
"So much inside. No words to let it out."
Your child understands everything. Follows your instructions. Laughs at the right moments. Has opinions and preferences and a personality bursting at the edges. But when they try to tell you — the words don't come.
"You are not failing. Your child is not failing. There is simply a bridge that hasn't been built yet. AAC builds that bridge — today, not someday."
🗣️ Social Communication
Domain B
Ages 2–18+
SLP Lead
B-220
📞 FREE National Autism Helpline: 9100 181 181 | pinnacleblooms.org

You Are Among Millions of Families Navigating This
Among children with autism, cerebral palsy, apraxia, intellectual disability, and other developmental conditions, communication challenges are the most universal experience. Families who introduce AAC report reduced meltdowns, reduced frustration, and — critically — increased spoken words.
1 in 36
Children Diagnosed
Children receive an autism diagnosis globally (CDC 2023)
~35%
Complex Communication Needs
Of autistic children require AAC support
70+
Countries Served
Pinnacle families served — across 20M+ therapy sessions
AAC is not giving up on speech. Research consistently shows children often develop more spoken language when they have AAC. The bridge helps build the destination.
PMC11506176
PMC10955541
ASHA AAC Practice Portal
CDC 2023

This Is a Wiring Difference. Not a Will Difference.
The Neuroscience
In children with complex communication needs, the neural pathways connecting Broca's area (speech production) and Wernicke's area (language comprehension) show differences in connectivity. The child's receptive language — understanding — often develops normally. It is the expressive output pathway that faces barriers: motor planning challenges, neural connectivity variation, or processing differences.
What This Means for Your Child
Your child's thinking is intact. Their understanding is intact. The problem is not intelligence — it is the output channel. Their thoughts are fully formed. The path from thought to spoken word is blocked, detoured, or inconsistent.
AAC provides an alternate output channel: symbols, pictures, devices. When you give them AAC, you are not replacing their voice — you are giving them a second route to the same destination.
"This is a wiring difference, not a word shortage." — Romski & Sevcik: AAC does not inhibit speech development; it supports it.

Where Your Child Is on the Communication Journey
There is no "too early" for AAC. There is no prerequisite score to qualify. The only question is: does your child need more communication tools than speech alone provides? If yes — AAC begins today.
1
12–18 Months
First words, pointing, gestures
2
18–24 Months
50 words + word combinations
3
2–3 Years
2-word phrases, questions
4
3–5 Years
Sentences, storytelling
5
5+ Years
Full conversation, dialogue
↑ Your child may be anywhere here — and AAC meets them exactly where they are. AAC is relevant across: Autism Spectrum Disorder | Cerebral Palsy | Apraxia of Speech | Intellectual Disability | Down Syndrome | Rare Genetic Syndromes | Traumatic Brain Injury
PMC9978394
WHO/UNICEF CCD Package (2023)
WHO NCF 2018

Clinically Validated. Home-Applicable. Life-Changing.
⭐⭐⭐⭐ Level I Evidence
Systematic Review + Multiple RCTs
Source | Finding | |
ASHA AAC Practice Portal (2024) | AAC is evidence-based for children who cannot rely on speech alone across all ages and diagnoses | |
Romski & Sevcik (multiple RCTs) | Children using AAC develop significantly more spoken words than matched controls without AAC | |
NCAEP Evidence-Based Practices (2020) | Aided language stimulation classified as evidence-based practice for autism | |
Pinnacle Network: 20M+ Sessions | 92% improvement in Expressive Communication Readiness Index with structured AAC implementation | |
WHO NCF (2018) | Communication-access interventions reduce behavioral challenges by addressing unmet communication needs |
❌ Myth
"AAC will stop my child from talking."
✅ Truth
FALSE. Decades of research show the opposite — AAC supports and often accelerates speech emergence.
❌ Myth
"My child isn't ready for AAC."
✅ Truth
FALSE. There are no prerequisites. Communication is a right, not a reward.
📞 FREE: 9100 181 181 | PMC11506176 | PMC10955541 | NCAEP 2020 | ASHA Practice Portal | WHO NCF 2018

AAC Introduction — Building Your Child's First Voice System
AAC (Augmentative and Alternative Communication) refers to every form of communication other than spoken words: symbols, pictures, devices, sign language, communication boards, apps. "Augmentative" means supplementing existing speech. "Alternative" means replacing speech for those who cannot use it.
Getting started with AAC is the foundational phase — selecting the right tools, setting them up, and beginning the consistent modeling process that teaches your child that symbols can carry their thoughts into the world. This is not a last resort. This is the first response to communication need.
Domain
B: Social Communication
Ages
2–18+
Duration
Ongoing
Frequency
All waking hours
Lead
Speech-Language Pathologist
Formal Clinical Term: Aided Augmentative and Alternative Communication Implementation — Introductory Phase

The Consortium of Experts Behind Every AAC Implementation
AAC success crosses therapy boundaries because the brain doesn't organize by therapy type. Communication is everyone's job — and it takes a team to build a bridge that lasts.
Speech-Language Pathologist (LEAD)
Conducts AAC evaluation; selects vocabulary; designs symbol layout; implements aided language stimulation; tracks Expressive Communication Readiness Index.
Occupational Therapist
Assesses motor access; recommends mounting solutions, keyguards, and styluses for children with physical interaction challenges.
BCBA / ABA Therapist
Builds motivation to communicate; uses reinforcement to establish AAC as functional communication; reduces problem behavior from communication frustration.
Special Educator
Integrates AAC into classroom vocabulary and academic activities; coordinates school-based implementation; trains paraprofessionals.
Family / Caregivers (ESSENTIAL)
The most important AAC partners. Model AAC at home. Create communication opportunities. Ensure AAC is available everywhere. Their commitment determines outcomes.
WHO/UNICEF Nurturing Care Framework
ASHA AAC Practice Portal

What AAC Unlocks — Layer by Layer
AAC does not target communication in isolation — it opens a cascade of developmental outcomes that span behavior, social connection, academics, and long-term independence.
1
🎯 Primary
Functional expressive communication — conveying wants, needs, thoughts, feelings reliably
2
Secondary
Reduced behavioral challenges, social connection, academic participation, autonomy
3
Long-Term
Spoken language emergence, literacy development, quality of life, independent living readiness
Observable Indicators — What Progress Looks Like
✅ Child approaches AAC device when they want something
✅ Child selects symbols to communicate (not just to press buttons)
✅ Meltdowns decrease as communication succeeds
✅ Child attempts to show caregivers symbols — initiating, not just responding
✅ Spoken words increase alongside AAC use
PMC10955541
NCAEP 2020
ASHA AAC Practice Portal

Your AAC Starting Toolkit — 9 Materials, One Goal: A Voice for Your Child
These 9 materials form the evidence-based starter ecosystem for AAC. You don't need all 9 immediately. Start with core word boards and modeling materials — they cost almost nothing. Build from there.
# | Material | Price Range | First Step? | |
1 | Core Word Communication Boards | ₹200–1,500 (or FREE) | ✅ Start here | |
2 | AAC Apps on Tablets | ₹3,000–25,000 | ✅ Start here | |
3 | Symbol Cards & PECS Starter Kits | ₹500–5,000 | ✅ Start here | |
4 | Aided Language Stimulation Materials | ₹200–2,000 | ✅ Essential | |
5 | Low-Tech Communication Books | ₹500–3,000 | 🔜 Within first month | |
6 | Visual Scene Displays | ₹200–1,500 | 🔜 Within first month | |
7 | Choice Boards for Everyday Routines | ₹100–500 | ✅ Start here | |
8 | Access Solutions & Mounting Equipment | ₹500–20,000+ | ⚙️ OT evaluation needed | |
9 | Family Training & Coaching Resources | ₹500–10,000 | ✅ Start NOW |
Zero-Cost AAC Start: Print a free core word board (PrAACtical AAC / AssistiveWare free downloads) + commit to modeling while you talk. This costs ₹0 and begins immediately.

Every Child Deserves a Voice — Regardless of Budget
The WHO/UNICEF equity principle in action: no family should be locked out of AAC by cost. Every material in this toolkit has a zero-cost version. Free materials can start the journey — no child should wait for a purchased system before receiving their first words.
Commercial Option | DIY / Free Alternative | |
Printed/laminated core word board kit (₹200–1,500) | Download free from PrAACtical AAC, AssistiveWare, or ARASAAC. Print at any print shop. Laminate at home with plastic sleeves. | |
AAC app (₹3,000–25,000) | Free apps: LetMeTalk (Android), Cboard (web-based), AAC Speech Buddy. Functional for starting — upgrade to robust app when possible. | |
PECS starter kit (₹500–5,000) | Print symbols from ARASAAC (free, open-source). Laminate, add Velcro. Create exchange system with a binder and sentence strip. | |
Modeling boards (₹200–2,000) | Print duplicate boards (same as child's board). One for child, one for adult to model with. Free. | |
Communication book (₹500–3,000) | Download PODD templates (some free). Print in A4, laminate, bind in a ring binder with divider tabs. Total cost: under ₹500. | |
Visual scene displays (₹200–1,500) | Take photos of child's actual spaces. Print A4, add sticky labels with symbol names. Free. | |
Choice boards (₹100–500) | Take photos of actual food/toys from home. Print 2x2 grid, laminate. ~₹50. |
"Free materials can start the journey. No child should wait for a purchased system before receiving their first words." — Pinnacle Blooms SLP Consortium
PMC9978394
WHO NCF 2018
WHO/UNICEF CCD Package

Before You Begin — What Every Family Must Know
🔴 STOP — Do Not Proceed Without This
AAC is NOT optional. AAC is the child's voice. Never withhold AAC as punishment. Never restrict AAC access "until they try speaking first." Never remove the device because it's inconvenient. Restricting a child's AAC is restricting their fundamental right to communicate.
🟡 Proceed With Awareness
PECS implementation should follow its established phase protocol. Access solutions for children with motor challenges require OT evaluation. AAC apps chosen without SLP input may not have appropriate vocabulary organization. Vocabulary must include words for reporting pain, illness, and problems — never limit to "positive" words only.
🟢 You Are Ready When
You have at least one communication tool (even a printed board). You understand the modeling principle: point to symbols while you talk. You have committed to keeping AAC available everywhere, always. You have connected with an SLP. You have accepted: AAC does not stop speech. It opens everything.
Clinical Safety Note: For children with significant motor access needs (inability to reliably touch a standard touchscreen), do not delay — contact an OT for access assessment immediately.
📞 9100 181 181 — FREE AAC guidance in 16+ languages
📞 9100 181 181 — FREE AAC guidance in 16+ languages
ASHA AAC Scope of Practice

The AAC Environment — Making Communication Happen Everywhere
AAC is not a therapy-room tool. It lives in every space your child inhabits — and consistency across environments is what builds real communication. Here is how to set up every room.
Living Room
Core word board on a low shelf, at child's eye and reach level. Always accessible, never locked away.
Kitchen
Meal choice board on the fridge at eye level. Visual meal symbols help during the highest-motivation communication moment: food.
Child's Room
Bedtime visual board on the bedside table, accessible from bed. Routine predictability supports communication during transitions.
School Bag
Laminated backup board for outings — waterproof and always with the child, regardless of where the day goes.
Tablet / Device
AAC app in a protective case, always charged. Charge every night at the same time — like a phone. Never during peak communication times.
"We're going to put your board here — see? Right at your height. So whenever you want to say something, it's here. And I'll use mine to show you how the words work."

60-Second Pre-Session Check — Before Every AAC Practice Session
The best AAC session is one that starts right. A 5-minute window of readiness is worth more than 30 minutes of struggle. Run through this quick check before every session.
✅ Is your child fed and not hungry? (Hunger creates dysregulation that blocks learning)
✅ Is your child rested? (Within 2 hours of nap/sleep is often too tired)
✅ Is your child in a calm, alert state? (Not already escalated or overwhelmed)
✅ Has your child not had a meltdown in the last 30 minutes?
✅ Is the environment relatively calm? (No high-sensory stimulation competing)
✅ Are YOU as the parent calm and available? (Your regulation affects theirs)
✅ Is the AAC material charged and accessible?
🟢 6–7 YES = GO
Begin modeling session. This is an optimal window.
🟡 4–5 YES = MODIFY
Simplify the session. Use the AAC board during a preferred activity only.
🔴 3 or fewer YES = POSTPONE
Today's best AAC practice is a calm, connected moment — not a formal session. Try again in 30–60 minutes.

Step 1 of 6
The Invitation — Making AAC the Natural Start to Communication
Begin every AAC interaction by making communication irresistible, not mandatory. Create an opportunity where your child has a genuine reason to communicate — motivation is the foundation of every AAC breakthrough.
What To Do
Hold up a preferred snack: "What do you want?" (while touching "want" on your board). Open their favorite app but pause: "What next?" (while touching "more"). Set up a favorite activity incompletely — leave out a piece, then wait expectantly.
What To Say
Keep language simple, purposeful, and modeled on the AAC: "What do you want?" [touch WANT] "More?" [touch MORE] "Help?" [touch HELP]
Timing & Waiting
Wait 5–10 seconds after creating the opportunity before prompting. This processing time is not silence to fill — it is the child's brain forming a response. Count silently.
What NOT To Do
Don't demand: "Use your words — point to what you want." Don't pre-empt: give the answer before they have time to attempt. Don't flood: too many words confuse the communication opportunity.
ABA Motivation Principle: Communication is taught most effectively when the child has genuine motivation to communicate. Creating want is the first step.

Step 2 of 6
Engagement — Capturing Attention Before Teaching Language
A child cannot learn AAC when dysregulated, distracted, or disinterested. Engagement means the child's attention is on you, the AAC, and the communication opportunity — without force.
01
Follow Their Lead
Begin with whatever is capturing the child's interest — the preferred toy, activity, or routine. Bring AAC into that context, not the other way around.
02
Face-to-Face Positioning
Get at the child's eye level. Reduce distance. This is not about demanding eye contact — it is about being within the child's natural attention field.
03
Joint Attention
Both of you attending to the same thing — the AAC board, the desired object, the activity. The shared focus creates the communication context.
04
Match Their Energy
If the child is excited, bring enthusiasm. If they are calm, be calm. Emotional congruence opens communication channels.
Engagement Indicators — Your Child Is Ready
- They look toward you, the board, or the desired item
- They move toward the AAC or reach toward it
- They pause their current activity with a glance toward you
- They make any attempt at vocalization or gesture
NCAEP 2020 — Joint attention interventions: evidence-based for autism

Step 3 of 6 — The Core Technique
Aided Language Stimulation — The Single Most Powerful Thing You Can Do for AAC
While you talk to your child — touch the symbols on their AAC board that match your key words.
"Do you WANT [touch WANT] more DRINK [touch DRINK]?"
"Time to GO [touch GO] — we're going OUT [touch OUT]."
"That's FUNNY [touch FUNNY]! I LIKE [touch LIKE] this!"
Children learn spoken language by hearing thousands of words in context. AAC users learn symbol-language by seeing thousands of modeled messages in context. You are being their language model — in their modality. This is the most evidence-based, most powerful, and most freely available AAC intervention that exists.
Execution Checklist
- Have your modeling board / duplicate board accessible
- Touch words as you say them — not after
- Use a calm, natural pace — not slow and clinical
- Model frequently — aim for 50+ models per day across all routines
- Don't require the child to touch anything yet — input precedes output
NCAEP 2020
Romski & Sevcik Research
ASHA AAC Practice Portal

Step 4 of 6
Repetition Is How Language Becomes Automatic
Unlike many therapies where you count "reps per session," AAC modeling has no ceiling. The principle is: model constantly, across every routine, throughout the entire day. This is not formal therapy — it is communication embedded in life.
Routine | AAC Modeling Opportunities | |
Breakfast | WANT / MORE / DONE / LIKE / NOT LIKE / ALL DONE | |
Getting Dressed | HELP / GO / WAIT / STOP / THIS | |
Play Time | WANT / THAT / MORE / GO / STOP / FUNNY / LIKE | |
Bath Time | WATER / DONE / MORE / HELP / HOT / COLD | |
Bedtime | WANT / BOOK / SONG / MORE / DONE / TIRED |
Total daily models target: 50–100+ touchpoints across routines. Model the same word in different routines ("MORE juice", "MORE puzzle", "MORE tickles"). Vary who is modeling — both parents, grandparents, siblings. Vary the AAC tool for generalization.
"3 excellent models are worth more than 30 ignored ones." — When the child disengages, shift routines or activities. Quality models always beat quantity forced.
PMC11506176
Aided Language Stimulation Dosage Research

Step 5 of 6
Celebrate Every Attempt — Communication Is Winning
Every time a child uses AAC — any use: touching a symbol, looking at the board, reaching toward it — that attempt must be immediately reinforced with a natural response. The reinforcer is not a sticker. It is getting what they communicated for.
When your child touches "WANT COOKIE" on their board — give the cookie. Immediately. With enthusiasm. Without demands. Without "say it with your mouth too." The communication worked. That is everything.
"WANT COOKIE! You told me! Here you go!" [give cookie immediately]
"MORE! Yes — more! Here's more!" [extend the activity immediately]
"HELP! You asked for help! I'm coming!" [respond within 3 seconds]
Celebrate the attempt, not just perfection: A child who reaches toward the board — even without touching a symbol — is communicating intentionally. Honor it. Respond to it. Celebrate it.
📞 9100 181 181
📞 9100 181 181
BACB Guidelines
ABA Reinforcement Principles
NCAEP 2020

Step 6 of 6
Every Communication Session Ends Gently — Never Abruptly
Abrupt endings to engagement can dysregulate children who struggle with transitions. A gentle, predictable close prevents post-session frustration and sets up the next session for success. Children who trust the ending are more willing to begin again.
01
Step A — Warning (2 Minutes Before Ending)
"Two more times, then all done." [touch TWO + MORE + ALL DONE on board] Show a visual timer if available (or count on fingers).
02
Step B — Signal (When Ending)
"All done!" [touch ALL DONE on board] Acknowledge the session warmly: "You did great telling me what you wanted. Your board helped."
03
Step C — Transition (Next Activity)
"Now we're going to..." [touch GO + NEXT on board] Bridge to the next preferred activity — not a demand, an invitation.
If Child Resists Ending: Honor the communication. If they grab the board or the tablet, that IS communication. Respond: "You want MORE? Okay — two more, then all done." Involve the child in putting the board in its "home" spot — this builds ownership and routine.
NCAEP 2020
Visual Timer Evidence
Transition Support for Autism

60 Seconds of Data Now = Months of Progress Clarity
Data is not about proving your child is learning fast enough. It is about seeing the journey clearly — and adjusting the path when the data says to. Record within 5 minutes of every session.
Field | What to Capture | Example | |
Date & Time | When the session occurred | March 10, 2026, 7:30am (breakfast) | |
AAC Attempts | How many times child touched/pointed to board | 3 times | |
Independent vs Prompted | Were they independent or did you prompt? | 2 independent, 1 prompted | |
Response Quality | What symbols? Any novel combinations? | WANT + MILK (new combination!) | |
Your Modeling Count | Rough count of your models | ~15 models during breakfast | |
Child Affect | Was child calm, engaged, distressed? | Calm and interested |
📋 Google Form Tracker
GPT-OS® Daily AAC Session Tracker — B-220
techniques.pinnacleblooms.org/tracker/aac-daily-b220
techniques.pinnacleblooms.org/tracker/aac-daily-b220
📱 GPT-OS® In-App
Expressive Communication Readiness Index → AAC Competency Index → Daily Session Log
📥 PDF Download
B-220 AAC Session Tracking Sheet — 4 weeks
techniques.pinnacleblooms.org/b220-tracker
techniques.pinnacleblooms.org/b220-tracker
BACB Data Collection Standards
Cooper, Heron & Heward Applied Behavior Analysis
📞 9100 181 181

Sessions Don't Always Go Perfectly. That's Not Failure. That's Data.
Every difficult session is information. Understanding why something didn't work is how you refine your approach — and how your child eventually breaks through.
❓ "My child completely ignores the board/device."
Why: AAC is new. Ignoring is normal for the first weeks/months. The child needs to see many models before attempting use.
Fix: Keep modeling. Don't require touching. Wait. Model during preferred activities only for now.
Fix: Keep modeling. Don't require touching. Wait. Model during preferred activities only for now.
❓ "My child hits the board away or throws the tablet."
Why: Possibly overwhelmed, or the session started when they weren't in a ready state.
Fix: Check the readiness gate (Card 13). Reduce pressure. Try a choice board instead — lower stakes.
Fix: Check the readiness gate (Card 13). Reduce pressure. Try a choice board instead — lower stakes.
❓ "My child only touches one symbol repeatedly (e.g., always 'MORE')."
Why: 'MORE' is powerful — it works. They're using what works.
Fix: Celebrate it! Then begin expanding: model 'MORE WHAT?' and touch MORE + MILK, MORE + PLAY.
Fix: Celebrate it! Then begin expanding: model 'MORE WHAT?' and touch MORE + MILK, MORE + PLAY.
❓ "My child used to use the board and now has stopped."
Why: Regression is normal. Check: Is the board accessible? Has routine changed? Is child unwell?
Fix: Reduce demands, increase modeling, return to highly motivating contexts.
Fix: Reduce demands, increase modeling, return to highly motivating contexts.
❓ "I'm not consistent — I forget to model."
Why: Modeling is a new habit for YOU, not just a new skill for your child.
Fix: Post a reminder on the fridge. Set a phone alarm for mealtimes. One modeling-rich routine per day beats zero perfect days.
Fix: Post a reminder on the fridge. Set a phone alarm for mealtimes. One modeling-rich routine per day beats zero perfect days.
❓ "My child is becoming frustrated during AAC time."
Fix: Stop. Breathe. This session ends now. Resume when regulated. Never push through a dysregulated AAC session.
"Session abandonment is not failure. It is data that says: try again when we're both ready."

No Two Children Are Identical. Adapt AAC to Yours.
AAC is not one-size-fits-all. Adapting the system to your child's unique profile — motor needs, sensory sensitivities, learning style, and age — is what makes the difference between a tool that sits on a shelf and one that changes a life.
1
Easier Version
2-choice boards only | Photo-based (real images) | 1 board per context | Partner-assisted always
2
Standard
Core word board (8–12 symbols) | Symbol-based (line drawings) | Multiple boards by room | Partially prompted
3
More Advanced
Full PODD or robust AAC app | Text-supplemented symbols | Single dynamic display device | Increasingly independent
🔴 Motor Challenges
OT assessment for access solutions first. Keyguards, mounts, or switch access before vocabulary decisions.
🟡 Sensory Sensitivities
Reduce AAC session length. Try during proprioceptive-calming activities (swinging, heavy work) — regulation helps language.
🟢 Visual Learners
Visual scene displays first (photos of real environments) — more intuitive than abstract symbols for many children.
🔵 Strong Memorizers
Begin with LAMP Words for Life (motor planning approach) — consistent motor patterns build quickly and generalize well.
ASHA AAC Practice Portal
Clinical Practice Guidelines SLP/OT/ABA

Week 1–2: The Input Phase
Progress: 15%
In weeks 1–2, your job is not to teach. Your job is to model. Model and wait. Model and wait. The brain is absorbing everything even when you cannot see it working.
✅ These Are Success Signs
- Child allows AAC to be present without pushing it away
- Child watches when you model on the board
- Child looks toward the board when communication is happening
- ONE independent touch on a symbol — even accidental — is a WIN
- Meltdown during communication is 3 seconds shorter than last week
❌ Not Expected Yet (And That's Fine)
- Independent, spontaneous symbol selection — comes in weeks 4–8
- Consistent daily AAC use — builds over months
- Two-symbol combinations — comes after single symbols are established
A child who allows the board to exist in their environment and occasionally looks at it after 2 weeks of modeling: this is 100% on track.
PMC11506176
Early AAC Implementation Research

Week 3–4: The Consolidation Phase
Progress: 40%
The synaptic pathways between symbol recognition and intentional selection are beginning to strengthen. This is neural pathway formation made visible through behavior — and it is one of the most exciting phases in an AAC journey.
✅ Child approaches the AAC board when they want something — they know it's there
✅ Child touches a symbol with intent (not just randomly pressing)
✅Specific symbol selections — WANT for wanting, DONE for finishing
✅ A reduction in frustrated behaviors at moments when AAC is available
✅ Child beginning to bring the tablet to you — initiating communication
✅ First novel combination (e.g., MORE + MILK when they've only practiced MORE before)
When to Expand: If your child is consistently selecting 3–4 symbols independently → it's time to increase vocabulary. Add symbols that open new contexts.
"You may notice you're more confident too. You've started to hear your child's communication attempts that you may have missed before."
"You may notice you're more confident too. You've started to hear your child's communication attempts that you may have missed before."
Neuroplasticity + AAC Development Research
PMC11506176

Week 5–8: The Mastery Phase — AAC Becomes Your Child's Language
Progress: 65%
✅ Consistent daily spontaneous AAC use across at least 3 different routines
✅ Two-symbol combinations emerging (WANT + SNACK, GO + OUTSIDE, HELP + ME)
✅ AAC used to comment (not just request) — FUNNY, LIKE, NO LIKE
✅ Child frustrated when AAC is inaccessible — they rely on it now
✅ Family members other than primary caregiver can understand child via AAC
✅Spoken words may begin to emerge or increase alongside AAC use
Session Frequency
2–3 structured modeling sessions per week + continuous incidental AAC throughout all daily routines. Sessions now 10–20 minutes.
AAC Competency Target
Pre-intentional → Emerging Intentional ✅ → Consistent Core Vocabulary (target this stage)
PMC11506176
AAC Dosage Research
ASHA Data

Every Symbol Is a Sentence. Every Touch Is a Victory.
In typical language development, we celebrate every word a child says. We video it. We call the grandparents. We screenshot it and share it. AAC milestones deserve the same celebration. These moments are just as real, just as meaningful, just as worth honoring.
First Independent Symbol Touch
Even if prompted 95% of the time — this is intentional communication.
First Unprompted Approach
They know communication lives in the board. That understanding is everything.
First Two-Symbol Combination
This is grammar. This is a sentence. This is your child writing their first story.
First Communication Outside Trained Routines
Generalization — the AAC is truly theirs now.
First Refusal with AAC
NO / STOP / NOT THAT — self-advocacy is born. Celebrate this loudly.
First Spoken Word After AAC Begins
The bridge is working. Both routes to communication are opening.
"Your child just said something. It may not have been spoken aloud. But a symbol was chosen, a message was sent, and you understood. That is communication. That is connection. That is everything."
When to Contact Your SLP or the Pinnacle Helpline — Now, Not Later
🚨 Contact Your SLP or Call 9100 181 181 If:
- Child shows regression — was using symbols, now completely stopped (especially if sudden)
- Child appears frustrated or distressed every time AAC is introduced, even after weeks of gentle exposure
- Child has not shown any orientation toward the AAC after 4 weeks of consistent modeling
- Child is unable to access the AAC physically — motor access needs assessment
- Child's speech has regressed alongside communication challenges (rule out medical causes)
- AAC is being refused by school or other caregivers — this is an advocacy situation requiring professional support
- You are questioning whether AAC is right — this uncertainty deserves professional guidance
✅ NOT a Red Flag — Normal AAC Development
- Slow to start using independently (normal — months of input precede output)
- Inconsistent use day to day (normal — all communication is inconsistent early)
- Preferring one symbol repeatedly (normal — generalize from there)
- Not combining symbols yet after 4 weeks (normal — single symbols first)
📞FREE: 9100 181 181 (24x7, 16+ languages) | ✉️ care@pinnacleblooms.org
Where This Fits in Your Child's Communication Journey
B-220 is not the beginning of the story, and it is not the end. It is the foundational bridge — the moment when communication possibility becomes communication reality. Here is where you stand, and where the path leads.
1
B-218
Limited Vocabulary for Communication
2
B-219
Receptive But Not Expressive Language
3
B-220 ← YOU ARE HERE
Getting Started with AAC
4
B-221
Building Vocabulary on AAC
5
B-222
AAC in the Classroom
Next-Level Options (What Comes After)
- B-221: Building Vocabulary on AAC
- B-222: AAC in the Classroom
- B-223: AAC for Children with Motor Challenges
- B-225: AAC and Speech Development Together
Lateral Options (If Modification Needed)
- C-domain: Emotional Regulation techniques
- D-domain: Autism-specific communication techniques
"Your child is not done. They are on a journey — and AAC is the beginning of a long, rich communication life."
Explore Related Communication Techniques
Core word boards and modeling boards carry across all AAC techniques — the materials you've already gathered work for every technique below. You already have a head start.

B-218: Limited Vocabulary
🔵 Prerequisite — techniques.pinnacleblooms.org/social-communication

B-219: Receptive Not Expressive
🔵 Prerequisite — techniques.pinnacleblooms.org/social-communication

B-221: Building AAC Vocabulary
🟢 Next Step — techniques.pinnacleblooms.org/social-communication

B-222: AAC in Classroom
🟢 Next Step — techniques.pinnacleblooms.org/social-communication

B-223: AAC + Motor Challenges
⚙️ Specialist — techniques.pinnacleblooms.org/social-communication

B-225: AAC + Speech Together
🟢 Recommended — techniques.pinnacleblooms.org/social-communication

Communication Is One Domain. Your Child Is Twelve.
AAC success is amplified when other domains are addressed simultaneously. A child who is dysregulated (Domain C) will have more difficulty with AAC. A child with sensory challenges (Domain A) may need environmental modifications before AAC can be optimally used. GPT-OS® sees the whole child — not just the communication domain.
AbilityScore® Assessment
See your child's full developmental profile across all 12 domains → pinnacleblooms.org/ability-score
Request Assessment
Call 9100 181 181 to connect with a specialist who evaluates all 12 developmental domains together.
WHO NCF 2018
UNICEF 2025 Country Profiles
GPT-OS® Architecture
📞 9100 181 181

The First Symbol Was 'MORE' at Dinner. Everything Changed After That.
Arjun's Story — Before AAC
Arjun was 4 years old and had no reliable way to communicate. He would scream at mealtimes — not because he was misbehaving, but because we couldn't understand what he wanted. Fifteen-minute dinners became hour-long struggles. We dreaded them.
After 12 Weeks with AAC
Arjun now uses a core word board and a tablet app. He tells us WANT + DOSA every morning. He tells us DONE when he's finished. Last week he told his dad FUNNY during a cartoon. Not a request. Just a comment. Connection.
"AAC didn't stop him from talking. He says more words now than before. The board and the app opened something in him. He knew we finally understood." — Parent, Pinnacle Blooms Network, Hyderabad
Before AAC, our daughter's meltdowns lasted 45 minutes on average. After 8 weeks of modeling, her first independent symbol was HELP. Just HELP. She told us she needed help. The meltdown that day was 4 minutes. She had words. She used them.
"The most common thing parents report at the 8-week AAC review is not the symbols their child has learned. It is the reduction in behavioral distress. When communication works — behavior changes. Because behavior was communication all along." — Pinnacle SLP Consortium
Isolation Is the Enemy of AAC Success. Community Is the Fuel.
"I was trying to do AAC alone and failing. Then I found other parents who were 6 months ahead of me. They told me to just keep modeling. They told me it takes months. They told me their child barely touched the board for 8 weeks and then one day — words. I kept going because they kept going." — AAC Parent, Pinnacle Community
WhatsApp Group
AAC Families — Getting Started. Join: wa.me/919100181181 (message "AAC FAMILY" to be added)
Online Forum
pinnacleblooms.org/community/aac — share experiences, ask questions, find encouragement
Local Parent Meetups
Organized by Pinnacle centers in your city. Find your nearest center: pinnacleblooms.org/centers
Peer Mentoring
Connect with an experienced AAC family who is 6–12 months ahead of you. Request: care@pinnacleblooms.org
"Your experience will one day help another family. Consider sharing your journey." | 📞 9100 181 181
AAC Is a Team Sport. Here Is Your Team.
🗣️ Speech-Language Pathologist with AAC Expertise
An SLP with AAC specialization can conduct a formal AAC evaluation, recommend the appropriate system, guide vocabulary selection, and coach your family through implementation. This is not optional — it is the foundation of every successful AAC journey.
🖐️ Occupational Therapist
For children with motor access challenges, OT assessment for mounting, keyguards, or alternative access is essential before the child becomes frustrated with an inaccessible system.
Find Pinnacle Centers with AAC Specialists
70+ locations across India with verified AAC specialists. → pinnacleblooms.org/centers/aac
Teleconsultation Available
Can't reach a center? Book an online AAC consultation: → pinnacleblooms.org/teleconsult
FREE AAC Helpline
📞9100 181 181 — 24x7, 16+ languages. For: AAC starter guidance, system recommendations, center locations, family coaching.
CIN: U74999TG2016PTC113063
DPIIT: DIPP8651
MSME: TS20F0009606
Pinnacle Blooms Network® Verified AAC Specialists
The Evidence Behind AAC — For the Curious and the Skeptical
Every recommendation in this guide is grounded in peer-reviewed research. Here is the evidence hierarchy and the five foundational studies every family and therapist should know.
01
ASHA AAC Practice Portal (2024)
AAC is evidence-based for individuals who cannot rely on speech alone, regardless of age or diagnosis. asha.org/practice-portal/aac
02
Romski & Sevcik (2005, 2010)
Multiple RCTs: children using AAC develop more spoken words than matched controls. The speech myth is definitively busted. Journal of Speech, Language, and Hearing Research.
03
NCAEP Evidence-Based Practices (2020)
Aided language stimulation (modeling) classified as evidence-based practice for autism. ncaep.fpg.unc.edu
04
PMC11506176 — Systematic Review (2024)
AAC intervention outcomes across 8–12 week timelines, with communication competency gains documented in children.
05
WHO Nurturing Care Framework (2018)
Communication access interventions aligned with responsive caregiving — one of five core nurturing care components in 54 countries. nurturing-care.org/ncf-for-ecd
"All children deserve responsive caregiving — including children with complex communication needs." — WHO/UNICEF CCD Package (2023)
How GPT-OS® Turns Your Sessions Into a Personalized Pathway
Every session you record feeds a system that learns your child's patterns, anticipates their next steps, and surfaces the right recommendations at the right moment — so you are never navigating the AAC journey without a map.
AAC Competency Index
Pre-intentional → Emerging → Consistent → Expanding → Generative
Expressive Communication Readiness
Where your child stands vs developmental benchmarks
Communication Partner Readiness
How effectively family members are modeling
TherapeuticAI® Recommendations
When to expand vocabulary, add materials, or seek additional professional support
Privacy Assurance: Your child's data is governed under DPDP Act (India) + ISO/IEC 27001 standards. Data is used only to serve your child's therapy outcomes. It is never sold. Your anonymized aggregate data helps every child like yours.
pinnacleblooms.org/gpt-os | 📞 9100 181 181
pinnacleblooms.org/gpt-os | 📞 9100 181 181

Watch: 9 Materials That Help Getting Started with AAC
This page is the deep-dive companion to Reel B-220. Where the reel names the materials, this page shows you how to use them — step by step, with the evidence behind each.
▶ Reel B-220
"So much inside. No words to let it out. Here are 9 materials to build the bridge."
Runtime: ~75 seconds | Domain: B — Social Communication | Therapist: Pinnacle Blooms SLP Consortium
Runtime: ~75 seconds | Domain: B — Social Communication | Therapist: Pinnacle Blooms SLP Consortium
Related Reels — Watch Next
B-219
Child Has Receptive But Not Expressive Language
B-221
Building Vocabulary on AAC
B-222
AAC in the Classroom
🔔 Follow for more: youtube.com/pinnacleblooms | instagram.com/pinnacleblooms
NCAEP 2020 — Video modeling as evidence-based practice
NCAEP 2020 — Video modeling as evidence-based practice

If One Person Can't Implement AAC, It Doesn't Work. Everyone Needs to Know.
If only one parent models AAC, the child experiences inconsistency that slows learning. Both parents, grandparents, the babysitter, and the teacher need to understand the basics. Consistency across caregivers multiplies impact.

📥 Family AAC Starter Guide (1-page PDF)
What AAC is, the 3 things every family member must do (Model, Respond, Keep Available), the 1 thing they must never do (withhold access). Download: techniques.pinnacleblooms.org/b220-family-guide

🧓 "Explain to Grandparents" Simplified Version
"Arjun uses a picture board to tell us what he wants. When he points to a picture, give him what it shows and say the word. That's it. That's all you need to do."

📋 Teacher/School Communication Template
Download: B-220 School Communication Letter Template — for requesting AAC access, staff training, and IEP goals. techniques.pinnacleblooms.org/b220-school-letter
WhatsApp Family Summary: "We're starting AAC with [child's name]. Here's the guide: [link]. The key is: model with the board while you talk to them. Point to the pictures. That's the most important thing."
PMC9978394
WHO CCD Package Caregiver Training Evidence

The Questions Every AAC Family Asks
❓ Will AAC stop my child from learning to talk?
No. This is the most common fear and the most thoroughly researched question in AAC. Decades of research — including multiple RCTs — show children using AAC develop more spoken words than matched children without AAC. The bridge helps build the destination.
❓ How old does my child have to be to start AAC?
There is no minimum age. Children as young as 12–18 months can benefit from AAC introduction when speech is insufficient. Earlier is better. There is no age too young.
❓ What if my child has some speech? Do they still need AAC?
AAC is appropriate for any child whose speech is not reliably sufficient to meet their communication needs — whether they have no words, 5 words, or 50 words. "Augmentative" means supplementing existing speech, not replacing it.
❓ Which AAC system is best — board, app, device?
No single system is universally best. A speech-language pathologist with AAC expertise can evaluate your child's motor access, cognitive level, and communication needs. Call 9100 181 181 to connect with an SLP.
❓ My child's school says they're not ready for AAC. What do I do?
There are no prerequisites for AAC — this is a well-established clinical and legal principle. Ask the school to clarify their position in writing. Request an SLP AAC evaluation. Contact Pinnacle Helpline for advocacy support: 9100 181 181.
❓ How long before my child starts independently using AAC?
Typically 3–6 months of consistent daily modeling before consistent independent use emerges. Some children begin in weeks; others take longer. Consistent input for months before expecting output is normal.
❓ Can AAC be used with Indian languages?
Yes. Several AAC systems support Tamil, Telugu, Hindi, Kannada, Marathi, and more. Contact Pinnacle for language-specific recommendations: 9100 181 181.
❓ Is AAC expensive?
The most powerful AAC tool — modeling — costs nothing. Core word boards are free to print. More robust systems range from ₹3,000 (apps) upward. Start free, expand as needed.

Your Child's Voice Is Ready. Are You?
"You don't have to know everything about AAC to begin. You need one board, one commitment to model, and one belief: your child has something to say. AAC gives them the way to say it."
20M+
1:1 Sessions
Evidence-backed therapy sessions delivered
97%+
Measured Improvement
Families reporting measurable communication gains
70+
Centers
Across India with verified AAC specialists
70+
Countries
Pinnacle families served globally
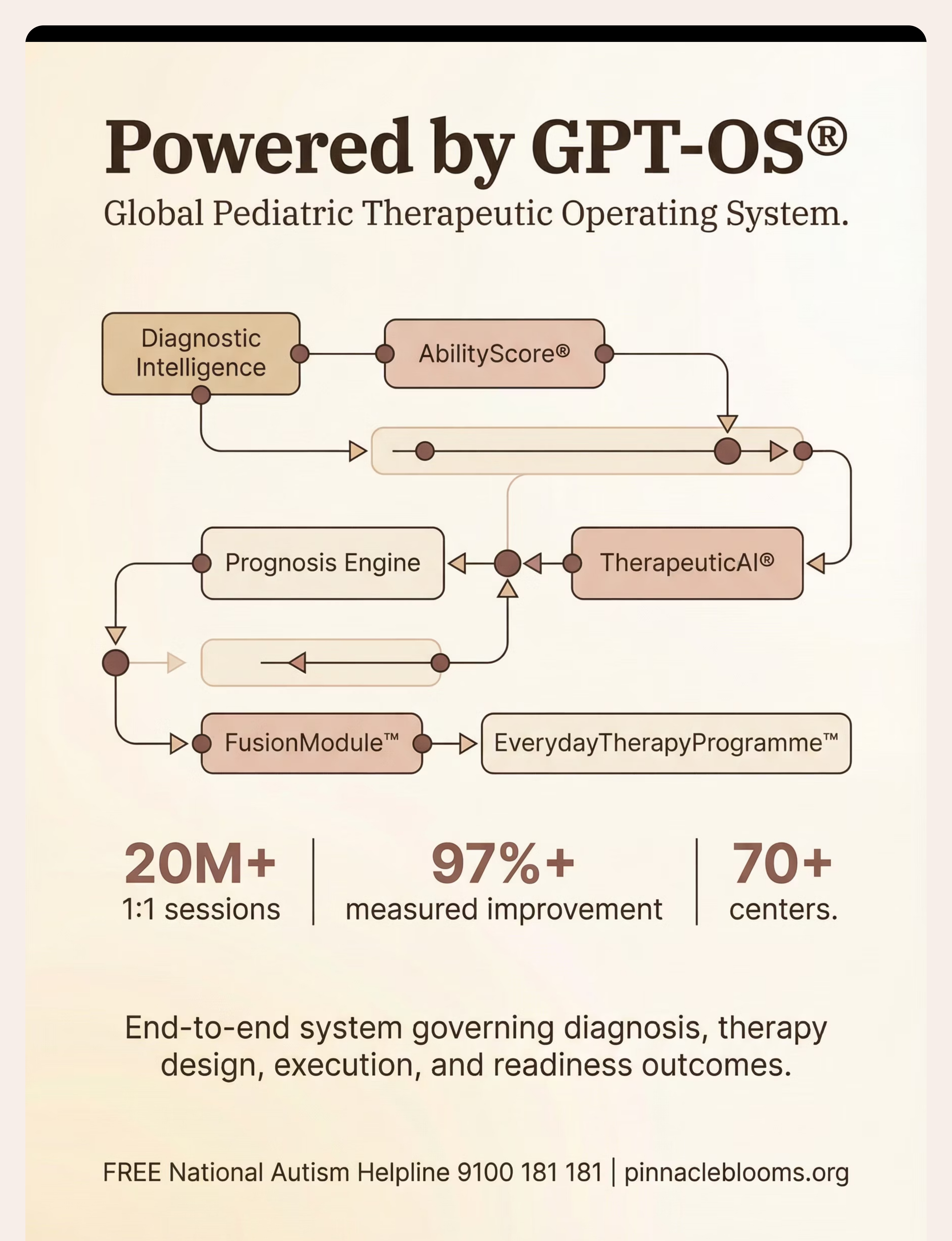
📞9100 181 181 — FREE | 24x7 | 16+ languages | Pinnacle Blooms Network® | GPT-OS® Powered
Preview of 9 materials that help getting started with aac Therapy Material
Below is a visual preview of 9 materials that help getting started with aac therapy material. The pages shown help educators, therapists, and caregivers understand the structure and content of the resource before use. Materials should be used under appropriate professional guidance.



















Share this resource
Help others discover thisLink copied!

The Pinnacle Promise — To Every Family, Every Child, Everywhere
"Every child communicates. Every child deserves the tools to make that communication heard. Pinnacle Blooms Network® commits to ensuring that no family navigates the AAC journey alone — with evidence, expertise, and community available to every parent in every language, across every center, every day." — Pinnacle Blooms Network® Consortium
Endorsed By
Pediatric SLPs | Pediatric OTs | BCBA/ABA Therapists | Special Educators | NeuroDevelopmental Pediatricians | Families | WHO/UNICEF Framework Alignment
→ Your Next Step: B-221
"Your child has started with AAC. Now let's build their vocabulary — beyond core words, into full expressive language." techniques.pinnacleblooms.org/social-communication/building-vocabulary-on-aac-b221
📞FREE National Autism Helpline: 9100 181 181 | 🌐 pinnacleblooms.org | ✉️ care@pinnacleblooms.org
© 2025 Pinnacle Blooms Network®, unit of Bharath Healthcare Laboratories Pvt. Ltd. CIN: U74999TG2016PTC113063 | DPIIT: DIPP8651 | MSME: TS20F0009606 | GSTIN: 36AAGCB9722P1Z2. All rights reserved. GPT-OS® is a registered trademark.
Educational Disclaimer: This content is educational. It does not replace assessment by a licensed speech-language pathologist specializing in AAC. AAC evaluation and implementation should be guided by professionals who can assess individual motor, cognitive, and communication needs. Individual results may vary. Statistics represent aggregate outcomes across the Pinnacle Blooms Network.
#AAC
#AugmentativeAlternativeCommunication
#GettingStartedWithAAC
#EveryoneDeservesAVoice
#AutismAAC
#CoreWords
#AACModeling
#PinnacleBlooms
