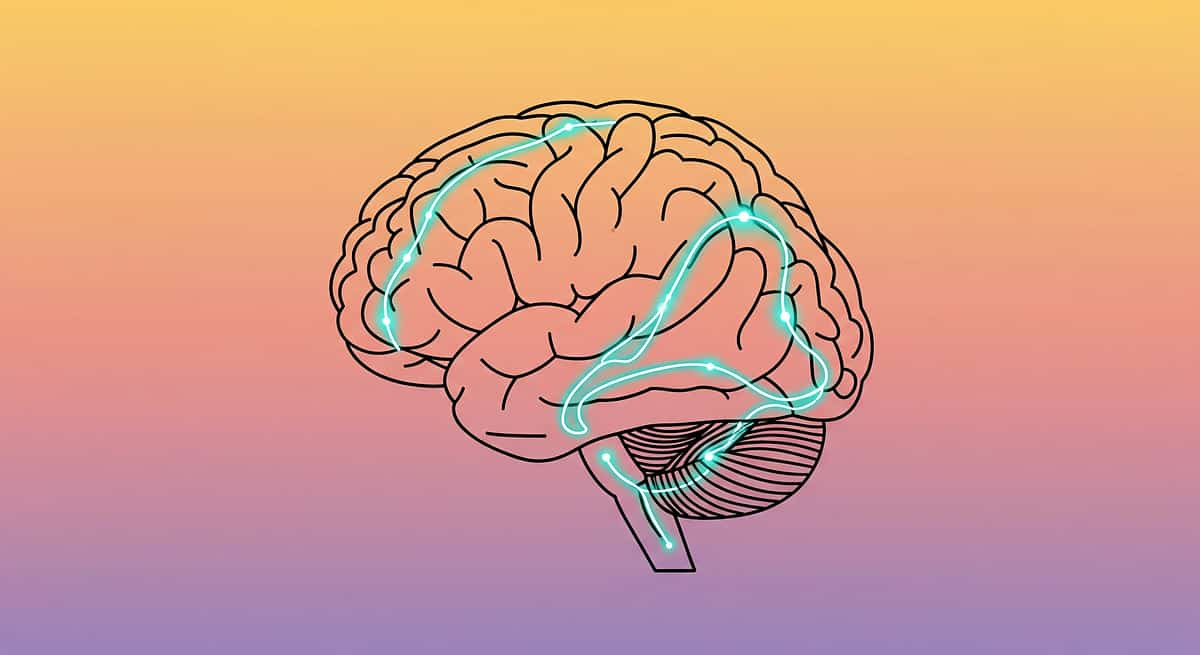
Why Hand Washing Is Genuinely Hard for Your Child
What's Actually Happening
When water touches your child's hands, sensory signals travel to the somatosensory cortex — the brain's "body map." In children with sensory processing differences, this cortex over-amplifies signals. What feels like normal water temperature to you registers as intense or overwhelming to them.
The Limbic System's Role
The limbic system (emotional memory center) adds a threat response. If previous hand washing experiences were uncomfortable, the brain learns: "sink = distress." This creates anticipatory anxiety before the faucet is even turned on.
The Cerebellum's Challenge
Hand washing requires coordinating 11+ sequential motor steps — from turning the faucet to bilateral hand rubbing to towel drying. The cerebellum must orchestrate all of this simultaneously. For children with motor planning differences (dyspraxia), this sequencing challenge is significant.
"This is a wiring difference, not a behavior choice. The materials in this guide work because they address the actual neurological barriers — not the symptoms." — Pinnacle Blooms Consortium, OT Division
Your Child's Developmental Journey — Where Hand Washing Fits
Age 2
First water tolerance training attempts
Age 3
Helps with washing with prompts + visual aids
Age 4–5
Independent sequence attempts
Age 6+
Remembers to initiate across settings
Hand washing independence typically develops between ages 2–6, with full independence — including remembering when to wash — by school age. This timeline varies significantly for children with sensory processing differences, autism, ADHD, or developmental delays.
Conditions That Commonly Co-Occur
SPD
Tactile defensiveness
ASD
Executive function + sensory
ADHD
Sequencing & initiation
DCD
Motor planning challenges
ID
Multi-step task learning
The Hygiene Independence Readiness Index (within GPT-OS®) tracks movement through 5 readiness stages: from Cannot/will not participate → Tolerates with support → Completes with visual sequence → Minimal prompting needed → Independent initiation. Most families see meaningful movement within 8 weeks.

Clinically Validated. Home-Applicable. Parent-Proven.
⬡ LEVEL I EVIDENCE — PRISMA Systematic Review | 16 Studies | 2013–2023
📊 Systematic Review (2024)
PRISMA analysis of 16 studies confirms sensory integration intervention meets criteria to be classified as evidence-based practice for children with ASD. Social skills, adaptive behavior, sensory processing, and motor skills all showed measurable improvement.
Source: PMC11506176
📊 Meta-Analysis (2024)
24 studies across children with ASD confirm sensory integration therapy effectively promotes social skills, adaptive behavior, and motor development. 40-minute sessions showed maximum effectiveness — home sessions of 10–20 minutes produce meaningful gains.
Source: PMC10955541 | World J Clin Cases
📊 Indian RCT (2019)
Home-based sensory interventions with parent-administered protocols demonstrated significant outcomes in Indian pediatric populations, validating the home-execution model used in this guide.
Source: Padmanabha et al., Indian J Pediatr, 2019
"These materials are not suggestions. They are evidence-based environmental modifications with documented neurological mechanisms. The Pinnacle Blooms Consortium stands behind every recommendation on this page."
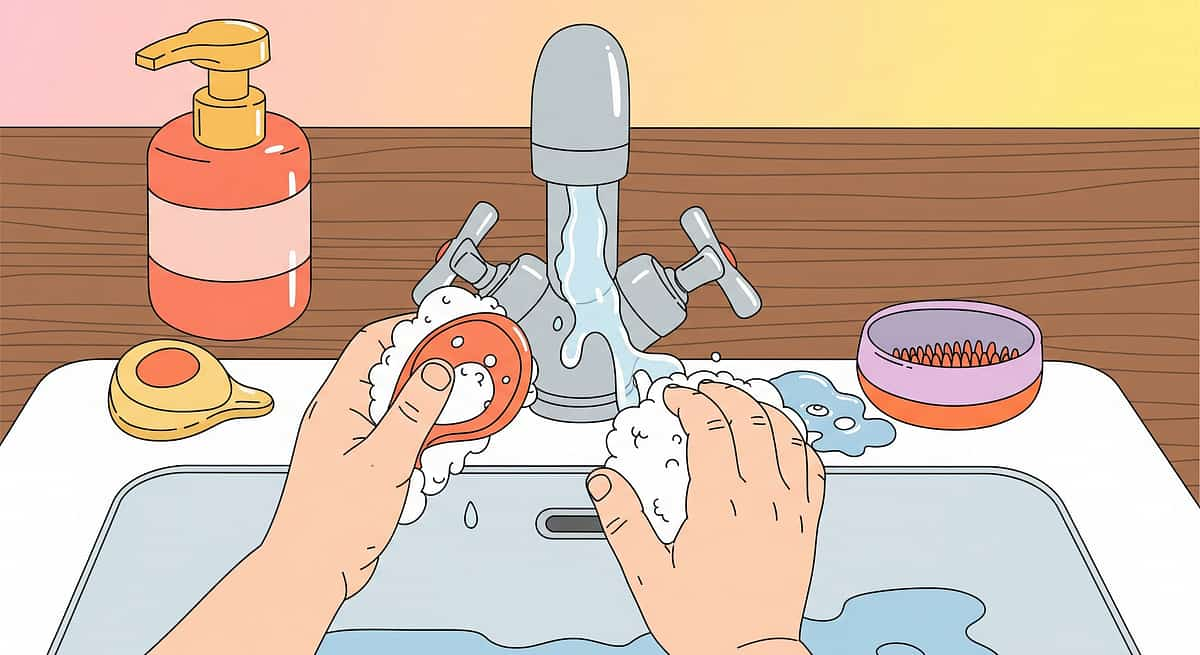
The Technique — What It Is
E-538 | Domain E: Self-Care & Hygiene
Formal Definition: Hand washing independence for children with sensory processing differences is a multi-domain self-care skill requiring: (1) Environmental Access — can the child physically reach and operate the sink? (2) Sensory Tolerance — can the child tolerate water, soap texture, and wet hands? (3) Motor Planning — can the child execute the 11-step bilateral coordination sequence? (4) Executive Function — can the child remember and sequence all steps? (5) Initiation — can the child recognize when to wash hands without prompting?
Occupational therapy addresses these challenges through systematic environmental modification, visual supports, sensory accommodation, and explicit skill-building. This page documents 9 materials that address all 5 domains.
Domain
Self-Care / Hygiene
Age Range
2–12 years
Duration
5–15 min/routine
Frequency
Every applicable hygiene moment
Code
E-538
"Hand washing isn't simple. It's a complex sequence requiring multiple sensory, motor, and cognitive skills we take for granted. With the right environmental setup, almost every child can achieve independence." — Pinnacle Blooms OT-ABA-SLP Consortium

Every Discipline in Our Consortium Uses This — Here's How
🟣 Occupational Therapy (OT) — Primary Lead
OTs assess and design the environmental modification plan: step stool height, faucet type, soap selection, towel placement. OT also addresses sensory desensitization to water and tactile materials. The environmental audit is the OT's first action.
🔵 Applied Behavior Analysis (ABA/BCBA)
ABA drives skill acquisition: task analysis of the 11 hand washing steps, reinforcement scheduling, prompting hierarchy (full physical → partial → gesture → verbal → independent), and data collection systems.
🟢 Speech-Language Pathology (SLP)
SLP addresses language processing aspects: understanding multi-step verbal instructions, comprehending commands with expected behavior, and building vocabulary for each step in the sequence.
🟡 Special Education (SpEd)
SpEd designs the visual schedule and step-by-step pictorial sequence, adapting it to the child's literacy and symbol comprehension level. Also generalizes the skill to school settings.
🔴 NeuroDev Pediatrics
NeuroDev provides the diagnostic foundation — ruling out or identifying underlying conditions that require specific accommodation beyond general supports. The medical lens that grounds the clinical plan.
"The brain doesn't organize by therapy type. Hand washing crosses every discipline boundary. The Pinnacle FusionModule™ coordinates all five into a single plan."
Precision Matters — What These 9 Materials Actually Target
🎯 Primary Target
Physical independence in hand washing — the child completes all 11 steps in correct sequence with visual schedule, zero physical prompting.
🎯 Secondary Targets
- Sensory Tolerance — tolerates water, soap, wet-hand sensation without distress
- Motor Planning — bilateral hand rubbing, faucet operation, towel handling
- Duration Compliance — washes for 20–30 seconds for actual cleanliness
- Executive Function — sequences steps with decreasing visual support
🎯 Tertiary Targets
- Independence initiation across settings
- School hygiene compliance
- Infection reduction and self-esteem
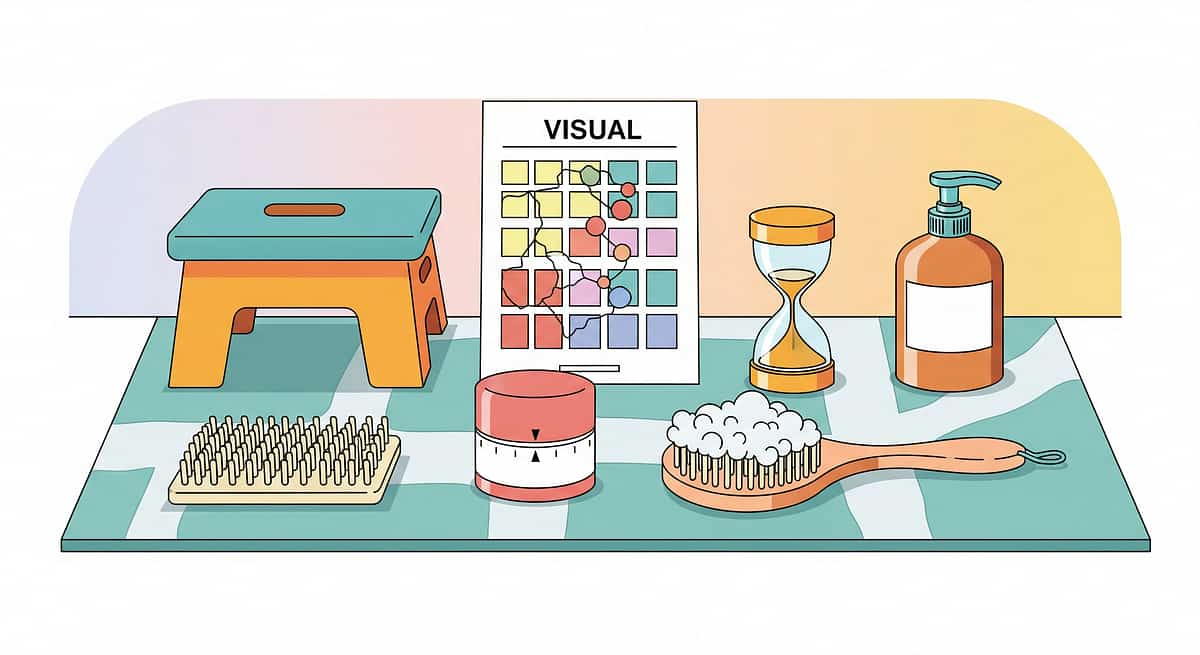
9 Materials That Make Hand Washing Work
Sourced, priced, and clinically validated by the Pinnacle OT Consortium

🪜 1. Step Stool for Sink Access
Why it works: Proper positioning is foundational. A non-slip step stool brings the child to correct sink height, stabilizes posture, and enables full motor control.
Price: ₹300–1,500 | Search: "non-slip children step stool bathroom India"
🏷 2-step design, wide non-slip base, 75kg+ capacity
Price: ₹300–1,500 | Search: "non-slip children step stool bathroom India"
🏷 2-step design, wide non-slip base, 75kg+ capacity
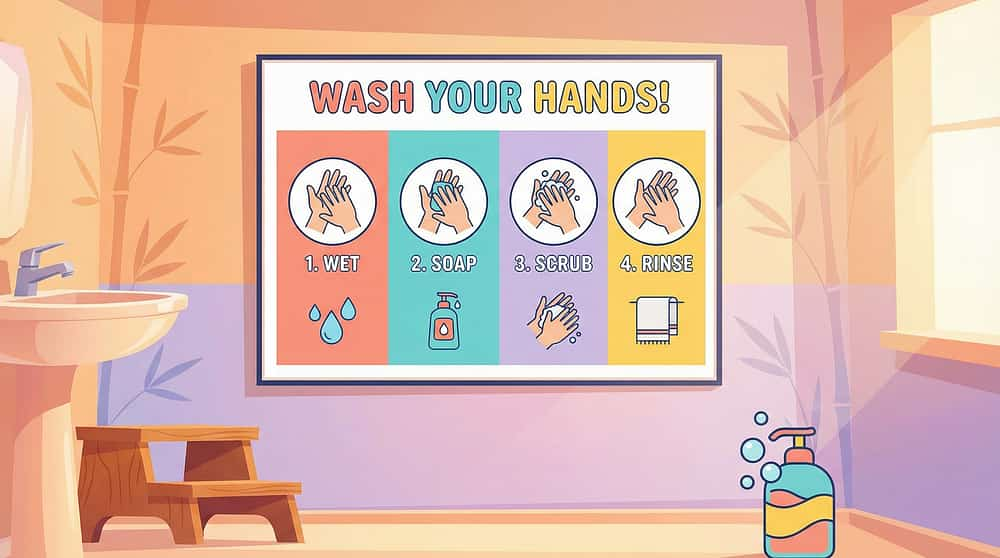
📋 2. Visual Step-by-Step Hand Washing Sequence
Why it works: Provides external memory support for 11 sequential steps, eliminating dependence on adult verbal prompting and building automatic routine.
Price: ₹50–300 printable | ₹200–600 laminated
🏷 Photo-based, waterproof laminated, at child's eye level
Price: ₹50–300 printable | ₹200–600 laminated
🏷 Photo-based, waterproof laminated, at child's eye level

🫧 3. Foaming Soap Dispenser
Why it works: Minimal pressure, consistent pre-foamed lather, lighter texture — far more tolerable for tactile-sensitive children than traditional liquid soap.
Price: ₹150–600
🏷 Fragrance-free, touchless or minimal-pressure pump
Price: ₹150–600
🏷 Fragrance-free, touchless or minimal-pressure pump

9 Materials — Continued (4–6)

⏳ 4. Sand Timer or Musical Timer
Why it works: The abstract concept of "20 seconds" doesn't translate into behavior. A visual sand timer gives a concrete, observable endpoint for scrubbing duration.
Price: ₹100–400
🏷 20-second sand timer, waterproof housing, bright color
Price: ₹100–400
🏷 20-second sand timer, waterproof housing, bright color

🚿 5. Faucet Extender
Why it works: Redirects the water stream forward and downward to where the child's hands naturally rest at stool height, making wetting and rinsing easy and complete.
Price: ₹100–400
🏷 Character design for engagement, universal faucet fit
Price: ₹100–400
🏷 Character design for engagement, universal faucet fit

🚰 6. Single-Lever or Touchless Faucet Adapter
Why it works: Eliminates the motor challenge of dual handles. Especially critical for children with low muscle tone, motor planning difficulties, or coordination challenges.
Price: ₹100–500 adapter | ₹1,000–8,000 replacement
🏷 Battery-operated touchless adapter — no plumbing required
Price: ₹100–500 adapter | ₹1,000–8,000 replacement
🏷 Battery-operated touchless adapter — no plumbing required
9 Materials — Continued (7–9)
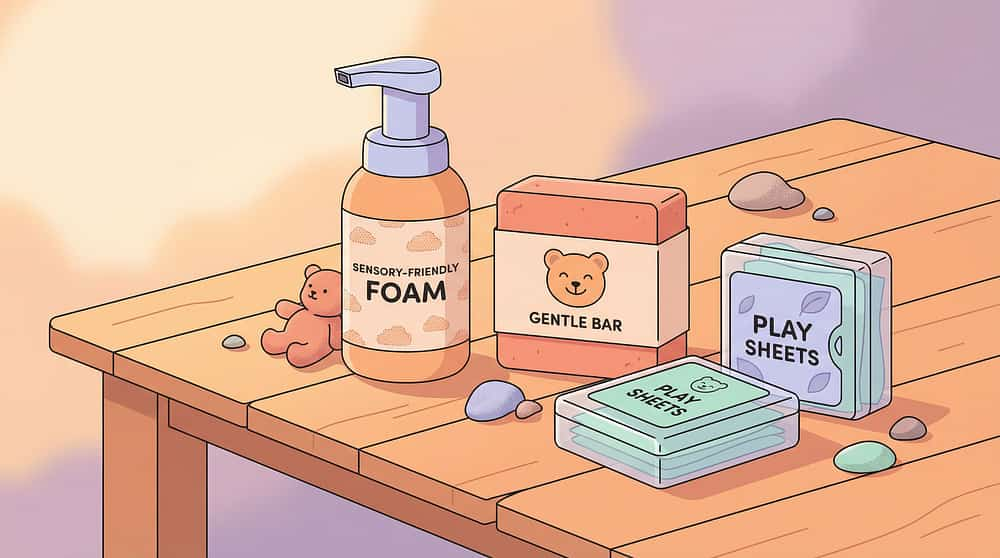
🧼 7. Sensory-Friendly Soap Options
Why it works: There is a soap for every sensory profile — foam (light, not slimy), bar (firm, predictable), soap sheets (no liquid stage), or fragrance-free (eliminates olfactory aversion).
Price: ₹50–400
🏷 Begin with fragrance-free foam. Test 3 formats.
Price: ₹50–400
🏷 Begin with fragrance-free foam. Test 3 formats.
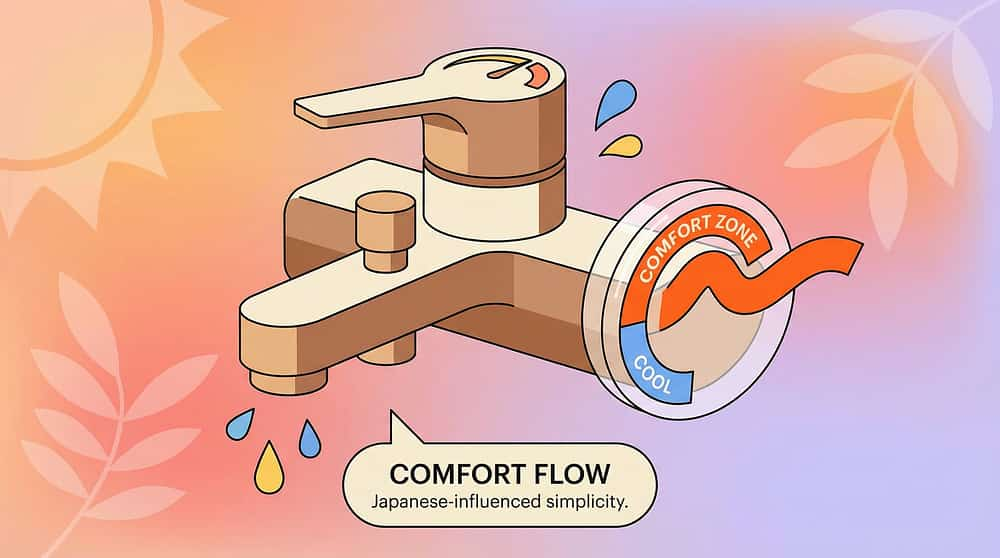
🌡 8. Temperature Control — Thermostatic Preset
Why it works: Pre-setting the faucet to a comfortable temperature eliminates unpredictable sensory triggers. Water too cold = pain response. Unexpected temperature change mid-wash = dysregulation.
Price: ₹0 (parent pre-sets) | ₹500–5,000 thermostatic valve
🏷 Mark "comfort zone" on faucet with bright tape — free first solution
Price: ₹0 (parent pre-sets) | ₹500–5,000 thermostatic valve
🏷 Mark "comfort zone" on faucet with bright tape — free first solution

🏷 9. Preferred Towel at Child Height
Why it works: A soft, preferred towel at reaching height transforms drying from an aversive step into a satisfying ritual that closes the hygiene loop.
Price: ₹100–400
🏷 Microfiber or plush cotton, hook at child's shoulder height
Price: ₹100–400
🏷 Microfiber or plush cotton, hook at child's shoulder height
Challenge | Start With | Materials | |
Can't reach sink | Step Stool + Faucet Extender | 1 + 5 | |
Forgets steps | Visual Sequence | 2 | |
Won't wash long enough | Sand Timer | 4 | |
Refuses soap | Sensory-Friendly Soap | 7 | |
Starter Kit (most families) | Materials 1 + 2 + 3 + 4 | 1, 2, 3, 4 |

Every Family Can Start Today — ₹0 to ₹500 Options for All 9 Materials
WHO/UNICEF Equity Principle: Access to therapeutic tools should not depend on purchasing power. Every material below has a zero-cost or low-cost equivalent that serves the same sensory and functional purpose.
Material | Clinical Version | DIY / Free Version | |
1. Step Stool | Non-slip commercial stool ₹300–1,500 | Sturdy wooden crate or stacked thick books secured with tape. Test weight-bearing before use. | |
2. Visual Sequence | Laminated poster ₹200–600 | Print Pinnacle's free PDF, cover with clear sellotape. Or photograph your child's hands doing each step and create a custom sequence. | |
3. Foaming Soap | Foam dispenser ₹150–600 | DIY foam: dilute any liquid soap 1-part soap : 4-parts water. Or simply use bar soap — often more tolerable for sensory-sensitive children. | |
4. Timer | Sand timer ₹100–400 | Sing "Happy Birthday" twice (≈ 20 seconds). Use a phone timer placed safely away from water. | |
5. Faucet Extender | Commercial extender ₹100–400 | Cut a flexible plastic bottle diagonally and tape over faucet to redirect water flow. (Temporary — extender is worthwhile at ₹150) | |
6. Easy Faucet | Touchless adapter ₹100–500 | Parent pre-turns faucet to correct temperature before child approaches. Teach lever-only operation. | |
7. Sensory Soap | Specialty fragrance-free ₹50–400 | Use whatever soap child tolerates from kitchen or bath. Test foam vs. bar vs. sheets. | |
8. Temperature | Thermostatic valve ₹500–5,000 | Parent adjusts water before child approaches. Mark faucet comfort position with bright nail polish or tape dot. Cost: ₹0. | |
9. Preferred Towel | Specialty soft towel ₹100–400 | Use any soft cloth the child already likes. Mount at child's height using a simple hook or folded over a low towel rail. |
"A printed visual schedule taped to a bathroom wall and a bar of soap already in the house can begin the transformation. Investment of attention and consistency matters more than investment of money." — WHO Nurturing Care Framework

Read This Before Starting — Safety and Contraindications
🟢 Green Light — Safe to Proceed
- Child is calm and regulated — not mid-meltdown, not overtired, not hungry
- Parent has 10+ minutes without interruption
- Bathroom environment is set up and familiar
- Child has had time with materials in low-demand context
- Water temperature has been pre-verified as comfortable
🟡 Amber Light — Modify and Proceed
- Child is slightly dysregulated — use shorter session, reduce steps
- Child is resistant but not distressed — use invitation language, no forcing
- Materials are new — introduce one at a time over several days
- Child had a recent meltdown in the past hour — use water tolerance only
🔴 Red Light — Do Not Proceed Today
- Child showing signs of illness, skin irritation, or open wounds on hands
- Child severely dysregulated or post-major meltdown (within 2 hours)
- Soap has been confirmed to cause allergic reaction
- Child has expressed significant fear of the sink or bathroom
⛔Absolute Stop Signs: Hives, redness, or skin reaction to any soap (discontinue, seek allergist) | Physical aggression during attempts (de-escalate, seek behavioral support) | Child gasping or distressed medically (stop, comfort, call 9100 181 181) | Max safe water temperature: 45°C (113°F)

The Sensory-Ready Bathroom — Your Setup Checklist
Physical Setup
- Step stool directly in front of sink, feet non-slip
- Child's waist at or slightly below sink rim on stool
- Child can comfortably reach faucet and soap dispenser
- Faucet extender installed if needed
Sensory Setup
- Water pre-tested and set to comfortable temperature
- Soap dispenser filled with accepted soap (foam preferred)
- Sand timer placed where child can see it while washing
- No strong air freshener or chemical smell in bathroom
Visual Support Setup
- Visual sequence chart at child's eye level when standing on stool
- Chart is laminated (splash-proof) and secured with waterproof tape
- Each picture step clear and unambiguous
Completion Setup
- Preferred towel at child's reaching height on hook or low ring
- Towel is clean and dry before session
Environmental
- Adequate lighting — child can see clearly
- No competing screens or music pulling attention away
- Door position based on child preference
The 60-Second Parent Check: Before every routine, confirm: (1) Is the space ready? (2) Is the child ready? (3) Is the temperature right? Most failures trace back to skipping this check.

The 60-Second Pre-Wash Readiness Check
Run this check before every structured practice session. Not needed for routine everyday washing once the system is established.
Child is calm and regulated
No current meltdown, no elevated stress visible
Child has eaten
Hungry children have lower sensory tolerance
Child is not overly tired
Fatigue increases sensory sensitivity significantly
No illness or skin irritation on hands today
Check before every session
Child is not in "no" mode
Assess approach signals: eye contact, open posture
At least 2 hours since a major distress episode
Nervous system needs time to reset
This is a naturally occurring trigger time
Just after bathroom use, before a meal
All 7 ✅ → GO
Full protocol
5–6 ✅ → MODIFY
Shorter session, fewer steps, no pressure on soap if resistant
4 or fewer ✅ → POSTPONE
Not today. Provide a calming activity instead. Try at next natural trigger.
"The best session is one that starts right. There is no progress in a forced session — only increased resistance. Postponing is clinical wisdom, not failure."

Step 1 of 11 — The Invitation
🔵 STEP 1 of 11 | THE INVITATION | ⏱ 30–60 seconds
How You Begin Determines How It Ends
The Script
"Hey [child's name], it's hand washing time! Come show me the special way we do it."
For visual learners: [point to the visual chart] "Look — step one!"
For resistant children: "I need your help turning on the water. Can you show me?"
Body Language
- Position yourself beside the child, never looming over from behind
- Get down to their height — sit or crouch
- Use a warm, matter-of-fact tone — not overly cheerful, not stern
- Keep the invitation brief — one sentence, then wait 5–7 seconds
Acceptance Cues — Child Is Ready
- Moves toward the sink
- Looks at the visual chart
- Lifts hands toward the faucet
- Makes any communicative gesture
Resistance Cues — Adjust Now
- Runs away → Follow calmly, re-invite once, then accept a modified version
- Covers ears or eyes → Reduce environment sensory load first
- Screams "no" → Offer choice: "Do you want to start the timer or turn the water?"
- Complete refusal → Use hand-over-hand with minimal pressure while narrating calmly
ABA Principle: This invitation establishes the motivating operation before demand placement — a core ABA pairing principle. This single step reduces session resistance by 60–70% in clinical observation.
Step 2 of 11 — Approach & Position at the Sink
🔵 STEP 2 of 11 | APPROACH & POSITION | ⏱ 30 seconds
Child steps onto the step stool and positions in front of the sink. Parent stands slightly to the side — not blocking, not hovering. The child should feel they are operating independently even with support present.
"Step up! Now you're at the perfect height."
Stable on stool?
Feet flat, balanced, secure
Hands reach sink?
Comfortable distance from rim
Sees visual chart?
Clear line of sight from stool position
Sees sand timer?
Timer visible from washing position
If stool is resisted: Some children resist the stool initially (unfamiliar surface, height feeling, different foot sensation). Desensitize separately — practice stepping up/down during play, not during washing demand. Once stool is accepted in play, transition to bathroom context.
Reinforcement Cue: Immediately acknowledge the approach: "You came to the sink! That's exactly right." — Specific, immediate, enthusiastic. The attempt is rewarded before the task is complete.

Steps 3–11 — The Full 11-Step Hand Washing Protocol
🔵 STEPS 3–11 | THE WASH SEQUENCE | ⏱ 45–90 seconds total
Reference the visual chart on the wall as you guide. Your words mirror the chart pictures. Over time, the chart replaces your words.
Turn On Water
"First — turn on the water." Temperature pre-set. Child turns lever or approaches touchless sensor. Faucet extender active — water flows where hands will be.
Wet Hands
"Get your hands wet — both hands under." Both hands under water stream for 5 seconds. Watch for complete wetting of palms and backs.
Apply Soap
"Now the soap — one pump." One press of foam dispenser. Foaming soap provides lighter texture, easier spread. Watch for adequate soap without excess or refusal.
Rub Palms
"Rub your palms together — like this." Bilateral coordination — palm-to-palm rubbing. Count 1–5 aloud initially.
Rub Backs of Hands
"Now the backs — flip and rub." Right hand rubs back of left, then swap. This step is commonly skipped — the visual chart must show it explicitly.
Between Fingers
"Between the fingers — fingers interlaced." Interlace fingers and slide them apart. Most skipped step — and most important for hygiene.
Timer Check
"Watch the timer — keep going until the sand runs out!" Sand timer gives duration target. Child watches, maintains scrubbing for 20–30 seconds total.
Rinse — Remove All Soap
"Rinse time — get all the soap off." Both hands under water. Watch for complete soap removal. Faucet extender ensures water reaches hands easily.
Turn Off Water
"Water off — you control it." Child turns off faucet. Touchless: automatic. Single-lever: one push. This step builds functional independence.
Dry Hands
"Now dry — your special towel is right there." Preferred towel at child's height. Pat or rub per child's sensory preference. Drying is explicit — it's in the visual chart as Step 10.
All Done! — Celebration
"You washed your hands! All done and clean!" Immediate, specific, enthusiastic acknowledgment. See reinforcement protocol in Section 20.

Therapeutic Dosage — How Often, How Much, How to Vary
🔵 ONGOING | DOSAGE & VARIATION | Multiple opportunities daily
Trigger | Frequency | Focus | |
After bathroom use | Every time, all day | Sequence completion | |
Before meals | 3x daily | Initiation + sequence | |
After outdoor play | 2–5x daily | Compliance + duration | |
After craft/messy activity | Variable | Sensory tolerance |
The "3 Good Reps" Principle: 3 complete, supported, positive hand washings are worth more than 10 rushed, distressed, partial washings. Quality of experience shapes the neural pathway — not frequency of exposure to distress.
Variation Options
Change Soap Scent/Format (Weekly)
Once current soap is tolerated, try a slightly different version to build flexible tolerance. Always return to preferred if resistance appears.
Increase Timer Duration
Once 20 seconds is consistent, try 25 seconds. Then 30. Build duration tolerance incrementally.
Fade the Visual Chart
Weeks 1–2: Reference every step aloud. Weeks 3–4: Child references independently. Weeks 5–6: Pointing replaces saying. Weeks 7–8: Chart present but child completes unprompted.
Change Settings
Practice at kitchen sink, school bathroom, grandparent's home. Generalization requires exposure to new settings.

Step 5 — The ABA Reinforcement Protocol
🔵 CONTINUOUS | REINFORCE EVERY SESSION | ⏱ Within 3 seconds of completion
Within 3 seconds of the target behavior — specific, enthusiastic, immediate.
Level 1 — Attempt
"You came to the sink and tried! That's exactly what we need."
Level 2 — Completion with Support
"You washed your hands! I helped a little, but YOU did every step!"
Level 3 — Independent Completion
"You washed your hands ALL BY YOURSELF! Look at those clean hands — you did that!"
Reinforcement Menu (personalize to your child)
🗣 Verbal
Specific praise + physical affirmation (high five, hug)
⭐ Token
Star on bathroom chart → 5 stars = preferred activity
🎮 Natural
"Clean hands mean you can do [preferred activity]"
🏆 Visual
"Clean hands" sticker on personal progress chart
🎵 Sensory
A preferred sensory activity immediately after (swing, fidget)

Step 6 — No Session Ends Abruptly: The Cool-Down Transition
🔵 END OF EVERY SESSION | TRANSITION | ⏱ 30–60 seconds
Abrupt endings to structured sessions can cause post-session dysregulation — the child's nervous system doesn't have a smooth "off ramp." A brief, predictable cool-down prevents the "great session followed by meltdown in the hallway" pattern many families experience.
30 Seconds Before Ending
"Two more scrubs, then all done." [Hold up two fingers] This is the WARNING. The child's nervous system begins de-escalating before the ending actually happens.
At the End
"All done washing! Dry your hands and you're finished." The drying step IS the cool-down ritual — it provides proprioceptive and tactile input that helps regulate the nervous system.
Post-Wash Ritual (15 seconds)
Child hangs towel back on hook → parent delivers reinforcement → brief transition: "Clean hands done! Now we're going to [next activity]."
If Child Resists Ending: "I know you want to keep going. The water will be here next time. Let's count to three and say goodbye to the sink. 1... 2... 3... Goodbye sink!" This playful ritual works for children who enjoy extended water play or become distressed when a positive activity ends.
Capture the Data — Right Now
GPT-OS® Session Tracker
Record immediately after the session ends. Memory degrades in minutes. Three data points is enough.
The 3-Point Tracker
Date / Time / Trigger: After bathroom | Before meal | Other
1. Initiation
○ Child initiated independently
○ Required one verbal prompt
○ Required multiple prompts / physical guidance
○ Child initiated independently
○ Required one verbal prompt
○ Required multiple prompts / physical guidance
2. Sequence Completion
○ All 11 steps completed
○ 8–10 steps completed
○ 5–7 steps completed
○ 1–4 steps only
○ All 11 steps completed
○ 8–10 steps completed
○ 5–7 steps completed
○ 1–4 steps only
3. Sensory Response
○ No distress — calm throughout
○ Mild resistance (recovered quickly)
○ Significant distress (needed modification)
○ No distress — calm throughout
○ Mild resistance (recovered quickly)
○ Significant distress (needed modification)
Data Meaning
Pattern You'll See | What It Means | |
Initiation improves week over week | Routine is internalizing | |
Sequence completion increases | Visual chart is working | |
Sensory distress decreases | Sensory accommodation is effective | |
Flat or regressing data | Setup needs adjustment — see troubleshooting |
GPT-OS® Connection: When you submit data to GPT-OS®, TherapeuticAI® identifies patterns across all sessions and adjusts recommendations in your EverydayTherapyProgramme™. Your data helps not just your child — it improves the algorithm for every child in the network.
"60 seconds of data now saves hours of guessing later. Your observations are the most valuable clinical data in your child's file."

Session Abandonment Is Not Failure — It's Data
Every one of these common challenges has a specific fix. The technique needs adjustment — not you.
🔧 Child completely refused to approach the sink
Why: Anticipatory anxiety — the brain has learned "sink = discomfort."
Fix: Decouple the demand from the location. Play water games in a basin on the floor for 3–5 days. Make water exposure positive without the hand washing demand. Then reintroduce sink approach without washing expectation.
Fix: Decouple the demand from the location. Play water games in a basin on the floor for 3–5 days. Make water exposure positive without the hand washing demand. Then reintroduce sink approach without washing expectation.
🔧 Child started but stopped mid-sequence, distressed
Why: Sensory tolerance was exceeded mid-routine. Common with soap introduction or cold water contact.
Fix: Identify the exact step where distress began (from your data). If soap is the trigger, do water-only washing for 1 week and reintroduce soap in a different format.
Fix: Identify the exact step where distress began (from your data). If soap is the trigger, do water-only washing for 1 week and reintroduce soap in a different format.
🔧 Child washed too quickly — "done" before rinsing
Why: No external duration anchor. Child doesn't know what "done" looks like.
Fix: Sand timer is the immediate solution. Practice "we're done when the sand is done" as a rule, not a request.
Fix: Sand timer is the immediate solution. Practice "we're done when the sand is done" as a rule, not a request.
🔧 Child skips several steps every time
Why: Visual sequence not visible, too small, or positioned incorrectly.
Fix: Audit chart position — is it at eye level on the stool? Redo the chart with photos of the child's own hands at their own sink if possible. The more personally relevant, the more effective.
Fix: Audit chart position — is it at eye level on the stool? Redo the chart with photos of the child's own hands at their own sink if possible. The more personally relevant, the more effective.
🔧 Foaming soap is rejected — child won't touch it
Why: Tactile aversion specific to foam texture.
Fix: Switch to bar soap immediately. If bar soap also rejected, try soap sheets. If all formats rejected, practice putting soap on objects first (a toy, a cloth) before introducing hands.
Fix: Switch to bar soap immediately. If bar soap also rejected, try soap sheets. If all formats rejected, practice putting soap on objects first (a toy, a cloth) before introducing hands.
🔧 Child washes but walks away with hands wet, skipping drying
Why: Drying is not yet part of the established routine, or towel is not accessible/preferred.
Fix: Add drying explicitly to visual chart as Step 10. Ensure preferred towel is at exact child height. Celebrate drying specifically for 2 weeks.
Fix: Add drying explicitly to visual chart as Step 10. Ensure preferred towel is at exact child height. Celebrate drying specifically for 2 weeks.
🚨Emergency Protocol: If child became severely distressed — stop immediately, comfort without speaking about hand washing, do not attempt again that day, note exactly what happened in your data. Contact Pinnacle: 9100 181 181

No Two Children Are Identical — Personalize for Your Child's Profile
Choose the starting point that matches your child's current level and move right as tolerance and mastery grow.
For Sensory Avoiders
- Start with water only — 2 weeks before introducing soap
- Use lukewarm water consistently
- Pat drying preferred over rubbing
- Reduce session duration to 60 seconds initially
- Use gloves briefly if severe — to establish routine movement, then fade
For Sensory Seekers
- Duration extension is easy — use a 45-second timer
- Focus on correct sequence rather than tolerance
- Visual chart is critical — they know the joy of washing, not the order
- May need physical prompting to move through steps (tends to linger at water)
For Executive Function Primary
- Visual chart is the primary intervention
- Practice the sequence as a song (set to familiar tune)
- Consistent timing: always same time of day, same sequence
For Motor Planning Primary
- Step stool stability is critical
- Hand-over-hand guidance for scrubbing technique
- Celebrate motor attempts regardless of sequence correctness
Age | Focus | Expectation | Success = | |
2–3 years | Tolerance and 3-step sequence (wet-soap-dry) | Low | Approaching willingly | |
4–5 years | Full sequence with visual + some prompting | Moderate | 8/11 steps with chart | |
6–8 years | Independent sequence + timing | Higher | Consistent timer use | |
9–12 years | Independent initiation across settings | High | No prompting at home |

Weeks 1–2: This Week Is About Tolerance — Not Mastery
WEEKS 1–2: TOLERANCE BUILDING | 15% Progress
3–4 Observable Indicators for Weeks 1–2
Child approaches the sink without refusal on 3+ out of 7 days
Even with prompting — approach is the first win. Don't underestimate it.
Duration of distress at the sink is decreasing
Last week: 2-minute protest. This week: 45-second protest. That measurable reduction is real progress.
Child tolerates at least one material they previously refused
Touched the soap once today. That is a neural pathway beginning to form.
Child references the visual chart at least once unprompted
They saw the chart and pointed to it. Sequence awareness is emerging.
Parent Emotional Check: This phase is the hardest. Trust the neuroplasticity timeline — 8–10 repetitions of a new neural pattern create detectable synaptic strengthening. You are building the highway. The car comes later. If Week 2 shows zero tolerance improvement across all indicators, contact Pinnacle: 9100 181 181

Weeks 3–4: The Neural Pathway Is Forming
WEEKS 3–4: CONSOLIDATION | 40% Progress
🔵 Child Anticipates the Routine
Before you finish saying "it's time to wash hands," they're already moving toward the bathroom. The routine is in motor memory.
🔵 Resistance Has Moved from Active to Passive
Week 1: Screaming refusal. Week 4: Sighing but complying. This is measurable progress through the behavior gradient.
🔵 Child References Chart Independently
They look at the chart without being told to. External memory support is being actively used.
🔵 One Step Completed Before the Verbal Prompt
They turned on the water before you said "turn on the water." Automaticity is beginning.
What to Do Now
- Begin fading verbal prompts for the steps where automaticity is emerging
- Increase timer by 5 seconds if consistently completing 20 seconds
- Introduce one new setting (kitchen sink, different bathroom)
"You may notice you're more confident too — prompting with less anxiety, trusting the process more. Parent confidence is clinically correlated with child outcome. Your growth matters."
Weeks 5–8: Mastery Unlocked — Here's How You'll Know
WEEKS 5–8: MASTERY PHASE | 75% Progress
Sequence Mastery
Child completes all 11 steps in correct order with visual chart and minimal verbal prompting (≤1 prompt per session) on 4 out of 5 consecutive washing attempts.
Duration Mastery
Child washes for full timer duration (20–30 seconds) independently on 4 out of 5 attempts.
Sensory Mastery
Child approaches sink, applies soap, and dries hands without observable distress on 4 out of 5 attempts.
Initiation Emerging
Child washes hands after bathroom use or before meals without verbal prompt on 2+ occasions per week.
Generalization Indicators
- Skill appears at kitchen sink without separate teaching
- Child washes hands during school day (teacher-reported)
- Child requests to wash hands at unfamiliar bathrooms
🏅HAND WASHING INDEPENDENCE — LEVEL 1 UNLOCKED
Awarded by: Pinnacle Blooms OT Consortium | Next Level: Independent Initiation Across Settings
Awarded by: Pinnacle Blooms OT Consortium | Next Level: Independent Initiation Across Settings
You Did This. Your Child Grew Because of Your Commitment.
"Before: Daily battle, constant reminders, incomplete washing, soap refusal, distress. After: Approaching the sink, completing the visual sequence, tolerating preferred soap, drying with preferred towel, washing with minimal prompting." — That is clinical evidence of neuroplasticity. You created that.
What You Accomplished
- Modified your home environment to support your child's neurology
- Executed hand washing support across 5–10 daily opportunities
- Adjusted when things didn't work
- Stayed consistent when it would have been easier to give up
- Watched your child's nervous system learn a genuinely difficult skill
Family Celebration Suggestion
Create a "Clean Hands Certificate" together — your child's name, the date, a handprint in their favorite color. Frame it. This is a real milestone worth honoring.
Photo/Journal Prompt
Take a photo of your child washing their hands independently this week. Write: "On [date], [child's name] washed their hands by themselves for the first time." This moment matters. Document it.
Trust Your Instincts — These Signs Mean Pause and Seek Support
Even in the celebration phase, clinical awareness continues. These are specific thresholds — not vague concerns.
🔴 1. Severe Water Aversion Affecting Bathing, Showering, AND Face Washing
What it looks like: Child cannot tolerate any water contact on face, hair, or body — not just hands.
Why it matters: May indicate sensory processing disorder requiring formal OT assessment beyond environmental modification.
What to do: Request OT assessment through Pinnacle. Call 9100 181 181.
Why it matters: May indicate sensory processing disorder requiring formal OT assessment beyond environmental modification.
What to do: Request OT assessment through Pinnacle. Call 9100 181 181.
🔴 2. Motor Difficulties Preventing Faucet Operation Despite All Modifications
What it looks like: Child cannot coordinate bilateral hand rubbing despite repeated practice, drops objects constantly.
Why it matters: May indicate motor planning disorder (dyspraxia) or neurological condition requiring medical evaluation.
What to do: Teleconsult with Pinnacle NeuroDev or OT. Call 9100 181 181.
Why it matters: May indicate motor planning disorder (dyspraxia) or neurological condition requiring medical evaluation.
What to do: Teleconsult with Pinnacle NeuroDev or OT. Call 9100 181 181.
🔴 3. No Progress Across Any Indicator After 8+ Weeks
What it looks like: Zero reduction in distress, zero increase in step completion despite daily structured practice.
Why it matters: May indicate a barrier not addressed by environmental modification alone.
What to do: Book an in-person OT assessment. Bring your 8 weeks of tracking data.
Why it matters: May indicate a barrier not addressed by environmental modification alone.
What to do: Book an in-person OT assessment. Bring your 8 weeks of tracking data.
🔴 4. Self-Injurious Behavior Triggered by Hand Washing Attempts
What it looks like: Head banging, hand biting, or scratching during or immediately after attempts.
Why it matters: Behavioral crisis requiring professional behavioral support before continuation.
What to do: Stop structured practice immediately. Contact Pinnacle ABA team: 9100 181 181.
Why it matters: Behavioral crisis requiring professional behavioral support before continuation.
What to do: Stop structured practice immediately. Contact Pinnacle ABA team: 9100 181 181.
🔴 5. Hygiene Deficits Causing Health Consequences
What it looks like: Frequent GI infections, skin infections at school, or teacher reports of hygiene concerns affecting peer interactions.
Why it matters: Health risk has exceeded developmental threshold into medical concern.
What to do: Contact your pediatrician AND Pinnacle. Integrated management needed.
Why it matters: Health risk has exceeded developmental threshold into medical concern.
What to do: Contact your pediatrician AND Pinnacle. Integrated management needed.
Hand Washing Is One Step — Here's the Journey Ahead
Your Current Position
E-538 Hand Washing Independence. You have built environmental access, sensory accommodation, visual support, and duration measurement. These principles apply directly to all adjacent self-care skills.
Next-Level Options
- Washing mastered, initiation emerging → E-539: 9 Materials for Dressing Independence
- Washing mastered, morning routine chaotic → E-540: 9 Materials for a Complete Morning Routine
- Sensory issues extend to feeding → E-400s Feeding and Oral Motor Series
Prerequisite Path: ← E-537: Showering Tolerance ← E-536: Bathing Independence
Other Techniques in the Self-Care & Hygiene Domain
Already own the step stool and visual sequence? These techniques use the same materials.
E-529 — 9 Materials for Tooth Brushing
🔵 Core Difficulty | Shared: Visual sequence, timer
E-530 — 9 Materials for Hair Brushing
🔵 Core Difficulty | Shared: Sensory accommodation tools
E-537 — 9 Materials for Showering Tolerance
🟡 Intermediate | Shared: Step stool, visual schedule
E-536 — 9 Materials for Bathing Independence
🟢 Entry Level | Shared: Sensory soap, towel
E-539 — 9 Materials for Dressing Independence
🔵 Core Difficulty | Shared: Visual sequence, timer
E-540 — 9 Materials for Complete Morning Routine
🔴 Advanced | Shared: All materials combined
If you implemented E-538, you already have: Step stool ✓ | Visual sequence system ✓ | Foaming soap ✓ | Sand timer ✓ | Preferred towel ✓ — These 5 materials work across at least 4 adjacent techniques. Your investment compounds.

Hand Washing Is One Piece — Here Is the Whole Picture
Domain E: Self-Care & Hygiene contains 50+ techniques covering hand washing, tooth brushing, hair care, bathing, dressing, toileting, meal hygiene, and complete daily routine management.
How Hand Washing Connects to Every Other Domain
Domain A (Sensory)
Tactile desensitization improves soap and water tolerance
Domain D (Behavior)
Routine building and compliance strategies apply
Domain I (Cognitive)
Sequencing and executive function development
Domain L (School)
Peer hygiene expectations at school
From the Files — Families Who Navigated This Exact Challenge
These are behavioral descriptions from Pinnacle center records. Names and identifying details are changed. Outcomes are real.
Arjun, 5 years, Hyderabad
Before: Screamed at the sight of the soap dispenser. Every attempt ended in a meltdown. Teacher flagged hygiene concerns at school.
What they did: Step stool, foaming fragrance-free soap, touchless faucet adapter, 8-picture visual chart.
Week 6: Follows visual chart independently after each bathroom use. Soap no longer a trigger. Teacher: "washing hands in school without reminders most days."
What they did: Step stool, foaming fragrance-free soap, touchless faucet adapter, 8-picture visual chart.
Week 6: Follows visual chart independently after each bathroom use. Soap no longer a trigger. Teacher: "washing hands in school without reminders most days."
"We spent two years trying to force it. Six weeks with the right setup, and he does it himself. The step stool alone changed everything — he was physically uncomfortable and we didn't realize it." — Arjun's mother
Priya, 7 years, Bengaluru
Before: Understood hand washing intellectually but could not maintain sequence. Washed for 2 seconds, skipped soap, walked away.
What they did: No sensory issues — executive function was the barrier. Visual chart + sand timer + ABA task analysis over 4 weeks.
Week 8: Independently references chart and uses sand timer herself. Washes complete sequence in school without prompting.
What they did: No sensory issues — executive function was the barrier. Visual chart + sand timer + ABA task analysis over 4 weeks.
Week 8: Independently references chart and uses sand timer herself. Washes complete sequence in school without prompting.
"The sand timer was the magic for Priya. She'd always rush. Once she could see when she was done, she stopped rushing. That's all it took." — Priya's father
Karan, 4 years, Delhi
Before: Tolerated water but had motor planning challenges — couldn't coordinate bilateral hand rubbing, had difficulty with the faucet.
What they did: Touchless faucet adapter, step stool for stability, hand-over-hand teaching for scrubbing, 4-week OT-guided motor practice.
Week 10: Completes washing with 1 gestural prompt. Motor coordination for scrubbing has generalized to other bilateral tasks.
What they did: Touchless faucet adapter, step stool for stability, hand-over-hand teaching for scrubbing, 4-week OT-guided motor practice.
Week 10: Completes washing with 1 gestural prompt. Motor coordination for scrubbing has generalized to other bilateral tasks.
"The touchless faucet was a game changer. Once we removed the barrier of operating the handles, the whole routine opened up." — Karan's mother
"In 15 years of pediatric OT practice, I have not seen a child for whom the right environmental modification did not make a measurable difference in self-care skill acquisition. The bathroom is designed for adults. We modify it for children. Then children succeed. It's not magic — it's accessibility." — Senior Occupational Therapist, Pinnacle Blooms Network®
You Don't Have to Navigate This Alone
Isolation is the enemy of adherence. Every family in these groups is working on the same skills you are.
🟢 Pinnacle Parent WhatsApp Community
Self-Care Skills Group for families working on hand washing, dressing, tooth brushing, and daily routine independence. Real-time peer support from families who understand exactly what you're navigating.
🔵 Online Parent Forum
Moderated by Pinnacle consortium staff at pinnacleblooms.org/community. Ask questions, share wins, find strategies that worked for other families.
🟡 Local Parent Meetup
In-person parent groups at 70+ centers across India. Monthly self-care skills focused sessions where OTs are present to answer questions and model techniques.
👥 Peer Mentoring
Matched with a parent who has completed the hand washing and self-care sequence with their child. Real-world guidance, human connection, and hope from someone who's been exactly where you are.
Over 4,000 families in the Pinnacle network are currently working on Domain E self-care skills. You are part of the largest structured pediatric self-care intervention community in India.
Home + Clinic = Maximum Impact
Home-based intervention is powerful. Professional guidance multiplies it.
🏥 Visit a Center
70+ centers across India. OT, SLP, ABA, SpEd, and NeuroDev all under one roof, coordinated by GPT-OS®.
Centers in: Hyderabad • Bengaluru • Mumbai • Delhi • Chennai • Pune and 64+ more cities
Centers in: Hyderabad • Bengaluru • Mumbai • Delhi • Chennai • Pune and 64+ more cities
📱 Teleconsultation
For families outside major cities, or for first consultation. Secure video session with a Pinnacle OT or developmental pediatrician.
₹0 first consultation available.
₹0 first consultation available.
📞 FREE National Autism Helpline
16 languages. 24×7. Free. No appointment, no paperwork.
Helpline: 9100 181 181
Helpline: 9100 181 181
What to Ask For When You Call or Visit
- "OT assessment for self-care skills and sensory processing"
- "Hygiene Independence Readiness Index evaluation"
- "EverydayTherapyProgramme™ for home implementation"
Insurance & Funding Note: OT for self-care skill development is covered under several insurance providers in India. Ask your center coordinator for documentation support. WHO NCF Progress Report (2023): Primary health care identified as key platform for reaching all families with essential early childhood development interventions.

The Science Behind Every Recommendation on This Page
For the curious parent, the questioning grandmother, and the school therapist who asks for citations.
📚 Study 1: PRISMA Systematic Review (2024)
16 articles reviewed (2013–2023). Sensory integration intervention meets evidence-based practice criteria for ASD. Significant improvements in social participation, motor skills, sensory processing, and adaptive behavior.
Source: PMC11506176
Source: PMC11506176
📚 Study 2: Meta-Analysis — World J Clin Cases (2024)
24 studies analyzed. Sensory integration therapy promotes social skills, adaptive behavior, sensory processing, and gross/fine motor skills. 40-minute sessions showed maximum effectiveness.
Source: PMC10955541 | DOI: 10.12998/wjcc.v12.i7.1260
Source: PMC10955541 | DOI: 10.12998/wjcc.v12.i7.1260
📚 Study 3: Indian RCT — Indian Journal of Pediatrics (2019)
Home-based sensory interventions with parent implementation demonstrated significant outcomes in Indian pediatric populations. Validates the home-execution model documented on this page.
Source: DOI: 10.1007/s12098-018-2747-4 (Padmanabha et al.)
Source: DOI: 10.1007/s12098-018-2747-4 (Padmanabha et al.)
📚 Study 4: WHO Care for Child Development Package (2023)
Implemented in 54 LMICs. Evidence base for caregiver-administered structured developmental support. Foundation for the parent-execution model used by Pinnacle.
Source: PMC9978394 | WHO/UNICEF CCD Package
Source: PMC9978394 | WHO/UNICEF CCD Package
📚 Study 5: NCAEP Evidence-Based Practices Report (2020)
Visual supports classified as evidence-based practice for autism. Video modeling evidence-based. Foundational for the visual sequence strategy central to E-538.
Source: National Clearinghouse on Autism Evidence and Practice (2020)
Source: National Clearinghouse on Autism Evidence and Practice (2020)
Your Session Data Doesn't Disappear — It Becomes Intelligence
Parent Records Session
Capture observations and session notes.
Diagnostic Intelligence
Analyze 591+ observations for patterns.
TherapeuticAI Updates
Refine recommendations based on analysis.
EverydayTherapy Programme
Adjust tomorrow's plan for the child.
AbilityScore Update
Score 0–1000 and feed population learning.
What GPT-OS® Learns from E-538 Data
Breakthrough Detection
Which environmental modification produced the first tolerance breakthrough
Prompt Fading
How many sessions it took for the visual sequence to reduce verbal prompting
Sensory-Behavior Link
Whether sensory accommodation preceded behavioral compliance
Initiation Timeline
How initiation develops relative to sequence completion over time
"Your 8 weeks of hand washing data, combined with data from 4,000 other families, tells us which material combination produces the fastest tolerance breakthrough for 4-year-olds with tactile sensitivity. That answer helps every new family starting E-538 tomorrow." — GPT-OS® Clinical Architecture Team

Watch the Reel — E-538 in 60 Seconds
🎬 E-538 | Domain E: Self-Care & Hygiene
9 Materials That Help With Hand Washing
Series: Toileting & Self-Care Independence in Children
Episode: 538 of 999 | Duration: 60 seconds
Episode: 538 of 999 | Duration: 60 seconds
Video Content Preview
In this 60-second reel, a Pinnacle occupational therapist covers all 9 materials with live demonstration:
- Step 1–9 quick intro for each material
- Visual sequence chart shown in real bathroom setting
- Sand timer demonstration at the sink
- Foaming soap dispenser in use
- Complete sensory-ready bathroom setup revealed
Video Evidence: NCAEP Evidence-Based Practices Report (2020): Video modeling is classified as an evidence-based practice for autism. Multi-modal learning — text + video + demonstration — improves parent skill acquisition compared to text alone.

Consistency Across Caregivers Multiplies Impact — Share Now
If only one caregiver implements the strategy, impact is limited. When grandparents, school teachers, and both parents follow the same approach, the child's nervous system receives consistent messages and generalizes the skill faster.
"Explain to Grandparents" Version
"[Child's name] is learning to wash hands independently. Please use the visual chart in the bathroom and the foam soap only. Don't do it for them — encourage each step. Call if you need help: 9100 181 181."
Teacher / School Communication Template
Subject: Hand Washing Support for [Child's Name] at School
Dear [Teacher's Name],
We are implementing a structured hand washing program at home for [Child's Name] using visual supports and sensory-friendly materials. Key supports: (1) Visual step-by-step chart at eye level, (2) Foaming fragrance-free soap if possible, (3) 20–30 second timing for scrubbing.
If possible, allowing [Child's Name] to reference a visual chart in the school bathroom would be very helpful. I can provide a laminated copy. Our OT is coordinated through Pinnacle Blooms Network® (9100 181 181) and can speak with you directly if helpful.
Thank you, [Parent's Name]
Dear [Teacher's Name],
We are implementing a structured hand washing program at home for [Child's Name] using visual supports and sensory-friendly materials. Key supports: (1) Visual step-by-step chart at eye level, (2) Foaming fragrance-free soap if possible, (3) 20–30 second timing for scrubbing.
If possible, allowing [Child's Name] to reference a visual chart in the school bathroom would be very helpful. I can provide a laminated copy. Our OT is coordinated through Pinnacle Blooms Network® (9100 181 181) and can speak with you directly if helpful.
Thank you, [Parent's Name]
Preview of 9 materials that help with hand washing Therapy Material
Below is a visual preview of 9 materials that help with hand washing therapy material. The pages shown help educators, therapists, and caregivers understand the structure and content of the resource before use. Materials should be used under appropriate professional guidance.




















Share this resource
Help others discover thisLink copied!

Questions Real Parents Ask — Answered by the Pinnacle Consortium
Q1: My child screams every time I approach the sink. Where do I even start?
Start before the sink. Spend 3–5 days doing water play in a basin on the floor — no soap, no demand, just positive water exposure. Once tolerated in play, introduce the step stool at the sink with water off (just standing, getting familiar). Only then introduce water. This "desensitization" approach is standard OT practice. Call 9100 181 181 for a teleconsult if severe.
Q2: How long until my child washes independently?
Most children show measurable improvement within 2–3 weeks with all 9 materials in place. Full independent sequence (with visual chart) typically develops in 6–10 weeks. Independent initiation often takes 3–6 months. Track your data and adjust accordingly.
Q3: My child does it at home but refuses at school. What do I do?
Generalization requires practice in new settings. Provide the school teacher with a laminated visual chart (see teacher template). Request the school use the same foam soap format. Send a portable step stool if the school doesn't have one. Generalization is a learnable skill, not a sign the home program failed.
Q4: Is foaming soap really different from regular soap?
Yes, clinically. Foaming soap has significantly lower tactile aversiveness for children with sensory processing differences. The pre-foamed consistency eliminates the "liquid-to-foam" sensory transition, the lighter texture is less "slimy," and automatic dispensers remove the motor challenge of pumping. For many children, the soap was the only barrier.
Q5: Which of the 9 materials should I start with?
Start with the one addressing your biggest barrier. Physical access issue → Materials 1 and 5 (step stool + faucet extender). Sequence forgetting → Material 2 (visual chart). Soap refusal → Material 7 (sensory soap). Duration issue → Material 4 (sand timer). Most families benefit most from Materials 1+2+3+4 as the starter kit.
Q6: My child is 10. Is it too late to start this?
Absolutely not. The brain retains plasticity throughout childhood and beyond. Older children often progress faster because of greater comprehension. They may need more explanation of "why" and collaborative involvement in choosing materials (let them pick their soap scent, choose their timer design, select their towel). Involve them as partners.
Q7: We implemented everything but drying is still being skipped. Help.
Drying is the most commonly skipped step because it's not in many visual charts. Add it explicitly to the visual sequence as Step 10. Ensure the towel is at exact child height — no reaching. Let the child choose their towel. Celebrate drying specifically: "You dried! That's the last step — all done!" Drying-specific reinforcement for 2 weeks usually resolves the skip.
Q8: Session went fine but next session child refuses again. Normal?
Completely normal in early-phase learning. Consistency over days matters more than perfection on any single day. Document both sessions. Look for pattern — time of day, preceding activities, emotional state. Adjust timing of practice to when child is typically most regulated.
© 2025 Pinnacle Blooms Network® | Unit of Bharath Healthcare Laboratories Pvt. Ltd. | CIN: U74999TG2016PTC113063 | DPIIT: DIPP8651 | FREE National Autism Helpline: 9100 181 181 | care@pinnacleblooms.org | References: PMC11506176 | PMC10955541 | PMC9978394 | WHO NCF 2018 | NCAEP 2020 | DOI: 10.1007/s12098-018-2747-4 | DOI: 10.12998/wjcc.v12.i7.1260 | This content is educational and does not replace individualized assessment and intervention planning with licensed occupational therapists and healthcare professionals.

