
"Every single night, it's a war. And I don't know why."
The moment you say "bath time," your child's whole body changes — screaming, running, going completely limp. Getting her from the living room to the bathroom takes 20 minutes of negotiating, carrying, and sometimes crying — both of you. Once she's finally in the water she's fine, but when it's time to get out the meltdown starts all over again.
Daily Living Skills · Episode I-791

You Are Not Failing.
Your child's nervous system is speaking a language you haven't been taught yet. Tonight, we teach it to you.
9 Materials
A precision toolkit that transforms the nightly battle into a predictable, peaceful routine.
Multi-Disciplinary
Built by OTs, ABA therapists, SLPs, and NeuroDev Pediatricians — reviewed together, not in silos.
Home-Executable
Every material and every protocol step is designed for parents and caregivers — no clinic required.
Evidence-Based
Draws from Level I systematic review and RCT evidence. Clinically validated and parent-proven.
Pinnacle Blooms Network® | Occupational Therapy Lead | ABA Support | SLP Integration | NeuroDev Review | WHO Nurturing Care Framework (2018)

67 Million Families Are Navigating This Exact Battle Tonight.
You are among millions of families navigating this exact challenge. The struggle you feel every night is real, documented, understood — and solvable.
80%
Experience Sensory Differences
of children diagnosed with autism experience significant sensory processing differences that make bath time difficult. PRISMA Systematic Review, 2024 — PMC11506176
67M+
Children Worldwide
with neurodevelopmental differences face daily living transition challenges as a primary family stressor. WHO Global Report, 2023
1 in 4
Indian Families
with a child diagnosed with ASD report bath time as the single most challenging daily routine. Padmanabha et al., Indian J Pediatr, 2019

This is a wiring difference. Not a behavior choice.
Three systems in your child's brain are being overwhelmed simultaneously — and none of it is stubbornness, defiance, or bad parenting.
Understanding the neuroscience changes everything about how you respond.
Three Systems Simultaneously Overwhelmed
🧠 Executive Function (Prefrontal Cortex)
Bath time requires stopping a preferred activity, shifting attention, executing a multi-step sequence, and starting again in reverse. This demands cognitive flexibility that is genuinely underdeveloped in many neurodivergent children — not stubbornness.
🌊 Sensory Processing (Somatosensory + Vestibular Cortex)
Water temperature, tactile pressure of washcloths, sounds of running water, the backward head tilt during rinsing, the sudden cold of towel-drying — each registers as unpredictable threat input in a nervous system wired for hypervigilance.
⚡ Emotional Regulation (Amygdala + Limbic System)
When executive function AND sensory systems are simultaneously overwhelmed, the amygdala triggers fight (screaming, kicking), flight (running away), or freeze (going limp). This is not defiance. This is a nervous system in distress.

What Your Child Actually Experiences
The moment "bath time" is announced, their brain calculates an impossible task: stop what I'm doing (which feels urgent), navigate a room full of unpredictable sensations, and do it all again in reverse to get out. The word "bath time" can trigger the same alarm system that fire sirens trigger in most people.
Why the same child can be "fine in the water"
Once the transition crisis is over, the water itself may feel regulating. Many sensory-sensitive children love water. The problem is the TRANSITION — not the bath.
Why some nights are fine and others are disasters
Regulatory capacity depends on accumulated stress from the day. It is not random — it is the result of what came before bath time.
Why warnings don't work
Abstract words don't communicate predictability to a dysregulated nervous system. Visual and physical cues are required — words alone are insufficient.
Why the routine breaking down is communication
Your child's attempt to refuse or escape is their nervous system's attempt to regain control over an overwhelming situation.
Frontiers in Integrative Neuroscience (2020) — Framework for evaluating sensory integration treatment in ASD — DOI: 10.3389/fnint.2020.556660

Your Child Is Here. Here Is Where We're Heading.
Ages 1–2
All children resist transitions. For neurodivergent children, resistance may be more intense and longer in duration.
Ages 2–3
Verbal warnings begin helping typical children. Neurodivergent children may need visual + physical supports indefinitely.
Ages 3–4
Simple sequences understood, but abstract time ("5 minutes") still meaningless without visual anchors.
Ages 4–6
Most typical children manage with standard warnings. Structured supports remain essential for neurodivergent children.
Ages 6–10+
Independence is possible with the right scaffold. That's where this technique operates.
"Your child is not behind — they are developing along a different, equally valid pathway. These 9 materials are the scaffold that makes the pathway navigable."
Bath time transition difficulties frequently co-occur with: Autism Spectrum Disorder · ADHD · Sensory Processing Disorder · Anxiety Disorders · Developmental Delay · PDA Profile. WHO Care for Child Development Package (2023) | PMC9978394

Clinically Validated. Home-Applicable. Parent-Proven.
🛡️ LEVEL I — SYSTEMATIC REVIEW + RCT EVIDENCE
This toolkit draws from the highest tier of clinical evidence available in pediatric therapy. Every material recommendation is grounded in research replicated across multiple studies and populations.
Intervention | Evidence Grade | Key Finding | |
Visual Schedules | Level I | Evidence-Based Practice for ASD — NCAEP 2020 | |
Visual Timers | Level I | Reduces transition meltdowns — Multiple RCTs | |
First-Then Boards | Level I | Strong ABA contingency evidence — BACB Standards | |
Sensory Modifications | Level II | Systematic review: effective for daily living — PMC11506176 | |
Hair Washing Adaptations | Level II–III | Clinical consensus OT guidelines — AOTA 2020 | |
Post-Bath Regulation | Level II | Sensory integration theory + RCT support — PMC10955541 |
Key Meta-Analytic Finding: PRISMA Systematic Review (2024, 16 studies, 2013–2023): Sensory integration intervention meets criteria to be considered evidence-based practice for children with ASD — promoting social skills, adaptive behavior, sensory processing, and motor skills. — PMC11506176
India-Specific RCT: Padmanabha et al. (Indian Journal of Pediatrics, 2019): Home-based sensory interventions demonstrated significant outcomes in Indian pediatric populations. — DOI: 10.1007/s12098-018-2747-4

The Bath Time Transition Support Protocol
Parent alias: "Making Bath Time Work"
Definition
A structured, home-executable intervention framework combining visual predictability tools (schedules, timers, countdown systems), sensory modification materials (washing tools, temperature indicators, hair-washing adaptations), and regulation supports (bath engagement materials, post-bath comfort items) to address the neurological and behavioral challenges of transitioning into, through, and out of bath time routines.
Specification Badges
📅Age Range: 2–10 years
⏱️Session: Daily (bath time)
🔁Frequency: Every bath — consistency is the mechanism
🏠Setting: Home bathroom
👨👩👧Who Executes: Parent / Caregiver / Guardian
⏱️Session: Daily (bath time)
🔁Frequency: Every bath — consistency is the mechanism
🏠Setting: Home bathroom
👨👩👧Who Executes: Parent / Caregiver / Guardian
Domain Badges
🔵 Daily Living Skills · 🔵 Sensory Processing · 🔵 Emotional Regulation · 🔵 Executive Function · 🔵 Adaptive Behavior
Canon Material Categories
Visual Schedules · Visual Timers · First-Then Boards · Transition Objects · Sensory Wash Tools · Temperature Indicators · Hair Washing Solutions · Bath Engagement Toys · Post-Bath Regulation Items

This Technique Crosses Therapy Boundaries — Because the Brain Doesn't Organize by Therapy Type.
🟤 Occupational Therapist (PRIMARY LEAD)
Addresses sensory processing differences during bath, selects and grades sensory washing tools, designs the environmental setup, prescribes post-bath regulation strategies, and trains parents in sensory accommodation techniques.
🟣 ABA / BCBA Therapist
Designs the visual schedule and First-Then board systems, establishes reinforcement schedules for compliance with bath routine steps, implements countdown protocols, and tracks transition behavior data across sessions.
🔵 Speech-Language Pathologist
Integrates bath time as a language-rich routine (labeling body parts, water concepts, sequencing vocabulary), supports children with limited language to communicate sensory discomfort, and uses bath time as a natural context for requesting and commenting.
🟢 NeuroDev Pediatrician
Reviews the underlying sensory and regulatory profile, confirms no medical contraindications, monitors developmental progression, and determines when professional in-clinic sensory integration therapy is indicated beyond home execution.
"At Pinnacle, these four disciplines review every technique together. What you're reading is not one therapist's opinion — it is the convergent wisdom of a multi-disciplinary consortium across 70+ centers and 20 million+ sessions."
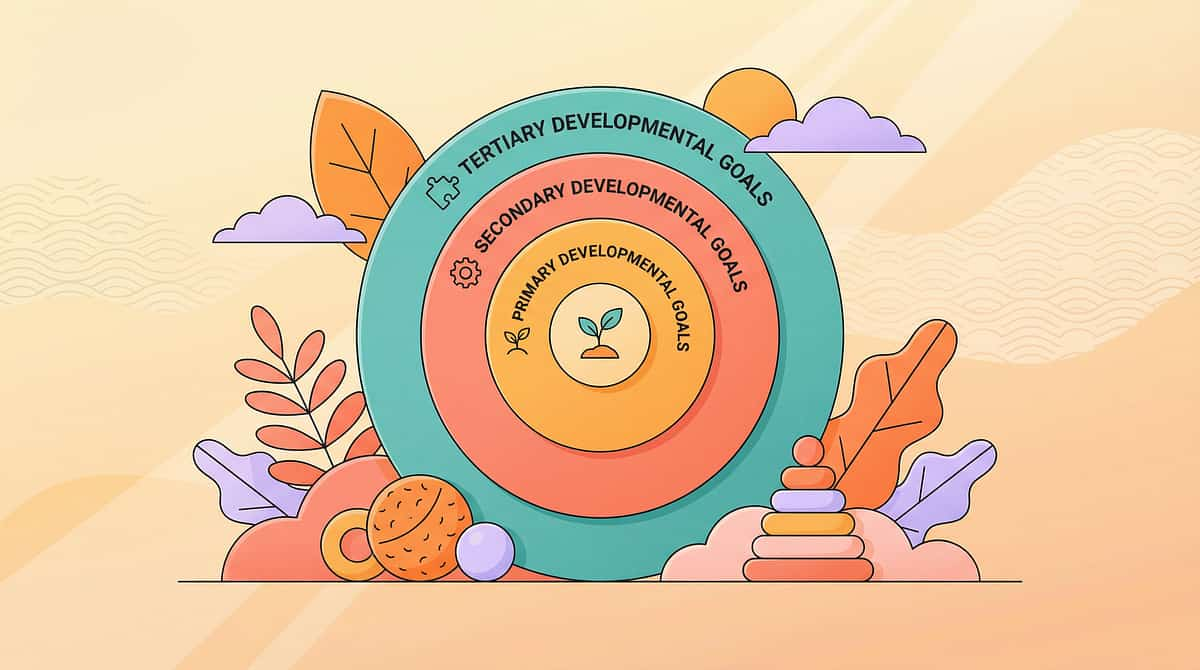
Nine Materials. Three Concentric Rings of Developmental Impact.
The ultimate goal of these nine materials extends far beyond a single bath. Transition compliance and sensory tolerance are the immediate targets, but the long-term impact ripples across your child's daily living independence, your family's evening wellbeing, and the quality of your child-parent relationship.
Target | What You'll See | Timeline | |
Transition compliance | Walks to bathroom with ≤2 prompts | Weeks 3–6 | |
Sensory tolerance | Accepts washing without crying | Weeks 2–5 | |
Exit compliance | Gets out when timer ends | Weeks 2–4 | |
Routine participation | Completes steps with visual support | Weeks 4–8 | |
Independence | Self-initiates bath routine | Weeks 8–16 |

Material 1 of 9
🗓️ Visual Schedule for Bath Time Routine
Canon Category
Visual Schedules / Activity Boards
What It Solves
The prefrontal cortex can't hold the full sequence in working memory. Externalizing it onto a wall removes the cognitive load entirely — the brain doesn't have to hold what the wall can hold.
Price Range
₹200–800 (commercial) | ₹0 (DIY with printer + laminator)
What to Look For
- Laminated, velcro-based, bathroom-safe
- Child-height mounting — they must be able to see and touch it
- Picture-based (not word-based) for pre-readers
- Steps that mirror your actual routine in sequence
DIY ₹0 Version
Phone photos of each step → Print → Laminate with tape → Velcro dots from craft shop → ₹50 total. Same visual predictability mechanism as a ₹800 commercial board.

Material 2 of 9
⏱️ Visual Timer (Waterproof / Tub-Visible)
Canon Category
Timers / Time Awareness Tools
What It Solves
"Five more minutes" is meaningless to a child without time perception. A visual timer makes time concrete, visible, and non-arguable — the red disc shrinking IS the time disappearing. This single insight resolves the most common exit meltdown trigger.
Price Range
₹500–2,000 (Time Timer / sand timer)
What to Look For
- Red-disc countdown style (Time Timer) — shrinking red section is universally understood
- Waterproof or water-resistant for bathroom environments
- Visible from inside the tub — placement matters
- Sand timer alternative: visible, tactile, and satisfying to watch
DIY ₹0 Version
Sand timer (₹50) or phone countdown visible on a shelf at safe distance from water. Same time-visibility function at a fraction of the cost.

Material 3 of 9
📋 First-Then Board
Canon Category
First-Then Boards / Contingency Visuals
What It Solves
The amygdala needs to know the demand is finite and leads somewhere good. First-Then makes the deal visible and non-negotiable — the brain can see both the demand AND the reward simultaneously, which reduces the threat calculation that drives refusal.
Price Range
₹150–600
What to Look For
- Two-section velcro board — "FIRST" and "THEN" clearly labeled
- Portable — can be shown at the point of transition announcement
- Bath-area safe — laminated or wipeable
- Large enough for child to see clearly from a distance
DIY ₹0 Version
Sheet of cardboard divided in two, laminated pictures of "bath" and the THEN reward. Same contingency communication mechanism — the board is the vessel, the principle is the medicine.
Material 4 of 9
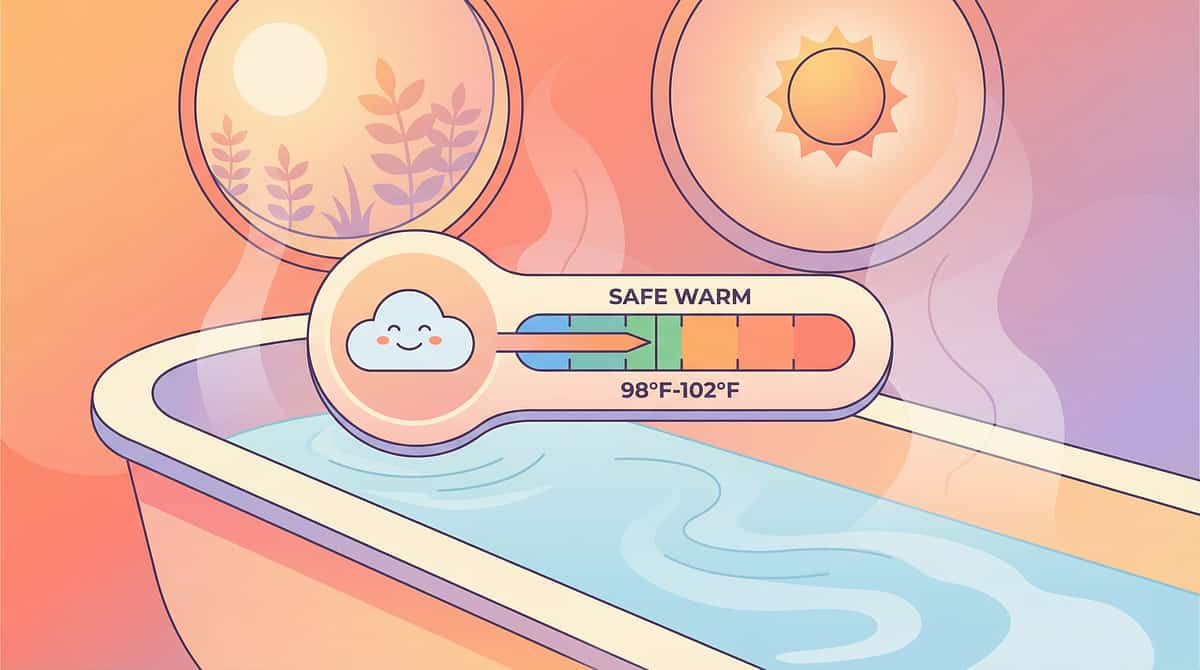
🌡️ Water Temperature Indicator
Canon Category
Sensory Assessment Tools / Safety Tools
What It Solves
Temperature anxiety is about unpredictability. A thermometer gives the child verifiable, objective proof the water is safe before they enter. Transferring the authority of "water is safe" from parent's word to a visible indicator removes the argument and restores child agency.
Price Range
₹300–1,200
What to Look For
- Floating duck or animal thermometer — child-friendly and engaging
- Color-change indicator — green = safe, red = too hot
- Child can hold and read it themselves (agency transfer)
- Safe temperature range: 37–38°C (98–100°F)
DIY ₹0 Version
Elbow-in-water test + consistent verbal agreement with child: "I checked it — it's the same as yesterday." Slightly less visual but achieves the same predictability function when done consistently.

Material 5 of 9
🦆 Bath Toys & Sensory Water Play Materials
Canon Category
Water Play / Sensory Engagement / Cause-Effect Toys
What It Solves
Makes the tub a destination, not a demand. Motivation to enter. Occupation that regulates during the bath. When the tub contains something exciting, the child's brain calculates "I want to go there" rather than "I have to go there." This single shift changes the entry trajectory entirely.
Price Range
₹200–1,500
What to Look For
- Pouring and filling cups — cause-effect water play is deeply regulating
- Cause-effect water toys — squirting, watermill, color-mixing
- Bath-only rotation set — keeps novelty high by rotating monthly
- Pre-placed in tub before announcing bath — the anticipation is the invitation
DIY ₹0 Version
Kitchen cups, small plastic containers, bath-safe household objects. Same cause-effect water play function. The principle is water + control + predictability — not the brand.

Material 6 of 9
🧽 Gentle Sensory Washing Tools
Canon Category
Sensory Wash Tools / Tactile Accommodation
What It Solves
A standard washcloth can feel like sandpaper to a tactile-sensitive child. This is not an exaggeration — it is the neurological reality of a tactile-defensive sensory system. The right washing tool eliminates the sensory trigger entirely. The bath continues; the pain stops.
Price Range
₹150–800
What to Look For
- Soft silicone scrubber — gentle, predictable, child can hold it themselves
- Ultra-soft microfiber cloth — finer fibers, less tactile alarm
- Bath mitts — child can control how firm the touch is
- Let the child choose — autonomy over the sensory input reduces threat response
DIY ₹0 Version
Old soft t-shirt cut into washcloths. Bare-hand washing (no tool — parent's hand is the softest option for many children). Same tactile accommodation principle.
Material 7 of 9
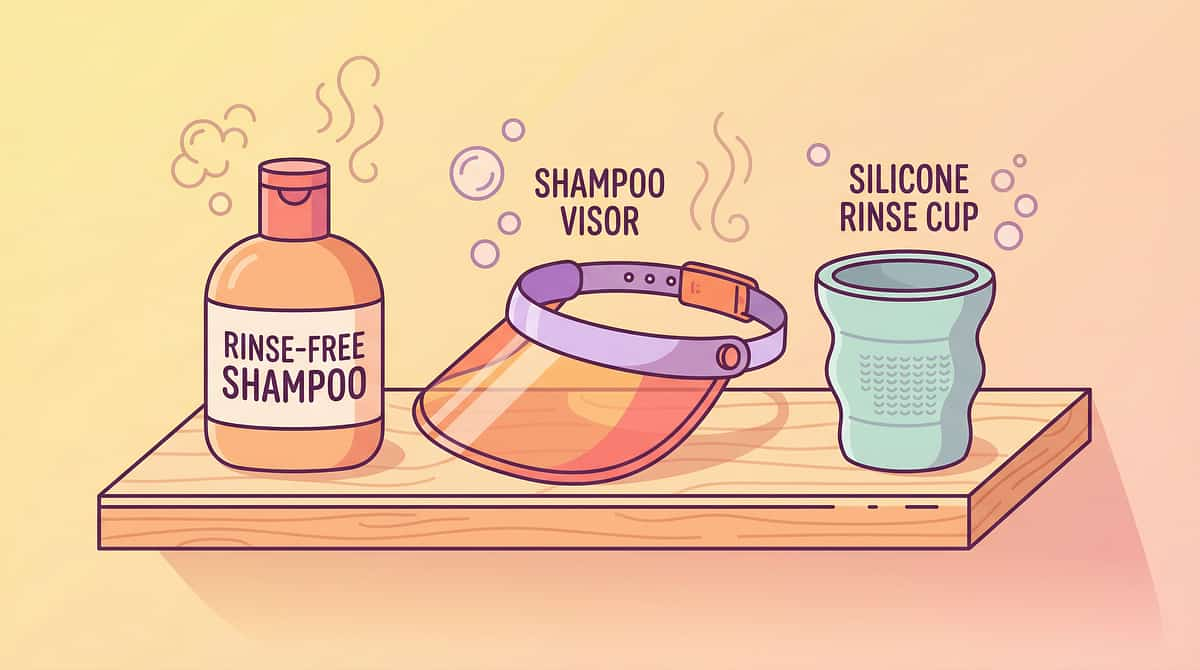
🚿 Hair Washing Solutions
Rinse-Free Shampoo · Shampoo Visor · Silicone Rinse Cup
Canon Category
Hair Washing Aids / Self-Care Accommodation Tools
What It Solves
Water on the face triggers vestibular + tactile alarm systems simultaneously — a double hit that overwhelms even children who tolerate the rest of the bath. These tools eliminate or control that trigger, making hair washing survivable before making it comfortable.
Price Range
₹200–1,000
What to Look For
- Shampoo rinse visor — keeps water entirely off face; game-changer for most children
- Rinse-free foam shampoo — eliminates rinsing entirely as first step
- Silicone-edge rinse cup — parent controls water direction precisely
- Child leans forward instead of back — removes vestibular tilt trigger
Implementation Note
Introduce hair washing as a separate, timed sub-event within bath. "Hair wash is only until the sand runs out — watch the timer." Making it finite and visible changes the experience entirely.

Material 8 of 9
🔢 Transition Warning & Countdown Tools
Canon Category
Transition Supports / Countdown Systems
What It Solves
Children don't resist endings — they resist surprises. Visible countdowns make the ending gradual, predictable, and therefore survivable. Each countdown step is a small, manageable grief — not a sudden loss. The system turns "it's over" into "it's almost over, almost over, almost over — over."
Price Range
₹100–800
What to Look For
- Numbered countdown cards — hold up 5, then 4, then 3, then 2, then 1
- Color-change light timer — ambient countdown signal, no adult required
- Transition song speaker — same song every time signals "time to get out"
- Can be paired with visual timer (Material 2) for dual countdown system
DIY ₹0 Version
Write 5-4-3-2-1 on cardboard squares. Hold them up in sequence. Same visual countdown function. The progression itself is the therapeutic mechanism, not the format.

Material 9 of 9
🛁 Post-Bath Comfort & Regulation Items
Canon Category
Transition Objects / Comfort Items / Regulation Tools
What It Solves
Getting out of the bath is a sensory transition: warm water → cold air, wet → drying. Without the right support, this transition can dysregulate a child who was perfectly calm in the water. The right post-bath kit makes this transition regulating, not dysregulating.
Price Range
₹300–1,500
What to Look For
- Soft hooded towel — encloses warmth, reduces cold air shock
- Warm-able robe or towel (dryer/radiator) — pre-warmed wrapping is deeply organizing
- Ultra-soft towels — no scratchy textures during vulnerable post-bath state
- Specific comfort toy that "waits" outside the tub — reunited post-bath creates a reliable anchor
Pinnacle Canon Verified Products
🐻Soft Animal Comfort Toy — ₹425 (post-bath transition object)
⭐Reward Sticker Book 1800+ stickers — ₹364
🏆Rosette Reward Jar — ₹589
⭐Reward Sticker Book 1800+ stickers — ₹364
🏆Rosette Reward Jar — ₹589

Every Material in This Toolkit Has a ₹0 Version. No Family Is Excluded.
WHO/UNICEF Principle: Context-specific, equity-focused interventions. These materials work because of the neurological principle they embody — not the brand on the label.
Material | Commercial | DIY ₹0 Version | |
Visual Schedule | ₹200–800 | Phone photos → Print → Laminate with tape → Velcro dots from craft shop → ₹50 total | |
Visual Timer | ₹500–2,000 | Sand timer (₹50) or phone countdown visible on a shelf | |
First-Then Board | ₹150–600 | Sheet of cardboard divided in two with laminated pictures | |
Temperature Indicator | ₹300–1,200 | Elbow-in-water test + consistent verbal agreement with child | |
Bath Toys | ₹200–1,500 | Kitchen cups, small plastic containers, bath-safe household objects | |
Sensory Wash Tools | ₹150–800 | Old soft t-shirt cut into washcloths; bare-hand washing | |
Hair Wash Visor | ₹200–1,000 | Visor cap from ₹30 bazaar purchase; child leans forward instead of back | |
Countdown Cards | ₹100–800 | Write 5-4-3-2-1 on cardboard squares | |
Post-Bath Comfort | ₹300–1,500 | Thickest softest towel in house + warm it on radiator |
"Bath time peace is not a product you buy. It is a neurological accommodation you provide. These materials are just the vehicle — the principle is what matters. Any family, anywhere, can begin tonight."

The Pre-Session Safety Gate. Read Before Every Bath.
🔴 RED — Absolute Stop Conditions
Do not begin bath time if any of these are present:
- Child is in full meltdown before bath is announced — baseline dysregulation too high
- Child shows signs of illness: fever, ear pain, skin infection, new rash
- Child has an open wound or skin condition requiring medical advice
- Caregiver is severely dysregulated — your nervous system regulates theirs
- Child has exhibited self-injurious behavior in the last 30 minutes
🟡 AMBER — Modify Conditions
These don't stop bath, but require protocol adjustment:
- Child had a difficult day — use minimal-demand version (shorter bath, fewer steps)
- Child missed usual sleep or meal — reduce expectations, increase reinforcement
- Caregiver is stressed but functional — implement extra self-regulation before initiating
🟢 GREEN — Go Conditions
- Child is in calm-alert state
- At least 30 minutes since last high-demand activity
- Caregiver feels regulated and prepared
- Visual supports are in place and ready before bath is announced
"If your child says it hurts, it hurts. Sensory experience is subjective and real. Forcing through expressed pain creates trauma associations that multiply future resistance. Accommodate, do not overpower."
Material Safety: Water temp 37–38°C · Electrical devices minimum 1.5m from water · Sand timers: check for breakage risk · Small velcro pieces: out of reach for mouthing children · Bath toys: weekly mold check, squeeze water out after every bath.

Spatial Precision Prevents 80% of Bath Time Failures Before They Start.
Announce bath ONLY after space is fully prepared.
The setup is not a courtesy — it is the intervention. An unprepared bathroom is the number one cause of protocol failure in weeks 1–2.
Sensory Environment Tuning
- Sound: Running water before child enters the bathroom
- Light: Warm/dim if tolerated — overhead bright lights can be overstimulating
- Smell: Same soap/shampoo as last time — novel smells = sensory alarm
- Temperature: Bathroom warm — transition from clothes to wet is less jarring
Pre-Bath Setup Checklist (parent executes before announcing)
- □ Water temperature pre-set to 37–38°C
- □ Visual schedule mounted at child eye-level beside tub
- □ Visual timer placed where child can see from tub
- □ First-Then board visible at bathroom entrance
- □ Bath toys pre-placed in tub (anticipation motivator)
- □ Post-bath towel pre-warmed and ready outside tub
- □ Preferred pajamas laid out visibly near bath area
- □ Lighting adjusted (softer lamp if child is light-sensitive)
- □ All washing tools laid out in order of use

The Best Bath Time Session Is One That Starts Right.
60 seconds now saves 40 minutes of crisis later. Observe your child for 60 seconds before announcing bath — this single habit changes the entire trajectory of the evening.
Indicator | Go ✅ | Modify ⚠️ | Postpone ❌ | |
Child's affect | Calm-alert, playing | Mildly fussy | Distressed, crying | |
Body language | Relaxed movement | Slightly tense | Rigid, avoidant | |
Time since last demand | 30+ min | 15–30 min | Less than 15 min | |
Last meal | 45+ min ago | 30 min ago | Hungry / just ate | |
Recent event | Low-demand day | Moderate day | School, therapy, difficult event | |
Sleep last night | Normal | Slightly short | Very short / disturbed |
✅ GO
Proceed with full protocol as described in Steps 1–6.
⚠️ MODIFY
Use shortened version — fewer steps required, more reinforcement, earlier exit option.
❌ POSTPONE
Offer calming activity now, reattempt in 30 minutes. One skipped bath is better than a traumatizing bath.
"Am I regulated right now? Am I dreading this? My nervous system will telegraph my state to my child before I say a single word. Pause. Breathe. I am the co-regulator."

① of 6 Protocol Steps
Step 1: The Invitation
Every bath begins with an invitation. Never a command. The 10-minute warning sequence is the intervention — not a courtesy. Begin here, not at "time for a bath."
10 Minutes Before Bath
"Hey [name], in ten minutes we're going to have your bath. After bath, it's [preferred THEN activity]. Let me show you on the schedule." Walk to First-Then board. Point to bath picture. Point to preferred THEN. No debate, no negotiation — just information.
5 Minutes Before Bath
"Five more minutes of [current activity]. Look at the timer — see the red part? When it's gone, bath time starts." Point to timer. State calmly and return to where child can see you.
1 Minute Before Bath
"One more minute. I'm going to the bathroom to check the water. You can come see the toys when the timer ends." Walk toward bathroom — movement cues the transition physically, not just verbally.
Acceptance cues to look for: Child looks at First-Then board · Child moves toward bathroom (even reluctantly) · Child shows the timer to parent · Child asks about the THEN activity.
Resistance response: Child ignores → restate once calmly, then proceed physically toward bathroom. Child runs → stay calm, restate "Timer ended. Bath toys are waiting." Child escalates → assess Modify or Postpone.
Resistance response: Child ignores → restate once calmly, then proceed physically toward bathroom. Child runs → stay calm, restate "Timer ended. Bath toys are waiting." Child escalates → assess Modify or Postpone.

② of 6 Protocol Steps
Step 2: The Engagement
The child is moving toward the bathroom. Now deepen the draw. Each action at this stage transfers control to the child — reducing anxiety by increasing agency.
At the Bathroom Entrance
"Look — I checked the temperature. The thermometer says [color/number]. Is that okay for you? Want to check it yourself?" Hand child the thermometer. Let them confirm the water is safe. This single act transfers control and reduces anxiety.
At the Tub Edge
"Look what's in there waiting. [Name the specific toys]. The [duck] was asking about you." Point to toys, not to the demand. The tub contains something good.
Undressing Sequence
Use visual schedule if child has it — point to "undress" picture. Child can mark it as done. "You're on step [number] on the schedule. You're doing it."
Entering the Water
"Can you check if the water is right? Put one foot in first." Child's foot in first gives them control of the entry pace. "The timer is set. You can see how much bath time you have."
Reinforcement cue — deliver within 3 seconds of each step completion: "You did that. That was hard and you did it." Specific, behavioral, immediate. Timing: 1–3 minutes from bathroom entrance to in-water.

③ of 6 Protocol Steps
Step 3: The Therapeutic Action
The bath itself is therapy when you know what you're doing. Sequence matters. Regulation before washing. Announcement before touch. Consistency before expectation.
Sensory Regulation Phase (First 3–5 Minutes)
Allow unstructured water play with bath toys before washing begins. Child regulates in water, anxiety drops. Washing attempts while child is still anxious multiply resistance. This is not wasted time — it is the protocol.
Body Washing (with Gentle Sensory Tools)
Warm the washing tool in bath water first. Announce each body part before touching: "Now I'm washing your right arm." Use consistent, predictable pressure. Wash in the same body sequence every time. Offer choices: "Shall I use the silicone scrubber or the soft cloth today?"
Hair Washing (with Accommodation)
Use shampoo visor / rinse cup / rinse-free shampoo per child's tolerance. Announce: "Hair wash next. Visor on. Ready? Head forward." Time it: "Hair wash is only until the sand runs out — watch the timer." Celebrate immediately after: "Hair done. That was brave."
Child Response Spectrum:✅ Ideal — Child engages with toys, tolerates washing, refers to schedule, watches timer. ✅ Acceptable — Child complains verbally but allows washing; watches timer; accepts exit prompt. ⚠️ Concerning — Child becomes more agitated during wash, escalating — consider Adapt protocol. Duration: 10–20 minutes total.

④ of 6 Protocol Steps
Step 4: The Countdown Exit
The exit from the tub is the hardest transition. It must be gradual, visible, and inevitable. "3 good reps of the countdown > 10 forced exits." Consistency of the system is the medicine.
5 Minutes Before Exit
"Five minutes left. Look at the timer — see the red section? It's shrinking." Hold up 5 fingers simultaneously.
3 Minutes Before Exit
"Three more minutes. One toy goes to sleep." Remove one bath toy from tub — physical marker of approaching end.
2 Minutes Before Exit
"Two more minutes. Another toy goes to sleep." Remove second toy. The tub is getting quieter.
1 Minute Before Exit
"One minute. Can you see the warm towel waiting for you? And your pajamas?" Make the THEN physically visible — towel is right there.
Timer Ends
"Timer's done. The schedule says it's time. Warm towel is ready. [THEN activity] is next." Don't ask. State. Help child physically if needed — maintain warm tone throughout.
Sensory-Seeker
Remove toys earlier; lightly drain water; extra-warm towel as sensory draw out.
Anxious Child
More countdown steps (10-8-5-3-2-1); transition song playing at exit signal.
Non-Verbal Child
Visual countdown cards held up physically by parent — no words required.

⑤ of 6 Protocol Steps
Step 5: Reinforce & Celebrate
Timing matters more than magnitude. Within 3 seconds. Every time. Specific praise anchors the exact behavior you want repeated — generic praise ("good job!") tells the child nothing useful.
For entering the bath
"You got in. I saw how hard that was. You did it."
For tolerating hair wash
"Hair done. You were so brave for that."
For exiting on timer
"You heard the timer and you got out. That was huge."
For completing full routine
"You did the whole schedule. Every step. That's something to be proud of."
Reinforcement Type | Examples | When to Use | |
Natural consequence | Start the THEN activity immediately | Every bath | |
Token / Sticker | ⭐ Sticker on bath chart | Daily | |
Verbal | Specific praise statement | Every step | |
Tangible | Small preferred treat | New milestones | |
Social | 5 minutes preferred parent play | Weekly goal met |
"Celebrate the attempt, not just the success. 'You tried hair washing today even though it was hard. That counts. That's data. That's progress.'"

⑥ of 6 Protocol Steps
Step 6: The Cool-Down (Post-Bath Regulation)
Getting out of the water is its own sensory transition. Do it right. The warm-to-cold shift, the wet-to-dry tactile change — these are neurological events that require intentional support.
The entire post-bath sequence should flow within 90 seconds — warm, purposeful, and leading directly to the promised THEN activity. Delay between exit and reward breaks the contingency that makes the timer work.
"Exhale. The bath is over. Your voice needs to celebrate, not collapse with relief. The child is reading your state. Warm, calm completion — not 'finally it's over' energy."
🐻 A specific stuffed animal or comfort toy that "waits" outside the tub and is reunited post-bath creates a reliable anchor for the exit transition. Soft Animal Comfort Toy — ₹425 →

60 Seconds of Data Now Saves Hours of Guessing Later.
What to Record (simple version)
Data Point | How to Record | Why It Matters | |
Entry: How many prompts to get in? | Tally (0, 1, 2, 3+) | Tracks transition compliance trend | |
Exit: Meltdown at timer? | Yes/No | Tracks exit regulation | |
Hair wash: Completed? | Yes/No/Partial | Tracks sensory tolerance | |
Overall rating: 1–5 | Single number | Tracks family functioning |
Form Fields
- Date
- Entry compliance (1–5 scale)
- Exit compliance (1–5 scale)
- Any meltdowns? Yes/No
- Hair washing completed? Yes/No
- Overall session rating (1–5)
- Notes (one sentence)
Trend Awareness
"3 bad baths in a row means something changed — check sleep, illness, school stress, schedule disruption. 3 good baths in a row means the system is working — don't change it."
This data feeds your child's Daily Living Transition Readiness Index in the GPT-OS® platform. Your 60 seconds tonight makes tomorrow's recommendation smarter.

Session Abandonment Is Not Failure. It Is Data. Let's Decode It.
The 7 most common bath time failure modes — and what to do next time.
① Child refused to enter bathroom at all
Why: Transition demand was too abrupt despite warnings, or baseline dysregulation too high.
Next time: Extend warning sequence to 15 minutes. Add First-Then before entering bathroom zone. Check Readiness more carefully.
Next time: Extend warning sequence to 15 minutes. Add First-Then before entering bathroom zone. Check Readiness more carefully.
② Child entered but screamed through entire wash
Why: Likely sensory trigger — specific tool, water temperature, sequence surprise.
Next time: Identify the specific trigger (log it). Switch washing tool. Slow down. Announce every touch before making it.
Next time: Identify the specific trigger (log it). Switch washing tool. Slow down. Announce every touch before making it.
③ Hair washing caused complete meltdown
Why: Water-on-face is a vestibular + tactile double trigger — most common failure point.
Next time: Try rinse-free shampoo. Introduce visor for one bath before rinsing with it. Do hair washing at a separate time if needed.
Next time: Try rinse-free shampoo. Introduce visor for one bath before rinsing with it. Do hair washing at a separate time if needed.
④ Timer ended but child refused to get out
Why: Timer is new — trust in its authority isn't established yet. Or the THEN activity isn't compelling enough.
Next time: Upgrade the THEN reward. Honor the promise every single time without exception.
Next time: Upgrade the THEN reward. Honor the promise every single time without exception.
⑤ Great entry but meltdown post-bath during drying
Why: Post-bath sensory transition (temperature change + tactile drying) was dysregulating.
Next time: Warmer towel. Slower, firmer drying pressure. Move from wet to warm faster.
Next time: Warmer towel. Slower, firmer drying pressure. Move from wet to warm faster.
⑥ Works some nights but not others
Why: Normal. Regulatory capacity varies with accumulated daily stress. The inconsistency IS the data.
Next time: Compare "good bath" days vs "bad bath" days — sleep, school, diet. Find the pattern.
Next time: Compare "good bath" days vs "bad bath" days — sleep, school, diet. Find the pattern.
⑦ Child became physically aggressive during bath
Next step: This is a red flag. Consult the Red Flags card and contact Pinnacle helpline: 9100 181 181
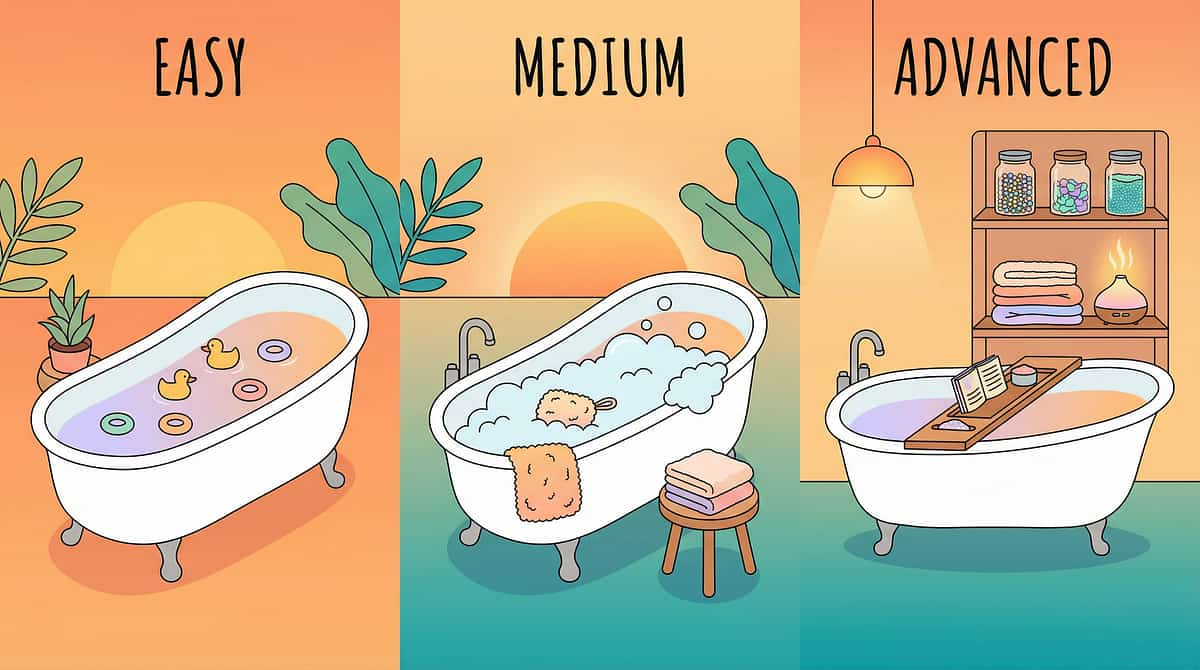
No Two Children Are Identical. Here's How to Tune This Protocol to Yours.
← Easier Version
High-stress days or skill-building phase: 15–20 min warning, 10 min bath, washing limited to essentials, hair washing skipped or separate, more reinforcement, lower expectations.
Balanced Version
Standard protocol most days — full sequence as described in Steps 1–6. This is the target operating mode for weeks 2 onward.
Harder Version →
Mastery phase: Fade visual supports gradually. Child sets the timer themselves. Child washes own body with guidance fading. Child announces readiness to exit rather than waiting for timer.
Sensory-Seeker (Loves Water, Hard to Exit)
Progressive toy removal during countdown · Slightly drain water as environmental cue · Very warm towel as "pull" out of tub · Extra-brief cozy post-bath snuggle as THEN.
Sensory-Avoider / Tactile Defensive
Temperature checking ritual is child-controlled · Child chooses all washing tools from a small menu · Child's own hand guides parent's hand during hair wash · Every touch announced before contact · Deep pressure post-bath.
Non-Verbal / Minimally Verbal Child
Real photos on visual schedule (not drawings) · Timer must be highly visual (red disc, not digital) · PECS-style choice boards for tool selection · More physical guidance with verbal narration.
Older Child (8–10 Years)
Child creates own schedule with parent guidance · Child self-monitors with timer · Child chooses THEN from approved menu · Gradually transfer all self-care steps to child.

ACT IV — THE PROGRESS ARC
Weeks 1–2: Installation, Not Mastery.
Here's what real progress looks like in the Foundation Phase.
15%
Foundation Phase
Weeks 1–2 are the trust-building and pattern-establishment phase. The system is being installed.
3min
Measurable Neurological Adaptation
If your child tolerates the bath for 3 minutes longer than last week, that is real progress — even if you can't see it yet.
✅ What You Should See (Realistic)
- Child recognizes the First-Then board is associated with bath time
- Timer creates slightly less explosive exit reaction (even if still difficult)
- At least one bath this week was shorter and less distressing than before
- Child begins to look at the visual schedule without being prompted
- Hair washing completed at least once with the new tool
⏳ What Is NOT Progress Yet (And That's Okay)
- Child enthusiastically going to bath (that's week 6+)
- Zero meltdowns (weeks 3–4 goal)
- Exit compliance without protest (weeks 2–4 goal)
📞 Need Support in Week 1?
If Week 1 is crisis-level — call 9100 181 181. Our OT team can guide you through it.

Weeks 3–4: The Schedule Is No Longer New.
Your child's brain has begun to expect it. Synaptic pathways connecting "bath time announcement" → "schedule appears" → "safety signal" are strengthening. Predictability = safety. Safety = reduced threat response = reduced meltdown.
40%
Neural Pathway Formation Phase
The nervous system is learning that bath time is predictable — and predictability is the mechanism of change.
✅ Consolidation Indicators (specific, observable)
Child walks toward bathroom within 3 minutes of timer announcement without physical guidance · Child checks visual schedule without prompting · Child references timer during bath: "How much time left?" · Hair washing protest has decreased in duration or intensity · At least 2 baths this week completed without full meltdown · Child mentions "First-Then" concept spontaneously.
What Parents Notice at This Stage
"I'm less anxious myself when I say 'bath time.' That changes the energy I bring into the bathroom, which changes my child's response. We're both regulating together."
When to Increase Intensity
If child is mastering entry → begin working on exit compliance more specifically. If exit is mastered → begin hair washing tolerance building. Never work on two new fronts simultaneously.

Weeks 5–8: Mastery Doesn't Mean Perfect. It Means Consistent, Manageable, and Child-Led.
75%
Mastery Phase 🏆
The routine is reliably predictable and the child is beginning to self-manage key elements of the protocol.
Criterion | Mastery Definition | How to Measure | |
Entry compliance | Into bathroom within 5 min of announcement, ≤1 prompt | Track over 5 baths | |
Routine following | Completes 5+ of 7 routine steps with visual schedule | Check schedule marks | |
Exit compliance | Exits within 2 min of timer end, ≤1 protest | Timer data log | |
Sensory tolerance | Accepts full wash including hair, ≤1 complaint stop | Session log | |
Generalization | Routine holds in new bathroom (travel/grandparents) | Field test |
🏆 BATH TIME MASTERY BADGE awarded when: 5 consecutive baths completed with ≤1 prompt for entry, ≤1 protest at exit, hair wash completed 3 of 5 baths.
Generalization Indicators (highest mastery marker): Child manages bath routine at grandparents' house · Child announces "bath time" approaching before parent does · Child selects own washing tools and timer duration · Child teaches a sibling the routine.

Even After Success, These Signs Mean Pause and Call.
🔴 Physical Aggression During Bath
Child hits, bites, scratches, or throws objects during bath time in a way that creates safety risk.
Action: Pause protocol. Call Pinnacle: 9100 181 181 for behavioral consultation.
Action: Pause protocol. Call Pinnacle: 9100 181 181 for behavioral consultation.
🔴 Complete Water Avoidance / Phobia
After 4+ weeks of consistent protocol, child still cannot tolerate any water contact despite all accommodations.
Action: OT sensory integration therapy clinic evaluation needed — beyond home-based capacity.
Action: OT sensory integration therapy clinic evaluation needed — beyond home-based capacity.
🔴 Sudden Regression After Established Routine
Child who was managing bath suddenly returns to week-1 levels of distress after weeks of progress.
Action: Medical evaluation first (ear infection, skin sensitivity, illness). Then behavioral review.
Action: Medical evaluation first (ear infection, skin sensitivity, illness). Then behavioral review.
🔴 Self-Injurious Behavior
Child bangs head, bites self, or otherwise injures during bath time.
Action: Immediate professional consultation. Do not continue bath protocol without therapist guidance.
Action: Immediate professional consultation. Do not continue bath protocol without therapist guidance.
🔴 Significant Sleep/Eating Disruption
Bath time battles are now disrupting sleep onset or appetite.
Action: Teleconsultation with Pinnacle NeuroDev team.
Action: Teleconsultation with Pinnacle NeuroDev team.
🟡 AMBER — Monitor: Meltdown duration increasing despite consistent protocol (>Week 3) · New sensory sensitivity appearing during bath · Child making statements about fear that seem disproportionate.
Escalation Pathway: Self-resolve (home protocol adjustment) → Pinnacle Teleconsultation → Clinic Visit (OT + Behavioral Assessment) → Intensive Intervention Program
📞FREE HELPLINE: 9100 181 181 | Available 16 languages | pinnacleblooms.org
📞FREE HELPLINE: 9100 181 181 | Available 16 languages | pinnacleblooms.org

You're Not Done. You're on a Developmental GPS. Here's What's Next.
Bath entry was hardest
→ Next: I-793 Dressing Transitions (same entry challenge pattern)
Sensory issues dominated
→ Next: I-810 Sensory Integration Deep Dive
Exit compliance was biggest win
→ Next: I-792 Bedtime Transitions (applies same timer/countdown system)
Hair washing remains impossible
→ Specialist technique: Hair Washing Desensitization Protocol
From "I Dread Bath Time Every Night" to "She Sometimes Asks for a Bath."
Arjun, 5 years, Chennai — Before
"Bath time started 45 minutes before the bath — the screaming started the moment we walked near the bathroom. We were physically carrying him in while he kicked. Once in the water he'd be fine, but getting him out was another 30-minute war. We dreaded it every single night."
Arjun, 5 years, Chennai — After (Week 7)
"Last Tuesday he pointed to the bath picture on his schedule before I said anything. He still protests at the timer sometimes, but it's 5 minutes, not 45. Hair washing is still hard — we use the rinse cup now — but it's manageable. We don't dread evenings anymore."
"Arjun's case illustrates the transition-dominant pattern. His bath sensory tolerance was actually adequate — the dysregulation was entirely in the entry and exit transitions. Visual schedule + countdown exit solved 80% of the challenge before we even addressed the sensory components." — OT Specialist, Pinnacle Chennai Center
Priya, 7 years, Hyderabad — Before
"Hair washing was the worst thing in our lives. She would scream like we were hurting her. I was washing her hair once every two weeks because I couldn't face it more often."
Priya, 7 years, Hyderabad — After (Weeks 3–6)
"Week 3, I used the rinse-free shampoo for the first time. She didn't scream. I cried. Week 6, she let me use the visor for a water rinse. Two weeks ago she asked me to do it herself."
"Hair washing distress is vestibular + tactile + unpredictability triple activation. We rarely need to eliminate all triggers — neutralizing the dominant ones changes the entire experience." — OT Specialist, Pinnacle Hyderabad (via teleconsult)
Note: Illustrative cases. Outcomes vary by individual profile, severity, and implementation consistency.

The Questions Every Parent Asks After Reading This Guide.
Q1: My child is 9 years old. Is it too late to start?
No. The brain retains neuroplasticity throughout childhood and into adolescence. 9 is not late — it is a different starting point. The protocol may need adaptation for a 9-year-old's self-awareness and emerging autonomy (let them help design the schedule, choose the timer, select the THEN activity). Outcomes may take slightly longer to achieve but are absolutely possible.
Q2: We've tried visual schedules before and they didn't work. Why would this be different?
The most common reason visual schedules fail: introduced during crisis (not before), inconsistently used, or the THEN reward wasn't motivating enough. This protocol uses visual schedules as one layer within a multi-tool system. Implementation matters more than the tool itself. Have you tried them in the full sequence described in Steps 1–6?
Q3: My child can't read. Will this still work?
Yes. This protocol uses pictures, not words. Real photos of your own bathroom, your own child's routine, work better than symbols for most children. The timer uses visual depletion (red disc shrinking), not numbers. All tools are visual or physical — reading is not required.
Q4: How do I handle it when the THEN activity isn't motivating anymore?
Rotate THEN options regularly. Keep a list of 5–6 highly preferred activities and rotate them so no single one loses its motivating value. Let the child choose from the menu — self-selection increases engagement. Survey what's currently capturing your child's interest and add it temporarily.
Q5: My partner doesn't believe in these tools. They think we should just "be firm."
This is an extremely common family disagreement. Without the right tools, "being firm" escalates into physical confrontation, which creates trauma associations that take months to reverse. Share the brain science card and the evidence grade card. Invite them to try the protocol for 3 weeks before evaluating. Results are the most persuasive argument.
Q6: Can I use this with a child who has no diagnosis?
Yes. Many neurotypical children experience bath time transition difficulties as a normal developmental phase, especially between ages 2–5. These tools support any child whose nervous system is struggling with transitions and sensory demands — diagnosis or not.
Q7: What's the minimum — if we can only do one thing?
The visual timer for the exit transition. If your child's biggest challenge is getting OUT of the bath, a visible countdown timer that they can watch reduces the surprise element of the ending — which is the primary meltdown trigger for most children. Start there.
Q8: How long before I should expect to see improvement?
First signs: Week 1–2. Meaningful reduction in meltdown frequency: Week 3–4. Reliable compliance: Week 5–8. Full mastery: 8–16 weeks with consistent daily implementation. Progress is not linear — expect good weeks and bad weeks. The trend over 4 weeks matters more than any single bath.
Didn't find your answer? → Ask GPT-OS®: pinnacleblooms.org/ask → Book teleconsultation: pinnacleblooms.org/teleconsult → Call FREE helpline: 9100 181 181 (16 languages, 24×7)
Preview of 9 materials that help with bath time transition Therapy Material
Below is a visual preview of 9 materials that help with bath time transition therapy material. The pages shown help educators, therapists, and caregivers understand the structure and content of the resource before use. Materials should be used under appropriate professional guidance.



















Share this resource
Help others discover thisLink copied!

From Fear to Mastery. One Technique at a Time.
— The Pinnacle Blooms Consortium
Our Mission
"We exist to transform every home into a proven, personalized, multi-disciplinary pediatric therapy environment — available 24×7, guided by GPT-OS® intelligence, validated by 20 million real sessions, and built on the belief that every child deserves the tools their nervous system needs to thrive."
Consortium Disciplines
🟤 Occupational Therapy | 🔵 Speech-Language Pathology | 🟣 ABA/BCBA | 🟢 Special Education | ⚕️ NeuroDev Pediatrics | 🔬 Clinical Research Organization
Medical Disclaimer
This content is educational in nature and does not replace individualized professional assessment and intervention. Persistent transition difficulties, sensory processing differences, and self-care challenges may be associated with autism spectrum disorder, ADHD, sensory processing disorder, anxiety disorders, and other conditions requiring clinical evaluation. If challenges are severe, persistent, or involve safety concerns, please consult a qualified occupational therapist, developmental pediatrician, or behavioral specialist. Individual results vary by underlying condition, severity profile, implementation consistency, and child-specific factors.
Statutory Identifiers
© 2025–2026 Pinnacle Blooms Network® | Unit of Bharath Healthcare Laboratories Pvt. Ltd.
CIN: U74999TG2016PTC113063 | DPIIT: DIPP8651 | MSME: Udyog Aadhaar TS20F0009606 | GSTIN: 36AAGCB9722P1Z2
GPT-OS®, AbilityScore®, TherapeuticAI®, FusionModule™, EverydayTherapyProgramme™ are registered marks / proprietary assets of Bharath Healthcare Laboratories Pvt. Ltd. All rights reserved.
CIN: U74999TG2016PTC113063 | DPIIT: DIPP8651 | MSME: Udyog Aadhaar TS20F0009606 | GSTIN: 36AAGCB9722P1Z2
GPT-OS®, AbilityScore®, TherapeuticAI®, FusionModule™, EverydayTherapyProgramme™ are registered marks / proprietary assets of Bharath Healthcare Laboratories Pvt. Ltd. All rights reserved.
← Previous: I-790 Mealtime Transitions
🔄 Return to Top
→ Next: I-792 Bedtime Transitions
Browse All Techniques → | Pinnacle Home → | 📞FREE Helpline: 9100 181 181 | Built by Mothers. Engineered as a System.
