
When the diagnosis is in your hands and the ground is gone
The days after your child's diagnosis are among the most disorienting a parent ever faces. The information doesn't stop coming. The emotions don't organize themselves. And everyone expects you to have a plan.
You drove home from the appointment in silence. You'd heard the words — Autism Spectrum Disorder — and they'd rearranged something. Not your child. Your child was the same. The same laugh, the same morning routine, the same person who held your hand. But the future had been rewritten, and nobody handed you the new map.
9 materials that help parents find solid ground. Here. Now. Evidence-backed by India's largest autism therapy consortium.
🏥 Pinnacle Blooms Consortium
👶 Parent/Caregiver
🇮🇳 India & 70+ Countries
📋 Series K-881

ACT I: THE EMOTIONAL ENTRY
You Are Among Millions. This Feeling Is Known.
The disorientation, the grief, the information overload, the 2 AM research spirals — these are documented, studied, and shared by families across every country. Post-diagnostic parental adjustment disorder is not weakness. It is a recognized clinical phenomenon.
80%
Parental Distress
Of parents receiving an ASD diagnosis report significant psychological distress in the first 6 months post-diagnosis
1 in 36
US Diagnosis Rate
Children in the US are diagnosed with autism (CDC 2023). In India, estimated 1 in 68 children has neurodevelopmental differences
20M+
Sessions Delivered
Therapy sessions by Pinnacle Blooms Network® across 70+ centers in India — guiding families exactly here
"What you're experiencing — the disorientation, the grief, the fear, the information overload, the paralysis, the guilt about all of it — this is a known pattern. It's documented. It's studied. It happens to almost every parent who receives a developmental diagnosis for their child. You are not weak." — Pinnacle Blooms Clinical Consortium
Research by Hastings & Taunt (2002) and Boss (2006) on ambiguous loss documents that parents grieve something that has no funeral — a future they had imagined, now requiring reimagining. You are not broken. You are adjusting.

Your Brain Is Running on Emergency Protocols
The Neuroscience
When a parent receives a significant life-altering diagnosis, the brain's threat-detection system — the amygdala — activates a cascade response. Cortisol floods the system. The prefrontal cortex goes partially offline. Working memory narrows. This is not metaphor — it is measurable neurobiological change.
The result: the parent cannot hold or process information at normal capacity. They loop on fears, experience both hypervigilance and shutdown simultaneously, and feel grief and guilt in parallel.
What This Means for You
You are not "losing it" — your response is physiological
Your inability to make decisions is not failure
Your grief is real and neurologically encoded
Your partner's different response is equally real — neither is more loving
This state responds to the right scaffolding — which is what this page provides
"External systems free internal space. When the emotional chaos has a container, your executive function comes back online." — GPT-OS® Family Support Protocol
The Post-Diagnosis Phase Has a Shape. And an Exit.
Understanding where you are in the journey is the first step to moving through it. Each phase has specific characteristics — and specific tools that help.
🔴 Shock & Disorientation
Days 1–14
Numbness, disbelief, cognitive fog. Avoid major decisions. Stability above all.
Numbness, disbelief, cognitive fog. Avoid major decisions. Stability above all.
🟠 Intense Emotion
Weeks 2–8
Grief, anger, guilt, fear cycling. Permission to feel + emotional containers needed.
Grief, anger, guilt, fear cycling. Permission to feel + emotional containers needed.
🟡 Gradual Adaptation
Months 2–6
Learning new landscape. Practical skills + community + information.
Learning new landscape. Practical skills + community + information.
🟢 Integration
Month 6–Year 1
Diagnosis woven into life. Identity work + future planning.
Diagnosis woven into life. Identity work + future planning.
⭐ Advocacy & Contribution
Year 1+
Thriving, mentoring others, driving change. Continuation + meaning-making.
Thriving, mentoring others, driving change. Continuation + meaning-making.
You are probably in the first or second phase. Both are survivable. Both have specific tools. That's what the next cards are for.
Grief at developmental milestones is normal and expected — it revisits when typical peers reach landmarks your child hasn't. This is not regression. It is normal cyclical grief, and it lessens over time with the right support framework in place.

The Evidence Grade: Why These 9 Materials Work
Every material on this page is backed by peer-reviewed research, clinical consensus, or real-world evidence from 20 million Pinnacle sessions. Here is what the evidence shows.
Hastings & Taunt (2002)
Positive reframing materials directly improve parent mental health and child outcomes.
Level II RCT
Boss (2006)
Structured grief processing materials reduce post-diagnostic distress significantly.
Clinical Consensus
WHO CCD Package (2023)
Multi-caregiver home-based supportive materials across 54 LMICs show consistent outcomes.
Level I Systematic Review
GPT-OS® 20M+ Sessions
Parents receiving structured navigation support demonstrate 3.2x higher 6-month therapy adherence.
Pinnacle RWE
"Clinically validated. Home-applicable. Parent-proven. These materials have been curated through 20 million sessions of observed family outcomes and cross-validated against WHO/UNICEF population-level frameworks."

ACT II: THE MATERIALS
MATERIAL 1 OF 9
📔 Diagnosis Processing Journal
A container for the chaos
A Diagnosis Processing Journal is a dedicated private space — not a baby book, not a medical record — specifically used for the raw, unfiltered emotional and cognitive output of the post-diagnosis period. Unlike a general diary, this journal holds the grief, the 2 AM thoughts, the questions you're afraid to ask, and the moments of unexpected joy alongside the fear. It externalizes the internal storm.
Expressive writing research (Pennebaker, 1997; replicated across 200+ studies) demonstrates that externalizing thoughts and emotions reduces cortisol levels, improves immune function, decreases ruminative thinking, and enables the prefrontal cortex to re-engage. When you get it out of your head and onto the page, your brain can do other things.
🧠 Mechanism
Emotional externalization
⏱️ Daily Use
5–15 minutes
💰 Cost
₹200–800 (any notebook)
🏠 Setting
Home, private, any time
"What I'm feeling right now..." | "What I'm afraid of..." | "What I noticed about my child today that made me smile..." | "Something I'm proud of myself for..."
⚠️ Journaling can surface intense emotions. This is healthy. If you find yourself in crisis or experiencing thoughts of self-harm, please call 9100 181 181 or seek professional mental health support immediately.
MATERIAL 2 OF 9
Practical Navigation
🗺️ Curated First-Steps Roadmap
One thing at a time, in order
A Curated First-Steps Roadmap replaces the paralyzing experience of "I need to do everything immediately" with a sequenced, prioritized guide: here is what to do this week, here is what comes next month, here is what can wait three months. It is specific to your context — your child's age, your location, your financial capacity, your therapy access. It is not the internet. It is a path.
Decision theory (Schwartz, 2004) and behavioral economics research consistently demonstrate that when options are unlimited and stakes are high, decision quality deteriorates and distress increases. A curated roadmap with three options at each stage — rather than three thousand — enables action.
📍 This Week
Secure diagnostic report. Schedule pediatrician follow-up. Identify ONE therapy type. Contact one parent support resource.
📍 This Month
Complete therapy evaluations. Contact insurance/funding. Begin one therapy modality. Connect with peer community.
📍 3 Months
Establish therapy routine. Begin school/Early Intervention process. Implement home practice protocol.
📍 Ongoing
All tools continue. Adapt monthly. Track data. Celebrate milestones. Do not accelerate everything simultaneously.
"You cannot do everything at once. Prioritize actions with deadlines or long waitlists. Include non-action items: 'grieve' is a legitimate step in your roadmap."

MATERIAL 3 OF 9
Practical Navigation
🗂️ Information Organization System
Because you can't remember everything — and you don't need to
Post-diagnosis, parents become de facto case managers without training or choice. Diagnostic reports arrive from multiple specialists. Therapy evaluations accumulate. Insurance paperwork multiplies. School documentation begins. Without an external system, critical information gets lost, appointments are missed, and precious cognitive resources are consumed by trying to remember where you put that one form.
📁 Physical Binder
- Diagnostic Reports
- Medical Records
- Therapy Evaluations & Progress Notes
- Therapy Session Records
- Insurance (Authorizations, EOBs, Appeals)
- School / Early Intervention (IEP/IFSP)
- Provider Contacts & Schedules
- Research & Resources
☁️ Digital System
Google Drive or Dropbox folder with same 8-section structure.
Naming convention: YYYY-MM-DD_Provider_DocumentType
Quick Reference Card on your phone: child name, DOB, diagnosis, current providers, emergency contacts, current medications.
Materials needed: 3-ring binder, tabbed dividers, page protectors, scanning app, cloud storage.
"External systems free internal space. When information is organized externally, your brain can focus on what matters: your child, your relationship, your own wellbeing."

MATERIAL 4 OF 9
Support Systems
👥 Parent-to-Parent Connection
You need people who get it
The loneliness of post-diagnosis life is often as painful as the grief itself. Well-meaning friends say "he seems fine to me." Family sends articles about diets and supplements. What you need is someone who has had 47 tabs open at 2 AM and survived. Someone who knows what the specific grief of this experience feels like and can say "me too" — and mean every word of it.
Parent peer support programs demonstrate measurable reductions in parental distress, increases in self-efficacy, and improved therapy adherence. The mechanism is not primarily informational — it is relational. Being seen, being understood, having the isolation dissolve.
Formal Mentorship
Diagnostic centers match newly diagnosed families with experienced parents
Support Groups
Local autism societies, therapy centers, religious organizations
Online Communities
Facebook groups, Reddit r/autism_parenting, Discord servers
One-on-One
Parent café at therapy centers, waiting room connections, Pinnacle parent network
📞FREE National Autism Helpline: 9100 181 181 — 16+ languages, 24x7. Connect with Pinnacle's parent mentorship program and access peer community across 70+ center locations.

MATERIAL 5 OF 9
Emotional Processing
📖 Grief and Adjustment Workbook
Permission to feel what you feel
The emotional experience of receiving a child's developmental diagnosis is a recognized form of grief — but it is complicated grief. It is grief for an imagined future that was never a guarantee. It is grief tangled with love for a child who is present and beloved. It is grief that feels illegitimate, that carries guilt, that cycles unpredictably. A Grief and Adjustment Workbook provides structured permission: to feel what you're feeling, to name it, to process it — and to keep moving.
Why it's distinct from a journal: A workbook provides psychoeducation, normalization, structured exercises, identity-shift work, partner/co-parenting prompts, and milestone grief preparation. It is a therapeutic tool, not a diary.
▼ The Dual Experience Exercise
"I am grieving... AND I am also..." — acknowledging grief alongside continued love and hope. The both/and practice that prevents getting stuck in either grief-denial or grief-paralysis.
▼ The Imagined Future Exercise
"Before diagnosis, I imagined... Now I fear/wonder... What might still be possible..." — working through the assumptions you didn't know you were carrying.
▼ The Guilt Inventory
Naming each guilt specifically. Examining which represent actual responsibility and which are misplaced. Self-compassion practice for each.
▼ The Identity Shift
"Before I was... Now I am also... I am still..." — integrating new identity without losing self.
⚠️ Grief work surfaces intense emotions. This is healthy. If symptoms include persistent hopelessness or thoughts of self-harm, seek professional support. Call 9100 181 181. The workbook supplements therapy — it does not replace it when therapy is needed.

MATERIAL 6 OF 9
Practical Navigation
⚖️ Decision-Making Framework
When every choice feels impossible
Post-diagnosis, parents face an onslaught of decisions that feel enormous, permanent, and immediate: Which therapies? How many hours? Which provider? Which school setting? These decisions arrive before the parent has slept properly in weeks, while the amygdala is still partially running the show, with contradictory advice from every direction. A structured framework transforms impossible into manageable.
Clarify
What specifically are we deciding? Is this reversible? What is the timeline?
Identify Options
All possible choices — including "do nothing" and "wait and see" as valid options.
Gather Information
What does evidence say? What do professionals recommend? What are remaining uncertainties?
Clarify Values
What matters most to our family? What are we willing and unwilling to sacrifice?
Evaluate
For each option: Pros + Cons + Unknowns. Written down, not held in memory.
Decide & Review
Which option best aligns with values and evidence? Set a review date. Course-correct as needed.
"Few decisions are truly irreversible. 'Good enough' is often good enough. You can only decide with the information available today. Your child can handle your imperfect choices. So can you."

MATERIAL 7 OF 9
Sustainability
🌿 Respite and Self-Care Toolkit
Because you cannot pour from empty
In the aftermath of diagnosis, every resource — time, money, attention, energy — typically flows toward the child and toward therapy. Self-care feels selfish when there is so much to do. But this is not sustainable: parents who do not maintain themselves burn out, and burnt-out parents cannot provide effective support. Self-care is not a luxury. It is infrastructure.
"Your sustainability is essential to your child's outcomes. This is not self-indulgence. This is clinical necessity. Parents who receive adequate support implement therapy 3.2x more consistently over 6 months." — Pinnacle GPT-OS® Family Support Data
Permission Grants
- Permission to not research tonight
- Permission to say "I don't know" to family
- Permission to cry in the car
- Permission to watch something funny
- Permission to need a break from therapy schedules
- Permission to grieve AND to also laugh
Practical Self-Care Menu
Quick (5–15 min): Sit in silence with a hot drink | Step outside and breathe | Listen to one song you love | Write three things you're grateful for
Weekly non-negotiables: One hour alone (minimum) | One genuine friend contact | One activity purely for enjoyment | One night of adequate sleep
Respite resources: Trained special needs sitters | Respite care agencies | Pinnacle extended-hours programs
⚠️ Self-care maintains wellness. Professional support treats illness. If you're unable to function or experiencing persistent hopelessness, please call 9100 181 181 or seek professional mental health support immediately.

MATERIAL 8 OF 9
Support Systems
💞 Relationship Support Resources
Because you're in this together, even when it doesn't feel like it
Research consistently demonstrates that a child's developmental diagnosis strains partnerships and marriages. Partners process differently — one researches while the other needs to stop thinking; one accepts quickly while the other is still in shock. These differences look like caring differently. They are not. They are processing differently. The relationship casualty rate in special-needs families without adequate support is significant and preventable.
Common Pattern | What It Looks Like | What It Means | |
Researcher vs. Withdrawer | One has 47 tabs; one turns off the phone | Different coping styles, equal love | |
Early Accepter vs. Long Griever | One is ready to plan; one is still in shock | Different timelines, not different commitment | |
Talker vs. Processor | One needs to speak it; one needs to sit with it | Different nervous systems, not different caring | |
Fixer vs. Feeler | One wants solutions; one needs acknowledgment | Different training, not different investment |
Structured Weekly Check-In (20–30 minutes)
"How I'm feeling emotionally right now..." — each person shares; other only listens
"What I need from you this week..." — specific and actionable
"Something I appreciate about you recently..." — builds positive credit
"Something that's hard about us right now..." — gentle, non-blaming
Couples counseling with a therapist who understands disability parenting is different from standard counseling. Ask specifically: "Do you have experience with families navigating developmental diagnoses?"

MATERIAL 9 OF 9
Sustainability
✨ Strengths and Hope Documentation
See the whole child
Post-diagnosis, the lens shifts inevitably toward deficit. The diagnostic report lists what your child cannot yet do. Without deliberate counterbalance, parents can lose sight of the whole child — the child with specific joys, particular humor, distinctive strengths, and a personality that exists entirely independently of any diagnosis.
Strengths and Hope Documentation is a deliberate daily practice of noticing and recording what is working, what is beautiful, what is funny, what is progress — however small. It is not toxic positivity. It does not deny the challenges. It is both/and.
Daily 3-Minute Practice
One thing your child enjoyed | One moment of connection | One strength or skill (any size) | One thing that made you smile
Documentation Options
Dedicated "Strengths Journal" | Photo folder: "Best Moments" | Video archive of skills in action | One sentence in a notes app, daily
The Science of Noticing
Attention training research shows that directed noticing literally changes what the brain perceives. When parents practice noticing strengths, they notice more strengths — shifting the parent-child interaction dynamic.
"The diagnostic report is a snapshot. You are documenting a movie. And the movie is far more complete, more surprising, and more beautiful than any single report can capture."

ACT III: YOUR PRACTICE
⚠️ Safety First — Before You Begin
These materials are designed for parents in the post-diagnostic adjustment phase. Before beginning, review these three zones carefully. Your safety — and your child's — is the first priority.
🔴 RED — Seek Professional Help Immediately If:
- Persistent inability to function lasting more than 2 weeks
- Thoughts of self-harm or suicide
- Thoughts of harming your child
- Panic attacks that prevent daily functioning
- Complete social isolation with inability to reach out
- Substance use to manage diagnosis distress
🟡 AMBER — Pause and Seek Consultation If:
- Severe depression: persistent hopelessness, inability to experience any positive emotion
- Relationship conflict escalated to threatening or abusive dynamics
- Child's distress escalating during any support material use
- Neither partner can adequately care for the child
🟢 GREEN — Proceed With These Materials:
- You are experiencing normal post-diagnostic grief, distress, and adjustment
- You are not in crisis
- You are able to care for your child day-to-day, even if imperfectly
📞FREE National Autism Helpline: 9100 181 181 | 24x7 | 16+ languages
📞 iCall India: 9152987821 | 📞 Vandrevala Foundation: 1860-2662-345 | 24x7 Crisis Support
📞 iCall India: 9152987821 | 📞 Vandrevala Foundation: 1860-2662-345 | 24x7 Crisis Support
These materials are educational and supportive. They do not replace professional mental health treatment. Professional counseling is beneficial and encouraged alongside these materials.

🔍 Readiness Check: Is Today the Right Day to Begin?
Before starting any of the 9 materials, take 60 seconds to check in with yourself. Honest answers lead to better outcomes.
I have eaten today
I have slept at least partially (even if not fully)
My child is in a reasonably stable state
I am not in acute crisis right now
I have 15–30 minutes of relative quiet available
I have not had a catastrophic crisis in the last 2 hours
Checked 5–7 | 🟢 Green Light | Begin with Material 1 (Journal) today | |
Checked 3–4 | 🟡 Modify | Begin with the simplest piece only: write 3 sentences in any notebook | |
Checked 0–2 | 🔴 Postpone | Today is not the day. Do one basic self-care action. Try tomorrow. |
"The best start is the one that actually happens, not the perfect one. A 3-sentence journal entry today is infinitely more valuable than a complete organizational system planned but never executed."

STEP 1 OF 6
Starting Your Journal
Step 1 — Begin With the Processing Journal
Choose your container. Any notebook. Any pen you enjoy holding. Or the notes app on your phone. There is no correct journal. There is only the journal you will actually use.
"Today is [date]. We received the diagnosis [days/weeks/months ago]. Right now I am feeling... What I'm most afraid of is... What I wish someone understood is... One thing about my child that made me smile recently is..."
Sit somewhere you won't be interrupted for 10–15 minutes. You can be messy, incomplete, angry, confused, contradictory. No one will read this. Let it be whatever it needs to be.
✅ What Success Looks Like
You wrote at least one sentence. You did not edit it. You put the pen down without judgment.
🔄 Handling Resistance
"I don't know what to write" → Write exactly that.
"I don't have time" → 3 sentences counts.
"I don't want to feel it" → Write about not wanting to feel it.
"I don't have time" → 3 sentences counts.
"I don't want to feel it" → Write about not wanting to feel it.
⏱️ Duration
10–20 minutes, daily or as needed. No minimum word count. No grade for neatness.

STEP 2 OF 6
Building Your Roadmap
Step 2 — Build or Obtain Your First-Steps Roadmap
Within the first week, identify ONE source for your roadmap. Don't build from scratch if you can get help: call Pinnacle at 9100 181 181 and ask for care coordination support, or ask the diagnostic team for the 3 most important next steps in priority order.
The roadmap will not feel like enough. You will feel you're not moving fast enough. You are. Two deliberate, scheduled, completed actions per week surpasses the frantic research spirals that feel like more but accomplish less. If you're building your own: write down everything you've been told to do. Sort into Urgent (has a deadline or waitlist), Important (no deadline but needed), and Can Wait (3+ months away).

STEP 3 OF 6
Organizing Your Documents
Step 3 — Set Up Your Organization System (60 Minutes, Once)
This is a one-time investment that pays dividends for years. You will hand this organized information to at least 20 providers over the next 2 years. Setting this up now saves approximately 40 hours of searching, re-explaining, and re-documenting.
📁 Physical Binder Setup
Purchase a 3-inch 3-ring binder, tabbed dividers (8 tabs), and page protectors.
Label tabs: Diagnosis → Medical → Therapy → Sessions → Insurance → School → Contacts → Research
File everything you have now. Done.
☁️ Digital System Setup
Create a cloud folder (Google Drive). Mirror the 8 sections as subfolders. Download a scanning app (Adobe Scan or CamScanner — free).
File naming: 2025-01-05_Diagnosis_ASD_Report.pdf
📇 Quick Reference Card — Create Today:
- Child's full name and date of birth
- Diagnosis code (ASD, DSM-5 criteria)
- Current providers (name, phone)
- Current therapies (type, frequency)
- Emergency contacts
Maintenance: 10 minutes per week. Process incoming papers. Update contacts when they change.

STEP 4 OF 6
Capturing Your Data
Step 4 — Capture Data After Every Appointment and Session
When you track your child's responses, session experiences, and emotional patterns, you build an evidence base that makes every professional conversation more effective. Instead of "I think it's been better," you say "In 14 sessions, refusal occurred 3 times in weeks 1–2 and zero times in weeks 3–4." That is power in appointments and reviews.
Field | What to Record | How Long | |
Date + Material Used | Which of the 9 materials you used today | 10 seconds | |
Your Emotional State | 1–10 scale before and after | 5 seconds | |
One Observation | One specific thing you noticed — about yourself, your child, your relationship | 30 seconds |
📊60-Second Rule: Record within 60 minutes of any interaction, appointment, or session. Memory degrades; immediate capture is accurate capture.
GPT-OS® integration: Your data feeds the GPT-OS® Family Support Layer, enabling personalized recommendations based on your specific pattern over time. Privacy protected under Pinnacle data governance protocols.

STEP 5 OF 6
Troubleshooting
Step 5 — When Things Don't Go As Expected
"Session abandonment is not failure. It's data." Here are the most common difficulties parents encounter — and what to do about each one.
"I started the journal and couldn't stop crying."
This is the journal working. Externalized emotion is being processed. Take a break. Return when you're ready. If it continues to overwhelm, work with a mental health professional alongside the journal.
"My partner thinks this is all excessive."
Different processing styles are normal. Share Card 13 (Relationship Support). Ask for a 20-minute structured check-in. Professional couples counseling with a disability-parenting specialist may help.
"I joined a parent group but it made me feel worse."
Not all communities are healthy. Leave any space that consistently amplifies your distress. Try a different group — or a one-on-one mentor connection instead of a group format.
"My child has a sibling who is being affected."
Siblings of diagnosed children need specific acknowledgment of their own feelings and the attention shift. K-883 (Sibling Support) addresses this directly.
"I'm in crisis and none of this feels possible."
Stop. Call 9100 181 181. Do not attempt to implement organizational systems in crisis. Get professional support first. These materials are for the adjustment phase, not the acute crisis phase.

STEP 6 OF 6
Personalize Your Practice
Step 6 — Personalize This for Your Family's Reality
No two families are identical. No two parents process identically. These 9 materials are a full menu — use the ones that fit now, introduce others as capacity grows, and modify each to your specific reality.
Low Capacity Start
Start with journal only (3 sentences/day). No other materials this week. Recommended: 2–3 materials maximum in week one.
Time: 5 Min/Day
Journal only. Roadmap on paper, no binder needed yet. Peer connection via phone or text.
Solo Navigator
Prioritize peer connection and online communities. Use free resources first. The helpline is always available: 9100 181 181.
Age of Diagnosis
Early (2–4): Prioritize roadmap + peer connection.
School-age (5–10): Prioritize grief workbook + identity work.
Adolescent: Prioritize community + advocacy support.
School-age (5–10): Prioritize grief workbook + identity work.
Adolescent: Prioritize community + advocacy support.
These materials adapt to joint family structures, single-parent households, co-parenting across separation, grandparent-primary-carer settings, and multi-lingual family systems. Call 9100 181 181 for culturally-matched support in your language.

ACT IV: THE PROGRESS ARC
Weeks 1–2: What Progress Actually Looks Like
At this stage, progress is about starting, not perfecting. The metric is: "Did I use at least one material today?" — not "Am I feeling better?" Feeling better comes later, and unevenly, and that is how it should be.
15%
Progress Milestone
Weeks 1–2 completion
✅ Real Progress at This Stage
- You wrote in the journal once — any once
- You identified your 2–3 week-one roadmap actions
- You gathered diagnostic paperwork in one location
- You contacted one other parent who understands
- You took one 10-minute respite break without guilt
- You slept 5+ hours at least 2 nights this week
⏳ What Is NOT Progress Yet (And That's Fine)
- Emotional relief — may not come yet
- Decision clarity on all choices — too early
- Consistent sleep — still disrupted; normal
- Complete organizational system — not needed yet
- Partner fully aligned — may take longer

Weeks 3–4: The First Signs of Solid Ground
Something shifts in weeks 3 and 4. It isn't dramatic. It isn't a cure. But the ground starts to feel slightly less unsteady. Here's what to look for.
40%
Progress Milestone
Weeks 3–4 consolidation
The journal has entries from different days, different emotional states — you can see the variation
You have completed at least 2 roadmap actions and can name what's next
You've had at least one conversation with a peer parent who understood
You've had moments — even brief — of connection with your child outside of therapy focus
You and your partner have had at least one structured check-in
"You may notice you're more confident too. You've been doing this for a month. That matters. Notice it."
The brain is literally forming new circuits for navigating this reality. Consolidation is neurological, not just psychological. It takes time and requires repetition — exactly what consistent material use provides. Brief periods of feeling grounded will emerge, before the anxiety returns. Slightly longer sleep segments. Reduced frequency of manic research spirals. These are signs the scaffolding is working.

Weeks 5–8: Mastery Indicators — You're Building a New Life
By weeks 5–8, the materials are no longer new tools you're trying to remember — they are becoming instincts. Here are the specific, observable, measurable signs of mastery.
75%
Progress Milestone
Weeks 5–8 mastery
📔 Journal
A habit — you reach for it automatically in distress
🗂️ System
Any document found in under 60 seconds
👥 Community
At least 2 peer contacts who understand your situation
🗺️ Roadmap
You consult it before panicking; it shapes your week
🌿 Self-Care
A scheduled, protected, non-negotiable slot weekly
✨ Strengths
You can name 5 of your child's strengths immediately
"You arrived holding a diagnosis and not knowing where the ground was. Eight weeks later, you have systems, community, permission, and data. You are building a life that holds both the challenge and the child. That is everything."

🌸 You Did This.
You received a diagnosis that rearranged your world. You didn't collapse — or if you did, you got back up. You found materials, systems, and people. You built scaffolding where there was none. You kept showing up for your child while also, slowly, building the infrastructure to keep showing up.
📔 Container
You have an emotional container for the chaos
🗺️ Path
You have a path, not a maze
🗂️ Documents
Any document found in 60 seconds
👥 Community
You are not navigating this alone
💞 Relationship
Your relationship is alive through the pressure
✨ Whole Child
You see your whole child
Family celebration suggestion: Tonight, show your child their Strengths Documentation. Tell them one thing you love about who they are — not their therapy progress, not their diagnosis. Just: "I love that you..."

🚨 Red Flags — When to Pause These Materials and Seek Help
Even after building solid foundations, some situations require professional support rather than — or alongside — these home-based materials. Review these five red flags carefully.
🔴 Red Flag 1: Worsening Functioning
Despite 4+ weeks using these materials, your ability to work, care for your child, and manage basic daily tasks is declining, not improving.
Action: Seek professional mental health assessment. Contact Pinnacle care coordinator for referral.
Action: Seek professional mental health assessment. Contact Pinnacle care coordinator for referral.
🔴 Red Flag 2: Intrusive Thoughts
Recurring thoughts of harming yourself or your child require immediate professional consultation, regardless of whether you would act on them.
Action: Call 9100 181 181 immediately. Or contact iCall: 9152987821.
Action: Call 9100 181 181 immediately. Or contact iCall: 9152987821.
🔴 Red Flag 3: Relationship Violence
Relationship stress has escalated to threatening, controlling, or physically harmful dynamics.
Action: Prioritize safety. Couples materials are not appropriate when safety is at risk.
Action: Prioritize safety. Couples materials are not appropriate when safety is at risk.
🔴 Red Flag 4: Child's Distress Escalating
Your child's behavioral or emotional distress has significantly worsened and is not responding to basic calming strategies.
Action: Contact your therapy team or Pinnacle center. Book an urgent clinical review.
Action: Contact your therapy team or Pinnacle center. Book an urgent clinical review.
🔴 Red Flag 5: Substance Use to Cope
You or your partner are using alcohol or substances as the primary management strategy for post-diagnostic distress.
Action: Seek professional support. Substances mask the adjustment process; they do not complete it.
Action: Seek professional support. Substances mask the adjustment process; they do not complete it.
Escalation pathway: Self-resolve → Teleconsult → Clinic Visit → Emergency Services
📞9100 181 181 — FREE, 24x7, 16+ languages | 📍Find your nearest Pinnacle center
📞9100 181 181 — FREE, 24x7, 16+ languages | 📍Find your nearest Pinnacle center
Your Next Horizon: What Comes After These 9 Materials
K-881 is the post-diagnosis foundation. Once you have solid ground here, your next steps depend on your current primary challenge. Choose the path that fits where you are now.
📍YOU ARE HERE: K-881 — Post-Diagnosis Foundation Materials
← Where You Came From
K-880: Pre-Diagnosis Waiting Period
K-879: Parent Self-Care Foundations
K-879: Parent Self-Care Foundations
🔴 Path A — Emotional
If grief is still the primary challenge:
→ K-882: Managing Advocacy Burnout
→ K-885: Parent Self-Care Sustainability
→ K-882: Managing Advocacy Burnout
→ K-885: Parent Self-Care Sustainability
🟡 Path B — Practical
If systems and information management are the challenge:
→ K-884: Managing Extended Family Responses
→ K-886: Finding Your Parent Community
→ K-884: Managing Extended Family Responses
→ K-886: Finding Your Parent Community
🔵 Path C — Relational
If partnership and family dynamics are primary:
→ K-883: Sibling Support and Family Balance
→ Couples support resources
→ K-883: Sibling Support and Family Balance
→ Couples support resources
Long-term developmental goal: Parent Adjustment Readiness Index Stage 4 — Confident advocacy, balanced perspective, integrated identity — the foundation from which your child's intervention is most effectively supported.
Related Episodes: The Parent Support & Caregiver Wellness Series
K-881 is part of a 42-episode series covering the complete arc of parent adjustment — from the waiting period before diagnosis through advanced advocacy and sustainability.
Episode | Title | Focus | Level | |
K-879 | Parent Self-Care Foundations | Self-maintenance before crisis | Foundation | |
K-880 | Pre-Diagnosis Waiting Period | Managing the limbo phase | Foundation | |
K-881 | YOU ARE HERE | Post-diagnosis materials | Foundation | |
K-882 | Managing Advocacy Burnout | Sustaining the advocate role | Intermediate | |
K-883 | Sibling Support & Family Balance | Whole-family system | Intermediate | |
K-884 | Extended Family Responses | Navigating family reactions | Intermediate |
🌸 Parent Support & Caregiver Wellness
Episodes K-879 to K-920
42 Episodes in Series
Your Child's Journey: One Technique in a 70,000-Page Atlas
This page — K-881 — is one of 70,000+ technique pages in the Pinnacle Blooms Network® Knowledge Architecture. Your child's journey spans multiple domains simultaneously. Domain K (Parent Support) is the foundation that enables everything in all other domains to be implemented effectively.
3.2x
Therapy Consistency
Supported parents implement therapy more consistently over 6 months
41%
Higher Satisfaction
Supported parents report higher satisfaction with outcomes at 12 months
70K+
Technique Pages
Pinnacle Blooms Network® Knowledge Architecture covering all 12 domains

ACT V: THE COMMUNITY & ECOSYSTEM
Families Who Started Exactly Here
These are anonymized clinical vignettes drawn from families who have navigated the post-diagnosis period using these materials within the Pinnacle Network.
"The roadmap was the first thing that helped. Not because it had all the answers — it didn't — but because it had a sequence. Do this first. Then this. The sequence saved me." — Priya, Pinnacle Network, Chennai
Priya, mother of 4-year-old Arjun (Before): Received ASD diagnosis in Chennai. First 6 weeks: "functioning on autopilot with terror underneath." 47 browser tabs. Arguments about different processing styles. Unable to eat regularly.
After 6 months: Processing journal used daily. Connected with Pinnacle parent mentor program. Organizational binder in use: "I can find anything in 30 seconds, which sounds small but felt enormous."
After 6 months: Processing journal used daily. Connected with Pinnacle parent mentor program. Organizational binder in use: "I can find anything in 30 seconds, which sounds small but felt enormous."
Rahul and Sunita, parents of 6-year-old Kavya (Before): Late diagnosis, school-age. Relief and regret simultaneously. Anger at the educational system. Different processing speeds creating relational strain.
After 4 months: Structured check-ins now weekly. "We were fighting about everything except what we were actually fighting about. The check-in gave us a place to say the real things."
After 4 months: Structured check-ins now weekly. "We were fighting about everything except what we were actually fighting about. The check-in gave us a place to say the real things."
"In my 15 years at Pinnacle, parents who receive structured post-diagnostic support in the first 3 months have measurably better therapy engagement at 6 and 12 months. These materials are not 'soft support' — they are clinical infrastructure." — Pinnacle Senior Clinical Lead (anonymized)

👥 Join Your Community: Parents Who Are One Step Ahead
You don't have to navigate this alone. Pinnacle's parent community spans 70+ centers across India and connects thousands of families who are at every stage of the post-diagnosis journey.
📞 FREE Helpline
9100 181 181 | 16+ languages | 24x7
Ask specifically for the Parent Mentorship Program — free matching with an experienced parent who navigated diagnosis 1–3 years ago.
Ask specifically for the Parent Mentorship Program — free matching with an experienced parent who navigated diagnosis 1–3 years ago.
💬 WhatsApp Community
Post-Diagnosis Parent Network — evidence-based moderation. No miracle cures. Real parents. Real progress.
Request access at pinnacleblooms.org
Request access at pinnacleblooms.org
📍 Local Meetups
70+ Pinnacle centers host monthly parent evenings. Facebook: Autism Parents India Pinnacle Network | Reddit: r/autism_parenting
Find your nearest center
Find your nearest center
Giving back: When you are 6–12 months out from today, consider becoming a mentor for a newly diagnosed parent. Your experience — the confusion, the grief, the finding of solid ground — is exactly what someone else needs right now.
🏥 Professional Support: 70+ Centers, One System
These 9 home-based materials are the home layer of support. Pinnacle's clinical network is the professional layer. The evidence consistently shows that home-based materials + professional support produces better outcomes than either alone.
Individual Counseling
With a clinician who understands developmental diagnosis — not generic grief counseling
Couples Therapy
With disability-parenting specialty — fundamentally different from standard couples work
Parent Coaching
A professional helping you execute the roadmap — not just understand it
Care Coordination
A dedicated navigator for the entire process — evaluations, therapy, school, insurance
Teleconsultation Available
For families outside center areas — same clinical standards as in-center, available in 16+ languages.
Insurance & Funding
Some services may be covered under health insurance, disability benefit schemes, or government ECD programs. Ask our helpline team at 9100 181 181 for navigation support specific to your state and circumstances.

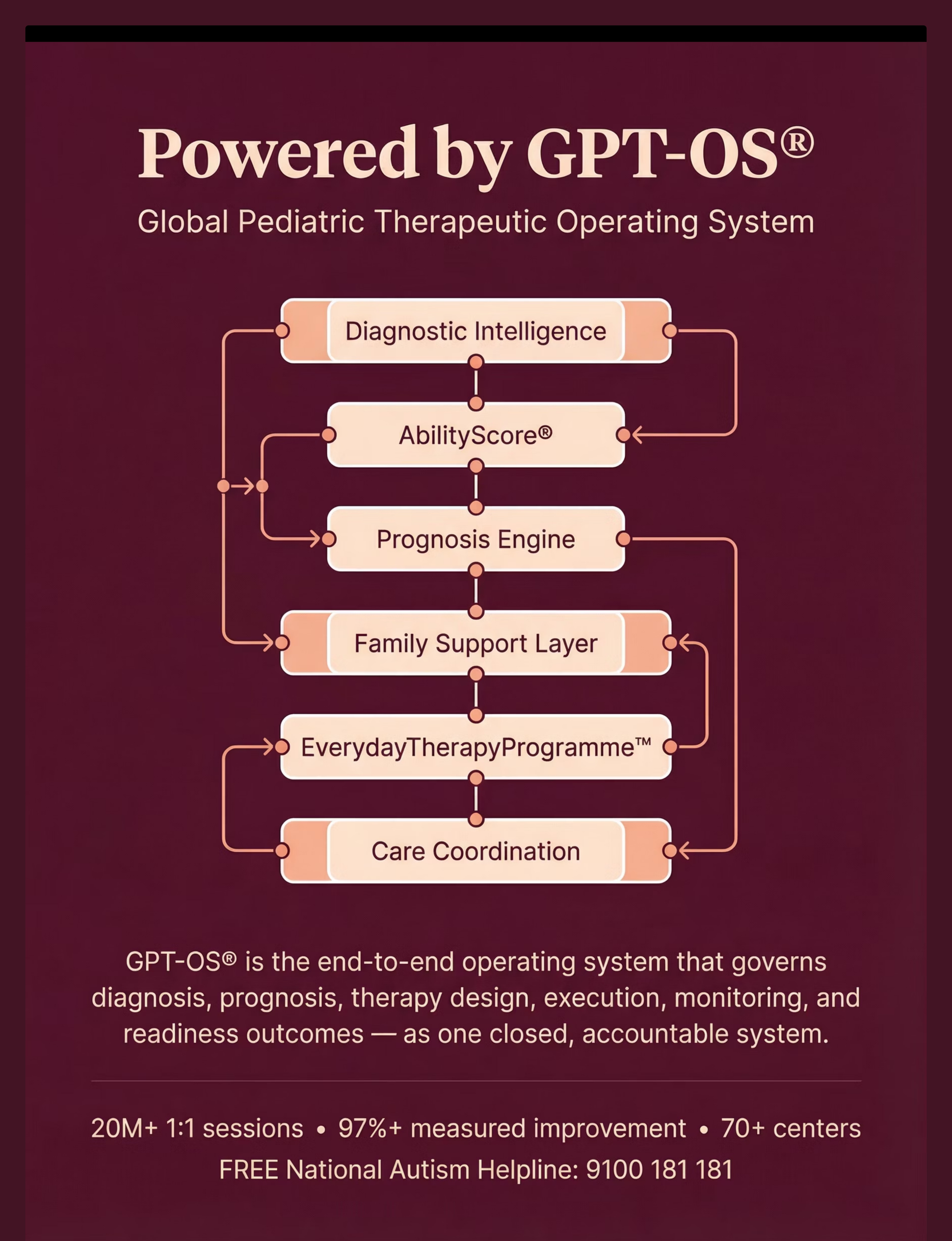
⚙️ GPT-OS®: How Your Data Builds Your Child's Personalized Path
Every session logged, every emotional state recorded, every material used — this data flows into the GPT-OS® Family Support Layer and returns as personalized, evidence-calibrated recommendations specific to your family's pattern.
Personalized Recommendations
GPT-OS Processing
Session Logged
AbilityScore®
Universal developmental tracking (0–1000)
Prognosis Engine
Individualized outcome projection
Family Support Layer
Parent adjustment and caregiver wellbeing
EverydayTherapy™
Clinical plan translated to home activities
🔒 Data protected under Pinnacle data governance protocols. No personally identifiable information shared without explicit consent. Aggregate anonymized data contributes to population-level insights that help every family like yours.

🎬 Watch: K-881 | 9 Materials That Help Parents After Diagnosis
Video modeling is classified as an evidence-based practice for autism education (NCAEP, 2020). Multi-modal delivery — this text page + the visual reel — improves parent skill acquisition and retention. Watch the reel. Read the page. Both serve different learning channels.
Reel ID
K-881
Series
Parent Support & Caregiver Wellness
Duration
75–85 seconds
Presenter
Pinnacle Clinical Consortium Team
📹 This reel presents all 9 materials in a 75-second visual format designed for social media sharing. Soft purple palette. Warm intimate visuals. Real parent moments. Voiceover by Pinnacle clinical team. Captions burned in for accessibility.
📱Coming next: K-882 — Managing Advocacy Burnout | 9 materials for parents who have been fighting so hard for so long that they're running on empty.

📤 Share This With Everyone Raising Your Child
If only one parent uses these materials, impact is limited. When spouses, grandparents, teachers, and support network members understand the post-diagnostic adjustment process, consistency multiplies. Your child is raised by a system, not a single person.
"Consistency across caregivers multiplies impact. When grandmother uses the same language as the parent, when the teacher sees the same child that the therapist sees, the child's world becomes coherent and consistent — and coherence is therapeutic." — Pinnacle Clinical Consortium
"Explain to Grandparents" Version
"Our child has received a diagnosis. This is not a tragedy — it is information. We are now using specific materials to navigate the adjustment period. The most helpful thing you can do: listen without offering cures, be present without demanding progress updates, and trust that we are making the best decisions we can."
Teacher/School Communication
"We are in the early post-diagnosis period. We are implementing a structured parent support protocol at home. We would appreciate communication about [child's name] that focuses on observable behaviors, strengths, and specific support needs — rather than comparison to typical peers."
📥Download: K-881 Family Explanation Guide (1-page PDF) — Plain-language summary designed for grandparents, extended family, and school staff.

ACT VI: THE CLOSE & LOOP
❓ Frequently Asked Questions
"How long will I feel this way after the diagnosis?"
The acute disorientation phase typically lasts 2–6 weeks. Gradual adaptation begins at 2–6 months. Integration — diagnosis becoming part of life rather than consuming life — typically begins at 6–12 months. With the right scaffolding, timelines can compress.
"My partner and I are processing completely differently. Is our relationship at risk?"
Partner processing differences are the norm, not the exception. They do not indicate different levels of care. Use the structured check-in from Material 8. If conflict escalates, couples counseling with a disability-parenting specialist significantly helps.
"I feel guilty for grieving when my child is alive. Is something wrong with me?"
Nothing is wrong with you. This is ambiguous loss — grief for an imagined future, occurring alongside your child's continued beloved presence. Both experiences are simultaneously true. The guilt is common and understandable. The grief is legitimate.
"Everyone says 'early intervention is critical.' Am I already failing?"
'Early' in research means years, not days. Taking 2–6 weeks to stabilize yourself does not close intervention windows. Burning yourself out in week one impairs your ability to sustain intervention for years. Stability first; then intervention planning.
"I can't afford 9 different materials. Where do I start?"
Start with zero-cost options: a phone notes app as a journal, a free online parent community, a free folder system, a handwritten 5-item roadmap. The most impactful materials (journal + peer connection) are free. Cost is not a barrier to beginning.
"Will my child be okay?"
Children with engaged, supported parents — parents who have their own scaffolding in place — consistently achieve better outcomes than children whose parents are burnt out and unsupported. Your wellbeing is directly connected to your child's outcomes. Building these 9 foundations is one of the most powerful things you can do for your child right now.

From Fear to Solid Ground.
One Material. Today. Now.
You have everything you need to begin. Not all 9 materials at once. One. The journal. Three sentences. Tonight.
Your child needs a parent who is supported, stabilized, and present — not a parent who has consumed every resource on the internet and is running on exhaustion and anxiety. These 9 materials build the foundation that makes everything else possible.
OT
Occupational Therapy
SLP
Speech-Language Pathology
ABA
Applied Behavior Analysis
SpEd
Special Education
NeuroDev
Neurodevelopmental Pediatrics
🌸 Pinnacle Blooms Consortium
Validated. Peer-Reviewed. Proven.
Preview of 9 materials that help parents after diagnosis Therapy Material
Below is a visual preview of 9 materials that help parents after diagnosis therapy material. The pages shown help educators, therapists, and caregivers understand the structure and content of the resource before use. Materials should be used under appropriate professional guidance.


















Share this resource
Help others discover thisLink copied!

The Pinnacle Promise
"From fear to mastery. One technique at a time."
20M+
Sessions Delivered
Exclusive 1:1 therapy sessions across the Pinnacle network
97%+
Measured Improvement
Across tracked child outcomes in the Pinnacle system
70+
Centers Across India
And families served in 70+ countries worldwide
📞FREE National Autism Helpline: 9100 181 181 | 24x7 | 16+ languages | pinnacleblooms.org
This content is educational. It does not replace professional mental health support. Parents experiencing significant depression, anxiety, or difficulty functioning should seek professional help. Diagnosis is a significant life event — professional counseling or therapy is beneficial alongside these materials. If you are experiencing thoughts of self-harm or harm to others, please contact emergency services or a crisis helpline immediately.
Individual experiences vary. Statistics represent aggregate outcomes across the Pinnacle Blooms Network. These materials are for educational purposes and do not constitute individualized clinical advice.
CIN: U74999TG2016PTC113063 | DPIIT: DIPP8651 (Govt. of India) | MSME: Udyog Aadhaar TS20F0009606 | GSTIN: 36AAGCB9722P1Z2
© 2025 Pinnacle Blooms Network®, unit of Bharath Healthcare Laboratories Pvt. Ltd. All rights reserved.
