
Sensory Solutions Series — Episode 32
Ages 2–12 Years
She's Not Being Dramatic. Everyday Sounds Are Hurting Her.
The moment you walk into a store, her hands go to her ears. The blender, the vacuum, the hand dryer in public bathrooms — she screams like she's in pain. Birthday parties are impossible. School assemblies end in meltdowns. You can't go to restaurants, movies, or crowded places. People think she's being dramatic. She's not. The sounds that don't bother anyone else are physically hurting her.
You are not failing. Your child's nervous system is speaking.
When a child covers their ears at sounds that don't bother anyone else, it's not drama — it's auditory over-responsivity. Their brain's volume dial is turned all the way up. The fire alarm that startles you is shattering her. The blender you barely notice is an assault on her nervous system. The birthday singing that makes you smile triggers her fight-or-flight response.
This page was built for you — by a consortium of Occupational Therapists, Speech-Language Pathologists, Board Certified Behavior Analysts, Special Educators, NeuroDevelopmental Pediatricians, and parents who have walked this exact path. What follows are 9 materials that help protect the nervous system and make the sound world survivable.
🧠 Auditory Processing + Sound Sensitivity
🏠 Home + School + Community
Pinnacle Blooms Network® | Built by Mothers. Engineered as a System. | Powered by GPT-OS® Therapy Intelligence
Research: WHO Nurturing Care Framework (2018) validates that early identification and parental awareness directly impacts outcomes.

You Are Among Millions of Families Navigating This Exact Challenge
Sound sensitivity is not rare. It is not unusual. It is not something your family alone faces. Across the world — from Hyderabad to Houston, from Mumbai to Melbourne — millions of families are navigating the exact moment when their child covers their ears and the world becomes too loud. The numbers tell a story of how widespread this experience truly is.
80%
Sensory Difficulties in Autism
of children diagnosed with autism display sensory processing difficulties, including auditory over-responsivity
Source: PRISMA Systematic Review, 2024 (PMC11506176)
1 in 6
Sensory Processing Differences
children experiences clinically significant sensory processing differences that affect daily functioning
Source: Meta-analysis, World Journal of Clinical Cases, 2024
5–16%
School-Age Sound Sensitivity
of school-age children worldwide exhibit sound sensitivity sufficient to interfere with classroom participation and social engagement
Source: SPD Foundation epidemiological data
Research: PMC11506176 | PMC10955541 | DOI: 10.12998/wjcc.v12.i7.1260

The Volume Dial Your Child Cannot Control
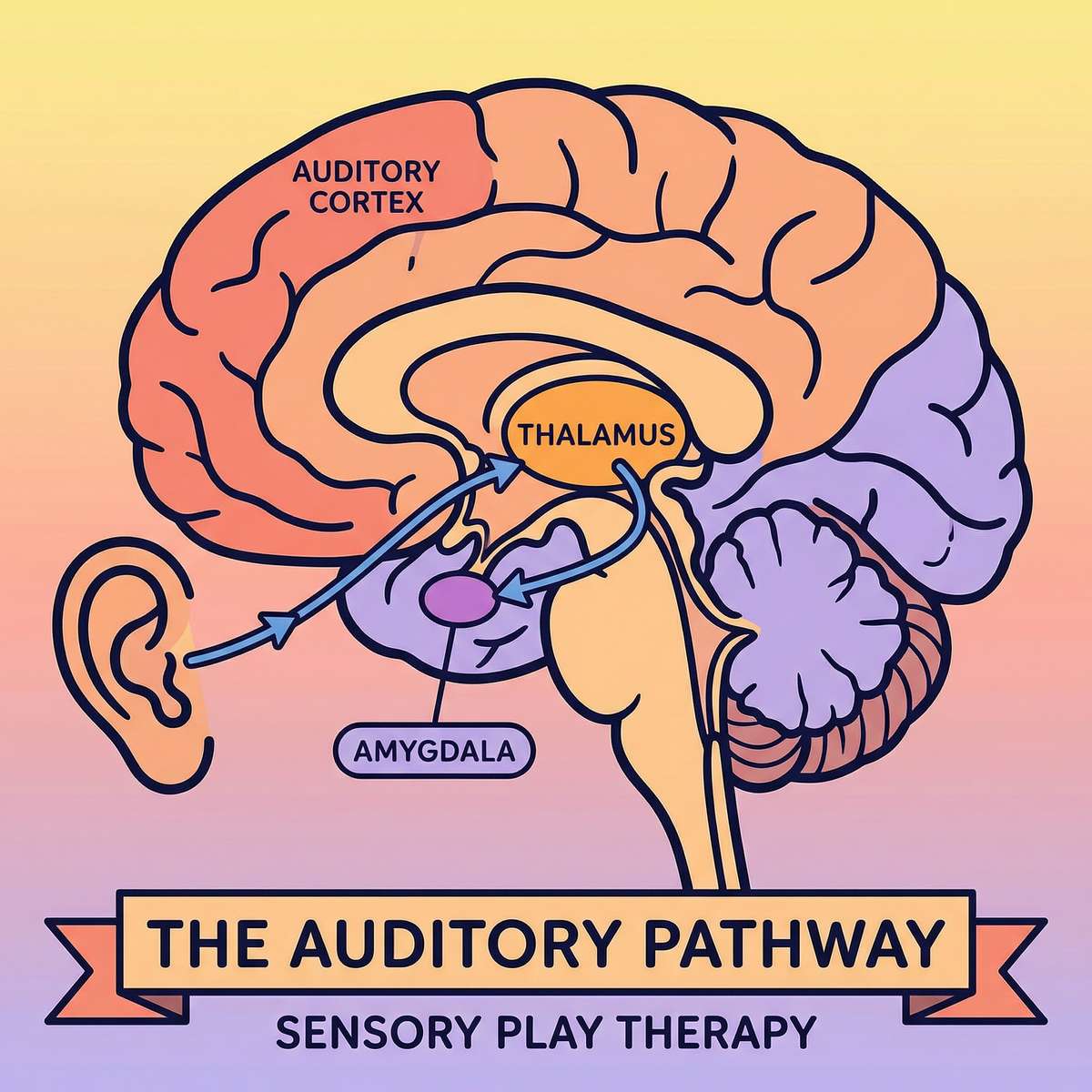
The auditory pathway: sound enters the ear → travels to the auditory cortex → processed by the brain's filtering system. In auditory over-responsivity, the filtering system fails to dampen sound adequately, and the amygdala triggers fight-or-flight.
What's Happening in Your Child's Brain
Your child's brain processes sound differently from a neurotypical brain. Here is precisely what happens:
The Volume Dial Is Stuck on Maximum
In typical auditory processing, the brain adjusts sound intensity — turning down background noise, filtering what matters from what doesn't. In auditory over-responsivity, this filtering system is underperforming. Every sound registers at near-maximum intensity. The refrigerator hum that you don't notice? She hears it at the same volume as your voice.
The Threat Detector Is Oversensitive
The amygdala — the brain's danger alarm — interprets loud or sudden sounds as genuine threats. A hand dryer triggers the same neurological response as a predator's growl would. This is not a conscious choice. This is a hardwired neurological response. Covering ears, fleeing, crying, or melting down are protective responses to genuine sensory distress.
This Is a Wiring Difference, Not a Behavior Choice
Your child is not being dramatic. She is not seeking attention. Her nervous system genuinely perceives everyday sounds as assaultive. Understanding this changes everything — from blame to compassion, from punishment to protection.
Research: Frontiers in Integrative Neuroscience (2020): Comprehensive framework for evaluating sensory integration/sensory processing treatment in ASD. DOI: 10.3389/fnint.2020.556660

The Developmental Map: Where Your Child Is and Where They're Heading
0–6 Months
Startle response to loud sounds (typical). Auditory system beginning to calibrate. This is the earliest stage of sound processing development.
6–18 Months
Beginning to filter foreground from background. Over-responsive children may already show distress with household sounds like vacuums or mixers.
18 Months–3 Years ⚠️
PRIMARY IDENTIFICATION WINDOW. Sound sensitivity becomes clearly visible — fear of specific sounds, avoidance of noisy environments, meltdowns triggered by everyday noise. This is when most parents first notice.
3–6 Years
Sound sensitivity impacts school readiness — cafeteria noise, fire drills, group activities become barriers to participation. Anticipatory anxiety about sounds may develop.
6–12 Years
With appropriate intervention, many children develop coping strategies and tolerance. Without intervention, avoidance patterns and anxiety may solidify. The window for neuroplasticity-driven change remains open.
Your child is somewhere on this timeline. Every point has a forward path. Sound sensitivity commonly co-occurs with tactile sensitivity, visual sensitivity, vestibular processing differences, anxiety, and social withdrawal. The auditory system does not operate in isolation.
Research: WHO Care for Child Development (CCD) Package — age-specific evidence-based recommendations. Implemented in 54 low- and middle-income countries. PMC9978394 | WHO/UNICEF CCD Package (2023)

Evidence Grade: Level I-II — Systematic Review + RCT Supported
🛡️
EVIDENCE GRADE
STRONG
16 studies from 2013–2023 confirm sensory integration intervention meets criteria to be considered evidence-based practice for children with ASD.
Key Finding
A PRISMA-model systematic review (2024) analyzing 16 articles established that sensory integration therapy, including auditory-focused interventions, demonstrates significant effectiveness for children with autism spectrum disorder. An Indian RCT (Padmanabha et al., 2019) specifically validated home-based sensory interventions with measurable outcomes in the Indian pediatric population.
What This Means for You
The materials and strategies on this page are not opinions. They are drawn from peer-reviewed clinical research, validated across populations, and implemented across 70+ Pinnacle Blooms centers serving children from 70+ countries. The evidence says: these work.
Clinically validated. Home-applicable. Parent-proven.
- 🔗 PubMed: PMC11506176 — Systematic Review of Sensory Integration for ASD
- 🔗 DOI: 10.1007/s12098-018-2747-4 — Padmanabha et al., Indian Journal of Pediatrics, 2019
- 🔗 PMC10955541 — Meta-analysis, World Journal of Clinical Cases, 2024

Domain A: Sensory Processing
Code: SEN-AUD-DEF
Auditory Protection & Tolerance-Building Materials Protocol
Parent-Friendly Name: "Sound Survival Kit"
A structured approach to managing auditory over-responsivity through nine categories of materials that serve three functions: protect the nervous system from overload, provide control over the auditory environment, and gradually build tolerance through supported exposure. This is not about blocking all sound forever — it is about giving the child tools to survive and then thrive in a world that is genuinely too loud for their nervous system.
👶 Ages 2–12 years
⏱️ Ongoing Daily Strategy
🏠 Home + School + Community
📦 9 Material Categories

This Technique Crosses Therapy Boundaries
Because the brain doesn't organize by therapy type, this protocol draws from multiple clinical disciplines. Each professional contributes unique expertise to help your child navigate the sound world with confidence.
Occupational Therapist (Primary Lead)
Leads sensory processing evaluation. Designs sensory diet including auditory protection strategies. Administers therapeutic listening programs. Develops environmental modifications for home and school. Builds tolerance protocols through graded sensory exposure.
Speech-Language Pathologist
Addresses auditory filtering difficulties affecting speech comprehension. Works on auditory processing for language development. Adapts communication strategies for noisy environments. Monitors how sound sensitivity impacts social communication.
Board Certified Behavior Analyst
Develops antecedent strategies to prevent sound-triggered meltdowns. Creates systematic desensitization protocols. Teaches functional communication to request accommodation. Builds coping skill chains and tracks behavioral data on sound tolerance.
Special Educator
Implements classroom accommodations for sound sensitivity. Creates visual supports and schedules including sound warnings. Adapts instructional delivery to minimize auditory overwhelm. Coordinates with family on consistency across environments.
NeuroDevelopmental Pediatrician
Evaluates auditory sensitivity within broader developmental profile. Rules out medical contributions to sound intolerance. Coordinates multi-disciplinary intervention planning. Monitors developmental progression over time.
Research: Adapted UNICEF/WHO Nurturing Care Framework for SLPs (2022): Multiple disciplines contribute to nurturing care components. DOI: 10.1080/17549507.2022.2141327

Precision Targets: What These 9 Materials Address
Understanding what we're targeting helps you measure progress and celebrate the right milestones. These materials work across three tiers of developmental impact.
1
🎯 Primary Target: Auditory Modulation
Reduce the distress response to everyday sounds. Build the child's ability to tolerate typical environmental noise without fight-or-flight activation.
Measure: Decrease in ear-covering frequency, reduction in sound-triggered meltdowns, ability to remain in previously impossible environments.
2
🎯 Secondary Targets
- Environmental Participation — Ability to attend parties, school events, restaurants, public spaces
- Anticipatory Anxiety Reduction — Decrease in worry about upcoming sounds and noisy environments
- Self-Regulation — Independent use of tools without parent prompting
- Social Engagement — Ability to participate in group activities despite auditory sensitivity
3
🎯 Tertiary Developmental Gains
- Sensory Integration Maturation — Neuroplastic changes in auditory processing efficiency
- Anxiety Regulation — Broader emotional regulation capacity
- Self-Advocacy — Child learns to identify need and request accommodation
- Academic Access — Improved classroom participation
Research: Meta-analysis (World J Clin Cases, 2024): Sensory integration therapy effectively promoted social skills, adaptive behavior, sensory processing, and motor skills across 24 studies. PMC10955541

Your Sound Survival Kit — 9 Materials at a Glance
# | Material | Purpose | Price Range | Professional Required? | |
1 | Noise-Reducing Headphones / Ear Defenders | Turn down the world's volume | ₹800–4,000 | No | |
2 | White Noise Machine / Sound Masking | Mask unpredictable sounds | ₹500–3,000 | No | |
3 | Noise-Canceling Headphones | Active technology blocks sound | ₹3,000–15,000 | No | |
4 | Therapeutic Listening Programs | Recalibrate the auditory system | ₹5,000–30,000 | ⚠️ Yes — OT Required | |
5 | Visual Schedules / Sound Warnings | Predictability reduces distress | ₹0–500 | No | |
6 | Fidget Tools / Regulation Objects | Other senses regulate auditory overload | ₹100–800 | No | |
7 | Quiet Space / Sensory Retreat Area | Escape when the world is too loud | ₹500–10,000 | No | |
8 | Calming Music / Chosen Soundscape | Replace assault with choice | ₹500–5,000 | No | |
9 | Social Stories / Sound Preparation | Understanding and preparing for challenges | ₹0–1,000 | No |
Essential Starters (Begin Here): 1) Noise-reducing headphones — essential first purchase. 2) Visual warnings for predictability — free to create at home. 3) Quiet space accessible at home and school — can be a corner with cushions.
Total Investment Range: ₹0 (DIY strategies only) to ₹30,000 (complete professional toolkit)
Total Investment Range: ₹0 (DIY strategies only) to ₹30,000 (complete professional toolkit)

Can't Buy Everything? Start With What You Have.
The Pinnacle Blooms Consortium believes every family deserves access to effective intervention — regardless of budget. Here are clinician-approved DIY alternatives you can start using today.

White Noise → Use a Fan
A consistent fan provides steady background masking sound. Free white noise apps on your phone work too. YouTube white noise videos with screen off. Air purifiers provide a consistent hum that softens jarring sounds.

Visual Schedules → Draw Them
Simple drawings or printed pictures showing what sounds to expect today. Countdown with fingers before turning on the blender. Verbal warnings given consistently before every loud sound. These cost nothing and transform unpredictability into safety.

Quiet Space → A Corner with Cushions
A tent made from bedsheets. A closet cleared and lined with pillows. A corner with heavy curtains. Any space that reduces sound levels and gives the child control to retreat when the world becomes too loud.

Social Stories → Write Your Own
"Tomorrow we go to Grandma's house. There will be many people talking. The TV may be loud. I can wear my headphones. I can go to the quiet room if I need a break. It's okay to ask for help."
⚠️ What Has No DIY Equivalent: Noise-reducing headphones (improvised ear covering doesn't protect adequately), noise-canceling headphones (active technology cannot be replicated), therapeutic listening programs (random music is NOT therapeutic — specific protocols and equipment are required under professional guidance).

Before You Begin: Safety Non-Negotiables
Your child's safety is the foundation of every strategy on this page. Before introducing any material, review these critical guidelines carefully.
🔴 Contraindications — When NOT to Use
- Therapeutic listening programs: NOT without professional evaluation and guidance. Incorrect use can dysregulate rather than help. Contraindicated with seizure history, certain ear conditions.
- Noise-canceling headphones: Can be disorienting for some children. Introduce gradually. Not for situations where hearing safety sounds is critical (crossing roads, around vehicles).
🔴 Material Safety Checks
- Headphone fit: Too tight causes headache and discomfort; too loose doesn't protect. Check sizing for child's head.
- Volume levels: If using music through headphones, monitor volume. Very loud music to drown out environment can damage hearing.
- White noise placement: Don't place machines too close to the child's ears. Monitor comfortable volume levels.
- Fidget tools: Check for choking hazards appropriate to child's age and oral behaviors.
- Quiet space: Ensure the child can exit freely. Never lock or restrict. The space is a choice, not a containment.
🔴 Red Line — Stop If You See
- Child becomes MORE distressed with a specific material (not every tool suits every child)
- Physical pain complaints about ears after headphone use
- Behavioral regression — increased meltdowns or withdrawal when a new strategy is introduced
- Signs of ear infection (pulling at ears, fever, drainage)
Trust your instincts — if something feels wrong, pause and ask.
Research: Indian Journal of Pediatrics RCT (2019): Home-based sensory intervention safety protocols established for parent-administered sessions. DOI: 10.1007/s12098-018-2747-4
Preparing Your Home for Sound-Sensitive Living
Your home environment is the foundation of your child's sound survival strategy. Strategic placement of tools and thoughtful environmental modifications create a sensory-friendly space where your child can feel safe.
1
Quiet Zone (Essential)
Identify one corner or small room in your home as the designated quiet retreat. Line with soft furnishings — cushions, rugs, heavy curtains that absorb sound. This is your child's safe harbor when the world becomes too loud.
2
Headphone Station
Keep noise-reducing headphones in 3 locations — near the front door (for going out), in the child's room (for sleeping/studying), and in the main living area (for daily use). Accessibility prevents crisis.
3
Sound Warning Board
Place a simple visual schedule near the kitchen or living room showing today's potentially loud activities. "10:00 AM — Vacuum (use headphones)" / "4:00 PM — Mixer for cooking"
4
White Noise Placement
Bedroom — for sleep. Study area — for focus. Between the child's space and noise sources — as a buffer. Strategic placement maximizes sound masking effectiveness.
5
Fidget Basket
Small container near the child's usual spots with regulation objects — stress ball, textured items, weighted objects. Always within arm's reach when auditory overload strikes.
Environmental Modifications: Tennis balls on chair legs to reduce scraping sounds. Soft-close cabinets and doors where possible. Reduce unnecessary auditory stimuli — turn off background TV when not being watched. Identify and fix buzzing/humming sources (flickering lights, loose appliances).
Research: Sensory Integration Theory (Ayres): Environmental setup is a core principle. Meta-analysis confirms structured environment is most effective. PMC10955541

Act III: The Execution
Pre-Session Readiness Assessment (60-Second Check)
Before introducing any new auditory material or strategy, run this checklist. The best session is one that starts right. Pushing through when the child isn't ready teaches the nervous system that these tools come with stress — the opposite of what we want.
01
✅ Child is fed and hydrated
Hunger amplifies sensory sensitivity significantly
02
✅ Child has slept adequately
Fatigue lowers sensory thresholds across all channels
03
✅ No recent meltdown within the past hour
The nervous system needs recovery time between episodes
04
✅ Child is in a relatively calm state
Not already overstimulated in other sensory channels
05
✅ No signs of illness
Especially ear infection or headache — rule these out first
06
✅ Environment is at manageable sound level
Start calm before building challenge
07
✅ You (the parent) are calm and regulated
Your anxiety is contagious to the nervous system
✅ All Checked → GO
Proceed with introduction
⚠️ 1–2 Unchecked → MODIFY
Simplified, shorter version. One tool only.
🛑 3+ Unchecked → POSTPONE
Protection day. Try again tomorrow.
Research: ABA Principles: Antecedent manipulation and setting events determine intervention effectiveness.

Material 1: Introducing Noise-Reducing Headphones
The Essential First Tool — Never Force, Always Invite
Day 1–3: Familiarization
Place the headphones where the child can see and touch them. Don't put them on the child's head. Let them be curious. If the child picks them up — wonderful. If not — they're just part of the environment now. Say: "These are your sound helpers. They make loud things quieter."
Day 4–7: Modeling
You wear them. A sibling wears them. Show that they're safe, comfortable, and that people look okay wearing them. Let the child try putting them on a stuffed animal or doll. Normalize them as everyday objects.
Day 7–14: Supported Trial
During a calm moment (NOT during a meltdown), offer: "Would you like to try your sound helpers?" If yes — celebrate. If no — that's okay. The headphones stay available. Try again tomorrow.
Day 14+: Functional Use
Once the child accepts wearing them, introduce during a mildly challenging sound environment. Gradually move to more challenging settings. The child learns: headphones = I can survive this.
Key Insight: Having headphones available creates safety — even if the child doesn't always use them. Knowing protection is accessible reduces anticipatory anxiety. Keep headphones in backpack, car, and at school.
Troubleshooting
- Child refuses to wear them → Don't force. Try different styles (headband vs. over-ear). Desensitize to the sensation on their head first.
- Child wears them but still distressed → The environment may be too challenging. Step back to a less noisy setting.
- Headphones cause discomfort → Check fit. Try different sizes. Some children prefer earplugs to over-ear styles.
Price: ₹800–4,000 | Recommended: Peltor Kids, Loop Earplugs, child-sized ear defenders

Material 2: Setting Up White Noise — Your Auditory Buffer Zone
What White Noise Does
White noise fills the auditory space with consistent, predictable sound that masks jarring environmental noises. The brain stops straining to monitor for threatening sounds because the background is consistently filled. Unpredictable sounds are more distressing than consistent ones — white noise removes the unpredictability.
Setup Protocol
Start in the Bedroom
Place white noise machine in the child's bedroom first (for sleep — where benefit is most immediate and noticeable).
Calibrate Volume
Start at low volume. Gradually increase to the level where environmental sounds are softened but the child can still hear you speaking.
Experiment with Noise Colors
White noise (higher frequency), pink noise (softer), brown noise (deeper). Your child's preference matters — let them choose which feels most soothing.
Extend Placement
Add to study area and between child's space and noise sources. Strategic positioning creates auditory buffer zones throughout the home.
DIY: Fan for background sound. White noise apps on phone. Air purifier hum. YouTube white noise videos with screen off.
Price: ₹500–3,000

Material 3: Active Noise Cancellation — For Severe Sensitivity
Active noise-canceling headphones use technology to counteract sound waves, providing deeper reduction than passive ear defenders. They are particularly effective for continuous low-frequency sounds — airplane engines, vehicle noise, HVAC systems — that passive headphones may not fully address.
When to Choose Active Over Passive
- Child has severe sensitivity that passive ear defenders don't adequately address
- Frequent exposure to persistent low-frequency sounds (travel, vehicles, busy roads)
- Child benefits from combined cancellation + calming music (portable sound sanctuary)
- Multiple challenging environments in a single day requiring sustained protection
Introduction Protocol
Follow the same graduated approach as noise-reducing headphones (Material 1). Active noise canceling can feel strange — the sudden quiet can be disorienting for some children. Introduce in familiar, comfortable settings first. Let the child control when they turn the feature on and off.
Safety Notes
Can be disorienting. Introduce gradually. Ensure child can hear safety-critical sounds when needed. Battery-dependent — keep charged. Not recommended when hearing environmental awareness is essential.
Cost Consideration: ₹3,000–15,000 — significantly more expensive than passive defenders. For many children, passive protection is sufficient. Active cancellation is worth the investment for severe cases where passive protection alone isn't enough.

Material 4: Therapeutic Listening — Recalibrating the Auditory System
⚠️ THIS MATERIAL REQUIRES PROFESSIONAL GUIDANCE. Therapeutic listening programs are NOT background music. Incorrect use can dysregulate rather than help. Always work with a qualified Occupational Therapist.
Therapeutic listening programs use specially designed, filtered music to gently challenge and gradually recalibrate the auditory system over weeks to months. Unlike sudden exposure (which causes distress), these programs introduce modified sound in controlled therapeutic doses.
Programs Used at Pinnacle Blooms
Integrated Listening Systems (iLs)
Multi-sensory approach combining auditory, balance, and movement for comprehensive nervous system retraining
Therapeutic Listening
Modified music with frequency filtration that systematically challenges the auditory system at therapeutic levels
The Listening Program
Progressive auditory training that builds tolerance through carefully sequenced sound experiences
Safe and Sound Protocol
Polyvagal-based intervention targeting middle ear muscles and vagal regulation for calming the nervous system
What Parents Should Know
- Professional evaluates appropriateness for YOUR child specifically
- Specific equipment and protocols are prescribed individually
- Improvement is gradual — weeks to months, not days
- Combine with protection strategies for immediate relief while therapeutic listening works long-term
Price: ₹5,000–30,000 (program + equipment)

Materials 5 & 6: Visual Warnings + Fidget Tools

Material 5: Visual Warnings — Predictability Reduces Distress
Unpredictable sounds are more distressing than expected ones. Visual schedules with sound warnings give the nervous system time to prepare. Warning allows bracing rather than being ambushed.
Implementation
- Create a daily schedule showing potentially loud events: "10 AM — Vacuum" / "3 PM — Mixer"
- Use countdown before loud appliances: "Blender in 5... 4... 3... 2... 1..."
- Work with school to provide advance warning of fire drills, assemblies
- Color-code expected sound levels: 🟢 Quiet → 🟡 Moderate → 🔴 Loud
Price: ₹0–500 | DIY: Draw or print simple schedules. Verbal warnings cost nothing.

Material 6: Fidget Tools — Other Senses Regulate Auditory Overload
When the auditory system is overwhelmed, engaging other sensory channels helps regulate the nervous system overall. Squeezing, manipulating, or holding weighted objects grounds the body while the ears are under assault.
Recommended Tools
- Stress balls and squeeze toys
- Textured objects (smooth stones, spiky balls)
- Weighted lap pad
- Putty or theraputty
- Chewable jewelry (for oral seekers)
Keep a small "regulation kit" in the child's backpack — always accessible wherever you go.
Price: ₹100–800

Materials 7, 8 & 9: Quiet Space + Music + Social Stories

Material 7: Quiet Space — Escape When the World Is Too Loud
Having a quiet space to retreat to is essential. Sound-absorbing materials reduce sound levels. The child learns they CAN escape when needed, reducing panic about being trapped in noise.
Setup: Canopy tent, corner with heavy curtains, closet converted with cushions. Include soft lighting, comfort objects, headphones available. Rules: This space is always accessible. No one follows to scold. This is safety.
Price: ₹500–10,000 | DIY: Bedsheet tent, pillow corner, curtained nook

Material 8: Calming Music — Replace Assault with Choice
When the child controls the sound, it becomes less threatening. Personal music with familiar, calming songs replaces overwhelming environmental noise with chosen sound. Control transforms the experience from passive victim to active participant.
Implementation: Build playlists together. Different playlists for different situations — calming, focusing, transitioning. Old phone or MP3 player loaded with the child's choices.
Price: ₹500–5,000 | DIY: Old phone + curated playlist

Material 9: Social Stories — Understand and Prepare
Social stories help children understand their own sensitivity and develop coping strategies. Preparation stories before challenging events reduce anxiety by creating predictability and rehearsing coping.
Example: "Tomorrow we go to the birthday party. There will be singing and clapping. I can wear my headphones. I can go to the quiet room if I need. I can squeeze my stress ball. It's okay to ask Mama for help."
Price: ₹0–1,000 | DIY: Write your own with your child's specific challenges, tools, and strategies

Your Sound Sensitivity Tracker
Track your child's progress weekly. This data drives personalization and helps you see patterns your instincts might miss. Consistent tracking transforms subjective impressions into clear, actionable insights.
Track These Weekly
- Number of ear-covering episodes per day (average)
- Meltdowns triggered by sound (count)
- New environments tolerated with tools
- Duration of time in noisy environments before needing break
- Which tools were used and which were most helpful
- Child's self-initiation of tool use (independent vs. prompted)
Rating Scale (Parent Report)
1 = Unable to tolerate any normal-volume environment
2 = Manages only with constant protection and supervision
3 = Tolerates some challenging sounds with support
4 = Uses tools appropriately across most situations
5 = Independently manages most auditory challenges

When Things Don't Go as Planned
"My child refuses to wear headphones."
Don't force. Try different styles — some children hate over-ear but accept earplugs. Desensitize to the sensation gradually. Start by wearing them loosely around neck. Let them see peers or siblings wearing them. Make headphones part of pretend play. Patience is the protocol.
"The white noise machine seems to make things worse."
Try a different noise color. White noise is higher frequency; some auditory-sensitive children do better with brown noise (deeper, less sharp). Or the volume is too high — lower it significantly. Some children prefer nature sounds over pure noise.
"We see no improvement after 4 weeks."
Track which specific sounds remain challenging. Some improvements are subtle — fewer meltdowns, faster recovery, willingness to attempt previously avoided situations. If genuinely no improvement, consult an OT for sensory evaluation. The child may need a comprehensive sensory diet beyond these materials.
"Sound sensitivity seems to be getting worse."
Check for illness (ear infection), increased stress, sleep disruption, or changes in routine. Sensitivity amplifies when the child is tired, stressed, or overstimulated in other sensory channels. If worsening persists, seek professional evaluation immediately.
"School won't accommodate."
Request a formal meeting. Bring this page as documentation. Sound sensitivity accommodations can be written into education plans. Specific requests: ear defenders permitted at all times, advance warning of fire drills, access to quiet space, preferential seating away from speakers.
Every Child's Sound Profile Is Unique — Adapt This Protocol
There is no single-size approach to auditory over-responsivity. Your child's specific pattern determines which materials and strategies to prioritize. Find the profile that most closely matches your child below.
Sensitive to SPECIFIC Sounds
(vacuum, blender, hand dryers)
Focus on: Noise-reducing headphones before known triggers + visual warnings + social stories specific to those sounds. The targeted approach.
Overwhelmed by ALL Noise
(crowded environments, general sound levels)
Focus on: Noise-canceling headphones + white noise in home + quiet space as essential retreat + strict environmental modifications. The protective bubble approach.
ANTICIPATORY ANXIETY
(fears the possibility of loud sounds)
Focus on: Visual schedules + social stories + headphones AVAILABLE at all times + gradual supported exposure. The predictability approach.
Also SEEKS Certain Sounds
(loves music, hums constantly)
Focus on: Chosen music/soundscapes + therapeutic listening programs (professional guided) + using preferred sounds as regulation tools. The replacement approach.
For children with MULTIPLE sensory sensitivities: This page addresses auditory. The nervous system is interconnected. Explore related techniques: A-030 (Tactile), A-033 (Vestibular), A-035 (Visual). A comprehensive sensory diet — designed by an OT — addresses the whole child.

Act IV: The Progress Arc
What to Expect: Weeks 1-2
25%
Progress
Tolerance-building phase
You May See
- Child tolerates headphones for increasing durations
- Slight decrease in ear-covering frequency (even 10% is meaningful)
- Child begins to associate headphones with relief
- Willingness to attempt one previously avoided environment WITH tools
- Child uses visual schedule or countdown without distress
- Parent reports feeling less hypervigilant about sound management
This Is Normal in Weeks 1-2
- Child still needs constant prompting to use tools
- Meltdowns still occur — they may be slightly shorter or less intense
- Some tools work, others don't yet
- Inconsistency between days (good days and hard days)
This is the tolerance-building phase. The nervous system is beginning to learn that these tools provide safety. Neural association takes repetition. Keep going.

Weeks 3-4: Neural Pathways Are Forming
50%
Progress
Consolidation phase
Look For These Signs
- Child begins to reach for headphones independently before entering noisy situations
- Ability to remain in challenging environments longer (even minutes more is progress)
- Decreased recovery time after auditory overload episodes
- Child may start verbalizing: "It's too loud" or "I need my headphones" (functional communication)
- White noise becomes part of routine (child may request it)
- Some previously terrifying sounds downgraded to "uncomfortable"
Consolidation Markers: Behavioral changes signaling neural pathway formation — the child spontaneously generalizes strategies to new settings. She reaches for headphones before YOU remind her. This is the brain learning.
<
Parent Milestone: You may notice you're more confident too. You're scanning environments less anxiously. You have a plan. Your stress is decreasing alongside your child's. That matters deeply.

Weeks 5-8: Mastery Emerging
75%
Progress
Mastery phase
Mastery Criteria (Observable and Measurable)
Independent Tool Selection
Without prompting in 70%+ of situations — the child chooses the right tool for the right moment
Environmental Tolerance
Previously impossible environments tolerated for functional duration — full birthday party, entire restaurant meal, school assembly
Self-Advocacy
Child communicates needs to teachers, peers, and family members independently and clearly
Flexible Coping
Child uses different strategies for different situations — headphones for the store, fidget tool for classroom, quiet space at home
Meltdown Reduction
Decreased frequency of sound-triggered meltdowns by 50%+ compared to baseline tracking
Generalization Indicators: Strategy appearing in new contexts the parent didn't explicitly train. The child asks to bring headphones to a new place. Creates their own quiet space at grandma's house. Tells a friend "loud sounds hurt my ears."
When to Move to Next Level: If mastery criteria met for 2+ consecutive weeks, the child is ready for graduated challenge — slightly more difficult auditory environments WITH tools available but not pre-deployed.

You Did This. Your Child Grew Because of Your Commitment.
Five to eight weeks ago, you arrived on this page scared, exhausted, and watching your child suffer through a world that was too loud. Today:
Tools That Work
Your child has a Sound Survival Kit
World Reopened
Your family can go places again
Managing, Not Just Enduring
Your child is learning to navigate
Advocate with Confidence
You understand the neuroscience
This is not a small thing. Every headphone offered with patience. Every visual schedule drawn. Every meltdown navigated with calm instead of panic. Every environment attempted when it would have been easier to stay home. YOU did this.
Family Celebration Suggestion: Go somewhere your child couldn't go before — with tools in hand. A restaurant. A movie. A party. Document the moment. This is the new baseline. 📸Journal Prompt: Take a photo of your child in a previously impossible environment, coping. Save it. On hard days, look at it. Progress is real.

Clinical Guardrails — When to Pause and Seek Professional Guidance
1
🔴 Worsening Sensitivity Despite Tool Use (4+ weeks)
What it looks like: Sound tolerance is decreasing, not increasing. Meltdowns are more frequent or intense. The child is withdrawing more.
What to do: Stop, evaluate, consult OT. There may be an underlying condition (hearing change, anxiety escalation, misophonia) requiring different intervention.
2
🔴 Physical Pain Complaints About Ears
What it looks like: Child reports ear pain, pulls at ears, shows signs of infection.
What to do: Audiological and ENT evaluation. Rule out medical causes before continuing sensory strategies.
3
🔴 Complete Avoidance of All Sound Environments
What it looks like: Child refuses to leave the house, quiet space becomes a permanent residence, social withdrawal accelerates.
What to do: This may indicate anxiety escalation beyond sensory processing. Psychological evaluation alongside OT.
4
🔴 Headphone Dependency Without Tolerance
What it looks like: Child wears headphones 100% of waking hours, panics without them, no graduated tolerance developing.
What to do: Consult OT to rebalance protection vs. exposure. Pure protection without tolerance-building creates dependency.
5
🔴 Regression in Other Developmental Areas
What it looks like: Language decreasing, social engagement dropping, sleep severely disrupted.
What to do: Comprehensive developmental evaluation. Sound sensitivity may be one symptom of a broader change.
Trust your instincts — if something feels wrong, pause and ask.
Your Developmental GPS — Where This Technique Leads
Your child's journey through sensory processing doesn't end here. This technique connects to a broader network of developmental support, each path tailored to your child's unique profile and response.
Lateral Alternatives
Environmental Modification Approach
Focus on changing the environment rather than equipping the child — for families where environmental control is more feasible
Systematic Desensitization Protocol
ABA-led approach for children who respond to structured behavioral interventions with data-driven exposure hierarchies

Explore Related Techniques

A-030: 9 Materials for Touch Sensitivity
When your child avoids or craves tactile input — the tools that help them navigate the world of texture, temperature, and touch

A-031: Body Awareness Difficulties
Proprioceptive processing challenges — when the body doesn't know where it is in space

A-033: Movement Seeking Behavior
Vestibular processing and constant motion — strategies for the child who never stops moving

A-034: Crashing and Bumping Behavior
Proprioceptive seeking through impact — understanding why your child crashes into everything

A-035: Light Sensitivity
Visual over-responsivity — when lights and visual input overwhelm the nervous system

A-036: Sensory Meltdowns
When overall sensory overload overwhelms all systems — the comprehensive meltdown management guide
Parent Support Techniques
- 🔗K-892: Living with a Sound-Sensitive Child
- 🔗K-893: School Accommodations for Sensory Processing
- 🔗K-894: When Multiple Senses Are Affected
This Technique Is One Piece of a Larger Plan
Sound sensitivity does not exist in isolation. The nervous system is interconnected. Auditory over-responsivity often co-occurs with tactile sensitivity, visual sensitivity, vestibular processing differences, anxiety, and social withdrawal. GPT-OS® maps your child's complete developmental profile across all 12 domains.
Research: WHO/UNICEF Nurturing Care Framework: Five components of nurturing care require holistic developmental monitoring. WHO NCF (2018) | UNICEF 2025 Country Profiles

Act V: Community & Ecosystem
Real Outcomes from Real Families
🎉 Birthday Party Victory
"Birthday parties used to be impossible. The singing, the clapping, the noise — she would scream and we'd have to leave within 5 minutes. We stopped accepting invitations."
After (8 weeks): "Now with her headphones and knowing she can go to a quiet spot when needed, she actually stays. She sang happy birthday last week — with her ear defenders on, and with a smile. That's everything."
— Parent, Pinnacle Network
📚 School Transformation
"Fire drills were traumatic. The cafeteria was impossible. He would come home from school exhausted and melting down every day."
After (6 weeks): "His teacher keeps ear defenders at his desk. He wears them for assemblies. He has a quiet pass to leave the cafeteria when he needs to. He's actually making friends now because he can stay in the room."
— Parent, Pinnacle Network
"Sound sensitivity creates a shrinking world. Every tool that makes one environment survivable expands that world back. The goal is never to eliminate sensitivity — it's to equip the child to live fully despite it." — Pinnacle Blooms Therapist
Note: Illustrative cases. Individual outcomes vary by child profile.

You Are Not Alone in This — Join Families Who Understand
If only one parent executes these strategies, impact is limited. When grandmother, teacher, babysitter, and both parents all understand and support the same approach — the child's progress accelerates exponentially.
Sensory Processing Parent WhatsApp Community
Connect with families navigating sound sensitivity specifically — share experiences, ask questions, find support
Pinnacle Parent Forum
Online community for parent-to-parent support across all therapy domains and techniques
Local Pinnacle Parent Meetups
Meet families near your center — face-to-face connection with people who truly understand
Peer Mentoring: Connect with a parent who has navigated auditory over-responsivity successfully. They've been where you are. Their experience is your shortcut. Consistency across caregivers multiplies impact.
Research: WHO NCF: Community engagement is a core principle. Parent support networks improve intervention outcomes.
When You Need Professional Guidance
Pinnacle Blooms Services for Sound Sensitivity
Occupational Therapy — Sensory Integration
Comprehensive sensory processing evaluation and intervention
Therapeutic Listening Programs
iLs, TLP, and Safe and Sound Protocol under professional guidance
AbilityScore® Assessment
Comprehensive developmental baseline across all 12 domains
EverydayTherapyProgramme™
Daily home protocols including auditory protection and desensitization
Assessment Path
1
AbilityScore® Assessment
Comprehensive developmental baseline
2
Sensory Evaluation
Identify auditory patterns and triggers
3
Individualized Sensory Diet
Auditory-specific materials and protocols
4
Ongoing Tracking
Sensory Regulation Index monitoring
📞FREE National Autism Helpline: 9100 181 181 (16+ languages, 24/7)
🌐 pinnacleblooms.org | 📧 care@pinnacleblooms.org
🌐 pinnacleblooms.org | 📧 care@pinnacleblooms.org
Published Evidence Supporting This Technique
Every material and strategy on this page is grounded in peer-reviewed clinical research. Below is the complete reference library for clinicians, program leads, and parents who want to verify the evidence themselves.
PMC11506176
PRISMA Systematic Review (2024): 16 studies confirm sensory integration intervention is evidence-based for ASD
PMC10955541
Meta-analysis (World J Clin Cases, 2024): Sensory integration therapy promotes social skills, adaptive behavior, sensory processing, motor skills
DOI: 10.1007/s12098-018-2747-4
Padmanabha et al. (Indian J Pediatr, 2019): Home-based sensory interventions RCT with significant outcomes in Indian pediatric population
PMC9978394
WHO Care for Child Development (CCD) Package implementation across 54 countries — evidence-based caregiver recommendations
DOI: 10.3389/fnint.2020.556660
Frontiers in Integrative Neuroscience: Framework for evaluating sensory processing treatment in ASD
DOI: 10.1080/17549507.2022.2141327
Adapted UNICEF/WHO Nurturing Care Framework for SLPs (2022)
WHO NCF (2018)
WHO Nurturing Care Framework — nurturing-care.org/ncf-for-ecd/
NCAEP (2020)
National Clearinghouse on Autism Evidence and Practice — Evidence-Based Practices Report
🔗 SPD Foundation — spdfoundation.net | AOTA — American Occupational Therapy Association guidelines on sensory processing intervention
GPT-OS® — The World's First Therapeutic Operating System
GPT-OS® is not an app. It is a sovereign therapeutic intelligence system that governs assessment, treatment planning, session delivery, progress tracking, and outcome measurement across 70+ centers, 20M+ therapy sessions, and 70+ countries.
Diagnostic Intelligence Layer
Identifies auditory over-responsivity within the comprehensive AbilityScore® developmental profile — mapping your child's unique sensory landscape across all domains
Sensory Regulation Index
Tracks progression from severe sensitivity → protection-dependent → graduated tolerance → flexible coping → independent management with precision metrics
FusionModule™
Coordinates OT sensory work with anxiety management and environmental adaptation across all therapy disciplines simultaneously
EverydayTherapyProgramme™
Daily home protocols including auditory protection strategies, desensitization activities, and environmental modifications — therapy continues between sessions
Readiness Tracking
Measures readiness for life, not just therapy completion — quantified across Environmental Adaptability Index and Anxiety & Stress Regulation Index
This page is one of 70,000+ technique pages in the GPT-OS® knowledge system — the largest structured pediatric intervention knowledge base on Earth.

📺 Watch: 9 Materials That Help When Child Covers Ears
Reel ID: A-032
Series: Sensory Solutions — Ep. 32
Duration: 60 Seconds
Domain: Auditory Processing
This 60-second visual guide walks through all 9 materials with real-world demonstrations. See children using noise-reducing headphones in challenging environments. Watch the transformation from distress to coping. Share with caregivers who learn better through video.
Research: Video modeling is classified as an evidence-based practice for autism (NCAEP, 2020). Multi-modal learning improves parent skill acquisition and retention.
Share This With Your Family
Consistency across caregivers multiplies impact. When grandmother, teacher, babysitter, and both parents all understand and support the same approach — the child's progress accelerates.
📥Download: Family Guide (1-Page PDF) — Simplified version for grandparents and extended family
📥Download: Teacher Communication Template — Formal accommodation request for school
📥Download: Teacher Communication Template — Formal accommodation request for school
"Explain to Grandparents" Version: "[Child's name] is very sensitive to sounds — this is how their brain works, not a behavior choice. Please warn them before making loud sounds. They have special headphones that help. If they cover their ears or want to go to a quiet place, that's okay — let them. Don't tell them to 'be brave' or 'get used to it.' This is neurological."

Act VI: The Close & Loop
Frequently Asked Questions
Will my child grow out of sound sensitivity?
Many children's sensitivity decreases with maturation, appropriate intervention, and coping strategy development. Some individuals retain heightened auditory sensitivity into adulthood but manage it effectively with tools and self-awareness. The goal is not elimination but management — your child learning to navigate the sound world with confidence.
Are noise-reducing headphones safe for everyday use?
Yes, for environmental noise reduction. They lower volume without blocking completely. However, balance protection with participation. The goal is headphones enabling participation, not headphones as permanent isolation. Monitor ear health periodically.
How is auditory over-responsivity different from hyperacusis?
They overlap significantly. Hyperacusis involves physical pain from sounds comfortable to typical listeners, often measurable audiologically. Auditory over-responsivity is a broader sensory processing pattern. Practical intervention is similar for both — protection plus graduated tolerance.
Can I use these strategies without a professional?
8 of the 9 materials can be implemented at home without professional guidance. Therapeutic listening programs (Material 4) require professional evaluation and monitoring. For comprehensive sensory evaluation and individualized planning, professional guidance from an OT is recommended.

More Questions, Answered
My child is also sensitive to touch/light/movement. Should I address sound first?
Start with whichever sensitivity most limits daily functioning. Often that's sound, because it's hardest to control in the environment. But a comprehensive sensory diet — designed by an OT — addresses multiple domains simultaneously. Explore related techniques: A-030 (touch), A-035 (light), A-033 (movement).
How do I get school to accommodate?
Request a formal meeting. Bring documentation of your child's sensory profile. Specific accommodations to request: ear defenders permitted at all times, advance fire drill warnings, quiet space access, preferential seating away from noise sources. These can be written into education plans.
How much should I expect to spend?
Start with ₹800–4,000 for noise-reducing headphones — the single most impactful purchase. Visual schedules, social stories, and many strategies are free. Complete toolkit ranges ₹0 to ₹30,000 depending on which materials your child needs.
Is this the same as autism?
Sound sensitivity occurs frequently in autism but is not exclusive to it. Children without autism can have auditory over-responsivity. Children with ADHD, anxiety, sensory processing disorder, and other conditions may also experience it. The materials and strategies on this page help regardless of diagnostic label.

The Sound World Doesn't Have to Be an Assault. Start Today.
You have the knowledge. You understand the science. You know the 9 materials. You have the protocol. Your child's nervous system is waiting for protection and support. Every day you act is a day their world gets a little bigger, a little safer, a little more navigable.
🟢 Start This Technique Today
GPT-OS® guided session launcher — personalized to your child's auditory profile. Begin with Material 1 and watch the transformation unfold.
🔵 Book an AbilityScore® Assessment
Comprehensive sensory evaluation at your nearest Pinnacle Blooms center. 📞 9100 181 181 — available in 16+ languages, 24/7.
⚪ Explore Next Technique: A-033
Continue the Sensory Solutions Series with Movement Seeking Behavior — for children who also need vestibular processing support.
Validated by the Pinnacle Blooms Consortium: OT • SLP • ABA • SpEd • NeuroDev • CRO • Parents
Preview of 9 materials that help when child covers ears Therapy Material
Below is a visual preview of 9 materials that help when child covers ears therapy material. The pages shown help educators, therapists, and caregivers understand the structure and content of the resource before use. Materials should be used under appropriate professional guidance.




















Share this resource
Help others discover thisLink copied!

From Fear to Mastery. One Technique at a Time.
You arrived on this page scared, confused, and watching your child suffer through a world that was too loud. Now you understand the neuroscience. You have 9 materials. You have a protocol. You have a community. You have a system.
This is what Pinnacle Blooms was built for.
Built by mothers who lived this. Engineered by clinicians who treat this every day. Powered by GPT-OS® — the therapeutic intelligence system governing 20M+ sessions with 97%+ measured improvement across 70+ centers serving children from 70+ countries.
Pinnacle Blooms Network®
Unit of Bharath Healthcare Laboratories Pvt. Ltd.
Unit of Bharath Healthcare Laboratories Pvt. Ltd.
📞 FREE National Autism Helpline: 9100 181 181 (16+ languages, 24/7)
🌐 pinnacleblooms.org | techniques.pinnacleblooms.org
📧 care@pinnacleblooms.org
🌐 pinnacleblooms.org | techniques.pinnacleblooms.org
📧 care@pinnacleblooms.org
CIN: U74999TG2016PTC113063 | DPIIT: DIPP8651 | MSME: TS20F0009606 | GSTIN: 36AAGCB9722P1Z2
Medical Disclaimer: This content is educational. It does not replace assessment by a licensed occupational therapist, audiologist, or healthcare provider. Persistent sound sensitivity may indicate sensory processing differences, hyperacusis, or other conditions requiring professional evaluation. Therapeutic listening programs require professional guidance. Individual results may vary. Statistics represent aggregate outcomes across the Pinnacle Blooms Network. Auditory processing timelines vary significantly between children.
© 2025 Pinnacle Blooms Network®, unit of Bharath Healthcare Laboratories Pvt. Ltd. All rights reserved.
