
His hands reach before his brain can stop them.
You're at the grocery store. His fingers trail across every surface — the cold metal shelves, the rough cardboard boxes, the smooth plastic bottles. At home, he touches the walls as he walks down the hallway. He grabs your face, presses his palm against the TV screen, runs his fingers through the rice container you forgot to close. People stare. Family members say "just tell him to stop." But you've tried. A thousand times. He can't stop. Because this isn't defiance.
When touching isn't a behavior problem — it's a nervous system that needs input.
You are not failing. Your child's nervous system is speaking. And now you'll learn exactly how to answer it.
🛡️ Pinnacle Blooms Consortium — OT • ABA • SLP • SpEd • NeuroDev

You Are Not Alone — The Numbers
The constant touching, grabbing, and seeking is one of the most frequently reported sensory behaviors by parents across every continent, culture, and economic class. This is not a rare problem — and it has proven solutions.
—
Sensory Difficulties
of children with autism display sensory processing difficulties — tactile seeking is among the most common presentations
—
ASD Prevalence
children in the United States are diagnosed with ASD (CDC, 2023); India estimates 1 in 100 (INCLEN, 2018)
—
Families Worldwide
families worldwide are navigating sensory processing challenges in their children right now
You are among millions of families navigating this exact challenge.
📚 PRISMA Systematic Review (Children, 2024) | PMC11506176 · Meta-analysis: World J Clin Cases, 2024 | PMC10955541 · CDC MMWR, 2023 | INCLEN Study, Indian J Pediatr, 2018

What's Happening in Your Child's Brain

Your child's somatosensory cortex — the brain's touch processing center — is under-registering tactile input. Think of it like a radio with the volume turned too low. The brain needs the signal louder, more intense, more frequent to register that touch has occurred.
So your child's hands reach for everything — not because they want to misbehave, but because their brain is turning the volume dial up, desperately trying to hear the signal.
This is called tactile hypo-responsiveness or tactile seeking. The nervous system's registration threshold for touch input is higher than typical, requiring more intense or more frequent tactile stimulation to achieve neurological satisfaction.
This is a wiring difference, not a behavior choice.
When you understand this, everything changes. You stop fighting the need. You start feeding it — strategically, with the right materials, at the right dose, in the right way.
📚 Frontiers in Integrative Neuroscience (2020) | DOI: 10.3389/fnint.2020.556660 · Dunn's Model of Sensory Processing — neurological threshold framework

Where This Sits in Development
Ages 2–7 are when tactile seeking behaviors become most visible and most concerning for parents. This is also the most responsive window for intervention — the brain's neuroplasticity is at peak capacity.
0–12 Months
Mouthing and sensory exploration is developmentally expected
12–24 Months
Exploratory touching is appropriate and healthy at this stage
2–4 Years ★
PEAK SEEKING PERIOD — Tactile seeking may intensify if nervous system needs aren't met
4–7 Years
Modulation period — sensory diet strategies take hold with consistent intervention
7+ Years
Self-regulation with minimal external support becomes achievable
What commonly co-occurs: Proprioceptive seeking (crashing, jumping, pushing), oral seeking (mouthing non-food items), difficulty with fine motor tasks, challenges with self-regulation during transitions.
Here is where we're heading: From uncontrolled seeking → structured seeking → self-regulated modulation → independent sensory management.
📚 WHO Care for Child Development (CCD) Package | PMC9978394 · UNICEF MICS Developmental Indicators (197 countries) · WHO/UNICEF CCD Implementation Report (2023)

The Evidence Behind This Technique
🛡️ EVIDENCE LEVEL: I–II (Systematic Review + RCTs)
80%
Strong Evidence Base
Confidence meter reflecting robust research across multiple study designs
16 studies (2013–2023) confirm sensory integration intervention meets criteria as evidence-based practice for children with ASD. A 2024 meta-analysis across 24 studies demonstrated that sensory-material-based interventions effectively promote social skills, adaptive behavior, sensory processing, and motor development.
Key Finding: Home-based sensory interventions using structured materials produced statistically significant improvements in tactile modulation, with Indian RCT data confirming parent-administered protocols achieve clinical outcomes comparable to clinic-based delivery.
Effect Size: Moderate-to-large across sensory processing and adaptive behavior domains (d = 0.45–0.78).
Clinically validated. Home-applicable. Parent-proven.
📚 PRISMA Systematic Review (Children, 2024) | PMC11506176 · Meta-analysis (World J Clin Cases, 2024) | PMC10955541 · Padmanabha et al., Indian J Pediatr, 2019 | DOI: 10.1007/s12098-018-2747-4 · NCAEP Evidence-Based Practices Report (2020)

Technique A-030
Domain A — Sensory Processing
Structured Tactile Satiation Protocol
Parent-Friendly Name: "Feed the Hands" — 9 Materials for Constant Touching
Definition
A multi-material sensory regulation intervention that provides structured, high-intensity tactile input through 9 evidence-based material categories, designed to satisfy the nervous system's tactile hunger so that uncontrolled touching of inappropriate surfaces and objects decreases. The child's hands receive what they need — so they stop seeking what they shouldn't.
Domain
A — Sensory Processing & Regulation
Age Range
2–12 years (with modifications)
Session Duration
10–20 minutes
Frequency
2–3 times daily (sensory diet integration)
Difficulty
Intro → Core (9 levels)
Canon Materials: Fidget Tools, Sensory Bins, Therapy Putty/Dough, Textured Clothing, Weighted Blanket, Brushing Protocol Tools, Heavy Work Equipment, Touch-and-Feel Books/Boards, Texture Zones

Who Uses This Technique — The Consortium Behind It
This technique crosses therapy boundaries because the brain doesn't organize by therapy type.
Occupational Therapist (OT) — Primary Lead
Designs the sensory diet, selects materials based on the child's Sensory Profile® assessment, determines dosage and intensity. The OT calibrates which of the 9 materials your child needs most and in what sequence.
Board Certified Behavior Analyst (BCBA)
Structures the reinforcement schedule, tracks behavioral data on touching frequency, applies functional analysis to determine if the touching serves a sensory function vs. attention function. Ensures the sensory protocol reduces problem behavior measurably.
Speech-Language Pathologist (SLP)
Addresses oral tactile seeking that often co-occurs (mouthing, licking). Integrates tactile regulation into communication sessions where the child needs to be regulated to attend and respond.
NeuroDevelopmental Pediatrician
Rules out medical causes for excessive tactile seeking, monitors for neurological red flags, adjusts medication interactions if applicable. Confirms the sensory profile diagnosis.
📚 Adapted UNICEF/WHO Nurturing Care Framework for SLPs (2022) | DOI: 10.1080/17549507.2022.2141327

What This Targets — Precision, Not Randomness
Observable Behavior Indicators: Before — child touches 15+ inappropriate surfaces per hour → After — child self-directs to appropriate sensory material when need arises.
📚 Meta-analysis (World J Clin Cases, 2024) | PMC10955541

What You Need — The 9 Materials
Every material serves a precise neurological purpose. Below is the complete clinical material set — with what it does, why it works, and what it costs.
# | Material | What It Does | Price Range | |
1 | Fidget Toys | Pop-its, tangles, spiky balls, chain links, sensory rings — gives hands an acceptable outlet. When hands have something appropriate to touch, they don't need to touch everything else. | ₹100–800 | |
2 | Sensory Bins | Rice, sand, water beads, pasta, dried beans with scoops/cups — floods the system with high-volume tactile input. After hands dig through rice and sand, they don't need to grab everything in sight. | ₹300–1,500 | |
3 | Therapy Putty + Dough | Resistive putty, playdough, kinetic sand, slime — resistive touch that regulates. Hands that squeeze and stretch don't need to grab everything else. | ₹200–800 | |
4 | Textured Clothing | Fleece, corduroy, sherpa, velvet, textured inner-seam garments — wearable tactile input all day. When satisfying texture is worn on the body, hands need less from everything else. | ₹500–2,000 | |
5 | Weighted Blanket / Lap Pad | 5–10% of child's body weight, glass bead or poly-pellet fill — deep pressure calms seeking. When the body feels grounded, hands don't need to reach everywhere. | ₹1,500–6,000 | |
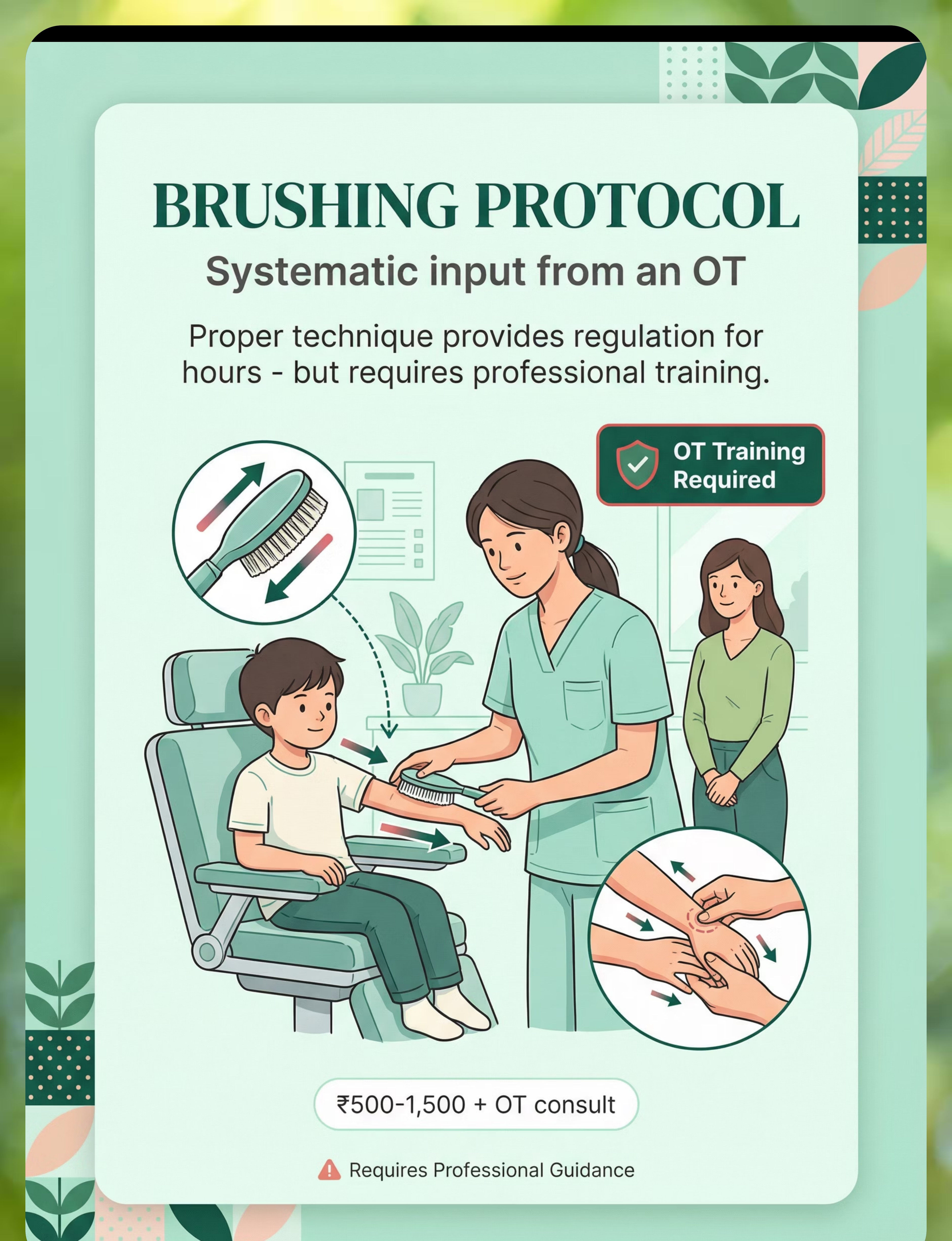
6 | Brushing Protocol Tools | Wilbarger-type surgical brush + joint compression — systematic OT-guided input that provides regulation for hours. ⚠️ Requires professional OT training. | ₹500–1,500 + OT consult | |
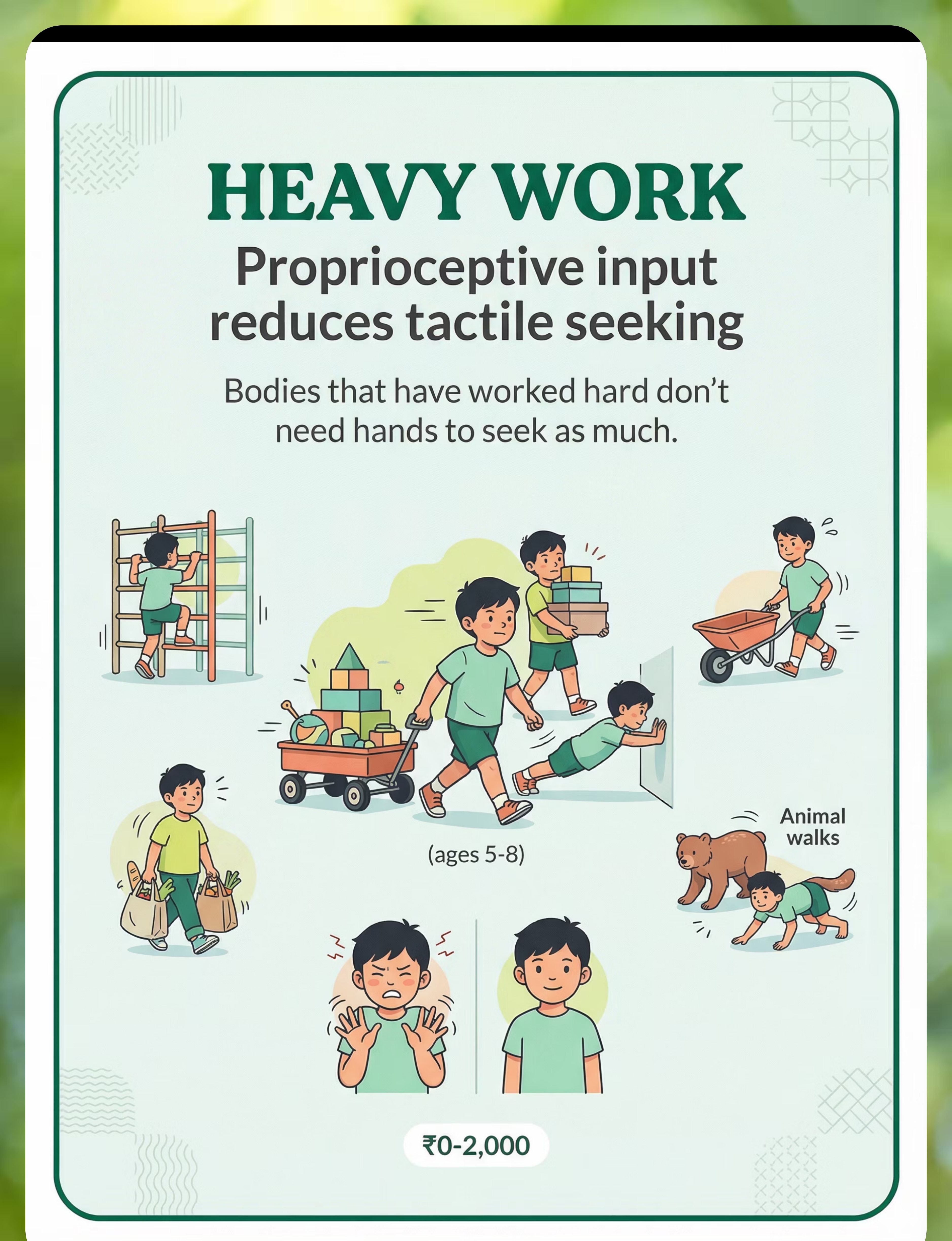
7 | Heavy Work Activities | Carrying, pushing, pulling, climbing, animal walks, wheelbarrow walks — proprioceptive input reduces tactile seeking. Bodies that have worked hard don't need hands to seek as much. | ₹0–2,000 | |
8 | Touch-and-Feel Books / Texture Boards | Multi-texture books, fabric sample boards, texture matching games — structured exploration for tactile curiosity. When curiosity has an appropriate outlet, random touching decreases. | ₹300–1,500 | |
9 | Texture Zones | Dedicated wall/floor area with varied textures — cork, carpet, bubble wrap, felt, faux grass. Design the environment for touching. Give permission and outlet where it's welcome. | ₹500–5,000 |
Total Investment Range: ₹3,900–21,100 (start with materials 1–3 for under ₹1,500)
🏅 Pinnacle Recommends — Clinically Validated Material Selection

Can't Buy It? Make It. Zero-Cost Alternatives That Work.
Every parent, regardless of economic status, can execute this technique TODAY. The WHO Nurturing Care Framework emphasizes equity-focused interventions using household materials — validated across 54 low- and middle-income countries.
Buy This | Make This (₹0) | Why It Works | |
Fidget toys (₹100–800) | Rubber bands on a water bottle, paper clips linked in a chain, smooth stones from outside | Same fine motor engagement + tactile feedback loop | |
Sensory bin (₹300–1,500) | Steel thali filled with raw rice + 5 hidden small toys + 2 spoons | Identical proprioceptive-tactile flooding mechanism | |
Therapy putty (₹200–800) | Homemade atta dough (2 cups atta + ½ cup oil + water) or wet sand | Same resistive input; add turmeric for color | |
Textured clothing (₹500–2,000) | Safety-pin a piece of velvet/silk/jute inside shirt collar or cuff | Continuous tactile contact at same body points | |
Weighted blanket (₹1,500–6,000) | Fill a pillowcase with 1–2 kg of rice, sew shut | Same deep pressure principle (ensure 5–10% body weight) | |
Touch-and-feel boards (₹300–1,500) | Glue fabric scraps (silk, sandpaper, cotton, jute, foam) onto cardboard squares | Identical texture discrimination training | |
Texture zone (₹500–5,000) | Tape different materials (bubble wrap, felt, sandpaper, towel, foil) to one wall section | Same environmental design principle |
⚠️Non-Negotiable Exception: The Wilbarger Brushing Protocol (Material #6) requires a specific surgical-grade brush AND professional OT training. Do NOT substitute. Do NOT attempt without guidance.
📚 WHO Nurturing Care Framework (2018) — equity-focused interventions | PMC9978394 · CCD Package — household-material intervention efficacy across 54 LMICs

⚠️ Safety First — Read Before You Begin
🔴 DO NOT PROCEED IF
- Child has open wounds, skin infections, or eczema flare on hands/arms
- Child is in active meltdown or severe distress (wait for calm)
- Child has known allergy to any material (latex, wheat/gluten in dough, specific fabrics)
- Child is under 2 years — choking hazard with small sensory bin items
- Brushing protocol attempted WITHOUT trained OT guidance
🟡 MODIFY AND MONITOR
- Child has tactile defensiveness IN ADDITION to seeking (mixed profile) — start with only materials the child voluntarily approaches
- Child mouths/eats non-food items — use only food-safe sensory bin fillers (rice, pasta, lentils) and supervise constantly
- Weighted blanket — NEVER exceed 10% of child's body weight; NEVER use during sleep for children under 5 without pediatric clearance
🟢 SAFE TO PROCEED WHEN
- Child is fed, rested, and in a relatively calm/alert state
- Environment is clear of genuine hazards (sharp objects, fragile items)
- You have 15–20 minutes of uninterrupted time
- You've read the full protocol (Cards 13–19)
RED LINE — Stop immediately if you observe: Child becomes severely distressed (not just mildly resistant) · Skin irritation, redness, or allergic reaction · Child stuffs material into nose, ears, or swallows non-food items · Breathing difficulty with weighted items
📚 Padmanabha et al., Indian J Pediatr, 2019 — home-based safety protocols | DOI: 10.1007/s12098-018-2747-4

Set Up Your Space — The Sensory Station

Station Layout
01
Texture Zone
Wall-mounted panel with varied textures (cork, carpet, bubble wrap, felt)
02
Floor Mat
Washable covering under sensory bin area for easy cleanup
03
Sensory Bin + Materials
Laid out in order of use — not all at once
04
Parent Position
Seated BESIDE child (not across — parallel play position)
05
Storage Basket
Child-reachable basket with fidgets, putty, and touch books
Setup Checklist:✅ Visual timer visible to child (if used to visual schedules) · ✅ One "finished" basket for materials when done · ✅ Quiet environment — no TV, minimal background noise · ✅ Temperature comfortable (tactile processing is affected by cold) · ✗ REMOVE: TV/tablet, breakable items, distracting toys, clutter
📚 Ayres Sensory Integration Theory — environmental setup as core principle | PMC10955541

ACT III: THE EXECUTION
Is Your Child Ready? — 60-Second Pre-Flight Check
Check | Ready? | |
Child has eaten within the last 2 hours | ✅ / ❌ | |
Child has slept adequately (not overtired) | ✅ / ❌ | |
Child is not in active meltdown or crying | ✅ / ❌ | |
Child is not ill (fever, stomach upset, congestion) | ✅ / ❌ | |
No significant stressor in the last 30 minutes | ✅ / ❌ | |
Child is not engrossed in a preferred activity | ✅ / ❌ |
All ✅ → GO
Begin with Step 1 (Card 14)
1–2 ❌ → MODIFY
Use simplified version: offer just 1 fidget toy or 2 minutes of putty play. No full protocol today.
3+ ❌ → POSTPONE
Offer a calming activity instead (deep pressure hug, weighted blanket, quiet book). Try again in 2–3 hours.
The best session is one that starts right.

STEP 1 of 6
The Invitation — Bring Your Child In
⏱️ Duration: 30–60 seconds
"Look what I have for your hands today! Want to come feel this with me?"
Present ONE material — the one your child is most likely to approach willingly. Start with the easiest "yes." If your child loves squishy textures, start with putty. If they love digging, start with the sensory bin.
Body Language
- Sit on the floor at child's level
- Hold the material in your own hands first (modeling)
- Smile. No urgency. No demand.
- Offer, don't insist.
Reading Your Child's Response
Acceptance looks like: Child approaches, reaches for material, looks interested, moves toward you.
Resistance looks like: Child turns away, says no, moves to another part of the room → Wait 30 seconds. Try once more. If still no, offer a different material. If still no, postpone — this is data, not failure.

STEP 2 of 6
The Engagement — Hands Meet Material
⏱️ Duration: 1–3 minutes
"Feel how squishy/bumpy/heavy this is! Your hands really like this, don't they?"
Material Introduction Protocol
- Place the material IN the child's hands (or near them if the child prefers to self-initiate)
- Let the child explore freely for 30–60 seconds — NO instructions yet
- Narrate what you see: "You're squeezing it so hard!" "Your fingers found the bumpy part!"
- Match the child's energy — if they're vigorous, mirror that enthusiasm
Engaged
Eyes on material, hands active, body calm or excited in a regulated way → Continue
Tolerating
Minimal interaction but not pulling away → Give more time, add gentle narration
Avoiding
Pushing away, whining, turning head → Switch to a different material from the 9
Reinforcement Cue: When the child engages for more than 10 seconds, deliver specific praise: "Your hands are doing such great work exploring that!"

STEP 3 of 6
The Therapeutic Action — Feeding the Nervous System
⏱️ Duration: 5–10 minutes (core therapeutic window)
This is the main event. The child's hands are now actively receiving structured tactile input. Your job is to sustain engagement and deepen the sensory experience.
Fidget Toys
Guide through different grip patterns — squeeze with whole hand, pinch with two fingers, roll between palms, press with thumbs. Each grip pattern activates different mechanoreceptors.
Sensory Bin
Hide 5 small objects inside. Ask the child to find them using only touch (no looking). This transforms random digging into purposeful tactile discrimination.
Putty / Dough
Progress from free squeeze → roll into a snake → pull apart → flatten → hide small objects inside for the child to extract. Each action increases proprioceptive-tactile integration.
Weighted Blanket / Lap Pad
Place across the child's lap during a quiet tabletop activity. The deep pressure organizes the nervous system's baseline arousal, reducing the drive to seek through the hands.
Heavy Work
Carry a basket of books from one room to another. Push a loaded laundry basket. Wheelbarrow walks. Animal walks — bear walk, crab walk. Intense proprioceptive input calms tactile seeking.
Duration of Exposure: The child dictates pace within your time frame. If deeply engaged at 10 minutes, let them go to 15. If they lose interest at 5 minutes, that's today's dose. Don't force.
Ideal
Calm, focused, hands busy, body relaxed
Acceptable
Intermittent engagement, some breaks, returns to material
Concerning
Escalating dysregulation, distress → Move to cool-down (Card 19)

STEP 4 of 6
Repeat & Vary — Therapeutic Dosage
⏱️ Duration: 3–5 minutes · Target Repetitions: 3–5 cycles with variations each cycle
Variation Within a Session — Rotate Through 2–3 Materials
1
Cycle 1
Putty squeeze (60 seconds)
2
Cycle 2
Sensory bin treasure hunt (90 seconds)
3
Cycle 3
Texture board matching game (60 seconds)
Why Vary? Different materials activate different mechanoreceptor types — Meissner's corpuscles for light touch, Pacinian corpuscles for deep pressure, Ruffini endings for sustained stretch. Variety = comprehensive nervous system satiation.
Satiation Indicators — The Child Has Had Enough When:
- Hands slow down naturally
- Child looks away or toward another activity
- Body posture changes from alert to droopy
- Child says "all done" or pushes materials away gently
3 good repetitions are worth more than 10 forced ones.

STEP 5 of 6
Reinforce & Celebrate — The Power of Immediate Praise
"Your hands worked SO hard today! Look at everything they explored! You touched the squishy putty, you dug through the rice, you felt all those textures. Your hands are strong and smart!"
Timing: Within 3 seconds of the desired behavior or session end
Specificity: Name WHAT they did, not just "good job"
Enthusiasm: Match or slightly exceed the child's energy level
Specificity: Name WHAT they did, not just "good job"
Enthusiasm: Match or slightly exceed the child's energy level
Reinforcement Menu Options
01
Verbal Praise
Always — specific, immediate, enthusiastic
02
Physical Celebration
High-five or preferred physical celebration
03
Preferred Activity Access
2–3 minutes of a favorite activity, earned by session participation
04
Token or Sticker
If using a token economy system
05
Natural Consequence
"Your hands did such great work, now they're ready for [next activity]!"
Celebrate the attempt, not just the success. A child who sat for 2 minutes today when yesterday was 30 seconds has made measurable progress.

STEP 6 of 6
The Cool-Down — Transition Back to Baseline
⏱️ Duration: 1–2 minutes
Transition Warning Script
"Two more squeezes of the putty, then we're all done." "One more... and all done! Time to put the putty in the box."
Cool-Down Activity (60–90 Seconds of Calming Input)
01
Slow, Firm Hand Press
Parent presses child's hands between their own palms, 3-second hold
02
Warm Towel Wrap
Wrap hands in a warm towel for soothing sensory closure
03
Deep Pressure Hug
5–10 seconds, firm — organizes the nervous system
04
Weighted Lap Pad
1–2 minutes during transition to next activity
Material Put-Away Ritual: Have the child help put materials back in the storage basket. This teaches: (1) closure, (2) motor planning, (3) routine compliance, and (4) that the materials are always available — reducing anxiety about access.
Transition Cue:"Sensory time is done. Your hands are calm and ready for [next activity]."
If the child resists ending: Offer a "transition fidget" — one small fidget toy they can take with them to the next activity. This bridges the gap between structured sensory time and the real world.

Capture the Data — 60 Seconds, Right Now
Do this while the session is fresh. Three data points. That's all.
Data Point | Record This | How | |
Duration | How many minutes did your child engage with materials today? | Number (e.g., 8 min) | |
Materials Used | Which of the 9 materials did your child use? | List (e.g., putty, sensory bin) | |
Regulation Level | After the session, how regulated was your child? | Scale: 1 (dysregulated) → 5 (calm & organized) |
Optional Bonus Data Points:
- Number of times child independently reached for a sensory material instead of an inappropriate surface
- Biggest win of the session (one sentence)
60 seconds of data now saves hours of guessing later.

What If It Didn't Go as Planned?
Most sessions don't go perfectly. Here's what happened and what to do.
Problem 1: "My child refused to touch any material."
This is data. Start with the material closest to what your child already seeks. If they touch walls, offer the texture board. If they grab your face, offer putty at face height. Meet the need where it already lives.
Problem 2: "My child threw the materials."
Throwing is often proprioceptive seeking layered on top of tactile seeking. Redirect to heavy work first (carry a stack of books, push a laundry basket), THEN offer the tactile materials. The body needs to be regulated before the hands can explore.
Problem 3: "My child got overstimulated and melted down."
Too much, too fast. Next session, start with ONE material only, for 2 minutes only. Build up slowly. The nervous system needs gradual loading, not flooding.
Problem 4: "My child wanted to eat the sensory bin materials."
Normal for children who also mouth/orally seek. Switch to food-safe fillers ONLY (rice, lentils, pasta). Supervise 100% of the time. Offer a chewy tube simultaneously to meet the oral need.
Problem 5: "The session lasted 90 seconds before my child walked away."
90 seconds IS a session. This is success. Tomorrow, aim for 2 minutes. Build in 30-second increments. Neuroplasticity is built in repetitions, not marathons.
Problem 6: "My child only wanted one material and ignored the rest."
Perfect. One material that works is worth more than 9 that are ignored. Stay with what works for 2 weeks. Then introduce a second material alongside the preferred one.
Session abandonment is not failure — it's data.
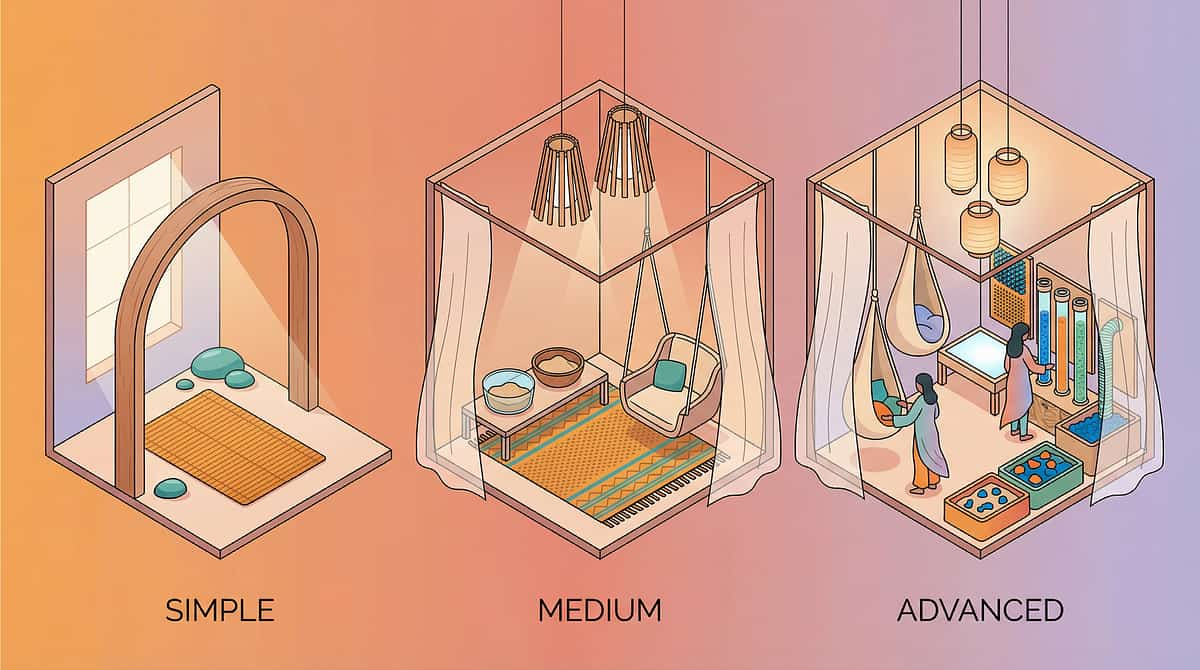
Adapt & Personalize — No Two Children Are Identical
Easier Version (Bad Days / Beginners)
1 material only · 2–3 minutes · Parent-led exploration · Heavy reinforcement for any engagement · No demands, pure free exploration
Standard Version
2–3 materials in rotation · 10–15 minutes · Parent-guided with some child choice · Structured activities within each material · Data recording after session
Advanced Version (Breakthroughs / Older Children)
4–5 materials in planned sequence · 15–20 minutes · Child-directed with parent observing · Texture discrimination games, blindfolded touch activities · Child self-records data
Sensory Seeker vs. Mixed Profile
Pure Tactile Seeker | Mixed Seeker + Avoider | |
Go bold: deep textures, heavy pressure, intense materials | Start gentle: soft fabrics, light putty, warm materials first | |
Progress quickly through materials | Stay with one material for 3+ sessions before adding | |
Sessions can be energetic and vigorous | Sessions should be calm and quiet | |
Add challenges: blindfold games, texture matching | Remove challenges: free exploration only |
Age Modifications
Ages 2–3
Parent does hand-over-hand. Avoid small parts. Use large sensory bin items. Supervise mouthing.
Ages 4–6
Child takes the lead. Introduce structured games (find the hidden toy, match the texture).
Ages 7–12
Add cognitive overlay — texture journal, sensory science experiments, self-monitoring charts.

ACT IV: THE PROGRESS ARC
Week 1–2: What to Expect
15%
Progress
You're building the foundation — habit formation is the goal
What You WILL See
- Child begins to tolerate the sensory station setup (may not fully engage yet)
- Brief moments of focused material exploration (30 seconds to 3 minutes)
- Child may start approaching the materials storage basket independently
- Slight reduction in intensity of inappropriate touching episodes
What You Will NOT See Yet
- ❌ Elimination of constant touching
- ❌ Long sustained engagement
- ❌ Self-regulation without prompting
- ❌ Generalization to other environments
If your child tolerates the sensory bin for 30 seconds longer than last week — that's real, measurable progress.
Parent Emotional Preparation: This phase is about building the habit — yours and theirs. The technique needs consistency to work. Aim for at least 5 sessions in the first 2 weeks. Perfection is not required. Showing up is.

Week 3–4: Consolidation Signs
40%
Progress
Neural pathways are forming — the brain is learning a new route
Consolidation Indicators
- Child anticipates sensory time — may go to the materials basket on their own
- Shows preference for specific materials (this is personalization emerging)
- Duration of engagement increases (5–10 minutes becomes common)
- You notice fewer "don't touch" conflicts during the hour AFTER a session
Neural Pathway Formation Signs
- Child begins to choose sensory materials INSTEAD of touching inappropriate surfaces (this is the brain creating a new pathway)
- You see the child's body calm visibly during or after material use
- Spontaneous self-regulation: child reaches for fidget without prompting
When to increase frequency or intensity: If the child asks for sensory time → increase to 3x/day. If the child blasts through one material in 2 minutes → introduce a second material in the same session.
You may notice you're more confident too. By week 3, the protocol feels natural. You're reading your child's cues faster. That's not luck — that's clinical skill building.

Week 5–8: Mastery Indicators
75%
Progress
Mastery zone — self-regulation is emerging
🏅 Mastery Criteria — Specific, Observable, Measurable
1
Independent Selection
Child independently selects and uses a sensory material when experiencing tactile seeking urges (without parent prompt) — observed at least 3 times per week
2
50%+ Reduction
Frequency of inappropriate touching has reduced by 50% or more (compare to baseline)
3
Functional Regulation
Child can sit through a meal or car ride with a fidget tool and remain regulated
4
Sustained Engagement
Session duration of 10+ minutes with sustained engagement is routine
5
Daily Integration
At least 3 of the 9 materials are integrated into the child's daily routine
Generalization Check
- Does the skill appear outside the home? (School, grandparent's house, public outings)
- Does the child use materials in the absence of the specific setup?
- Can another caregiver run the protocol with similar results?
When to progress to the next level: If all 5 mastery criteria are met for 2 consecutive weeks → the child is ready for advanced techniques (texture discrimination games, community-based sensory regulation, peer sensory play).

🎉 Celebrate This Win
You did this.
Eight weeks ago, your child's hands couldn't stop reaching for everything. You couldn't walk through a store without constant redirection. Family outings were exhausting.
Today, your child reaches for a fidget toy instead of the glass shelf. They dig through their sensory bin before school and walk out the door calmer. They squeeze putty during homework time and their focus holds.
Your child grew because of your commitment. Not because of a magic material — because you showed up, session after session, and answered your child's nervous system in the language it needed.
Family Celebration
Let your child show a grandparent or family member their sensory station. Let them be the "teacher." This reinforces mastery and builds pride.
📸 Document This Milestone
Take a photo or video of your child using their favorite sensory material. Date it. In 6 months, you'll look back and see the distance traveled.

🔴 Red Flags — When to Pause and Seek Professional Guidance
Even in the celebration zone, watch for these signs:
🔴 Seeking Is INCREASING
Tactile seeking is increasing despite 4+ weeks of consistent protocol → The sensory diet may not be calibrated correctly. Seek OT reassessment.
🔴 Pain-Level Input
Child is seeking pain-level input (pressing hands hard against sharp edges, slapping surfaces forcefully, biting own hands) → This exceeds typical seeking and may indicate self-injurious behavior requiring BCBA consultation.
🔴 New Behaviors Emerging
If tactile seeking decreases but new seeking behaviors appear (excessive spinning, head banging, visual stimming increase) → The nervous system may need a broader sensory diet. Consult OT.
🔴 Aggression During Sessions
Child becomes aggressive during or after sessions → Functional analysis needed. The materials may be creating frustration rather than regulation. BCBA consultation required.
🔴 No Change After 6 Weeks
No change whatsoever after 6 weeks of daily implementation → Re-evaluate: Is the sensory profile accurate? Is there an underlying medical condition? NeuroDev Pediatrician review recommended.
Escalation Pathway
1
1. Self-Resolve
Adjust materials, timing, or difficulty (Card 22)
2
2. Teleconsult
Book a virtual session with a Pinnacle OT → 9100 181 181
3
3. Clinic Visit
Schedule an in-person sensory processing evaluation
Trust your instincts — if something feels wrong, pause and ask.
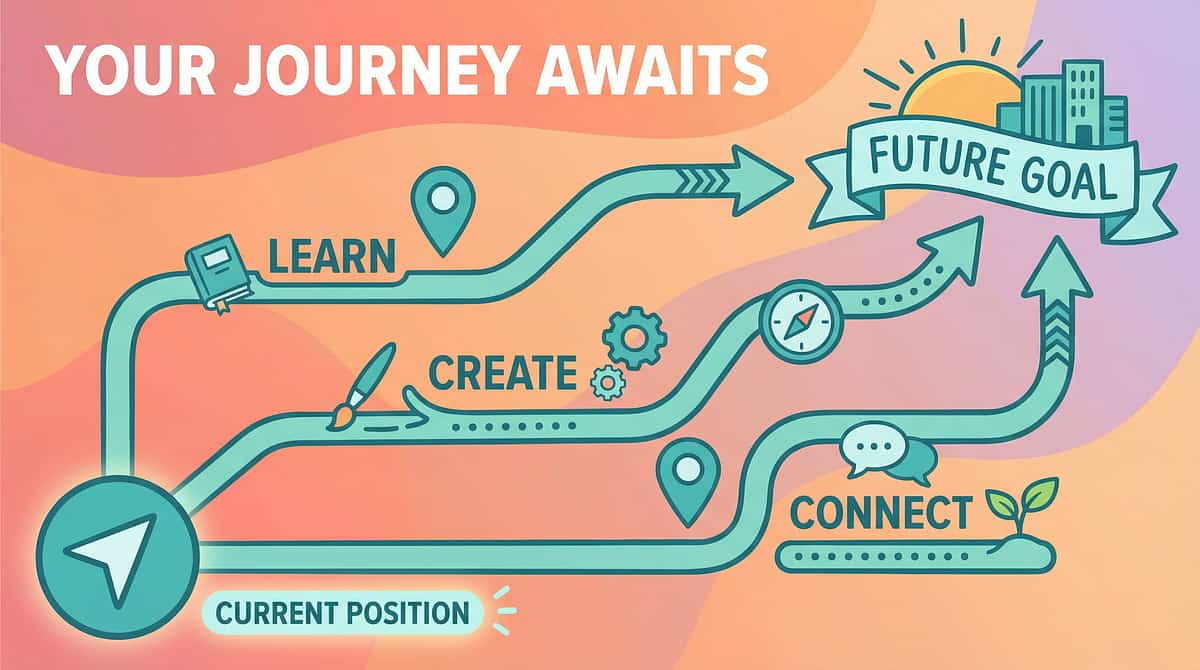
The Progression Pathway — Where You've Been, Where You're Going
{ "general": [ { "text": "<h4>Developmental Progression Pathway</h4>" } ], "step": [ { "text": "<h4>Touch Sensitivity (A-001)</h4><p>Prerequisite sensory technique</p>" }, { "text": "<h4>Sand Play Avoidance (A-009)</h4><p>Prerequisite behavior pattern</p>" }, { "text": "<h4><b>Touches Everything 9 Materials (A-030)</b></h4><p>Current technique position</p>" }, { "text": "<h4>Tactile Discrimination Games (A-045)</h4><p>Next-level tactile skills</p>" }, { "text": "<h4>Community Sensory Regulation (A-052)</h4><p>Next-level social regulation</p>" ;" }, { "text": "<h4>Self-Monitoring for Sensory Needs (A-061)</h4><p>Next-level self-awareness</p>" } ] }
Lateral Alternatives (if this approach didn't resonate): Proprioceptive-focused pathway (heavy work emphasis) · Oral motor pathway (if mouthing co-occurs) · Environmental modification pathway (texture zone focus).
Long-term developmental goal: Independent sensory self-regulation — the child recognizes their own tactile needs and independently selects and uses appropriate strategies without adult prompting.

Related Techniques — Domain A: Sensory Processing & Regulation
Technique | Difficulty | You Own Materials? | Material Overlap | |
A-001: Touch Sensitivity — 9 Materials | 🟢 Intro | ✅ Yes | Fidgets, putty, textured items overlap | |
A-009: Sand Play Avoidance — 9 Materials | 🟢 Intro | ✅ Yes | Sensory bin materials | |
A-015: Clothing Sensitivity — 9 Materials | 🟡 Core | ✅ Partial | Textured clothing | |
A-045: Tactile Discrimination Games | 🟡 Core | ✅ Yes | Touch-and-feel boards | |
A-052: Community Sensory Regulation | 🔴 Advanced | ⚠️ Requires fidget travel kit | Portable fidget set | |
A-061: Self-Monitoring Sensory Needs | 🔴 Advanced | ✅ Yes | Tracking materials |
You already own materials for most of these. The 9 materials from A-030 cross-link to multiple techniques in Domain A.
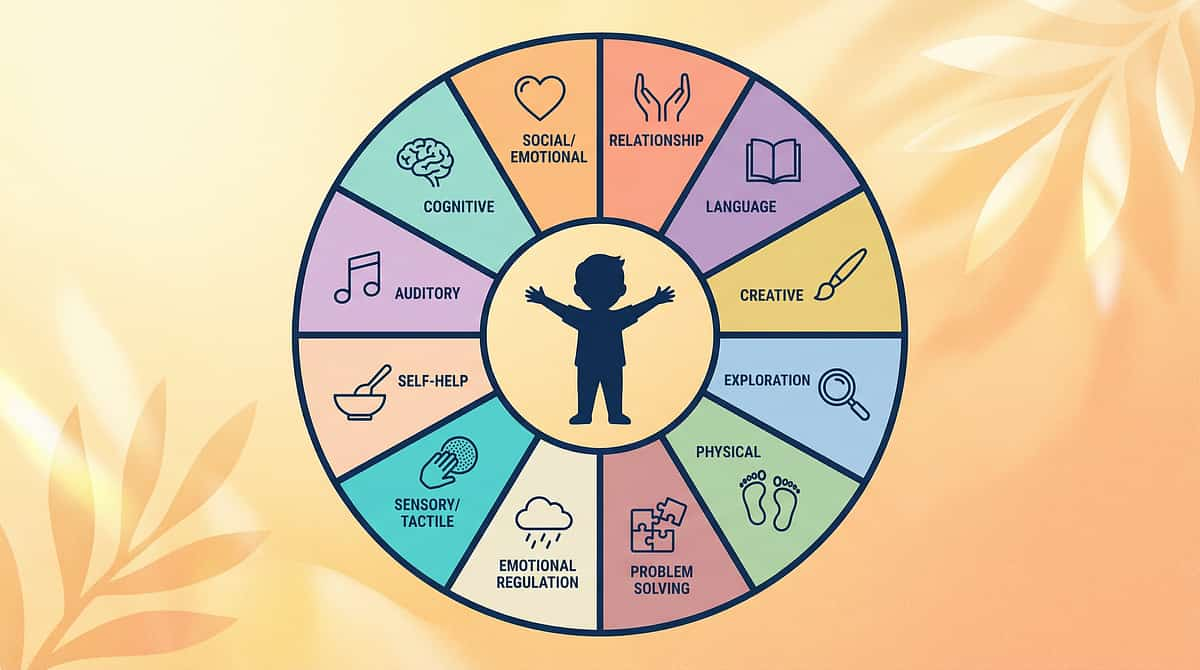
Your Child's Full Developmental Map
This technique is one piece of a larger plan. A child who gains tactile regulation (Domain A) is better prepared for fine motor tasks (Domain B), sustained attention for communication (Domain C), social play without sensory barriers (Domain D), and self-care independence (Domain E).
GPT-OS® sees the connections between domains. When you track progress in this technique, the system identifies which related domains to prioritize next, creating a personalized developmental pathway unique to your child.

ACT V: COMMUNITY & ECOSYSTEM
Families Who've Been Here
Arjun's Story (Name Changed)
Before: 4-year-old Arjun touched every surface constantly — walls, furniture, people's faces, food displays at the store. His mother couldn't take him shopping. Family outings had stopped.
After (Week 6): Arjun now carries a small fidget ring on outings. Before entering a store, he gets 5 minutes with his sensory bin. His mother reports a 70% reduction in inappropriate touching. They went to a restaurant last week — the first time in 8 months.
"Now he has his fidgets and sensory time before outings. We're not trapped at home anymore." — Parent, Pinnacle Network
Priya's Story (Name Changed)
Before: 6-year-old Priya was constantly touching classmates in school — not aggressively, but persistently. She couldn't keep her hands to herself. Teachers were calling daily.
After (Week 8): Her school desk has a texture strip attached underneath. She uses therapy putty for 3 minutes before circle time. Teacher calls have stopped. Priya self-reports: "My hands were busy so they didn't bother anyone."
From the Therapist's Notes: "Priya's Sensory Profile showed severe tactile seeking with average tactile discrimination. The putty addressed seeking while the desk texture strip provided continuous background input. The combination was key."

Connect With Other Parents
You are not alone in this. Thousands of parents are navigating the same challenge.
Tactile Seeking Parent Support Group
WhatsApp community for parents using sensory materials to manage touching behaviors. Share wins, ask questions, get peer support.
Pinnacle Parent Forum
Online discussion board moderated by Pinnacle therapists. Post questions, read guides, connect with parents nationwide.
Local Pinnacle Parent Meetup
Monthly in-person gatherings at your nearest Pinnacle center. Meet families navigating similar journeys. Check your city's schedule.
Peer Mentoring
Connect 1:1 with a parent who has already completed this technique journey with their child. They've been where you are.
Your experience helps others — consider sharing your journey.

Your Professional Support Team
Home + Clinic = Maximum Impact. Home-based intervention is powerful. Professional guidance makes it precise.
🗺️ Find Your Center
70+ Pinnacle Blooms centers across India — find personalized sensory processing support near you.
📞 Teleconsultation
Can't visit a center? Book a virtual session with a Pinnacle OT who specializes in sensory processing.
FREE National Autism Helpline (16+ languages):
📞9100 181 181
📞9100 181 181
Therapist Matching — Request a Specialist in:
- Sensory Integration (OT)
- Behavioral assessment of tactile seeking (BCBA)
- Communication impacts of sensory dysregulation (SLP)
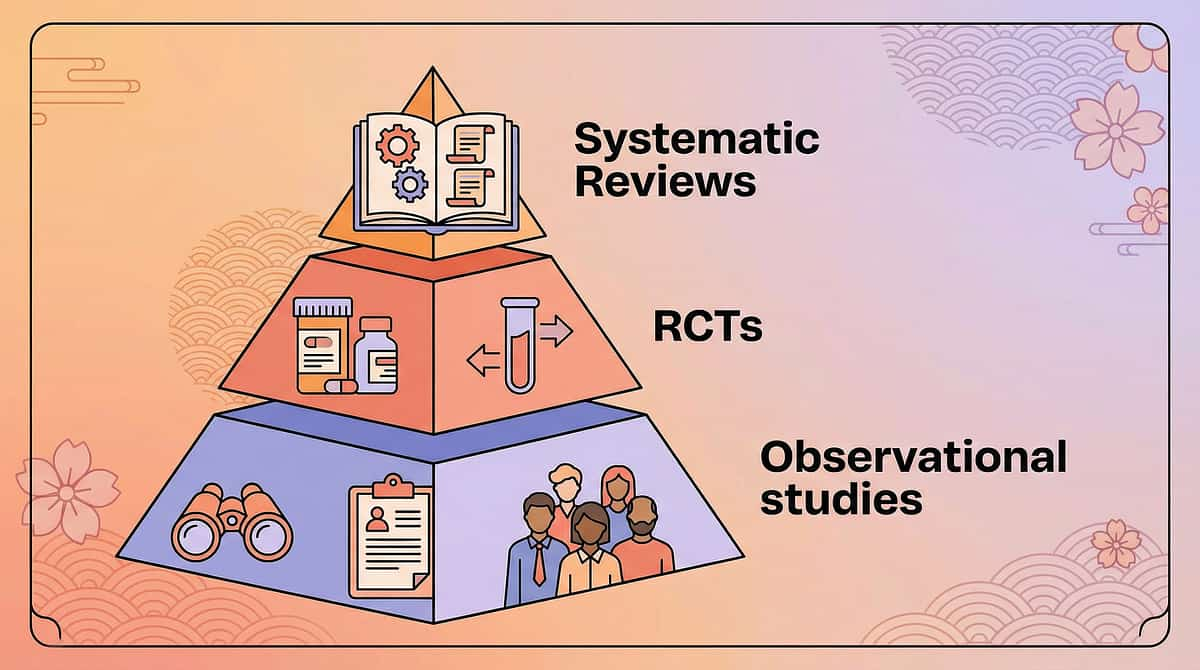
The Research Library — For the Curious Parent
1
SR
Systematic Reviews & Meta-Analyses
2
RCTs
Randomized Controlled Trials
3
Cohort
Cohort & Case-Control Studies
4
Expert
Expert Consensus & Guidelines
Key Studies Supporting This Technique
PRISMA Systematic Review (2024)
16 articles confirming sensory integration as evidence-based practice for ASD → PMC11506176
Meta-Analysis (World J Clin Cases, 2024)
24 studies showing effectiveness across social skills, adaptive behavior, sensory processing, motor skills → PMC10955541
Indian RCT (Padmanabha et al., 2019)
Home-based sensory interventions in Indian pediatric population with significant outcomes → DOI: 10.1007/s12098-018-2747-4
Frontiers in Integrative Neuroscience (2020)
Neurological framework for sensory processing treatment in ASD → DOI: 10.3389/fnint.2020.556660
WHO Nurturing Care Framework (2018)
Global framework for responsive caregiving and early intervention → nurturing-care.org
WHO CCD Package Implementation (2023)
Caregiver-delivered interventions across 54 countries → PMC9978394
NCAEP Evidence-Based Practices Report (2020)
Classification of sensory integration as evidence-based for autism → ncaep.fpg.unc.edu
Deeper reading for the curious parent.

How GPT-OS® Uses Your Data
Powered by GPT-OS® — Global Pediatric Therapeutic Operating System
What GPT-OS® Learns From THIS Technique's Data
- Your child's preferred material type (tactile, proprioceptive, or combined)
- Optimal session duration for your child's profile
- Time-of-day effects on engagement
- Cross-session improvement trajectory
Privacy & Data Protection
🔒 Encrypted
All data encrypted and stored securely
🔒 Never Sold
Your child's data is never sold or shared without consent
🔒 Anonymized
Aggregate data contributes to research that helps all children
🔒 Compliant
Indian DPDP Act and international data protection standards
GPT-OS® Module Map: Diagnostic Intelligence → AbilityScore® → Prognosis Engine → TherapeuticAI® → Archeyathic → FusionModule™ → EverydayTherapyProgramme™ → Ranonsamore® | 20M+ 1:1 sessions • 97%+ measured improvement • 70+ centers

🎬 Watch the Reel
Reel A-030
Domain A — Sensory Processing
Reel Title: "9 Materials That Help When Your Child Touches Everything"
A Pinnacle Blooms OT demonstrates each of the 9 materials with a child, showing correct usage, parent positioning, and expected child responses. Duration: 60–90 seconds.
Why Watch This: Video modeling is classified as an evidence-based practice for autism (NCAEP, 2020). Seeing the technique demonstrated through video reinforces the text instructions you've read and activates a different learning modality. Parents who watch AND read show significantly higher implementation fidelity.

Share This With Your Family
Consistency across caregivers multiplies impact. If only one parent executes this technique, it works. If grandparents, school teachers, and all caregivers align — it transforms.
Share via WhatsApp
Pre-formatted message with page link — send to family, therapists, and teachers in seconds
Share via Email
Email template with summary and link for caregivers who prefer email
Copy Link
techniques.pinnacleblooms.org/sensory-processing/tactile-seeking-touches-everything
📄 Downloadable Resources
Family Guide (1-Page PDF)
A simplified version of this entire page — materials, protocol, do's and don'ts — designed for grandparents, teachers, and other caregivers.
"Explain to Grandparents" Version
A warm, non-clinical explanation of why your child touches everything and what the family can do to help. Written at a comfort level for elders.
Teacher Communication Template
A ready-to-send letter for your child's school explaining the sensory seeking behavior, the materials your child uses, and how the classroom can support regulation.
📚 WHO CCD Package — multi-caregiver training as critical for intervention generalization | PMC9978394

ACT VI: THE CLOSE & LOOP
Frequently Asked Questions
1
Q1: How long until I see results?
Most parents notice increased tolerance and engagement within 1–2 weeks. Meaningful behavioral change (reduced inappropriate touching) typically emerges by weeks 3–4. Mastery-level self-regulation takes 5–8 weeks of consistent implementation.
2
Q2: Can I use all 9 materials at once?
No. Start with 1–2 materials. Introduce one new material per week. Flooding a child with 9 materials simultaneously is overwhelming, not therapeutic.
3
Q3: What if my child's school won't allow sensory materials?
Share the Teacher Communication Template (Card 37). Many schools accommodate sensory tools when presented with professional documentation. Pinnacle can provide a letter of recommendation for school-based sensory accommodations.
4
Q4: Is this technique safe for neurotypical children?
Yes. Tactile seeking exists on a spectrum. Neurotypical children who are sensory-seeking benefit from the same materials. There are no contraindications for typically developing children.
5
Q5: Will my child become dependent on these materials?
The goal is to reduce dependence over time, not increase it. As the nervous system matures and self-regulation develops, reliance on external materials naturally decreases. The progression pathway (Card 28) builds toward independence.
6
Q6: Can I combine this with my child's existing therapy?
Absolutely. This technique is designed to complement clinic-based OT, ABA, and SLP. Share this page with your child's therapist — they can calibrate your home protocol with their clinic goals.
7
Q7: The brushing protocol scares me. Do I have to do it?
No. The brushing protocol (Material #6) is optional and REQUIRES professional OT training. The other 8 materials can be used independently. Never attempt brushing without trained guidance.
8
Q8: My child touches people (grabs faces, leans on strangers). Will this help?
Yes, but with an important addition. Social touching is both a sensory AND social skill issue. The sensory materials address the physiological need. You'll also want to explore social boundary techniques in Domain D (Social Skills).
Didn't find your answer?
Your Next Step — Start Now
You've read the science. You've seen the evidence. You have the protocol. The materials are accessible.
There is nothing between you and starting — except starting.
🟢 Start This Technique Today
Begin with the Readiness Check (Card 13) right now. Launch GPT-OS® Guided Session (coming soon).
📞 Book a Consultation
Schedule with a Pinnacle OT for personalized sensory assessment.
9100 181 181
9100 181 181
🔄 Explore Next Technique
A-001: Touch Sensitivity · A-045: Tactile Discrimination Games · Browse all Domain A techniques
🛡️ Validated by the Pinnacle Blooms Consortium — OT • SLP • ABA • SpEd • NeuroDev • CRO
Preview of 9 materials that help when child touches everything Therapy Material
Below is a visual preview of 9 materials that help when child touches everything therapy material. The pages shown help educators, therapists, and caregivers understand the structure and content of the resource before use. Materials should be used under appropriate professional guidance.


















Share this resource
Help others discover thisLink copied!

The Pinnacle Promise
🛡️ Pinnacle Blooms Network®
Built by Mothers. Engineered as a System.
"From fear to mastery. One technique at a time."
A parent arrived on this page scared, confused, and exhausted. They leave empowered — with the science, the materials, the protocol, the data, the community, and the professional support to transform their child's nervous system response.
This is one of 70,000+ intervention technique pages — the largest structured pediatric intervention knowledge base on Earth.
Pediatric Therapeutic OTT Platform
Evidence-based content at scale
Hyperlocal Therapeutic Marketplace
Materials matched to techniques
70+ Physical Centers
Nationwide clinical support
Legal Disclaimer: This content is educational. It does not replace assessment by a licensed occupational therapist or healthcare provider. Persistent sensory seeking behavior may require comprehensive sensory processing evaluation. Brushing protocols require professional training — do not attempt without OT guidance. Individual results may vary. Statistics represent aggregate outcomes across the Pinnacle Blooms Network. Sensory processing timelines vary significantly between children.
© 2025 Pinnacle Blooms Network®, unit of Bharath Healthcare Laboratories Pvt. Ltd. All rights reserved. CIN: [001000300] | DPIIT: [001005000] | MSME: [001005400] | GSTIN: [03193000]
FREE National Autism Helpline (16+ languages): 9100 181 181
Execution layer of GPT-OS® — Global Pediatric Therapeutic Operating System
