
Your Child Won't Touch Paint, Playdough, or Sand — And You Don't Know Why
It's art time at preschool. Every other child has paint-covered hands and enormous grins. Your child stands at the edge of the table, arms crossed, tears building. "Don't make me touch it." At home, the playdough sits untouched. The sandbox is a no-go zone. Birthday party craft time? Guaranteed meltdown.
You are not failing. Your child's nervous system is speaking. Their brain registers these textures the way yours might register touching a hot stove — as a genuine threat. This is neurological, not behavioral. And there is a clear, evidence-based path forward.
Sensory Solutions • Episode 6
Age: 18 months – 8 years
Domain: SEN-TAC

You Are Not Alone — The Numbers
When your child screams at finger paint, it feels like you're the only family dealing with this. You're not. A 2024 PRISMA systematic review confirmed that sensory processing difficulties are present in the vast majority of children on the autism spectrum — and tactile defensiveness is one of the most common patterns.
80%
Autism + Sensory
Of children with autism experience sensory processing difficulties, with tactile defensiveness among the most prevalent
1 in 6
Global Sensory Patterns
Children globally show sensory processing patterns that meaningfully impact daily life and participation
18M+
Families Affected
Families worldwide navigate texture aversion — the same art tables, the same sandboxes, the same birthday party craft stations
In India alone, with an estimated 2–3 million children on the autism spectrum, texture aversion affects hundreds of thousands of families. You are among millions. And the evidence points to a clear way forward.
Sources: PRISMA Systematic Review 2024 (PMC11506176) | Meta-Analysis: World J Clin Cases 2024 (PMC10955541) | WHO Global Prevalence Data

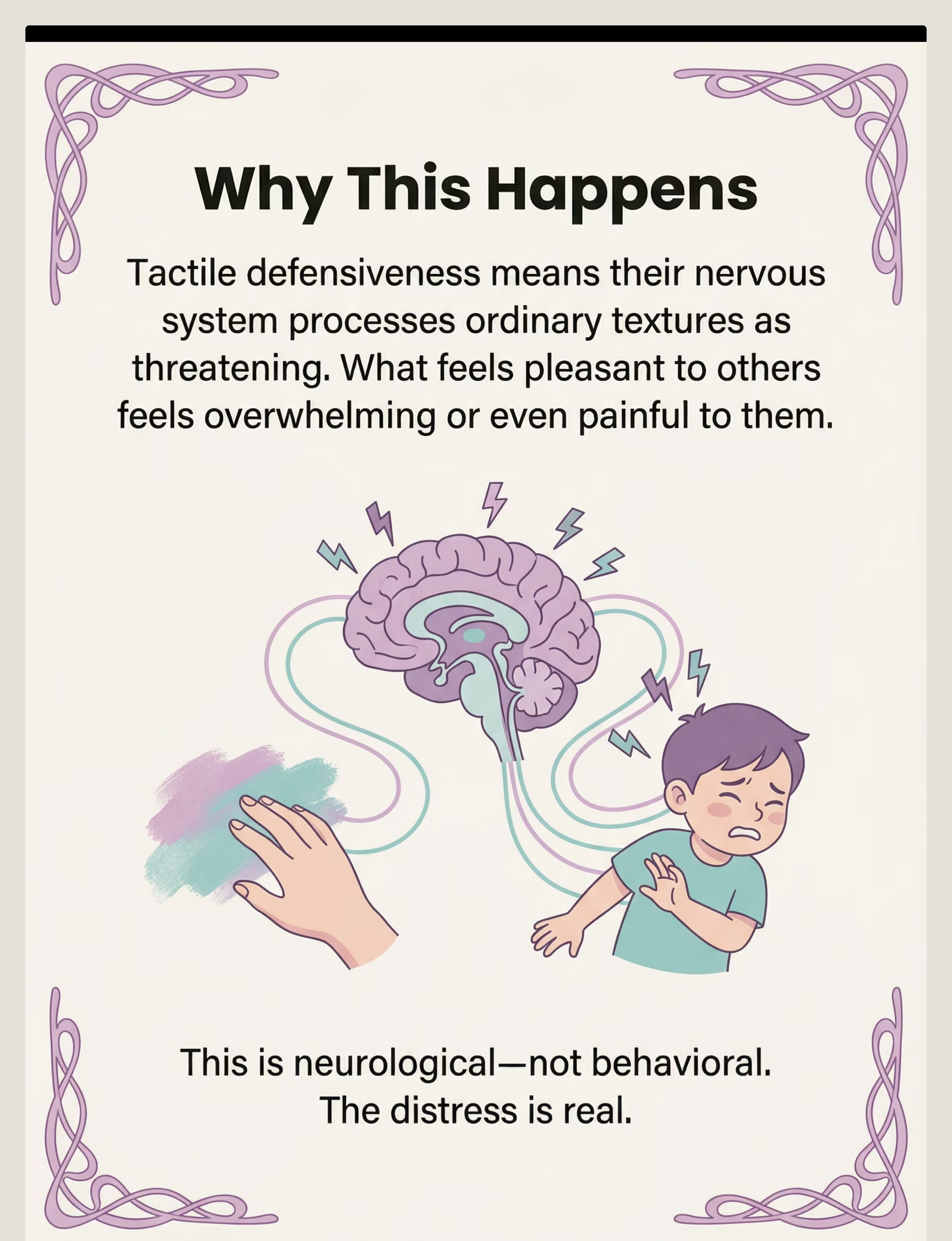
What's Happening in Your Child's Brain
The Clinical Term
Tactile Over-Responsivity (formerly called Tactile Defensiveness)
What It Means
Their somatosensory cortex — the brain region that processes touch — has a lower threshold for registering input. Textures that feel neutral or pleasant to most people are processed as intense, uncomfortable, or genuinely threatening.
When paint touches their fingers, their nervous system fires a protective alarm. The sticky sensation creates a "trapped" feeling — the mess won't come off, and their brain interprets this as danger.
This Is a Wiring Difference, Not a Behavior Choice
The distress you see — the pulling away, the crying, the rigid hands held up and away from the table — is their nervous system's genuine protective response. As real as your reaction to touching something scalding.
What It Looks Like
Paint on fingers triggers the same brain alarm system as a physical threat. The child isn't being dramatic. They aren't looking for attention. They are responding to a genuine neurological signal that says: danger, remove this now.
Source: SPD Foundation | Frontiers in Integrative Neuroscience 2020 (DOI: 10.3389/fnint.2020.556660)

Where This Sits in Development
Tactile defensiveness typically becomes visible between 12–24 months, when children are expected to explore textures through play. It peaks during the preschool years (2–4), when art activities, sensory bins, and sandbox play become central to the curriculum.
0–12 Months
Emerging sensory preferences, mouthing, early texture exploration begins
12–24 Months ⚡
Typical emergence window for tactile defensiveness — avoids new textures, resists messy play
2–4 Years ⚡
Peak challenge zone — preschool demands messy play and art. Social impact begins here
4–6 Years
Without intervention, avoidance patterns solidify. With intervention, gradual tolerance builds steadily
6–8 Years
School activities demand texture tolerance. Intervention enables meaningful participation with peers
Common co-occurrences: Auditory sensitivity, vestibular differences, food texture aversions, and clothing sensitivities often appear alongside tactile defensiveness. The trajectory with intervention shows measurable progress within 8–12 weeks. The goal is participation at the child's tolerance level — not forced enjoyment.
Sources: WHO Care for Child Development (CCD) Package (PMC9978394) | UNICEF Developmental Monitoring Indicators

The Evidence Behind This Technique
Evidence Level I–II
Systematic Reviews + RCTs
Systematic Review (2024)
16 articles from 2013–2023 confirm sensory integration intervention meets criteria to be considered evidence-based practice for children with ASD. Clinically validated for tactile desensitization protocols.
PubMed: PMC11506176
Meta-Analysis (2024)
Across 24 studies, sensory integration therapy effectively promoted social skills, adaptive behavior, sensory processing, and gross/fine motor skills.
PubMed: PMC10955541 | DOI: 10.12998/wjcc.v12.i7.1260
Indian RCT (2019)
Home-based sensory interventions demonstrated significant outcomes when administered by trained parents, validating the home-execution model used in this guide.
DOI: 10.1007/s12098-018-2747-4 — Padmanabha et al., Indian Journal of Pediatrics
NCAEP Classification (2020)
Sensory integration is classified as an evidence-based practice for autism by the National Clearinghouse on Autism Evidence and Practice. Recognized across OT, ABA, and special education disciplines.
Clinically validated. Home-applicable. Parent-proven.

The Technique: Gradual Texture Desensitization Through Material Hierarchy
Parent-Friendly Name: "The Gentle Texture Path"
A systematic, child-led approach to reducing tactile defensiveness during messy play by introducing 9 carefully sequenced therapeutic materials — from dry and non-threatening to wet and sticky. Each material is selected because it addresses a specific barrier: stickiness, unpredictability, loss of control, or residue on hands.
The child progresses at their own pace through a texture tolerance ladder, with every step celebrated as success. This is not forcing your child to touch things. This is giving them the right materials, in the right order, with the right supports, so their nervous system can safely expand its tolerance window.
Domain
Sensory Processing — Tactile (SEN-TAC)
Age Range
18 months – 8 years
Session Duration
10–20 minutes per session
Frequency
3–5 sessions per week

Who Uses This Technique
This technique crosses therapy boundaries — because the brain doesn't organize by therapy type. Four disciplines integrate gradual texture desensitization into their practice, each contributing a distinct and essential role.
Occupational Therapist (OT)
Primary Lead. Designs the sensory diet, selects materials based on the child's sensory profile, creates the texture tolerance ladder, and monitors desensitization progress. OTs understand the neurological basis of tactile defensiveness and calibrate the "just-right challenge."
Speech-Language Pathologist (SLP)
Uses modified versions for oral-motor desensitization — when texture aversion extends to food textures, the SLP bridges from hand-based texture tolerance to oral exploration. The same graduated approach applies seamlessly.
Board Certified Behavior Analyst (BCBA)
Designs the reinforcement schedule, creates the graduated exposure chart, manages antecedent strategies (environment setup, readiness checks), and troubleshoots avoidance behavior. ABA ensures the child is motivated to engage, not forced.
Special Educator (SpEd)
Adapts classroom art, craft, and sensory activities to the child's current tolerance level. Ensures the IEP includes sensory accommodations. Bridges therapy goals into school participation and peer activities.
Source: Adapted UNICEF/WHO Nurturing Care Framework for SLPs (2022) — DOI: 10.1080/17549507.2022.2141327

What This Technique Targets
Gradual texture desensitization is not a single-outcome intervention. It creates ripples across multiple developmental domains — from immediate tactile tolerance to long-term school readiness and social confidence.
Observable Progress Indicators
- Child approaches messy materials voluntarily — even if using tools
- Duration of texture contact increases week over week
- Distress signals (crying, pulling away, rigid hands) decrease measurably
- Child accepts cleanup as part of the process — not as a rescue
- Child attempts new textures without prompting from adults
Source: Meta-analysis (World J Clin Cases, 2024) — PMC10955541

What You Need — The 9 Materials
These 9 materials are sequenced from least to most threatening for the tactile-defensive child — dry to wet, firm to soft, tools to hands, controlled to open-ended. You do not need all 9 to start. Begin with Material 1.

1. Dry Sensory Bins
Rice, beans, pasta in shallow bins. Entry-level, predictable, non-sticky.
Pinnacle Recommends

2. Theraputty / Therapy Dough
Firm resistance, clean release. Builds proprioceptive tolerance.
Pinnacle Recommends

3. Mess-Free Paint Options
Paint in sealed bags — art without touching. Maximum control, minimum threat.
DIY Friendly

4. Tools for Messy Play
Brushes, scoops, tongs — a barrier between hands and texture. The essential bridge.
DIY Friendly

5. Kinetic Sand
Sticks to itself, not to hands. The "clean messy" material that surprises children.
Pinnacle Recommends

6. Gloves for Messy Play
Full participation with protection. Gloves are bridges, not crutches.
Essential

7. Washable Paints + Instant Wipes
Control reduces fear. Knowing cleanup is instant changes everything for these children.
Control Strategy

8. Cloud Dough
Flour + oil — silky, moldable, less sticky than playdough. A gentle wet-texture introduction.
DIY Friendly

9. Graduated Exposure Chart
Visual progress tracker — every step is a win. The child's roadmap and celebration board.
Essential System
Essential Starters: Dry Sensory Bins + Tools + Washable Paint with Wipes. Total investment: ₹550–1,400 for the core kit.

DIY & Zero-Cost Alternatives
Every family deserves access to this technique, regardless of budget. The therapeutic principle — not the brand — creates the sensory effect. Dry before wet. Firm before soft. Tools before hands. Controlled before uncontrolled.
Buy This | Make This at Home | Approx. Cost | |
Commercial Dry Sensory Bin Kit | Dried rice colored with food coloring, dried pasta, dried lentils, birdseed — from kitchen | ₹50 | |
Clinical-grade Theraputty | Mix 2 parts cornstarch + 1 part hair conditioner — non-sticky, firm dough that washes off easily | ₹30 | |
Crayola Color Wonder Kit | Paint in sealed zip-lock bag, taped to table — child squishes colors through the bag | ₹20 | |
Messy Play Tool Set | Kitchen items: wooden spoons, plastic tongs, silicone spatulas, measuring cups, foam brushes | ₹0 | |
Commercial Kinetic Sand | Mix 4 cups fine sand + 2 cups cornstarch + 1 cup vegetable oil (similar, not identical) | ₹80 | |
Child Gloves Pack | Disposable food-handling gloves from any medical store | ₹50 | |
Washable Finger Paints | Any washable paint + wet washcloths + baby wipes placed within arm's reach | ₹100 | |
Cloud Dough Kit | 8 cups flour + 1 cup vegetable oil (add food coloring for interest) | ₹40 | |
Laminated Exposure Chart | Poster board + drawn steps + stickers from local shop | ₹50 |
Zero-Cost Version: Use only kitchen items — rice, pasta, flour, oil, plastic bags. The therapeutic principle remains identical.
⚠️ When clinical-grade matters: Theraputty resistance levels and kinetic sand's clean-release property are difficult to replicate exactly at home. Consider purchasing these if budget allows. Source: WHO Nurturing Care Framework (2018) — PMC9978394

⚠️ Safety First — Before You Begin
Read this card before your first session. These guidelines protect your child's nervous system and ensure the intervention builds trust rather than trauma. Safety is not optional — it is the foundation the entire technique rests on.
🔴 DO NOT PROCEED IF:
- Child is in active distress or post-meltdown — wait until regulated
- Known allergies to materials (latex, wheat for cloud dough, food allergies for edible bins)
- Child is actively mouthing objects AND materials include choking hazards
- Skin condition is active on hands (open wounds, eczema flare)
- Child is ill, exhausted, or hungry
🟡 MODIFY AND PROCEED WITH CAUTION:
- Child is resistant but not distressed — use observation-only mode (Level 1)
- Child under 2 years — use only large, non-chokable materials
- Child has oral sensitivities — avoid food-based materials initially
- First time attempting this technique — start with dry sensory bin only
🟢 PROCEED:
- Child is calm, fed, rested, and in a regulated state
- Materials are age-appropriate and allergy-safe
- Cleanup supplies are within arm's reach
- Environment is calm, low-stimulation, no audience pressure
- Parent has read the protocol and has realistic expectations
🛑 Red Line Behaviors — Stop Immediately If: Child shows extreme distress that doesn't de-escalate within 60 seconds | Self-injurious behavior (scratching, biting hands) | Vomiting or gagging reaction | Child cannot be redirected or soothed. Source: Padmanabha et al., Indian J Pediatr, 2019 (DOI: 10.1007/s12098-018-2747-4)
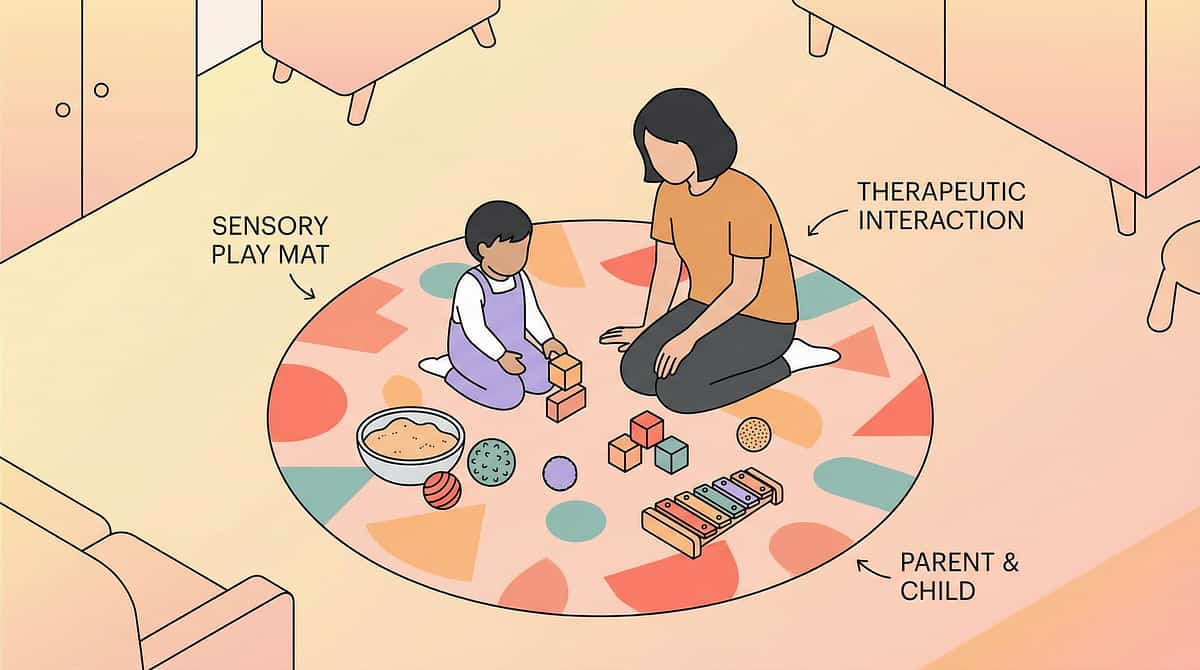
Set Up Your Space
Your environment is an active ingredient in this technique. A poorly set-up space increases sensory load before the session even begins. A well-set-up space communicates safety, predictability, and control — the three things a tactile-defensive child's nervous system needs most.
1
Messy Play Area
Low table or floor mat. Materials in the center. Child can see everything at once — no surprises.
2
Cleanup Station — Within Arm's Reach
Wet cloths, wipes, water basin placed directly beside the play area. This is the single most critical setup element for tactile-defensive children. Not on another table. Not across the room. Right there.
3
Child Position
Seated, materials at elbow height, able to leave freely. Never trapped. Always in control of proximity.
4
Parent Position
Beside the child at the same level — not hovering overhead. Beside communicates partnership; hovering communicates surveillance.
5
Tools and Gloves Visible
Accessible and child-selectable at all times. The child can choose freely — this is the foundation of child-led desensitization.
Lighting
Soft, natural — harsh fluorescent adds sensory load
Sound
Quiet — no background TV or loud music
Temperature
Comfortable — cold hands increase tactile sensitivity
Clothing
Smock or old clothes — removes adult anxiety about mess

Is Your Child Ready? — 60-Second Check
The best session is one that starts right. Take 60 seconds before every session to run through this checklist. Readiness is not a nicety — it's a clinical variable that determines whether today's session builds tolerance or sets it back.
✅ The Go Checklist
- Child is calm and regulated — no recent meltdown
- Child has eaten recently — not hungry
- Child is rested — not overtired
- No illness or physical discomfort
- No recent distressing event (argument, unexpected change)
- Cleanup supplies are visible and within child's reach
- Child knows they can stop at any time — verbalize this
All ✅ → GO
Begin with Step 1 — The Invitation. Full protocol ahead.
Most ✅, child slightly off → MODIFY
Start at observation only (Level 1). Place materials where child can see them. Reduce expectations. This is still progress.
Multiple ❌ → POSTPONE
Do a preferred calming activity instead. Try again when conditions are met. Postponing is not failure — it is data.
"The best session is one that starts right."

Step 1 — The Invitation (30–60 seconds)
Protocol Step 1 of 6
"Look what I found! I'm going to play with this rice. You can watch, or you can try. There are scoops if you want to use a tool. And see? Wipes are right here if anything gets on your hands."
Body Language Guidance
- Sit at the child's level, beside them — not across
- Begin playing with the material yourself — model enjoyment
- Do NOT place material on the child or in their space
- Keep your body relaxed, voice calm and inviting
- Let the child approach at their own pace
Acceptance Cues 🟢
- Child looks at material with curiosity
- Child moves closer to the tray
- Child reaches for a tool
- Child says "What is that?" or "Can I see?"
Resistance Cues — Modify 🟡
- Child turns away → "That's okay. It will be here if you want to look later."
- Child says "No" → "No problem. You can just watch me play."
- Child shows distress → Stop. Move to calming activity. Try another day.
Timing: 30–60 seconds for the invitation. Do not extend if child doesn't engage — today might be an observation day, and that's Level 1 success.

Step 2 — The Engagement (1–3 minutes)
Protocol Step 2 of 6
If the child accepted the invitation, it's time to gently deepen engagement. Present the material slowly, at the child's arm's length, tool-first — always offer a tool before expecting hand contact. Introduce one texture at a time — never multiple new textures in a single session.
"This rice is so smooth! Listen to the sound it makes when I pour it. Want to try pouring with this cup?"
Engaged 😊
Reaching for material, using tools, asking for more, smiling. Continue and reinforce enthusiastically.
Tolerating 😐
Watching, staying near, touching briefly, accepting tool play. Continue at current level. Don't push further today.
Avoiding 😟
Turning away, showing discomfort but not distress. Honor the boundary. This is data, not failure.
Reinforcement Cue: When the child makes ANY move toward the material — looking, approaching, touching with a tool, touching briefly with a finger — immediately reinforce within 3 seconds. "You touched it! That was brave!" "You're using the scoop — great idea!" "You looked right at it — that's your first step!"

Step 3 — The Therapeutic Action (3–7 minutes)
Protocol Step 3 of 6
This is the active ingredient — the moment the nervous system receives input it can process without triggering a full protective response. The child interacts with the selected material at whatever level they can tolerate. There is no single "correct" level. The correct level is the one that creates engagement without distress.
For Dry Sensory Bin (Entry-Level)
- Child pours rice with a cup — maximum tool distance
- Child stirs rice with a spoon — shorter tool
- Child touches rice with one fingertip — brief direct contact
- Child places palm on rice surface — sustained contact
- Child scoops rice with hands — active engagement
For Theraputty (Firm-Texture Level)
- Child watches parent squeeze and stretch
- Child pokes putty with one finger
- Child squeezes with both hands — proprioceptive input
- Child pulls, rolls, flattens — active manipulation
Common Execution Errors
- ❌ Placing material ON the child's hands → Always let the child initiate contact
- ❌ Saying "See? It's not so bad!" → Invalidates their genuine experience
- ❌ Comparing to peers → "Your friend likes it" adds shame, not motivation
- ❌ Removing the tool too soon → Tools are bridges, not crutches to eliminate
Child Response Spectrum
- ✅Ideal: Voluntary contact, exploring, relaxed body language
- ✅Acceptable: Tool-only play, brief fingertip touches, watching with interest
- ⚠️Concerning: Escalating distress, rigid body, crying → Move to cool-down
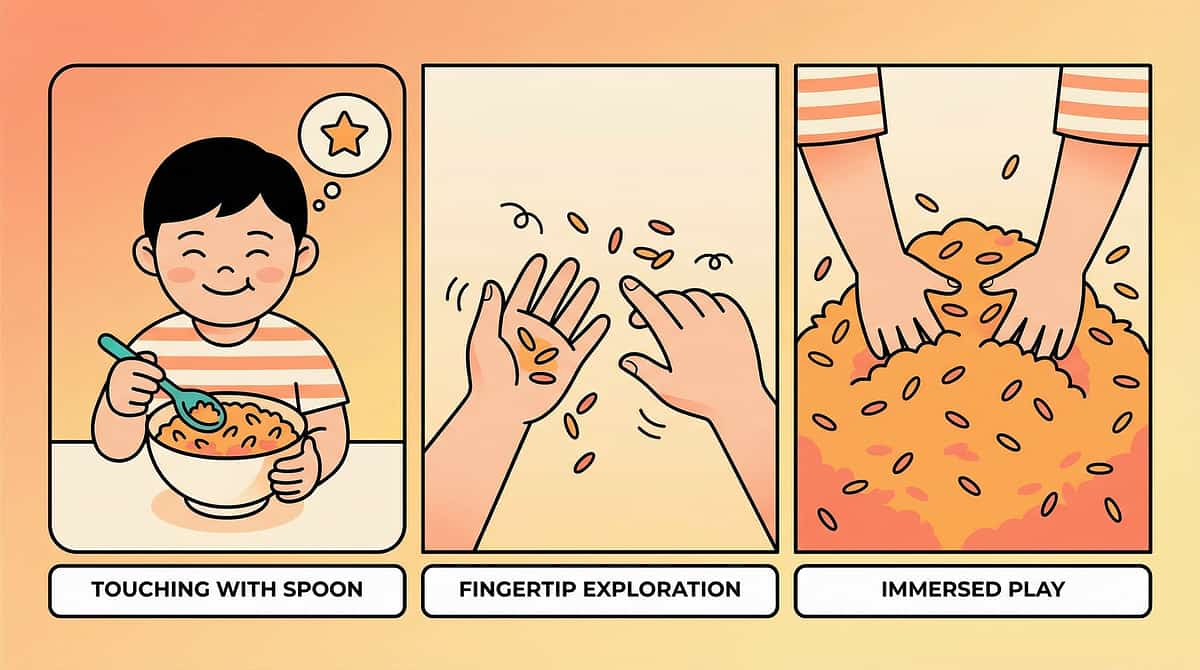
Step 4 — Repeat & Vary (3–5 minutes)
Protocol Step 4 of 6
Repetition builds neural pathways. Variation maintains engagement. The goal is 3–5 meaningful interactions — not forced repetitions. Quality of engagement matters far more than quantity of attempts.
"3 good reps > 10 forced reps" — Quality of engagement matters more than quantity.
Same Material, New Action
- Pour rice → Hide small toy in rice → Find the toy
- Squeeze putty → Flatten putty → Roll putty into snake
- Push paint in bag → Trace letters on bag → Mix new color
Same Action, Slight Variation
- Touch with right hand → Touch with left hand
- Use spoon → Use shorter spoon → Use fingers with spoon nearby
- One finger touch → Two finger touch → Brief palm touch
Satiation Indicators — When to Move On
Watch carefully for these signals. When you see them, move to Step 5. Do not push beyond satiation — it erases the progress built in this session.
Looking away from the material or becoming distracted
Slowing engagement, saying "all done" or "I'm done"
Reaching for the cleanup supplies independently
Body tension returning after a previously relaxed period

Step 5 — Reinforce & Celebrate
Protocol Step 5 of 6
The Rule: Reinforce within 3 seconds. Be specific. Be enthusiastic. Vague praise ("Good job!") is less effective than specific, immediate reinforcement that names exactly what the child did. Your child's nervous system needs to learn that texture contact is safe — and specific praise accelerates that learning.
"You touched the rice with your whole hand! That was so brave!"
"You used the brush to paint — you made art today!"
"You looked right at the kinetic sand — that's your first step and I'm proud of you!"
"You put on the gloves all by yourself and finger-painted! Look at what you created!"
Celebrate the Attempt, Not Just the Success
✅ Looking at the material → "You looked at it! Great start!"
✅ Standing near → "You're right next to it! That's progress!"
✅ Tool use → "You're painting with the brush — amazing!"
✅ Brief touch → "You touched it! Your hands did great!"
✅ Extended play → "You played for 3 whole minutes! That's incredible!"
A child who looked at the playdough today and said "not yet" has made real progress. They stayed. They considered. That's a neurological win. Reinforcement options: high-fives, verbal praise, stickers on exposure chart, preferred activity after session, or displaying the artwork proudly.

Step 6 — The Cool-Down (1–2 minutes)
Protocol Step 6 of 6
How a session ends matters as much as how it begins. An abrupt ending creates negative associations. A warm, predictable transition teaches the child that messy play has a safe, controlled conclusion — and that they will feel clean and comfortable again within moments.
Verbal Warning
"Two more pours, then all done." → "One more squeeze, then we clean up." → "Last one coming up!"
Cleanup Ritual
Child wipes hands — or parent helps gently. Make cleanup calm and unhurried. This is part of the therapy, not a rescue from it.
Deep Pressure Input
Firm hand squeeze, arm compression, or hug. This organizing, calming proprioceptive input helps the nervous system settle after stimulation.
Transition Cue
"Rice is all done. Now let's go [preferred next activity]." A clear, positive bridge to what comes next.
If Child Resists Ending
"I know you're having fun! The rice will be here tomorrow." Set a visual timer for 1 more minute, then follow through calmly. Never abruptly remove materials — this creates negative associations with the activity.
If Child Is Relieved It's Over
"You did it! You stayed for the whole time. That's amazing." Do not guilt them for wanting to stop. "The wipes are right here — let's get your hands clean." Their relief is valid information about their current tolerance level.

Capture the Data — Right Now (60 Seconds)
Record these data points within 60 seconds of session end, while your memory is fresh. Tracking transforms guesswork into a clear picture of your child's progress. Over weeks, these simple data points reveal patterns that neither you nor your therapist could see otherwise.
1. Texture Level Reached
Which material? What level of contact?
Observation / Tool / Brief Touch / Sustained / Active Play
2. Duration of Contact
How many seconds or minutes of actual contact with the texture? Even 10 seconds counts — record it.
3. Distress Level (1–5)
1 = Calm, engaged
2 = Mild discomfort, continued
3 = Moderate, needed support
4 = High distress, shortened session
5 = Full meltdown, session ended
2 = Mild discomfort, continued
3 = Moderate, needed support
4 = High distress, shortened session
5 = Full meltdown, session ended
Tracking Format — Date: ___ | Material: ___ | Level: Obs / Tool / Fingertip / Palm / Active Play | Duration: ___ seconds/minutes | Distress: 1 / 2 / 3 / 4 / 5 | Notes: ___
"60 seconds of data now saves hours of guessing later."

What If It Didn't Go as Planned?
Most sessions don't go perfectly. When a session goes sideways, the technique needs adjustment — not the parent. Every difficult session contains information about your child's current threshold. Here is how to read that information and respond.
"My child wouldn't even look at the material."
That's okay. Place the material where they can see it from a distance. Play with it yourself. Let curiosity build naturally — proximity without pressure. Try again in 2–3 days. This IS Level 1 progress.
"They used tools but screamed when rice accidentally touched their hand."
Accidental contact with an immediate exit strategy (wipes available) is actually therapeutic progress. Acknowledge it: "Oops, rice touched you! Here's a wipe." Don't make it a big deal. Next time, they'll know the wipe is there.
"They played for 30 seconds and then wanted to stop."
30 seconds of engagement is success. Measure against yesterday's zero seconds — not against an arbitrary target duration. Build by 10–15 seconds per week. Compounding is invisible until suddenly it isn't.
"They had a full meltdown."
Move immediately to calming strategy. Do not continue. Note what triggered the escalation. Restart next session one level BELOW today's starting point. This is not failure — this is precise data about their current threshold.
"They will only play with the dry rice — they won't try anything else."
Perfect. Stay with dry rice for 2–3 weeks. Build deep comfort before introducing the next texture. The texture hierarchy exists for a reason — dry rice IS the therapeutic foundation.
"My spouse/grandparent forced them to touch it and now they're more avoidant."
Share Card 37 (family guide) with all caregivers immediately. Forced exposure sets back progress. Rebuild trust by returning to the level BEFORE the forced exposure. Consistency across all caregivers is non-negotiable.
"Session abandonment is not failure — it's data."
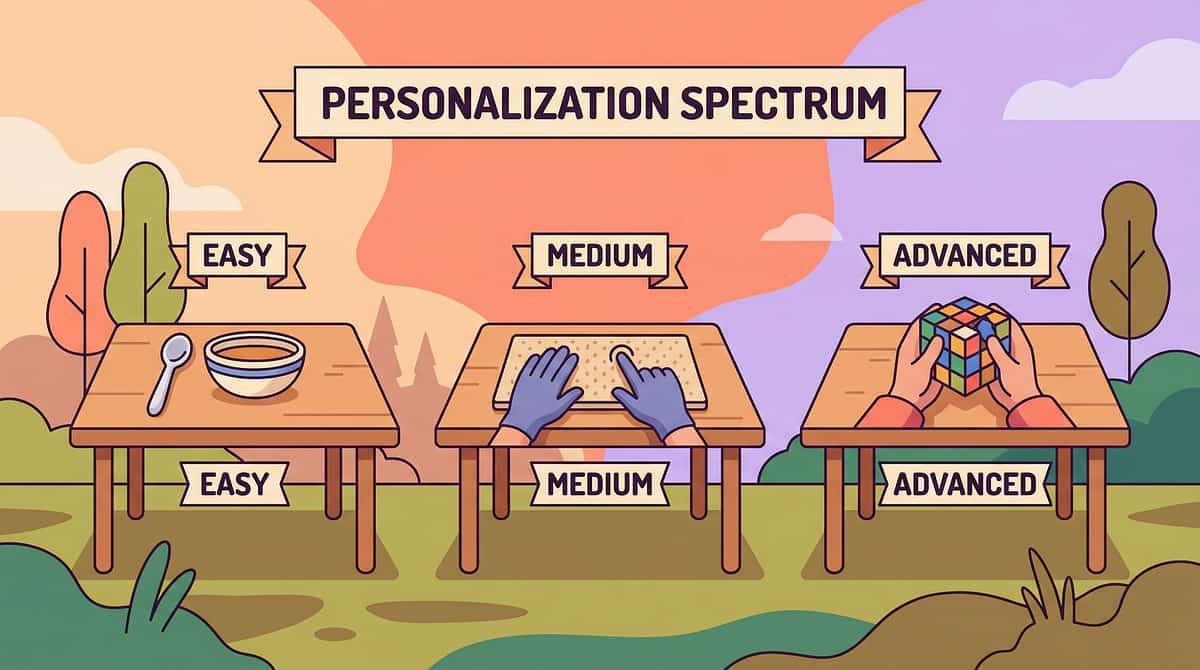
Adapt & Personalize
No two children are identical. The protocol is a framework, not a rigid script. Adjust the approach based on your child's sensory profile, age, and the specific texture barriers they face. The hierarchy remains the same — only the pace and entry point change.
Easier (Bad Days)
Observation only. Material visible but no expectation. Parent plays alone. Zero pressure on the child. Presence near the materials IS the session.
Standard Protocol
Tool exploration → brief fingertip contact → guided play at child's pace. The full six-step sequence as described in Cards 14–19.
Harder (Breakthrough Days)
Direct hand contact → multiple textures → wet textures → peer play alongside another child. Reserve for consistently high-tolerance sessions.
18 Months – 3 Years
Use only large, non-chokable materials. Keep sessions under 5 minutes. Expect mostly tool play. Mouthing supervision is essential throughout every session.
3–5 Years
Prime age for exposure charts — social motivation is emerging. Child can verbalize preferences. 10–15 minute sessions. Can participate in creating their own exposure chart.
5–8 Years
Understands the "brave" framing. Peer participation becomes a powerful motivator. 15–20 minute sessions. Can track their own progress independently.
Sensory Seeker Modification: If your child also seeks proprioceptive input (craves squeezing, pressing), theraputty and kinetic sand may be well-received. Focus on firm pressure textures first before introducing lighter touch materials.

Week 1–2: What to Expect
Progress Arc
Phase 1 of 3
This first phase is the hardest — not because nothing is happening, but because what is happening is invisible. Neural pathways are forming beneath the surface. Your child sat within arm's reach of the dry sensory bin today. Yesterday, they wouldn't enter the room. That is real neurological progress.
What You Will See
- Child tolerates the material being in the room (reduced avoidance response)
- Child may begin watching parent play with materials at observation level
- Duration near the material increases from seconds to minutes
- Child may touch a tool that touched the material
- Distress signals may decrease from Level 4–5 to Level 2–3
What Is Not Progress Yet
- Child does NOT yet happily finger paint like peers
- Child does NOT voluntarily plunge hands into materials
- Child may still say "no" to direct contact consistently
"If your child tolerates the material for 3 seconds longer than last week — that's real progress."
Parent Emotional Preparation: This is the hardest phase. You will feel like nothing is happening. Trust the neuroscience. Synaptic connections are forming. Consistency now is the investment that pays in weeks 3–8.

Week 3–4: Consolidation Signs
Progress Arc
Phase 2 of 3
Something shifts around week three. You may notice it first in small moments — your child asks if you're doing "the rice thing" today. They walk toward the sensory bin rather than away from it. These moments are not coincidences. They are consolidation: your child's nervous system is beginning to predict safety rather than threat.
Anticipating the Activity
Child asks "Are we doing the rice today?" or brings the material container to you. Anticipation without dread is a major neurological milestone.
Showing Material Preference
Child shows preference for certain materials over others. This self-awareness and preference-expression is a sign of engaged, active processing — not passive endurance.
Confident Tool Play
Tool play becomes sustained and confident. Child experiments with different tools, invents new ways to use them, directs the activity. They are leading now.
Spontaneous Direct Touch
Child may attempt brief direct touch without prompting — often when they think you're not watching. Don't over-react. A quiet "I saw that, well done" is enough.
When to Increase Difficulty
If child consistently scores Distress Level 1–2 with current material across 3+ sessions, introduce the next material on the hierarchy. Comfortable with dry rice → try theraputty or kinetic sand. Comfortable with theraputty → try mess-free paint bags.
Parent Milestone
"You may notice you're more confident too. You've stopped holding your breath when they approach the materials. You've started to trust your own facilitation. That parent confidence is therapeutic in itself — children read our bodies, not just our words."
Week 5–8: Mastery Indicators
Progress Arc
Phase 3 of 3
By weeks 5–8, the protocol shifts from building initial tolerance to consolidating generalized participation. Mastery does not mean your child loves every texture. It means they can participate — with or without accommodations — without significant distress. That is the clinical definition of success.
Voluntary Choice
Child voluntarily chooses a messy play activity from available options without prompting or negotiation
Direct Hand Contact
Direct hand contact with at least 2–3 texture types achieved across multiple sessions
Sustained Play
5+ minutes of continuous engagement without distress signals or requests to stop early
Independent Cleanup
Child uses cleanup supplies independently — knows where wipes are, uses them calmly as a natural part of the session
Generalization Emerging
Tolerance extends to other settings — school, a friend's home, a birthday party craft station. The skill has left the home protocol
🏆 Mastery Unlocked when: Child participates in a group messy play activity — at school or socially — with or without accommodations — without significant distress. Not all children will reach this level with all textures, and that is okay. Participation with accommodations IS success.

🎉 Celebrate This Win
"You did this. Your child grew because of your commitment."
Remember Where You Started
Card 01 — a child standing at the edge of the art table, arms crossed, tears building, unable to touch what every other child was enjoying freely.
Where You Are Now
A child who approaches materials with curiosity. Who uses tools confidently. Who may touch textures briefly, or with gloves, or even with bare hands. Who participates — in their own way, at their own level.
That Bridge? You Built It.
Every session where nothing seemed to happen was building neural pathways. Every time you placed the wipes within arm's reach, you were saying: "I trust you to decide." Every fingertip touch you celebrated like a masterpiece was teaching your child that progress at any level matters.
Family Celebration Suggestions
- Display the child's artwork — even the mess-free bag painting counts as real art
- Take a photo of their hands in kinetic sand and frame it
- Put a star — or ten — on their exposure chart
- Tell them: "Remember when you couldn't look at the rice? Today you played in it."
- Share the milestone with their therapist — this data matters clinically
📸 Document this milestone. Take photos. Write a note. Your future self will need this evidence on the hard days when progress feels invisible again. The arc is long, and today is proof that it bends toward participation.

🚩 Red Flags — When to Pause and Seek Professional Guidance
Home-based gradual desensitization is effective for the vast majority of children with mild to moderate tactile defensiveness. However, some presentations require professional assessment and clinical-grade sensory integration therapy. Trust your instincts — if something feels wrong, pause and ask.
🚩 Food Intake Severely Limited
Texture aversion is so severe it significantly limits food intake — child eats fewer than 10 foods, all of one texture. This crosses into a feeding disorder requiring specialist intervention alongside tactile desensitization.
🚩 Clothing Tolerance Near Zero
Child cannot tolerate ANY clothing textures, with severely limited dressing options that are affecting daily functioning and school participation. This level of severity warrants a comprehensive sensory profile assessment.
🚩 No Improvement After 8 Weeks
Extreme distress that does not improve with gradual exposure over 8+ weeks of consistent practice (3–5 sessions per week). Plateau without any indicators from the progress arc in Cards 23–25.
🚩 Social Isolation Significant
Texture avoidance is significantly impacting peer relationships — child is unable to participate in any group activities involving potential texture contact.
🚩 Self-Injury Related to Texture
Scratching skin to bleeding, biting hands to remove texture sensation. Any self-injurious behavior triggered by texture contact requires immediate professional consultation.
🚩 Regression in Previously Tolerated Textures
Child was managing certain textures and is now avoiding them again. Regression without a clear environmental trigger warrants professional review of the sensory profile.
Continue at Home
Mild to moderate presentation with steady progress. Use modifications from Cards 21–22.
Book a Teleconsultation
Personalized guidance from a Pinnacle OT. Call 📞 9100 181 181 or visit pinnacleblooms.org/teleconsult
Visit a Clinic
Comprehensive sensory profile assessment at your nearest Pinnacle Blooms center. pinnacleblooms.org/centers

The Progression Pathway
This technique does not exist in isolation. It sits within a structured domain of tactile sensory interventions, each building on the foundation of the last. Knowing where you are on this map helps you and your therapist navigate the full journey from tactile defensiveness to participation.
Lateral Alternatives
If this approach didn't fully resonate with your child's profile, these related techniques address adjacent components:
- A-004: Light Touch Aversion — focuses on unexpected or light touch rather than messy texture
- A-005: Unexpected Touch Reactions — addresses the startle and surprise component of touch
- R-201: Sensory Diet Basics — broader sensory regulation approach across all sensory systems
Long-Term Developmental Goal
Full participation in age-appropriate activities involving varied textures — in classroom, social, and daily living settings — with or without accommodations. The measure of success is not whether a child loves finger paint. It is whether they can be present, engaged, and at ease in a world that includes it.

Related Techniques in the Tactile Sensory Domain
The 9 materials you have assembled for this technique work across the entire tactile domain. Your investment in this protocol seeds the next six techniques automatically. You already own the materials — the approach simply shifts.
A-003: General Touch Sensitivity
The foundational prerequisite technique. Addresses broad tactile over-responsivity before specific texture work begins. Intro Level — materials you already own.
Intro Level
A-004: Light Touch Aversion
Addresses the specific distress response to light, unexpected, or incidental touch — a hairbrush, a tag on a shirt, a peer brushing past in the hallway.
Core Level
A-007: Clothing Texture Sensitivities
Applies the same graduated desensitization hierarchy to fabric textures — seams, tags, sock tightness, waistbands. High daily-life impact for most families.
Core Level
A-008: Grooming Sensitivities
Hairbrushing, nail cutting, face washing, teeth brushing. The same nervous system response in a different context — daily living routines that can become daily battles.
Core Level
A-009: Temperature Sensitivities
Addresses over-responsivity to temperature variations in food, water, and environmental contact. Often co-occurs with tactile defensiveness in the same children.
Core Level
A-010: Food Texture Aversions
The oral-motor companion to messy play desensitization. When the same child who avoids sand also refuses mixed textures, mushy foods, or foods that change texture while chewing.
Advanced Level
🔗 Browse Full Domain: techniques.pinnacleblooms.org/sensory/tactile — "You already own materials for all of these."
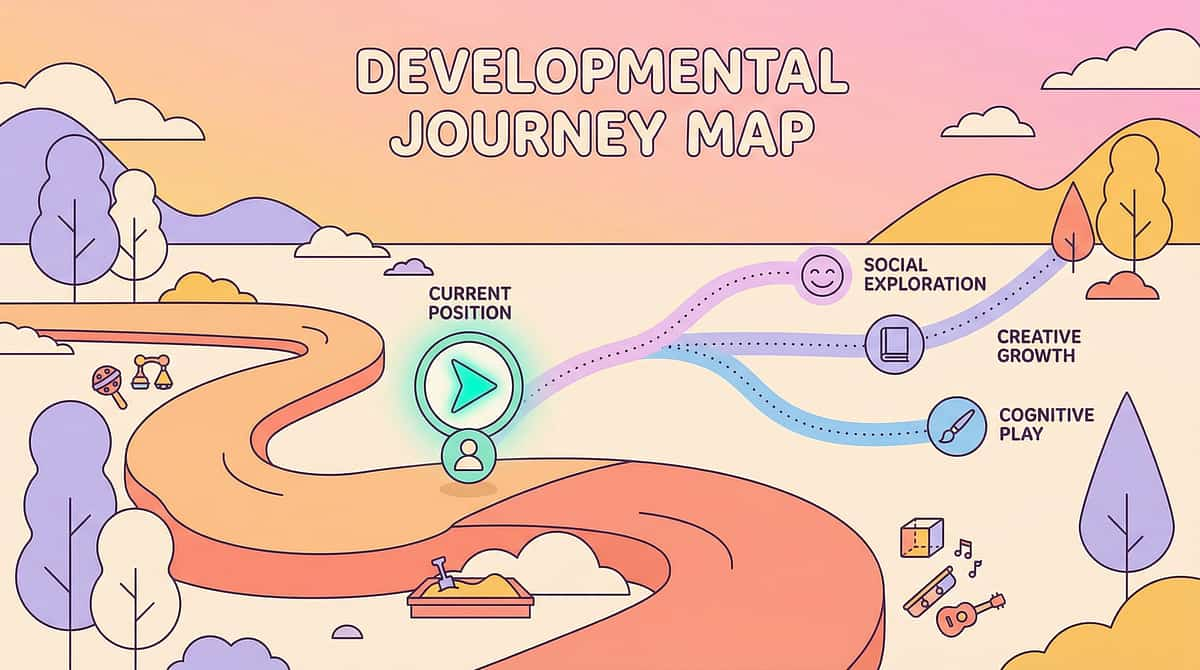
Your Child's Full Developmental Map
Messy play tolerance is one thread in a much larger developmental fabric. The skills built here — sensory regulation, self-efficacy, participation with peers — feed into every other developmental domain your child is working on simultaneously.
How Messy Play Tolerance Connects
- Domain B — Motor Skills: Fine motor development through manipulation of textures
- Domain D — Social Skills: Peer participation in art, craft, and group sensory play
- Domain F — Cognitive: School readiness through art, science, and sensory exploration activities
- Domain J — Feeding: Hand-to-mouth tolerance feeding into food texture acceptance
- Domain G — Daily Living: Tolerating hand contact with food, water, and everyday surfaces
The Bigger Picture
Every technique in the Pinnacle Blooms library is mapped to this 12-domain wheel. As your child progresses through the tactile sensory domain, their gains ripple outward — creating openings in motor skills, social participation, and daily independence that were closed before.
The GPT-OS® platform tracks progress across all 12 domains simultaneously, showing you how work in one area is activating change in others.
📱 Launch GPT-OS® Assessment → pinnacleblooms.org/gpt-os — See your child's full developmental profile across all 12 domains

Families Who've Been Here
Two anonymized vignettes from the Pinnacle Blooms Network — representing the thousands of families who began exactly where you are now, and who built the bridge one session at a time.
Priya's Story — 4 Years Old
Before: Priya (name changed) screamed at the sight of finger paint. Art time at preschool meant sitting in the corner alone. Every birthday party craft station was a crisis. Her mother felt helpless and increasingly isolated from other parents whose children "just played."
After 12 weeks: Priya now paints with brushes independently. She voluntarily touched kinetic sand in week 6. By week 10, she wore gloves and finger-painted alongside peers. Her mother cried — not from frustration, but watching her daughter create art with her friends for the first time.
"Priya's profile showed severe tactile over-responsivity. We started with dry rice bins using long-handled scoops. The graduated exposure chart was her roadmap — she would point to the next step and say 'maybe tomorrow.' That self-awareness is the intervention working." — From the Therapist's Notes
Arjun's Story — 2.5 Years Old
Before: Arjun (name changed) wouldn't eat with his hands. He had used a fork since 18 months — not precocity, but avoidance. Sand at the park triggered full meltdowns. His father questioned whether he was "too soft" on his son, carrying guilt that had no place being there.
After 8 weeks: Arjun plays in dry sensory bins for 10+ minutes. He tolerates cloud dough with both hands. He ate a piece of roti with his fingers for the first time at week 7. His father now sets up the sensory bin daily — it has become their morning routine and a ritual they both look forward to.

Connect With Other Parents
You are not a solo operator navigating a challenge that no one else understands. You are part of a global community of parents who set up sensory bins, celebrate fingertip touches, and learn to read their child's nervous system one session at a time. That community is here — and it is powerful.
Tactile Sensory Support Group
A WhatsApp community for parents navigating texture aversion. Share wins, ask questions, get real-time support from parents a few weeks ahead of you on the same path.
Join Now
Pinnacle Parent Forum
Online community for sharing strategies, celebrating milestones, and finding solidarity. Moderated by Pinnacle Blooms clinicians. Evidence-informed discussion in a warm, peer-led space.
pinnacleblooms.org/community
Local Parent Meetups
Organized by your nearest Pinnacle Blooms center. In-person connection with families navigating similar journeys. Children welcome — sensory-friendly environments by design.
pinnacleblooms.org/centers
Peer Mentoring
Connect with a parent who has completed this journey and is willing to share their experience, answer your specific questions, and provide genuine peer support week by week.
pinnacleblooms.org/peer-mentor
"Your experience helps others. When you share your journey, the next family who arrives here finds it a little less lonely."

Your Professional Support Team
Home practice is powerful. Clinical support is amplifying. The combination of consistent home sessions and professional guidance produces outcomes that neither approach achieves alone. Here is how to access the professional layer of your child's support system.
🗺 Find Your Nearest Pinnacle Blooms Center
70+ centers across India, staffed by OTs who specialize in sensory processing disorders and tactile defensiveness.
- Interactive map: pinnacleblooms.org/centers
- Therapist matching by specialty — request OT for tactile defensiveness specifically
- Comprehensive Sensory Profile-2 or SPM-2 assessment available
📞 FREE National Autism Helpline
9100 181 181
Available in 18+ languages
Monday–Saturday, 9 AM – 7 PM IST
Available in 18+ languages
Monday–Saturday, 9 AM – 7 PM IST
📱 Teleconsultation — Anywhere in the World
Book a virtual session with a Pinnacle OT who specializes in sensory processing. For families anywhere — urban, rural, or international.
What a Professional Adds
- Comprehensive sensory profile assessment (Sensory Profile-2 or SPM-2)
- Individualized texture hierarchy calibrated to your child's specific profile
- Clinical-grade materials and a controlled therapeutic environment
- Progress monitoring with standardized measures over time
- Coordination with school, SLP, BCBA, and other members of the team
"Home + clinic = maximum impact."

The Research Library — For the Curious Parent
You deserve to know that what you are doing has been studied, validated, and published in peer-reviewed journals. These are not opinion-based recommendations. They are evidence-based practices backed by systematic reviews, meta-analyses, and randomized controlled trials. Here is the full stack.
Level I — Systematic Reviews
📄"Sensory Integration Intervention for Children with ASD: PRISMA Model Systematic Review" (Children, 2024) — 16 articles confirming evidence-based practice status → PubMed: PMC11506176
📄"Efficacy of Sensory Integration Therapy in Children with Autism: Meta-Analysis" (World J Clin Cases, 2024) — 24 studies demonstrating effectiveness → PubMed: PMC10955541
Level II — Randomized Controlled Trials
📄"Home-Based Sensory Interventions in Indian Children with ASD" (Padmanabha et al., Indian J Pediatr, 2019) — validates parent-administered sensory intervention → DOI: 10.1007/s12098-018-2747-4
Level III — Clinical Guidelines
📄 NCAEP Evidence-Based Practices Report (2020) — classifies sensory integration as evidence-based practice for autism
📄 WHO Nurturing Care Framework (2018) — global framework for early childhood development
📄 WHO Nurturing Care Framework (2018) — global framework for early childhood development
Foundational Works
📄 Ayres, A.J. — Sensory Integration and the Child (1979, revised 2005)
📄 Dunn, W. — Living Sensationally: Understanding Your Senses (2008)
📄 Miller, L.J. — Sensational Kids: Hope and Help for SPD (2006, 2014)
📄 Dunn, W. — Living Sensationally: Understanding Your Senses (2008)
📄 Miller, L.J. — Sensational Kids: Hope and Help for SPD (2006, 2014)
WHO/UNICEF References
📄 WHO Care for Child Development (CCD) Package — PMC9978394
📄 UNICEF Developmental Monitoring Indicators (2025)
📄 UNICEF Developmental Monitoring Indicators (2025)

How GPT-OS® Uses Your Data
Every session you track becomes an input that makes the system smarter — for your child, and for the millions of children whose families use the same platform. Here is exactly what happens to your data, how it serves your child, and how it is protected.
What GPT-OS® Learns From This Technique
- Your child's texture tolerance profile — which textures, which levels
- Rate of progress — how quickly tolerance is building session to session
- Optimal session duration and frequency for your child's specific profile
- Which materials are most effective for your child's response pattern
- When to recommend progressing to the next technique in the hierarchy
Privacy & Data Protection
- ✅ All data encrypted in transit and at rest
- ✅ Your child's data is never sold or shared with third parties
- ✅ You control your data — view, download, or delete at any time
- ✅ Compliant with Indian DPDP Act and international data protection standards
"Your data helps every child like yours." Population-level patterns from 20M+ sessions make individual recommendations smarter. When aggregate data confirms that dry rice bins are the optimal starting point for severe tactile defensiveness, that insight helps the next family who arrives at Card 01.

Watch the Reel — Sensory Solutions, Episode 6
Reel ID: A-006
Sensory Processing — Tactile Defensiveness
Sensory Solutions Series
Watch a Pinnacle Blooms therapist demonstrate all 9 materials in sequence — showing correct presentation technique, child response cues, and the graduated approach from dry sensory bin through to washable paint. This is the protocol brought to life in a real therapeutic session.
Dry Sensory Bin Invitation
The full invitation sequence — parent modeling, tool offering, response to approach and resistance cues
Theraputty Demonstration
Firm resistance, clean release property shown in real time. Tool-first approach to hand engagement
Mess-Free Paint Bag Setup
Exact setup method — paint quantity, bag sealing, table-taping technique, and child-led color mixing
Tool Progression in Real Time
Long-handle to short-handle to fingers — watching a child move through the progression naturally within a single session
Kinetic Sand vs. Regular Sand
Side-by-side comparison showing why clean-release property changes the child's experience entirely
Cloud Dough Recipe Demo
Live kitchen preparation — 8 cups flour, 1 cup oil — and introduction to a child at Level 2 tolerance
Graduated Exposure Chart Creation
How to build the chart with a child, use stickers as reinforcement, and make it a collaborative roadmap rather than an adult-imposed checklist

Share This With Your Family
Consistency across caregivers multiplies impact. If only one parent executes this technique, progress is limited to one person's presence. When every caregiver — spouse, grandparent, nanny, teacher — understands the approach, the child's entire world becomes therapeutic. Share this page today.
Key Messages for All Caregivers
- ✅ This is neurological, not behavioral — the distress is genuinely real
- ✅ Never force texture contact — it creates trauma, not tolerance
- ✅ Tools and gloves are bridges to participation, not weakness
- ✅ Celebrate every step — not just the end goal
- ✅ Wipes within arm's reach. Always. Non-negotiable.
Share Now
📥 Downloadable Family Guide (1-Page PDF)
"Understanding Your Grandchild's Texture Sensitivity" — a simplified, compassionate version for extended family members who may be skeptical or confused about why the child can't "just touch" things.
🏫 Teacher Communication Template
A pre-written letter to share with your child's preschool or school teacher — explaining your child's sensory needs, the accommodations that enable participation, and how the classroom can support rather than inadvertently undermine progress.
Link: techniques.pinnacleblooms.org/sensory/messy-play-avoidance-materials — Send this exact page to every adult in your child's life who interacts with messy play, art, or outdoor sensory activities.

Frequently Asked Questions
These are the questions parents ask most often — across thousands of consultations, support group conversations, and helpline calls. Clear, honest, evidence-grounded answers.
"Is my child being manipulative by avoiding messy play?"
No. Tactile defensiveness is a neurological pattern. Their nervous system genuinely processes textures as threatening. This is not a choice — any more than flinching when you touch a hot stove is a choice. The SPD Foundation classifies this as tactile over-responsivity: a measurable difference in sensory processing, not a behavioral strategy.
"Will they grow out of it?"
Some children show natural improvement as their nervous system matures. However, structured gradual desensitization significantly accelerates progress and prevents secondary effects: social isolation, anxiety around activities, and limited fine motor development. Waiting without intervention risks avoidance patterns becoming deeply entrenched.
"How long will this take?"
Initial indicators emerge in weeks 1–2. Consolidation signs appear in weeks 3–4. Mastery indicators typically emerge between weeks 5–8 with consistent practice (3–5 sessions per week). Full generalization across all textures and settings may take months. Progress is individual — the arc is real, but the pace varies.
"Should I remove the tools and gloves to make them touch directly?"
No. Tools and gloves are legitimate therapeutic accommodations that enable participation. Many children voluntarily progress to direct touch over time as comfort builds organically. Removing accommodations before the child is ready creates regression and negative associations with the entire activity.
"Can I do this at the same time as professional OT?"
Absolutely — and it is highly recommended. Home practice between professional OT sessions amplifies outcomes significantly. Share your tracking data (Card 20) with your OT so they can calibrate their clinical sessions to match your home progress precisely.
"My child is fine with textures THEY create but panics at unexpected mess."
Very common. Self-initiated texture contact is processed differently by the brain than unexpected contact — the child has control in the first scenario and not the second. Build progressively from self-initiated → predictable → gradually less predictable texture exposure as tolerance grows.
"Will accommodations like gloves be needed forever?"
Most children gradually reduce their need for accommodations as tolerance builds. Some children will always prefer certain accommodations for specific textures — and that is a completely acceptable long-term outcome. The goal is participation, not perfection. Gloves at age 8 that enable full art class participation are a success, not a failure.
"What if one parent forces texture contact when I'm not there?"
Share this page (Card 37) with all caregivers immediately. Forced exposure without graduated desensitization can increase defensiveness and create texture-related trauma. The approach must be unified across all adults in the child's life. Consistency is the active ingredient that makes the protocol work.
Didn't find your answer? → Ask GPT-OS®: pinnacleblooms.org/gpt-os | Book a teleconsultation: pinnacleblooms.org/teleconsult | FREE Helpline: 📞 9100 181 181
Your Next Step — Start Now
You arrived at this page with a question. You are leaving with a protocol, 9 materials, a 6-step execution guide, a progress arc, a safety framework, and a community. There is one thing left: to begin. Your child's nervous system is ready to be met with patience and the right materials. You are ready to meet it.
🟣 Start This Technique Today
Launch a GPT-OS® guided session — personalized to your child's profile, calibrated to their current tolerance level, and tracked automatically.
📞 Book a Consultation
Connect with a Pinnacle Blooms OT who specializes in tactile defensiveness. Virtual or in-person, anywhere in India and beyond.
FREE Helpline: 9100 181 181
→ Explore Next Technique
Browse the full Tactile Sensory Domain or jump directly to A-007: Clothing Texture Sensitivities — your materials already apply.
OT
Occupational Therapy
SLP
Speech-Language Pathology
ABA
Applied Behavior Analysis
SpEd
Special Education
NeuroDev
Neurodevelopmental Pediatrics
Validated by the Pinnacle Blooms Consortium
Preview of 9 materials that help when child avoids messy play Therapy Material
Below is a visual preview of 9 materials that help when child avoids messy play therapy material. The pages shown help educators, therapists, and caregivers understand the structure and content of the resource before use. Materials should be used under appropriate professional guidance.



















Share this resource
Help others discover thisLink copied!

The Pinnacle Promise
"From fear to mastery. One technique at a time."
A parent arrived on this page scared, confused, and exhausted. By Card 05, they understood the science. By Card 12, they had materials and a setup plan. By Card 22, they knew the protocol step by step. By Card 30, they could see their child's full developmental journey. By Card 37, their whole family was aligned.
Now the loop restarts — with the next technique, and the next, and the next. Until your home becomes a therapeutic environment as powerful as any clinic.
🌐 Explore More Techniques
techniques.pinnacleblooms.org
→ Next Recommended Technique
A-007: Clothing Texture Sensitivities
↑ Return to Top
Your Child Won't Touch Paint, Playdough, or Sand
🌐pinnacleblooms.org | 📞9100 181 181 | 📧 care@pinnacleblooms.org
Built by Mothers. Engineered as a System. 20M+ therapy sessions. 97%+ measured improvement.
CIN: U74999TG2016PTC113063 | DPIIT: DIPP8651 | MSME: TS20F0009606
⚠️ Disclaimer: This content is educational and does not replace assessment by a licensed occupational therapist. Tactile defensiveness exists on a spectrum — severe cases may require professional sensory integration therapy. If your child's texture aversion significantly impacts daily functioning, eating, or causes extreme distress, please consult a qualified professional. Individual results may vary. Statistics represent aggregate outcomes across the Pinnacle Blooms Network. © 2025 Pinnacle Blooms Network®. All rights reserved. Powered by GPT-OS® | techniques.pinnacleblooms.org
