
When Bath Time Becomes a Battlefield
It's hair wash night. The moment your child realizes it, the panic starts — before a single drop of water falls. You are not failing. Your child's nervous system is speaking in the only language it knows. Today, you found the tools to help it feel safe.
Ages 2–12 Years
Evidence-Based
Home-Executable
OT + ABA + NeuroDev

You Are Among Millions of Families Navigating This Exact Challenge
Hair washing intolerance is one of the most commonly reported sensory challenges across autism, SPD, ADHD, and anxiety. Globally, millions of caregivers experience exactly the bath-time battle you described. India's 8–13 million children estimated to have autism means sensory grooming difficulties affect an enormous number of families across every state, every income level, every language.
80%
Sensory Difficulty
of children with autism experience sensory processing difficulties affecting daily routines
1 in 36
ASD Prevalence
children diagnosed with autism spectrum disorder globally (CDC, 2023)
21M+
Therapy Sessions
delivered by Pinnacle — including sensory desensitization for hair washing
"You are among millions of families navigating this exact challenge. What you are feeling tonight — the exhaustion, the guilt, the love — is universal. What you are about to learn is evidence-based."
PRISMA systematic review (2024): 80% of children with autism display sensory processing difficulties. Meta-analysis of 24 studies confirms sensory integration therapy effectiveness. | PMC11506176 | PMC10955541

This Is a Wiring Difference — Not a Behavior Problem
The Neuroscience of Water Sensitivity
When water touches your child's head, here is what happens in milliseconds:
- Somatosensory Cortex receives the tactile input — water temperature, pressure, unpredictable flow
- Amygdala misclassifies the sensation as a threat signal
- Sympathetic nervous system fires a survival response — fight, flight, or freeze
- The child experiences genuine fear — not drama, not manipulation
The scalp contains the densest concentration of thermoreceptors and mechanoreceptors in the body — making it one of the most sensitive surfaces to unexpected wet stimulation.
What This Means For You
"My child isn't being dramatic. Their brain genuinely processes water on their head as dangerous."
"The panic response I see — the grabbing, the screaming, the pulling away — is their nervous system doing exactly what it was designed to do when it senses threat. It just doesn't know the threat isn't real."
"The solution isn't to force them through it. The solution is to modify the sensory input so the brain stops receiving the threat signal."
This is a wiring difference. It can change with the right tools, the right approach, and the right time.
Frontiers in Integrative Neuroscience (2020): Neurological basis for sensory-based interventions in ASD. | DOI: 10.3389/fnint.2020.556660

Your Child Is Here. Here Is Where We're Heading.
Hair washing difficulty typically peaks between ages 2–6 and is most acute during the period when sensory processing differences are most pronounced, language to communicate distress is still developing, and the child cannot yet understand WHY water won't harm them.
Ages 0–2
Basic bathing tolerance emerges
Ages 2–4
Hair washing challenge peaks here
Ages 4–7
Tolerating with supports (Goal Zone)
Ages 7–12+
Independent hair washing (Mastery)
Comorbidity Awareness
Hair washing intolerance is most commonly observed in children with: Autism Spectrum Disorder (tactile defensiveness), Sensory Processing Disorder, ADHD (low frustration tolerance + sensory reactivity), Anxiety disorders (anticipatory fear), and hypersensitivity to temperature and unexpected touch.
Most children do not naturally outgrow water sensitivity without intervention. They need graduated exposure, appropriate tools, and a nervous system that has been systematically shown — again and again — that water is safe.
WHO Care for Child Development Package (2023) | PMC9978394

Clinically Validated. Home-Applicable. Parent-Proven.
Evidence Grade: Level I–II
Systematic Reviews + RCTs + Meta-Analyses
PRISMA Systematic Review (2024)
16 studies (2013–2023): Sensory integration intervention meets criteria as evidence-based practice for children with ASD across sensory processing, motor, and adaptive behavior domains.
→ PMC11506176
Meta-Analysis, World Journal of Clinical Cases (2024)
24 studies confirming sensory integration therapy effectively promotes sensory processing, adaptive behavior, and self-care skills.
→ PMC10955541 | DOI: 10.12998/wjcc.v12.i7.1260
Indian RCT — Indian Journal of Pediatrics (2019)
Home-based sensory interventions for Indian children demonstrated significant outcomes in sensory tolerance and daily living skills.
→ DOI: 10.1007/s12098-018-2747-4 (Padmanabha et al.)
NCAEP Evidence-Based Practices Report (2020)
Visual supports and structured routines classified as evidence-based practices for autism — directly supporting timer and schedule use in hair washing protocols.
Key Finding: Sensory-based material interventions combined with graduated exposure, child control, and predictability supports produce measurable improvement in grooming tolerance within 8–12 weeks of consistent implementation.

The Calm Hair Wash Toolkit — What It Is
Formal Technique Identity
Formal Name: Sensory-Modified Hair Washing with Material Scaffolding
Parent-Friendly Name: The Calm Hair Wash Toolkit
Series: E-536 | Self-Care Independence
Age Range: 2–12 years
Frequency: 2–3x per week
Session Duration: 5–15 minutes
What This Technique Does
Sensory-Modified Hair Washing is an occupational therapy framework that uses 9 targeted materials to systematically remove, reduce, or reframe the sensory triggers that cause hair washing distress. Unlike "push through and hope" approaches, this technique modifies the sensory input at the source — eliminating face water contact, providing child-controlled tools, and building predictability through visual supports.
The goal is not perfection. The goal is progressive tolerance — moving from "cannot tolerate any hair washing" to "tolerates hair washing with minimal support" over 8–12 weeks.
Shampoo Rinse Cup with Soft Silicone Edge
Shampoo Visor or Halo Shield
Dry Washcloth for Face Protection
Handheld Shower Head with Adjustable Flow
Tear-Free and Sensory-Friendly Shampoo
Bath Toys and Distraction Items
Visual Timer for Predictable Duration
Warm Towel or Robe for Immediate Comfort
Social Story or Visual Schedule for Hair Washing

The Consortium Behind This Technique
"The brain doesn't organize by therapy type. Hair washing touches sensory processing, behavior, communication, and development simultaneously. Every discipline has a role."
Occupational Therapist (OT) — Primary Lead
Designs the sensory modification protocol. Selects tools based on the child's tactile defensiveness profile. Runs desensitization sessions.
ABA / BCBA Therapist
Structures reinforcement schedules for each successful hair washing attempt. Designs token economy or reward systems. Provides data collection frameworks.
Special Education Specialist
Creates the social story with appropriate literacy level and visual supports. Trains parents in visual support implementation.
NeuroDevelopmental Pediatrician
Rules out co-occurring conditions. Determines whether pharmaceutical support is warranted. Provides medical clearance for home implementation.
Pediatric SLP
Supports language strategies during washing — counting words, simple instruction sequences, emotional vocabulary to validate the child's experience.
Adapted UNICEF/WHO Nurturing Care Framework for SLPs (2022) | DOI: 10.1080/17549507.2022.2141327
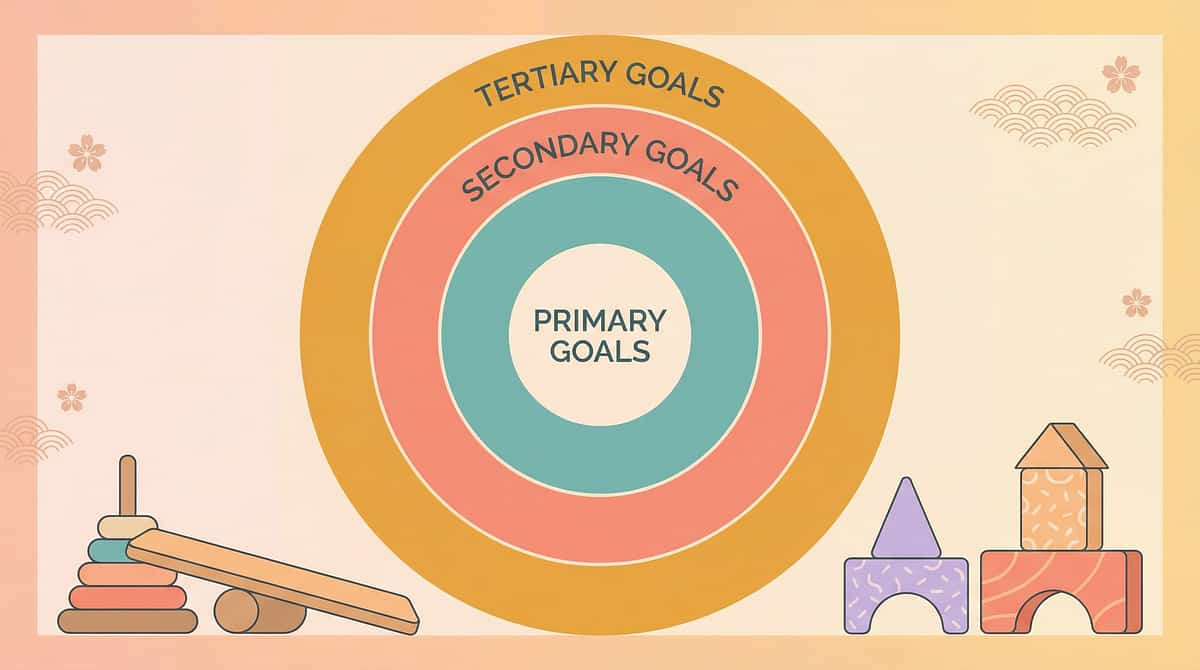
This Isn't a Random Activity. It's a Precision Tool.
Every element of the Calm Hair Wash Toolkit is aimed at a specific, measurable outcome. Understanding what you're targeting helps you know when it's working.
Primary Target
Water/Touch Tolerance During Grooming: Child can complete hair washing with less than 2 minutes of active distress. Hair is washed at full hygiene frequency (2–3x per week).
Secondary & Tertiary Targets
Anticipatory Anxiety: Child transitions to bathroom without meltdown when hair washing is announced.
Child Agency: Child participates in selecting tools, controlling water direction, or holding protective equipment.
Long-term: Child progresses toward self-administered hair washing by age 8–10.
Meta-analysis (World J Clin Cases, 2024): Sensory integration therapy promoted social, adaptive behavior, sensory processing, and motor skills across 24 studies. | PMC10955541

Your Hair Washing Toolkit — Shop in 3 Clicks
Every material is available today. Starter kit estimated at ₹500–800.

Material 1: Shampoo Rinse Cup with Soft Silicone Edge
Category: Self-Care Tools / Sensory Bathing Equipment
Price Range: ₹200–500
⭐ Look for cups with a wide, flexible silicone edge that creates a forehead seal. Search: "shampoo rinse cup silicone edge baby" on Amazon.in

Material 2: Shampoo Visor / Halo Shield
Category: Self-Care Tools / Head Protection
Price Range: ₹150–400
⭐ Adjustable band for secure fit without pressure. Search: "shampoo visor baby children" on Amazon.in

Material 3: Soft Washcloth (Child-Chosen)
Category: Sensory Comfort Materials / Soft Textiles
Price Range: ₹50–150
⭐ Let child choose color — ownership increases cooperation. Search: "soft washcloth baby cotton" on Amazon.in

Material 4: Handheld Shower Head with Adjustable Flow
Category: Bathroom Modification Equipment
Price Range: ₹500–1,500
⭐ Choose models with "gentle rain" and "mist" settings. Search: "handheld shower head adjustable flow" on Amazon.in
Material 5: Tear-Free Sensory-Friendly Shampoo
Category: Sensory Products / Personal Care
Price Range: ₹150–400
⭐ Fragrance-free or child-approved scent only. Search: "tear free shampoo children fragrance free" on Amazon.in

Your Hair Washing Toolkit — Materials 6–9

Material 6: Visual Timer (Sand or Digital)
Category: Visual Supports / Transition Tools
Price Range: ₹200–800
⭐ Also available via Pinnacle Recommends: Reinforcement / Reward Item (₹589) | Transition Object (₹425). Search: "visual timer sand hourglass children" on Amazon.in
Material 7: Bath Toys (Engagement / Distraction)
Category: Play Materials / Bath Time
Price Range: ₹100–800
⭐ Engagement and distraction principle drives the therapeutic effect. Search: "bath toys children waterproof" on Amazon.in
Material 8: Warm Hooded Towel or Soft Bathrobe
Category: Sensory Comfort Materials / Post-Activity Soothing
Price Range: ₹200–600
⭐ Immediate warmth is the reward the brain remembers. Search: "hooded bath towel children soft" on Amazon.in

Material 9: Social Story Materials (Blank Book / Printed Cards)
Category: Visual Supports / Social Stories
Price Range: ₹100–300 (or free — print at home)
Starter Kit Recommendation (₹500–800 total):✅ Rinse Cup with Silicone Edge + Visual Timer + Warm Towel = Immediate results for most children

Every Family Can Do This — Including Yours, Today
WHO/UNICEF Equity Principle: No child should miss therapy because of a postal code or a price tag.
Material | Buy It | Make / Substitute It | Why It Works | |
Rinse Cup | Silicone-edged rinse cup ₹200–500 | Soft plastic cup + fold a strip of wet chamois leather along the rim | The soft rim principle is the same — prevent face contact | |
Shampoo Visor | Adjustable visor ₹150–400 | Cut the brim off a soft sun hat; sew to fit securely | Creates same physical water barrier | |
Washcloth | Any soft washcloth ₹50–150 | Old soft cotton t-shirt cut into a square | Same tactile-comfort protection principle | |
Handheld Shower | ₹500–1,500 | Soft squeeze bottle with small holes in cap | Child-controlled water flow at low pressure | |
Tear-Free Shampoo | Branded product ₹150–400 | Baby shampoo (most are tear-free by default) | Same no-sting principle | |
Visual Timer | Sand/digital timer ₹200–800 | Sand in a clear bottle or phone timer with visible screen | Same predictability — child can see time passing | |
Warm Towel | Hooded towel ₹200–600 | Regular towel warmed on a radiator or in dryer for 3 minutes | Same warmth and pressure comfort | |
Social Story | Printed cards ₹100–300 | Hand-drawn stick figures on paper; phone photos of your bathroom | Personalized = more effective; your child's own bathroom is the best image |
Zero-Cost Version: Squeeze bottle + old soft washcloth + phone timer + hand-drawn schedule cards = ₹0 complete toolkit
WHO NCF (2018): Equity-focused interventions using household materials. CCD Package implemented across 54 LMICs. | PMC9978394

Read This Before You Start. Every Time.
🔴 RED — STOP. Do Not Proceed
- Child is visibly ill, feverish, or in active meltdown before entering bathroom
- There are open wounds, skin infections, or ear tubes (consult OT/pediatrician first)
- Child has recently had a seizure or shows signs of post-ictal state
- You are emotionally dysregulated yourself — children read parent anxiety and it amplifies theirs
🟡 AMBER — MODIFY. Proceed with Adaptation
- Child slept poorly and is dysregulated but not in crisis → Shorten session to 60-second rinse only
- Child is hungry → Feed first; hair washing on empty stomach intensifies sensory sensitivity
- Child showing pre-meltdown signs → Begin cool-down activities before bath
- Missing rinse cup or visor → Use washcloth method only; skip full rinse if needed
🟢 GREEN — PROCEED
- Child is fed, rested, and in a regulated state
- All materials within arm's reach before bath begins
- Water temperature tested and confirmed comfortable (inner wrist test)
- You have 15 minutes of unhurried time and a warm towel ready
STOP IF YOU SEE: Breath-holding for more than 3 seconds, child turns blue around lips, vomiting, child goes limp or non-responsive, injury from thrashing. Stop immediately and comfort before any continuation.
📞Emergency Helpline: 9100 181 181
Indian Journal of Pediatrics RCT (2019): Safety protocols for parent-administered home sensory interventions. | DOI: 10.1007/s12098-018-2747-4
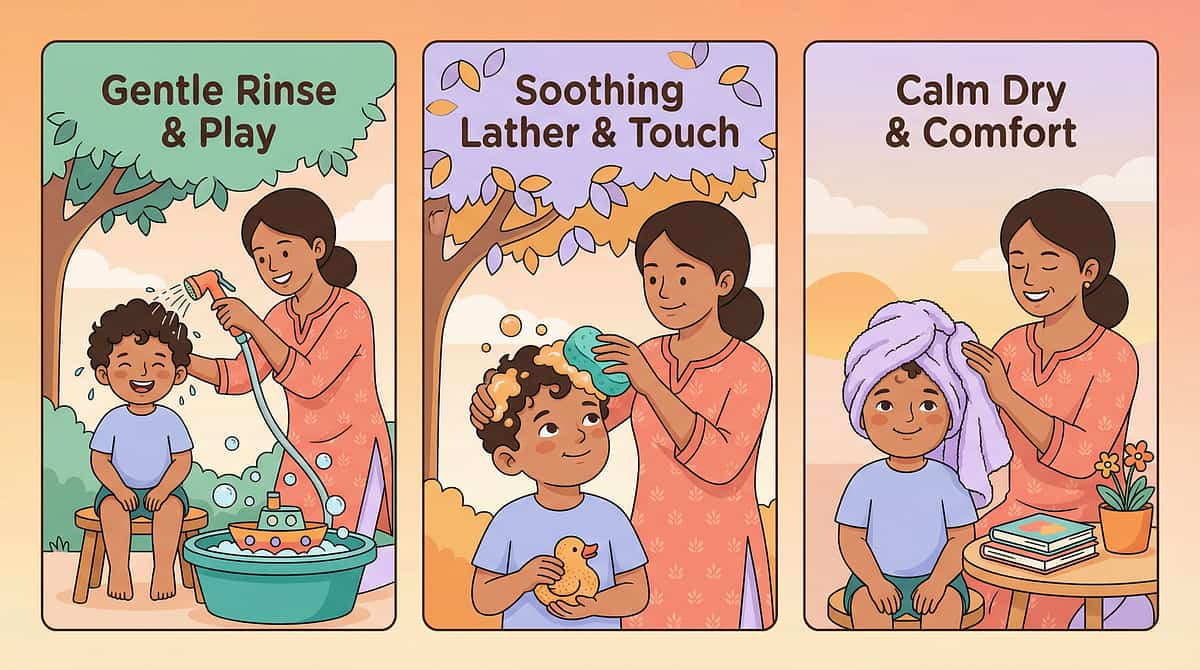
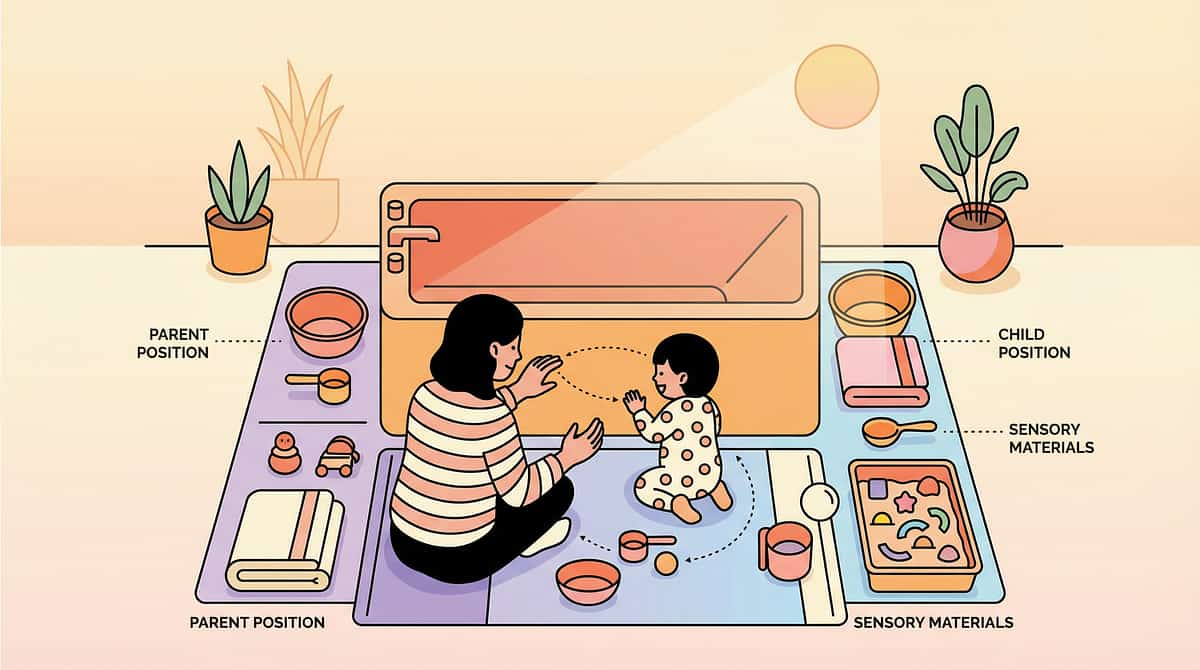
The Right Setup Makes the Technique. Wrong Setup Breaks It.
Bathroom Setup Checklist
- Visual schedule posted at child eye-level (before bath begins)
- Timer positioned where child can see it from tub
- All materials within arm's reach of parent (rinse cup, shampoo, washcloth, toys)
- Warm towel on hook, visible to child ("It's waiting for you")
- Parent kneels or sits — never stands looming over child
- Water running to temperature BEFORE child enters bathroom
- Bathroom door closed (reduces noise distraction and temperature drop)
Remove From the Space
- Harsh fluorescent lighting (use warm bulb or lamp if possible)
- Siblings who will distract or escalate
- Your phone (unless using as timer — position on ledge, not in hand)
- Any toys the child might grab and refuse to relinquish
Sensory Environment
- Lighting: Warm, dim is better than bright overhead
- Sound: Soft music or white noise can help; no sudden loud sounds
- Temperature: Bathroom pre-warmed; water confirmed comfortable before child enters
Sensory Integration Theory (Ayres): Environmental setup is a core treatment principle. Structured environment + 1:1 individual treatment maximally effective. | PMC10955541

60 Seconds. Before Every Session.
"The best session is one that starts right."
Icon | Indicator | Status | If NO | |
🍽️ | Child ate a full meal in last 2 hours | ✅ / ❌ | Feed first — 20 min minimum | |
😴 | Child had adequate sleep last night | ✅ / ❌ | Shorten session significantly | |
🧘 | Child is in regulated state (not in meltdown) | ✅ / ❌ | 10 min calm activity first | |
⏱ | You have 15 uninterrupted minutes | ✅ / ❌ | Postpone to later | |
🌡️ | No signs of illness/fever | ✅ / ❌ | Postpone to next day | |
💊 | Medications given if typically prescribed | ✅ / ❌ | Follow medical guidance | |
🧸 | Transition object available | ✅ / ❌ | Grab before entering |
🟢 ALL GREEN → PROCEED
Move to full protocol (Steps 1–6)
🟡 2–3 AMBER → MODIFY
Use rinse cup/visor only. Timer set to 30 seconds. End at first sign of escalation. Maximum distraction from start.
🔴 ANY RED → POSTPONE
5 minutes high-preference activity, then revisit tomorrow. Document reason. Consistency beats frequency.
"Session abandonment is not failure. It's the smartest thing you can do for next session."

Step 1 of 6
⏱ 30–60 Seconds
The Invitation
The Opening Script (Exact Words)
"Okay [child's name], I've got your special hair washing stuff ready. Want to come see the [rinse cup / visor / timer]? You're in charge of [the cup / holding the washcloth / watching the timer] today."
Why This Works
Every session begins with an INVITATION, not a command. The child is given a role (not a directive). The language previews the tools they will control. This activates motivation before demand.
Body Language
- Crouch or kneel to child's eye level
- Relaxed, open posture (no crossed arms)
- Calm, warm vocal tone — your nervous system is contagious
- Hold up the rinse cup or timer as a visual prompt
Reading the Response
Acceptance Cues: Child looks at you, moves toward bathroom, touches the material, asks a question about it.
Resistance Signals: Turns away, screams "NO", runs. Response: "Okay, let's come back in 5 minutes. I'm going to set the cup on the bath for when you're ready."
ABA Pairing Procedures: Establishing motivating operations before demand placement. OT "Just-Right Challenge" principle.

Step 2 of 6
⏱ 1–3 Minutes
The Engagement
Material Introduction Script
"Here's the rinse cup. See the soft edge? Watch — it's going to make a seal on your forehead and the water goes BACK over your hair, not on your face. Want to try it on your arm first?"
How to Present
- Demonstrate on your own arm or head first
- Offer the material for the child to TOUCH before it touches them
- Describe what will happen before it happens: "I'm going to put this cup against your forehead now — it'll feel soft, like this"
- Start with the least threatening material (usually the washcloth the child holds)
Child Response Indicators
Engagement: Reaches for material, asks questions, tries it on arm.
Tolerance: Doesn't resist; passive but not distressed.
Avoidance: Pushes material away, looks away, escalates.
Reinforcement Cue
The moment child TOUCHES the material voluntarily → "Yes! You touched it! That's brilliant." This is the most important moment in the session.
PMC11506176: Structured material introduction meets evidence-based practice criteria.

Step 3 of 6
⏱ Core Washing Sequence
The Therapeutic Action
Phase A: Face Protection First (Non-Negotiable)
Before any water, face protection is in place. Option 1: Rinse cup pressed to forehead — confirm seal. Option 2: Shampoo visor on head — confirm fit. Option 3: Child holds dry washcloth firmly over eyes.
"Your face is protected. Water cannot reach you. Ready?"
Phase B: Shampoo Application
Warm shampoo in hands first (30 seconds in palms). Apply to hair only — not directly to scalp. Gentle, predictable strokes — announce each: "I'm moving to the back of your head now." Use minimum amount → minimum rinse time needed.
Phase C: Rinse — The Highest-Distress Phase
Set visual timer BEFORE pouring. "Watch the timer. When the red is gone, we're done. Ready? 30 seconds." First pour: at back of head, away from face entirely. Slow, steady stream — not sudden pour. If child holds handheld shower: let THEM direct the water. End at timer — always, even if not perfect.
Duration Progression
Start at 20–30 seconds of rinsing. Build by 10 seconds per week as tolerance grows.
Child Response Spectrum
Ideal: Calm, watching timer, no face water contact achieved.
Acceptable: Mild protest but completion; face protection held throughout.
Concerning: Face protection fails and water reaches face → Stop, dry face immediately, reassure.
PMC10955541: Home sessions 10–20 minutes. Core therapeutic action: 40–60% of session.
Step 4 of 6
⏱ 3–5 Minutes Total
Repeat and Vary
1
Week 1–2
1 rinse cycle of 20–30 seconds. Maximum child support. Cup or visor required.
2
Week 3–4
1–2 rinse cycles of 30–45 seconds. Child begins choosing between cup and visor.
3
Week 5–8
Full wash + 2 rinse cycles of 45–60 seconds each. Child controls handheld shower for final rinse.
Variation Options to Maintain Engagement
- Switch between rinse cup and visor across sessions (child chooses)
- Let child pour the FIRST cup of water themselves (onto back of head)
- Change the bath toy or video each session
- Count out loud together: "1...2...3...4...5 — halfway!"
- Let child control the handheld shower for the final rinse
Satiation Indicators — Child Has Had Enough
- Sustained crying for more than 60 seconds
- Asking repeatedly to stop
- Covering materials or pulling at parent's hands
- Escalating from distress to aggression
"3 good repetitions are worth more than 10 forced ones. End on a calm note every time."
SI therapy dosage: 2–3 sessions/week, 8–12 weeks typical protocol. | PMC10955541

Step 5 of 6
⏱ Immediately After Last Rinse
Reinforce and Celebrate
Reinforcement Script — Within 3 Seconds
"[Child's name]! You DID it! Your hair is clean — you're amazing! You watched the timer all the way down. That was SO brave."
Reinforcement Timing Principle
- Immediate (within 3 seconds) beats Delayed (5 minutes later)
- Specific ("You held the washcloth the whole time!") beats Generic ("Good job!")
- Enthusiastic tone matters — match your energy to the achievement
Reinforcement Menu Options
- Access to high-preference activity (screen time, favorite toy)
- Sensory reward (warm towel wrap, back rub)
- Social reward: "You choose tonight's bedtime story!"
Celebrate the Attempt, Not Just the Success
"You got IN the tub and you held the washcloth. That's real progress. We'll do the timer again next time."
If your child uses a token board: award 1–3 tokens immediately after rinse completion. These accumulate toward a chosen reinforcer. Token economy shows strong evidence in autism intervention.
ABA Reinforcement Principles: Immediate, specific reinforcement. Token economy: multiple systematic reviews. BACB ethical guidelines.

Step 6 of 6
⏱ 1–2 Minutes
The Cool-Down
"Two more seconds of water, then ALL DONE. Watch the timer — almost there..."
Immediate Post-Rinse Sequence
- Wrap in warm towel immediately — this is the reward the brain remembers
- Say: "All done. Hard part is over. Here's your warm cozy towel."
- Press towel gently around head — deep pressure is calming
- Let child sit or stand — do not rush drying
Cool-Down Activity (1–2 Minutes)
- Deep pressure back rub with towel while drying
- Child's favorite sensory activity immediately after
- Quiet music + warm wrap sitting together
- Naming the accomplishment: "Tell me one thing you did today"
Material Put-Away Ritual
If child is able: involve them in putting rinse cup/visor back on shelf. Creates ownership and signals the transition to play time is FULLY complete.
If Child Resists Ending
"Bath is all done. The water is off. Your towel is here. All done." Use visual schedule to point to: [bath picture] → [towel picture] → [play picture]
NCAEP (2020): Visual supports and transition cues are evidence-based practices for autism. Structured transition reduces post-session dysregulation.

60 Seconds of Data Now. Hours of Clarity Later.
"Within 60 seconds of ending the session, record these 3 things. Don't trust your memory — trust your notes."
Field | What to Record | How | |
Session Duration | How many minutes/seconds did the full wash take? | Write the number | |
Distress Level | Rate child's peak distress: 1 (none) → 5 (severe meltdown) | Circle the number | |
Completion | Full wash ✅ / Partial (hair only, no full rinse) 🔶 / Abandoned ❌ | Check one |
Optional Bonus Data
- Which material worked best today?
- What triggered the most distress?
- Any new behavior (positive or concerning)?
Quick Data Template (Copy to WhatsApp or Notes App):
📋 E-536 Hair Wash Log
Date: ___ Duration: ___min Distress: /5 Complete: ✅🔶❌
Materials used: _____ Notes: _____
📋 E-536 Hair Wash Log
Date: ___ Duration: ___min Distress: /5 Complete: ✅🔶❌
Materials used: _____ Notes: _____
📞Helpline: 9100 181 181 — ask our team to help you set up your data tracking system
ABA Data Collection Standards: Continuous and discontinuous measurement as standard behavior-analytic practice. Cooper, Heron & Heward (Applied Behavior Analysis, 8th ed.)

The Technique Needs Adjustment. Not You.
"Most sessions don't go perfectly. Here are the 7 most common challenges — and what to do."
Problem 1: Child Refused to Enter the Bathroom
Why: Anticipatory anxiety has associated "bathroom" with distress.
Fix: Practice the social story at least 1 hour before bath. Enter bathroom together for non-bath activities to decouple "bathroom = bath time."
Fix: Practice the social story at least 1 hour before bath. Enter bathroom together for non-bath activities to decouple "bathroom = bath time."
Problem 2: Calm Until Rinsing Started, Then Full Meltdown
Why: Face water contact still occurring despite cup/visor, or duration exceeded tolerance threshold.
Fix: Check rinse cup seal. Reduce rinse time to 15 seconds. Add washcloth backup even when using cup. Let child HOLD the cup themselves.
Fix: Check rinse cup seal. Reduce rinse time to 15 seconds. Add washcloth backup even when using cup. Let child HOLD the cup themselves.
Problem 3: Won't Tolerate Anything on Their Head
Why: Head hypersensitivity extends to any object near/on head.
Fix: Desensitize to head touch separately during calm play. Try handheld shower controlled BY CHILD — they direct water away from face with nothing on their head.
Fix: Desensitize to head touch separately during calm play. Try handheld shower controlled BY CHILD — they direct water away from face with nothing on their head.
Problem 4: Distraction Isn't Working
Why: Anxiety has captured attention fully; distraction stimulus isn't engaging enough.
Fix: Upgrade to a MORE compelling distractor — child's absolute favorite video/show used ONLY during hair washing.
Fix: Upgrade to a MORE compelling distractor — child's absolute favorite video/show used ONLY during hair washing.
Problem 5: Timer Ended but Hair Still Has Shampoo
Why: Not enough time budgeted or too much shampoo used.
Fix: Use MINIMAL shampoo (marble-sized amount for short hair). Start timer after shampoo is worked in. Two short rinse sessions with a 30-second break beats one long one.
Fix: Use MINIMAL shampoo (marble-sized amount for short hair). Start timer after shampoo is worked in. Two short rinse sessions with a 30-second break beats one long one.
Problem 6: Warm Towel Trick Not Working
Why: Post-bath sensory overload — dripping water, cold air, wet hair sensation.
Fix: Have hooded towel cover wet hair IMMEDIATELY before child exits tub. Dry hair first. Consider hair dryer on COOL setting if tolerated.
Fix: Have hooded towel cover wet hair IMMEDIATELY before child exits tub. Dry hair first. Consider hair dryer on COOL setting if tolerated.
Problem 7: Progress Then Regression
Why: Normal. Regression occurs during illness, life transitions, schedule changes, or growth spurts.
Fix: Return to Week 1 protocol temporarily. Don't panic — regression is not starting over, it's a pause. Most regressions resolve within 1–2 weeks.
Fix: Return to Week 1 protocol temporarily. Don't panic — regression is not starting over, it's a pause. Most regressions resolve within 1–2 weeks.
"Session abandonment is not failure — it's data. What happened tells you exactly what to adjust."
📞Still stuck? Helpline: 9100 181 181
No Two Children Are Identical. Neither Is Their Toolkit.
Sensory AVOIDER (Over-Responsive)
- Start with cup/visor + washcloth TOGETHER (maximum protection)
- Extremely warm water (test carefully)
- Work quickly and efficiently; minimum handling
- Maximum distraction from start
- Extra long warm towel wrap after
Sensory SEEKER (Under-Responsive)
- Water play first, then transition into hair wash
- May prefer handheld shower they can control and play with
- Firmer scalp massage with fingers may actually be calming
- May need LESS time than expected once fear is addressed
Ages 2–4
Parent does everything. Child's only "job" is to hold the washcloth. Purely passive involvement. Focus on face protection and timer.
Ages 4–7
Child holds visor/cup/washcloth. Child watches timer. Child can pour ONE cup of water on own hair. Social story reviewed before.
Ages 7–12
Child progresses toward self-administered washing. Parent is supervisor, not operator. Child controls handheld shower. Timer managed by child.
Individualized intervention planning: Core principle across OT (sensory profile), ABA (function-based), SLP (communication profile).
Week 1–2: Small Wins. Real Wins.
15%
Progress Milestone
Week 1–2 baseline: Neural pathways beginning to form
What You WILL Likely See ✅
- Child enters bathroom with less anticipatory escalation (not zero — less)
- Face water contact reduced significantly with rinse cup/visor
- At least one session where timer completion achieved without full meltdown
- Child looks at or touches the rinse cup without immediate distress
What You Will NOT See Yet ❌
- Child requesting hair washing
- Zero distress during rinsing
- Independent participation
- Generalization to other bathing contexts
The Invisible Progress — Don't Miss This: The brain is forming a new association: "Hair washing → rinse cup → face is protected → I survived." This is happening even when the session was hard. Neural pathway formation is not visible in behavior in week 1. Trust the data.
"If your child tolerates the cup on their forehead for 3 seconds longer than last week — that is real, measurable neurological progress."
PMC11506176: Sensory integration outcomes emerge across 8–12 week timelines. Early-phase indicators: tolerance and participation, not mastery.

Week 3–4: The Brain Is Rewiring. Here's How You'll Know.
40%
Consolidation Phase
Week 3–4: Neural pathway forming; behavioral consolidation emerging
Consolidation Indicators — Watch for These
🔵 Child enters bathroom without needing to be carried or physically prompted on most days
🔵 Child picks up the rinse cup or positions visor themselves without being asked
🔵 Child completes 2 full timer cycles without full meltdown
🔵 Child begins asking questions about the tools ("Will the cup be there?") — anxiety is shifting from panic to curiosity
🔵 Post-bath distress reduces in duration — child calms faster after completion
Behavioral Change: Neural Pathway Forming. When a child begins to ANTICIPATE the tool rather than ANTICIPATE the distress — the amygdala threat response is beginning to de-link from hair washing. This is the moment OTs call "the shift."
When to Increase Intensity: If Week 3–4 shows consistent GREEN sessions → extend timer by 10 seconds. Add shampoo if not yet included.
"You may notice you're more confident too. Your calm energy is measurably changing the experience for your child."
Neuroplasticity: Synaptic strengthening through structured repeated input. Behavioral consolidation markers align with neural adaptation curves.
Week 5–8: You're Approaching Mastery. Here's What It Looks Like.
75%
Mastery Approach
Week 5–8: Observable mastery criteria being met on majority of sessions
🏆 Mastery Badge Unlock Criteria
Full Wash Tolerance
Child tolerates full hair washing (shampoo + complete rinse) with ONE protective tool (cup OR visor) and minimal verbal distress on 4 of 5 consecutive sessions
Timer to Completion
Child watches timer to completion without attempting to stop the rinse early on the majority of sessions
Post-Bath Recovery
Calm return to baseline occurs within 3 minutes of session end
Generalization
Child begins to tolerate water on head in other contexts — pool, rain — indicating neural transfer of safety learning
When to Stay and Strengthen: If child is at 3 of 5 successful sessions — stay 2 more weeks. Premature progression increases regression risk. Mastery here means readiness to progress to E-537: Getting Dressed Independently.
PMC10955541 + BACB mastery criteria standards: Specific, observable, measurable mastery criteria across 24 studies.

You Did This. Your Child Grew Because of Your Commitment.
Dear parent — Eight weeks ago, you were scratched, sobbed on, and exhausted after another bath time battle. You felt judged for your child's unwashed hair. You wondered if it would ever get better. It got better because you showed up.
You studied the tools. You prepared the space. You kept your voice calm even when the session was hard. You wrote down the data when you wanted to forget the whole thing. You came back the next session, and the one after that.
Your child's nervous system learned to feel safe during hair washing because you created the conditions for that safety — consistently, patiently, and with extraordinary love.
✅ Hair Washing Transformed
From distressing to tolerable
✅ Face Water Panic Reduced
Systematically and measurably
✅ Child Agency Gained
Your child now participates in their own grooming
✅ Toolkit That Works
You have the knowledge to adapt it for any challenge ahead
Family Celebration Suggestion: Let your child choose tonight's dinner. Frame it: "You worked SO hard on hair washing. You've earned this choice."
📞Share your story: 9100 181 181 |care@pinnacleblooms.org

Even in the Win Zone — Know These Signs.
"Trust your instincts. If something feels wrong, pause and ask."
🔴 Red Flag 1: Distress INCREASING After 4+ Weeks
Sessions getting harder, not easier. Meltdowns more severe and frequent. May indicate the sensory processing challenge is more complex than a home protocol can address alone — or there's an undiagnosed anxiety component. Action: Pause home sessions. Book OT assessment immediately.
🔴 Red Flag 2: Child Is Self-Injuring
Head-banging, biting self, scratching self during rinse. Action: Stop session immediately. Contact Pinnacle: 9100 181 181 for same-day guidance.
🔴 Red Flag 3: Avoidance Spreading to Other Water Contexts
Child now avoids face washing, teeth brushing, hand washing. Action: Professional OT sensory profile assessment needed. Don't expand home protocol without guidance.
🔴 Red Flag 4: Regression After Illness Lasting 2+ Weeks
Returns to Week 1 behavior and stays there after recovering from illness. Action: Resume Week 1 protocol + teleconsult to reassess approach.
🔴 Red Flag 5: Parent-Child Relationship Deteriorating
Bath time is creating fear, resentment, or avoidance of the parent generally. This is the most important red flag. Action: Immediately pause. Contact helpline.
Escalation Pathway: Self-monitor → 9100 181 181 teleconsult → Nearest Pinnacle center assessment → Full sensory integration program
📞Emergency: 9100 181 181 (24x7 | FREE)
WHO NCF: Primary healthcare as platform for early identification. Referral pathways integrated into service delivery models.
You're Not Done. You're on a Journey.
Hair washing mastery is one milestone in the Self-Care Independence arc — a 6-milestone journey from dependent to independent grooming by age 10–12.
Long-Term Developmental Goal: By age 10–12, independently complete the full morning hygiene routine without parental assistance — enabling social participation, school independence, and self-esteem.
Connected Domains: Hair washing tolerance connects directly to Domain A (Sensory Processing — the root cause), Domain C (Emotional Regulation — managing anxiety), Domain D (Behavior — compliance with routine demands), and Domain K (Life Skills — long-term independent living preparedness).
Other Techniques in the Self-Care Series
"You may already own materials for some of these — your toolkit transfers."
Technique | Code | Difficulty | Materials You Already Have | |
9 Materials for Hair Brushing | E-530 | 🟢 Intro | Soft washcloth ✅ | |
9 Materials for Haircut Preparation | E-531 | 🟡 Core | Visual timer ✅, social story ✅ | |
9 Materials for Hair Brushing Meltdowns | A-010 | 🟢 Intro | Distraction items ✅ | |
9 Materials for Face Washing Sensitivity | E-534 | 🟢 Intro | Rinse cup ✅, washcloth ✅ | |
9 Materials for Teeth Brushing | E-535 | 🟡 Core | Timer ✅, social story ✅ | |
9 Materials for Nail Trimming Tolerance | E-538 | 🟡 Core | Social story ✅, reward items ✅ |
Domain E — Self-Care & Grooming Independence
Organization follows Pinnacle 128 Canon Materials taxonomy + 20 Category classification system + 999 Reels Master.

This Technique Is One Piece of a Larger Plan.
Connected Domains
Hair washing tolerance connects directly to:
- Domain A (Sensory): The sensory processing difference is the root cause
- Domain C (Emotional Regulation): Managing anxiety and distress before/during bath
- Domain D (Behavior): Compliance with routine demands
- Domain K (Life Skills): Long-term independent living preparedness
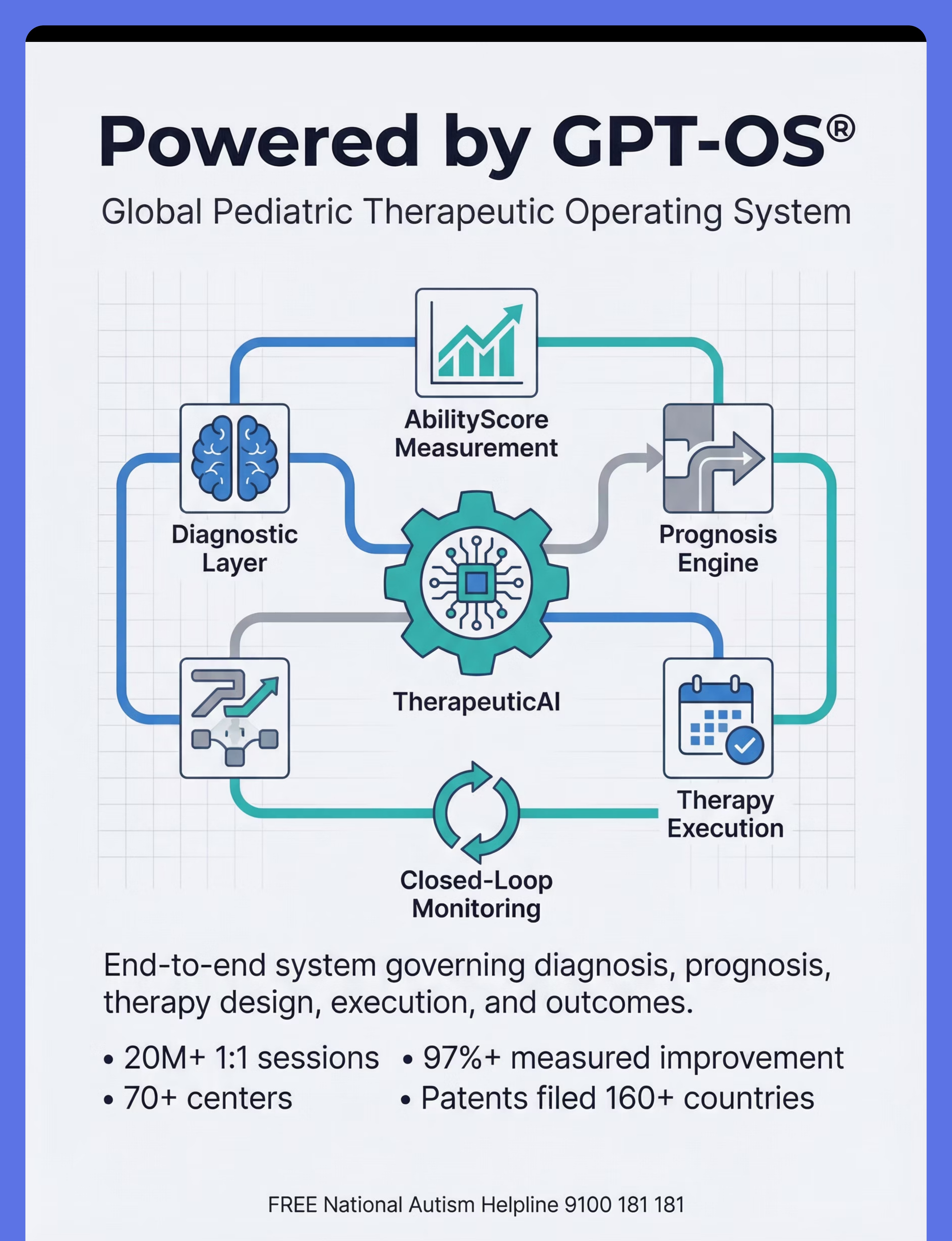
GPT-OS® Full Profile
When your child is enrolled in GPT-OS®, this technique is automatically tracked within their personalized developmental plan across all 12 domains. Progress here updates their AbilityScore® and adjusts future technique recommendations.
WHO/UNICEF Nurturing Care Framework: Five components of nurturing care require holistic developmental monitoring. UNICEF 2025 Country Profiles: 42 indicators per country.

From the Families. For the Families.
These are clinical narratives from Pinnacle Network families. Names changed. Behavioral details preserved.
Arjun, 6 years, Hyderabad
Before: "Bath time was 45 minutes of war. He'd start crying when he heard the water running from the next room. Hair washing took two people — one to hold him, one to wash. We were skipping it for 10 days at a time."
Approach: Started with rinse cup + washcloth. Shampoo visor introduced Week 3. Timer from Day 1.
After (Week 8): "He's not perfectly calm. But he gets in the tub, holds the cup himself, and watches the timer. It takes 8 minutes. Both of us aren't crying afterward. That's everything."
OT Notes: "Arjun's breakthrough came when he realized he controlled the cup. The shift from 'this is being done to me' to 'I am doing this' is the pivotal therapeutic moment."
Priya, 4 years, Bangalore
Before: "She would become so distressed that she'd vomit during hair washing. We went to dry shampoo for 3 months just to get through."
Approach: Dry shampoo maintained while trust rebuilt. Rinse cup introduced Week 4 only on hair sides (not crown). Timer: 10 seconds to start.
After (Week 10): "She asks for her 'magic cup' before bath. She says 'timer on' herself. She still doesn't love it. But she does it. Every three days. Without vomiting."
OT Notes: "Priya needed the slowest possible graduated approach. The dry shampoo bridge was essential — there was no shortcut."
Karthik, 9 years, Chennai
Before: "A 9-year-old having meltdowns about hair washing. I felt ashamed. Other parents thought I was making it up or that we were dirty."
Approach: Social story created first (photos of his bathroom, his tools). Handheld shower given to him to hold — he directed all water. Full autonomy within the process.
After (Week 6): "He washes his own hair now. 100%. He uses the handheld shower. He sets the timer on his phone. The first time he did it completely alone, I cried in the hallway."
📞Share your story: 9100 181 181

You Are Not the Only Parent Fighting This Battle.
Isolation is the enemy of adherence. Community is the accelerant.
Join the Community
→ WhatsApp: Pinnacle Self-Care Parents Circle — Request Link via 9100 181 181
Topics: Self-Care Challenges | Bath Time Battles | Sensory Grooming
Local Pinnacle Parent Meetups
Your nearest Pinnacle center hosts monthly Parent Circles where caregivers share strategies, troubleshoot challenges, and celebrate milestones together. All meetups include a therapist facilitator.
Peer Mentoring
"I was where you are. Now I can help."
Pinnacle's Peer Mentor Program connects newly-struggling parents with experienced parents who have navigated the same challenges. All peer mentors are trained and supervised by Pinnacle therapists.
→ Request a peer mentor: 9100 181 181
Your Experience Helps Others
"Consider sharing your journey once you've made progress. Your story may be the thing that keeps another parent from giving up on bath night."
WHO NCF: Community engagement as core principle. Over 1,000 individuals from 111 countries contributed to the framework. Parent support networks improve intervention outcomes.

Home + Clinic = Maximum Impact.
Home-based intervention works best when powered by professional guidance. Pinnacle's 70+ centers and teleconsultation services bring specialist support to every family.
Occupational Therapist
Sensory processing assessment, desensitization protocol design, and direct sensory integration therapy.
→ Book OT Consultation: 9100 181 181
ABA / BCBA Therapist
Reinforcement program design, token economy, and session troubleshooting.
→ Book ABA Consultation: 9100 181 181
NeuroDev Pediatrician
Diagnostic clarity (ASD, SPD, ADHD) and medical safety clearance for home implementation.
→ Book Developmental Assessment: 9100 181 181
Teleconsultation
70% of Pinnacle's services are available via secure teleconsultation. You do not need to be near a physical center.
When a Pinnacle OT observes home bath time via teleconsultation video, they can identify specific sensory triggers, adjust the protocol in real-time, and train both parents simultaneously in one session. Pinnacle works with multiple insurance partners and government funding schemes.
📞FREE National Autism Helpline: 9100 181 181 | 24x7 | 16 Languages
WHO NCF Progress Report (2023): 48% increase in countries adopting ECD policies. | WHO NCF 2018–2023

For the Curious Parent Who Wants to Go Deeper.
PRISMA Systematic Review (2024)
"Sensory integration intervention as evidence-based practice for ASD: 16 studies, 2013–2023"
Meta-Analysis: World Journal of Clinical Cases (2024)
"Sensory integration therapy: 24 studies confirming promotion of adaptive behavior, sensory processing, and motor skills"
→ PMC10955541 | DOI: 10.12998/wjcc.v12.i7.1260
Indian RCT: Indian Journal of Pediatrics (2019)
"Home-based sensory interventions for Indian children: significant outcomes in daily living and sensory tolerance"
→ DOI: 10.1007/s12098-018-2747-4 | Padmanabha et al.
WHO Nurturing Care Framework (2018)
"Evidence-based caregiving practices implemented across 54 LMICs; household-material interventions validated"
→ nurturing-care.org | PMC9978394
NCAEP Evidence-Based Practices Report (2020)
"Visual supports and structured routines as evidence-based practices for autism"
Frontiers in Integrative Neuroscience (2020)
"Neurological basis for sensory-based interventions: somatosensory cortex and amygdala mechanisms"
→ DOI: 10.3389/fnint.2020.556660

Your Data Is a Contribution to Every Child Like Yours.
You Record Session Data
GPT-OS Processes Patterns
Your Child Gets Better
Population-Level Insight
What GPT-OS® Learns from E-536 Data
- Which combination of materials (cup + timer vs. cup + distraction) produces fastest tolerance gains
- At what week families experience the consolidation shift
- Which child sensory profiles respond best to which material sequence
- What regression triggers are most common and how to prevent them
What It Does NOT Collect
- Names, addresses, or personally identifiable information without explicit consent
- Video or audio without consent
- Any data beyond what you choose to enter
Privacy Assurance
All data processed under India's Digital Personal Data Protection Act 2023. Data stored on India-sovereign servers. DPIIT recognized startup (DIPP8651).
"Your data helps every child like yours." Every E-536 tracking record you submit makes the next version of GPT-OS® smarter — and makes the next family more likely to get the right tool in the right order on the first try.
📞9100 181 181 | pinnacleblooms.org

See the Materials in Action
E-536
Series: Toileting & Self-Care Independence
Episode 536
Reel Identity: E-536: 9 Materials That Help With Hair Washing | Domain: E — Self-Care | Format: 9-Material Showcase (75–85 seconds)
→ Watch on YouTube/Pinnacle Platform: E-536 — 9 Materials That Help With Hair Washing
"In this reel, I demonstrate all 9 materials in a real bath setting. You can see exactly how the silicone-edge cup creates the forehead seal, how the child holds the washcloth, and how the timer is positioned. Watch it before your first session." — Pinnacle OT Specialist, Sensory Processing Domain
Connected Reels in This Series
- A-010: Hair Brushing Meltdowns | A-018: Child Refuses Haircuts
- E-530: Hair Brushing | E-531: Haircut Preparation | E-538: Nail Trimming Tolerance
NCAEP (2020): Video modeling is evidence-based practice for autism. Multi-modal learning improves parent skill acquisition.

Consistency Across Caregivers Multiplies Impact. 5x.
If only one adult in your child's life knows this technique — it's limited. If every caregiver knows it — it transforms.
📱 Share Instantly
Share via WhatsApp | Share via Email | Copy Link
📄 Download Resources
E-536 Family Guide — One Page, All 9 Materials (PDF) | Hair Washing Visual Schedule — Print & Laminate | 8-Week Progress Tracker (PDF)
Explain to Grandparents — Simplified Version
"[Child's name] has a special way to wash hair that their therapist recommended. (1) Use the special cup with the soft edge — it keeps water off their face. (2) Set the timer before starting — they watch it the whole time. (3) Wrap them in the warm towel the moment you finish. That's it. Please don't change the routine — consistency is how they learn."
Teacher / School Communication Template
"[Child's name] is working with a Pinnacle OT on hair washing tolerance (Program Code: E-536). Key supports: visual schedules, predictable routines, face protection tools. Please contact us if you observe grooming-related distress at school."
📞Helpline: 9100 181 181
WHO CCD Package: Multi-caregiver training is critical for intervention generalization and maintenance. | PMC9978394

Your Questions. Clinical Answers.
Q1: How often should we do hair washing sessions?
A: 2–3 times per week is the therapeutic sweet spot. More frequent is not more effective; less frequent delays neural pathway formation. Even during the hardest early weeks, maintain the 2–3x frequency. Consistency drives the sensory learning.
Q2: My child is 10 years old — is it too late for this to work?
A: No. Neuroplasticity is present throughout childhood and adolescence. Older children (7–12) often progress faster because they have better language to participate in the social story and can hold the handheld shower themselves. Age 10 is not late — it is an opportunity.
Q3: Do we have to use all 9 materials, or can we start with one?
A: Start with what addresses your child's BIGGEST trigger. For most children: rinse cup + visual timer is the minimum effective combination. The rinse cup eliminates face water. The timer provides predictability. Add other materials as tolerance builds.
Q4: The rinse cup isn't creating a full seal. What am I doing wrong?
A: Press the cup's silicone edge FIRMLY against the forehead before tilting to pour. Position it before the pour begins — not mid-pour. Practice on yourself first. Practice on child outside the bath (dry) so they feel the correct pressure before it happens live.
Q5: My child hates the visual timer — it makes them more anxious.
A: Introduce the timer BEFORE bath during the social story review. If timer anxiety persists, switch to a sand hourglass — less "countdown" feel, more visual flow. Or use verbal counting (1–20) instead of a physical timer.
Q6: Should we wash hair every day while desensitizing?
A: Reduce to 2–3x per week MAXIMUM. Daily washing extends the sensory challenge and prevents tolerance from consolidating. Dry shampoo can bridge hygiene on off-days.
Q7: My child has both hair washing AND face washing problems.
A: Work on one at a time. Hair washing first (higher hygiene necessity). The tools you develop — rinse cup, visual timer, social story — directly transfer. Once hair washing mastery occurs (Week 6–8), face washing often becomes significantly easier.
Q8: Progress is very slow. Is something wrong?
A: Slow progress is still progress. The 8-week timeline is an average — many children take 12–16 weeks. What matters is DIRECTION: each week slightly better than the last. If you see plateau (no improvement for 3+ weeks), contact the helpline — a protocol adjustment is needed, not more time on the same approach.
Preview of 9 materials that help with hair washing Therapy Material
Below is a visual preview of 9 materials that help with hair washing therapy material. The pages shown help educators, therapists, and caregivers understand the structure and content of the resource before use. Materials should be used under appropriate professional guidance.


















Share this resource
Help others discover thisLink copied!

Bath time can be calm. Start this technique today.
"You have the knowledge. You have the tools. You have everything you need."
✅ Validated by the Pinnacle Blooms Consortium
🔵 OT | 🟣 ABA | 🟡 SpEd | 🟢 SLP | 🔴 NeuroDev
20M+ Sessions | 97%+ Improvement | 70+ Centers
📞 FREE National Autism Helpline
9100 181 181 | 24x7 | 16 Languages | No appointment needed
Pinnacle Blooms Network® | Built by Mothers. Engineered as a System.
OT | SLP | ABA/BCBA | SpEd | NeuroDev | CRO | Pediatrics | WHO-Aligned | UNICEF-Aligned | DPIIT Recognized
"From fear to mastery. One technique at a time."
This page is one of 70,000+ evidence-linked technique pages on the GPT-OS® platform — the world's largest structured pediatric intervention knowledge base. Every page is built to the same standard: PubMed-referenced, WHO/UNICEF-aligned, home-executable, and parent-empowering.
Medical Disclaimer:This content is educational. It does not replace individualized assessment and intervention planning with licensed occupational therapists and healthcare professionals. Persistent sensory sensitivities affecting daily bathing routines may indicate underlying conditions requiring professional evaluation. Individual results may vary. Statistics represent aggregate outcomes across the Pinnacle Blooms Network.
CIN: U74999TG2016PTC113063 | DPIIT: DIPP8651 | MSME: TS20F0009606 | GSTIN: 36AAGCB9722P1Z2
© 2025 Pinnacle Blooms Network®, unit of Bharath Healthcare Laboratories Pvt. Ltd. All rights reserved. | techniques.pinnacleblooms.org | pinnacleblooms.org | 9100 181 181
