
"She Doesn't Look at Things the Way Other Kids Do."
You're at the park, and your daughter is crouched down, her head tilted almost horizontal, peering at a toy from below. At home, she presses her face against books, looking at pages from the side rather than straight on. You took her to the eye doctor. Vision is 20/20. Perfect. But the looking continued — tilted, angled, close, sideways.
You are not failing. Your child's visual processing system is speaking a language you haven't been taught yet — until now. This is your complete guide to understanding and supporting angle-looking behaviour, built by the Pinnacle Blooms Consortium of paediatric therapists, neurodevelopmental physicians, and clinical researchers.
Pinnacle Blooms Network®
Validated by 20M+ Therapy Sessions
Powered by GPT-OS®

You Are Not Alone — The Numbers Behind Angle-Looking
You are among millions of families worldwide who have watched their child examine the world from angles that seem baffling. This is not rare. This is not random. And most importantly — this is understood by clinical science and treatable through structured intervention.
1
Children with ASD
display sensory processing difficulties including visual processing differences — PRISMA Systematic Review, Children (2024) | PMC11506176
2
US Children with ASD
Identified by the CDC (2023). In India, estimated 1 in 100 — approximately 13 million families navigating sensory processing challenges.
3
Atypical Visual Behaviours
65–90% of children with ASD demonstrate unusual visual examination, peripheral vision preference, or close-proximity viewing — Research in Autism Spectrum Disorders, 2024
Angle-looking is one of the most commonly reported visual behaviours in paediatric autism and sensory processing difference populations. The fact that standard eye exams come back normal is itself a diagnostic clue — because this isn't about the eyes. It's about how the brain processes what the eyes see.
Source: PRISMA Systematic Review (2024), PMC11506176 | Meta-analysis, World J Clin Cases (2024), PMC10955541 | CDC MMWR (2023)

Not a Vision Problem. A Visual Processing Difference.
The Science — What's Happening
Your child's eyes work perfectly. The lens focuses, the retina captures, the optic nerve transmits. But between the eye and perception, there's a processing layer — the visual cortex and its connections — and that's where the difference lives.
When visual information enters the brain, it travels two parallel routes. The ventral stream processes what something is (object recognition, detail, colour). The dorsal stream processes where something is (spatial awareness, movement, position). In many children with sensory processing differences, these streams process information at different rates or with different sensitivities.
What This Means in Plain English
Sensory Seeking: Your child's visual cortex craves specific input — light patterns, shadows, edge contrasts — that are more intense from certain angles. The tilted head creates visual effects that satisfy a neurological hunger.
Sensory Filtering: Central vision delivers high-density information. For a child whose brain amplifies visual input, peripheral vision may be less overwhelming. The angle is the filter.
Perceptual Difference: Some children's visual processing systems genuinely work more efficiently from atypical perspectives. The angle isn't dysfunction — it's optimisation for their particular neural architecture.
Self-Regulation: The predictable, controllable visual experience from angle-looking provides nervous system regulation. It calms. It organises. It grounds. This is a wiring difference, not a behaviour choice.
Reference: Frontiers in Integrative Neuroscience (2020), DOI: 10.3389/fnint.2020.556660

Where Angle-Looking Sits in Your Child's Development
Understanding where your child is on the developmental timeline helps frame the intervention window — and grounds your expectations with clarity and hope.
1
6–12 Months
Visual tracking and fixation developing. Some angle-looking may appear as normal visual exploration.
2
12–24 Months
Visual preferences emerge. Children with processing differences may begin showing consistent angle-looking or peripheral vision preference. ← Early identification window
3
2–4 Years
Angle-looking behaviours typically become most noticeable. Standard eye exams return normal. ← Most common referral age
4
4–7 Years
Without intervention, behaviour may become more rigid. With appropriate sensory input, significant improvement is documented. ← Intervention sweet spot
5
7–10 Years
Visual processing flexibility continues to develop. Children with supported intervention show increasing ability to shift between visual modes.
The WHO Care for Child Development (CCD) Package, implemented across 54 low- and middle-income countries, establishes that visual processing development is influenced by both neurological maturation and environmental input quality. Age-specific, evidence-based caregiver recommendations can significantly alter visual processing trajectories.
Reference: WHO CCD Package (2023) | PMC9978394 | UNICEF MICS indicators for developmental monitoring

Evidence Grade: LEVEL I–II — Systematic Review + Clinical Consensus
Level I–II Evidence
Strong Evidence Base
Clinically Validated
1
PRISMA Systematic Review (2024)
16 peer-reviewed articles from 2013–2023 confirm that sensory integration intervention meets criteria to be classified as evidence-based practice for children with ASD. Visual processing interventions are specifically included. | PMC11506176
2
Meta-Analysis, World J Clinical Cases (2024)
Across 24 studies, SI therapy effectively promoted social skills, adaptive behaviour, sensory processing, and gross/fine motor skills. Individual 1:1 sessions showed maximum effectiveness. | PMC10955541 | DOI: 10.12998/wjcc.v12.i7.1260
3
Indian Paediatric RCT (2019)
Home-based sensory interventions demonstrated significant outcomes in Indian paediatric populations, establishing feasibility and efficacy of parent-administered protocols. | DOI: 10.1007/s12098-018-2747-4 (Padmanabha et al., Indian J Pediatr)
4
WHO Nurturing Care Framework (2018)
Establishes that early identification and structured caregiver-administered interventions directly impact developmental outcomes across sensory processing domains. | nurturing-care.org/ncf-for-ecd/
Clinically validated. Home-applicable. Parent-proven.

Visual Angle Exploration Technique
Technique A-068
The Visual Angle Exploration Technique is a structured, multi-material sensory integration intervention designed for children who consistently examine objects, people, and environments from unusual visual perspectives. Rather than eliminating angle-looking behaviour, this technique provides appropriate visual input that satisfies the child's neurological needs, introduces tools that channel the visual interest constructively, and gradually builds visual flexibility — expanding the child's visual repertoire while respecting their processing differences.
This technique combines light/shadow exploration, magnification tools, peripheral vision activities, visual filtering, multi-angle tools, visual detail materials, movement tracking, visual-vestibular integration, and direct gaze building into a cohesive home-executable protocol.
1
Domain
Sensory Processing / Visual Behaviours / Restricted & Repetitive Behaviours
2
Age Range
2–10 years
3
Session Duration
10–20 minutes
4
Frequency
3–5 sessions per week
5
Setting
Home + School + Therapy

This Technique Crosses Therapy Boundaries — Because the Brain Doesn't Organise by Therapy Type
Effective intervention for visual processing differences draws on multiple disciplines. Understanding each specialist's role helps you coordinate care and maximise outcomes for your child.
Occupational Therapy (OT) — Primary Lead
Your OT uses this technique to address visual sensory processing, visual-motor integration, and visual-vestibular coordination. The OT assesses the function of angle-looking (seeking, filtering, or regulating) and selects materials and strategies accordingly. Environmental modifications and sensory diet components are OT-driven.
Applied Behaviour Analysis (ABA) — Secondary
Your BCBA addresses the behavioural dimensions: when angle-looking interferes with learning engagement, social interaction, or safety. ABA contributes reinforcement scheduling, data collection protocols, and systematic skill-building through direct gaze activities.
Speech-Language Pathology (SLP) — Secondary
Your SLP addresses how angle-looking impacts communication — specifically joint attention, social gaze, and face-to-face engagement that underpin language development. The direct gaze building and shared visual activities bridge visual processing to communication.
NeuroDevelopmental Paediatrics — Contributing
Your developmental paediatrician rules out visual impairment, assesses the broader developmental profile, and monitors medical factors that may influence visual processing. The specialist who sees the whole child.
Reference: Adapted UNICEF/WHO Nurturing Care Framework for SLPs (2022) | DOI: 10.1080/17549507.2022.2141327
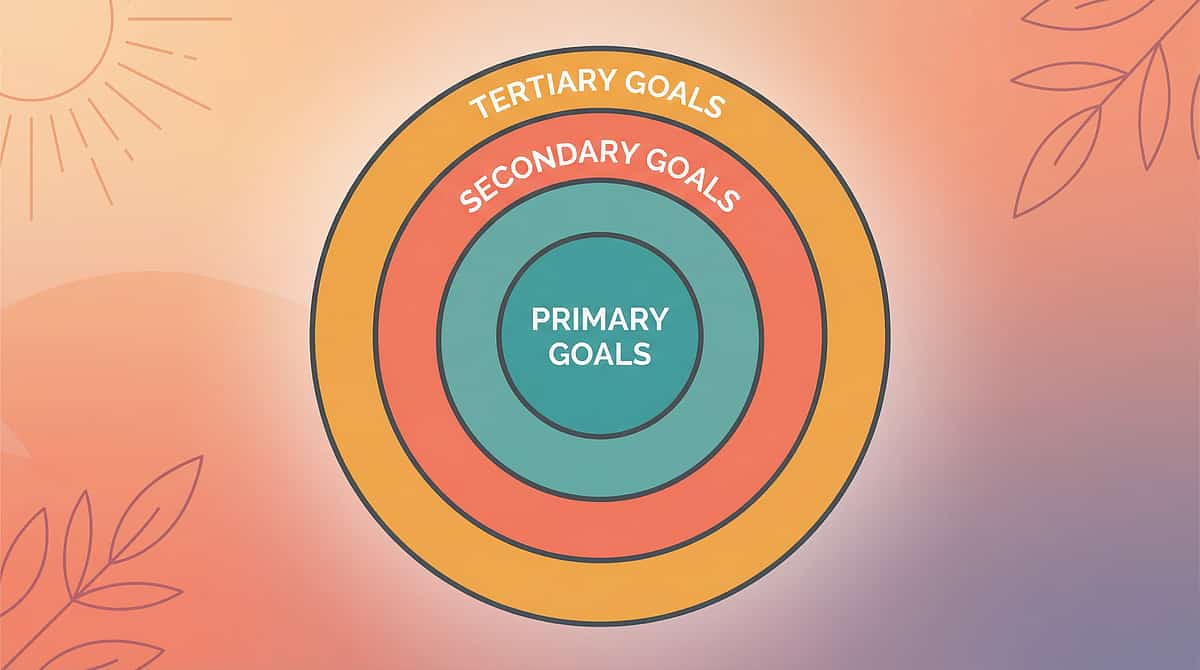
Precision Targets: What This Technique Addresses
This technique operates across three concentric levels of impact — from the core visual processing changes at the centre to broader developmental gains in the outer rings.
You'll know it's working when you see: increased time spent in direct/central viewing → willingness to engage with visual materials from typical distances → decreased distress when angle-looking is gently interrupted → spontaneous use of provided visual tools → emerging flexibility between viewing modes.
Reference: Meta-analysis, PMC10955541 — SI therapy effectively promoted social skills (primary), adaptive behaviour (secondary), sensory processing and motor skills (tertiary)

Your 9 Therapeutic Materials — Everything You Need
Each material category targets a specific aspect of visual processing. Together they form a complete sensory toolkit. Essential starters: light table/shadow materials + magnifying glass + kaleidoscope. Total Investment Range: ₹200–4,000.

1. Light & Shadow Materials | ₹500–4,000
Light tables, translucent building blocks, shadow puppet kits, flashlights, coloured transparent sheets, prisms, glow-in-the-dark materials. Canon: Sensory Visual Tools

2. Magnification & Close-Up Tools | ₹200–2,500
Magnifying glasses (various sizes), jeweller's loupes, child-safe microscopes, bug viewers, digital microscopes. Canon: Visual Exploration Tools

3. Peripheral Vision Activity Materials | ₹300–1,500
Peripheral awareness cards, motion detection toys, bubble machines, side-appearing pop-up toys, LED motion toys. Canon: Visual Processing Activities

4. Visual Filtering Materials | ₹300–2,000
Coloured overlay sheets, tinted reading strips, visual field reducers, anti-glare materials, Irlen-style lenses (if assessed). Canon: Sensory Modulation Tools

5. Multi-Angle Exploration Materials | ₹200–1,500
Kaleidoscopes, periscopes, angled mirror sets, fun-house mirrors, bendable cameras/scopes, prisms. Canon: Perspective Exploration Tools

6. Visual Detail & Pattern Materials | ₹200–1,500
I-Spy books, detailed pattern books, visual discrimination activities, hidden picture puzzles, mandala colouring. Canon: Visual Attention Materials

7. Movement & Visual Tracking Materials | ₹300–2,500
Lava lamps, liquid motion timers, marble runs, bubble tubes, sand timers, Newton's cradle. Canon: Visual Tracking Tools

8. Visual-Vestibular Integration Equipment | ₹500–3,000
Swings, balance boards, therapy balls, spinning equipment (therapeutically graded), visual-motor games. Canon: Sensory Integration Equipment

9. Direct Gaze Building Materials | ₹200–1,000
Peek-a-boo games, face-to-face musical activities, pop-up toys, bubble blowers, preferred positioning items. Canon: Social Visual Engagement Tools
Zero-Cost Alternatives: Execute This Technique TODAY with Household Items
The WHO Nurturing Care Framework emphasises equity-focused interventions accessible to every family regardless of economic status. This card ensures no family is excluded. The therapeutic principle remains identical — the sensory input pathway, the neurological mechanism, and the behavioural outcome are the same regardless of cost.
1
Light & Shadow → DIY
Flashlights for shadow play. Translucent materials on sunny windows. Plastic container with phone flashlight underneath as a light box. Coloured cellophane over a torch. Shadow puppet shows with hands outdoors.
2
Magnification → DIY
A drop of water on plastic wrap creates a natural magnifier. Smartphone camera zoom function for digital magnification. Holding items at different distances to explore visual detail in novel ways.
3
Peripheral Vision → DIY
"What moved?" game — move an object in the child's peripheral field. Ball tracking without turning the head. Bubble tracking in side vision. Side-appearing games (pop something up at the edge of vision).
4
Visual Filtering → DIY
Coloured cellophane sheets as overlays. Sunglasses for bright environments. Reducing visual clutter in rooms. Creating a visually calm corner with a sheet or blanket tent. Window films to soften light.
5
Multi-Angle Tools → DIY
Homemade kaleidoscope (tube + mirrors + beads). Mirror play at angles. Periscope from mirrors and tubes. Taking photos from unusual angles on a phone — this validates the perspective interest. Reflections in water, foil, and spoons.
6
Visual Detail → DIY
Drawing intricate patterns together. "Find the detail" games with magazine pictures. Close-up nature photography walks using a phone camera. Creating homemade I-Spy boards from household items.
7
Movement Tracking → DIY
Glitter jar (water + glitter in a sealed bottle). Watching bubbles. Balloon with slow leak floating down. Rain on windows. Clouds. Leaves in wind. Water flowing from a tap or in a stream.
8
Visual-Vestibular → DIY
Tracking objects while swinging on a playground swing. Simple balance on one foot while watching a moving target. Catching and throwing. Gentle spinning with visual fixation points on a rotating chair.
9
Direct Gaze → DIY
Peek-a-boo (timeless, zero-cost, clinically validated). Blowing bubbles toward the child. Singing face-to-face. Favourite toys held at eye level for direct viewing. Hide-and-reveal games at the child's pace.
Reference: WHO NCF (2018) | PMC9978394 — CCD Package efficacy with household materials across 54 LMICs

⚠️ Safety Gate: Read Before You Start
1
🔴 DO NOT PROCEED IF:
Child has NOT had a comprehensive eye exam in the past 12 months • Child is currently ill, feverish, or recently had a seizure • Child is in acute distress or post-meltdown • You have not identified whether your child is a visual sensory seeker or avoider • Child has diagnosed photosensitive epilepsy (requires medical clearance for light activities)
2
🟡 MODIFY AND PROCEED WITH CAUTION IF:
Child shows signs of eye strain (rubbing eyes, squinting, headache) — reduce intensity and duration • Using visual filtering tools without professional assessment — use only non-prescription overlays • Child becomes over-focused on any single material, especially light play — implement time boundaries • Working on visual-vestibular activities without OT assessment — start very gently
3
🟢 PROCEED WITH CONFIDENCE WHEN:
Comprehensive eye exam completed, vision confirmed as functional • Child is fed, rested, and relatively regulated • Materials prepared and environment set up (see Card 12) • Likely function of angle-looking identified through observation • Professional guidance received (ideal) or careful self-observation documented
🛑 STOP IMMEDIATELY AND CONSULT A PROFESSIONAL IF: Child's angle-looking suddenly changes in character • Child reports pain, headache, or visual disturbance • Child develops new eye-crossing or eye-deviation • Child shows severe distress across 3+ consecutive sessions • You notice regression in visual skills or daily functioning. MATERIAL SAFETY: Never allow direct flashlight beam into eyes • Never use magnifying glasses in direct sunlight (fire/burn risk) • Use only shatterproof child-safe mirrors • Lava lamps — heat hazard, manage cords • Age-appropriate choking hazard assessment for all small parts • Grade spinning/vestibular activities very carefully.
Reference: Indian J Pediatr RCT (2019) — Safety protocols for parent-administered sensory sessions | DOI: 10.1007/s12098-018-2747-4
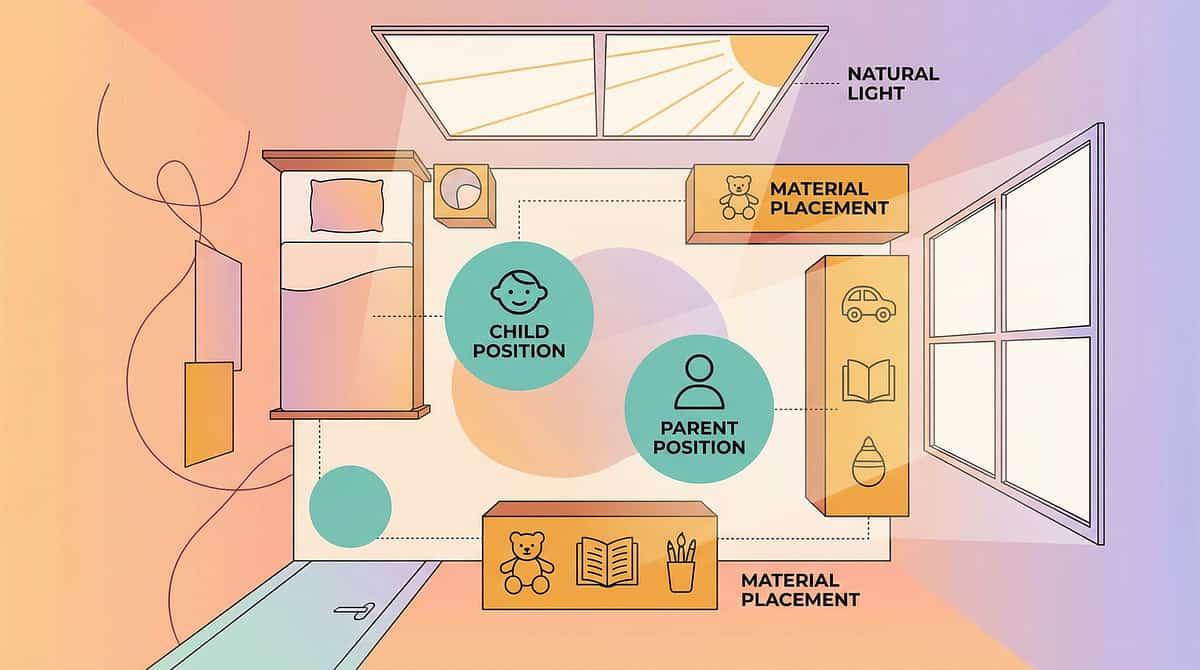
Set Up Your Space: The Visual Processing Environment
Environment is a core therapeutic principle in sensory integration theory. A well-prepared space can double the effectiveness of every session. Take 5 minutes to set up before each session.
REMOVE from the Space
- Screens (TV, tablet, phone) — competing visual stimuli
- Overhead fluorescent lighting if possible (use warm, indirect light)
- Visual clutter on walls and surfaces
- Bright or patterned items not part of the session
- Siblings or pets — 1:1 focus is essential
OPTIMISE the Space
- Lighting: Warm, adjustable. Dimmer if available. Ability to darken room for shadow/light activities.
- Sound: Quiet background. No music unless part of direct gaze activities.
- Surface: Mat or carpet for floor activities. Table for fine visual work.
- Materials: Set out only the current session's focus — one or two categories. Store the rest accessibly but out of sight.
Reference: Ayres Sensory Integration Theory — Environmental setup as a core principle | PMC10955541 — 1:1 individual sessions in structured environments showed maximum effectiveness

Pre-Session Readiness Check (60 Seconds)
Before every session, run this quick check. Starting when the child is ready makes a greater difference than any material or technique choice. "The best session is one that starts right."
01
Physical Readiness
Child has eaten within the past 2 hours (not hungry) • Not overtired or just waking from a nap • No signs of illness — fever, congestion, or eye rubbing
02
Emotional Regulation
No meltdown in the past 30 minutes • Child is in a relatively calm, alert state • Not in a highly stimulated or over-aroused state
03
Environment Ready
Materials are prepared and Card 12 environment is set • You have 15–20 minutes of uninterrupted time • Screens off, space prepared
1
✅ All GREEN → GO
Proceed to Card 14. Start the session at full protocol.
2
⚠️ 1–2 AMBER → MODIFY
Simplified version: only most preferred material, shorter duration (5–8 min), no demanding activities. Focus on sensory provision materials.
3
🛑 3+ RED → POSTPONE
Not today. Offer a calming visual activity (glitter jar, bubble watching) without protocol structure. Return tomorrow.

Step 1: The Invitation (30–60 seconds)
Step 1 of 6
What to Say
"I have something really interesting to show you. Want to come see?"
OR, for a child who is currently angle-looking: "I see you're looking at that — you're really studying it! I have something that makes looking at things even MORE interesting. Come look with me."
Body Language
- Get to the child's level physically
- Hold the first material at the child's preferred viewing angle — not yours
- Express genuine curiosity about what they're looking at
- No demands. This is an invitation only.
What Acceptance Looks Like
- Child approaches or shifts attention toward you or the material
- Child makes brief eye contact or orients body toward you
- Child reaches for the material
- Child pauses their current activity
What Resistance Looks Like & How to Modify
- Child ignores you → Move the material into their peripheral field. Wait. Don't repeat.
- Child moves away → Place the material where the child was looking. Step back. Let curiosity work.
- Child becomes upset → Abandon the invitation. This is data, not failure. Try again later.
Timing: 30–60 seconds. If acceptance hasn't occurred, pause and try a different material or a different time.
Reference: ABA Pairing Procedures — establishing motivating operations before demand placement | OT "Just-Right Challenge" principle

Step 2: The Engagement (1–3 minutes)
Step 2 of 6
Present the session's primary material using the child's natural visual orientation. If the child prefers peripheral viewing, introduce the material at the periphery and let them bring it to centre on their terms. If the child examines things closely, hold the material at their preferred close distance first, then gradually increase distance.
For Light/Shadow Materials
Turn on the light table or flashlight in a dimmed room. Place translucent materials on the surface. Let the child explore freely first — this is their visual world being honoured. No guidance required yet.
For Magnification Tools
Offer the magnifying glass near an object the child is already interested in. "Look through this — you can see it even closer!" Position it at their natural examination distance.
For Multi-Angle Tools
Present the kaleidoscope or periscope. "Look inside this — you can see the WHOLE world differently!" This validates their perspective interest directly and powerfully.
✅ Engaged (ideal)
Child actively explores, shows interest, extends interaction → Continue
⚠️ Tolerating (acceptable)
Child allows material nearby, briefly looks → Continue gently, don't push
🛑 Avoiding (concerning)
Child turns away, pushes material, shows distress → Stop. Try different material or postpone.
When the child engages with the material, even briefly: "You're looking at that! I can see you're really interested!" — immediate, specific, warm reinforcement.

Step 3: The Therapeutic Action (3–8 minutes)
Step 3 of 6
Core Intervention Phase
This is the active therapeutic phase. Select ONE primary material category per session and use it as the vehicle for the therapeutic action. The specific action depends on the identified function of your child's angle-looking.
IF SEEKING (craves visual effects)
Primary Material: Light & Shadow OR Movement Tracking. Provide rich, directed visual experiences. "Let's make shadows dance!" Create light patterns together. Track the lava lamp flow. You are feeding the visual system what it needs.
IF FILTERING (avoids visual overwhelm)
Primary Material: Visual Filters OR Peripheral Vision Activities. Introduce filtering tools. Try coloured overlays on a book. Work in a visually simplified space. Use peripheral awareness activities that honour the side-vision preference. You are giving the filtering system proper tools.
IF CLOSE-EXAMINING (gets very close to objects)
Primary Material: Magnification Tools OR Visual Detail Materials. Offer magnifying glasses. Introduce I-Spy books with rich detail. "You can see everything super close through this!" — channelling the detail hunger appropriately.
IF PERSPECTIVE-INTERESTED (loves angles and unusual views)
Primary Material: Multi-Angle Exploration OR Visual-Vestibular Integration. Kaleidoscope exploration. Periscope play. "Let's see the room from a COMPLETELY new angle!" Mirror play at different positions. You are validating the perspective interest.
Common Execution Errors: Forcing a material the child doesn't want → Follow the child's interest • Moving too fast to direct viewing expectations → Build from where the child IS • Removing the child's preferred angle-looking before offering alternatives → Always add before you subtract • Talking too much → Let the visual experience dominate. Duration: 3–8 minutes of active engagement. 5 minutes of genuine engagement is worth more than 15 minutes of tolerance.

Step 4: Repeat & Vary (3–5 minutes)
Step 4 of 6
Target Repetitions: 3–5 meaningful interactions with the material. NOT forced — read the child. After the child has explored the primary material, introduce a variation: light table → add different coloured translucent blocks • magnifying glass → examine a different object • kaleidoscope → turn it to create new patterns • movement tracking → switch from lava lamp to marble run.
1
Satiation Indicators
The child has had enough when they: turn away or physically move from the material • visual attention shifts to other things • restlessness or fidgeting replaces focused engagement • repetitive use without apparent interest (going through the motions)
2
The Golden Rule
3 good repetitions > 10 forced repetitions. If the child gives you 3 genuine, engaged interactions, that's a successful session. Honour the signal. Stop before the child disengages entirely.
Bridging Toward Flexibility (for sessions 3+): After 3+ sessions with the child's preferred material, begin gentle bridges. If using light table: place a preferred toy ON the light table in direct-view position. If using magnifier: hold the object at slightly increasing distances. If using kaleidoscope: look at the same thing together — the child through the kaleidoscope, you directly. "We see the same thing differently!"
Reference: SI literature — 2–3 sessions per week for 8–12 weeks as typical protocol

Step 5: Reinforce & Celebrate (1 minute)
Step 5 of 6
Reinforcement must happen within 3 seconds of the desired behaviour. Immediate reinforcement creates the neural connection that makes progress stick.
✨"You looked at that with me! That was amazing!"
✨"I love how you used the magnifying glass to see the details!"
✨"You found so many things on the light table! Your eyes are so good at finding things!"
✨"We looked at things together — that was really fun!"
Key Principles
- Timing: Within 3 seconds of the desired behaviour — always
- Specificity: Name EXACTLY what the child did well — not "good job"
- Celebrate the attempt, not just the success. If the child looked at the magnifier for 2 seconds, THAT was progress. Reinforce those 2 seconds.
Reinforcement Options
- Verbal praise (enthusiastic, specific)
- Preferred activity access (1 minute of favourite visual experience)
- Token/sticker toward a larger reward
- High-five, thumbs up, or preferred physical celebration
- Extended time with the session material (natural reinforcer)

Step 6: The Cool-Down (1–2 minutes)
Step 6 of 6
Transitions are often the hardest part for children with sensory processing differences. A predictable, gentle cool-down routine protects the positive tone of the session and prepares the child for what comes next.
1
Transition Warning
"Two more looks, then we're all done with the [material name]." Count down: "One more… and… all done! Great looking today!" Predictable endings reduce resistance significantly.
2
Cool-Down Activity (1–2 minutes)
Offer a familiar, calming visual experience: glitter jar watching • slow bubble blowing • looking at a favourite picture at the child's chosen angle (yes — let them angle-look during cool-down. This is earned sensory time).
3
Material Put-Away Ritual
If the child is able: "Can you put the magnifying glass in the box?" This builds routine and ownership. Participation in tidy-up is itself a therapeutic activity.
4
Transition to Next Activity
"Looking time is all done. Now it's [next activity] time." Use a visual schedule if available. If the child resists ending: offer a "one more" extension (once only), then remain firm and warm.
Reference: NCAEP Evidence-Based Practices Report (2020) — Visual supports and transition strategies

Capture the Data — 60 Seconds, Right Now
Record these 3 data points immediately after the session, before you forget. 60 seconds of data now saves hours of guessing later. This data powers the GPT-OS® personalisation engine and tracks your child's genuine progress across weeks.
1. Duration of Engagement
How many total minutes did the child actively engage with the therapeutic materials? (Not the entire session — just active engagement time.)
☐ < 1 minute ☐ 1–3 minutes ☐ 3–5 minutes ☐ 5–10 minutes ☐ 10+ minutes
☐ < 1 minute ☐ 1–3 minutes ☐ 3–5 minutes ☐ 5–10 minutes ☐ 10+ minutes
2. Viewing Mode Used
Did you observe any direct/central viewing during the session, or was all viewing from angles/periphery?
☐ All angle/peripheral ☐ Mostly angle, some direct ☐ Mixed ☐ Mostly direct, some angle ☐ All direct
☐ All angle/peripheral ☐ Mostly angle, some direct ☐ Mixed ☐ Mostly direct, some angle ☐ All direct
3. Child's Response Overall
☐ Resisted/avoided ☐ Tolerated ☐ Engaged ☐ Enthusiastic ☐ Requested more
Quick Notes (optional): Which material category today? __________ Any breakthrough moment? __________ Any concern? __________
Reference: BACB Data Collection Standards — Cooper, Heron & Heward, Applied Behaviour Analysis

What If It Didn't Go as Planned? (That's Normal.)
Every experienced therapist knows: the sessions that don't go as planned teach you the most about your child. Here are the most common challenges and their evidence-informed responses.
"My child refused to engage with ANY material."
This is data, not failure. Try: (1) Placing the material in the child's natural angle-looking space and walking away. (2) Using the material yourself with visible curiosity — modelling, not directing. (3) A completely different material category next session. (4) A different time of day in a different regulatory state.
"My child became fixated on the light table and wouldn't stop."
Light play is powerfully reinforcing for visual seekers. Use a visual timer ("3 more minutes of light time"). Build a structured light-play routine with clear boundaries. This fixation actually confirms the function — visual seeking — which guides your approach precisely.
"My child got upset when I tried the direct gaze activities."
Direct gaze building is the LAST skill in the progression, not the first. Skip it until materials 1–8 have built trust and visual flexibility. When you return to it, start with peek-a-boo (low demand, high reward) and follow the child's tolerance carefully.
"My child used the magnifying glass as a toy, not a tool."
PERFECT. Play IS the vehicle. Let them explore the magnifier as a toy first. When they're comfortable, start introducing objects to examine through it. The tool becomes functional through play, not instruction.
"The session lasted 2 minutes before my child walked away."
A 2-minute session where the child engaged is a WIN. Week 1 may be 2 minutes. Week 4 may be 8 minutes. Week 8 may be 15 minutes. Track the trend, not the individual session.
"My child prefers their angle-looking over any material I offer."
This is the baseline, not failure. The angle-looking behaviour has been meeting a neurological need for months or years. The materials need time to become viable alternatives. Continue offering consistently — consistency wins.
"Session abandonment is not failure — it's data."
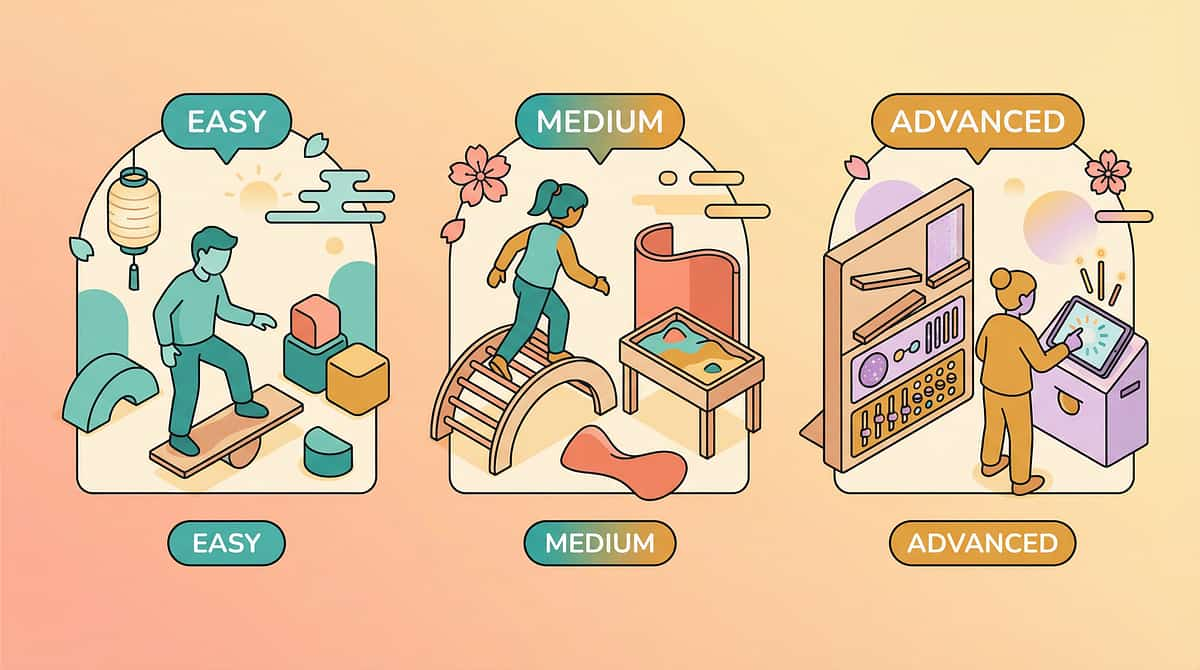
Adapt This to YOUR Child
No two children are identical. This protocol is a framework, not a prescription. Use the sliders and variations below to calibrate every session to where your child actually is today — not where you hope they'll be.
1
← EASIER
Tough days, early sessions, younger children: • Only sensory provision materials (light, shadow, magnification, movement) • Sessions 5–8 minutes • No direct gaze expectations • Child leads entirely • One material per session
2
STANDARD
Typical sessions: • Full 6-step protocol, one primary material category • 10–15 minute sessions • Gentle bridging toward visual flexibility • Data collection each session
3
HARDER →
Breakthroughs, older children, advanced sessions: • Multi-material sessions (2–3 categories) • Visual-vestibular integration activities • Active direct gaze building • Longer engagement targets • Novel materials introduced
Sensory Profile Variations
Visual SEEKER: Lead with Light & Shadow, Movement Tracking, Visual Detail. These children LOVE visual richness — feed it appropriately. Challenge: setting boundaries around over-engagement.
Visual AVOIDER: Lead with Visual Filtering, simplified visual environments. Use Peripheral Vision Activities that honour the side-vision preference. Challenge: building tolerance for direct viewing gradually.
Age Modifications
Ages 2–3: Parent-led play. Short sessions. Sensory exploration focus. No cognitive demands.
Ages 4–6: Guided exploration. Introducing tool use (magnifiers, kaleidoscopes). Beginning flexibility activities.
Ages 7–10: Collaborative activities. Cognitive engagement (I-Spy, seek-and-find). Active direct gaze building. Self-monitoring beginning to emerge.

Week 1–2: Building the Foundation
Progress Arc
~15% of Journey
What Progress Actually Looks Like
You may see:
- Child tolerates the presence of materials (even if not actively using them)
- Brief moments — seconds — of engagement with preferred materials
- Reduced resistance to the session routine
- Curiosity toward one or two material categories
- Angle-looking continues at the same frequency — this is normal and expected
What You Will NOT Yet See
- Significant changes in angle-looking behaviour
- Sustained direct viewing
- Independent use of visual tools
- Generalisation to other settings
"If your child reaches for the magnifying glass on their own — even once — that's real progress."
Patience metric: You are building new neural pathways. The brain rewires through consistent, repeated, positive sensory experience. Two weeks is the beginning of the beginning.
Reference: PMC11506176 — SI intervention outcomes emerge across 8–12 week timelines

Week 3–4: Neural Pathways Forming
Progress Arc
~40% of Journey
This is where the protocol begins to feel real. The child starts showing you, through their behaviour, what their visual system genuinely needs — and that information is gold.
1
Consolidation Indicators
Child anticipates the session routine — goes to the session space, looks for materials. Sustained engagement with preferred materials increases to 2–5 minutes consistently.
2
Preference Emergence
Child may show clear preference for specific materials — this is functional communication about their sensory needs. Brief moments of direct viewing during preferred activities appear, fleeting but measurable.
3
Generalisation Seeds
Child may begin using a magnifier, kaleidoscope, or light play outside of formal sessions. Interest in visual detail emerging — pointing, examining objects from multiple angles rather than one rigid angle.
4
When to Increase Intensity
If the child engages for 5+ minutes consistently with minimal resistance, consider adding a second material category or extending sessions to 15–20 minutes.
"You may notice you're more confident too. You're reading your child's visual behaviour with new understanding. That confidence is therapeutic — children sense when their parent understands."

Week 5–8: Visual Flexibility Emerging
Progress Arc
~75% of Journey
This is the payoff phase — where the weeks of consistent sessions begin to show up as real, measurable changes in your child's visual world. What you track on your data sheets will tell the story.
Mastery Criteria
- Child independently selects and uses visual tools from the material set
- Direct viewing duration increases — measurable on your tracking sheets
- Angle-looking decreases in frequency and/or rigidity during sessions
- Child tolerates gentle interruption of angle-looking with minimal distress
- Visual engagement with faces/people shows improvement (even brief)
Generalisation Indicators
- Visual flexibility appearing in settings beyond the session: school, outings, mealtimes
- Child uses provided strategies spontaneously
- Reduced reliance on extreme angle-looking for self-regulation — may use materials instead
Mastery Unlocked — Badge Criteria:
- ☑️ Child can shift between angle-viewing and direct-viewing in the same session
- ☑️ Child uses at least 3 material categories independently
- ☑️ Direct viewing duration exceeds 30 seconds for preferred activities
- ☑️ Angle-looking, while still present, no longer significantly interferes with learning or social engagement
Reference: PMC10955541 — Mastery criteria from behavioural measurement standards | BACB criteria

🎉 You Did This. Your Child Grew Because of Your Commitment.
Five to eight weeks. Multiple sessions per week. Material preparation. Data collection. Patience through sessions that didn't go as planned. Adapting. Persevering. Understanding your child's visual world when no one else could explain it.
Your child walked into this protocol with rigid angle-looking and no alternatives. Now they have a toolkit of visual experiences, emerging flexibility, and a parent who understands that different vision is not broken vision.
📸 Document It
Take a photo of your child engaging with their favourite visual tool. Record this milestone in your journal or GPT-OS® tracker.
🤝 Share It
Share with your partner, family, or support community. Let your child see you celebrate THEM — "You are amazing at discovering how things look!"
🌱 Build on It
The angle-looking may not be gone entirely — and that's okay. Different vision became flexible vision. Your child can now see the world from many angles — including the ones that work for learning and connection.

🔴 Red Flags — When to Pause and Seek Professional Guidance
Stop the Protocol and Consult a Professional immediately if you observe any of the following indicators. These are medical and clinical signals that fall outside the scope of home protocol management.
1. New Eye-Turning or Eye-Crossing
If one or both eyes begin turning in, out, up, or down — this could indicate developing strabismus or another ocular-motor issue requiring ophthalmological evaluation. This is medical, not sensory.
2. Behavioural Regression
If angle-looking increases significantly, becomes more rigid, or the child loses previously acquired visual skills — this could indicate a concurrent process needing professional assessment beyond the home protocol.
3. Consistent Distress During Sessions
If the child shows high distress (prolonged crying, self-injurious behaviour, severe avoidance) across 3+ consecutive sessions despite modifications — the protocol needs professional recalibration.
4. Physical Complaints
If the child reports or indicates headaches, eye pain, or visual disturbance (squinting, eye rubbing after sessions) — pause and consult both a developmental optometrist and OT before resuming.
5. Loss of Functional Skills
If visual behaviour begins interfering MORE with daily activities, learning, or safety after starting the protocol — something needs adjustment. Professional consultation required immediately.
Escalation Pathway: Self-resolve (adjust difficulty, try different materials) → Teleconsultation with Pinnacle OT → Clinic visit for comprehensive reassessment
📞Pinnacle FREE National Autism Helpline: 9100 181 181 (16+ languages, 24/7)
Trust your instincts — if something feels wrong, pause and ask.
Your Child's Visual Processing Pathway
This technique sits within a larger ecosystem of Pinnacle Blooms interventions. Understanding where you are — and where you can go — helps you build a coherent, progressive programme for your child's development.
Long-Term Developmental Goal: Visual Processing Index → Functional visual attention across environments → Academic visual readiness → Social visual engagement → Independent visual regulation

Related Techniques in Sensory Processing / Visual Behaviours
Your investment in this technique's materials gives you an immediate head start on several related protocols. The Pinnacle techniques library is designed so that each technique reinforces the next.
A-066: Child Spins Objects | Intro
Materials you already own: ✅ magnification tools, movement tracking. Builds the visual-motor foundation this technique sits upon.
techniques.pinnacleblooms.org/sensory-processing/object-spinning
techniques.pinnacleblooms.org/sensory-processing/object-spinning
A-069: Child Stares at Lights or Spinning | Core
Materials you already own: ✅ light/shadow, visual filters, movement tracking. Natural next step for children who responded strongly to light-based materials.
techniques.pinnacleblooms.org/sensory-processing/light-staring
techniques.pinnacleblooms.org/sensory-processing/light-staring
A-070: Child Covers Ears | Core
Materials overlap: sensory regulation tools. Addresses auditory sensitivities that frequently co-occur with visual processing differences.
techniques.pinnacleblooms.org/sensory-processing/ear-covering
techniques.pinnacleblooms.org/sensory-processing/ear-covering
A-071: Child Avoids Eye Contact | Advanced
Materials you already own: ✅ direct gaze building, face-to-face activities. Builds directly on the social gaze work begun in this protocol.
techniques.pinnacleblooms.org/sensory-processing/eye-contact
techniques.pinnacleblooms.org/sensory-processing/eye-contact
A-072: Overwhelmed in Busy Places | Core
Materials you already own: ✅ visual filtering, environmental tools. Addresses broader sensory overwhelm in community settings.
techniques.pinnacleblooms.org/sensory-processing/overwhelm-management
techniques.pinnacleblooms.org/sensory-processing/overwhelm-management
A-075: Unusual Sensory Responses | Advanced
Materials overlap: comprehensive sensory toolkit. For children whose visual behaviour is part of a broader multi-sensory processing profile.
techniques.pinnacleblooms.org/sensory-processing/unusual-responses
techniques.pinnacleblooms.org/sensory-processing/unusual-responses
You already own materials for several of these techniques. Your investment multiplies.
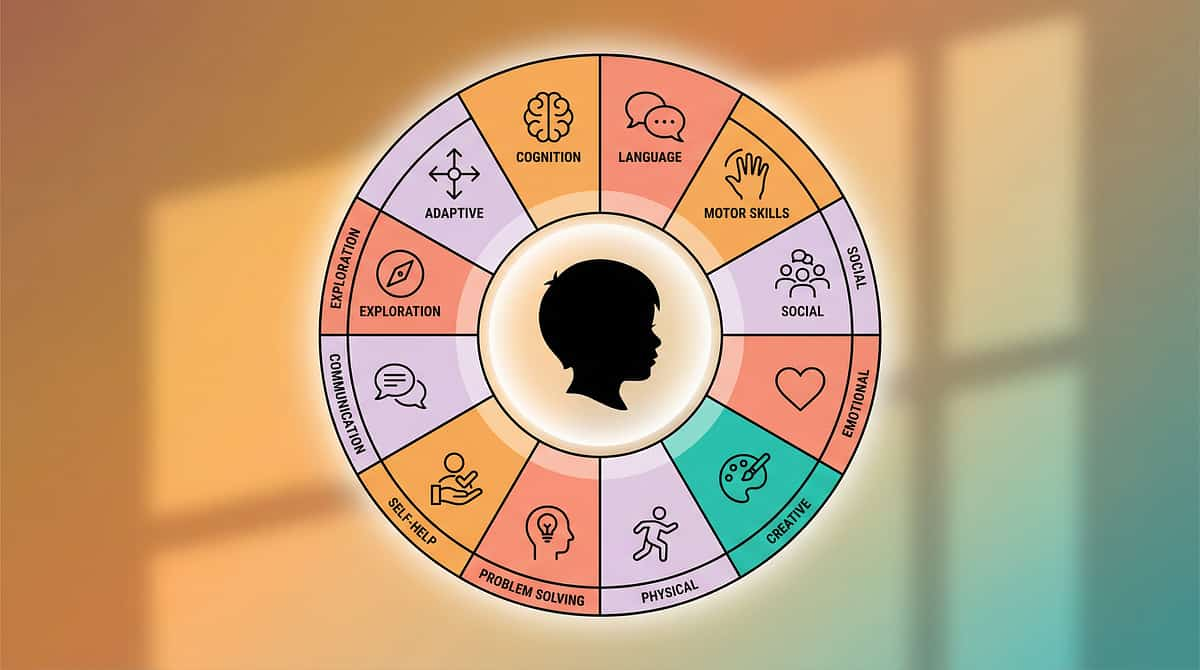
One Technique, One Piece of a Larger Plan
Visual processing is Domain A of a 12-domain developmental framework. This technique directly addresses Domain A — with meaningful secondary contributions to communication, cognition, and behavioural regulation.
This technique is one piece of a larger plan. Your child's development is a journey across all 12 domains — and GPT-OS® maps the complete landscape, identifying which techniques to prioritise at each stage of your child's individual trajectory.
Reference: WHO/UNICEF Nurturing Care Framework — Five components of nurturing care require holistic developmental monitoring

From Families Who've Been Where You Are
"Everything at an angle. Every single thing. That's how my daughter saw the world — tilted, close-up, from the corner of her eye. The eye doctors couldn't explain it; her vision was perfect. We stopped fighting it and started understanding it. Light tables for her shadow fascination. Magnifying glasses for her close-up interest. Kaleidoscopes that made angles fun and shareable. Slowly, her visual flexibility grew. She still has her ways of seeing — I think she notices light and shadow that most of us miss. But now she can also look at books, look at faces, engage with the world in ways that work for learning and connection. Different vision became flexible vision."
— Parent, Pinnacle Network
"The moment I understood that my son wasn't being 'difficult' — that his brain was processing visual information differently — everything changed. I stopped saying 'look at me properly' and started saying 'let's look at this together in a way that feels good.' The materials gave him options. The protocol gave me confidence. The data showed me it was working, even when progress felt invisible day-to-day."
— Parent, Pinnacle Network
Note: Illustrative cases; outcomes vary by child profile. Individual results reflect diverse response patterns across the Pinnacle Blooms Network.

You Are Not Doing This Alone
The families who make the most progress are those who build a community around their child's journey. Connection with other parents who truly understand — who have sat on the same floor with the same tilted-headed child — is itself therapeutic.
Visual Processing Support — WhatsApp Community
A moderated parent WhatsApp community specifically for families navigating visual processing differences. Share session notes, ask questions, and celebrate wins with parents who understand exactly what you mean.
Pinnacle Blooms Online Parent Forum
The Visual Behaviours Group within the Pinnacle online forum is an active community of parents, caregivers, and therapists. Searchable archives of thousands of real-world protocol questions and answers.
Local Pinnacle Parent Meetup
Face-to-face connection with families at your nearest Pinnacle centre. Monthly meetups facilitated by Pinnacle therapists. Find your nearest centre community and see the schedule.
Peer Mentoring Programme
Connect with a parent who has completed this protocol and achieved measurable progress. Peer mentors are trained by Pinnacle and matched by child profile and geographic location.
"Your experience helps others — consider sharing your journey."
Home + Clinic = Maximum Impact
The home protocol is designed for parent execution — and it works. But pairing it with professional clinical support maximises both safety and outcomes. Here is your professional support team and how to access them.
Occupational Therapist — Primary
Sensory processing assessment, visual-motor evaluation, individualised sensory diet, environmental modification guidance. This is the specialist who understands why your child sees differently. Lead clinician for this protocol.
Developmental Optometrist
Visual processing assessment beyond the standard eye exam — evaluates eye teaming, tracking, and perceptual processing. This is the specialist who sees the brain behind the eyes. Essential for ruling out structural visual differences.
Developmental Paediatrician
Comprehensive evaluation, medical oversight, comorbidity assessment, medication management if indicated. This is the specialist who sees the whole child — and coordinates the multidisciplinary team.
Behavioural Specialist (BCBA)
Functional behaviour assessment of angle-looking, data-driven intervention design, reinforcement optimisation. This is the specialist who helps the behaviour become functional and measurably tracks change over time.
📍Find Your Nearest Pinnacle Centre — 70+ locations across India | 📞FREE National Autism Helpline: 9100 181 181 — 16+ languages, 24/7 | 💻Teleconsultation Available — For families in remote locations or other countries

The Science Behind This Technique — For the Curious Parent
This protocol is grounded in peer-reviewed research. For parents, therapists, and programme leads who want to go deeper, here is the evidence foundation that underpins every card in this guide.
1. PRISMA Systematic Review (2024)
"Sensory Integration Intervention for Children with Autism Spectrum Disorder" — 16 articles, 2013–2023. Confirms SI meets evidence-based practice criteria. Visual processing interventions specifically included. 🔗PubMed: PMC11506176
2. Meta-Analysis, World J Clinical Cases (2024)
Across 24 studies: SI therapy effectively promoted social skills, adaptive behaviour, sensory processing, and motor skills. Individual 1:1 sessions showed maximum effectiveness. 🔗DOI: 10.12998/wjcc.v12.i7.1260 | PMC10955541
3. Indian Paediatric RCT (Padmanabha et al., 2019)
Home-based sensory interventions in Indian paediatric ASD population. Significant outcomes established for parent-administered protocols. 🔗DOI: 10.1007/s12098-018-2747-4
4. WHO Care for Child Development Package (2023)
CCD implemented across 54 LMICs. Age-specific caregiver recommendations with household materials demonstrate measurable developmental impact. 🔗PMC9978394
5. Frontiers in Integrative Neuroscience (2020)
Comprehensive framework for evaluating sensory processing treatment in ASD — establishing the neurological basis for sensory-based interventions. 🔗DOI: 10.3389/fnint.2020.556660
6. UNICEF/WHO Nurturing Care Framework for SLPs (2022)
Multi-disciplinary contribution to nurturing care components — establishing the SLP role in visual-communication bridge interventions. 🔗DOI: 10.1080/17549507.2022.2141327
Additional Resources: SPD Star Foundation: spdstar.org • American Occupational Therapy Association: aota.org • College of Optometrists in Vision Development: covd.org • NCAEP Evidence-Based Practices Report (2020) • WHO Nurturing Care Framework: nurturing-care.org
How GPT-OS® Transforms Your Session Data into Personalised Guidance
Every 60-second data entry from Card 20 feeds into the GPT-OS® personalisation engine — building an increasingly precise picture of your child's unique visual processing profile and trajectory.
What GPT-OS® Learns
- Which material categories generate the longest engagement for YOUR child
- Whether your child's profile maps to seeking, filtering, or perceptual difference
- Optimal session timing and duration for maximum response
- Progression rate relative to population benchmarks (20M+ session comparison)
- When to advance to the next technique in the pathway
What You Receive
- Real-time technique difficulty recommendations
- Material category prioritisation based on your child's patterns
- Alert flags if response patterns suggest professional reassessment
- Personalised week-by-week milestone targets
- Connection to families with similar response profiles
Privacy & Data Protection: Your child's data is encrypted, anonymised for population-level analysis, and governed under DPDPA (India), GDPR (EU), and HIPAA (US) compliance frameworks. Your data helps every child like yours — while your child's identity remains protected.

Watch: 9 Materials That Help When a Child Looks from Angles
Reel A-068
Sensory Solutions — Episode 68
75–85 seconds
This reel shows each of the 9 materials in action, demonstrated by Pinnacle therapists with real therapeutic interactions. See how light tables, magnifiers, kaleidoscopes, and visual tracking materials are used in both clinical and home settings — exactly as described in this protocol.
"9 Materials That Help When Child Looks from Angles" — The reel that brought you here. Share it with families who need to see it.
Video embed placeholder — Reel A-068. Duration: 75–85 seconds. Available on the Pinnacle Blooms YouTube channel and within the GPT-OS® platform.
Reference: NCAEP (2020) — Video modelling is an evidence-based practice for autism intervention

Consistency Across Caregivers Multiplies Impact
A technique practised at home but not understood at school or by grandparents loses half its power. Every adult in your child's life who understands — and accommodates — their visual processing difference is a co-therapist.
"Explain to Grandparents" Version
Your grandchild looks at things from unusual angles — tilted head, close up, from the side. This isn't a vision problem; their eyes are fine. Their brain processes visual information differently. We're using special materials (light tables, magnifying glasses, kaleidoscopes) to give their brain what it needs and help them develop more flexible looking over time.
You can help by: (1) Not forcing them to "look properly." (2) Joining them in exploring things from their angle. (3) Using the magnifying glass or kaleidoscope together. Every caregiver who understands helps.
Teacher Communication Template
[Child's name] has visual processing differences that result in looking at objects and materials from unusual angles. This is a neurological processing difference, not defiance or inattention.
Helpful accommodations include: allowing some flexibility in viewing position • reducing visual complexity in their work area • providing visual breaks • positioning materials accessibly. Please contact us to discuss further.
Share This Page
📱 WhatsApp | 📧 Email | 🔗 Copy Link
Reference: WHO CCD Package — Multi-caregiver training critical for intervention generalisation | PMC9978394

Frequently Asked Questions
Is angle-looking a sign of autism?
Angle-looking is commonly associated with autism and sensory processing differences, but it can also occur in other developmental contexts. It is one behavioural indicator among many and should be assessed within a comprehensive developmental evaluation. If it is persistent and accompanied by other developmental concerns, professional evaluation is recommended.
Will my child grow out of this?
Some degree of visual exploration flexibility develops naturally with age, but persistent, rigid angle-looking typically benefits from structured intervention. Without support, the behaviour may become more entrenched. With the Visual Angle Exploration protocol, children develop alternative visual strategies and increasing flexibility over an 8–12 week timeline.
Should I stop my child from looking at things from angles?
No. Abruptly stopping the behaviour removes a coping mechanism without addressing the underlying need. The protocol adds appropriate alternatives first, builds visual flexibility gradually, and reduces rigid angle-looking as the child develops more visual options. Always add before you subtract.
How long before I see improvement?
Initial tolerance and engagement typically emerge in weeks 1–2. Consolidation signs in weeks 3–4. Measurable visual flexibility in weeks 5–8. However, every child's timeline is individual. The tracking data from your sessions is the most accurate progress indicator — not the calendar.
Can I do this without a professional?
The home protocol is designed for parent execution. However, a comprehensive eye exam is essential before starting, and occupational therapy assessment optimises the approach by identifying the specific function of your child's angle-looking. Professional support enhances — but is not required for — beginning the protocol.
What if my child has both angle-looking AND light sensitivity?
These commonly co-occur. The protocol addresses both through the visual filtering materials. Start with filtering and sensory provision materials before introducing light-based activities. Consult with a developmental optometrist for individualised guidance on the balance between light exposure and filtering.
Is this covered by insurance?
Occupational therapy assessment and treatment for sensory processing differences is covered by many insurance plans in India and internationally. The home materials are out-of-pocket but include zero-cost DIY alternatives. Contact the Pinnacle helpline (9100 181 181) for insurance guidance specific to your location.
Can school implement this too?
Yes. The teacher communication template (Card 37) provides a starting point. Many material categories (magnifying glasses, visual detail books, kaleidoscopes) can be incorporated into classroom accommodations. Formal accommodation plans can be developed with school collaboration and OT support.

Your Next Step — Start Now
You've read the science. You understand the brain. You have the materials list and the complete protocol. Your child's visual processing journey begins with one session — and that session begins today.
🟢 Start This Technique Today
Download the complete tracking sheet, set up your space using Card 12, and run Session 1 using Cards 14–19. The first session takes 15 minutes and requires only household materials to begin.
🔵 Book a Professional Consultation
Connect with a Pinnacle OT specialising in visual processing for personalised assessment and protocol optimisation. Available in-clinic at 70+ locations or via teleconsultation for remote families.
⚪ Explore the Next Technique
Continue building your child's sensory processing toolkit with the next technique in the pathway. View the complete progression map at Card 28 to choose your next step.
OT
SLP
ABA
Special Education
NeuroDevelopmental Paediatrics
CRO
Validated by the Pinnacle Blooms Consortium
Preview of 9 materials that help when child looks from angles Therapy Material
Below is a visual preview of 9 materials that help when child looks from angles therapy material. The pages shown help educators, therapists, and caregivers understand the structure and content of the resource before use. Materials should be used under appropriate professional guidance.




















Share this resource
Help others discover thisLink copied!

From Fear to Mastery. One Technique at a Time.
Pinnacle Blooms Network®
Built by Mothers. Engineered as a System.
You arrived on this page confused — "Why does she look at everything sideways?" You leave empowered with a clinically validated protocol, 9 therapeutic materials (with zero-cost alternatives), a 6-step session structure, progress tracking tools, and a clear pathway forward.
Your child sees the world from angles most people never notice. That's not broken vision. That's different vision. And now it's becoming flexible vision.
20M+
Exclusive 1:1 Sessions
Exclusive therapy sessions across the Pinnacle Blooms Network powering GPT-OS® intelligence
97%+
Measured Improvement
Across validated outcome measures for children completing the full protocol
70+
Centres Across India
With teleconsultation available worldwide for families in remote locations
160+
Countries
Patents filed across 160+ countries for the GPT-OS® Global Paediatric Therapeutic Operating System
📞FREE National Autism Helpline: 9100 181 181 (16+ languages, 24/7) | 🌐pinnacleblooms.org | ✉️care@pinnacleblooms.org
Medical Disclaimer: This content is educational. It does not replace assessment by a licensed occupational therapist, developmental optometrist, or healthcare provider. Persistent unusual visual behaviours should be evaluated comprehensively — including vision assessment — to rule out visual impairments and understand the child's sensory processing profile. Individual results may vary. Statistics represent aggregate outcomes across the Pinnacle Blooms Network.
Statutory Identifiers: CIN: U74999TG2016PTC113063 | DPIIT: DIPP8651 (Govt. of India) | MSME: TS20F0009606 | GSTIN: 36AAGCB9722P1Z2 | ISO 13485: Medical Device QMS | ISO/IEC 27001: Information Security
© 2026 Pinnacle Blooms Network®, unit of Bharath Healthcare Laboratories Pvt. Ltd. All rights reserved.
