
9 Materials That Help With Clumsiness
Trips over nothing, bumps into everything, drops things constantly — their body doesn't know where it is in space.
Motor Solutions Series — Episode 105
Proprioceptive Processing — Body Awareness
Ages 3–10 Years
"She walks into door frames like she doesn't see them. He knocks over his drink at every meal. She falls off chairs for no reason. He breaks things without meaning to. She's covered in bruises and we don't know how. Other kids call him clumsy — but it's constant, not occasional."

Understanding the Problem
They're Not Careless. Their Body Doesn't Know Where It Is.
If your child trips over nothing, bumps into everything, and drops things constantly — they're not being careless. Their brain isn't getting clear signals about where their body is in space. It's like navigating with a blurry map.
What Parents See
- Trips over nothing visible
- Bumps into walls and door frames
- Knocks things over at the table
- Falls off chairs — seemingly for no reason
- Covered in unexplained bruises
- Uses too much or too little force
What's Actually Happening
The proprioceptive system uses receptors in muscles, joints, and tendons to create a "body map" that guides movement. When this system is under-responsive or poorly integrated, the child genuinely doesn't know where their body is without looking — they use incorrect force, and struggle to plan movements through space.
This is neurological, not carelessness, laziness, or lack of attention.

Clinical Context
Understanding Proprioceptive Processing Differences
Clinical Terms: Proprioceptive Processing Differences / Developmental Coordination Disorder (DCD) / Dyspraxia
Clumsiness that goes beyond typical childhood unsteadiness often reflects differences in proprioceptive processing — the body's ability to sense where it is in space, how much force to use, and how to plan and execute movements.
Under-Responsive
Brain doesn't receive enough proprioceptive signal. Body map is weak or unclear. Child seeks heavy input — crashing, pushing, bumping.
Poor Discrimination
Brain receives signal but can't interpret it well. Body map is inaccurate. Child uses wrong force, misjudges distances, has clumsy fine motor skills.
Poor Integration
Proprioceptive info doesn't integrate with other senses. Worse when not looking at body. Poor motor planning and difficulty with novel movements.
DCD/Dyspraxia affects 5–6% of school-age children. It is not related to intelligence, vision, or muscle strength and frequently co-occurs with ADHD, autism, and specific learning disabilities.
Common Signs
Does This Sound Like Your Child?
Proprioceptive processing differences show up in many ways throughout daily life. Recognizing the pattern is the first step toward getting the right support.
At Home & Meals
- Knocks over drinks at every meal
- Falls off chairs or sits down too hard
- Slams doors without meaning to
- Breaks pencils writing
- Can't open jars or containers
- Covered in unexplained bruises
- Tires easily during physical activities
Moving Through Space
- Trips over nothing visible
- Bumps into furniture, walls, door frames
- Struggles with stairs or uneven surfaces
- Difficulty judging distances
- Seems unaware of body position without looking
- Doesn't notice obstacles in their path
Play & School
- Can't catch, throw, or kick a ball well
- Avoids playground equipment and sports
- Difficulty learning new motor skills
- May lean on things or move constantly
- Seeks intense crashing or jumping
- Difficulty learning to ride a bike or swim
Remember: This is not carelessness. The child genuinely does not receive accurate information about where their body is in space. They are often as surprised as you are when they trip or knock something over.

9 Materials That Sharpen the Body Map
Here are 9 evidence-informed materials that provide the proprioceptive input needed to help your child's brain build a clearer, more accurate body map — reducing the tripping, bumping, and dropping over time.
Weighted Blanket / Lap Pad
Deep pressure wakes up the body map
Therapy Ball
Unstable surface trains body awareness
Crash Pad / Crash Mat
Safe crashing delivers big body input
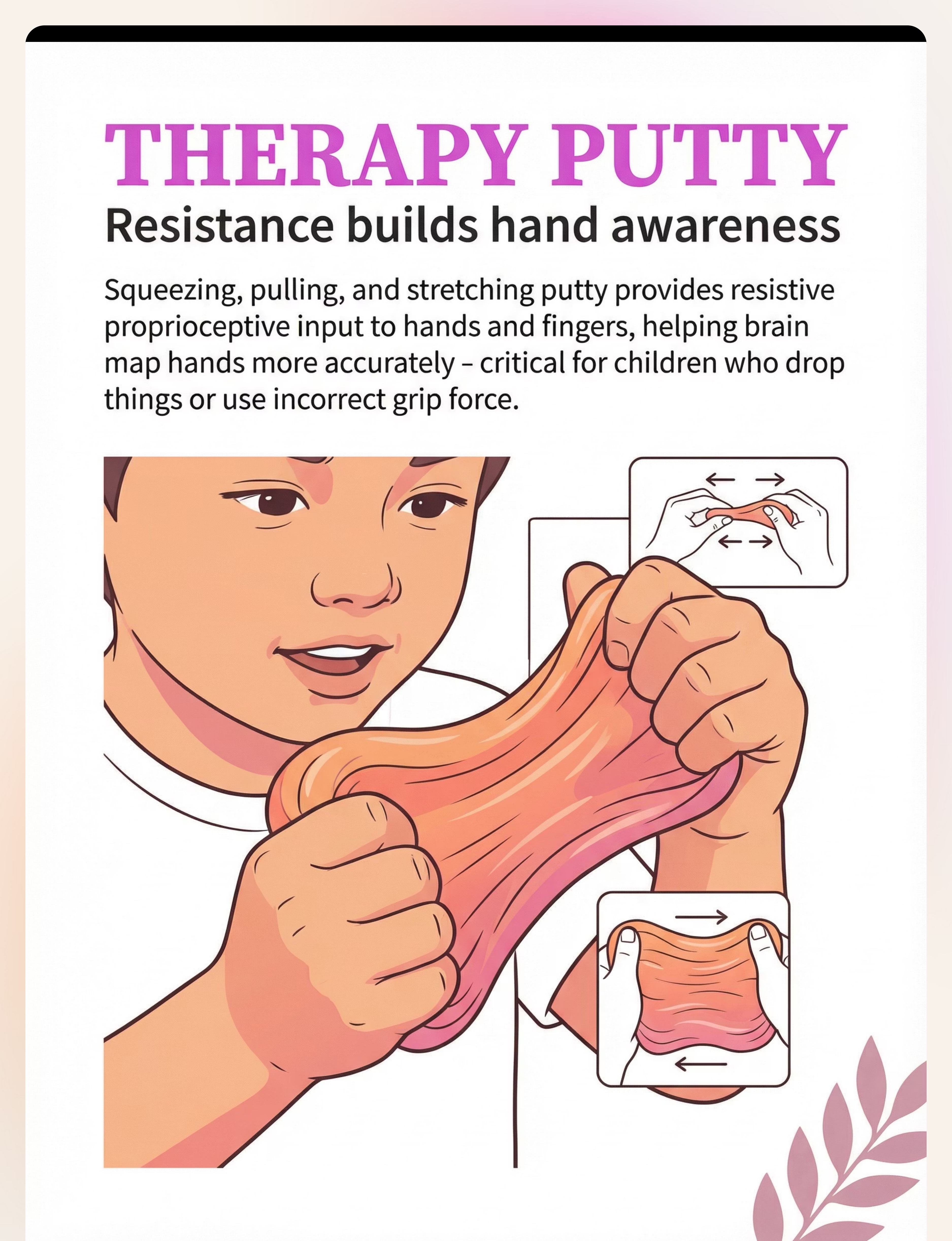
Therapy Putty
Resistance builds hand awareness
Body Sock / Resistance Tunnel
360° pressure maps the whole body at once
Obstacle Course Materials
Motor planning in action
Heavy Work Tools
Pushing, pulling, carrying = body calibration
Compression Clothing
All-day proprioceptive awareness
Balance Board / Wobble Board
Train the proprioceptive-motor loop

Material 1 of 9
Deep Pressure
Weighted Blanket / Weighted Lap Pad
Deep pressure wakes up the body map. Weighted blankets and lap pads provide deep pressure input that activates proprioceptors throughout the body. This sustained, even pressure helps the brain create a clearer sense of where the body is in space.
Why It Helps
When used before activities requiring coordination — homework, meals, transitions — the deep pressure "wakes up" the proprioceptive system and creates a more accurate body map. Many children also use weighted items during seated activities to reduce fidgeting and improve body awareness in the chair.
The calming effect also reduces the hyperactivity and fidgeting that some children use to seek proprioceptive input. Effect is temporary but builds over time with consistent use.
How to Use It
- Before activities: 15–20 minutes wrapped in blanket before coordination-demanding tasks
- During seated tasks: Lap pad during meals, homework, or circle time
- For sleep: Can use throughout the night if properly sized and child can move freely
- Frequency: Daily use recommended for consistent proprioceptive development

Material 1 — Weighted Blanket
What · Why · Where · How · When
Weighted Blanket / Lap Pad: Full Parent Guide
WHAT
A blanket or pad filled with evenly distributed weight — typically plastic pellets, glass beads, or rice/beans in a DIY version. Available in full blanket size or compact lap pad for seated use. Also available as weighted stuffed animals and weighted vests for movement activities.
WHY
Proprioceptors — the sensors in muscles and joints — respond to sustained pressure. A weighted blanket essentially "reminds" every part of the body it touches that it exists. This continuous signal helps the brain build and maintain a more accurate body map.
WHERE
At home on the couch, in bed, or at the homework table. At school: a weighted lap pad can be used discreetly under the desk. During any seated task where body awareness and stability are needed.
HOW
Drape over the child's lap or wrap around the body. For blankets, general guideline is 10% of body weight plus 1–2 pounds — consult your OT for a specific recommendation. DIY: fill a pillowcase evenly with dried rice or beans (2–3 kg for a lap pad). Use fleece or soft fabric outer for comfort.
WHEN
15–20 minutes before coordination activities. During meals, homework, or any task requiring sustained seated body awareness. At bedtime for calming. Build into daily routines for cumulative benefit over weeks and months.
Safety: Follow weight guidelines — typically 10% of body weight plus 1–2 pounds. Never use on children under 2 or children who cannot remove the blanket themselves. Do not cover face or head. Supervise initial use. Consult your OT for specific recommendations.

Material 2 of 9
Active Proprioception
Therapy Ball (Peanut Ball, Exercise Ball)
Unstable surface trains body awareness. Sitting or lying on an unstable surface like a therapy ball requires constant proprioceptive feedback. The body must continuously sense and adjust position to maintain balance — creating intensive proprioceptive input to muscles and joints throughout the body.
Why It Helps
This active engagement strengthens the connection between proprioceptive receptors and the brain. Active sitting on unstable surfaces provides ongoing proprioceptive input throughout seated tasks — this is more effective than static sitting for building body awareness. The body learns to maintain awareness while the mind focuses elsewhere, improving automatic proprioceptive processing.
Activities to Try
- Sitting at desk or table for homework or meals
- Prone (belly) over ball, reaching for objects on floor
- Bouncing while catching or throwing
- Rolling forward and back, side to side
- Wall push-ups with hands on ball
- Sitting and doing arm exercises
Sizing matters: When seated, child's hips and knees should be at 90 degrees with feet flat on floor. Start with a peanut ball (more stable) and progress to a round ball over time. Use on non-slip surface and inspect regularly for damage.

Material 2 — Therapy Ball
What · Why · Where · How · When
Therapy Ball: Full Parent Guide
WHAT
An inflatable ball used as a seating or exercise surface. Options include round exercise balls (sized by child height), peanut-shaped balls (more stable for beginners), ball chairs (ball in a frame for desk use), and BOSU balls (flat-bottom half-ball for standing activities).
WHY
The unstable surface forces the body to make constant micro-adjustments, activating proprioceptors in the core, legs, hips, and back simultaneously. This continuous "conversation" between body and brain strengthens proprioceptive pathways over time — especially when combined with cognitive tasks like homework.
WHERE
At a homework table or desk. In a therapy room. In a classroom (ball chair). Any space where the child needs to sit for an extended period. Outdoors for bouncing and movement activities.
HOW
Start with the peanut ball — more stability, less intimidating. Sit with feet flat and hips at 90 degrees. Combine with academic tasks for best results. Progress to round ball as confidence and skill build. For prone activities, drape the child belly-down over the ball and have them reach for objects on the floor.
WHEN
During homework, meals, or any seated task. Replace the regular chair with the ball seat for the full session. Alternate with regular seating as needed. Use bouncing activities as a "reset" before demanding tasks.

Material 3 of 9
High-Intensity Input
Crash Pad / Crash Mat
Safe crashing delivers big body input. Crash pads provide a safe surface for the heavy impact that proprioceptive-seeking children crave. Jumping, crashing, and landing delivers intensive proprioceptive input through joints and muscles — this "big input" helps calibrate the proprioceptive system.
Why It Helps
Crashing provides HIGH-INTENSITY proprioceptive input that can "reset" an under-responsive proprioceptive system. The impact teaches the brain to register proprioceptive information more accurately. It also provides a safe outlet for the crashing and bumping behavior that proprioceptive-seeking children often display unsafely elsewhere — redirecting an instinct into a therapeutic activity.
Safe Jumping Progression
- Step onto pad from floor level
- Small hop onto pad (2–3 inches)
- Jump from low step (6–8 inches)
- Jump from higher surface (12–18 inches) — supervised
- Running jump from short distance
Follow crashing with activities requiring controlled movement to transfer the heightened body awareness.
DIY Option: Large beanbag chair, stacked couch cushions, or an old mattress on the floor all work well. The key is a THICK, SOFT landing surface that absorbs impact while still delivering proprioceptive feedback. Place away from walls and furniture.

Material 3 — Crash Pad
What · Why · Where · How · When
Crash Pad / Crash Mat: Full Parent Guide
WHAT
A large, thick foam-filled mat or beanbag designed to safely absorb the impact of jumping and crashing. Commercial crash pads are the most durable option. DIY alternatives: large beanbag (6+ feet), stacked foam mats, an old mattress, or couch cushions enclosed in a sheet.
WHY
Children with proprioceptive differences often crave intense impact because their nervous system needs strong signals to register body position. Crash pads give them that input safely, preventing the dangerous crashing into furniture, walls, and siblings that happens when the need goes unmet.
WHERE
In a dedicated play area, sensory room, or any space with enough room to jump and land safely. Away from walls, furniture, and breakable objects. Can be used in a backyard or garage. Therapy centers often have a crash pad area.
HOW
Set clear rules about safe jumping before you begin. Always supervise. Start with low heights and progress slowly. Allow the child to jump, crash sideways, or roll onto the pad. After crashing, guide them into an activity requiring controlled, precise movement — such as building blocks or pouring — to use the heightened body awareness.
WHEN
Use as a regulatory tool before activities requiring coordination. Use when the child is seeking intense input through unsafe behaviors. 10–15 minutes of crash pad time before homework or meals can significantly improve seated body awareness. Not for diving headfirst.

Material 4 of 9
Resistive Input
Therapy Putty / Resistive Putty
Resistance builds hand awareness. Therapy putty provides resistive proprioceptive input specifically to hands and fingers. Squeezing, pulling, pinching, and stretching putty requires the muscles and joints of the hands to work against resistance — generating proprioceptive feedback that helps the brain map the hands more accurately.
Why It Matters for Clumsiness
This is critical for children who drop things, use incorrect grip force, or have poor hand awareness. Children who grip too hard OR too soft both benefit — the resistance teaches the brain what appropriate force feels like. Just 5–10 minutes of putty work before fine motor activities measurably improves performance.
Resistance Levels (Progression)
- Tan: Extra soft — minimal resistance (beginners)
- Yellow: Soft — light resistance
- Red: Medium — moderate resistance
- Green: Firm — challenging resistance
- Blue: Extra firm — maximum resistance

Material 4 — Therapy Putty
What · Why · Where · How · When
Therapy Putty: Full Parent Guide
WHAT
A silicone-based resistive putty available in graded resistances, from extra soft (tan) to extra firm (blue). Also includes hand exercise balls, grip strengtheners, and DIY alternatives such as stiff playdough or cornstarch-and-conditioner dough (for similar but less graded resistance).
WHY
The hands have a dense concentration of proprioceptors. When those receptors receive clear, calibrated input through resistance, the brain's "hand map" sharpens — improving grip force regulation, object manipulation, and hand awareness. Without this, the brain cannot accurately gauge how hard to hold a pencil, a cup, or a friend's hand.
WHERE
At home before writing or drawing tasks. During quiet reading time (the hands work while the mind reads). In the classroom before handwriting. In therapy sessions as a warm-up. Portable enough to take anywhere — in a bag or backpack.
HOW
Start with tan or yellow (softest). Activities: squeeze and release, pull apart with both hands, pinch and pull, roll into ball then flatten, hide small objects and find them, form letters or shapes. Use the firmness that requires effort without causing pain or frustration. Progress to firmer resistances over weeks.
WHEN
5–10 minutes before any fine motor task: writing, cutting, eating with utensils, craft activities. Use as a "hand warm-up" — just like athletes warm up muscles before a game. Store in an airtight container. Supervise younger children; not for mouthing.

Material 5 of 9
Whole-Body Input
Body Sock / Resistance Tunnel
360° pressure maps the whole body at once. A body sock is a stretchy fabric sack that the child climbs inside. When they push against the fabric from inside, they receive proprioceptive feedback across their ENTIRE body surface simultaneously.
Why It Helps
This 360-degree input helps create a complete, unified body map — showing the brain where ALL body parts are at once, in relationship to each other. This is particularly powerful for children whose body parts feel "disconnected" or whose movement is uncoordinated because different body parts aren't mapped together. Use before coordinated movement activities to establish unified body awareness.
Body Sock Activities
- Push outward in all directions (static input)
- Make shapes (star, ball, letter) while inside
- Animal walks inside sock (crawling, crab walk)
- Roll side to side while inside
- Push against wall while inside
- Move from lying to sitting to standing inside sock
Safety: Always ensure a face/head opening for breathing. Never use with face covered. Some children feel claustrophobic initially — introduce gradually and always supervise. Fabric must be stretchy enough to provide resistance but not so tight as to restrict circulation or movement.

Material 5 — Body Sock
What · Why · Where · How · When
Body Sock / Resistance Tunnel: Full Parent Guide
WHAT
A large sack made of 4-way stretch Lycra or spandex fabric. Child climbs inside and pushes against the fabric walls. Available commercially (Harkla, Fun and Function, SENSORY4U) or DIY with Lycra fabric sewn into a bag shape. Must have a face/head opening for safety.
WHY
Most proprioceptive activities target one region of the body at a time. The body sock is unique in that it provides simultaneous whole-body feedback — every push activates receptors across the entire surface. This helps the brain integrate body parts into a unified map rather than sensing arms, legs, and torso as disconnected pieces.
WHERE
In a sensory corner at home, in a therapy room, or any space with enough room to move safely. Works well indoors. Should be on a soft or carpeted surface in case the child loses balance inside the sock.
HOW
Help the child step in feet-first. Encourage them to push outward against the fabric in all directions. Guide them through movements — make a star shape, curl into a ball, do a crab walk. Pair with verbal body-part awareness prompts: "Can you push with just your left arm?" This adds motor planning challenge.
WHEN
5–10 minutes before coordinated movement activities or PE. After a stressful or disorganized period to "re-integrate" the body. In the evening as a calming whole-body input before homework or wind-down routines. Introduce gradually — some children need several sessions to feel comfortable.

Material 6 of 9
Motor Planning
Obstacle Course Materials (Tunnels, Cones, Balance Items)
Motor planning in action. Obstacle courses require complex motor planning — the brain must sequence movements, judge distances, coordinate body parts, and adjust to changing challenges. This integrated challenge trains the proprioceptive system in real-world context.
Why It Helps
Regular obstacle course practice improves the automatic proprioceptive processing that clumsy children lack. The variety of challenges — crawling, stepping, jumping, balancing — provides diverse proprioceptive input that no single material can match. The goal is SUCCESSFUL navigation, not difficulty. Adjust the course to ensure more successes than failures, building confidence alongside coordination.
Sample Course
- Crawl through tunnel
- Step on 4 stepping stones
- Walk along tape line (balance beam)
- Jump into 3 hula hoops
- Weave through 5 cones
- Crash onto crash pad
DIY Version: Couch cushions as stepping stones. Chairs with a blanket as a tunnel. Tape lines on floor to walk along. Hula hoops to jump in. Pool noodles as hurdles. Cardboard boxes as tunnels. The key is VARIETY and SEQUENCING of challenges.

Material 6 — Obstacle Course
What · Why · Where · How · When
Obstacle Course Materials: Full Parent Guide
WHAT
A sequence of movement challenges using pop-up tunnels, stepping stones/balance pods, cones, tape balance beams, hula hoops, small hurdles, and crash pads. Household items work beautifully. The key is creating a SEQUENCE of varied physical challenges that must be completed in order.
WHY
Motor planning — knowing what your body needs to do before it does it — is a core deficit in children with proprioceptive differences. Obstacle courses force this planning in a playful, low-stakes environment. The brain practices "read the challenge → plan the movement → execute → adjust → move on" repeatedly, building automatic motor planning over time.
WHERE
Indoors in a living room, hallway, or playroom. Outdoors in a yard or garden. In a therapy center's gym space. At school during movement breaks. Any space large enough to set up 4–8 sequential elements safely.
HOW
Start with 2–3 simple elements. Walk through the course with your child first, naming each challenge. Then let them navigate independently. Celebrate successful navigation. Add complexity over weeks: 4–5 elements, then 6–8, then balance challenges, then speed elements. Change the course weekly to prevent memorization and keep the motor planning challenge fresh.
WHEN
After school as a physical reset before homework. On weekends as play. Before PE or sports as a warm-up. When the child seems "disconnected" from their body. Stop before frustration — the session should always end on a success. Aim for 15–20 minutes of active course navigation.

Material 7 of 9
Heavy Work
Heavy Work Tools (Wagon, Wheelbarrow, Push Cart)
Pushing, pulling, carrying = body calibration. Heavy work — pushing, pulling, carrying, lifting — provides intensive proprioceptive input through major muscle groups and joints. This is often called the most powerful proprioceptive input available.
Why It Helps
When children push weighted wagons, carry heavy items, or do wheelbarrow walking, their muscles and joints are fully engaged — sending strong, clear signals to the brain about body position and movement. This input helps calibrate the entire proprioceptive system. Effects last 1–2 hours typically, making heavy work ideal as a preparatory activity before coordination-demanding tasks.
Daily Heavy Work Opportunities
- Carry laundry basket to washing machine
- Push grocery cart at the store
- Carry backpack to school
- Help carry groceries from car
- Push sibling in stroller
- Help with gardening or yard work
- Vacuum (push/pull motion)
- Wipe tables down with resistance

Material 7 — Heavy Work Tools
What · Why · Where · How · When
Heavy Work Tools: Full Parent Guide
WHAT
Any tool that involves moving against resistance with large muscle groups. Includes: wagons (with weight added), toy wheelbarrows, push carts, backpacks with added weight, laundry baskets for carrying, resistance bands for pulling. Activities using body weight — wall push-ups, floor push-ups, wheelbarrow walking — also count.
WHY
Heavy work is considered the most organizing proprioceptive input because it simultaneously activates large muscle groups AND compresses joints. This creates a loud, clear proprioceptive signal that even an under-responsive system can register. It "wakes up" the body map more effectively than lighter input activities.
WHERE
At home doing chores. In the yard doing outdoor work. At the grocery store pushing the cart. In therapy: wheelbarrow walking, pulling weighted sleds, carrying weighted items. At school: carrying materials between classrooms, helping with setup and cleanup. Heavy work opportunities are everywhere once you look for them.
HOW
Add weight to wagons or backpacks gradually. Supervise wheelbarrow walking — adult holds child's legs while child walks on hands. Ensure effort is challenging but not straining. Teach proper body mechanics: bend knees, keep back straight when lifting. Frame as "helping" tasks — children engage more when they feel purposeful and capable.
WHEN
Build into daily routines so proprioceptive input happens every 2–3 hours. Use before coordination-demanding activities — meals, homework, PE. Effects last 1–2 hours. When the child seems "lost" in their body or particularly disconnected, 10–15 minutes of heavy work can provide an immediate reset.
Safety: Ensure weight is appropriate — challenging but not straining. Watch for fatigue. Stop if child complains of pain. Teach proper body mechanics early to protect developing joints and back.

Material 8 of 9
Continuous Input
Compression Clothing (Compression Shirt, Shorts)
All-day proprioceptive awareness. Compression clothing provides constant, even pressure across body surfaces throughout the day. This ongoing proprioceptive input helps maintain body awareness during all activities — not just dedicated therapy sessions.
Why It Helps
For clumsy children, compression wear serves as a continuous reminder of where their body is in space. The steady sensory input can improve attention to body position and reduce the "lost in space" feeling that leads to bumping and tripping. Particularly useful for children who show improved coordination immediately after active proprioceptive input but lose it quickly — the compression maintains that heightened body awareness throughout the school day.
Wearing Protocol
- Start: 1–2 hours to assess tolerance
- Build: Gradually increase to full-day wear if tolerated
- Activities: Can wear during sports, school, and daily activities
- Fit: Snug but comfortable — child should not resist wearing it
- Tip: Have multiple sets for rotation and washing

Material 8 — Compression Clothing
What · Why · Where · How · When
Compression Clothing: Full Parent Guide
WHAT
Form-fitting athletic garments that apply consistent, even pressure to the body. Includes compression shirts, shorts, full-body suits, athletic rash guards, tight leggings, and sensory compression vests. Clinical options include SPIO (Stabilizing Pressure Input Orthosis). Regular athletic compression wear (Under Armour, swimsuits) also works effectively.
WHY
Unlike therapy activities that provide brief, intense proprioceptive input, compression clothing works passively and continuously. The body surface feels its own boundaries all day long, giving the brain an ongoing "you are here" signal. This is particularly valuable during school hours when active proprioceptive activities aren't possible.
WHERE
Worn under regular clothing at school — discreet and practical. During sports and PE for enhanced body awareness during movement. At home during homework or mealtimes. Can be worn all day once tolerance is established. Some children wear it only during specifically challenging times (school, sports).
HOW
Choose garments that fit snugly but allow full range of motion. The child should feel even pressure but not restriction. Should not leave marks or cause discomfort. Start with the least intrusive option (a compression shirt) and expand from there. Let the child be part of choosing — sensory comfort is critical for consistent wear.
WHEN
Start with 1–2 hours per day and build gradually. Wear during school, during sports, or whenever coordination and body awareness are most needed. Never force a child to wear compression clothing if it causes distress — the goal is comfort plus input. Watch for numbness, color changes, or complaints of tightness.

Material 9 of 9
Proprioceptive-Motor Loop
Balance Board / Wobble Board
Train the proprioceptive-motor loop. Balance boards require continuous proprioceptive engagement to maintain stability. Standing on an unstable surface forces the body to constantly sense position and make micro-adjustments — training the proprioceptive-motor loop that clumsy children struggle with.
Why It Helps
The immediate feedback — wobble or fall if body position isn't sensed and corrected — builds the automatic proprioceptive processing that should happen unconsciously. Over time, this improves overall balance and coordination during all activities. The goal is training the brain to sense and correct automatically, without conscious thought — exactly what coordinated movement requires.
Balance Progression
- Stand with both feet, holding support
- Stand with both feet, no support (brief)
- Stand with both feet, no support (extended)
- Stand while doing arm movements
- Stand while catching and throwing
- Stand while doing academic tasks
- One-foot standing (advanced)
Safety first: Have a stable support nearby initially (wall, chair, adult hand). Use on non-slip surface. Start with less unstable options and progress gradually. Stop if frustration or fatigue occurs.

Material 9 — Balance Board
What · Why · Where · How · When
Balance Board / Wobble Board: Full Parent Guide
WHAT
An unstable platform that rocks, tilts, or wobbles when stood upon. Options include wobble boards (circular with rocker bottom), skateboard-style balance boards, balance pods (individual stepping stones), BOSU balls, and DIY versions (wood plank on a tennis ball, or a 2x4 balance beam on the floor).
WHY
Coordinated children sense their body position automatically — they don't have to think about balance while doing other things. Clumsy children must consciously concentrate on both body position AND the task, which is exhausting and impossible. Balance boards train the automatic layer of proprioceptive processing, eventually freeing up attention for the task at hand.
WHERE
In a living room or playroom. In a therapy gym. In front of a TV for passive use during shows. At a standing desk or table for homework. On a non-slip surface with clear space around to step off safely.
HOW
Start with an adult hand for support. Practice standing still, then add small weight shifts. Once stable without support, introduce dual tasks: throw and catch a ball, follow verbal instructions, do spelling drills. These dual-task activities train the brain to maintain body awareness while attention is directed elsewhere — the real skill transfer needed for daily life.
WHEN
Daily practice of 10–15 minutes produces the best results. Use during TV time to make passive activities proprioceptively active. Use before PE or sports as a warm-up for the proprioceptive system. Track progress monthly — wobble board performance is a visible, motivating measure of improvement for children and parents alike.

Materials Summary
Your 9-Material Toolkit at a Glance
Each material targets a different dimension of proprioceptive input — from brief intense bursts to all-day passive awareness. The best results come from combining multiple approaches into a consistent daily routine.
Deep Pressure
- Weighted Blanket/Lap Pad
- Body Sock
- Compression Clothing
Active Proprioception
- Therapy Ball
- Crash Pad
- Balance Board
Resistive Input
- Therapy Putty
- Heavy Work Tools
Motor Planning
- Obstacle Course Materials

Getting Started
Essential Starters & Most Impactful Materials
Not sure where to begin? Start with these three foundational materials, then build your toolkit over time as you see what works best for your child.
Begin Here — Essential Starters
Weighted Lap Pad
Immediate proprioceptive grounding for seated activities. Affordable, discreet, easy to use at home and school.
Crash Pad or Beanbag
Safe outlet for heavy impact. Highly motivating for kids. Can be DIY with couch cushions or an old mattress.
Therapy Putty
Portable, affordable hand proprioception. Immediate use before any fine motor task. Easy to introduce at any age.
Most Impactful Overall
Heavy Work Tools
Most organizing proprioceptive input available. Engages largest muscle groups. Build into daily chores and routines.
Crash Pad
Intensive input that children genuinely crave and enjoy. Redirects unsafe crashing behavior into therapeutic activity.
Obstacle Course
Combines proprioception with motor planning — addressing both the sensory and coordination dimensions of clumsiness simultaneously.

Age Guide
Which Materials Work Best at Every Age
Proprioceptive needs evolve with age. Tailoring material selection to developmental stages ensures maximum engagement and therapeutic benefit, supporting your child's journey from energetic exploration to independent self-regulation.
Toddlers (2-4)
Focus on energetic play and exploration with materials offering immediate, clear input.
- Crash Pad
- Body Sock
- Therapy Ball
- Weighted Lap Pad
Preschool (4-6)
Introduce more structured activities and fine motor engagement, building on earlier foundations.
- Wagon/Push Toys
- Simple Obstacle Courses
- Therapy Putty
- All Toddler Activities
School Age (6-10)
Encourage skill development, dual-tasking, and deeper engagement with proprioceptive tools.
- Balance Board
- Weighted Blanket
- Compression Clothing
- More Complex Heavy Work
Tweens (10+)
Promote independence, discreet support, and integrating tools into daily routines for self-regulation.
- Self-Directed Heavy Work
- Discreet Compression Garments
- Balance Board (standing desk)
- Yoga & Mindful Movement

Budget Guide
Build Your Toolkit on Any Budget
Creating a supportive environment doesn't have to break the bank. Many effective proprioceptive tools can be made or purchased affordably, with options to scale up as your child's needs evolve.
Low Cost (Under $20)
- Therapy Putty: Simple, portable hand resistance.
- DIY Crash Pad: Layered couch cushions or old mattresses.
- DIY Obstacle Course: Pillows, blankets, furniture.
- Small Therapy Ball: Basic playground or exercise balls.
- DIY Balance Board: Plywood on a tennis ball or a 2x4 beam.
Mid-Range ($20-$60)
- Standard Therapy Ball: Durable inflatable balls for active sitting.
- Body Sock: Stretchy fabric for deep pressure and body awareness.
- Basic Balance Board: Entry-level wobble or rocker boards.
- Push Toys/Small Wagon: Provides heavy work through pushing.
- Compression Clothing: Affordable sensory shirts or vests.
Investment ($60+)
- Weighted Blanket: Therapeutic weight for calming and sleep.
- Commercial Crash Pad: Durable, purpose-built sensory safety.
- Advanced Balance Board: Multi-directional or adjustable designs.
- Heavy Work Tools: Specialized items like resistance bands or heavier wagons.
- Full Obstacle Course Kits: Ready-made components for complex setups.

Daily Routine
Build Proprioceptive Input Into Every Day
Proprioceptive development requires consistent input over time — not occasional therapy sessions. The goal is to weave opportunities into existing routines so the body receives input every 2–3 hours throughout the waking day.
1
Morning
Wake with weighted blanket pressure. Carry backpack to door. Wall push-ups (5–10) before leaving. Carry own items to car or bus.
2
At School
Weighted lap pad during seated work. Chair push-ups between tasks. Carry classroom materials. Movement breaks with heavy work activities.
3
After School
Crash pad time (10–15 min). Obstacle course or heavy play. Therapy ball sitting for homework. Therapy putty during reading.
4
Evening
Help with chores involving carrying or pushing. Body sock time (5–10 min). Balance board while watching TV. Weighted blanket for sleep.
Weekly Goal: Aim for proprioceptive input every 2–3 hours during waking time. Track weekly, not daily — proprioceptive development is slow but real. Celebrate small milestones along the way.

School Accommodations
Supporting Your Child at School
Many proprioceptive strategies can be implemented discreetly at school with teacher cooperation. These accommodations reduce injury risk, improve participation, and help your child learn more effectively.
Classroom
- Seat away from high-traffic areas (aisles, doors)
- Weighted lap pad for seated work
- Movement breaks for heavy work
- Reduce desk clutter to minimize knock-overs
- Non-spill containers for drinks
PE Class
- Modify activities for success
- Allow extra time for skill learning
- Partner with a supportive peer
- Focus on personal progress, not comparison
- Provide alternative ways to participate
Fine Motor Tasks
- OT consultation for handwriting support
- Keyboarding as alternative when appropriate
- Adapted scissors and pencil grips as needed
- Extra time for fine motor tasks
- Compression clothing under uniform
Progress Tracking
How to Track Real Progress Over Time
Proprioceptive development is slow — it happens over weeks and months, not days. Track weekly or monthly, not daily. Use specific, observable metrics so you can see real change even when it feels invisible.
What to Measure Weekly
- Frequency of bumping/tripping per day
- Number of items dropped or knocked over at meals
- Falls from chairs per week
- New bruises per week
- Participation in physical activities
- Confidence in motor challenges (self-reported)
Celebration Milestones
First week without falling off a chair
Successfully navigated the obstacle course
Caught a ball for the first time
Went a full day without bumping into door frames
Tried a new physical activity willingly

For Parents
You See It. You Feel It. Here's the Truth.
"You watch your child navigate the world like they're wearing a blindfold. They walk into walls that are clearly there. They knock over their drink at EVERY meal. They come home from school with new bruises and can't explain how. People call them clumsy, careless, not paying attention — but you see the genuine surprise on their face when they trip. They're not ignoring obstacles; they genuinely don't seem to know they're there."
You are not imagining it. And it is not your child's fault, and it is not yours either. The brain's "body map" is unclear — they genuinely don't know where their body is sometimes. When we give their brain consistent, intensive proprioceptive input, that map gets clearer. The bumping and tripping reduces. They become more confident in their body. This takes time and consistency — but it works.
What Success Actually Looks Like: Not becoming a star athlete. Success is walking across the room without bumping into furniture. Success is eating a meal without knocking over a drink. Success is trying a physical activity without being paralyzed by fear of failure. Success is feeling at home in their own body.
Parent Guidance
What Helps — and What Doesn't
Understanding how to respond to clumsiness makes a profound difference in your child's emotional wellbeing and their ability to make progress. Here's what the evidence — and experienced parents — tell us.
What Helps
- Recognize this is neurological, not behavioral
- Build daily proprioceptive input into routines
- Frame heavy work as "helping" — children engage better with purpose
- Celebrate effort and progress, not just outcomes
- Provide safe crash/impact opportunities before frustration builds
- Work with school on accommodations
- Consider OT evaluation if clumsiness significantly impacts daily life
Common Mistakes to Avoid
- Assuming child is careless or not paying attention
- Punishing clumsiness as a behavioral issue
- Protecting child from ALL physical activities (they need practice)
- Expecting quick improvement — proprioceptive development is slow
- Providing input occasionally instead of daily
- Not addressing the emotional impact of clumsiness
- Comparing to typically developing peers
Red Flags
When to Seek Professional Evaluation
These materials support proprioceptive development in children with typical-range coordination difficulties. However, some situations require professional assessment by a licensed occupational therapist or developmental pediatrician.
Seek evaluation if:
- Clumsiness is significantly worse than peers and not improving
- Coordination difficulties interfere with daily activities and learning
- Child has frequent injuries requiring medical attention
- Motor difficulties are causing significant emotional distress
- Child is avoiding all physical activities and play
Also seek evaluation if:
- Developmental milestones (walking, running, jumping) were significantly delayed
- Coordination problems are getting worse over time, not better
- Signs of possible underlying neurological condition
- Child has been diagnosed with ADHD or autism and also shows these patterns
- Self-esteem or social participation is significantly affected
Developmental Coordination Disorder (DCD) / Dyspraxia affects 5–6% of school-age children and frequently co-occurs with ADHD (50%), autism, and learning disabilities. A formal diagnosis opens doors to school accommodations, therapy funding, and structured support.
Save This
Save This for Your Clumsy Kiddo 📌
Follow for more motor solutions — practical, evidence-informed materials and activities that help children with coordination differences feel grounded, capable, and confident in their bodies.
Save
Bookmark this page for easy reference when you need material recommendations quickly.
Share
Know another parent or teacher who needs this? Share it — awareness is the first step to support.
Coming Next
9 Materials for the Child Who Can't Sit Still — the next episode in the Motor Solutions Series.

Powered By
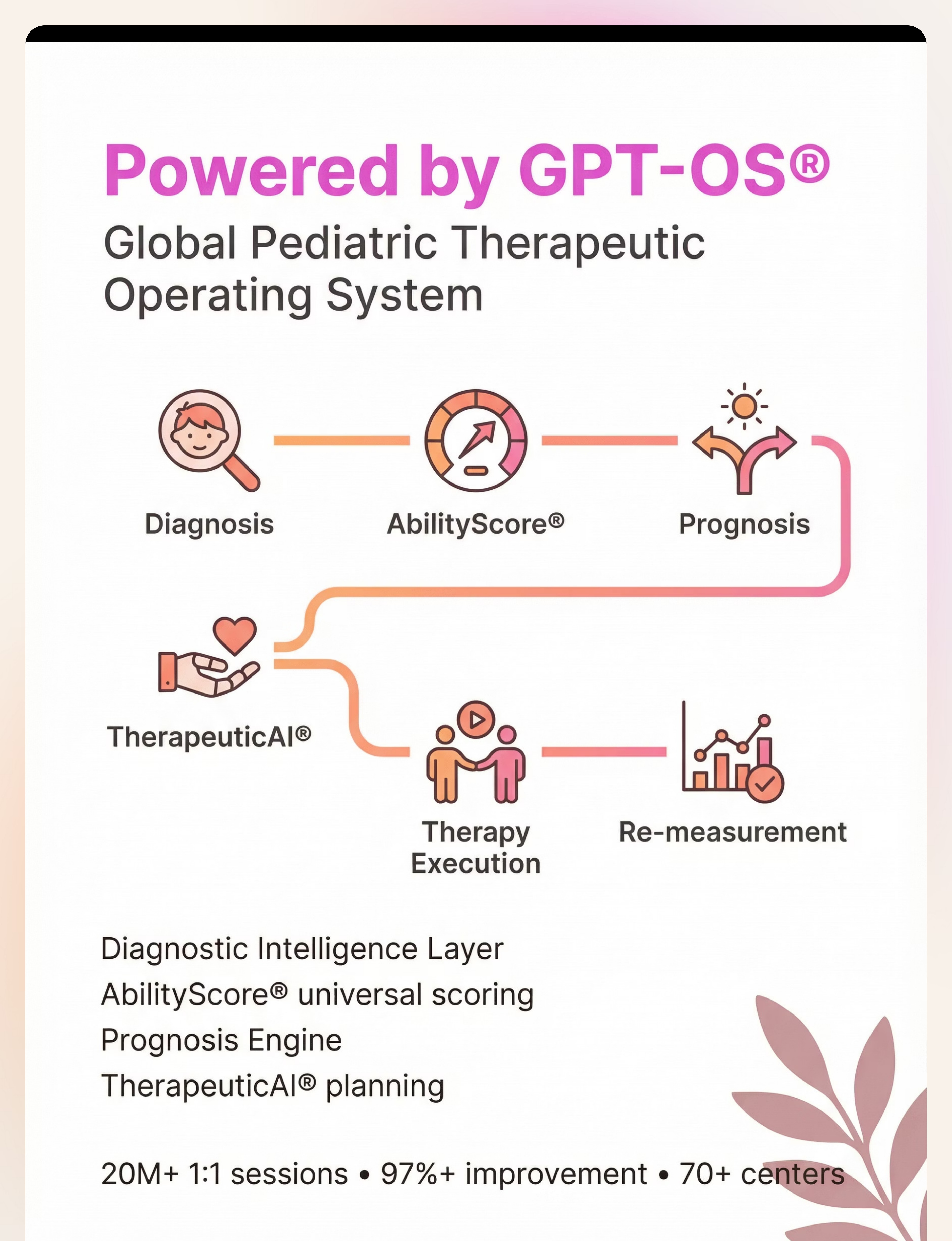
Powered by GPT-OS®
Global Pediatric Therapeutic Operating System
GPT-OS® is the end-to-end operating system that governs diagnosis, prognosis, therapy design, execution, monitoring, and readiness outcomes in child development — as one closed, accountable system. These strategies come from the clinical intelligence that has powered over 20 million 1:1 therapy sessions.
Diagnostic Intelligence Layer
Converts 591+ structured observations across 349 skills and 79 developmental abilities into standardized diagnostic clarity.
AbilityScore®
A patented universal developmental score (0–1000) that establishes baseline, severity, and longitudinal change across domains.
Prognosis Engine
Predicts developmental trajectories and risk windows using historical response patterns from 19M+ real therapy sessions.
TherapeuticAI®
Determines therapy focus, intensity, sequencing, and escalation thresholds — always under licensed human clinical authority.
EverydayTherapyProgramme™
Translates clinical plans into daily, home-executable micro-interventions so therapy continues beyond sessions.
FusionModule™
Coordinates speech, OT, behavior, special education, and medical inputs into a single converged therapeutic pathway.
This is not software. This is therapeutic infrastructure. Observation → Score → Plan → Execute → Re-measure → Adapt. Plans change only when the child's data changes.

Real-World Evidence
Measured Outcomes. Readiness, Not Assumptions.
Progress is defined by readiness for life — not therapy completion. GPT-OS evaluates outcomes using standardized readiness indexes that reflect real-world functional capability.
20M+
Exclusive 1:1 Sessions
Across converged therapy disciplines
97%+
Measured Improvement
Across one or more readiness indexes
70+
Centers
Operating under a single clinical system
Daily Living & Independence Index — Clumsiness Progression
Requires constant supervision for safety → Occasional bumping/tripping with reduced injury risk → Navigates most environments safely → Age-appropriate coordination for daily tasks → Participates in physical activities confidently.
Readiness Indexes Tracked
- Communication Readiness Index
- Behavioral Self-Regulation Index
- Learning & Academic Readiness Index
- Social Participation Index
- Daily Living & Independence Index
- Emotional Regulation Index
- Caregiver Dependence Reduction Index

Parent Story
"Normal-Kid Clumsy Now — Not Constant"
"He used to come home with new bruises every day. We couldn't figure out how. After working on his body awareness, he actually watches where he's going. He still bumps into things sometimes, but it's normal-kid clumsy now, not constant."
— Parent, Pinnacle Network. Illustrative case; outcomes vary by child profile.
Pinnacle measures readiness for real life — including safe, coordinated navigation through daily environments. Progress is gradual, consistent, and real. The goal is functional coordination for daily life, not athletic perfection.
For structured, personalized guidance for your child: Contact the FREE National Autism Helpline — available in 18+ languages. Call 9100 181 181 or visit pinnacleblooms.org

About
Pinnacle Blooms Network®
Built by Mothers. Engineered as a System.
Pinnacle is the execution layer of GPT-OS® — delivering therapy, daily programs, digital continuity, and marketplace access at population scale. From diagnosis to daily life readiness, Pinnacle operationalizes therapeutic intelligence into real-world outcomes for children and families.
Pediatric Therapeutic OTT Platform
On-demand therapy guidance, parent education, and EverydayTherapyProgramme™ delivery — accessible anytime, anywhere.
Hyperlocal Therapeutic Marketplace
Connects families to verified therapists, centers, programs, and resources — mapped to the child's AbilityScore® and readiness needs.
Center Network Execution
70+ physical centers operating under GPT-OS® standards with measurable clinical accountability and real-world outcome tracking.
Contact Us
FREE National Helpline (18+ languages)
📞 +91 9100 181 181
🌐 pinnacleblooms.org
✉️ care@pinnacleblooms.org
📞 +91 9100 181 181
🌐 pinnacleblooms.org
✉️ care@pinnacleblooms.org
Request AbilityScore® Assessment
A structured developmental assessment that establishes your child's baseline across 349 skills and 79 developmental abilities — the foundation of a personalized therapeutic pathway.

Statutory Information
Pinnacle Blooms Network® — Statutory Identifiers
20M+ sessions • 97%+ measured improvement • 70+ centers • Global IP protection across 160+ countries
CIN | U74999TG2016PTC113063 | |
DPIIT | DIPP8651 (Govt. of India) | |
MSME | Udyog Aadhaar: TS20F0009606 | |
GSTIN | 36AAGCB9722P1Z2 | |
ISO 13485 | Medical Device Quality Management System | |
ISO/IEC 27001 | Information Security Management |
© 2025 Pinnacle Blooms Network®. All rights reserved. Patents filed across 160+ countries. GPT-OS®, AbilityScore®, TherapeuticAI®, EverydayTherapyProgramme™, and FusionModule™ are proprietary systems of Pinnacle Blooms Network®.
Preview of 9 materials that help with clumsiness Therapy Material
Below is a visual preview of 9 materials that help with clumsiness therapy material. The pages shown help educators, therapists, and caregivers understand the structure and content of the resource before use. Materials should be used under appropriate professional guidance.


















Share this resource
Help others discover thisLink copied!

Important Disclaimer
Educational Content — Not a Clinical Substitute
This content is educational. It does not replace assessment by a licensed occupational therapist or developmental pediatrician. Significant coordination difficulties should be evaluated professionally. If your child's clumsiness causes injury, limits participation, or significantly impacts daily life, please consult a qualified professional.
Individual results may vary. Statistics represent aggregate outcomes across the Pinnacle Blooms Network. The materials and strategies presented here are intended to raise awareness and support families — they are not a diagnosis, treatment plan, or clinical prescription.
Related Episodes in the Motor Solutions Series
- A-102: Poor Balance (vestibular overlap)
- A-104: Can't Catch a Ball
- A-106: Bumps Into Things
- A-107: Uses Too Much Force
- A-108: Uses Too Little Force
- A-109: Difficulty with Bike Riding
Sources & Clinical Foundation
- SPD Foundation: Proprioception and Sensory Integration
- Ayres, A.J. — Sensory Integration and the Child (1979, rev. 2005)
- Miller, L.J. — Sensational Kids (2006)
- Zwicker et al. — Developmental Coordination Disorder: A Review and Update (2012)
© 2025 Pinnacle Blooms Network®. Motor Solutions Series — Episode A-105. #Proprioception #BodyAwareness #PinnacleBlooms
